AS BETTER medical care allows. Splenorenal Shunt. An Ideal Procedure in the Pacific. See Invited Critique at end of article ORIGINAL ARTICLE
|
|
|
- Theodore Todd
- 5 years ago
- Views:
Transcription
1 Splenorenal Shunt ORIGINAL ARTICLE An Ideal Procedure in the Pacific Linda L. Wong, MD; Cedric Lorenzo, MD; Whitney M. Limm, MD; Livingston M. Wong, MD Hypothesis: Splenorenal shunt, an accepted treatment to prevent recurrent variceal bleeding, is an ideal procedure for patients with psychosocial issues or limited access to tertiary medical centers. Methods: We retrospectively reviewed the medical records of 34 patients (32 distal splenorenal shunts and 2 central splenorenal shunts) treated from January 1, 1995, through December 31, 2001, for demographic data, substance abuse status, psychosocial factors, previous treatments, Child class, length of hospital stay, operative transfusions, complications, and outcome. Results: Of the 34 patients, 17 were from surrounding Pacific islands (as many as 3800 miles away from Honolulu, Hawaii). Sixteen patients were Child class A, and 18 were Child class B. Twenty-four patients were either homeless, actively involved in substance abuse, or being treated for psychiatric problems, and 20 patients were either uninsured or insured by third-party payers that did not cover liver transplantation. Four patients underwent distal splenorenal shunt for a failed transjugular intrahepatic portosystemic shunt. Patients received a mean of 1.3 U of packed red blood cells (range, 0-5 U), and 15 received no blood transfusions. Mean length of hospital stay was 12.7 days (9 days postoperatively). Perioperative mortality was 8.8%. Three patients rebled postoperatively, 2 because of gastric ulcers and 1 because of an inadequate shunt. The 1-year survival rate was 95% in the 20 patients for whom data were available. Conclusions: Splenorenal shunt is an important treatment for noncompliant patients or patients living in remote areas where access to specialized treatments, such as endoscopy, transjugular intrahepatic portosystemic shunt, ultrasonography, and liver transplantation, is limited. We can achieve acceptable morbidity and mortality in this group of patients, although follow-up can be difficult. Arch Surg. 2002;137: From the Department of Surgery, St Francis Medical Center, University of Hawaii School of Medicine, Honolulu. AS BETTER medical care allows patients to live longer with complications of cirrhosis, variceal bleeding will become more prevalent. Liver transplantation is the ultimate option for complications of liver disease, but the harsh reality is that there are simply not enough livers for all patients with end-stage liver disease. Despite splitliver techniques, adult-sized live-donor liver transplants, and donors with expanded criteria, many patients will still die as a result of end-stage liver disease. Thus, it is important for liver surgeons and hepatologists to determine which patients are truly viable candidates for transplantation and which should be treated in a more palliative way. Surgical shunts, the distal splenorenal shunt in particular, are an excellent choice for control of recurrent variceal bleeding. Rebleeding and encephalopathy rates are low, and shunt patency is excellent. 1-6 Patients undergo a minimum of follow-up diagnostic studies, and this also appears to be cost-effective. 7 Surgical shunts have been used to treat patients with variceal bleeding, as a definitive treatment and as a bridge to liver transplantation in patients with reasonable hepatic synthetic function. 4,7,8 See Invited Critique at end of article Transjugular intrahepatic portosystemic shunts (TIPSs) have also been 1125
2 Sociodemographic and Disease Characteristics of 34 Patients With Splenorenal Shunts No. of Characteristic Patients of residence Oahu, Hawaii 18 Maui, Hawaii 8 Guam 4 Hawaii (Big ), Hawaii 2 American Samoa 1 Truk 1 Cause of liver disease Hepatitis C and alcoholic liver disease 15 Alcoholic liver disease 5 Hepatitis B 3 Cryptogenic cirrhosis 3 Hepatitis C 2 Hepatitis B and C and alcoholic liver disease 2 Autoimmune disease/primary biliary cirrhosis 2 Noncirrhotic portal hypertension 2 Psychosocial factor Alcohol, active use 13 Alcohol, past abuse 9 Intravenous drug abuse 10 Other illicit drug use 7 Smoking 22 Currently unemployed 19 Homeless 5 Documented history of psychiatric disorder 4 Incarcerated 1 Insurance status Insured 14 Insured, but liver transplantation not covered 18 Uninsured 2 Liver transplantation status Had subsequent liver transplantation 1 Placed on waiting list but removed for noncompliance 2 Awaiting a transplant and on list 2 Not a candidate for transplantation 29 used to treat variceal bleeding. This interventional radiologic procedure, in which a communication is created between the portal vein and a hepatic vein, nearly revolutionized treatment for variceal bleeding in the early 1990s because of its minimally invasive approach. After several years of mainstream use, however, enthusiasm has waned because of problems with shunt stenosis or occlusion. Ultrasonography studies and venograms are necessary for close follow-up, and reinterventions to maintain or salvage the shunt are frequently required In Hawaii, we have a unique population of patients who frequently come from distant Pacific s for treatment of complicated medical problems. Medical care in these remote areas is often limited to primary care and basic general surgical procedures in good-risk patients. If more complex problems are present or patients are a poor risk, such as those with variceal bleeding, referral to the tertiary care centers in Honolulu, Hawaii, on the island of Oahu, is generally required. Once the problem is addressed and the patient returns home, follow-up care and compliance are often minimal. Many areas do not have access to blood banks, endoscopy, abdominal ultrasonography, or interventional radiology. Several tertiary care centers on Oahu have the ability to perform TIPS, and about 60 such procedures were performed at our medical center from January 1, 1995, through December 31, It is often impossible to reevaluate the TIPS with ultrasonograms in patients who have no access to ultrasonography or who cannot return to Honolulu because of financial constraints. Because of problems with compliance and follow-up, we have increasingly recommended splenorenal shunts. In this article, we review our experience with this procedure. SUBJECTS AND METHODS We retrospectively reviewed the medical records of all patients who underwent splenorenal shunt during the 6-year period from January 1, 1995, through December 31, Demographic data, including age, sex, race, and island of residence, were noted. We also recorded the cause of the liver disease, the number of variceal bleeding episodes, and previous treatments. Psychosocial issues, including history of smoking, use of alcohol or other drugs, documented psychiatric history, living arrangements, and insurance status, were noted. Finally, information on encephalopathy, ascites, bilirubin, prothrombin time, and albumin were reviewed to calculate a Child-Pugh score. Patients were then classified as follows: Child A indicates a Child-Pugh score of less than 7; Child B, Child-Pugh score of 7 to 9; and Child C, Child-Pugh score of 10 or higher. In terms of the treatment, we noted the type of splenorenal shunt, the number of blood transfusions required during surgical treatment, the length of the hospital stay, and whether the procedure was elective or semiurgent. Those patients undergoing elective splenorenal shunt were not bleeding at the time of admission but had bled recently on previous admissions. Semiurgent splenorenal shunt implied that the patient was bleeding on hospital admission but was stabilized for at least 3 days before surgical treatment and was not actively bleeding at the time of the operation. We also reviewed the medical records for postoperative complications and rebleeding. Follow-up visits were recorded for patients who lived on Oahu. Patients on the neighboring Hawaiian s and other Pacific s were monitored by their local primary care physician, and follow-up by our group was made via telephone calls or clinic notes. For those patients who were supposedly lost to follow-up, we called all physicians involved, attempted to contact patients at their last known addresses and telephone numbers, and searched all published obituaries in both major newspapers in Hawaii from the time of the operation until the present. RESULTS During the 6-year period from January 1, 1995, to December 31, 2001, 34 splenorenal shunts were performed by our group of surgeons. The mean patient age was 50.4 years, and there were 24 men and 10 women. Nineteen patients were white, 10 were Asian (Japanese, 2; Chinese, 2; Korean, 2; Filipino, 2; and Vietnamese, 1) and 5 were Pacific ers (Chamorran, 3; Samoan, 1; and Marshallese, 1). A little more than half the patients were from Oahu, the island on which these splenorenal shunts were performed at 3 tertiary medical centers (Table). 1126
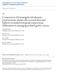
