Enlarged anterior cervical diskectomy and fusion in the treatment of severe localised ossification of the posterior longitudinal ligament
|
|
|
- Elaine Banks
- 5 years ago
- Views:
Transcription
1 Lei et al. Journal of Orthopaedic Surgery and Research (2016) 11:129 DOI /s z RESEARCH ARTICLE Open Access Enlarged anterior cervical diskectomy and fusion in the treatment of severe localised ossification of the posterior longitudinal ligament Tao Lei, Hui Wang, Tong Tong, Qinghua Ma, Linfeng Wang and Yong Shen * Abstract Background: Severe localised ossification of the posterior longitudinal ligament (OPLL) should be directly removed by anterior approach, but the exposure during anterior cervical diskectomy and fusion (ACDF) is restricted and may increase the risk of a cerebrospinal fluid (CSF) leak. Corpectomy is facilitated to extirpate the ossification, but it is relatively more invasive. The purpose of this study was to investigate the feasibility and clinical outcome of enlarged ACDF in treating severe localised OPLL. Methods: Twenty-four selective patients with severe localised OPLL who underwent enlarged ACDF from January 2011 to July 2013 were retrospectively investigated. The Japanese Orthopaedic Association (JOA) scales, visual analogue scale (VAS), occupyingrate(or),fusedsegmentheight (FSH), sagittal segmental alignment (SSA), range of motion (ROM), and complications were investigated. Results: After a mean 34.9-month follow-up, the mean JOA score increased from 9.5 ± 1.4 preoperatively to 14.1 ± 1.5 at the final follow-up (p < 0.05), while OR decreased from 58.9 ± 6.1 % pre- to 10.6 ± 5.5 % postoperatively (p < 0.05). The average VAS was 6.1 ± 1.8 preoperatively and 2.1 ± 1.4 at the final follow-up (p < 0.05). The SSA angles at the final follow-up increased 2.2 compared to the preoperative values (p < 0.05). The mean FSH increased 2.4 mm from pre- to postoperatively, but decreased 2.7 mm from postoperatively to final follow-up. The cervical ROM was not obviously reduced at the final follow-up (p > 0.05) because only one level was fixed. There were three cases of cerebrospinal fluid leakage, one case of haematoma, and one case showed transient neurological deterioration. Conclusions: Enlarged ACDF is an effective procedure for treating selective patients with severe localised OPLL. Using this technique, the retrovertebral OPLL can be removed through a one-level diskectomy and a corpectomy can be avoided. Trial registration: This study has been registered with the ResearchRegistry and the unique identifying number is researchregistry1365 (K ). It was retrospectively registered at 21 June 2016 and the first participant to the trial was at 4 January Keywords: Cervical, Anterior cervical diskectomy and fusion, Severe, Ossification of the posterior longitudinal ligament, Decompression * Correspondence: shenyonglaoshi@126.com Department of Spine Surgery, The Third Hospital of Hebei Medical University, The Key Laboratory of Orthopedic Biomechanics of Hebei Province, 139 Ziqiang Street, Shijiazhuang , Hebei, People s Republic of China The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Lei et al. Journal of Orthopaedic Surgery and Research (2016) 11:129 Page 2 of 8 Background Ossification of the posterior longitudinal ligament (OPLL) is a common cause of cervical myelopathy in Asian countries. Localised OPLL, with ossified mass on the disk space or at the posterior margin of vertebral body [1], is an indication of anterior decompression. However, severe OPLL with occupying rate (OR) more than 50 % poses a significant challenge for spinal surgeons. The exposure of the conventional diskectomy and intervertebral fusion is restricted, which may increase the risk of cerebrospinal fluid (CSF) leak and iatrogenic cord damage [2, 3]. Some surgeons prefer anterior corpectomy and fusion (ACCF) which is facilitated to extirpate the ossification [2, 4 6]. However, the ACCF is invasive with more intraoperative blood loss and higher postoperative complications [7, 8]. More importantly, the only partly involved vertebral body and the adjacent normal intervertebral disks were unfortunately sacrificed in the ACCF. Thus, how to safely and effectively remove the severe ossification through onelevel diskectomy needs to be further studied. In this article, a surgical technique of enlarged anterior cervical diskectomy and fusion (ACDF) was performed with common surgical instruments to excise the localised mass in selective patients, and ACCF was avoided in all cases. The clinical and radiological outcomes were evaluated. Methods Between January 2011 and July 2013, a total of 121 patients underwent surgical treatment for cervical OPLL in our department. We chose to perform anterior decompression when the pathological extent did not exceed three intervertebral levels; 24 consecutive patients presenting with localised OPLL underwent enlarged ACDF and were studied retrospectively. Inclusion criteria for this technique were as follows: (1) the retrovertebral OPLL was limited within half of the adjacent vertebral bodies (Fig. 1), and (2) the OR, defined as the maximum thickness of OPLL divided by anterior posterior diameter of the bony spinal canal on axial CT image, was more than 50 %. Patients with myelopathy caused by ossified disk herniation or spondylosis, with cervical ossification of the ligamentum flavum, or with a history of injury or previous surgery were excluded. This study had been approved by Ethics Committee of The Third Hospital of HeBei Medical University, and all patients signed informed consent. The approval number for this study is K The study comprised 15 men and 9 women with a mean age of 54.6 ± 8.1 years (39 67 years). Mean duration of symptoms was 18.6 months. All patients had upper- or lower-limb numbness in various degrees. X- rays, CT, and MRI of the cervical spine were conducted as radiological evaluation. Fig. 1 Indication for enlarged ACDF: the retrovertebral OPLL should be within half of the adjacent vertebral bodies (as dotted line illustrates) Surgical technique Under general anaesthesia, the cervical spine was exposed through a standard right-sided approach. After confirmation via