Ultrasound-guided Supraclavicular Brachial Plexus Block
|
|
|
- Tiffany Flowers
- 6 years ago
- Views:
Transcription
1 PICTORIAL REVIEW Ultrasound-guided Supraclavicular Brachial Plexus Block 1 Faisal Rasool, 2 Armin Bartsch, 3 Aamer B Ahmed, 3 Atul Gaur IJUTPC Ultrasound-guided Supraclavicular Brachial Plexus Block 1 Specialist Registrar, Department of Anaesthesia, University Hospitals of Leicester NHS Trust, Leicester, LE3 9QP United Kingdom 2 Clinical Fellow in Anaesthesia, Department of Anaesthesia, University Hospitals of Leicester NHS Trust, Leicester, LE3 9QP United Kingdom 3 Consultant Anaesthetist, Department of Anaesthesia, University Hospitals of Leicester NHS Trust, Leicester, LE3 9QP United Kingdom Correspondence: Atul Gaur, Consultant Anaesthetist, Department of Anaesthesia, Glenfield Hospital, University Hospitals of Leicester NHS Trust, Leicester, LE3 9QP, United Kingdom, atul.gaur@uhl-tr.nhs.uk Peripheral nerve blocks have certain advantages over general anaesthesia such as associated analgesia, minimal side effects and a more rapid recovery. 1-3 The supraclavicular brachial plexus block provides reliable anaesthesia of the entire upper limb with excellent conditions for tourniquet application. Kulenkampf in 1911 described a technique based on an injection made at the supraclavicular part of the brachial plexus associated with a short onset of action. 4 Despite a few modifications, the supraclavicular approach remained risk prone owing to its association with a high incidence of pneumothorax. 5 After Grange et al performed first Doppler guided block in 1978, the evolution of real time ultrasound guided blocks (with or without nerve stimulation) resulted in ease of performance, increased safety profile, and a better quality block. 6,7 Ultrasound has played a significant role in re-establishing the supraclavicular brachial plexus block in perioperative care. However, a thorough understanding of the anatomy, sonoanatomy, sonotechniques including scanning and needling is essential to ensure a safe and high quality block. 8 ANATOMY The anterior rami of the cervical and first thoracic spinal nerves (C5-8 and T1) form the brachial plexus. The brachial plexus originates in the neck as roots and terminates in the axilla as cords, giving off various branches along its course. The roots of the brachial plexus emerge between the scalenus anterior and scalenus medius muscles to form trunks which cross the floor of posterior triangle. Each trunk divides into anterior and posterior divisions and rearranges to form the cords at the outer border of the Fig. 1: Schematic diagram of brachial plexus first rib to continue down into the axilla. Thus the roots of the brachial plexus are situated between the scalene muscles, divisions behind the clavicle and cords in the axilla. The roots and trunks along with their branches form the supraclavicular aspect whilst the cords and their branches form the infraclavicular portion of the brachial plexus (Fig. 1). The scalenus anterior muscle originates from the tubercles on the C3-6 cervical vertebrae and descends forwards and laterally to be inserted onto the scalene tubercle and adjacent part of the first rib. The phrenic nerve (C3-5) courses on the scalenus anterior within the prevertebral fascia, leaving its medial border near its lower edge and runs between the subclavian artery and vein to enter thorax. International Journal of Ultrasound and Applied Technologies in Perioperative Care, January-April 2010;1(1):
2 Faisal Rasool et al The subclavian artery arises behind the sternoclavicular joint from the brachiocephalic artery on the right side; and on the left side, more caudally in thorax directly from the aortic arch. The subclavian artery arches superiorly and laterally, anterior to the cervical pleura and behind the anterior scalene muscle. It continues as axillary artery at the outer border of first rib. The scalenus anterior divides subclavian artery into three parts; the first part lies from its origin to the scalenus anterior, second part lays posterior, and third part, lateral to the scalenus anterior up to the lateral border of first rib where it continues into axilla as axillary artery. The subclavian artery gives rise to four main branches, i.e. vertebral artery, thyrocervical trunk, internal thoracic (or mammary) artery and costocervical trunk. All branches originate from first part of the subclavian artery on the left side, and the costocervical trunk originates from the second part of the subclavian artery on the right side. The vertebral artery is the first branch of the subclavian artery which arises from its upper margin and ascends in neck between longus colli and scalenus anterior. It passes in front of the transverse process of C7 vertebra and through the transverse foramina of upper six cervical vertebrae. The sympathetic plexus runs along the vertebral artery. It is closely related to the middle and inferior cervical sympathetic ganglia which are connected by ansa subclavian. The thyrocervical trunk is the second branch which arises lateral to the vertebral artery from upper convexity of the subclavian artery. It divides into the transverse cervical, suprascapular and inferior thyroid arteries. The transverse cervical and suprascapular arteries pass laterally across scalenus anterior and the phrenic nerve and then lie in the lower part of the posterior triangle in front of the trunks of brachial plexus. The ascending cervical, a branch of either the inferior thyroid artery or thyrocervical trunk, ascends upwards and medial to the phrenic nerve. The internal thoracic artery is the third branch which originates from the inferior side of the subclavian artery. The costocervical trunk originates from first part of the subclavian artery on the left and from the second part on the right side. It courses backwards on pleura and divides into the