3 Northern Marianas Wake Midway Hawaii Palau Guam Marshall s Johnston Palmyra To Asia Micronesia Papau New Guinea Nauru Solomon s Tuvalu Howland/Baker Kiribati Tokalau Jarvis Australia Coral Sea Vanuatu New Caledonia Wallis Fiji Norfolk Western Samoa Tonga American Samoa Cook Niue French Polynesia Pitcairn New Zealand Patients in the Pacific s travel long distances to Honolulu, Hawaii, for treatment of variceal bleeding. The arrows indicate flight paths taken to reach tertiary medical centers in Honolulu. Eight patients were from Maui, a Hawaiian island (approximately 90 miles from Oahu), 4 patients were from Guam (3800 miles away), 2 patients were from the Big of Hawaii (210 miles away), 1 patient was from American Samoa (2598 miles away), and 1 patient was from Truk, a Northern Marianas island (approximately 3500 miles away) (Figure). All patients from islands other than Oahu were brought in by air ambulance. Endoscopy was not available in Samoa and Truk. At the time of these transfers, Doppler ultrasonography and interventional radiology were not available on any of these islands except Oahu. Twenty-four of 34 patients undergoing splenorenal shunt had hepatitis C, alcoholic liver disease, or a combination of these diseases. Three patients had cryptogenic cirrhosis, and 2 patients had autoimmune disease or primary biliary cirrhosis. Two patients had noncirrhotic portal hypertension, including 1 with lymphoma and leukemia and another with schistosomiasis (Table). With regard to psychosocial issues, 22 patients were either actively using alcohol or had abused alcohol in the past; 22 patients also had a history of smoking, with 14 currently smoking. Ten patients had a history of intravenous drug abuse, and 7 patients used other illicit drugs (cocaine, heroin, and methamphetamine). Eleven patients were currently employed, and 19 were currently unemployed, not including patients who were retired or disabled. Four patients had documented psychiatric problems for which they were being treated. Five patients were homeless, and 1 patient was imprisoned at the time of surgical treatment (Table). Of the 34 patients who underwent splenorenal shunt, 14 patients had insurance that would also cover liver transplantation, if necessary. Eighteen patients had either state government or Pacific subsidized medical insurance that either did not cover liver transplantation or might cover it in a transplant center outside Hawaii, provided that certain criteria were met. Two patients were uninsured (Table). Three patients underwent central splenorenal shunt because of massive splenomegaly and ascites in addition to bleeding, and the remaining 31 patients underwent distal splenorenal shunt with splenopancreatic-gastric disconnection. Fifteen operations were performed on an elective basis. The remaining 19 patients were admitted urgently for a variceal bleeding episode and stabilized for 3 to 8 days prior to undergoing surgical treatment. No patient was actively bleeding at the time of the operation. In patients for whom the information was available, 31 had a mean of 3 bleeding episodes before surgical treatment. Nine patients had operations following their first bleeding episode because of severe esophageal and gastric varices, and 4 patients underwent distal splenorenal shunt for a failed TIPS. Sixteen patients were Child class A, and 18 patients were Child class B on the day of the operation. Blood transfusions at the time of surgical treatment were from 0 to 5 U of packed red blood cells. The mean transfusion was 1.3 U, and 15 patients did not receive any transfusion. The mean length of hospital stay was 12.7 days total or 9 days postoperatively. Two patients had early bleeding postoperatively that was related to gastric ulcers, but no interventions other 1127
4 than transfusions and endoscopy were necessary. Rebleeding occurred in 1 patient who had an incomplete splenopancreatic-gastric disconnection and an extremely large left coronary vein. He underwent placement of a transjugular, intrahepatic, portosystemic shunt, which was complicated by portal vein thrombosis 4 months postoperatively. He then required a modified Sugiura procedure (gastric devascularization and esophageal transection) for recurrent bleeding because he was not a candidate for transplantation. No patient died intraoperatively or in the 7 days following surgical treatment. Three patients died in the 30- day period after splenorenal shunt. One patient died of massive liver failure on postoperative day 17. Another patient died on postoperative day 9 because of respiratory failure and a fungal infection probably related to steroid use for her autoimmune disease. The third patient died of complications related to acute pancreatitis on postoperative day 26. Of the 31 patients who survived the perioperative period, 3 patients are known to have died of unrelated causes at 8 months, 3 years, and 4 years following the operation. Of the remaining patients, 24 are known to be alive, and 5 have been lost to follow-up; 3 patients who have been lost to follow-up have not appeared on any published obituary list since their operation. Two patients live in Guam and have not been seen by physicians there. Of the 20 patients for whom data are available and who survived the perioperative period, the 1-year survival rate was 95%. COMMENT Multiple studies have confirmed the efficacy of splenorenal shunts. In series with 32 to 296 patients, perioperative mortality has ranged from 0% to 14%. 1,3,4,6,12-14 Shunt patency rates have been 92% to 94%, 1,3,5,13 and the likelihood of rebleeding has been 3.8% to 14%. 1,3,4,6,12-14 The rate of portosystemic encephalopathy has been reported to be 5% to 19%. 1,3-5,12-14 Maintenance of portal circulation by splenopancreatic disconnection plays a role in the development of encephalopathy. Spina et al 15 demonstrated in 27 of 131 patients that those who underwent distal splenorenal shunt with splenopancreatic disconnection were much less likely to develop chronic encephalopathy (0% vs 17% in patients with no splenopancreatic disconnection). Those 18 patients (14%) who developed chronic encephalopathy tended to have abolished portal perfusion. Jin and Rikkers 16 also confirmed that early portal vein thrombosis following distal splenorenal shunt contributed significantly to the development of both encephalopathy and severe ascites. Nonsurgical TIPS is used to control variceal bleeding and treat refractory ascites. This is a minimally invasive procedure performed by interventional radiologists with high technical success rates (greater than 90%) and excellent initial control of bleeding in most series. 9,10,17 Unfortunately, TIPS stenosis occurs in 50% to 70% of patients and accounts for a rebleeding rate of 15% to 30%. Encephalopathy also occurs in about 15% to 30% of patients, and TIPS can be used as a bridge to liver transplantation in patients with recurrent variceal bleeding. Early reports even suggested that TIPS could decrease blood loss at transplantation because of decreased portal hypertension. 20,21 Later studies, however, demonstrated that blood loss, operative time, and length of hospital stay were not affected by the presence of a TIPS before liver transplantation A number of groups have directly compared outcome in patients undergoing distal splenorenal shunt vs TIPS. Two retrospective studies on Child class A and B patients demonstrated that patients who underwent TIPS had significantly higher rebleeding rates because of shunt stenosis and required more interventions. 12,13 Helton et al 25 conducted a prospective, randomized trial of 40 patients with Child class A or B scores and variceal bleeding; 20 underwent distal splenorenal shunt, and 20 underwent TIPS. The 30-day mortality was higher in patients who underwent TIPS (20% vs 0% in patients who underwent distal splenorenal shunt). The patients who underwent TIPS also had significantly more rebleeding episodes, diagnostic studies, shunt revisions, and rehospitalizations. Total charges for a patient who underwent TIPS were $ vs $ for a patient who underwent distal splenorenal shunt. Finally, a decision analysis model by Zacks et al 7 of Child class A patients with cirrhosis and variceal bleeding demonstrated that a patient who underwent TIPS survived a mean of 1.96 years and required 1.7 procedures at a cost of $41685 compared with a patient who underwent distal splenorenal shunt, survived 1.86 years, and required 1.0 procedures at a cost of $ They concluded that distal splenorenal shunt was more cost-effective. Most will agree that distal splenorenal shunt is the procedure of choice for a Child class A patient with variceal bleeding. For patients who are Child class B or C, the possibility of a liver transplant looms in the future and often plays a role in deciding between TIPS or distal splenorenal shunt. Menegaux et al 26 studied 38 patients who underwent liver transplantation; 25 had TIPS, and 32 had splenorenal shunt prior to transplantation. Patients who had a pretransplantation TIPS required fewer blood transfusions at the time of the operation and had shorter operative times and shorter hospital and intensive care unit stays. Abouljoud et al 27 reviewed 35 patients with liver transplants, 18 with previous TIPS, and 17 with previous distal splenorenal shunt. No difference in the intraoperative transfusion requirement was noted, although the operative time was longer in the distal splenorenal shunt group. There were 3 deaths in the distal splenorenal shunt group compared with no deaths in the TIPS group. Intraoperative hemodynamics were better in the TIPS group because portal vein pressures were significantly higher. Both studies suggested that TIPS was perhaps a more favorable choice as a bridge to transplantation. In general, it is difficult to study this group of patients in large, randomized, controlled prospective trials. These patients are frequently unreliable and noncompliant, with diseases that are often self-induced and ongoing. One study even reported that 19% of patients were lost to follow-up. 5 Unfortunately, we have often been unable to document many of these psychosocial factors 1128
