BROCHURE. Introductory course
|
|
|
- Gwen Sullivan
- 5 years ago
- Views:
Transcription
1 BROCHURE C P A P i n a m b u l a n c e s e r v i c e Introductory course
2 This brochure was written in connection with the introduction of CPAP into the ambulance service at University Hospital Northern Norway. The authors of the brochure are Lars-Jøran Andersson, Morten Lyngås Føyen and Johannes Strand. As authors we wish to give special thanks to Ole Magnus Filseth, who made his compendium on respiratory physiology available to us. Portions of this brochure quote directly from it. In addition to this, we have used Knut Dybwik s book on respiratory treatment as a source for the brochure. Johannes Strand did the layout and design. 2
3 It has been decided to introduce CPAP into the ambulances at the University Hospital of Northern Norway. This brochure has been written as part of this introduction. The brochure will be an introduction about what CPAP is and will provide the necessary basics for using the tool in an ambulance. In addition to this, all personnel will receive a day of training in the CPAP before it is put into service. Within emergency medicine, CPAP has traditionally been a procedure that was only available inside the hospital. The reason we wish to start using CPAP in the ambulance service is that early treatment contributes to shorter hospital stays and better care for the patient. CPAP is an advanced form of care. Knowledge of the indications and contraindications is therefore important. Successful CPAP treatment demands good cooperation between the provider and the patient, and alertness by the provider. Serious complications with CPAP are rare and the treatment can, when necessary, be quickly stopped. We believe that CPAP treatment will be used relatively seldom, but for the individual patient the treatment can offer a significant health advantage. It is important that one knows the equipment well so that the threshold for using it will be low. In the ambulance service, CPAP treatment will be prescribed by the doctor in the same way as medicinal treatment. I n t r o d u c t i o n What is CPAP and how does it work? CPAP treatment requires that the patient breathes in a closed tubal system that registers a continuous positive airway pressure. In our case, this will be a CPAP mask that is driven by the oxygen we have in the vehicles. In the ambulance service, CPAP is used for patients with serious respiratory failure. The indications will be: Pulmonary edema, asthma and COPD. CPAP improves oxygenation for these patients in three ways: 1. By causing the patient to breathe with a higher lung volume, which will increase the diffusion surface (reducing shunting). The resting lung volume (functional residual capacity - FRC) increases and atelectatic tissue (collapsed lung tissue) is inflated and atelectasis is prevented from reforming By displacing pulmonary fluid in lung congestion. Positive airway pressure reduces venous return to the heart (lowers preload ). In left ventricle failure, the heart s per minute volume will increase as a consequence of reduced preload. 3. By better lung compliance (respiration becomes easier and the quantity of CO2 in the blood is thereby reduced). It is easier for the patient to breathe with a lung that is inflated than when the resting volume of the lung is reduced. In other words, CPAP works in several ways to improve the patient s oxygenation. In order to have a good understanding of how this works, we must delve a little deeper into respiratory physiology... Don t worry, the explanation is coming ;-) Some unfamiliar words and expressions?
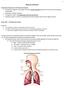
4 A n a t o m y a n d p h y s i o l o g y Airways The upper and lower airways have the task of conducting air to and from the lungs. In addition, they take care of filtering, warming and humidifying the air. Lungs The inner surface of the lungs of an adult person has an area the size of a tennis court. The primary tasks of the lungs can be divided into three main functions; oxygen uptake, carbon dioxide elimination and ph regulation. The alveoli are covered with a single layer of flat epithelial cells which form a thin membrane between the air in the alveoli and the blood in the capillaries. In addition, Lung capacity and volume Expiratory reserve volume approx ml Inspiratory reserve volume approx ml A healthy adult male has a total lung capacity (TLC) of approx. 6 liters, that is, the quantity of air found in the lungs after maximal inspiration. The tidal volume (TV) is the volume that is inspired in normal respiration and is approx. 0.5 liter. After normal expiration, a healthy adult male could expire approx. 1.5 liter. This is called expiratory reserve volume (ERV). What is left in the lungs is called residual volume (RV). the alveoli are covered with a lipoprotein (surfactant), which reduces the surface tension and thereby prevents the alveoli from closing at the same time that it ensures that they don t also over-distend. The lungs are very elastic and can be compared to a rubber band. A network of elastic fibers is found all over the lungs. From the resting position of the lungs, this can be stretched out and filled with air. For this to happen, the force that will expand the lung must overcome the elastic forces of the lung tissue. In addition, there is the elastic resistance found in the chest wall. Residual volume approx ml Vital capacity approx ml Tidal volume at rest is approx. 500 ml If you add ERV and RV you get functional residual capacity (FRC), which is the normal resting volume of the lungs. (During CPAP treatment, FRC is increased.) If after normal inspiration you continue to breathe in as much as you can, you obtain an inspiratory reserve volume (IRV), that is approx. 3 liters. 4
