TOTW Burns in children October 2007
|
|
|
- Charleen Lambert
- 5 years ago
- Views:
Transcription
1 TOTW Burns in children October 2007 A J Pittaway FRCA Andrew.pittaway@seattlechildrens.org Before reading the tutorial, consider this case scenario and answer the following questions (answers & discussion follow): A 5 year old boy is brought to your hospital at midnight from a housefire. He had been rescued from his upstairs bedroom by a neighbour who had subsequently jumped to the ground with him. His rescuer, who suffered a fractured ankle, tells you that when he found him in his smoke-filled room, he was deeply asleep and his sheets were smouldering. On examination he is sleepy but rouseable and cries when disturbed. His pyjamas are charred across the chest and left arm. His respiratory rate is 25/min, pulse 130/min, BP 75/40 and capillary refill time 4 seconds. A pulse oximeter reads 99%. You notice soot around his nostrils. Which of the following statements are true? 1) His vital signs are normal 2) His conscious level is of no concern 3) The story is suggestive of smoke inhalation 4) Dehydration is the likely cause of the observed vital signs 5) Based on the story, he is unlikely to need early intubation 6) The priority of treatment is to dress any burns 7) Burns which encircle the chest are generally harmless 8) Fluid loss from the burn in the early stages would account for the vital signs 9) The extent of the burn can be estimated from the rule of 9 10) Appropriate early fluid therapy for this child is warmed saline 0.9% 20ml/kg 11) Pulse oximeters can be relied upon in this scenario 12) Other injuries must be excluded by thorough examination Epidemiology Cutaneous burns, or thermal injury, can be conveniently divided into scalds and flame burns. Flame burns are frequently associated with flammable liquids spilt onto clothing. Scalds are burns specifically caused by contact with hot liquids. They also often involve clothing, which prolongs the duration of harmful contact between hot liquid and skin. In the developed world, 70% of burnt children are under 4 years of age, typically from impoverished backgrounds. The highest incidence is 1-2 years, with boys more affected than girls. Most fatalities occur in house fires, where death by smoke inhalation is the usual cause. The World Health Organisation (WHO) estimated that fire associated burns were responsible for 320,000 deaths worldwide in Mortality following a burn occurs as a bimodal distribution. Early deaths occur due to Airway loss (eg smoke
2 inhalation), carbon monoxide poisoning, refractory shock or co-existing trauma. With good resuscitation techniques, this early mortality can be reduced to 5%. Late mortality often occurs as a result of wound sepsis and multi-organ failure. A co-ordinated mutidisciplinary approach to patient care can also reduce this late mortality. Children are particularly prone to burns due to the inability to recognise danger in the younger age groups and the risk taking behaviours of the older child (particularly boys). Children have thinner skin, lose proportionately more fluid, are more prone to hypothermia and mount a greater Systemic Inflammatory Response than adults. Pathophysiology 2 factors determine the severity of a burn its temperature and the duration of contact with it. Cell death occurs exponentially quickly as temperature rises. Temperatures as low as 40 degrees C can rapidly inflict significant injury in young children. Scalds caused by water below its boiling point in brief contact (the majority of such injuries) are not surprisingly less severe than scalds caused by liquids e.g. cooking oil at higher temperature, or liquids which are in skin contact for a longer time. Infants or those children physically unable to move themselves away from the burning agent are susceptible to this latter mechanism. Flame burns are higher temperature and cause the most severe injuries. Histologically, the burnt skin consists of a central coagulated, necrotic area surrounded by zones of venous stasis and hyperaemia. The capillary leakage that occurs in these outer 2 areas is the result of both direct heating and secondary inflammation. Burnt epidermis permits large evaporative fluid losses of up to 200ml/m 2 /hr. These and other fluid losses cause hypoalbuminaemia and the clinical picture of shock. Nevertheless, in the first hour after a burn, the commonest cause of death is smoke inhalation. The burning contents of enclosed rooms contain a lethal mixture of hot, noxious gases, soot particles and depleted oxygen. Early Management of Significant Burns Despite the temptation to immediately attend to the burn, it is vital to remember the ABCDE approach to a victim of trauma. Severely burnt children may well have other major injuries not obviously apparent, either as a result of an associated blast injury or in their efforts to escape the fire e.g. by jumping from a window. Airway & Inhalational injury The Airway, Breathing and Circulation should be rapidly assessed while administering high-flow oxygen and establishing monitoring. The cervical spine may require immobilisation with collar, sandbags and tape or manual inline stabilisation (with an assistant). Further history should be obtained. Airway may be affected either by inhalational injury (which if present increases mortality by up to 50%) or by obvious
