The role of radiation therapy in palliative care of children with advanced cancer: Clinical outcomes and patterns of care
|
|
|
- Scott Patterson
- 5 years ago
- Views:
Transcription
1 Received: 27 July 2016 Revised: 1 September 2016 Accepted: 9 September 2016 DOI: /pbc RESEARCH ARTICLE Pediatric Blood & Cancer The American Society of Pediatric Hematology/Oncology The role of radiation therapy in palliative care of children with advanced cancer: Clinical outcomes and patterns of care Sumeeta Varma 1 Debra L. Friedman 2 Mark J. Stavas 1 1 Department of Radiation Oncology, Vanderbilt University Medical Center, Nashville, Tennessee 2 Division of Pediatric Hematology-Oncology, Vanderbilt University Medical Center, Nashville, Tennessee Correspondence Sumeeta Varma, Department of Radiation Oncology, Vanderbilt University Medical Center, 2220 Pierce Avenue, Preston Research Building, Ste B-1003, Nashville, TN sumeeta.varma@vanderbilt.edu Abstract Background: There are few published data to guide the use and timing of palliative radiation therapy (RT) in children. We aimed to determine the clinical outcomes of palliative RT in children and the relationship with palliative care and hospice referrals. Procedure: A retrospective chart review was performed on all patients younger than 18 years who received palliative RT in our clinic from January 2005 to January Results: In the specified time period, 50 children underwent 83 courses of palliative RT. Median survival after treatment was 124 days (range, days). Fifteen courses were delivered to children in the last 30 days of life (dol). Palliative RT was successful in 89% of courses delivered before the last 30 dol versus 28% of courses delivered in the last 30 dol (p < , Fisher s exact test). At the time of data collection, 43 children were deceased. Altogether, 88% of children who received palliative RT were also referred to our institution s pediatric palliative care team or to hospice at some time in their course. Of the children who died, 74% were referred to hospice and 34% were on hospice while receiving palliative RT. For children not already on hospice, the median time to hospice referral was 96 days after the last fraction (range, days). Conclusions: Palliative RT is effective in children with advanced cancer, although less so in the last 30 dol. With careful care coordination and multidisciplinary collaboration, RT can be successfully integrated into supportive and end-of-life care for children with advanced cancer. KEYWORDS end of life, hospice, palliative care, patterns of care, radiation oncology, radiotherapy 1 INTRODUCTION Radiation therapy (RT) is a well-established modality for palliation of symptoms from metastatic and locally advanced cancer. For adult patients, there is a sizable body of literature, including prospective randomized clinical trials and evidence-based clinical guidelines, regarding the epidemiology and effectiveness of various radiotherapy approaches for palliation of bone pain, 1,2 symptomatic brain metastases, 3 5 spinal cord compression, 6 8 and other symptoms. However, the indications and outcomes after palliative radiation in pediatric patients remain underreported. Several small single institutional studies have demonstrated improved symptoms burden with radiation However, the optimal timing, delivery, and role of palliative radiation in the continuum of end-of-life care remain unknown. Here we explore the use of palliative radiation in advanced pediatric malignancies with Abbreviations: RT, radiation therapy; dol, days of life a focus on the timing of radiation during the disease course relative to palliative care and hospice referrals. 2 METHODS A retrospective chart review was performed on all patients younger than 18 years who received palliative radiation therapy at Vanderbilt University Medical Center between January 2005 and January Treatment courses were classified as palliative, rather than definitive, in intent if they were so designated by the treating radiation oncologist in treatment planning or consultation notes. If treatment intent was not explicitly stated in the available documents, it was assigned based on a comprehensive review of the chart by a designated investigator (S.V.). In general, RT was considered to be palliative in children with advanced cancer who were ineligible for or whose disease had persisted/progressed through standard of care first-line therapy, and Pediatr Blood Cancer 2017; 64: e26359 wileyonlinelibrary.com/journal/pbc c 2016 Wiley Periodicals, Inc. 1of7
2 2of7 VARMA ET AL. in whom the goal of RT was amelioration or prevention of a specific symptom. In most cases, patients had in fact undergone multiple unsuccessful lines of systemic, cure-directed therapy. Data were abstracted from patient charts and managed using REDCap electronic data capture tools hosted at Vanderbilt University. 12 The study was reviewed and approved by the Institutional Review Board of Vanderbilt University. For each patient, patient gender, tumor histology, time of death or last follow-up after palliative RT, whether and when palliative care and hospice referrals were placed, and for deceased patients, the location of death (hospital vs. home vs. inpatient hospice) were recorded. For each palliative radiation course, data recorded included patient age, site treated, presenting symptom for palliation, radiation dose, number of fractions, elapsed treatment days, whether the course was completed as prescribed, and symptom response. Symptom response was determined by review of clinic and inpatient notes from the end of RT to death or last follow-up. Symptoms were considered to have responded if any provider documented any of the following: (1) patient or parent report of subjective improvement in the symptom, (2) improvement in relevant physical examination parameters such as work of breathing or abdominal distension, or (3) decrease in medical treatment required for the symptom such as pain medication or supplemental oxygen. Statistical analysis was performed using Microsoft Excel (ver ). Relationships between treatment variables and palliative outcomes were evaluated using Fisher s exact test. The threshold for statistical significance was set at a two-tailed p value < RESULTS In the specified time period, 50 pediatric patients underwent 83 courses of palliative RT: 37 patients underwent a single palliative RT course, 4 patients underwent 2 courses, and 9 patients underwent 3 or more courses. Patient characteristics and indications for palliative RT are summarized in Table 1. The median age at the time of RT was 10.3 years (range, 2 months to 18 years). The most common histologies treated were neuroblastoma (23%), rhabdomyosarcoma (18%), Ewing s sarcoma (9.6%), and osteosarcoma (4.8%). Common treatment sites included the extremities (27%), spine (21%), abdominopelvic cavity (19%), head and neck (13%), and brain (10%). The most common presenting symptom for palliation was pain, representing 58% of palliative RT courses. Additional target symptoms included neurologic symptoms (e.g., spinal cord compression, headache, vision changes, ataxia, neurogenic bladder) in 20% of palliative RT courses and dyspnea in 10% of courses. Eleven palliative RT courses (13% of total) were performed in asymptomatic patients felt to be at high risk for symptoms from a known disease site, such as impending pathologic fracture or lesions approaching but not yet compressing the spinal cord. The median number of RT fractions delivered for each palliative course was 6 (range, 1 32) and the median number of elapsed days was 9 (range, 0 47). In eight cases (10% of courses), treatment was terminated early TABLE 1 Characteristics of patients and radiation treatment delivered in 83 palliative RT courses, January 2005 to January 2015 Median (range) or % (n) Age 10.3 years ( years) Gender Male 60% (50) Female 40% (33) Anatomic site Extremity 27% (22) Spine 20% (17) Abdomen/pelvis 19% (16) Head and neck 13% (11) Brain 10% (8) Thoracic 7.2% (6) Liver 1.2% (1) Other 2.4% (2) Histology Neuroblastoma 23% (19) Rhabdomyosarcoma 18% (15) Ewing s sarcoma 10% (8) Leukemia 7.2% (6) Osteosarcoma 4.8% (4) Other sarcoma 4.8% (4) Lymphoma 2.4% (2) Wilms tumor 2.4% (2) Brainstem glioma 1.2% (1) Ependymoma 1.2% (1) Malignant astrocytoma 1.2% (1) Other 24% (20) Indication/target symptom a Pain 58% (48) Neurologic symptoms 21% (17) Asymptomatic 13% (11) Dyspnea 10% (8) Other 10% (8) Total dose delivered 2,000 cgy (150 5,974 cgy) No. of fractions 6 fractions (1 32 fractions) Elapsed days 9 days (0 47 days) Completed prescribed course? Yes 90% (75) No 10% (8) a More than one target symptom was permitted per course. because of the declining clinical status of the patient or parental preference. Evaluation of symptom response was possible for 79 of 84 palliative RT courses. When response was not evaluable, it was generally due to the patient transferring care or enrolling in hospice shortly after completing RT, and subsequent lack of clinical notes or detailed updates from outside providers. Of the courses for which response was
