Pattern and outcome of pediatric head injuries in the Suez Canal Region: A follow-up study
|
|
|
- Ronald Ball
- 5 years ago
- Views:
Transcription
1 Original Article Pattern and outcome of pediatric head injuries in the Suez Canal Region: A follow-up study Hoda Atwa 1, Nouran B. AbdAllah 1, Heba Abd El Gawad 2 1 Department of Pediatrics, Faculty of Medicine, Suez Canal University, Suez, Egypt 2 Pediatric Department of Ministry of Health Hospital, Ismailia ABSTRACT Background: A significant number of children sustain a head injury every year. Despite this, few studies in Egypt have provided detailed information about these injuries. Aim: The aim of this study was to investigate the epidemiology and outcome of head injury among children presenting to the emergency department in the Suez Canal University Hospital. Materials and Methods: A clinical follow-up study including 70 patients, aged 18 years or less, who presented to the emergency department, with head injuries, in the period from March 2014 to February Patients were grouped according to their ages into three subgroups: <2, 2 5, and >5 years old. Collected data included patients demographics, causes, severity, timing of injuries, and the eventual outcome after a follow-up period of 3 months. Severity of head injury was based on the general level of consciousness using the Pediatric Glasgow Coma Scale. The functional outcome at final follow-up was assessed using the King s Outcome Scale for Childhood Head Injury. Results: Male-to-female ratio was 1.4 : 1. The highest incidence was in the age group of 2 5 years. The main causes were traffic injury and falls (35.7% for each), followed by home injuries (21%) and sport-related injuries (7%). Regarding the severity of injury, 81% of children had mild injury, 13% had moderate injury, and 6% had severe injury. Concussion was the commonest type of head injury (56%), followed by skull fractures (23%). The functional outcome was assessed at the time of discharge, and 3 months later. Good recovery was achieved in 91% of children; moderate disability was present in 7% of children; and less than 2% of children showed sustained severe disability. Conclusion: Children aged 5 years or less comprised 75% of children who presented to the hospital following head injury. Falls and road traffic accidents were the commonest causes of injury. Most injuries were of mild severity, and concussion was the commonest encountered type of injury. Assessment of functional outcome showed good recovery in most children. Enforcement of strict effective regulations and observing safety measures during driving by authorities is needed to reduce traffic accidents. Health education programs for parents about careful supervision and first aid should be provided to help prevent child head injury and its disastrous consequencest. Received: 14 November 2016, Accepted: 12 January 2017 Key Words: Head injury, pediatric, severity. Corresponding Author: Nouran B. AbdAllah, MD, Department of Pediatrics, Faculty of Medicine, Suez Canal University, Suez, Egypt, Tel.: , nouranboym2@hotmail.com. ISSN: , Vol. 92, No.1 INTRODUCTION Head injury is recognized as a major public health problem that is a frequent cause of death and disability in young people, and makes considerable demands on health services [1]. Traumatic head injury is defined as an acquired injury to the head, caused by an external physical force, resulting in total or partial functional disability or psychosocial impairment, with an associated altered state of consciousness. Types of head injury include scalp injury, skull fracture, concussion, contusion, intracranial or subarachnoid hemorrhage, epidural or subdural hematoma, intraventricular hemor rhage, and diffuse axonal injury [2]. The injury commonly causes a variety of physical, emotional, cognitive, and behavioral impairments [3]. Head injury in children accounts for a large number of emergency department visits and hospital admissions, and remains a major cause of death and disability in children over 1 year of age [2]. Approximately 75% of children admitted to hospitals with injury have a head injury, and 70% of injury deaths are due to head injuries in the USA [4]. In industrialized countries, traumatic brain injuries affect 191/ children annually in persons aged 0 19 years [5]. The WHO notes that 98% of all child injury mortality occurs in the world s poorest countries, and the rate of these deaths is five times higher than among industrialized nations [6]. Children in developing countries are especially vulnerable to injury due to challenging living conditions, increasing road traffic, lack of safe play areas, and absence of childcare options [7,8]. Comprehensive information about pediatric head injuries is necessary for planning management strategies Personal non-commercial use only. EPX copyright All rights reserved DOI: /EPX
2 Pattern and outcome of pediatric head injuries and intervention priorities that can respond effectively and appropriately to local conditions, and is recognized by the WHO as a key priority for strategic research [9-11]. Unfortunately, the epidemiology of pediatric traumatic head injuries is difficult to be adequately described mainly due to inconsistency of the definition and classification. Patients with mild traumatic brain injury may not present to the hospital and the ones who present may be discharged from the emergency department without adequate documentation. Severe injury may result in death at the place of accident. Differences in data collection tools and admission criteria may also cause discrepancies in collected data [12]. In Egypt, besides these difficulties, epidemiological data and updated statistical records for pediatric traumatic head injuries are often lacking and difficult to extract from routinely collected data [13]. In this study, we describe the epidemiology of pediatric head injury in the Suez Canal Region, highlighting on the patient s demographics, nature and etiology of injuries, clinical presentation, and the functional outcome of children attended at the Suez Canal University Hospital suffering head injury. MATERIALS AND METHODS The study is a clinical follow-up study including 70 children aged 18 years or less, who presented at the Emergency Department of Suez Canal University Hospital, Ismailia, Egypt, after sustaining a head injury from March 2014 to February Children were examined at the time of presentation in the emergency department and they were followed up for a 3-month duration. Our hospital is a referral hospital; patients from the whole Suez Canal Region attend the emergency department. Patients were grouped according to their ages into three subgroups: <2, 2 5, and >5 years old. Severity of head injury was based on the general level of consciousness using the Pediatric Glasgow Coma Scale (PGCS) with the following criteria; mild: PGCS of 13 15, and an indication of altered consciousness; moderate: PGCS of 9 12, an indication of altered consciousness and reduced