3 thermal injury to the face. Whilst the latter is usually obvious, indicators of the former may be more subtle. The following features point to an inhalational injury: History - was the child burnt in an enclosed space/explosion? Was there loss of consciousness? Exam soot around the nose/mouth/in sputum, burning of eyelash/brow & nasal hairs. Drooling, dysphonia/phagia, stridor. Approximately 60% of flame facial burns will have an associated smoke inhalational injury. Inhalation of hot dry gases tends to cause supraglottic injury, whereas steam inhalation also results in deeper, parenchymal injury. The shockwave from a blast can cause a mixture of chest injuries: barotrauma & contusion to the lung and blunt trauma. Any suspicion that an inhalational injury has occurred should make you consider immediate, elective intubation. Airway oedema can develop very quickly and make late attempts at securing the airway extremely difficult. There are several considerations about the endotracheal tube which are particular to burns patients: Expect to use a smaller tube than calculated due to airway oedema. Once intubated, do not cut the endotracheal tube, as facial swelling can be dramatic and bury the end of an inappropriately short tube somewhere within the mouth. The tube should also be inserted sufficiently far that the distal end is not drawn out of the trachea by the effects of mucosal oedema. A tracheostomy, whilst ideal, might not be feasible for a prolonged period if the tissues of the neck are injured. It is useful to site a nasogastric tube at the same time to allow gastric decompression and early feeding, which is important in any burn >10%. Breathing Tachypnoea, hypoxia and eventual cyanosis suggests a lung parenchymal thermal injury which will almost certainly require ventilatory support. Invasive arterial monitoring, if available, prevents the need for repeated blood sampling and provides important metabolic, respiratory and haemodynamic information. An Acute Respiratory Distress Syndrome frequently supervenes which requires specialist critical care, including protective ventilation strategies, regular bronchoalveolar lavage and timely tracheostomy insertion if required. Circumferential burns to the chest (or abdomen in infants) can restrict chest wall excursion and require urgent excision escharotomy. This procedure is not without difficulties the potential for severe blood loss, hypothermia and positioning are considerations.
4 Carbon monoxide poisoning Fire produces carbon monoxide (CO) when organic chemicals burn in low oxygen environments. Inhaled CO combines with haemoglobin with 200 times the affinity of oxygen to form carboxyhaemoglobin. Thus, less oxygen is delivered to the tissues. Pulse oximeters cannot distinguish oxyhaemoglobin from carboxyhaemoglobin, giving erroneously high (in fact, apparently normal) readings. If possible, carboxyhaemoglobin level should be measured (some blood gas analysers do this) and if between 5-20%, the child should remain on high-flow oxygen which speeds the dissociation of carboxyhaemoglobin. Metabolic acidosis and coma are associated with levels >20%. Whilst hyperbaric therapy is the treatment of choice where available, use intubation and 100% oxygen where it is not. Other poisons e.g. cyanide can sometimes accompany the incomplete combustion of common household plastics. Cyanide poisoning presents as metabolic acidosis, coma and unusually high venous oxygen saturation (cyanide prevents cells from using oxygen). Circulation Hypovolaemic shock occurring in the first few hours after a significant burn must be assumed to be due to another injury, which must be sought. Obtain the largest venous access possible, preferably in 2 unburnt sites. Burnt skin can be cannulated if necessary, although the skin creases over the femoral vessels are often spared. Finding unburnt sites for non-invasive monitoring can be problematic; non-invasive blood pressure measurement may be difficult with extensive limb burns and non-adhesive ECG electrodes can be stapled directly to burnt skin. Urine output measurement, ideally via urinary catheter is essential to monitor haemodynamic status and guide ongoing fluid resuscitation in the shocked burnt victim. Send blood samples for full count, electrolytes, glucose and cross-match. Haematocrit rises initially as a result of plasma loss but anaemia may then follow due to haemolysis, recurring surgical blood loss and sepsisinduced marrow suppression. A significant catabolism develops; early excision and skin cover can reduce this hypermetabolic state, although protracted protein loss can occur up to a year after burn injury. Fluid calculation Shocked children should initially be managed as would any shocked child: warmed i.v. saline 0.9% boluses of 20ml/kg. Non-shocked children with burns of greater than 10% will require intravenous fluid resuscitation according to the following (Parkland) formula: % burn x weight in kg x 4 ml The tpye of fluid used is generally a crystalloid such as compound sodium lactate (Hartmanns) or 0.9% saline. Colloid has not been shown to confer any additional benefit in the early stages of burn management.