5 The elastic forces in the lungs and chest wall during expiration (breathing out) contract the lung back into the resting position. Expiration is therefore normally a passive act. In technical literature, the term compliance is used for the lungs elasticity. Hypoxia: Reduction of the oxygen supply in the tissues, despite adequate blood supply, is usually due to hypoxemia. Hypoxemia: Reduced oxygenation of the blood causes hypoxia. In practice, hypoxemia and hypoxia are often used interchangeably. Ischemia: Lack of oxygen in tissue, which is due to reduced blood supply in the tissue, as for example in angina pectoris. Asphyxia: Lack of oxygen in the inspired air, or absence of air to breath, synonymous with asphyxiation. Hypercapnia: Increased quantity of CO2 in the blood, synonymous with hypercapnia. Hypercapnia is a strong stimulus to increase respiration. Attempt to hold your breath while you measure oxygen saturation and you will experience a strong need to inhale before oxygen saturation falls. Hypocapnia: Reduced quantity of CO2in the blood, for example, a hyperventilating episode. The body s oxygen supply Hemoglobin (Hb): Oxygen-bearing molecules in erythrocytes. Every hemoglobin molecule can bind to four O2 molecules. Each gram of hemoglobin can bind to 1.34 ml of oxygen. If we want to indicate whether hemoglobin is bound to oxygen or not, we can distinguish between oxyhemoglobin (oxygen is bound) and deoxyhemoglobin. The quantity of hemoglobin in the body is normally g/dl. SaO2: Oxygen saturation in arterial blood. When all hemoglobin in the blood is saturated with oxygen, SaO2 is 100%. If SaO2 is, for example, 60%, this means that 60% of the binding sites for oxygen are bound to oxygen. SpO2: The organism s oxygen supply depends upon its ability to take up oxygen and the ability to transport it out of the body. Under normal circumstances, the oxygen supply depends upon the following factors. 1. Hemoglobin level 2. Oxygen saturation 3. Cardiac minute volume In order to obtain an adequate supply of oxygen, it is often possible to influence these three factors even by simple means outside of the hospital. The designation for arterial oxygen saturation when it is measured in the peripheral arterial blood using a pulse oximeter. The pulse oximeter distinguishes between oxygenated and deoxygenated hemoglobin using light with different wave lengths. With correct use and interpretation, SpO2 will correspond to SaO2. Words and Expressions... R e s p i r a t o r y p h y s i o l o g y 5
6 S t a t i c A i r w a y C o l l a p s e Functional residual capacity (FRC) is the quantity of air that is left in the lungs after normal expiration. When you breathe out and reach FRC, you are doing fine. You can then begin to breathe in, which will be both easy and natural. You can also choose to continue to breathe out until you reach residual volume, which is the amount of air which is left in the lungs after maximum expiration; it will feel heavier. Ordinarily we do not think about when we should stop breathing out and begin to breathe in, this is controlled by the respiratory center in the brainstem. Thus we choose unconsciously when we should begin to inhale. Even though the choice is unconscious, it is sensible and oriented toward ensuring good ventilation with the least possible effort. The functional residual capacity is determined therefore by the equilibrium between the forces that work in opposite directions. Some forces contribute to pulling the lungs out (filling the lungs), such as the elastic forces in the chest wall and muscle tone in the diaphragm, while the elastic forces of the lung tissue work oppositely (empty the lungs). In order to empty the lungs further once we have reached FRC, we must use the muscles to force expiration. FRC varies significantly, also within an individual patient. FRC is greater when standing then when lying down. FRC is reduced in collapse (atelectasis) of the lung tissue and in all of the processes that reduce the area of the lungs (pleural fluid, obesity and distended abdomen). FRC is reduced also by general anesthesia (narcosis) because of the loss of muscle tone in the diaphragm. In a normal healthy young adult all of the lung s segments will be open at the end of a normal expiration. But when we breathe out to the maximum, the small airways that exist farthest down in the lungs are closed. This is called static airway collapse. The lung volume at which this occurs is called closing capacity. We do not need to worry about this as long as it occurs after we have reached the functional residual capacity in expiration. Closing capacity is determined by the lung tissue s elastic properties. Closing capacity can be highly elevated in COPD. When closing capacity is higher than FRC, it means that portions of the airways collapse during normal breathing. This leads to an improper relationship between ventilation and circulation in the lungs. Circulated lung segments are not ventilated (shunt). The result will be poorer oxygenation of the blood. Closing capacity is an innate property of lung tissue and is independent of other processes. The functional residual capacity, on the other hand, can be influenced. A patient with an elevated closing capacity and worsening of COPD will thus benefit from measures that increase functional residual capacity. To raise into an upright position in order to get atelectatic (collapsed) lung tissue to open is an example of a measure that will increase FRC. CPAP is able to contribute to the opening of atelectatic tissue and will also make it easier to breathe with greater volume. S t a t i c a i r w a y c o l l a p s e In a COPD patient, resting elasticity in the lung tissue is reduced, such that the point at which the lungs begin to close by themselves ( c l o s i n g c a p a c i t y ) Closing capacity in a COPD patient is reached during normal expiration. This is a static airway collapse. Closing capacity in a healthy person Vital capacity approx ml Residual volume approx ml Tidal volume at rest approx. 500 ml 6
7 Dynamic airway collapse When we breathe out hard (forced expiration), the diaphragm, stomach and chest wall muscle is used to press together the chest cavity. Instead of negative pressure (as with ordinary expiration) we now have a positive pressure both in the chest cavity and around the lungs. We obtain a large pressure differential and we should expect a large expulsion of air from the airway. Along the airways a gradual fall in pressure from 85 to 0 cm H2O will occur. The pressure in the airways will be lower than the pressure around the lungs. If the airways were rigid tubes this would not mean much, but the alveolar passages and bronchioles are held distended by the surrounding elastic tissue and the bronchioles have cartilage that can only resist a certain outer pressure. In this case, we have a total or partial collapse of the airways that lasts until the forced expiration ceases. One has then a dynamic airway collapse, because it is related to the air expelled out of the lungs. If a person exhales with less force, the airway will remain open during expiration. In normal people, the dynamic airway collapse will show itself to be the upper limit of how fast the lungs take to empty of air (approx. 