responsiveness; severe: PGCS of 3 8, representing coma or altered consciousness [14]. Inclusion criteria All individuals under 18 years old of both sexes who experienced one or a combination of head trauma were targeted in the study. Head trauma included scalp injury, skull fracture, concussion, contusion, intracranial hemorrhage, penetrating injury, and diffuse axonal injury. Diagnosis was confirmed clinically and radiologically. Exclusion criteria Patients declared dead on arrival, patients with preexisting neurological disorders or bleeding disorders, and child abuse trauma were excluded. The information collected included demographic information (age, sex, residence), information about head injury (time, type, location, cause, and severity of injury), and clinical symptoms (loss of consciousness, vomiting, drowsiness, etc.), computed tomography (CT) findings, further management, and functional outcome at final follow-up using the King s Outcome Scale for Childhood Head Injury [15]. Our sample included all children presenting to the emergency department during the period from March 2014 to February Statistical analysis Statistical analysis was performed using the statistical package for the social sciences (version 20; IBM Corp., Chicago, Illinois, USA). Continuous variables were expressed as mean and SD. Discrete variables were expressed as frequencies and percentages. Quantitative data analysis was performed using χ2-test, Fisher s exact test, and Student s t-test as appropriate. P values of 0.05 or less were regarded as significant. Differences were statistically significant if p value is less than or equal to Ethical consideration Ethical approval declaring agreement with the principles in the Declaration of Helsinki was obtained from the Suez Canal University Ethics Council prior to the study. The parents of children gave their verbal consent to participate in this study. RESULTS Head injuries were most common among boys (41, 59%), with a male/female ratio equal to 1.4 : 1. The highest incidence of head injuries occurred in children aged less than 5 years (53, 75.7%), with most head injuries among the 2 5-year age group (33, 47%). The mean age at injury was 4.29 years (SD=3.9, range: 3 months 16 years). Most children were resident in urban areas (46, 65%). More than half (56%) of the children have had their head injuries outdoors, and most observed injuries (63%) occurred during daytime while children were at play, or during school time. Most children (59%) arrived at hospital by private vehicles, and the remainder (41%) arrived by ambulances. Most children (82%) arrived at hospital accompanied with one of their parents (Table 1). 12
3 Attwa et al.. Table 1: Demographic data of children with head injury, Suez Canal Region, Egypt ( ) Demographic data N=70 [n (%)] Sex Female Male Age (years) <2 2 5 >5 Residency Urban Rural Injury place Outdoors Indoors Injury time Daytime Mode of transport to hospital Private vehicle Ambulance Companion at arrival Parents Relatives or foreigner )41( 29 )59( 41 )28.8( 20 )47( 33 )24.2( 17 )65( 46 )35( 24 )56( 39 )44( 31 )63( 44 )59( 41 )41( 29 )83( 58 )17( 12 There was predominance of falls and road traffic accidents as primary causes of injury, and both resembled the cause of injury in 72% of children. Home injuries were present in 21% of patients, most of them in the 2 5-year age group, while sport-related injuries were the cause in 7% of overall children. There was a significant association between cause and age group (χ2=18.03 and p<0.05) (Table 2). Table 2: Cause of head injury by different age groups, Suez Canal Region, Egypt ( ) Cause of injury Age groups [n (%)] <2 years N(%) 2 5 years N (%) >5 years N (%) Total (N=70) N (%) Road traffic accident 3 (12) 13 (52) 9 (36) 25 (35.7) Fall 14 (56) 10 (40) 1 (4) 25 (35.7) Home injury 3 (20) 7 (47) 5 (33) 15 (21.4) Sport-related 0 (0) 3 (60) 2 (40) 5 (7.1) Total 20 (28.6) 33 (47) 17 (24.2) 70 (100) χ2=18.03, and P=
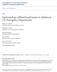
4 Pattern and outcome of pediatric head injuries Concussion was the co mmon est recorded type of head injury, it was pres ent in 56% of cases, followed by skull fractures in 23%, brain contusions and extradural hematoma in 4% for each, and intracerebral hematoma in 3% of children as shown in Fig. 1 Fig. 1: Distribution of types of head injury, Suez Canal Region, Egypt, Regarding severity of head injury, most children (81%) had mild injury, 13% had moderate injury, and 6% had severe injury. Clinically, 64% of patients were fully conscious and alert at presentation with a Glasgow Coma Scale equal to 15. Moderate to severe coma was reported in 19% of patients. Loss of consciousness was reported in 47% of children as presenting manifestation in the emergency room; signs of increased intracranial pressure were present in 41%, deficits including mono/hemiparesis, facial palsy, or aphasia in 11%, signs of lateralization in 10%, and abnormal pupillary response in 9% of children. Most children showed normal CT brain, while 40% of CT studies showed pathological findings in the form of skull fractures (42%), brain edema or brain contusions (14%) for each, extradural or intracerebral hematoma (4%) for each, and subdural hematoma in 4% of these pathological scans. On follow-up, the majority of children (61%) were subjected to a 24-h observation and then discharged; 21% were in need for inpatient ward admission; 12% were critically ill, and were admitted in the ICU. A minority comprising 6% of children were subjected to neurosurgical interventions mainly for evacuation of intracranial bleeding. Functional outcome after head injury was assessed at the time of discharge from hospital, and a final followup after 3 months using the King s Outcome Scale for Childhood Head Injury. It showed the following: 91% of children showed good recovery, 7% showed moderate disability, and less than 2% showed severe disability (Table 3). However, the final functional outcome showed no association with patient s ages or severity of head injury. Table 3: Early and late King s Outcome Scale for Childhood Head Injury (KOSCHI) in relation to different age groups in pediatric head injuries, Suez Canal Region, Egypt, Outcome < 2 Years (n=20) 2-5 Years (n=33) > 5 Years (n=17) Total (n=70) Good Recovery Early Late 20 (100) 20 (100) 24 (72) 28 (84) 14 (82) 16 (94) 58 (83) 64 (91) X2= P = Moderate Disability Early Late 6 (18) 4 (12) 2 (11) 1 (05) 8 (11) 5 (7) X2=0.043 P = Severe Disability Early Late 3 (9) 1 (3) 1 (05) 0 (00) 4 (6) 1 (01) X2=0.312 P = Total Early: 24 hours, Late: 3 months 14