intraoperative radiography, the conventional discectomy was performed by a curette. The inferior border of the cephalad and the superior border of the caudal vertebral bodies were partly excised with an 8-mm common osteotome to enlarge the intervertebral space as wedge-shaped (Fig. 2). A drill was used to slantly polish the posterior rim of the adjacent vertebral bodies to expose the entire OPLL and to slightly thin the ossified mass (Fig. 3). A microcurette was used to lever the posterior longitudinal ligament at the lateral weak area without ossification, and a gap then appeared between the ossified mass and the spinal cord (Fig. 3). The OPLL was gently lifted and meticulously separated from the dura mater by a blunt microdissector, and then excised by a 1-mm Kerrison rongeur from the middle to either the cephalad or caudal. There was less oppression behind the posterior rim of the vertebral bodies, and the enlarged intervertebral space would facilitate undercutting the retrovertebral OPLL (Fig. 4). If the ossified mass was mainly on the right side, the operating table was leaned 10 to the left side to facilitate removing the lateral mass. In six patients, the ossified mass adhered to
3 Lei et al. Journal of Orthopaedic Surgery and Research (2016) 11:129 Page 3 of 8 Fig. 2 The inferior border of the cephalad and the superior border of the caudal vertebral bodies were partly excised to enlarge the intervertebral space as wedge-shaped, and the bone fragments could be used for bone grafting the dura or the dura itself was ossified; hence, the floating method was adopted. A drill was used to carefully abrade the ossified mass until it became paper thin, and the reexpanded dura mater was observed. A suitable PEEK cage, filled with autologous bone fragments harvested from excising adjacent vertebral bodies angularly, was inserted and fixed using a locking plate (Fig. 5). Clinical and radiological evaluation Follow-up was conducted in all patients. Plain radiographs or CT scans were obtained at 0, 3, and 12 months postoperatively and annually thereafter. MRI scans were dependent on the clinical status. The following parameters were investigated: (1) neurological function, evaluated by the Japanese Orthopaedic Association (JOA) scoring system; (2) neck pain, assessed with visual analogue scale (VAS); (3) sagittal segmental alignment (SSA), defined as the angle between the line along the superior endplate of the cephalad vertebrae and the line along the inferior endplate of the caudal vertebrae; (4) fused segment height (FSH), measured as the distance between the midline of the involved cranial and caudal vertebral body on radiographs; (5) range of motion (ROM) of the cervical spine was measured as the Cobb angle of C2 7 on flexion/extension lateral radiographs; (6) OR, measured on axial CT images; and (7) fusion, confirmed by the presence of trabecular bone bridging on CT scan. Fig. 3 The posterior rim of the vertebral bodies was slantly polished to expose the entire OPLL and the ossified mass was slightly thinned with a burr. A microcurette was used to lever the posterior longitudinal ligament, then a gap appeared between the ossified mass and the spinal cord
4 Lei et al. Journal of Orthopaedic Surgery and Research (2016) 11:129 Page 4 of 8 Fig. 4 The retrovertebral ossification was excised using a 1-mm Kerrison rongeur, thus the second oppression after expansion of the dural sac could be avoided Statistical analysis Statistical analysis was performed using SPSS version 16.0 (SPSS, Inc., Chicago, IL). Preoperative and last follow-up data were compared using paired t test. A p value less than 0.05 was considered statistically significant. Results Table 1 summarises the clinical data for the 24 patients. The operative levels were C4 5 in 7 patients (29 %), C5 6 in 12 patients (50 %), and C6 7 in 5 patients (21 %). The mean follow-up was 34.9 months (range, months). The mean operative time was ± 21.6 min, with the mean blood loss of ± 57.1 ml. The mean JOA score increased from 9.5 (range, 7 12) at preoperation to 13.5 (range, 10 16) at the 3-month follow-up and 14.1 (range 11 17) at the final follow-up (p < 0.05). The average improvement rate (IR) was 64.3 % ± 15.1 %. Six (25 %) patients were graded as excellent, 14 (58.3 %) as good, and 4 (16.7 %) as fair. The average VAS was 6.1 ± 1.8 preoperatively, 3.2 ± 1.6 at the 3-month follow-up, and 2.1 ± 1.4 at the final follow-up (p < 0.05). The imaging of a typical case is shown in Fig. 6a f. The radiological outcomes are shown in Table 2. The OR decreased from 58.9 ± 6.1 % preoperatively to 10.6 ± 5.5 % postoperatively, which was statistically significant (p < 0.001). SSA angles at the final follow-up demonstrated a slight loss of correction (1.4 ) compared with postoperation, but increased 2.2 from preoperation, which was statistically significant (p < 0.001). The mean FSH increased 2.4 mm Fig. 5 A suitable PEEK cage filled with autologous bone fragments was inserted and fixed by plate-screw osteosynthesis
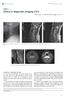
5 Lei et al. Journal of Orthopaedic Surgery and Research (2016) 11:129 Page 5 of 8 Table 1 Clinical data before and after surgery for 24 study patients Item Value Age at operative, years 54.6 ± 8.1 (39 67) Sex Male 15, female 9 Symptom duration, months 18.6 ± 10.3 (3 38) Follow-up period, months 34.9 ± 7.9 (24 52) Number of operated levels C4 5 7 (29 %) C (50 %) C6 7 5 (21 %) Operative time, min ± 21.6 (75 170) Blood loss, ml ± 57.1 ( ) JOA score Before surgery 9.5 ± 1.4 (7 12) Three month after surgery 13.5 ± 1.5 (10 16) # At the last follow-up 14.1 ± 1.5 (11 17) # IR at the last follow-up, % 64.3 ± 15.1 ( ) Neck VAS Before surgery 6.1 ± 1.8 (3 9) Three month after surgery 3.2 ± 1.6 (0 6) # At the last follow-up 2.1 ± 1.4 (0 4) # Complication, number of patients Transient minor neurological deterioration 1 CSF leakage 3 Subcutaneous hematoma 1 Values are expressed as the mean ± standard deviation (range) # P < 0.05, compared with the data before surgery from pre- to postoperatively and decreased 2.7 mm from postoperatively to the final follow-up, but there was no statistical significance when compared with preoperative