600 to 700 l/min, far above what we have need for under all physiological circumstances). The tendency to dynamic collapse increases when the airways are narrowed down, as in the case of pulmonary edema or asthma. It means that large portions of the airways will have collapsed before one has reached FRC. This means also that the lungs contain trapped air that does not come out. This air is under pressure and will form a resistance that must be overcome in the next inspiration. This phenomenon is called auto- PEEP or air trapping. CPAP reduces the pressure differential and therefore combats auto-peep. Blood flow and pressure in lung circulation The circulatory system consists of the greater (systemic) circulation and the lesser (lung) circulation. The greater and the lesser circulations are joined in a series. This does not apply to the fetus or persons with simple congenital heart failure. Flow through the pulmonary vascular bed varies as does systemic circulation between 5 l/min at rest to 25 l/min with high activity (in the well-trained). The tendency to dynamic collapse increases when airways are narrowed, as with pulmonary edema or asthma... Blood flow in the pulmonary circulation will therefore be equal to the blood flow in the systemic circulation. The pressure in the pulmonary arteries is only 1/6 of the pressure in the aorta. This means that if we measure systolic blood pressure at 120 mmhg, the pressure in the pulmonary arteries will be approx. 20 mmhg. A consequence of the lower pressure in the pulmonary arteries is that the blood flow to the lungs is more dependent upon gravity, such that at any time the lowest lying portions of the lungs have the best blood flow. Blood flow in the lungs will change with the patient s position. In lowerlying areas, there will be a tendency to poor ventilation, in the higherlying areas the tendency will be to poor perfusion. For the lungs overall, the relationship between ventilation and perfusion is good, nearly 1:1. Normally the driving pressure in lung circulation is determined by the difference between the pulmonary artery pressure and the pulmonary venous pressure. Clinical points: If a person has positive pressure in the airways (for example, CPAP or respiratory treatment), we can get a situation in which the driving pressure (blood pressure) is determined by the difference between the pulmonary arterial pressure and airway pressure. With a combination of high airway pressure and low pulmonary artery pressure, we can get a situation where the airway pressure is greater than the pulmonary arterial pressure in all or part of the lung. In a situation such as this, we will not get any blood flow to the actual area and the entire circulation could be affected. D y n a m i c a i r w a y c o l l a p s e 7
8 I n d i c a t i o n s Indications The indication for CPAP treatment in the ambulance service must be serious respiratory failure. In practice this will be asthma, COPD and heart failure/pulmonary edema. Respiratory failure We have respiratory failure when the gas exchange in the lungs leads to reduced oxygen saturation in the blood. If the respiratory failure is serious, we often see also an increase in carbon dioxide in the blood (hypercapnia). A series of conditions can cause respiratory failure, such as injuries, pneumonia, collapse of lung tissue (atelectasis), airway obstruction, drug reactions (for example, opiates) and sepsis. Patients with COPD can go about with chronic respiratory failure, but with gradual worsening as a consequence of airway infections. When assessing a patient with respiratory failure, it is necessary, in addition to oxygen saturation, to evaluate respiratory rate and depth, respiratory pattern, withdrawals, use of accessory muscles, psychic condition and whether the labor of breathing is tiring the patient. When we use CPAP in the ambulance, the patient must have a serious respiratory failure and one of the following conditions must also be suspected: pulmonary edema, COPD or asthma. P u l m o n a r y e d e m a The most frequent cause of pulmonary edema is heart failure. Certain toxins and various forms of overhydration can also cause pulmonary edema. Heart failure means that the heart s function as a pump is failing. Heart failure is a condition that can have different causes, for example, infarction, arrhythmia, valvular disease, infection, sepsis and cardiomyopathy. When the heart (left side) fails, the blood pressure in the pulmonary circulation is higher. Because of the elevated pressure, fluid leaks out into the space between the capillaries and the alveoli, then into the alveoli and leads to pulmonary edema. A patient with pulmonary edema will appear to be very affected. It can often be difficult to distinguish pulmonary edema from worsening of COPD or pneumonia. The treatment of heart failure depends upon the cause. For example, it might be PCI or valve surgery. Pre-hospital, the possibilities are medicinal treatment, positioning, oxygen and CPAP. In coronary disease (infarct) thrombolysis will also be a treatment option. In order to relieve the heart, the patient is positioned with the upper body high and is treated with nitro preparations (nitrolingual every 5 to 10 minutes), morphine (start dose of 2.5 to 5 mg) and diuretics (Furosemide 10 to 40 mg). CPAP has an effect on heart failure because the increase in airway pressure that CPAP provides leads to fluid being pushed back into the bloodstream. CPAP gives results also because it helps the patient to breathe at a higher lung volume, opens the lungs and reduces atelectasis formation. All these measures lead to lower blood flow in the heart and this is exactly the point. The heart receives less blood that must be pumped further, and is relieved. This means also that the patient must be monitored because the treatment can work so strongly that it leads the patient over into circulatory shock. Treatment of acute heart failure is a balancing art. S y m p t o m s a n d s i g n s : Agitation or anxiety Confusion and disorientation because of hypoxia Poor general condition, weakness Chest pain Cough - frothy, possible bloody expectorate Increasing shortness-of-breath and air hunger Increased respiratory rate Gurgling respiration and crackling sounds over the lungs Skin: Gray and cold sweats Cyanosis Jugular vein stasis Edema in the ankles and legs Drop in blood pressure Tachycardia and arrhythmia 8