5 Attwa et al.. DISCUSSION Clinical features of head trauma in pediatrics is similar in many countries. However, comprehensive information about regional head trauma epidemiology is necessarily needed for planning management strategies and intervention priorities [1]. Our study comprised all children (n=70) who were attended at the emergency department during the 1-year period from March 2014 to February 2015, in the Suez Canal University Hospital, and suffering head injury. There was some predominance of boys over girls (male/female=1.4 : 1), which is in keeping with other studies throughout the world [15,16]. This can be attributed to the more adventurous and aggressive behavior of boys. The majority of injured children were in the 2 5-year age group. This is possible because in this age, children are more independent and are starting to explore the environment, but may have not yet fully learned to assess the risks in their surroundings [16]. The main causes of injury were traffic injury and falls, and both accounted for about 72%. Traffic injury and falls were the most common causes in other studies, accounting for approximately three-quarters to four-fifths of all head injuries in the studies [17 19]. In our study, falls were frequent in children younger than 2 years old, while traffic injury was frequent in the 2 5-year old age group. Some studies indicated that in younger ages, falling is more common, and there was a positive relation between increasing age and prevalence of motor accident. The vulnerability of children on the street may be because of the relative imbalance of strength and coordination in childhood [18 20]. More than half (56%) of children have had their head injuries outdoors. This is most probably due to the fact that older children spend more time outdoors (e.g. playing), whereas younger ones are mostly confined indoors. Jamison and Kaye found that over half the injuries occurring outdoors occurred mainly with children that are less likely to be under direct parental supervision [21]. Osmond et al. [22] stated that CT of the brain is a valuable investigation tool for the diagnosis and management of pediatric head injuries. In this study, CT scan of the brain was done for all children because the clinical predictors of positive CT findings unfortunately have low sensitivity in pediatrics [23]. About 40% of children had abnormal features in their scans such as skull fracture, brain edema, or hemorrhage. Although this method can help the physician to diagnose more confidently, yet, due to its side effects, special indications for CT scan with the lowest complications in children were set [24]. Concussion was the commonest encountered type of head injury, followed by skull fractures and intracranial bleeds. In most studies, concussion was the predominant type of head injury in children [13,17,25]. However, diagnosis is often challenging because signs and symptoms of concussion can be subtle, and may not be easily identified [26]. In this study, severity of head injuries was distributed as follows: 81% mild, 13% moderate, and 6% had severe head injury in contrast to the study performed in Alexandria University Hospital by Kamel [27]. Mild head injury was present in 50% of the children, moderate in 37%, and severe in 13%. There were statistically significant differences for head injury severity in different age groups. The statistics of the Centers for Disease Control and Prevention of Traumatic Head Injury in USA, in 2013 reported that severity among children ranges between 80 and 90% for mild, 7 8% for moderate, and 5 8% for severe traumatic brain injury [28, 29]. The relation between childhood traumatic head injury and functional outcome is complex, and to a large extent remains unexplained even after grouping children into traditional classifications according to their ages, or the severity of their injury [30]. In our study, the majority of children showed good recovery without any residual deficits. Good recovery was achieved in 91% of children, moderate disability was present in 7% of children, and less than 2% of children showed sustained severe disability. Anderson and colleagues reported that the factors which have been shown to predict the functional outcome were: the severity of injury, location of injury, age at the time of injury, time since injury, family factors, and the premorbid function of the child [31,32]. LIMITATIONS Our study limitations are mainly related to the small sample size and hence the difficulty to study the relationship between the type, severity, and outcome of injury and the sociodemographic characteristics of the children. Also, we did not follow-up our patients in terms of behavioral or cognitive changes. CONCLUSION Children under 5 years of age suffer more frequently head injuries caused by traffic injury and falls. Most injuries were mild in severity, and children did not need significant medical intervention. The majority of children achieved good recovery at the end of follow-up. It is important to minimize all the risk factors in the environment of homes and public areas as possible. There is need for stricter enforcement of laws, especially on the use of protective devices and helmet use, compliance with speed limits, and the development of safe public transportation for the prevention of head injury. Health education programs for parents to improve their knowledge about childhood head injury causes, preventive measures, and first aid should be implemented to emphasize the importance of parental/ caregivers supervision. 15
6 Pattern and outcome of pediatric head injuries CONFLICT OF INTEREST There are no conflicts of interest. REFERENCES 1. Danov R. Pediatric traumatic head injuries. In: Slobounov S, Sebastianelli WJ, editors. Foundations of sport-related brain injuries. Boston, MA: Springer US; pp Parkin P, Maguire J. Clinically important head injuries after head trauma in children. Lancet 2009; 374: Sumich AI, Nelson MR, McDeavitt JT. Traumatic brain injury: a Pediatric Perspective. In: Zasler N, Katz DI, Zafonte RD, editors. Brain injury medicine: principles and Practice. New York, NY: Demos Medical Publishing; pp Jagannathan J, Okonkwo D. Long-term outcomes and prognostic factors in pediatric patients with severe traumatic brain injury. J Neurosurg Pediatr 2008; 2: Quayle K, Holmes J, Kuppermann N. Epidemiology of blunt head trauma in children in U.S. emergency departments. N Engl J Med 2014; 371: Arias E, MacDorman MF, Strobino DM. Annual summary of vital statistics. Pediatrics 2003; 112: Keenan HT, Bratton SL. Epidemiology and outcomes of pediatric traumatic brain injury. Dev Neurosci 2006; 28: Collins C, Comstock R. Epidemiology of pediatric injuries presenting to emergency department. Pediatrics 2010; 125: Husum H, Wisborg T. Rural prehospital trauma systems improve trauma outcome in low-income countries. J Trauma 2003; 54: World Health Organization. International Classification of Functioning, Disability and Health. Geneva, Switzerland: WHO; Critchley G, Memon A. Epidemiology of head injury. In: Whitfield P, Thomas E, editors Head injury: a multidisciplinary approach. Cambridge, UK: Cambridge University Press; pp Montaser T, Hasan A, Ibrahim A. Epidemiology of moderate and severe traumatic brain injury in Cairo University Hospital in Scand J Trauma Resusc Emerg Med 2013; 21(Suppl 2): Halawa EF, Barakat A, Ibrahim H, Moawad E. Epidemiology of non-fatal injuries among