Reversal of hypotension with naloxone
|
|
|
- Felix Morrison
- 5 years ago
- Views:
Transcription
1 Reversal of hypotension with naloxone Thomas L. Higgins, M.D. Edward D. Sivak, M.D. Department of Pulmonary Disease Naloxone (Narcan) is an opiate antagonist widely used for reversal of narcotic overdose. Its mode of action appears to be displacement of opiates from receptor sites in the central nervous system and gut. 1 Recent evidence suggests that the body produces endogenous opiatelike substances in response to stress and that these substances produce opioid effects, including hypotension; this hypotension can be blocked or reversed by administration of naloxone. 3 ' 4 Scattered case reports suggest naloxone might have clinical utility in reversing septic or hypovolemic shock. 5 ' 6 Naloxone was administered to three patients with septic or cardiogenic shock, and a blood pressure response was observed in all three on six of nine separate occasions. The purpose of our report is to confirm previous observations of the antihypotensive effect of intravenous naloxone in septic shock and to report on a previously unreported temporary antihypotensive effect in cardiogenic shock. Case reports Case 1. A 70-year-old woman had been successfully treated with radiation therapy for a catecholamine-secreting chromaffin paraganglioma. She had remained in the hospital for total parenteral nutrition and on the 63rd hospital day had an 283
2 284 Cleveland Clinic Quarterly anterolateral myocardial infarction and respiratory failure. Morphine sulfate, 2 mg, was given during intubation, and subsequently the patient became normotensive. Four hours later, the blood pressure fell abruptly from 116/90 to 84/60 mm Hg. Dobutamine, 4.5 ig/kg/ min, for presumed pump failure had no effect. Naloxone, 0.4 mg, was given and a rise in blood pressure to 134/102 mm Hg was noted. The dobutamine was discontinued and dopamine instituted when the blood pressure fell to 70/62 one hour later. Despite increasing doses from 3 to 10 jug/kg/min, no effect was observed. Although no morphine was administered for 5 hours, administration of naloxone, 0.4 mg, raised the pressure to 84/66 mm Hg and an additional 0.8 mg produced a rise to 108/72 mm Hg. Cardiac output rose from 1.52 to 3.57 L/min. The central venous pressure and central venous wedge pressure remained constant. Despite increasing doses of dopamine to 23 jug/kg, the blood pressure again fell to 78/56 mm Hg after 30 minutes. Levarterenol, 20 jug/kg/min, was added and the patient's blood pressure was successfully maintained. No further naloxone was administered. The levarterenol and dopamine were later tapered and discontinued. Case 2. A 35-year-bld man with rectal carcinoma metastatic to the liver was admitted for intrahepatic artery chemotherapy with 5-fluorouracil and mitomycin-c. On the seventh hospital day progressive shortness of breath developed. A chest roentgenogram disclosed a left lower lobe infiltrate for which antibiotics were started. Within the next few hours, the blood pressure fell to 60/50 mm Hg. Methylprednisolone (SoluMedrol) was administered intravenously for presumed septic shock. Respiratory failure developed and morphine sulfate, 7.5 mg, was given for Vol. 48, No. 1 intubation. The blood pressure remained at 75/52 mm Hg, despite fluid challenge and dopamine, 19 jlig/kg/min, and levarterenol, 90 fig/kg/min. Naloxone, 0.8 mg, was administered with no significant response. A second dose of 0.8 mg was given 4 hours later; blood pressure rose from 60/0 to 78/57 mm Hg and fell to 67/57 mm Hg after 30 minutes. A third dose was given 40 minutes after the second, and the blood pressure rose to 76/59 mm Hg. Dopamine, 30 jug/kg/min, was also administered during this time. Two hours later ventricular fibrillation developed refractory to lidocaine therapy and the patient died. Case 3. A 51-year-old woman with systemic lupus erythematosus involving the central nervous system, liver, and kidneys was receiving cyclophosphamide (Cytoxan), 150 mg/dl and methylprednisolone, 20 mg intravenously, every 6 hours. Hypotension, tachypnea, and tachycardia developed. Blood cultures drawn a day earlier revealed grampositive cocci. Naloxone, 0.8 mg, produced a change in blood pressure from 93/64 to 149/96 mm Hg. Three hours later, the pressure fell to 75/44 mm Hg following diagnostic thoracentesis. Dopamine, 5.5 /ig/kg, and naloxone, 0.8 mg, were administered simultaneously and pressure rose to 101/57 mm Hg. Methylprednisolone, 1.0 g intravenously, every 8 hours for three doses was administered for septic shock. The patient's pressure remained normal and the dopamine was tapered and discontinued over 10 hours. Thirty hours from the initial hypotension, the pressure again fell to 74/64 mm Hg. Dopamine was started, 10 jtig/kg/min, and progressively increased to 50 /tg/kg/min without response. Naloxone, 0.8 mg, produced no change. Levarterenol, 10 through 100 /ig/kg/min, was ineffective,
3 Summer 1981 Reversal of hypotension with naloxone 1 o CM + o CM + Oi < < < z z z < u a.s c C r G g ^» *«S-=ï. g di z < z Bi oi oi < ^Oi + o c a D I >. "00 bo M C- S S bo 'So o o CM CM u u \ I* J J3 CO CO p- r» <T>.E c H "S CM Tf V \ \ c -H 0 in to D <u c c o o «^ O «S E EQ -Q a -C O CM co (O } CM S M COCO CO o d d T3 i- S O S.S V w bjd -I _ C «O 1,1 S ^ a v t o C/3 X
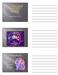