5 Half of this volume should be given over the first 8 hours since the burn occurred and the rest over the next 16 hours. This is in addition to the normal daily fluid requirements of the child. This formula is a guide only, and should be used in conjunction with regular clinical assessment and measurement of urine output, which should be maintained at >2 ml/kg/hour in children Of note, significant over resuscitation with fluids can result in abdominal or extremity compartment syndrome or severe pulmonary insult causing worsening gas exchange. There has recently been renewed interest in resuscitation using oral rehydration. This may be appropriate for minor burns <10-15%, however one must be cautious in the patient with more extensive burns due to the high incidence of ileus. Neurological Assessment A rapid assessment of conscious state is part of the trauma primary survey. Reduced conscious state could have many causes such as head injury, hypoxia, inhalation of toxins, shock or pre-existing disease states (e.g. diabetes). Exposure & Secondary survey It is important to fully undress the child to estimate the full extent of the burn, but once done ensure the child is covered again as rapid heat loss occurs. Warm the room if necessary. If taking the child to theatre, turn off the air-conditioning and aim for a warm thermoneutral environment. This reduces the patient s energy expenditure a well as helping to prevent hypothermia. Although beyond the remit of this article, it is important to think of significantly burnt children as trauma victims and conduct a thorough head to toe examination once the initial stabilisation has been completed. Further supportive measures. Optimal dietary support is extremely important in view of the hypermetabolic state; a patient with a burn of 40% Body Surface Area can lose up to 25% of body weight in 3 weeks of not optimally supported. Starting enteral feeds as soon as practically possible can help to prevent gastroparesis and meet the high metabolic demand. Some centres are using partial Beta blockade (e.g. propranolol to decrease heart rate by 20%) in children who remain tachycardic after the initial resuscitation phase despite appropriate fluid replacement and adequate analgesia. This further reduces the hypermetabolic state. This has been associated with an increased net protein balance and reduced energy expenditure.
6 Burn assessment Severity is related to surface area affected and depth. Also, burns to certain areas of the body warrant specialist attention e.g. hands, feet and perineum in order to achieve a good functional outcome. Area This is often assessed with the aid of charts ( to request a chart). The familiar rule of 9 and adult burn charts are not suitable for use in children younger than 14 years because of the variation in the relative size of their heads and limbs with age. A useful rule states that the area of the child s hand (palm and adducted fingers) is approximately equal to 1% of their total body surface area, whatever their age. Depth Burns are classified into groups dependent upon depth: Superficial epidermis only; skin appears red, no blisters Partial thickness epidermis/dermis; skin appears pink/mottled, some blisters Full thickness dermis/deeper layers, appears white/charred, painless (although marginal areas may still be painful) Superficial burns are painful but heal rapidly. Partial thickness come in 2 varieties those in which epidermal islands persist around sweat glands and hair follicles and those more severe burns in which these islands are destroyed. The former are painful and take up to 2 weeks to spontaneously heal. The latter may be less painful (due to destruction of nerves) but take longer to heal and may require surgical excision and grafting in order to do so. Full thickness burns require early excision and grafting to reduce infection and improve morbidity and mortality. In practice, the exact depth of many partial thickness burns are difficult to determine with accuracy on initial presentation, however surgical management often comprises early cleaning and covering in theatre under anaesthesia. Further management Analgesia Burnt children are likely to experience significant pain titrate boluses of i.v. morphine 0.1mg/kg until comfortable, carefully observing their level of sedation. Ketamine, if used for anaesthesia/dressing changes, provides excellent analgesia. Later, oral analgesics are preferred though beware non-steroidal anti-inflammatory drugs because of the observed predisposition to gastric stress-ulceration. Wound care