5 at the time the patient is admitted to the hospital with acute variceal bleeding. Four such patients in our series underwent distal splenorenal shunt after their TIPS had occluded, and we had determined these patients to be noncompliant or unsuitable candidates for transplantation. This approach has been described by Selim et al 28 who performed conversion of failed TIPS to distal splenorenal shunts in 4 patients with Child class A or B cirrhosis; however, these conversions were done for primarily technical reasons. For the noncompliant patient and the patient who is not a candidate for a transplant, distal splenorenal shunt is the ideal procedure. Studies have consistently shown its efficacy and cost-effectiveness and the lack of need for future interventions. We have been able to perform distal splenorenal shunt with acceptable morbidity and mortality in patients who are frequently at a great distance from tertiary medical centers or who have significant psychosocial issues. Following a TIPS closely with ultrasonograms or venograms is simply not possible in such situations because these tests are either not available or the patients are lost to follow-up and will only seek treatment with acute rebleeding. Thus, we propose that the 2 most important factors in deciding whether to use TIPS or distal splenorenal shunt are Child status and patient compliance or psychosocial factors. We have shown data here that most centers would be reluctant to report, but they reflect the reality of the nature of these patients. The presence of factors such as active substance abuse, homelessness, lack of social or financial support, and distance from tertiary medical centers that can treat endstage liver disease must be noted prior to any decision. These factors are generally discussed in determining appropriateness for liver transplantation and should be discussed before deciding between TIPS and distal splenorenal shunt as well. Although we would ideally like to study this issue in a controlled, prospective fashion, the nature of these patients will probably never allow for such a study. This study was presented as a poster at the 73rd Annual Meeting of the Pacific Coast Surgical Association, Las Vegas, Nev, February 17, 2002, and published after peer review and revision. Corresponding author: Linda L. Wong, MD, 2226 Liliha St, Suite 402, Honolulu, HI ( REFERENCES 1. Nagsue N, Kohno H, Ogawa Y, et al. Appraisal of distal splenorenal shunt in the treatment of esophageal varices: an analysis of prophylactic, emergency, and elective shunts. World J Surg. 1989;13: Henderson MJ. Role of distal splenorenal shunt for long-term management of variceal bleeding. World J Surg. 1994;18: Orozco H, Mercado MA, Garcia JG, et al. Selective shunts for portal hypertension: current role of a 21-year experience. Liver Transpl Surg. 1997;3: Jenkins RL, Gedaly R, Pomposelli JJ, et al. Distal splenorenal shunt: role, indications, and utility in the era of liver transplantation. Arch Surg. 1999;134: Knechtle SJ, Alessandro AM, Armbrust MJ, et al. Surgical portosystemic shunts for treatment of portal hypertensive bleeding: outcome and effect on liver function. Surgery. 1999;126: Henderson MJ, Warren WD, Millikan WJ, et al. Distal splenorenal shunt with splenopancreatic disconnection: a 4-year assessment. Ann Surg. 1989;10: Zacks SL, Sandler RS, Biddle AK, et al. Decision analysis of transjugular intrahepatic portosystemic shunt versus distal splenorenal shunt for portal hypertension. Hepatology. 1999;29: Rikkers LF, Jin G, Lagnas AN, et al. Shunt surgery during the era of liver transplantation. Ann Surg. 1997;226: LaBerge JM, Somberg KA, Lake JR, et al. Two-year outcome following transjugular intrahepatic portosystemic shunt for variceal bleeding: results in 90 patients. Gastroenterology. 1995;108: Caldwell DM, Ring EJ, Rees CR, et al. Multicenter investigation of the role of transjugular intrahepatic portosystemic shunt in the management of portal hypertension. Radiology. 1995;196: Haskal ZJ, Pentecost MJ, Soulen MC, et al. Transjugular intrahepatic portosystemic shunt stenosis and revision: early and midterm results. AJR Am J Roentgenol. 1994;163: Henderson JM, Nagel A, Curtas S, et al. Surgical shunts and tips for variceal decompression in the 1990s. Surgery. 2000;128: Khaitiyar JS, Luthra SK, Prasad N, et al. Transjugular intrahepatic portosystemic shunt versus distal splenorenal shunt: a comparative study. Hepatogastroenterology. 2000;47: Orozco H, Mercado MA. The evolution of portal hypertension surgery: lessons from 1000 operations and 50 years experience. Arch Surg. 2000;135: Spina GP, Santambrogio R, Opocher E, et al. Factors predicting chronic hepatic encephalopathy after distal splenorenal shunt: a multivariate analysis of clinical and hemodynamic variables. Surgery. 1993;114: Jin G, Rikkers L. The significance of portal vein thrombosis after distal splenorenal shunt. Arch Surg. 1991;126: Rossle M, Haag K, Ochs A. The transjugular intrahepatic portosystemic stent-shunt procedure for variceal bleeding. N Engl J Med. 1994;330: Sanyal AJ, Freeman A, Shiffman ML, et al. Portosystemic encephalopathy after transjugular intrahepatic portosystemic shunt: results of a prospective, controlled study. Hepatology. 1994;20: Somberg KA, Riegler JL, LaBerge JM, et al. Hepatic encephalopathy after transjugular intrahepatic portosystemic shunts: incidence and risk factors. Am J Gastroenterol. 1995;90: Woodle ES, Darcy M, White HM, et al. Intrahepatic portosystemic vascular stents: a bridge to hepatic transplantation. Surgery. 1993;113: Menegaux F, Baker E, Keeffe EB, et al. Impact of transjugular intrahepatic portosystemic shunt on orthotopic liver transplantation. World J Surg. 1994;18: Millis M, Imagawa D, Olthoff K, et al. TIPS: impact on liver transplantation. Transplant Proc. 1995;27: Somberg KA, Lombardero MS, Lawlor SM, et al. Impact of transjugular intrahepatic portosystemic shunts on liver transplantation: a controlled analysis. Transplant Proc. 1995;27: Somberg KA, Lombardero MS, Lawlor SM, et al. A controlled analysis of the transjugular intrahepatic portosystemic shunt in liver transplant recipients. Transplantation. 1997;63: Helton WS, Maves R, Wicks K, et al. Transjugular intrahepatic portasystemic shunt vs surgical shunt in good-risk cirrhotic patients: a case-control comparison. Arch Surg. 2001;136: Menegaux F, Keeffe EB, Baker E, et al. Comparison of transjugular and surgical portosystemic shunts on the outcome of liver transplantation. Arch Surg. 1994; 129: Abouljoud MS, Levy MF, Rees CR, et al. A comparison of treatment of transjugular intrahepatic portosystemic shunt or distal splenorenal shunt in the management of variceal bleeding prior to liver transplantation. Transplantation. 1995; 59: Selim N, Fendley MJ, Boyer TD, et al. Conversion of failed transjugular intrahepatic portosystemic shunt to distal splenorenal shunt in patients with Child A or B cirrhosis. Ann Surg. 1998;227:
Virtual Mentor American Medical Association Journal of Ethics December 2008, Volume 10, Number 12:
 Virtual Mentor American Medical Association Journal of Ethics December 2008, Volume 10, Number 12: 805-809. CLINICAL PEARL Indications for Use of TIPS in Treating Portal Hypertension Elizabeth C. Verna,
Virtual Mentor American Medical Association Journal of Ethics December 2008, Volume 10, Number 12: 805-809. CLINICAL PEARL Indications for Use of TIPS in Treating Portal Hypertension Elizabeth C. Verna,
Surgical Rescue of Surgical Failures
 HPB Surgery, 1999, Vol. 11, pp. 151-155 Reprints available directly from the publisher Photocopying permitted by license only (C) 1999 OPA (Overseas Publishers Association) N.V. Published by license under
HPB Surgery, 1999, Vol. 11, pp. 151-155 Reprints available directly from the publisher Photocopying permitted by license only (C) 1999 OPA (Overseas Publishers Association) N.V. Published by license under
PAPER. Role, Indications, and Utility in the Era of Liver Transplantation
 Distal Splenorenal Shunt PAPER Role, Indications, and Utility in the Era of Liver Transplantation Roger L. Jenkins, MD; Roberto Gedaly, MD; James J. Pomposelli, MD, PhD; Elizabeth A. Pomfret, MD, PhD;
Distal Splenorenal Shunt PAPER Role, Indications, and Utility in the Era of Liver Transplantation Roger L. Jenkins, MD; Roberto Gedaly, MD; James J. Pomposelli, MD, PhD; Elizabeth A. Pomfret, MD, PhD;
Preliminary study of the permeability and safety of covered stents-grafts in pediatric TIPS
 Preliminary study of the permeability and safety of covered stents-grafts in pediatric TIPS Poster No.: C-0354 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Bueno Palomino, L. Zurera Tendero,
Preliminary study of the permeability and safety of covered stents-grafts in pediatric TIPS Poster No.: C-0354 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Bueno Palomino, L. Zurera Tendero,
Evidence-Base Management of Esophageal and Gastric Varices
 Evidence-Base Management of Esophageal and Gastric Varices Rino Alvani Gani Hepatobiliary Division Department of Internal Medicine Faculty of Medicine Universitas Indonesia Cipto Mangunkusumo National
Evidence-Base Management of Esophageal and Gastric Varices Rino Alvani Gani Hepatobiliary Division Department of Internal Medicine Faculty of Medicine Universitas Indonesia Cipto Mangunkusumo National
AASLD PRACTICE GUIDELINE. The Role of Transjugular Intrahepatic Portosystemic Shunt in the Management of Portal Hypertension. Preamble.