4 286 Cleveland Clinic Quarterly Vol. 48, No. 1 and the patient died. Postmortem examination revealed Staphylococcus aureus bronchopneumonia of the entire right lung. Results Naloxone was administered to three patients on nine occasions, and produced a greater than 10% change in mean arterial pressure (MAP) on six of nine trials. The Table summarizes the changes in MAP and the relation of the naloxone response to administration of opiates, corticosteroids, and pressor agents. In patient 1, 0.4 mg naloxone produced a 66% rise in MAP on the first occasion approximately 4 hours after the administration of 2 mg of morphine sulfate. Prior to this the patient was normotensive. One hour later (5 hours after the administration of morphine, the patient again became hypotensive. Although dopamine, 23 jug/kg/min; and dobutamine, 4.7 jug/kg/min, were being administered, the patient remained hypotensive until mg of naloxone was administered. On each occasion, the onset of naloxone's action was apparent at 30 to 60 seconds, reaching a maximum at 2 minutes and then gradually decreasing over 20 to 60 minutes. Levarterenol was administered following naloxone therapy and was effective in maintaining the blood pressure thereafter. Before the administration of 0.8 mg of naloxone, patient 2 was receiving dopamine, 19 jug/kg/min, and levarterenol, 90 /tg/kg/min, which maintained blood pressure at 75/52 mm Hg. In addition, methylprednisolone (Solu- Medrol), 1.0 g, had been administered 3 hours previously. The first dose of naloxone, 0.8 mg, produced no response and a second dose 4 hours later (7 hours after 1.0 g methylprednisolone) produced only a 21% increase in MAP. A final dose of naloxone, 0.8 mg, produced only 8.3% increase in MAP. Patient 3 initially responded to 0.8 mg of naloxone despite a regularly administered dose of 20 mg of methylprednisolone. After the initial dosage of naloxone, 0.8 mg, a 54% rise in MAP occurred within 2 minutes and fell gradually over the next 3 hours. A subsequent dose of 0.8 mg of naloxone produced a comparable 52% rise, which was maintained with dopamine therapy. Hypotension again developed and was refractory to treatment with 50 ig/ kg/min dopamine, 100 jug/kg levarterenol, or naloxone. Discussion Results of recent work have shown that the body produces opiatelike substances known as endorphins and enkephalins. These peptides bind opioid receptors in the brain and gut and have a spectrum of action similar to that of exogenous opioids. 1 There are several types of endorphins, all of which share a common N-terminal sequence identical to the pentapeptide metenkephalin. Much of the work involves study of the 31-amino acid molecule /?- endorphin, which encompasses the smaller a, y, and S endorphin molecules. 7 /^-endorphin is released in response to stress. 2 Furthermore, the release of [iendorphin appears to be closely related to the release of adrenocorticotrophin (ACTH), the two substances sharing a common precursor called pro-opiocortin. 1,7 Faden and Holaday 8 have postulated that there are selective advantages to the release of /^-endorphin in response to stress, especially severe injury. These advantages include reduction of blood pressure to aid in coagulation and relief of anxiety and pain. Administration of naloxone can prevent hypotension in
5 Summer 1981 Reversal of hypotension with naloxone 287 animals subjected to experimentally induced volume depletion or endotoxins. ' The mechanism of blood pressure reduction by endorphins is uncertain and may involve release of serotonin or histamine or vagal mediation of cardiac contractility. 8 In contrast, there is evidence that /^-endorphin acts as a central level in regulating blood pressure by interacting with a receptors. 9 We were unable to demonstrate the mechanism of action in our patients, but the rise in cardiac output noted in patient 1 and the lack of response to the centrally acting dopamine while response to peripherally acting levarterenol was maintained argues more for a peripheral vascular rather than a central nervous system mode of action. In addition, the absence of a change in pulse rate in any of the patients is against any sympathetic response. Prior steroid administration has been reported to interfere with the action of naloxone on blood pressure. 6 This interference was observed in patient 2, but not in patient 3 who was receiving maintenance therapy (methylprednisolone, 20 mg every 6 hours). Since /^-endorphin is thought to be tied to the same feedback mechanism as ACTH, it has been postulated that administration of corticosteroids suppresses the release of endorphins via negative feedback. 10 The use of corticosteroids may, therefore, exert an antihypotensive effect by preventing endorphin release. The lack of response to naloxone in steroid-treated patients may be due to extreme vasodilation no longer responsive to the antiendorphin effects of the agent, or that central receptors may be blocked with a weaker agent (steroids) preventing a more significant antihypotensive effect. What advantages does naloxone have over conventional agents for increasing blood pressure, such as levarterenol and dopamine? Aside from our observation that naloxone may be effective when dopamine fails, there are theoretical advantages of naloxone over the other pressor agents. Dopamine and levophed raise not only blood pressure but also pulmonary capillary wedge pressure and myocardial oxygen consumption. This may be undesirable in any critically ill patient, particularly one with myocardial ischemia. Dopamine in doses above 20 jug/kg/min and levarterenol cause tachycardia, vasoconstriction of the splanchnic and renal vasculature, and often a reduction in urine output. Naloxone, which has no effects aside from narcotic antagonism, should not have these undesirable side effects. 1 The need for repeated doses of naloxone prompted us to use a continuous drip of naloxone (unpublished data); this appears to be a preferable mode of administration. Naloxone is said to have no effects aside from narcotic antagonism and does not usually produce tachycardia, vasoconstriction, or changes in myocardial output. 1 However, hypertensive crisis, acutc pulmonary edema, and myocardial irritability have been reported following naloxone reversal of anesthesia. 11 " 13 Sudden death following administration of naloxone to reverse anesthesia in two healthy young women has also been reported. 14 Although the author postulates the cause of death to be ventricular fibrillation precipitated by hypoxia and an abrupt increase in blood catecholamine levels secondary to naloxone, idiosyncratic reaction could not be excluded. 14 We did not observe any immediate changes in heart rate or rhythm in our patients. However, the concern about possible effects of bolus administration of naloxone and the need for repeated doses has prompted us to change the mode of administration