9 A s t h m a / C O P D Chronic obstructive pulmonary disease is a composite designation for emphysema and chronic bronchitis, often caused by smoking. Some patients need home oxygen. Medicinal treatment includes inhalations, for example, salbutamol (ventoline) and ipratropium bromide (ipraxa) and steroids (for example pulmicort). With worsening, steroids may be given by I.V. or peroral, extra treatment with inhalations, theophylline (aminophylline) and oxygen. If a patient with worsening COPD needs intubation, it will often be a long respiratory handling. Early CPAP treatment can reduce the need for intubation. CPAP makes it easier for the patient to breathe at a higher lung volume (higher FRC), which allows more parts of the lungs to be ventilated. In other words, the tendency to static collapse of alveoli is reduced. Furthermore, CPAP reduces the tendency to dynamic airway C o n t r a - i n d i c a t i o n s Risk of aspiration If the patient vomits, the mask can fill up with vomit and the patient can aspirate. It is important to assess this risk before securing the mask with the straps. Lowered consciousness If the patient s consciousness is reduced, such that the patient risks not being able to maintain a free airway, the patient should not receive CPAP. Increased intracranial pressure CPAP can contribute to increased intracranial pressure because of increased intrathoracic pressure. It should not be used when there is a suspicion of head injury or brain hemorrhage. Pneumothorax CPAP, like intubation, causes higher airway pressure which can lead to worsening of pneumothorax. S y m p t o m s a n d s i g n s : Known primary disease Agitation/anxiety Problems speaking entire sentences Lowering consciousness, possible coma Dyspnea at rest Wheezing Exhales through pursed lips Cough, coughs up mucus Fever Increased respiratory rate Shallow breathing Use of accessory muscles Reduced respiratory sounds, wheezes Tachycardia, rise in blood pressure, fall in blood pressure, arrhythmia, cardiac arrest collapse because the pressure differential is less. Many COPD patients try to obtain this effect by breathing out through pursed lips. Systolic blood pressure <90 mmhg CPAP leads to higher intrathoracic pressure, something that can reduce blood flow to the heart. If the patient is about to go into circulatory shock, establishing CPAP can lead to circulatory collapse. Major bleeding Risk that the patient can develop circulatory shock which can worsen with the use of CPAP. Epiglottitus All manipulation with airways can lead to worsening of the condition. I n d i c a t i o n s a n d c o n t r a - i n d i c a t i o n s 9
10 C P A P t r e a t m e n t i n p r a c t i c e Equipment There are a number of types of CPAP systems. From CPAP functions in advanced respirators to simple systems that connect to an ordinary flow meter. The system we have chosen for the ambulance division of UNN is of the simple type. The system consists of a CPAP generator with integrated PEEP manometer and safety valve, mask and hood. This is coupled with ordinary oxygen tubing directly with the oxygen outlet in the vehicle or the portable O2 cylinder. The equipment is for one-time use and is disposed of after use. Assembly/start-up Have all equipment available before starting, ensure safety and inform the patient. Choose the correct mask size. Connect the tube to the flow meter. Start the flow at 15 l/minute. Put the mask on the patient so that it fits snugly. Secure the mask using the accompanying straps (when the patient accepts the mask). Adjust the flow to the PEEP pressure desired. Flow of 25 l/min is required to reach the highest PEEP resistance. SpO2 and blood pressure will be measured during the CPAP treatment. Maximum air or O2 flow - 30 l/minute. Flow/PEEP resistance Calculating oxygen Flow liter/minute 10 liter/min 15 liter/min 20 liter/min 25 liter/min Oxygen consumption CPAP/PEEP (cm H2O) Our CPAP system will normally use 15 to 25 liters of oxygen/minute. This means that the treatment is very oxygen-demanding and we must keep watch on how much oxygen we have available in the ambulance and how long a time we can continue the treatment. For long transport, a replacement of oxygen bottles underway must be planned for with pauses in the treatment. Patient experience/communication, requirements for success An indication for CPAP treatment is respiratory failure in connection with COPD and heart failure/pulmonary edema. Shortness-of-breath often leads to significant agitation and anxiety. In CPAP treatment, the mask is placed snugly over the patient s face and the patient experiences having to breath out against a resistance. Volume x pressure = available oxygen 5 liters x 200 bar = 1000 liters available oxygen liter per min 1000 liters 20 liter/minute = MAX treatment time = 50 minutes 10
11 It is not unusual for patients to accept the treatment poorly and try to remove the mask. For the treatment to succeed it is important for the patient to cooperate. Be calm and inform the patient of what is taking place. Sit together with the patient. Let the patient himself hold the mask snugly over the nose and mouth. Do not secure the mask before the patient is cooperating well and accepts the treatment. Observation and documentation Good patient examination and good observation are crucial in deciding that CPAP treatment should be started. During actual treatment, good observation is crucial for evaluating whether the patient is getting a result from the treatment, but also to prevent complications from arising that force us to break off or whether there is a failure in the equipment which requires fixing (leaks, lack of oxygen etc.) Note Consciousness, GCS should be scored, but it is a crude tool in this situation, assess also whether the patient is beginning to be sleepy and worn out. (CPAP treatment requires that the patient is awake and can keep the airways free.) Respiratory rate (RR), Respiratory pattern (superficial, accessory muscles etc.), Spo2. Pulse (rate, amplitude and regularity), skin (warm, cold, dry, clammy). Blood pressure. Temperature Documentation All observations and measures that are performed should be documented, also CPAP treatment. In addition to the usual vital parameters, it is important in CPAP treatment to document PEEP/CPAP pressure. Pressure is given in cm H2O, also document O2 l/min, also document how long the patient receives CPAP treatment. Also, be careful to document the changes in respiration of the patient (RR. SpO2). CPAP can be looked up in the ambulance reference under the category of medications. Put in the PEEP/CPAP pressure and draw a line through the boxes for it and show when the treatment occurred, show with gaps in the line when there were pauses in the treatment, or when the treatment ended. (see table) NOTE: CPAP treatment is administered Watch to see that the patient is exhaling through the port in the mask/cpap generator. In order for the patient to be able to exhale it is important that it does not become blocked! Also, be watchful with regard to the risk of aspiration in CPAP treatment. Never leave the patient during CPAP treatment! Sources of error PEEP/CPAP pressure Pause in treatment The Flow-Safe CPAP system is very simple and easy to assemble. Nevertheless errors can arise in the system. The most frequent is leaks, most frequently around the mask. If the mask does not fit tightly, there will not be the desired pressure in the system and consequently not the desired effect. It is also important that the CPAP generator is properly connected to the mask so that there is no harm to the O2 tubing, and that the O2 tubing is firmly connected to the flow meter. The system also requires adequate flow to reach the desired pressure. C P A P t r e a t m e n t i n p r a c t i c e 11
