MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION
|
|
|
- Shanna Curtis
- 5 years ago
- Views:
Transcription
1 CLINICAL POLICY MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION DOCUMENT REF: PCLASCORD (Version No. 1.4) Name and designation of policy author(s) Approved by (committee, group, manager) Kate Parker-Metastatic Spinal Cord Compression Coordinator Dr. Peter Robson - Consultant Clinical Oncologist and Joint Network Lead for MSCC Dr. Peter Robson - Consultant Clinical Oncologist and Joint Network Lead for MSCC Approving signature Date approved Review date Review type (annual, three yearly) Target audience Links to other strategies, policies, procedures Protective Marking Classification Electronic approval received 5 th October 2018 October 2021 Three yearly Clinical staff Metastatic Spinal Cord Compression Pathway Guidelines for Cheshire and Merseyside (GCLAMSCC) Internal This document replaces V1.3 Issue Date: 5 th October 2018 Page 1 of 10 Filename: PCLASCORD Issue No: 1.4
2 Consultation: Impact Assessment Dee-Anne Bentley Document Control Manager Fraud Assessment Authorised by Date Authorised Comments 11 th September 2012 No requirement for full impact assessment N/A N/A N/A Circulation/Dissemination: Date added into Q-Pulse 9 th October 2018 Date notice posted in the Team Brief 9 th October 2018 Date document posted on the intranet 9 th October 2018 Version History: Date Version Author name and designation Summary of main changes Dr. Peter Robson - Consultant First version. 1.0 Clinical Oncologist and Joint Network Lead for MSCC June 2012 July February Dr. Peter Robson - Consultant Clinical Oncologist and Joint Network Lead for MSCC Dr. Peter Robson - Consultant Clinical Oncologist and Joint Network Lead for MSCC July Dr. Peter Robson - Consultant Clinical Oncologist and Joint Network Lead for MSCC Kate Parker-Metastatic Spinal Cord Compression Co-ordinator October Dr. Peter Robson - Consultant Clinical Oncologist and Joint Network Lead for MSCC Scheduled review Due to the ongoing implementation of a CCC network coordinator post, the new post holder will be involved in updating this document with Dr. Robson. Current content of policy is still relevant. Review date to be extended for a further 4 months. Scheduled review from July Current content still valid. A new Network Co-ordinator has been appointed full review will take place in 6 months. Small changes to reflect updates to network guidance issued in December 17. One change to section 7.1, point 4 to describe how referrals are made into CCC in absence of MSCC co-ordinator (i.e. leave or out of hours) Issue Date: 5 th October 2018 Page 2 of 10 Filename: PCLASCORD Issue No: 1.4
3 1.0 Introduction In November 2008 the National Institute for Health and Clinical Excellence (NICE) published guideline CG75 (Metastatic spinal cord compression: diagnosis and management of adults at risk of and with metastatic spinal cord compression (1)). In response to this the Merseyside and Cheshire Cancer Network (MCCN) formed the Metastatic Spinal Cord Compression (MSCC) Group that reports directly to the Non-Surgical Oncology Group (NSOG). In September 2010 this group published guidelines on the management and treatment of this group of patients in our region (2). The latest version of these guidelines was issued in December The group has also published Primary care network guidance for this condition and a patient information sheet to be given to those patients at greatest risk of developing the condition (3). As part of this body of work policies are being written for the management of patients with MSCC within The Walton Centre for Neurology and Neurosurgery NHSFT (Walton) and The Clatterbridge Cancer Centre NHSFT (CCC). 2.0 Purpose The aim of this policy is to define the management of patients who have been diagnosed with MSCC and are admitted to CCC for treatment with palliative radiotherapy. The intended outcomes are to streamline the treatment and rehabilitation process leading to the patients being mobilized and discharged or transferred back to the referring or local hospital in a timely fashion following completion of radiotherapy (as recommended in NICE GC75). This policy will lead to less complications associated with extended bed rest (e.g. chest infections, pulmonary emboli, poor mobility) and allow patients to be transferred back to a local facility more readily. Issue Date: 5 th October 2018 Page 3 of 10 Filename: PCLASCORD Issue No: 1.4
4 3.0 Scope This guidance is intended to apply to all patients receiving palliative radiotherapy for MSCC or impending cord compression at CCC. This does not apply to patients treated with radiotherapy following a surgical decompression. 4.0 Responsibilities This policy is the responsibility of the Network MSCC leads and will be audited by the MSCC network group. 5.0 Laws & Regulations None applicable 6.0 Definitions None applicable 7.0 Main Body of Policy 7.1 Network Guidance for management prior to admission to CCC Following the publication of the MSCC guidelines by the Network in September 2010 the following are now in place; 1. Patients at high risk of developing MSCC are to be given written and verbal information about the condition (Breast, Lung, Prostate and Myeloma). 2. Patients presenting with red flag symptoms but no neurology will have a whole spine MRI within 1 week. 3. Patients with neurological signs or symptoms are admitted to their local hospital, put on bed rest, given Dexamethasone 16mg and have a full spine MRI within 24 hours. 4. Confirmed cases of MSCC/impending MSCC are referred directly to Clatterbridge MSCC Coordinator via the Network referral pathway. During Issue Date: 5 th October 2018 Page 4 of 10 Filename: PCLASCORD Issue No: 1.4