Egyptian children:a community based cross-sectional survey. BMC Public Health 2015; 15: Anderson V, Catroppa C, Haritou F. Identifying factors contributing to child and family outcome in children. J Neurol Neurosurg Psychiatry 2005; 76: Crouchman M, Rossiter L, Colaco T. A practical outcome scale for pediatric head injury. Arch Dis Child 2001; 84: Yeates KO, Taylor HG. Neurobehavioural outcomes of head injury in children and adolescents. Pediatr Rehabil 2005; 8: Elsayed HF, Zekry MO, Abbas HM, Abdelhamid S, Hyder A. Pattern and severity of childhood unintentional injuries in Ismailia city, Egypt. Afr Saf Promot J 2012; 10: World Health Organization and Ministry of Health (Egypt). Injury surveillance: a tool for decision making. Annual Injury Surveillance Report, Egypt. Geneva, Switzerland: WHO; Razzak J, Luby S, Laflamme L, Chotani H. Injuries among children in Karachi, Pakistan, what, where and how. Public Health 2004; 118: Paget SP, Beath AW, Barnes EH, Waugh MC. Use of King s Outcome Scale for Childhood Head Injury in the evaluation of outcome in childhood traumatic brain injury. Dev Neurorehabil 2012; 15: Jamison DL, Kaye HH. Accidental head injury in childhood. Arch Dis Child. 1974;49: Osmond M, Klassen T, Wells G. A clinical decision rule for the use of computed tomography in children with minor head injury. CMAJ 2010; 182: Maguire J, Boutis K, Uleryk E. Should a head injured child receive a head CT scan? A systematic review of clinical prediction rules. Pediatrics 2009; 124: Atci B, Albayrak S, Durda E. Retrospective analysis of patients admitted to the emergency department with head trauma within 2 years. Internet J Emerg Med 2013; 8: Mahapatra A. Head injury in children. In: Mahapatra 16
7 Attwa et al.. A, Kamal R, editors. A text book of head injury. Delhi, India: Modern Publications; pp Bazarian J, Veenema T, Brayer A. Knowledge of concussion guidelines among practitioners caring for children. Clin Pediatr 2001; 40: Kamel HE. Study of head injuries in young children [Thesis]. Alexandria, Egypt: Faculty of Medicine, Alexandria University; Mannix R, Florence TB, Lois K. Neuroimaging for pediatric head trauma: do patient and hospital characteristics influence who gets imaged? Acad Emerg Med 2010; 17: Centers for Disease Control and Prevention. National Center For Injury Control And Prevention: how many people have TBI?; 2013 [cited 2016 Dec 12]. Available at: http// brain injury/statistics. 30. Dhandapani SS, Manju D, Mahapatra AK. Prognostic significance of age in traumatic brain injury. J Neurosci Rural Pract 2012; 3: Taylor G. Research on outcomes of pediatric traumatic brain injury. Dev Neuropsychol 2004; 25: Anderson V, Spencer-Smith M, Leventer R. Childhood brain insult: can age at insult help us predict outcome? Brain 2009; 132:
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Pediatric head trauma: the evidence regarding indications for emergent neuroimaging
 DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study of Paediatric Head Injuries and Its Outcome Raje Vinayak, Raje Vaishali, Pednekar Akshay,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study of Paediatric Head Injuries and Its Outcome Raje Vinayak, Raje Vaishali, Pednekar Akshay,
Analysis of pediatric head injury from falls
 Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
PEDIATRIC MILD TRAUMATIC HEAD INJURY
 PEDIATRIC MILD TRAUMATIC HEAD INJURY October 2011 Quality Improvement Resources Illinois Emergency Medical Services for Children is a collaborative program between the Illinois Department of Public Health
PEDIATRIC MILD TRAUMATIC HEAD INJURY October 2011 Quality Improvement Resources Illinois Emergency Medical Services for Children is a collaborative program between the Illinois Department of Public Health
Systematic Review. General Paediatric Concussion Search. OVID Medline: 1. exp Brain Concussion/ 2. concuss$.tw.
 Systematic Review General Paediatric Concussion Search OVID : 1. exp Brain Concussion/ 2. concuss$.tw. 3. ((mild or minor or minimal) adj (traumatic brain or tbi)).tw. 4. mtbi.tw 5. exp Brain Injury/ 6.
Systematic Review General Paediatric Concussion Search OVID : 1. exp Brain Concussion/ 2. concuss$.tw. 3. ((mild or minor or minimal) adj (traumatic brain or tbi)).tw. 4. mtbi.tw 5. exp Brain Injury/ 6.
Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. Railway accidents injured pedal cyclist
 Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. ICD Code ICD-9 E800-E807(.3) E810-E816, E818-E819(.6) E820-E825(.6) E826-E829(.1) ICD-10-CA V10-V19 (including all
Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. ICD Code ICD-9 E800-E807(.3) E810-E816, E818-E819(.6) E820-E825(.6) E826-E829(.1) ICD-10-CA V10-V19 (including all
Author Manuscript. Received Date : 27-Oct Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 Received Date : 27-Oct-2016 Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017 Article type ABSTRACT : Original Contribution
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 Received Date : 27-Oct-2016 Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017 Article type ABSTRACT : Original Contribution
The significance of traumatic haematoma in the
 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
O ne million patients are treated annually in United
 859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
Can we abolish skull x-rays for head injury?
 ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
Phenytoin versus Levetiracetam for Prevention of Early Posttraumatic Seizures: A Prospective Comparative Study
 136 Original Article Phenytoin versus Levetiracetam for Prevention of Early Posttraumatic Seizures: A Prospective Comparative Study Kairav S. Shah 1 Jayun Shah 1 Ponraj K. Sundaram 1 1 Department of Neurosurgery,
136 Original Article Phenytoin versus Levetiracetam for Prevention of Early Posttraumatic Seizures: A Prospective Comparative Study Kairav S. Shah 1 Jayun Shah 1 Ponraj K. Sundaram 1 1 Department of Neurosurgery,
Research Article Analysis of Repeated CT Scan Need in Blunt Head Trauma
 Hindawi Publishing Corporation Emergency Medicine International Volume 2013, Article ID 916253, 5 pages http://dx.doi.org/10.1155/2013/916253 Research Article Analysis of Repeated CT Scan Need in Blunt
Hindawi Publishing Corporation Emergency Medicine International Volume 2013, Article ID 916253, 5 pages http://dx.doi.org/10.1155/2013/916253 Research Article Analysis of Repeated CT Scan Need in Blunt
Correlation of Computed Tomography findings with Glassgow Coma Scale in patients with acute traumatic brain injury
 Journal of College of Medical Sciences-Nepal, 2014, Vol-10, No-2 ABSTRACT OBJECTIVE To correlate Computed Tomography (CT) findings with Glasgow Coma Scale (GCS) in patients with acute traumatic brain injury
Journal of College of Medical Sciences-Nepal, 2014, Vol-10, No-2 ABSTRACT OBJECTIVE To correlate Computed Tomography (CT) findings with Glasgow Coma Scale (GCS) in patients with acute traumatic brain injury