 AASLD PRACTICE GUIDELINE The Role of Transjugular Intrahepatic Portosystemic Shunt in the Management of Portal Hypertension Thomas D. Boyer 1 and Ziv J. Haskal 2 Preamble The recommendations in this article
AASLD PRACTICE GUIDELINE The Role of Transjugular Intrahepatic Portosystemic Shunt in the Management of Portal Hypertension Thomas D. Boyer 1 and Ziv J. Haskal 2 Preamble The recommendations in this article
TIPS. D Patch Royal Free Hospital London UK
 TIPS D Patch Royal Free Hospital London UK TIPS Technique Ascites Budd Chiari Variceal Bleeding Historical Experimental Development 1967 Piccone Shunt between recanalized umbilical vein and saphenous
TIPS D Patch Royal Free Hospital London UK TIPS Technique Ascites Budd Chiari Variceal Bleeding Historical Experimental Development 1967 Piccone Shunt between recanalized umbilical vein and saphenous
V ariceal haemorrhage is a major cause of mortality and
 270 LIVER DISEASE The role of the transjugular intrahepatic portosystemic stent shunt (TIPSS) in the management of bleeding gastric : clinical and haemodynamic correlations D Tripathi, G Therapondos, E
270 LIVER DISEASE The role of the transjugular intrahepatic portosystemic stent shunt (TIPSS) in the management of bleeding gastric : clinical and haemodynamic correlations D Tripathi, G Therapondos, E
Michele Bettinelli RN CCRN Lahey Health and Medical Center
 Michele Bettinelli RN CCRN Lahey Health and Medical Center Differentiate the types of varices Identify glue preparations utilized when treating gastric varices Review the process of glue administration
Michele Bettinelli RN CCRN Lahey Health and Medical Center Differentiate the types of varices Identify glue preparations utilized when treating gastric varices Review the process of glue administration
Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
 CLINICAL IMAGES Ochsner Journal 17:311 316, 2017 Ó Academic Division of Ochsner Clinic Foundation Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
CLINICAL IMAGES Ochsner Journal 17:311 316, 2017 Ó Academic Division of Ochsner Clinic Foundation Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
Contraindications. Indications. Complications. Currently TIPS is considered second or third line therapy for:
 Contraindications Absolute Relative Primary prevention variceal bleeding HCC if centrally located Active congestive heart failure Obstruction all hepatic veins Thomas D. Boyer, M.D. University of Arizona
Contraindications Absolute Relative Primary prevention variceal bleeding HCC if centrally located Active congestive heart failure Obstruction all hepatic veins Thomas D. Boyer, M.D. University of Arizona
Use of transjugular intrahepatic portosystemic shunt in liver disease
 Vol. XVIII No. 3 JOURNAL OF VASCULAR NURSING PAGE 83 Use of transjugular intrahepatic portosystemic shunt in liver disease Patricia Ann Radovich, RN, MSN, CCRN, FCCM Persons with cirrhosis have many complications.
Vol. XVIII No. 3 JOURNAL OF VASCULAR NURSING PAGE 83 Use of transjugular intrahepatic portosystemic shunt in liver disease Patricia Ann Radovich, RN, MSN, CCRN, FCCM Persons with cirrhosis have many complications.
Factors Predicting Survival after Transjugular Intrahepatic Portosystemic Shunt Creation: 15 Years Experience from a Single Tertiary Medical Center
 Factors Predicting Survival after Transjugular Intrahepatic Portosystemic Shunt Creation: 15 Years Experience from a Single Tertiary Medical Center Jen-Jung Pan, MD, PhD, Chaoru Chen, PhD, James G. Caridi,
Factors Predicting Survival after Transjugular Intrahepatic Portosystemic Shunt Creation: 15 Years Experience from a Single Tertiary Medical Center Jen-Jung Pan, MD, PhD, Chaoru Chen, PhD, James G. Caridi,
EDUCATION PRACTICE. Management of Refractory Ascites. Clinical Scenario. The Problem
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1187 1191 EDUCATION PRACTICE Management of Refractory Ascites ANDRÉS CÁRDENAS and PERE GINÈS Liver Unit, Institute of Digestive Diseases, Hospital Clínic,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1187 1191 EDUCATION PRACTICE Management of Refractory Ascites ANDRÉS CÁRDENAS and PERE GINÈS Liver Unit, Institute of Digestive Diseases, Hospital Clínic,
Portogram shows opacification of gastroesophageal varices.
 Portogram shows opacification of gastroesophageal varices. http://clinicalgate.com/radiologic-hepatobiliary-interventions/ courtesyhttp://emedicine.medscape.com/article/372708-overview DR.Thulfiqar Baiae
Portogram shows opacification of gastroesophageal varices. http://clinicalgate.com/radiologic-hepatobiliary-interventions/ courtesyhttp://emedicine.medscape.com/article/372708-overview DR.Thulfiqar Baiae
GI bleeding in chronic liver disease
 GI bleeding in chronic liver disease Stuart McPherson Consultant Hepatologist Liver Unit, Freeman Hospital, Newcastle upon Tyne and Institute of Cellular Medicine, Newcastle University. Case 54 year old
GI bleeding in chronic liver disease Stuart McPherson Consultant Hepatologist Liver Unit, Freeman Hospital, Newcastle upon Tyne and Institute of Cellular Medicine, Newcastle University. Case 54 year old
VARICEAL BLEEDING. Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta.
 VARICEAL BLEEDING Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta Disclosures: None OUTLINE Pathophysiology of portal hypertension Splanchnic
VARICEAL BLEEDING Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta Disclosures: None OUTLINE Pathophysiology of portal hypertension Splanchnic
TUBERCULOSIS CONTROL IN THE WHO WESTERN PACIFIC REGION In the WHO Western Pacific Region 2002 Report
 TUBERCULOSIS CONTROL IN THE WHO WESTERN PACIFIC REGION 2000 Tuberculosis Control In the WHO Western Pacific Region 2002 Report World Health Organization Office for the Western Pacific Region iii TUBERCULOSIS
TUBERCULOSIS CONTROL IN THE WHO WESTERN PACIFIC REGION 2000 Tuberculosis Control In the WHO Western Pacific Region 2002 Report World Health Organization Office for the Western Pacific Region iii TUBERCULOSIS
Barbara Rus Gadžijev Peter Popovič Klinični inštitut za radiologijo UKC Ljubljana
 STROKOVNI SESTANEK ZDRUŽENJA HEMATOLOGOV SLOVENIJE IN ZDRUŽENJA ZA TRANSFUZIJSKO MEDICINO, Terme Zreče, 17.-18.4.2015 Barbara Rus Gadžijev Peter Popovič Klinični inštitut za radiologijo UKC Ljubljana goals,
STROKOVNI SESTANEK ZDRUŽENJA HEMATOLOGOV SLOVENIJE IN ZDRUŽENJA ZA TRANSFUZIJSKO MEDICINO, Terme Zreče, 17.-18.4.2015 Barbara Rus Gadžijev Peter Popovič Klinični inštitut za radiologijo UKC Ljubljana goals,
Left-sided portal hypertension with a patent splenic vein: An impossible or a not-so-uncommon scenario?