12 CPAP treatment (Continuous Positive Airway Pressure) REFERENCE HANDBOOK CPAP provides positive airway pressure both with inhalation and exhalation. Pre-hospital CPAP care means that we can avoid intubation and long intensive care for some patients. For pulmonary edema, good results are obtained by starting CPAP treatment before beginning medicinal treatment. For COPD/asthma, inhalation treatment with salbutamol and ipratropium bromide should be attempted before beginning CPAP. Indications Serious respiratory failure and suspicion of at least one of these conditions: Pulmonary edema COPD Asthma Contra-indications Risk of aspiration Lowered consciousness Increased intracranial pressure Pneumothorax Hypotension (systolic BT <95 mmhg) Major hemorrhaging Epiglottitis Before beginning, the following should be performed: Listen to the patient Check that we have enough oxygen, and possibly make a plan to order more. Start-up Have all equipment available for start-up, check for safety and inform the patient. Chose the correct mask size. Start CPAP system at a moderate setting (flow at 15 liters) Place the mask on the patient so that it fits snugly. When/if the patient accepts the mask, secure the mask using the accompanying straps. Adjust to the desired PEEP pressure. Usually a pressure between 5 and 10 cm H 2 O It is not unusual that patients accept the treatment poorly and attempt to remove the mask. In order for the treatment to succeed, it is important that the patient cooperate. Be calm and inform the patient about what is happening. Sit together with the patient. Let the patient himself hold the mask tightly over the nose and mouth and do not fasten the mask on the patient before the patient cooperates well and accepts the treatment. Monitoring/Evaluation Monitoring of SaO 2, BP and pulse at least every five minutes to begin with. Evaluate the treatment result continually. Pause or termination of the CPAP-treatment should be evaluated when other measures have had time to work; when the patient is improving significantly; if contra-indications arise during treatment; if the patient will not accept the mask or if the patient gets worse from the treatment.
CPAP. Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device. Charlottesville Albemarle Rescue Squad - CPAP
 CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory System. Chapter 9
 Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
ALCO Regulations. Protocol pg. 47
 For the EMT-Basic Objectives Understand ALCO regulations relative to monitoring pulse oximetry by the EMT-B Review the signs and symptoms of respiratory compromise. Understand the importance of adequate
For the EMT-Basic Objectives Understand ALCO regulations relative to monitoring pulse oximetry by the EMT-B Review the signs and symptoms of respiratory compromise. Understand the importance of adequate
Respiratory Physiology
 Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Respiratory Emergencies. Lesson Goal. Lesson Objectives 9/10/2012
 Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
Tuesday, December 13, 16. Respiratory System
 Respiratory System Trivia Time... What is the fastest sneeze speed? What is the surface area of the lungs? (hint... think of how large the small intestine was) How many breaths does the average person
Respiratory System Trivia Time... What is the fastest sneeze speed? What is the surface area of the lungs? (hint... think of how large the small intestine was) How many breaths does the average person
Lab 4: Respiratory Physiology and Pathophysiology
 Lab 4: Respiratory Physiology and Pathophysiology This exercise is completed as an in class activity and including the time for the PhysioEx 9.0 demonstration this activity requires ~ 1 hour to complete
Lab 4: Respiratory Physiology and Pathophysiology This exercise is completed as an in class activity and including the time for the PhysioEx 9.0 demonstration this activity requires ~ 1 hour to complete
Chronic Obstructive Pulmonary Disease
 136 PHYSIOLOGY CASES AND PROBLEMS Case 24 Chronic Obstructive Pulmonary Disease Bernice Betweiler is a 73-year-old retired seamstress who has never been married. She worked in the alterations department
136 PHYSIOLOGY CASES AND PROBLEMS Case 24 Chronic Obstructive Pulmonary Disease Bernice Betweiler is a 73-year-old retired seamstress who has never been married. She worked in the alterations department
Appendix E Choose the sign or symptom that best indicates severe respiratory distress.
 Appendix E-2 1. In Kansas EMT-B may monitor pulse oximetry: a. after they complete the EMT-B course b. when the service purchases the state approved pulse oximeters c. when the service director receives
Appendix E-2 1. In Kansas EMT-B may monitor pulse oximetry: a. after they complete the EMT-B course b. when the service purchases the state approved pulse oximeters c. when the service director receives
Respiratory System Mechanics
 M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
LUNGS. Requirements of a Respiratory System
 Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
PULMONARY FUNCTION. VOLUMES AND CAPACITIES
 PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
Continuous Positive Airway Pressure (CPAP) Paramedic Learner Package
 Continuous Positive Airway Pressure (CPAP) Paramedic Learner Package www.lhsc.on.ca/bhp 1 This page left blank intentionally. Table of Contents Introduction & Expectations... 4 Learning Objectives... 4
Continuous Positive Airway Pressure (CPAP) Paramedic Learner Package www.lhsc.on.ca/bhp 1 This page left blank intentionally. Table of Contents Introduction & Expectations... 4 Learning Objectives... 4
Bronchoconstriction is also treated with medications that inhibit bronchiolar constriction such as: Ipratropium (Atrovent)
 Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Respiratory System. December 20, 2011
 Respiratory System December 20, 2011 Nasal Cavity: Contains cilia (hair cells) to prevent particles from entering the respiratory tract Mucus does the same, in addition to warming and moistening the air
Respiratory System December 20, 2011 Nasal Cavity: Contains cilia (hair cells) to prevent particles from entering the respiratory tract Mucus does the same, in addition to warming and moistening the air
Condensed version.