6 288 Cleveland Clinic Quarterly Vol. 48, No. 1 to a bolus of 0.0 to 0.2 mg followed by continuous intravenous drip. Summary Although our analysis lacks comparison with a control population, intravenous injection of 0.4 to 0.8 mg of naloxone can effect a change in blood pressure in patients who have not recently received high-dose steroids. In addition, the observed antihypotensive effects of naloxone were recorded at a time sufficiently beyond morphine administration to suggest additional benefits of the agent. An effect was noted in a patient who failed to have a response to dopamine and dobutamine, but no effect was observed if a response to levarterenol was absent. Improved survival has already been demonstrated in animals subjected to experimental endotoxic or hypovolemic shock when naloxone was administered. 3,4 Our observations, along with these experiments, suggest that naloxone may have clinical utility in hypotensive states and that large scale studies would be appropriate. References 1. Jaffe JH, Martin WR. Opioid analgesics and antagonists. In: Gilman AG, Goodman LS, Gilman A, eds. Goodman and Gilman's The Pharmacologic Basis of Therapeutics. 6th ed. New York: MacMillan Publishing Co, 1980: Rossier J, French ED, Rivier C, Ling N, Guillemin R, Bloom FE. Foot-shock induced stress increases /^endorphin levels in blood but not brain. Nature 1977; 270: Holaday JW, Faden AI. Naloxone reversal of endotoxin hypotension suggests role of endorphins in shock. Nature 1978; 275: Faden AI, Holaday JW. Opiate antagonists; a role in the treatment of hypovolemic shock. Science 1979; 205: Tiengo M. Naloxone in irreversible shock. Lancet 1980; 2: Peters WP, Johnson MW, Wright RE, Mitch WE. Correction of hypotension by naloxone. Clin Res 1980; 28: 241 A. 7. Adler MW. Opioid peptides. Life Sei 1980; 26: Faden AI, Holaday JW. Experimental endotoxin shock; the pathophysiologic function of endorphins and treatment with opiate antagonists. J Infect Dis 1980; 142: Kunos G, Farsang C, Ramirez-Gonzales MD. /?-endorphin; possible involvement in the antihypertensive effect of central a-receptor activation. Science 1981; 211: Guillemin R, Vargo T, Rossier J, et al. ß- endorphin and adrenocorticotropin are secreted concomitantly by the pituitary gland. Science 1977; 197: Tanaka GY. Hypertensive reaction to naloxone. JAMA 1974; 228: Flacke JW, Flacke WE, Williams GD. Acute pulmonary edema following naloxone reversal of high-dose morphine anesthesia. Anesthesiology 1977; 47: Michaelis LL, Hickey PR, Clark TA, Dixon WM. et al. Ventricular irritability associated with the use of naloxone hydrochloride. Ann Thorac Surg 1974; 18: Andree RA. Sudden death following naloxone administration. Anesth Analg 1980; 59:
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Case year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50
 Case 1 65 year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50 Case 1 65 year old female nursing home resident with
Case 1 65 year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50 Case 1 65 year old female nursing home resident with
Titrating Critical Care Medications
 Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Antihypertensive Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE
 DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
SHOCK. Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital
 SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
Vasoactive Medications. Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis
 Vasoactive Medications Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis Objectives List components of physiology involved in blood pressure Review terminology related
Vasoactive Medications Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis Objectives List components of physiology involved in blood pressure Review terminology related
ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments
 ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
Evidence-Based. Management of Severe Sepsis. What is the BP Target?
 Evidence-Based Management of Severe Sepsis Michael A. Gropper, MD, PhD Professor and Vice Chair of Anesthesia Director, Critical Care Medicine Chair, Quality Improvment University of California San Francisco
Evidence-Based Management of Severe Sepsis Michael A. Gropper, MD, PhD Professor and Vice Chair of Anesthesia Director, Critical Care Medicine Chair, Quality Improvment University of California San Francisco
Lecture Notes. Chapter 2: Introduction to Respiratory Failure
 Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Swans and Pressors. Vanderbilt Surgery Summer School Ricky Shinall
 Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall Shock, Swans, Pressors in 15 minutes 4 Reasons for Shock 4 Swan numbers to know 7 Pressors =15 things to know 4 Reasons for Shock Not enough
Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall Shock, Swans, Pressors in 15 minutes 4 Reasons for Shock 4 Swan numbers to know 7 Pressors =15 things to know 4 Reasons for Shock Not enough
Swans and Pressors. Vanderbilt Surgery Summer School Ricky Shinall
 Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall SHOCK Hypotension SHOCK Hypotension SHOCK=Reduction of systemic tissue perfusion, resulting in decreased oxygen delivery to the tissues.
Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall SHOCK Hypotension SHOCK Hypotension SHOCK=Reduction of systemic tissue perfusion, resulting in decreased oxygen delivery to the tissues.
Taking the shock factor out of shock
 Taking the shock factor out of shock Julie Antonellis, BS, LVT, VTS (ECC) Northern Virginia Regional Director for the VALVT Technician Supervisor VCA Animal Emergency Critical Care Business owner Antonellis
Taking the shock factor out of shock Julie Antonellis, BS, LVT, VTS (ECC) Northern Virginia Regional Director for the VALVT Technician Supervisor VCA Animal Emergency Critical Care Business owner Antonellis
EMT. Chapter 10 Review
 EMT Chapter 10 Review 1. The term shock is MOST accurately defined as: A. a decreased supply of oxygen to the brain. B. cardiovascular collapse leading to inadequate perfusion. C. decreased circulation
EMT Chapter 10 Review 1. The term shock is MOST accurately defined as: A. a decreased supply of oxygen to the brain. B. cardiovascular collapse leading to inadequate perfusion. C. decreased circulation
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the
 Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
When Fluids are Not Enough: Inopressor Therapy
 When Fluids are Not Enough: Inopressor Therapy Problems in Neonatology Neonatal problem: hypoperfusion Severe sepsis Hallmark of septic shock Secondary to neonatal encephalopathy Vasoplegia Syndrome??
When Fluids are Not Enough: Inopressor Therapy Problems in Neonatology Neonatal problem: hypoperfusion Severe sepsis Hallmark of septic shock Secondary to neonatal encephalopathy Vasoplegia Syndrome??
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
CHAPTER II DRUG INDUCED PULMONARY DISEASES. BY J. jayasutha lecturer department of pharmacy practice Srm college of pharmacy SRM UNIVERSITY
 CHAPTER II DRUG INDUCED PULMONARY DISEASES BY J. jayasutha lecturer department of pharmacy practice Srm college of pharmacy SRM UNIVERSITY Drug Induced Pulmonary Disorders Is almost always a diagnosis
CHAPTER II DRUG INDUCED PULMONARY DISEASES BY J. jayasutha lecturer department of pharmacy practice Srm college of pharmacy SRM UNIVERSITY Drug Induced Pulmonary Disorders Is almost always a diagnosis
Blood Pressure. a change in any of these could cause a corresponding change in blood pressure
 Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Medical Management of Acute Heart Failure
 Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Shock. Shao Mian Emergency Department,Zhongshan Hospital
 Shock Shao Mian Emergency Department,Zhongshan Hospital What is shock THE BEGINNINGS OF UNDERSTANDING: THE LATE 19TH CENTURY THE AGE OF REASON: 1890 1925 THE MODERN ERA: BLALOCK S EPIPHANY POSTMODERNISM:
Shock Shao Mian Emergency Department,Zhongshan Hospital What is shock THE BEGINNINGS OF UNDERSTANDING: THE LATE 19TH CENTURY THE AGE OF REASON: 1890 1925 THE MODERN ERA: BLALOCK S EPIPHANY POSTMODERNISM:
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Adenosine. poison/drug induced. flushing, chest pain, transient asystole. Precautions: tachycardia. fibrillation, atrial flutter. Indications: or VT
 Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
FAILURE IN PATIENTS WITH MYOCARDIAL INFARCTION
 Br. J. clin. Pharmac. (1982), 14, 187S-19lS BENEFICIAL EFFECTS OF CAPTOPRIL IN LEFT VENTRICULAR FAILURE IN PATIENTS WITH MYOCARDIAL INFARCTION J.P. BOUNHOURE, J.G. KAYANAKIS, J.M. FAUVEL & J. PUEL Departments
Br. J. clin. Pharmac. (1982), 14, 187S-19lS BENEFICIAL EFFECTS OF CAPTOPRIL IN LEFT VENTRICULAR FAILURE IN PATIENTS WITH MYOCARDIAL INFARCTION J.P. BOUNHOURE, J.G. KAYANAKIS, J.M. FAUVEL & J. PUEL Departments
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
Norepinephrine (Levophed )
 Norepinephrine (Levophed ) Scope C3IFT CCT Generic Name: Norepinephrine Trade Name: Levophed Chemical Class: Therapeutic Class: Actions: Pharmacokinetics: Vasopressor Vasopressor Mechanism of Action: Norepinephrine
Norepinephrine (Levophed ) Scope C3IFT CCT Generic Name: Norepinephrine Trade Name: Levophed Chemical Class: Therapeutic Class: Actions: Pharmacokinetics: Vasopressor Vasopressor Mechanism of Action: Norepinephrine
Pediatric Sepsis Treatment:
 Disclosures Pediatric Sepsis Treatment: (treat) Early & (reevaluate) Often None June 11, 2018 Leslie Dervan, MD MS Pacific Northwest Sepsis Conference 1 Agenda Sepsis: pathophysiology at-a-glance Pediatric
Disclosures Pediatric Sepsis Treatment: (treat) Early & (reevaluate) Often None June 11, 2018 Leslie Dervan, MD MS Pacific Northwest Sepsis Conference 1 Agenda Sepsis: pathophysiology at-a-glance Pediatric
Means failure of heart to pump enough blood to satisfy the need of the body.
 Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Pediatric Code Blue. Goals of Resuscitation. Focus Conference November Ensure organ perfusion
 Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
What would be the response of the sympathetic system to this patient s decrease in arterial pressure?
 CASE 51 A 62-year-old man undergoes surgery to correct a herniated disc in his spine. The patient is thought to have an uncomplicated surgery until he complains of extreme abdominal distention and pain
CASE 51 A 62-year-old man undergoes surgery to correct a herniated disc in his spine. The patient is thought to have an uncomplicated surgery until he complains of extreme abdominal distention and pain
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency
 Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
VENTRICULAR FIBRILLATION. 1. Safe scene, standard precautions. 2. Establish unresponsiveness, apnea, and pulselessness. 3. Quick look (monitor)
 LUCAS COUNTY EMS SUMMARY PAGES VENTRICULAR FIBRILLATION 2. Establish unresponsiveness, apnea, and pulselessness 3. Quick look (monitor) 4. Identify rhythm 5. Provide 2 minutes CPR if unwitnessed by EMS
LUCAS COUNTY EMS SUMMARY PAGES VENTRICULAR FIBRILLATION 2. Establish unresponsiveness, apnea, and pulselessness 3. Quick look (monitor) 4. Identify rhythm 5. Provide 2 minutes CPR if unwitnessed by EMS
Nitroglycerin and Heparin Drip Interfacility Protocols
 Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Hypotension in the Neonate
 Neonatal Nursing Education Brief: Hypotension in the Neonate http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/ Neonatal
Neonatal Nursing Education Brief: Hypotension in the Neonate http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/ Neonatal
Shock and Vasopressors. Nina E. Glass, MD TACS Fellow SICU Didactic Curriculum 9/24/14
 Shock and Vasopressors Nina E. Glass, MD TACS Fellow SICU Didactic Curriculum 9/24/14 Review Question Unilaterally diminished breath sounds A. Figure 1 B. Figure 2 C. Both D. Neither Related Specialties
Shock and Vasopressors Nina E. Glass, MD TACS Fellow SICU Didactic Curriculum 9/24/14 Review Question Unilaterally diminished breath sounds A. Figure 1 B. Figure 2 C. Both D. Neither Related Specialties
SHOCK Susanna Hilda Hutajulu, MD, PhD
 SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
Drug Profiles Professional Responder
 Entonox Classification Medical Gas Entonox (50% oxygen 50% nitrous oxide) Effects Potent analgesic, weak anesthetic Onset Rapid Peak Immediate Indications Relief of moderate to severe pain Cardiac-related
Entonox Classification Medical Gas Entonox (50% oxygen 50% nitrous oxide) Effects Potent analgesic, weak anesthetic Onset Rapid Peak Immediate Indications Relief of moderate to severe pain Cardiac-related
LeMone & Burke Ch 30-32
 LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
Heart Failure. Dr. Alia Shatanawi
 Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
DOBUTamine INJECTION, USP R x only
 DOBUTamine INJECTION, USP R x only DESCRIPTION Dobutamine Injection, USP is 1,2-benzenediol, 4-[2-[[3-(4-hydro-xyphenyl)-1- methylpropyl]amino]ethyl]-hydrochloride, (±). It is a synthetic catecholamine.
DOBUTamine INJECTION, USP R x only DESCRIPTION Dobutamine Injection, USP is 1,2-benzenediol, 4-[2-[[3-(4-hydro-xyphenyl)-1- methylpropyl]amino]ethyl]-hydrochloride, (±). It is a synthetic catecholamine.
Nurse Driven Fluid Optimization Using Dynamic Assessments
 Nurse Driven Fluid Optimization Using Dynamic Assessments 2016 1 WHAT WE BELIEVE We believe that clinicians make vital fluid and drug decisions every day with limited and inconclusive information Cheetah
Nurse Driven Fluid Optimization Using Dynamic Assessments 2016 1 WHAT WE BELIEVE We believe that clinicians make vital fluid and drug decisions every day with limited and inconclusive information Cheetah
Admission of patient CVICU and hemodynamic monitoring
 Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
4/5/2018. Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY. I have no financial disclosures
 Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY I have no financial disclosures 1 Objectives Why do we care about sepsis Understanding the core measures by Centers for Medicare
Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY I have no financial disclosures 1 Objectives Why do we care about sepsis Understanding the core measures by Centers for Medicare
Medical Treatment for acute Decompensated Heart Failure. Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011
 Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms. Introduction to the Algorithms
 Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
EMT. Chapter 14 Review
 EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
Diagnosis & Management of Heart Failure. Abena A. Osei-Wusu, M.D. Medical Fiesta
 Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Cardiovascular Management of Septic Shock
 Cardiovascular Management of Septic Shock R. Phillip Dellinger, MD Professor of Medicine Robert Wood Johnson Medical School/UMDNJ Director, Critical Care Medicine and Med/Surg ICU Cooper University Hospital
Cardiovascular Management of Septic Shock R. Phillip Dellinger, MD Professor of Medicine Robert Wood Johnson Medical School/UMDNJ Director, Critical Care Medicine and Med/Surg ICU Cooper University Hospital
Adverse drug reactions. Dr. Mark Haworth MBChB DA MRCA
 Adverse drug reactions Dr. Mark Haworth MBChB DA MRCA Types of drug reaction The appearance of known side effects to a drug e.g. respiratory depression following the administration of opioid analgesics
Adverse drug reactions Dr. Mark Haworth MBChB DA MRCA Types of drug reaction The appearance of known side effects to a drug e.g. respiratory depression following the administration of opioid analgesics
Physiology #14. Heart Failure & Circulatory Shock. Mohammad Ja far Tuesday 5/4/2016. Turquoise Team. Page 0 of 13
 45 Physiology #14 Heart Failure & Circulatory Shock Mohammad Ja far Tuesday 5/4/2016 Turquoise Team Page 0 of 13 Heart Failure: It s a condition in which the heart can t perform its function properly;
45 Physiology #14 Heart Failure & Circulatory Shock Mohammad Ja far Tuesday 5/4/2016 Turquoise Team Page 0 of 13 Heart Failure: It s a condition in which the heart can t perform its function properly;
Useful diagnostic measures: chest x ray to check pulmonary edema, ECG and ECHO to detect cardiac abnormalities (1).
