Anaesthesia and intensive care for major burns
|
|
|
- Clinton Bryant
- 5 years ago
- Views:
Transcription
1 Anaesthesia and intensive care for major burns Sophie Bishop MBChB (Euro) FRCA Simon Maguire MBChB, FRCA Matrix reference 2A02, 2C01 Key points Crystalloid is the fluid of choice for resuscitation, volume calculated by the Parkland formula¼4mlkg 21 (%burn) 21. Hypovolaemic shock in the first few hours after a burn injury is never due to the burn alone. Primary and secondary survey should follow ATLS principles (do not get distracted by the burn). Blood loss during debridement and grafting can be significant and insidious. Major burns require a dedicated multidisciplinary team for adequate management. Sophie Bishop MBChB (Euro) FRCA Specialist Registrar Department of Anaesthesia Regional Centre for Burns and Plastic Surgery University Hospital of South Manchester Manchester M23 9LT UK Simon Maguire MBChB, FRCA Department of Anaesthesia Regional Centre for Burns and Plastic Surgery University Hospital of South Manchester Southmoor Road Manchester M23 9LT UK Tel: þ Fax: þ simonmaguire@doctors.org.uk (for correspondence) 118 Major burns are systemic injuries requiring input from multiple specialities. There are cases of new burns per year presenting to emergency departments in England and Wales, with around 10% of these being admitted to hospital. Of these, cases are complex and require the services of a regional adult burns unit. The majority of the others will be managed by hospitals with a plastic surgery service. Important considerations in the clinical outcome for these patients are early resuscitation, multidisciplinary team management, early surgical debridement, and prevention of complications. Anaesthesia in this group of patients can be challenging with profound hypermetabolism, pain management issues, alteration of drug pharmacokinetics, potential airway problems, temperature control, and substantial blood loss. Overall, the mortality rate among hospitalized burn patients in a recent review of European data was 13.9% (4 28.3%). 1 Major risk factors for death are older age, a higher total percentage of burned surface area, inhalation injury [mortality rate 27.6% ( %)], and chronic diseases. There appears to be no sex-related difference in survival after thermal injury. 2 Multi-organ failure and sepsis are the most frequently reported causes of death. The main causes of early death (,48 h) are burn shock and inhalation injury. Initial assessment and resuscitation History The history of a burn injury can give valuable information about the nature and extent of the burn, the likelihood of inhalation injury, the depth of burn, and the probability of other injuries. A patient s full medical history must be obtained on admission to the emergency department, as this may be the only time that a first-hand history is obtainable. Primary survey The initial management of a severely burnt patient is similar to that of any trauma patient. The burn injury must not distract from this sequential assessment, otherwise serious associated injuries may be missed. Airway with cervical spine control All burn patients should receive 100% oxygen (O 2 ) through a non-rebreathing mask on presentation. An assessment must be made as to whether the airway is compromised or is at risk of compromise. Initial compromise of the airway is almost always due to a low Glasgow Coma Score (GCS) and not the burn. Early tracheal intubation should be considered in the presence of any of the following features: stridor, hypoxaemia or hypercapnia, a GCS of,8, deep facial burns, full-thickness neck burns and oropharyngeal oedema. If intubation is required at this early stage, it is usually technically easy as swelling of the airway has not yet occurred. An uncut tracheal tube (size 8.0 mm or above) is used to allow subsequent bronchoscopy. Succinylcholine is safe in the first 24 h after a burn after this time, its use is contraindicated due to the risk of hyperkalaemia leading to cardiac arrest, thought to be due to release of potassium from extrajunctional acetylcholine receptors. This can persist up to 1 year post-burn. Inhalation injury Inhalation injury is defined as the aspiration of superheated gases, steam, hot liquids, or noxious products of incomplete combustion. It is almost never seen in association with flash burns or other forms of brief, albeit high temperature, exposure. True inhalation injury is doi: /bjaceaccp/mks001 Advance Access publication 23 February, 2012 Continuing Education in Anaesthesia, Critical Care & Pain Volume 12 Number & The Author [2012]. Published by Oxford University Press on behalf of the British Journal of Anaesthesia. All rights reserved. For Permissions, please journals.permissions@oup.com