5 leave or out of hours this information will be collected via Triage (CCC Hotline) and passed to the on-call team. 5. The Clinical Oncologist assesses which patients require a surgical opinion (based on symptoms, extent of disease, fitness) 6. A case discussion if required is held between the Consultant spinal surgeon and the Consultant oncologist (and if required a Consultant radiologist). A decision is made about the most appropriate management. 7. Patients are transferred to the appropriate hospital for treatment. 8. Prior to transfer, patients with instability pain who are unsuitable for surgical intervention should be fitted with an appropriate brace. 9. Patient information leaflet should be provided and management guidelines should be clearly documented. 7.2 Management following acceptance for treatment at CCC On acceptance by our hospital the patient should be transferred rapidly to CCC to allow treatment within 24 hours of the diagnosis of MSCC being made on MRI. Patients will be planned urgently by their own team (if available) or the on call team. Planning and treatment should be undertaken at the weekends and on Bank Holidays. Radiotherapy fractionation will depend on the tumour type, the stage of presentation and the neurological status of the patient; 1. A single 8Gy fraction is appropriate for pain relief in patients who have had no neurological function for >48 hours (these patients should ideally be transferred back to the referring hospital on the same day). 2. Palliative treatment 8Gy single or 20Gy/5# at depth is standard for most cases of MSCC Gy/10# at depth is sometimes used in patients with a better prognosis. 4. Radical treatments may be considered in certain circumstances (e.g. plasmacytoma). Issue Date: 5 th October 2018 Page 5 of 10 Filename: PCLASCORD Issue No: 1.4
6 On admission to the ward at CCC patients should; 1. Be maintained in a flat position (or at an angle if medically unable to lie flat). 2. Receive planning and treatment with palliative radiotherapy. 3. Commence or continue on Dexamethasone 16mg daily with a proton pump inhibitor. 4. Commence low molecular weight heparin (unless contraindicated). 5. Full medical admission with neurological assessment and documentation of function, continence and pain. 6. The outcome of any surgical discussion should be documented in the medical notes. 7. Full nursing, nutritional and venous thrombo-embolism assessment with anti-embolism stockings (documentation of level of function, continence and pain). 8. Referral to palliative care team if appropriate. 9. Do Not Resuscitate assessment if appropriate. 10. MDT Discharge planning should commence on admission with an aim to discharge home or transfer back to the appropriate location on completion of treatment. 11. Further investigation should be considered if appropriate for staging or diagnosis of an unknown primary (e.g. CT scan/ blood tests) biopsy may be more appropriate to do after referral back to the local hospital. 12. Further treatment may be added if appropriate (e.g. hormones/ zoledronic acid). In certain circumstances (e.g. the fit patient with no neurological deficit) the Consultant may decide that bed rest and high dose steroids are not required. This should be documented clearly in the notes. Issue Date: 5 th October 2018 Page 6 of 10 Filename: PCLASCORD Issue No: 1.4
7 7.4 Rehabilitation and discharge After commencement of radiotherapy patients continue on bed rest and 16mg Dexamethasone until completion of the 2 nd fraction of treatment. The patient should receive bed exercises (active or passive depending on functional state). Following the second fraction of radiotherapy further treatment depends upon the neurological status of the patient; 1. No neurological deficit (e.g. incidental finding on MRI) a. bed exercises b. Allow to sit up and gradually mobilize using the mobilization pathway (page 10) over a 24 hour period. c. Reduce steroids by a half every 2 days (aim to discharge home on 2mg daily for the next week). d. Stop LMWH and anti-embolism stockings once mobile. e. Referral Physiotherapy and Occupational Therapy (OT) if patient function indicates. 2. Intermediate patients a. Refer to Physiotherapy/OT and follow the mobilization pathway (page 10). b. Continue bed exercises. c. Reduce steroids by half every 2 days (aim to discharge home on 2mg daily for the next week). d. Stop LMWH and anti-embolism stockings once mobile. 3. Complete neurological loss (no power or sensation) a. Refer to physiotherapy/ot to help guide through change in function. b. Allow to sit up gradually to 45 degrees if comfortable. c. Continue bed exercises. Issue Date: 5 th October 2018 Page 7 of 10 Filename: PCLASCORD Issue No: 1.4
8 d. Reduce steroids rapidly over next 3 days. Any patients who experience increased pain or neurological deterioration on mobilization should be returned to lying flat and be reviewed by the medical team. Patients who experience instability pain should be assessed and fitted with an appropriate brace by the appliance department. These patients should then be mobilized to the point where they remain comfortable. Issue Date: 5 th October 2018 Page 8 of 10 Filename: PCLASCORD Issue No: 1.4
9 7.5 Mobilization pathway for patients with MSCC - To mobilise within pain limitations - If significant increase in pain, or changes in neurological symptoms then go back to Box A Day bed rest A - bed exercises (active/ assisted or passive) Day 3 - Gradually sit to 45 degrees - assess neurology, obs/mews, pain over a 24 hour period Does the patient have any new neurological/ functional deficits or significant increase in pain? Yes No Lie flat and go back to Box A Continue to gradual sitting (up to 90 degrees) Does the patient have any new neurological/ functional deficits or significant increase in pain? Yes No Continue to unsupported sitting, transferring and mobilising as symptoms allow IF SIGNIFICANT INCREASE IN PAIN, OR CHANGES IN NEUROLOGICAL SYMPTOMS THEN GO BACK TO BOX A AND REVIEW BY MEDICAL TEAM If significant mechanical pain consider a brace/support Issue Date: 5 th October 2018 Page 9 of 10 Filename: PCLASCORD Issue No: 1.4
10 8.0 Audit Management of patients with MSCC is audited by the MCCN MSCC group. Audits of the process from diagnosis to management are performed on a yearly basis. Audit of treatments and outcomes of patients at all treatment centres are presented at the biannual MSCC collaborative case review meeting. Results of these audits are presented to the MCCN Non-Surgical Oncology Group. The MSCC group is also subject to Peer review as part of the Acute Oncology measures (4). 9.0 References 9.1 Internet 1. NICE guidance MSCC Pathway Guidelines for Cheshire and Merseyside December MCCN MSCC Primary Care Network Guidance Care_Network_Guideline_Version_1.1.pdf 9.2 Publications National Cancer Peer Review Programme. Evidence Guide for: Trusts Acute Oncology. Issue Date: 5 th October 2018 Page 10 of 10 Filename: PCLASCORD Issue No: 1.4