FSH (p >0.05). Instrument subsidence, defined as a loss of FSH more than 3 mm at the last follow-up compared to postoperation, occurred in five patients (range mm). The IR of these five patients with subsidence was 55.1 ± 13.1 % at the final follow-up, slightly less than that of the other 19 patients (66.7 ± 14.9 %), but there was no statistically significant difference (p > 0.05). The ROM decreased from 34.9 ± 7.7 preoperatively to 26.2 ± 7.2 at the 3-month follow-up (p < 0.001), but recovered to 31.4 ± 7.2 at the final follow-up without significant difference (p > 0.05). Solid osseous union was noted in 21 patients (87.5 %) at 3 months postoperatively. A fusion rate of 100 % was achieved at 1-year follow-up. Transient minor neurological deterioration, manifesting with the weakness of right arm occurred in one case (4.2 %) after operation, but diminished after methylprednisolone pulse treatment. Intraoperatively, CSF leakage occurred in three patients due to the tight adhesion. Timely treatment was performed, including covering with artificial dura, tamping with a gelatin sponge, suturing platysma myoides densely and placing drainage beside the wound. Postoperative management included bed rest with head elevation between 10 and 20, remove drainage until the CSF drainage volume falls below 50 ml per 24 h, continuous local pressure and anti-infection measures. The CSF leakage stopped after 3 to 5 days, and the wound healed successfully. One case (4.2 %) presented dyspnea caused by subcutaneous haematoma, which was cured by reopening the incision and later closure without neurological deterioration. There was no occurrence of instrumented failure during follow-up. Fig. 6 A 62-year-old man with localised OPLL received enlarged ACDF. Preoperative (a) lateral and (b) axial CT scans show OPLL behind C4/5 and part of C5 vertebral body, and the OR was 62 %. Preoperative T2-weighted (c) sagittal MRI show severe cord compression with increased signal intensity. Two years postoperatively, (d) lateral and (e) axial CT scans show that the intervertebral space (C4/5) was enlarged as wedge-shaped and the ossified mass was thoroughly removed. Two years postoperatively, (f) sagittal MRI shows adequate decompression at the C4/5 level but with residual signal intensity
6 Lei et al. Journal of Orthopaedic Surgery and Research (2016) 11:129 Page 6 of 8 Table 2 Radiological results of surgery in 24 study patients Item Value OR, % Before surgery 58.9 ± 6.1 (51 72) After surgery 10.6 ± 5.5 (0 18) # SSA angle, degrees Before surgery 0.5 ± 4.4 ( ) Immediate after surgery 4.1 ± 2.9 ( ) # Three month after surgery 3.2 ± 3.1 ( ) # At the last follow-up 2.7 ± 3.2 ( ) # FSH, mm Before surgery 32.8 ± 2.1 ( ) Immediate after surgery 35.2 ± 2.2 ( ) # Three month after surgery 33.4 ± 2.4 ( ) At the last follow-up 32.5 ± 2.4 ( ) ROM, degrees Before surgery 34.9 ± 7.7 ( ) Three month after surgery 26.2 ± 7.2 ( ) # At the last follow-up 31.4 ± 7.2 ( ) Values are expressed as the mean ± standard deviation (range) # P < 0.05, compared with the data before surgery Discussion Ossification of the posterior longitudinal ligament (OPLL) is a common spinal disorder in Asian countries. Severe OPLL with OR more than 50 % is a great challenge for spinal surgeons because the huge ossified mass indents the spinal cord deeply. Studies have reported that the anterior approach has better outcomes and long-term benefits than the posterior approach [5, 9 12]. OPLL localised to an interspace is an indication for anterior decompression. However, ACDF is highly technically demanding because the limited operative space may increase the risk of CSF leak and iatrogenic neurological deterioration [2], and the retrovertebral OPLL below or above the disk level cannot be easily removed [3]. Though the ACCF with larger operating space was more selected to extirpate the OPLL, it was associated with longer hospital stays, greater blood loss, andmorecomplications[2,7,8,13,14].anotherdisadvantage of ACCF was sacrificing the adjacent intervertebral disk that was not involved in the localised OPLL. In this study, all patients were strictly selected on the basis of CT sagittal reconstruction with the retrovertebral OPLL less than half of adjacent vertebral bodies (Fig. 1). Enlarged diskectomy with wedge shape and polishing the posterior rim of the vertebrae provided a wide exposure of OPLL. The retrovertebral ossified mass could be removed though only one-level diskectomy, thus corpectomy could be avoided. This procedure was similar with Williams-Isu method in the area of drilling [15, 16]. A wide operative field was yielded by resecting the vertebral bodies above and below the intervertebral space to perform decompression safely and steadily. But in our method, autologous bone graft was gained by common osteotome and placed in a PEEK cage, simplifying the complicated bone grafting in sandwich method [16]. Grauvogel [17] used piezosurgery to remove the retrovertebral osteophytes in anterior discectomy. However, the bone removal had to be done only tactually in a blind way [17] and the piezosurgery was not available in most institutions in China. In our technique, the polishing and resecting were performed with direct view, and the drill, curette and microdissector were instruments of daily use. The OR decreased from 58.9 % preoperatively to 10.6 % postoperatively and the IR was 64.3 ± 15.1 %. Furthermore, only one level intervertebral disk space was fixed and the cervical ROM recovered at the last follow-up through the compensation by other segments. Therefore, the conclusion could be drawn that the enlarged ACDF can achieve good functional recovery by removing the OPLL thoroughly and retaining more cervical move function. However, controversy exists about removing the part of the adjacent vertebral body. Previous studies [18, 19] suggested that the endplate should be reserved to prevent graft subsidence. In our opinion, partly resecting the neighbouring vertebrae could provide wider operative field for decompression and autologous cancellous bone for interbody fusion. The wedge-shaped intervertebral space, with ventral narrower but dorsal wider side, could retain more