3 VARMA ET AL. 3of7 TABLE 2 Success rate of palliative RT courses by indication, duration, and timing % (n) All evaluable courses 77% (61) Indication/target symptom Pain 80% (37) Neurologic symptoms 71% (10) Asymptomatic 100% (9) Dyspnea 62% (5) Other 50% (4) No. of fractions a 10 fractions 82% (46) > 10 fractions 94% (15) Timing in disease course Last 30 days of life 28% (4) >30 days of life 89% (57) b a Completed courses only. b p < evaluable, 80% of courses undertaken for pain resulted in symptom improvement, as did 71% of courses for neurologic symptoms and 62% of courses for dyspnea (Table 2). Of the 11 palliative RT courses delivered for prevention of impending symptoms, in 9 cases follow-up documentation indicated that the patient remained free of the symptom until death or last follow-up, and in the remaining 2 cases there were insufficient clinical notes to determine whether the patient developed symptoms before death (Table 2). From this point forward in our analysis, palliative RT courses were considered successful if they either led to symptom improvement in a symptomatic patient or were delivered to an asymptomatic patient and the patient remained free of the feared symptom. The overall rate of successful palliative RT courses was 77%. Characteristics of the unsuccessful courses are presented in Table 3. Unsuccessfully treated sites included the abdomen/pelvis (35% of unsuccessful courses), spine (23%), thoracic (18%), brain (12%), head and neck (6%), and extremity (6%). The most common unsuccessfully treated histologies were rhabdomyosarcoma (23%), leukemias (18%), and neuroblastoma (12%), and the most common unsuccessfully treated symptom was pain (53%). Thirty-five percent of unsuccessful courses were courses terminated early. Of the 50 individual patients treated, 43 were deceased and 7 were still living at the time of data collection. Median survival after palliative RT was 124 days, with a range from 1 day to 1141 days (Fig. 1A). Fifteen palliative RT courses were delivered to patients in the last 30 days of life (dol); seven of these were in the last 7 dol. To examine the effect of timing on the utility of palliative RT, we compared courses delivered to patients in the last 30 dol with those delivered earlier in the disease course. Palliative RT delivered in the last 30 dol had a 28% success rate, whereas courses delivered earlier than the last 30 dol had an 89% success rate (Table 1). This difference was statistically significant (p < ). Details of the patients who received palliative RT in the last 7 dol are presented in Table 4. Of note, five of the TABLE 3 Characteristics of unsuccessful completed palliative RT courses (n = 17) Median (range) or % (n) Anatomic site Abdomen/pelvis 35% (6) Spine 23% (4) Thoracic 18% (3) Brain 12% (2) Head and neck 6% (1) Extremity 6% (1) Histology Rhabdomyosarcoma 23% (4) Leukemia 18% (3) Neuroblastoma 12% (2) Wilms tumor 6% (1) Lymphoma 6% (1) Ewing s sarcoma 6% (1) Other a 23% (4) Indication/Target symptom Pain 53% (9) Neurologic symptoms 18% (3) Dyspnea 18% (3) Other b 23% (4) Total dose delivered 800 cgy (150 5,974 cgy) No. of fractions 3 (1 29) Completed prescribed course? Yes 65% (11) No 35% (6) a Other histologies included NUT midline carcinoma, mesoblastoma, signet ring colorectal carcinoma, and high-grade malignant neoplasm not otherwise specified. b Other indications included nerve root compression, hemoptysis, and abdominal distension. seven patients terminated RT early. None of the seven courses were successful. We also examined the relationship between fractionation and success of palliative RT. Completed palliative RT courses prescribed in 10 fractions had a success rate of 82% and completed courses prescribed in >10 fractions had a success rate of 94%, which was not a statistically significant difference (p = 0.43; Table 2). Sixty percent of patients were referred to our institution s pediatric palliative care team at some time in their trajectory (Table 5), and 28% of patients already had pediatric palliative care team involvement before palliative RT (Fig. 1B). Thirty-two patients were referred to hospice (64% of total cohort, 74% of deceased patients), and hospice referral was discussed with two additional families who declined referral. Eleven patients (22% of total cohort, 34% of those who received hospice care) were already enrolled in hospice when they presented for palliative RT (Fig. 1C). For those patients not already enrolled in hospice, the median time to hospice referral was 96 days after the last palliative RT fraction (range, days). The median time from
4 4of7 VARMA ET AL. TABLE 4 Characteristics and outcomes of patients receiving palliative RT in the last 7 days of life Patient Age (years) Histology Site Symptom Systemic disease status/concurrent problems Prescribed treatment (dose/# Fx) Delivered treatment (dose/# Fx) Days to death Location of death Acute myelogenous leukemia Infratemporal fossa mass Pain Progressive bony infiltration, leukemia cutis/gram-negative bacteremia 10.5Gy/3fx 7Gy/2fx 5 Hospital (floor) 2 8 Ewing s sarcoma R lung & chest wall Hemoptysis, chest pain Nootherdisease sites/anemia 25 Gy/5 fx 5 Gy/1 fx 1 ICU Neuroblastoma L hemithorax Respiratory distress No other disease sites/febrile neutropenia, hypokalemia 7.5Gy/5fx 1.5Gy/1fx 1 ICU Acute myelogenous leukemia Lumbar spine Spinal cord compression Disseminated leptomeningeal disease/hydrocephalus 20 Gy/5 fx 20 Gy/5 fx 2 ICU 5 10 Burkitt s lymphoma Abdomen/pelvis Pain Multiple abdominal masses, abdominal and bilateral iliac LNs/Fever, cardiac dysfunction 9Gy/6fx 4.5Gy/3fx 3 Hospital (floor) 6 14 Ewing s sarcoma Brain Altered mental status Progressive lung and visceral metastases/thrombocytopenia, weight loss 30 Gy/10 fx 18 Gy/6 fx 5 Unknown a 7 5 Wilms tumor Abdomen/pelvis Pain, psoas muscle dysfunction Multifocal progressive disease throughout abdomen and pelvis/urinary outlet obstruction, renal failure 8Gy/1fx 8Gy/1fx 6 Hospital (floor) a Patient was discharged from hospital with hospice care 1 day after RT.
5 VARMA ET AL. 5of7 hospice referral to death was 36.5 days (range, days). Of the 43 patients who died, the location of death was identified for 31 (72%), and of these, 55% died at home, 32% in the hospital, and 13% at an inpatient hospice facility (Table 5). 4 DISCUSSION FIGURE 1 Timing in days of palliative RT completion relative to (A) death or last follow-up, (B) first contact with the palliative care team, and (C) hospice enrollment TABLE 5 Supportive and end-of-life care patterns for 50 children treated with palliative RT Median (range) or % (n) Status a Alive 14% (7) Deceased 86% (43) Palliative care and hospice involvement Palliative care only 14% (7) Hospice only 18% (9) Both 46% (23) Neither 12% (6) Hospice length of stay 36.5 days (4 243) Location of death b Home 55% (17) Hospital 32% (10) Inpatient/residential hospice 13% (4) a Atthetimeofdataanalysis. b Of 31 patients whose location of death could be determined by the chart review. Radiation therapy is a well-established and widely used modality to palliate symptoms from advanced cancers. While palliative RT in adults is informed by large-scale clinical trials 2,3,6 and patterns of care analyses, there is little comparable literature to guide the use of palliative RT in children. Our study contributes to this literature by reporting a 10-year single-institution series of pediatric palliative RT patients, with a focus on the timing of palliative RT in the illness trajectory. Clinical outcomes in our cohort affirm that RT is effective for palliation of pain, dyspnea, neurologic, and other symptoms in children with advanced cancer. Our symptom response rates are consistent with previously reported series including the overall 84% response rate Koontz s metastatic Ewing s sarcoma series, 16 and symptom-specific response rates of 80% for bone pain, 55% for dyspnea/chest pain, and 58% for neurologic symptoms in Rahn s series of diverse histologies. 11 Interestingly, 13% of the RT courses in our cohort were to asymptomatic disease sites, where either the physician or the patient/family was concerned that symptoms could quickly develop. For example, two children were treated for large C1 C2 metastases before developing any symptoms of spinal cord compression. To our knowledge, the frequency and outcomes of such prophylactic palliative treatment have not previously been described. In our cohort, no child treated for symptom prevention was documented to develop the symptom, though of course it remains speculative how they would have fared without RT. The success rate of palliative RT in our cohort was significantly lower for children in their last 30 dol. This is unsurprising given the usual dynamics of RT response 17,18 and is consistent with growing consideration of RT in the last 30 dol as a potential overuse metric for adult patients. 19,20 Whether the designation of overuse is appropriate for palliative RT in children in the last 30 dol is unclear, as prognostication to this level of specificity can be extremely challenging and some children in their last 30 dol did appear to benefit. Experienced clinician judgment, potentially augmented by published survival prediction models, can often produce reasonable life expectancy estimates at least in general terms of hours, days, weeks, or months. Life expectancy on the order of days to weeks should probably attenuate clinician and family expectations of benefit from RT, though attempting treatment may still be reasonable for intractable symptoms. Most children in our cohort treated in the last 7 dol were unable to complete the prescribed course, and none appeared to have symptom improvement from the dose they did receive. Many of these children had widely disseminated progressive disease or other serious medical problems at the time palliative RT was attempted, likely driving their short survival. If palliative RT is attempted for an intractable focal symptom when life expectancy is on the order of days, strong consideration should be given to
