Osteochondral fractures of the dome of the talus
|
|
|
- Francis Garey Melton
- 5 years ago
- Views:
Transcription
1 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Osteochondral fractures of the dome of the talus IF Anderson, KJ Crichton, T Grattan-Smith, RA Cooper and D Brazier J Bone Joint Surg Am. 1989;71: This information is current as of July 25, 2010 Reprints and Permissions Publisher Information Click here to order reprints or request permission to use material from this article, or locate the article citation on jbjs.org and click on the [Reprints and Permissions] link. The Journal of Bone and Joint Surgery 20 Pickering Street, Needham, MA
2 Copyright 1989 by The Journal of Bone and Joint Surgery, Incorporated Osteochondral Fractures of the Dome of the Talus* BY IAN F. ANDERSON, MB., B.S., F.R.A.C.R.t1, KEN J. CRICHTON, MB., B.S., GRAD.DIP.SPORT SC.t, CROWS NEST, TONY GRATTAN-SMITH, MB., B.S., F.R.A.C.R.1, ROBERT A. COOPER, M.B., B.S., D.D.U., F.R.A.C.P., AND DAVID BRAZIER, M.B., B.S., F.R.A.C.R4, ST. LEONARDS, NEW SOUTH WALES, AUSTRALIA From the Department of Diagnostic Radiology. Royal North Shore Hospital of Sydney. St. Leonards, and the North Sydney Orthopaedic and Sports Medicine Clinic, Crows Nest ABSTRACT: Twenty-four patients who had an osteochondral fracture of the dome of the talus were examined by plain radiography, magnetic resonance imaging, computerized tomography, and, when mdicated, scintigraphy. When plain radiographs of the ankle are relied on for the diagnosis of an osteochondral fracture of the talus, many lesions remain undiagnosed. Stage-I osteochondral fractures show no diagnostic changes on plain radiographs, and Stage-Il lesions are usually subtle and, therefore, are often overlooked by both radiologists and clinicians. The use of scintigraphy as a screening procedure and of magnetic resonance imaging for patients who have positive scintiscans showed that osteochondral fractures are more common than has previously been indicated in the literature. Scintigraphy should be used to assess patients when there is clinical suspicion of an osteochondral fracture but the plain radiographs appear to be negative. Patients who have positive scintiscans should be assessed by magnetic resonance imaging. Patients who have abnormal plain radiographs will derive no major benefits from magnetic resonance imaging; for all but one of these patients, computerized tomography was adequate for staging the fracture. Sprains of the ligaments of the ankle are the most frequent injury in sports4 #{176}.Although most such injuries are confined to the ligaments, the possibility ofan osteochondral fracture of the dome of the talus must be considered in these patients and in those who continue to complain of pain and disability despite apparently normal plain radiographs. Such fractures of the dome of the talus have been well reviewed and discussed in the 1iterature Although, in the past, they were often called osteochondritis dissecans ofthe talus, there is now general agreement that these lesions are actually osteochondral fractures and that they can be * No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject ofthis article. No funds were received in support of this study. t North Sydney Orthopaedic and Sports Medicine Clinic, 286 Pacific Highway, Crows Nest, New South Wales 2065, Australia. Please address requests for reprints to Dr. Anderson. Royal North Shore Hospital of Sydney, St. Leonards, New South Wales 2065, Australia. produced by trauma on both the medial and lateral aspects of the talus. Delay in establishing the diagnosis is common, as the initial radiographs may be negative or the evidence of fracture may be so subtle that it is overlooked. In addition, the symptoms are usually blamed entirely on the associated ligamentous injury, confusing the diagnosis and contributing to the delay. Most often the diagnosis is not made until after the fracture has progressed to a more advanced stage 316. In 1959, Berndt and Harty wrote a paper on osteochondral fractures of the talus. They noted that 191 lesions of the dome of the talus, variously called osteochondritis dissecans or osteochondral fractures, had been reported in the literature, and they added twenty-one cases. Their article reviewed and discussed the entity, rationalized the nomenclature, and proposed the name of transchondral fracture. They suggested that approximately 0.09 per cent of all fractures are transchondral fractures of the talus. Using abovethe-knee amputation specimens, they were able to reproduce fractures of both the medial and lateral aspects of the dome of the talus that were similar to those encountered clinically. Lateral fractures were produced by inversion and dorsiflexion, and medial fractures, by strong lateral rotation of the tibia on a plantar-flexed and inverted foot. Berndt and Harty proposed a four-stage classification system for these fractures, as follows: Stage I - there is a localized area of subchondral trabecular compression; Stage II - the fragment is incompletely separated; Stage III - the fragment is completely separated but undisplaced; Stage lila - the fragment is detached and rotated; and Stage IV - the fragment is displaced or inverted in its fracture bed. Since the work of Berndt and Harty, the development of new imaging techniques has made the diagnosis of osteochondral fractures easier. Computerized tomography shows bone in great detail, and now magnetic resonance imaging can show articular cartilage and subtle changes in bone marrow as well as bone detail. The purpose of this study was to assess whether the traditionally difficult diagnosis and staging of osteochondral fractures can be done more accurately with the aid of these newer imaging modalities. Materials and Methods In January 1988, as part of an over-all musculoskeletal program, the radiology department at the Royal North Shore VOL. 71-A, NO. 8, SEPTEMBER
3 F. ANDERSON ET AL. TABLE I DATA ON PATIENTS WHO HAD POST-TRAUMATIC DISABILITY OF THE ANKLE (GROUP I) AND PATIENTS WHO WERE DIAGNOSED ON THE BASIS OF RADIOGRAPHS MADE IMMEDIATELY A FTER AN INVERS ION INJURY (GR OUP 2) Review of Staging Site of Delay in First First Subsequent Computerized Magnetic Case Sex, Age Fract. Diagnosis Radiograph* Radiograph* Radiographs* Scintigraphy* Tomography Res. Imaging (Yrs.) (Mos.) Group I I M, 28 Post. med lilt I 2 M, 36 Mid. lat III and IIA III and IIA 3 F, 69 Ant. med Normal I 4 M, 39 Post. lat Ill III and ha 5 M, 27 Post. lat NP + Normal I 6 F, 31 Post. med ha ha 7 M,28 Post. med IIandIIA IlandIlA 8 F, 29 Mid. med IIA IIA 9 F, 39 Mid. med Normal I 10 F, 29 Mid. med NP + Normal I 11 F,21 Ant.med IlA IIA 12 F, 63 Post. med IIA ha 13 M, 26 Post. med III Ill 14 M, 22 Ant. med. Group 2 Post. lat M, 19 Post. med NP Ill III 16 M, 20 Post. lat NP NP III III 17 F, 12 Post. lat NP NP II II 18 M, 20 Post. lat NP + III III 19 F, 30 Post. lat NP NP IV Postop. 20 F, 27 Mid. lat NP NP II II 21 F, 44 Post. lat NP NP Normal II 22 M, 21 Post. lat NP III III M, 21 Mid. med III and ha III and IIA 24 F, 25 Ant. lat NP NP III III IIA III IIA III normal examination; + fracture present on radiographs or increased uptake on scintiscans; and NP not performed. *--. t Computerized tomography was performed three months after the initial diagnosis was made with the aid of magnetic resonance imaging. The fracture had progressed to Stage III. Hospital of Sydney embarked on a study of the ankle joint by magnetic resonance imaging. One or two ankles were examined each week, for a total of fifty-six ankles in a ninemonth period. Thirty of the fifty-six patients had been seen for posttraumatic chronic disability of the ankle, the cause of which had remained undiagnosed despite adequate plain radiographs. Most of these patients had been referred from the North Sydney Orthopaedic and Sports Medicine Clinic. The fourteen patients in Group 1 were selected from these patients. Group 2 consisted of ten patients who had been diagnosed as having an osteochondral fracture of the talus on the basis of plain radiographs and who were referred for staging of the fracture with the aid of magnetic resonance imaging. Most of these patients were referred from the hospital s casualty department. For all patients, there was an attempt to establish the mechanism of injury. Scintigraphy of the ankle was performed on all of the patients in Group 1, and the ankles of both groups were examined by computerized tomography and magnetic resonance imaging. Magnetic resonance imaging was performed with a 1.5- tesla system (Signa; General Electric Medical Systems, Milwaukee, Wisconsin), with the ankle joint placed in a cylindrical extremity coil having a 16.5-centimeter diameter. After the plane of the articular surface of the talus was determined in a coronal localizing series, a sagittal Tlweighted series was made in a plane 90 degrees to the articular surface ofthe talus. Additional Tl series were made in the coronal and axial planes. A pulse-repetition time of 600 to 800 milliseconds and an echo time of twenty milliseconds were used with two acquisitions. Images of threemillimeter-thick slices were obtained, with a one-millimeter gap between the slices, on a 256-by-256 matrix. The sagittal series was made with a sixteen-centimeter field of view, and the field was reduced to twelve centimeters for the coronal and axial series. A T2 spin-echo sequence was then made in whatever plane would contribute most to the diagnosis and staging. ThE JOURNAL OF BONE AND JOINT SURGERY