Update on Management of Malignant Spinal Cord Compression. Heino Hugel Consultant in Palliative Medicine University Hospital Aintree
 Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
CP80 Version: V01. Acute Oncology Management Service Date approved: 8 th May 2015 Date ratified: 1 st June 2015 Review date: 1 st June 2017
 STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
PATHWAY MANAGEMENT OF METASTATIC SPINAL CORD COMPRESSION (MSCC) THE CHRISTIE, GREATER MANCHESTER & CHESHIRE
 PATHWAY MANAGEMENT OF METASTATIC SPINAL CORD COMPRESSION (MSCC) THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V3 MSCC Network
PATHWAY MANAGEMENT OF METASTATIC SPINAL CORD COMPRESSION (MSCC) THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V3 MSCC Network
Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway
 Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway Version 2: May 2012 To be read in conjunction with NICE CG75 Developed by consensus by: Dr Peter Robson, Consultant Oncologist,
Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway Version 2: May 2012 To be read in conjunction with NICE CG75 Developed by consensus by: Dr Peter Robson, Consultant Oncologist,
Recognition & Treatment of Malignant Spinal Cord Compression Study Day
 Recognition & Treatment of Malignant Spinal Cord Compression Study Day 11 th May 2017 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk Clinical
Recognition & Treatment of Malignant Spinal Cord Compression Study Day 11 th May 2017 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk Clinical
GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. Version:
 GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V4 Acute Oncology Group
GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V4 Acute Oncology Group
Palliative Care Emergencies
 Palliative Care Emergencies LAURA BARNFIELD What might constitute an emergency in Palliative Care? 1 Palliative Care Emergencies Major haemorrhage Metastatic Spinal Cord Compression (MSCC) Superior Vena
Palliative Care Emergencies LAURA BARNFIELD What might constitute an emergency in Palliative Care? 1 Palliative Care Emergencies Major haemorrhage Metastatic Spinal Cord Compression (MSCC) Superior Vena
Malignant Spinal Cord Compression (MSCC) Clinical Advisor Coordinator
 Malignant Spinal Cord Compression (MSCC) Clinical Advisor Coordinator Induction Training 2016 Version Control This is a controlled document please destroy all previous versions on receipt of a new version.
Malignant Spinal Cord Compression (MSCC) Clinical Advisor Coordinator Induction Training 2016 Version Control This is a controlled document please destroy all previous versions on receipt of a new version.
Metastatic Spinal Disease
 Metastatic Spinal Disease Mr Neil Chiverton Consultant Spinal Surgeon, Sheffield Objectives The scale and nature of the problem NICE recommendations Surgical decision making Case illustrations Incidence
Metastatic Spinal Disease Mr Neil Chiverton Consultant Spinal Surgeon, Sheffield Objectives The scale and nature of the problem NICE recommendations Surgical decision making Case illustrations Incidence
Acute Oncology Induction Training Specification
 Acute Oncology Induction Training Specification Author: Acute Oncology/Cancer of Unknown Primary Clinical Network Group (AO/CUP CNG) V. 2.0 Agreed: 30.11.2012 Reviewed: May 2015 Review : May 2016 MCCN
Acute Oncology Induction Training Specification Author: Acute Oncology/Cancer of Unknown Primary Clinical Network Group (AO/CUP CNG) V. 2.0 Agreed: 30.11.2012 Reviewed: May 2015 Review : May 2016 MCCN
MSCC CARE PATHWAYS & CASE STUDIES. By Michael Balloch Spine CNS
 MSCC CARE PATHWAYS & CASE STUDIES By Michael Balloch Spine CNS Aims To be familiar with the routes of MSCC prentaion How the guidelines work in practice Routes of presentation Generic intervention Managing
MSCC CARE PATHWAYS & CASE STUDIES By Michael Balloch Spine CNS Aims To be familiar with the routes of MSCC prentaion How the guidelines work in practice Routes of presentation Generic intervention Managing
LCA Lung Clinical Forum. 21 st October 2014
 LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
Management of Acute Oncological emergencies
 Management of Acute Oncological emergencies Malignant Spinal cord compression (MSCC) Neutropenic sepsis Superior vena caval obstruction Hypercalcemia Hyponatremia Bowel obstruction Brain Metastasis with
Management of Acute Oncological emergencies Malignant Spinal cord compression (MSCC) Neutropenic sepsis Superior vena caval obstruction Hypercalcemia Hyponatremia Bowel obstruction Brain Metastasis with
agreed MSCC pathways and guidelines).
 Referral of Patients with Spinal Metastatic Disease and Suspected Metastatic Spinal Cord Compression (to be used in association with locally West Midlands Clinical Networks and Clinical Senate Coversheet
Referral of Patients with Spinal Metastatic Disease and Suspected Metastatic Spinal Cord Compression (to be used in association with locally West Midlands Clinical Networks and Clinical Senate Coversheet
Spinal cord compression
 Spinal cord compression Urology Department Patient Information Leaflet Introduction If you have been diagnosed with cancer, you need to know about spinal cord compression and the warning signs. This leaflet
Spinal cord compression Urology Department Patient Information Leaflet Introduction If you have been diagnosed with cancer, you need to know about spinal cord compression and the warning signs. This leaflet
Spinal cord compression: what it means and how it can be treated
 Spinal cord compression: what it means and how it can be treated Patient Information Oncology Department Author ID: Acute Oncology Nurse Specialist Leaflet Number: CC 036 Version: 2.1 Name of Leaflet:
Spinal cord compression: what it means and how it can be treated Patient Information Oncology Department Author ID: Acute Oncology Nurse Specialist Leaflet Number: CC 036 Version: 2.1 Name of Leaflet:
Acute Oncology Services Clinical Forum: Metastatic Spinal Cord Compression. Tuesday 17 th September 2013
 Acute Oncology Services Clinical Forum: Metastatic Spinal Cord Compression Tuesday 17 th September 2013 Welcome, Introduction and Aims of the Event Dr Tom Newsom-Davis, LCA AOS Pathway Chair Why MSCC?
Acute Oncology Services Clinical Forum: Metastatic Spinal Cord Compression Tuesday 17 th September 2013 Welcome, Introduction and Aims of the Event Dr Tom Newsom-Davis, LCA AOS Pathway Chair Why MSCC?
Developing spinal cord compression care guidelines at WPH
 Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Dr Bernie Foran, Suzanne Hodson, Liz Kirkham, Rebecca Mills, Jan Siddall, Rebecca Walsh,
Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Dr Bernie Foran, Suzanne Hodson, Liz Kirkham, Rebecca Mills, Jan Siddall, Rebecca Walsh,
Metastatic Spinal Cord Compression
 Metastatic Spinal Cord Compression Dr Zacharias Tasigiannopoulos Clinical Oncologist Colney centre Department of Oncology Norwich, UK Introduction 2-5% of cancer patients have an episode of MSCC Initial
Metastatic Spinal Cord Compression Dr Zacharias Tasigiannopoulos Clinical Oncologist Colney centre Department of Oncology Norwich, UK Introduction 2-5% of cancer patients have an episode of MSCC Initial
Recognition & Treatment of Malignant Spinal Cord Compression Study Day
 Recognition & Treatment of Malignant Spinal Cord Compression Study Day 16 th October 2014 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk
Recognition & Treatment of Malignant Spinal Cord Compression Study Day 16 th October 2014 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk
Guidelines for the Management. Malignant Spinal Cord Compression. Final Guideline
 Guidelines for the Management Of Malignant Spinal Cord Compression Final Guideline 1. Introduction 1.1 Aetiology of MSCC 1.2 Use of the guidelines 2. Summary of Pathway 2.1 Algorithms 2.2 Role of the MSCC
Guidelines for the Management Of Malignant Spinal Cord Compression Final Guideline 1. Introduction 1.1 Aetiology of MSCC 1.2 Use of the guidelines 2. Summary of Pathway 2.1 Algorithms 2.2 Role of the MSCC
Suspected spinal cord compression form
 Suspected spinal cord compression form Enter this form into the notes at the appropriate date in the Progress / Evaluation sheets. Please copy this form to Lisa Lewis, Medical PA (ext 4551), for audit
Suspected spinal cord compression form Enter this form into the notes at the appropriate date in the Progress / Evaluation sheets. Please copy this form to Lisa Lewis, Medical PA (ext 4551), for audit
Vertebroplasty. Radiology Department. Patient information leaflet
 Vertebroplasty Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a vertebroplasty. It explains what is involved and the possible risks. The benefits
Vertebroplasty Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a vertebroplasty. It explains what is involved and the possible risks. The benefits
(i) This FAQ does not deal with clinical issues (eg What is the definition of a stroke unit? or
 STROKE INTEGRATED PERFORMANCE MEASURE RETURN (IPMR) FREQUENTLY ASKED QUESTIONS (FAQ) Prepared by NHS North West, Lancashire & Cumbria Cardiac & Stroke Network, Cheshire and Merseyside Clinical Networks
STROKE INTEGRATED PERFORMANCE MEASURE RETURN (IPMR) FREQUENTLY ASKED QUESTIONS (FAQ) Prepared by NHS North West, Lancashire & Cumbria Cardiac & Stroke Network, Cheshire and Merseyside Clinical Networks
Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH
 Document Control Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH Author Author s job title Consultant T&O Directorate Scheduled Care Department
Document Control Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH Author Author s job title Consultant T&O Directorate Scheduled Care Department
Cancer of Unknown Primary (CUP) Protocol
 1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
Developing spinal cord compression care guidelines at WPH
 Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Bernie Foran, Suzanne Hodson, Jane Mason, Rebecca Mills, Jan Siddall, Rebecca Walsh, Clare
Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Bernie Foran, Suzanne Hodson, Jane Mason, Rebecca Mills, Jan Siddall, Rebecca Walsh, Clare
National Optimal Lung Cancer Pathway
 National Optimal Lung Cancer Pathway This document was produced by the Lung Clinical Expert Group 2017 Document Title: National Optimal Lung Cancer Pathway and Implementation Guide Date of issue: August
National Optimal Lung Cancer Pathway This document was produced by the Lung Clinical Expert Group 2017 Document Title: National Optimal Lung Cancer Pathway and Implementation Guide Date of issue: August
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Oncologic Emergencies: When to call the Radiation Oncologist
 Oncologic Emergencies: When to call the Radiation Oncologist Dr. Shrinivas Rathod Radiation Oncologist Radiation Oncology Program CancerCare Manitoba and University of Manitoba Disclosures Speaker s name:
Oncologic Emergencies: When to call the Radiation Oncologist Dr. Shrinivas Rathod Radiation Oncologist Radiation Oncology Program CancerCare Manitoba and University of Manitoba Disclosures Speaker s name:
NICE BULLETIN Diagnosis & treatment of prostate cancer
 Diagnosis & treatment of prostate cancer NICE provided the content for this booklet which is independent of any company or product advertised Diagnosis and treatment of prostate cancer Introduction In
Diagnosis & treatment of prostate cancer NICE provided the content for this booklet which is independent of any company or product advertised Diagnosis and treatment of prostate cancer Introduction In
Falls The Assessment, Prevention and Management of Patient Falls (Adult Services) 1.34
 SECTION: 1 PATIENT CARE Including Physical Healthcare POLICY /PROCEDURE: 1.34 NATURE AND SCOPE: SUBJECT (Title): POLICY AND PROCEDURE - TRUST WIDE FALLS: THE ASSESSMENT, PREVENTION AND MANAGEMENT OF PATIENT
SECTION: 1 PATIENT CARE Including Physical Healthcare POLICY /PROCEDURE: 1.34 NATURE AND SCOPE: SUBJECT (Title): POLICY AND PROCEDURE - TRUST WIDE FALLS: THE ASSESSMENT, PREVENTION AND MANAGEMENT OF PATIENT
NICE National Institute for Health and Clinical Excellence Metastic Spinal Cord Compression
 NICE - Metastic Spinal Cord Compression 26/11/2008 (Livello 2) NICE National Institute for Health and Clinical Excellence Metastic Spinal Cord Compression Documento Documento Documento Documento file:///c
NICE - Metastic Spinal Cord Compression 26/11/2008 (Livello 2) NICE National Institute for Health and Clinical Excellence Metastic Spinal Cord Compression Documento Documento Documento Documento file:///c