centrum for reconstructing intervertebral height and sagittal segmental alignment. Although obvious subsidence was observed in five patients, the neurological recovery was not influenced. There was a slight loss of SSA angles at the final follow-up compared with postoperatively, but segmental lordosis (2.2 ) was corrected from preoperatively. One reason was that intraoperative distraction with a Caspar spreader may remedy the postoperative loss. Another reason was the PKKP cage had less rigid and subsidence than titanium cage [20], and the anterior platescrew osteosynthesis was good at obtaining the vertebral height [21], segmental lordosis [22] and initial stability. Another important reason was that graft subsidence and loss of cervical lordosis appeared to occur mainly during the first 6 weeks after surgery [23]. In the current study, solid osseous union was noted in 21 patients at 3-month followup, which may prevent the further loss of FSH and SSA. With regard to the complications, there were 12.5 % patients with CSF leakage which was consistent with previous reports [24]. The main reason was the tight adhesion with dural mater or the dural ossification in severe OPLL. In anterior procedure, the first key step was to find the nonossified ligament, the weak part of OPLL [6]. If the meticulous dissection is performed from the nonossified plane, in most cases, a thin but extant
7 Lei et al. Journal of Orthopaedic Surgery and Research (2016) 11:129 Page 7 of 8 dural plane will be evident and the CSF leak will be avoided. Even if the CSF leakage occurs, it could be cured by conservative treatment [5, 6, 24]. Though the neurological deterioration in one patient was minor and transient, the surgeon s manipulation should be careful and gentle. The following should be considered regarding enlarged ACDF. First, the selective bone cutting proportion is essential to perform safe surgery. In our experience, the retrovertebral OPLL should be within 1 2 of adjacent vertebral bodies. Thus, it could be removed through onelevel discectomy and the residual vertebral body could be enough to be implanted with screws. Second, a short plate should be used without destroying the adjacent levels. Third, after removing of the major ossified mass, the residual osteophyte at the posterior edge of the vertebrae must be probed meticulously and removed completely. The second oppression after expansion of the dural sac could be avoided. Fourth, this technique is also effective in removing large disk herniation or extrusion, hypertrophied PLL, or any other compression anterior to the cervical spinal cord because the ossification was the most technically challenging. Limitation The current study has some limitations. First, this study was only a retrospective study with a limited number of 24 patients because of the rarity of this condition. Second, long-term follow-up studies and a comparison between this method and other types of procedures are necessary, which the authors plan to conduct in the future. Conclusions Enlarged ACDF is a relatively effective procedure for treating severe localised OPLL. Using this technique, the retrovertebral OPLL can be removed with common surgical instruments through one-level discectomy and the corpectomy can be avoided. The clinical and radiographic outcomes of this technique are satisfying at short-term follow-up. Additional file Additional file 1: Raw Data. (XLS 31 kb) Abbreviations ACCF: Anterior corpectomy and fusion; ACDF: Anterior cervical diskectomy and fusion; CSF: Cerebrospinal fluid; FSH: Fused segment height; JOA: Japanese Orthopaedic Association; OPLL: Ossification of the posterior longitudinal ligament; OR: Occupying rate; ROM: Range of motion; SSA: Sagittal segmental alignment; VAS: Visual analogue scale Acknowledgements We thank Dr. Jia Li for assistance with preparation of this manuscript. Funding This study receives no financial support. Availability of data and materials The dataset supporting the conclusions of this article is included within the Additional file 1. Authors contributions TL carried out the conception and design of the study and acquisition and interpretation of the data and drafted the manuscript. HW, TT, QHM and LFW were responsible for the data collection and measurement of radiographic data. YS performed all the surgeries and revised the manuscript critically and gave final approval of the version to be published. All authors read and approved the final manuscript. Competing interests This material has not been published and is not under consideration elsewhere. The authors declare that they have no competing interests. Consent for publication Written informed consent for publication was obtained from the participants. All authors read and approved the final manuscript. Ethics approval and consent to participate This study had been approved by Ethics Committee of The Third Hospital of HeBei Medical University, and all patients signed informed consent. This study has been registered with the ResearchRegistry and the unique identifying number is researchregistry1365. Received: 26 June 2016 Accepted: 21 September 2016 References 1. Hirabayashi K, Miyakawa J, Satomi K, Maruyama T, Wakano K. Operative results and postoperative progression of ossification among patients with ossification of posterior longitudinal ligament. Spine (Phila Pa 1976). 1981;6: Epstein NE. Cervical surgery for ossification of the posterior longitudinal ligament: one spine surgeon s perspective. Surg Neurol Int. 2014;5 Suppl 3:S Ying Z, Xinwei W, Jing Z, Shengming X, Bitao L, Tao Z, et al. Cervical corpectomy with preserved posterior vertebral wall for cervical spondylotic myelopathy: a randomized control clinical study. Spine (Phila Pa 1976). 2007;32: Banjeri D, Acharya R, Behari S, Chhabra DK, Jain VK. Corpectomy for multi-level cervical spondylosis and ossification of the posterior longitudinal ligament. Neurosurg Rev (Germany). 1997;20: Chen Y, Chen D, Wang X, Lu X, Guo Y, He Z, et al. Anterior corpectomy and fusion for severe ossification of posterior longitudinal ligament in the cervical spine. Int Orthop. 