Disclosures: This presenter has no financial relationships with commercial interests.
|
|
|
- Maximillian Walsh
- 6 years ago
- Views:
Transcription
1 Session: L337 Session: L424 My Ulnar Neuropathy Has Resolved. Now I Have to Go for Spine Surgery in the Prone Surrender Position Ihab R. Kamel, M.D. Temple University Hospital, Philadelphia, PA Disclosures: This presenter has no financial relationships with commercial interests. Stem Case and Key Questions Content A 53-year-old male, 182 cm tall and weighing 87 kg, has history of hypertension, diabetes mellitus, smoking, bilateral ulnar neuropathy and spinal stenosis. The patient is complaining of severe back and lower extremity pain. He is a carpenter. Three years earlier he developed bilateral perioperative ulnar neuropathy after knee surgery in the supine position. The patient reports that he had tingling, pain, and motor weakness after the procedure. Motor weakness was incapacitating as he lost his grip and could not hold things. Patient noticed slow and gradual improvement of his sensory symptoms during the first six months after surgery. Motor weakness of both hands slowly improved, but persisted beyond the first postoperative year and completely resolved after fourteen months postoperatively. He was on disability for fifteen months until his symptoms completely resolved. His current medications include glyburide, hydrochlorothiazide, and ibuprofen prn. 1. Is perioperative peripheral nerve injury (PPNI) a significant problem in the practice of anesthesiology? What is the incidence? 2. What are the risk factors for PPNI? Is this patient at risk? 3. Which surgical procedures are considered high-risk for PPNI? 4. What are the mechanisms of PPNI? What is the etiology of PPNI? 5. What is the clinical presentation of perioperative ulnar nerve injury? 6. What is the prognosis of perioperative ulnar neuropathy? A year ago he had endoscopic sinus surgery without any complications. The patient mentions that he notified the anesthesiologist of his previous history of ulnar neuropathy and the anesthesiologist padded his elbows during the surgery, and that is why it went fine. The patient is very concerned that he may develop ulnar neuropathy again, especially when positioned in the prone surrender position under general anesthesia. Page 1
2 7. The patient relates the uneventful endoscopic sinus surgery to the fact that the anesthesiologist padded his elbows. Is this the only reason he did not develop ulnar neuropathy? What would you tell the patient? The patient presents for lumbar laminectomy and fusion with neuromonitoring. The surgical procedure will be performed in the prone surrender (also known as superman or ventral decubitus) position. 8. During preoperative evaluation you notice that the patient is very muscular and he has limited range of motion of the upper extremity. Is this concerning? Why? 9. Does the prone surrender position pose any risk to the brachial plexus or the ulnar nerve? Why? Induction of general anesthesia and endotracheal intubation was uneventful. The patient is positioned in the prone surrender position. 10. How would you position the patient s head and neck? 11. How would you position the shoulders and arms? 12. How would you position the forearm? 13. After placement of the arterial line, how would you position the wrist? The neuromonitoring team will monitor somatosensory evoked potentials (SSEP) while stimulating both the ulnar and the median nerves. 14. What is the role of SSEP in monitoring peripheral nerves under general anesthesia? During the procedure, the right upper extremity SSEP signals show a 70% decrease in amplitude and 40% increase in latency. 15. Is this concerning? 16. In response to the right upper extremity SSEP change, how would you modify the position of the upper extremity? 17. Does mean arterial pressure (MAP) affect nerve conduction and SSEP signals? What is the best MAP for the patient? The upper extremity SSEP changes resolved with upper extremity position modification. The surgery commenced and ended uneventfully. In the post-anesthesia care unit (PACU) the patient reports no symptoms of ulnar neuropathy. Examination reveals no change from preoperative neurological evaluation. Page 2
3 18. Is the patient still at risk for perioperative ulnar neuropathy? 19. What instructions would you give to the patient for the post-operative period? The patient had L2-L5 laminectomy and fusion with cage instrumentation. Four days postoperatively the patient experienced severe radicular pain and lower extremity weakness. The diagnosis of cage malposition was made, and the patient is coming back for revision of the instrumentation in the lateral decubitus position under general anesthesia. 20. Does the lateral decubitus position pose any risk to the brachial plexus or the ulnar nerve? What are the mechanisms of perioperative upper extremity nerve injury in the lateral decubitus position? 21. How would you position the dependent upper extremity? Would you use a chest roll? 22. How can you monitor perfusion in the dependent upper extremity to detect hypoperfusion due to compression of the dependent neurovascular bundle? 23. How would you position the non-dependent upper extremity? 24. How would you position the head and neck? 25. Is documentation of perioperative anesthetic management important in this case? Model Discussion Content Perioperative peripheral nerve injury (PPNI) is a rare but significant perioperative complication that can result in significant patient disability. The reported incidence of PPNI is % [1, 2]. According to the closed claims study, PPNI is the second leading cause of anesthesia malpractice litigation accounting for 16% of cases [3]. The incidence of perioperative peripheral ulnar nerve injury in surgical patients is 0.5% [2]. Ulnar neuropathy is the most common site of PPNI [2] and it comprises 28% of all anesthesia-related nerve injury malpractice claims [3]. Risk Factors Risk factors for ulnar neuropathy include very thin and very obese patients, male gender, and prolonged hospitalization [4]. Pre-existing asymptomatic abnormal conduction in the contralateral ulnar nerve has been observed in patients who developed postoperative ulnar neuropathies [5]. Preexisting subclinical neuropathy may manifest clinically in the perioperative period when patients are subject to certain predisposing factors [4, 6]. Induced and prolonged hypotension has been associated with perioperative ulnar nerve injury [7]. Positioning during anesthesia has been related to ulnar neuropathy [2]. Hypertension (Hazard ratio (HR) 2.2), diabetes mellitus (HR 2.4), renal disease (HR 1.9), coronary artery disease (HR 1.7), and smoking (HR 2.1) have been associated with PPNI injury [1]. This patient is considered high-risk for the development of perioperative ulnar nerve injury because of the previous history of ulnar neuropathy, existing co-morbidities, and his gender. In addition to patient related risk factors, he will be placed in the prone surrender position for a prolonged Page 3
4 period of time under general anesthesia. Orthopedic and neurosurgical procedures are considered high-risk for PPNI injury [1]. Etiology of PPNI The main mechanism of PPNI is peripheral nerve ischemia leading to disruption of the physiologic functions and slowing of conduction. Persistence of ischemia for prolonged periods of time will lead to PPNI. Mechanisms of PPNI include: Stretch: Stretch of the peripheral nerve 5-15% beyond the resting length can cause ischemia due to compression of intraneural capillaries and stretch of the fibers. Compression: Compression leads to damage of the nerve fibers and compression of blood supply. Direct trauma: Direct trauma leads to disruption of nerve fibers. Inflammation: Recent evidence suggests an inflammatory etiology of ulnar neuropathy with a favorable response to high-dose steroids [8]. Males have significantly less fat content on the medial aspect of the elbow and significantly larger tubercle of the coronoid process (1.5 times) compared to females [9]. Women have a significantly higher fat content (2-19 times) on the medial aspect of the elbow than men; while men have a thickened and more developed flexor retinaculum [2]. Men are more susceptible to direct pressure on unmyelinated ulnar nerve fibers than women [10]. The mechanism