Respiratory Distress Syndrome
|
|
|
- Amice Terry
- 6 years ago
- Views:
Transcription
1
2 Respiratory Distress Syndrome -Introduction: Generally speaking, there s an overlap between the presentations of cardiac and respiratory illnesses in neonates. Also there s a considerable overlap between the respiratory illnesses themselves in neonates. Thus, it s important to understand how to approach such patients in order to narrow the differential diagnosis list and identify the presenting illness, so that to manage it correctly. If the correct diagnosis of the presenting illness was missed, there might be a chance that the used measures in management will worsen the patient s condition. For example, cyanosis as a symptom might of respiratory or cardiac in origin. In cyanosis of respiratory origin, O2 supplement is an integral part in its management and O2 saturation should be maintained near its normal level as much as possible. But in cases of transposition of the great vessels; cyanosis of cardiac origin, O2 saturation should be maintained around 65-75% in order not result in pulmonary hypertension. The causes of respiratory distress/ illnesses in neonates can be divided into pulmonary extrapulmonary causes. *Extrapulmonary causes: Cardiovascular (Congenital heart diseases, hypovolemia), Hematologic (Polycythemia, anemia), Metabolic Disturbances (Acidosis, hypoglycemia), Others (Hypothermia, CNS hemorrhage, drug use, macroglossia. In macroglossia,a feature of hypothyroidism, the tongue will flip back obstructing the airway. It can be managed initially with placing the neonate in a prone position or placing a mouth piece to prevent the tongue from flipping back. *Pulmonary causes: 1-Upper airway obstruction, like in choanal atresia. Choanal atresia is a congenital disorder where the back of the nasal passage (choana) is blocked, usually by abnormal bony or soft tissue (membranous) due to failed recanalization of the nasal fossae during fetal development. (Wikipedia). When the patient is calm, he/she ll be cyanosed. But the patient s color will turn into pink (normal) when he/she cries (due to the opening of the mouth). This is the classical presentation of choanal atresia. The diagnosis is confirmed using a CT scan. It s managed initially by placement of a mouth piece to sustain their breath, then it s corrected surgically. 2-Larnygomalacia: weakened muscles of the larynx resulting in collapse of the airway during expiration.* It s managed by cauterization and it ll resolve around the age of 2 yrs. (the dr didn t specify which part of the larynx exactly, and different treatment measures are written in Wikipedia.) * The mechanism of the obstruction in laryngomalacia is described as the following in Wikipedia: soft, immature cartilage of the upper larynx collapses inward during inhalation, causing airway and
3 obstruction. in older patients, especially those with neuromuscular conditions resulting in weakness of the muscles of the throat. 3-Tracheomalacia: is a condition characterized by flaccidity of the tracheal support cartilage which leads to tracheal collapse especially when increased airflow is demanded. (from Wikipedia. It was mentioned by the dr without explaining it.) 4-Vascular ring: is a very rare condition that presents with stridor or wheezes in addition to some gastrointestinal symptoms. Proper investigation begins with the use of barium study, in which an indentation of the esophagus is seen as a result of the blood vessel encircling it (bearing in mind that the trachea is encircled too).confirmed the diagnosis is done using an MRI. It s managed by surgical correction. Other pulmonary causes that should be kept in mind in suspected cases: respiratory distress syndrome (RDS), transient tachypna of the newborn (TTN), pulmonary hypoplasia,, meconium aspiration, congenital pneumonia, diaphragmatic hernia, persistent pulmonary hypertension of the newborn, RDS Previously called hyaline membrane disease. It s difficult to differentiate RDS from congenital pneumonia and TTN on clinical presentation. Although some full term infants are at risk for developing RDS (infants of diabetic mothers, c/s deliveries, white race), It s a disease of prematurity. -Approaching the Patient: A full history should be taken, a thorough physical examination should be conducted, CBC and other relevant lab investigations and imaging studies must be done to rule out extrapulmonary causes of the presenting signs and symptoms. (Like: hypoglycemia, polycythemia, hypotensive, acidosis). Each condition has its own clues. *History: the relevant details of history history: in such conditions are mainly found in the perinatal -Prenatal: maternal age (advanced maternal age increase the risk of trisomy 21 and other genetic syndromes.), history of gestational diabetes (would direct our thinking to TTN, RDS, hypoglycemia, transposition of the great vessels), HTN (leads to IUGR, polycythemia, hypoglycemia), drug intake (Lithium intake leads to Ebstein's anomaly*. Adminstration of sedatives to the mother would result in either fetal respiratory depression or apnea), PROM suggests neonatal sepsis. -Natal: prematurity is a known risk factor for RDS. Post-term delivery or presence of meconium when the membrane is ruptured increase the risk for meconium aspiration syndrome. Mode of delivery (C/S suggests TTN). Oligohydramnios is a major cause of pulmonary hypoplasia.