2009;33: Chen Y, Yang L, Liu Y, Yang H, Wang X, Chen D. Surgical results and prognostic factors of anterior cervical corpectomy and fusion for ossification of the posterior longitudinal ligament. PLoS One. 2014;9:e Song KJ, Lee KB, Song JH. Efficacy of multilevel anterior cervical discectomy and fusion versus corpectomy and fusion for multilevel cervical spondylotic myelopathy: a minimum 5-year follow-up study. Eur Spine J. 2012;21: Liu Y, Hou Y, Yang L, Chen H, Wang X, Wu X, et al. Comparison of 3 reconstructive techniques in the surgical management of multilevel cervical spondylotic myelopathy. Spine (Phila Pa 1976). 2012;37:E Sakai K, Okawa A, Takahashi M, Arai Y, Kawabata S, Enomoto M, et al. Fiveyear follow-up evaluation of surgical treatment for cervical myelopathy caused by ossification of the posterior longitudinal ligament: a prospective comparative study of anterior decompression and fusion with floating method versus laminoplasty. Spine (Phila Pa 1976). 2012;37: Tani T, Ushida T, Ishida K, Iai H, Noguchi T, Yamamoto H. Relative safety of anterior microsurgical decompression versus laminoplasty for cervical myelopathy with a massive ossified posterior longitudinal ligament. Spine (Phila Pa 1976). 2002;27: Iwasaki M, Okuda S, Miyauchi A, Sakaura H, Mukai Y, Yonenobu K, et al. Surgical strategy for cervical myelopathy due to ossification of the posterior longitudinal ligament: part 2. Advantages of anterior decompression and fusion over laminoplasty. Spine (Phila Pa 1976). 2007;32:
8 Lei et al. Journal of Orthopaedic Surgery and Research (2016) 11:129 Page 8 of Chen Y, Guo Y, Lu X, Chen D, Song D, Shi J, et al. Surgical strategy for multilevel severe ossification of posterior longitudinal ligament in the cervical spine. J Spinal Disord Tech. 2011;24: Wada E, Suzuki S, Kanazawa A, Matsuoka T, Miyamoto S, Yonenobu K. Subtotal corpectomy versus laminoplasty for multilevel cervical spondylotic myelopathy: a long-term follow-up study over 10 years. Spine (Phila Pa 1976). 2001;26: Fessler RG, Steck JC, Giovanini MA. Anterior cervical corpectomy for cervical spondylotic myelopathy. Neurosurgery. 1998;43: discussion Kogure K, Isu T, Node Y, Tamaki T, Kim K, Morimoto D, et al. Technical arrangement of the Williams-Isu method for anterior cervical discectomy and fusion. J Nippon Med Sch. 2015;82(1): Kim K, Isu T, Morimoto D, Sugawara A, Kobayashi S, Teramoto A. Cervical anterior fusion with the Williams-Isu method: clinical review. J Nippon Med Sch. 2012;79(1): Grauvogel J, Scheiwe C, Kaminsky J. Use of Piezosurgery for removal of retrovertebral body osteophytes in anterior cervical discectomy. Spine J. 2014;14: Lim TH, Kwon H, Jeon CH, Kim JG, Sokolowski M, Natarajan R, et al. Effect of endplate conditions and bone mineral density on the compressive strength of the graft-endplate interface in anterior cervical spine fusion. Spine (Phila Pa 1976). 2001;26: Cheng CC, Ordway NR, Zhang X, Lu YM, Fang H, Fayyazi AH. Loss of cervical endplate integrity following minimal surface preparation. Spine (Phila Pa 1976). 2007;32: Niu CC, Liao JC, Chen WJ, Chen LH. Outcomes of interbody fusion cages used in 1 and 2-levels anterior cervical discectomy and fusion: titanium cages versus polyetheretherketone (PEEK) cages. J Spinal Disord Tech. 2010;23(5): Jiang SD, Jiang LS, Dai LY. Anterior cervical discectomy and fusion versus anterior cervical corpectomy and fusion for multilevel cervical spondylosis: a systematic review. Arch Orthop Trauma Surg. 2012;132(2): Kwon WK, Kim PS, Ahn SY, et al. Analysis of associating factors with C2-7 sagittal vertical axis after 2-level anterior cervical fusion: comparison between plate augmentation and stand-alone cages. Spine (Phila Pa 1976) Epub ahead of print. 23. Park Y, Maeda T, Cho W, Riew KD. Comparison of anterior cervical fusion after two-level discectomy or single-level corpectomy: sagittal alignment, cervical lordosis, graft collapse, and adjacent-level ossification. Spine J. 2010;10: Joseph V, Kumar GS, Rajshekhar V. Cerebrospinal fluid leak during cervical corpectomy for ossified posterior longitudinal ligament: incidence, management, and outcome. Spine (Phila Pa 1976). 2009;34: Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
) ACDF. (Japanese Orthopaedic Association,JOA) ACCF (175.4±12.1ml VS 201.3±80.4ml) ACDF JOA VAS (P=0.000),ACCF :A : X(2015)
 2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
Disclosures: T. Yoshii: None. T. Yamada: None. T. Taniyama: None. S. Sotome: None. T. Kato: None. S. Kawabata: None. A. Okawa: None.
 Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Cervical myelopathy is a common disease that is
 TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
Rick C. Sasso MD Professor Chief of Spine Surgery Clinical Orthopaedic Surgery Indiana University School of Medicine
 Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA
 AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
Abstract Study Design Systematic review. Weerasak Singhatanadgige 1 Worawat Limthongkul 1 Frank Valone III 2 Wicharn Yingsakmongkol 1 K.
 702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report
 Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy
 THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Fixation of multiple level anterior cervical disc using cages versus cages and plating
 Elsayed and Sakr The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2019) 55:12 https://doi.org/10.1186/s41983-019-0062-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Elsayed and Sakr The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2019) 55:12 https://doi.org/10.1186/s41983-019-0062-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Case Report Two-year follow-up results of artificial disc replacement C7-T1
 Int J Clin Exp Med 2016;9(2):4748-4753 www.ijcem.com /ISSN:1940-5901/IJCEM0018942 Case Report Two-year follow-up results of artificial disc replacement C7-T1 Yi Yang 1, Litai Ma 1, Shan Wu 1, Ying Hong
Int J Clin Exp Med 2016;9(2):4748-4753 www.ijcem.com /ISSN:1940-5901/IJCEM0018942 Case Report Two-year follow-up results of artificial disc replacement C7-T1 Yi Yang 1, Litai Ma 1, Shan Wu 1, Ying Hong
Jing Tao Zhang 1, Lin Feng Wang 1, Yue Ju Liu 2, Jun Ming Cao 1, Jie Li 1, Shuai Wang 1 and Yong Shen 1*
 Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Effect of Swallowing Function After ROI-C Anterior Cervical Interbody Fusion
 Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI /s
 Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Unanswered Questions. Laminoplasty is best
 Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
PARADIGM SPINE. Anterior Cervical Fusion Cage. Cervical Interbody Fusion
 PARADIGM SPINE Anterior Cervical Fusion Cage Cervical Interbody Fusion DESIGN RATIONALE The OptiStrain TM C* interbody fusion cage follows well established biomechanical principles: The slot design of
PARADIGM SPINE Anterior Cervical Fusion Cage Cervical Interbody Fusion DESIGN RATIONALE The OptiStrain TM C* interbody fusion cage follows well established biomechanical principles: The slot design of
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossi cation of the posterior longitudinal ligament
 Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up
 Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis
 Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic resonance imaging study evidence
 See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
Outcomes and revision rates following multilevel anterior cervical discectomy and fusion
 Original Study Outcomes and revision rates following multilevel anterior cervical discectomy and fusion Joseph L. Laratta 1, Hemant P. Reddy 2, Kelly R. Bratcher 1, Katlyn E. McGraw 1, Leah Y. Carreon
Original Study Outcomes and revision rates following multilevel anterior cervical discectomy and fusion Joseph L. Laratta 1, Hemant P. Reddy 2, Kelly R. Bratcher 1, Katlyn E. McGraw 1, Leah Y. Carreon
Risk Factors for Hinge Fracture Associated with Surgery Following Cervical Open-Door Laminoplasty
 CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
EFSPINE CERVICAL COMBINED SET DISC PROTHESIS ORGANIZER BOX
 EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Shen Qiang 1, Ding Hao 1, Zhu Zong-hao 1, Zhu Liang 1, Wei Xiao-kang 1, He Xu-feng 2
 20 48 20161125 Chinese Journal of Tissue Engineering Research November 25, 2016 Vol.20, No.48 Anterior cervical discectomy and fusion versus anterior cervical corpectomy and fusion for treating two-level
20 48 20161125 Chinese Journal of Tissue Engineering Research November 25, 2016 Vol.20, No.48 Anterior cervical discectomy and fusion versus anterior cervical corpectomy and fusion for treating two-level
Clinical and radiological outcomes following hybrid surgery in the treatment of multi-level cervical spondylosis: over a 2-year follow-up
 Shi et al. Journal of Orthopaedic Surgery and Research (2015) 10:185 DOI 10.1186/s13018-015-0330-5 RESEARCH ARTICLE Open Access Clinical and radiological outcomes following hybrid surgery in the treatment
Shi et al. Journal of Orthopaedic Surgery and Research (2015) 10:185 DOI 10.1186/s13018-015-0330-5 RESEARCH ARTICLE Open Access Clinical and radiological outcomes following hybrid surgery in the treatment
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion
 Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp 41 45 2000, Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul
Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp 41 45 2000, Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul
Department of Neurological Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
 online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
Technique Guide. ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Long Term Results of Anterior Corpectomy and Fusion for Cervical Spondylotic Myelopathy
 Long Term Results of Anterior Corpectomy and Fusion for Cervical Spondylotic Myelopathy Rui Gao., Lili Yang., Huajiang Chen, Yang Liu, Lei Liang, Wen Yuan* Department of Spine Surgery, Changzheng Orthopedic
Long Term Results of Anterior Corpectomy and Fusion for Cervical Spondylotic Myelopathy Rui Gao., Lili Yang., Huajiang Chen, Yang Liu, Lei Liang, Wen Yuan* Department of Spine Surgery, Changzheng Orthopedic
C-THRU Anterior Spinal System
 C-THRU Anterior Spinal System Surgical Technique Manufactured From Contents Introduction... Page 1 Design Features... Page 2 Instruments... Page 3 Surgical Technique... Page 4 Product Information... Page
C-THRU Anterior Spinal System Surgical Technique Manufactured From Contents Introduction... Page 1 Design Features... Page 2 Instruments... Page 3 Surgical Technique... Page 4 Product Information... Page
Cervical Curvature Became More Lordotic in Flexion Post-Operatively Regardless of Type of Surgical Approach in Cervical Spondylotic Myelopathy
 Cervical Curvature Became More Lordotic in Flexion Post-Operatively Regardless of Type of Surgical Approach in Cervical Spondylotic Myelopathy Wen-Kai Chou 1, Andy Chien 1, Ya-Wen Kuo 1, Chia-Chin Lin
Cervical Curvature Became More Lordotic in Flexion Post-Operatively Regardless of Type of Surgical Approach in Cervical Spondylotic Myelopathy Wen-Kai Chou 1, Andy Chien 1, Ya-Wen Kuo 1, Chia-Chin Lin
ORIGINAL PAPER. Department of Orthopedic Surgery, Chubu Rosai Hospital, Nagoya, Japan ABSTRACT
 Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device
 Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
CMEARTICLE * * * Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed
 Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Outcomes of Secondary Laminoplasty for Patients with Unsatisfactory Results after Anterior Multilevel Cervical Surgery
 online ML Comm www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.57.1.36 J Korean Neurosurg Soc 57 (1) : 36-41, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical
online ML Comm www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.57.1.36 J Korean Neurosurg Soc 57 (1) : 36-41, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical
Comparisons of three anterior cervical surgeries in treating cervical spondylotic myelopathy
 Zhu et al. BMC Musculoskeletal Disorders 2014, 15:233 RESEARCH ARTICLE Open Access Comparisons of three anterior cervical surgeries in treating cervical spondylotic myelopathy RuoFu Zhu *, HuiLin Yang,
Zhu et al. BMC Musculoskeletal Disorders 2014, 15:233 RESEARCH ARTICLE Open Access Comparisons of three anterior cervical surgeries in treating cervical spondylotic myelopathy RuoFu Zhu *, HuiLin Yang,