2 likely to be present if the burn was received in an enclosed space with delayed escape or rescue. Three distinct clinical entities are possible. Upper airway thermal injury (above larynx) This usually occurs above the glottis, as by the time hot gases reach the larynx, the heat energy has been dissipated. The pharynx and epiglottis may have significant thermal injury which can swell dramatically. Clinical signs include inspiratory stridor, change in voice/hoarseness, and a swollen uvula. Lower airway thermal injury (below larynx) Inhalation of products of incomplete combustion causes sloughing of the airway s epithelium, mucus secretion, inflammation, atelectasis, and airway obstruction. Clinical signs include dyspnoea, coughing wheezing, and the production of copious secretions. Findings at bronchoscopy include carbonaceous deposits, oedema, bronchial mucosal erythema, haemorrhage, and ulceration. Bronchial lavage with 1.4% bicarbonate solution has been used to neutralize acidic deposits and remove soot contamination. Injury as a result of noxious gases Carbon monoxide (CO) poisoning should be suspected in any unconscious patient. The clinical symptoms of CO poisoning include nausea and vomiting, headache, hypotension, convulsions, and coma. The amount of carboxyhaemoglobin (HbCO) formed depends on inspired CO concentration and duration of exposure, and helps to diagnose inhalation injuries but correlates poorly with severity of toxicity and outcome. The oxyhaemoglobin (HbO 2 ) dissociation curve is shifted to the left, and the cellular cytochrome oxidase system is inhibited, causing tissue hypoxia and metabolic acidosis. Pulse oximetry cannot differentiate between HbO 2 and HbCO and will overestimate the true oxygen saturation. Arterial blood gas analysis using a co-oximeter is required. Treatment is with 100% oxygen which will decrease the elimination half-life of CO from 4 h to under 1 h it is reduced further to under 30 min with hyperbaric O 2 at 3 atm but this is rarely practical. It should be considered in pregnant or comatose patients, those with HbCO levels.40%, or patients failing to respond to conventional therapy. Patients with HbCO levels.25 30% should be ventilated. Cyanide poisoning should be suspected in burn patients with an unexplained and persistent lactic acidosis, despite adequate fluid resuscitation. Breathing Breathing, chest movement, and tracheal position should be assessed clinically. There are several ways that a burn injury can compromise respiration. Mechanical restriction of breathing Deep dermal or full-thickness circumferential burns of the chest may severely restrict chest wall movement and relieving escharotomies may be necessary to allow adequate ventilation. These are rarely, if ever, needed before admission to a burn service. Blast injury Penetrating injuries can cause tension pneumothoraces, and the blast itself can cause lung contusions and alveolar trauma which may lead to adult respiratory distress syndrome. Circulation Two large-bore i.v. cannulae should be inserted through the unburnt skin if possible and baseline bloods sent. Traditional sites for i.v. access may be unavailable and unusual peripheral venous sites or central venous access is required (usual indications for central venous line insertion also apply). The groins are usually spared so femoral venous cannulation is often possible. Burns are not the cause of immediate hypovolaemia. If there are features of hypovolaemic shock, the patient is almost certainly bleeding from other injuries. Warmed Hartmann s solution should be started and titrated to cardiovascular signs, but if stable can be run slowly until the burn calculation is made (see the Exposure and estimation and Fluids sections). Disability A brief assessment of the conscious level should be made using the GCS score and pupils examined. Exposure and estimation Expose and ensure all jewellery and watches are removed from burnt limbs. The patient should be examined (including the back log roll if appropriate) to get an accurate estimate of the burn area and to check for any concomitant injuries. Burn patients become hypothermic easily, so should be covered and warmed as soon as possible. Burns are classified by total body surface area (TBSA) and depth. A standard Lund Browder chart is readily available in most emergency departments for a quick assessment of BSA burnt. If this is not available, the Rule of Nines is fairly accurate in adult patients (Fig. 1). Fluids I.V. fluid resuscitation is required in adults if the burn involves more than 15% BSA or 10% with smoke inhalation. The Parkland formula is the most widely used resuscitation guideline and is 4 ml kg 21 (%burn) 21 which predicts the fluid requirement for the first 24 h after the burn injury. Starting from the time of burn injury (not time of presentation), half of the fluid is given in the first 8 h and the remaining half is given over the next 16 h. The fluid of choice is Hartmann s solution. Any fluid already given should be deducted from the calculated requirement. A urinary catheter Continuing Education in Anaesthesia, Critical Care & Pain j Volume 12 Number