 I m Stu 3 Condensed version smcvicar@uwhealth.org Listen 1. Snoring 2. Gurgling 3. Hoarseness 4. Stridor (inspiratory/expiratory) 5. Wheezing 6. Grunting Listen Crackles Wheezing Stridor Absent Crackles
I m Stu 3 Condensed version smcvicar@uwhealth.org Listen 1. Snoring 2. Gurgling 3. Hoarseness 4. Stridor (inspiratory/expiratory) 5. Wheezing 6. Grunting Listen Crackles Wheezing Stridor Absent Crackles
Approach to type 2 Respiratory Failure
 Approach to type 2 Respiratory Failure Changing Nature of NIV Not longer just the traditional COPD patients Increasingly Obesity Neuromuscular Pneumonias 3 fold increase in patients with Ph 7.25 and below
Approach to type 2 Respiratory Failure Changing Nature of NIV Not longer just the traditional COPD patients Increasingly Obesity Neuromuscular Pneumonias 3 fold increase in patients with Ph 7.25 and below
Appendix (i) The ABCDE approach to the sick patient
 Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Chapter 11: Respiratory Emergencies
 29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
Respiratory Pathophysiology Cases Linda Costanzo Ph.D.
 Respiratory Pathophysiology Cases Linda Costanzo Ph.D. I. Case of Pulmonary Fibrosis Susan was diagnosed 3 years ago with diffuse interstitial pulmonary fibrosis. She tries to continue normal activities,
Respiratory Pathophysiology Cases Linda Costanzo Ph.D. I. Case of Pulmonary Fibrosis Susan was diagnosed 3 years ago with diffuse interstitial pulmonary fibrosis. She tries to continue normal activities,
The Respiratory System Structures of the Respiratory System Structures of the Respiratory System Structures of the Respiratory System Nose Sinuses
 CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Chapter 10 Respiration
 1 Chapter 10 Respiration Introduction/Importance of the Respiratory System All eukaryotic organisms need oxygen to perform cellular respiration (production of ATP), either aerobically or anaerobically.
1 Chapter 10 Respiration Introduction/Importance of the Respiratory System All eukaryotic organisms need oxygen to perform cellular respiration (production of ATP), either aerobically or anaerobically.
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation.
 Chapter 1: Principles of Mechanical Ventilation TRUE/FALSE 1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation. F
Chapter 1: Principles of Mechanical Ventilation TRUE/FALSE 1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation. F
Chapter 10. The Respiratory System Exchange of Gases. Copyright 2009 Pearson Education, Inc.
 Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
ADVANCED ASSESSMENT Respiratory System
 ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Using an Inhaler and Nebulizer
 Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
Overview. The Respiratory System. Chapter 18. Respiratory Emergencies 9/11/2012
 Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP)
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) Continuous Positive Airway Pressure (CPAP) may be used as an adjunctive therapy for the treatment of patients with suspected Acute Pulmonary Edema, Chronic Obstructive
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) Continuous Positive Airway Pressure (CPAP) may be used as an adjunctive therapy for the treatment of patients with suspected Acute Pulmonary Edema, Chronic Obstructive
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Capnography. Capnography. Oxygenation. Pulmonary Physiology 4/15/2018. non invasive monitor for ventilation. Edward C. Adlesic, DMD.
 Capnography Edward C. Adlesic, DMD University of Pittsburgh School of Dental Medicine 2018 North Carolina Program Capnography non invasive monitor for ventilation measures end tidal CO2 early detection
Capnography Edward C. Adlesic, DMD University of Pittsburgh School of Dental Medicine 2018 North Carolina Program Capnography non invasive monitor for ventilation measures end tidal CO2 early detection
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Cardiovascular and Respiratory Disorders
 Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Unit 9. Respiratory System 16-1
 Unit 9 Respiratory System 16-1 Works together with the circulatory system Exchange of gases between atmosphere, blood, and cells If respiratory system and/or circulatory system fails, death will occur
Unit 9 Respiratory System 16-1 Works together with the circulatory system Exchange of gases between atmosphere, blood, and cells If respiratory system and/or circulatory system fails, death will occur
Chapter 10. Respiratory System and Gas Exchange. Copyright 2005 Pearson Education, Inc. publishing as Benjamin Cummings
 Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
Phases of Respiration. Chapter 18: The Respiratory System. Structures of the Respiratory System. Structures of the Respiratory System
 Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Training. Continuous Positive Airway Pressure (CPAP)
 Training The training module will follow the national standard curriculum as it relates to the application and use of CPAP. The proposed curriculum will closely resemble the following algorithm utilizing
Training The training module will follow the national standard curriculum as it relates to the application and use of CPAP. The proposed curriculum will closely resemble the following algorithm utilizing
Can be felt where an artery passes near the skin surface and over a
 1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
Circulatory System. and. Respiratory System. Ari Min, Yerim Lee and Min Ji Song THE HEART LUNGS. Monday, May 23, 2011
 Human Anatomy Circulatory System and THE HEART Respiratory System LUNGS Ari Min, Yerim Lee and Min Ji Song Purpose of the Circulatory System Function of circulatory system: exchange gases with cardiovascular
Human Anatomy Circulatory System and THE HEART Respiratory System LUNGS Ari Min, Yerim Lee and Min Ji Song Purpose of the Circulatory System Function of circulatory system: exchange gases with cardiovascular
The Respiratory System. Dr. Ali Ebneshahidi
 The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
Chapter 19 - Respiratory_Emergencies
 Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
About the Respiratory System. Respiratory System. Human Respiratory System. Cellular Respiration. Nostrils. Label diagram
 Respiratory System Human Respiratory System A system to deliver oxygen (O2) to body cells & get rid of carbon dioxide (CO2) as a waste through cellular respiration. Two systems involved: Respiratory &
Respiratory System Human Respiratory System A system to deliver oxygen (O2) to body cells & get rid of carbon dioxide (CO2) as a waste through cellular respiration. Two systems involved: Respiratory &
Pulmonary circulation. Lung Blood supply : lungs have a unique blood supply system :
 Dr. Ali Naji Pulmonary circulation Lung Blood supply : lungs have a unique blood supply system : 1. Pulmonary circulation 2. Bronchial circulation 1- Pulmonary circulation : receives the whole cardiac
Dr. Ali Naji Pulmonary circulation Lung Blood supply : lungs have a unique blood supply system : 1. Pulmonary circulation 2. Bronchial circulation 1- Pulmonary circulation : receives the whole cardiac
Why do you breathe? What is oxygen used for? Where does CO2 come from?
