Quantitative studies of human urinary excretion of uropontin
|
|
|
- Norma Green
- 5 years ago
- Views:
Transcription
1 Kidney International, Vol. 53 (1998), pp Quantitative studies of human urinary excretion of uropontin WEI MIN, HIROSHI SHIRAGA, CHARLES CHALKO, STANLEY GOLDFARB, G.GOPAL KRISHNA, and JOHN R. HOYER Departments of Pediatrics and Medicine, University of Pennsylvania and the Children s Hospital of Philadelphia, Philadelphia, Pennsylvania, USA Quantitative studies of human urinary excretion of uropontin. Uropontin is the urinary form of osteopontin, an aspartic acid-rich phosphorylated glycoprotein. Uropontin has been previously shown to be a potent inhibitor of the nucleation, growth and aggregation of calcium oxalate crystals and the binding of these crystals to renal epithelial cells. Quantitative data defining the excretion of this protein are necessary to determine its role in urinary stone formation. In the present studies, we determined uropontin excretion rates of normal humans. Urine samples were obtained under conditions of known dietary intake from young adult human volunteers with no history, radiographic or laboratory evidence of renal disease. Urinary concentrations of uropontin were measured by a sensitive ELISA employing an affinity purified polyclonal antiserum to uropontin. Thirteen normal subjects ingested a constant diet providing 1 gram of calcium, 1 gram of phosphorus, 150 meq of sodium and 1 gram of protein per kilogram of body wt per day during an eight day study period. The relationship of urinary volume to uropontin excretion was assessed by varying fluid intake on the last four days of the study to change the mean urine volume/24 hr by 500 ml. Urine collected in six hour aliquots for eight days was analyzed for uropontin by ELISA, and for calcium, and creatinine. Daily uropontin excretion of 13 individual subjects was g/24 hr (mean 1 SD). The mean urinary levels (1.9 g/ml) detected in the present study are sufficient for inhibition of crystallization; our previous studies have demonstrated that the nucleation, growth and aggregation of calcium oxalate crystals and their binding to renal cells in vitro are inhibited by this concentration of purified uropontin. In contrast to the regular pattern of diurnal variation of calcium excretion seen in most subjects, uropontin excretion showed no regularity of diurnal variation and was not directly related to either calcium or creatinine excretion or changes in urinary volume. However, uropontin concentration varied inversely with urine volume (P 0.001), so that the highest uropontin concentrations occurred when urine volume was the lowest. We conclude that the physiologic characteristic of an inverse relationship of uropontin concentration to urine volume favors protection from urinary crystallization of calcium oxalate by uropontin. Our quantitative definition of urinary uropontin excretion of normal adults provides the basis for the evaluation of uropontin excretion by individuals who have formed urinary stones. The majority of urinary stones are composed of calcium salts and the predominant constituent of most urinary calculi is calcium oxalate [1, 2]. Urine excreted by normal individuals, as well as stone-formers, is often supersaturated with respect to calcium Key words: uropontin, stone formation, glycoprotein, calcium oxalate crystals. Received for publication June 27, 1997 and in revised form August 20, 1997 Accepted for publication August 21, by the International Society of Nephrology oxalate. However, the complex process of stone formation is inhibited by substances in urine that raise the concentrations of calcium and oxalate that are required for new crystal formation, growth and aggregation and inhibit adhesion of crystals to renal epithelial cells [2 5]. Although small molecules, such as magnesium, pyrophosphate and citrate have been shown to be inhibitory [6], the majority of the inhibition of calcium oxalate crystallization in urine appears to be provided by its protein constituents [2, 7]. A variety of inhibitory activities have been reported for several human urinary proteins, including nephrocalcin, Tamm-Horsfall protein and uropontin [5, 7 10]. At present, the relative contributions of these proteins to the inhibition of stone formation is not known. The urinary form of osteopontin (uropontin) was initially isolated by monoclonal antibody immunoaffinity purification from normal human urine as an inhibitor of calcium oxalate crystal growth [10]. Subsequently, this aspartic acid-rich phosphorylated glycoprotein was shown to also be a potent inhibitor of calcium oxalate nucleation, aggregation and binding to renal epithelial cells [5, 11]. Although the immunologic characteristics of osteopontin isolated from different tissues are not identical [12], the structural basis of these differences has not been defined and the terms, urinary osteopontin and its contraction, uropontin are used interchangeably. Studies of osteopontin secreted by mouse renal cells in culture have also demonstrated potent inhibition of calcium oxalate crystallization [13, 14]. Furthermore, uropontin is incorporated into calcium oxalate monohydrate stones [15 17]. Renal production of osteopontin has been well established by in situ hybridization, light and ultrastructural immunochemical localization in mouse, rat and human kidneys [18 21]. Osteopontin has been ultrastructurally localized to the cells of the descending thin limb of Henle s loop and papillary surface epithelium of normal rat and mouse kidneys. Localization in distal nephron segments (thick ascending limb and distal convoluted tubule) has been less consistently detected. The more focal distribution within the distal nephron may reflect mild subclinical tubular injury, since a marked up-regulation of osteopontin expression in the distal nephron is induced by several forms of renal injury [summarized in 20]. With respect to calcium oxalate stone disease, it is noteworthy that osteopontin expression was markedly increased in distal nephrons of rats given ethylene glycol to induce hyperoxaluria [22] and that osteopontin production of cultured primate renal epithelial cells is stimulated by exposure to calcium oxalate crystals [23]. Since quantitative information concerning normal rates of 189
2 190 Min et al: Quantitative studies of uropontin excretion uropontin excretion and effects of factors that influence its excretion is required to precisely define the role of uropontin in stone formation, a quantitative immunoassay for urinary uropontin was developed in our laboratory. In the present studies, this enzyme linked immunoassay (ELISA) employing affinity-purified polyclonal antibodies to uropontin was used to characterize normal urinary uropontin excretion. Urine samples from each of a group of normal adults were obtained during an eight day period under conditions of known dietary intake. The diurnal pattern of uropontin excretion was determined and relationships of uropontin excretion to urinary volume, calcium and creatinine excretion were analyzed. These studies provide the first quantitative data concerning normal patterns of urinary excretion of uropontin. They show that the quantities of uropontin excreted are sufficient to make an important contribution to the inhibition of calcium oxalate crystallization in normal urine. METHODS Subject selection Normal adult volunteers (aged 19 to 35 years old) were admitted to the General Clinical Research Center of the Hospital of the University of Pennsylvania. These individuals were free of a history of kidney stone disease or radiographic evidence of kidney stone disease. Serum calcium and creatinine and urinary calcium and creatinine excretion per 24 hours were measured prior to entry; individuals with abnormal values ( 300 mg calcium per 24 hr for men and 250 mg calcium per 24 hr for women; 4 mg calcium per kilogram body wt per 24 hr) were excluded from this study. The subjects ingested a defined diet containing 1 gram of calcium, 1 gram of phosphate, 150 meq of sodium and 1 gram of protein per kilogram of body wt per day throughout the study period. After a three day period of equilibration to this diet, a series of 32 consecutive six-hour collections of urine were obtained from each subject during a period of eight days. In order to evaluate the relationship of urinary volume to uropontin excretion, oral water intake on the last four days of the study was either increased or decreased on average by more than 500 ml/day in 11 of 13 subjects ( 1000 ml change in 9 subjects) from that ingested during the first four days. The total volume and concentrations of calcium, creatinine, sodium, potassium, phosphate and uropontin were determined using aliquots from each of the six hour collections. Sodium azide (0.02%) and two protease inhibitors, Phenyl methyl sulfonyl fluoride (PMSF; 0.5 mm; Sigma) and N-ethyl maleimide (NEM; 1.0 mm; Sigma) were added to urine samples that were kept at 4 C prior to assay for uropontin. The majority of samples were assayed within three weeks after collection and stability during more prolonged storage for this set of samples was demonstrated by repeating assays after longer intervals including those exceeding a year after initial assay. Immunoassay Our previously described enzyme-linked immunoassay (ELISA) for uropontin [10] was modified as follows to more optimally detect uropontin in urine samples. Protein solutions diluted with a 0.5 M ethylenediaminetetraacetic acid (EDTA) buffer, ph 9.3 were used to directly coat 96-well polyvinyl chloride microtiter plates (Dynatech) for 15 hours at 4 C. The washing buffer contained 0.01 M Tris, M NaCl, 5 mm CaCl 2, 0.05% Tween 20 at ph 7.6. The blocking buffer contained 8 mg/ml of bovine serum albumin (BSA) in the washing buffer. All immunoassays for uropontin were performed using a series of twofold dilutions of a single preparation of affinity purified uropontin on each plate as standards. Concentrations of uropontin in samples were calculated using the curve derived from the optical densities of the standards run on the same plate. Each sample was measured in triplicate at four dilutions with the initial dilution of urine being 1:80 or 1:100. If the mean optical densities of at least two dilutions of a urine did not fall within the linear portion of the standard curve for that plate, the assay for that sample was repeated using an appropriate series of dilutions. The primary antibody was an affinity-purified polyclonal rabbit anti-uropontin prepared in our laboratory as described below and the secondary antibody was an affinity purified peroxidase conjugated goat anti-rabbit IgG (Jackson ImmunoResearch, West Grove, PA, USA). Preparation of monospecific polyclonal antibodies to uropontin Polyclonal antibodies to uropontin was prepared by immunizing rabbits with uropontin isolated by immunoaffinity purification using monoclonal antibody ZH2 beads as previously described [10, 18]. After multiple exposures of this antiserum to a urinary protein fraction that had been coupled to Sepharose 4B beads, a monospecific anti-uropontin antiserum (pup-1) was obtained. The immobilized urinary protein fraction used for the affinity removal of antibodies with undesired specificities was a DEAEcellulose batch eluate [7] that had been previously depleted of uropontin by exposure to ZH2 beads. After affinity purification, pup-1 did not react with any other urinary proteins by ELISA or by Western blotting. All immunoassays were performed using dilutions of the same preparation of affinity purified uropontin on each plate as standards. Levels of sodium, potassium, phosphate, calcium and creatinine were determined by standard techniques [24]. All data were analyzed by using paired or unpaired t-tests and linear correlation using the Statworks program for the Macintosh computer. RESULTS Immunoassay The sensitivity of detection provided by several types of ELISAs employing polyclonal and/or monoclonal antibodies to uropontin was evaluated prior to adopting the assay for uropontin used in the present studies. Since calcium influences the conformation of osteopontin [12], EDTA was added to some coating buffers in preliminary studies to determine if the absence of calcium influenced uropontin coating. Concentrations of uropontin between 5 and 50 nanograms per ml were detected by the affinity purified antiserum, pup-1 in an ELISA employing microtiter plates directly coated with samples that had been diluted in an EDTA buffer. Direct comparisons showed that the ELISA using this polyclonal antiserum was roughly 10 times more sensitive than a comparable procedure employing monoclonal antibody ZH2. Undiluted urine inhibited detection of uropontin and this protein was less reliably detected if solutions containing low or no EDTA were used to coat microtiter plates. EDTA concentrations 0.1 M allowed better detection from solutions that contained other proteins; in the studies reported here, dilutions in 0.5 M EDTA,
3 Min et al: Quantitative studies of uropontin excretion 191 Fig. 1. Mean daily excretion of uropontin by 13 normal adult subjects during a period of eight days (, mean 1 SD); mean daily excretion by the group. ph 9.3 were used for all samples. The assay was validated in recovery studies in which purified uropontin was added to diluted urine samples. The recovery of uropontin added to 23 samples that had been sufficiently diluted ( 1:100) was %. Significantly less uropontin ( %) was recovered after an initial tenfold dilution of urine samples (P 0.003). The mean coefficient of variation for multiple determinations performed on 81 individual urine samples was 24.0%. Although the coefficient of variation was not linearly related to the concentration of uropontin in individual samples, variability was greatest at the lowest concentrations. More than 2/3 of the samples with uropontin concentrations of 1.0 g/ml had a coefficient of variation 50%, whereas only a sixth of the samples with 1.0 g/ml showed this extent of variability. Protein concentrations of the uropontin standard determined by the Lowry method and by quantitative aminoacid analysis after alkaline hydrolysis showed close agreement. By comparison, analysis using Coomassie Blue dye binding assay greatly underestimated uropontin concentrations. Rates of uropontin excretion The mean daily excretion of uropontin over the eight day period of collections for the group of 13 subjects was g/24 hr. Values for individual subjects (mean SD) ranged on individual days from 274 to 11,140 g (Fig. 1). When factored for body size, the mean rate of uropontin excretion was g/kg/24 hr. The rate of uropontin excretion by the 9 male subjects ( g/kg/24 hr) was not significantly higher than that of the female subjects ( g/kg/24 hr; P 0.397). Analysis of individual collection periods showed that the highest concentrations of uropontin were detected in the six hour collections with the lowest volumes (Fig. 2) and demonstrated that an inverse relationship between urine volume and uropontin concentration generally prevailed (r value 0.532). To explore this relationship, the average oral water intake of 11 subjects during the last four days of the study was changed by more than 500 ml/day from that during the first four days. Ten of these subjects showed a mean change in urinary volume/24 hours that exceeded 500 ml. The uropontin excretion of g/24 hr during the four days with lower urine volumes was not Fig. 2. Comparison of the uropontin concentration to the urinary volume in the six hour collections from each of the 13 normal subjects shown in Figure 1. The correlation coefficient for these 416 samples is (P 0.001). significantly greater than the excretion of g/24 hr during the four days that these 10 subjects had higher urine volumes (P 0.1 by paired t-test). The mean urinary volume in the 20 periods of four days for these 10 subjects was 1000 to 2000 ml/24 hr in nine periods, 2000 to 3000 ml in six periods, 3000 to 3600 ml in four periods, and 940 ml in one period. The mean urine volumes for the six periods of four days of the other three subjects ranged from 974 to 1602 ml. Further analysis of the relationship of uropontin excretion to urinary volume demonstrated no significant differences based on the volume of urine in the six hour collections. For example, the mean uropontin excretion in collections containing more than 750 ml was larger than the mean excretion in collections with a smaller volume in four of the subjects and was smaller in six subjects. The overall rate of uropontin excretion in collections 750 ml was g/6 hr, and in collections 750 ml was g/6 hr. Furthermore, analysis of individuals showed that mean uropontin excretion in collections 750 ml/6 hr was not significantly greater than mean level in the collections 750 ml/6 hr of the same subject (N 10, P by paired t-test). Overall, the mean urinary volume of the 13 subjects was ml/day. Thus, the mean concentration of uropontin was g/ml (57 nmol/liter based on the peptide molecular weight of 33,000). The majority of subjects showed a regular pattern of diurnal variation in calcium excretion (Fig. 3). In the seven subjects with an established rhythm, the lowest calcium excretion occurred during the first quadrant of the day (between 12 midnight and 6 a.m.) in 55 of the combined total of 56 days that they were studied. By contrast, the rate of uropontin excretion of these individuals showed less variability during the periods of the day and no regular diurnal variation (Fig. 3). For the entire group, the rate ranged from g/6 hr in the second quadrant to g/6 hr in the third quadrant. Thus, the highest ratio
4 192 Min et al: Quantitative studies of uropontin excretion Fig. 3. Excretion of calcium (F) and uropontin (E) in the series of 32 consecutive urine samples from one of the subjects. A regular pattern of diurnal variation is shown in which the lowest rate of calcium excretion is present during the six hour period between 12 midnight and 6 a.m. in each of the eight days of study. DISCUSSION Fig. 4. Comparison of the rates of uropontin excretion to calcium excretion per six hours in 416 urine collections showed no significant relationship. The regression line, y x had an r value of 0.1. of uropontin to calcium regularly occurred in the quadrant with the lowest calcium excretion. Overall, no significant relationship between uropontin and calcium excretion was seen in either the six hour collections (Fig. 4) or in excretion per 24 hours with the regression line, y x for the 104 total daily collections having an r value of only 0.2. Comparison of the rates of urinary uropontin excretion to creatinine excretion per 24 hours also showed no significant relationship. The r values for the linear regression line of 24 hour collections and six hour values were 0.2 and 0.3, respectively. The mean creatinine excretion for the 13 subjects was 19.9 mg of creatinine per kilogram body wt per 24 hours. The rate of creatinine excretion was highly reproducible with the average SEM for the 24 hour collections of individual subjects being 4.2% (range from 0.96 to 13.1%) of the mean creatinine excretion for that subject. There was no significant relationship in the rate of uropontin excretion to the excretion of sodium, potassium or phosphate. These studies demonstrate that the mean concentration of uropontin (1.914 g/ml, or 57 nm) that prevails in normal adult human urine exceeds levels that will substantially influence several aspects of calcium oxalate crystallization in vitro. A significant inverse relationship between uropontin concentration and urinary volumes was shown (Fig. 2) with high concentrations of uropontin being present when urinary volumes were low and contained higher concentrations of mineral constituents. The relationship of uropontin excretion to that of calcium was examined in detail, since hypercalciuria is a well known factor increasing the risk of stone formation. Since calcium excretion shows a diurnal pattern of variation, urine samples were collected at six hourly intervals. Whereas the majority of subjects showed a diurnal pattern of calcium excretion, there was no regular pattern of diurnal variation of uropontin excretion (Fig. 3). Thus, the highest ratios of uropontin to calcium were regularly observed between midnight and 6 a.m., when the rate of calcium excretion was lowest. The uropontin excretion was not significantly related to calcium excretion in six hour collections (Fig. 4) or per 24 hours. The concentrations of uropontin in normal urine over a period of eight days demonstrated in the present study exceeded the levels that substantially decrease calcium oxalate crystal growth and aggregation [11] and the binding of calcium oxalate crystals to renal epithelial cells [5]. By contrast, the 50% inhibition of calcium oxalate monohydrate (COM) nucleation using a seeded nucleation assay occurred at a concentration of uropontin (200 nm) that is roughly tenfold higher than the concentrations required for equivalent inhibition of crystal growth, aggregation or adherence to renal epithelial cells [5, 11]. These studies using a seeded nucleation assay suggest only a modest contribution of uropontin to nucleation inhibition. However, studies using an unseeded nucleation assay showed inhibition of nucleation at concentrations of mouse osteopontin as low as 10 nm [14]. These latter studies indicate a much greater capacity for inhibition of nucleation. In summary, the levels of uropontin prevailing in normal urine are sufficient to make a considerable contribution to the inhibition of calcium oxalate crystallization and thereby to be protective against the most common cause of urinary stone formation. Definition of the relative contributions of uropontin and other urinary protein inhibitors of crystallization and risk factors such as
5 Min et al: Quantitative studies of uropontin excretion 193 high urine calcium and/or oxalate and low urine citrate, their potential interactions and their precise roles in urinary stone formation provide important goals for future studies. ACKNOWLEDGMENTS This study was supported by grants from the National Institutes of Health (RO1 DK33501 and General Clinical Research Center MO1 RR 00040) and the DCI Research & Development Fund. Dr. Chalko was supported by NIH fellowship training grant 5T32DK Coleman Terrell provided technical assistance. Reprint requests to John R. Hoyer, M.D., The Children s Hospital of Philadelphia, 34th St. and Civic Center Blvd., Philadelphia, Pennsylvania , USA. hoyer@ .chop.edu APPENDIX Abbreviations used in this study are: ELISA, enzyme linked immunoassay; PMSF, phenyl methyl sulfonyl fluoride; NEM, N-ethyl maleimide; EDTA, ethylenediaminetetraacetic acid; BSA, bovine serum albumin; pup-1, monospecific anti-uropontin antiserum; COM, calcium oxalate monohydrate. REFERENCES 1. HERRING LC: Observations in the analysis of ten thousand urinary calculi. J Urol 88: , COE FL, PARKS JH, ASPLIN JR: The pathogenesis and treatment of kidney stones. N Engl J Med 327: , MEYER JL, SMITH LH: Growth of calcium oxalate crystals; II. Inhibition by natural urinary crystal growth inhibitors. Invest Urol 13:36 39, EDYVANE KA, HIBBERD CM, HARNETT RM, MARSHALL VR, RYALL RL: Macromolecules inhibit calcium oxalate crystal growth and aggregation in whole urine. Clin Chim Acta 167: , LIESKE JC, LEONARD R, TOBACK FG: Adhesion of calcium oxalate monohydrate crystals to renal epithelial cells is inhibited by specific anions. Am J Physiol 268:F604 F612, FLEISCH H: Inhibitors and promotors of stone formation. Kidney Int 13: , NAKAGAWA Y, ABRAM V, KEZDY FJ, KAISER ET, COE FL: Purification and characterization of the principal inhibitor of calcium oxalate monohydrate crystal growth in human urine. J Biol Chem 258: , ASPLIN J, DEGANELLO S, NAKAGAWA Y, COE FL: Evidence that nephrocalcin and urine inhibit nucleation of calcium oxalate monohydrate crystals. Am J Physiol 261:F824 F830, HESS B, NAKAGAWA Y, COE FL: Inhibition of calcium oxalate monohydrate crystal aggregation by urine proteins. Am J Physiol 257:F99 F106, SHIRAGA H, MIN W, VANDUSEN WJ, CLAYMAN MD, MINER D, TERRELL CH, SHERBOTIE JR, FOREMAN JW, PRZYSIECKI C, NEILSON EG, HOYER JR: Inhibition of calcium oxalate crystal growth in vitro by uropontin: Another member of the aspartic acid-rich protein superfamily. Proc Natl Acad Sci USA 89: , ASPLIN JR, ARSENAULT D, PARKS JH, COE FL, HOYER JR: Contribution of human uropontin to urine inhibition of calcium oxalate crystallization. Kidney Int 53: , HOYER JR, OTVOS L JR, URGE L: Osteopontin in urinary stone formation. Ann N Y Acad Sci 760: , WORCESTER EM, BLUMENTHAL SS, BESHENSKY A: The calcium oxalate crystal growth inhibitor protein produced by mouse kidney cortical cells in culture is osteopontin. J Bone Miner Res 7: , WORCESTER EM, BESHENSKY AM: Osteopontin inhibits nucleation of calcium oxalate crystals. Ann N Y Acad Sci 760: , HOYER JR, WIKOFF W, BOCK SC: Selective incorporation of uropontin into urinary calcium oxalate monohydrate stones. (abstract) JAm Soc Nephrol 3:684, KOHRI K, SUZUKI Y, YOSHIDA K, YAMAMOTO K, AMASAKI N, YAMATE T, UMEKAWA T, IGUCHI M, SINOHARA H, KURITA T: Molecular cloning and sequencing of cdna encoding urinary stone protein, which is identical to osteopontin. Biochem Biophys Res Comm 184: , MCKEE MD, NANCI A, KHAN SR: Ultrastructural immunodetection of osteopontin and osteocalcin as major matrix components of renal calculi. J Bone Miner Res 10: , LOPEZ CA, HOYER JR, WILSON PD, WATERHOUSE P, DENHARDT DT: Heterogeneity of osteopontin expression among nephrons in mouse kidneys and enhanced expression in sclerotic glomeruli. Lab Invest 69: , KLEINMAN JG, BESHENSKY A, WORCESTER EM, BROWN D: Expression of osteopontin, a urinary inhibitor of stone mineral crystal growth, in rat kidney. Kidney Int 47: , MADSEN KM, ZHANG L, SHAMAT A-RA, SIEGFRIED S, CHA J-H: Ultrastructural localization of osteopontin in the kidney: Induction by lipopolysaccharide. J Am Soc Nephrol 8: , BROWN LF, BERSE B, VANDEWATER L, PAPADOPOULOS-SERGIOU A, PERRUZZI CA, MANSEAU EJ, DVORAK HF, SENGER DR: Expression and distribution of osteopontin in human tissues; widespread association with luminal epithelial surfaces. Molec Biol Cell 3: , KOHRI K, NOMURA S, KITAMURA Y, NAGATA T, YOSHIOKA K, IGUCHI M, YAMATE T, UMEKAWA T, SUZUKI Y, SINOHARA H: Structure and expression of the mrna encoding urinary stone protein (osteopontin). J Biol Chem 268: , LIESKE JC, HAMMES MS, HOYER JR, TOBACK FG: Renal cell osteopontin production is stimulated by calcium oxalate monohydrate crystals. Kidney Int 51: , WASSERSTEIN A, STOLLEY P, GOLDFARB S, AGUS Z: Case control study of risk factors for nephrolithiasis. Miner Electrolyte Metab 13:85 95, 1987
Contribution of human uropontin to inhibition of calcium oxalate crystallization
 Kidney International, Vol. 53 (1998), pp. 194 199 Contribution of human uropontin to inhibition of calcium oxalate crystallization JOHN R. ASPLIN, DENISE ARSENAULT, JOAN H. PARKS, FREDRIC L. COE, and JOHN
Kidney International, Vol. 53 (1998), pp. 194 199 Contribution of human uropontin to inhibition of calcium oxalate crystallization JOHN R. ASPLIN, DENISE ARSENAULT, JOAN H. PARKS, FREDRIC L. COE, and JOHN
Control of calcium oxalate crystal structure and cell adherence by urinary macromolecules
 Kidney International, Vol. 53 (1998), pp. 952 957 Control of calcium oxalate crystal structure and cell adherence by urinary macromolecules JEFFREY A. WESSON, ELAINE M. WORCESTER, JOHN H. WIESSNER, NEIL
Kidney International, Vol. 53 (1998), pp. 952 957 Control of calcium oxalate crystal structure and cell adherence by urinary macromolecules JEFFREY A. WESSON, ELAINE M. WORCESTER, JOHN H. WIESSNER, NEIL
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
RISK FACTORS AND TREATMENT STRATEGIES FOR URINARY STONES Review of NASA s Evidence Reports on Human Health Risks
 Mayo Clinic O Brien Urology Research Center RISK FACTORS AND TREATMENT STRATEGIES FOR URINARY STONES 2017 Review of NASA s Evidence Reports on Human Health Risks John C Lieske, MD July 27, 2017 What types
Mayo Clinic O Brien Urology Research Center RISK FACTORS AND TREATMENT STRATEGIES FOR URINARY STONES 2017 Review of NASA s Evidence Reports on Human Health Risks John C Lieske, MD July 27, 2017 What types
Identification and qualitative Analysis. of Renal Calculi
 Identification and qualitative Analysis of Renal Calculi 1 -Renal Calculi: Kidney stones, renal calculi or renal lithiasis (stone formation) are small, hard deposits that form inside your kidneys. The
Identification and qualitative Analysis of Renal Calculi 1 -Renal Calculi: Kidney stones, renal calculi or renal lithiasis (stone formation) are small, hard deposits that form inside your kidneys. The
OxisResearch A Division of OXIS Health Products, Inc.
 OxisResearch A Division of OXIS Health Products, Inc. BIOXYTECH pl GPx Enzyme Immunoassay Assay for Human Plasma Glutathione Peroxidase For Research Use Only. Not For Use In Diagnostic Procedures. Catalog
OxisResearch A Division of OXIS Health Products, Inc. BIOXYTECH pl GPx Enzyme Immunoassay Assay for Human Plasma Glutathione Peroxidase For Research Use Only. Not For Use In Diagnostic Procedures. Catalog
Role of Tamm-Horsfall protein and uromodulin in calcium oxalate crystallization
 Brazilian Journal of Medical and Biological Research (2002) 35: 1165-1172 Role of THP and UM in calcium oxalate crystallization ISSN 0100-879X 1165 Role of Tamm-Horsfall protein and uromodulin in calcium
Brazilian Journal of Medical and Biological Research (2002) 35: 1165-1172 Role of THP and UM in calcium oxalate crystallization ISSN 0100-879X 1165 Role of Tamm-Horsfall protein and uromodulin in calcium
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
G. Manish. et.al/ 1(4) pp
 Fractions from Coconut water (Cocos nucifera) influencing in vitro calcium oxalate crystal growth Manish Gandhi * 1, Tandon Chanderdeep 2, Puri Sanjeev 3, Singla Surindar *1, *1 Department of Biochemistry,
Fractions from Coconut water (Cocos nucifera) influencing in vitro calcium oxalate crystal growth Manish Gandhi * 1, Tandon Chanderdeep 2, Puri Sanjeev 3, Singla Surindar *1, *1 Department of Biochemistry,
Correspondence between stone composition and urine supersaturation in nephrolithiasis
 Kidney International, Vol. 51 (1997), pp. 894 900 Correspondence between stone composition and urine supersaturation in nephrolithiasis JOAN H. PARKS, MARK COWARD, and REDRIC L. COE Program in Nephrology,
Kidney International, Vol. 51 (1997), pp. 894 900 Correspondence between stone composition and urine supersaturation in nephrolithiasis JOAN H. PARKS, MARK COWARD, and REDRIC L. COE Program in Nephrology,
Europium Labeling Kit
 Europium Labeling Kit Catalog Number KA2096 100ug *1 Version: 03 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 Principle of the Assay...
Europium Labeling Kit Catalog Number KA2096 100ug *1 Version: 03 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 Principle of the Assay...
Osteopontin Is a Critical Inhibitor of Calcium Oxalate Crystal Formation and Retention in Renal Tubules
 J Am Soc Nephrol 14: 139 147, 2003 Osteopontin Is a Critical Inhibitor of Calcium Oxalate Crystal Formation and Retention in Renal Tubules JEFFREY A. WESSON,* RICHARD J. JOHNSON, MARRILDA MAZZALI, ANNE
J Am Soc Nephrol 14: 139 147, 2003 Osteopontin Is a Critical Inhibitor of Calcium Oxalate Crystal Formation and Retention in Renal Tubules JEFFREY A. WESSON,* RICHARD J. JOHNSON, MARRILDA MAZZALI, ANNE
The Nuts and Bolts of Kidney Stones. Soha Zouwail Consultant Chemical Pathology UHW Renal Training Day 2019
 The Nuts and Bolts of Kidney Stones Soha Zouwail Consultant Chemical Pathology UHW Renal Training Day 2019 Urinary Calculi Prevalence and incidence of kidney stones increasing across the world Environmental
The Nuts and Bolts of Kidney Stones Soha Zouwail Consultant Chemical Pathology UHW Renal Training Day 2019 Urinary Calculi Prevalence and incidence of kidney stones increasing across the world Environmental
Urolithiasis. Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery
 Urolithiasis Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery Urolithiasis: Why should we care? Affects 5% of US men and women Men twice as
Urolithiasis Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery Urolithiasis: Why should we care? Affects 5% of US men and women Men twice as
SUPPLEMENTARY FIGURES
 SUPPLEMENTARY FIGURES Supplementary Figure 1: immunoprecipitation with anti-casr antibody The Casr protein was expressed in transiently transfected HEK cells. Cell lysates from HEK cells were subjected
SUPPLEMENTARY FIGURES Supplementary Figure 1: immunoprecipitation with anti-casr antibody The Casr protein was expressed in transiently transfected HEK cells. Cell lysates from HEK cells were subjected
Identification of structural domains in inter- -trypsin inhibitor involved in calcium oxalate crystallization
 Kidney International, Vol. 53 (1998), pp. 1727 1735 Identification of structural domains in inter- -trypsin inhibitor involved in calcium oxalate crystallization HIROSHI KOBAYASHI, KIYOSHI SHIBATA, MICHIO
Kidney International, Vol. 53 (1998), pp. 1727 1735 Identification of structural domains in inter- -trypsin inhibitor involved in calcium oxalate crystallization HIROSHI KOBAYASHI, KIYOSHI SHIBATA, MICHIO
School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR
 1 School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR URINARY (RENAL) STONE FORMATION An Overview What are Urinary (Renal)
1 School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR URINARY (RENAL) STONE FORMATION An Overview What are Urinary (Renal)
Renal Physiology II Tubular functions
 Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
NEPHROLITHIASIS Etiology, stone composition, medical management, and prevention
 NEPHROLITHIASIS Etiology, stone composition, medical management, and prevention Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Epidemiology Prevalence 2-3%, maybe in
NEPHROLITHIASIS Etiology, stone composition, medical management, and prevention Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Epidemiology Prevalence 2-3%, maybe in
Diet and fluid prescription in stone disease
 http://www.kidney-international.org & 2006 International Society of Nephrology mini review Diet and fluid prescription in stone disease EN Taylor 1 and GC Curhan 1,2 1 Renal Division, Department of Medicine,
http://www.kidney-international.org & 2006 International Society of Nephrology mini review Diet and fluid prescription in stone disease EN Taylor 1 and GC Curhan 1,2 1 Renal Division, Department of Medicine,
Medical Approach to Nephrolithiasis. Seth Goldberg, MD September 15, 2017 ACP Meeting
 Medical Approach to Nephrolithiasis Seth Goldberg, MD September 15, 2017 ACP Meeting DISCLOSURES Seth Goldberg, MD Assistant Professor of Medicine Research support Abbott Kadmon Otsuka Pfizer Introduction
Medical Approach to Nephrolithiasis Seth Goldberg, MD September 15, 2017 ACP Meeting DISCLOSURES Seth Goldberg, MD Assistant Professor of Medicine Research support Abbott Kadmon Otsuka Pfizer Introduction
GLP-2 ELISA. For the quantitative determination of GLP-2 in human serum and plasma samples.
 GLP-2 ELISA For the quantitative determination of GLP-2 in human serum and plasma samples. For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number: 48-GP2HU-E01.1 Size: 96 wells Version:
GLP-2 ELISA For the quantitative determination of GLP-2 in human serum and plasma samples. For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number: 48-GP2HU-E01.1 Size: 96 wells Version:
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Renal Pharmacology. Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics BIMM118
 Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics Renal Pharmacology Kidneys: Represent 0.5% of total body weight, but receive ~25% of the total arterial blood
Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics Renal Pharmacology Kidneys: Represent 0.5% of total body weight, but receive ~25% of the total arterial blood
TSH (Human) ELISA Kit
 TSH (Human) ELISA Kit Catalog Number KA0197 96 assays Version: 03 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 Principle of the Assay...
TSH (Human) ELISA Kit Catalog Number KA0197 96 assays Version: 03 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 Principle of the Assay...
24-h uric acid excretion and the risk of kidney stones
 http://www.kidney-international.org & 2008 International Society of Nephrology original article 24-h uric acid excretion and the risk of kidney stones GC Curhan 1,2,3 and EN Taylor 1,2 1 Department of
http://www.kidney-international.org & 2008 International Society of Nephrology original article 24-h uric acid excretion and the risk of kidney stones GC Curhan 1,2,3 and EN Taylor 1,2 1 Department of
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Influence of Urinary Stones on the Composition of a 24-Hour Urine Sample
 Clinical Chemistry 49:2 281 285 (2003) General Clinical Chemistry Influence of Urinary Stones on the Composition of a 24-Hour Urine Sample Norbert Laube, 1* Michael Pullmann, 2 Stefan Hergarten, 2 and
Clinical Chemistry 49:2 281 285 (2003) General Clinical Chemistry Influence of Urinary Stones on the Composition of a 24-Hour Urine Sample Norbert Laube, 1* Michael Pullmann, 2 Stefan Hergarten, 2 and
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance
 Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
1. remove: waste products: urea, creatinine, and uric acid foreign chemicals: drugs, water soluble vitamins, and food additives, etc.
 Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
The Immunoassay Guide to Successful Mass Spectrometry. Orr Sharpe Robinson Lab SUMS User Meeting October 29, 2013
 The Immunoassay Guide to Successful Mass Spectrometry Orr Sharpe Robinson Lab SUMS User Meeting October 29, 2013 What is it? Hey! Look at that! Something is reacting in here! I just wish I knew what it
The Immunoassay Guide to Successful Mass Spectrometry Orr Sharpe Robinson Lab SUMS User Meeting October 29, 2013 What is it? Hey! Look at that! Something is reacting in here! I just wish I knew what it
Schedule of taking calcium supplement and the risk of nephrolithiasis
 Kidney International, Vol. 65 (2004), pp. 1835 1841 Schedule of taking calcium supplement and the risk of nephrolithiasis SOMNUEK DOMRONGKITCHAIPORN,WICHAI SOPASSATHIT, WASANA STITCHANTRAKUL, SURASING
Kidney International, Vol. 65 (2004), pp. 1835 1841 Schedule of taking calcium supplement and the risk of nephrolithiasis SOMNUEK DOMRONGKITCHAIPORN,WICHAI SOPASSATHIT, WASANA STITCHANTRAKUL, SURASING
EFFECT OF DIETARY CATION-ANION DIFFERENCE ON MINERAL BALANCE IN WEANLING HORSES. Authors:
 EFFECT OF DIETARY CATION-ANION DIFFERENCE ON MINERAL BALANCE IN WEANLING HORSES 1999 Animal Science Research Report Authors: Story in Brief Pages 182-188 S.R. Cooper, D.R. Topliff, D.W. Freeman, J.E. Breazile
EFFECT OF DIETARY CATION-ANION DIFFERENCE ON MINERAL BALANCE IN WEANLING HORSES 1999 Animal Science Research Report Authors: Story in Brief Pages 182-188 S.R. Cooper, D.R. Topliff, D.W. Freeman, J.E. Breazile
Na + Transport 1 and 2 Linda Costanzo, Ph.D.
 Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
It is truly an honor to contribute to this issue of Seminars in
 Physiology of Acid-Base Balance: Links With Kidney Stone Prevention Mitchell L. Halperin, Surinder Cheema Dhadli, and Kamel S. Kamel Two processes permit the urine ph and the medullary interstitial ph
Physiology of Acid-Base Balance: Links With Kidney Stone Prevention Mitchell L. Halperin, Surinder Cheema Dhadli, and Kamel S. Kamel Two processes permit the urine ph and the medullary interstitial ph
Mouse C-peptide EIA. Cat. No. YII-YK013-EX FOR LABORATORY USE ONLY
 Mouse C-peptide EIA Cat. No. YII-YK013-EX FOR LABORATORY USE ONLY TOYO 2CHOME, KOTO-KU, TOKYO, 135-0016, JAPAN http://www.cosmobio.co.jp e-mail : export@cosmobio.co.jp Phone : +81-3-5632-9617 FAX : +81-3-5632-9618
Mouse C-peptide EIA Cat. No. YII-YK013-EX FOR LABORATORY USE ONLY TOYO 2CHOME, KOTO-KU, TOKYO, 135-0016, JAPAN http://www.cosmobio.co.jp e-mail : export@cosmobio.co.jp Phone : +81-3-5632-9617 FAX : +81-3-5632-9618
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
11/05/1431. Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate
 Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Functions of Proximal Convoluted Tubules
 1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
For more information about how to cite these materials visit
 Author(s): Michael Heung, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Michael Heung, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics
 This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion
This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion
24 Hours Urinary Citrate Levels and Frequency of Hypocitraturia among patients with Recurrent Nephrolithiasis
 ORIGINAL ARTICLE 24 Hours Urinary Citrate Levels and Frequency of Hypocitraturia among patients with Recurrent Nephrolithiasis AHMED BILAL 1, ABDUL GHAFFAR 2, ANUSHA GHAFFAR 3, M. RAFIQUE 4 ABSTRACT Background:
ORIGINAL ARTICLE 24 Hours Urinary Citrate Levels and Frequency of Hypocitraturia among patients with Recurrent Nephrolithiasis AHMED BILAL 1, ABDUL GHAFFAR 2, ANUSHA GHAFFAR 3, M. RAFIQUE 4 ABSTRACT Background:
CONTENTS. STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1
 CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
EQUILIBRIUM VERSUS SUPERSATURATED URINE HYPOTHESIS IN CALCIUM SALT UROLITHIASIS: A NEW THEORETICAL AND PRACTICAL APPROACH TO A CLINICAL PROBLEM
 Scanning Microscopy Vol. 13, No. 2-3, 1999 (Pages 261-265) 0891-7035/99$5.00+.25 Scanning Microscopy International, Chicago Equilibrium (AMF O Hare), model for IL calcium 60666 USA salt urolithiasis EQUILIBRIUM
Scanning Microscopy Vol. 13, No. 2-3, 1999 (Pages 261-265) 0891-7035/99$5.00+.25 Scanning Microscopy International, Chicago Equilibrium (AMF O Hare), model for IL calcium 60666 USA salt urolithiasis EQUILIBRIUM
Anatomy/Physiology Study Guide: Unit 9 Excretory System
 Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
GLP-2 (Rat) ELISA. For the quantitative determination of glucagon-like peptide 2 (GLP-2) in rat serum and plasma
 GLP-2 (Rat) ELISA For the quantitative determination of glucagon-like peptide 2 (GLP-2) in rat serum and plasma For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number: 48-GP2RT-E01
GLP-2 (Rat) ELISA For the quantitative determination of glucagon-like peptide 2 (GLP-2) in rat serum and plasma For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number: 48-GP2RT-E01
Urine Stone Screen requirements
 Urine Stone Screen requirements Unique Identifying Index Number LP/PA/CB/CBSP030 Version number 4 Issue Date (this version) 03.08.15 Document Type Accreditation or Licensing Standard to which this applies
Urine Stone Screen requirements Unique Identifying Index Number LP/PA/CB/CBSP030 Version number 4 Issue Date (this version) 03.08.15 Document Type Accreditation or Licensing Standard to which this applies
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
CITRATE IS ATRICARBOXYLIC acid normally
 Causes of Hypocitraturia in Recurrent Calcium Stone Formers: Focusing on Urinary Potassium Excretion Somnuek Domrongkitchaiporn, MD, Wasana Stitchantrakul, MSc, and Wachira Kochakarn, MD Background: Multiple
Causes of Hypocitraturia in Recurrent Calcium Stone Formers: Focusing on Urinary Potassium Excretion Somnuek Domrongkitchaiporn, MD, Wasana Stitchantrakul, MSc, and Wachira Kochakarn, MD Background: Multiple
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
NATURAL HISTORY AND SURVIVAL OF PATIENTS WITH ASCITES. PATIENTS WHO DO NOT DEVELOP COMPLICATIONS HAVE MARKEDLY BETTER SURVIVAL THAN THOSE WHO DEVELOP
 PROGNOSIS Mortality rates as high as 18-30% are reported for hyponatremic patients. High mortality rates reflect the severity of underlying conditions and are not influenced by treatment of hyponatremia
PROGNOSIS Mortality rates as high as 18-30% are reported for hyponatremic patients. High mortality rates reflect the severity of underlying conditions and are not influenced by treatment of hyponatremia
URINARY CRYSTALS. by Geoffrey K. Dube and Robert S. Brown
 URINARY CRYSTALS by Geoffrey K. Dube and Robert S. Brown A 26 year-old man presents with a fever and weakness. His WBC is 133,000, with 83% blasts. Creatinine is 2.0 mg/dl and serum uric acid is 15.4 mg/dl.
URINARY CRYSTALS by Geoffrey K. Dube and Robert S. Brown A 26 year-old man presents with a fever and weakness. His WBC is 133,000, with 83% blasts. Creatinine is 2.0 mg/dl and serum uric acid is 15.4 mg/dl.
See external label 2 C-8 C Σ=96 tests Cat # 3122Z MICROWELL ELISA THYROID STIMULATING HORMONE (TSH) ENZYME IMMUNOASSAY TEST KIT TSH.
 DIAGNOSTIC AUTOMATION, INC. 23961 Craftsman Road, Suite D/E/F, Calabasas, CA 91302 Tel: (818) 591-3030 Fax: (818) 591-8383 onestep@rapidtest.com technicalsupport@rapidtest.com www.rapidtest.com See external
DIAGNOSTIC AUTOMATION, INC. 23961 Craftsman Road, Suite D/E/F, Calabasas, CA 91302 Tel: (818) 591-3030 Fax: (818) 591-8383 onestep@rapidtest.com technicalsupport@rapidtest.com www.rapidtest.com See external
Quantitative protein estimation of Urine
 Quantitative protein estimation of Urine 1 In a healthy renal and urinary tract system, the urine contains no protein or only trace amounts. The presence of increased amounts of protein in the urine can
Quantitative protein estimation of Urine 1 In a healthy renal and urinary tract system, the urine contains no protein or only trace amounts. The presence of increased amounts of protein in the urine can
TSH ELISA Kit Medical Device Licence No.: 16419
 TSH ELISA Kit Medical Device Licence No.: 16419 Enzyme immunoassay kit for the quantitative determination of TSH concentration in serum. Catalog Number: SL100305 Catalog Number: SL100306 Catalog Number:
TSH ELISA Kit Medical Device Licence No.: 16419 Enzyme immunoassay kit for the quantitative determination of TSH concentration in serum. Catalog Number: SL100305 Catalog Number: SL100306 Catalog Number:
Evaluation of different urinary constituent ratios in renal stone formers
 Available online at www.scholarsresearchlibrary.com Annals of Biological Research, 2010, 1 (3) : 50-55 (http://scholarsresearchlibrary.com/archive.html) ISSN 0976-1233 CODEN (USA): ABRNBW Evaluation of
Available online at www.scholarsresearchlibrary.com Annals of Biological Research, 2010, 1 (3) : 50-55 (http://scholarsresearchlibrary.com/archive.html) ISSN 0976-1233 CODEN (USA): ABRNBW Evaluation of
Normal Renal Function
 Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
MEDICAL STONE MANAGEMENT MADE EASY PRACTICAL ADVICE
 MEDICAL STONE MANAGEMENT MADE EASY PRACTICAL ADVICE Comprehensive Kidney Stone Center at Duke University Medical Center Durham, North Carolina Glenn M. Preminger, M.D. UCLA State-of-the Art Urology 02
MEDICAL STONE MANAGEMENT MADE EASY PRACTICAL ADVICE Comprehensive Kidney Stone Center at Duke University Medical Center Durham, North Carolina Glenn M. Preminger, M.D. UCLA State-of-the Art Urology 02
Renal Physiology - Lectures
 Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Renal Data from Asia Africa
 Saudi J Kidney Dis Transpl 2013;24(4):838-843 2013 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Renal Data from Asia Africa Metabolic Evaluation in First-Time
Saudi J Kidney Dis Transpl 2013;24(4):838-843 2013 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Renal Data from Asia Africa Metabolic Evaluation in First-Time
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
Human Creatinine Urinary Detection Kit
 Human Creatinine Urinary CATALOG NO: IRAAKT2509 Detection Kit LOT NO: SAMPLE INTENDED USE The Urinary Creatinine kit is designed to quantitatively measure creatinine present in urine samples. BACKGROUND
Human Creatinine Urinary CATALOG NO: IRAAKT2509 Detection Kit LOT NO: SAMPLE INTENDED USE The Urinary Creatinine kit is designed to quantitatively measure creatinine present in urine samples. BACKGROUND
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
Histology Urinary system
 Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
human Total Cathepsin B Catalog Number: DY2176
 human Total Cathepsin B Catalog Number: DY2176 This DuoSet ELISA Development kit contains the basic components required for the development of sandwich ELISAs to measure natural and recombinant human Total
human Total Cathepsin B Catalog Number: DY2176 This DuoSet ELISA Development kit contains the basic components required for the development of sandwich ELISAs to measure natural and recombinant human Total
Original article: 24 hours urinary analysis for renal stones promoters and inhibitors in North India
 Original article: 24 hours urinary analysis for renal stones promoters and inhibitors in North India Singh Kanchan*, Singh A.K**, Roy Ajanta*** *, *** Assistant Professor & Professor Dept. of Biochemistry,
Original article: 24 hours urinary analysis for renal stones promoters and inhibitors in North India Singh Kanchan*, Singh A.K**, Roy Ajanta*** *, *** Assistant Professor & Professor Dept. of Biochemistry,
Adhesion of uric acid crystals to the surface of renal epithelial cells
 Am J Physiol Renal Physiol 278: F989 F998, 2000. Adhesion of uric acid crystals to the surface of renal epithelial cells RIMA M. KOKA, ERICK HUANG, AND JOHN C. LIESKE Department of Medicine, The University
Am J Physiol Renal Physiol 278: F989 F998, 2000. Adhesion of uric acid crystals to the surface of renal epithelial cells RIMA M. KOKA, ERICK HUANG, AND JOHN C. LIESKE Department of Medicine, The University
I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a.
 I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a. Renal fascia b. Perinephric fat (Adipose) capsule c. Fibrous
I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a. Renal fascia b. Perinephric fat (Adipose) capsule c. Fibrous
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Urinary system. Lab-7
 Urinary system Lab-7 Excretion: processes that remove wastes and excess materials from the body Urinary system (kidneys): excretes nitrogenous wastes, excess solutes, and water The Kidneys Regulate Water
Urinary system Lab-7 Excretion: processes that remove wastes and excess materials from the body Urinary system (kidneys): excretes nitrogenous wastes, excess solutes, and water The Kidneys Regulate Water
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Mouse GLP-2 EIA FOR LABORATORY USE ONLY
 YK142 Mouse GLP-2 EIA FOR LABORATORY USE ONLY Kasumigaseki place, 3-6-7, Kasumigaseki, Chiyoda-ku, Tokyo 100-0013 Japan http://www.sceti.co.jp/english/export e-mail exp-pet@sceti.co.jp
YK142 Mouse GLP-2 EIA FOR LABORATORY USE ONLY Kasumigaseki place, 3-6-7, Kasumigaseki, Chiyoda-ku, Tokyo 100-0013 Japan http://www.sceti.co.jp/english/export e-mail exp-pet@sceti.co.jp
5.Which part of the nephron removes water, ions and nutrients from the blood?
 Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
1. Anatomy / Vascularisation. 2. Urine concentration. 3. Axial heterogeneity of some segments
 Lise BANKIR 1. Anatomy / Vascularisation 2. Urine concentration 3. Axial heterogeneity of some segments Rat kidney. Arterial filling with Microfil silicone rubber Alcian Blue staining Filling of arterial
Lise BANKIR 1. Anatomy / Vascularisation 2. Urine concentration 3. Axial heterogeneity of some segments Rat kidney. Arterial filling with Microfil silicone rubber Alcian Blue staining Filling of arterial
Summary 255 Research Summary
 Chapter 10 Summary Nephrolithiasis remains a public health problem around the world, affecting 12% of the adult population. The prevalence and incidence of kidney stones are increasing with global warming,
Chapter 10 Summary Nephrolithiasis remains a public health problem around the world, affecting 12% of the adult population. The prevalence and incidence of kidney stones are increasing with global warming,
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Chapter 20 Diseases of the kidney:
 Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
Citation 泌尿器科紀要 (2004), 50(7):
 TitleRole of the urinary calcium in the Author(s) Murayama, Tetsuo; Sakai, Naoki; Tak Tetsuo Citation 泌尿器科紀要 (24), 5(7): 451-455 Issue Date 24-7 URL http://hdl.handle.net/2433/113414 Right Type Departmental
TitleRole of the urinary calcium in the Author(s) Murayama, Tetsuo; Sakai, Naoki; Tak Tetsuo Citation 泌尿器科紀要 (24), 5(7): 451-455 Issue Date 24-7 URL http://hdl.handle.net/2433/113414 Right Type Departmental
After studying this lecture, you should be able to...
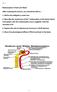 Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Oxalate (urine, plasma)
 Oxalate (urine, plasma) 1 Name and description of analyte 1.1 Name of analyte Oxalate 1.2 Alternative names 1.3 NLMC code To follow 1.4. Function of analyte Oxalate is a metabolic end product primarily
Oxalate (urine, plasma) 1 Name and description of analyte 1.1 Name of analyte Oxalate 1.2 Alternative names 1.3 NLMC code To follow 1.4. Function of analyte Oxalate is a metabolic end product primarily
TEPZZ _6 76A_T EP A1 (19) (11) EP A1. (12) EUROPEAN PATENT APPLICATION published in accordance with Art.
 (19) TEPZZ _6 76A_T (11) EP 3 162 376 A1 (12) EUROPEAN PATENT APPLICATION published in accordance with Art. 13(4) EPC (43) Date of publication: 03.0.17 Bulletin 17/18 (21) Application number: 172173.0
(19) TEPZZ _6 76A_T (11) EP 3 162 376 A1 (12) EUROPEAN PATENT APPLICATION published in accordance with Art. 13(4) EPC (43) Date of publication: 03.0.17 Bulletin 17/18 (21) Application number: 172173.0
PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE
 PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE - OBJECTIVES: 1- The simple examination of urine. 2- To detect some of the normal organic constituents of urine. 3- To detect some of the
PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE - OBJECTIVES: 1- The simple examination of urine. 2- To detect some of the normal organic constituents of urine. 3- To detect some of the
Pathogenesis and clinical course of mixed calcium oxalate and uric acid nephrolithiasis
 Kidney International, Vol. 22 (1982), pp. 366 3 70 Pathogenesis and clinical course of mixed calcium oxalate and uric acid nephrolithiasis STEPHANIE MILLMAN, AMY L. STRAUSS, JOAN H. PARKS, AND FREDRIC
Kidney International, Vol. 22 (1982), pp. 366 3 70 Pathogenesis and clinical course of mixed calcium oxalate and uric acid nephrolithiasis STEPHANIE MILLMAN, AMY L. STRAUSS, JOAN H. PARKS, AND FREDRIC
See external label 96 tests ULTRASENSITIVE THYROID STIMULATING HORMONE (u-tsh) TSH Ultra Sensitive
 DIAGNOSTIC AUTOMATION, INC. 21250 Califa Street, Suite 102 and 116, Woodland Hills, CA 91367 Tel: (818) 591-3030 Fax: (818) 591-8383 onestep@rapidtest.com technicalsupport@rapidtest.com www.rapidtest.com
DIAGNOSTIC AUTOMATION, INC. 21250 Califa Street, Suite 102 and 116, Woodland Hills, CA 91367 Tel: (818) 591-3030 Fax: (818) 591-8383 onestep@rapidtest.com technicalsupport@rapidtest.com www.rapidtest.com
Furosemide: Properties, Alternatives, and the Medication Approval Process. Heather Brown EMS 209-Advanced Pharmacology Don Knox
 Furosemide: Properties, Alternatives, and the Medication Approval Process Heather Brown EMS 209-Advanced Pharmacology Don Knox Pre-hospital treatment of critical patients is a key factor in determining
Furosemide: Properties, Alternatives, and the Medication Approval Process Heather Brown EMS 209-Advanced Pharmacology Don Knox Pre-hospital treatment of critical patients is a key factor in determining
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Hydration status affects osteopontin expression in the rat kidney
 Original Article J Vet Sci 2016, 17(3), 269-277 ㆍ http://dx.doi.org/10.4142/jvs.2016.17.3.269 JVS Hydration status affects osteopontin expression in the rat kidney Su-Youn Lee 1, Sae-Jin Lee 1, Hong-Lin
Original Article J Vet Sci 2016, 17(3), 269-277 ㆍ http://dx.doi.org/10.4142/jvs.2016.17.3.269 JVS Hydration status affects osteopontin expression in the rat kidney Su-Youn Lee 1, Sae-Jin Lee 1, Hong-Lin
NORMAL POTASSIUM DISTRIBUTION AND BALANCE
 NORMAL POTASSIUM DISTRIBUTION AND BALANCE 98% of body potassium is contained within cells, principally muscle cells, and is readily exchangeable. Only 2% is in ECF. Daily intake exceeds the amount in ECF.
NORMAL POTASSIUM DISTRIBUTION AND BALANCE 98% of body potassium is contained within cells, principally muscle cells, and is readily exchangeable. Only 2% is in ECF. Daily intake exceeds the amount in ECF.
Dependence of upper limit of metastability on supersaturation in
 Kidney International, Vol. 52 (1997), pp. 162 168 CLINICAL NEPHROLOGY_- EPIDEMIOLOGY - CLINICAL TRIALS Dependence of upper limit of metastability on supersaturation in nephrolithiasis JOHN R. ASPLIN, JOAN
Kidney International, Vol. 52 (1997), pp. 162 168 CLINICAL NEPHROLOGY_- EPIDEMIOLOGY - CLINICAL TRIALS Dependence of upper limit of metastability on supersaturation in nephrolithiasis JOHN R. ASPLIN, JOAN
Human Apolipoprotein A1 EIA Kit
 A helping hand for your research Product Manual Human Apolipoprotein A1 EIA Kit Catalog Number: 83901 96 assays 1 Table of Content Product Description 3 Assay Principle 3 Kit Components 3 Storage 4 Reagent
A helping hand for your research Product Manual Human Apolipoprotein A1 EIA Kit Catalog Number: 83901 96 assays 1 Table of Content Product Description 3 Assay Principle 3 Kit Components 3 Storage 4 Reagent
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