 Cardiogenic shock Etiology The most common cause of cardiogenic shock is LV dysfunction and necrosis as a result of acute myocardial infarction (AMI) (1). Acute valvular insufficiency or stenosis prevents
Cardiogenic shock Etiology The most common cause of cardiogenic shock is LV dysfunction and necrosis as a result of acute myocardial infarction (AMI) (1). Acute valvular insufficiency or stenosis prevents
Pheochromocytoma Crisis Presenting as Fulminant Cardiopulmonary Failure: A Case Report
 170 Pheochromocytoma Crisis Presenting as Fulminant Cardiopulmonary Failure: A Case Report Chun-Wen Chiu 1, Cheng-Hsiung Chen 2 Fulminant cardiopulmonary failure in a patient with pheochromocytoma is a
170 Pheochromocytoma Crisis Presenting as Fulminant Cardiopulmonary Failure: A Case Report Chun-Wen Chiu 1, Cheng-Hsiung Chen 2 Fulminant cardiopulmonary failure in a patient with pheochromocytoma is a
Cardiovascular Disorders. Heart Disorders. Diagnostic Tests for CV Function. Bio 375. Pathophysiology
 Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker
 PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE
 Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
The Pharmacology of Hypotension: Vasopressor Choices for HIE patients. Keliana O Mara, PharmD August 4, 2018
 The Pharmacology of Hypotension: Vasopressor Choices for HIE patients Keliana O Mara, PharmD August 4, 2018 Objectives Review the pathophysiology of hypotension in neonates Discuss the role of vasopressors
The Pharmacology of Hypotension: Vasopressor Choices for HIE patients Keliana O Mara, PharmD August 4, 2018 Objectives Review the pathophysiology of hypotension in neonates Discuss the role of vasopressors
Sepsis Pathophysiology
 Sepsis Pathophysiology How Kids Differ From Adults Steve Standage Pediatric Critical Care Medicine Seattle Children's Hospital University of Washington School of Medicine Disclosures & Preamble No agenda,
Sepsis Pathophysiology How Kids Differ From Adults Steve Standage Pediatric Critical Care Medicine Seattle Children's Hospital University of Washington School of Medicine Disclosures & Preamble No agenda,
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen
 Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT.
 HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
Post Resuscitation Care
 Princess Margaret Hospital f Children PAEDIATRIC ACUTE CARE GUIDELINE Post Resuscitation Care Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Princess Margaret Hospital f Children PAEDIATRIC ACUTE CARE GUIDELINE Post Resuscitation Care Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Control of blood tissue blood flow. Faisal I. Mohammed, MD,PhD
 Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Agonists: morphine, fentanyl Agonists-Antagonists: nalbuphine Antagonists: naloxone
 Opioid Definition All drugs, natural or synthetic, that bind to opiate receptors Agonists: morphine, fentanyl Agonists-Antagonists: nalbuphine Antagonists: naloxone Opioid agonists increase pain threshold
Opioid Definition All drugs, natural or synthetic, that bind to opiate receptors Agonists: morphine, fentanyl Agonists-Antagonists: nalbuphine Antagonists: naloxone Opioid agonists increase pain threshold
John Park, MD Assistant Professor of Medicine
 John Park, MD Assistant Professor of Medicine Faculty photo will be placed here park.john@mayo.edu 2015 MFMER 3543652-1 Sepsis Out with the Old, In with the New Mayo School of Continuous Professional Development
John Park, MD Assistant Professor of Medicine Faculty photo will be placed here park.john@mayo.edu 2015 MFMER 3543652-1 Sepsis Out with the Old, In with the New Mayo School of Continuous Professional Development
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Dilemmas in Septic Shock
 Dilemmas in Septic Shock William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center A 62 year-old female presents to the ED with fever,
Dilemmas in Septic Shock William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center A 62 year-old female presents to the ED with fever,
Sepsis is an important issue. Clinician s decision-making capability. Guideline recommendations
 Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012 Clinicians decision-making capability Guideline recommendations Sepsis is an important issue 8.7%
Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012 Clinicians decision-making capability Guideline recommendations Sepsis is an important issue 8.7%
Effects of intravascular volume expansion on the
 Br. J. Pharmac. (1984), 83,443-448 ffects of intravascular volume expansion on the cardiovascular response to naloxone in a canine model of severe endotoxin shock S. F. vans1, C.J. Hinds & J.G. Varley
Br. J. Pharmac. (1984), 83,443-448 ffects of intravascular volume expansion on the cardiovascular response to naloxone in a canine model of severe endotoxin shock S. F. vans1, C.J. Hinds & J.G. Varley
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Septic Shock. Rontgene M. Solante, MD, FPCP,FPSMID
 Septic Shock Rontgene M. Solante, MD, FPCP,FPSMID Learning Objectives Identify situations wherein high or low BP are hemodynamically significant Recognize complications arising from BP emergencies Manage
Septic Shock Rontgene M. Solante, MD, FPCP,FPSMID Learning Objectives Identify situations wherein high or low BP are hemodynamically significant Recognize complications arising from BP emergencies Manage
Cardiogenic shock: Current management
 Cardiogenic shock: Current management Janine Pöss Universitätsklinikum des Saarlandes Klinik für Innere Medizin III Kardiologie, Angiologie und internistische Intensivmedizin Homburg/Saar I have nothing