3 Fig 1 Wallace Rule of Nines. Reproduced from: Hettiaratchy S, Papini R. Initial management of a major burn: II assessment and resuscitation. Br Med Jnl 2004; 329: &2004. With permission from BMJ Publishing Group Ltd. should be inserted and hourly urine output is a used as a guide to resuscitation. In adults, at least 0.5 ml kg 21 h 21 should be passed. Example of calculation of fluid resuscitation in burns A 32-yr-old man weighing 80 kg with a 30% flame burn was admitted at 23:00 h. His burn occurred at 22:00 h. He has already received 1000 ml of crystalloid from the emergency services. (i) Total fluid requirement for first 24 h 4ml(30% TBSA)(80 kg)¼9600 ml in 24 h (ii) Half to be given in first 8 h, half over the next 16 h Will receive 4800 ml during 0 8 h and 4800 ml during 8 24 h (iii) Subtract any fluid already received and calculate hourly infusion rate for first 8 h 4800 (for first 8 h) 1000 (fluid already received)¼3800 ml Burn occurred at 22:00 h, so 8 h point is 06:00 h. It is now 23:00 h, so need 3800 ml over next 7 h. 3800/7¼543 ml h 21 from 23:00 to 06:00 h (iv) Calculate hourly infusion rate for next 16 h Divide figure in (ii) by 16 to give fluid infusion rate. Needs 4800 ml over 16 h: 4800/16¼300 ml h 21 from 06:00 to 22:00 h the next day. Table 1 British Burns Association referral criteria for patients with burn injuries 3 Complex burn injuries include any of the following Extremes of age Under 5 yr or more than 60 yr Site involved (dermal or Face or hands or perineum or feet; or any flexure full-thickness loss) particularly the neck or axilla; or any circumferential dermal or full-thickness burn of the limbs, torso, or neck Inhalation injury Any significant such injury, excluding pure carbon monoxide poisoning Mechanism of injury Chemical injury (.5% TBSA); exposure to ionizing radiation injury; high pressure steam injury; high tension electrical injury; hydrofluoric acid injury (.1% TBSA); suspicion of non-accidental burn injury; adult or paediatric Size of skin injury with dermal,16 yr old with.5% TBSA; 16 yr or over.10% or full-thickness loss TBSA Pre-exisitng co-morbidities Significant cardiorespiratory disease; diabetes; pregnancy; immunosuppression; hepatic impairment, cirrhosis Associated injuries Crush injuries; fractures; head injury; penetrating injuries Analgesia Full-thickness burns are painless; however, a mixed picture is common and the patient should receive i.v. morphine titrated against response. While all hospitals will be involved in the initial resuscitation of burn victims, complex burn injuries should be referred to and managed in a burns unit (Table 1). 3 If you are not sure whether a burn should be referred, discuss the case with your local burns unit. Anaesthesia and surgery for burns Inpatient burn injury care should be provided only by specialists trained in burn care in a burns unit. 4 This is a reflection on the team approach to burn injuries, the resources, and infrastructure necessary to provide both critical care and the long-term management of the patient in terms of the planning and timing of surgical procedures. Recent trends in patient care have focused on early excision and wound coverage, aiming to remove the full-thickness injury and get biological closure. This potentially reduces the risk of wound infection and the development of sepsis. The risk of this approach is the physiological insult of surgery to a patient who may well be deteriorating rapidly from their initial injuries. The most important and difficult clinical decisions are often made by the team at this stage. Escharotomy and decompressive therapies These are necessary when a number of factors come into play. The patient will have a full-thickness circumferential burn resulting in an eschar (from French eschare meaning scar or scab) which acts as a non-compliant tourniquet. When there is an additional insult from the accumulation of extracellular fluid as a result of 120 Continuing Education in Anaesthesia, Critical Care & Pain j Volume 12 Number