6 6of7 VARMA ET AL. single-fraction treatment to increase the likelihood that the patient will actually receive a therapeutic dose. Even for children earlier in their disease trajectory, shorter palliative RT courses have the important advantage of imposing fewer burdens on the child and family. Our results did not indicate a greater likelihood of success with protracted RT courses, >10 fractions. However, with conventional fractionation sizes, longer courses may offer more durable response and less long-term toxicity. With median survival on the order of 3 4 months, late effects should be of less concern in this population, though we did see a few multiyear survivors. There is growing interest in stereotactic radiation in the pediatric population, exemplified by the current Children s Oncology Group phase II clinical trial for metastatic Ewing s sarcoma in which a secondary outcome is the feasibility of stereotactic body radiation therapy. Hypofractionated stereotactic radiation might prove useful in the palliative setting as well, for children in whom durability of response and/or late effects are of concern. Our data are reassuring that children receiving palliative RT were able to access other important supportive care and end-of-life services. Altogether, 88% of children treated with palliative RT were also referred to either our institution s pediatric palliative care team or hospice, including 22% of the cohort who were already enrolled in hospice when they received RT. This is in contrast to the adult population, where access to palliative RT while enrolled in hospice can be quite limited. 15,21,22 For those children referred to hospice after palliative RT, this tended to happen weeks to months later, further suggesting that palliative RT and hospice were utilized with distinctive roles and timing in the continuum of care. This is again in contrast to our experience (S.V. and M.J.S.) with adult palliative RT patients, for whom hospice and palliative RT are often treated as competing options of last resort when nothing more can be done with systemic therapy. The median time from hospice referral to death in this pediatric cohort was 36.5 days, which is 5 6 days shorter than that reported in other studies of pediatric oncology patients in hospice. 23,24 This does raise the prospect that palliative RT might delay some hospice referrals, but may also reflect broader institutional or regional differences. These considerations highlight the importance of close multidisciplinary collaboration in the care of children for whom palliative RT is considered. Selecting patients who are likely to benefit from RT and matching the appropriate RT strategy to the patient depends on a clear understanding of the child s disease trajectory, global medical condition, prognosis and prognostic awareness, and other symptom management options if RT is infeasible or unsuccessful. The primary pediatric oncologist has a key role to play, utilizing their expertise about the primary disease and usually a long-standing relationship with the child and family to rationally time the introduction of other specialists and services. Direct communication and cross-disciplinary education among pediatric oncologists, radiation oncologists, pediatric palliative care physicians, and other pediatric specialists, such as pain management or critical care, can help determine the best interventions for each child at different points in their course of illness. Our ability to optimize dose and fractionation for palliative RT in children would also benefit tremendously from pooling of data across centers. Multi-institutional retrospective analyses would be beneficial, as would the prospective study of symptom response to RT for various pediatric cancer histologies and symptoms. Some of these data could even be collected in the context of clinical trials for definitive therapies, as a secondary outcome to the primary survival and progression endpoints. Given the collaborative relationships within pediatric oncology clinical trials groups, it should be possible to develop evidence-based recommendations for palliative RT in children whose goals have shifted from cure to symptom control. Our study has several important limitations. It represents a singleinstitution experience, and the small number of patients precludes extensive hypothesis testing or multivariate analysis. In addition, although the charting of RT treatment details is relatively standardized, extraction of other key data points from patient charts required more subjective inference. This was particularly the case for assessing symptom onset and response, given the diversity of symptoms, absence of standardized scales from our routine clinical charting, and in some cases multiple simultaneous interventions directed at the same symptom (e.g., titration of opioids just before RT). ACKNOWLEDGEMENTS Study data were managed using REDCap electronic data capture tools hosted at Vanderbilt University, which are supported by grant UL1 TR from NCATS/NIH. CONFLICT OF INTEREST The authors declare that there is no conflict of interest. REFERENCES 1. Kim EY, Chapman TR, Ryu S, et al. ACR Appropriateness Criteria( R ) non-spine bone metastases. J Palliat Med. 2015;18(1): Lutz S, Berk L, Chang E, et al. Palliative radiotherapy for bone metastases: an ASTRO evidence-based guideline. Int J Radiat Oncol Biol Phys. 2011;79(4): Regine WF, Rogozinska A, Kryscio RJ, Tibbs PA, Young AB, Patchell RA. Recursive partitioning analysis classifications I and II: applicability evaluated in a randomized trial for resected single brain metastases. Am J Clin Oncol. 2004;27(5): Gaspar LE, Mehta MP, Patchell RA, et al. The role of whole brain radiation therapy in the management of newly diagnosed brain metastases: a systematic review and evidence-based clinical practice guideline. J Neurooncol. 2010;96(1): Linskey ME, Andrews DW, Asher AL, et al. The role of stereotactic radiosurgery in the management of patients with newly diagnosed brain metastases: a systematic review and evidence-based clinical practice guideline. J Neurooncol. 2010;96(1): Expert Panel on Radiation Oncology-Bone Metastases: Lo SS, Ryu S, Chang EL, et al. ACR Appropriateness Criteria R Metastatic Epidural Spinal Cord Compression and Recurrent Spinal Metastasis. J Palliat Med. 2015;18(7): Savage P, Sharkey R, Kua T, et al. Malignant spinal cord compression: NICE guidance, improvements and challenges. QJM Mon J Assoc Phys. 2014;107(4): Loblaw DA, Mitera G, Ford M, Laperriere NJ. A 2011 updated systematic review and clinical practice guideline for the management of malignant extradural spinal cord compression. Int J Radiat Oncol Biol Phys. 2012;84(2):
7 VARMA ET AL. 7of7 9. Bhasker S, Bajpai V, Turaka A. Palliative radiotherapy in paediatric malignancies. Singapore Med J. 2008;49(12): Paulino AC. Palliative radiotherapy in children with neuroblastoma. Pediatr Hematol Oncol. 2003;20(2): Rahn DA, Mundt AJ, Murphy JD, Schiff D, Adams J, Murphy KT. Clinical outcomes of palliative radiation therapy for children. Pract Radiat Oncol. 2015;5(3): Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap) a metadata-driven methodology and workflow process for providing translational research informatics support. JBiomedInform.2009;42(2): McDonald R, Chow E, Lam H, Rowbottom L, Soliman H. International patterns of practice in radiotherapy for bone metastases: a review of the literature. J Bone Oncol. 2014;3(3 4): Ellsworth SG, Alcorn SR, Hales RK, McNutt TR, DeWeese TL, Smith TJ. Patterns of care among patients receiving radiation therapy for bone metastases at a large academic institution. Int J Radiat Oncol Biol Phys. 2014;89(5): Stavas M, Arneson K, Friedman J, Misra S. From whole brain to hospice: patterns of care in radiation oncology. J Palliat Med. 2014;17(6): Koontz BF, Clough RW, Halperin EC. Palliative radiation therapy for metastatic Ewing sarcoma. Cancer. 2006;106(8): Walasek T, Sas-Korczyńska B, Dąbrowski T, et al. Palliative thoracic radiotherapy for patients with advanced non-small cell lung cancer and poor performance status. Lung Cancer Amst Neth. 2015;87(2): Meeuse JJ, van der Linden YM, van Tienhoven G, et al. Efficacy of radiotherapy for painful bone metastases during the last 12 weeks of life: results from the Dutch Bone Metastasis Study. Cancer. 2010;116(11): Patel A, Dunmore-Griffith J, Lutz S, Johnstone PAS. Radiation therapy in the last month of life. Rep Pract Oncol Radiother J Gt Cancer Cent Pozn Pol Soc Radiat Oncol. 2014;19(3): Panoff J, Simoneaux RV, Shah N, et al. Radiation therapy at end of life in children. J Palliat Med. 2015;18(2): Jarosek SL, Virnig BA, Feldman R. Palliative radiotherapy in Medicare-certified freestanding hospices. J Pain Symptom Manage. 2009;37(5): Yeung HN, Mitchell WM, Roeland EJ, et al. Palliative radiation before hospice: the long and the short of it. J Pain Symptom Manage. 2014;48(6): Thienprayoon R, Lee SC, Leonard D, Winick N. Hospice care for children with cancer: where do these children die? J Pediatr Hematol Oncol. 2015;37(5): Klopfenstein KJ, Hutchison C, Clark C, Young D, Ruymann FB. Variables influencing end-of-life care in children and adolescents with cancer. J Pediatr Hematol Oncol. 2001;23(8): How to cite this article: Varma, S, Friedman, DL, Stavas, ML. The role of radiation therapy in palliative care of children with advanced cancer: Clinical outcomes and patterns of care. Pediatr Blood Cancer. 2017;64:e /pbc.26359