Cardiogenic shock: Current management Janine Pöss Universitätsklinikum des Saarlandes Klinik für Innere Medizin III Kardiologie, Angiologie und internistische Intensivmedizin Homburg/Saar I have nothing
Shock, Hemorrhage and Thrombosis
 Shock, Hemorrhage and Thrombosis 1 Shock Systemic hypoperfusion due to: Reduction in cardiac output Reduction in effective circulating blood volume Hypotension Impaired tissue perfusion Cellular hypoxia
Shock, Hemorrhage and Thrombosis 1 Shock Systemic hypoperfusion due to: Reduction in cardiac output Reduction in effective circulating blood volume Hypotension Impaired tissue perfusion Cellular hypoxia
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abdomen, and aorta, as causes of shock, point-of-care ultrasonography in assessment of, 915 917 Abdominal compartment syndrome, trauma patient
Note: Page numbers of article titles are in boldface type. A Abdomen, and aorta, as causes of shock, point-of-care ultrasonography in assessment of, 915 917 Abdominal compartment syndrome, trauma patient
Septic shock. Babak Tamizi Far M.D Isfahan university of medical sciences
 Septic shock Babak Tamizi Far M.D Isfahan university of medical sciences Definitions Used to Describe the Condition of Septic Patients Approximately 750,000 cases of severe sepsis or septic shock occur
Septic shock Babak Tamizi Far M.D Isfahan university of medical sciences Definitions Used to Describe the Condition of Septic Patients Approximately 750,000 cases of severe sepsis or septic shock occur
6 th Floor and 7 East Nurses Guide Intravenous Drip List Approved for RN Administration University of Kentucky Chandler Medical Center
 RATE Abciximab (Reopro) Alteplase (tpa, Activase) All units 6S and 6W ONLY Platelet aggregation inhibitor Thrombolytic agent Bolus: 0.25 mg/kg IV over 5 min Infusion: 0.125 0.9 mg/kg (max 90 mg); 10% of
RATE Abciximab (Reopro) Alteplase (tpa, Activase) All units 6S and 6W ONLY Platelet aggregation inhibitor Thrombolytic agent Bolus: 0.25 mg/kg IV over 5 min Infusion: 0.125 0.9 mg/kg (max 90 mg); 10% of
SHOCK. Pathophysiology
 SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United
 Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Shock. Perfusion. The cardiovascular system s circulation of blood and oxygen to all the cells in different tissues and organs of the body
 Shock Chapter 10 Shock State of collapse and failure of the cardiovascular system Leads to inadequate circulation Without adequate blood flow, cells cannot get rid of metabolic wastes The result- hypoperfusion
Shock Chapter 10 Shock State of collapse and failure of the cardiovascular system Leads to inadequate circulation Without adequate blood flow, cells cannot get rid of metabolic wastes The result- hypoperfusion
Pathophysiology. Tutorial 3 Hemodynamic Disorders
 Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow,
 1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow, cannot get rid of metabolic wastes Results in hypoperfusion
1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow, cannot get rid of metabolic wastes Results in hypoperfusion
Special circulations, Coronary, Pulmonary. Faisal I. Mohammed, MD,PhD
 Special circulations, Coronary, Pulmonary Faisal I. Mohammed, MD,PhD 1 Objectives Describe the control of blood flow to different circulations (Skeletal muscles, pulmonary and coronary) Point out special
Special circulations, Coronary, Pulmonary Faisal I. Mohammed, MD,PhD 1 Objectives Describe the control of blood flow to different circulations (Skeletal muscles, pulmonary and coronary) Point out special
Unit 4 Problems of Cardiac Output and Tissue Perfusion
 Unit 4 Problems of Cardiac Output and Tissue Perfusion Lemone and Burke Ch 30-32 Objectives Review the anatomy and physiology of the cardiovascular system. Identify normal heart sounds and relate them
Unit 4 Problems of Cardiac Output and Tissue Perfusion Lemone and Burke Ch 30-32 Objectives Review the anatomy and physiology of the cardiovascular system. Identify normal heart sounds and relate them
DBL DOBUTAMINE HYDROCHLORIDE INJECTION
 Name of medicine Dobutamine Hydrochloride DBL DOBUTAMINE HYDROCHLORIDE INJECTION Data Sheet New Zealand Presentation DBL Dobutamine Hydrochloride Injection is a sterile solution containing in each 20 ml
Name of medicine Dobutamine Hydrochloride DBL DOBUTAMINE HYDROCHLORIDE INJECTION Data Sheet New Zealand Presentation DBL Dobutamine Hydrochloride Injection is a sterile solution containing in each 20 ml
MWLCEMS SYSTEM Continuing Education Packet Management of the Acute MI Patient
 MWLCEMS SYSTEM Continuing Education Packet Management of the Acute MI Patient In this CE we will discuss the patient presenting with an acute ST-Elevation Myocardial Infarction (STEMI) Definition: Myocardial
MWLCEMS SYSTEM Continuing Education Packet Management of the Acute MI Patient In this CE we will discuss the patient presenting with an acute ST-Elevation Myocardial Infarction (STEMI) Definition: Myocardial
Frank Sebat, MD - June 29, 2006
 Types of Shock Hypovolemic Shock Low blood volume decreasing cardiac output. AN INTEGRATED SYSTEM OF CARE FOR PATIENTS AT RISK SHOCK TEAM and RAPID RESPONSE TEAM Septic or Distributive Shock Decrease in
Types of Shock Hypovolemic Shock Low blood volume decreasing cardiac output. AN INTEGRATED SYSTEM OF CARE FOR PATIENTS AT RISK SHOCK TEAM and RAPID RESPONSE TEAM Septic or Distributive Shock Decrease in
*Sections or subsections omitted from the full prescribing information are not listed.