 RESPIRATORY SYSTEM How You Breathe Why do you breathe? What is oxygen used for? Where does CO2 come from? Respiration: exchange of gases between air & your body cells 1. Outside air (O2) lungs metabolism
RESPIRATORY SYSTEM How You Breathe Why do you breathe? What is oxygen used for? Where does CO2 come from? Respiration: exchange of gases between air & your body cells 1. Outside air (O2) lungs metabolism
The Respiratory System
 13 PART A The Respiratory System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Organs of the Respiratory
13 PART A The Respiratory System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Organs of the Respiratory
Firefighter Pre-Hospital Care Program Recruit Presentation. Respiratory Emergencies
 Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Capnography: The Most Vital Sign
 Capnography: The Most Vital Sign Mike McEvoy, PhD, NRP, RN, CCRN Cardiac Surgical ICU RN & Chair Resuscitation Committee Albany Medical Center EMS Coordinator Saratoga County, NY www.mikemcevoy.com CO
Capnography: The Most Vital Sign Mike McEvoy, PhD, NRP, RN, CCRN Cardiac Surgical ICU RN & Chair Resuscitation Committee Albany Medical Center EMS Coordinator Saratoga County, NY www.mikemcevoy.com CO
3. Identify the importance in the prehospital setting for the administration of nebulized bronchodilator.
 TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
PULMONARY FUNCTION TESTS
 Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Foundation in Critical Care Nursing. Airway / Respiratory / Workbook
 Foundation in Critical Care Nursing Airway / Respiratory / Workbook Airway Anatomy: Please label the following: Tongue Larynx Epiglottis Pharynx Trachea Vertebrae Oesophagus Where is the ET (endotracheal)
Foundation in Critical Care Nursing Airway / Respiratory / Workbook Airway Anatomy: Please label the following: Tongue Larynx Epiglottis Pharynx Trachea Vertebrae Oesophagus Where is the ET (endotracheal)
Northwest Community EMS System Continuing Education Class Credit Questions Respiratory Assessment January 2012
 Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete Reminder: You must schedule to take the class post-test with your assigned hospital EMS Coordinator/educator or their designee
Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete Reminder: You must schedule to take the class post-test with your assigned hospital EMS Coordinator/educator or their designee
COMPREHENSIVE RESPIROMETRY
 INTRODUCTION Respiratory System Structure Complex pathway for respiration 1. Specialized tissues for: a. Conduction b. Gas exchange 2. Position in respiratory pathway determines cell type Two parts Upper
INTRODUCTION Respiratory System Structure Complex pathway for respiration 1. Specialized tissues for: a. Conduction b. Gas exchange 2. Position in respiratory pathway determines cell type Two parts Upper
Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since.
 1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
Julie Zimmerman, MSN, RN, CCRN Clinical Nurse Specialist
 Julie Zimmerman, MSN, RN, CCRN Clinical Nurse Specialist Objectives Define capnography vs. end tidal CO2 (EtCO 2 ) Identify what normal vs. abnormal EtCO2 values mean and what to do Understand when to
Julie Zimmerman, MSN, RN, CCRN Clinical Nurse Specialist Objectives Define capnography vs. end tidal CO2 (EtCO 2 ) Identify what normal vs. abnormal EtCO2 values mean and what to do Understand when to
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing
 Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Unit 1 Exam: Respiratory and Circulatory Systems
 Name Date Unit 1 Exam: Respiratory and Circulatory Systems Multiple Choice. Please make your best selection. 1. Respiration is the process of: (a) Sucking air into the lungs (b) Converting glucose into
Name Date Unit 1 Exam: Respiratory and Circulatory Systems Multiple Choice. Please make your best selection. 1. Respiration is the process of: (a) Sucking air into the lungs (b) Converting glucose into
Unit 14: The Respiratory System
 Unit 14: The Respiratory System See what you already know! 1. Fill in the diagram on your own 2. Collaborate with your partner The Respiratory System The major function of the respiratory system is gas
Unit 14: The Respiratory System See what you already know! 1. Fill in the diagram on your own 2. Collaborate with your partner The Respiratory System The major function of the respiratory system is gas
Oxygenation. Chapter 45. Re'eda Almashagba 1
 Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Respiratory System. Organization of the Respiratory System
 Respiratory System In addition to the provision of oxygen and elimination of carbon dioxide, the respiratory system serves other functions, as listed in (Table 15 1). Respiration has two quite different
Respiratory System In addition to the provision of oxygen and elimination of carbon dioxide, the respiratory system serves other functions, as listed in (Table 15 1). Respiration has two quite different
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Yesterday we spoke of the increased airway resistance and its two examples: 1) emphysema, where we have destruction of the alveolar wall and thus reducing the area available for
بسم هللا الرحمن الرحيم Yesterday we spoke of the increased airway resistance and its two examples: 1) emphysema, where we have destruction of the alveolar wall and thus reducing the area available for
Respiratory Emergencies
 29698_CH11_Q_p001_012 4/12/05 2:03 PM Page 1 MEDICAL EMERGENCIES S E C T I O N 4 C H A P T E R Respiratory Emergencies 11 Workbook Activities The following activities have been designed to help you. Your
29698_CH11_Q_p001_012 4/12/05 2:03 PM Page 1 MEDICAL EMERGENCIES S E C T I O N 4 C H A P T E R Respiratory Emergencies 11 Workbook Activities The following activities have been designed to help you. Your
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Function: to supply blood with, and to rid the body of
 1 2 3 4 5 Bio 1102 Lec. 7 (guided): Chapter 10 The Respiratory System Respiratory System Function: to supply blood with, and to rid the body of Oxygen: needed by cells to break down food in cellular respiration
1 2 3 4 5 Bio 1102 Lec. 7 (guided): Chapter 10 The Respiratory System Respiratory System Function: to supply blood with, and to rid the body of Oxygen: needed by cells to break down food in cellular respiration
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Biology. A Guide to the Natural World. Chapter 30 Lecture Outline Transport and Exchange 1: Blood and Breath. Fifth Edition.