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Pediatric Traumatic Brain Injury. Seth Warschausky, PhD Department of Physical Medicine and Rehabilitation University of Michigan
 Pediatric Traumatic Brain Injury Seth Warschausky, PhD Department of Physical Medicine and Rehabilitation University of Michigan Modules Module 1: Overview Module 2: Cognitive and Academic Needs Module
Pediatric Traumatic Brain Injury Seth Warschausky, PhD Department of Physical Medicine and Rehabilitation University of Michigan Modules Module 1: Overview Module 2: Cognitive and Academic Needs Module
Factors associated with Outcome in Patients Admitted with Traumatic Brain Injury at the University Teaching Hospital, Lusaka, Zambia
 ORIGINAL ARTICLE Factors associated with Outcome in Patients Admitted with Traumatic Brain Injury at the University Teaching Hospital, Lusaka, Zambia K. Mwala, J.C Munthali, L. Chikoya Department of Surgery,
ORIGINAL ARTICLE Factors associated with Outcome in Patients Admitted with Traumatic Brain Injury at the University Teaching Hospital, Lusaka, Zambia K. Mwala, J.C Munthali, L. Chikoya Department of Surgery,
Instructional Course #34. Review of Neuropharmacology in Pediatric Brain Injury. John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD
 Instructional Course #34 Review of Neuropharmacology in Pediatric Brain Injury John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD Outline of Course 1. Introduction John Pelegano MD 2. Neuropharmocologic
Instructional Course #34 Review of Neuropharmacology in Pediatric Brain Injury John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD Outline of Course 1. Introduction John Pelegano MD 2. Neuropharmocologic
PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES
 PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES INTRODUCTION: Traumatic Brain Injury (TBI) is an important clinical entity in acute care surgery without well-defined guidelines
PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES INTRODUCTION: Traumatic Brain Injury (TBI) is an important clinical entity in acute care surgery without well-defined guidelines
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Mild Traumatic Brain Injury
 Mild Traumatic Brain Injury Concussions This presentation is for information purposes only, not for any commercial purpose, and may not be sold or redistributed. David Wesley, M.D. Outline Epidemiology
Mild Traumatic Brain Injury Concussions This presentation is for information purposes only, not for any commercial purpose, and may not be sold or redistributed. David Wesley, M.D. Outline Epidemiology
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Correspondence should be addressed to Sorayouth Chumnanvej;
 Neurology Research International Volume 2016, Article ID 2737028, 7 pages http://dx.doi.org/10.1155/2016/2737028 Research Article Assessment and Predicting Factors of Repeated Brain Computed Tomography
Neurology Research International Volume 2016, Article ID 2737028, 7 pages http://dx.doi.org/10.1155/2016/2737028 Research Article Assessment and Predicting Factors of Repeated Brain Computed Tomography
Head Injury: Classification Most Severe to Least Severe
 Head Injury: Classification Most Severe to Least Severe Douglas I. Katz, MD Professor, Dept. Neurology, Boston University School of Medicine, Boston MA Medical Director Brain Injury Program, HealthSouth
Head Injury: Classification Most Severe to Least Severe Douglas I. Katz, MD Professor, Dept. Neurology, Boston University School of Medicine, Boston MA Medical Director Brain Injury Program, HealthSouth
BACKGROUND AND SCIENTIFIC RATIONALE. Protocol Code: ISRCTN V 1.0 date 30 Jan 2012
 BACKGROUND AND SCIENTIFIC RATIONALE Protocol Code: ISRCTN15088122 V 1.0 date 30 Jan 2012 Traumatic Brain Injury 10 million killed or hospitalised every year 90% in low and middle income countries Mostly
BACKGROUND AND SCIENTIFIC RATIONALE Protocol Code: ISRCTN15088122 V 1.0 date 30 Jan 2012 Traumatic Brain Injury 10 million killed or hospitalised every year 90% in low and middle income countries Mostly
Head injury in children
 Head injury in children Michael Kim, MD Department of Emergency Medicine University of Wisconsin- Madison #1 cause of death and disability Bimodal distribution 62,000 hospitalization 564,000 ED visits
Head injury in children Michael Kim, MD Department of Emergency Medicine University of Wisconsin- Madison #1 cause of death and disability Bimodal distribution 62,000 hospitalization 564,000 ED visits
Concussion. Concussion is a disturbance of brain function caused by a direct or indirect force to the head.
 Concussion Concussion is a disturbance of brain function caused by a direct or indirect force to the head. Disturbances of brain tissue is largely related to neurometabolic dysfunction rather then structural
Concussion Concussion is a disturbance of brain function caused by a direct or indirect force to the head. Disturbances of brain tissue is largely related to neurometabolic dysfunction rather then structural
Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
A bout million patients present to UK hospitals
 420 ORIGINAL ARTICLE Application of the Canadian CT head rules in managing minor head injuries in a UK emergency department: implications for the implementation of the NICE guidelines H Y Sultan, A Boyle,
420 ORIGINAL ARTICLE Application of the Canadian CT head rules in managing minor head injuries in a UK emergency department: implications for the implementation of the NICE guidelines H Y Sultan, A Boyle,
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 Through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 Through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
A Comprehensive Study on Post Traumatic Temporal Contusion in Adults
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/318 A Comprehensive Study on Post Traumatic Temporal Contusion in Adults R Renganathan 1, P John Paul 2, Heber Anandan
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/318 A Comprehensive Study on Post Traumatic Temporal Contusion in Adults R Renganathan 1, P John Paul 2, Heber Anandan
A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage
 July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score
 Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
Overview of Abusive Head Trauma: What Everyone Needs to Know. 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012
 Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Kristin s Head Trauma Board Questions 11/07/14
 Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
STUDY OF C-REACTIVE PROTEIN IN ACUTE ISCHEMIC STROKE Medhini V. J 1, Hally Karibasappa 2
 STUDY OF C-REACTIVE PROTEIN IN ACUTE ISCHEMIC STROKE Medhini V. J 1, Hally Karibasappa 2 HOW TO CITE THIS ARTICLE: Medhini V. J, Hally Karibasappa. Study of C-Reactive Protein in Acute Ischemic Stroke.
STUDY OF C-REACTIVE PROTEIN IN ACUTE ISCHEMIC STROKE Medhini V. J 1, Hally Karibasappa 2 HOW TO CITE THIS ARTICLE: Medhini V. J, Hally Karibasappa. Study of C-Reactive Protein in Acute Ischemic Stroke.