4 OSTEOCHONDRAL FRACTURES OF THE DOME OF THE TALUS Figs. 1-A through l-d: Case 14. Figs. 1-A and 1-B: Magnetic resonance images made nine months after injury. The intermediate image (pulse-repetition time, 2000 milliseconds; echo time, twenty milliseconds) and a T2-weighted image (pulse-repetition time, 2000 milliseconds; echo time, seventy milliseconds) show the presence of a subchondral cyst in the anteromedial aspect of the talar dome (arrowhead). For the computerized tomography, a 9800 system (General Electric) was used to produce most of the images. Adjacent 1.5-millimeter slices were acquired in a semicoronal plane, and a high-resolution bone algorithm with appropriate window settings for bone detail was used. Protocols for computerized tomography of the ankle were described previously by Solomon et al. Three-phase bone scintiscans were made, with flow study and early and delayed views after injection with technetium methylene diphosphonate; imaging was done in anterior and in both right and left lateral projections. The role of scintigraphy as a method of assessing the likelihood of FIG. 1-C Fig. 1-C: The cyst is well delineated on computerized tomography. Fig. 1-D: The cyst (arrowhead) is seen on this Tl-weighted axial image (pulse-repetition time, 600 milliseconds; echo time, twenty milliseconds). A large lateral fracture is also present. VOL. 71-A, NO. 8. SEPTEMBER 1989
5 1 146 I. F. ANDERSON ET AL. i;-..y 1. #{149}: #{149} FIG. 2-A Figs. 2-A, 2-B, and 2-C: Case 1. Fig. 2-A: Normal anteroposterior plain radiograph made eight weeks after injury. an osteochondral fracture in a patient who has normal radiographs has been previously recognized l.t2.23#{149} Group 1 Results (Table I) Surprisingly, of the thirty patients who had undiagnosed post-traumatic disability of the ankle, seventeen (57 per cent) had an osteochondral fracture of the ankle. Three patients had an osteochondral fracture of the tibial plafond only and were excluded from the series. The remaining fourteen patients had fifteen fractures of the dome of the talus. One patient (Case 14) had both a medial and a lateral fracture (Figs. 1-A through 1-D). We believe that this is the first reported case of a double osteochondral fracture of the talus. There were seven men and seven women, and the average age was 34.8 years (range, twenty-one to sixty-nine years). The average delay in diagnosis was 17.6 months. Although the plain radiographs of all of these patients had been initially reported as normal, in five patients (36 per cent) an osteochondral fracture of the talus was in fact visible on review. Eleven (73 per cent) of the fifteen fractures were on the medial aspect of the dome of the talus. The site of the fracture was clearly shown by magnetic resonance imaging with an axial image through the fracture. Both the medial and lateral fractures most commonly occurred posteriorly on the dome of the talus. A typical scintigraphic pattern was seen in eleven of the fifteen fractures in Group 1 (Fig. 2-B); however, three patients (Cases 3, 5, and 10) had variations in the typical pattern. One of these patients (Case 5), in addition to having uptake of the isotope in the area of the dome fracture, also had generalized uptake throughout the ankle joint that was consistent with synovitis. This patient, who owned a gymnasium, had continued to instruct aerobic classes until the diagnosis was made, nine months after the initial injury. The other two patients (Cases 3 and 10) are of particular FIG. 2-B Scintiscan made ten weeks after injury clearly demonstrates increased uptake on the medial aspect of the talus. FIG. 2-C A Ti-weighted image (pulse-repetition time, 600 milliseconds; echo time, twenty milliseconds) showing a decreased signal intensity (arrowhead) on the superomedial aspect of the talus. The appearance is that of trabecular compression and the fracture is Stage I. After the ankle was immobilized in a plaster cast, the symptoms recurred. Computerized tomography showed progression of the fracture to Stage III. interest in that they differed from the remainder of the series. Magnetic resonance imaging in these patients showed a decreased signal intensity from the subchondral marrow on THE JOURNAL OF BONE AND JOINT SURGERY
6 OSTEOCHONDRAL FRACTURES OF THE DOME OF THE TALUS 1147 Figs. 3-A and 3-B: Case 3. Fig. 3-A: Intermediate image made after injury, showing an area of decreased signal intensity (arrowhead) in the subchondral cancellous bone of the anteromedial aspect of the dome of the talus (pulse-repetition time, 2000 milliseconds; echo time, twenty milliseconds). Fig. 3-B: T2-weighted image showing an increased signal intensity(arrowhead) in the same area as in Fig. 3-A (pulse-repetition time, 2000 milliseconds; echo time, seventy milliseconds). This change in signal would indicate bone-marrow edema and cannot be detected on either plain radiographs or on computerized tomography images. the Tl-weighted images. On the T2 series, however, the affected area produced an increased signal intensity, signifying the presence of fluid (Fig. 3-B). All of the other patients had a decreased signal intensity on both the Tl and the T2-weighted images. This is thought to represent edema in the marrow, without major bone damage. One of the two patients (Case 3) had a negative bone scan, and the other (Case 10) had very weak uptake in the area of the fracture, suggesting minimum osteoblastic activity. The typical scintigraphic appearance in the remaining eight patients made it possible to predict that an osteochondral fracture would almost certainly be found on magnetic resonance imaging. However, this scintigraphic pattern can also be seen in patients who have avascular necrosis that is due to other causes, as well as in those who have a neoplasm of bone, an infection, or another injury of bone. Consequently, the finding of this pattern of uptake, although most suggestive, is not diagnostic of an osteochondral fracture. All fourteen patients were also examined by comput- FIG. 4-A FIG. 4-B Figs. 4-A and 4-B: Case 17. Fig. 4-A: Plain radiograph made twenty-four hours after injury, showing a subtle fracture of the lateral aspect of the talar dome (arrowheads). Fig. 4-B: Tl-weighted image showing an extensive area of decreased signal intensity (arrowheads) affecting more than 30 per cent of the dorsolateral aspect of the talus in this three-millimeter slice (pulse-repetition time, 600 milliseconds; echo time, twenty milliseconds). The cortex on the medial side of the fracture is intact, and the fracture is Stage II. The examination was performed with the patient s ankle in a plaster cast, two weeks after injury. VOL. 71-A, NO. 8, SEPTEMBER 1989
7 1 148 I. F. ANDERSON ET AL. FIG. 5-A FIG. 5-B Figs. 5-A through 5-E: Case 8. Fig. 5-A: No abnormality can be seen on this plain radiograph that was made immediately after injury. Fig. 5-B: Five months later, rarefaction has appeared at the superomedial aspect of the talus. The cortex appears normal. Sclerosis surrounds the area of rarefaction. erized tomography. In nine patients, the staging of the fracture corresponded to the staging assigned after magnetic resonance imaging. Of the five Stage-I patients, no abnormality could be detected by computerized tomography in four (Cases 3, 5, 9, and 10). Unfortunately, there was a delay of three months before computerized tomography could be performed on the fifth patient (Case 1), during which time the fracture had progressed from Stage I to Stage III. In one patient (Case 4), the cystic component was not demonstrated on computerized tomography. Group 2 During the nine-month period of the study, ten osteochondral fractures were diagnosed by plain radiography immediately after an inversion injury and were referred to us for staging with the aid of magnetic resonance imaging and computerized tomography. There were five men and five women, and the average age was 23.9 years (range, twelve to forty-four years). Eight of the ten fractures occurred on the lateral side of the talus, most of them posteriorly. Computerized tomography was unable to demonstrate the Stage-Il fracture in one patient (Case 2 1). In the other nine patients, the results of cornputerized tomography and magnetic resonance imaging were comparable. No definite symptoms emerged to aid in the diagnosis of an osteochondral fracture. The Group- 1 patients, however, fell into one of two patterns. The patients who had a Stage-hA fracture (to be described later) complained of a recurrent, diffuse ache in the ankle, which increased with exercise. Exercise also caused a low level of swelling. Symptom-free periods were common. The other patients in Group 1 all complained ofan unremitting ache, which dated back to the initial inversion injury. An increase in weightbearing caused an increase in pain and development of swelling. The signs and symptoms in all Group-2 patients were ligamentous injury with swelling of the ankle, pain, limitation of movement, and bruising. The presence of a fracture was further suspected if there was tenderness in the space between the talus and the tib- Comparison of the Two Groups The two groups differed, most notably with regard to the considerable delay in diagnosis in most of the Group- 1 patients. The Group- 1 patients were, on average, older than those in Group 2 (34.8 compared with 23.9 years). Lateral fractures were more common in Group 2; they were seen earlier and were more often diagnosed by plain radiographs. As has also been noted by other authors6, a thin sliver of bone was separated at the sites of the lateral fractures, whereas the medial fractures had a tendency to be cupshaped. FIG. 5-C An additional thirteen months later, sclerosis and the area of rarefaction are more definite. There is irregularity of the cortex on the medial aspect of the talus, suggesting some compression of the area. THE JOURNAL OF BONE AND JOINT SURGERY
8 OSTEOCHONDRAL FRACTURES OF THE DOME OF THE TALUS 1149 iofibular syndesmosis, as described by Davidson et al. In patients who had a medial fracture, a similar tenderness was encountered when the medial aspect of the talus was palpated in plantar flexion. In attempting to determine the mechanism of injury, a common history was obtained. All of the Group-2 patients, and all but three of the Group- 1 patients, had had a severe inversion injury and a so-called sprain. The degree of associated plantar flexion and dorsiflexion was usually difficult to determine. The mechanism, as described by two patients (Cases 3 and 9), was more of a vertical compression than an inversion, although some inversion had certainly occurred. One patient (Case 14), who had both a medial and a lateral fracture, had had forced eversion prior to inversion. Discussion The most remarkable feature in this series was how commonly an osteochondral fracture of the talus was found in patients who complained of chronic disability after a socalled sprain of the ankle. This injury was found more frequently than has been previously reported The major factors that appeared to be responsible for the increased frequency were the ease with which magnetic resonance imaging made possible earlier and more certain diagnosis of an osteochondral fracture of the talus and our increased interest in and awareness of this entity. A fracture changes the magnetic resonance-imaging signal intensity of bone marrow, and the change often involves a surprisingly large surrounding area (Fig. 4-B). The normally high-intensity signal of cancellous bone on both Tl and T2-weighted images is due to marrow fat (short Ti and short T2). After trauma, there is decreased Ti signal intensity from the cancellous bone surrounding the fracture, due to edematous reaction in the acute and subacute stages (Figs. 3-A and 3-B) and to deposition of fibrous tissue and fibrocartilage in more chronic injuries. This change is easily demonstrated, allowing detection of the most subtle fractures. Computerized tomography is ideal for assessing the progress of an osteochondral fracture and for demonstrating the formation of subchondral cysts. In our experience, however, computerized tomography was unable to detect a Stage-I lesion, but missed only one Stage-Il lesion (Case 21). The staging of osteochondral fractures that was proposed by Berndt and Harty has been generally accepted. However, there has been some difficulty and confusion, mostly surrounding the diagnosis of Stage-I lesions. Davidson et al. reported two Stage-I fractures, neither of which was illustrated or discussed. Five Stage-I fractures were reported by Berndt and Harty, but only three were illustrated and only one was discussed. Osseous changes were reported in the three illustrated cases; these lesions should have been classified as Stage II. Three fractures were classified as Stage I in the series that was reported by Blom and Strijk. In their discussion, under Classification, the staging appeared to have been arrived at by the appearance of the fracture on plain radiographs, although the visible changes on which the staging was based were not described. Flick and Gould illustrated one so-called Stage-I frac- FIG. 5-D FIG. 5-E Figs. 5-D and 5-E: Intermediate and T2-weighted magnetic resonance images made an additional three months later, twenty-two months after injury, showing localized deformity of the anteromedial aspect of the talar dome. The intermediate image (pulse-repetition time, 2000 milliseconds; echo time, twenty milliseconds) demonstrates a cavity, which is shown to contain fluid in the T2-weighted image (pulse-repetition time, 2000 milliseconds; echo time, seventy milliseconds). There is some depression of the cortex on the articular surface. The lesion is Stage IIA, and there is a subchondral cyst. VOL. 71-A, NO. 8. SEPTEMBER 1989
9 1 150 I. F. ANDERSON ET AL. I I I 1IA III FIG. 6 IV Modified staging system of Berndt and Harty. The addition of Stage IIA enables the development of subchondral cysts as a sequela of Stage I to be recognized and classified. See text for full explanation. ture, but this fracture had actually started as Stage II and progressed to Stage IV. In three of the series3, difficulties were reported in differentiating between Stages II and III, and these stages were combined. Using the advantages that are provided by magnetic resonance imaging, we re-examined the staging criteria of Berndt and Harty and made modifications (Fig. 6). Stage I - Subchondral Trabecular Compression No diagnostic changes are visible on the plain radiographs in trabecular compression. However, if an osteochondral fracture is suspected clinically and the plain radiograph is negative, scintigraphy can aid in assessing whether or not bone has been injured. If it has, the diagnosis can then be established by magnetic resonance imaging. As previously discussed, an area of abnormality in the cancellous bone marrow of the talus was present on the Tlweighted image in two patients; this area was shown to be largely fluid on the T2-weighted image. With further study of the ability of magnetic resonance imaging to show marrow edema, it may be advisable in the future to form a subgroup within Stage I, perhaps Stage IA, to separately classify this change. These lesions differ from the other Stage-I lesions in their appearance on magnetic resonance images and scintiscans, and probably also in their prognosis. and A typical Stage-I lesion is shown in Figs. 2-A, 2-B, 2-C. Stage II - Incomplete Separation of the Fragment Incomplete separation of the osteochondral fragment can be assessed well by either computerized tomography or magnetic resonance imaging (Fig. 4-B). Assignment of this stage to a fracture requires the demonstration of the attachment of the fragment. Stage I/A - Formation of a Subchondral Cyst Stage-I fractures may progress not only to an attached or unattached fragment, but to formation of a subchondral cyst, as was reported by Flick and Gould. This sequel of a Stage-I fracture, with resorption of necrotic trabeculae and formation of a cyst, was seen in eight of our patients (Table I). A Stage-hA classification allows this change to be recognized. Rhaney and Lamb suggested that subchondral cysts develop in areas of post-traumatic necrosis of bone. They found metaplastic cartilage, and osteoclastic activity with cellular and vascular granulation tissue in the wall of the cysts, which was histologically similar to that seen at fracture sites. Ondrouch, Ferguson, and Resnick et al. have supported these findings. Resnick et al. noted frequent cornmunications between the joint space and the subchondral cysts as well as dislocated pieces of articuiar cartilage within the cysts. The pathogenesis of osteonecrosis was well presented by Sweet and Madewell. They described the progressive stages of the host response that follows the initial death of hematopoietic cells, bone, and bone marrow. The response, consisting of fluid transudate, fibrin production, and inflammatory-cell infiltration, progresses to form a reactive interface around the area of osteonecrosis. This sharp line of demarcation can be appreciated by magnetic resonance imaging in more chronic lesions, the abnormal area being well separated from the surrounding normal bone marrow. As the interface between living and dead bone is delineated by THE JOURNAL OF BONE AND JOINT SURGERY
10 OSTEOCHONDRAL FRACTURES OF THE DOME OF THE TALUS 1151 INJURY PLAIN RADIOGRAPH Os ABNORMAL ( Shows teochondral fracture) V N NORMAL SCINTIGRAPH NEGATIVE C.T. POSITIVE OTHER DIAGNOSIS AND TREATMENT \/ M.R.I. TREATMENT for (C.T. progress monitoring) used FIG. 7 The diagnosis of osteochondral fracture should always be considered in a patient who has a problem of the ankle that persists for more than six weeks after an inversion injury. CT. = computerized tomography and M.R.I. = magnetic resonance imaging. by osteoblastic activity and resorption of the necrotic debris, it is not difficult to envisage the formation of a cyst. A typical appearance of a cyst on magnetic resonance imaging is shown in Figs. 1-A, 1-B, 1-C, 5-D, and 5-E. Stage III - Unattached, Undisplaced Fragment When an attachment to the talus cannot be demonstrated, but the fragment is undisplaced, the fracture is Stage II. In the T2-weighted image, the presence of synovial fluid around a large fragment can help to differentiate between Stages II and III. In practice, however, this advantage of magnetic resonance imaging does not appear to be important, and computerized tomography is the better means of identifying small, separated fragments. It is sometimes difficult to identify loose bodies on magnetic resonance images, although this problem is rapidly being overcome with the development of gradient-echo techniques. Nevertheless, magnetic resonance imaging currently appears to have no major advantage over computerized tomography in defining the staging of this group of fractures. Stage-lilA fractures, as described in Berndt and Harty s system of classification, apparently refers to a theoretical transient position of the fragment. This stage has not been accepted as important by other authors, and it was not encountered in our series. Stage IV - Displaced Fragment The only patient who had a Stage-IV lesion in this series was operated on before magnetic resonance imaging could be arranged. However, magnetic resonance imaging was performed two months postoperatively to assess the progress after treatment, and the defect was noted to be filled with fluid. An additional examination was planned to see if fibrocartilage filled the defect, as has been shown to occur in similar osteochondral defects in the knee joint. The natural history of an osteochondral fracture has been discussed in the. Irrespective of stage, healing of the fragment can occur only if the fracture is undisplaced or is reduced and immobilized until union can take place. The blood supply of the compressed or separated fragment is interrupted at the fracture line with continuing movement, and the ingrowing capillaries are sheared off. In addition, Stage-il lesions can progress to Stage The alternating application and release of pressure against the attachment of the Stage-il lesion eventually causes separation. When this occurs, healing is prevented, as the fragment becomes avascular and is encased in fibrous or fibrocartilaginous tissue. To summarize, trauma may produce a Stage-I to Stage- IV lesion at the time of injury, or a fracture may progress from an initial Stage I or II to Stage IIA, ifi, or IV, if it is inadequately immobilized. We do not know why Group-i patients predominantly had fractures of the medial side of the dome of the talus and patients in Group 2 mainly had lateral fractures; however, similar findings were reported by Blom and Strijk. The relationship between osteochondral fractures and trauma has been discussed3 6 8 All of the lateral fractures in these previous series were associated directly with a preceding inversion injury that caused a sprain of the ankle, whereas the medial lesions occasionally did not appear to follow recognized trauma. All of our patients in Group 2 had a sprain of the ankle that was severe enough for them to visit the casualty department of our hospital and to warrant immediate radiographic examination. In contrast, VOL. 71-A, NO. 8, SEPTEMBER 1989
11 1152 I. F. ANDERSON ET AL. six of the fourteen patients in Group 1, all of whom had a medial lesion, had some delay in seeking medical advice and in having an initial radiographic examination. The explanation for this apparent difference in the severity of symptoms may simply be that the severity of the associated ligamentous injury is greater with lateral lesions. Our treatment for Stage-I and Stage-Il fractures has been immobilization for six weeks. Even though healing may appear to have occurred, these patients should be followed for at least three years, as the lesion may progress to a higher stage at a later date. The experience of most authors, in the long term, has been that conservative treatment is often disappointing and that an operation is eventually necessary.2,8,14.15,22 An operation has been our treatment of choice for patients who have a Stage-hA, III, or IV fracture. In StagehA lesions, the cyst is deroofed and the base of the crater is drilled down to bleeding bone. Stage-Ill and Stage-IV fractures are managed by arthroscopic removal of the separated fragment, followed by curetting or drilling of the fracture bed down to bleeding bone. Although we have not yet established a firm regimen of treatment, it is planned to follow this group of patients as an ongoing study. We have, however, established a diagnostic protocol (Fig. 7). Whatever the final treatment regimen may be, staging, and, particularly, differentiating between Stage-I! and Stage-Ill fractures, is important. Patients who are suspected clinically of having an osteochondral fracture, but who have apparently negative plain radiographs, should be assessed by scintigraphy, and those who have positive scintiscans should have magnetic resonance imaging. Magnetic resonance imaging does not offer any major benefits to patients who have an abnormal plain radiograph; computerized tomography was shown to be adequate for staging the fractures in this group of patients in all but one instance. If plain radiography had been the only diagnostic procedure that was performed in our patients, fourteen of the fractures would not have been diagnosed. NOTE: The authors thank Hanimex Pty..the Australian agent for Fuji film. for their help in preparing the illuorations, and Sandra Huggett and Gillian Barber for their help. References 1. ALEXANDER, A. H., and LICHTMAN, D. M. : Surgical Treatment of Transchondral Talar-Dome Fractures (Osteochondritis Dissecans). Long-Term Follow-up. J. Bone and Joint Surg., 62-A: , June BERNDT, A. L., and HARTY, MICHAEL: Transchondral Fractures (Osteochondritis Dissecans) of the Talus. J. Bone and Joint Surg., 41-A: , Sept BLOM, J. M. H., and STRIJK, S. P. : Lesions of the Trochlea Tali. Osteochondral Fractures and Osteochondritis Dissecans of the Trochlea Tali. Radiol. Clin., 44: , BRAND, R. L. ; BLACK, H. M.; and Cox, J. S.: The Natural History of Inadequately Treated Ankle Sprain. Am. J. Sports Med., 5: , CAMERON, B. M. : Osteochondritis Dissecans of the Ankle Joint. Report of a Case Simulating a Fracture of the Talus. J. Bone and Joint Surg., 38-A: , 884, July CANALE, S. T., and BELDING, R. H.: Osteochondral Lesions of the Talus. J. Bone and Joint Surg., 62-A: , Jan COLTART, W. D.: Aviator s Astragalus. J. Bone and Joint Surg., 34-B(4): , DAVIDSON, A. M. ; STEELE, H. D. ; MACKENZIE, D. A. ; and PENNY, J. A. : A Review of Twenty-one Cases of Transchondral Fracture of the Talus. J. Trauma, 7: , FERGUSON, A. B., JR. : The Pathological Changes in Degenerative Arthritis of the Hip and Treatment by Rotational Osteotomy. J. Bone and Joint Surg., 46-A: , Sept FIORE, R. D., and LEARD, J. S.: A Functional Approach in the Rehabilitation of the Ankle and Rear Foot. Athlet. Train., 15: , I 1. FLICK, A. B., and GOULD, NATHANIEL: Osteochondritis Dissecans of the Talus (Transchondrai Fractures of the Talus): Review of the Literature and New Surgical Approach for Medial Dome Lesions. Foot and Ankle, 5: , HUYLEBROEK, J. F. ; MARTENS, M. ; and SIMoN, J. P. : Transchondral Talar Dome Fracture. Arch. Orthop. and Traumat. Surg., 104: , KEENE, J. S., and LANGE, R. H.: Diagnostic Dilemmas in Foot and Ankle Injuries. J. Am. Med. Assn., 256: , MUKHERJEE, S. K., and YOUNG, A. B.: Dome Fracture of the Talus. A Report of Ten Cases. J. Bone and Joint Surg., 55-B(2): , NEWBERG, A. H.: Osteochondral Fractures of the Dome of the Talus. British J. Radiol., 52: , O FARRELL, T. A., and COSTELLO, B. G. : Osteochondritis Dissecans of the Talus. The Late Results of Surgical Treatment. J. Bone and Joint Surg., 64-B(4): , ONDROUCH, A. S.: Cyst Formation in Osteoarthritis. J. Bone and Joint Surg., 45-B(4): , RESNICK, DONALD; NIWAYAMA, GEN; and COUTTS, R. D.: Subchondral Cysts (Geodes) in Arthritic Disorders: Pathologic and Radiographic Appearance of the Hip Joint. Am. J. Roentenol., 128: , RHANEY, K., and LAMB, D. W.: The Cysts of Osteoarthritis of the Hip. A Radiological and Pathological Study. J. Bone and Joint Surg., 37- B(4): , SoLoMON, M. A. ; GILULA, L. A. ; OLon, L. M.; OL0Fr, JOAN; and COMPTON, TERRY: Scanning of the Foot and Ankle: 1. Normal Anatomy. Am. J. Roentgenol., 146: , SWEET, D. E., and MADEWELL, J. E. : Pathogenesis of Osteonecrosis. in Diagnosis of Bone and Joint Disorders. With Emphasis on Articular Abnormalities, edited by D. Resnick and Gen Niwayama. Vol. 3, pp Philadelphia, W. B. Saunders, THOMPSON, J. P., and LOOMER, R. L.: Osteochondral Lesions of the Talus in a Sports Medicine Clinic. A New Radiographic Technique and Surgical Approach. Am. J. Sports Med., 12: , Evaluation of Transchondral Dome Fractures of the Talus. J. Foot Surg., 26: WELLS, D., ant OL0FF-S0L0M0N, J.: Radiographic , ThE JOURNAL OF BONE AND JOINT SURGERY
Posttraumatic subchondral bone contusions and fractures of the talotibial joint: Occurrence of kissing lesions
 KISSING CONTUSIONS CHAPTER 7 Posttraumatic subchondral bone contusions and fractures of the talotibial joint: Occurrence of kissing lesions Elizabeth S. Sijbrandij 1, Ad P.G. van Gils 1, Jan Willem K.
KISSING CONTUSIONS CHAPTER 7 Posttraumatic subchondral bone contusions and fractures of the talotibial joint: Occurrence of kissing lesions Elizabeth S. Sijbrandij 1, Ad P.G. van Gils 1, Jan Willem K.
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2, Patrick Smith, M.D. 2, and Larry S. Matthews, M.D. 2
 Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Persistent ankle pain after inversion lesions: what the radiologist must look for
 Persistent ankle pain after inversion lesions: what the radiologist must look for Poster No.: P-0118 Congress: ESSR 2016 Type: Authors: Keywords: DOI: Educational Poster R. Leao, L. C. Zattar-Ramos, E.
Persistent ankle pain after inversion lesions: what the radiologist must look for Poster No.: P-0118 Congress: ESSR 2016 Type: Authors: Keywords: DOI: Educational Poster R. Leao, L. C. Zattar-Ramos, E.
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
June 2013 Case Study. Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital
 June 2013 Case Study Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital Chief Complaint: Right ankle pain HPI: A 10 year old female dancer presents to the clinic with a five day history
June 2013 Case Study Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital Chief Complaint: Right ankle pain HPI: A 10 year old female dancer presents to the clinic with a five day history
A Patient s Guide to Osteochondritis Dissecans of the Talus. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Osteochondritis Dissecans of the Talus Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly
A Patient s Guide to Osteochondritis Dissecans of the Talus Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
17/10/2017. Foot and Ankle
 17/10/2017 Alicia M. Yochum RN, DC, DACBR, RMSK Foot and Ankle Plantar Fasciitis Hallux Valgus Deformity Achilles Tendinosis Posterior Tibialis Tendon tendinopathy Stress Fracture Ligamentous tearing Turf
17/10/2017 Alicia M. Yochum RN, DC, DACBR, RMSK Foot and Ankle Plantar Fasciitis Hallux Valgus Deformity Achilles Tendinosis Posterior Tibialis Tendon tendinopathy Stress Fracture Ligamentous tearing Turf
Post-traumatic osteonecrosis of distal tibia
 Injury Extra (2007) 38, 262 266 www.elsevier.com/locate/inext CASE REPORT Post-traumatic osteonecrosis of distal tibia D. Chakravarty a, *, A. Khanna a,1, A. Kumar b,2 a Department of Orthopaedics, Peterborough
Injury Extra (2007) 38, 262 266 www.elsevier.com/locate/inext CASE REPORT Post-traumatic osteonecrosis of distal tibia D. Chakravarty a, *, A. Khanna a,1, A. Kumar b,2 a Department of Orthopaedics, Peterborough
Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions
 Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions Orthopaedic Opinion Online is a website designed to provide information to patients who have
Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions Orthopaedic Opinion Online is a website designed to provide information to patients who have
From the Middlesex Hospital, London
 INSTABILITY OF THE FOOT AFFER INJURIES TO THE LATERAL LIGAMENT OF THE ANKLE M. A. R. FREEMAN, LONDON, ENGLAND From the Middlesex Hospital, London The tendency for the foot to give way (a complaint here
INSTABILITY OF THE FOOT AFFER INJURIES TO THE LATERAL LIGAMENT OF THE ANKLE M. A. R. FREEMAN, LONDON, ENGLAND From the Middlesex Hospital, London The tendency for the foot to give way (a complaint here
Outline. Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t
 Ankle Injuries Outline Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t Anatomy: Ankle Mortise Bony Anatomy Lateral Ligament Complex Medial Ligament Complex Ankle Sprains
Ankle Injuries Outline Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t Anatomy: Ankle Mortise Bony Anatomy Lateral Ligament Complex Medial Ligament Complex Ankle Sprains
MR imaging of the knee in marathon runners before and after competition
 Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
IMAGING TECHNIQUES CHAPTER 4. Imaging techniques
 IMAGING TECHNIQUES Imaging techniques 23 4.1. Conventional radiographic findings Conventional radiography, tomography, arthrography and stress views have traditionally been used for imaging the ankle and
IMAGING TECHNIQUES Imaging techniques 23 4.1. Conventional radiographic findings Conventional radiography, tomography, arthrography and stress views have traditionally been used for imaging the ankle and
Transchondral Fractures of the Talus on an lnversion Injury of the Ankle: A Frequently Overlooked Diagnosis
 0196-6011 /87/0807-0362$02.00/0 THE JOURNAL OF ORTHOPAEO~C AND SPORTS PHYSICAL THERAPY Copyright 0 1987 by The Orthopaedic and Sports Physical Therapy Sections of the American Physical Therapy Association
0196-6011 /87/0807-0362$02.00/0 THE JOURNAL OF ORTHOPAEO~C AND SPORTS PHYSICAL THERAPY Copyright 0 1987 by The Orthopaedic and Sports Physical Therapy Sections of the American Physical Therapy Association
Avascular Necrosis of the Foot. Dr. Hema Choudur MD, FRCPC Associate Professor. Dept. of Radiology. McMaster University, Hamilton, Canada.
 Avascular Necrosis of the Foot Dr. Hema Choudur MD, FRCPC Associate Professor. Dept. of Radiology. McMaster University, Hamilton, Canada. Avascular Necrosis: Pathophysiology Ischemia to the bone from oxygen
Avascular Necrosis of the Foot Dr. Hema Choudur MD, FRCPC Associate Professor. Dept. of Radiology. McMaster University, Hamilton, Canada. Avascular Necrosis: Pathophysiology Ischemia to the bone from oxygen
Ankle Replacement Surgery
 Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation *
 Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Ankle Arthroscopy PAULO ROCKETT, M.D. Porto Alegre Brazil
 Ankle Arthroscopy PAULO ROCKETT, M.D. Porto Alegre Brazil Ankle sprains are among the most common injuries in sports and at work. Between 20 and 40% of patients treated with conservative therapy may have
Ankle Arthroscopy PAULO ROCKETT, M.D. Porto Alegre Brazil Ankle sprains are among the most common injuries in sports and at work. Between 20 and 40% of patients treated with conservative therapy may have
October 1999, Supplement 1 Volume 15 Number 7
 October 1999, Supplement 1 Volume 15 Number 7
October 1999, Supplement 1 Volume 15 Number 7
Musculoskeletal Imaging What to order? Brian Cole, MD
 Musculoskeletal Imaging What to order? Brian Cole, MD my background: 1994 University of Illinois 1998 MD University of Illinois College of Medicine 1999-2003 Diagnostic Radiology Mayo Clinic 2004 Fellowship
Musculoskeletal Imaging What to order? Brian Cole, MD my background: 1994 University of Illinois 1998 MD University of Illinois College of Medicine 1999-2003 Diagnostic Radiology Mayo Clinic 2004 Fellowship
emoryhealthcare.org/ortho
 COMMON SOCCER INJURIES Oluseun A. Olufade, MD Assistant Professor, Department of Orthopedics and PM&R 1/7/18 GOALS Discuss top soccer injuries and treatment strategies Simplify hip and groin injuries in
COMMON SOCCER INJURIES Oluseun A. Olufade, MD Assistant Professor, Department of Orthopedics and PM&R 1/7/18 GOALS Discuss top soccer injuries and treatment strategies Simplify hip and groin injuries in
The Kienböck disease and scaphoid fractures. Mariusz Bonczar
 The Kienböck disease and scaphoid fractures Mariusz Bonczar The Kienböck disease and scaphoid fractures Mariusz Bonczar Kienböck disease personal experience My special interest for almost 25 years Thesis
The Kienböck disease and scaphoid fractures Mariusz Bonczar The Kienböck disease and scaphoid fractures Mariusz Bonczar Kienböck disease personal experience My special interest for almost 25 years Thesis
A Patient s Guide to Osteochondritis Dissecans of the Knee
 A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
July 2011 Case of the Month. By Matt Grady, MD
 July 2011 Case of the Month By Matt Grady, MD CC: Knee Pain - Osteochondritis Dissecans or not? A Case Comparison HPI: The first patient is a 12 year old female swimmer with right knee pain. The pain started
July 2011 Case of the Month By Matt Grady, MD CC: Knee Pain - Osteochondritis Dissecans or not? A Case Comparison HPI: The first patient is a 12 year old female swimmer with right knee pain. The pain started
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
The prevalence of osteochondritis
 Brief Communication Communication abrégée OSTEOCHONDRITIS DISSECANS OF THE TALAR DOME TREATED WITH AN OSTEOCHONDRAL AUTOGRAFT Edward Chang, BSc(PT);* Eric Lenczner, MD The prevalence of osteochondritis
Brief Communication Communication abrégée OSTEOCHONDRITIS DISSECANS OF THE TALAR DOME TREATED WITH AN OSTEOCHONDRAL AUTOGRAFT Edward Chang, BSc(PT);* Eric Lenczner, MD The prevalence of osteochondritis
Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation
 Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings
 Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Reinsertion of an inverted osteochondral lesion of the talus; a case report
 Reinsertion of an inverted osteochondral lesion of the talus; a case report T. Schepers MD PhD, P.P. De Rooij MD, E.M.M. Van Lieshout PhD, P. Patka MD PhD Erasmus MC, University Medical Center Rotterdam,
Reinsertion of an inverted osteochondral lesion of the talus; a case report T. Schepers MD PhD, P.P. De Rooij MD, E.M.M. Van Lieshout PhD, P. Patka MD PhD Erasmus MC, University Medical Center Rotterdam,
Radiologic Imaging Magnetic Resonance Imaging (MRI)
 Radiologic Imaging X-ray has always been the golden rule in diagnosing and treating podiatric patients. Unfortunately, for some patients the diagnosis is not as evident. That is when we need to utilize
Radiologic Imaging X-ray has always been the golden rule in diagnosing and treating podiatric patients. Unfortunately, for some patients the diagnosis is not as evident. That is when we need to utilize
Osteochondritis Dissecans
 Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Ankle impingement syndromes - pictorial review.