4 *Physical examination: the type of the associated respiratory distress signs should be exactly mentioned in addition to the presence of chest deformities. *Investigations and Imaging Studies: chest X-ray must be obtained to aid in differentiating between the suspected pulmonary causes.(it s considered as a part of the chest physical examination until 2 yrs of age.) -Disease Course: The newborn looks normal after delivery, then signs and symptoms of respiratory distress start to develop after 30 minutes of delivery. The signs and symptoms reach their peak after 2 hours, then the chance for the patient to die is highest after hours of delivery. If the neonate survived the aforementioned course, after 72 hrs, some RDS patients will start to produce endogenous surfactant and consequently, the clinical picture will improve. RDS was a major cause of death in neonates. Nowadays, the availability of surfactant improved the outcome of RDS significantly. -Ruling Out Other Possible Causes: Congenital pneumonia is difficult to differentiate from st RDS, especially during the 1 48 hours of the disease course because the chest X-ray appears normal. After 24 hours of congenital pneumonia course, the classical consolidations of pneumonia can be seen on a chest X-ray. As a precautional measure, empirical antibiotic treatment should be started in such instances until the exact cause of the signs and symptoms is identified. (Group B Streptococci is a frequent cause of congenital pneumonia) This part was done by Mohammad Nayef :D True wisdom comes to each of us when we realize how little we understand about life, ourselves and the world around us. Socrates. Dedication takes a lifetime, but dreams last for a night!
5 after 72 hours, patients start producing their own surfactant, and recovery will happen. Recovery is prolonged by baro-trauma or oxidative injury. So it's important to manage the amount of oxygen and the ventilator set up used which makes a difference in their survival, complications and length of hospitalization. Always remember that the number one risk factor for RDS is prematurity, although it can happen is other cases, but it's early onset after birth. From Nelson Essentials: Surfactant is produced in 32-34th weeks of gestations, and by the 36th, sufficient surface-active material is produced by the type II cells in the lung, is secreted into the alveolar lumen, and is excreted into the amniotic fluid. The concentration of lecithin in amniotic fluid indicates fetal pulmonary maturity. The ratio of lecithin(changes) to sphingomyelin(constant) L/S is determined. An L/S ratio of 2:1 indicated pulmonary maturity. The presence of minor phospholipids, such as phosphatidylgylcerol, also is indicative of fetal lung maturity and may be useful when L/S ratio is borderline or possibly affected by maternal diabetes. The absence of phosphatidylgylcerol suggests that surfactant might not be mature. Physical Examination should be: 1- brief but thorough 2- checking for signs of respiratory distress: Tachypnea, as the normal respiratory rate for full terms is up to 60, so if you are having more than 60, then he/she is tachypnic. Grunting Nasal Flaring Retractions Cyanosis 3- Temperature, blood pressure, and skin perfusion.
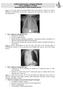
6 This is a typical/classical RDS X ray; we can see tracheal tube inside the trachea, ground glass appearance ورقة راشش عليها ملح و فلفل),(زي and air bronchogram because there are altelectatic changes in the alveoli, some are open and others closed so this is how it appears (radiolucent shadows). Always remember that RDS is none homogenous disease, due to partial alveolar pressure which is different from one area to another. Surfactant works to homogenize the pressure, and this reduces the chances to develop pneumothorax from mechanical ventilations, which RDS can complicate into.
7 Here you can see white out lung, which means that the lung and liver have similar color. White out means we have sever RDS; the lung is very stiff, barely any air in the lungs. (Nilson adds: even obliterating the distinction between the atelectatic lungs and the heart) What might decrease the risk of RDS: pregnancies with chronic or pregnancy-associated hypertension prolonged rupture of membranes antenatal corticosteroid prophylaxis (Major factor is changing the survival in many patients, and given 2 doses after the age of 24 weeks of gestations, 12 hours apart.) All of this is due to steroid release. If the patient was stressed in uterus, this will lead to excessive steroids production, which will promote the surfactant release. Surfactant is needed most for reducing the surface tension (among other jobs but this is the most important). In utero, the alveoli are filled with fluids and once you are born, you need higher pressure to open the alveoli.