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
Fusion Device. Surgical Technique. Cervical Interbody Fusion with Trabecular Metal Technology
 TM-S Fusion Device Surgical Technique Cervical Interbody Fusion with Trabecular Metal Technology 2 TM-S Fusion Device Surgical Technique Disclaimer This surgical technique is not intended for use in the
TM-S Fusion Device Surgical Technique Cervical Interbody Fusion with Trabecular Metal Technology 2 TM-S Fusion Device Surgical Technique Disclaimer This surgical technique is not intended for use in the
Original Article Clinics in Orthopedic Surgery 2013;5:
 Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Clinical and radiographic outcome of dynamic cervical implant (DCI) arthroplasty for degenerative cervical disc disease: a minimal five-year follow-up
 Wang et al. BMC Musculoskeletal Disorders (2018) 19:101 https://doi.org/10.1186/s12891-018-2017-7 RESEARCH ARTICLE Open Access Clinical and radiographic outcome of dynamic cervical implant (DCI) arthroplasty
Wang et al. BMC Musculoskeletal Disorders (2018) 19:101 https://doi.org/10.1186/s12891-018-2017-7 RESEARCH ARTICLE Open Access Clinical and radiographic outcome of dynamic cervical implant (DCI) arthroplasty
Zongyu Zhang 1, Yawei Li 2 and Weimin Jiang 1*
 Zhang et al. BMC Musculoskeletal Disorders (2018) 19:119 https://doi.org/10.1186/s12891-018-2033-7 RESEARCH ARTICLE Open Access A comparison of zero-profile anchored spacer (ROI-C) and plate fixation in
Zhang et al. BMC Musculoskeletal Disorders (2018) 19:119 https://doi.org/10.1186/s12891-018-2033-7 RESEARCH ARTICLE Open Access A comparison of zero-profile anchored spacer (ROI-C) and plate fixation in
Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament
 Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament - A Multicenter Retrospective Study - Mitsumasa Hayashida,
Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament - A Multicenter Retrospective Study - Mitsumasa Hayashida,
Surgical technique. SynCage-C short
 Surgical technique SynCage-C short Table of contents Implants 2 Indications/contra-indications 3 Surgical technique 4 Image intensifier control Warning This description is not sufficient for immediate
Surgical technique SynCage-C short Table of contents Implants 2 Indications/contra-indications 3 Surgical technique 4 Image intensifier control Warning This description is not sufficient for immediate
Commander Cervical Cage - SURGICAL TECHNIQUE
 Commander Cervical Cage - SURGICAL TECHNIQUE D e s i g n e d to c l o s e l y f i t yo u! Commander Cervical Cage - SURGICAL TECHNIQUE Indications Commander cervical cages are designed primarly for restoring
Commander Cervical Cage - SURGICAL TECHNIQUE D e s i g n e d to c l o s e l y f i t yo u! Commander Cervical Cage - SURGICAL TECHNIQUE Indications Commander cervical cages are designed primarly for restoring
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty
 Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Posterior longitudinal ligament resection in anterior cervical discectomy
 Elayouty et al. Egyptian Journal of Neurosurgery (2019) 33:3 https://doi.org/10.1186/s41984-018-0006-7 Egyptian Journal of Neurosurgery RESEARCH Open Access Posterior longitudinal ligament resection in
Elayouty et al. Egyptian Journal of Neurosurgery (2019) 33:3 https://doi.org/10.1186/s41984-018-0006-7 Egyptian Journal of Neurosurgery RESEARCH Open Access Posterior longitudinal ligament resection in
ARCH Laminoplasty System
 Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Cervical Spine Surgery: Approach related outcome
 Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Original Article Application of Zero-P on anterior cervical decompression and bone fusion
 Int J Clin Exp Med 2017;10(4):7077-7083 www.ijcem.com /ISSN:1940-5901/IJCEM0049328 Original Article Application of Zero-P on anterior cervical decompression and bone fusion Yuxiang Xiao, Yongxiang Shi,
Int J Clin Exp Med 2017;10(4):7077-7083 www.ijcem.com /ISSN:1940-5901/IJCEM0049328 Original Article Application of Zero-P on anterior cervical decompression and bone fusion Yuxiang Xiao, Yongxiang Shi,
Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review and meta-analysis
 Eur Spine J (201) 22:158 159 DOI 10.1007/s00586-01-2817-2 ORIGINAL ARTICLE Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review
Eur Spine J (201) 22:158 159 DOI 10.1007/s00586-01-2817-2 ORIGINAL ARTICLE Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review
Ossification of the posterior longitudinal ligament
 J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
Cervical Motion Preservation
 Spinal Disorders D. Pelinkovic, M. D. M&M Orthopaedics 1259 Rickert Drive Naperville, IL 1900 Ogden Ave Aurora, IL Cervical Motion Preservation Neck Pain Symptoms Trapezius myalgia ( Phosphates Bengston
Spinal Disorders D. Pelinkovic, M. D. M&M Orthopaedics 1259 Rickert Drive Naperville, IL 1900 Ogden Ave Aurora, IL Cervical Motion Preservation Neck Pain Symptoms Trapezius myalgia ( Phosphates Bengston
SpineFAQs. Cervical Disc Replacement
 SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
Surgical Technique INTERSOMATIC CERVICAL CAGE
 R INTERSOMATIC CERVICAL CAGE NEOCIF IMPLANTS NEOCIF is an implant designed to make anterior cervical interbody fusion (ACIF) easier and to remove the need for structural autologous graft. The cage is made
R INTERSOMATIC CERVICAL CAGE NEOCIF IMPLANTS NEOCIF is an implant designed to make anterior cervical interbody fusion (ACIF) easier and to remove the need for structural autologous graft. The cage is made
Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with Thoracolumbar Fractures
 Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Original Investigation. Byung-Wan CHOI. INTRODUCTION Ossification of the posterior longitudinal ligament ABSTRACT
 DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement
 Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement Thomas T. Lee, M.D., Glen R. Manzano, B.S., and Barth A.
Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement Thomas T. Lee, M.D., Glen R. Manzano, B.S., and Barth A.
