Review Article Brachial Plexus Injuries in Adults: Evaluation and Diagnostic Approach
|
|
|
- Susanna Carroll
- 5 years ago
- Views:
Transcription
1 ISRN Orthopedics, Article ID , 9 pages Review Article Brachial Plexus Injuries in Adults: Evaluation and Diagnostic Approach Vasileios I. Sakellariou, 1 Nikolaos K. Badilas, 2 George A. Mazis, 1 Nikolaos A. Stavropoulos, 1 Helias K. Kotoulas, 2 Stamatios Kyriakopoulos, 2 Ioannis Tagkalegkas, 2 and Ioannis P. Sofianos 2 1 First Department of Orthopedic Surgery, Athens University Medical School, Attikon University General Hospital, Chaidari,12462Athens,Greece 2 Department of Orthopedic Surgery, General HospitalofLevadia,32100,Levadia,Greece Correspondence should be addressed to Vasileios I. Sakellariou; bsakellariou@gmail.com Received 7 October 2013; Accepted 6 November 2013; Published 9 February 2014 Academic Editors: P. V. Kumar and M. M. Tomaino Copyright 2014 Vasileios I. Sakellariou et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. The increased incidence of motor vehicle accidents during the past century has been associated with a significant increase in brachial plexus injuries. New imaging studies are currently available for the evaluation of brachial plexus injuries. Myelography, CT myelography, and magnetic resonance imaging (MRI) are indicated in the evaluation of brachial plexus. Moreover, a series of specialized electrodiagnostic and nerve conduction studies in association with the clinical findings during the neurologic examination can provide information regarding the location of the lesion, the severity of trauma, and expected clinical outcome. Improvements in diagnostic approaches and microsurgical techniques have dramatically changed the prognosis and functional outcomeofthesetypesofinjuries. 1. Introduction Brachial plexus is a complex network of nerves, which is responsible for the innervation of the upper extremity. It is formed in the posterior cervical triangle by the union of ventral rami of 5th, 6th, 7th, and 8th cervical nerve roots and 1st thoracic nerve root. This composite nerve network can be divided into roots, trunks, divisions, and cords. The roots, trunks, and divisions lie in the posterior triangle of the neck, whereas the cords lie in the axillary fossa. Cords are further divided in the major nerve branches of the upper extremity [1](Figure 1). Roots and trunks lie in the supraclavicular space; the divisions are located posterior to the clavicle, while cords and branches lie infraclavicularly [2]. Branches that arise from different portions of brachial plexus are shown in the following figure (Figure 2). All three cords of the plexus lie above and laterally to the medial portion of axillary artery. Medial cord crosses the artery, passing inferiorly, to reach the medial surface of the middle portion of the artery. Posterior cord is located behind the middle portion of the artery and lateral cord lies laterally to the middle portion of the artery. The names of the cords of brachial plexus imply their relationship to the middle portion of the axillary artery (Figure3). Anatomic variants of brachial plexus are observed in more than 50% of the cases [3]. Most common variants are associated with the contribution of C4 (prefixed) or with the contribution of T2 nerve root to the plexus (postfixed) (Figure 4). It is estimated that C4 nerve root contributes to the formation of brachial plexus in 28 62% of cases, according to cadaveric studies [2, 4]. T2 nerve root contributes to the formation of brachial plexus in 16 73% of cases [2, 5, 6]. These contributions may vary in size. 2. Pathology The type of brachial plexus injury depends mainly on the location of injury within the nerve route, that is, within
2 2 ISRN Orthopedics er Sup ior l era Lat dle Mid d cor Inferior rd r co rio te Pos d Me ial d cor Figure 1: Classic form of brachial plexus. Dorsal scapular nerve Suprascapular nerve Subclavius nerve Lateral pectoral nerve Thoracodorsal nerve Musculocutaneous nerve Axillary nerve Upper and lower subscapular nerve Radial nerve Median nerve Medial pectoral nerve Ulnar nerve Long thoracic nerve Medial cutaneous nerve of the arm Medial cutaneous nerve of forearm Figure 2: Roots, trunks, divisions, cords, and terminal branches of brachial plexus. the rootlets, the roots or within the intervertebral foramina through which they pass. In each spinal segment, roots are formed from the union of the dorsal (sensory) and ventral (motor) rootlets that exit the spinal column and pass through the corresponding intervertebral foramen. Cell bodies of sensory neurons are located in the dorsal root ganglia, outside the spinal cord. The rootlets that form cervical roots are located within the spinal cord and lack connective tissue and meningeal coating. As a result to this anatomic peculiarity, rootlets are vulnerable to avulsion injuries from the spinal cord. Spinal nerves have the ability to move freely within the intervertebral foramina,
3 ISRN Orthopedics 3 Dorsal scapular nerve Suprascapular nerve Subclavius nerve Lateral pectoral nerve Musculocutaneous nerve Median nerve Axillary artery Long thoracic nerve Radial nerve Medial pectoral nerve Medial cutaneous nerve of forearm Teres minor muscle Ulnar nerve Axillary vein Medial cutaneous nerve of the arm Figure 3: Relationships of brachial plexus and its portions of the axillary artery. Prefixed C4 T2 Postfixed (a) (b) Figure 4: Cephalad (prefixed) and caudal shift (postfixed) of roots that consist of brachial plexus. since they do not have any attachments on them. However, there are fibrous attachments that may be found at the C4 to levels, which tie spinal nerves down to transverse processes, after their exit from intervertebral foramina. This does not apply to the spinal nerves of the levels and. This anatomical variance explains the comparatively greater incidence of avulsion injuries of the lower two roots of the brachial plexus comparing to the higher anatomic levels [7]. The most important step when examining a brachial plexus injury is to determine whether it affects the roots and is defined as preganglionic (proximal to the dorsal root ganglion) or postganglionic [8] (Figure 5). Determination of the distance of the level of injury from the spinal cord offers very important information. In case of a preganglionic injury, the nerve is avulsed from spinal cord, separating motor neurons from the motor centers of the ventral horns of the spinal cord. Sensory neurons remain intact at the level of dorsal root ganglion, which explains why sensory nerve action potentials are preserved in preganglionic lesions. Preganglionic lesions are not repairable and alternative working motor nerves need to be transferred in order to restore part of the functionality of the upper limp. Contrarily, postganglionic lesions may be restored spontaneously (in case of axonotmesis) or may be repaired surgically. In these lesions, both sensory and motor action potentials are influenced since both sensory and motor rootlets are ruptured.
4 4 ISRN Orthopedics Dorsal root ganglion Avulsion Stretch (a) (b) (c) Rupture (d) Figure 5: (a) Normal anatomy of rootlets and roots. (b) Avulsive preganglionic injury. (c, d) Postganglionic injury. 3. Epidemiology It is difficult to specify the exact number of patients with brachial plexus injuries per year. However, due to the increasing participation in extreme sports and the increased number of motor vehicle accidents survivors, there is global increase in the incidence of brachial plexus injuries [9 14]. There is a significant predilection in male gender and ages between 15 and 25 years old [13, 15 17]. Narakas found that 70% of traumatic brachial plexus lesions are due to traffic accidents and70%oftheminvolvetheuseofmotorcycles[18]. 4. Classification of Peripheral Nerves Injuries Myelinated peripheral nerve fibers are surrounded by Schwann cells. Every nerve fiber with the accompanying Schwann cells is surrounded by a layer of delicate connective tissue, called endoneurium. Groups of nerve fibers compose the fascicles, which are enveloped within a layer of collagen, the perineurium. Most nerves consist of different number of fascicles, which are bundled together by loose collagen fibers, concentrated at the periphery in a relatively thick outer layer, the epineurium. Historically, peripheral nerve injuries are described by the classification systems of Seddon and Sunderland. The classification proposed by Seddon describes three groups of nerve injuries: neurapraxia, axonotmesis, and neurotmesis [19]. Neurapraxia is defined as the presence of nerve dysfunction without macroscopic lesion of the nerve. Transmission ofnerveimpulsesisinterruptedatthesiteoflesion,which lasts for a short period of time, lasting from a few hours to few months, depending on the area and the severity of the injury. Tinel sign is not elicited during physical examination. Nerve conduction techniques reveal lack of conductivity at the point of the lesion, yet conductivity distally to the injury is normal. This is a pathognomonic finding in neurapraxia [20]. In axonotmesis, the axial continuity of some individual nerve Table 1: Comparison of Seddon and Sunderland classifications of nerve injury. Sunderland Seddon Histopathology 1 Neurapraxia Functional but not anatomical disorganization 2 Axonotmesis Intact endoneurium and perineurium 3 Axonotmesis Intact perineurium 4 Axonotmesis Intact epineurium 5 Neurotmesis Disruption of all layers fibers is interrupted, but perineurium and epineurium are preserved. Neurotmesis is defined as a complete disruption of the axon, along with every part of the connective tissue of the peripheral nerve. Spontaneous recovery of the affected nerve axon cannot be expected. Without surgical intervention, this kind of injury may lead to the creation of a nonfunctional neuroma. In the classification described by Sunderland, the group of axonotmesis is graded in three degrees, suggesting that different anatomic disruption leads to correspondingly different prognosis [21](Table 1). 5. Mechanism of Injury Brachial plexus injuries (BPIs) most commonly affect the supraclavicular zone. Infraclavicular and retroclavicular lesions are less common. Roots and trunks get more easily affected comparing to cords and terminal branches. Two level injuries occur and should be included in differential diagnosis. At the level of supraclavicular region, avulsion injuries are observed after violent lateral head and neck turn away from the ipsilateral shoulder (Figure 6), resulting in the,,androotoruppertrunkdisruption.avulsion injuries can be also observed in the case of forceful traction of the upper limp. When the upper limp is abducted above
5 ISRN Orthopedics 5 Figure 6: Upper brachial plexus injury occurs when the head and neck are moved away from the ipsilateral shoulder violently. Figure 7: Lower brachial plexus injury occurs when the upper limp is abducted above the level of head with considerable force. the level of head with considerable force, avulsion injury of - roots or lower trunk is possible (Figure 7). Brachial plexus injuries of the distal part of infraclavicular level are usually caused by high energy trauma in shoulder region. These injuries can be accompanied by rupture of the axillary artery. Seventy to seventy-five percent of traumatic brachial plexus injuries are located in the supraclavicular region. 75% of them involve total plexus lesions (-), - root injuries account for 20 25% of traumatic BPIs, whereas isolated - root lesions account for 2 3.5% of traumatic BPIs. Total brachial plexus injuries usually involve rupture of - roots and avulsion of - roots [22]. Open brachial plexus injuries may be observed; however, these are much less common comparing to closed BPIs. Iatrogenic lesions of brachial plexus have been reported during various surgical procedures, including mastectomies, resections of the first rib, and carotid-subclavian bypass operations [23 25]. The outcome of a traumatic brachial plexus injury depends mainly on patient s age, the type of the injured nerve, the level of injury, the time of surgical intervention, and concomitant diseases (Table 2). 6. Physical Examination Brachial plexus injuries are often accompanied by other severe injuries. These injuries may hinder the diagnosis of a nerve injury until patient s recovery. For this reason, high level of suspicion is mandatory in case of an injury of the shoulder girdle or any trauma involving fracture of the first rib or rupture of the axillary artery. Clinically, brachial plexus injuries can be divided according to their location into injuries of the upper plexus (Erb s palsy) and of the lower plexus (Klumpke s palsy). A detailed examination of brachial plexus and its terminal branches can be performed within a few minutes in case of cooperative patients. In supraclavicular injuries, the shoulder is adducted and internally rotated, whereas the elbow is pronated. Suprascapular nerve injuries, which are located at or posterior to the suprascapular notch, are associated with the presence of
6 6 ISRN Orthopedics Table 2: Factors that affect the prognosis of a peripheral nerve injury. Factor Mechanism of injury Age Type of nerve Level of injury Pain Time of surgical intervention Other factors Result High energy injuries have worse prognosis Avulsion injuries have worse prognosis than acute ruptures Worse prognosis with concomitant vascular injury Better prognosis in young patients Exclusively sensory or motor nerves have better functional recovery than mixed nerves Supraclavicular lesions have worse prognosis than infraclavicular Upper trunk lesions have the best prognosis Patients with persistent pain for more than 6 months after traumatic BPI have less possibilities for recovery Fibrosis and degeneration of target organs at the time of surgical intervention are related to poor prognosis Concomitant diseases (infections, etc.) are related to worse prognosis tenderness over the notch, muscle weakness during shoulder abduction, and external rotation. Lesions at the level of spinoglenoid notch are related to isolated weakness of infraspinatus muscle [26]. Palsy of long thoracic nerve is clinically evident with a defect during scapular abduction, while dorsal scapular nerve deficit will affect the stabilization of the scapula. Injuries at the infraclavicular level may have been generated by high energy trauma mechanisms at the shoulder level and may be potentially associated with rupture of the axillary artery. Axillary, suprascapular, and musculocutaneous nerves are most likely the affected nerves at that level of injury [22, 27]. The evaluation of median, ulnar, and radial nerve is performed by the examination of wrist and fingers. The musculocutaneous nerve as well as high lesions of radial nerve is examined by the flexion and extension of the elbow. The axillary nerve, which is a branch of the posterior cord, is examined with active shoulder abduction and deltoid muscle strength. Injury to the posterior cord may affect the function of radial nerve and the muscles that it enervates. Latissimus dorsi is innervated by the thoracodorsal nerve, which is also a branch of the posterior cord and is located closely to the posterior wall of axillary fossa. Pectoralis major receives innervation by the medial and lateral nerves, which are branches of medial and lateral cord, respectively. Lateral anterior thoracic nerve innervates the clavicle, whereas medial anterior thoracic nerve innervates the sternocostal head of the muscle. The muscle can be palpated as the patient adducts his arm under resistance. Proximally, the suprascapular nerve is a terminal nerve branch at the level of trunks. Table 3: Terminal branches of brachial plexus and their action. Nerve Muscle Action Dorsal scapular () Rhomboid Stabilization of scapula Serratus Long thoracic () Abduction of scapula anterior Suprascapular () Medial () and lateral pectoral () Subscapular () Thoracodorsal () Musculocutaneous () Ulnar (, ) Median (,,, ) Radial (,, ) Axillary () Supraspinatus Infraspinatus Abduction of shoulder External rotation of shoulder Pectoralis major Adducts the shoulder Pectoralis minor Stabilizes the scapula Subscapularis and teres major Internal rotation of shoulder Latissimus dorsi Adduction of shoulder Biceps brachii Flexion of elbow and brachialis Flexor carpi ulnaris Intrinsic muscles of hand Pronators of forearm Flexors of wrist and fingers Supinator Triceps brachii Extensors of wrist and fingers Deltoid and teres minor Flexion of wrist and fingers Abduction of fingers Pronation of forearm Flexion of wrist and fingers Supination of forearm Extension of elbow, wrist, and fingers Abduction of shoulder Motor function of terminal branches is presented in Table 3. Apart from motor dysfunction, sensory deficient is an additional sign to examine. Clinical findings suggestive of a root avulsion injury are (1) reported constrictive or caustic pain in an otherwise insensitive upper limb; (2) when scapular muscles, serratus anterior, and rhomboid are not functioning, dorsal scapular as well as long thoracic nerve is formed just distally to roots; (3) Horner syndrome-lid ptosis, meiosis (constricted pupil), enopthalmos, and loss of hemifacial sweating (anhidrosis) ( root is in proximity to sympathetic ganglion and avulsion injuries occur frequently to both these two structures). Moreover, preganglionic lesions are seldom accompanied by serious vascular injuries, fractures of cervical spine, and dysfunction of spinal cord. 7. Diagnostic Approach 7.1. Imaging Studies. Radiographic imaging after a neck or shoulder girdle injury may reveal evidence of a concomitant neurological lesion. Radiographs of cervical spine, shoulder girdle,humerus,andchestshouldbeobtained.cervicalspine radiographs should be evaluated for fractures, which could
7 ISRN Orthopedics 7 imply that spinal cord is in danger. Moreover, the presence of fracture in the transverse process of a cervical vertebra indicates possible root avulsion at the same level. Clavicle fractures are also indicative of a possible brachial plexus injury. Clavicle radiographs can reveal fractures of the first or second rib, which may suggest injury to the overlying part of brachial plexus. In addition, a meticulous inspection of a chest radiograph can reveal past rib fractures, which are very important in case that transfer of intercostal nerves is planned, since intercostal nerves are frequently injured by fractures of the corresponding ribs. When phrenic nerve is injured, this is indicated by thepresenceofelevatedandparalyzedhemidiaphragm. Computed tomography (CT), along with computed tomographic myelography (CTM), contributes greatly to the evaluation of the level of nerve injury [28 30]. In case of a cervical root avulsion a pseudomeningocele could be formed, in the process of dura mater healing. Immediately after the injury, blood clots appear at the avulsion point. These clots become apparent in myelography as overshadowing at the pointofthelesionandaround.duringthefirstdaysafter the injury, a positive finding may be unreliable, as the dura mater may have been ruptured without concomitant cervical root avulsion. For this reason, CT myelography must be performed 3 to 4 weeks posttraumatically in order to assure that there is enough time for blood clots to be absorbed and for the formation of pseudomeningocele which is an indicative sign of root avulsion injury in CTM. Myelographic studies in combination with magnetic resonance imaging are essentially a T2 sequence, which points out the contrast of spinal cord and roots to cerebrospinal fluid. Compared to CT, MRI has certain advantages. It is a noninvasive method which can depict more lesions apart from root injuries and a formed pseudomeningocele. It can depict brachial plexus almost in total. It can reveal posttraumatic neuromas, along with the concomitant inflammatory response and edema of the surrounding tissues. However, there are a lot of possible mistakes in brachial plexus injuries imagining with conventional MRI. The slices that are taken have relatively large distance between them, in order to reassure acceptable signal to noise ratio (SNRs), with thecostoflowresolutionandinabilitytodiagnosecertain underlying lesions. Moreover, there are artifacts caused by motion such as swallowing, tremor, respiratory, and cardiac movements of the chest, as well as cerebrospinal fluid flow interference which could downgrade the quality of imaging [31]. Even if newer MRI imaging modalities with improved diagnostic results are available, improvements have to be made to reduce artifacts and interferences, in order to establish MRI as a reliable method in detecting brachial plexus root lesions Histamine Test. Its purpose is to differentiate preganglionic and postganglionic lesions, but nowadays it is rarely performed. The intradermal injection of histamine causes triple response (red reaction due to capillary dilatation, wheal due to fluid extravasation from increased permeability, and flare due to arteriolar dilatation and to axon reflex in sensory nerve). If there is response with flare in an otherwise unconscious skin area, then the lesion has to be proximal to the dorsal root ganglion, which means that it must be a root avulsion injury. On the contrary, when the lesion is postganglionic the test will be negative as the continuity between the skin and dorsal root ganglion will have been interrupted Electrodiagnostic Tests. Electrodiagnostic tests are an integral part of both preoperative and intraoperative evaluation, providing that there is proper conduction and evaluation of their results. Electrodiagnostic evaluation may confirm the diagnosis, pinpoint the lesions, determine the severity of axial discontinuity, and eliminate other clinical entities from differential diagnosis. They are valuable tools, whichmustbeusedinconjunctionwithmeticulousphysical examination and adequate imaging evaluation, and not as their substitute. In closed injuries, electromyography (EMG) and nerve conduction velocity studies (NVCs) may be performed 3-4 weeks after the injury, when the conduction of the potentials has stopped along a nerve with postganglionic injury due to Wallerian degeneration. Serial testing in conjunction with repeated physical examination every few months can document and quantify ongoing reinnervation or denervation. Electromyography (EMG) tests muscles at rest and during activity. Denervation changes (fibrillation potentials) can be seen as early as 10 to 14 days after injury in proximal muscles and as late as 3 to 6 weeks in distal muscles. The presence of voluntary motor unit potentials with limited fibrillation potentials signifies better prognosis than the cases where there is absence of motor unit potentials and many fibrillation potentials. Nerve conduction velocity studies (NCSs) are performed along with EMG. In posttraumatic brachial plexus injuries, the amplitude of compound muscle action potentials is generallylowandisrelatedtothetotalamountoffunctional muscle fibers. Sensory nerve action potentials are very important in localizing a lesion as preganglionic or postganglionic. SNAPs will be preserved in lesions proximal to the dorsal root ganglia, due to the fact that the sensory nerve cell bodies are intact within the dorsal root ganglion. For this, in preganglionic injuries there are normal SNAPs in an otherwise insensate dermatome and muscle action potentials (MAPs) are absent. SNAPs will be absent in a postganglionic or combined pre- and postganglionic lesion. Due to the overlapping sensory innervation, especially in the index finger, attention has to be paid when the localization of preganglionic lesion is based on SNAPs exclusively. It has to be notified that there are obvious restrictions in the diagnostic capacity of electrodiagnostic tests. The diagnostic benefit of EMG/NCSs is related to the experience and the capability of the clinician to interpret the results of these tests. Early signs of muscle recovery may be detected on EMG (occurrence of nascent potentials, decreased number of fibrillation potentials, appearance of or an increased number of motor unit potentials). These signs contribute to expected
8 8 ISRN Orthopedics Table 4: Neurophysiological findings in traumatic peripheral nerve injuries, in each category, respectively, according to Seddon classification. Neurapraxia Axonotmesis Neurotmesis Conduction Normal/mild Usually normal velocity reduction Absent CMAP frequency Normal/reduced Reduced Absent SNAP frequency Reduced Reduced Absent Abnormal Probably spontaneous Absent present potentials in EMG Present Source: [8]. clinical recovery in weeks or months. However, EMG recovery does not always ensure relevant clinical recovery. In addition, EMG evidence of ongoing reinnervation may not be detected in lesions where target end organs are more distal. The use of intraoperative electrodiagnostic tests is an integral part of brachial plexus surgery. Combined electrodiagnostic techniques like nerve action potentials (NAPs), somatosensory evoked potentials (SSEPs), and compound muscle action potentials (CMAPs) may give adequate additional information in order to help the surgeon in decision making [32 34](Table 4). 8. Conclusion Knowledge of topographic anatomy (origin, course, and relations of the involved roots with the neighboring anatomic elements), anatomy and physiology of central and peripheral nervous system, and connections of roots, trunks, and nerves with target organs, as well as their sensory innervation in combination with repeated, thorough, and recorded clinical examination, are the keystones of diagnostic evaluation of brachial plexus injuries. Plain radiographs, computed tomography, CT myelography, and magnetic resonance imaging with or without contrast and electrodiagnostic tests are invaluable accessory tools in the evaluation and diagnostic approach of traumatic brachial plexus injuries, each with its own sensitivity and specificity. Each of these techniques plays an important part in intraoperative and postoperative diagnosis and evaluation. In order to optimize the anticipated results, the use of each diagnostic method within the appropriate time frame is of paramount importance. Conflict of Interests None of the authors has a secondary interests such as financial gain and a conflict of interest with the mentioned commercial identities in this paper. References [1] R. S. Snell, Clinical Anatomy, Lippincott Williams & Wilkins, 8th edition, [2] A.Kerr, Brachialplexusofnervesinman.Thevariationsinits formation and branches, American Journal of Anatomy,vol.23, article 285, [3]I.I.Uysal,M.Şeker, A. K. Karabulut et al., Brachial plexus variations in human fetuses, Neurosurgery, vol. 53, no. 3, pp , [4] B. Senecail, Le plexus brachial de l Homme [Ph.D. thesis],1975. [5] H. Adolphi, Uber das Verhalten der zweiten Brustnerven zum plexus brachialis beim Menschen, Anatomischer Anzeiger,vol. 15, pp , [6] K. Hirasawa, Uber den pelxus brachialis mitterlung die wurzeln des plexus brachial, in ImpressioSeparataexActis Scholac Medicinalis, Univeritatis Imperialis Kiotoensis, Paris, France, [7] A. Y. Shin and R. J. Spinner, Clinically relevant surgical anatomy and exposures of the brachial plexus, Hand Clinics, vol. 21, no. 1, pp. 1 11, [8] J. Gregory, A. Cowey, M. Jones, S. Pickard, and D. Ford, The anatomy, investigations and management of adult brachial plexus injuries, Orthopaedics and Trauma, vol. 23, no. 6, pp , [9] Y. Allieu and P. Cenac, Is surgical intervention justifiable for total paralysis secondary to multiple avulsion injuries of the brachial plexus? Hand Clinics, vol. 4, no. 4, pp , [10] R. J. Azze, R. Mattar Jr., M. C. Ferreira, R. Starck, and A. C. Canedo, Extraplexual neurotization of brachial plexus, Microsurgery,vol.15,no.1,pp.28 32,1994. [11] K. E. Brandt and S. E. Mackinnon, A technique for maximizing biceps recovery in brachial plexus reconstruction, Journal of Hand Surgery,vol.18,no.4,pp ,1993. [12] G. Brunelli and L. Monini, Direct muscular neurotization, Journal of Hand Surgery,vol.10,no.6,pp ,1985. [13] K. Doi, K. Muramatsu, Y. Hattori et al., Restoration of prehension with the double free muscle technique following complete avulsion of the brachial plexus. Indications and longterm results, Journal of Bone and Joint Surgery A, vol. 82, no. 5, pp , [14]K.Doi,N.Kuwata,K.Muramatsu,Y.Hottori,andS.Kawai, Double muscle transfer for upper extremity reconstruction following complete avulsion of the brachial plexus, Hand Clinics,vol.15,no.4,pp ,1999. [15]J.M.Malone,J.M.Leal,J.Underwood,andS.J.Childers, Brachial plexus injury management through upper extremity amputation with immediate postoperative prostheses, Archives of Physical Medicine and Rehabilitation,vol.63,no.2,pp.89 91, [16] Y. Allieu, Evolution of our indications for neurotization. Our concept of functional restoration of the upper limb after brachial plexus injuries, Annales de Chirurgie de la Main et du Membre Superieur,vol.18,no.2,pp ,1999. [17] A. S. Dubuisson, D. G. Kline, A. P. Amar, J. P. Gruen, M. Kliot, and S. Yamada, Brachial plexus injury: a survey of 100 consecutive cases from a single service, Neurosurgery, vol.51, no.3,pp ,2002. [18] A. O. Narakas, The treatment of brachial plexus injuries, International Orthopaedics,vol.9,no.1,pp.29 36,1985. [19] H. J. Seddon, Three types of nerve injury, Brain,vol.66,no.4, pp , [20] S. E. Mackinnon, Nerve grafts, in The Unfavorable Result in Plastic Surgery, R. M. Goldwyn and M. N. Cohen, Eds., Lippincott, Williams & Wilkins, Philadelphia, Pa, USA, 2001.
9 ISRN Orthopedics 9 [21] S. Sunderland, A classification of peripheral nerve injuries producing loss of function, Brain, vol. 74, no. 4, pp , [22] S. L. Moran, S. P. Steinmann, and A. Y. Shin, Adult brachial plexus injuries: mechanism, patterns of injury, and physical diagnosis, Hand Clinics, vol. 21, no. 1, pp , [23] S. H. Horowitz, Brachial plexus injuries with causalgia resulting from transaxillary rib resection, Archives of Surgery, vol. 120, no. 10, pp , [24] J. D. Sinow and B. L. Cunningham, Postmastectomy brachial plexus injury exacerbated by tissue expansion, Annals of Plastic Surgery,vol.27,no.4,pp ,1991. [25] R.Luosto,P.Ketonen,P.T.Harjola,andA.Jarvinen, Extrathoracic approach for reconstruction of subclavian and vertebral arteries, Scandinavian Journal of Thoracic and Cardiovascular Surgery,vol.14,no.2,pp ,1980. [26] J. A. Liveson, M. J. Bronson, and M. A. Pollack, Suprascapular nerve lesions at the spinoglenoid notch: report of three cases and review of the literature, Journal of Neurology Neurosurgery and Psychiatry,vol.54,no.3,pp ,1991. [27] P. Burge, G. Rushworth, and N. Watson, Patterns of injury to the terminal branches of the brachial plexus. The place for early exploration, JournalofBoneandJointSurgeryB,vol.67,no.4, pp , [28] A. Nagano, N. Ochiai, H. Sugioka, T. Hara, and N. Tsuyama, Usefulness of myelography in brachial plexus injuries, Journal of Hand Surgery,vol.14,no.1,pp.59 64,1989. [29] G.A.Carvalho,G.Nikkhah,C.Matthies,G.Penkert,andM. Samii, Diagnosis of root avulsions in traumatic brachial plexus injuries: value of computerized tomography myelography and magnetic resonance imaging, JournalofNeurosurgery,vol.86, no. 1, pp , [30] A. T. Walker, J. C. Chaloupka, A. C. J. De Lotbiniere, S. W. Wolfe, R.Goldman,andE.L.Kier, Detectionofnerverootletavulsion on CT myelography in patients with birth palsy and brachial plexus injury after trauma, American Journal of Roentgenology, vol. 167, no. 5, pp , [31] E. Volle, J. Assheuer, J. P. Hedde, and R. Gustorf-Aeckerle, Radicular avulsion resulting from spinal injury: assessment of diagnostic modalities, Neuroradiology, vol. 34, no. 3, pp , [32] W. F. Brown and J. Veitch, AAEM minimonograph 42: intraoperative monitoring of peripheral and cranial nerves, Muscle and Nerve,vol.17,no.4,pp ,1994. [33] J. R. Daube and C. M. Harprer, Surgical monitoring of cranial and peripgheral nerves, in Neuromonitoring in Surgery, J.E. Desmadt, Ed., Elsevier, Amsterdam, The Netherlands, [34] R.J.SpinnerandD.G.Kline, Surgeryforperipheralnerveand brachial plexus injuries or other nerve lesion, Muscle Nerve,vol. 23, pp , 2000.
10 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Journal of Diabetes Research International Journal of Journal of Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Journal of Obesity Journal of Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Journal of Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
BRACHIAL PLEXUS INJURY INVESTIGATION, LOCALIZATION AND TREATMENT. Presented By : Dr.Pankaj Jain
 BRACHIAL PLEXUS INJURY INVESTIGATION, LOCALIZATION AND TREATMENT Presented By : Dr.Pankaj Jain EMBRYOLOGY l Brachial plexus (BP) is developed at 5 weeks of gestation l Afferent fibers develop from neuroblast
BRACHIAL PLEXUS INJURY INVESTIGATION, LOCALIZATION AND TREATMENT Presented By : Dr.Pankaj Jain EMBRYOLOGY l Brachial plexus (BP) is developed at 5 weeks of gestation l Afferent fibers develop from neuroblast
If head is rapidly forced away from shoulder the injury is generally at C5,C6. If arm is rapidly abducted the lesion is generally at C8-T1.
 BRACHIAL PLEXUS Etiology Generally caused by MVA in adults. Generally males aged 15 to 25 years old. Naracas: Rule of seven seventies. 70% occur secondary to MVA; 70% involve motorcycles or bicycles. 70%
BRACHIAL PLEXUS Etiology Generally caused by MVA in adults. Generally males aged 15 to 25 years old. Naracas: Rule of seven seventies. 70% occur secondary to MVA; 70% involve motorcycles or bicycles. 70%
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
*Our main subject is the brachial plexus but it's important to understand the spinal cord first in order to understand the brachial plexus.
 *Our main subject is the brachial plexus but it's important to understand the spinal cord first in order to understand the brachial plexus. *Vertebral column is formed by the union of 33 sequential vertebrae
*Our main subject is the brachial plexus but it's important to understand the spinal cord first in order to understand the brachial plexus. *Vertebral column is formed by the union of 33 sequential vertebrae
Neurophysiological Diagnosis of Birth Brachial Plexus Palsy. Dr Grace Ng Department of Paed PMH
 Neurophysiological Diagnosis of Birth Brachial Plexus Palsy Dr Grace Ng Department of Paed PMH Brachial Plexus Anatomy Brachial Plexus Cords Medial cord: motor and sensory conduction for median and ulnar
Neurophysiological Diagnosis of Birth Brachial Plexus Palsy Dr Grace Ng Department of Paed PMH Brachial Plexus Anatomy Brachial Plexus Cords Medial cord: motor and sensory conduction for median and ulnar
Adult Brachial Plexus Injuries: Introduction and the Role of Surgery
 Adult Brachial Plexus Injuries: Introduction and the Role of Surgery Tim Hems Scottish National Brachial Plexus Injury Service Department of Orthopaedic Surgery, Queen Elizabeth University Hospital, GLASGOW.
Adult Brachial Plexus Injuries: Introduction and the Role of Surgery Tim Hems Scottish National Brachial Plexus Injury Service Department of Orthopaedic Surgery, Queen Elizabeth University Hospital, GLASGOW.
BRACHIAL PLEXUS. DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae
 THE BRACHIAL PLEXUS DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae SCHEMA OF THE BRACHIAL PLEXUS THE BRACHIAL PLEXUS PHRENIC NERVE supraclavicular
THE BRACHIAL PLEXUS DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae SCHEMA OF THE BRACHIAL PLEXUS THE BRACHIAL PLEXUS PHRENIC NERVE supraclavicular
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Brachial plexuses and axillary lymph nodes
 Brachial plexuses and axillary lymph nodes Introduction about nervous system nervous system central nervous system periphral nervous system brain spinal cord 31 pairs of spinal nerves 12 paris of cranial
Brachial plexuses and axillary lymph nodes Introduction about nervous system nervous system central nervous system periphral nervous system brain spinal cord 31 pairs of spinal nerves 12 paris of cranial
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck.
 Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
Upper Limb Muscles Muscles of Axilla & Arm
 Done By : Saleh Salahat Upper Limb Muscles Muscles of Axilla & Arm 1) Muscles around the axilla A- Muscles connecting the upper to thoracic wall (4) 1- pectoralis major Origin:- from the medial half of
Done By : Saleh Salahat Upper Limb Muscles Muscles of Axilla & Arm 1) Muscles around the axilla A- Muscles connecting the upper to thoracic wall (4) 1- pectoralis major Origin:- from the medial half of
Axilla and Brachial Region
 L 4 A B O R A T O R Y Axilla and Brachial Region BRACHIAL PLEXUS 5 Roots/Rami (ventral rami C5 T1) 3 Trunks Superior (C5, C6) Middle (C7) Inferior (C8, T1) 3 Cords Lateral Cord (Anterior Superior and Anterior
L 4 A B O R A T O R Y Axilla and Brachial Region BRACHIAL PLEXUS 5 Roots/Rami (ventral rami C5 T1) 3 Trunks Superior (C5, C6) Middle (C7) Inferior (C8, T1) 3 Cords Lateral Cord (Anterior Superior and Anterior
Human Anatomy Biology 351
 1 Human Anatomy Biology 351 Upper Limb Exam Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
1 Human Anatomy Biology 351 Upper Limb Exam Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
MUSCLES. Anconeus Muscle
 LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
Upper limb Arm & Cubital region 黃敏銓
 Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Obstetric Brachial Plexus Injuries. Surgery department grand rounds Bassam MJ Addas, FRCSC Neurological Surgery, KAUH
 Obstetric Brachial Plexus Injuries. Surgery department grand rounds Bassam MJ Addas, FRCSC Neurological Surgery, KAUH Definition Obstetric versus birth palsy Obstetric versus congenital palsy Not all birth
Obstetric Brachial Plexus Injuries. Surgery department grand rounds Bassam MJ Addas, FRCSC Neurological Surgery, KAUH Definition Obstetric versus birth palsy Obstetric versus congenital palsy Not all birth
Chapter 14. The Nervous System. The Spinal Cord and Spinal Nerves. Lecture Presentation by Steven Bassett Southeast Community College
 Chapter 14 The Nervous System The Spinal Cord and Spinal Nerves Lecture Presentation by Steven Bassett Southeast Community College Introduction The Central Nervous System (CNS) consists of: The spinal
Chapter 14 The Nervous System The Spinal Cord and Spinal Nerves Lecture Presentation by Steven Bassett Southeast Community College Introduction The Central Nervous System (CNS) consists of: The spinal
Al-Balqa Applied University
 Al-Balqa Applied University Faculty Of Medicine *You can use this checklist as a guide to you for the lab. the items on this checklist represent the main features of the models that you have to know for
Al-Balqa Applied University Faculty Of Medicine *You can use this checklist as a guide to you for the lab. the items on this checklist represent the main features of the models that you have to know for
Nerve Injury. 1) Upper Lesions of the Brachial Plexus called Erb- Duchene Palsy or syndrome.
 Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
Peripheral Nervous Sytem: Upper Body
 Peripheral Nervous Sytem: Upper Body MSTN121 - Neurophysiology Session 10 Department of Myotherapy Cervical Plexus Accessory nerve (CN11 + C1-5) Motor: trapezius and sternocleidomastoid Greater auricular
Peripheral Nervous Sytem: Upper Body MSTN121 - Neurophysiology Session 10 Department of Myotherapy Cervical Plexus Accessory nerve (CN11 + C1-5) Motor: trapezius and sternocleidomastoid Greater auricular
imaging sequences obtained in brachial plexopathy with/without TOS MR Imaging Sequences Associated Anatomic Structures or Pathologic Conditions
 Brachial plexus imaging sequences obtained in brachial plexopathy with/without TOS MR Imaging Sequences Associated Anatomic Structures or Pathologic Conditions Sagittal TSE T2WI through cervical spine
Brachial plexus imaging sequences obtained in brachial plexopathy with/without TOS MR Imaging Sequences Associated Anatomic Structures or Pathologic Conditions Sagittal TSE T2WI through cervical spine
3 Mohammad Al-Mohtasib Areej Mosleh
 3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
Muscles of the Upper Limb
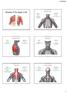 Muscles of the Upper Limb anterior surface of ribs 3 5 coracoid process Pectoralis minor pectoral nerves protracts / depresses scapula Serratus anterior Subclavius ribs 1-8 long thoracic nerve rib 1 ----------------
Muscles of the Upper Limb anterior surface of ribs 3 5 coracoid process Pectoralis minor pectoral nerves protracts / depresses scapula Serratus anterior Subclavius ribs 1-8 long thoracic nerve rib 1 ----------------
Brachial Plexopathy in a Division I Football Player
 www.fisiokinesiterapia.biz Brachial Plexopathy in a Division I Football Player Brachial Plexus Injuries in Sport Typically a transient neurapraxia - 70% of injured players said they did not always report
www.fisiokinesiterapia.biz Brachial Plexopathy in a Division I Football Player Brachial Plexus Injuries in Sport Typically a transient neurapraxia - 70% of injured players said they did not always report
Scapular and Deltoid Regions
 M1 Gross and Developmental Anatomy Scapular and Deltoid Regions Dr. Peters 1 Outline I. Skeleton of the Shoulder and Attachment of the Upper Extremity to Trunk II. Positions and Movements of the Scapula
M1 Gross and Developmental Anatomy Scapular and Deltoid Regions Dr. Peters 1 Outline I. Skeleton of the Shoulder and Attachment of the Upper Extremity to Trunk II. Positions and Movements of the Scapula
Faculty of Dental Medicine and Surgery. Sem 4 Peripheral nervous system and nerve plexus Dr. Abbas Garib Alla
 Faculty of Dental Medicine and Surgery Sem 4 Peripheral nervous system and nerve plexus Dr. Abbas Garib Alla PNS Terminology Ganglia neuron cell bodies Peripheral nerves neuronal axons PNS neuroglia Satellite
Faculty of Dental Medicine and Surgery Sem 4 Peripheral nervous system and nerve plexus Dr. Abbas Garib Alla PNS Terminology Ganglia neuron cell bodies Peripheral nerves neuronal axons PNS neuroglia Satellite
Synapse Homework. Back page last question not counted. 4 pts total, each question worth 0.18pts. 26/34 students answered correctly!
 Synapse Homework Back page last question not counted 26/34 students answered correctly! 4 pts total, each question worth 0.18pts Business TASS hours extended! MWF 1-2pm, Willamette 204 T and Th 9:30-10:30am,
Synapse Homework Back page last question not counted 26/34 students answered correctly! 4 pts total, each question worth 0.18pts Business TASS hours extended! MWF 1-2pm, Willamette 204 T and Th 9:30-10:30am,
Management of Brachial Plexus & Peripheral Nerves Blast Injuries. First Global Conflict Medicine Congress
 Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Assessment of the Brachial Plexus EMG Course CNSF Halifax Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University
 Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
Brachial plexus lesions
 Brachial plexus lesions SGH Course 11.01.18 Esther Vögelin and Team Handchirurgie und Chirurgie der peripheren Nerven, Universitätsspital Bern Surgical anatomy of the brachial plexus 5-3-6-3-5 5 Roots:
Brachial plexus lesions SGH Course 11.01.18 Esther Vögelin and Team Handchirurgie und Chirurgie der peripheren Nerven, Universitätsspital Bern Surgical anatomy of the brachial plexus 5-3-6-3-5 5 Roots:
G24: Shoulder and Axilla
 G24: Shoulder and Axilla Syllabus - Pg. 2 ANAT 6010- Medical Gross Anatomy David A. Morton, Ph.D. Objectives Upper limb Systemically: Bones (joints) Muscles Nerves Vessels (arteries/veins) Fascial compartments
G24: Shoulder and Axilla Syllabus - Pg. 2 ANAT 6010- Medical Gross Anatomy David A. Morton, Ph.D. Objectives Upper limb Systemically: Bones (joints) Muscles Nerves Vessels (arteries/veins) Fascial compartments
The grouping of nerves connecting the C4 to Th1 junctions of the spinal cord to the left and right arms.
 THE BRACHIAL The grouping of nerves connecting the C4 to Th1 junctions of the spinal cord to the left and right arms. CONTENTS Brachial plexus Brachial plexus anatomy MRI of brachial plexus Dermatome(C8-T1)
THE BRACHIAL The grouping of nerves connecting the C4 to Th1 junctions of the spinal cord to the left and right arms. CONTENTS Brachial plexus Brachial plexus anatomy MRI of brachial plexus Dermatome(C8-T1)
Repair of Severe Traction Lesions of the Brachial Plexus
 Repair of Severe Traction Lesions of the Brachial Plexus LAURENT SEDEL, M.D. Since 1972, the author has performed 259 brachial plexus repairs and various associated secondary procedures. The best results
Repair of Severe Traction Lesions of the Brachial Plexus LAURENT SEDEL, M.D. Since 1972, the author has performed 259 brachial plexus repairs and various associated secondary procedures. The best results
Upper limb Pectoral region & Axilla
 Upper limb Pectoral region & Axilla 黃敏銓 mchuang@ntu.edu.tw 1 Pectoral region Intercostal nerve Anterior branch of lateral cutaneous branch Lateral cutaneous branch Anterior cutaneous branch Anterior cutaneous
Upper limb Pectoral region & Axilla 黃敏銓 mchuang@ntu.edu.tw 1 Pectoral region Intercostal nerve Anterior branch of lateral cutaneous branch Lateral cutaneous branch Anterior cutaneous branch Anterior cutaneous
The use of thoracodorsal nerve transfer in restoration of irreparable C5 and C6 spinal nerve lesions
 British Journal of Plastic Surgery (2005) 58, 541 546 The use of thoracodorsal nerve transfer in restoration of irreparable C5 and C6 spinal nerve lesions M.M. Samardzic*, D.M. Grujicic, L.G. Rasulic,
British Journal of Plastic Surgery (2005) 58, 541 546 The use of thoracodorsal nerve transfer in restoration of irreparable C5 and C6 spinal nerve lesions M.M. Samardzic*, D.M. Grujicic, L.G. Rasulic,
Anatomy of the Shoulder Girdle. Prof Oluwadiya Kehinde FMCS (Orthop)
 Anatomy of the Shoulder Girdle Prof Oluwadiya Kehinde FMCS (Orthop) www.oluwadiya.com Bony Anatomy Shoulder Complex: Sternum(manubrium) Clavicle Scapula Proximal humerus Manubrium Sterni Upper part of
Anatomy of the Shoulder Girdle Prof Oluwadiya Kehinde FMCS (Orthop) www.oluwadiya.com Bony Anatomy Shoulder Complex: Sternum(manubrium) Clavicle Scapula Proximal humerus Manubrium Sterni Upper part of
Key Relationships in the Upper Limb
 Key Relationships in the Upper Limb This list contains some of the key relationships that will help you identify structures in the lab. They are organized by dissection assignment as defined in the syllabus.
Key Relationships in the Upper Limb This list contains some of the key relationships that will help you identify structures in the lab. They are organized by dissection assignment as defined in the syllabus.
Nerve Conduction Studies and EMG
 Nerve Conduction Studies and EMG Limitations of other methods of investigations of the neuromuscular system - Dr Rob Henderson, Neurologist Assessment of Weakness Thanks Peter Silburn PERIPHERAL NEUROPATHY
Nerve Conduction Studies and EMG Limitations of other methods of investigations of the neuromuscular system - Dr Rob Henderson, Neurologist Assessment of Weakness Thanks Peter Silburn PERIPHERAL NEUROPATHY
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
The arm: *For images refer back to the slides
 The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
PNS and ANS Flashcards
 1. Name several SOMATIC SENSES Light touch (being touched by a feather), heat, cold, vibration, pressure, pain are SOMATIC SENSES. 2. What are proprioceptors; and how is proprioception tested? PROPRIOCEPTORS
1. Name several SOMATIC SENSES Light touch (being touched by a feather), heat, cold, vibration, pressure, pain are SOMATIC SENSES. 2. What are proprioceptors; and how is proprioception tested? PROPRIOCEPTORS
Muscle Action Origin Insertion Nerve Innervation Chapter Page. Deltoid. Trapezius. Latissimus Dorsi
 Muscle Action Origin Insertion Nerve Innervation Chapter Page All Fibers Abduct the shoulder (glenohumeral joint) Deltoid Anterior Fibers Flex the shoulder (G/H joint) Horizontally adduct the shoulder
Muscle Action Origin Insertion Nerve Innervation Chapter Page All Fibers Abduct the shoulder (glenohumeral joint) Deltoid Anterior Fibers Flex the shoulder (G/H joint) Horizontally adduct the shoulder
BRACHIAL PLEXUS 11/12/2014 كيف تتكون الضفيرة FORMATION ENLARGEMENT (INTUMESCENCE) OF THE SPINAL CORD. Grey matter. Cervical intumescence - C 6 - T 2
 BRACHIAL PLEXUS Prof. Fawzy Elnady ENLARGEMENT (INTUMESCENCE) OF THE SPINAL CORD Grey matter Cervical intumescence - C 6 - T 2 Lumbar intumescence - L 4 S 2 كيف تتكون الضفيرة FORMATION The ventral rami
BRACHIAL PLEXUS Prof. Fawzy Elnady ENLARGEMENT (INTUMESCENCE) OF THE SPINAL CORD Grey matter Cervical intumescence - C 6 - T 2 Lumbar intumescence - L 4 S 2 كيف تتكون الضفيرة FORMATION The ventral rami
SHOULDER PAIN. A Real Pain in the Neck. Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017
 SHOULDER PAIN A Real Pain in the Neck Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017 THE SHOULDER JOINT (S) 1. glenohumeral 2. suprahumeral 3. acromioclavicular 4. scapulocostal
SHOULDER PAIN A Real Pain in the Neck Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017 THE SHOULDER JOINT (S) 1. glenohumeral 2. suprahumeral 3. acromioclavicular 4. scapulocostal
Anatomy of the Musculoskeletal System
 Anatomy of the Musculoskeletal System Kyle E. Rarey, Ph.D. Department of Anatomy & Cell Biology and Otolaryngology University of Florida College of Medicine Outline of Presentation Vertebral Column Upper
Anatomy of the Musculoskeletal System Kyle E. Rarey, Ph.D. Department of Anatomy & Cell Biology and Otolaryngology University of Florida College of Medicine Outline of Presentation Vertebral Column Upper
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone
 *the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
Human Anatomy Biology 351
 nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
The Clavicle Right clavicle Deltoid tubercle: Conoid tubercle, conoid ligamen Impression for the
 The Clavicle Muscle Attachment Sites in the Upper Limb Pectoralis major Right clavicle Smooth superior surface of the shaft, under the platysma muscle tubercle: attachment of the deltoid Acromial facet
The Clavicle Muscle Attachment Sites in the Upper Limb Pectoralis major Right clavicle Smooth superior surface of the shaft, under the platysma muscle tubercle: attachment of the deltoid Acromial facet
Clinical examination of the shoulder girdle
 Clinical of the shoulder girdle CHAPTER CONTENTS Symptoms referred to the shoulder girdle........ e72 Symptoms referred from the shoulder girdle...... e72 History........................... e72 Inspection.........................
Clinical of the shoulder girdle CHAPTER CONTENTS Symptoms referred to the shoulder girdle........ e72 Symptoms referred from the shoulder girdle...... e72 History........................... e72 Inspection.........................
FUNCTIONAL ANATOMY OF SHOULDER JOINT
 FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
Spinal Cord and Spinal Nerves. Spinal Cord. Chapter 12
 Chapter 12 Spinal Cord and Spinal Nerves 1 Spinal Cord Extends from foramen magnum to second lumbar vertebra Segmented: Cervical, Thoracic, Lumbar & Sacral Gives rise to 31 pairs of spinal nerves Not uniform
Chapter 12 Spinal Cord and Spinal Nerves 1 Spinal Cord Extends from foramen magnum to second lumbar vertebra Segmented: Cervical, Thoracic, Lumbar & Sacral Gives rise to 31 pairs of spinal nerves Not uniform
Chapter 13: The Spinal Cord and Spinal Nerves
 Chapter 13: The Spinal Cord and Spinal Nerves Spinal Cord Anatomy Protective structures: Vertebral column and the meninges protect the spinal cord and provide physical stability. a. Dura mater, b. Arachnoid,
Chapter 13: The Spinal Cord and Spinal Nerves Spinal Cord Anatomy Protective structures: Vertebral column and the meninges protect the spinal cord and provide physical stability. a. Dura mater, b. Arachnoid,
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns
 213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns CLAVICLE Examine an isolated clavicle and compare it with a clavicle on an articulated skeleton. Viewed from above,
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 1: Proximal bones, plexuses and patterns CLAVICLE Examine an isolated clavicle and compare it with a clavicle on an articulated skeleton. Viewed from above,
12 Anatomy and Physiology of Peripheral Nerves
 12 Anatomy and Physiology of Peripheral Nerves Introduction Anatomy Classification of Peripheral Nerves Sensory Nerves Motor Nerves Pathologies of Nerves Focal Injuries Regeneration of Injured Nerves Signs
12 Anatomy and Physiology of Peripheral Nerves Introduction Anatomy Classification of Peripheral Nerves Sensory Nerves Motor Nerves Pathologies of Nerves Focal Injuries Regeneration of Injured Nerves Signs
Original Article Selective neurotization of the radial nerve in the axilla using intercostal nerve to treat complete brachial plexus palsy
 Int J Clin Exp Med 2016;9(11):22880-22885 www.ijcem.com /ISSN:1940-5901/IJCEM0032455 Original Article Selective neurotization of the radial nerve in the axilla using intercostal nerve to treat complete
Int J Clin Exp Med 2016;9(11):22880-22885 www.ijcem.com /ISSN:1940-5901/IJCEM0032455 Original Article Selective neurotization of the radial nerve in the axilla using intercostal nerve to treat complete
Traumatic Brachial Plexus Preganglionic Injury: What to look for at MR Neurography?
 Traumatic Brachial Plexus Preganglionic Injury: What to look for at MR Neurography? Poster No.: C-1225 Congress: ECR 2017 Type: Authors: Keywords: DOI: Educational Exhibit D. Binaghi 1, M. Socolovsky 2,
Traumatic Brachial Plexus Preganglionic Injury: What to look for at MR Neurography? Poster No.: C-1225 Congress: ECR 2017 Type: Authors: Keywords: DOI: Educational Exhibit D. Binaghi 1, M. Socolovsky 2,
Spinal nerves. Aygul Shafigullina. Department of Morphology and General Pathology
 Spinal nerves Aygul Shafigullina Department of Morphology and General Pathology Spinal nerve a mixed nerve, formed in the vicinity of an intervertebral foramen, where fuse a dorsal root and a ventral root,
Spinal nerves Aygul Shafigullina Department of Morphology and General Pathology Spinal nerve a mixed nerve, formed in the vicinity of an intervertebral foramen, where fuse a dorsal root and a ventral root,
Netter's Anatomy Flash Cards Section 6 List 4 th Edition
 Netter's Anatomy Flash Cards Section 6 List 4 th Edition https://www.memrise.com/course/1577581/ Section 6 Upper Limb (66 cards) Plate 6-1 Humerus and Scapula: Anterior View 1.1 Acromion 1.2 Greater tubercle
Netter's Anatomy Flash Cards Section 6 List 4 th Edition https://www.memrise.com/course/1577581/ Section 6 Upper Limb (66 cards) Plate 6-1 Humerus and Scapula: Anterior View 1.1 Acromion 1.2 Greater tubercle
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5. September 30, 2011
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
Case 3. Your Diagnosis?
 Case 3 45 year-old presenting with a history of injury to the right shoulder whilst working in the freezing work. He was loading a sheep over an incline with his arm around the sheep. He felt pain in the
Case 3 45 year-old presenting with a history of injury to the right shoulder whilst working in the freezing work. He was loading a sheep over an incline with his arm around the sheep. He felt pain in the
region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla.
 1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
The Muscular System. Chapter 10 Part C. PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College
 Chapter 10 Part C The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.9: Muscles Crossing the Shoulder
Chapter 10 Part C The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.9: Muscles Crossing the Shoulder
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T
 THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
The Spinal Cord, Spinal Nerves, and Spinal Reflexes
 13 The Spinal Cord, Spinal Nerves, and Spinal Reflexes PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Spinal Cord, Spinal Nerves, and Spinal
13 The Spinal Cord, Spinal Nerves, and Spinal Reflexes PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Spinal Cord, Spinal Nerves, and Spinal
7/31/2012 THE SHOULDER JOINT CLARIFICATION OF TERMS OSTEOLOGY OF THE GH JOINT(BONES)
 THE SHOULDER JOINT T H E G L E N O H U M E R AL ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumerual joint) = scapula and Lippert, p115 OSTEOLOGY
THE SHOULDER JOINT T H E G L E N O H U M E R AL ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumerual joint) = scapula and Lippert, p115 OSTEOLOGY
MUSCLES OF SHOULDER REGION
 Dr Jamila EL Medany OBJECTIVES At the end of the lecture, students should: List the name of muscles of the shoulder region. Describe the anatomy of muscles of shoulder region regarding: attachments of
Dr Jamila EL Medany OBJECTIVES At the end of the lecture, students should: List the name of muscles of the shoulder region. Describe the anatomy of muscles of shoulder region regarding: attachments of
Human Anatomy. Spinal Cord and Spinal Nerves
 Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Gross Anatomy Questions That Should be Answerable After October 27, 2017
 Gross Anatomy Questions That Should be Answerable After October 27, 2017 1. The inferior angle of the scapula of a woman who was recently in an automobile accident seems to protrude making a ridge beneath
Gross Anatomy Questions That Should be Answerable After October 27, 2017 1. The inferior angle of the scapula of a woman who was recently in an automobile accident seems to protrude making a ridge beneath
Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for
 Chapter 13 Outline Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for what you need to know from Exhibits 13.1 13.4 I. INTRODUCTION A. The spinal cord and spinal nerves
Chapter 13 Outline Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for what you need to know from Exhibits 13.1 13.4 I. INTRODUCTION A. The spinal cord and spinal nerves
Practical 2 Worksheet
 Practical 2 Worksheet Upper Extremity BONES 1. Which end of the clavicle is on the lateral side (acromial or sternal)? 2. Describe the difference in the appearance of the acromial and sternal ends of the
Practical 2 Worksheet Upper Extremity BONES 1. Which end of the clavicle is on the lateral side (acromial or sternal)? 2. Describe the difference in the appearance of the acromial and sternal ends of the
Slide 1. Slide 2. Slide 3. The Role Of Plastic Surgery In Reducing A Patient s Disability Score A Reconstructive Approach. Peripheral Nerve Surgery
 Slide 1 The Role Of Plastic Surgery In Reducing A Patient s Disability Score A Reconstructive Approach Andrew I. Elkwood MD FACS Director of the Center for Treatment of Paralysis and Reconstructive Nerve
Slide 1 The Role Of Plastic Surgery In Reducing A Patient s Disability Score A Reconstructive Approach Andrew I. Elkwood MD FACS Director of the Center for Treatment of Paralysis and Reconstructive Nerve
This figure (of humerus) is from Dr. Maher's newest slides. -Its added here just for consideration-
 This figure (of humerus) is from Dr. Maher's newest slides. -Its added here just for consideration- Slides of Anatomy Please note : These slides are Dr. Maher Hadidi s slides of spring 2016 and were edited
This figure (of humerus) is from Dr. Maher's newest slides. -Its added here just for consideration- Slides of Anatomy Please note : These slides are Dr. Maher Hadidi s slides of spring 2016 and were edited
CHAPTER 13 LECTURE OUTLINE
 CHAPTER 13 LECTURE OUTLINE I. INTRODUCTION A. The spinal cord and spinal nerves mediate reactions to environmental changes. B. The spinal cord has several functions. 1. It processes reflexes. 2. It is
CHAPTER 13 LECTURE OUTLINE I. INTRODUCTION A. The spinal cord and spinal nerves mediate reactions to environmental changes. B. The spinal cord has several functions. 1. It processes reflexes. 2. It is
BPBP. Brachial Plexus Birth Palsy BPBP BPBP 11/2/2015. Traction or compression injury during birth. ~ 1 : 1000 live births R > L (LAO presentation)
 Brachial Plexus Birth Palsy Donald S. Bae, MD Boston Children s Hospital BPBP Traction or compression injury during birth ~ 1 : 1000 live births R > L (LAO presentation) Risk factors: macrosomia, difficult
Brachial Plexus Birth Palsy Donald S. Bae, MD Boston Children s Hospital BPBP Traction or compression injury during birth ~ 1 : 1000 live births R > L (LAO presentation) Risk factors: macrosomia, difficult
Surgical repair of brachial plexus injury: a multinational survey of experienced peripheral nerve surgeons
 Neurosurg Focus 16 (5):Preview Article 1, 2004, Click here to return to Table of Contents Surgical repair of brachial plexus injury: a multinational survey of experienced peripheral nerve surgeons ALLAN
Neurosurg Focus 16 (5):Preview Article 1, 2004, Click here to return to Table of Contents Surgical repair of brachial plexus injury: a multinational survey of experienced peripheral nerve surgeons ALLAN
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi. E. mail:
 Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
Anterior deltopectoral approach for axillary nerve neurotisation
 Journal of Orthopaedic Surgery 2012;20(1):66-70 Anterior deltopectoral approach for axillary nerve neurotisation J Terrence Jose Jerome Department of Orthopedics, Hand and Reconstructive Microsurgery,
Journal of Orthopaedic Surgery 2012;20(1):66-70 Anterior deltopectoral approach for axillary nerve neurotisation J Terrence Jose Jerome Department of Orthopedics, Hand and Reconstructive Microsurgery,
Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes
 Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes 1 This lab involves the second section of the exercise Spinal Cord, Spinal Nerves, and the Autonomic Nervous System,
Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes 1 This lab involves the second section of the exercise Spinal Cord, Spinal Nerves, and the Autonomic Nervous System,
Variations of median nerve and musculocutaneous nerve: Cadeveric study
 Original article: Variations of median nerve and musculocutaneous nerve: Cadeveric study 1Dr.VaishaliBondge*, 2 Dr. Ashok Khade, 3 Dr. P.H.Shingare 1Assistant Professor, Grant Medical College, Mumbai,
Original article: Variations of median nerve and musculocutaneous nerve: Cadeveric study 1Dr.VaishaliBondge*, 2 Dr. Ashok Khade, 3 Dr. P.H.Shingare 1Assistant Professor, Grant Medical College, Mumbai,
ANATOMY OF SPINAL CORD. Khaleel Alyahya, PhD, MEd King Saud University School of
 ANATOMY OF SPINAL CORD Khaleel Alyahya, PhD, MEd King Saud University School of Medicine @khaleelya OBJECTIVES At the end of the lecture, students should be able to: Describe the external anatomy of the
ANATOMY OF SPINAL CORD Khaleel Alyahya, PhD, MEd King Saud University School of Medicine @khaleelya OBJECTIVES At the end of the lecture, students should be able to: Describe the external anatomy of the
WEEKEND THREE HOMEWORK
 WEEKEND THREE HOMEWORK READING ASSIGNMENTS Salvo Massage Therapy Principles and Practice 4 th Edition Muscolino The Muscular System Manual Muscolino The Muscle and Bone Palpation Manual Ch. 19 Skeletal
WEEKEND THREE HOMEWORK READING ASSIGNMENTS Salvo Massage Therapy Principles and Practice 4 th Edition Muscolino The Muscular System Manual Muscolino The Muscle and Bone Palpation Manual Ch. 19 Skeletal
Nerve Transfers for Adult Traumatic Brachial Plexus Palsy (Brachial Plexus Nerve Transfer)
 DOI 10.1007/s11420-006-9027-y ORIGINAL ARTICLE Nerve Transfers for Adult Traumatic Brachial Plexus Palsy (Brachial Plexus Nerve Transfer) Rachel S. Rohde, MD & Scott W. Wolfe, MD # Hospital for Special
DOI 10.1007/s11420-006-9027-y ORIGINAL ARTICLE Nerve Transfers for Adult Traumatic Brachial Plexus Palsy (Brachial Plexus Nerve Transfer) Rachel S. Rohde, MD & Scott W. Wolfe, MD # Hospital for Special
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Classification of the nervous system. Prof. Dr. Nikolai Lazarov 2
 1 1. Formation and general organization 2. Spinal ganglia 3. Zonal and segmental innervation 4. Dorsal rami of the spinal nerves 5. Ventral rami of the spinal nerves 6. Cervical plexus Classification of
1 1. Formation and general organization 2. Spinal ganglia 3. Zonal and segmental innervation 4. Dorsal rami of the spinal nerves 5. Ventral rami of the spinal nerves 6. Cervical plexus Classification of
Fig Cervical spinal nerves. Cervical enlargement C7. Dural sheath. Subarachnoid space. Thoracic. Spinal cord Vertebra (cut) spinal nerves
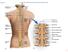 Fig. 13.1 C1 Cervical enlargement C7 Cervical spinal nerves Dural sheath Subarachnoid space Thoracic spinal nerves Spinal cord Vertebra (cut) Lumbar enlargement Medullary cone T12 Spinal nerve Spinal nerve
Fig. 13.1 C1 Cervical enlargement C7 Cervical spinal nerves Dural sheath Subarachnoid space Thoracic spinal nerves Spinal cord Vertebra (cut) Lumbar enlargement Medullary cone T12 Spinal nerve Spinal nerve
Magnetic Resonance Imaging of Adult Traumatic Brachial Plexus Injuries
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 8 Ver. XI (Aug. 2017), PP 57-62 www.iosrjournals.org Magnetic Resonance Imaging of Adult Traumatic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 8 Ver. XI (Aug. 2017), PP 57-62 www.iosrjournals.org Magnetic Resonance Imaging of Adult Traumatic
Anatomy and Physiology II. Review Shoulder Girdle New Material Upper Extremities - Bones
 Anatomy and Physiology II Review Shoulder Girdle New Material Upper Extremities - Bones Anatomy and Physiology II Shoulder Girdle Review Questions From Last Lecture Can you identify the following muscles?
Anatomy and Physiology II Review Shoulder Girdle New Material Upper Extremities - Bones Anatomy and Physiology II Shoulder Girdle Review Questions From Last Lecture Can you identify the following muscles?
Muscles in the Shoulder, Chest, Arm, Stomach, and Back
 Muscles in the Shoulder, Chest, Arm, Stomach, and Back Shoulder Muscles Deltoid Supraspinatus Infraspinatus Teres Major Teres Minor Subscapularis Deltoid (Delts) Function: Raises the upper arm Origin:
Muscles in the Shoulder, Chest, Arm, Stomach, and Back Shoulder Muscles Deltoid Supraspinatus Infraspinatus Teres Major Teres Minor Subscapularis Deltoid (Delts) Function: Raises the upper arm Origin:
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Brachial Plexus Injuries
 Brachial Plexus Injuries 1 / 6 2 / 6 3 / 6 Brachial Plexus Injuries A brachial plexus injury (BPI), also known as brachial plexus lesion, is an injury to the brachial plexus, the network of nerves that
Brachial Plexus Injuries 1 / 6 2 / 6 3 / 6 Brachial Plexus Injuries A brachial plexus injury (BPI), also known as brachial plexus lesion, is an injury to the brachial plexus, the network of nerves that
BILATERAL RARE NEURO VASCULAR VARIATIONS OF UPPER LIMB A CASE REPORT
 BILATERAL RARE NEURO VASCULAR VARIATIONS OF UPPER LIMB A CASE REPORT *N. B. S. Parimala Department of Anatomy, Dr. Pinnamaneni Siddhartha Institute of Medical Sciences & Research Foundation, Chinnaoutpalli,
BILATERAL RARE NEURO VASCULAR VARIATIONS OF UPPER LIMB A CASE REPORT *N. B. S. Parimala Department of Anatomy, Dr. Pinnamaneni Siddhartha Institute of Medical Sciences & Research Foundation, Chinnaoutpalli,
The Arm and Cubital Fossa
 The Arm and Cubital Fossa Dr. Andrew Gallagher School of Anatomical Sciences University of the Witwatersrand Introduction The ARM (BRACHIUM) is the most proximal segment of the upper limb musculoskeletal
The Arm and Cubital Fossa Dr. Andrew Gallagher School of Anatomical Sciences University of the Witwatersrand Introduction The ARM (BRACHIUM) is the most proximal segment of the upper limb musculoskeletal
ANATOMY OF THE BRACHIAL PLEXUS
 Chapter 1 ANATOMY OF THE BRACHIAL PLEXUS Hideo Kawai The brachial plexus is formed from five spinal nerves: C5, C6, C7, C8 and T1. Each spinal nerve (plexus root) is the result of an intramedullary mixture
Chapter 1 ANATOMY OF THE BRACHIAL PLEXUS Hideo Kawai The brachial plexus is formed from five spinal nerves: C5, C6, C7, C8 and T1. Each spinal nerve (plexus root) is the result of an intramedullary mixture
Abduction of arm until your hand rich your head. Flexion of forearm at elbow joint. Extension of arm at elbow joint. Flexion of fingers 10.
 Num. answer 1. Medialy With the manubrium ( sternum ), and laterally with the acromion of the scapula 2. 1. Trapezius 2. Levator scapulae 3. Rhomboids 3. 1. Pectoralis major 2. Pectoralis minor 3. Latissiumus
Num. answer 1. Medialy With the manubrium ( sternum ), and laterally with the acromion of the scapula 2. 1. Trapezius 2. Levator scapulae 3. Rhomboids 3. 1. Pectoralis major 2. Pectoralis minor 3. Latissiumus
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Early treatment of birth palsy
 Early treatment of birth palsy The Hong King Society for Surgery of the Hand Dr. W.L.TSE Department of Orthopaedics & Traumatology Prince of Wales Hospital WL Tse Early management how? Early management:
Early treatment of birth palsy The Hong King Society for Surgery of the Hand Dr. W.L.TSE Department of Orthopaedics & Traumatology Prince of Wales Hospital WL Tse Early management how? Early management:
Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader. Lab Leaders: STATION I BRACHIAL PLEXUS
 Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader Lab Leaders: STATION I BRACHIAL PLEXUS A. Posterior cervical triangle and axilla B. Formation of plexus 1. Ventral rami C5-T1 2. Trunks
Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader Lab Leaders: STATION I BRACHIAL PLEXUS A. Posterior cervical triangle and axilla B. Formation of plexus 1. Ventral rami C5-T1 2. Trunks
Al Hess MD NERVE REPAIR
 Al Hess MD NERVE REPAIR Historical Aspects 300 BC Hippocrates, description of nervous system 200 AD Galen of Pergamon, nerve injury, questioned possibility of regeneration 600 AD Paul of Arginia, first
Al Hess MD NERVE REPAIR Historical Aspects 300 BC Hippocrates, description of nervous system 200 AD Galen of Pergamon, nerve injury, questioned possibility of regeneration 600 AD Paul of Arginia, first
Peripheral nerve injury
 Peripheral nerve injury Classification of peripheral nerve injury: I. Seddon classification: 1. Neurapraxia: conduction block with or without demyelination (the axon, endoneurium, perineurium and epineurium
Peripheral nerve injury Classification of peripheral nerve injury: I. Seddon classification: 1. Neurapraxia: conduction block with or without demyelination (the axon, endoneurium, perineurium and epineurium