8 Example to understand the idea: A brand new balloon if given to a child to inflate won't do it, but you as an adult can, and if you inflate it, and deflate it and then given it to the child he will be able to inflate it (The hardest is the first time). Now let's take that balloon and fill it with water and then release the water out. The balloon will collapse and even more pressure is needed to open it. This is how the lungs of a newborn are, once the fluid is out, you need higher pressure to open up the alveoli. Surfactant decreases the surface tension, and that aids in breathing and decreases the work needed to open up and start the gas exchange. From Nilson Essentials: Strategies to prevent preterm birth: 1- Maternal cervical cerclage (Treatment for cervical incompetence is a surgical procedure called cervical cerclage, in which the cervix is sewn closed during pregnancy.) 2- Treatment of infections 3- Bed rest 4- Administration of tocolytic medications (anti-contraction medications or labor repressants, like Terbutaline, Indomethacin, Nifedipine, Magnesium sulfate.) Surfactant is made and stored by type 2 pneumocytes. When we want to deliver surfactant, we given exogenously through the endotracheal tube when the patient needs it. The doctor said he won't discuss or talk about the rescue or prophylaxis as they are advanced to our stage. From Nilson Essentials: (Just if you got a question or anything to be in the safe side) If premature delivery is unavoidable, the mother is given betamethasone and thus to the fetus to stimulate fetal lung production of surfactant and this requires multiple doses for at least 24 hours. Complications include: Patent Ductus Arteriosus, Pulmonary Air Leaks, Brunchopulmonary Dysplasia(Chronic Lung Disease), and Retinopathies. The second problem is: Transient Tachypnea of the Newborn: It's a mild and self-limiting disease, due to increased respiratory rate (tachypnea is in the name of the disease after all), no retractions, and there is mild cyanosis. FiO 2 is lower than 0.4, and the baby is usually term infants but product of C/S. Normally when a mother goes into labor,
9 because of uterine contractions, there will be catecholamine release and this will help the resorption of the fluid in the lung, aided by squeezing through the birth canal. Going through C/S will put the baby at risk of having that fluid in the lung and develop transient tachypnea of the newborn. The problem is there is fluids present in the lungs, maternal IV fluids associated. CXR with prominent vascular markings. This X-ray is classical for Transient Tachypnea of the Newborn. From Nilson Essentials: CXR Shows prominent central vascular markings, fluid in lung fissures, overaeration, and occasionally a small pleuaral effusion. You need to rule out pneumonia. We used to put patients on oxygen and antibiotics immediately, but now we wait for about 6 hours, some wait for 24 hours, and if the patient is not responding we start them on antibiotics. But here in the hospital because of the crowdedness, we start at 6 hours. So if the demand on oxygen increased, or oxygen is needed beyond 6 hours, or he/she is not responding, you need to think of another cause. Another disease that might present with cyanosis and respiratory distress:
10 Neonatal Meconium Aspiration Syndrome: We can't prevent all MAS, because the mother might have meconium in the liquor, and when the membrane ruptures, we do suction for perineum, and if the baby didn't breath we do suction through an endotracheal tube. Why does this happen in utero? If the baby has fetal distress or hypoxia, the patient due to hypoxia will have relaxation of the anal sphincter, and the will lead to the passage of the meconium into the amniotic fluid. When the blood supply gets better, gasping happens, and then he/she aspirates the meconium. On Chest X-Ray (CXR): Increased density, irregular infiltrates Areas of hyperexpansion, areas of collapse(due to ball valve mechanism) Fluffy non-homogeneous infiltrates May be hard to distinguish from retained fluid, pneumonia
11 **Notice in the CXR that the particles are bigger than those in RDS. One of the complications of call valve mechanism is that air will keep going into the alveoli and tension increases leading to rupture and pneumothorax, making those patients difficult to ventilate, as they might have PPH (Persistent Pulmonary Hypertension), with right to left shunting caused by increased pulmonary vascular resistance. Comorbid diseases include those associated with in utero asphyxia that initiated the passage of meconium. From Nilson Essentials: Treatment: general supportive care and assisted ventilation. Infants with PPHN should be treated for PPHN. If sever hypoxia doesn't subside with conventional or high frequency ventilation, surfactant therapy, and inhaled nitric oxide, Extracorporeal membrane oxygenation (ECMO) may be beneficial.
12 This part was done by your colleague Ahmad Abbadi.. In memory of Claymore.. My favorite manga and book I have ever read. "My existence was nothing more to her than a stone by the side of the road. I wasn't enough to fill her belly. Or perhaps I didn't even get reflected in her eyes. I couldn't even hate the beast that killed Teresa. It was me, overcome by fear, that I could not forgive." -Clare, Claymore, Scene 24: Marked for Death, Part 7. "Being thrown away by humans, devoted to them even though you aren't one of them... and once they are finished with you, they have you end your life yourself... and not even an ounce of gratitude for all that. On the contrary: for your whole life you are hated and reviled. It really is idiotic. We are a different species after all. Once you start seeing things that way, it all becomes very easy to accept. Do humans shed tears for the birds, pigs, cows and sheep that become their food? Of course they don't. They are a different species after all. That is nature. That is the truth. That is Providence. Your way of thinking up to now was the warped one." -Riful of the West, Claymore, Scene 43: The Witch's Maw, Part 3. To all our friends, thank you for every precious memory.. The best is yet to come :) And Happy Birthday Mohammad Nayef :P Now you can't say that I didn't make it a special Bday Your colleagues: Ahmad Abbadi, Mohammad Nayef.