7 Leave blisters intact. Cold irrigation and compresses can be soothing but run the risk of excessive heat loss and should only be used for <10 minutes in situations with superficial/partial thickness burns of <10-15%. Cling film may be applied loosely to protect and prevent fluid loss. Cover burns with sterile towels and avoid repeated exposure. Wound infection is a major cause of late fatality following a burn; gram negative bacterial colonisation occurs early, despite aseptic techniques in cleaning the wound. Suitable dressings should be applied early both to prevent it and to provide some analgesia. A variety of silver (Ag) based dressings are commonly used due to their antimicrobial gram-negative, gram positive and anti-fungal activity. Antibiotics should not be used prophylactically. Care must be taken to diagnose sepsis and wound infection; this can be difficult as frequently the patient s temperature increases due to the raised metabolism. If a patient is unwell, particularly with fever, rash, drowsiness, low serum sodium concentration and lymphopaenia, one must exclude other causes of sepsis (eg line related infection) and consider the diagnosis of toxic shock syndrome. This is potentially fatal and should be treated with antibiotics and fluids. Consider further dressing change and possibly fresh frozen plasma. Other Anaesthetic Considerations Suxamethonium is safe to use, if indicated, in the first 24 hours after a burn. Following this, concerns about acutely causing severe hyperkalaemia precludes its use for up to a year. To complicate matters, resistance to non-depolarising muscle relaxants is often seen for up to 3 months. In the acute situation, ketamine is the intravenous induction agent of choice (2mg/kg), particularly in cases of hypovolaemia. Clearly, it is very important to try to fluid resuscitate any hypovolaemic patient prior to anaesthetising them, just as in any other emergency situation. If you suspect a significant inhalational injury with impending upper airway obstruction, treat the patient as you would any such case: either a gaseous induction, maintaining spontaneous breathing, or if you have one and are confident of your skills (and the child!), an awake fibreoptic technique (impossible in non-cooperative children). In the extreme and catastrophic case of complete, sudden upper airway obstruction you should be prepared to perform an emergency surgical airway. Having an appropriately-skilled (i.e. ENT) surgical colleague scrubbed and standing by with the necessary instruments to hand can be immensely reassuring in such cases. Final Points The most effective strategy for burns management involves prevention. Widespread education, safety procedures and devices such as smoke alarms can help to prevent many thousands of deaths per year.
8 Finally, it is important to remember occasionally burns are caused by non-accidental injury. If this is suspected due to pattern of injury, delay in presentation or inconsistencies in the history it must be investigated with experienced colleagues to prevent further future injury to the child. Answers to MCQ & Discussion 1)F 2)F 3)T 4)F 5)F 6)F 7)F 8)F 9)F 10)T 11)F 12)T The history has several clues as to the likely type and extent of the injuries. He was found deeply asleep, probably unconscious, in an enclosed burning room (his sheets were smouldering). The fact that the rescuer sustained a broken ankle suggests he may also have traumatic injury. The pattern of charring to his pyjamas raises the possibility of circumferential chest burn. His initial vital signs indicate that he is shocked. The reduced level of consciousness in the context of soot around the nostrils strongly suggests an inhalational injury, despite the normal pulse oximeter reading. He will require early definitive airway management. After giving high inspired oxygen and applying an immobilising hard cervical collar resuscitation proceeds according to the familiar ABCDE approach. Upon removing his pyjamas, he is seen to have an extensive area of pink blistered skin across his chest and left arm. Unfortunately, no burns chart is available so the extent of the burnt area is estimated using the child s palm + adducted fingers = 1% rule. Using this method the burn, which has partial thickness characteristics, is estimated at 20%. Using the Parkland formula (and assuming a weight of [age+4] x2 i.e. [5+4] x2=18kg), the fluid bolus required over the ensuing 24 hours is: 20x18x4=1440ml. 720ml should be given over the first 8 hours since the burn and the rest over the next 16 hours. This is in addition to the normal daily maintenance requirements. Estimated weight enables calculation of drug doses e.g. morphine bolus 0.1mg/kg = 1.8mg. Endotracheal tube size is estimated in the usual way: age/4+4 i.e. 5/4+4=5. It is prudent to have smaller tube sizes available than the estimated size in case of airway oedema. References Black RG, Kinsella J. Anaesthetic management for burns patients. BJA CEACCP, Dec 2001; 1: Cockcroft S, Way C. Burns and smoke inhalation. Anaesth. and Int. Care Med. 2002; 3:8:
9 Hilton PJ, Hepp M. Immediate care of the burned patient. BJA CEACCP, Aug 2001; 1: Fraser JF, Venkatesh BS. Recent Advances in the Management of Burns. In: Australasian Anaesthesia 2005; Australia and New Zealand College of Anaesthetists. Fenlon S, Nene S. Burns in Children. BJA CEACCP, May 2007; 7: Instructor Manual: Advanced Paediatric Life Support, 4 th Ed White MC, Thornton K, Young AER. Early Diagnosis and Treatment of Toxic Shock Syndrome in Paediatric Burns. Burns 2005; 31:
Trauma in children. Paediatric burns and associated injuries
 Paediatric burns and associated injuries Reprinted with revisions from Pittaway AJ. Managing Paediatric Burns. Anaesthesia Tutorial of the Week 78 (2007) A J Pittaway* and N Hardcastle *Correspondence
Paediatric burns and associated injuries Reprinted with revisions from Pittaway AJ. Managing Paediatric Burns. Anaesthesia Tutorial of the Week 78 (2007) A J Pittaway* and N Hardcastle *Correspondence
BURNS MODULE. In the paediatric population consider non-accidental injury as a mechanism for burn injuries.
 BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test
 Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department
 Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
EmergencyKT: Management of Thermal Injury in Adult Patients
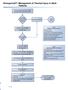 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
Burns Management in the Emergency Department
 Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
COBIS Management of airway burns and inhalation injury PAEDIATRIC
 COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
Burns. A Comprehensive Review Assessment & Management
 Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Paediatric Shock. Dr Andrew Pittaway Department of Anaesthesia Bristol Royal Hospital for Children Bristol, UK
 Paediatric Shock Dr Andrew Pittaway Department of Anaesthesia Bristol Royal Hospital for Children Bristol, UK Self-assessment: 1. What is the definition of shock? 2. List the different pathophysiological
Paediatric Shock Dr Andrew Pittaway Department of Anaesthesia Bristol Royal Hospital for Children Bristol, UK Self-assessment: 1. What is the definition of shock? 2. List the different pathophysiological
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Responsibility This guideline applies to teams of health professions caring for burn patients.
 Page 1 of 9 Guideline: Initial Assessment & Management of Burn Injuries Purpose This document provides a guideline for the initial assessment and management of burn patients. It is not intended as a full
Page 1 of 9 Guideline: Initial Assessment & Management of Burn Injuries Purpose This document provides a guideline for the initial assessment and management of burn patients. It is not intended as a full
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1
 Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1 For questions 1 through 3, consider the following scenario: A three year old comes with burns to her face and chest after a kerosene
Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1 For questions 1 through 3, consider the following scenario: A three year old comes with burns to her face and chest after a kerosene
Management of Acute Burn Injuries: The First 24 Hours
 Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
ANAESTHESIA FOR BLEEDING TONSIL
 ANAESTHESIA FOR BLEEDING TONSIL BY Dr.S.C.Ganeshprabu, MD., D.A., Professor of Anaesthesiology, Madurai Medical College & Govt. Rajaji Hospital, Madurai -652 020. A 5-year-old child who had tonsillectomy
ANAESTHESIA FOR BLEEDING TONSIL BY Dr.S.C.Ganeshprabu, MD., D.A., Professor of Anaesthesiology, Madurai Medical College & Govt. Rajaji Hospital, Madurai -652 020. A 5-year-old child who had tonsillectomy
Fire Deaths. Dr Julie McAdam Consultant Forensic Pathologist Glasgow University
 Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
Final FRCA Written PAEDIATRICS Past Paper Questions November March 2014
 Final FRCA Written PAEDIATRICS Past Paper Questions November 1996- March 2014 March 2014 A 5-year-old patient presents for a myringotomy and grommet insertion as a day case. During your pre-operative assessment
Final FRCA Written PAEDIATRICS Past Paper Questions November 1996- March 2014 March 2014 A 5-year-old patient presents for a myringotomy and grommet insertion as a day case. During your pre-operative assessment
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
BLS, ILS, ALS OTEP BURNS BURN INTRODUCTION TYPES OF BURNS
 BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns.
 Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Burn injury. A : patent airway with smoking inhalation, stridor. D: E4V5M6,pupil 2mm RTLBE
 Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Wisecracks 1. What are the indications for an escharotomy 2. What are the primary considerations in mechanical ventilation of burn patients
 Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Burn Injuries & Its Management M JARI.MD
 Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Shruti Dholakia L Chigaru Author Position Fellow CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Shruti Dholakia L Chigaru Author Position Fellow CATS Consultant Document Owner E. Polke Document
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers
 Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Aviation Rescue Swimmer Course
 Aviation Rescue Swimmer Course Primary Survey LT 5.4 December 2003 1 Objectives List the procedures used in a primary survey. Demonstrate primary survey procedures used in a mock trauma (moulage) scenario
Aviation Rescue Swimmer Course Primary Survey LT 5.4 December 2003 1 Objectives List the procedures used in a primary survey. Demonstrate primary survey procedures used in a mock trauma (moulage) scenario
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Critical Care of the Post-Surgical Patient
 Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
NOTE If it is necessary to perform abdominal thrusts, expose the abdominal area prior to pressing on the abdomen.
 ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
HeartCode PALS. PALS Actions Overview > Legend. Contents
 HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
CETEP PRE-TEST For questions 1 through 3, consider the following scenario:
 CETEP PRE-TEST For questions 1 through 3, consider the following scenario: A two and half month infant comes to the health centre looking very lethargic. Her mother reports that the infant has felt very
CETEP PRE-TEST For questions 1 through 3, consider the following scenario: A two and half month infant comes to the health centre looking very lethargic. Her mother reports that the infant has felt very
Chapter 29. Objectives. Objectives 01/09/2013. Burns
 Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Appendix (i) The ABCDE approach to the sick patient
 Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Burns and Scalds. Treatment and Management. Accident and Emergency Department. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Advanced Paediatric Nursing. Burn Trauma. 26 April Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH
 Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
OUTLINE SHEET 5.4 PRIMARY SURVEY
 ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Paediatric Emergency Prompt Cards
 Paediatric Emergency Prompt Cards Introduced July 2016 Prompt cards are designed to be used by any member of the resus team If you have any comments or suggestions, please contact helen.collyer-merritt@sash.nhs.uk
Paediatric Emergency Prompt Cards Introduced July 2016 Prompt cards are designed to be used by any member of the resus team If you have any comments or suggestions, please contact helen.collyer-merritt@sash.nhs.uk
Emergency First Response (EFR) Skills Assessment Sheets V4 June 2017
 Emergency First Response () Skills Assessment Sheets V4 June 2017 Airway management & ventilation Airway management & ventilation Trauma jaw thrust 1 Hand positions 2 Perform jaw thrust / mouth open 3
Emergency First Response () Skills Assessment Sheets V4 June 2017 Airway management & ventilation Airway management & ventilation Trauma jaw thrust 1 Hand positions 2 Perform jaw thrust / mouth open 3
Emergency Room Resuscitation of the Unstable Trauma Patient
 Emergency Room Resuscitation of the Unstable Trauma Patient Goals of trauma resuscitation Maintain: Systemic oxygenation Systemic perfusion Neurologic function Approach to unstable trauma patient Primary
Emergency Room Resuscitation of the Unstable Trauma Patient Goals of trauma resuscitation Maintain: Systemic oxygenation Systemic perfusion Neurologic function Approach to unstable trauma patient Primary
Brief summary of the NICE guidelines December 2013
 Brief summary of the NICE guidelines December 2013 Intravenous fluid therapy in adults in hospital the relevance to Emergency Department Care Applicable to patients 16 years and older receiving i.v. fluids
Brief summary of the NICE guidelines December 2013 Intravenous fluid therapy in adults in hospital the relevance to Emergency Department Care Applicable to patients 16 years and older receiving i.v. fluids
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES
 INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
Wound Care in the Community. Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts
 Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Chapter 24 Soft Tissue Injuries Presentation Notes
 Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
CONTROLLED DOCUMENT. Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) Controlled Document Number: CG259
 Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor:
Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor:
Burn wounds - Determining the size and type degree
 1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
Homework Assignment Complete and Place in Binder
 Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
MICHIGAN. State Protocols. Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.
 MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
Knowledge Objectives (2 of 2) Skills Objectives. Death Scene Considerations. Introduction 12/20/2013
 Fire and Explosion Deaths and Injuries Knowledge Objectives (1 of 2) Identify the effects of fire and explosion on the human body. Discuss the various issues involved in fire or explosion death investigation.
Fire and Explosion Deaths and Injuries Knowledge Objectives (1 of 2) Identify the effects of fire and explosion on the human body. Discuss the various issues involved in fire or explosion death investigation.
