Magnetic Resonance Imaging Demonstrates Lack of Precision in Needle Placement by the Infraclavicular Brachial Plexus Block Described by Raj Et Al.
|
|
|
- Augustus Brooks
- 5 years ago
- Views:
Transcription
1 Magnetic Resonance Imaging Demonstrates Lack of Precision in Needle Placement by the Infraclavicular Brachial Plexus Block Described by Raj Et Al. Øivind Klaastad, MD*, Finn G. Lilleås, MD, Jan S. Røtnes, MD, PhD, Harald Breivik, MD, PhD*, and Erik Fosse, MD, PhD *Department of Anesthesiology and The Interventional Centre, The National Hospital, Oslo, Norway The infraclavicular brachial plexus block first described by Raj et al. was supposed to anesthetize all the main peripheral nerves of the brachial plexus without the risk of pneumothorax. However, in performing the block, we have had difficulties finding the nerves at the cord level. Therefore, we questioned whether the recommended needle direction (the Raj line ) guides the needle close enough to the cords. We therefore designed an anatomic study to answer this question and to assess the risks of entering the pleura and axillary vein. Ten volunteers were examined noninvasively in an open model magnetic resonance scanner. The Raj line deviated greatly from a defined location on the cords by a mean of 26 (range 14 39) mm, always caudad, and posterior to the target in nine cases. Further, the needle trajectory s shortest distance to the pleura was only 10 (0 27) mm, and in one case, it hit the pleura. Finally, the Raj line s distance to the axillary vein was also short, 11 (0 18) mm. We conclude that a modification of the method is necessary to guide the needle closer to the cords and further away from the pleura and the axillary vein. A more lateral needle insertion seems beneficial. Implications: Using a magnetic resonance scanner, the anatomical basis of Raj s infraclavicular method for brachial plexus blockade was examined in volunteers. The results show that the method should be modified to make it more precise and to provide less risk of complications. (Anesth Analg 1999;88:593 8) The axillary and musculocutaneous nerves are difficult to anesthetize using the axillary brachial plexus approach because of their proximal takeoff (1). The infraclavicular technique described by Raj et al. (2) was designed to avoid this difficulty by blocking all the main terminal nerves with minimal or no risk of pneumothorax. Additional advantages of this method include blockade of the intercostobrachial nerve and the ability to perform the block with the arm in any position. The target for local anesthetic injection by using Raj et al. s method is the cord level of the brachial plexus proximal to the formation of the five main terminal nerves: the axillary, musculocutaneous, radial, median, and ulnar nerves. The cords are located between the outer border of the first rib and the lateral border of the pectoralis minor muscle (Fig. 1). Beneath this muscle, the cords embrace the axillary artery longitudinally, surrounding the artery according to their names: the lateral, posterior, and medial cords. The Accepted for publication December 11, Address correspondence and reprint requests to Dr. Ø. Klaastad, Department of Anesthesiology, The National Hospital (Rikshospitalet), Trondheimsveien 132, 0570 Oslo, Norway. axillary vein is positioned caudad to the artery. Using the infraclavicular method described by Raj et al. (2), the patient is supine with the arm preferably abducted to 90. The point of needle insertion is 2.5 cm below the inferior border of the clavicle, either on a paramedian line through the point at which the subclavian artery is palpated dipping under the clavicle or, alternatively, on a paramedian line through the midpoint of the clavicle. The needle is directed laterally toward the brachial artery at an angle of 45 to the skin, the Raj line. A nerve stimulator aids in exact positioning of the needle. The method does not specify toward which part of the palpable brachial artery the needle should be directed. In the present study, we chose the point at which the lateral border of the pectoralis major muscle crosses the brachial artery. Except for the original article by Raj et al. (2), we found no references describing clinical experience with the method. Raj et al. (2) reported a success rate of approximately 95% in 200 patients ( success was not defined) and that the danger of penetrating blood vessels was the same as that using other approaches. In our experience, however, it has often been necessary to redirect the needle several times to obtain an 1999 by the International Anesthesia Research Society /99/$5.00 Anesth Analg 1999;88:
2 594 REGIONAL ANESTHESIA AND PAIN MANAGEMENT KLAASTAD ET AL. ANESTH ANALG MRI AND RAJ S INFRACLAVICULAR BLOCK 1999;88:593 8 Table 1. Demographic Data Volunteer Gender Age (yr) Height (cm) Weight (kg) 1 M F M M F M F F F M Mean sd Range Figure 1. Front view of infraclavicular anatomy, right side, illustrated by segmented magnetic resonance images merged with a correlated surface picture of the identical person. Note the clavicle and the two first costae. The coracoid process with an adjacent small lateral part of the scapula is seen medial to caput humeri. The axillary artery is found cephalad to its accompanying vein, the vein with a larger diameter than the artery. Longitudinally, the artery is embraced by the cords of the brachial plexus. The pectoralis major muscle (dark area) and the pectoralis minor muscle (gray area) are presented only with the parts caudad to the axillary vein. A needle is positioned according to Raj s infraclavicular method to block the brachial plexus, with the tip of the needle at the skin entry site. appropriate motor response with the nerve stimulator. We therefore questioned whether the recommended needle direction brings the needle close enough to the brachial plexus. Because the brachial plexus is easily demonstrated by magnetic resonance imaging (MRI) with direct multiplanar imaging capability and superior soft-tissue resolution (3), we designed a MRI study of the relevant anatomy and the needle trajectory of Raj s method on volunteers. To determine the risk of pneumothorax and axillary vein puncture, the distances from the needle trajectory to the pleura and axillary vein were also measured. Finally, we assessed whether two landmarks described by Raj et al. for derivation of the needle entry point (the point at which the subclavian artery is palpated dipping under the clavicle and the midpoint of the clavicle) are interchangeable. Methods After approval of the protocol by the regional ethical committee, 10 healthy volunteers (Table 1) gave their written, informed consent for MRI of their brachial plexus anatomy. The volunteers were examined in an open MRI scanner (4), without the use of any needle. With the open design of the scanner, it was possible to position the volunteers exactly as if they were to receive an infraclavicular block, with the arm abducted at 90. Sagittal images were obtained using threedimensional T 1 -weighted gradient echo sequence; from these images, multiplanar coronal and axial images were reconstructed. The scanning parameters were: TR/TE 34/15, flip angle 60, slice thickness 2 mm, matrix , FOV , receive bandwidth 12, NEX 1, and number of slices 124. This resulted in a total scanning time of 8 min 46 s. To simulate and evaluate the needle advancement using Raj s infraclavicular method in the threedimensional MRI of each volunteer, three anatomical key points were determined in the images. These points were the point of needle insertion, the final position of the needle point, and a target. The first two points were defined according to Raj s method; the third was defined for the present study. The Raj line is the line between the point of needle insertion and the final position of the needle point. Other lines and points in the study model aid in defining the three key points. The points were determined in coronal (frontal), sagittal (paramedian), and axial (transverse) planes, examples of which are shown for Volunteer 9 (Figs. 2 4). The target had to be on the cords and defined in a standardized fashion. To achieve this, the position of two anteroposterior lines in coronal planes were marked (Fig. 2). The first line abutted the superior border of the clavicle and went through the midaxis of the subclavian artery. This line was assumed to pass through the point at which the subclavian artery is palpated dipping under the clavicle. The second line went through the junction of the brachial artery (its midaxis) and the lateral edge of the pectoralis major muscle. This line was expected to pass through our defined palpable point of the brachial artery. A sagittal plane was then constructed through the point at which a perpendicular line from the most anterocaudad point of the coracoid process hit the plane between the two described anteroposterior lines.. The target was defined as the middle point of all nerve
3 ANESTH ANALG REGIONAL ANESTHESIA AND PAIN MANAGEMENT KLAASTAD ET AL ;88:593 8 MRI AND RAJ S INFRACLAVICULAR BLOCK Figure 2. Coronal magnetic resonance image, right side (Volunteer 9). The large, dark, central area of the picture is the right lung. The axillary artery is depicted in almost its complete length, whereas only a shorter distal part of the corresponding vein is seen caudad to the artery. Only one of the cords, above the artery, is distinctly discernible in this image. A cross-section of the clavicle (c), is seen lateral to the artery. The coracoid process (cp) is located medial to the superior aspect of caput humeri. The following symbols positions are marked by white bullets, not by the asterisks. T defined target on the cords of the brachial plexus, I point of needle insertion, F final position of the needle point once the simulated needle was advanced according to Raj s method, 1 point at which the subclavian artery is palpated dipping under the clavicle, 2 point at which the brachial artery is palpated at the junction with the lateral border of the pectoralis major muscle. None of the five described points are located in the given coronal image. However, their anteroposterior projections to this coronal image are marked as T*, I*, F*, 1*, and 2*, respectively. The needle direction recommended by using Raj s method (the Raj line ) is projected to the present coronal plane as line I*-2*. I*-T* corrected needle direction. structures around the artery in this sagittal plane (Fig. 3). The needle insertion point was determined primarily by constructing a sagittal plane through the defined anteroposterior line in the subclavian artery. In this plane, a point 25 mm below the inferior border of the clavicle was marked. The anterior projection of this point to the skin surface then defined the needle entry point (Fig. 2). The final position of the needle point was determined where the Raj line hit the sagittal plane through the defined target. The Raj line was defined by the crossing of two planes, of which the first went through the needle insertion point and the defined anteroposterior line in the brachial artery. The second plane was derived in the axial plane after drawing two lines through the needle insertion point: the first line tangentially to the skin and the other 45 to the tangent, Figure 3. Sagittal magnetic resonance image, right side (Volunteer 9). An illustration from a magnified part of the image is in the right lower corner. Ant anterior, Post posterior. The clavicle (c) and the coracoid process (cp) are indicated by arrows. The image goes through a defined target (T; the middle point of all nerve structures around the artery) on the cords. The final position of the needle point (F) is defined as the point at which the needle direction recommended by Raj s method (the Raj line ) hits this plane. T and F are represented in their true positions and are marked by white bullets. The black bullets show the position of the three cords of the brachial plexus (pl) posterior to the pectoralis minor muscle (pmi) and caudad to the cp. The cords are positioned cephalad to the artery (A), which is cephalad to the axillary vein (V). In this sagittal plane, the Raj line s distance to axillary vein wall was measured, and the true distance between T and F could be controlled. posterolaterally (Fig. 4). The plane perpendicular to the axial plane through the 45 line was the second plane defining the Raj line. The two referred landmarks were determined in coronal planes. The point at which the subclavian artery is palpated dipping under the clavicle was taken as the junction of the subclavian artery (its midaxis) and the superior border of the clavicle. The midpoint of the clavicle was defined as the midpoint of the distance between the laterocephalad and mediocephalad ends of the clavicle. The deviation of the Raj line from the target was measured both by distance and angle in the coronal and axial planes. The true distance between the points was calculated using the measurements in axial and coronal planes and could be controlled by direct measurement in the sagittal plane through the defined target. To better evaluate these measurements, the simulated needle depth (the length of the needle beneath the skin) before and after redirection of the needle was also measured in axial planes.
4 596 REGIONAL ANESTHESIA AND PAIN MANAGEMENT KLAASTAD ET AL. ANESTH ANALG MRI AND RAJ S INFRACLAVICULAR BLOCK 1999;88:593 8 Figure 4. Axial magnetic resonance image, right side, seen from below (Volunteer 9). Ant anterior, Post posterior, Lat lateral, Med medial. The large central, dark, rounded area is the right lung. Three points to be described are marked by white bullets. The plane goes through the point of needle insertion (I). By coincidence, the final position of the needle point (F) is also found in the same axial plane in this volunteer. However, the defined target (T) on the cords is cephalad to the present axial plane. T* the caudad projection of T. The needle direction recommended by Raj s method (the Raj line ) is the line I-F, 45 to the skin. The corrected needle direction in the axial plane (I-T*) is anterior to the Raj line in this volunteer by 7. The shortest distance from the Raj line to the pleura was controlled in axial planes between the needle insertion point and the final position of the needle point. The distance from the final position of the needle point to the nearest axillary vein wall (posterior or anterior vein wall) was measured in the sagittal plane through the defined target. The distance between two landmarks (where the subclavian artery dips under the clavicle and the midpoint of the clavicle) was measured in coronal planes. The results are presented as means sd or means (range). Results The trajectory of the needle direction recommended by Raj et al. (2) deviated from our target on the cords by 26 (14 39) mm (Table 2). To reach the target a cephalad redirection of the needle (in the coronal plane) by 17 (12 25) mm or 17 (13 21) was necessary in all the volunteers. In the axial plane, the Raj line deviated by 18 mm or 10 from the target, with a larger range of deviation than in the coronal plane: from 9 mm or 4 anterior to 30 mm or 17 posterior to the target. Only in Volunteer 1 did the needle direction pass on the anterior side of the target. In the remaining nine volunteers, the needle trajectory passed posterior to the target by 19 (7 30) mm or 11 (5 17). Although the imprecision of the Raj line is similar in the coronal and axial planes when measured in millimeters, it is larger in the coronal than the axial plane when measured in degrees. These seemingly discrepant results are caused by the projection of the needle being shorter in the coronal than the axial plane. The deviation of the Raj line in the axial plane implies that the target could be reached in this plane by a mean needle angle to the skin of 35 (28 49) ; that is, by a mean of 10 less than that recommended in Raj s method. The length of the simulated needle beneath the skin before and after repositioning was considerable, with mean values of 81 and 70 mm, respectively. The shortest mean distance between the needle trajectory and the pleura was 10 (0 27) mm. In Volunteer 2 (female, 160 cm tall, weighed 50 kg), the needle would have touched the pleura. In seven other volunteers, the distance was 10 mm. At the sagittal level of our defined target, the mean distance of the needle course from the axillary vein (either its posterior or anterior part) was of 11 (0 18) mm. In Volunteer 8, the Raj line touched the posterior wall of the vein. Only in Volunteer 1 did the needle trajectory pass on the anterior side of the vein (by 3 mm). Among the remaining eight volunteers, the Raj line passed posterior to the vein in the space between the vein and the pleura. In five of these eight volunteers, the simulated needle passed within 15 mm of the posterior vein wall. The midpoint of the clavicle was found lateral to the crossing of the subclavian artery with the superior border of the clavicle by 17 (9 23) mm. Only in Volunteer 4 was the distance 10 mm. Discussion On average, the Raj line deviated from the target by 26 mm in the caudad-posterior direction, which fits our clinical observations. Patient anatomic variability may contribute to difficulties in finding the cords with the needle. The additional needle passes required are uncomfortable and may increase the risk of complications, especially of pneumothorax and vessel puncture. Finally, the time for performance of the block is prolonged. Therefore, our findings strongly suggest a modification of Raj s method, either as to the point of needle insertion or needle direction. Our study further demonstrates that the method carries a risk of pneumothorax. A needle angle to the skin of 35 can hit the cords. However, with the range of this angle, there may be uncertainty as to when the needle is steep enough, as seen in our volunteers. If the nerves are not found because of an imprecise
5 ANESTH ANALG REGIONAL ANESTHESIA AND PAIN MANAGEMENT KLAASTAD ET AL ;88:593 8 MRI AND RAJ S INFRACLAVICULAR BLOCK Table 2. Results Volunteer Deviation (mm) Deviation ( ) Needle depth (mm) Sagittal Coronal a Axial b Coronal a Axial b Before After Pleura (mm) Vein (mm) c Landmarks (mm) d Mean sd Range a In all cases, the needle was deviated caudally to the target. b The results are presented by their absolute values. Except for Volunteer 1, the needle direction was posterior to the target. In Volunteer 1, the needle passed 9 mm anterior to the target and required a 4 posterior redirection to hit the target. The required needle angle to the skin in the axial plane to hit the target may be calculated by subtracting the degrees in the Deviation Axial ( ) column from the method-recommended 45 for Volunteers 2 10, then adding the degrees for Volunteer 1. c In Volunteer 8, the simulated needle hit the posterior vein wall. In Volunteer 1, the needle passed 3 mm anterior to the vein. In the remaining eight volunteers, the needle course was posterior to the vein. d In all volunteers, the midpoint of the clavicle was lateral to the point at which the subclavian artery dipped under the clavicle. needle position in the coronal plane, deeper insertion could result in pneumothorax. The risk of hitting the axillary vein is also evident from our study. Compression of the bleeding point and evaluation of the hematoma size are difficult in this location because of the presence of the pectoralis major and minor muscles between the skin and the vessel. The danger of hitting the axillary vein with a needle has not been documented in the literature. However, we think that, by using an optimal infraclavicular method, the risk of puncturing vessels should be as small as possible to avoid at least theoretical risks from a hematoma (e.g., local tenderness, discoloration, nerve injury, and compromised regional circulation). We expect a nerve stimulator to induce motor stimulation of the nerves before the needle touches the arterial wall. Therefore, measurements to determine the relationship between the needle and the axillary artery were not performed. The finding that the midpoint of the clavicle is located lateral (17 mm) to where the subclavian artery dips under the clavicle indicates that these reference points are not interchangeable for clinical purposes. One may maintain that the accuracy of needle placement is not so important as long as the injection of local anesthetic is still inside the fascial sheath of the brachial plexus. However, the question of how freely the local anesthetic spreads within the fascial sheath is still unsettled (1). Performing the blocks with the aid of a nerve stimulator, we strive for a needle point position yielding a motor response from a brachial plexus nerve by an amperage of 0.5 ma with an impulse duration of 0.1 ms. Although data in humans are lacking, such a setting probably corresponds to a distance of only a few millimeters, if that, between the needle point and the stimulated nerve (5). From this perspective, it seems unsatisfactory to use a method with an imprecision of 20 mm. Further, the selection of our target for the direction of the needle should be considered. If the target had been chosen at a more proximal point on the cords, the Raj line would have deviated even more in the coronal plane. By contrast, a more distal (lateral) target would have yielded less imprecision in the coronal plane. However, a more distal target could end in an area that may be more easily reached by using an axillary approach (6). Taken together, we think that the target selected in our model is appropriate for controlling the infraclavicular method described by Raj et al. There are several other infraclavicular methods of clinical interest (7 10). None of them has been studied using MRI. The method of Moorthy et al. (9) positions the point of needle insertion above the clavicle, but the needle point ends up in the infraclavicular area. However, we considered it rational first to study the original method of Raj et al. (2) because it was the first modern infraclavicular method and is probably the principle inspiration for variant infraclavicular techniques. Our ultimate goal is to find an infraclavicular method that seems anatomically precise using MRI and that has little risk of complications. According to unpublished information from Raj (ASRA meeting, San Diego, CA, 1996), he has changed his point of needle insertion to be on a line between the pulsation of the subclavian and the brachial artery and 2.5 cm from this line s crossing with the inferior border of the clavicle. As before, the needle is directed
6 598 REGIONAL ANESTHESIA AND PAIN MANAGEMENT KLAASTAD ET AL. ANESTH ANALG MRI AND RAJ S INFRACLAVICULAR BLOCK 1999;88:593 8 toward the brachial artery at an angle of 45 to the skin. This modified approach seems rational, making the insertion point more lateral and bringing the needle in a line that roughly corresponds to the course of the brachial plexus. We expect the modified method to be more precise in hitting the cords of the brachial plexus and to carry less risk of complications than the original method. However, this should be confirmed in a MRI study. In conclusion, our MRI findings suggest that the difficulties we had in finding the nerves by using Raj et al. s original infraclavicular method were caused by the method being too anatomically imprecise. The simultaneous risks of pneumothorax and axillary vein puncture also make a modification of the method necessary. Bringing the needle insertion point more lateral, as in Raj s modification of the infraclavicular block, probably represents a major improvement. 2. Raj PP, Montgomery SJ, Nettles D, Jenkins MT. Infraclavicular brachial plexus block: a new approach. Anesth Analg 1973;52: Posniak HV, Olson MC, Dudiak CM, et al. MR imaging of the brachial plexus. AJR Am J Roentgenol 1993;161: Jolesz FA, Blumenfeld SM. Interventional use of magnetic resonance imaging. Magn Reson Q 1994;10: Ford DJ, Pither C, Raj PP. Comparison of insulated and uninsulated needles for locating peripheral nerves with a peripheral nerve stimulator. Anesth Analg 1984;63: Winnie AP. Guest discussion. Anesth Analg 1973;52: Sims JK. A modification of landmarks for infraclavicular approach to brachial plexus block. Anesth Analg 1977;56: Whiffler K. Coracoid block: a safe and easy technique. Br J Anaesth 1981;53: Moorthy SS, Schmidt SI, Dierdorf SF, et al. A supraclavicular lateral paravascular approach for brachial plexus regional anesthesia. Anesth Analg 1991;72: Kilka HG, Geiger P, Mehrkens HH. Die vertikale infraklavikulare Blockade des Plexus brachialis. Eine neue Methode zur Anasthesie der oberen Extremitat. Eine anatomische und klinische Studie. Anaesthesist 1995;44: We thank Terje Tillung (The Interventional Center) for processing the images and Per Øyvind Hvidsten (The Norwegian Defense Research Establishment) for developing the three-dimensional visualization software. References 1. Brown DL, Bridenbaugh LD. The upper extremity: somatic blockade. In: Cousins MJ, Bridenbaugh PO, eds. Neural blockade in clinical anesthesia and management of pain. Philadelphia: Lippincott-Raven, 1998:
Infraclavicular brachial plexus blocks aim at the
 REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
Infraclavicular brachial plexus blocks have been designed
 The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Distribution of Local Anesthetic in Axillary Brachial Plexus Block
 Anesthesiology 2002; 96:1315 24 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Distribution of Local Anesthetic in Axillary Brachial Plexus Block A Clinical and Magnetic
Anesthesiology 2002; 96:1315 24 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Distribution of Local Anesthetic in Axillary Brachial Plexus Block A Clinical and Magnetic
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist
 Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone
 *the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
Ultrasound-guided supraclavicular block
 THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
The relationship of the musculocutaneous nerve to the brachial plexus evaluated by MRI
 DOI 10.1007/s10877-015-9807-3 ORIGINAL RESEARCH The relationship of the musculocutaneous nerve to the brachial plexus evaluated by MRI Trygve Kjelstrup 1,2 Axel R. Sauter 3 Per K. Hol 2,4 Received: 23
DOI 10.1007/s10877-015-9807-3 ORIGINAL RESEARCH The relationship of the musculocutaneous nerve to the brachial plexus evaluated by MRI Trygve Kjelstrup 1,2 Axel R. Sauter 3 Per K. Hol 2,4 Received: 23
The Language of Anatomy. (Anatomical Terminology)
 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The arm: *For images refer back to the slides
 The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla.
 1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
A study of the anatomy of the caudal space using magnetic resonance imaging
 British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
INTRODUCTION. Getting the best scan. Choosing a probe. Choosing the frequency
 Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
*Our main subject is the brachial plexus but it's important to understand the spinal cord first in order to understand the brachial plexus.
 *Our main subject is the brachial plexus but it's important to understand the spinal cord first in order to understand the brachial plexus. *Vertebral column is formed by the union of 33 sequential vertebrae
*Our main subject is the brachial plexus but it's important to understand the spinal cord first in order to understand the brachial plexus. *Vertebral column is formed by the union of 33 sequential vertebrae
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
USRA OF THE UPPER EXTREMITY
 USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear Transducer
 ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
Sonographic Mapping of the Normal Brachial Plexus
 AJNR Am J Neuroradiol 24:1303 1309, August 2003 Sonographic Mapping of the Normal Brachial Plexus Xavier Demondion, Pascal Herbinet, Nathalie Boutry, Christian Fontaine, Jean-Paul Francke, and Anne Cotten
AJNR Am J Neuroradiol 24:1303 1309, August 2003 Sonographic Mapping of the Normal Brachial Plexus Xavier Demondion, Pascal Herbinet, Nathalie Boutry, Christian Fontaine, Jean-Paul Francke, and Anne Cotten
Fascial Compartments of the Upper Arm
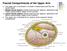 Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block
 Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Diana Mathioudakis DEAA EDIC AFRCA. consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d)
 & Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
& Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
Magnetic Resonance Angiography
 Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
A New Anterior Approach for Fluoroscopy-guided Suprascapular Nerve Block
 Original Article Korean J Pain 2012 July; Vol. 25, No. 3: 168-172 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.3.168 A New Anterior Approach for Fluoroscopy-guided Suprascapular
Original Article Korean J Pain 2012 July; Vol. 25, No. 3: 168-172 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.3.168 A New Anterior Approach for Fluoroscopy-guided Suprascapular
Definition of Anatomy. Anatomy is the science of the structure of the body and the relation of its parts.
 Definition of Anatomy Anatomy is the science of the structure of the body and the relation of its parts. Basic Anatomical Terms Anatomical terms for describing positions: Anatomical position: Supine position:
Definition of Anatomy Anatomy is the science of the structure of the body and the relation of its parts. Basic Anatomical Terms Anatomical terms for describing positions: Anatomical position: Supine position:
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Jake Hutchins, M.D. Aaron Berg, D.O.
 Jake Hutchins, M.D. Aaron Berg, D.O. Jacob Hutchins is on the speaker s bureau, is a consultant, and has received research funding from Pacira Pharmaceuticals He also is a consultant for Insitu Biologics,
Jake Hutchins, M.D. Aaron Berg, D.O. Jacob Hutchins is on the speaker s bureau, is a consultant, and has received research funding from Pacira Pharmaceuticals He also is a consultant for Insitu Biologics,
The infraclavicular brachial plexus block by the coracoid approach is clinically effective: an observational study of 150 patients
 253 Regional Anesthesia and Pain The infraclavicular brachial plexus block by the coracoid approach is clinically effective: an observational study of 150 patients [Le bloc infraclaviculaire du plexus
253 Regional Anesthesia and Pain The infraclavicular brachial plexus block by the coracoid approach is clinically effective: an observational study of 150 patients [Le bloc infraclaviculaire du plexus
Ex. 1 :Language of Anatomy
 Collin College BIOL 2401 : Human Anatomy & Physiology Ex. 1 :Language of Anatomy The Anatomical Position Used as a reference point when referring to specific areas of the human body Body erect Head and
Collin College BIOL 2401 : Human Anatomy & Physiology Ex. 1 :Language of Anatomy The Anatomical Position Used as a reference point when referring to specific areas of the human body Body erect Head and
A Frame of Reference for Anatomical Study. Anatomy and Physiology Mr. Knowles Chapter 1 Liberty Senior High School
 A Frame of Reference for Anatomical Study Anatomy and Physiology Mr. Knowles Chapter 1 Liberty Senior High School Anatomical Terms of Direction and Position Created for communicating the direction and
A Frame of Reference for Anatomical Study Anatomy and Physiology Mr. Knowles Chapter 1 Liberty Senior High School Anatomical Terms of Direction and Position Created for communicating the direction and
MUSCLES. Anconeus Muscle
 LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
Axilla and Brachial Region
 L 4 A B O R A T O R Y Axilla and Brachial Region BRACHIAL PLEXUS 5 Roots/Rami (ventral rami C5 T1) 3 Trunks Superior (C5, C6) Middle (C7) Inferior (C8, T1) 3 Cords Lateral Cord (Anterior Superior and Anterior
L 4 A B O R A T O R Y Axilla and Brachial Region BRACHIAL PLEXUS 5 Roots/Rami (ventral rami C5 T1) 3 Trunks Superior (C5, C6) Middle (C7) Inferior (C8, T1) 3 Cords Lateral Cord (Anterior Superior and Anterior
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
The Arm and Cubital Fossa
 The Arm and Cubital Fossa Dr. Andrew Gallagher School of Anatomical Sciences University of the Witwatersrand Introduction The ARM (BRACHIUM) is the most proximal segment of the upper limb musculoskeletal
The Arm and Cubital Fossa Dr. Andrew Gallagher School of Anatomical Sciences University of the Witwatersrand Introduction The ARM (BRACHIUM) is the most proximal segment of the upper limb musculoskeletal
Plantar Flexion Seems More Reliable than Dorsiflexion with Labat s Sciatic Nerve Block: A Prospective, Randomized Comparison
 Plantar Flexion Seems More Reliable than Dorsiflexion with Labat s Sciatic Nerve Block: A Prospective, Randomized Comparison Manuel Taboada, MD*, Peter G. Atanassoff, MD, Jaime Rodríguez, MD, PhD*, Joaquín
Plantar Flexion Seems More Reliable than Dorsiflexion with Labat s Sciatic Nerve Block: A Prospective, Randomized Comparison Manuel Taboada, MD*, Peter G. Atanassoff, MD, Jaime Rodríguez, MD, PhD*, Joaquín
Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta.
 Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta. Fig-3: Showing high formation of Median nerve. Fig-1: Showing atypical formation of cords of Brachial plexus. 1 = Upper
Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta. Fig-3: Showing high formation of Median nerve. Fig-1: Showing atypical formation of cords of Brachial plexus. 1 = Upper
Slides of Anatomy. Spring Dr. Maher Hadidi, University of Jordan
 Slides of Anatomy Please note : These slides are Dr. Maher Hadidi s slides of spring 2016 and were edited by the Premed Academic Team to fit the slides of spring 2019. Spring 2019 Dr. Maher Hadidi, University
Slides of Anatomy Please note : These slides are Dr. Maher Hadidi s slides of spring 2016 and were edited by the Premed Academic Team to fit the slides of spring 2019. Spring 2019 Dr. Maher Hadidi, University
Finite Difference Modeling of the Anisotropic Electric Fields generated by Stimulating Needles used for Catheter Placement
 > REPLACE THIS LINE WITH YOUR PAPER IDENTIFICATION NUMBER (DOUBLE-CLICK HERE TO EDIT) < 1 Finite Difference Modeling of the Anisotropic Electric Fields generated by Stimulating Needles used for Catheter
> REPLACE THIS LINE WITH YOUR PAPER IDENTIFICATION NUMBER (DOUBLE-CLICK HERE TO EDIT) < 1 Finite Difference Modeling of the Anisotropic Electric Fields generated by Stimulating Needles used for Catheter
The goal of this article is to describe the. Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation.
 Pain Physician 2011; 14:45-53 ISSN 1533-3159 Technique Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation Jie Zhu, MD 1, Frank Falco, MD 1,2, C. Obi Onyewu, MD 1, Youssef
Pain Physician 2011; 14:45-53 ISSN 1533-3159 Technique Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation Jie Zhu, MD 1, Frank Falco, MD 1,2, C. Obi Onyewu, MD 1, Youssef
MUSCLE MECHANICS AND CONTROL
 MUSCLE MECHANICS AND CONTROL STRUCTURE OF A SKELETAL MUSCLE NEUROVASCULAR BUNDLE - CONTAINS THE BLOOD VESSELS AND THE NERVES TO A MUSCLE SKELETAL MUSCLE - LONGITUDINAL SECTION MUSCLE ATTACHMENTS: TENDONS
MUSCLE MECHANICS AND CONTROL STRUCTURE OF A SKELETAL MUSCLE NEUROVASCULAR BUNDLE - CONTAINS THE BLOOD VESSELS AND THE NERVES TO A MUSCLE SKELETAL MUSCLE - LONGITUDINAL SECTION MUSCLE ATTACHMENTS: TENDONS
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5. September 30, 2011
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
The Elbow Scanning Protocol
 The Elbow Scanning Protocol Diagnostic Imaging of the Elbow: Introduction The elbow maybe considered as consisting of four quadrants, anterior, medial, lateral and posterior. Ultrasound would normally
The Elbow Scanning Protocol Diagnostic Imaging of the Elbow: Introduction The elbow maybe considered as consisting of four quadrants, anterior, medial, lateral and posterior. Ultrasound would normally
Richard Dobrusin DO FACOFP
 Richard Dobrusin DO FACOFP Define Thoracic Outlet Syndrome (TOS) Describe the Mechanisms of Dysfunction List Diagnostic tests for (TOS) Understand (TOS) referral patterns Discuss Treatment Options Definition:
Richard Dobrusin DO FACOFP Define Thoracic Outlet Syndrome (TOS) Describe the Mechanisms of Dysfunction List Diagnostic tests for (TOS) Understand (TOS) referral patterns Discuss Treatment Options Definition:
3 Mohammad Al-Mohtasib Areej Mosleh
 3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
Introduction to Ultrasound Guided Region Anesthesia
 Introduction to Ultrasound Guided Region Anesthesia Brian D. Sites, MD Dept of Anesthesiology Dartmouth-Hitchcock Medical Center INTRODUCTION Welcome to Introduction to Ultrasound Guided Regional Anesthesia.
Introduction to Ultrasound Guided Region Anesthesia Brian D. Sites, MD Dept of Anesthesiology Dartmouth-Hitchcock Medical Center INTRODUCTION Welcome to Introduction to Ultrasound Guided Regional Anesthesia.
6.4 The Ankle. Body Divided into Planes. Health Services: Unit 6 Arms and Legs. Body Movement Vocabulary
 6.4 The Ankle Body Movement Vocabulary When fitness professionals refer to movement of the body, the pattern of movement is described from the anatomical position This position can best be described as
6.4 The Ankle Body Movement Vocabulary When fitness professionals refer to movement of the body, the pattern of movement is described from the anatomical position This position can best be described as
Levels of the anatomical cuts of the upper extremity RADIUS AND ULNA right
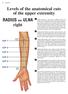 11 CHAPTER 2 Levels of the anatomical cuts of the upper extremity AND right CUT 1 CUT 4 1 2 3 4 5 6 Isolated fixation of the radius is difficult at this level because of the anterolateral vessels and the
11 CHAPTER 2 Levels of the anatomical cuts of the upper extremity AND right CUT 1 CUT 4 1 2 3 4 5 6 Isolated fixation of the radius is difficult at this level because of the anterolateral vessels and the
Carlos Torres MD, FRCPC, Associate Professor of Radiology Department of Radiology, University of Ottawa
 Carlos Torres MD, FRCPC, Associate Professor of Radiology Department of Radiology, University of Ottawa catorres@toh.on.ca None 1. Simplify the complex imaging anatomy of the BP using clear anatomical
Carlos Torres MD, FRCPC, Associate Professor of Radiology Department of Radiology, University of Ottawa catorres@toh.on.ca None 1. Simplify the complex imaging anatomy of the BP using clear anatomical
ULTRASOUND-GUIDED peripheral
 392 392 CANADIAN JOURNAL OF ANESTHESIA Images in Anesthesia Cadaveric ultrasound imaging for training in ultrasound-guided peripheral nerve blocks: upper extremity ULTRASOUND-GUIDED peripheral nerve blocks
392 392 CANADIAN JOURNAL OF ANESTHESIA Images in Anesthesia Cadaveric ultrasound imaging for training in ultrasound-guided peripheral nerve blocks: upper extremity ULTRASOUND-GUIDED peripheral nerve blocks
Ultrasound Guided Injections
 Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
Upper Limb Muscles Muscles of Axilla & Arm
 Done By : Saleh Salahat Upper Limb Muscles Muscles of Axilla & Arm 1) Muscles around the axilla A- Muscles connecting the upper to thoracic wall (4) 1- pectoralis major Origin:- from the medial half of
Done By : Saleh Salahat Upper Limb Muscles Muscles of Axilla & Arm 1) Muscles around the axilla A- Muscles connecting the upper to thoracic wall (4) 1- pectoralis major Origin:- from the medial half of
G24: Shoulder and Axilla
 G24: Shoulder and Axilla Syllabus - Pg. 2 ANAT 6010- Medical Gross Anatomy David A. Morton, Ph.D. Objectives Upper limb Systemically: Bones (joints) Muscles Nerves Vessels (arteries/veins) Fascial compartments
G24: Shoulder and Axilla Syllabus - Pg. 2 ANAT 6010- Medical Gross Anatomy David A. Morton, Ph.D. Objectives Upper limb Systemically: Bones (joints) Muscles Nerves Vessels (arteries/veins) Fascial compartments
Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion
 Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
Brachial plexuses and axillary lymph nodes
 Brachial plexuses and axillary lymph nodes Introduction about nervous system nervous system central nervous system periphral nervous system brain spinal cord 31 pairs of spinal nerves 12 paris of cranial
Brachial plexuses and axillary lymph nodes Introduction about nervous system nervous system central nervous system periphral nervous system brain spinal cord 31 pairs of spinal nerves 12 paris of cranial
Introduction to The Human Body
 1 Introduction to The Human Body FOCUS: The human organism is often examined at seven structural levels: chemical, organelle, cell, tissue, organ, organ system, and the organism. Anatomy examines the structure
1 Introduction to The Human Body FOCUS: The human organism is often examined at seven structural levels: chemical, organelle, cell, tissue, organ, organ system, and the organism. Anatomy examines the structure
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Forensic Archaeology & Forensic Anthropology. ADJ14 Advanced Criminal Investigations
 Forensic Archaeology & Forensic Anthropology ADJ14 Advanced Criminal Investigations Anthropology & Archaeology Anthropology is the study of the biological and cultural aspects of all humans in all places
Forensic Archaeology & Forensic Anthropology ADJ14 Advanced Criminal Investigations Anthropology & Archaeology Anthropology is the study of the biological and cultural aspects of all humans in all places
SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE CORNISH TECHNIQUE
 THE JOURNAL OF NEW YORK SCHOOL OF REGIONAL ANESTHESIA SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE BY CORHISH PB Author Affiliation: Nelson, New Zealand This essay is based on a project which has
THE JOURNAL OF NEW YORK SCHOOL OF REGIONAL ANESTHESIA SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE BY CORHISH PB Author Affiliation: Nelson, New Zealand This essay is based on a project which has
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
JlntSocPlastination, Vol4:16-22,
 JlntSocPlastination, Vol4:16-22, 1990 16 SECTIONAL ANATOMY: STANDARDIZED METHODOLOGY Alexander Lane, Coordinator of Anatomy and Physiology, Triton College, Visiting Associate Professor, University of Illinois
JlntSocPlastination, Vol4:16-22, 1990 16 SECTIONAL ANATOMY: STANDARDIZED METHODOLOGY Alexander Lane, Coordinator of Anatomy and Physiology, Triton College, Visiting Associate Professor, University of Illinois
Ultrasound-guided infraclavicular axillary vein cannulation for central venous access {
 British Journal of Anaesthesia 93 (2): 188 92 DOI: 10.1093/bja/aeh187 Advance Access publication June 25, 2004 Ultrasound-guided infraclavicular axillary vein cannulation for central venous access { A.
British Journal of Anaesthesia 93 (2): 188 92 DOI: 10.1093/bja/aeh187 Advance Access publication June 25, 2004 Ultrasound-guided infraclavicular axillary vein cannulation for central venous access { A.
Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS
 Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS Assistant Professor of Surgery Vascular Endovascular Surgery Louisiana State University Health - Shreveport Disclosures None Objective
Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS Assistant Professor of Surgery Vascular Endovascular Surgery Louisiana State University Health - Shreveport Disclosures None Objective
Brachial Plexus Nerve Block with CT Guidance for Regional Pain Management: Initial Results 1
 Technical Developments Suresh K. Mukherji, MD Archana Wagle, MD Diane M. Armao, MD Sunil Dogra, MD Index terms: Brachial plexus, 276.126 Computed tomography (CT), guidance, 276.1211 Interventional procedures,
Technical Developments Suresh K. Mukherji, MD Archana Wagle, MD Diane M. Armao, MD Sunil Dogra, MD Index terms: Brachial plexus, 276.126 Computed tomography (CT), guidance, 276.1211 Interventional procedures,
The Brachial Plexus and Thoracic Outlet Syndrome
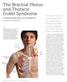 The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
Key Relationships in the Upper Limb
 Key Relationships in the Upper Limb This list contains some of the key relationships that will help you identify structures in the lab. They are organized by dissection assignment as defined in the syllabus.
Key Relationships in the Upper Limb This list contains some of the key relationships that will help you identify structures in the lab. They are organized by dissection assignment as defined in the syllabus.
POSTERIOR 1. situated behind: situated at or toward the hind part of the body :
 ANATOMICAL LOCATION Anatomy is a difficult subject with a large component of memorization. There is just no way around that, but we have made every effort to make this course diverse and fun. The first
ANATOMICAL LOCATION Anatomy is a difficult subject with a large component of memorization. There is just no way around that, but we have made every effort to make this course diverse and fun. The first
Practical 2 Worksheet
 Practical 2 Worksheet Upper Extremity BONES 1. Which end of the clavicle is on the lateral side (acromial or sternal)? 2. Describe the difference in the appearance of the acromial and sternal ends of the
Practical 2 Worksheet Upper Extremity BONES 1. Which end of the clavicle is on the lateral side (acromial or sternal)? 2. Describe the difference in the appearance of the acromial and sternal ends of the
Bony Thorax. Anatomy and Procedures of the Bony Thorax Edited by M. Rhodes
 Bony Thorax Anatomy and Procedures of the Bony Thorax 10-526-191 Edited by M. Rhodes Anatomy Review Bony Thorax Formed by Sternum 12 pairs of ribs 12 thoracic vertebrae Conical in shape Narrow at top Posterior
Bony Thorax Anatomy and Procedures of the Bony Thorax 10-526-191 Edited by M. Rhodes Anatomy Review Bony Thorax Formed by Sternum 12 pairs of ribs 12 thoracic vertebrae Conical in shape Narrow at top Posterior
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
BILATERAL RARE NEURO VASCULAR VARIATIONS OF UPPER LIMB A CASE REPORT
 BILATERAL RARE NEURO VASCULAR VARIATIONS OF UPPER LIMB A CASE REPORT *N. B. S. Parimala Department of Anatomy, Dr. Pinnamaneni Siddhartha Institute of Medical Sciences & Research Foundation, Chinnaoutpalli,
BILATERAL RARE NEURO VASCULAR VARIATIONS OF UPPER LIMB A CASE REPORT *N. B. S. Parimala Department of Anatomy, Dr. Pinnamaneni Siddhartha Institute of Medical Sciences & Research Foundation, Chinnaoutpalli,
Lab no 1 Structural organization of the human body
 Physiology Lab Manual Page 1 of 6 Lab no 1 Structural organization of the human body Physiology is the science which deals with functions of the body parts, and how they work. Since function cannot be
Physiology Lab Manual Page 1 of 6 Lab no 1 Structural organization of the human body Physiology is the science which deals with functions of the body parts, and how they work. Since function cannot be
Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries
 Cronicon OPEN ACCESS ANAESTHESIA Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries Susmita Bhattacharyya, KalyanBrata Mandal,
Cronicon OPEN ACCESS ANAESTHESIA Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries Susmita Bhattacharyya, KalyanBrata Mandal,
Anatomy and Physiology
 Anatomy and Physiology Anatomy---Study of Structure Gross anatomy Systemic anatomy Regional anatomy Microscopic anatomy Physiology---Study of Function Neurophysiology Muscle physiology Respiratory Renal
Anatomy and Physiology Anatomy---Study of Structure Gross anatomy Systemic anatomy Regional anatomy Microscopic anatomy Physiology---Study of Function Neurophysiology Muscle physiology Respiratory Renal
Body Planes & Positions
 Learning Objectives Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how it is used to reference the body. Distinguish
Learning Objectives Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how it is used to reference the body. Distinguish
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D.
 Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D. Cleveland Clinic, Cleveland OH 1 Complications during central venous catheterization (CVC) occur 2% -15% of the
Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D. Cleveland Clinic, Cleveland OH 1 Complications during central venous catheterization (CVC) occur 2% -15% of the
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck.
 Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
The pectoral region. University of Babylon College of Medicine Dr.HaythemAli Alsayigh M.B.CH.B.-F.I.M.B.S. Surgical Clinical Anatomy
 The pectoral region University of Babylon College of Medicine Dr.HaythemAli Alsayigh M.B.CH.B.-F.I.M.B.S. Surgical Clinical Anatomy Objective Study the Bones and Joints A. Clavicle (collarbone) B. Scapula
The pectoral region University of Babylon College of Medicine Dr.HaythemAli Alsayigh M.B.CH.B.-F.I.M.B.S. Surgical Clinical Anatomy Objective Study the Bones and Joints A. Clavicle (collarbone) B. Scapula
Shoulder Arthroscopy Portals
 Shoulder Arthroscopy Portals Alper Deveci and Metin Dogan 7 7.1 Bony Landmarks Before starting shoulder arthroscopy, the patient must be positioned and draping applied. Then the bony landmarks are identified
Shoulder Arthroscopy Portals Alper Deveci and Metin Dogan 7 7.1 Bony Landmarks Before starting shoulder arthroscopy, the patient must be positioned and draping applied. Then the bony landmarks are identified
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Ultrasound identification of nerve cords in the infraclavicular fossa: a clinical study
 O R I G I N A L A R T I C L E Ultrasound identification of nerve cords in the infraclavicular fossa: a clinical study A. DI FILIPPO 1, S. ORANDO 1, A. LUNA 1, L. GIANESELLO 2, A. BOCCACCINI 2, M. C. CAMPOLO
O R I G I N A L A R T I C L E Ultrasound identification of nerve cords in the infraclavicular fossa: a clinical study A. DI FILIPPO 1, S. ORANDO 1, A. LUNA 1, L. GIANESELLO 2, A. BOCCACCINI 2, M. C. CAMPOLO
Imbibe Bone marrow aspiration needle. Operative technique
 Imbibe Bone marrow aspiration needle Operative technique Imbibe Bone Marrow Aspiration Needle Imbibe Bone marrow aspiration needle Contents 1. Smart design... 3 2. Operative technique... 4 Posterior iliac
Imbibe Bone marrow aspiration needle Operative technique Imbibe Bone Marrow Aspiration Needle Imbibe Bone marrow aspiration needle Contents 1. Smart design... 3 2. Operative technique... 4 Posterior iliac
RESONANCE IMAGING NERVES ON MAGNETIC. James D. Collins, MD, Marla L. Shaver, Poonam Batra, MD, and Kathleen Brown, MD Los Angeles, California
 NERVES ON MAGNETIC RESONANCE IMAGING James D. Collins, MD, Marla L. Shaver, Poonam Batra, MD, and Kathleen Brown, MD Los Angeles, California Nerves are often visualized on magnetic resonance imaging (MRI)
NERVES ON MAGNETIC RESONANCE IMAGING James D. Collins, MD, Marla L. Shaver, Poonam Batra, MD, and Kathleen Brown, MD Los Angeles, California Nerves are often visualized on magnetic resonance imaging (MRI)
Hip arthroscopy using the Smith & Nephew Hip Access System
 Hip Series Technique Guide *smith&nephew HIP ACCESS SYSTEM Hip Arthroscopy System Hip arthroscopy using the Smith & Nephew Hip Access System Victor M. Ilizaliturri, Jr., M.D. Hip arthroscopy using the
Hip Series Technique Guide *smith&nephew HIP ACCESS SYSTEM Hip Arthroscopy System Hip arthroscopy using the Smith & Nephew Hip Access System Victor M. Ilizaliturri, Jr., M.D. Hip arthroscopy using the
Evidence Based Approach to Shoulder Injections
 Evidence Based Approach to Shoulder Injections Bradley Sandella, DO Christiana Care Sports Medicine Joseph Straight, MD First State Orthopaedics Objectives Relevant Anatomy Indications for injections Injection
Evidence Based Approach to Shoulder Injections Bradley Sandella, DO Christiana Care Sports Medicine Joseph Straight, MD First State Orthopaedics Objectives Relevant Anatomy Indications for injections Injection
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Vascular Access (venous (peripheral and central) and arterial)
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Introduction. Chapter 1. Structure and Function. Introduction. Anatomy and Physiology Integrated. Anatomy and Physiology Integrated Anatomy
 Introduction Chapter 1 An Introduction to A&P Study strategies crucial for success Attend all lectures, labs, and study sessions Read your lecture and laboratory assignments before going to class or lab
Introduction Chapter 1 An Introduction to A&P Study strategies crucial for success Attend all lectures, labs, and study sessions Read your lecture and laboratory assignments before going to class or lab
First stage Lec.1 : Introduction. Asst.Lec.Dr.ABDULRIDHA ALASADY
 First stage 2018-2019 Lec.1 : Introduction Asst.Lec.Dr.ABDULRIDHA ALASADY Anatomy the study of the structure and shape of the body and body parts & their relationships to one another aided by dissection
First stage 2018-2019 Lec.1 : Introduction Asst.Lec.Dr.ABDULRIDHA ALASADY Anatomy the study of the structure and shape of the body and body parts & their relationships to one another aided by dissection
Anatomical Terminology
 Anatomical Terminology Dr. A. Ebneshahidi Anatomy Anatomy : is the study of structures or body parts and their relationships to on another. Anatomy : Gross anatomy - macroscopic. Histology - microscopic.
Anatomical Terminology Dr. A. Ebneshahidi Anatomy Anatomy : is the study of structures or body parts and their relationships to on another. Anatomy : Gross anatomy - macroscopic. Histology - microscopic.
Upper limb Pectoral region & Axilla
 Upper limb Pectoral region & Axilla 黃敏銓 mchuang@ntu.edu.tw 1 Pectoral region Intercostal nerve Anterior branch of lateral cutaneous branch Lateral cutaneous branch Anterior cutaneous branch Anterior cutaneous
Upper limb Pectoral region & Axilla 黃敏銓 mchuang@ntu.edu.tw 1 Pectoral region Intercostal nerve Anterior branch of lateral cutaneous branch Lateral cutaneous branch Anterior cutaneous branch Anterior cutaneous
Ultrasound Physics & Terminology
 Ultrasound Physics & Terminology This module includes the following: Basic physics terms Basic principles of ultrasound Ultrasound terminology and terms Common artifacts seen Doppler principles Terms for
Ultrasound Physics & Terminology This module includes the following: Basic physics terms Basic principles of ultrasound Ultrasound terminology and terms Common artifacts seen Doppler principles Terms for