Spinal Cord Compression Diagnosis and Management. Information for Shared Care Centres and Community Staff
 Reference: CG1412 Written by: Dr Daniel Yeomanson Peer reviewer Dr Jeanette Payne Approved: August 2016 Approved by D&TC: 10 th June 2016 Review Due: August 2019 Intended Audience This document contains
Reference: CG1412 Written by: Dr Daniel Yeomanson Peer reviewer Dr Jeanette Payne Approved: August 2016 Approved by D&TC: 10 th June 2016 Review Due: August 2019 Intended Audience This document contains
Recognition & Treatment of Malignant Spinal Cord Compression
 Recognition & Treatment of Malignant Spinal Cord Compression Acute Oncology Study Day 15 th March 2018 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Yorkshire & the Humber Weston
Recognition & Treatment of Malignant Spinal Cord Compression Acute Oncology Study Day 15 th March 2018 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Yorkshire & the Humber Weston
Acute Oncology Martin Eatock Consultant Medical Oncologist NICaN Medical Director
 Acute Oncology 2014 Martin Eatock Consultant Medical Oncologist NICaN Medical Director Patients admitted with cancer have a longer than average stay Berger et al. Clin Medicine (2013) Questions If your
Acute Oncology 2014 Martin Eatock Consultant Medical Oncologist NICaN Medical Director Patients admitted with cancer have a longer than average stay Berger et al. Clin Medicine (2013) Questions If your
Red Flags for serious spinal pathology: A collaborative approach
 Red Flags for serious spinal pathology: A collaborative approach Professor James Selfe DSc, PhD, MA, GD Phys (Distinction), FCSP Serious Spinal Pathology Background Collaboration Communication Solutions
Red Flags for serious spinal pathology: A collaborative approach Professor James Selfe DSc, PhD, MA, GD Phys (Distinction), FCSP Serious Spinal Pathology Background Collaboration Communication Solutions
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Protocol for emergency surgical intervention in patients with a brain tumour v3
 Protocol for emergency surgical intervention in patients with a brain tumour v3 West Midlands Cancer Alliance Coversheet for Cancer Alliance Expert Advisory Group Agreed Documentation This sheet is to
Protocol for emergency surgical intervention in patients with a brain tumour v3 West Midlands Cancer Alliance Coversheet for Cancer Alliance Expert Advisory Group Agreed Documentation This sheet is to
Disclosures. Disclosures 27/01/2019. Modern approach and pitfalls in metastatic spine surgery. None.. Jeremy Reynolds
 Modern approach and pitfalls in metastatic spine surgery Jeremy Reynolds Spine Lead Oxford Bone and Soft Tissue Sarcoma Service MSCC Lead Thames Valley Cancer Network Clinical Lead Oxford Spine 1 Disclosures
Modern approach and pitfalls in metastatic spine surgery Jeremy Reynolds Spine Lead Oxford Bone and Soft Tissue Sarcoma Service MSCC Lead Thames Valley Cancer Network Clinical Lead Oxford Spine 1 Disclosures
Brain Tumour Scoping project
 Brain Tumour Scoping project 2012-13 Kim Ainsworth, AHP Lead, North London Cancer Network Louise Platt, Therapy Team Lead Neurosurgery, NHNN Sharon Cavanagh, LWBC Lead, Living with and Beyond Cancer Quick
Brain Tumour Scoping project 2012-13 Kim Ainsworth, AHP Lead, North London Cancer Network Louise Platt, Therapy Team Lead Neurosurgery, NHNN Sharon Cavanagh, LWBC Lead, Living with and Beyond Cancer Quick
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice Review of Clinical Guideline (CG75) Metastatic spinal cord compression: diagnosis and management of adults at risk of
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice Review of Clinical Guideline (CG75) Metastatic spinal cord compression: diagnosis and management of adults at risk of
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
Please make sure that you complete a self-assessment survey for each type of rehab program that your organization provides.
 Oncology Rehab s Framework Self-Assessment Tool Inpatient Rehab Survey for Oncology Rehab INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered in many different settings
Oncology Rehab s Framework Self-Assessment Tool Inpatient Rehab Survey for Oncology Rehab INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered in many different settings
Author(s) Approval date: 12/05/16. Committee. June Operational Date: Review: Version No. 1.1 Supercedes 1.0 Links to other policies
 Reference No: Title: Author(s) Ownership: Approval by: Operational Date: Systemic Anti-Cancer Therapy (SACT) Guidelines for Peritoneal Mesothelioma Professor Richard Wilson (Consultant/Chair in Cancer
Reference No: Title: Author(s) Ownership: Approval by: Operational Date: Systemic Anti-Cancer Therapy (SACT) Guidelines for Peritoneal Mesothelioma Professor Richard Wilson (Consultant/Chair in Cancer
CANCER REHABILITATION PATHWAY - HAEMATOLOGY
 CANCER REHABILITATION PATHWAY - HAEMATOLOGY Statement: To be used in conjunction with Brain and CNS Rehabilitation Care Pathway as appropriate Diagnosis and Care Planning: The following symptom pathways
CANCER REHABILITATION PATHWAY - HAEMATOLOGY Statement: To be used in conjunction with Brain and CNS Rehabilitation Care Pathway as appropriate Diagnosis and Care Planning: The following symptom pathways
What is Acute Oncology? Kay McCallum Acute Oncology Advanced Nurse Practitioner John Radcliffe Hospital Oxford September 2015
 What is Acute Oncology? Kay McCallum Acute Oncology Advanced Nurse Practitioner John Radcliffe Hospital Oxford September 2015 What is Acute Oncology? Outline of Talk Concept of Acute Oncology Service (AOS)
What is Acute Oncology? Kay McCallum Acute Oncology Advanced Nurse Practitioner John Radcliffe Hospital Oxford September 2015 What is Acute Oncology? Outline of Talk Concept of Acute Oncology Service (AOS)
BRIEFING PAPER THE USE OF RED FLAGS TO IDENTIFY SERIOUS SPINAL PATHOLOGY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. Version:
 BRIEFING PAPER THE USE OF RED FLAGS TO IDENTIFY SERIOUS SPINAL PATHOLOGY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Jackie Turnpenney Version: Accountable Committee:
BRIEFING PAPER THE USE OF RED FLAGS TO IDENTIFY SERIOUS SPINAL PATHOLOGY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Jackie Turnpenney Version: Accountable Committee:
Cancer Services Position & Recovery Plan June 2015
 Appendix 6 Cancer Services Position & Recovery Plan June 2015 Introduction The Trust is required to achieve 85% compliance for patients on a 62 day pathway from the referral date to the date they receive
Appendix 6 Cancer Services Position & Recovery Plan June 2015 Introduction The Trust is required to achieve 85% compliance for patients on a 62 day pathway from the referral date to the date they receive
Acute Oncology. Protocols & Competencies Acute Oncology Introduction
 Acute Oncology Protocols & Competencies Acute Oncology Introduction Acute Oncology elearning Module Throughout the Acute Oncology FACTS elearning courses you will be able to access Network Protocols by
Acute Oncology Protocols & Competencies Acute Oncology Introduction Acute Oncology elearning Module Throughout the Acute Oncology FACTS elearning courses you will be able to access Network Protocols by
Appendix 4 Urology Care Pathways
 Appendix 4 Urology Care Pathways Cancer Care Pathways outline the steps and stages in the patient journey from referral through to diagnostics, staging, treatment, follow up, rehabilitation and if applicable
Appendix 4 Urology Care Pathways Cancer Care Pathways outline the steps and stages in the patient journey from referral through to diagnostics, staging, treatment, follow up, rehabilitation and if applicable
National Cancer Action Team. Rehabilitation Care Pathway Poor Mobility and Loss of Function
 National Cancer Action Team Rehabilitation Care Pathway Poor Mobility and Loss of Function Diagnosis & Care Planning Assess respiratory status especially in people with preexisting respiratory disease
National Cancer Action Team Rehabilitation Care Pathway Poor Mobility and Loss of Function Diagnosis & Care Planning Assess respiratory status especially in people with preexisting respiratory disease
Palliative treatments for lung cancer: What can the oncologist do?
 Palliative treatments for lung cancer: What can the oncologist do? Neil Bayman Consultant Clinical Oncologist GM Cancer Palliative Care and Lung Cancer Education Event Manchester, 31 st January 2017 Most
Palliative treatments for lung cancer: What can the oncologist do? Neil Bayman Consultant Clinical Oncologist GM Cancer Palliative Care and Lung Cancer Education Event Manchester, 31 st January 2017 Most
Guideline for the Identification and Management of Delirium (Including use of the THINK DELIRIUM Support Tool)
 Guideline for the Identification and Management of Delirium (Including use of the THINK DELIRIUM Support Tool) B27/2009 1. Introduction 1.1 Delirium is a common problem which occurs in about 15-20 out
Guideline for the Identification and Management of Delirium (Including use of the THINK DELIRIUM Support Tool) B27/2009 1. Introduction 1.1 Delirium is a common problem which occurs in about 15-20 out
Cervical laminectomy for spinal cord compression. Information for patients Neurosurgery
 Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician GMCN ROYAL WOLVERHAMPTON HOSPITALS The Royal Wolverhampton Hospitals Trust Lung MDT (11-2C-1) - 2011/12 Dr Angela Morgan
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician GMCN ROYAL WOLVERHAMPTON HOSPITALS The Royal Wolverhampton Hospitals Trust Lung MDT (11-2C-1) - 2011/12 Dr Angela Morgan
Bladder Cancer Guidelines
 Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
A Best Practice Clinical Care Pathway for Major Amputation Surgery
 A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
GUIDELINES FOR THE DIAGNOSIS AND MANAGEMENT OF ADULTS AT RISK OF AND WITH METASTATIC SPINAL CORD COMPRESSION
 GUIDELINES FOR THE DIAGNOSIS AND MANAGEMENT OF ADULTS AT RISK OF AND WITH METASTATIC SPINAL CORD COMPRESSION Policy author Accountable Executive Lead Approving body Policy reference Consultant Palliative
GUIDELINES FOR THE DIAGNOSIS AND MANAGEMENT OF ADULTS AT RISK OF AND WITH METASTATIC SPINAL CORD COMPRESSION Policy author Accountable Executive Lead Approving body Policy reference Consultant Palliative
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Re-audit of Radiotherapy Waiting Times 2005
 Abstract Re-audit of Radiotherapy Waiting Times 2005 E. Summers, M Williams Royal College of Radiologists, 38 Portland Place, London W1B 4JQ, UK Aim: To determine current waiting times for radiotherapy
Abstract Re-audit of Radiotherapy Waiting Times 2005 E. Summers, M Williams Royal College of Radiologists, 38 Portland Place, London W1B 4JQ, UK Aim: To determine current waiting times for radiotherapy
Audit and Implementation Guide: Clinical guidelines for the pre and post operative physiotherapy management of adults with lower limb amputations
 2nd Edition- 2016 Audit and Implementation Guide: Clinical guidelines for the pre and post operative physiotherapy British Association of Chartered Physiotherapists in Amputee Rehabilitation NICE has accredited
2nd Edition- 2016 Audit and Implementation Guide: Clinical guidelines for the pre and post operative physiotherapy British Association of Chartered Physiotherapists in Amputee Rehabilitation NICE has accredited
The European Board of Urology
 Page 1 of 15 The European Board of Urology Sub-specialty certification application: Prostate cancer, A - General information A1 - APPLICATION IDENTIFICATION 1a. Application code blank 1b. EBU internal
Page 1 of 15 The European Board of Urology Sub-specialty certification application: Prostate cancer, A - General information A1 - APPLICATION IDENTIFICATION 1a. Application code blank 1b. EBU internal
National Cancer Peer Review Sarcoma. Julia Hill Acting Deputy National Co-ordinator
 National Cancer Peer Review Sarcoma Julia Hill Acting Deputy National Co-ordinator Improving Outcomes Guidance The Intentions of Improving Outcomes for People with Sarcoma Changes in the provision of care
National Cancer Peer Review Sarcoma Julia Hill Acting Deputy National Co-ordinator Improving Outcomes Guidance The Intentions of Improving Outcomes for People with Sarcoma Changes in the provision of care