Key words: Professional Med J 2018;25(8): CERVICAL LAMINOPLASTY
 The Professional Medical Journal DOI: 10.29309/TPMJ/18.4872 1. MBBS Post graduate Trainee, 2. MBBS, FCPS Associate Professor 3. MBBS, FCPS Associate Professor 4. MBBS Honorary Researcher, 5. MBBS, FCPS
The Professional Medical Journal DOI: 10.29309/TPMJ/18.4872 1. MBBS Post graduate Trainee, 2. MBBS, FCPS Associate Professor 3. MBBS, FCPS Associate Professor 4. MBBS Honorary Researcher, 5. MBBS, FCPS
PILLAR AL. Anterior Lumbar Interbody Fusion (ALIF) and Partial Vertebral Body Replacement (pvbr) PEEK Spacer System OPERATIVE TECHNIQUE
 PILLAR AL PEEK Spacer System Anterior Lumbar Interbody Fusion (ALIF) and Partial Vertebral Body Replacement (pvbr) OPERATIVE TECHNIQUE Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE TECHNIQUE 3 OPERATIVE
PILLAR AL PEEK Spacer System Anterior Lumbar Interbody Fusion (ALIF) and Partial Vertebral Body Replacement (pvbr) OPERATIVE TECHNIQUE Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE TECHNIQUE 3 OPERATIVE
Usefulness of Intraoperative Computed Tomography in Complication Management after Spine Surgery
 THIEME Techniques in Neurosurgery 193 Usefulness of Intraoperative Computed Tomography in Complication Management after Spine Surgery Johannes Kerschbaumer 1 Christian Franz Freyschlag 1 Marcel Seiz-Rosenhagen
THIEME Techniques in Neurosurgery 193 Usefulness of Intraoperative Computed Tomography in Complication Management after Spine Surgery Johannes Kerschbaumer 1 Christian Franz Freyschlag 1 Marcel Seiz-Rosenhagen
Original Article Application of structural autologous cervical laminae as bone graft in anterior cervical discectomy and fusion
 Int J Clin Exp Med 2016;9(7):14012-14017 www.ijcem.com /ISSN:1940-5901/IJCEM0026133 Original Article Application of structural autologous cervical laminae as bone graft in anterior cervical discectomy
Int J Clin Exp Med 2016;9(7):14012-14017 www.ijcem.com /ISSN:1940-5901/IJCEM0026133 Original Article Application of structural autologous cervical laminae as bone graft in anterior cervical discectomy
Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy
 . 6. Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy WAN Jun, XU Tian-tong*, SHEN Qing-feng, LI Hui-nan and XIA Ying-peng Abstract
. 6. Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy WAN Jun, XU Tian-tong*, SHEN Qing-feng, LI Hui-nan and XIA Ying-peng Abstract
ORIGINAL PAPER. Department of Orthopedic Surgery,Nagoya University Graduate School of Medicine,Nagoya,Japan 2
 Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Adjacent Segment Degeneration Following Anterior Cervical Discectomy and Fusion Versus the Bryan Cervical Disc Arthroplasty
 e-issn 1643-3750 DOI: 10.12659/MSM.905178 Received: 2017.05.05 Accepted: 2017.05.22 Published: 2017.06.02 Adjacent Segment Degeneration Following Anterior Cervical Discectomy and Fusion Versus the Bryan
e-issn 1643-3750 DOI: 10.12659/MSM.905178 Received: 2017.05.05 Accepted: 2017.05.22 Published: 2017.06.02 Adjacent Segment Degeneration Following Anterior Cervical Discectomy and Fusion Versus the Bryan
Solitaire Anterior Spinal System
 Surgical Technique Solitaire Anterior Spinal System Independent Stabilization for the Anterior Column Available in Titanium and Contents Introduction... Page 1 Design Features... Page 2 Instruments...
Surgical Technique Solitaire Anterior Spinal System Independent Stabilization for the Anterior Column Available in Titanium and Contents Introduction... Page 1 Design Features... Page 2 Instruments...
Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures
 Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures Guangdong Chen, MD; Zongping Luo, MD, PhD; Badri Nalajala, MD; Tao Liu, MD, PhD; Huilin Yang, MD, PhD abstract Full article available
Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures Guangdong Chen, MD; Zongping Luo, MD, PhD; Badri Nalajala, MD; Tao Liu, MD, PhD; Huilin Yang, MD, PhD abstract Full article available
Clinical and radiological results of two hybrid reconstructive techniques in noncontiguous 3-level cervical spondylosis
 J Neurosurg Spine 21:944 950, 2014 AANS, 2014 Clinical and radiological results of two hybrid reconstructive techniques in noncontiguous 3-level cervical spondylosis Clinical article *Lisheng Kan, M.D.,
J Neurosurg Spine 21:944 950, 2014 AANS, 2014 Clinical and radiological results of two hybrid reconstructive techniques in noncontiguous 3-level cervical spondylosis Clinical article *Lisheng Kan, M.D.,
Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
We performed CT myelography in 38 patients
 Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
Anterior cervical diskectomy icd 10 procedure code
 Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
Retro-odontoid pseudotumors are mass lesions formed
 SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
The Predictable Factors of the Postoperative Kyphotic Change of Sagittal Alignment of the Cervical Spine after the Laminoplasty
 Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
VLIFT System Overview. Vertebral Body Replacement System
 VLIFT System Overview Vertebral Body Replacement System VLIFT System System Description The VLIFT Vertebral Body Replacement System consists of a Distractible In Situ (DIS) implant, which enables the surgeon
VLIFT System Overview Vertebral Body Replacement System VLIFT System System Description The VLIFT Vertebral Body Replacement System consists of a Distractible In Situ (DIS) implant, which enables the surgeon
Dynamic Mri of the Cervical Spine An Important Tool in Planning Surgical Treatment of Cervical Compressive Myelopathy
 International Journal of Neurosurgery 2018; 2(1): 17-22 http://www.sciencepublishinggroup.com/j/ijn doi: 10.11648/j.ijn.20180201.14 Dynamic Mri of the Cervical Spine An Important Tool in Planning Surgical
International Journal of Neurosurgery 2018; 2(1): 17-22 http://www.sciencepublishinggroup.com/j/ijn doi: 10.11648/j.ijn.20180201.14 Dynamic Mri of the Cervical Spine An Important Tool in Planning Surgical
Treatment for thoracic ossification of posterior longitudinal ligament with posterior circumferential decompression: complications and managements
 Yang et al. Journal of Orthopaedic Surgery and Research (2016) 11:153 DOI 10.1186/s13018-016-0489-4 RESEARCH ARTICLE Open Access Treatment for thoracic ossification of posterior longitudinal ligament with
Yang et al. Journal of Orthopaedic Surgery and Research (2016) 11:153 DOI 10.1186/s13018-016-0489-4 RESEARCH ARTICLE Open Access Treatment for thoracic ossification of posterior longitudinal ligament with
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Anterior cervical discectomy and fusion surgery versus total disc replacement: A comparative study with minimum of 10-year follow-up
 www.nature.com/scientificreports Received: 5 July 2017 Accepted: 16 November 2017 Published: xx xx xxxx OPEN Anterior cervical discectomy and fusion surgery versus total disc replacement: A comparative
www.nature.com/scientificreports Received: 5 July 2017 Accepted: 16 November 2017 Published: xx xx xxxx OPEN Anterior cervical discectomy and fusion surgery versus total disc replacement: A comparative
Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Comparing anterior cervical fusion using titanium cage with hydroxyapatite and with autograft
 Asian Biomedicine Vol. 4 No. 1 February 2010; 147-152 Brief communication (Original) Comparing anterior cervical fusion using titanium cage with hydroxyapatite and with autograft Prakit Tienboon a, Surapon
Asian Biomedicine Vol. 4 No. 1 February 2010; 147-152 Brief communication (Original) Comparing anterior cervical fusion using titanium cage with hydroxyapatite and with autograft Prakit Tienboon a, Surapon
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