 Khan et al. 108 CASE REPORT PEER REVIEWED OPEN ACCESS Left-sided portal hypertension with a patent splenic vein: An impossible or a not-so-uncommon scenario? Iftikhar Khan, Ghassan Ramahi, Saif Zaabi,
Khan et al. 108 CASE REPORT PEER REVIEWED OPEN ACCESS Left-sided portal hypertension with a patent splenic vein: An impossible or a not-so-uncommon scenario? Iftikhar Khan, Ghassan Ramahi, Saif Zaabi,
Preoperative elective transjugular intrahepatic portosystemic shunt for cirrhotic patients undergoing abdominal surgery
 REVIEW ARTICLE Annals of Gastroenterology (2017) 31, 330-337 Preoperative elective transjugular intrahepatic portosystemic shunt for cirrhotic patients undergoing abdominal Deepanshu Jain a, Ejaz Mahmood
REVIEW ARTICLE Annals of Gastroenterology (2017) 31, 330-337 Preoperative elective transjugular intrahepatic portosystemic shunt for cirrhotic patients undergoing abdominal Deepanshu Jain a, Ejaz Mahmood
Update in abdominal Surgery in cirrhotic patients
 Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Title: Cholestasis after TIPS placement in a patient with primary sclerosing cholangitis: an uncommon complication
 Title: Cholestasis after TIPS placement in a patient with primary sclerosing cholangitis: an uncommon complication Authors: Alejandro Salagre García, Carolina Muñoz Codoceo, Elena Gómez Domínguez, Inmaculada
Title: Cholestasis after TIPS placement in a patient with primary sclerosing cholangitis: an uncommon complication Authors: Alejandro Salagre García, Carolina Muñoz Codoceo, Elena Gómez Domínguez, Inmaculada
Tranjugular Intrahepatic Portosystemic Shunt
 Tranjugular Intrahepatic Portosystemic Shunt Christopher Selhorst July 25, 2005 BIDMC Radiology Overview Portal Hypertension Indications, Contraindications The Procedure Case Review Complications Outcomes
Tranjugular Intrahepatic Portosystemic Shunt Christopher Selhorst July 25, 2005 BIDMC Radiology Overview Portal Hypertension Indications, Contraindications The Procedure Case Review Complications Outcomes
Current status of hepatic surgery in Korea
 Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Management of Cirrhotic Complications Uncontrolled Ascites. Siwaporn Chainuvati, MD Siriraj Hospital Mahidol University
 Management of Cirrhotic Complications Uncontrolled Ascites Siwaporn Chainuvati, MD Siriraj Hospital Mahidol University Topic Definition, pathogenesis Current therapeutic options Experimental treatments
Management of Cirrhotic Complications Uncontrolled Ascites Siwaporn Chainuvati, MD Siriraj Hospital Mahidol University Topic Definition, pathogenesis Current therapeutic options Experimental treatments
Review Article Role of Self-Expandable Metal Stents in Acute Variceal Bleeding
 Hindawi Publishing Corporation International Journal of Hepatology Volume 2012, Article ID 418369, 6 pages doi:10.1155/2012/418369 Review Article Role of Self-Expandable Metal Stents in Acute Variceal
Hindawi Publishing Corporation International Journal of Hepatology Volume 2012, Article ID 418369, 6 pages doi:10.1155/2012/418369 Review Article Role of Self-Expandable Metal Stents in Acute Variceal
U cause of death in patients with end-stage liver
 Transjugular Intrahepatic Portosystemic Shunt in Patients With End-Stage liver Disease: Results in 85 Patients- Nicolas Jabbour, * Albert?. Zajko, # Philip D. Orons, # William Irish, * Fabio Bartoli, *
Transjugular Intrahepatic Portosystemic Shunt in Patients With End-Stage liver Disease: Results in 85 Patients- Nicolas Jabbour, * Albert?. Zajko, # Philip D. Orons, # William Irish, * Fabio Bartoli, *
INTERNATIONAL HEALTH REGULATIONS
 W O R L D H E A L T H ORGANIZATION ORGANISATION MONDIALE DE LA SANTÉ REGIONAL OFFICE FOR THE WESTERN PACIFIC BUREAU RÉGIONAL DU PACIFIQUE OCCIDENTAL REGIONAL COMMITTEE WPR/RC63/9 Sixty-third session 29
W O R L D H E A L T H ORGANIZATION ORGANISATION MONDIALE DE LA SANTÉ REGIONAL OFFICE FOR THE WESTERN PACIFIC BUREAU RÉGIONAL DU PACIFIQUE OCCIDENTAL REGIONAL COMMITTEE WPR/RC63/9 Sixty-third session 29
REVIEW OF TUBERCULOSIS EPIDEMIOLOGY
 Part I REVIEW OF TUBERCULOSIS EPIDEMIOLOGY 1. 2. 3. Estimated Tuberculosis Burden 7 Tuberculosis Case Notification 10 Prevalence and Tuberculin Surveys 22 PART 1 5 TABLE 1: Latest notification of tuberculosis
Part I REVIEW OF TUBERCULOSIS EPIDEMIOLOGY 1. 2. 3. Estimated Tuberculosis Burden 7 Tuberculosis Case Notification 10 Prevalence and Tuberculin Surveys 22 PART 1 5 TABLE 1: Latest notification of tuberculosis
Liver Transplantation Evaluation: Objectives
 Liver Transplantation Evaluation: Essential Work-Up Curtis K. Argo, MD, MS VGS/ACG Regional Postgraduate Course Williamsburg, VA September 13, 2015 Objectives Discuss determining readiness for transplantation
Liver Transplantation Evaluation: Essential Work-Up Curtis K. Argo, MD, MS VGS/ACG Regional Postgraduate Course Williamsburg, VA September 13, 2015 Objectives Discuss determining readiness for transplantation
King Abdul-Aziz University Hospital (KAUH) is a tertiary
 Modelling Factors Causing Mortality in Oesophageal Varices Patients in King Abdul Aziz University Hospital Sami Bahlas Abstract Objectives: The objective of this study is to reach a model defining factors
Modelling Factors Causing Mortality in Oesophageal Varices Patients in King Abdul Aziz University Hospital Sami Bahlas Abstract Objectives: The objective of this study is to reach a model defining factors
Management of Ascites and Hepatorenal Syndrome. Florence Wong University of Toronto. June 4, /16/ Gore & Associates: Consultancy
 Management of Ascites and Hepatorenal Syndrome Florence Wong University of Toronto June 4, 2016 6/16/2016 1 Disclosures Gore & Associates: Consultancy Sequana Medical: Research Funding Mallinckrodt Pharmaceutical:
Management of Ascites and Hepatorenal Syndrome Florence Wong University of Toronto June 4, 2016 6/16/2016 1 Disclosures Gore & Associates: Consultancy Sequana Medical: Research Funding Mallinckrodt Pharmaceutical:
The Effect of Transjugular Intrahepatic Portosystemic Shunt on Platelet Counts in Patients With Liver Cirrhosis
 The Effect of Transjugular Intrahepatic Portosystemic Shunt on Platelet Counts in Patients With Liver Cirrhosis Omar I. Massoud, MD, PhD, and Nizar N. Zein, MD Dr Massoud is an associate professor of medicine
The Effect of Transjugular Intrahepatic Portosystemic Shunt on Platelet Counts in Patients With Liver Cirrhosis Omar I. Massoud, MD, PhD, and Nizar N. Zein, MD Dr Massoud is an associate professor of medicine
Action Plan to Reduce the Double Burden of Malnutrition in the Western Pacific Region. Dr Katrin Engelhardt, MPH Technical Lead, Nutrition DNH/WPRO
 Action Plan to Reduce the Double Burden of Malnutrition in the Western Pacific Region Dr Katrin Engelhardt, MPH Technical Lead, Nutrition DNH/WPRO 37 countries and areas Mongolia China Republic of Korea
Action Plan to Reduce the Double Burden of Malnutrition in the Western Pacific Region Dr Katrin Engelhardt, MPH Technical Lead, Nutrition DNH/WPRO 37 countries and areas Mongolia China Republic of Korea
AN UPDATE ON REGIONAL STATISTICS ACTIVITIES AND PARTNERSHIP PROGRAM - Paper 4
 INAUGURAL MEETING OF THE PACIFIC STATISTICS METHODS BOARD 3-4 TH MAY 2018 AN UPDATE ON REGIONAL STATISTICS ACTIVITIES AND PARTNERSHIP PROGRAM - Paper 4 1. THE TEN YEAR PACIFIC STATISTICS STRATEGY 2010-2020
INAUGURAL MEETING OF THE PACIFIC STATISTICS METHODS BOARD 3-4 TH MAY 2018 AN UPDATE ON REGIONAL STATISTICS ACTIVITIES AND PARTNERSHIP PROGRAM - Paper 4 1. THE TEN YEAR PACIFIC STATISTICS STRATEGY 2010-2020
The role of TIPS in the management of liver transplant candidates
 Original Article The role of TIPS in the management of liver transplant candidates United European Gastroenterology Journal 217, Vol. 5(8) 11 117! Author(s) 217 Reprints and permissions: sagepub.co.uk/journalspermissions.nav
Original Article The role of TIPS in the management of liver transplant candidates United European Gastroenterology Journal 217, Vol. 5(8) 11 117! Author(s) 217 Reprints and permissions: sagepub.co.uk/journalspermissions.nav
Esophageal Varices Beta-Blockers or Band Ligation. Cesar Yaghi MD Hotel-Dieu de France University Hospital Universite Saint Joseph