National Hospital for Neurology and Neurosurgery. Muscle biopsy Centre for Neuromuscular Diseases
 National Hospital for Neurology and Neurosurgery Muscle biopsy Centre for Neuromuscular Diseases If you would like this document in another language or format or if you require the services of an interpreter
National Hospital for Neurology and Neurosurgery Muscle biopsy Centre for Neuromuscular Diseases If you would like this document in another language or format or if you require the services of an interpreter
Decision Making Flowchart for Metastatic Spinal Cord Compression and Pathological Spinal Fractures
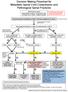 Decision Making Flowchart for Metastatic Spinal Cord Compression and Pathological Spinal Fractures All Referrals (see notes): Spinal Surgeons Locally or Trauma SpR at UHW Oncology SpR at Velindre / Singleton
Decision Making Flowchart for Metastatic Spinal Cord Compression and Pathological Spinal Fractures All Referrals (see notes): Spinal Surgeons Locally or Trauma SpR at UHW Oncology SpR at Velindre / Singleton
North West London Trauma Network Spinal Pathway and Protocols
 North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
Radiotherapy symptoms control in bone mets. Francesco Cellini GemelliART. Ernesto Maranzano,MD. Session 5: Symptoms management
 Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Acute Oncology: Service Provision in Smaller Cancer Centres Ernie Marshall Clatterbridge Centre for Oncology
 Acute Oncology: Service Provision in Smaller Cancer Centres Ernie Marshall Clatterbridge Centre for Oncology Whiston Hospital St Helen s Hospital 350,000 population ~1000 beds Regional Plastics Unit DGH
Acute Oncology: Service Provision in Smaller Cancer Centres Ernie Marshall Clatterbridge Centre for Oncology Whiston Hospital St Helen s Hospital 350,000 population ~1000 beds Regional Plastics Unit DGH
Health Board/Region: All-Wales
 Peer Review: Cancer Sub-site: Gynaecology Health Board/Region: All-Wales Cycle: Second Date of review: February 2018 This report describes the findings and themes observed by clinical review panels during
Peer Review: Cancer Sub-site: Gynaecology Health Board/Region: All-Wales Cycle: Second Date of review: February 2018 This report describes the findings and themes observed by clinical review panels during
Cancer Survivorship NEURO-ONCOLOGY PATIENT SURVIVORSHIP PLAN. Resources and Tools for the Multidisciplinary Team
 NEURO-ONCOLOGY PATIENT SURVIVORSHIP PLAN Cancer Survivorship Resources and Tools for the Multidisciplinary Team Your survivorship care plan is a summary of your tumor treatments and recommendations for
NEURO-ONCOLOGY PATIENT SURVIVORSHIP PLAN Cancer Survivorship Resources and Tools for the Multidisciplinary Team Your survivorship care plan is a summary of your tumor treatments and recommendations for
Exclude referred pain from the neck, diaphragm, heart, lungs, & polymyalgia rheumatica YES. NSAIDs/analgesics as required
 Shoulder Pain Clinical Presentation info for GPs who refer into PAH more info History and Examination Exclude referred pain from the neck, diaphragm, heart, lungs, & polymyalgia rheumatica more info for
Shoulder Pain Clinical Presentation info for GPs who refer into PAH more info History and Examination Exclude referred pain from the neck, diaphragm, heart, lungs, & polymyalgia rheumatica more info for
National Standards for Acute Oncology Services
 Cancer National Specialist Advisory Group National Standards for Acute Oncology Services June 2016 TABLE OF CONTENTS 1. PURPOSE... 2 2. INTRODUCTION... 2 3. STRATEGIC CONTEXT... 4 4. SCOPE OF ACUTE ONCOLOGY
Cancer National Specialist Advisory Group National Standards for Acute Oncology Services June 2016 TABLE OF CONTENTS 1. PURPOSE... 2 2. INTRODUCTION... 2 3. STRATEGIC CONTEXT... 4 4. SCOPE OF ACUTE ONCOLOGY
North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO)
 North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO) UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Original Prepared by NMcL April 2016
North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO) UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Original Prepared by NMcL April 2016
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012
 Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
How a fully integrated Acute Oncology Service can benefit the busy medical unit
 How a fully integrated Acute Oncology Service can benefit the busy medical unit Dr. Pauline Leonard MD FRCP Consultant Medical Oncologist Whittington Health Over the next 35 mins Briefly remind you of
How a fully integrated Acute Oncology Service can benefit the busy medical unit Dr. Pauline Leonard MD FRCP Consultant Medical Oncologist Whittington Health Over the next 35 mins Briefly remind you of
Your Orthotics service is changing
 Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Manchester Cancer Colorectal Pathway Board: Guidelines for management of colorectal hepatic metastases
 Manchester Cancer Colorectal Pathway Board: Guidelines for management of colorectal hepatic metastases Date: April 2015 Date for review: April 2018 1. Principles The recognised specialist HPB MDT for Greater
Manchester Cancer Colorectal Pathway Board: Guidelines for management of colorectal hepatic metastases Date: April 2015 Date for review: April 2018 1. Principles The recognised specialist HPB MDT for Greater
Cancer of Unknown Primary Service
 Cancer of Unknown Primary Service Dr Maurice Fernando Consultant In Specialist Palliative Care and CUP lead Doncaster and Bassetlaw Hospitals NHS FT Wakefield meeting -14-07-2016 CUP service CUP MDT
Cancer of Unknown Primary Service Dr Maurice Fernando Consultant In Specialist Palliative Care and CUP lead Doncaster and Bassetlaw Hospitals NHS FT Wakefield meeting -14-07-2016 CUP service CUP MDT
NON MALIGNANT BRAIN TUMOURS Facilitator. Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol
 NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
DOCUMENT CONTROL PAGE
 DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
Venous Thromboembolism (VTE) Prevention and Treatment of VTE in Patients Admitted to Hospital