superior intercostal and deep cervical arteries near the neck of first rib. The trunks of brachial plexus and third part of subclavian artery lie lateral to scalenus anterior in floor of posterior triangle, enclosed within prevertebral fascia. The dorsal scapular artery (DSA) occasionally originates from third part of subclavian artery. The DSA courses along with, or through, brachial plexus as it passes in front of scalenus medius before entering into the mass of levator scapulae to form scapular anastomosis. The DSA is frequently replaced by deep branch of the transverse cervical artery (TCA). Occasionally, the TCA or suprascapular artery or both directly originate from third part of subclavian artery in which case they are intimately related with the brachial plexus. Other contents of posterior triangle include the external jugular vein, accessory nerve (XI cranial nerve), lesser occipital nerve, greater auricular nerve, transverse cervical nerves and supraclavicular nerves (Fig. 2). ULTRASOUND PROBE Fig. 2: Brachial plexus The brachial plexus is scanned using a high frequency 5 to 14 MHz, linear ultrasound probe. It is important to adjust the ambient light and ultrasound machine settings by selecting appropriate depth of field, frequency, focus, and gain to optimise the ultrasound image. Probe Position (Oblique Placement) The brachial plexus can be scanned either in coronal or para sagittal planes in supraclavicular area. The ultrasound probe held in an oblique plane (coronal or sagittal) scans the brachial plexus both in longitudinal and horizontal 40 JAYPEE
3 Ultrasound-guided Supraclavicular Brachial Plexus Block directions as compared to a single (horizontal or longitudinal) plane when the probe is held either parallel or vertical to the clavicle. The sonoanatomy is more detailed when ultrasound probe is placed obliquely. Various needle approaches (anterior, posterior, medial or lateral) have been described with reference to the placement of the ultrasound probe. Sonoanatomy The subclavian artery is a prominent landmark identified immediately superior to first rib as a pulsatile hypoechoic tennis ball like image on ultrasound. The first rib appears as a bright hyperechoic rim with a drop out bony acoustic shadow. The brachial plexus normally appears superior, superolateral and/or superomedial to subclavian artery as multiple hypoechoic ovals/circles, often described as a honeycomb pattern or bunch of grapes. The brachial plexus may acquire a triangular, linear or vertical (or oblique) arrangement of trunks/division/cords around subclavian artery in supraclavicular region on ultrasound scan (Figs 3 and 4). The pleura is seen as a hyperechoic line at same level as that of the rib but appears more shiny than the rib. Pleura moves and shines more with breathing. The hyperechoic pleural shadow does not have a drop out acoustic shadow, which differentiates it from the rib shadow (Fig. 5). The scalenus anterior and medius muscles appear as hypoechoic structures on ultrasound scan and can be followed commencing from their origin to the point of insertion on first rib. The phrenic nerve lies on anterior surface of scalenus anterior from C4-7 level in neck (Fig. 6). The long thoracic and dorsal scapular nerves pass through middle scalene muscle and may appear as holes or hypoechoic structures. Often part of brachial plexus passes through scalenus anterior or medius muscles and is seen as small round or oval hyperechoic or hypoechoic structures. The thyrocervical trunk and transverse cervical artery often appear similar to nerve trunks on ultrasound scan. The pulsations of smaller arteries or branches are easily masked by the strong pulsations of subclavian artery. These vessels may fall in nerve block needle trajectory or course along or through the brachial plexus. This poses a threat of vascular injury, hematoma formation or inadvertent intravascular injection Colour Doppler may help in differentiation of brachial plexus from arteries by demonstrating colour enhancement. Thus ideally the proposed nerve block Fig. 3: Supraclavicular brachial plexus arranged in triangular pattern. Plexus is seen as rounded to oblong hypoechoic structures surrounded by hyperechoic rim. Subclavian artery (SA) is seen as large rounded hypoechoic structure which is pulsatile in real time and can be further confirmed by colour Doppler Fig. 4: Supraclavicular brachial plexus arranged as vertical/obliquely arranged circles. Plexus is seen as hypoechoic round structure (marked area) Fig. 5: Showing pleura and rib. Rib is seen as linear hyperechoic area with acoustic shadowing, pleura is visualised as hyperechoic structure without acoustic shadow. SA, subclavian artery; BPL, brachial plexus International Journal of Ultrasound and Applied Technologies in Perioperative Care, January-April 2010;1(1):
4 Faisal Rasool et al needle trajectory should be routinely scanned with Colour Flow Doppler (Figs 7A and B). In addition, veins are collapsible and may be identified by applying and releasing pressure with help of ultrasound probe while scanning. PATIENTS POSITION FOR SUPRACLAVICULAR BRACHIAL PLEXUS BLOCK The supraclavicular block may be performed with patient in supine, supine with 45 head up and in lateral positions (Figs 8A to C). Fig. 6: Showing phrenic nerve (PN) as hyperechoic structure on anterior surface of scalenus anterior (SA) muscle. IJV, internal jugular vein; CCA, common carotid artery A Patient in Supine Position The patient lays supine with head turned to the contralateral side. The pillow may be arranged as shown in Figure 8A to provide space for needle insertion. Supine Posterior Approach The ultrasound probe is held in an oblique coronal plane in supraclavicular fossa and the needle is directed medially and posteriorly as described by Chan et al (Fig. 9). In a similar approach, the ultrasound probe is held in oblique parasagittal plane and needle is directed anteriorly and caudally as described by Searle and Gopinath (Fig. 10). This technique is described in a separate article in this issue. 16 Supine Posterior Approach with 45 Head Up This position improves patient s comfort besides facilitating needle insertion. It is especially helpful when patient is unable B Figs 7A and B: Showing a branch of subclavian artery coursing through brachial plexus on colour Doppler. SA, subclavian artery Fig. 8A: Supine position 42 JAYPEE
5 Ultrasound-guided Supraclavicular Brachial Plexus Block Fig. 8B: Supine with 45 head up position Fig. 9: Showing probe placed in oblique coronal plane Fig. 8C: Lateral position Fig. 10: Showing probe placed in oblique parasagittal plane to tolerate a total supine position due to cardiorespiratory compromise or other postural issues. The ultrasound probe is placed in oblique coronal or parasagittal plane. The needle enters medially and anteriorly, or caudally and anteriorly depending on ultrasound probe placement method, as described above. Supine Anterior Approach The ultrasound probe is placed in an oblique coronal or parasagittal plane and needle is introduced from the anterior side of probe. The needle is directed posteriorly and medially to approach the brachial plexus. This approach is not in common use. The copula of the lung is located above and posterior to the subclavian artery and needle may pass very close to it. Also, the needling procedure may be challenging as needle trajectory may have to acquire a steep angle to reach brachial plexus. Coronal Placement of Probe The ultrasound probe is placed parallel to clavicle in supraclavicular fossa. The needle enters either from (a) lateral end of probe and advanced medially and posteriorly or (b) medial end of probe and advanced laterally and posteriorly using an in-plane technique. 13,6 Presence of the subclavian artery can compromise needle access to some parts of plexus which may result in higher failure rates. Manipulation of the artery to lift it away using needle tip has been described but may cause inadvertent intravascular injection or hematoma formation due to arterial puncture. Patient in Lateral Position using Posterior Approach The patient is positioned in lateral position with the side to be blocked up as described by Gaur et al. 11 This position International Journal of Ultrasound and Applied Technologies in Perioperative Care, January-April 2010;1(1):
6 Faisal Rasool et al allows the anaesthetist, needling site, line of needle insertion and ultrasound machine all to be aligned to improve nerve block procedure and operator comfort. Also, block in lateral position is ideal for pregnant patients. The probe has more space to move, angle or tilt in all directions to optimize image quality. Thus there is more freedom to obtain a safe plane of scan away from adjacent structures such as the thyrocervical trunk, pleura, etc. Fig. 11: Showing probe placed in oblique parasaggital plane in lateral position The ultrasound probe is placed in the supraclavicular fossa in an oblique parasagittal plane and needle is directed anteriorly and medially and steered towards brachial plexus (Fig. 11). A few patients have restricted neck movement or a pit in the supraclavicular fossa with a prominent trapezius muscle. It is difficult to perform the block in supine position in such patients. The lateral position still allows needle insertion through trapezius to reach brachial plexus as there is enough space on posterior aspect of the shoulder for needle maneuvering in such patients (Figs 12A to D). In addition, space on posterior side of probe and patient facilitates catheter placement when required. Needle Insertion Technique Patients are examined, informed and prepared as for traditional supraclavicular brachial plexus block. The ultrasound probe is cleaned and covered in a sterile cover, the patient s skin is prepared and procedure is performed with cap, gown and sterile gloves on. Both short bevel and Huber tip nerve block needles have been used for block procedures. Local anaesthetic is applied locally onto the skin at needle entry point. A 50 to 100 mm long needle is inserted 1 to 2 cm away from the proximal border of ultrasound probe. The needle is introduced in the Figs 12A to D: Patients with a dip in supraclavicular fossa and prominent trapezius muscle. The probe placed in oblique parasagittal plane in lateral position. (A) Patient in supine position (B) Patient in lateral position (C) Ultrasound probe in supraclavicular fossa (D) Needle is introduced through trapezius muscle due to a big dip in supraclavicular fossa 44 JAYPEE
7 Ultrasound-guided Supraclavicular Brachial Plexus Block posterior triangle near anterior border of trapezius muscle at an angle of 0 to 45 for a supraclavicular brachial plexus block. The in-plane (IP) approach is commonly used for supraclavicular brachial plexus blocks. It is safe to insert needle initially in the superficial plane until needle is visualised on ultrasound scan. Once this needle is seen as a hyperechoic line, it is steered towards the brachial plexus (Figs 13A and B). It is important to track the needle tip throughout to avoid complications such as haemothorax or pneumothorax. Often the inferior belly of omohyoid prevents smooth entry of needle towards brachial plexus; however the needle may be easily steered in from upper or lower border of omohyoid muscle. Combitech needling is a combination of landmark and ultrasound guided in-plane needling techniques. This enhances the safety of block as needle is steered in deeper planes only under ultrasound guidance. To perform combitech needling, an optimum scan of brachial plexus is obtained; a temporary landmark a blanched rectangle on skin is created by pressing firmly with ultrasound probe (Fig. 14A). Ultrasound probe is then lifted off the skin and needle is inserted in superficial subcutaneous plane in centre of the blanched rectangle (Figs 14B and C). Subsequently, ultrasound probe is replaced over needle and once needle is visualised, it is steered into deeper planes towards brachial plexus under real time ultrasound guidance (Fig. 14D). A B Figs 13A and B: (A) Showing needle as hyperechoic linear structure approaching brachial plexus using in-line needling technique, (B) Showing needle within brachial plexus using in-line needling technique. SA, subclavian artery; BPL, brachial plexus Figs 14A to D: Combitech needling (A) Ultrasound probe in parasagittal plane pressure is applied onto skin (B) Probe is lifted off the skin and a blanched rectangle is created (C) Needle is introduced subcutaneously in centre of blanched rectangle (D) Probe is replaced over needle International Journal of Ultrasound and Applied Technologies in Perioperative Care, January-April 2010;1(1):
8 Faisal Rasool et al A few specialised ultrasound needles are also available on the commercial market; however, their usefulness is yet to be demonstrated. These needles have serrations or pits on the needle surface which are claimed to improve their visibility. Sonoanatomy after LA Injection Once the needle tip is positioned near the brachial plexus, a small aliquot of 1 to 2 ml of local anaesthetic (LA) is injected to confirm the position of needle-tip by observing its spread (Fig. 15).This is followed by injection of another 10 to 30 ml of LA solution. Care must be taken not to inject when faced with a high resistance to the injection. Also, on introduction of LA, a comet tail artifact may appear at needle tip due to the deposition of multiple small air bubbles. If neither the spread of local anaesthetic nor the comet tail artifact is seen at needle tip, it is likely that the needle-shaft is being mistaken for needle-tip. In this situation probe should be moved to carefully scan, align and relocate the needletip. Initial injection of local anaesthetic can be made either (a) near the 12 to 2 o clock or (b) 4 to 6 o clock positions in reference to the subclavian artery. When local anaesthetic is initially deposited at 4 to 6 o clock position then air bubbles (accidently) introduced with the injectate do not compromise image quality during rest of the procedure. On the other hand initial injection near 12 to 2 o clock position improves image quality around 4 to 6 o clock where structures such as thyrocervical trunk or pleura are situated, hence any injury to these structures can be avoided when needle is directed in a deeper plane (Figs 16 and 17). A single injection is sufficient to produce excellent analgesia when block is performed along with a general anaesthetic. However, when the block is performed as a sole anaesthetic technique, a rapid onset is required. Multiple injections enhance the spread of local anaesthetic thus facilitate rapid onset and quality of block. 17 The needle is usually repositioned through hydrodissected areas (pockets) created by local anaesthetic around brachial plexus. 17,18 Hemidiaphragmatic paralysis is not as commonly seen after a supraclavicular approach as with the interscalene approach for brachial plexus block. Phrenic nerve paresis following supraclavicular brachial plexus has been observed in up to 67% of the patients in one series. 19 Since the phrenic nerve adheres to scalenus anterior by prevertebral fascia, this is invariably blocked when local anaesthetic spreads on the anterior surface of the muscle. After completing the local anaesthetic injection, anterior surface of scalenus anterior at C5-7 level should be scanned to detect this spread (Fig. 18). Catheter Placement The authors find that the lateral position offers a suitable alternative for catheter placement due to adequate space for needle maneuverability (Fig. 19). Local anaesthetic solution or dextrose 5% is injected to distend the sheath or space around brachial plexus prior to insertion of a catheter. Fig. 15: Showing spread of local anaesthetics as hypoechoic area bathing the plexus near needle-tip at 12 to 1 o clock position. LA, local anaesthetic; SA, subclavian artery Fig. 16: Showing spread of local anaesthetics around brachial plexus. LA, local anaesthetic; SA, subclavian artery 46 JAYPEE
9 Ultrasound-guided Supraclavicular Brachial Plexus Block Fig. 17: Showing spread of local anaesthetics around brachial plexus and needle is repositioned near 5 to 6 o clock position Fig. 18: Showing local anaesthetic spread as irregular hypoechoic area inferior to phrenic nerve (PN) and around brachial plexus at C6 level. PN, phrenic nerve; SA, scalenus anterior muscle; LA, local anaesthetic; BPL, brachial plexus Fig. 19: Showing supraclavicular block catheter placement in lateral position The correct placement of catheter is confirmed by injecting local anaesthetic and visualising its spread. The catheter produces multiple hyperechoic spots on ultrasound scan. The catheter position can also be confirmed by injecting a small volume (1 ml) of air at the end of the procedure which creates an artifact and changes the quality of the ultrasound image. 20 REFERENCES 1. Mulroy M, Larkin K, Batra M, et al. Femoral Nerve block with 0.25% or 0.5% bupivacaine improves postoperative analgesia following outpatient arthroscopic anterior cruciate ligament repair. Reg Anaesth Pain Med 2001;26 (1): Chan VW, Peng PW, Kaszas Z, Middleton WJ, Muni R, Anastakis DG, GrahamBA. A comparative study of general International Journal of Ultrasound and Applied Technologies in Perioperative Care, January-April 2010;1(1):
10 Faisal Rasool et al anaesthesia, intravenous regional anaesthesia, and axillary block for outpatient hand surgery: Clinical outcome and cost analysis. Anaesth Analg 2001;93: Pavlin DJ, Rapp SE, Polissar NL, Malmgren JA, Koerschgen M, Keyes H. Factors affecting discharge time in adult outpatients. Anaesth Analg 1998;87: Kulenkampf D. Anaesthesia of the brachial plexus. Zentralbl Chir 1911;38: David L Brown, Donald R Cahill, L Donald Bridenbaugh. Anatomic Analysis of a Method to Prevent Pneumothorax. Anaesth Analg 1993;76: LA Grange, PA Foster, LK Pretorius:Application of the Dopler Ultrasound flow detector in supraclavicular brachial plexus block- British Journal of Anaesthesia, 1978;50(9): Stephan R Williams, Philippe Chouinard, Geneviève Arcand, Patrick Harris, Monique Ruel, Daniel Boudreault, François Girard. Ultrasound Guidance Speeds Execution and Improves the Quality of Supraclavicular Block-Anaesth Analg 2003; 97: Berthier F, Lepage D, Henry Y, Vuillier F, Christophe JL, Boillot A, Samain E, Tatu L. Anatomical basis for ultrasound-guided regional anaesthesia at the junction of the axilla and the upper arm: Surgical and Radiologic Anatomy August 2009;08: Vincent WS Chan, et al. Ultrasound-Guided Supraclavicular Brachial Plexus Block Anaesth Analg 2003;97: Cash et al. Spatial mapping of the brachial plexus using threedimensional ultrasound. The British Journal of Radiology 2005;78: Kaur J, Gaur A, Kapila N. Ultrasound guided supraclavicular brachial plexus block and the thyrocervical trunk. Presented at Association of Anaesthetists Annual scientific meeting in Torquay in September Kaur J, Gaur A, Lin E, et al. Supraclavicular brachial plexus block in lateral position- Gaur approach. Presented at European Society of Regional Anaesthesia Annual Congress in Italy in September, Vincent WS Chan, Anahi P, Regan R, Olusegun O. Ultrasound- Guided Supraclavicular Brachial Plexus Block. Anaesth Analg 2003;97: Chan VW, Perlas A, Rawson R, Odukoya O. Ultrasound-guided supraclavicular brachial plexus block. Anaesth Analg 2003; 97: Perlas A, Chan VW, Simons M. Brachial plexus examination and localisation using ultrasound and electrical stimulation: A volunteer study. Anaesthesiology 2003;99: A Searle, G Niraj, Ultrasound Guided Brachial Plexus Block at the supraclavicular Level: A New Parasagittal Approach. International Journal of Ultrasound and Applied Technologies in Perioperative Care, January-April 2010;1(1): Gaertner E, Estebe JP, Zamfir A, et al. Infraclavicular plexus block: Multiple injection versus single injection. Reg Anaesth: Pain Med 2002;27: Fanelli G, Casati A, Beccaria P, et al. Interscalene brachial plexus anaesthesia with small volumes of ropivacaine 0.75%: Effects of the injection technique on the onset time of nerve blockade. Eur J Anaesthesiol 2001;18: Knoblanche GE. The incidence and aetiology of phrenic nerve blockade associated with supraclavicular brachial plexus block. Anaesth Intensive Care 1979;7(4): Gray AT. Ultrasound-guided regional anaesthesia: Current state of the art. Anaesthesiology 2006;104: JAYPEE
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear Transducer
 ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Ultrasound-guided supraclavicular block
 THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
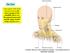 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Interscalene brachial plexus blockade - indications, anatomy, practical performance
 08RC2 Interscalene brachial plexus blockade - indications, anatomy, practical performance Urs Eichenberger Department of Anaesthesiology and Pain Therapy, University Hospital of Bern, Switzerland Saturday,
08RC2 Interscalene brachial plexus blockade - indications, anatomy, practical performance Urs Eichenberger Department of Anaesthesiology and Pain Therapy, University Hospital of Bern, Switzerland Saturday,
Neck-2. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
Diana Mathioudakis DEAA EDIC AFRCA. consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d)
 & Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
& Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
3 Mohammad Al-Mohtasib Areej Mosleh
 3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
INTRODUCTION. Getting the best scan. Choosing a probe. Choosing the frequency
 Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
THE AORTA AND IT S MAJOR BRANCHES
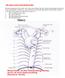 1 THE AORTA AND IT S MAJOR BRANCHES The aorta commences at the aortic valve, above the vestible of the left ventricle and terminates at the level of the fourth lumbar vertebra (L4), where it bifurcates
1 THE AORTA AND IT S MAJOR BRANCHES The aorta commences at the aortic valve, above the vestible of the left ventricle and terminates at the level of the fourth lumbar vertebra (L4), where it bifurcates
STERNUM. Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts:
 STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
Veins of the Face and the Neck
 Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
The Neck. BY: Lina Abdullah & Rahaf Jreisat
 The Neck BY: Lina Abdullah & Rahaf Jreisat Boundaries of the Neck: generally from base of the skull to root of the neck Superior margin :From superior nuchal line of occipital bone up to mastoid process
The Neck BY: Lina Abdullah & Rahaf Jreisat Boundaries of the Neck: generally from base of the skull to root of the neck Superior margin :From superior nuchal line of occipital bone up to mastoid process
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta.
 Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta. Fig-3: Showing high formation of Median nerve. Fig-1: Showing atypical formation of cords of Brachial plexus. 1 = Upper
Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta. Fig-3: Showing high formation of Median nerve. Fig-1: Showing atypical formation of cords of Brachial plexus. 1 = Upper
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
THE DESCENDING THORACIC AORTA
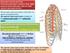 Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
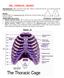 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli.
 Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli. Rectus Capitis Anterior. Rectus Capitis Lateralis. Rectus Capitis
Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli. Rectus Capitis Anterior. Rectus Capitis Lateralis. Rectus Capitis
thoracic cage inlet and outlet landmarks of the anterior chest wall muscles of the thoracic wall sternum joints ribs intercostal spaces diaphragm
 Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Day 5 Respiratory & Cardiovascular: Respiratory System
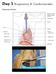 Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
MUSCLES. Anconeus Muscle
 LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Superficial (and Intermediate) Cervical Plexus Block
 Superficial (and Intermediate) Cervical Plexus Block Indications: -Tympanomastoid surgery. When combined with the auricular branch of the vagus ( nerve of arnold ) by infiltrating subcutaneously into the
Superficial (and Intermediate) Cervical Plexus Block Indications: -Tympanomastoid surgery. When combined with the auricular branch of the vagus ( nerve of arnold ) by infiltrating subcutaneously into the
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck.
 Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
The arm: *For images refer back to the slides
 The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns
 213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns CLAVICLE Examine an isolated clavicle and compare it with a clavicle on an articulated skeleton. Viewed from above,
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns CLAVICLE Examine an isolated clavicle and compare it with a clavicle on an articulated skeleton. Viewed from above,
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
Review Article Axillary Brachial Plexus Block
 Anesthesiology Research and Practice Volume 2011, Article ID 173796, 5 pages doi:10.1155/2011/173796 Review Article Axillary Brachial Plexus Block Ashish R. Satapathy and David M. Coventry Department of
Anesthesiology Research and Practice Volume 2011, Article ID 173796, 5 pages doi:10.1155/2011/173796 Review Article Axillary Brachial Plexus Block Ashish R. Satapathy and David M. Coventry Department of
The Language of Anatomy. (Anatomical Terminology)
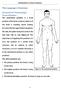 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
Anatomy for anaesthetists
 VOL 17 NO 1 ANESTHESIA JANUARY 1962 Anatomy for anaesthetists (4) The thoracic inlet and the first rib HAROLD ELLIS, MCh, FRCS Senior Lecturer in Surgery, Westminster Hospital Illustrated by MISS MARGARET
VOL 17 NO 1 ANESTHESIA JANUARY 1962 Anatomy for anaesthetists (4) The thoracic inlet and the first rib HAROLD ELLIS, MCh, FRCS Senior Lecturer in Surgery, Westminster Hospital Illustrated by MISS MARGARET
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Anatomy and Physiology II. Spine
 Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
USRA OF THE UPPER EXTREMITY
 USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Upper Limb Muscles Muscles of Axilla & Arm
 Done By : Saleh Salahat Upper Limb Muscles Muscles of Axilla & Arm 1) Muscles around the axilla A- Muscles connecting the upper to thoracic wall (4) 1- pectoralis major Origin:- from the medial half of
Done By : Saleh Salahat Upper Limb Muscles Muscles of Axilla & Arm 1) Muscles around the axilla A- Muscles connecting the upper to thoracic wall (4) 1- pectoralis major Origin:- from the medial half of
Muscle Action Origin Insertion Nerve Innervation Chapter Page. Deltoid. Trapezius. Latissimus Dorsi
 Muscle Action Origin Insertion Nerve Innervation Chapter Page All Fibers Abduct the shoulder (glenohumeral joint) Deltoid Anterior Fibers Flex the shoulder (G/H joint) Horizontally adduct the shoulder
Muscle Action Origin Insertion Nerve Innervation Chapter Page All Fibers Abduct the shoulder (glenohumeral joint) Deltoid Anterior Fibers Flex the shoulder (G/H joint) Horizontally adduct the shoulder
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Vascular Access (venous (peripheral and central) and arterial)
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Mediastinum and pericardium
 Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Copyright 2010 Pearson Education, Inc.