of perioperative ulnar neuropathy is multifactorial and not clearly understood. In the ASA closed claims study, the mechanism of ulnar neuropathy was explicitly stated in only 9% of malpractice claims [3]. Patient predisposition plays an important role as mentioned above. Predisposed individuals may develop ulnar neuropathy when subject to perioperative precipitating factors. The ulnar nerve has a superficial path along the medial epicondyle of the humerus (figure 1). The ulnar collateral artery and vein run in close proximity to the ulnar nerve and may be affected by external pressure leading to reduced perfusion, ischemia and nerve injury [11]. Compression of the ulnar nerve and its blood supply at the area of the tubercle of the coronoid may lead to ischemia. The ulnar nerve is relatively more sensitive to ischemia compared to the median and the radial nerves. Flexion of the elbow leads to elongation (stretch) of the ulnar nerve. Flexion of the elbow is associated with a decrease in the cross-sectional area of the cubital tunnel and ulnar nerve resulting in a significant increase in the intraneural and extaneural pressures causing a reduction in the perfusion pressure which can lead to ischemia [12]. Stretch of the ulnar nerve by elevation of the shoulder, flexion of the elbow, and dorsiflexion of the wrist, leads to a marked increase in the intraneural pressure [13]. Prolonged and profound hypotension can lead to peripheral nerve ischemia, especially in the presence of nerve stretch or compression in predisposed individuals. The ulnar nerve runs a superficial course around the elbow and is vulnerable to compression. Padding the elbows is helpful but is not the only mechanism to protect the ulnar nerve. Perioperative ulnar nerve injury can occur despite of appropriate padding. Compression of the ulnar nerve can Page 4
5 occur if the forearm is in the prone position. Flexion of the elbow stretches the ulnar nerve. The supine arms tucked position used in endoscopic sinus surgery is a low-risk position for PPNI because of the lack of elbow flexion and direct pressure on the ulnar nerve at the elbow. Usually the forearm is in the neutral position and minimal direct pressure against elbow exists. Clinical Presentation and Prognosis Perioperative ulnar neuropathy presents as a sensory deficit in 47% of the cases, while 53% of the deficits are mixed sensory and motor. Bilateral symptoms of ulnar neuropathy develop in 9% of the cases [4]. Fifty-three percent of patients with perioperative ulnar neuropathy regain complete recovery of sensory and motor functions by the first postoperative year. Six percent regain complete recovery of sensory and motor function but still complain of pain. At one year, 41% of patients have persistent deficits. Patients with sensory deficits have a better chance of complete recovery (80%) compared to patients with mixed motor and sensory deficits (35%) [4]. Preoperative Evaluation Identifying the pattern of PPNI during preoperative evaluation of the patient is important because patients with motor symptoms have worse prognosis compared to those with sensory symptoms. Assessment of the range of motion and what positions can be tolerated by the patient is important, especially in high-risk patients. Because the patient is muscular, it is important to check the range of elbow extension that would be tolerated by the patient [14]. Extension of the elbow may overstretch the median nerve, leading to injury. Muscular patients and patients with limited elbow extension range may be at risk for median nerve injury if the arm is fully extended under general anesthesia. The reduced range of extension in these patients may lead to similar contraction of median nerve, making it more prone to overstretch. Overstretch of the median nerve under general anesthesia may occur when the arm is extended beyond the position tolerated by the awake patient [14, 15]. It is important to explain to the patient that the etiology of ulnar neuropathy is multifactorial and not completely understood. The prone surrender position is a high-risk position that stresses upper extremity peripheral nerves including the ulnar nerve. Patient predisposition plays a role in the development of perioperative ulnar neuropathy. Given his history, he is considered high-risk for perioperative ulnar nerve injury. The prone Surrender (Superman) Position In the prone surrender (superman) position, injury can occur along the entire length of the brachial plexus. Patients placed in the prone surrender (superman) position had a significantly higher incidence of position-related impending upper extremity nerve injury detected by SSEP compared to patients positioned in the supine arms tucked, supine arms out, and prone arms tucked positions [16]. Stretch is the main mechanism of injury. If the head is directed away from the arm, this can stretch the brachial plexus. Abduction of the shoulder greater than 90, depression of the shoulder girdle, and elbow flexion can stretch the brachial plexus. Pronation of the forearm can increase direct pressure Page 5
6 over the ulnar nerve at the elbow. The head of the humerus may compress the neurovascular bundle in the axilla thus leading to nerve damage. In a steep, prone Trendelenburg position the brachial plexus may be compressed between the clavicle and the first rib, especially with use of shoulder braces. Forearm supination significantly minimizes direct pressure over the ulnar nerve at the elbow (2 mmhg) compared with the neutral (69 mmhg) and prone (95 mmhg) forearm positions. Neutral forearm position resulted in significantly less pressure compared to the prone forearm position, however more pressure compared to the supine forearm position [11]. When patients are placed in the prone surrender position, the head and the neck should be in the neutral position (figure 2). Extreme head flexion and extension can stretch the brachial plexus and should be avoided. If the head is directed away from the arm, this can stretch the brachial plexus; therefore lateral neck rotation should be avoided. Although patients may comfortably tolerate arm abduction greater than 90 in the prone surrender position [15], it is advisable to limit the shoulder abduction to less than 90 in order to avoid overstretching of the brachial plexus (figure 3). Depression of the shoulder girdle should be avoided. Lateral rotation of the arm should be avoided as it can stretch the brachial plexus. The longitudinal axis of the forearm should be parallel to the longitudinal axis of patient to avoid outward rotation of the arm. Extreme elbow flexion should be avoided and the forearm should be placed in a neutral position to minimize the direct pressure on the ulnar nerve at the elbow (figure 4). The forearm should be at or below the table mattress surface. The elbow and the inner aspect of the upper arm should be padded with foam to avoid direct pressure on the nerves. Foam padding around the elbow should not be tight (e.g. due to tight Velcro straps) to avoid compression of the ulnar nerve. The medial aspect of the upper arm should be padded to avoid direct pressure caused by the frame supporting the chest (e.g. Wilson frame). Prolonged overextension of wrist over the wrist board placed for arterial lines should be avoided as it may stretch the median nerve [15, 17]. Neuromonitoring Somatosensory evoked potential (SSEP) monitoring has been used to detect peripheral nerve conduction abnormalities under general anesthesia. Conduction abnormalities indicate peripheral nerve stress and impending injury during surgery in variable intraoperative positions [16, 18-24]. Conduction changes detected by SSEP may indicate position-related impending peripheral nerve injury. In a retrospective study of 1000 consecutive spine cases, position modification of the upper extremity led to resolution of 92% of upper extremity SSEP changes [16]. Significant SSEP change indicating impending upper extremity nerve injury is usually defined as a reduction in amplitude of 50% or more, and/or an increase in latency of 10% or more [16]. Significant SSEP changes indicate abnormal conduction and impending nerve injury. If the changes persist for a prolonged period of time, permanent nerve injury may occur [11]. The use of SSEP to monitor extremity nerve function and guide position modification of the upper extremity into a more favorable Page 6
7 position for the peripheral nerve may protect peripheral nerves from injury under general anesthesia. The incidence of position related significant upper extremity SSEP changes during spine surgery ranges from 1.8 % to 15% depending on the type of spine surgery, the operative position, and patient group [16, 18-24]. Position modification strategies include: correcting extreme elbow flexion and extension, decreasing shoulder abduction, releasing tight safety straps, releasing tight foam pad straps, releasing shoulder traction on tucked arms (caused by taping down the shoulder), and moving the upper extremity into the original position if the position has been modified. After position modification of the upper extremity, the SSEP signal should be rechecked for resolution of SSEP change (usually after 10 minutes) [16]. Mean arterial blood pressure (MAP) Perfusion of the peripheral nerve depends on perfusion pressure. The perfusion pressure is the difference between the MAP and local tissue pressure, in this case the intraneural and extraneural pressures. Increased intraneural and extaneural pressures due to operative positioning, will lead to a reduction of the perfusion pressure. Maintaining MAP and avoiding hypotension will help maintain tissue perfusion to the nerve. Appropriately increasing MAP can lead to the resolution of significant SSEP conduction change. The MAP within the physiologic range that leads to resolution of the SSEP conduction changes is considered the best for the patient. Before adjusting MAP, attempts should be made to modify the upper extremity position, which usually results in resolution of the SSEP change. Postoperative Evaluation Most cases of perioperative ulnar nerve injury do not manifest immediately postoperatively. Fewer than 10% of ulnar neuropathies are noted in the PACU. Initial symptoms are usually noted more than 24 hours after the procedure, and appear within 2-7 days in 90% of patients (median 3 days) [3, 4]. Ulnar nerve injury has been associated with prolonged hospitalization. New onset ulnar nerve injury occurred in hospitalized patients admitted to the internal medicine service. During hospitalization, the patients are usually lying in the supine position in bed with the elbows flexed and the forearms placed on the chest or the abdomen. Elbow flexion can stretch the ulnar nerve, and the prone position of the forearm leads to compression of the ulnar nerve by increasing direct pressure at the elbow. Patients should be advised to avoid this position and avoid keeping their arm in one position for prolonged periods of time during the postoperative period [25]. The lateral Decubitus Position Patients placed in the lateral decubitus position had a significantly higher incidence of position-related impending upper extremity nerve injury detected by SSEP compared to patients positioned in the supine arms tucked, supine arms out, and prone arms tucked positions [16]. The lateral decubitus position may lead to nerve injury through stretch and compression. The dependent neurovascular Page 7
8 bundle can be compressed between the head of the humerus and the chest. Compression of the brachial plexus can lead to direct nerve injury while compression of the axillary artery can lead to decreased perfusion and ischemia of the peripheral nerves. The stretch of the non-dependent brachial plexus can lead to injury. Direct pressure on the ulnar nerve at the non-dependent elbow may lead to nerve compression and injury. Overextension of the dependent elbow can stretch the median nerve. The head and neck should be in the neutral position (figure 6). Extreme flexion and extension of the head can stress the brachial plexus and should be avoided. Lateralization of the cervical spine can stretch the contralateral brachial plexus. A chest roll is useful to prevent compression of the dependent brachial plexus between the thorax and the humeral head. The roll is placed under the chest and not the axilla. It is a chest roll-not an axillary roll (figure 7). The anesthesiologist can place his or her hands in the axilla while placing the chest roll to make sure it is appropriately positioned under the chest and not in the axilla. Intravenous fluid 1000 ml bags are usually used as chest rolls. However, the use of an inflatable pillow beneath the dependent chest was associated with significantly less pressure beneath the dependent shoulder and chest compared to a 1000 ml intravenous fluid bag or gel-pads [26]. The non-dependent arm should be positioned on an elevated arm rest (figure 8). The arm rest should be padded with a soft pad. In addition, gel or foam padding should be placed under the elbow. The arm should be horizontal and at the same level of the non-dependent shoulder joint. Shoulder abduction greater than 90 should be avoided. Padding the dependent elbow while avoiding overextension to prevent stretching of the median nerve is important (figure 9). The metal bars supporting the non-dependent arm should be clear of the dependent arm to avoid radial nerve compression. The forearm should be in the supine position to minimize pressure on the ulnar nerve at the elbow. If an arterial line is in place in the dependent extremity, it can be used to monitor and assess the perfusion. Documentation In general, it is very important to document key aspects and details of perioperative patient management. The anesthetic record and preoperative evaluation form should clearly reflect the anesthesiologist s perioperative management. In high-risk cases, like this case, details of preoperative anesthesia evaluation and discussion should be well documented. This includes documentation of preoperative neurological deficits, history of ulnar neuropathy, and key points discussed with the patient while obtaining informed consent. One of the most common causes of litigation in the practice of medicine is not informing the patient of the possible perioperative complications preoperatively. Details of intraoperative positioning should be clearly and legibly documented in the anesthetic record. Although there is no guarantee that PPNI can be completely prevented-especially in high-risk patients-anesthesiologists should apply current knowledge, guidelines, recommendations, and Page 8
9 practice standards. It is imperative that the anesthesiologist documents what was done, because if it is not documented it was not done. Page 9
10 Page 10
11 Page 11
12 Page 12
13 Page 13
14 Page 14
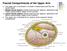
15 Legend: Figure 1.Anatomy of the ulnar nerve at the elbow Figure 2. Proper head and neck positioning in the prone surrender position. The head should be in the neutral position. Extreme head flexion and extension can stretch the brachial plexus and should be avoided. If the head is directed away from the arm, this can stretch the brachial plexus; therefore lateral neck rotation should be avoided. Figure 3. Proper shoulder positioning in the prone surrender position. Shoulder should be abducted < 90 degrees to ovoid stretching of the brachial plexus. Depression of the shoulder girdle should be avoided. Lateral rotation of the arm should be avoided as it can stretch the brachial plexus. Figure 4. Proper elbow, forearm and wrist positioning in the prone surrender position. The forearm should be in supinated position to reduce direct pressure on the ulnar nerve. The upper extremity should be padded. Avoid extreme wrist flexion over supporting board after placing the arterial catheter. The longitudinal axis of the forearm should be parallel to the longitudinal axis of patient to Page 15
16 avoid outward rotation of the arm. Extreme elbow flexion should be avoided and the forearm should be placed in a neutral position to minimize the direct pressure on the ulnar nerve at the elbow. The forearm should be at or below the table mattress surface. The elbow and the inner aspect of the upper arm should be padded with foam to avoid direct pressure on the nerves. The medial aspect of the upper arm should be padded to avoid direct pressure caused by the frame supporting the chest (e.g. Wilson frame). Prolonged overextension of wrist over the wrist board placed for arterial lines should be avoided as it may stretch the median nerve. Figure 5. Incidence of position-related impending upper extremity peripheral nerve injury during spine surgery. The investigators used SSEP to identify reversible upper extremity SSEP changes and compared them between the 5 standard operative positions. The prone superman position(also know as surrender position) and lateral decubitus position has significantly higher incidence of impending upper extremity position-related nerve injury compared to the supine arms out, supine arms tucked and prone arms tucked. Figure 6. Proper positioning of the head and neck in the lateral decubitus position. The head and neck should be in the neutral position. Extreme flexion and extension of the head can stress the brachial plexus and should be avoided. Lateralization of the cervical spine can stretch the contralateral brachial plexus. Figure 7.Proper placement of the axillary roll. It should be placed under the chest and not in the axilla. A chest roll is useful to prevent compression of the dependent brachial plexus between the thorax and the humeral head. The roll is placed under the chest and not the axilla. It is a chest roll-not an axillary roll. The anesthesiologist can place his or her hands in the axilla while placing the chest roll to make sure it is appropriately positioned under the chest and not in the axilla. Figure 8. Proper positioning of the non-dependent arm in the lateral decubitus position. The nondependent arm should be positioned on an elevated arm rest. The arm rest should be padded with a soft pad. In addition, gel or foam padding should be placed under the elbow. The arm should be horizontal and at the same level of the non-dependent shoulder joint. Shoulder abduction greater than 90 should be avoided. Figure 9.Proper positioning of the dependent arm in the lateral decubitus position. Padding the dependent elbow while avoiding overextension to prevent stretching of the median nerve is important. The metal bars supporting the non-dependent arm should be clear of the dependent arm to avoid radial nerve compression. The forearm should be in the supine position to minimize pressure on the ulnar nerve at the elbow. References 1. Welch MB, Brummett CM, Welch TD, Tremper KK, Shanks AM, Guglani P, Mashour GA. Perioperative peripheral nerve injuries: a retrospective study of 380,680 cases during a 10-year period at a single institution. Anesthesiology. 2009; 111(3): Cassoria L, Lee JW. Patient positioning in anesthesia. In: Miller RD, ed. Miller s Anesthesia, 7th Page 16
17 edition. Elsevier, Philadelphia, 2009: Cheney FW, Domino KB, Caplan RA, Posner KL. Nerve injury associated with anesthesia: a closed claims analysis. Anesthesiology. 1999; 90(4): Warner MA, Warner ME, Martin JT. Ulnar neuropathy. Incidence, outcome, and risk factors in sedated or anesthetized patients. Anesthesiology. 1994; 81(6): Alvine FG, Schurrer ME. Postoperative ulnar-nerve palsy. Are there predisposing factors? J Bone Joint Surg Am. 1987; 69(2): Stoelting RK. Postoperative ulnar nerve palsy--is it a preventable complication? Anesth Analg. 1993; 76(1): Swenson JD, Bull DA. Postoperative ulnar neuropathy associated with prolonged ischemia in the upper extremity during coronary artery bypass surgery. Anesth Analg Dec; 85(6): Staff NP, Engelstad J, Klein CJ, Amrami KK, Spinner RJ, Dyck PJ, Warner MA, Warner ME, Dyck PJ. Post-surgical inflammatory neuropathy. Brain. 2010; 133(10): Contreras MG, Warner MA, Charboneau WJ, Cahill DR. Anatomy of the ulnar nerve at the elbow: potential relationship of acute ulnar neuropathy to gender differences. Clin Anat. 1998; 11(6): Morell RC, Prielipp RC, Harwood TN, James RL, Butterworth JF. Men are more susceptible than women to direct pressure on unmyelinated ulnar nerve fibers. Anesth Analg. 2003; 97(4): Prielipp RC, Morell RC, Walker FO, Santos CC, Bennett J, Butterworth J. Ulnar nerve pressure: influence of arm position and relationship to somatosensory evoked potentials. Anesthesiology. 1999; 91(2): Gelberman RH, Yamaguchi K, Hollstien SB, Winn SS, Heidenreich FP Jr, Bindra RR, Hsieh P, Silva MJ. Changes in interstitial pressure and cross-sectional area of the cubital tunnel and of the ulnar nerve with flexion of the elbow. An experimental study in human cadavera. J Bone Joint Surg Am. 1998; 80(4): Pechan J, Julis I. The pressure measurement in the ulnar nerve. A contribution to the pathophysiology of the cubital tunnel syndrome. J Biomech. 1975; 8(1): Warner MA. Patient positioning. In: Barash PG, Cullen BF, Stoelting RK eds. Clinical anesthesia 5th ed. Lippincot Williams & Wilkins, Phildelphia 2006: American Society of Anesthesiologists Task Force on Prevention of Perioperative Peripheral Neuropathies. Practice advisory for the prevention of perioperative peripheral neuropathies: an updated report by the American Society of Anesthesiologists Task Force on prevention of perioperative peripheral neuropathies. Anesthesiology. 2011; 114(4): Kamel IR, Drum ET, Koch SA, Whitten JA, Gaughan JP, Barnette RE, Wendling WW. The use of somatosensory evoked potentials to determine the relationship between patient positioning and impending upper extremity nerve injury during spine surgery: a retrospective analysis. Anesth Analg. 2006; 102(5): Chowet AL, Lopez JR, Brock-Utne JG, Jaffe RA. Wrist hyperextension leads to median nerve conduction block: implications for intra-arterial catheter placement. Anesthesiology. 2004; 100(2): Page 17
18 18. Jones SC, Fernau R, Woeltjen BL.Use of somatosensory evoked potentials to detect peripheral ischemia and potential injury resulting from positioning of the surgical patient: case reports and discussion. Spine J. 2004; 4(3): Schwartz DM, Sestokas AK, Hilibrand AS, Vaccaro AR, Bose B, Li M, Albert TJ. Neurophysiological identification of position-induced neurologic injury during anterior cervical spine surgery. J Clin Monit Comput. 2006; 20 (6): Chung I, Glow JA, Dimopoulos V, Walid MS, Smisson HF, Johnston KW, Robinson JS, Grigorian AA. Upper-limb somatosensory evoked potential monitoring in lumbosacral spine surgery: a prognostic marker for position-related ulnar nerve injury. Spine J. 2009; 9(4): Jahangiri FR, Holmberg A, Vega-Bermudez F, Arlet V. Preventing position-related brachial plexus injury with intraoperative somatosensory evoked potentials and transcranial electrical motor evoked potentials during anterior cervical spine surgery. Am J Electroneurodiagnostic Technol. 2011; 51(3): Davis SF, Abdel Khalek M, Giles J, Fox C, Lirette L, Kandil E. Detection and prevention of impending brachial plexus injury secondary to arm positioning using ulnar nerve somatosensory evoked potentials during transaxillary approach for thyroid lobectomy. Am J Electroneurodiagnostic Technol. 2011; 51(4): Jellish WS, Sherazee G, Patel J, Cunanan R, Steele J, Garibashvilli K, Baldwin M, Anderson D, Leonetti JP. Somatosensory evoked potentials help prevent positioning-related brachial plexus injury during skull base surgery. Otolaryngol Head Neck Surg. 2013; 149(1): O'Brien MF, Lenke LG, Bridwell KH, Padberg A, Stokes M. Evoked potential monitoring of the upper extremities during thoracic and lumbar spinal deformity surgery: a prospective study. J Spinal Disord. 1994; 7(4): Warner MA, Warner DO, Harper CM, Schroeder DR, Maxson PM. Ulnar neuropathy in medical patients. Anesthesiology. 2000; 92(2): Gonzalez Della Valle A, Salonia-Ruzo P, Peterson MG, Salvati EA, Sharrock NE. Inflatable pillows as axillary support devices during surgery performed in the lateral decubitus position under epidural anesthesia. Anesth Analg. 2001; 93(5): Page 18
Disclosures. Closed Claims Reports: Review of Anesthetic Complications. ASA Closed Claims Database. Outline
 Closed Claims Reports: Review of Anesthetic Complications Disclosures Funded by NHLBI & Hamilton Endowment Funds (UCSF Department of Anesthesia). Jae-Woo Lee, MD Associate Professor in Residence University
Closed Claims Reports: Review of Anesthetic Complications Disclosures Funded by NHLBI & Hamilton Endowment Funds (UCSF Department of Anesthesia). Jae-Woo Lee, MD Associate Professor in Residence University
COMPLETION PROJECT POSITIONING THE PATIENT IN THE OR Source- Alexander s Care of the Patient in Surgery
 COMPLETION PROJECT POSITIONING THE PATIENT IN THE OR Source- Alexander s Care of the Patient in Surgery Name Date 1. The systems involved with anesthesia, positioning and operative procedures are: a. b.
COMPLETION PROJECT POSITIONING THE PATIENT IN THE OR Source- Alexander s Care of the Patient in Surgery Name Date 1. The systems involved with anesthesia, positioning and operative procedures are: a. b.
 Anestesiología Mexicana de Revista C CONFERENCIAS MAGISTRALES Vol. 33. Supl. 1, Abril-Junio 2010 pp S220-S228 Perioperative nerve injuries and risk management Richard C. Prielipp, M.D., MBA, FCCM* * JJ
Anestesiología Mexicana de Revista C CONFERENCIAS MAGISTRALES Vol. 33. Supl. 1, Abril-Junio 2010 pp S220-S228 Perioperative nerve injuries and risk management Richard C. Prielipp, M.D., MBA, FCCM* * JJ
Positioning patients for spine surgery: Avoiding uncommon position-related complications
 Online Submissions: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v5.i4.425 World J Orthop 2014 September 18; 5(4): 425-443 ISSN 2218-5836 (online) 2014
Online Submissions: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v5.i4.425 World J Orthop 2014 September 18; 5(4): 425-443 ISSN 2218-5836 (online) 2014
Lowe Plastic Surgery (LPS)
 Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology University of Washington, Seattle, WA
 ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
Official Definition. Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist.
 Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla.
 1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome)
 A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
MUSCLES. Anconeus Muscle
 LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
Chapter 8 8/23/2016. Body Mechanics and Patient Mobility. Introduction to Body Mechanics and Patient Mobility
 Chapter 8 Body Mechanics and Patient Mobility All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Introduction to Body Mechanics and Patient Mobility
Chapter 8 Body Mechanics and Patient Mobility All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Introduction to Body Mechanics and Patient Mobility
PRACTICE advisories are systematically developed
 PRACTICE PARAMETERS Practice Advisory for the Prevention of Perioperative Peripheral Neuropathies 2018 An Updated Report by the American Society of Anesthesiologists Task Force on Prevention of Perioperative
PRACTICE PARAMETERS Practice Advisory for the Prevention of Perioperative Peripheral Neuropathies 2018 An Updated Report by the American Society of Anesthesiologists Task Force on Prevention of Perioperative
Nerve Injury. 1) Upper Lesions of the Brachial Plexus called Erb- Duchene Palsy or syndrome.
 Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
Fractures of the shoulder girdle, elbow and fractures of the humerus. H. Sithebe 2012
 Fractures of the shoulder girdle, elbow and fractures of the humerus H. Sithebe 2012 Fractures of the Clavicle (mid-shaft). Fractures of the clavicle Fractures of the clavicle Treatment- conservative.
Fractures of the shoulder girdle, elbow and fractures of the humerus H. Sithebe 2012 Fractures of the Clavicle (mid-shaft). Fractures of the clavicle Fractures of the clavicle Treatment- conservative.
Why can t we get good baseline motor evoked potentials in this. patient? Laura Hemmer, M.D. Antoun Koht, M.D.
 Why can t we get good baseline motor evoked potentials in this SNACC Neuromonitoring Subcommittee Linda Aglio, M.D., M.S. Laura Hemmer, M.D. Antoun Koht, M.D. David L. Schreibman, M.D. patient? Laura Hemmer,
Why can t we get good baseline motor evoked potentials in this SNACC Neuromonitoring Subcommittee Linda Aglio, M.D., M.S. Laura Hemmer, M.D. Antoun Koht, M.D. David L. Schreibman, M.D. patient? Laura Hemmer,
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem Solving Torso
 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
Analysis of box-tie related suspension nerve injuries
 Analysis of box-tie related suspension nerve injuries I have used the term box-tie to refer to takate-kote style ties, encompassing the arms and upper torso, used for suspension. The purpose of this document
Analysis of box-tie related suspension nerve injuries I have used the term box-tie to refer to takate-kote style ties, encompassing the arms and upper torso, used for suspension. The purpose of this document
Profession experiences
 WACHARIN SRISUK Bangkok Hospital Udon,HOD Education :2000 Bachelor of Nursing science, Thai Red Cross College of Nursing Profession experiences :2000-2014 @Professional Orthopaedic OR Nurse at King Chulalongkorn
WACHARIN SRISUK Bangkok Hospital Udon,HOD Education :2000 Bachelor of Nursing science, Thai Red Cross College of Nursing Profession experiences :2000-2014 @Professional Orthopaedic OR Nurse at King Chulalongkorn
RADIOGRAPHY OF THE ELBOW & HUMERUS
 RADIOGRAPHY OF THE ELBOW & HUMERUS Patient Position: ELBOW AP Projection in same plane Part Position: Hand in ; patient Centered to Humeral epicondyles Central Ray: Structures Shown: AP Elbow Criteria
RADIOGRAPHY OF THE ELBOW & HUMERUS Patient Position: ELBOW AP Projection in same plane Part Position: Hand in ; patient Centered to Humeral epicondyles Central Ray: Structures Shown: AP Elbow Criteria
Upper limb Arm & Cubital region 黃敏銓
 Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Sports Medicine Unit 16 Elbow
 Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Joint Range of Motion Assessment Techniques. Presentation Created by Ken Baldwin, M.Ed Copyright
 Joint Range of Motion Assessment Techniques Presentation Created by Ken Baldwin, M.Ed Copyright 2001-2006 Objectives Understand how joint range of motion & goniometric assessment is an important component
Joint Range of Motion Assessment Techniques Presentation Created by Ken Baldwin, M.Ed Copyright 2001-2006 Objectives Understand how joint range of motion & goniometric assessment is an important component
Intra-operative neurologic injuries: Avoidance and prompt response
 Intra-operative neurologic injuries: Avoidance and prompt response James S. Harrop MD, FACS Professor Neurological and Orthopedic Surgery Director, Division of Spine and Peripheral Nerve Surgery Nsurg
Intra-operative neurologic injuries: Avoidance and prompt response James S. Harrop MD, FACS Professor Neurological and Orthopedic Surgery Director, Division of Spine and Peripheral Nerve Surgery Nsurg
INTRODUCTION Cubital Tunnel Syndrome
 INTRODUCTION Cubital Tunnel Syndrome Diagram of the ulnar nerve supplying the muscles of forearm and hand Cubital Tunnel is a condition that refers to the ulnar nerve being compressed around the elbow.
INTRODUCTION Cubital Tunnel Syndrome Diagram of the ulnar nerve supplying the muscles of forearm and hand Cubital Tunnel is a condition that refers to the ulnar nerve being compressed around the elbow.
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi. E. mail:
 Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven
 Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven 55 years old woman Latarjetprocedure ASA-1, 49 kg. NKDA Informed consent for RA ISB with catheter uneventful throughout, rate 4/4/60 according
Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven 55 years old woman Latarjetprocedure ASA-1, 49 kg. NKDA Informed consent for RA ISB with catheter uneventful throughout, rate 4/4/60 according
Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report
 SHORT REPORT Eur J Anat, 10 (3): 61-66 (2006) Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report K. Ramachandran, I. Kanakasabapathy and
SHORT REPORT Eur J Anat, 10 (3): 61-66 (2006) Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report K. Ramachandran, I. Kanakasabapathy and
The Elbow and Radioulnar Joints Kinesiology. Dr Cüneyt Mirzanli Istanbul Gelisim University
 The Elbow and Radioulnar Joints Kinesiology Dr Cüneyt Mirzanli Istanbul Gelisim University 1 The Elbow & Radioulnar Joints Most upper extremity movements involve the elbow & radioulnar joints. Usually
The Elbow and Radioulnar Joints Kinesiology Dr Cüneyt Mirzanli Istanbul Gelisim University 1 The Elbow & Radioulnar Joints Most upper extremity movements involve the elbow & radioulnar joints. Usually
NEWBORN NURSES POLICY AND PROCEDURES. PURPOSE: Varying positions helps to stimulate physiological functioning and provides rest.
 NEWBORN NURSES POLICY AND PROCEDURES SUBJECT: POSITIONING EFFECTIVE DATE: 6/91 PURPOSE: Varying positions helps to stimulate physiological functioning and provides rest. POLICY: 1. The nurse will vary
NEWBORN NURSES POLICY AND PROCEDURES SUBJECT: POSITIONING EFFECTIVE DATE: 6/91 PURPOSE: Varying positions helps to stimulate physiological functioning and provides rest. POLICY: 1. The nurse will vary
Elbow Elbow Anatomy. Flexion extension. Pronation Supination. Anatomy. Anatomy. Romina Astifidis, MS., PT., CHT
 Elbow Elbow Anatomy Romina Astifidis, MS., PT., CHT Curtis National Hand Center Baltimore, MD October 6-8, 2017 Link between the arm and forearm to position the hand in space Not just a hinge Elbow = 70%
Elbow Elbow Anatomy Romina Astifidis, MS., PT., CHT Curtis National Hand Center Baltimore, MD October 6-8, 2017 Link between the arm and forearm to position the hand in space Not just a hinge Elbow = 70%
Arm Pain, Numbness, and Tingling: Etiologies and Treatment
 Arm Pain, Numbness, and Tingling: Etiologies and Treatment Steve Fowler MD Confluence Health Department of Physiatry Education Medical School: University of Utah Residency: Mayo Clinic Work Confluence
Arm Pain, Numbness, and Tingling: Etiologies and Treatment Steve Fowler MD Confluence Health Department of Physiatry Education Medical School: University of Utah Residency: Mayo Clinic Work Confluence
Inspection. Physical Examination of the Elbow. Anterior Elbow 2/14/2017. Inspection. Carrying angle. Lateral dimple. Physical Exam of the Elbow
 of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
Case Report Successful Closed Reduction of a Lateral Elbow Dislocation
 Case Reports in Orthopedics Volume 2016, Article ID 5934281, 5 pages http://dx.doi.org/10.1155/2016/5934281 Case Report Successful Closed Reduction of a Lateral Elbow Dislocation Kenya Watanabe, Takuma
Case Reports in Orthopedics Volume 2016, Article ID 5934281, 5 pages http://dx.doi.org/10.1155/2016/5934281 Case Report Successful Closed Reduction of a Lateral Elbow Dislocation Kenya Watanabe, Takuma
The Elbow Scanning Protocol
 The Elbow Scanning Protocol Diagnostic Imaging of the Elbow: Introduction The elbow maybe considered as consisting of four quadrants, anterior, medial, lateral and posterior. Ultrasound would normally
The Elbow Scanning Protocol Diagnostic Imaging of the Elbow: Introduction The elbow maybe considered as consisting of four quadrants, anterior, medial, lateral and posterior. Ultrasound would normally
Sick Call Screener Course
 Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Audit and Compliance Department 1
 Introduction to Intraoperative Neuromonitoring An intro to those squiggly lines Kunal Patel MS, CNIM None Disclosures Learning Objectives History of Intraoperative Monitoring What is Intraoperative Monitoring
Introduction to Intraoperative Neuromonitoring An intro to those squiggly lines Kunal Patel MS, CNIM None Disclosures Learning Objectives History of Intraoperative Monitoring What is Intraoperative Monitoring
Gross Anatomy Questions That Should be Answerable After October 27, 2017
 Gross Anatomy Questions That Should be Answerable After October 27, 2017 1. The inferior angle of the scapula of a woman who was recently in an automobile accident seems to protrude making a ridge beneath
Gross Anatomy Questions That Should be Answerable After October 27, 2017 1. The inferior angle of the scapula of a woman who was recently in an automobile accident seems to protrude making a ridge beneath
The Brachial Plexus and Thoracic Outlet Syndrome
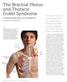 The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block
 Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
"Zero-Position" Functional Shoulder Orthosis for Postoperative. management of rotator cuff injuries.
 "Zero-Position" Functional Shoulder Orthosis for Postoperative Management of Rotator Cuff Injuries Jiro Ozaki, M.D. Ichiro Kawamura INTRODUCTION Many shoulder orthoses such as the airplane splint, the
"Zero-Position" Functional Shoulder Orthosis for Postoperative Management of Rotator Cuff Injuries Jiro Ozaki, M.D. Ichiro Kawamura INTRODUCTION Many shoulder orthoses such as the airplane splint, the
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics
 Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Nerves of Upper limb. Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh
 Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Goniometry. Wrist Flexion: Pt seated with forearm resting on table (use olecranon process & midline of ulna as reference for stationary arm)
 Goniometry Wrist Flexion: Pt seated with forearm resting on table (use olecranon process & midline of ulna as reference for stationary arm) Wrist Extension: Pt seated with forearm resting on table (Goniometer
Goniometry Wrist Flexion: Pt seated with forearm resting on table (use olecranon process & midline of ulna as reference for stationary arm) Wrist Extension: Pt seated with forearm resting on table (Goniometer
The Elbow and the cubital fossa. Prof Oluwadiya Kehinde
 The Elbow and the cubital fossa Prof Oluwadiya Kehinde www.oluwadiya.com Elbow and Forearm Anatomy The elbow joint is formed by the humerus, radius, and the ulna Bony anatomy of the elbow Distal Humerus
The Elbow and the cubital fossa Prof Oluwadiya Kehinde www.oluwadiya.com Elbow and Forearm Anatomy The elbow joint is formed by the humerus, radius, and the ulna Bony anatomy of the elbow Distal Humerus
Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader. Lab Leaders: STATION I BRACHIAL PLEXUS
 Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader Lab Leaders: STATION I BRACHIAL PLEXUS A. Posterior cervical triangle and axilla B. Formation of plexus 1. Ventral rami C5-T1 2. Trunks
Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader Lab Leaders: STATION I BRACHIAL PLEXUS A. Posterior cervical triangle and axilla B. Formation of plexus 1. Ventral rami C5-T1 2. Trunks
Peripheral Nerve Injuries of the Upper Limb.
 Peripheral Nerve Injuries of the Upper Limb www.fisiokinesiterapia.biz Definitions Radiculopathy Process affecting the nerve root, most commonly by a herniated disc Weakness in muscles supplied by the
Peripheral Nerve Injuries of the Upper Limb www.fisiokinesiterapia.biz Definitions Radiculopathy Process affecting the nerve root, most commonly by a herniated disc Weakness in muscles supplied by the
 Nerve Compression Syndromes Median Nerve Carpal Tunnel Syndrome Pronator Syndrome Ulnar Nerve Cubital Tunnel Syndrome Ulnar Tunnel Syndrome TOS www.fisiokinesiterapia.biz Carpal Tunnel Syndrome (CTS) Definition
Nerve Compression Syndromes Median Nerve Carpal Tunnel Syndrome Pronator Syndrome Ulnar Nerve Cubital Tunnel Syndrome Ulnar Tunnel Syndrome TOS www.fisiokinesiterapia.biz Carpal Tunnel Syndrome (CTS) Definition
G24: Shoulder and Axilla
 G24: Shoulder and Axilla Syllabus - Pg. 2 ANAT 6010- Medical Gross Anatomy David A. Morton, Ph.D. Objectives Upper limb Systemically: Bones (joints) Muscles Nerves Vessels (arteries/veins) Fascial compartments
G24: Shoulder and Axilla Syllabus - Pg. 2 ANAT 6010- Medical Gross Anatomy David A. Morton, Ph.D. Objectives Upper limb Systemically: Bones (joints) Muscles Nerves Vessels (arteries/veins) Fascial compartments
Section 11: Nerve damage associated with an operation under general anaesthetic
 Risks associated with your anaesthetic Section 11: Nerve damage associated with an operation under Summary This leaflet explains why it is possible that some nerve damage may occur during your. This is
Risks associated with your anaesthetic Section 11: Nerve damage associated with an operation under Summary This leaflet explains why it is possible that some nerve damage may occur during your. This is
Clinical examination of the wrist, thumb and hand
 Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS AND PAIN
 Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
STABILO-BED. Postural aids system in the lying position
 P O S T U R A L A I D S S Y S T E M STABILO-BED Postural aids system in the lying position STABILO-BED STABILO Version: 16.05.2018 STABILObed is the modular 1st medical class system that is used for precise
P O S T U R A L A I D S S Y S T E M STABILO-BED Postural aids system in the lying position STABILO-BED STABILO Version: 16.05.2018 STABILObed is the modular 1st medical class system that is used for precise
The Language of Anatomy. (Anatomical Terminology)
 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
OMT Without An OMT Table Workshop. Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP
 OMT Without An OMT Table Workshop Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP Cervical Somatic Dysfunction (C5 SR RR) - Seated 1. Patient position: seated. 2. Physician position: standing facing
OMT Without An OMT Table Workshop Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP Cervical Somatic Dysfunction (C5 SR RR) - Seated 1. Patient position: seated. 2. Physician position: standing facing
Assessment of the Brachial Plexus EMG Course CNSF Halifax Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University
 Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
The arm: *For images refer back to the slides
 The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
What is Kinesiology? Basic Biomechanics. Mechanics
 What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
Human Anatomy Biology 351
 1 Human Anatomy Biology 351 Upper Limb Exam Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
1 Human Anatomy Biology 351 Upper Limb Exam Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Hemiplegic Shoulder Power Point for staff education sessions
 Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
Pain Assessment Patient Interview (location/nature of symptoms), Body Diagram. Observation and Examination: Tests and Measures
 Examination of Upper Quarter Neurogenic Pain Jane Fedorczyk, PT, PhD, CHT Thomas Jefferson University, Philadelphia, PA Center of Excellence for Hand and Upper Limb Rehabilitation I. History Mechanism
Examination of Upper Quarter Neurogenic Pain Jane Fedorczyk, PT, PhD, CHT Thomas Jefferson University, Philadelphia, PA Center of Excellence for Hand and Upper Limb Rehabilitation I. History Mechanism
Physical Sense Activation Programme
 Flexion extension exercises for neck and upper back Sitting on stool Arms hanging by side Bend neck and upper back Breathe out Extend your neck and upper back Lift chest to ceiling Squeeze shoulder blades
Flexion extension exercises for neck and upper back Sitting on stool Arms hanging by side Bend neck and upper back Breathe out Extend your neck and upper back Lift chest to ceiling Squeeze shoulder blades
Common Elbow Problems
 Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Basic Care of Common Fractures Utku Kandemir, MD
 Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
PHYSIOTHERAPY PROTOCOLS FOR THE MANAGEMENT OF DIFFERENT TYPES OF BRACHIAL PLEXUS INJURIES
 PHYSIOTHERAPY PROTOCOLS FOR THE MANAGEMENT OF DIFFERENT TYPES OF BRACHIAL PLEXUS INJURIES Introduction As such, protocols in the management of brachial plexus injuries (BPI) are a bit of a misnomer. This
PHYSIOTHERAPY PROTOCOLS FOR THE MANAGEMENT OF DIFFERENT TYPES OF BRACHIAL PLEXUS INJURIES Introduction As such, protocols in the management of brachial plexus injuries (BPI) are a bit of a misnomer. This
Anatomy of the Musculoskeletal System
 Anatomy of the Musculoskeletal System Kyle E. Rarey, Ph.D. Department of Anatomy & Cell Biology and Otolaryngology University of Florida College of Medicine Outline of Presentation Vertebral Column Upper
Anatomy of the Musculoskeletal System Kyle E. Rarey, Ph.D. Department of Anatomy & Cell Biology and Otolaryngology University of Florida College of Medicine Outline of Presentation Vertebral Column Upper
Elbow. Chapter 2 LISTEN. Mechanism of Injury (If Applicable) Pain
 Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
Lab Workbook. ANATOMY Manual Muscle Testing Lower Trapezius Patient: prone
 ANATOMY Manual Muscle Testing Lower Trapezius Patient: prone Lab Workbook Fixation: place on hand below the scapula on the opposite side Test: adduction and depression of the scapula with lateral rotation
ANATOMY Manual Muscle Testing Lower Trapezius Patient: prone Lab Workbook Fixation: place on hand below the scapula on the opposite side Test: adduction and depression of the scapula with lateral rotation
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5. September 30, 2011
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
Complications of Treatment: Nonsurgical and Surgical
 Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
Repair of Severe Traction Lesions of the Brachial Plexus
 Repair of Severe Traction Lesions of the Brachial Plexus LAURENT SEDEL, M.D. Since 1972, the author has performed 259 brachial plexus repairs and various associated secondary procedures. The best results
Repair of Severe Traction Lesions of the Brachial Plexus LAURENT SEDEL, M.D. Since 1972, the author has performed 259 brachial plexus repairs and various associated secondary procedures. The best results
Introduction. Anatomy
 Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Upper limb injuries II. Traumatology RHS 231 Dr. Einas Al-Eisa
 Upper limb injuries II Traumatology RHS 231 Dr. Einas Al-Eisa Capsulitis = inflammatory lesion of the glenohumeral joint capsule leading to: thickening and loss of joint volume painful stiffness of the
Upper limb injuries II Traumatology RHS 231 Dr. Einas Al-Eisa Capsulitis = inflammatory lesion of the glenohumeral joint capsule leading to: thickening and loss of joint volume painful stiffness of the
Exercises to restore range of movement: Rotation
 Exercises to restore range of movement: Rotation Start position: Sitting upright with your back supported in a chair. Position your head so it is evenly balanced, looking forward. Avoid allowing your head
Exercises to restore range of movement: Rotation Start position: Sitting upright with your back supported in a chair. Position your head so it is evenly balanced, looking forward. Avoid allowing your head
Hands PA; Obl. Lat.; Norgaard s Thumb AP; Lat. PA. PA; Lat.: Obls.; Elongated PA with ulnar deviation
 Projections Region Basic projections Additional / Modified projections Upper Limbs Hands PA; Obl. Lat.; Norgaard s Thumb ; Lat. PA Fingers PA; Lat. Wrist PA; Lat. Obls. Scaphoid Lunate Trapezium Triquetral
Projections Region Basic projections Additional / Modified projections Upper Limbs Hands PA; Obl. Lat.; Norgaard s Thumb ; Lat. PA Fingers PA; Lat. Wrist PA; Lat. Obls. Scaphoid Lunate Trapezium Triquetral
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
Chiropractic Glossary
 Chiropractic Glossary Anatomy Articulation: A joint formed where two or more bones in the body meet. Your foot bone, for example, forms an articulation with your leg bone. You call that articulation an
Chiropractic Glossary Anatomy Articulation: A joint formed where two or more bones in the body meet. Your foot bone, for example, forms an articulation with your leg bone. You call that articulation an
1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint
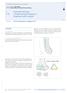 1 Executive Editor: Chris Colton Authors: Mariusz Bonczar, Daniel Rikli, David Ring 1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint Indication All 13-A type fractures, excluding
1 Executive Editor: Chris Colton Authors: Mariusz Bonczar, Daniel Rikli, David Ring 1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint Indication All 13-A type fractures, excluding
Instructions. Print out all three tabs of the guide to be used as a reference.
 Instructions For the Learner 1) The purpose of the observation checklist is to help evaluate the skills obtained from the course. It is also a reference and reminder for what was learned in this course.
Instructions For the Learner 1) The purpose of the observation checklist is to help evaluate the skills obtained from the course. It is also a reference and reminder for what was learned in this course.
Shoulder. 36 Shoulder medi orthopaedics
 Shoulder 36 Shoulder medi orthopaedics medi SAS multi Dual purpose 15 abduction / external rotation support post-operative immobilisation following: rotator cuff ruptures humeral head fractures prosthetic
Shoulder 36 Shoulder medi orthopaedics medi SAS multi Dual purpose 15 abduction / external rotation support post-operative immobilisation following: rotator cuff ruptures humeral head fractures prosthetic
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES. Clavicle fractures Proximal head of humerus fractures
 REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
82a Orthopedic Massage! Introduction - Thoracic Outlet"
 82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
Radiographic Positioning for Dogs
 Radiographic Positioning for Dogs Elbow Radiographs: Lateral View A routine elbow exam consists of a lateral, flexed lateral and craniocaudal view. When performing elbow radiographs, a quality control
Radiographic Positioning for Dogs Elbow Radiographs: Lateral View A routine elbow exam consists of a lateral, flexed lateral and craniocaudal view. When performing elbow radiographs, a quality control
Body Planes & Positions
 Learning Objectives Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how it is used to reference the body. Distinguish
Learning Objectives Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how it is used to reference the body. Distinguish
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Fascial Compartments of the Upper Arm
 Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Anatomy. Anatomy deals with the structure of the human body, and includes a precise language on body positions and relationships between body parts.
 Anatomy deals with the structure of the human body, and includes a precise language on body positions and relationships between body parts. Proper instruction on safe and efficient exercise technique requires
Anatomy deals with the structure of the human body, and includes a precise language on body positions and relationships between body parts. Proper instruction on safe and efficient exercise technique requires
Cubital Tunnel Syndrome
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
divided by the bones ( redius and ulna ) and interosseous membrane into :
 fossa Cubital Has: * floor. * roof : - Skin - superficial fasica - deep fascia ( include bicipital aponeurosis ) Structures within the roof : -cephalic and basilic veins -and between them median cubital
fossa Cubital Has: * floor. * roof : - Skin - superficial fasica - deep fascia ( include bicipital aponeurosis ) Structures within the roof : -cephalic and basilic veins -and between them median cubital
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
PTA 210 PTA Techniques. Patient Positioning and Draping
 PTA 210 PTA Techniques Patient Positioning and Draping Review Last Lecture 5 vital signs you are responsible for? What is patency? How do you test it? Pressing too hard with HR can cause Contraindications
PTA 210 PTA Techniques Patient Positioning and Draping Review Last Lecture 5 vital signs you are responsible for? What is patency? How do you test it? Pressing too hard with HR can cause Contraindications
 1 of 8 9/21/2006 1:02 PM Smith College Dept. of Athletics Program for The Average Division III Female Athlete Trainer : Timothy Bacon Introduction Core, functional and complementary exercises. Warm Up
1 of 8 9/21/2006 1:02 PM Smith College Dept. of Athletics Program for The Average Division III Female Athlete Trainer : Timothy Bacon Introduction Core, functional and complementary exercises. Warm Up
ORIGINAL ARTICLE. Department of Orthopedic Surgery, Mashad University of Medical Sciences, Mashad, Iran
 Arch Iranian Med 2003; 6 (3): 196 199 ORIGINAL ARTICLE INJECTION OF METHYLPREDNISOLONE AND LIDOCAINE IN THE TREATMENT OF MEDIAL EPICONDYLITIS: A RANDOMIZED CLINICAL TRIAL Mahmood Bahari MD, Mohammad Gharehdaghi
Arch Iranian Med 2003; 6 (3): 196 199 ORIGINAL ARTICLE INJECTION OF METHYLPREDNISOLONE AND LIDOCAINE IN THE TREATMENT OF MEDIAL EPICONDYLITIS: A RANDOMIZED CLINICAL TRIAL Mahmood Bahari MD, Mohammad Gharehdaghi
Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 4 Handout
 Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 4 Handout Please Note: Erik Dalton teaches his Myoskeletal Alignment Techniques with the expectation
Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 4 Handout Please Note: Erik Dalton teaches his Myoskeletal Alignment Techniques with the expectation
Peripheral Nerve Problems
 UW MEDICINE PATIENT EDUCATION Peripheral Nerve Problems How they develop and ways to treat them This handout explains how nerves work, what happens when they are injured, and how peripheral nerve problems
UW MEDICINE PATIENT EDUCATION Peripheral Nerve Problems How they develop and ways to treat them This handout explains how nerves work, what happens when they are injured, and how peripheral nerve problems
Chapter 32. Objectives. Objectives 01/09/2013. Spinal Column and Spinal Cord Trauma
 Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