 Please Note: This policy is currently under review and is still fit for purpose. Venous Thromboembolism (VTE) Prevention and Treatment of VTE in Patients Admitted to Hospital This procedural document supersedes
Please Note: This policy is currently under review and is still fit for purpose. Venous Thromboembolism (VTE) Prevention and Treatment of VTE in Patients Admitted to Hospital This procedural document supersedes
DRAFT FOR CONSULTATION. Clinical Commissioning Policy Proposition: Palliative radiotherapy for bone pain
 Clinical Commissioning Policy Proposition: Palliative radiotherapy for bone pain Information Reader Box (IRB) to be inserted on inside front cover for documents of 6 pages and over, with Publications Gateway
Clinical Commissioning Policy Proposition: Palliative radiotherapy for bone pain Information Reader Box (IRB) to be inserted on inside front cover for documents of 6 pages and over, with Publications Gateway
The use of surgery in the elderly. for management of metastatic epidural spinal cord compression
 The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
Rehabilitation and Metastatic Spinal Cord Compression
 Rehabilitation and Metastatic Spinal Cord Compression Pradeep Thumbikat MS, MSc, FRCS Consultant in Spinal Cord Injuries Sheffield Teaching Hospitals 1 Evidence for Rehabilitation Differences and similarities
Rehabilitation and Metastatic Spinal Cord Compression Pradeep Thumbikat MS, MSc, FRCS Consultant in Spinal Cord Injuries Sheffield Teaching Hospitals 1 Evidence for Rehabilitation Differences and similarities
Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Malignant Spinal cord Compression. Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania
 Malignant Spinal cord Compression Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania Background Statistics of SCC -1 Incidence of SCC Vertebral body metastases 85 % Para-vertebral (Lymphoma)
Malignant Spinal cord Compression Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania Background Statistics of SCC -1 Incidence of SCC Vertebral body metastases 85 % Para-vertebral (Lymphoma)
Spinal cord compression as a first presentation of cancer: A case report
 J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
Referral guide for acute oncology emergencies
 Referral guide for acute oncology emergencies 1 st Edition v 1.0 London Cancer March 2013 To be used in conjunction with London Cancer clinical guidelines for acute oncology emergencies; A Guide to Acute
Referral guide for acute oncology emergencies 1 st Edition v 1.0 London Cancer March 2013 To be used in conjunction with London Cancer clinical guidelines for acute oncology emergencies; A Guide to Acute
Suspected Pulmonary embolus Ambulatory Pathway. Document Title. Date Issued/Approved: Date Valid From: 11/11/17. Date Valid To: 11/05/18
 POLICY UNDER REVIEW Please note that this policy is under review. It does, however, remain current Trust policy subject to any recent legislative changes, national policy instruction (NHS or Department
POLICY UNDER REVIEW Please note that this policy is under review. It does, however, remain current Trust policy subject to any recent legislative changes, national policy instruction (NHS or Department
Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group. Policies for the Commissioning of Healthcare
 Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group Policies for the Commissioning of Healthcare Policy for Managing Back Pain Spinal /Facet Joint and Epidural
Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group Policies for the Commissioning of Healthcare Policy for Managing Back Pain Spinal /Facet Joint and Epidural
Faster Cancer Treatment Indicators: Use cases
 Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
National Optimal Lung Cancer Pathways. Dr Sadia Anwar Nottingham University Hospitals NHS Trust Clinical Lead for Lung Cancer
 National Optimal Lung Cancer Pathways Dr Sadia Anwar ttingham University Hospitals NHS Trust Clinical Lead for Lung Cancer Overview How NOLCP evolved How it relates to national guidance Pathways Implementation
National Optimal Lung Cancer Pathways Dr Sadia Anwar ttingham University Hospitals NHS Trust Clinical Lead for Lung Cancer Overview How NOLCP evolved How it relates to national guidance Pathways Implementation
ADJUVANT CHEMOTHERAPY...
 Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Proposed Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Proposed Health Technology Appraisal Radium-223 chloride for the treatment of bone metastases in castrate resistant prostate cancer Draft scope Draft
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Proposed Health Technology Appraisal Radium-223 chloride for the treatment of bone metastases in castrate resistant prostate cancer Draft scope Draft
Guideline for the Follow-up of Patients with Gynaecological Malignancies
 Guideline for the Follow-up of Patients with Gynaecological Malignancies Version History Version Date Summary of Change/Process 2.0 20.02.08 Endorsed by the Governance Committee 2.1 18.11.10 Circulated
Guideline for the Follow-up of Patients with Gynaecological Malignancies Version History Version Date Summary of Change/Process 2.0 20.02.08 Endorsed by the Governance Committee 2.1 18.11.10 Circulated
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Community and Mental Health Services. Palliative Care. Criteria and
 Community and Mental Health Services Specialist Palliative Care Service Referral Criteria and Guidance November 2018 Specialist Palliative Care Service Referrals These guidelines cover referrals for patients
Community and Mental Health Services Specialist Palliative Care Service Referral Criteria and Guidance November 2018 Specialist Palliative Care Service Referrals These guidelines cover referrals for patients
*Corresponding Author:
 Audit of venous thromboembolism prophylaxis administered to general surgical patients undergoing elective and emergency operations at National Hospital, Sri Lanka *Migara Seneviratne 1, Asanka Hemachandra
Audit of venous thromboembolism prophylaxis administered to general surgical patients undergoing elective and emergency operations at National Hospital, Sri Lanka *Migara Seneviratne 1, Asanka Hemachandra