The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting
 Original Article on Palliative Radiotherapy The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting Taylor R. Cushman 1, Shervin Shirvani 2, Mohamed Khan
Original Article on Palliative Radiotherapy The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting Taylor R. Cushman 1, Shervin Shirvani 2, Mohamed Khan
The use of surgery in the elderly. for management of metastatic epidural spinal cord compression
 The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
Original Article. Keywords: Pain; quality of life; radiation oncology
 Original Article Impact of a dedicated palliative radiation oncology service on the use of single fraction and hypofractionated radiation therapy among patients with bone metastases Sonia Skamene 1 *,
Original Article Impact of a dedicated palliative radiation oncology service on the use of single fraction and hypofractionated radiation therapy among patients with bone metastases Sonia Skamene 1 *,
Radiotherapy symptoms control in bone mets. Francesco Cellini GemelliART. Ernesto Maranzano,MD. Session 5: Symptoms management
 Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Spinal cord compression as a first presentation of cancer: A case report
 J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
Palliative radiotherapy in lung cancer
 New concepts and insights regarding the role of radiation therapy in metastatic disease Umberto Ricardi University of Turin Department of Oncology Radiation Oncology Palliative radiotherapy in lung cancer
New concepts and insights regarding the role of radiation therapy in metastatic disease Umberto Ricardi University of Turin Department of Oncology Radiation Oncology Palliative radiotherapy in lung cancer
Single-Fraction vs Multi-Fraction Radiotherapy in Palliative Bone Metastases Patients
 Single-Fraction vs Multi-Fraction Radiotherapy in Palliative Bone Metastases Patients Acknowledgements GVSU Statistical Consulting Center for help with statistical analysis GVSU Presidential Research Grant
Single-Fraction vs Multi-Fraction Radiotherapy in Palliative Bone Metastases Patients Acknowledgements GVSU Statistical Consulting Center for help with statistical analysis GVSU Presidential Research Grant
Impact of pre-treatment symptoms on survival after palliative radiotherapy An improved model to predict prognosis?
 Impact of pre-treatment symptoms on survival after palliative radiotherapy An improved model to predict prognosis? Thomas André Ankill Kämpe 30.05.2016 MED 3950,-5 year thesis Profesjonsstudiet i medisin
Impact of pre-treatment symptoms on survival after palliative radiotherapy An improved model to predict prognosis? Thomas André Ankill Kämpe 30.05.2016 MED 3950,-5 year thesis Profesjonsstudiet i medisin
Collection of Recorded Radiotherapy Seminars
 IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org The Role of Radiosurgery in the Treatment of Gliomas Luis Souhami, MD Professor Department of Radiation
IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org The Role of Radiosurgery in the Treatment of Gliomas Luis Souhami, MD Professor Department of Radiation
Using claims data to investigate RT use at the end of life. B. Ashleigh Guadagnolo, MD, MPH Associate Professor M.D. Anderson Cancer Center
 Using claims data to investigate RT use at the end of life B. Ashleigh Guadagnolo, MD, MPH Associate Professor M.D. Anderson Cancer Center Background 25% of Medicare budget spent on the last year of life.
Using claims data to investigate RT use at the end of life B. Ashleigh Guadagnolo, MD, MPH Associate Professor M.D. Anderson Cancer Center Background 25% of Medicare budget spent on the last year of life.
Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2
 Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2 Case 79 yo M with hx of T3N0 colon cancer diagnosed in 2008 metastatic liver disease s/p liver segmentectomy 2009
Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2 Case 79 yo M with hx of T3N0 colon cancer diagnosed in 2008 metastatic liver disease s/p liver segmentectomy 2009
The Role of Radiotherapy in Metastatic Breast Cancer. Shilpen Patel MD, FACRO Associate Professor Departments of Radiation Oncology and Global Health
 The Role of Radiotherapy in Metastatic Breast Cancer Shilpen Patel MD, FACRO Associate Professor Departments of Radiation Oncology and Global Health Indications for Palliative Pain Control Radiation Bone
The Role of Radiotherapy in Metastatic Breast Cancer Shilpen Patel MD, FACRO Associate Professor Departments of Radiation Oncology and Global Health Indications for Palliative Pain Control Radiation Bone
Selecting the Optimal Treatment for Brain Metastases
 Selecting the Optimal Treatment for Brain Metastases Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Understand the benefits, limitations,
Selecting the Optimal Treatment for Brain Metastases Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Understand the benefits, limitations,
9/19/2017. Palliative Radiotherapy We Can Actually Afford: A New Program Designed to Help Patients and Caregivers Save Resources
 Palliative Radiotherapy We Can Actually Afford: A New Program Designed to Help Patients and Caregivers Save Resources Christopher Abraham, MD Assistant Professor Department of Radiation Oncology Washington
Palliative Radiotherapy We Can Actually Afford: A New Program Designed to Help Patients and Caregivers Save Resources Christopher Abraham, MD Assistant Professor Department of Radiation Oncology Washington
ONLINE CONTINUING EDUCATION ACTIVITY
 ONLINE CONTINUING EDUCATION ACTIVITY Take free quizzes online at acsjournals.com/ce ARTICLE TITLE: Palliative Radiotherapy at the End of Life: A Critical Review CONTINUING MEDICAL EDUCATION ACCREDITATION
ONLINE CONTINUING EDUCATION ACTIVITY Take free quizzes online at acsjournals.com/ce ARTICLE TITLE: Palliative Radiotherapy at the End of Life: A Critical Review CONTINUING MEDICAL EDUCATION ACCREDITATION
The Role of Radiation Therapy in the Treatment of Brain Metastases. Matthew Cavey, M.D.
 The Role of Radiation Therapy in the Treatment of Brain Metastases Matthew Cavey, M.D. Objectives Provide information about the prospective trials that are driving the treatment of patients with brain
The Role of Radiation Therapy in the Treatment of Brain Metastases Matthew Cavey, M.D. Objectives Provide information about the prospective trials that are driving the treatment of patients with brain
Pediatric Oncology. Vlad Radulescu, MD
 Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY
 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Cancer is a group of more than 100 different diseases that are characterized by uncontrolled cellular growth,
BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Cancer is a group of more than 100 different diseases that are characterized by uncontrolled cellular growth,
Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis
 Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
There Is Something More We Can Do: An Introduction to Hospice and Palliative Care
 There Is Something More We Can Do: An Introduction to Hospice and Palliative Care presented to the Washington Patient Safety Coalition July 28, 2010 Hope Wechkin, MD Medical Director Evergreen Hospice
There Is Something More We Can Do: An Introduction to Hospice and Palliative Care presented to the Washington Patient Safety Coalition July 28, 2010 Hope Wechkin, MD Medical Director Evergreen Hospice
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM BRAIN METASTASES CNS Site Group Brain Metastases Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM BRAIN METASTASES CNS Site Group Brain Metastases Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
Management of single brain metastasis: a practice guideline
 PRACTICE GUIDELINE SERIES Management of single brain metastasis: a practice guideline A. Mintz MD,* J. Perry MD, K. Spithoff BHSc, A. Chambers MA, and N. Laperriere MD on behalf of the Neuro-oncology Disease
PRACTICE GUIDELINE SERIES Management of single brain metastasis: a practice guideline A. Mintz MD,* J. Perry MD, K. Spithoff BHSc, A. Chambers MA, and N. Laperriere MD on behalf of the Neuro-oncology Disease
NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) BONE (Version , 03/28/18)
 BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
Journal of Pediatric Sciences
 Journal of Pediatric Sciences Role of post-operative radiation therapy in single brain metastasis from clear cell sarcoma in children: a case report with systemic review Fadoua Rais, Naoual Benhmidou,
Journal of Pediatric Sciences Role of post-operative radiation therapy in single brain metastasis from clear cell sarcoma in children: a case report with systemic review Fadoua Rais, Naoual Benhmidou,
A new score predicting the survival of patients with spinal cord compression from myeloma
 Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
A prospective study of patients with impending spinal cord compression treated with palliative radiotherapy alone
 A prospective study of patients with impending spinal cord compression treated with palliative radiotherapy alone Item Type Article Authors O'Sullian, L.;Clayton-Lea, A.;McArdle, O.;McGarry, M.;Kenny,
A prospective study of patients with impending spinal cord compression treated with palliative radiotherapy alone Item Type Article Authors O'Sullian, L.;Clayton-Lea, A.;McArdle, O.;McGarry, M.;Kenny,
Palliative treatments for lung cancer: What can the oncologist do?