 Biology A Guide to the Natural World Chapter 30 Lecture Outline Transport and Exchange 1: Blood and Breath Fifth Edition David Krogh 30.1 The Cardiovascular System The Cardiovascular System The human cardiovascular
Biology A Guide to the Natural World Chapter 30 Lecture Outline Transport and Exchange 1: Blood and Breath Fifth Edition David Krogh 30.1 The Cardiovascular System The Cardiovascular System The human cardiovascular
Pancreas: digestive enzymes Liver: bile-helps to digest fat, stored in gallblader; breaks down toxins, makes some parts of blood
 1 2 3 Pancreas: digestive enzymes Liver: bile-helps to digest fat, stored in gallblader; breaks down toxins, makes some parts of blood 4 5 6 7 8 9 10 Highlights: - A pulse consists of two phases: contraction
1 2 3 Pancreas: digestive enzymes Liver: bile-helps to digest fat, stored in gallblader; breaks down toxins, makes some parts of blood 4 5 6 7 8 9 10 Highlights: - A pulse consists of two phases: contraction
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2
 2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
Human Circulation and Respiration Chapter 38
 Human Circulation and Respiration Chapter 38 Goals: 1. Compare closed and open circulatory systems. 2. Label the parts of the human heart. 3. Explain how blood travels through the heart; identify chambers
Human Circulation and Respiration Chapter 38 Goals: 1. Compare closed and open circulatory systems. 2. Label the parts of the human heart. 3. Explain how blood travels through the heart; identify chambers
The Respiratory System
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Packet #6 Cells: Internal Environment, part 2 (organ systems) Summer This Activity Packet belongs to:
 Packet #6 Cells: Internal Environment, part 2 (organ systems) Summer 2014 This Activity Packet belongs to: You should expect a variety of quizzes: announced, unannounced, open-notes and closed-notes. Packet
Packet #6 Cells: Internal Environment, part 2 (organ systems) Summer 2014 This Activity Packet belongs to: You should expect a variety of quizzes: announced, unannounced, open-notes and closed-notes. Packet
Coexistence of confirmed obstruction in spirometry and restriction in body plethysmography, e.g.: COPD + pulmonary fibrosis
 Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
6- Lung Volumes and Pulmonary Function Tests
 6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
Questions 1-3 refer to the following diagram. Indicate the plane labeled by the corresponding question number.
 Name: Grade: ANATOMY TEST Questions 1-3 refer to the following diagram. Indicate the plane labeled by the corresponding question number. 1. Plane #1 is the... 2. Plane #2 is the... 3. Plane #3 is the...
Name: Grade: ANATOMY TEST Questions 1-3 refer to the following diagram. Indicate the plane labeled by the corresponding question number. 1. Plane #1 is the... 2. Plane #2 is the... 3. Plane #3 is the...
Anatomy and Physiology
 Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Respiratory Physiology In-Lab Guide
 Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
2
 1 2 3 5 Major function of the Upper Respiratory tract is to warm, filter and humidify air. Discuss the consequences of intubation to the air passages and lungs e.g. dry O 2 delivered, mechanisms for moistening
1 2 3 5 Major function of the Upper Respiratory tract is to warm, filter and humidify air. Discuss the consequences of intubation to the air passages and lungs e.g. dry O 2 delivered, mechanisms for moistening
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
Respiratory System. Student Learning Objectives:
 Respiratory System Student Learning Objectives: Identify the primary structures of the respiratory system. Identify the major air volumes associated with ventilation. Structures to be studied: Respiratory
Respiratory System Student Learning Objectives: Identify the primary structures of the respiratory system. Identify the major air volumes associated with ventilation. Structures to be studied: Respiratory
Objectives. Health care significance of ARF 9/10/15 TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION
 TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION Louisa Chika Ikpeama, DNP, CCRN, ACNP-BC Objectives Identify health care significance of acute respiratory
TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION Louisa Chika Ikpeama, DNP, CCRN, ACNP-BC Objectives Identify health care significance of acute respiratory
Chapter Effects of Smoke on the Respiratory System Part 1 pages
 Chapter 18.1 Effects of Smoke on the Respiratory System Part 1 pages 412-416 ETS (Environmental Tobacco Smoke) Environmental Tobacco Smoke = ETS The smoke exhaled by active smokers. This smoke affects
Chapter 18.1 Effects of Smoke on the Respiratory System Part 1 pages 412-416 ETS (Environmental Tobacco Smoke) Environmental Tobacco Smoke = ETS The smoke exhaled by active smokers. This smoke affects
IRDS, Infantile Respiratory Distress Syndrome
 IRDS, Infantile Respiratory Distress Syndrome - RDS is the leading cause of death in the newborns, and the most common cause of death first 15 years of life (excluding the malformed babies). - RDS is the
IRDS, Infantile Respiratory Distress Syndrome - RDS is the leading cause of death in the newborns, and the most common cause of death first 15 years of life (excluding the malformed babies). - RDS is the
Cardiac Emergencies. A Review of Cardiac Compromise. Lawrence L. Lambert
 Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
Chapter 13. Respiratory Emergencies
 Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