4 resuscitation, there follows ischaemia and eventual necrosis of the affected compartment. Compartment pressures.40 mm Hg require decompression. Anaesthesia for wound debridement and grafting The conduct of anaesthesia will be predicted by the TBSA, degree of systemic insult, and planned area for debridement and grafting. There is a trend towards earlier intervention and burn excision with the application of skin substitutes if donor skin is limited or further harvesting is not appropriate. Monitoring can be a challenge in major cases when access to chest (ECG), arms (arterial pressure), and digits ( pulse oximetry) can be limited. Skin staples or subcutaneous needles attached to crocodile clips can be used for ECG monitoring. Alternative sites for pulse oximetry such as the nose, lips, or tongue may be necessary. An arterial line is essential for major excisions and a cardiac output monitor can be useful. Blood loss can be significant and occasionally insidious. In major deep burns, we plan for ml blood loss per % area excised, depending on the time post-burn (max 7 16 days) and the presence of infection. This can often be compounded by thrombocytopenia and prolonged coagulation time which requires close liaison with haematology and blood bank. The patient will be hypermetabolic with a systemic inflammatory response (SIRS)-type cardiovascular system and often on vasoactive substances. This, combined with anaesthesia and significant blood loss, can make interpretation of haemodynamic changes quite taxing. These patients often require multiple anaesthetics/operations for dressing changes and grafting and pain management is difficult. There is no evidence for improved outcome using TIVA vs inhalation anaesthesia and the technique used is an individual choice. With multiple anaesthetics, it is important to review the patient response to the previous event and adapt accordingly with the assumption that pain will be an escalating issue. Regional anaesthesia has a part to play but can be limited due to the large areas required to block and the risk of infection. There needs to be a multimodal approach to analgesia in these patients with consideration given to the early use of neuropathic pain agents, such as pregabalin, and opioids and psychology input. Acute perioperative pain may need benefit from agents such as ketamine in addition to the usual analgesic ladder. The time taken for application of major dressings is another consideration, particularly with regard to temperature homeostasis. There are many preoperative anaesthetic considerations for burn wound excision/grafting (Table 2). Critical care management In the first h after resuscitation in patients with major burns, the hormonal response and inflammatory mediators cause hypermetabolism, immunosuppression, and SIRS. Table 2 Anaesthetic considerations for burn wound excision/grafting Preoperative Intraoperative Postoperative Anaesthetic history Table 3 Complications of burns Complications from over-resuscitation 4 Excessive burn oedema Abdominal compartment syndrome Need for fasciotomies on unburned limbs Pulmonary oedema Prolongation of mechanical ventilation Excessive burn oedema Early complications Deep vein thrombosis (thrombo-prophylaxis) Stress ulcers (early enteral feeding/proton pump inhibitor) Adult respiratory distress syndrome Renal failure (from inadequate resuscitation, significant muscle breakdown, haemolysis, or sepsis) Hypothermia Temperature: hot theatre (328C), fluid warmers, monitor aim to lose,18c Infective complications Eyes (secondary infection of corneal burns) Pneumonia Burn wound Urinary tract infection (common with urinary catheters and burns to perineum) Sinuses and middle ear (complication of nasogastric feeding) Infective endocarditis Later complications Pulmonary fibrosis Chronic pain Analgesia: regional blocks TBSAþplanned surgery Monitoring limitations Early use of multimodal analgesia including pregabalin Co-morbidities Oesophageal Doppler High opioid use Airway assessment Hb/coagulation/electrolytes ensure blood products available if necessary Airway management, large minute ventilation, often high PEEP Neuromuscular blocking agents: avoid succinylcholine after 24 h, resistant to nondepolarizing muscle relaxants (NDMR) Others: ketamine, topical morphine Pain team involve early Vascular access Vasopressors/inotropes Location possible need for critical care Limited fasting Epinephrine used in soaked swabs to reduce blood loss Warm room If IPPVþhigh PEEP/airway pressures, consider procedure in room Positioning: prolonged procedure, may be proned Timing often prolonged procedure Clinical psychology involvement Physiotherapy Post-traumatic stress disorder Psychological (effects of severe illness, disfigurement and loss of independence) Depression Sleep disorder Fluid resuscitation and electrolyte management The fluid resuscitation aims to restore tissue perfusion avoiding end-organ ischaemia, preserving viable tissue and minimize tissue oedema. The Parkland formula is a guide and fluid resuscitation should be titrated against clinical response, invasive monitoring, Continuing Education in Anaesthesia, Critical Care & Pain j Volume 12 Number
5 and urine output (.0.5 ml kg 21 h 21 in adults). Invasive monitoring is necessary in the severely burnt patient to help guide both volume replacement and the use of ionotropes. The term fluid creep describes the excessive volumes of fluid used for resuscitation which has occurred in some burn patients with complications (Table 3). 5 Hypokalaemia, hypophosphataemia, hypocalcaemia, and hypomagnesaemia are common and should be treated. There is a phenomenon known as burn shock which describes a combination of hypovolaemic, distributive, and cardiogenic shock which is refractory to massive i.v. resuscitation. Experimental studies have looked at the use of hypertonic saline, high-dose ascorbic acid, or plasma exchange in this setting. Mechanical ventilation Usual lung protection strategies apply, and routine ventilatorassociated pneumonia prevention strategies should be implemented. Prophylactic corticosteroids or antibiotics have no role. 6 In patients with inhalation injury, early tracheal intubation, aggressive pulmonary toilet, bronchodilator therapy, and bronchoscopic lavage are all important. Hypothermia Patients with large burns reset their baseline temperature to 38.58C. This means that a patient with a core temperature of 378C is relatively hypothermic. Strategies to prevent hypothermia include a warmed room (ambient temperature C), warmed inspired air, warming blankets, and warmed fluids. This is also important to minimize the increase in basal metabolic rate caused by heat and evaporative water loss. Metabolism and nutrition The increase in basal metabolic rate is proportional to the size of the burn and the presence of infection, peaking at 7 10 days. This hypermetabolism can persist for up to 2 yr post-injury. Early enteral nutrition has been shown to improve survival in burn patients. Meeting nutritional requirements (high protein, high carbohydrate feeds) is crucial to prevent protein breakdown, decreased wound healing, immune suppression, and an increase in infective complications. Infection This is a significant cause of mortality in major burns (Table 3). Diagnosis of sepsis in burn patients is difficult as signs of SIRS induced by the burn are all normal findings, so regular microbiological surveillance is essential. Burn-specific criteria for sepsis include (three of the following with documented infection): 7 Temperature.39 and,36.58c Tachycardia.110 beats min 21 or.2 SD standard value for age Progressive tachypnoea (spontaneous ventilation: respiratory rate.25 or mechanically ventilated) Hyperglycaemia (plasma glucose.12.8 mmol litre 21 in the absence of diabetes mellitus) Thrombocytopenia (will not apply until 3 days after initial resuscitation; platelet count, ml 21 ) Inability to continue enteral feeding.24 h Protecting patients from infection is by primary excision and skin grafting, asepsis with regular dressing changes, and patient isolation. Psychological care/rehabilitation A multidisciplinary team of physiotherapists, psychologists, nurses, councillors, and occupational therapists are vital to aid rehabilitation and reduce long-term impairment. Acknowledgement We would like to acknowledge the UK National Burn Injury Database and thank Mr K. Dunn for advice on the manuscript. Declaration of interest None declared. References 1. Brusselaers N, Monstrey S, Vogelaers D, Hoste E, Blot S. Severe burn injury in Europe: a systematic review of the incidence, etiology, morbidity, and mortality. Crit Care 2010; 14: R Steinvall I, Fredrikson M, Bak Z, Sjoberg F. Mortality after thermal injury: no sex-related difference. J Trauma 2011; 70: British Burn Association. Available from (accessed 3 October 2010) 4. The Royal College of Anaesthetists. Guidelines on the Provision of Anaesthetic Services (Chapter 14: Guidance on the Provision of Burns and Plastics Anaesthesia). London: The Royal College of Anaesthetists Saffle JR. The phenomenon of fluid creep in acute burn resuscitation. J Burn Care Res 2007; 28: Latenser BA. Critical care of the burn patient: the first 48 hours. Crit Care Med 2009; 37: Greenhalgh DG, Saffle JR, Holmes JH, 4th et al. American Burn Association consensus conference to define sepsis and infection in burns. J Burn Care Res 2007; 28: Please see multiple choice questions Continuing Education in Anaesthesia, Critical Care & Pain j Volume 12 Number
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
BURNS MODULE. In the paediatric population consider non-accidental injury as a mechanism for burn injuries.
 BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Burns Management in the Emergency Department
 Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department
 Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
COBIS Management of airway burns and inhalation injury PAEDIATRIC
 COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns.
 Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test
 Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH
 Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Responsibility This guideline applies to teams of health professions caring for burn patients.
 Page 1 of 9 Guideline: Initial Assessment & Management of Burn Injuries Purpose This document provides a guideline for the initial assessment and management of burn patients. It is not intended as a full
Page 1 of 9 Guideline: Initial Assessment & Management of Burn Injuries Purpose This document provides a guideline for the initial assessment and management of burn patients. It is not intended as a full
EmergencyKT: Management of Thermal Injury in Adult Patients
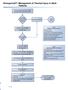 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
BLS, ILS, ALS OTEP BURNS BURN INTRODUCTION TYPES OF BURNS
 BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Critical Care of the Post-Surgical Patient
 Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Acute And perioperative care of the burn-injured patient. Anesthesiology, V 122, No 2
 Acute And perioperative care of the burn-injured patient Anesthesiology, V 122, No 2 Reporter:R4 沈士鈞 Supervisor: 蔡欣怡醫師 Pathophysiology Initial evaluation and management Anesthetic managemen nt Pathophysiology
Acute And perioperative care of the burn-injured patient Anesthesiology, V 122, No 2 Reporter:R4 沈士鈞 Supervisor: 蔡欣怡醫師 Pathophysiology Initial evaluation and management Anesthetic managemen nt Pathophysiology
Burn injury. A : patent airway with smoking inhalation, stridor. D: E4V5M6,pupil 2mm RTLBE
 Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline
 TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
ANAESTHESIA FOR BLEEDING TONSIL
 ANAESTHESIA FOR BLEEDING TONSIL BY Dr.S.C.Ganeshprabu, MD., D.A., Professor of Anaesthesiology, Madurai Medical College & Govt. Rajaji Hospital, Madurai -652 020. A 5-year-old child who had tonsillectomy
ANAESTHESIA FOR BLEEDING TONSIL BY Dr.S.C.Ganeshprabu, MD., D.A., Professor of Anaesthesiology, Madurai Medical College & Govt. Rajaji Hospital, Madurai -652 020. A 5-year-old child who had tonsillectomy
Burn Injuries & Its Management M JARI.MD
 Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
Paediatric Emergency Prompt Cards
 Paediatric Emergency Prompt Cards Introduced July 2016 Prompt cards are designed to be used by any member of the resus team If you have any comments or suggestions, please contact helen.collyer-merritt@sash.nhs.uk
Paediatric Emergency Prompt Cards Introduced July 2016 Prompt cards are designed to be used by any member of the resus team If you have any comments or suggestions, please contact helen.collyer-merritt@sash.nhs.uk
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers
 Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
EMERGENCYROOM BURN MANAGEMENT
 EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Acute Severe Asthma Document Control Information Author E Randle Author Position CATS Consultant Document Owner E Polke Document Owner Position Co-ordinator
Children s Acute Transport Service Clinical Guidelines Acute Severe Asthma Document Control Information Author E Randle Author Position CATS Consultant Document Owner E Polke Document Owner Position Co-ordinator
Wisecracks 1. What are the indications for an escharotomy 2. What are the primary considerations in mechanical ventilation of burn patients
 Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Advanced Paediatric Nursing. Burn Trauma. 26 April Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH
 Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
Management of Patients with Burns Chris Thompson. Contact:
 Management of Patients with Burns Chris Thompson. Contact: acdthompson@hotmail.com Introduction Anaesthetists are involved in resuscitation in the Emergency Department (ED), the operating room, the intensive
Management of Patients with Burns Chris Thompson. Contact: acdthompson@hotmail.com Introduction Anaesthetists are involved in resuscitation in the Emergency Department (ED), the operating room, the intensive
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
TOTW Burns in children October 2007
 TOTW Burns in children October 2007 A J Pittaway FRCA Andrew.pittaway@seattlechildrens.org Before reading the tutorial, consider this case scenario and answer the following questions (answers & discussion
TOTW Burns in children October 2007 A J Pittaway FRCA Andrew.pittaway@seattlechildrens.org Before reading the tutorial, consider this case scenario and answer the following questions (answers & discussion
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2
 CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Fire Deaths. Dr Julie McAdam Consultant Forensic Pathologist Glasgow University
 Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
CHEST INJURY PULMONARY CONTUSION
 CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Pediatric Code Blue. Goals of Resuscitation. Focus Conference November Ensure organ perfusion
 Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
HEAVY METALS : Review
 HEAVY METALS : Review INHALED TOXINS Dr. Tawfiq Almezeiny MBBS FRCPC (CCM) Introduction Airborne toxins typically produce local noxious effects on the airways and lungs. Examples of Inhalational exposure:
HEAVY METALS : Review INHALED TOXINS Dr. Tawfiq Almezeiny MBBS FRCPC (CCM) Introduction Airborne toxins typically produce local noxious effects on the airways and lungs. Examples of Inhalational exposure:
10. Severe traumatic brain injury also see flow chart Appendix 5
 10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
Surviving Sepsis Campaign. Guidelines for Management of Severe Sepsis/Septic Shock. An Overview
 Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Emergency Room Resuscitation of the Unstable Trauma Patient
 Emergency Room Resuscitation of the Unstable Trauma Patient Goals of trauma resuscitation Maintain: Systemic oxygenation Systemic perfusion Neurologic function Approach to unstable trauma patient Primary
Emergency Room Resuscitation of the Unstable Trauma Patient Goals of trauma resuscitation Maintain: Systemic oxygenation Systemic perfusion Neurologic function Approach to unstable trauma patient Primary
TEACHING BASIC LIFE SUPPORT (& ALS)
 TEACHING BASIC LIFE SUPPORT (& ALS) Anton Koželj, R.N., B. Sc., lecturer Faculty of Health Sciences, University of Maribor Žitna ulica 15, 2000 Maribor, Slovenia Fact s To know-how to perform basic life
TEACHING BASIC LIFE SUPPORT (& ALS) Anton Koželj, R.N., B. Sc., lecturer Faculty of Health Sciences, University of Maribor Žitna ulica 15, 2000 Maribor, Slovenia Fact s To know-how to perform basic life
Burn & Soft Tissue Service Orientation Slides
 Burn & Soft Tissue Service Orientation Slides Damien Wilson Carter, MD Director, Burn/Soft Tissue Service Sue Reeder, BSN, CWOCN Burn Resource Nurse Specialist Scope ALL Burn injuries (> Age 12) Cold injury/
Burn & Soft Tissue Service Orientation Slides Damien Wilson Carter, MD Director, Burn/Soft Tissue Service Sue Reeder, BSN, CWOCN Burn Resource Nurse Specialist Scope ALL Burn injuries (> Age 12) Cold injury/
Your anaesthetic for heart surgery
 Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Epidural Infusions for Pain Relief Including Discharge Advice
 Royal Manchester Children s Hospital Epidural Infusions for Pain Relief Including Discharge Advice Children s Pain Team- Information For Parents and Carers This leaflet aims to provide information for
Royal Manchester Children s Hospital Epidural Infusions for Pain Relief Including Discharge Advice Children s Pain Team- Information For Parents and Carers This leaflet aims to provide information for
Thrombolysis Delivery, Care, and Monitoring. 5 Acute Trusts - 6 Primary Care Trusts Ambulance Trust 4 Local Authorities
 Thrombolysis Delivery, Care, and Monitoring Documentation & Pathways Need to follow locally agreed policies and procedures Follow thrombolysis pathway? Need to complete Sits database Weight Dose matters!
Thrombolysis Delivery, Care, and Monitoring Documentation & Pathways Need to follow locally agreed policies and procedures Follow thrombolysis pathway? Need to complete Sits database Weight Dose matters!
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Final FRCA Written PAEDIATRICS Past Paper Questions November March 2014
 Final FRCA Written PAEDIATRICS Past Paper Questions November 1996- March 2014 March 2014 A 5-year-old patient presents for a myringotomy and grommet insertion as a day case. During your pre-operative assessment
Final FRCA Written PAEDIATRICS Past Paper Questions November 1996- March 2014 March 2014 A 5-year-old patient presents for a myringotomy and grommet insertion as a day case. During your pre-operative assessment
Management of severe burns
 Management of severe burns Who gets admitted to the ICU? Large % surface area burns >25% adults >15% children/elderly Inhalational or airway burns Multi-trauma Co-morbidities Burns centres Regional referral
Management of severe burns Who gets admitted to the ICU? Large % surface area burns >25% adults >15% children/elderly Inhalational or airway burns Multi-trauma Co-morbidities Burns centres Regional referral
Burn wounds - Determining the size and type degree
 1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Trial protocol - NIVAS Study
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
UMC HEALTH SYSTEM Lubbock, Texas :
 Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Trauma in children. Paediatric burns and associated injuries
 Paediatric burns and associated injuries Reprinted with revisions from Pittaway AJ. Managing Paediatric Burns. Anaesthesia Tutorial of the Week 78 (2007) A J Pittaway* and N Hardcastle *Correspondence
Paediatric burns and associated injuries Reprinted with revisions from Pittaway AJ. Managing Paediatric Burns. Anaesthesia Tutorial of the Week 78 (2007) A J Pittaway* and N Hardcastle *Correspondence
CLINICAL GUIDELINES ID TAG
 CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Guideline for the perioperative fluid management in children Kieran O Connor Anaesthetics ATICS Date Uploaded: 26/04/2016 Review
CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Guideline for the perioperative fluid management in children Kieran O Connor Anaesthetics ATICS Date Uploaded: 26/04/2016 Review
Northern Burn Care Operational Delivery Network Referral Information Pack
 Northern Burn Care Operational Delivery Network Referral Information Pack Northern Burn Care ODN Burns Referral Pack Pack includes: 1. NBCODN Burns services Contact information 2. Burns Referral Flow chart.
Northern Burn Care Operational Delivery Network Referral Information Pack Northern Burn Care ODN Burns Referral Pack Pack includes: 1. NBCODN Burns services Contact information 2. Burns Referral Flow chart.
Outline. Common causes of loss of consciousness. How to assess loss of consciousness. Emergency management of a patient with loss of consciousness.