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use GIAPREZA TM safely and effectively. See full prescribing information for GIAPREZA. GIAPREZA (angiotensin
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use GIAPREZA TM safely and effectively. See full prescribing information for GIAPREZA. GIAPREZA (angiotensin
Staging Sepsis for the Emergency Department: Physician
 Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
9/11/2012. Chapter 11. Learning Objectives. Learning Objectives. Endocrine Emergencies. Differentiate type 1 and type 2 diabetes
 Chapter 11 Endocrine Emergencies Learning Objectives Differentiate type 1 and type 2 diabetes Explain roles of glucagon, glycogen, and glucose in hypoglycemia Learning Objectives Discuss following medications
Chapter 11 Endocrine Emergencies Learning Objectives Differentiate type 1 and type 2 diabetes Explain roles of glucagon, glycogen, and glucose in hypoglycemia Learning Objectives Discuss following medications
Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium
 Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium MARIA E. MANDICH MD Fairbanks Memorial Hospital Emergency Department Attending Physician Interior Region EMS Council Medical Director
Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium MARIA E. MANDICH MD Fairbanks Memorial Hospital Emergency Department Attending Physician Interior Region EMS Council Medical Director
Cardiology. Objectives. Chapter
 1:44 M age 1121 Chapter Cardiology Objectives art 1: Cardiovascular natomy and hysiology, ECG Monitoring, and Dysrhythmia nalysis (begins on p. 1127) fter reading art 1 of this chapter, you should be able
1:44 M age 1121 Chapter Cardiology Objectives art 1: Cardiovascular natomy and hysiology, ECG Monitoring, and Dysrhythmia nalysis (begins on p. 1127) fter reading art 1 of this chapter, you should be able
Angina pectoris due to coronary atherosclerosis : Atenolol is indicated for the long term management of patients with angina pectoris.
 Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
Case I: Shock. A) What additional history would you like from the nursing home staff, patient s chart, and ambulance team?
 Case I: Shock It is your first night of call during your subinternship month, and you are asked by your resident to evaluate a patient in the emergency room. The patient is a 85yo female with a history
Case I: Shock It is your first night of call during your subinternship month, and you are asked by your resident to evaluate a patient in the emergency room. The patient is a 85yo female with a history
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
ACUTE HEART FAILURE. Julie Gorchynski MD, MSc, FACEP, FAAEM. Department of Emergency Medicine Emergency Residency Program UTHSC, San Antonio TCEP 2014
 ACUTE HEART FAILURE Julie Gorchynski MD, MSc, FACEP, FAAEM Department of Emergency Medicine Emergency Residency Program UTHSC, San Antonio TCEP 2014 No disclosures Objectives Overview Cases Current Therapy
ACUTE HEART FAILURE Julie Gorchynski MD, MSc, FACEP, FAAEM Department of Emergency Medicine Emergency Residency Program UTHSC, San Antonio TCEP 2014 No disclosures Objectives Overview Cases Current Therapy
Medical APMLE. Podiatry and Medical.
 Medical APMLE Podiatry and Medical http://killexams.com/exam-detail/apmle Question: 290 Signs and symptoms of hemolytic transfusion reactions include: A. Hypothermia B. Hypertension C. Polyuria D. Abnormal
Medical APMLE Podiatry and Medical http://killexams.com/exam-detail/apmle Question: 290 Signs and symptoms of hemolytic transfusion reactions include: A. Hypothermia B. Hypertension C. Polyuria D. Abnormal
Myocardial Infarction: Left Ventricular Failure
 CARDIOVASCULAR PHYSIOLOGY 93 Case 17 Myocardial Infarction: Left Ventricular Failure Marvin Zimmerman is a 52-year-old construction manager who is significantly overweight. Despite his physician's repeated
CARDIOVASCULAR PHYSIOLOGY 93 Case 17 Myocardial Infarction: Left Ventricular Failure Marvin Zimmerman is a 52-year-old construction manager who is significantly overweight. Despite his physician's repeated