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
-Tamara Wahbeh. -Razan Abu Rumman. Dr. Mohammed Al-Muhtaseb
 -2 -Tamara Wahbeh -Razan Abu Rumman Dr. Mohammed Al-Muhtaseb I tried to include everything the doctor mentioned in both the lecture and his slides in the simplest way possible, so hopefully there would
-2 -Tamara Wahbeh -Razan Abu Rumman Dr. Mohammed Al-Muhtaseb I tried to include everything the doctor mentioned in both the lecture and his slides in the simplest way possible, so hopefully there would
The Blue Baby. Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin
 The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
 NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
Neonatal Resuscitation. Dustin Coyle, M.D. Anesthesiology
 Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
1st Annual Clinical Simulation Conference
 1st Annual Clinical Simulation Conference Newborns with Acute Respiratory Distress: Diagnosis and Management Ma Teresa C. Ambat, MD Assistant Professor Division of Neonatology, Department of Pediatrics
1st Annual Clinical Simulation Conference Newborns with Acute Respiratory Distress: Diagnosis and Management Ma Teresa C. Ambat, MD Assistant Professor Division of Neonatology, Department of Pediatrics
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
A radiological perspective of assessing neonatal respiratory distress syndrome
 Original Research Article A radiological perspective of assessing neonatal respiratory distress syndrome Jayesh Shah 1, Nikhil Parvatkar 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident,
Original Research Article A radiological perspective of assessing neonatal respiratory distress syndrome Jayesh Shah 1, Nikhil Parvatkar 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident,
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
Presented By : Kamlah Olaimat
 Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Simulation 08: Cyanotic Preterm Infant in Respiratory Distress
 Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Respiratory Disorders in the Newborn: Identification and Diagnosis Hany Aly. DOI: /pir
 Respiratory Disorders in the Newborn: Identification and Diagnosis Hany Aly Pediatr. Rev. 2004;25;201-208 DOI: 10.1542/pir.25-6-201 The online version of this article, along with updated information and
Respiratory Disorders in the Newborn: Identification and Diagnosis Hany Aly Pediatr. Rev. 2004;25;201-208 DOI: 10.1542/pir.25-6-201 The online version of this article, along with updated information and
Surfactant Administration
 Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
1
 1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
Neonatal/Pediatric Cardiopulmonary Care. Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN. Other. Other Diseases
 Neonatal/Pediatric Cardiopulmonary Care Other Diseases Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN 3 Also known as Persistent Fetal Circulation (PFC) Seen most frequently in term, post-term
Neonatal/Pediatric Cardiopulmonary Care Other Diseases Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN 3 Also known as Persistent Fetal Circulation (PFC) Seen most frequently in term, post-term
Pulmonary Problems of the Neonate. Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA
 Pulmonary Problems of the Neonate Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA Lower Respiratory Diseases Ventilation/Perfusion Abnormalities
Pulmonary Problems of the Neonate Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA Lower Respiratory Diseases Ventilation/Perfusion Abnormalities
Screening for Critical Congenital Heart Disease
 Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Kofinas Perinatal Providing Care to the Unborn
 Alexander D. Kofinas, MD Director, Kofinas Perinatal Associate Professor, Clinical Obstetrics and Gynecology Cornell University, College of Medicine Patient instructions for the use of Indomethacin and
Alexander D. Kofinas, MD Director, Kofinas Perinatal Associate Professor, Clinical Obstetrics and Gynecology Cornell University, College of Medicine Patient instructions for the use of Indomethacin and
Neonatal/Pediatric Cardiopulmonary Care
 Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
New Zealand Data Sheet. Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml
 CUROSURF New Zealand Data Sheet Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml Presentation Sterile suspension in single-dose vials for intratracheal or intrabronchial administration.
CUROSURF New Zealand Data Sheet Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml Presentation Sterile suspension in single-dose vials for intratracheal or intrabronchial administration.
INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2
 2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2)
 Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2) - Case 1: a 32 weeks preterm developed RDS 4 hours after delivery. Chest X-ray shows:
Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2) - Case 1: a 32 weeks preterm developed RDS 4 hours after delivery. Chest X-ray shows:
Admission/Discharge Form for Infants Born in Please DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
PUMANI bcpap GUIDELINES FOR CLINICIANS. An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use
 An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
Radiological evaluation of neonatal lesions in 118 neonates
 Original Research Article ISSN: 394-006 (P) Radiological evaluation of neonatal thoracic lesions in 8 neonates Konark Sarvaiya *, Himanshu Singla, Nirav Patel, Jai Inder Dhillon, Babubhai Patel 3 nd year
Original Research Article ISSN: 394-006 (P) Radiological evaluation of neonatal thoracic lesions in 8 neonates Konark Sarvaiya *, Himanshu Singla, Nirav Patel, Jai Inder Dhillon, Babubhai Patel 3 nd year
Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS IN THE NEWBORN
 Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018 Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS
Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018 Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS
The high risk neonate
 The high risk neonate Infant classification by gestational (postmenstrual) age Preterm. Less than 37 completed weeks (259 days). Term. Thirty-seven to 416/7 weeks (260-294 days). Post-term. Forty-two weeks
The high risk neonate Infant classification by gestational (postmenstrual) age Preterm. Less than 37 completed weeks (259 days). Term. Thirty-seven to 416/7 weeks (260-294 days). Post-term. Forty-two weeks
BPD. Neonatal/Pediatric Cardiopulmonary Care. Disease. Bronchopulmonary Dysplasia. Baby Jane
 1 Neonatal/Pediatric Cardiopulmonary Care Disease 2 Bronchopulmonary Dysplasia 3 is a 33-day-old prematurely born girl who weighs 1420 g. At birth, her estimated gestational age was 28 weeks. Her initial
1 Neonatal/Pediatric Cardiopulmonary Care Disease 2 Bronchopulmonary Dysplasia 3 is a 33-day-old prematurely born girl who weighs 1420 g. At birth, her estimated gestational age was 28 weeks. Her initial
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy
 An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
IRDS, Infantile Respiratory Distress Syndrome
 IRDS, Infantile Respiratory Distress Syndrome - RDS is the leading cause of death in the newborns, and the most common cause of death first 15 years of life (excluding the malformed babies). - RDS is the
IRDS, Infantile Respiratory Distress Syndrome - RDS is the leading cause of death in the newborns, and the most common cause of death first 15 years of life (excluding the malformed babies). - RDS is the
Pediatrics. Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test. Definition. See online here
 Pediatrics Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test See online here Blue babies lack sufficient hemoglobin, resulting in the bluish discoloration of tissues, a term referred to as cyanosis.
Pediatrics Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test See online here Blue babies lack sufficient hemoglobin, resulting in the bluish discoloration of tissues, a term referred to as cyanosis.
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Respiratory Management in Pediatrics
 Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
There are four general types of congenital lung disorders:
 Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영
 When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
Apnea in the Newborn
 Apnea in the Newborn Developed by - Lisa Fikac, RNC-NIC, MSN Original Author - Stacey Cashwell, MSN, RN Expiration Date - 1/27/17 This continuing education activity is provided by Cape Fear Valley Health
Apnea in the Newborn Developed by - Lisa Fikac, RNC-NIC, MSN Original Author - Stacey Cashwell, MSN, RN Expiration Date - 1/27/17 This continuing education activity is provided by Cape Fear Valley Health
Karen Corlett, RN, MSN, CPNP-AC/PC Pediatric Nurse Practitioner Congenital Heart Surgery Unit Pediatric Cardiac Intensivists of North Texas Medical
 Karen Corlett, RN, MSN, CPNP-AC/PC Pediatric Nurse Practitioner Congenital Heart Surgery Unit Pediatric Cardiac Intensivists of North Texas Medical City Children s Hospital, Dallas Hypoxia Shortage of
Karen Corlett, RN, MSN, CPNP-AC/PC Pediatric Nurse Practitioner Congenital Heart Surgery Unit Pediatric Cardiac Intensivists of North Texas Medical City Children s Hospital, Dallas Hypoxia Shortage of
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Premature: is live born infants delivered before 37 wk from the 1 st day of the last menstrual period.
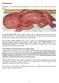 Prematurity Premature: is live born infants delivered before 37 wk from the 1 st day of the last menstrual period. Low birth weight (LBW): (birth weight
Prematurity Premature: is live born infants delivered before 37 wk from the 1 st day of the last menstrual period. Low birth weight (LBW): (birth weight
Shedding Light on Neonatal X-rays. Objectives. Indications for X-Rays 5/14/2018
 Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
TRAINING NEONATOLOGY SILVANA PARIS
 TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
Nitric Resource Manual
 Nitric Resource Manual OBJECTIVES Describe the biologic basis for inhaled nitric oxide therapy Describe the indications for inhaled nitric oxide therapy Describe the potential hazards, side effects and
Nitric Resource Manual OBJECTIVES Describe the biologic basis for inhaled nitric oxide therapy Describe the indications for inhaled nitric oxide therapy Describe the potential hazards, side effects and
ADMISSION/DISCHARGE FORM FOR INFANTS BORN IN 2019 DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 1 Any eligible inborn infant who dies in the delivery room or at any other location in your hospital within 12 hours after birth and prior to admission to the NICU is defined as a "Delivery Room Death."
1 Any eligible inborn infant who dies in the delivery room or at any other location in your hospital within 12 hours after birth and prior to admission to the NICU is defined as a "Delivery Room Death."
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Tracheoesophageal Fistula and Esophageal Atresia
 Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Scope This guideline is aimed at all Health care professionals involved in the care of infants within the Neonatal Service.
 Management of Newborn Infants born through Meconium-stained liquor University Hospitals of Leicester NHS NHS Trust March 2018 March 2021 Scope This guideline is aimed at all Health care professionals involved
Management of Newborn Infants born through Meconium-stained liquor University Hospitals of Leicester NHS NHS Trust March 2018 March 2021 Scope This guideline is aimed at all Health care professionals involved
disease, bronchopulmonary dysplasia, pulmonary hypoplasia and congenital diaphragmatic hernia.
 Neonatal Chest Imaging - What the Nurse Should Know Expires Monday, April 30, 2018 Nursing Michael J. Diament, M.D. Objectives 1. Describe a good technique for positioning a neonate for the purpose of
Neonatal Chest Imaging - What the Nurse Should Know Expires Monday, April 30, 2018 Nursing Michael J. Diament, M.D. Objectives 1. Describe a good technique for positioning a neonate for the purpose of
Uses 1,2,3 : Labeled: Prevention of respiratory distress syndrome in premature infants
 Brand Name: Surfaxin Generic Name: lucinactant Manufacturer 1 : Discovery Laboratories, Inc. Drug Class 2,3 : Synthetic lung surfactant Uses 1,2,3 : Labeled: Prevention of respiratory distress syndrome
Brand Name: Surfaxin Generic Name: lucinactant Manufacturer 1 : Discovery Laboratories, Inc. Drug Class 2,3 : Synthetic lung surfactant Uses 1,2,3 : Labeled: Prevention of respiratory distress syndrome
Tracheal Collapse: Medical Management Versus Implantable Stents
 What is Tracheal Collapse? The trachea (windpipe) is a large tube that is reinforced by cartilage rings. The trachea runs alongside of the esophagus (food pipe) and delivers air to the lungs. Tracheal
What is Tracheal Collapse? The trachea (windpipe) is a large tube that is reinforced by cartilage rings. The trachea runs alongside of the esophagus (food pipe) and delivers air to the lungs. Tracheal
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
Table 1: The major changes in AHA / AAP neonatal resuscitation guidelines2010 compared to previous recommendations in 2005
 Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
How to Recognize a Suspected Cardiac Defect in the Neonate
 Neonatal Nursing Education Brief: How to Recognize a Suspected Cardiac Defect in the Neonate https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Neonatal Nursing Education Brief: How to Recognize a Suspected Cardiac Defect in the Neonate https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) NICU POCKET GUIDE
 Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
From Buds to Branches to Tubes!
 : Respiratory and Ingestive Consequences of Premature Birth 2007 ASHA KAYPentax Lecture Session 1260 JL Miller, Ph.D. National Institutes of Health jmiller@cc.nih.gov From buds to branches to tubes, the
: Respiratory and Ingestive Consequences of Premature Birth 2007 ASHA KAYPentax Lecture Session 1260 JL Miller, Ph.D. National Institutes of Health jmiller@cc.nih.gov From buds to branches to tubes, the
PBL RESPIRATORY SYSTEM DR. NATHEER OBAIDAT
 PBL RESPIRATORY SYSTEM DR. NATHEER OBAIDAT Dr started to talk about his specialty at the hospital which is (ICU-Pulmonary-Internal Medicine). Pulmonary medical branch is a subspecialty of internal medicine.
PBL RESPIRATORY SYSTEM DR. NATHEER OBAIDAT Dr started to talk about his specialty at the hospital which is (ICU-Pulmonary-Internal Medicine). Pulmonary medical branch is a subspecialty of internal medicine.
NEONATOLOGY Healthy newborn. Neonatal sequelaes
 NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
PPHN (see also ECMO guideline)
 Children s Acute Transport Service Clinical Guidelines PPHN (see also ECMO guideline) Document Control Information Author P Brooke E.Randle Author Position Medical Student Consultant Document Owner E.
Children s Acute Transport Service Clinical Guidelines PPHN (see also ECMO guideline) Document Control Information Author P Brooke E.Randle Author Position Medical Student Consultant Document Owner E.
Provide guidelines for the management of mechanical ventilation in infants <34 weeks gestation.
 Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
SUMPh N. Testemitanu Radiology and Medical imaging department PEDIATRIC IMAGING. M. Crivceanschii, assistant professor
 SUMPh N. Testemitanu Radiology and Medical imaging department PEDIATRIC IMAGING M. Crivceanschii, assistant professor GOALS AND OBJECTIVES to be aware of the role of modern diagnostic imaging modalities
SUMPh N. Testemitanu Radiology and Medical imaging department PEDIATRIC IMAGING M. Crivceanschii, assistant professor GOALS AND OBJECTIVES to be aware of the role of modern diagnostic imaging modalities
Practical Application of CPAP
 CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
Transporting Children With Serious Respiratory Illness: A Presentation For Non-Specialty Teams
 Transporting Children With Serious Respiratory Illness: A Presentation For Non-Specialty Teams Laurie Gehrke, R.N., BSN, CPEN, CEN, CMTE Pediatric Transport Team Blank Children s Hospital Des Moines, Iowa
Transporting Children With Serious Respiratory Illness: A Presentation For Non-Specialty Teams Laurie Gehrke, R.N., BSN, CPEN, CEN, CMTE Pediatric Transport Team Blank Children s Hospital Des Moines, Iowa
** SURFACTANT THERAPY**
 ** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
Pitfalls of the Pediatric Chest and Abdomen SPR 2017
 Pitfalls of the Pediatric Chest and Abdomen SPR 2017 Richard I. Markowitz, MD, FACR Children s Hospital of Philadelphia Perelman School of Medicine University of Pennsylvania No Disclosures Cognitive Perceptual
Pitfalls of the Pediatric Chest and Abdomen SPR 2017 Richard I. Markowitz, MD, FACR Children s Hospital of Philadelphia Perelman School of Medicine University of Pennsylvania No Disclosures Cognitive Perceptual
The Turkish Journal of Pediatrics 2014; 56:
 The Turkish Journal of Pediatrics 2014; 56: 232-237 Original INSURE method (INtubation-SURfactant-Extubation) in early and late premature neonates with respiratory distress: factors affecting the outcome
The Turkish Journal of Pediatrics 2014; 56: 232-237 Original INSURE method (INtubation-SURfactant-Extubation) in early and late premature neonates with respiratory distress: factors affecting the outcome
USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014
 USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014 ino for Late Preterm and Term Infants with Severe PPHN Background:
USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014 ino for Late Preterm and Term Infants with Severe PPHN Background:
Research Roundtable Summary
 Research Roundtable Summary 10 TENTH in a Series of Seminars on MCHB-funded Research Projects Early Cortisol Deficiency and Bronchopulmonary Dysplasia October 18, 1995 Parklawn Building Potomac Conference
Research Roundtable Summary 10 TENTH in a Series of Seminars on MCHB-funded Research Projects Early Cortisol Deficiency and Bronchopulmonary Dysplasia October 18, 1995 Parklawn Building Potomac Conference
Acute Respiratory Failure
 Acute Respiratory Failure For family, friends and caregivers of a patient with acute respiratory failure in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information
Acute Respiratory Failure For family, friends and caregivers of a patient with acute respiratory failure in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information
DISEASES OF THE RESPIRATORY SYSTEM 2017 DR HEYAM AWAD LECTURE 1: RESPIRATORY DISTRESS SYNDROMES
 DISEASES OF THE RESPIRATORY SYSTEM 2017 DR HEYAM AWAD LECTURE 1: RESPIRATORY DISTRESS SYNDROMES This lecture covers two topics: neonatal respiratory distress syndrome (neonatal RDS) and adult respiratory
DISEASES OF THE RESPIRATORY SYSTEM 2017 DR HEYAM AWAD LECTURE 1: RESPIRATORY DISTRESS SYNDROMES This lecture covers two topics: neonatal respiratory distress syndrome (neonatal RDS) and adult respiratory
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
Etiological Study of Respiratory Distress in Newborn
 ORIGINAL RESEARCH www.ijcmr.com Etiological Study of P. Brahmaiah 1, K. Rami Reddy 2 ABSTRACT Introduction: Respiratory distress is one of the commonest disorder encountered within the first 48-72 hours
ORIGINAL RESEARCH www.ijcmr.com Etiological Study of P. Brahmaiah 1, K. Rami Reddy 2 ABSTRACT Introduction: Respiratory distress is one of the commonest disorder encountered within the first 48-72 hours
Credential Maintenance Program
 First Quarter of the Calendar 5 I. COMPETENCIES SHARED BETWEEN CRITICAL AND GENERAL CARE 3 7 0 A. Assess Patient Information 0 2 2. Patient history, for example, immunizations environmental pre-existing
First Quarter of the Calendar 5 I. COMPETENCIES SHARED BETWEEN CRITICAL AND GENERAL CARE 3 7 0 A. Assess Patient Information 0 2 2. Patient history, for example, immunizations environmental pre-existing
Chapter 55. Changes in the Airway With COPD. Manifestations of Severe COPD. Drugs Used to Treat Obstructive Pulmonary Disorders
 Chapter 55 Drugs Used to Treat Obstructive Pulmonary Disorders Changes in the Airway With COPD Manifestations of Severe COPD Air is trapped in the lower respiratory tract The alveoli degenerate and fuse
Chapter 55 Drugs Used to Treat Obstructive Pulmonary Disorders Changes in the Airway With COPD Manifestations of Severe COPD Air is trapped in the lower respiratory tract The alveoli degenerate and fuse
X-Plain Lung Cancer Reference Summary
 X-Plain Lung Cancer Reference Summary Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Lung cancer rates among Southeast
X-Plain Lung Cancer Reference Summary Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Lung cancer rates among Southeast
Standard of Newborn Care in the Age of Birth Plans. Stephanie Deal, MD Tiffany McKee-Garrett, MD
 Standard of Newborn Care in the Age of Birth Plans Stephanie Deal, MD Tiffany McKee-Garrett, MD Disclosure We have no relevant financial relationships with the manufacturers(s) of any commercial products(s)
Standard of Newborn Care in the Age of Birth Plans Stephanie Deal, MD Tiffany McKee-Garrett, MD Disclosure We have no relevant financial relationships with the manufacturers(s) of any commercial products(s)
Objectives. Apnea Definition and Pitfalls. Pathophysiology of Apnea. Apnea of Prematurity and hypoxemia episodes 5/18/2015
 Apnea of Prematurity and hypoxemia episodes Deepak Jain MD Care of Sick Newborn Conference May 2015 Objectives Differentiating between apnea and hypoxemia episodes. Pathophysiology Diagnosis of apnea and
Apnea of Prematurity and hypoxemia episodes Deepak Jain MD Care of Sick Newborn Conference May 2015 Objectives Differentiating between apnea and hypoxemia episodes. Pathophysiology Diagnosis of apnea and
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by
 24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
Neonatal Resuscitation
 Neonatal Resuscitation High Risk Deliveries A person trained in neonatal resuscitation is usually called to be present for the following deliveries: 1. Antepartum factors Maternal diabetes Pregnancy induced
Neonatal Resuscitation High Risk Deliveries A person trained in neonatal resuscitation is usually called to be present for the following deliveries: 1. Antepartum factors Maternal diabetes Pregnancy induced
NEONATAL-PERINATAL MEDICINE ROTATION Competency Based Goals and Objectives
 NEONATAL-PERINATAL MEDICINE ROTATION Competency Based Goals and Objectives Competency 1. Patient Care: Provide family centered patient care that is developmentally and age appropriate, compassionate, and
NEONATAL-PERINATAL MEDICINE ROTATION Competency Based Goals and Objectives Competency 1. Patient Care: Provide family centered patient care that is developmentally and age appropriate, compassionate, and
Pediatric Advanced Life Support Overview Judy Haluka BS, RCIS, EMT-P
 Pediatric Advanced Life Support Overview 2006 Judy Haluka BS, RCIS, EMT-P General Our Database is lacking in pediatrics Pediatrics are DIFFERENT than Adults not just smaller The same procedure may require
Pediatric Advanced Life Support Overview 2006 Judy Haluka BS, RCIS, EMT-P General Our Database is lacking in pediatrics Pediatrics are DIFFERENT than Adults not just smaller The same procedure may require
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA
 GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
HelmiLubis, RidwanMuchtarDaulay, WismanDalimunthe, Rini Savitri Daulay
 Congenital Malformation of the Lung and Airways HelmiLubis, RidwanMuchtarDaulay, WismanDalimunthe, Rini Savitri Daulay DivisiRespirologiDepartemenIlmuKesehatanAnak FakultasKedokteran Universitas Sumatera
Congenital Malformation of the Lung and Airways HelmiLubis, RidwanMuchtarDaulay, WismanDalimunthe, Rini Savitri Daulay DivisiRespirologiDepartemenIlmuKesehatanAnak FakultasKedokteran Universitas Sumatera
Neonatal Resuscitation in What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011
 Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
Long-gap Oesophageal Atresia
 Long-gap Atresia A guide for parents Nate (6 weeks old) Atresia Research Association Are there different types of OA? There are four main types of oesophageal atresia with or without TOF. These include
Long-gap Atresia A guide for parents Nate (6 weeks old) Atresia Research Association Are there different types of OA? There are four main types of oesophageal atresia with or without TOF. These include
PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني
 Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
PEDIATRIC RESPIRATORY ILLNESS MADE SIMPLE
 Copyright 2012 Joel Berezow, MD and The Pediatrics for Emergency Physicians Network All rights reserved. Duplication in whole or in part, or electronic transmission in any form, is prohibited THE PEDIATRICS
Copyright 2012 Joel Berezow, MD and The Pediatrics for Emergency Physicians Network All rights reserved. Duplication in whole or in part, or electronic transmission in any form, is prohibited THE PEDIATRICS
By Dr.Asmaa Al sanjary
 By Dr.Asmaa Al sanjary Preterm delivery is defined by a birth occurring before 37 completed weeks of gestation. Prematurity is multifactorial and its incidence has increased during the last decade in most
By Dr.Asmaa Al sanjary Preterm delivery is defined by a birth occurring before 37 completed weeks of gestation. Prematurity is multifactorial and its incidence has increased during the last decade in most