OBJECTIVES OF TRAINING FOR THE ANAESTHESIA TERM
 College of Intensive Care Medicine of Australia and New Zealand ABN: 16 134 292 103 Document type: Training Date established: 2007 Date last reviewed: 2014 OBJECTIVES OF TRAINING FOR THE ANAESTHESIA TERM
College of Intensive Care Medicine of Australia and New Zealand ABN: 16 134 292 103 Document type: Training Date established: 2007 Date last reviewed: 2014 OBJECTIVES OF TRAINING FOR THE ANAESTHESIA TERM
Current Trends in Burn Care
 Objectives Current Trends in Burn Care Jordan Murphy, BSN, CFRN Clinical Educator-KY/FL PHI Air Medical Describes normal skin anatomy. Differentiates pathophysiology related to etiology of injury. Identify
Objectives Current Trends in Burn Care Jordan Murphy, BSN, CFRN Clinical Educator-KY/FL PHI Air Medical Describes normal skin anatomy. Differentiates pathophysiology related to etiology of injury. Identify
UNIT 4: DISASTER MEDICAL OPERATIONS
 UNIT 4: DISASTER MEDICAL OPERATIONS PART 2 Patient Evaluation: How to perform a head-to-toe assessment to identify and treat injuries. Basic Treatment How to: Treat burns Dress and bandage wounds Treat
UNIT 4: DISASTER MEDICAL OPERATIONS PART 2 Patient Evaluation: How to perform a head-to-toe assessment to identify and treat injuries. Basic Treatment How to: Treat burns Dress and bandage wounds Treat
Your Anaesthetic Explained
 Your Anaesthetic Explained Patient Information Sheet Pre Admission Assessment Clinic Tel: 4920307 What is anaesthesia? The word anaesthesia means loss of sensation. If you have ever had a dental injection
Your Anaesthetic Explained Patient Information Sheet Pre Admission Assessment Clinic Tel: 4920307 What is anaesthesia? The word anaesthesia means loss of sensation. If you have ever had a dental injection
Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical]
![Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical] Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical]](/thumbs/87/96512765.jpg) Children s Acute Transport Service Clinical Guidelines Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical] Document Control Information Author D Lutman Author Position Head of Clinical
Children s Acute Transport Service Clinical Guidelines Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical] Document Control Information Author D Lutman Author Position Head of Clinical
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
CH 721 Hospital Care FINAL EXAMINATION. Semester 1, 2017
 SOLOMON ISLANDS NATIONAL UNIVERSITY School of Nursing and Allied Health Sciences Bachelor of Nursing: Child Health CH 721 Hospital Care FINAL EXAMINATION Semester 1, 2017 (End of semester 2 for BNCH Intake
SOLOMON ISLANDS NATIONAL UNIVERSITY School of Nursing and Allied Health Sciences Bachelor of Nursing: Child Health CH 721 Hospital Care FINAL EXAMINATION Semester 1, 2017 (End of semester 2 for BNCH Intake
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
HealthCare Training Service
 HealthCare Training Service Advanced Life Support Exam Time: Perusal Time: 20 minutes 5 minutes Total Marks: 25 Instructions: Read each question carefully. Using a pencil, record your response to each
HealthCare Training Service Advanced Life Support Exam Time: Perusal Time: 20 minutes 5 minutes Total Marks: 25 Instructions: Read each question carefully. Using a pencil, record your response to each
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Module I. Disasters and their Effects on the Population: Key Concepts
 PRE COURSE EXAM Place an x by the correct answer(s) on the answer sheet. Module I. Disasters and their Effects on the Population: Key Concepts 1. Which of the following best defines an event as a disaster?
PRE COURSE EXAM Place an x by the correct answer(s) on the answer sheet. Module I. Disasters and their Effects on the Population: Key Concepts 1. Which of the following best defines an event as a disaster?
EMERGENCYROOM BURN MANAGEMENT
 EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
DOCUMENT CONTROL PAGE
 DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
Ammonia (NH 3 ) B 1. Information and recommendations for paramedics and doctors at the site. BASF Chemical Emergency Medical Guidelines
 BASF Chemical Emergency Medical Guidelines Ammonia (NH 3 ) B 1 Information and recommendations for paramedics and doctors at the site Before approaching the patient the paramedics and doctors at the site
BASF Chemical Emergency Medical Guidelines Ammonia (NH 3 ) B 1 Information and recommendations for paramedics and doctors at the site Before approaching the patient the paramedics and doctors at the site
The assessment helps decide if the patient is an emergency, priority or non-urgent case.
 Emergency Triage Assessment and Treatment The World Health Organisation (WHO) has produced some useful guidelines about how to improve the care of our patients and their survival in hospital. This is a
Emergency Triage Assessment and Treatment The World Health Organisation (WHO) has produced some useful guidelines about how to improve the care of our patients and their survival in hospital. This is a
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Anaesthetic Plan And The Practical Conduct Of Anaesthesia. Dr.S.Vashisht Hillingdon Hospital
 Anaesthetic Plan And The Practical Conduct Of Anaesthesia Dr.S.Vashisht Hillingdon Hospital Anaesthetic Plan Is based on Age / physiological status of the patient (ASA) Co-morbid conditions that may be
Anaesthetic Plan And The Practical Conduct Of Anaesthesia Dr.S.Vashisht Hillingdon Hospital Anaesthetic Plan Is based on Age / physiological status of the patient (ASA) Co-morbid conditions that may be
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose.
 Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
 Manual: Section: Protocol #: Approval Date: Effective Date: Revision Due Date: 10/2019 LifeLine Patient Care Protocols Adult/Pediatrics AP1-011 10/2018 10/2018 FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
Manual: Section: Protocol #: Approval Date: Effective Date: Revision Due Date: 10/2019 LifeLine Patient Care Protocols Adult/Pediatrics AP1-011 10/2018 10/2018 FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version)
 Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
CLINICAL GUIDELINES ID TAG
 CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Guideline for the perioperative fluid management in children Kieran O Connor Anaesthetics ATICS Date Uploaded: 26/04/2016 Review
CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Guideline for the perioperative fluid management in children Kieran O Connor Anaesthetics ATICS Date Uploaded: 26/04/2016 Review
Pediatrics Grand Rounds 1 June University of Texas Health Science Center at San Antonio. Management of Burn Wounds. Management of Burn Wounds
 Management of Burn Wounds Management of Burn Wounds History of Burn Care Pathophysiology of Burn Lillian F. Liao, MD, MPH Division of Trauma and Emergency Surgery Department of Surgery UTHSCSA Acute burn
Management of Burn Wounds Management of Burn Wounds History of Burn Care Pathophysiology of Burn Lillian F. Liao, MD, MPH Division of Trauma and Emergency Surgery Department of Surgery UTHSCSA Acute burn
Anaesthesia and intensive care for major burns
 Anaesthesia and intensive care for major burns Sophie Bishop MBChB (Euro) FRCA Simon Maguire MBChB, FRCA Matrix reference 2A02, 2C01 Key points Crystalloid is the fluid of choice for resuscitation, volume
Anaesthesia and intensive care for major burns Sophie Bishop MBChB (Euro) FRCA Simon Maguire MBChB, FRCA Matrix reference 2A02, 2C01 Key points Crystalloid is the fluid of choice for resuscitation, volume
Management of Patients with Burns Chris Thompson. Contact:
 Management of Patients with Burns Chris Thompson. Contact: acdthompson@hotmail.com Introduction Anaesthetists are involved in resuscitation in the Emergency Department (ED), the operating room, the intensive
Management of Patients with Burns Chris Thompson. Contact: acdthompson@hotmail.com Introduction Anaesthetists are involved in resuscitation in the Emergency Department (ED), the operating room, the intensive
Cellular and Tissue Effects. Pathophysiology of the Burn Wound. Special Topics: Thermal Burns & Smoke Inhalation
 Special Topics: Thermal Burns & Smoke Inhalation MEDICAL RESPONDER AND RECEIVER SEMINAR; EXPLOSION AND BLAST INJURIES Pathophysiology of the Burn Wound The burn wound is the source of virtually all ill
Special Topics: Thermal Burns & Smoke Inhalation MEDICAL RESPONDER AND RECEIVER SEMINAR; EXPLOSION AND BLAST INJURIES Pathophysiology of the Burn Wound The burn wound is the source of virtually all ill
10. Severe traumatic brain injury also see flow chart Appendix 5
 10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
Sedation in Children
 CHILDREN S SERVICES Sedation in Children See text for full explanation and drug doses Patient for Sedation Appropriate staffing Resuscitation equipment available Monitoring equipment Patient suitability
CHILDREN S SERVICES Sedation in Children See text for full explanation and drug doses Patient for Sedation Appropriate staffing Resuscitation equipment available Monitoring equipment Patient suitability
11. Spinal cord injury
 11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