 Outline Common causes of loss of consciousness. How to assess loss of consciousness. Emergency management of a patient with loss of consciousness. Common causes of loss of consciousness Alterations in
Outline Common causes of loss of consciousness. How to assess loss of consciousness. Emergency management of a patient with loss of consciousness. Common causes of loss of consciousness Alterations in
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Shruti Dholakia L Chigaru Author Position Fellow CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Shruti Dholakia L Chigaru Author Position Fellow CATS Consultant Document Owner E. Polke Document
Pediatric Trauma Care
 2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
ADMINISTRATIVE REQUIREMENT MANUAL EFFECTIVE DATE
 PURPOSE: I. To establish the minimum requirements for a first responder training course in first aid, which all first responders must take, in order to meet the requirements of M.G.L. c. 111, 201 and 105
PURPOSE: I. To establish the minimum requirements for a first responder training course in first aid, which all first responders must take, in order to meet the requirements of M.G.L. c. 111, 201 and 105
DOCUMENT CONTROL PAGE
 DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
Written Guidelines for Laboratory Testing in Intensive Care - Still Effective After 3 Years
 Written Guidelines for Laboratory Testing in Intensive Care - Still Effective After 3 Years S. M. MEHARI, J. H. HAVILL Intensive Care Unit, Waikato Hospital, Hamilton, NEW ZEALAND ABSTRACT Objective: The
Written Guidelines for Laboratory Testing in Intensive Care - Still Effective After 3 Years S. M. MEHARI, J. H. HAVILL Intensive Care Unit, Waikato Hospital, Hamilton, NEW ZEALAND ABSTRACT Objective: The
Management of Acute Burn Injuries: The First 24 Hours
 Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
TACO CASE STUDIES RTC JUNE Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner
 TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
Appendix. Sedatives and Pain Medications. Gabapentin ( mg po q8h) or Pregabalin ( mg po q8h)
 Appendix Sedatives and Pain Medications Non-intubated patients Non-opioid analgesics Acetaminophen (500 1,000 mg po q6h) NSAID (Ibuprofen, Naprosyn, Celebrex) Gabapentin (100 300 mg po q8h) or Pregabalin
Appendix Sedatives and Pain Medications Non-intubated patients Non-opioid analgesics Acetaminophen (500 1,000 mg po q6h) NSAID (Ibuprofen, Naprosyn, Celebrex) Gabapentin (100 300 mg po q8h) or Pregabalin
Applicable to. Team Members Performing
 Protocol: Pediatric Burn Inhalation Injury Category Clinical Practice Protocol Number Approval Date November 1, 2016 Due for review November 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations
Protocol: Pediatric Burn Inhalation Injury Category Clinical Practice Protocol Number Approval Date November 1, 2016 Due for review November 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations
11. Spinal cord injury
 11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
Burns. A Comprehensive Review Assessment & Management
 Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Analgesia for chest trauma - RVI
 Analgesia for chest trauma - RVI Northern Network Initial Management Patients with blunt chest trauma will be managed in a standard fashion within the context of the well established trauma systems at
Analgesia for chest trauma - RVI Northern Network Initial Management Patients with blunt chest trauma will be managed in a standard fashion within the context of the well established trauma systems at
Appendix (i) The ABCDE approach to the sick patient
 Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
PAEDIATRIC ACUTE CARE GUIDELINE. Resuscitation Coma
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Resuscitation Coma Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Resuscitation Coma Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Introduction. Peripheral arterial disease. Hospital inpatient data - 5,498 FCE (2009/10), & 530 deaths in England alone
 1 Introduction 2 Introduction Peripheral arterial disease Affects 20% adults in Europe and North America In the UK 500-1000/million PAD, 1-2% require amputation LLA 8-15% in people with diabetes with up
1 Introduction 2 Introduction Peripheral arterial disease Affects 20% adults in Europe and North America In the UK 500-1000/million PAD, 1-2% require amputation LLA 8-15% in people with diabetes with up
OBJECTIVES OF TRAINING FOR THE ANAESTHESIA TERM
 College of Intensive Care Medicine of Australia and New Zealand ABN: 16 134 292 103 Document type: Training Date established: 2007 Date last reviewed: 2014 OBJECTIVES OF TRAINING FOR THE ANAESTHESIA TERM
College of Intensive Care Medicine of Australia and New Zealand ABN: 16 134 292 103 Document type: Training Date established: 2007 Date last reviewed: 2014 OBJECTIVES OF TRAINING FOR THE ANAESTHESIA TERM
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS)
 Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Wound Care in the Community. Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts
 Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
RESPIRATORY COMPLICATIONS AFTER SCI
 SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