 Esophageal Varices Beta-Blockers or Band Ligation Cesar Yaghi MD Hotel-Dieu de France University Hospital Universite Saint Joseph Esophageal Varices Beta-Blockers or Band Ligation? Risk of esophageal variceal
Esophageal Varices Beta-Blockers or Band Ligation Cesar Yaghi MD Hotel-Dieu de France University Hospital Universite Saint Joseph Esophageal Varices Beta-Blockers or Band Ligation? Risk of esophageal variceal
ACG & AASLD Joint Clinical Guideline: Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis
 ACG & AASLD Joint Clinical Guideline: Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis Guadalupe Garcia-Tsao, M.D., 1 Arun J. Sanyal, M.D., 2 Norman D. Grace,
ACG & AASLD Joint Clinical Guideline: Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis Guadalupe Garcia-Tsao, M.D., 1 Arun J. Sanyal, M.D., 2 Norman D. Grace,
Transjugular Intrahepatic
 Transjugular Intrahepatic Portosystemic Shunt (TIPS): A Clinical and Procedural Review Mark R. Werley, M.D. and John Briguglio, M.D. Lancaster Radiology Associates, Ltd. INTRODUCTION This article reviews
Transjugular Intrahepatic Portosystemic Shunt (TIPS): A Clinical and Procedural Review Mark R. Werley, M.D. and John Briguglio, M.D. Lancaster Radiology Associates, Ltd. INTRODUCTION This article reviews
Liver failure &portal hypertension
 Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
Transjugular Intrahepatic Portosystemic Shunt (TIPS) About your procedure
 Patient Education Transjugular Intrahepatic Portosystemic Shunt (TIPS) About your procedure This handout explains what a transjugular intrahepatic portosystemic shunt is and what to expect when you have
Patient Education Transjugular Intrahepatic Portosystemic Shunt (TIPS) About your procedure This handout explains what a transjugular intrahepatic portosystemic shunt is and what to expect when you have
Transjugular Intrahepatic Portosystemic Shunt for Acute Variceal Bleeding in Patients with Viral Liver Cirrhosis: Predictors of Early Mortality
 Early Mortality with TIPS for Variceal Bleeding Interventional Radiology Original Research Transjugular Intrahepatic Portosystemic Shunt for Acute Variceal Bleeding in Patients with Viral Liver Cirrhosis:
Early Mortality with TIPS for Variceal Bleeding Interventional Radiology Original Research Transjugular Intrahepatic Portosystemic Shunt for Acute Variceal Bleeding in Patients with Viral Liver Cirrhosis:
Risk factors for hepatic encephalopathy after transjugular intrahepatic portosystemic shunt placement in cirrhotic patients
 Oregon Health & Science University OHSU Digital Commons Scholar Archive 9-2014 Risk factors for hepatic encephalopathy after transjugular intrahepatic portosystemic shunt placement in cirrhotic patients
Oregon Health & Science University OHSU Digital Commons Scholar Archive 9-2014 Risk factors for hepatic encephalopathy after transjugular intrahepatic portosystemic shunt placement in cirrhotic patients
Variceal bleeding. Mainz,
 Variceal bleeding Mainz, 21.09.2008 Risk of complications 5 years 10 years Ascites 10 % 25 % HCC 10 % 25 % Bleeding < 5 % 5-10 % Enceph. < 5 % < 5 % Typical situation : Mortality 10 % to 40 % Sequence
Variceal bleeding Mainz, 21.09.2008 Risk of complications 5 years 10 years Ascites 10 % 25 % HCC 10 % 25 % Bleeding < 5 % 5-10 % Enceph. < 5 % < 5 % Typical situation : Mortality 10 % to 40 % Sequence
Surgical management of HCC. Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London
 Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding 1.1 Short title Acute upper GI bleeding
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding 1.1 Short title Acute upper GI bleeding
Information for patients (and their families) waiting for liver transplantation
 Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
The Leeds Teaching Hospitals NHS Trust Transjugular Intrahepatic Portosystemic Shunt (TIPS)
 n The Leeds Teaching Hospitals NHS Trust Transjugular Intrahepatic Portosystemic Shunt (TIPS) Information for patients Your liver doctor has recommended that you have a Transjugular Intrahepatic Portosystemic
n The Leeds Teaching Hospitals NHS Trust Transjugular Intrahepatic Portosystemic Shunt (TIPS) Information for patients Your liver doctor has recommended that you have a Transjugular Intrahepatic Portosystemic
Ascites Management. Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology
 Ascites Management Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology Disclosure 1. The speaker Atif Zaman, MD MPH have no relevant
Ascites Management Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology Disclosure 1. The speaker Atif Zaman, MD MPH have no relevant
Update on seasonal influenza in the Southern Hemisphere in
 Update on seasonal influenza in the Southern Hemisphere in 2011-2 Ian Barr WHO Collaborating Centre for Reference and Research on Influenza www.influenzacentre.org The Melbourne WHO Collaborating Centre
Update on seasonal influenza in the Southern Hemisphere in 2011-2 Ian Barr WHO Collaborating Centre for Reference and Research on Influenza www.influenzacentre.org The Melbourne WHO Collaborating Centre
MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT
 MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT Sherona Bau, ACNP The Pfleger Liver Institute 200 UCLA Medical Plaza, Suite 214 Los Angeles, CA 90095 September 30, 2017 I
MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT Sherona Bau, ACNP The Pfleger Liver Institute 200 UCLA Medical Plaza, Suite 214 Los Angeles, CA 90095 September 30, 2017 I
DRAFT. Angiography: Transjugular Intrahepatic Portosystemic Shunt (TIPS) What to expect. What is a transjugular intrahepatic portosystemic shunt?
 UW MEDICINE PATIENT EDUCATION Angiography: Transjugular Intrahepatic Portosystemic Shunt (TIPS) What to expect This handout explains a transjugular intrahepatic portosystemic shunt and what to expect when
UW MEDICINE PATIENT EDUCATION Angiography: Transjugular Intrahepatic Portosystemic Shunt (TIPS) What to expect This handout explains a transjugular intrahepatic portosystemic shunt and what to expect when
DOTTORATO DI RICERCA IN SCIENZE MEDICO-CHIRURGICHE GASTROENTEROLOGICHE E DEI TRAPIANTI TITOLO TESI FACTORS PREDICTING MORTALITY AFTER TIPS FOR
 Alma Mater Studiorum Università di Bologna DOTTORATO DI RICERCA IN SCIENZE MEDICO-CHIRURGICHE GASTROENTEROLOGICHE E DEI TRAPIANTI Ciclo XXII Settore/i scientifico-disciplinare/i di afferenza: MED/12 TITOLO
Alma Mater Studiorum Università di Bologna DOTTORATO DI RICERCA IN SCIENZE MEDICO-CHIRURGICHE GASTROENTEROLOGICHE E DEI TRAPIANTI Ciclo XXII Settore/i scientifico-disciplinare/i di afferenza: MED/12 TITOLO
Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated with stent failure
 Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
PORTAL HYPERTENSION. Tianjin Medical University LIU JIAN
 PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
WHO priorities for 2016 in US PICTs
 WHO priorities for 2016 in US PICTs By Dr Sevil Huseynova CLO for WHO Country Liaison Office in Northern Micronesia 1 (FSM, RMI, ROP) History: WHO s Mandate 1945, UN Conference, San Francisco 1948, 1 st
WHO priorities for 2016 in US PICTs By Dr Sevil Huseynova CLO for WHO Country Liaison Office in Northern Micronesia 1 (FSM, RMI, ROP) History: WHO s Mandate 1945, UN Conference, San Francisco 1948, 1 st
Clinical Study A Single-Institution Review of Portosystemic Shunts in Children: An Ongoing Discussion
 Hindawi Publishing Corporation HPB Surgery Volume 2010, Article ID 964597, 6 pages doi:10.1155/2010/964597 Clinical Study A Single-Institution Review of Portosystemic Shunts in Children: An Ongoing Discussion
Hindawi Publishing Corporation HPB Surgery Volume 2010, Article ID 964597, 6 pages doi:10.1155/2010/964597 Clinical Study A Single-Institution Review of Portosystemic Shunts in Children: An Ongoing Discussion
Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association
 CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
LIVER CIRRHOSIS. The liver extracts nutrients from the blood and processes them for later use.
 LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Comparison of transjugular intrahepatic portosystemic shunt with covered stent and balloon-occluded retrograde
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Comparison of transjugular intrahepatic portosystemic shunt with covered stent and balloon-occluded retrograde
World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 13 September 2007 ISSN
 Expanded Programme on Immunization World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 13 September 2007 ISSN 1814 3601 Monitoring Measles Surveillance and Progress Towards
Expanded Programme on Immunization World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 13 September 2007 ISSN 1814 3601 Monitoring Measles Surveillance and Progress Towards
The Management of Ascites & Hepatorenal Syndrome. Florence Wong University of Toronto. Falk Symposium March 14, 2008
 The Management of Ascites & Hepatorenal Syndrome Florence Wong University of Toronto Falk Symposium March 14, 2008 Management of Ascites Sodium Restriction Mandatory at all stages of ascites in order to
The Management of Ascites & Hepatorenal Syndrome Florence Wong University of Toronto Falk Symposium March 14, 2008 Management of Ascites Sodium Restriction Mandatory at all stages of ascites in order to
Hepatobiliary Malignancies Retrospective Study at Truman Medical Center
 Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
ALCOHOL AND DRUG TREATMENT SERVICES. Provided by the Alcohol and Drug Abuse Division (ADAD) Hawaiʻi Department of Health
 ALCOHOL AND DRUG TREATMENT SERVICES 2015 Provided by the Alcohol and Drug Abuse Division (ADAD) Hawaiʻi Department of Health EXECUTIVE SUMMARY This report focuses on alcohol and drug treatment services
ALCOHOL AND DRUG TREATMENT SERVICES 2015 Provided by the Alcohol and Drug Abuse Division (ADAD) Hawaiʻi Department of Health EXECUTIVE SUMMARY This report focuses on alcohol and drug treatment services
BULLETIN. World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 10 August 2006 ISSN
 BULLETIN World Health Organization Regional Office for the Western Pacific Expanded Programme on Immunization World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 10 August
BULLETIN World Health Organization Regional Office for the Western Pacific Expanded Programme on Immunization World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 10 August
Longterm follow up of transjugular intrahepatic portosystemic stent shunt (TIPSS) for the treatment of portal hypertension: results in 130 patients
 Gut 1996; 39: 479-485 Departments of Medicine A J Stanley R Jalan E H Forrest P C Hayes and Radiology D N Redhead Royal Infirmary of Edinburgh, Edinburgh Correspondence to: Dr A J Stanley, Department of
Gut 1996; 39: 479-485 Departments of Medicine A J Stanley R Jalan E H Forrest P C Hayes and Radiology D N Redhead Royal Infirmary of Edinburgh, Edinburgh Correspondence to: Dr A J Stanley, Department of
PAPER. Umbilical Hernia Repair in Patients With Signs
 PAPER Umbilical Hernia Repair in Patients With Signs of Portal Hypertension Surgical Outcome and Predictors of Mortality Sung W. Cho, MB, BS, MSc; Neil Bhayani, MD; Pippa Newell, MD; Maria A. Cassera,
PAPER Umbilical Hernia Repair in Patients With Signs of Portal Hypertension Surgical Outcome and Predictors of Mortality Sung W. Cho, MB, BS, MSc; Neil Bhayani, MD; Pippa Newell, MD; Maria A. Cassera,
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Transjugular intrahepatic portosystemic shunt (TIPS) Information for patients Sheffield Vascular Institute
 Transjugular intrahepatic portosystemic shunt (TIPS) Information for patients Sheffield Vascular Institute You have been given this leaflet because you need a procedure called a transjugular intrahepatic
Transjugular intrahepatic portosystemic shunt (TIPS) Information for patients Sheffield Vascular Institute You have been given this leaflet because you need a procedure called a transjugular intrahepatic
Evaluation Process for Liver Transplant Candidates
 Evaluation Process for Liver Transplant Candidates 2 Objectives Identify components of the liver transplant referral to evaluation Describe the role of the liver transplant coordinator Describe selection
Evaluation Process for Liver Transplant Candidates 2 Objectives Identify components of the liver transplant referral to evaluation Describe the role of the liver transplant coordinator Describe selection
Management of Cirrhosis Related Complications
 Management of Cirrhosis Related Complications Ke-Qin Hu, MD, FAASLD Professor of Clinical Medicine Director of Hepatology University of California, Irvine Disclosure I have no disclosure related to this
Management of Cirrhosis Related Complications Ke-Qin Hu, MD, FAASLD Professor of Clinical Medicine Director of Hepatology University of California, Irvine Disclosure I have no disclosure related to this
Liver Transplantation
 1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
NYU School of Medicine Department of Radiology Rotation-Specific House Staff Evaluation
 Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Risk factors for 5-day bleeding after endoscopic treatments for gastroesophageal varices in liver cirrhosis
 Original Article Page 1 of 9 Risk factors for 5-day bleeding after endoscopic treatments for gastroesophageal varices in liver cirrhosis Rui Sun*, Xingshun Qi* #, Deli Zou, Xiaodong Shao, Hongyu Li, Xiaozhong
Original Article Page 1 of 9 Risk factors for 5-day bleeding after endoscopic treatments for gastroesophageal varices in liver cirrhosis Rui Sun*, Xingshun Qi* #, Deli Zou, Xiaodong Shao, Hongyu Li, Xiaozhong
following the last documented transfusion; thereafter, evaluate the residual impairment(s).
 Adult Listings 5.01 Category of Impairments, Digestive System 5.02 Gastrointestinal hemorrhaging from any cause, requiring blood transfusion (with or without hospitalization) of at least 2 units of blood
Adult Listings 5.01 Category of Impairments, Digestive System 5.02 Gastrointestinal hemorrhaging from any cause, requiring blood transfusion (with or without hospitalization) of at least 2 units of blood
BULLETIN. World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 8 January 2006 ISSN
 BULLETIN World Health Organization Regional Office for the Western Pacific Expanded Programme on Immunization World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 8 January
BULLETIN World Health Organization Regional Office for the Western Pacific Expanded Programme on Immunization World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 8 January
Anaesthetic considerations and peri-operative risks in patients with liver disease
 Anaesthetic considerations and peri-operative risks in patients with liver disease Dr. C. K. Pandey Professor & Head Department of Anaesthesiology & Critical Care Medicine Institute of Liver and Biliary
Anaesthetic considerations and peri-operative risks in patients with liver disease Dr. C. K. Pandey Professor & Head Department of Anaesthesiology & Critical Care Medicine Institute of Liver and Biliary
Ontario s Paediatric Referral and Listing Criteria for Small Bowel and Liver- Small Bowel Transplantation
 Ontario s Paediatric Referral and Listing Criteria for Small Bowel and Liver- Small Bowel Transplantation Version 3.0 Trillium Gift of Life Network Ontario s Paediatric Referral and Listing Criteria for
Ontario s Paediatric Referral and Listing Criteria for Small Bowel and Liver- Small Bowel Transplantation Version 3.0 Trillium Gift of Life Network Ontario s Paediatric Referral and Listing Criteria for
Carvedilol or Propranolol in the Management of Portal Hypertension?