 Ankle impingement syndromes - pictorial review. Poster No.: P-0148 Congress: ESSR 2015 Type: Educational Poster Authors: R. D. T. Mesquita, J. Pinto, J. L. Rosas, A. Vieira ; Porto/PT, 1 2 2 3 1 1 3 Matosinhos/PT,
Ankle impingement syndromes - pictorial review. Poster No.: P-0148 Congress: ESSR 2015 Type: Educational Poster Authors: R. D. T. Mesquita, J. Pinto, J. L. Rosas, A. Vieira ; Porto/PT, 1 2 2 3 1 1 3 Matosinhos/PT,
Ankle impingement syndromes - pictorial review.
 Ankle impingement syndromes - pictorial review. Poster No.: P-0148 Congress: ESSR 2015 Type: Educational Poster Authors: R. D. T. Mesquita, J. Pinto, J. L. Rosas, A. Vieira ; Porto/PT, 1 2 2 3 1 1 3 Matosinhos/PT,
Ankle impingement syndromes - pictorial review. Poster No.: P-0148 Congress: ESSR 2015 Type: Educational Poster Authors: R. D. T. Mesquita, J. Pinto, J. L. Rosas, A. Vieira ; Porto/PT, 1 2 2 3 1 1 3 Matosinhos/PT,
Talus Fractures: When and Why on Screws and Plates
 Talus Fractures: When and Why on Screws and Plates Frank A. Liporace, MD Associate Professor Director of Orthopaedic Research New York University / Hospital for Joint Diseases, NY, NY Director Orthopaedic
Talus Fractures: When and Why on Screws and Plates Frank A. Liporace, MD Associate Professor Director of Orthopaedic Research New York University / Hospital for Joint Diseases, NY, NY Director Orthopaedic
Osteonecrosis - Spectrum of imaging findings
 Osteonecrosis - Spectrum of imaging findings Poster No.: C-1861 Congress: ECR 2016 Type: Educational Exhibit Authors: P. Ninitas, A. L. Amado Costa, A. Duarte, I. Távora ; Lisbon/ 1 1 2 1 1 2 PT, Costa
Osteonecrosis - Spectrum of imaging findings Poster No.: C-1861 Congress: ECR 2016 Type: Educational Exhibit Authors: P. Ninitas, A. L. Amado Costa, A. Duarte, I. Távora ; Lisbon/ 1 1 2 1 1 2 PT, Costa
Case Iselin's disease in a Thai boxer.
 Case 13609 Iselin's disease in a Thai boxer. Joris De Win 1, 3, Filip Vanhoenacker 2, 4, Els Goossens3 1: Department of Physical Medicine and Rehabilitation; University Ghent (UGent), Belgium; Email:de_win_joris@hotmail.com
Case 13609 Iselin's disease in a Thai boxer. Joris De Win 1, 3, Filip Vanhoenacker 2, 4, Els Goossens3 1: Department of Physical Medicine and Rehabilitation; University Ghent (UGent), Belgium; Email:de_win_joris@hotmail.com
CHAPTER 8. Elizabeth S. Sijbrandij 1, Ad P.G. van Gils 1, Jan Willem K. Louwerens 2, Eduard E. de Lange 3
 BONE VIABILITY CHAPTER 8 Osteochondritis dissecans of the talar dome: Evaluation of bone viability with dynamic gadolinium-enhanced MR imaging in comparison with dynamic bone scintigraphy. Elizabeth S.
BONE VIABILITY CHAPTER 8 Osteochondritis dissecans of the talar dome: Evaluation of bone viability with dynamic gadolinium-enhanced MR imaging in comparison with dynamic bone scintigraphy. Elizabeth S.
Ankle Sprain. 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) Website: philip-bayliss.com
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Ankle Sprain An Ankle sprain is one of the most common musculoskeletal injuries. Patients typically describe
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Ankle Sprain An Ankle sprain is one of the most common musculoskeletal injuries. Patients typically describe
Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
 Case Reports in Radiology Volume 2016, Article ID 8739362, 4 pages http://dx.doi.org/10.1155/2016/8739362 Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
Case Reports in Radiology Volume 2016, Article ID 8739362, 4 pages http://dx.doi.org/10.1155/2016/8739362 Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
Osteochondral Lesions of the Talus A Unique Surgical Approach. Mark J. Mendeszoon, DPM, FACFAS, FACFAOM
 Osteochondral Lesions of the Talus A Unique Surgical Approach Mark J. Mendeszoon, DPM, FACFAS, FACFAOM Introduction Osteochondral lesions of the talar dome can cause significant functional impairment and
Osteochondral Lesions of the Talus A Unique Surgical Approach Mark J. Mendeszoon, DPM, FACFAS, FACFAOM Introduction Osteochondral lesions of the talar dome can cause significant functional impairment and
Mary Lloyd Ireland, M.D. Associate Professor University of Kentucky Dept. of Orthopaedic Surgery and Sports Medicine Lexington, Kentucky
 Common Ankle Injuries: Diagnosis and Treatment Mary Lloyd Ireland, M.D. Associate Professor University of Kentucky Dept. of Orthopaedic Surgery and Sports Medicine Lexington, Kentucky Disclaimer Slide
Common Ankle Injuries: Diagnosis and Treatment Mary Lloyd Ireland, M.D. Associate Professor University of Kentucky Dept. of Orthopaedic Surgery and Sports Medicine Lexington, Kentucky Disclaimer Slide
Impingement Syndromes of the Ankle. Noaman W Siddiqi MD 5/4/2006
 Impingement Syndromes of the Ankle Noaman W Siddiqi MD 5/4/2006 Ankle Impingement Overview Clinical DX Increasingly recognized cause of chronic ankle pain Etiology can be soft tissue or osseous Professional
Impingement Syndromes of the Ankle Noaman W Siddiqi MD 5/4/2006 Ankle Impingement Overview Clinical DX Increasingly recognized cause of chronic ankle pain Etiology can be soft tissue or osseous Professional
4/28/2010. Fractures. Normal Bone and Normal Ossification Bone Terms. Epiphysis Epiphyseal Plate (physis) Metaphysis
 Fractures Normal Bone and Normal Ossification Bone Terms Epiphysis Epiphyseal Plate (physis) Metaphysis Diaphysis 1 Fracture Classifications A. Longitudinal B. Transverse C. Oblique D. Spiral E. Incomplete
Fractures Normal Bone and Normal Ossification Bone Terms Epiphysis Epiphyseal Plate (physis) Metaphysis Diaphysis 1 Fracture Classifications A. Longitudinal B. Transverse C. Oblique D. Spiral E. Incomplete
Osteochondral lesions were first described by Konig
 155 Osteochondral Lesions of the Talar Dome Alexander Finger, M.D., and Steven C. Sheskier, M.D. Osteochondral lesions were first described by Konig in 1888. 1 He theorized that spontaneous necrosis was
155 Osteochondral Lesions of the Talar Dome Alexander Finger, M.D., and Steven C. Sheskier, M.D. Osteochondral lesions were first described by Konig in 1888. 1 He theorized that spontaneous necrosis was
Priorities Forum Statement GUIDANCE
 Priorities Forum Statement Number 21 Subject Knee Arthroscopy including arthroscopic knee washouts Date of decision November 2016 Date refreshed March 2017 Date of review November 2018 Osteoarthritis of
Priorities Forum Statement Number 21 Subject Knee Arthroscopy including arthroscopic knee washouts Date of decision November 2016 Date refreshed March 2017 Date of review November 2018 Osteoarthritis of
Osteochondritis Dissecans of the Knee. M Lucas Murnaghan MD, MEd, FRCSC
 Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
Acute Ankle Injuries, Part 1: Office Evaluation and Management
 t June 08, 2009 Obesity [1] Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the
t June 08, 2009 Obesity [1] Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the
ruptures of the lateral ligaments of the
 The accuracy of three-dimensional magnetic resonance imaging in the diagnosis of ruptures of the lateral ligaments of the ankle* EDDY F. C. VERHAVEN, MD, MARYAM SHAHABPOUR, MD, FRANK W. J. HANDELBERG,
The accuracy of three-dimensional magnetic resonance imaging in the diagnosis of ruptures of the lateral ligaments of the ankle* EDDY F. C. VERHAVEN, MD, MARYAM SHAHABPOUR, MD, FRANK W. J. HANDELBERG,
Ankle Injuries. Ankle Sprain. Range of Motion. The most likely diagnosis is lateral ligament sprain. Dorsiflexion Plantarflexion Inversion
 Ankle Injuries Dr Peter Brukner, OAM Sports Physician Associate Professor Centre for Sports Medicine Research & Education The University of Melbourne Adjunct Professor School of Human Movement Studies
Ankle Injuries Dr Peter Brukner, OAM Sports Physician Associate Professor Centre for Sports Medicine Research & Education The University of Melbourne Adjunct Professor School of Human Movement Studies
MRI findings associated with distal. Tibiofibular Syndesmosis Injury
 Kevin W. Brown 1 William B. Morrison 1 Mark E. Schweitzer 1,2 J. ntoni Parellada 1 Henry Nothnagel 1 Received January 6, 2003; accepted after revision July 30, 2003. 1 Department of Radiology, Thomas Jefferson
Kevin W. Brown 1 William B. Morrison 1 Mark E. Schweitzer 1,2 J. ntoni Parellada 1 Henry Nothnagel 1 Received January 6, 2003; accepted after revision July 30, 2003. 1 Department of Radiology, Thomas Jefferson
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE
 THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
Triplane fracture of the ankle is an uncommon injury
 A Case Report & Literature Review Intramalleolar Triplane Fracture With Osteochondral Talar Defect Wendy L. Heusch, DO, and Henry W. Albers, MD Triplane fracture of the ankle is an uncommon injury that
A Case Report & Literature Review Intramalleolar Triplane Fracture With Osteochondral Talar Defect Wendy L. Heusch, DO, and Henry W. Albers, MD Triplane fracture of the ankle is an uncommon injury that
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
Magnetic resonance imaging of femoral head development in roentgenographically normal patients
 Skeletal Radiol (1985) 14:159-163 Skeletal Radiology Magnetic resonance imaging of femoral head development in roentgenographically normal patients Peter J. Littrup, M.D. 1, Alex M. Aisen, M.D. 2, Ethan
Skeletal Radiol (1985) 14:159-163 Skeletal Radiology Magnetic resonance imaging of femoral head development in roentgenographically normal patients Peter J. Littrup, M.D. 1, Alex M. Aisen, M.D. 2, Ethan
Skeletally Immature Athletes Ununited Osteochondral Fractures of the Distal Fibula
 Chronic, Painful Ankle Instability in Skeletally Immature Athletes Ununited Osteochondral Fractures of the Distal Fibula Brian D. Busconi,* MD, and Arthur M. Pappas, MD From the Department of Orthopedics
Chronic, Painful Ankle Instability in Skeletally Immature Athletes Ununited Osteochondral Fractures of the Distal Fibula Brian D. Busconi,* MD, and Arthur M. Pappas, MD From the Department of Orthopedics
BCCH Emergency Department LOWER LIMB INJURIES Resource pack
 1 BCCH Emergency Department LOWER LIMB INJURIES Resource pack Developed by: Rena Heathcote RN. 2 Knee Injuries The knee joint consists of a variety of structures including: 3 bones (excluding the patella)
1 BCCH Emergency Department LOWER LIMB INJURIES Resource pack Developed by: Rena Heathcote RN. 2 Knee Injuries The knee joint consists of a variety of structures including: 3 bones (excluding the patella)
CT Findings of Traumatic Posterior Hip Dislocation after Reduction 1
 CT Findings of Traumatic Posterior Hip Dislocation after Reduction 1 Sung Kyoung Moon, M.D., Ji Seon Park, M.D., Wook Jin, M.D. 2, Kyung Nam Ryu, M.D. Purpose: To evaluate the CT images of reduced hips
CT Findings of Traumatic Posterior Hip Dislocation after Reduction 1 Sung Kyoung Moon, M.D., Ji Seon Park, M.D., Wook Jin, M.D. 2, Kyung Nam Ryu, M.D. Purpose: To evaluate the CT images of reduced hips
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Physeal injuries of the ankle joint constitute 11% of all
 ORIGINAL ARTICLE Outcome of Physeal and Epiphyseal Injuries of the Distal Tibia With Intra-Articular Involvement Savvas P. Nenopoulos, MD, Vasilios A. Papavasiliou, MD, and Athanasios V. Papavasiliou,
ORIGINAL ARTICLE Outcome of Physeal and Epiphyseal Injuries of the Distal Tibia With Intra-Articular Involvement Savvas P. Nenopoulos, MD, Vasilios A. Papavasiliou, MD, and Athanasios V. Papavasiliou,
Imaging of Articular Cartilage
 Clinical Imaging of Articular Cartilage Imaging of Articular Cartilage Prof. Dr. K. Verstraete Ghent University Introduction : Articular Cartilage Histology and biochemical composition Review of Imaging
Clinical Imaging of Articular Cartilage Imaging of Articular Cartilage Prof. Dr. K. Verstraete Ghent University Introduction : Articular Cartilage Histology and biochemical composition Review of Imaging
MRI of Pediatric Ankle and Foot. Mahesh Thapa, MD Associate Professor Seattle Children s University of Washington School of Medicine
 MRI of Pediatric Ankle and Foot Mahesh Thapa, MD Associate Professor Seattle Children s University of Washington School of Medicine Disclosures Under contract with Lippincott Williams and Wilkins (LWW)
MRI of Pediatric Ankle and Foot Mahesh Thapa, MD Associate Professor Seattle Children s University of Washington School of Medicine Disclosures Under contract with Lippincott Williams and Wilkins (LWW)
Fractures in the Immature Foot
 Fractures in the Immature Foot Kaye E. Wilkins, M.D. Clinical Professor Orthopaedics & Pediatrics University of Texas Health Science Center at San Antonio San Antonio, Texas (210) 692-1613 e-mail: drkwilkins@aol.com
Fractures in the Immature Foot Kaye E. Wilkins, M.D. Clinical Professor Orthopaedics & Pediatrics University of Texas Health Science Center at San Antonio San Antonio, Texas (210) 692-1613 e-mail: drkwilkins@aol.com
Arthroscopy Of the Ankle.
 Arthroscopy Of the Ankle www.fisiokinesiterapia.biz Ankle Arthroscopy Anatomy Patient setup Portal placement Procedures Complications Anatomy Portals Anterior Anteromedial Anterolateral Anterocentral Posterior
Arthroscopy Of the Ankle www.fisiokinesiterapia.biz Ankle Arthroscopy Anatomy Patient setup Portal placement Procedures Complications Anatomy Portals Anterior Anteromedial Anterolateral Anterocentral Posterior
Calcaneal Fractures in Children
 Journal of Pediatric Orthopaedics 18:469-474 1998 Lippincott-Raven Publishers, Philadelphi a Calcaneal Fractures in Children Suguru Inokuchi, M.D., Norio Usami, M.D., Eiichi Hiraishi, M.D., and Takeshi
Journal of Pediatric Orthopaedics 18:469-474 1998 Lippincott-Raven Publishers, Philadelphi a Calcaneal Fractures in Children Suguru Inokuchi, M.D., Norio Usami, M.D., Eiichi Hiraishi, M.D., and Takeshi
Hand and wrist emergencies
 Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
Arthroscopic Treatment of Osteochondral Talar Defects
 Arthroscopic Treatment of Osteochondral Talar Defects Christiaan J.A. van Bergen, MD, Ruben Zwiers, MSc, and C. Niek van Dijk, MD, PhD Based on an original article: J Bone Joint Surg Am. 2013 Mar 20;95(6):519-25.
Arthroscopic Treatment of Osteochondral Talar Defects Christiaan J.A. van Bergen, MD, Ruben Zwiers, MSc, and C. Niek van Dijk, MD, PhD Based on an original article: J Bone Joint Surg Am. 2013 Mar 20;95(6):519-25.
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Post-traumatic Osteoarthritis
 Post-traumatic Osteoarthritis Once the hammer has hit Dr. Arno Smit - WROSC Hazelmere Golf & Country Club April 11, 2013 Post-traumatic osteo-arthritis Common sequela of high energy impact injury Progressively
Post-traumatic Osteoarthritis Once the hammer has hit Dr. Arno Smit - WROSC Hazelmere Golf & Country Club April 11, 2013 Post-traumatic osteo-arthritis Common sequela of high energy impact injury Progressively
A Pictorial Review of Congenital Tarsal Coalition
 A Pictorial Review of Congenital Tarsal Coalition Poster No.: C-2305 Congress: ECR 2011 Type: Educational Exhibit Authors: J. Jethwa, M. Tapp; Torquay/UK Keywords: Musculoskeletal joint, Musculoskeletal
A Pictorial Review of Congenital Tarsal Coalition Poster No.: C-2305 Congress: ECR 2011 Type: Educational Exhibit Authors: J. Jethwa, M. Tapp; Torquay/UK Keywords: Musculoskeletal joint, Musculoskeletal
Imaging of Ankle and Foot pain
 Imaging of Ankle and Foot pain Pramot Tanutit, M.D. Department of Radiology Faculty of Medicine, Prince of Songkla University 1 Outlines Plain film: anatomy Common causes of ankle and foot pain Exclude:
Imaging of Ankle and Foot pain Pramot Tanutit, M.D. Department of Radiology Faculty of Medicine, Prince of Songkla University 1 Outlines Plain film: anatomy Common causes of ankle and foot pain Exclude:
AAP Boot Camp KNEE AND ANKLE EXAM
 AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
Ankle Ligament Injury: Don t Worry- It s Only a Sprain Wes Jackson MD Orthopaedic Foot & Ankle
 Ankle Ligament Injury: Don t Worry- It s Only a Sprain Wes Jackson MD Orthopaedic Foot & Ankle Outline I. Epidemiology II. Classification and Types of Sprains III. Anatomy IV. Clinical Assessment and Imaging
Ankle Ligament Injury: Don t Worry- It s Only a Sprain Wes Jackson MD Orthopaedic Foot & Ankle Outline I. Epidemiology II. Classification and Types of Sprains III. Anatomy IV. Clinical Assessment and Imaging
Ankle Arthritis PATIENT INFORMATION. The ankle joint. What is ankle arthritis?
 PATIENT INFORMATION Ankle Arthritis The ankle joint The ankle is a very complex joint. It is actually made up of two joints: the true ankle joint and the subtalar ankle joint. The ankle joint consists
PATIENT INFORMATION Ankle Arthritis The ankle joint The ankle is a very complex joint. It is actually made up of two joints: the true ankle joint and the subtalar ankle joint. The ankle joint consists
Rakesh Patel, MD 4/9/09
 Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
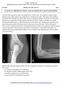 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 10/6/2012 Radiology Quiz of the Week # 93 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 10/6/2012 Radiology Quiz of the Week # 93 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Diagnosis of scaphoid fracture and dedicated extremity MRI
 504 Acta Ofthop Scand 1999; 70 (5): 504-508 Diagnosis of scaphoid fracture and dedicated extremity MRI Thomas Bretlau', Ole Maagaard Christensen*, Per Edstrom', Henrik S Thornsen' and Gunnar Schwarz Lausten2
504 Acta Ofthop Scand 1999; 70 (5): 504-508 Diagnosis of scaphoid fracture and dedicated extremity MRI Thomas Bretlau', Ole Maagaard Christensen*, Per Edstrom', Henrik S Thornsen' and Gunnar Schwarz Lausten2
Radiologic Pathologic Correlation of Intraosseous Lipomas. Tim Propeck 1, Mary Anne Bullard 1, John Lin 1, Kei Doi 2, William Martel 1
 Downloaded from www.ajronline.org by 148.251.232.83 on 04/10/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Radiologic Pathologic orrelation of Intraosseous
Downloaded from www.ajronline.org by 148.251.232.83 on 04/10/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Radiologic Pathologic orrelation of Intraosseous
Wilderness related musculoskeletal injury: role of bone scintigraphy
 Journal ofwilderness Medicine 4,407-411 (1993) ORIGINAL ARTICLE Wilderness related musculoskeletal injury: role of bone scintigraphy LISTON ORR, MD and ANDREW TAYLOR, Jr, MD* Department ofradiology, Emory
Journal ofwilderness Medicine 4,407-411 (1993) ORIGINAL ARTICLE Wilderness related musculoskeletal injury: role of bone scintigraphy LISTON ORR, MD and ANDREW TAYLOR, Jr, MD* Department ofradiology, Emory
Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A
 Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
Evaluation of Pediatric Foot Pain
 May 2006 Evaluation of Pediatric Foot Pain John Flibotte, Harvard Medical School Year III Our Patient AP is a 10 year old boy with chronic R foot pain 2 Anatomy of the Foot Manusov EG, et al. (1996), Part
May 2006 Evaluation of Pediatric Foot Pain John Flibotte, Harvard Medical School Year III Our Patient AP is a 10 year old boy with chronic R foot pain 2 Anatomy of the Foot Manusov EG, et al. (1996), Part
Sequalae of Ankle Sprains: Peri Articular Fractures of the Ankle in Sports Medicine.
 Sequalae of Ankle Sprains: Peri Articular Fractures of the Ankle in Sports Medicine www.fisiokinesiterapia.biz Chronic Ankle Pain The most common cause of chronic pain following an ankle sprain is a missed
Sequalae of Ankle Sprains: Peri Articular Fractures of the Ankle in Sports Medicine www.fisiokinesiterapia.biz Chronic Ankle Pain The most common cause of chronic pain following an ankle sprain is a missed
Utility of Dual-Energy CT to Evaluate Patients with Hip and Pelvis Pain in the ER Setting
 Utility of Dual-Energy CT to Evaluate Patients with Hip and Pelvis Pain in the ER Setting Johnson, T., Moran, E., Glazebrook, K., Leng, S., Fletcher, J., and McCollough, C. An educational review ER011
Utility of Dual-Energy CT to Evaluate Patients with Hip and Pelvis Pain in the ER Setting Johnson, T., Moran, E., Glazebrook, K., Leng, S., Fletcher, J., and McCollough, C. An educational review ER011
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium
 MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
"The Role of Dynamic Ultrasound and MRI in the poorly resolving ankle sprain."
 "The Role of Dynamic Ultrasound and MRI in the poorly resolving ankle sprain." Poster No.: P-0007 Congress: ESSR 2013 Type: Scientific Exhibit Authors: J. M. Zietkiewicz, P. Mercouris, M. C. Marshall;
"The Role of Dynamic Ultrasound and MRI in the poorly resolving ankle sprain." Poster No.: P-0007 Congress: ESSR 2013 Type: Scientific Exhibit Authors: J. M. Zietkiewicz, P. Mercouris, M. C. Marshall;
Achilles Tendonitis and Tears
 Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Clinical Case Series (vs. Case Study) Patient #1 Progression Male Soccer Athlete 5/26/2016
 Patellar Chondroplasty With Gel-One Cross-Linked Hyaluronate Injection for the Treatment of Grade III Patellar Chondromalacia in Collegiate Male Athletes: A Case Series David Tomchuk, MS, ATC, LAT, CSCS
Patellar Chondroplasty With Gel-One Cross-Linked Hyaluronate Injection for the Treatment of Grade III Patellar Chondromalacia in Collegiate Male Athletes: A Case Series David Tomchuk, MS, ATC, LAT, CSCS
New Evidence Suggests that Work Related Knee Pain with Degenerative Complications May Not Require Surgery
 4 th Quarter 2017 New Evidence Suggests that Work Related Knee Pain with Degenerative Complications May Not Require Surgery By: Michael Erdil MD, FACOEM Introduction It is estimated there are approximately
4 th Quarter 2017 New Evidence Suggests that Work Related Knee Pain with Degenerative Complications May Not Require Surgery By: Michael Erdil MD, FACOEM Introduction It is estimated there are approximately
Case Carpal coalition: 4 cases of a rare bony coalition between the capitate and trapezoid bone, with MRI findings in a symptomatic case.
 Case 12910 Carpal coalition: 4 cases of a rare bony coalition between the capitate and trapezoid bone, with MRI findings in a symptomatic case. M. Mespreuve 1, 2 K. De Cuyper 1 M. Vansevenant 1, 2 K. Verstraete
Case 12910 Carpal coalition: 4 cases of a rare bony coalition between the capitate and trapezoid bone, with MRI findings in a symptomatic case. M. Mespreuve 1, 2 K. De Cuyper 1 M. Vansevenant 1, 2 K. Verstraete
Clin Podiatr Med Surg 19 (2002) Index
 Clin Podiatr Med Surg 19 (2002) 335 344 Index Note: Page numbers of article titles are in bold face type. A Accessory soleus muscle, magnetic resonance imaging of, 300 Achilles tendon injury of, magnetic
Clin Podiatr Med Surg 19 (2002) 335 344 Index Note: Page numbers of article titles are in bold face type. A Accessory soleus muscle, magnetic resonance imaging of, 300 Achilles tendon injury of, magnetic
Sports Injuries of the Ankle and Ankle Arthritis. Mr Amit Amin Consultant Foot and Ankle Surgeon Parkside Hospital
 Sports Injuries of the Ankle and Ankle Arthritis Mr Amit Amin Consultant Foot and Ankle Surgeon Parkside Hospital Impingement Painful mechanical limitation of full ankle movement secondary to osseous
Sports Injuries of the Ankle and Ankle Arthritis Mr Amit Amin Consultant Foot and Ankle Surgeon Parkside Hospital Impingement Painful mechanical limitation of full ankle movement secondary to osseous
Anterior ankle impingement in sports Hrefna Thorbjorg Hakonardottir
 Anterior ankle impingement in sports Hrefna Thorbjorg Hakonardottir Anterior ankle impingement in sports Ankle impingement syndromes are classified by their anatomical location around the tibiotalar joint
Anterior ankle impingement in sports Hrefna Thorbjorg Hakonardottir Anterior ankle impingement in sports Ankle impingement syndromes are classified by their anatomical location around the tibiotalar joint
Monostotic Paget s Disease: A Case Report
 Chin J Radiol 2002; 27: 117-121 117 CASE REPORT Monostotic Paget s Disease: A Case Report CHI-CHEN HOU 1 CHI WEI LO 2 JINN-MING CHANG 1 CHING-CHERNG TZENG 3 Department of Diagnostic Radiology 1, Orthopedics
Chin J Radiol 2002; 27: 117-121 117 CASE REPORT Monostotic Paget s Disease: A Case Report CHI-CHEN HOU 1 CHI WEI LO 2 JINN-MING CHANG 1 CHING-CHERNG TZENG 3 Department of Diagnostic Radiology 1, Orthopedics
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/08/2012 Radiology Quiz of the Week # 102 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/08/2012 Radiology Quiz of the Week # 102 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