 Palliative treatments for lung cancer: What can the oncologist do? Neil Bayman Consultant Clinical Oncologist GM Cancer Palliative Care and Lung Cancer Education Event Manchester, 31 st January 2017 Most
Palliative treatments for lung cancer: What can the oncologist do? Neil Bayman Consultant Clinical Oncologist GM Cancer Palliative Care and Lung Cancer Education Event Manchester, 31 st January 2017 Most
Clinical Case Conference
 Clinical Case Conference Palliative radiation therapy for bone metastasis Jeff Burkeen, MD, PGY2 7/20/2015 1 Overview Epidemiology Pathophysiology Common presentations and symptoms Imaging Surgery Radiation
Clinical Case Conference Palliative radiation therapy for bone metastasis Jeff Burkeen, MD, PGY2 7/20/2015 1 Overview Epidemiology Pathophysiology Common presentations and symptoms Imaging Surgery Radiation
New Surgical Oncology Clinic at Nationwide Children s Hospital
 Hematology/Oncology & BMT New Surgical Oncology Clinic at Nationwide Children s Hospital This clinic offers convenient, comprehensive care for patients with cancer. Here, in one visit, pediatric patients
Hematology/Oncology & BMT New Surgical Oncology Clinic at Nationwide Children s Hospital This clinic offers convenient, comprehensive care for patients with cancer. Here, in one visit, pediatric patients
Integrating Palliative and Oncology Care in Patients with Advanced Cancer
 Integrating Palliative and Oncology Care in Patients with Advanced Cancer Jennifer Temel, MD Massachusetts General Hospital Cancer Center Director, Cancer Outcomes Research Overview 1. Why should we be
Integrating Palliative and Oncology Care in Patients with Advanced Cancer Jennifer Temel, MD Massachusetts General Hospital Cancer Center Director, Cancer Outcomes Research Overview 1. Why should we be
A new instrument for estimation of survival in elderly patients irradiated for metastatic spinal cord compression from breast cancer
 Rades et al. Radiation Oncology (2015) 10:173 DOI 10.1186/s13014-015-0483-8 RESEARCH A new instrument for estimation of survival in elderly patients irradiated for metastatic spinal cord compression from
Rades et al. Radiation Oncology (2015) 10:173 DOI 10.1186/s13014-015-0483-8 RESEARCH A new instrument for estimation of survival in elderly patients irradiated for metastatic spinal cord compression from
Oncologic Emergencies: When to call the Radiation Oncologist
 Oncologic Emergencies: When to call the Radiation Oncologist Dr. Shrinivas Rathod Radiation Oncologist Radiation Oncology Program CancerCare Manitoba and University of Manitoba Disclosures Speaker s name:
Oncologic Emergencies: When to call the Radiation Oncologist Dr. Shrinivas Rathod Radiation Oncologist Radiation Oncology Program CancerCare Manitoba and University of Manitoba Disclosures Speaker s name:
JMSCR Vol 06 Issue 12 Page December 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.15 Single Institutional Comparative
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.15 Single Institutional Comparative
Lara Kujtan, MD; Abdulraheem Qasem, MD
 The Treatment of Lung Cancer Between 2013-2014 at Truman Medical Center: A Retrospective Review in Fulfillment of the Requirements of Standard 4.6 (Monitoring Compliance with Evidence- Based Guidelines)
The Treatment of Lung Cancer Between 2013-2014 at Truman Medical Center: A Retrospective Review in Fulfillment of the Requirements of Standard 4.6 (Monitoring Compliance with Evidence- Based Guidelines)
MEASURE SPECIFICATIONS
 QOPI REPTING REGISTRY (QCDR) 2018 QOPI 5 QOPI 11 Chemotherapy administered to patients with metastatic solid tumor with performance status of 3, 4, or undocumented (Lower Score - Better) Combination chemotherapy
QOPI REPTING REGISTRY (QCDR) 2018 QOPI 5 QOPI 11 Chemotherapy administered to patients with metastatic solid tumor with performance status of 3, 4, or undocumented (Lower Score - Better) Combination chemotherapy
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM EPENDYMOMA Last Revision Date July 2015 1 CNS Site Group Ependymoma Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM EPENDYMOMA Last Revision Date July 2015 1 CNS Site Group Ependymoma Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2.
MEASURE SPECIFICATIONS
 QOPI REPTING REGISTRY (QCDR) 2018 QOPI5 Title Chemotherapy administered to patients with metastatic solid tumor with performance status of 3, 4, or undocumented (Lower Score - Better) Description Percentage
QOPI REPTING REGISTRY (QCDR) 2018 QOPI5 Title Chemotherapy administered to patients with metastatic solid tumor with performance status of 3, 4, or undocumented (Lower Score - Better) Description Percentage
Painful vertebral metastases are a frequent manifestation of malignancies
 2892 COMMUNICATION Palliative Radiation Therapy for Painful Vertebral Metastases A Practice Survey Tejpal Gupta, M.D., D.N.B. Rajiv Sarin, M.D. Department of Radiation Oncology, Tata Memorial Hospital,
2892 COMMUNICATION Palliative Radiation Therapy for Painful Vertebral Metastases A Practice Survey Tejpal Gupta, M.D., D.N.B. Rajiv Sarin, M.D. Department of Radiation Oncology, Tata Memorial Hospital,
Radiotherapy physics & Equipments
 Radiotherapy physics & Equipments RAD 481 Lecture s Title: An Overview of Radiation Therapy for Health Care Professionals Dr. Mohammed Emam Vision :IMC aspires to be a leader in applied medical sciences,
Radiotherapy physics & Equipments RAD 481 Lecture s Title: An Overview of Radiation Therapy for Health Care Professionals Dr. Mohammed Emam Vision :IMC aspires to be a leader in applied medical sciences,
Radiation Treatment for Breast. Cancer. Melissa James Radiation Oncologist August 2015
 Radiation Treatment for Breast Cancer Melissa James Radiation Oncologist August 2015 OUTLINE External Beam Radiation treatment. (What is Radiation, doctor?) Role of radiation. (Why am I getting radiation,
Radiation Treatment for Breast Cancer Melissa James Radiation Oncologist August 2015 OUTLINE External Beam Radiation treatment. (What is Radiation, doctor?) Role of radiation. (Why am I getting radiation,
Palliative radiotherapy for advanced Cancer: Are we giving it to the right patient at the right time?
 ORIGINAL ARTICLE Palliative radiotherapy for advanced Cancer: Are we giving it to the right patient at the right time? Syadwa Abdul Shukor, MD, Anita Zarina Bustam, FRCR Department of Clinical Oncology,
ORIGINAL ARTICLE Palliative radiotherapy for advanced Cancer: Are we giving it to the right patient at the right time? Syadwa Abdul Shukor, MD, Anita Zarina Bustam, FRCR Department of Clinical Oncology,
Local radiotherapy for palliation in multiple myeloma patients with symptomatic bone lesions
 Original Article Radiat Oncol J 2016;34(1):59-63 pissn 2234-1900 eissn 2234-3156 Local radiotherapy for palliation in multiple myeloma patients with symptomatic bone lesions Jeong Won Lee, MD, Jeong Eun
Original Article Radiat Oncol J 2016;34(1):59-63 pissn 2234-1900 eissn 2234-3156 Local radiotherapy for palliation in multiple myeloma patients with symptomatic bone lesions Jeong Won Lee, MD, Jeong Eun
Radiation Oncology Study Guide
 Radiation Oncology Study Guide For the Initial CertificationQualifying (Computer-Based) Examination General and Radiation Oncology This examination is designed to assess your understanding of the entire
Radiation Oncology Study Guide For the Initial CertificationQualifying (Computer-Based) Examination General and Radiation Oncology This examination is designed to assess your understanding of the entire
Palliative RT. Jiraporn Setakornnukul, M.D. Radiation Oncology Division Siriraj Hospital, Mahidol University
 Palliative RT Jiraporn Setakornnukul, M.D. Radiation Oncology Division Siriraj Hospital, Mahidol University Scope Brain metastasis Metastasis epidural spinal cord compression SVC obstruction Bone pain
Palliative RT Jiraporn Setakornnukul, M.D. Radiation Oncology Division Siriraj Hospital, Mahidol University Scope Brain metastasis Metastasis epidural spinal cord compression SVC obstruction Bone pain
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Radiotherapy and Brain Metastases. Dr. K Van Beek Radiation-Oncologist BSMO annual Meeting Diegem
 Radiotherapy and Brain Metastases Dr. K Van Beek Radiation-Oncologist BSMO annual Meeting Diegem 24-02-2017 Possible strategies Watchful waiting Surgery Postop RT to resection cavity or WBRT postop SRS
Radiotherapy and Brain Metastases Dr. K Van Beek Radiation-Oncologist BSMO annual Meeting Diegem 24-02-2017 Possible strategies Watchful waiting Surgery Postop RT to resection cavity or WBRT postop SRS
Stereotactic Radiosurgery for Brain Metastasis: Changing Treatment Paradigms. Overall Clinical Significance 8/3/13
 Stereotactic Radiosurgery for Brain Metastasis: Changing Treatment Paradigms Jason Sheehan, MD, PhD Departments of Neurosurgery and Radiation Oncology University of Virginia, Charlottesville, VA USA Overall
Stereotactic Radiosurgery for Brain Metastasis: Changing Treatment Paradigms Jason Sheehan, MD, PhD Departments of Neurosurgery and Radiation Oncology University of Virginia, Charlottesville, VA USA Overall
VINCENT KHOO. 8 th EIKCS Symposium: May 2013
 8 th EIKCS Symposium: May 2013 VINCENT KHOO Royal Marsden NHS Foundation Trust & Institute of Cancer Research St George s Hospital & University of London Austin Health & University of Melbourne Disclosures
8 th EIKCS Symposium: May 2013 VINCENT KHOO Royal Marsden NHS Foundation Trust & Institute of Cancer Research St George s Hospital & University of London Austin Health & University of Melbourne Disclosures
Gamma Knife Radiosurgery A tool for treating intracranial conditions. CNSA Annual Congress 2016 Radiation Oncology Pre-congress Workshop
 Gamma Knife Radiosurgery A tool for treating intracranial conditions CNSA Annual Congress 2016 Radiation Oncology Pre-congress Workshop ANGELA McBEAN Gamma Knife CNC State-wide Care Coordinator Gamma Knife
Gamma Knife Radiosurgery A tool for treating intracranial conditions CNSA Annual Congress 2016 Radiation Oncology Pre-congress Workshop ANGELA McBEAN Gamma Knife CNC State-wide Care Coordinator Gamma Knife
This LCD recognizes these two distinct treatment approaches and is specific to treatment delivery:
 National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: 77371, 77372, 77373 LCD ID Number: L33410 J-N FL Responsible
National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: 77371, 77372, 77373 LCD ID Number: L33410 J-N FL Responsible
State of the Art Radiotherapy for Pediatric Tumors. Suzanne L. Wolden, MD Memorial Sloan-Kettering Cancer Center
 State of the Art Radiotherapy for Pediatric Tumors Suzanne L. Wolden, MD Memorial Sloan-Kettering Cancer Center Introduction Progress and success in pediatric oncology Examples of low-tech and high-tech
State of the Art Radiotherapy for Pediatric Tumors Suzanne L. Wolden, MD Memorial Sloan-Kettering Cancer Center Introduction Progress and success in pediatric oncology Examples of low-tech and high-tech
Minesh Mehta, Northwestern University. Chicago, IL
 * Minesh Mehta, Northwestern University Chicago, IL Consultant: Adnexus, Bayer, Merck, Tomotherapy Stock Options: Colby, Pharmacyclics, Procertus, Stemina, Tomotherapy Board of Directors: Pharmacyclics
* Minesh Mehta, Northwestern University Chicago, IL Consultant: Adnexus, Bayer, Merck, Tomotherapy Stock Options: Colby, Pharmacyclics, Procertus, Stemina, Tomotherapy Board of Directors: Pharmacyclics
We have previously reported good clinical results
 J Neurosurg 113:48 52, 2010 Gamma Knife surgery as sole treatment for multiple brain metastases: 2-center retrospective review of 1508 cases meeting the inclusion criteria of the JLGK0901 multi-institutional
J Neurosurg 113:48 52, 2010 Gamma Knife surgery as sole treatment for multiple brain metastases: 2-center retrospective review of 1508 cases meeting the inclusion criteria of the JLGK0901 multi-institutional
GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. Version:
 GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V4 Acute Oncology Group
GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V4 Acute Oncology Group
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION. Mustafa Rashid Issa
 THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
All India Institute of Medical Sciences, New Delhi, INDIA. Department of Pediatric Surgery, Medical Oncology, and Radiology
 All India Institute of Medical Sciences, New Delhi, INDIA Department of Pediatric Surgery, Medical Oncology, and Radiology Clear cell sarcoma of the kidney- rare renal neoplasm second most common renal
All India Institute of Medical Sciences, New Delhi, INDIA Department of Pediatric Surgery, Medical Oncology, and Radiology Clear cell sarcoma of the kidney- rare renal neoplasm second most common renal
Hypofractionated radiation therapy for glioblastoma
 Hypofractionated radiation therapy for glioblastoma Luis Souhami, MD, FASTRO Professor McGill University Department of Oncology, Division of Radiation Oncology Montreal Canada McGill University Health
Hypofractionated radiation therapy for glioblastoma Luis Souhami, MD, FASTRO Professor McGill University Department of Oncology, Division of Radiation Oncology Montreal Canada McGill University Health
20. Background. Oligometastases. Oligometastases: bone (including spine) and lymph nodes
 125 20. Oligometastases Background The oligometastatic state can be defined as 1 3 isolated metastatic sites, typically occurring more than six months after successful treatment of primary disease. 1 In
125 20. Oligometastases Background The oligometastatic state can be defined as 1 3 isolated metastatic sites, typically occurring more than six months after successful treatment of primary disease. 1 In
Spinal Cord Compression Diagnosis and Management. Information for Shared Care Centres and Community Staff
 Reference: CG1412 Written by: Dr Daniel Yeomanson Peer reviewer Dr Jeanette Payne Approved: August 2016 Approved by D&TC: 10 th June 2016 Review Due: August 2019 Intended Audience This document contains
Reference: CG1412 Written by: Dr Daniel Yeomanson Peer reviewer Dr Jeanette Payne Approved: August 2016 Approved by D&TC: 10 th June 2016 Review Due: August 2019 Intended Audience This document contains
Quality of End-of-Life Care in Patients with Hematologic Malignancies: A Retrospective Cohort Study
 Quality of End-of-Life Care in Patients with Hematologic Malignancies: A Retrospective Cohort Study David Hui, Neha Didwaniya, Marieberta Vidal, Seong Hoon Shin, Gary Chisholm, Joyce Roquemore, Eduardo
Quality of End-of-Life Care in Patients with Hematologic Malignancies: A Retrospective Cohort Study David Hui, Neha Didwaniya, Marieberta Vidal, Seong Hoon Shin, Gary Chisholm, Joyce Roquemore, Eduardo