 E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
BRACHIAL PLEXUS. DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae
 THE BRACHIAL PLEXUS DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae SCHEMA OF THE BRACHIAL PLEXUS THE BRACHIAL PLEXUS PHRENIC NERVE supraclavicular
THE BRACHIAL PLEXUS DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae SCHEMA OF THE BRACHIAL PLEXUS THE BRACHIAL PLEXUS PHRENIC NERVE supraclavicular
Chapter 5: Other mediastinal structures. The Large Arteries. The Aorta. Ascending aorta
 Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Anterior triangle of neck
 Anterior triangle of neck Dept. of Anatomy Zhou Hong Ying Outline boundary and subdivisions of ant. triangle contents of the triangle Muscles: suprahyoid muscles, infrahyoid muscles Nerves: CNⅩ, CNⅪ, CNⅫ,
Anterior triangle of neck Dept. of Anatomy Zhou Hong Ying Outline boundary and subdivisions of ant. triangle contents of the triangle Muscles: suprahyoid muscles, infrahyoid muscles Nerves: CNⅩ, CNⅪ, CNⅫ,
Brachial plexuses and axillary lymph nodes
 Brachial plexuses and axillary lymph nodes Introduction about nervous system nervous system central nervous system periphral nervous system brain spinal cord 31 pairs of spinal nerves 12 paris of cranial
Brachial plexuses and axillary lymph nodes Introduction about nervous system nervous system central nervous system periphral nervous system brain spinal cord 31 pairs of spinal nerves 12 paris of cranial
Anatomy of thoracic wall
 Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
The pectoral region. University of Babylon College of Medicine Dr.HaythemAli Alsayigh M.B.CH.B.-F.I.M.B.S. Surgical Clinical Anatomy
 The pectoral region University of Babylon College of Medicine Dr.HaythemAli Alsayigh M.B.CH.B.-F.I.M.B.S. Surgical Clinical Anatomy Objective Study the Bones and Joints A. Clavicle (collarbone) B. Scapula
The pectoral region University of Babylon College of Medicine Dr.HaythemAli Alsayigh M.B.CH.B.-F.I.M.B.S. Surgical Clinical Anatomy Objective Study the Bones and Joints A. Clavicle (collarbone) B. Scapula
Upper limb Pectoral region & Axilla
 Upper limb Pectoral region & Axilla 黃敏銓 mchuang@ntu.edu.tw 1 Pectoral region Intercostal nerve Anterior branch of lateral cutaneous branch Lateral cutaneous branch Anterior cutaneous branch Anterior cutaneous
Upper limb Pectoral region & Axilla 黃敏銓 mchuang@ntu.edu.tw 1 Pectoral region Intercostal nerve Anterior branch of lateral cutaneous branch Lateral cutaneous branch Anterior cutaneous branch Anterior cutaneous
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Fascial Compartments of the Upper Arm
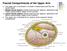 Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Ultrasound-guided Sciatic Nerve Blocks: Higher and Popliteal Approaches
 10.5005/jp-journals-10027-1026 K Kondov, S Fransis REVIEW ARTICLE Ultrasound-guided Sciatic Nerve Blocks: Higher and Popliteal Approaches K Kondov, S Fransis ABSTRACT Background and objective: In modern
10.5005/jp-journals-10027-1026 K Kondov, S Fransis REVIEW ARTICLE Ultrasound-guided Sciatic Nerve Blocks: Higher and Popliteal Approaches K Kondov, S Fransis ABSTRACT Background and objective: In modern
The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care settings,
 American Journal of Emergency Medicine (2011) xx, xxx xxx www.elsevier.com/locate/ajem Clinical Notes The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care
American Journal of Emergency Medicine (2011) xx, xxx xxx www.elsevier.com/locate/ajem Clinical Notes The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care
Infraclavicular brachial plexus blocks have been designed
 The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
ABDOMINAL WALL & RECTUS SHEATH
 ABDOMINAL WALL & RECTUS SHEATH Learning Objectives Describe the anatomy, innervation and functions of the muscles of the anterior, lateral and posterior abdominal walls. Discuss their functional relations
ABDOMINAL WALL & RECTUS SHEATH Learning Objectives Describe the anatomy, innervation and functions of the muscles of the anterior, lateral and posterior abdominal walls. Discuss their functional relations
Anatomy Lecture #19 AN INTRODUCTION TO THE THORAX April 3, 2012
 Page 1 بسم الله الرحمن الرحيم The Thoracic Wall Firstly, when we talk about thorax, we should begin with the thorax wall which means not only bones that construct the thorax but also the muscles which
Page 1 بسم الله الرحمن الرحيم The Thoracic Wall Firstly, when we talk about thorax, we should begin with the thorax wall which means not only bones that construct the thorax but also the muscles which
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE CORNISH TECHNIQUE
 THE JOURNAL OF NEW YORK SCHOOL OF REGIONAL ANESTHESIA SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE BY CORHISH PB Author Affiliation: Nelson, New Zealand This essay is based on a project which has
THE JOURNAL OF NEW YORK SCHOOL OF REGIONAL ANESTHESIA SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE BY CORHISH PB Author Affiliation: Nelson, New Zealand This essay is based on a project which has
slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments
 Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Regional Anaesthesia of the Thoracic Limb
 Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Anatomy of the Shoulder Girdle. Prof Oluwadiya Kehinde FMCS (Orthop)
 Anatomy of the Shoulder Girdle Prof Oluwadiya Kehinde FMCS (Orthop) www.oluwadiya.com Bony Anatomy Shoulder Complex: Sternum(manubrium) Clavicle Scapula Proximal humerus Manubrium Sterni Upper part of
Anatomy of the Shoulder Girdle Prof Oluwadiya Kehinde FMCS (Orthop) www.oluwadiya.com Bony Anatomy Shoulder Complex: Sternum(manubrium) Clavicle Scapula Proximal humerus Manubrium Sterni Upper part of
Thyroid and Parathyroid Glands
 Thyroid and Parathyroid Glands Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/ explanation Objectives: By the end of the lecture,
Thyroid and Parathyroid Glands Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/ explanation Objectives: By the end of the lecture,
THYROID & PARATHYROID. By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy
 THYROID & PARATHYROID By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy 1 OBJECTIVES By the end of the lecture, the student should be able to: Describe the shape, position, relations and structure of
THYROID & PARATHYROID By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy 1 OBJECTIVES By the end of the lecture, the student should be able to: Describe the shape, position, relations and structure of
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E
 Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Sonographic Mapping of the Normal Brachial Plexus
 AJNR Am J Neuroradiol 24:1303 1309, August 2003 Sonographic Mapping of the Normal Brachial Plexus Xavier Demondion, Pascal Herbinet, Nathalie Boutry, Christian Fontaine, Jean-Paul Francke, and Anne Cotten
AJNR Am J Neuroradiol 24:1303 1309, August 2003 Sonographic Mapping of the Normal Brachial Plexus Xavier Demondion, Pascal Herbinet, Nathalie Boutry, Christian Fontaine, Jean-Paul Francke, and Anne Cotten
FUNCTIONAL ANATOMY OF SHOULDER JOINT
 FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
Anatomy Lecture 8. In the previous lecture we talked about the lungs, and their surface anatomy:
 Anatomy Lecture 8 In the previous lecture we talked about the lungs, and their surface anatomy: 1-Apex:it lies 1 inch above the medial third of clavicle. 2-Anterior border: it starts from apex to the midpoint
Anatomy Lecture 8 In the previous lecture we talked about the lungs, and their surface anatomy: 1-Apex:it lies 1 inch above the medial third of clavicle. 2-Anterior border: it starts from apex to the midpoint
Upper limb Arm & Cubital region 黃敏銓
 Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Note : I put the sheet's info within the slides to easily understand this lecture Done by : Zaid Al-Ghnaneem
 Note : I put the sheet's info within the slides to easily understand this lecture Done by : Zaid Al-Ghnaneem Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including
Note : I put the sheet's info within the slides to easily understand this lecture Done by : Zaid Al-Ghnaneem Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including
Neck Ultrasound. Faculty Info: Amy Kule, MD
 Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Axilla and Brachial Region
 L 4 A B O R A T O R Y Axilla and Brachial Region BRACHIAL PLEXUS 5 Roots/Rami (ventral rami C5 T1) 3 Trunks Superior (C5, C6) Middle (C7) Inferior (C8, T1) 3 Cords Lateral Cord (Anterior Superior and Anterior
L 4 A B O R A T O R Y Axilla and Brachial Region BRACHIAL PLEXUS 5 Roots/Rami (ventral rami C5 T1) 3 Trunks Superior (C5, C6) Middle (C7) Inferior (C8, T1) 3 Cords Lateral Cord (Anterior Superior and Anterior
Yara saddam & Dana Qatawneh. Razi kittaneh. Maher hadidi
 1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
Regional Anaesthesia
 Regional Anaesthesia Basic Sciences Anaesthetic Course Dr Vassilis ATHANASSOGLOU FRCA Consultant Anaesthetist and Lecturer in Medicine Oxford University Hospitals NHS Trust, UK Geneva, 5th June 2017 Faculty
Regional Anaesthesia Basic Sciences Anaesthetic Course Dr Vassilis ATHANASSOGLOU FRCA Consultant Anaesthetist and Lecturer in Medicine Oxford University Hospitals NHS Trust, UK Geneva, 5th June 2017 Faculty
Surface anatomy of Cardiovascular system
 Surface anatomy of Cardiovascular system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The lines cover the front, side, and back of the thorax Midsternal
Surface anatomy of Cardiovascular system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The lines cover the front, side, and back of the thorax Midsternal
Diaphragm and intercostal muscles. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Infraclavicular brachial plexus blocks aim at the
 REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
Surgical Anatomy of the Neck. M. J. Jurkiewicz, John Bostwick. Surgical Clinics of North America, Vol 54, No 6, December 1974.
 Surgical Anatomy of the Neck M. J. Jurkiewicz, John Bostwick Surgical Clinics of North America, Vol 54, No 6, December 1974. The radical neck dissection is a safe, effective therapeutic procedure for eradication
Surgical Anatomy of the Neck M. J. Jurkiewicz, John Bostwick Surgical Clinics of North America, Vol 54, No 6, December 1974. The radical neck dissection is a safe, effective therapeutic procedure for eradication
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone
 *the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
Ultrasound Physics and Knobology Alan Macfarlane. Consultant Anaesthetist Glasgow Royal Infirmary
 Ultrasound Physics and Knobology Alan Macfarlane Consultant Anaesthetist Glasgow Royal Infirmary RAPM 2009; 34: 40-46 Ultrasound Proficiency Understanding US image generation and device operation Image
Ultrasound Physics and Knobology Alan Macfarlane Consultant Anaesthetist Glasgow Royal Infirmary RAPM 2009; 34: 40-46 Ultrasound Proficiency Understanding US image generation and device operation Image
The posterior abdominal wall. Prof. Oluwadiya KS
 The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
Chapter 28: The neck. Fascia of the neck
 Chapter 28: The neck Fascia of the neck The superficial fascia is a fatty areolar layer between the skin and the more obvious deep fascia. It contains the platysma muscles and the external jugular veins
Chapter 28: The neck Fascia of the neck The superficial fascia is a fatty areolar layer between the skin and the more obvious deep fascia. It contains the platysma muscles and the external jugular veins
Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of th
 Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of the fact that they support the least load. In humans,
Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of the fact that they support the least load. In humans,
PLEURAE and PLEURAL RECESSES
 PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
CARDIOVASCULAR DANIL HAMMOUDI.MD
 CARDIOVASCULAR DANIL HAMMOUDI.MD 18 Systemic Circulation Figure 19.19 Pulmonary Circulation Figure 19.18b 1. Thyroid gland 2. Trachea 3. Brachiocephalic 4. Common carotid 5. Internal jugular 6. Superior
CARDIOVASCULAR DANIL HAMMOUDI.MD 18 Systemic Circulation Figure 19.19 Pulmonary Circulation Figure 19.18b 1. Thyroid gland 2. Trachea 3. Brachiocephalic 4. Common carotid 5. Internal jugular 6. Superior