GUIDELINES FOR THE MANAGEMENT OF HEAD INJURIES IN REMOTE AND RURAL ALASKA
 GUIDELINES FOR THE MANAGEMENT OF HEAD INJURIES IN REMOTE AND RURAL ALASKA Approximately 800 patients with head injuries die or are hospitalized in the state of Alaska each year 1. In addition, thousands
GUIDELINES FOR THE MANAGEMENT OF HEAD INJURIES IN REMOTE AND RURAL ALASKA Approximately 800 patients with head injuries die or are hospitalized in the state of Alaska each year 1. In addition, thousands
The New England Journal of Medicine A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES
 A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES JOHN F. ANNEGERS, PH.D., W. ALLEN HAUSER, M.D., SHARON P. COAN, M.S., AND WALTER A. ROCCA, M.D., M.P.H. ABSTRACT Background The risk
A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES JOHN F. ANNEGERS, PH.D., W. ALLEN HAUSER, M.D., SHARON P. COAN, M.S., AND WALTER A. ROCCA, M.D., M.P.H. ABSTRACT Background The risk
Clarifying Murky Waters: Head Injuries in Children
 Clarifying Murky Waters: Head Injuries in Children Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Emergency Services 1 Case #1: Newborn Leo 2 month old dropped 4 feet onto
Clarifying Murky Waters: Head Injuries in Children Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Emergency Services 1 Case #1: Newborn Leo 2 month old dropped 4 feet onto
Head injuries in children. Dr Jason Hort Paediatrician Paediatric Emergency Physician, June 2017 Children s Hospital Westmead
 Head injuries in children Dr Jason Hort Paediatrician Paediatric Emergency Physician, June 2017 Children s Hospital Westmead Objectives Approach to minor head injury Child protection issues Concussion
Head injuries in children Dr Jason Hort Paediatrician Paediatric Emergency Physician, June 2017 Children s Hospital Westmead Objectives Approach to minor head injury Child protection issues Concussion
The prognostic value of injury severity, location of event, and age at injury in pediatric traumatic head injuries
 ORIGINAL RESEARCH The prognostic value of injury severity, location of event, and age at injury in pediatric traumatic head injuries Jonas G Halldorsson 1 Kjell M Flekkoy 2 Gudmundur B Arnkelsson 3 Kristinn
ORIGINAL RESEARCH The prognostic value of injury severity, location of event, and age at injury in pediatric traumatic head injuries Jonas G Halldorsson 1 Kjell M Flekkoy 2 Gudmundur B Arnkelsson 3 Kristinn
Traumatic brain injury (TBI) is a major cause of mortality, cognitive and
 Disorder: Traumatic Brain Injury (TBI) Essay Title: Paediatric Traumatic Brain Injury (TBI) Title: Associate Professor Name: Cathy Surname: Catroppa Qualifications: BBSc., DipEdPsych., M.Ed.Psych., PhD
Disorder: Traumatic Brain Injury (TBI) Essay Title: Paediatric Traumatic Brain Injury (TBI) Title: Associate Professor Name: Cathy Surname: Catroppa Qualifications: BBSc., DipEdPsych., M.Ed.Psych., PhD
Conceptualization of Functional Outcomes Following TBI. Ryan Stork, MD
 Conceptualization of Functional Outcomes Following TBI Ryan Stork, MD Conceptualization of Functional Outcomes Following Traumatic Brain Injury Ryan Stork, MD Clinical Lecturer Brain Injury Medicine &
Conceptualization of Functional Outcomes Following TBI Ryan Stork, MD Conceptualization of Functional Outcomes Following Traumatic Brain Injury Ryan Stork, MD Clinical Lecturer Brain Injury Medicine &
Pediatric Abusive Head Trauma
 Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
TITLE: Optimal Oxygen Saturation Range for Adults Suffering from Traumatic Brain Injury: A Review of Patient Benefit, Harms, and Guidelines
 TITLE: Optimal Oxygen Saturation Range for Adults Suffering from Traumatic Brain Injury: A Review of Patient Benefit, Harms, and Guidelines DATE: 11 April 2014 CONTEXT AND POLICY ISSUES Traumatic brain
TITLE: Optimal Oxygen Saturation Range for Adults Suffering from Traumatic Brain Injury: A Review of Patient Benefit, Harms, and Guidelines DATE: 11 April 2014 CONTEXT AND POLICY ISSUES Traumatic brain
Head trauma is a common chief complaint among children visiting
 Discussions in Surgery Validation of the Sainte-Justine Head Trauma Pathway for children younger than two years of age Sarah Spénard Serge Gouin, MDCM Marianne Beaudin, MD Jocelyn Gravel, MD, MSc Partial
Discussions in Surgery Validation of the Sainte-Justine Head Trauma Pathway for children younger than two years of age Sarah Spénard Serge Gouin, MDCM Marianne Beaudin, MD Jocelyn Gravel, MD, MSc Partial
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Language After Traumatic Brain Injury
 Chapter 7 Language After Traumatic Brain Injury 10/24/05 COMD 326, Chpt. 7 1 1 10/24/05 COMD 326, Chpt. 7 2 http://www.californiaspinalinjurylawyer.com/images/tbi.jpg 2 TBI http://www.conleygriggs.com/traumatic_brain_injury.shtml
Chapter 7 Language After Traumatic Brain Injury 10/24/05 COMD 326, Chpt. 7 1 1 10/24/05 COMD 326, Chpt. 7 2 http://www.californiaspinalinjurylawyer.com/images/tbi.jpg 2 TBI http://www.conleygriggs.com/traumatic_brain_injury.shtml
Index. Note: Page numbers of article titles are in bold face type.
 Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
TBI are twice as common in males High potential for poor outcome Deaths occur at three points in time after injury
 Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
To date, head injury remains the leading cause of. Outcome in patients with blunt head trauma and a Glasgow Coma Scale score of 3 at presentation
 J Neurosurg 111:683 687, 2009 Outcome in patients with blunt head trauma and a Glasgow Coma Scale score of 3 at presentation Clinical article Ro u k o z B. Ch a m o u n, M.D., Cl a u d i a S. Ro b e r
J Neurosurg 111:683 687, 2009 Outcome in patients with blunt head trauma and a Glasgow Coma Scale score of 3 at presentation Clinical article Ro u k o z B. Ch a m o u n, M.D., Cl a u d i a S. Ro b e r
102 Results RESULTS. Age Mean=S.D Range 42= years -84 years Number % <30 years years >50 years
 102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
Children diagnosed with skull fractures are often. Transfer of children with isolated linear skull fractures: is it worth the cost?
 clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
Epidemiology of blunt head trauma in children in U.S. Emergency Departments
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2014 Epidemiology of blunt head trauma in children in U.S. Emergency Departments Kimberly S. Quayle Washington University
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2014 Epidemiology of blunt head trauma in children in U.S. Emergency Departments Kimberly S. Quayle Washington University
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
Predicting the need for operation in the patient with an occult traumatic intracranial hematoma
 J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Traumatic head injury (THI) is a prevalent condition
 PEDIATRICS clinical article J Neurosurg Pediatr 15:529 534, 2015 Magnetic resonance imaging as an alternative to computed tomography in select patients with traumatic brain injury: a retrospective comparison
PEDIATRICS clinical article J Neurosurg Pediatr 15:529 534, 2015 Magnetic resonance imaging as an alternative to computed tomography in select patients with traumatic brain injury: a retrospective comparison
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision
 Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Objectives. Incidence TBI: Leading cause of death & disability due to trauma. 9th Annual NKY TBI Conference 3/27/2015
 Mild Traumatic Brain Injury & Symptom Assessment in Children Becky Cook, DNP, APRN Trauma Nurse Practitioner Objectives Discuss the incidence and mechanisms of injury of mild traumatic brain injury (mtbi)
Mild Traumatic Brain Injury & Symptom Assessment in Children Becky Cook, DNP, APRN Trauma Nurse Practitioner Objectives Discuss the incidence and mechanisms of injury of mild traumatic brain injury (mtbi)
Correlation of D-Dimer level with outcome in traumatic brain injury
 2014; 17 (1) Original Article Correlation of D-Dimer level with outcome in traumatic brain injury Pradip Prasad Subedi 1, Sushil Krishna Shilpakar 2 Email: Abstract Introduction immense. The major determinant
2014; 17 (1) Original Article Correlation of D-Dimer level with outcome in traumatic brain injury Pradip Prasad Subedi 1, Sushil Krishna Shilpakar 2 Email: Abstract Introduction immense. The major determinant
Chapter 2 Triage. Introduction. The Trauma Team
 Chapter 2 Triage Chapter 2 Triage Introduction Existing trauma courses focus on a vertical or horizontal approach to the ABCDE assessment of an injured patient: A - Airway B - Breathing C - Circulation
Chapter 2 Triage Chapter 2 Triage Introduction Existing trauma courses focus on a vertical or horizontal approach to the ABCDE assessment of an injured patient: A - Airway B - Breathing C - Circulation
Evaluation of Craniocerebral Trauma Using Computed Tomography
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 9 Ver. IV (Sep. 2014), PP 57-62 Evaluation of Craniocerebral Trauma Using Computed Tomography
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 9 Ver. IV (Sep. 2014), PP 57-62 Evaluation of Craniocerebral Trauma Using Computed Tomography
Prognostic indicators of childhood acute viral encephalitis
 ecommons@aku Community Health Sciences Department of Community Health Sciences December 1999 Prognostic indicators of childhood acute viral encephalitis E Bhutto Aga Khan University M Naim Aga Khan University
ecommons@aku Community Health Sciences Department of Community Health Sciences December 1999 Prognostic indicators of childhood acute viral encephalitis E Bhutto Aga Khan University M Naim Aga Khan University
ARTICLE. Intracranial Hemorrhage in Children Younger Than 3 Years
 Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Mini Research Paper: Traumatic Brain Injury. Allison M McGee. Salt Lake Community College
 Running Head: Mini Research Paper: Traumatic Brain Injury Mini Research Paper: Traumatic Brain Injury Allison M McGee Salt Lake Community College Abstract A Traumatic Brain Injury (also known as a TBI)
Running Head: Mini Research Paper: Traumatic Brain Injury Mini Research Paper: Traumatic Brain Injury Allison M McGee Salt Lake Community College Abstract A Traumatic Brain Injury (also known as a TBI)
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Cognitive Rehabilitation with Current Research and Transition of Care
 Cognitive Rehabilitation with Current Research and Transition of Care Mike Dichiaro, MD Pediatric Rehabilitation Medicine Carin Rowan, MPT Pediatric Physical Therapy Financial Disclosures No relevant financial
Cognitive Rehabilitation with Current Research and Transition of Care Mike Dichiaro, MD Pediatric Rehabilitation Medicine Carin Rowan, MPT Pediatric Physical Therapy Financial Disclosures No relevant financial
Copyright 2009 ACNN 1
 1 The focus of this information is children who have previously been evaluated and have an established diagnosis of concussion. The information contained herein is not intended for acute concussion management.
1 The focus of this information is children who have previously been evaluated and have an established diagnosis of concussion. The information contained herein is not intended for acute concussion management.
9/16/2018. Recognizing & Managing Seizures in Pediatric TBI. Objectives. Definitions and Epidemiology
 Recognizing & Managing Seizures in Pediatric TBI UW Medicine EMS & Trauma 2018 Conference September 17 and 18, 2018 Mark Wainwright MD PhD Herman and Faye Sarkowsky Professor of Neurology Division Head,
Recognizing & Managing Seizures in Pediatric TBI UW Medicine EMS & Trauma 2018 Conference September 17 and 18, 2018 Mark Wainwright MD PhD Herman and Faye Sarkowsky Professor of Neurology Division Head,
Continuum of Care: Post Acute Brain Injury Rehabilitation
 Continuum of Care: Post Acute Brain Injury Rehabilitation Laura Wiggs, PT, NCS, CBIS Mentis Neuro Rehabilitation Traumatic Brain Injury (TBI) When an outside mechanical force is applied to the head and
Continuum of Care: Post Acute Brain Injury Rehabilitation Laura Wiggs, PT, NCS, CBIS Mentis Neuro Rehabilitation Traumatic Brain Injury (TBI) When an outside mechanical force is applied to the head and
Table 3.1: Canadian Stroke Best Practice Recommendations Screening and Assessment Tools for Acute Stroke Severity
 Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Catastrophically Injured Children
 Catastrophically Injured Children The Challenges of Assessment, Treatment & Evaluation Through Development Dr. P. Rumney September 2011 Catastrophic Injury Legal & Not Medical definition Adult tools used
Catastrophically Injured Children The Challenges of Assessment, Treatment & Evaluation Through Development Dr. P. Rumney September 2011 Catastrophic Injury Legal & Not Medical definition Adult tools used
Children under the SABS: TBI
 Children under the SABS: TBI Thanks to my colleague and fellow Expert Panelist Dr. Peter Rumney, whose slide template and slide contents I have shamelessly plagiarized. Thanks to my colleague and fellow
Children under the SABS: TBI Thanks to my colleague and fellow Expert Panelist Dr. Peter Rumney, whose slide template and slide contents I have shamelessly plagiarized. Thanks to my colleague and fellow
Supplementary Online Content
 Supplementary Online Content Cooper DJ, Nichol A, Bailey M, et al. Effect of early sustained prophylactic hypothermia on neurologic outcomes among patients with severe traumatic brain injury: the POLAR
Supplementary Online Content Cooper DJ, Nichol A, Bailey M, et al. Effect of early sustained prophylactic hypothermia on neurologic outcomes among patients with severe traumatic brain injury: the POLAR
HEAD INJURIES IN INFANTS (0-1 YEARS)
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2017 vol. 121, no. 2 SURGERY ORIGINAL PAPERS HEAD INJURIES IN INFANTS (0-1 YEARS) D. Voinescu 1, V. Saceleanu 2 *, I. Luca-Husti 3, I. Rusu 5, A.V. Ciurea 3,4 Carol
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2017 vol. 121, no. 2 SURGERY ORIGINAL PAPERS HEAD INJURIES IN INFANTS (0-1 YEARS) D. Voinescu 1, V. Saceleanu 2 *, I. Luca-Husti 3, I. Rusu 5, A.V. Ciurea 3,4 Carol
Virtual Mentor American Medical Association Journal of Ethics August 2008, Volume 10, Number 8:
 Virtual Mentor American Medical Association Journal of Ethics August 2008, Volume 10, Number 8: 516-520. CLINICAL PEARL The Hazards of Stopping a Brain in Motion: Evaluation and Classification of Traumatic
Virtual Mentor American Medical Association Journal of Ethics August 2008, Volume 10, Number 8: 516-520. CLINICAL PEARL The Hazards of Stopping a Brain in Motion: Evaluation and Classification of Traumatic
Disclosure Statement. Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk.
 Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
CORE STANDARDS STANDARDS USED IN TARN REPORTS
 CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
Part 2: Prognosis in Penetrating Brain Injury
 Part 2: Prognosis in Penetrating Brain Injury J Trauma. 2001;51:S44 S86. INTRODUCTION AND METHODOLOGY Part 2 of this document presents early clinical indicators that may be prognostic of outcome among
Part 2: Prognosis in Penetrating Brain Injury J Trauma. 2001;51:S44 S86. INTRODUCTION AND METHODOLOGY Part 2 of this document presents early clinical indicators that may be prognostic of outcome among
Andrzej Żyluk 1, Agnieszka Mazur 1, Bernard Piotuch 1, Krzysztof Safranow 2
 POLSKI PRZEGLĄD CHIRURGICZNY 2013, 85, 12, 699 705 10.2478/pjs-2013-0107 Analysis of the reliability of clinical examination in predicting traumatic cerebral lesions and skull fractures in patients with
POLSKI PRZEGLĄD CHIRURGICZNY 2013, 85, 12, 699 705 10.2478/pjs-2013-0107 Analysis of the reliability of clinical examination in predicting traumatic cerebral lesions and skull fractures in patients with
NC DETECT Stroke Advisory Council November 1, 2018
 NC DETECT Stroke Advisory Council November 1, 2018 https://ncdetect.org amy_ising@med.unc.edu 2018 University of North Carolina at Chapel Hill and NC Division of Public Health, NC DHHS NC DETECT Background
NC DETECT Stroke Advisory Council November 1, 2018 https://ncdetect.org amy_ising@med.unc.edu 2018 University of North Carolina at Chapel Hill and NC Division of Public Health, NC DHHS NC DETECT Background
Summary of Pediatric Trauma Patients
 Santa Rosa Memorial Hospital Trauma Services Summary of Pediatric Trauma Patients Reporting Dates Jan 1, 2004 May 31, 2006 The mission of the Santa Rosa Memorial Hospital Trauma Services is to provide
Santa Rosa Memorial Hospital Trauma Services Summary of Pediatric Trauma Patients Reporting Dates Jan 1, 2004 May 31, 2006 The mission of the Santa Rosa Memorial Hospital Trauma Services is to provide
Extradural hematoma (EDH) accounts for 2% of all head injuries (1). In
 CASE REPORT Conservative management of extradural hematoma: A report of sixty-two cases A. Rahim H. Zwayed 1, Brandon Lucke-Wold 2 Zwayed ARH, Lucke-wold B. Conservative management of extradural hematoma:
CASE REPORT Conservative management of extradural hematoma: A report of sixty-two cases A. Rahim H. Zwayed 1, Brandon Lucke-Wold 2 Zwayed ARH, Lucke-wold B. Conservative management of extradural hematoma:
THOMAS G. SAUL, M.D., THOMAS B. DUCKER, M.D., MICHAEL SALCMAN, M.D., AND ERIC CARRO, M.D.
 J Neurosurg 54:596-600, 1981 Steroids in severe head injury A prospective randomized clinical trial THOMAS G. SAUL, M.D., THOMAS B. DUCKER, M.D., MICHAEL SALCMAN, M.D., AND ERIC CARRO, M.D. Department
J Neurosurg 54:596-600, 1981 Steroids in severe head injury A prospective randomized clinical trial THOMAS G. SAUL, M.D., THOMAS B. DUCKER, M.D., MICHAEL SALCMAN, M.D., AND ERIC CARRO, M.D. Department
School of Hard Knocks! Richard Beebe MS RN NRP MedicThink LLC
 School of Hard Knocks! Richard Beebe MS RN NRP MedicThink LLC Fall of a Teton How Bad is He Hurt? What REALLY happened inside Johnny s head? How common are these types of injuries? PONDER THIS What part
School of Hard Knocks! Richard Beebe MS RN NRP MedicThink LLC Fall of a Teton How Bad is He Hurt? What REALLY happened inside Johnny s head? How common are these types of injuries? PONDER THIS What part
The determination of eligible population for this measure requires administrative claims data.
 Overuse of Imaging Measure 6: Ratio of Magnetic Resonance Imaging Scans to Computed Tomography Scans for the Evaluation of Children with Atraumatic Headache Description This measure assesses the ratio
Overuse of Imaging Measure 6: Ratio of Magnetic Resonance Imaging Scans to Computed Tomography Scans for the Evaluation of Children with Atraumatic Headache Description This measure assesses the ratio
Clinical malnutrition in severe traumatic brain injury: Factors associated and outcome at 6 months
 Original Article Indian Journal of Neurotrauma (IJNT) 35 2007, Vol. 4, No. 1, pp. 35-39 Clinical malnutrition in severe traumatic brain injury: Factors associated and outcome at 6 months SS Dhandapani
Original Article Indian Journal of Neurotrauma (IJNT) 35 2007, Vol. 4, No. 1, pp. 35-39 Clinical malnutrition in severe traumatic brain injury: Factors associated and outcome at 6 months SS Dhandapani
Severe trauma presenting to the resuscitation room of a Hong Kong emergency department
 Hong Kong Journal of Emergency Medicine Severe trauma presenting to the resuscitation room of a Hong Kong emergency department TH Rainer, SY Chan, K Kwok, DTK Suen, W Lam, RA Cocks Background: Little is
Hong Kong Journal of Emergency Medicine Severe trauma presenting to the resuscitation room of a Hong Kong emergency department TH Rainer, SY Chan, K Kwok, DTK Suen, W Lam, RA Cocks Background: Little is
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Outcome of severe traumatic brain injury at a critical care unit: a review of 87 patients
 Original Article Outcome of severe traumatic brain injury at a critical care unit: a review of 87 patients E.A. Opondo, MBChB, MMed (Surg), General surgeon, North Kinangop Mission Hospital, Surgery Department
Original Article Outcome of severe traumatic brain injury at a critical care unit: a review of 87 patients E.A. Opondo, MBChB, MMed (Surg), General surgeon, North Kinangop Mission Hospital, Surgery Department
Traumatic Brain Injury
 General Information Traumatic Brain Injury What you need to know Complicated condition with high variability in etiology, severity, distribution of injury, and pattern of functional impairment (Klyce,
General Information Traumatic Brain Injury What you need to know Complicated condition with high variability in etiology, severity, distribution of injury, and pattern of functional impairment (Klyce,
ISSN X (Print) Research Article
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(5D):1760-1764 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(5D):1760-1764 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
2/13/13. Ann S. Botash, MD SUNY Upstate Medical University
 Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