Imaging for suspected glioma
 Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Radiotherapy in the management of optic pathway gliomas
 Turkish Journal of Cancer Vol.30/ No.1/2000 Radiotherapy in the management of optic pathway gliomas FARUK ZORLU, FERAH YILDIZ, MURAT GÜRKAYNAK, FADIL AKYOL, İ. LALE ATAHAN Department of Radiation Oncology,
Turkish Journal of Cancer Vol.30/ No.1/2000 Radiotherapy in the management of optic pathway gliomas FARUK ZORLU, FERAH YILDIZ, MURAT GÜRKAYNAK, FADIL AKYOL, İ. LALE ATAHAN Department of Radiation Oncology,
Advanced Cancer Care: A Primer on Palliative Radiation Oncology
 Tennessee Medicine E-Journal Volume 3 Issue 2 Article 13 September 2017 Advanced Cancer Care: A Primer on Palliative Radiation Oncology Benjamin Li Vanderbilt University School of Medicine, benjamin.c.li@vanderbilt.edu
Tennessee Medicine E-Journal Volume 3 Issue 2 Article 13 September 2017 Advanced Cancer Care: A Primer on Palliative Radiation Oncology Benjamin Li Vanderbilt University School of Medicine, benjamin.c.li@vanderbilt.edu
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
Wilms Tumor and Neuroblastoma
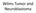 Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Stereotactic ablative body radiotherapy for renal cancer
 1 EVIDENCE SUMMARY REPORT Stereotactic ablative body radiotherapy for renal cancer Questions to be addressed 1. What is the clinical effectiveness of stereotactic ablative body radiotherapy for inoperable
1 EVIDENCE SUMMARY REPORT Stereotactic ablative body radiotherapy for renal cancer Questions to be addressed 1. What is the clinical effectiveness of stereotactic ablative body radiotherapy for inoperable
Palliative radiotherapy near the end of life for brain metastases from lung cancer: a populationbased
 Palliative radiotherapy near the end of life for brain metastases from lung cancer: a populationbased analysis Roel Schlijper Fellow Radiation Oncology BC Cancer, Prince George Disclosures No conflicts
Palliative radiotherapy near the end of life for brain metastases from lung cancer: a populationbased analysis Roel Schlijper Fellow Radiation Oncology BC Cancer, Prince George Disclosures No conflicts
Metastatic Spinal Cord Compression
 Metastatic Spinal Cord Compression Dr Zacharias Tasigiannopoulos Clinical Oncologist Colney centre Department of Oncology Norwich, UK Introduction 2-5% of cancer patients have an episode of MSCC Initial
Metastatic Spinal Cord Compression Dr Zacharias Tasigiannopoulos Clinical Oncologist Colney centre Department of Oncology Norwich, UK Introduction 2-5% of cancer patients have an episode of MSCC Initial
Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) in the treatment of oligometastatic disease
 Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) in the treatment of oligometastatic disease Reference: NHS England: 16032/P 2 NHS England INFORMATION READER BOX Directorate
Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) in the treatment of oligometastatic disease Reference: NHS England: 16032/P 2 NHS England INFORMATION READER BOX Directorate
and Strength of Recommendations
 ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
Second Neoplasms Working Group. CCSS Investigators Meeting June 2017
 Second Neoplasms Working Group CCSS Investigators Meeting June 2017 Second Neoplasms Working Group Overview Ongoing review, adjudication and entry of reported neoplasms into data set Initial review of
Second Neoplasms Working Group CCSS Investigators Meeting June 2017 Second Neoplasms Working Group Overview Ongoing review, adjudication and entry of reported neoplasms into data set Initial review of
Department of Orthopedic Surgery, Henan Province People s Hospital, Henan, People s Republic of China; 2
 Int J Clin Exp Med 2018;11(3):2465-2470 www.ijcem.com /ISSN:1940-5901/IJCEM0060812 Original Article Validation of a scoring system predicting survival and function outcome in patients with metastatic epidural
Int J Clin Exp Med 2018;11(3):2465-2470 www.ijcem.com /ISSN:1940-5901/IJCEM0060812 Original Article Validation of a scoring system predicting survival and function outcome in patients with metastatic epidural
Seizures in high-grade glioma patients:
 Seizures in high-grade glioma patients: a serious challenge in the end of life phase JAF Koekkoek,* EM Sizoo,* TJ Postma, JJ Heimans, HRW Pasman, L Deliens, MJB Taphoorn and JC Reijneveld BMJ Support Palliat
Seizures in high-grade glioma patients: a serious challenge in the end of life phase JAF Koekkoek,* EM Sizoo,* TJ Postma, JJ Heimans, HRW Pasman, L Deliens, MJB Taphoorn and JC Reijneveld BMJ Support Palliat
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT
 SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia
 A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia Gaurav Bahl, Karl Tennessen, Ashraf Mahmoud-Ahmed, Dorianne Rheaume, Ian Fleetwood,
A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia Gaurav Bahl, Karl Tennessen, Ashraf Mahmoud-Ahmed, Dorianne Rheaume, Ian Fleetwood,
Thoracic Recurrences. Soft tissue recurrence
 Stereotactic body radiotherapy for thoracic and soft malignancies Alexander Gottschalk, M.D., Ph.D. Associate Professor Director of CyberKnife Radiosurgery Department of Radiation Oncology University of
Stereotactic body radiotherapy for thoracic and soft malignancies Alexander Gottschalk, M.D., Ph.D. Associate Professor Director of CyberKnife Radiosurgery Department of Radiation Oncology University of
Demographic profile and utilization statistics of a Canadian inpatient palliative care unit within a tertiary care setting
 NAPOLSKIKH et al. CANADIAN CENTRE ACTIVITIES Demographic profile and utilization statistics of a Canadian inpatient palliative care unit within a tertiary care setting ABSTRACT Background J. Napolskikh
NAPOLSKIKH et al. CANADIAN CENTRE ACTIVITIES Demographic profile and utilization statistics of a Canadian inpatient palliative care unit within a tertiary care setting ABSTRACT Background J. Napolskikh
Modern management in vertebral metastasis
 43 B. Costachescu, C.E. Popescu Modern management in vertebral metastasis Modern management in vertebral metastasis B. Costachescu, C.E. Popescu Department of Neurosurgery, Division of Spine Surgery, University
43 B. Costachescu, C.E. Popescu Modern management in vertebral metastasis Modern management in vertebral metastasis B. Costachescu, C.E. Popescu Department of Neurosurgery, Division of Spine Surgery, University
Managing Bone Pain in Metastatic Disease. Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018
 Managing Bone Pain in Metastatic Disease Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018 None Disclosures Managing Bone Pain in Metastatic Disease This lecture will
Managing Bone Pain in Metastatic Disease Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018 None Disclosures Managing Bone Pain in Metastatic Disease This lecture will
PALLIATIVE CARE IN HEMATOLOGIC MALIGNANCIES KEDAR KIRTANE MD FRED HUTCHINSON CANCER RESEARCH CENTER UNIVERSITY OF WASHINGTON
 PALLIATIVE CARE IN HEMATOLOGIC MALIGNANCIES KEDAR KIRTANE MD FRED HUTCHINSON CANCER RESEARCH CENTER UNIVERSITY OF WASHINGTON DISCLOSURES OBJECTIVES To discuss how hematologic malignancies qualitatively
PALLIATIVE CARE IN HEMATOLOGIC MALIGNANCIES KEDAR KIRTANE MD FRED HUTCHINSON CANCER RESEARCH CENTER UNIVERSITY OF WASHINGTON DISCLOSURES OBJECTIVES To discuss how hematologic malignancies qualitatively
PALLIATIVE MEDICINE Nigel Sykes St Christopher s Hospice London UK
 Guttmann Conference June 2013 PALLIATIVE MEDICINE Nigel Sykes St Christopher s Hospice London UK Palliative Medicine What is Palliative Medicine and where did it come from? The extent and organisation
Guttmann Conference June 2013 PALLIATIVE MEDICINE Nigel Sykes St Christopher s Hospice London UK Palliative Medicine What is Palliative Medicine and where did it come from? The extent and organisation
CLINICAL APPLICATION OF LINEAR-QUADRATIC MODEL IN REIRRADIATION OF SYMPTOMATIC BONE METASTASES
 MEDICAL PHYSICS CLINICAL APPLICATION OF LINEAR-QUADRATIC MODEL IN REIRRADIATION OF SYMPTOMATIC BONE METASTASES L. REBEGEA 1,2, M. DUMITRU 1, D. FIRESCU 2,3 1 Sf. Ap. Andrei Emergency Clinical Hospital,
MEDICAL PHYSICS CLINICAL APPLICATION OF LINEAR-QUADRATIC MODEL IN REIRRADIATION OF SYMPTOMATIC BONE METASTASES L. REBEGEA 1,2, M. DUMITRU 1, D. FIRESCU 2,3 1 Sf. Ap. Andrei Emergency Clinical Hospital,
ACR TXIT TM EXAM OUTLINE
 ACR TXIT TM EXAM OUTLINE Major Domain Sub-Domain 1 Statistics 1.1 Study design 1.2 Definitions of statistical terms 1.3 General interpretation & analysis 1.4 Survival curves 1.5 Specificity/sensitivity
ACR TXIT TM EXAM OUTLINE Major Domain Sub-Domain 1 Statistics 1.1 Study design 1.2 Definitions of statistical terms 1.3 General interpretation & analysis 1.4 Survival curves 1.5 Specificity/sensitivity
Palliative Care: Mission and Strategic Imperative. Sarah E. Hetue Hill, PhD Ascension Healthcare
 Palliative Care: Mission and Strategic Imperative Sarah E. Hetue Hill, PhD Ascension Healthcare Ascension Palliative Care Definition Palliative Care is person-centered, holistic care delivered by an interdisciplinary
Palliative Care: Mission and Strategic Imperative Sarah E. Hetue Hill, PhD Ascension Healthcare Ascension Palliative Care Definition Palliative Care is person-centered, holistic care delivered by an interdisciplinary
Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study
 Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
Spinal cord compression as the initial presentation of colorectal cancer: case report and review of the literature
 Spinal cord compression as the initial presentation of colorectal cancer: case report and review of the literature Magdalena M. Gilg 1, Gerhard Bratschitsch 1, Ulrike Wiesspeiner 2, Roman Radl 1, Andreas
Spinal cord compression as the initial presentation of colorectal cancer: case report and review of the literature Magdalena M. Gilg 1, Gerhard Bratschitsch 1, Ulrike Wiesspeiner 2, Roman Radl 1, Andreas
Pelvic palliative radiotherapy for gynecological cancers present state of knowledge and pending research questions to answer
 Pelvic palliative radiotherapy for gynecological cancers present state of knowledge and pending research questions to answer Esten S. Nakken MD PhD Division of Cancer Medicine Oslo University Hospital
Pelvic palliative radiotherapy for gynecological cancers present state of knowledge and pending research questions to answer Esten S. Nakken MD PhD Division of Cancer Medicine Oslo University Hospital
Evaluation of prognostic scoring systems for bone metastases using single center data
 MOLECULAR AND CLINICAL ONCOLOGY 3: 1361-1370, 2015 Evaluation of prognostic scoring systems for bone metastases using single center data HIROFUMI SHIMADA 1, TAKAO SETOGUCHI 2, SHUNSUKE NAKAMURA 1, MASAHIRO
MOLECULAR AND CLINICAL ONCOLOGY 3: 1361-1370, 2015 Evaluation of prognostic scoring systems for bone metastases using single center data HIROFUMI SHIMADA 1, TAKAO SETOGUCHI 2, SHUNSUKE NAKAMURA 1, MASAHIRO
Pediatric electron intraoperative radiotherapy: results and innovations
 Pediatric electron intraoperative radiotherapy: results and innovations Felipe A. Calvo ESTRO Hospital General Universitario Gregorio Marañon Madrid, Spain 2017 IOeRT in pediatric cancer: results and innovations
Pediatric electron intraoperative radiotherapy: results and innovations Felipe A. Calvo ESTRO Hospital General Universitario Gregorio Marañon Madrid, Spain 2017 IOeRT in pediatric cancer: results and innovations
Subspecialty Inpatient Rotation: Pediatric Oncology at Memorial Sloan Kettering Cancer Center Senior Resident
 Subspecialty Inpatient Rotation: Pediatric Oncology at Memorial Sloan Kettering Cancer Center Senior Resident Residents: Pediatric residents at the PL3 level Prerequisites: Successful completion or waiver
Subspecialty Inpatient Rotation: Pediatric Oncology at Memorial Sloan Kettering Cancer Center Senior Resident Residents: Pediatric residents at the PL3 level Prerequisites: Successful completion or waiver
Alleinige Radiochirurgie und alleinige Systemtherapie zwei «extreme» Entwicklungen in der Behandlung von Hirnmetastasen?
 Department of Radiation Oncology Chairman: Prof. Dr. Matthias Guckenberger Alleinige Radiochirurgie und alleinige Systemtherapie zwei «extreme» Entwicklungen in der Behandlung von Hirnmetastasen? Matthias
Department of Radiation Oncology Chairman: Prof. Dr. Matthias Guckenberger Alleinige Radiochirurgie und alleinige Systemtherapie zwei «extreme» Entwicklungen in der Behandlung von Hirnmetastasen? Matthias
Significant Papers in Pediatric Oncology: Phase I Studies Current Status and Future Directions
 Significant Papers in Pediatric Oncology: Phase I Studies Current Status and Future Directions Susannah E. Koontz, PharmD, BCOP Clinical Pharmacy & Education Consultant Pediatric Hematology/Oncology and
Significant Papers in Pediatric Oncology: Phase I Studies Current Status and Future Directions Susannah E. Koontz, PharmD, BCOP Clinical Pharmacy & Education Consultant Pediatric Hematology/Oncology and
WHAT ARE PAEDIATRIC CANCERS
 WHAT ARE PAEDIATRIC CANCERS INTRODUCTION Childhood cancers are RARE 0.5% of all cancers in the West Overall risk that a child will develop cancer during first 15 years of life is 1 in 450 and 1 in 600
WHAT ARE PAEDIATRIC CANCERS INTRODUCTION Childhood cancers are RARE 0.5% of all cancers in the West Overall risk that a child will develop cancer during first 15 years of life is 1 in 450 and 1 in 600
8/2/2018. Acknowlegements: TCP SPINE. Disclosures
 A Presentation for the AAPM Annual meeting, Aug 2, 2018 Nashville, TN Stereotactic Radiosurgery for Spinal Metastases: Tumor Control Probability Analyses and Recommended Reporting Standards for Future
A Presentation for the AAPM Annual meeting, Aug 2, 2018 Nashville, TN Stereotactic Radiosurgery for Spinal Metastases: Tumor Control Probability Analyses and Recommended Reporting Standards for Future
IGRT Protocol Design and Informed Margins. Conflict of Interest. Outline 7/7/2017. DJ Vile, PhD. I have no conflict of interest to disclose
 IGRT Protocol Design and Informed Margins DJ Vile, PhD Conflict of Interest I have no conflict of interest to disclose Outline Overview and definitions Quantification of motion Influences on margin selection
IGRT Protocol Design and Informed Margins DJ Vile, PhD Conflict of Interest I have no conflict of interest to disclose Outline Overview and definitions Quantification of motion Influences on margin selection
The Canadian National System for Incident Reporting in Radiation Treatment (NSIR-RT) Taxonomy March 11, 2015
 The Canadian National System for Incident Reporting in Radiation Treatment (NSIR-RT) Taxonomy March 11, 2015 Taxonomy Data Category Number Description Data Fields and Menu Choices 1. Impact 1.1 Incident
The Canadian National System for Incident Reporting in Radiation Treatment (NSIR-RT) Taxonomy March 11, 2015 Taxonomy Data Category Number Description Data Fields and Menu Choices 1. Impact 1.1 Incident
Metastatic epidural spinal cord compression (MESCC)
 SPINE Volume 39, Number 9, pp E587 - E592 2014, Lippincott Williams & Wilkins LITERATURE REVIEW Direct Decompressive Surgery Followed by Radiotherapy Versus Radiotherapy Alone for Metastatic Epidural Spinal
SPINE Volume 39, Number 9, pp E587 - E592 2014, Lippincott Williams & Wilkins LITERATURE REVIEW Direct Decompressive Surgery Followed by Radiotherapy Versus Radiotherapy Alone for Metastatic Epidural Spinal
9:00-9:10 am Metastatic Epidural Cervical Spinal Cord Compression CSRS San Diego, 2015 Michael G. Fehlings, MD
 9:00-9:10 am Metastatic Epidural Cervical Spinal Cord Compression CSRS San Diego, 2015 Michael G. Fehlings, MD 1 BACKGROUND After the lungs and the liver, metastases most frequently arise in osseous tissues;
9:00-9:10 am Metastatic Epidural Cervical Spinal Cord Compression CSRS San Diego, 2015 Michael G. Fehlings, MD 1 BACKGROUND After the lungs and the liver, metastases most frequently arise in osseous tissues;
Isotopes and Palliative Radiotherapy for bone metastases
 Isotopes and Palliative Radiotherapy for bone metastases Rationale for Bone-seeking Isotope Therapies in Prostate Cancer > 90% of patients with advanced prostate cancer have bone metastases which can be
Isotopes and Palliative Radiotherapy for bone metastases Rationale for Bone-seeking Isotope Therapies in Prostate Cancer > 90% of patients with advanced prostate cancer have bone metastases which can be
Palliative radiotherapy for advanced malignancies in a changing oncologic landscape: guiding principles and practice implementation
 Review Article Palliative radiotherapy for advanced malignancies in a changing oncologic landscape: guiding principles and practice implementation Joshua A. Jones, Charles B. Simone II Department of Radiation
Review Article Palliative radiotherapy for advanced malignancies in a changing oncologic landscape: guiding principles and practice implementation Joshua A. Jones, Charles B. Simone II Department of Radiation