 Evidence Based Case Report Carvedilol or Propranolol in the Management of Portal Hypertension? Arranged by: dr. Saskia Aziza Nursyirwan RESIDENCY PROGRAM OF INTERNAL MEDICINE DEPARTMENT UNIVERSITY OF INDONESIA
Evidence Based Case Report Carvedilol or Propranolol in the Management of Portal Hypertension? Arranged by: dr. Saskia Aziza Nursyirwan RESIDENCY PROGRAM OF INTERNAL MEDICINE DEPARTMENT UNIVERSITY OF INDONESIA
Clinical guideline Published: 13 June 2012 nice.org.uk/guidance/cg141
 Acute upper gastrointestinal bleeding in over 16s: management Clinical guideline Published: June 2012 nice.org.uk/guidance/cg141 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Acute upper gastrointestinal bleeding in over 16s: management Clinical guideline Published: June 2012 nice.org.uk/guidance/cg141 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Bariatric Surgery For Patients With End-Organ Failure
 Bariatric Surgery For Patients With End-Organ Failure Arnold D. Salzberg, M.D. Andrew M. Posselt, M.D., PhD Divisions of Transplant and Minimally Invasive Surgery University of California, San Francisco
Bariatric Surgery For Patients With End-Organ Failure Arnold D. Salzberg, M.D. Andrew M. Posselt, M.D., PhD Divisions of Transplant and Minimally Invasive Surgery University of California, San Francisco
Removing Patients from the Liver Transplant Wait List: A Survey of US Liver Transplant Programs
 LIVER TRANSPLANTATION 14:303-307, 2008 ORIGINAL ARTICLE Removing Patients from the Liver Transplant Wait List: A Survey of US Liver Transplant Programs Kevin P. Charpentier 1 and Arun Mavanur 2 1 Rhode
LIVER TRANSPLANTATION 14:303-307, 2008 ORIGINAL ARTICLE Removing Patients from the Liver Transplant Wait List: A Survey of US Liver Transplant Programs Kevin P. Charpentier 1 and Arun Mavanur 2 1 Rhode
Presentation and mortality of primary biliary cirrhosis in older patients
 Age and Ageing 2000; 29: 305 309 Presentation and mortality of primary biliary cirrhosis in older patients JULIA L. NEWTON 1,DAVID E. JONES 2,JANE V. METCALF 2,JAY B. PARK 2,ALISTAIR D. BURT 2, MARGARET
Age and Ageing 2000; 29: 305 309 Presentation and mortality of primary biliary cirrhosis in older patients JULIA L. NEWTON 1,DAVID E. JONES 2,JANE V. METCALF 2,JAY B. PARK 2,ALISTAIR D. BURT 2, MARGARET
BULLETIN. World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 11 December 2006 ISSN
 BULLETIN World Health Organization Regional Office for the Western Pacific Expanded Programme on Immunization World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 11 December
BULLETIN World Health Organization Regional Office for the Western Pacific Expanded Programme on Immunization World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 11 December
TUBERCULOSIS CONTROL WHO WESTERN PACIFIC REGION
 TUBERCULOSIS CONTROL in WHO WESTERN PACIFIC REGION 2000 Report (Cases Notified in 1999) WORLD HEALTH ORGANIZATION Western Pacific Regional Office TUBERCULOSIS CONTROL IN WHO WESTERN PACIFIC REGION (Cases
TUBERCULOSIS CONTROL in WHO WESTERN PACIFIC REGION 2000 Report (Cases Notified in 1999) WORLD HEALTH ORGANIZATION Western Pacific Regional Office TUBERCULOSIS CONTROL IN WHO WESTERN PACIFIC REGION (Cases
Studies on the Results of the Nonshunting Procedures for Portal Hypertension*)
 Hiroshima Journal of Medical Sciences Vol. 32, No. 3, 241,...,246, September, 1983 HIJM 32-38 241 Studies on the Results of the Nonshunting Procedures for Portal Hypertension*) Motomu KODAMA, Tsuneo TAN
Hiroshima Journal of Medical Sciences Vol. 32, No. 3, 241,...,246, September, 1983 HIJM 32-38 241 Studies on the Results of the Nonshunting Procedures for Portal Hypertension*) Motomu KODAMA, Tsuneo TAN
Management of HepatoCellular Carcinoma
 9th Symposium GIC St Louis - 2010 Management of HepatoCellular Carcinoma Overview Pierre A. Clavien, MD, PhD Department of Surgery University Hospital Zurich Zurich, Switzerland Hepatocellular carcinoma
9th Symposium GIC St Louis - 2010 Management of HepatoCellular Carcinoma Overview Pierre A. Clavien, MD, PhD Department of Surgery University Hospital Zurich Zurich, Switzerland Hepatocellular carcinoma
MATERNAL AND CHILD HEALTH AND DISPARITIES FOR ASIAN AMERICANS, NATIVE HAWAIIANS, AND PACIFIC ISLANDERS
 MATERNAL AND CHILD HEALTH AND DISPARITIES FOR ASIAN AMERICANS, NATIVE HAWAIIANS, AND PACIFIC ISLANDERS Why does maternal and child health matter for realizing health justice in AA and NHPI communities?
MATERNAL AND CHILD HEALTH AND DISPARITIES FOR ASIAN AMERICANS, NATIVE HAWAIIANS, AND PACIFIC ISLANDERS Why does maternal and child health matter for realizing health justice in AA and NHPI communities?
Sandipan Ghose, Md. Azizul Hoque, Md. Khalilur Rahman, Mohd. Harun-or-Rashid
 Sandipan Ghose, Md. Azizul Hoque, Md. Khalilur Rahman, Mohd. Harun-or-Rashid Liver cirrhosis may be defined as a diffuse process characterized by fibrosis and conversion of normal liver architecture into
Sandipan Ghose, Md. Azizul Hoque, Md. Khalilur Rahman, Mohd. Harun-or-Rashid Liver cirrhosis may be defined as a diffuse process characterized by fibrosis and conversion of normal liver architecture into
Original Article PLATELET COUNT TO SPLEEN DIAMETER RATIO AS A PREDICTOR OF ESOPHAGEAL VARICES IN PATIENTS OF LIVER CIRRHOSIS DUE TO HEPATITIS C VIRUS
 Original Article AS A PREDICTOR OF ESOPHAGEAL VARICES IN PATIENTS OF LIVER CIRRHOSIS DUE TO HEPATITIS C VIRUS Khalid Amin 1, Dilshad Muhammad 2, Amin Anjum 3, Kashif Jamil 4, Ali Hassan 5 1 Associate Professor
Original Article AS A PREDICTOR OF ESOPHAGEAL VARICES IN PATIENTS OF LIVER CIRRHOSIS DUE TO HEPATITIS C VIRUS Khalid Amin 1, Dilshad Muhammad 2, Amin Anjum 3, Kashif Jamil 4, Ali Hassan 5 1 Associate Professor
DISEASE LEVEL MEDICAL EVIDENCE PROTOCOL
 DISEASE LEVEL MEDICAL EVIDENCE PROTOCOL 1. This Protocol sets out the medical evidence that must be delivered to the Administrator for proof of Disease Level. It is subject to such further and other Protocols
DISEASE LEVEL MEDICAL EVIDENCE PROTOCOL 1. This Protocol sets out the medical evidence that must be delivered to the Administrator for proof of Disease Level. It is subject to such further and other Protocols
Evaluation of Clinical, Biochemical and Ultrasound Parameters in Diagnosis of Oesophageal Varices
 Med. J. Cairo Univ., Vol. 78, No. 2, June: 105-109, 2010 www.medicaljournalofcairouniversity.com Evaluation of Clinical, Biochemical and Ultrasound Parameters in Diagnosis of Oesophageal Varices FAWZY
Med. J. Cairo Univ., Vol. 78, No. 2, June: 105-109, 2010 www.medicaljournalofcairouniversity.com Evaluation of Clinical, Biochemical and Ultrasound Parameters in Diagnosis of Oesophageal Varices FAWZY
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Transjugular Intrahepatic Portosystemic Shunts and Liver Transplantation in Patients With Refractory Hepatic Hydrothorax
 Transjugular Intrahepatic Portosystemic Shunts and Liver Transplantation in Patients With Refractory Hepatic Hydrothorax Mark A. Jeffries,* Sahira Kazanjian, Mark Wilson, Jeffrey Punch, and Robert J. Fontana*
Transjugular Intrahepatic Portosystemic Shunts and Liver Transplantation in Patients With Refractory Hepatic Hydrothorax Mark A. Jeffries,* Sahira Kazanjian, Mark Wilson, Jeffrey Punch, and Robert J. Fontana*
Diagnostic Procedures. Measurement of Hepatic venous pressure in management of cirrhosis. Clinician s opinion
 5 th AISF Post-Meeting Course Diagnostic and Therapeutic Invasive Procedures in Hepatology Rome, February 25 th Diagnostic Procedures Measurement of Hepatic venous pressure in management of cirrhosis Clinician
5 th AISF Post-Meeting Course Diagnostic and Therapeutic Invasive Procedures in Hepatology Rome, February 25 th Diagnostic Procedures Measurement of Hepatic venous pressure in management of cirrhosis Clinician
The largest outbreak of Ebola virus disease (EVD)
 Regional Analysis Ebola preparedness in the Western Pacific Region, 2014 Xu Zhen, a* Boris Pavlin, b* Raynal C. Squires, a Thilaka Chinnayah, a Frank Konings, a Chin-Kei Lee a and Li Ailan a on behalf
Regional Analysis Ebola preparedness in the Western Pacific Region, 2014 Xu Zhen, a* Boris Pavlin, b* Raynal C. Squires, a Thilaka Chinnayah, a Frank Konings, a Chin-Kei Lee a and Li Ailan a on behalf
Evaluation of liver and spleen stiffness using a ultrasound guided method: Accuracy of ARFI(R) measurements in liver disease patients
 Evaluation of liver and spleen stiffness using a ultrasound guided method: Accuracy of ARFI(R) measurements in liver disease patients Poster No.: C-3242 Congress: ECR 2010 Type: Topic: Authors: Keywords:
Evaluation of liver and spleen stiffness using a ultrasound guided method: Accuracy of ARFI(R) measurements in liver disease patients Poster No.: C-3242 Congress: ECR 2010 Type: Topic: Authors: Keywords:
