Spectrum of CT Findings in Pediatric Patients after Partial Liver Transplantation 1
|
|
|
- Jocelyn Price
- 6 years ago
- Views:
Transcription
1 EDUCATION EXHIBIT Spectrum of CT Findings in Pediatric Patients after Partial Liver Transplantation 1 53 Fumie Ametani, MD Kyo Itoh, MD Toshiya Shibata, MD Yoji Maetani, MD Koichi Tanaka, MD Junji Konishi, MD Liver transplantation is an accepted therapy for patients with severe liver diseases. In pediatric liver transplantation, the application of reduced-size and split-liver transplantation has expanded the donor pool. The development of living related donor partial liver transplantation has further increased the availability of donors. Complications in patients after living related transplantation include hepatic arterial thrombosis, portal venous stenosis and thrombosis, hepatic venous stenosis, biliary stenosis or leak, biloma formation, fatty liver, extrahepatic fluid collection, posttransplantation lymphoproliferative disorder, and organ rejection. Ultrasonography is the primary imaging modality for evaluation of the vascular system of patients after liver transplantation, and computed tomography is useful to help diagnose hepatic parenchymal abnormalities including infarction, congestion, and fatty change; intrahepatic biliary damage; and extrahepatic disorders, including abnormal fluid collections, varicose veins, and lymphadenopathy. Index terms: Liver, CT, Liver, transplantation, Liver, US, Transplantation, RadioGraphics 2001; 21: From the Departments of Nuclear Medicine and Diagnostic Imaging (F.A., Y.M., J.K.) and Transplantation and Immunology (K.T.), Graduate School of Medicine, Kyoto University, Kyoto, Japan; and the Department of Radiology, Kyoto University Hospital, 54 Shogoin Kawahara-cho, Sakyo-ku, Kyoto-shi, Kyoto-fu , Japan (K.I., T.S.). Presented as a scientific exhibit at the 1999 RSNA scientific assembly. Received March 2, 2000; revision requested May 22 and received June 20; accepted June 26. Address correspondence to K.I. ( kyo@kuhp.kyoto-u.ac.jp). RSNA, 2001 See also the article by Bassignani et al (pp 39 52) in this issue.
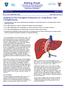
2 54 January-February 2001 RG Volume 21 Number 1 Introduction Liver transplantation is performed in an increasing number of patients with severe liver diseases. In pediatric cases, the number of cadaveric donor livers is not sufficient; therefore, living related donor partial liver transplantation or split-liver transplantation has become an important therapeutic option for pediatric patients with terminal liver diseases (1 3). Living related transplantation has some advantages, including the need for only a brief period of cold ischemia, the ability to perform preoperative measurement of the graft size and preoperative evaluation of the vascular anatomy of the donor liver, and the genetic proximity of donors and children. Living related transplantation has a disadvantage in that the donor source is limited to immediate relatives, mainly parents. Thus, the use of marginal donor sources is unavoidable, which may allow problems with ABO blood group system incompatibility, size mismatches, and steatotic grafts. The main complications in patients after living related transplantation include vascular stenosis and thrombosis, biliary stenosis or bilomas, fatty liver, extrahepatic fluid collection, posttransplantation lymphoproliferative disorder, and rejection. Ultrasonography (US) is a less invasive imaging modality than computed tomography (CT) and should be the first choice to evaluate vascular and biliary abnormalities in patients after transplantation. CT is also useful to help evaluate graft growth or possible complications after partial liver transplantation, and there are several reports of CT findings after whole liver transplantation (4 6). In this article, we illustrate the surgical anatomy during implantation and provide a spectrum of CT findings of various complications in pediatric patients after living related transplantation. Vascular complications include hepatic infarction due to hepatic arterial thrombosis, portal venous stenosis or thrombosis, and hepatic congestion due to hepatic venous anastomotic stenosis. Biliary complications include intrahepatic bile duct dilatation, intrahepatic bile duct stones or debris, and intrahepatic bilomas. Other abnormalities after transplantation include fatty liver, periportal collar, focal fluid collection, posttransplantation lymphoproliferative disorder, and rejection. Some complications specific to pediatric patients, including intrahepatic bile duct damage related to Figure 1. Diagram of the surgical anatomy during living related transplantation shows endto-end left hepatic venous (LHV), hepatic arterial (HA), and portal venous (PV) anastomoses and hepatic jejunostomy. BD = bile duct, GDA = gastroduodenal artery, IVC = inferior vena cava, SMV = superior mesenteric vein, SPV = splenic vein. ABO blood group system incompatibility and fatty liver, are also presented. Surgical Anatomy For most pediatric recipients in our institution, the donor liver graft was the left lobe or lateral segment (Fig 1). The partial liver graft was orthotopically implanted in the recipient after total hepatectomy, with care taken to keep the inferior vena cava intact to maintain constant caval blood flow. The left hepatic artery of the donor was anastomosed to the appropriate hepatic artery of the recipient in an end-to-end fashion with use of a surgical microscope. The portal venous anastomosis was performed in an end-to-end fashion between the donor s left portal vein and the recipient s main portal vein. When the available portal vein was too short, venous grafting was performed with use of the donor s ovarian vein or the recipient s inferior mesenteric vein (1). The hepatic venous anastomosis was performed in an end-to-end or end-to-side fashion between the donor s left hepatic vein and the recipient s hepatic vein orifice, while the inferior vena cava was preserved (7).
3 RG Volume 21 Number 1 Ametani et al 55 Figure 2. Hepatic infarction following hepatic arterial thrombosis in a 15-year-old girl after living related transplantation to treat biliary atresia. (a, b) Precontrast (a) and postcontrast (b) CT images obtained 11 days after transplantation show large wedge-shaped low-attenuation areas (arrows) in peripheral parts of the transplanted liver. Extrahepatic hematoma (arrowheads) is also seen. (c) Contrast-enhanced CT scan obtained 4 months after a and b shows that the liver has a different shape and is smaller. These changes are most likely due to focal areas of infarction. Regression of the hematoma is seen. c. In whole liver transplantation, biliary anastomosis is made in an end-to-end fashion between the donor s common bile duct and the recipient s common bile duct. In living related transplantation, biliary reconstruction is performed by means of hepatic jejunostomy with a Roux-en-Y limb anastomosis (1 3). Vascular Complications Vascular complications include thrombosis or stenosis of the hepatic artery, portal vein, or hepatic vein. Hepatic arterial thrombosis can result from anastomotic stenosis and usually occurs early after the surgery. Twisting or compression of the vein by the growing graft causes portal venous and hepatic venous stenoses, which may occur either early or late after the surgery. Vascular complications should be first diagnosed with Doppler US, and CT should then be performed to help detect any secondary changes to the hepatic parenchyma and other findings such as ascites or varices. In portal venous or hepatic venous stenosis, angiography is performed to help confirm the stenosis and to help guide balloon dilation of the stenosis and thrombolysis. Hepatic Infarction due to Hepatic Arterial Thrombosis Hepatic arterial thrombosis is the most common vascular complication in patients after liver transplantation, and it can lead to devastating complications, such as biliary stricture, leak, biloma, and hepatic infarction or necrosis. Hepatic arterial thrombosis is a major complication that frequently results in graft failure and is more common in children (9% 42%) than in adults (4% 12%) (8,9). Hepatic arterial thrombosis itself can be diagnosed with Doppler US, and any secondary damage to the liver and bile duct can be diagnosed with CT. Hepatic infarction is generally observed at CT as irregular and wedge-shaped low-attenuation lesions that are mainly in the periphery of the liver. The lesions are either not enhanced or are nonhomogeneously enhanced on contrast material enhanced CT scans (Fig 2).
4 56 January-February 2001 RG Volume 21 Number 1 Figure 3. Portal venous stenosis and thrombosis in a 4- year-old girl 3 years after living related transplantation to treat biliary atresia. The patient suddenly presented with gastrointestinal tract bleeding from esophageal varices. Portal venous thrombosis in the umbilical portion and decreased portal venous flow were found at Doppler US examination (not shown). (a, b) Contrast-enhanced CT images (a at a higher level than b) of the transplanted liver show a low-attenuation thrombus (arrow) in the umbilical portion of the left portal vein. (c) Percutaneous transhepatic portogram obtained 3 days after a and b depicts anastomotic obstruction (solid arrow) of the portal vein. The intrahepatic portal vein is not opacified. Arrowhead = splenic vein, open arrow = superior mesenteric vein. c. Portal Venous Stenosis or Thrombosis Portal venous complication after liver transplantation is uncommon and was seen in 1% 22% of patients in previous studies (8 10). Portal venous stenosis occurs more frequently in reduced-size liver transplantation than in whole liver transplantation owing to the limited length of the portal vein that can be obtained from the donor. Risk factors include decreased portal venous inflow, the presence of portosystemic shunts before transplantation, prior splenectomy, twisting or kinking of the vascular conduit, and tension in the portal venous interposition graft (10,11). Portal venous stenosis with thrombus formation in the immediate postoperative period is quickly diagnosed with Doppler US and is managed surgically. In most cases, portal venous stenosis develops slowly after transplantation and is suspected on the basis of the presence of gastrointestinal varices, ascites, and splenomegaly. At contrast-enhanced CT, portal venous thrombosis is seen as a low-attenuation filling defect in the intrahepatic portal vein. In such cases, the extrahepatic portal venous trunk is stenosed and difficult to recognize (Fig 3). Portal venous stenosis without thrombus formation can be diagnosed with contrast-enhanced CT in asymptomatic cases (Fig 4). Portal venous stenosis can be treated with balloon dilation (11), but when the thrombus extends completely to the periphery of the intrahepatic portal venous branches, it can no longer be treated with balloon dilation or
5 RG Volume 21 Number 1 Ametani et al 57 Figure 4. Extrahepatic portal venous stenosis in a 4- year-old boy 2 years 9 months after living related transplantation to treat biliary atresia. (a, b) Contrast-enhanced CT images (a at a higher level than b) show compression of the extrahepatic portal vein (arrow) by the fully grown transplanted liver. (c) Percutaneous transhepatic portogram obtained 3 days after a and b shows stenosis (arrow) at the anastomosis. Balloon dilation of the stenosis was performed. c. thrombolysis, and the patient must undergo repeat transplantation. Thus, early diagnosis of portal venous stenosis before formation of a complete thrombus is important. Hepatic Congestion due to Hepatic Venous Anastomotic Stenosis In living related transplantation, the hepatic vein is reconstructed by means of end-to-end or endto-side anastomosis without harvesting of the vena cava (7). Hepatic venous anastomotic stenoses may occur more frequently in living related transplantation than in whole liver transplantation (7,12). As a result of delayed hepatic venous stenosis, hepatic congestion, portal venous flow decrease, ascites, and varices could be noted. Doppler US should be used primarily for the diagnosis of hepatic venous stenosis, but in our experience US sometimes failed to depict the stenosis. In some cases, this failure may occur because the stenosis is caused by the graft growing and twisting. The stenosis may disappear, depending on patient posture, as when the patient is supine. Contrast-enhanced CT is useful in demonstrating congestive changes in the liver parenchyma as a manifestation of blocked outflow, but it is of
6 58 January-February 2001 RG Volume 21 Number 1 a. c. Figure 5. Hepatic congestion due to hepatic venous anastomotic stenosis in a 16-year-old girl after living related transplantation to treat biliary atresia. Four months after transplantation, the patient had decreased hepatic venous flow at Doppler US examination (not shown). Percutaneous liver biopsy revealed centrilobular hemorrhage, which is suggestive of hepatic venous anastomotic stenosis or occlusion. (a) Contrast-enhanced CT image obtained 5 months after transplantation shows irregular enhancement of the transplanted liver. This finding suggests hepatic congestion. (b) Percutaneous transhepatic venogram obtained 20 days after a helps confirm hepatic venous anastomotic stenosis (arrow). (c) Contrast-enhanced CT image obtained the day after venoplasty shows normal enhancement of the hepatic parenchyma. little help in depicting the stenosis itself (Fig 5). Once hepatic venous stenosis is suspected, we perform US-guided percutaneous transhepatic venography to confirm it, followed by balloon dilation of the stenotic site. Biliary Complications Despite significant improvements that coincide with technical and immunologic advances in living related transplantation, biliary complications remain a significant cause of morbidity. Biliary complications are commonly seen after liver transplantation and occur in approximately 13% 19% of cases (13,14). Children recovering from living related transplantation may have a higher frequency (38%) of biliary complications than do adults (15). In living related transplantation, biliary reconstruction is accomplished by means of b. hepatic jejunostomy. Complications include anastomotic leakage and stenosis, intrahepatic bile ductal stones or debris, and biloma. These complications are reported to be related to the surgical method of biliary reconstruction and to prolonged cold ischemia time, immunologic reactions, hepatic arterial thrombosis, ABO blood group system incompatibility between donor and recipient, and cytomegalovirus infection (15 17). Hepatic arterial insufficiency from either stenosis or thrombosis may lead to necrosis of the bile ductal epithelium, which may lead to bilomas, abscesses, and nonanastomotic bile leak (18,19). Anastomotic stenosis first causes cholangitis and does not always manifest as intrahepatic bile duct dilatation. CT, US, and magnetic resonance cholangiography do not reliably depict anastomotic stenosis, and percutaneous cholangiography is needed to diagnose the stenosis (20).
7 RG Volume 21 Number 1 Ametani et al 59 a. b. Figure 6. Intrahepatic bile duct dilatation in a 14-year-old boy 2 months after living related transplantation to treat biliary atresia. Results of liver function tests were abnormal. (a) Contrast-enhanced CT image shows intrahepatic bile duct dilatation (arrows) and perihepatic fluid collection (arrowhead). (b) Percutaneous transhepatic cholangiogram obtained 2 days after a reveals biliary anastomotic stenosis (arrow) and biloma (arrowhead) as a result of anastomotic bile leak. Figure 7. Bile duct damage due to hepatic arterial thrombosis in a 1-year-old female infant after living related transplantation to treat biliary atresia. Contrastenhanced CT image obtained 35 days after transplantation shows an irregularly shaped low-attenuation band that represents intrahepatic bile duct dilatation. Note the fusiform low-attenuation lesion (arrow). nosis can be induced by fibrosis around the anastomosis that results from postoperative bile leakage (Fig 6). Another main cause of anastomotic stenosis is hepatic arterial insufficiency. Because the blood supply of the biliary tree in the transplanted liver graft is entirely dependent on the hepatic artery, hepatic arterial stenosis frequently brings biliary complications. Biliary complications related to hepatic arterial thrombosis include either anastomotic stenosis or intrahepatic bile duct damage, which are depicted as irregular dilatation with fusiform morphology (Fig 7). In cases of ABO blood group system incompatibility between donor and recipient, the frequency of hepatic arterial thrombosis and biliary complications is reported to be high (17). In living related transplantation, ABO blood group system incompatibility is sometimes unavoidable because the possible donors are restricted. Intrahepatic Bile Duct Dilatation Intrahepatic Bile Duct Stones or Debris Intrahepatic bile duct dilatation is not specific to anastomotic stenosis, because a slight asymptomatic dilatation of the intrahepatic bile duct is often seen in transplanted livers. Intrahepatic bile duct dilatation with symptoms such as fever or jaundice should be considered as cholangitis due to biliary anastomotic stenosis. Anastomotic ste- Several factors can lead to the formation of biliary stones and sludge in the transplanted liver. In a previous report, most necrotic debris was found to be caused by bile duct wall ischemia
8 60 January-February 2001 RG Volume 21 Number 1 Figure 8. Intrahepatic bile duct damage due to hepatic arterial thrombosis and biliary stones in a 16-yearold girl after living related transplantation to treat biliary atresia. This is a case of ABO blood group system incompatibility. (a) Contrast-enhanced CT image obtained 2 months after transplantation shows intrahepatic bile duct dilatation due to anastomotic stricture. (b) Contrast-enhanced CT image obtained 4 months after transplantation shows small high-attenuation lesions (arrows) in the dilated intrahepatic bile duct. (c) Nonenhanced CT image obtained 8 months after transplantation demonstrates multiple high-attenuation lesions (arrows) in the dilated intrahepatic bile duct. due to hepatic arterial occlusion (21). Persistent sludge may ultimately become formed stones (21) (Fig 8). c. Intrahepatic Bilomas Intrahepatic peripheral cystic lesions that communicate with the bile duct may be caused by bile duct wall ischemia in patients with hepatic arterial thrombosis after liver transplantation (Fig 9). These bilomas could be infected and result in abscesses. Other Abnormalities Fatty Liver Low-attenuation changes in transplanted liver grafts imply various pathologic changes: cholestasis, fatty changes, acute cellular rejection, acute Figure 9. Intrahepatic biloma in a 16-year-old girl 2 months after living related transplantation to treat biliary atresia. Contrast-enhanced CT image shows multiple round low-attenuation areas (arrows) and intrahepatic bile duct dilatation (arrowheads).
9 RG Volume 21 Number 1 Ametani et al 61 Figure 11. Periportal collar in an 8-year-old girl 17 days after living related transplantation to treat biliary atresia. (a) Contrast-enhanced CT image demonstrates a central periportal low-attenuation area (arrows) and a small perihepatic fluid collection (arrowhead). (b) Contrast-enhanced CT image of a more cephalic section shows peripheral periportal collar signs (arrows). Biopsy performed the day after acquisition of these studies revealed acute purulent cholangitis and cholestasis. hepatitis, liver cell swelling, necrosis, centrilobular congestion, or necrosis. Recognition of the significance of low attenuation is important for the treatment of patients after liver transplantation. Fatty change occurs universally in response to hepatocytic toxic reactions, injury, or overnutrition. In patients after liver transplantation, fatty changes may be induced by either hyperalimentation or serious liver damage, and it is not possible to distinguish them on the basis of CT findings alone (Fig 10). Figure 10. Decreased liver parenchymal density in a 16-year-old girl 45 days after living related transplantation to treat biliary atresia. Contrast-enhanced CT image reveals homogeneous low-attenuation parenchyma of the transplanted liver, which is obviously less dense than the spleen. Microvesicular steatosis in the hepatic lobule was confirmed with 18-gauge needle biopsy. Periportal Collar The presence of a central or peripheral periportal collar at CT is not sufficiently sensitive, specific, or accurate to help reliably diagnose or exclude acute allograft rejection. Periportal collars are seen with greater frequency in patients a short time after transplantation and in those with ascites. This finding supports the role of generalized postoperative lymphedema in production of the sign, which is most likely caused by surgical interruption of the periportal lymphatic vessels (22) (Fig 11). Focal Fluid Collection Localized fluid collections are commonly seen after liver transplantation. They include hematomas, bilomas, and localized ascites. Distinction of infected and uninfected fluid is difficult with
10 62 January-February 2001 RG Volume 21 Number a. Figures 12, 13. (12) Intraperitoneal hematoma in an 11-year-old girl 30 days after living related transplantation to treat biliary atresia. Contrast-enhanced CT image reveals a large intraperitoneal hematoma (arrows). (13) Paraduodenal hematoma in a 9-year-old girl 28 days after living related transplantation to treat biliary atresia. Precontrast (a) and postcontrast (b) CT images show a high-attenuation focal fluid collection (arrow) at the paraduodenal space. CT. In most cases, high-attenuation fluid collections are hemorrhagic (Figs 12, 13). Localized low-attenuation fluid collections at the liver edge are extrahepatic bilomas in most cases. They usually regress in size without medical treatment, but sometimes require percutaneous drainage. Posttransplantation Lymphoproliferative Disorder Organ transplant recipients undergoing immunosuppressive therapy are at increased risk of developing malignancy. The Epstein-Barr virus has been associated with posttransplantation lymphoproliferative disorder and lymphoma in such patients. Abdominal examination of patients with posttransplantation lymphoproliferative disorder shows various findings, such as lymph node swelling (abdominal and retroperitoneal), splenic involvement, and extranodal involvement mainly in the liver and small intestine (Fig 14). In a recent report, extranodal involvement was seen more commonly than were splenic and nodal involvement in patients with abdominal posttransplantation lymphoproliferative disorder (23). Rejection The presence or absence of rejection cannot be determined with CT alone (22). In our limited experience with acute cellular rejection, the liver parenchyma showed low-attenuation changes at 13b. CT in some cases, but there was no specific finding at CT in others. When rejection is suspected, we perform both CT and US to rule out any causes other than rejection. Conclusions US is the primary imaging modality in the evaluation of patients after liver transplantation, because it can be performed easily at the bedside and is sensitive to blood flow. CT is another important imaging modality for the evaluation of not only liver grafts but also extrahepatic abnormalities. Both CT and US are noninvasive imaging modalities, and their findings are complementary in the treatment of patients after liver transplantation. Acknowledgment: The authors thank Takanori Sakurai, MD, for suggesting the pathologic findings. References 1. Tanaka K, Uemoto S, Tokunaga Y, et al. Living related liver transplantation in children. Am J Surg 1994; 168: Broelsch CE, Whitington PF, Emond JC, et al. Liver transplantation in children from living related donors. Ann Surg 1991; 214:
11 RG Volume 21 Number 1 Ametani et al 63 Figure 14. Posttransplantation lymphoproliferative disorder in a 9-year-old boy 2 years after living related transplantation to treat cryptogenic liver cirrhosis. The patient presented with sudden gastrointestinal tract bleeding. (a) Contrast-enhanced CT image shows a low-attenuation lymph node mass (arrows) that invades the duodenum. The node was proved to be Epstein-Barr virus lymphoma. (b) Contrast-enhanced CT image was obtained 10 months after a. After chemotherapy, abdominal lymphadenopathy is no longer seen. 3. Ozawa K, Tanaka K, Yamaoka Y, et al. An appraisal of pediatric liver transplantation from living relatives: initial clinical experiences in 20 pediatric liver transplantations from living relatives as donors. Ann Surg 1992; 216: Duppy D, Costello P, Lewis D, Jenkins R. Abdominal CT findings after liver transplantation in 66 patients. AJR Am J Roentgenol 1991; 156: Shyn PB, Goldberg HI. Abdominal CT following liver transplantation. Gastrointest Radiol 1992; 17: Holbert BL, Campbell WL, Skolnick ML. Evaluation of the transplanted liver and postoperative complications. Radiol Clin North Am 1995; 33: Egawa H, Inomata Y, Uemoto S, et al. Hepatic vein reconstruction in 152 living-related donor liver transplantation patients. Surgery 1997; 121: Langnas A, Marujo W, Stratta RJ, Wood RP, Shaw BW. Vascular complications after orthotopic liver transplantation. Am J Surg 1991; 161: Wozney P, Zajko AB, Bron KM, Point S, Starzl TE. Vascular complications after liver transplantation: a 5-year experience. AJR Am J Roentgenol 1986; 147: Lee J, Ben-Ami T, Yousefzadeh D, et al. Extrahepatic portal vein stenosis in recipients of living-donor allografts: Doppler sonography. AJR Am J Roentgenol 1996; 167: Funaki B, Rosenblum JD, Leef JA, Hackworth CA, Szymski GX, Alonso EM. Angioplasty treatment of portal vein stenosis in children with segmental liver transplants: mid-term results. AJR Am J Roentgenol 1997; 169: Broelsch CE, Emond JC, Whitington PF, Thistlethwaite JR, Baker AL, Lichtor JL. Application of reduced-size liver transplants as split grafts, auxiliary orthotopic grafts, and living related segmental transplants. Ann Surg 1990; 212: Lerut J, Gordon RD, Iwatsuki S, et al. Biliary tract complications in human orthotopic liver transplantation. Transplantation 1987; 43: Stratta RJ, Wood RP, Langnas AN, et al. Diagnosis and treatment of biliary tract complications after orthotopic liver transplantation. Surgery 1989; 106: Heffron TG, Emond JC, Whitington PF, et al. Biliary complications in pediatric liver transplantation. Transplantation 1992; 53: Zajko AB, Campbell WL, Logsdon GA, et al. Cholangiographic findings in hepatic artery occlusion after liver transplantation. AJR Am J Roentgenol 1987; 149: Sanchez-Urdazpal L, Sterioff S, Janes C, Schwerman L, Rosen C, Krom RAF. Increased bile duct complications in ABO incompatible liver transplant recipients. Transplant Proc 1991; 23: Kaplan SB, Zajko A, Koneru B. Hepatic bilomas due to hepatic artery thrombosis in liver transplant recipients: percutaneous drainage and clinical outcome. Radiology 1990; 174: Hoffer FA, Teele RL, Lillehei CW, Vacanti JP. Infected bilomas and hepatic artery thrombosis in infant recipients of liver transplants. Radiology 1988; 169: Zemel G, Zajko AB, Skolnick ML, Bron KM, Campbell WL. The role of sonography and transhepatic cholangiography in the diagnosis of biliary complications after liver transplantation. AJR Am J Roentgenol 1988; 151: Sheng R, Ramirez CB, Zajko AB, Campbell WL. Biliary stones and sludge in liver transplant patients: a 13-year experience. Radiology 1996; 198: Stevens SD, Heiken JP, Brunt E, Hanto DW, Flye MW. Low-attenuation periportal collar in transplanted liver is not reliable CT evidence of acute allograft rejection. AJR Am J Roentgenol 1991; 157: Pickhardt PJ, Siegel MJ. Posttransplantation lymphoproliferative disorder of the abdomen: CT evaluation in 51 patients. Radiology 1999; 213:
Stenoses of Vascular Anastomoses After Hepatic Transplantation: Treatment with Balloon Angioplasty
 167 Stenoses of Vascular Anastomoses After Hepatic Transplantation: Treatment with Balloon Angioplasty Nigel Raby1 Vascular complications after liver transplantation include occlusion or stenosis at the
167 Stenoses of Vascular Anastomoses After Hepatic Transplantation: Treatment with Balloon Angioplasty Nigel Raby1 Vascular complications after liver transplantation include occlusion or stenosis at the
The role of interventional radiology in complications after paediatric liver transplantation
 The role of interventional radiology in complications after paediatric liver transplantation J Cantrell, M Ch, FCRad (S) Wits onald Gordon Medical Centre, University of the Witwatersrand, Johannesburg,
The role of interventional radiology in complications after paediatric liver transplantation J Cantrell, M Ch, FCRad (S) Wits onald Gordon Medical Centre, University of the Witwatersrand, Johannesburg,
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options
 Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
TIAN AND OTHERS common hepatic artery. For LDLT, a microvascular technique was employed to anastomose the donor artery to either the right or left hep
 Original Article Treatment of Hepatic Artery Thrombosis After Orthotopic Liver Transplantation Ming Guo Tian, Wai Kuen Tso, 1 Chung Mau Lo, Chi Leung Liu and Sheung Tat Fan, Departments of Surgery and
Original Article Treatment of Hepatic Artery Thrombosis After Orthotopic Liver Transplantation Ming Guo Tian, Wai Kuen Tso, 1 Chung Mau Lo, Chi Leung Liu and Sheung Tat Fan, Departments of Surgery and
Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging
 Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging Jaimie D. Nathan, MD Associate Professor of Surgery and Pediatrics Associate Surgical Director, Liver Transplant
Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging Jaimie D. Nathan, MD Associate Professor of Surgery and Pediatrics Associate Surgical Director, Liver Transplant
Outcomes and Risk Factors for Failure of Radiologic Treatment of Biliary Strictures in Pediatric Liver Transplantation Recipients
 LIVER TRANSPLANTATION 12:821-826, 2006 ORIGINAL ARTICLE Outcomes and Risk Factors for Failure of Radiologic Treatment of Biliary Strictures in Pediatric Liver Transplantation Recipients Bhanu Sunku, 1
LIVER TRANSPLANTATION 12:821-826, 2006 ORIGINAL ARTICLE Outcomes and Risk Factors for Failure of Radiologic Treatment of Biliary Strictures in Pediatric Liver Transplantation Recipients Bhanu Sunku, 1
Liver transplantation has become an important
 3DCT Angiography for Detection of Vascular Complications in Pediatric Liver Transplantation Yu Fan Cheng, 1,2 Chao Long Chen, 3 Tung Liang Huang, 1 Tai Yi Chen, 1 Yaw Sen Chen, 3 Chih Chi Wang, 3 Leo Leung-chit
3DCT Angiography for Detection of Vascular Complications in Pediatric Liver Transplantation Yu Fan Cheng, 1,2 Chao Long Chen, 3 Tung Liang Huang, 1 Tai Yi Chen, 1 Yaw Sen Chen, 3 Chih Chi Wang, 3 Leo Leung-chit
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Hematologic Malignancies of the Liver : Spectrum of Disease. Zhou Jian
 Hematologic Malignancies of the Liver : Spectrum of Disease Zhou Jian 2015-7-8 Hematologic malignancies include a wide spectrum of lymphoproliferative and myeloproliferative disorders with nodal and extranodal
Hematologic Malignancies of the Liver : Spectrum of Disease Zhou Jian 2015-7-8 Hematologic malignancies include a wide spectrum of lymphoproliferative and myeloproliferative disorders with nodal and extranodal
Biliary Anatomy in Living-related Liver Transplantation
 The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
BILIARY TRACT COMPLICATIONS IN HUMAN ORTHOTOPIC LIVER TRANSPLANTATION 1,2
 004-33/8/430-004$02.00/0 TRANSPLANTATION Copyright (c) 98 by The Williams & Wilkins Co. Vol. 43, No. Printed in U.S.A. BILIARY TRACT COMPLICATIONS IN HUMAN ORTHOTOPIC LIVER TRANSPLANTATION,2 JAN LERUT,
004-33/8/430-004$02.00/0 TRANSPLANTATION Copyright (c) 98 by The Williams & Wilkins Co. Vol. 43, No. Printed in U.S.A. BILIARY TRACT COMPLICATIONS IN HUMAN ORTHOTOPIC LIVER TRANSPLANTATION,2 JAN LERUT,
Vascular Imaging in the Pediatric Abdomen. Jonathan Swanson, MD
 Vascular Imaging in the Pediatric Abdomen Jonathan Swanson, MD Goals and Objectives To understand the imaging approach, appearance, and clinical manifestations of the common pediatric abdominal vascular
Vascular Imaging in the Pediatric Abdomen Jonathan Swanson, MD Goals and Objectives To understand the imaging approach, appearance, and clinical manifestations of the common pediatric abdominal vascular
Imaging of liver and pancreas
 Imaging of liver and pancreas.. Disease of the liver Focal liver disease Diffusion liver disease Focal liver disease Benign Cyst Abscess Hemangioma FNH Hepatic adenoma HCC Malignant Fibrolamellar carcinoma
Imaging of liver and pancreas.. Disease of the liver Focal liver disease Diffusion liver disease Focal liver disease Benign Cyst Abscess Hemangioma FNH Hepatic adenoma HCC Malignant Fibrolamellar carcinoma
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
The role for contrast-enhanced ultrasonography outside of focal liver lesions
 The role for contrast-enhanced ultrasonography outside of focal liver lesions Paul S. Sidhu King s College Hospital, London, UK Introduction Contrast-enhanced ultrasonography (US) of focal liver lesions
The role for contrast-enhanced ultrasonography outside of focal liver lesions Paul S. Sidhu King s College Hospital, London, UK Introduction Contrast-enhanced ultrasonography (US) of focal liver lesions
The role of abdominal CT and MRI in detection of complications after transplantations of liver, kidney and pancreas.
 The role of abdominal CT and MRI in detection of complications after transplantations of liver, kidney and pancreas. Poster No.: C-1319 Congress: ECR 2015 Type: Educational Exhibit Authors: R. Muslimov,
The role of abdominal CT and MRI in detection of complications after transplantations of liver, kidney and pancreas. Poster No.: C-1319 Congress: ECR 2015 Type: Educational Exhibit Authors: R. Muslimov,
Overall Goals and Objectives for Transplant Hepatology EPAs:
 Overall Goals and Objectives for Transplant Hepatology EPAs: 1. DIAGNOSTIC LIST During the one-year Advanced Pediatric Transplant Hepatology Program, fellows are expected to develop comprehensive skills
Overall Goals and Objectives for Transplant Hepatology EPAs: 1. DIAGNOSTIC LIST During the one-year Advanced Pediatric Transplant Hepatology Program, fellows are expected to develop comprehensive skills
OPERATIVE TECHNIQUES AND HAZARDS
 OPERATIVE TECHNIQUES AND HAZARDS CHRIS O SULLIVAN MD FRCSI CONSULTANT HBP AND LIVER TRANSPLANT SURGEON FREEMAN HOSPITAL, N-UPON-TYNE CAVAL RECONSTRUCTION IN ORTHOTOPIC LIVER TRANSPLANTATION RESECTION OF
OPERATIVE TECHNIQUES AND HAZARDS CHRIS O SULLIVAN MD FRCSI CONSULTANT HBP AND LIVER TRANSPLANT SURGEON FREEMAN HOSPITAL, N-UPON-TYNE CAVAL RECONSTRUCTION IN ORTHOTOPIC LIVER TRANSPLANTATION RESECTION OF
Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation
 Kasr El Aini Journal of Surgery VOL., 9, NO 3 January 2008 19 Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation A. Ayad ; W. Tobar; M.Hassan; A.Hosny; M.El Shazly;
Kasr El Aini Journal of Surgery VOL., 9, NO 3 January 2008 19 Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation A. Ayad ; W. Tobar; M.Hassan; A.Hosny; M.El Shazly;
Ultrasound in Liver Trasplantation
 Ultrasound in Liver Trasplantation Poster No.: C-1892 Congress: ECR 2011 Type: Educational Exhibit Authors: B. Molinares, A. Marquez, M. Ochoa, S. Alvarez; CO Keywords: Ultrasound-Spectral Doppler, Ultrasound-Colour
Ultrasound in Liver Trasplantation Poster No.: C-1892 Congress: ECR 2011 Type: Educational Exhibit Authors: B. Molinares, A. Marquez, M. Ochoa, S. Alvarez; CO Keywords: Ultrasound-Spectral Doppler, Ultrasound-Colour
Liver Transplantation
 1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
The role of cholangiography with t-tube in the liver transplantation
 The role of cholangiography with t-tube in the liver transplantation Poster No.: C-0362 Congress: ECR 2012 Type: Educational Exhibit Authors: S. Magalhães, I. Ferreira, A. B. Ramos, F. Reis, M. Ribeiro
The role of cholangiography with t-tube in the liver transplantation Poster No.: C-0362 Congress: ECR 2012 Type: Educational Exhibit Authors: S. Magalhães, I. Ferreira, A. B. Ramos, F. Reis, M. Ribeiro
Obliterative hepatocavopathy ultrasound and cavography findings
 doi:10.2478/v10019-008-0020-6 case report Obliterative hepatocavopathy ultrasound and cavography findings Ramazan Kutlu Department of Radiology, Inonu University School of Medicine, Malatya, Turkey ackgound.
doi:10.2478/v10019-008-0020-6 case report Obliterative hepatocavopathy ultrasound and cavography findings Ramazan Kutlu Department of Radiology, Inonu University School of Medicine, Malatya, Turkey ackgound.
Early Posttransplantation Portal Vein Stenosis Following Living Donor Liver Transplantation: Percutaneous Transhepatic Primary Stent Placement
 LIVER TRANSPLANTATION 13:530-536, 2007 ORIGINAL ARTICLE Early Posttransplantation Portal Vein Stenosis Following Living Donor Liver Transplantation: Percutaneous Transhepatic Primary Stent Placement Gi-Young
LIVER TRANSPLANTATION 13:530-536, 2007 ORIGINAL ARTICLE Early Posttransplantation Portal Vein Stenosis Following Living Donor Liver Transplantation: Percutaneous Transhepatic Primary Stent Placement Gi-Young
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
Journal of Medical Imaging and Radiation Oncology
 Journal of Medical Imaging and Radiation Oncology 62 (2018) 504 511 MEDICAL IMAGING PICTORIAL ESSAY Imaging in pancreas transplantation complications: Temporal classification Paula Gallego Ferrero and
Journal of Medical Imaging and Radiation Oncology 62 (2018) 504 511 MEDICAL IMAGING PICTORIAL ESSAY Imaging in pancreas transplantation complications: Temporal classification Paula Gallego Ferrero and
NYU School of Medicine Department of Radiology Rotation-Specific House Staff Evaluation
 Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Radiology Rounds A Newsletter for Referring Physicians Massachusetts General Hospital Department of Radiology
 Radiology Rounds A Newsletter for Referring Physicians Massachusetts General Hospital Department of Radiology Imaging for Pre-Transplant Evaluation of Living Donor Liver Transplantation Imaging plays a
Radiology Rounds A Newsletter for Referring Physicians Massachusetts General Hospital Department of Radiology Imaging for Pre-Transplant Evaluation of Living Donor Liver Transplantation Imaging plays a
'fi. Special Article. Vascular Complications After Liver Transplantation: A 5-Year Experience
 657 'fi I Special Article Vascular Complications After Liver ation: A 5-Year Experience Paul Wozney 1 Albert B. Zajko 1 Klaus M. Bran 1 Stuart Point 1 Thomas E. Stard During the past 5 years, 104 angiographic
657 'fi I Special Article Vascular Complications After Liver ation: A 5-Year Experience Paul Wozney 1 Albert B. Zajko 1 Klaus M. Bran 1 Stuart Point 1 Thomas E. Stard During the past 5 years, 104 angiographic
Case Report INTRODUCTION CASE REPORT
 Case Report J Korean Soc Transplant 2016;30:89-93 http://dx.doi.org/10.4285/jkstn.2016.30.2.89 Late Hepatic Venous Outflow Obstruction Following Inferior Vena Cava Stenting in Patient with Deceased Donor
Case Report J Korean Soc Transplant 2016;30:89-93 http://dx.doi.org/10.4285/jkstn.2016.30.2.89 Late Hepatic Venous Outflow Obstruction Following Inferior Vena Cava Stenting in Patient with Deceased Donor
Percutaneous Transhepatic Cholangiography and Biliary Drainage in Pediatric Liver Transplant Patients
 Jonathan M. Lorenz 1 Brian Funaki Jeffrey A. Leef Jordan D. Rosenblum Thuong Van Ha Received June 27, 2000; accepted after revision August 16, 2000. 1 All authors: Department of Radiology, The University
Jonathan M. Lorenz 1 Brian Funaki Jeffrey A. Leef Jordan D. Rosenblum Thuong Van Ha Received June 27, 2000; accepted after revision August 16, 2000. 1 All authors: Department of Radiology, The University
Sonographic Evaluation of Venous Obstruction in Liver Transplants
 Sonography of Venous Obstruction in Liver Transplants Hepatobiliary Imaging Original Research Wui K. Chong 1 Jason C. Beland 1,2 Susan M. Weeks 1,3 Chong WK, Beland JC, Weeks SM Keywords: Doppler sonography,
Sonography of Venous Obstruction in Liver Transplants Hepatobiliary Imaging Original Research Wui K. Chong 1 Jason C. Beland 1,2 Susan M. Weeks 1,3 Chong WK, Beland JC, Weeks SM Keywords: Doppler sonography,
Abdomen Sonography Examination Content Outline
 Abdomen Sonography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 Anatomy, Perfusion, and Function Pathology, Vascular Abnormalities, Trauma, and Postoperative Anatomy
Abdomen Sonography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 Anatomy, Perfusion, and Function Pathology, Vascular Abnormalities, Trauma, and Postoperative Anatomy
Guidelines, Policies and Statements D5 Statement on Abdominal Scanning
 Guidelines, Policies and Statements D5 Statement on Abdominal Scanning Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D5 Statement on Abdominal Scanning Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Treatment of choice for end stage renal disease Imaging to establish baseline and diagnosis of potential complications Review common surgical
 Treatment of choice for end stage renal disease Imaging to establish baseline and diagnosis of potential complications Review common surgical techniques Review normal appearance Discuss US diagnosis of
Treatment of choice for end stage renal disease Imaging to establish baseline and diagnosis of potential complications Review common surgical techniques Review normal appearance Discuss US diagnosis of
Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association
 CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
THE first human liver transplantation was performed in 1963 (1).
 305 "'t,.1 Albert B. Zajko, M.D. Klaus M. Bron, M.D. Thomas E. Starzl, M.D. David H. Van Thiel, M.D. J. Carlton Gartner, M.D. Shunzaburo Iwatsuki, M.D. Byers W. Shaw, Jr., M.D. Basil J. Zitelli, M.D. J.
305 "'t,.1 Albert B. Zajko, M.D. Klaus M. Bron, M.D. Thomas E. Starzl, M.D. David H. Van Thiel, M.D. J. Carlton Gartner, M.D. Shunzaburo Iwatsuki, M.D. Byers W. Shaw, Jr., M.D. Basil J. Zitelli, M.D. J.
PORTAL HYPERTENSION. Tianjin Medical University LIU JIAN
 PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
Spontaneous portosystemic venous shunts in liver cirrhosis: Anatomy, pathophysiology, hemodynamic changes and imaging findings
 Spontaneous portosystemic venous shunts in liver cirrhosis: Anatomy, pathophysiology, hemodynamic changes and imaging findings Poster No.: C-3193 Congress: ECR 2010 Type: Educational Exhibit Topic: Vascular
Spontaneous portosystemic venous shunts in liver cirrhosis: Anatomy, pathophysiology, hemodynamic changes and imaging findings Poster No.: C-3193 Congress: ECR 2010 Type: Educational Exhibit Topic: Vascular
Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated with stent failure
 Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Biliary Atresia. Karen F. Murray, MD Professor of Pediatrics Director, Hepatobiliary Program Seattle Children s
 Biliary Atresia Karen F. Murray, MD Professor of Pediatrics Director, Hepatobiliary Program Seattle Children s Biliary Atresia Incidence: 1/8,000-15,000 live births Girls > boys 1.5:1 The most common cause
Biliary Atresia Karen F. Murray, MD Professor of Pediatrics Director, Hepatobiliary Program Seattle Children s Biliary Atresia Incidence: 1/8,000-15,000 live births Girls > boys 1.5:1 The most common cause
State of the Art Imaging for Hepatic Malignancy: My Assignment
 State of the Art Imaging for Hepatic Malignancy: My Assignment CT vs MR vs MRCP Which one to choose for HCC vs Cholangiocarcinoma What special protocols to use for liver tumors Role of PET and Duplex US
State of the Art Imaging for Hepatic Malignancy: My Assignment CT vs MR vs MRCP Which one to choose for HCC vs Cholangiocarcinoma What special protocols to use for liver tumors Role of PET and Duplex US
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Biliary cancers: imaging diagnosis. Study of 30 cases
 Biliary cancers: imaging diagnosis. Study of 30 cases N Hammoune, S Semlali, M Eddarai, T. Amil, M Zentar, S. El Kandri,, M Benameur,, S Chaouir. Radiology Department. Mohamed V Military Hospital. Rabat-
Biliary cancers: imaging diagnosis. Study of 30 cases N Hammoune, S Semlali, M Eddarai, T. Amil, M Zentar, S. El Kandri,, M Benameur,, S Chaouir. Radiology Department. Mohamed V Military Hospital. Rabat-
Hilar cholangiocarcinoma. Frank Wessels, Maarten van Leeuwen, UMCU utrecht
 Hilar cholangiocarcinoma Frank Wessels, Maarten van Leeuwen, UMCU utrecht Content Anatomy Biliary strictures (Hilar) Cholangiocarcinoom Staging Biliary tract 1 st order Ductus hepatica dextra Ductus hepaticus
Hilar cholangiocarcinoma Frank Wessels, Maarten van Leeuwen, UMCU utrecht Content Anatomy Biliary strictures (Hilar) Cholangiocarcinoom Staging Biliary tract 1 st order Ductus hepatica dextra Ductus hepaticus
Hepatic venous congestion (HVC) from deprivation
 Cryopreserved Iliac Artery is Indispensable Interposition Graft Material for Middle Hepatic Vein Reconstruction of Right Liver Grafts Shin Hwang, Sung-Gyu Lee, Chul-Soo Ahn, Kwang-Min Park, Ki-Hun Kim,
Cryopreserved Iliac Artery is Indispensable Interposition Graft Material for Middle Hepatic Vein Reconstruction of Right Liver Grafts Shin Hwang, Sung-Gyu Lee, Chul-Soo Ahn, Kwang-Min Park, Ki-Hun Kim,
Role of magnetic resonance cholangiography (MRC) in the detection of biliary complications after orthotopic liver transplantation (OLT)
 Role of magnetic resonance cholangiography (MRC) in the detection of biliary complications after orthotopic liver transplantation (OLT) Poster No.: B-227 Congress: ECR 2010 Type: Topic: Scientific Paper
Role of magnetic resonance cholangiography (MRC) in the detection of biliary complications after orthotopic liver transplantation (OLT) Poster No.: B-227 Congress: ECR 2010 Type: Topic: Scientific Paper
MAKING CONNECTIONS. Los Angeles Medical Center
 MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Results of Choledochojejunostomy in the Treatment of Biliary Complications After Liver Transplantation in the Era of Nonsurgical Therapies
 Results of Choledochojejunostomy in the Treatment of Biliary Complications After Liver Transplantation in the Era of Nonsurgical Therapies Brian R. Davidson, Rakesh Rai, Ashim Nandy, Nilesh Doctor, Andrew
Results of Choledochojejunostomy in the Treatment of Biliary Complications After Liver Transplantation in the Era of Nonsurgical Therapies Brian R. Davidson, Rakesh Rai, Ashim Nandy, Nilesh Doctor, Andrew
Ischemic-type biliary lesions (ITBL) are reported to. Prevention of Ischemic-Type Biliary Lesions by Arterial Back-Table Pressure Perfusion
 Prevention of Ischemic-Type Biliary Lesions by Arterial Back-Table Pressure Perfusion Christian Moench, * Kerstin Moench, Ansgar W. Lohse, Jochen Thies, * and Gerd Otto * Ischemic-type biliary lesions
Prevention of Ischemic-Type Biliary Lesions by Arterial Back-Table Pressure Perfusion Christian Moench, * Kerstin Moench, Ansgar W. Lohse, Jochen Thies, * and Gerd Otto * Ischemic-type biliary lesions
Endovascular Treatment of Active Bleeding after Liver Transplant
 Endovascular Treatment of Active Bleeding after Liver Transplant Ali Harman, 1 Fatih Boyvat, 1 Baris Hasdogan, 1 Cuneyt Aytekin, 1 Hamdi Karakayali, 2 Mehmet Haberal 2 Objectives: To evaluate the incidence
Endovascular Treatment of Active Bleeding after Liver Transplant Ali Harman, 1 Fatih Boyvat, 1 Baris Hasdogan, 1 Cuneyt Aytekin, 1 Hamdi Karakayali, 2 Mehmet Haberal 2 Objectives: To evaluate the incidence
بسم الله الرحمن الرحيم أوتيتم من العلم إال قليال وما
 بسم الله الرحمن الرحيم أوتيتم من العلم إال قليال وما 1 2 Goals of the Lecture: What is the portal vein? How common is PVT? What conditions are associated with PVT? How does patient with PVT present? How
بسم الله الرحمن الرحيم أوتيتم من العلم إال قليال وما 1 2 Goals of the Lecture: What is the portal vein? How common is PVT? What conditions are associated with PVT? How does patient with PVT present? How
Can Doppler Sonography Discern Between Hemodynamically Significant and Insignificant Portal Vein Stenosis After Adult Liver Transplantation?
 Vascular and Interventional Radiology Original Research Mullan et al. Sonography of Portal Vein Stenosis Vascular and Interventional Radiology Original Research Charles P. Mullan 1 Bettina Siewert Robert
Vascular and Interventional Radiology Original Research Mullan et al. Sonography of Portal Vein Stenosis Vascular and Interventional Radiology Original Research Charles P. Mullan 1 Bettina Siewert Robert
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Extensive Use of Split Liver for Pediatric Liver Transplantation: A Single-Center Experience
 ORIGINAL ARTICLES Extensive Use of Split Liver for Pediatric Liver Transplantation: A Single-Center Experience Marco Spada, Bruno Gridelli, Michele Colledan, Andrea Segalin, Alessandro Lucianetti, Wanda
ORIGINAL ARTICLES Extensive Use of Split Liver for Pediatric Liver Transplantation: A Single-Center Experience Marco Spada, Bruno Gridelli, Michele Colledan, Andrea Segalin, Alessandro Lucianetti, Wanda
Percutaneous Transhepatic Stent Placement in the Management of Portal Venous Stenosis After Curative Surgery for Pancreatic and Biliary Neoplasms
 Vascular and Interventional Radiology Original Research Kim et al. Transhepatic Stent Placement for Postsurgical Stenosis Vascular and Interventional Radiology Original Research Kyung Rae Kim 1 Gi-Young
Vascular and Interventional Radiology Original Research Kim et al. Transhepatic Stent Placement for Postsurgical Stenosis Vascular and Interventional Radiology Original Research Kyung Rae Kim 1 Gi-Young
DR. DO NGUYEN TIN CHILDREN HOSPITAL 1
 DR. DO NGUYEN TIN CHILDREN HOSPITAL 1 BACKGROUND Congenital extrahepatic porto-systemic shunt (CEPS), known as Abernethy malformation, is a rare malformation. Intestinal and/or splenic venous blood bypasses
DR. DO NGUYEN TIN CHILDREN HOSPITAL 1 BACKGROUND Congenital extrahepatic porto-systemic shunt (CEPS), known as Abernethy malformation, is a rare malformation. Intestinal and/or splenic venous blood bypasses
Portal Venous Thrombosis: Tumor VS Bland Thrombus
 June 2015 Portal Venous Thrombosis: Tumor VS Bland Thrombus SERGIO ALFARO, HARVARD MEDICAL SCHOOL YEAR III GILLIAN LIEBERMAN, MD Overview 2 Index Patient History Portal Venous Thrombosis (PVT) Imaging
June 2015 Portal Venous Thrombosis: Tumor VS Bland Thrombus SERGIO ALFARO, HARVARD MEDICAL SCHOOL YEAR III GILLIAN LIEBERMAN, MD Overview 2 Index Patient History Portal Venous Thrombosis (PVT) Imaging
Liver Transplantation for Biliary Atresia: 19-Year, Single-Center Experience
 Liver Transplantation for Biliary Atresia: 19-Year, Single-Center Experience L Thomas Chin 1, Anthony M D Alessandro 1, Stuart J Knechtle 1, Luis A Fernandez 1, Glen Leverson 1, Robert H Judd 2, Elizabeth
Liver Transplantation for Biliary Atresia: 19-Year, Single-Center Experience L Thomas Chin 1, Anthony M D Alessandro 1, Stuart J Knechtle 1, Luis A Fernandez 1, Glen Leverson 1, Robert H Judd 2, Elizabeth
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The authors have declared no conflicts of interest.
 Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
LIVER TRANSPLANTATION
 LIVER TRANSPLANTATION Selection 0 / Patients and Results Late Mortality and Morbidity After Liver Transplantation S. Iatsuki. T.E. Starzl. R.D. Gordon, C.O. Esquivel. S. Todo, A.G. Tzakis, L. Makoka. J.W.
LIVER TRANSPLANTATION Selection 0 / Patients and Results Late Mortality and Morbidity After Liver Transplantation S. Iatsuki. T.E. Starzl. R.D. Gordon, C.O. Esquivel. S. Todo, A.G. Tzakis, L. Makoka. J.W.
Diagnosis and Endovascular Treatment of Common Vascular Complications in the Post Liver Transplant Patient: A Pictorial Essay
 Diagnosis and Endovascular Treatment of Common Vascular Complications in the Post Liver Transplant Patient: A Pictorial Essay Michael O Neill, MD 1, Jamie Rosenkrantz, MD 2, Jason Salsamendi, MD 1, Shree
Diagnosis and Endovascular Treatment of Common Vascular Complications in the Post Liver Transplant Patient: A Pictorial Essay Michael O Neill, MD 1, Jamie Rosenkrantz, MD 2, Jason Salsamendi, MD 1, Shree
Case 8038 Renal allograft complicated with renal artery stenosis
 Case 8038 Renal allograft complicated with renal artery stenosis Santiago I, Canelas A, Pinto AP Section: Cardiovascular Published: 2009, Nov. 30 Patient: 61 year(s), male Clinical History A 61-year-old
Case 8038 Renal allograft complicated with renal artery stenosis Santiago I, Canelas A, Pinto AP Section: Cardiovascular Published: 2009, Nov. 30 Patient: 61 year(s), male Clinical History A 61-year-old
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign
 Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Jaundice. Agnieszka Dobrowolska- Zachwieja, MD, PhD
 Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Preliminary study of the permeability and safety of covered stents-grafts in pediatric TIPS
 Preliminary study of the permeability and safety of covered stents-grafts in pediatric TIPS Poster No.: C-0354 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Bueno Palomino, L. Zurera Tendero,
Preliminary study of the permeability and safety of covered stents-grafts in pediatric TIPS Poster No.: C-0354 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Bueno Palomino, L. Zurera Tendero,
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
Role of Gd-EOB-DTPA enhanced MR Imaging in the evaluation of the transplanted liver: Advantages and Limitations
 Role of Gd-EOB-DTPA enhanced MR Imaging in the evaluation of the transplanted liver: Advantages and Limitations Robinson Yu, MD, Amir A. Borhani, MD, Alessandro Furlan, MD, Matthew T. Heller, MD, Mitchell
Role of Gd-EOB-DTPA enhanced MR Imaging in the evaluation of the transplanted liver: Advantages and Limitations Robinson Yu, MD, Amir A. Borhani, MD, Alessandro Furlan, MD, Matthew T. Heller, MD, Mitchell
Paediatric Liver Transplant Programme Wits Donald Gordon Medical Centre
 Paediatric Liver Transplant Programme Wits Donald Gordon Medical Centre J Loveland, J Botha, R Britz, B Strobele, S Rambarran, A Terblanche, C Kock, P Walabh, M Beretta, M Duncan et al 1817 reveal the
Paediatric Liver Transplant Programme Wits Donald Gordon Medical Centre J Loveland, J Botha, R Britz, B Strobele, S Rambarran, A Terblanche, C Kock, P Walabh, M Beretta, M Duncan et al 1817 reveal the
Renal Transplant Surgery
 Renal Transplant Surgery Mr Somaiah Aroori MS MD EBS in HPB FRCS Consultant HPB & Renal Transplant Surgeon SWTC, Derriford Hospital, Plymouth Over next few minutes Aim to cover Details of Transplant procedure
Renal Transplant Surgery Mr Somaiah Aroori MS MD EBS in HPB FRCS Consultant HPB & Renal Transplant Surgeon SWTC, Derriford Hospital, Plymouth Over next few minutes Aim to cover Details of Transplant procedure
Personal Profile. Name: 劉 XX Gender: Female Age: 53-y/o Past history. Hepatitis B carrier
 Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
CASE REPORT CECT EVALUATION OF AN ISOLATED LONG SEGMENT IVC THROMBUS IN A PATIENT WITH ACUTE ON CHRONIC PANCREATITIS: A CASE REPORT
 CECT EVALUATION OF AN ISOLATED LONG SEGMENT IVC THROMBUS IN A PATIENT WITH ACUTE ON CHRONIC PANCREATITIS: A Pronami Borah 1, Biswajit Borah 2, Kangkana Mahanta 3, Rudra K. Gogoi 4 HOW TO CITE THIS ARTICLE:
CECT EVALUATION OF AN ISOLATED LONG SEGMENT IVC THROMBUS IN A PATIENT WITH ACUTE ON CHRONIC PANCREATITIS: A Pronami Borah 1, Biswajit Borah 2, Kangkana Mahanta 3, Rudra K. Gogoi 4 HOW TO CITE THIS ARTICLE:
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
University of Colorado Health Sciences Center, Denver Colorado ******************** ******************
 University of Colorado Health Sciences Center, Denver Colorado ******************** 1988-2005 ****************** Disclosures No disclosures Case 53 M presents with sudden onset of upper abdominal pain
University of Colorado Health Sciences Center, Denver Colorado ******************** 1988-2005 ****************** Disclosures No disclosures Case 53 M presents with sudden onset of upper abdominal pain
CT abdomen and pelvis
 CT abdomen and pelvis General indications: Assessment of vague abdominal symptoms (pain, colics,distenstion,...) Varifecation of a lesion discovered by other diagnostic modalities as US, barium,ivp, Staging
CT abdomen and pelvis General indications: Assessment of vague abdominal symptoms (pain, colics,distenstion,...) Varifecation of a lesion discovered by other diagnostic modalities as US, barium,ivp, Staging
All-in-one sleeve patch graft venoplasty for multiple hepatic vein reconstruction in living donor liver transplantation
 DOI:10.1111/j.1477-2574.2012.00442.x HPB Technical Report All-in-one sleeve patch graft venoplasty for multiple hepatic vein reconstruction in living donor liver transplantation Chao-Long Chen*, Anthony
DOI:10.1111/j.1477-2574.2012.00442.x HPB Technical Report All-in-one sleeve patch graft venoplasty for multiple hepatic vein reconstruction in living donor liver transplantation Chao-Long Chen*, Anthony
Imaging of Whole-Organ Pancreas Transplants 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Radiological Investigations of Abdominal Trauma
 76 77 Investigations of Abdominal Trauma Introduction: Trauma to abdominal organs is a common cause of patient morbidity and mortality among trauma patients. Causes of abdominal trauma include blunt injuries,
76 77 Investigations of Abdominal Trauma Introduction: Trauma to abdominal organs is a common cause of patient morbidity and mortality among trauma patients. Causes of abdominal trauma include blunt injuries,
Primary Living-Donor Liver Transplantation at the University of Chicago
 ANNALS OF SURGERY Vol. 232, No. 1, 104 111 2000 Lippincott Williams & Wilkins, Inc. Primary Living-Donor Liver Transplantation at the University of Chicago Technical Aspects of the First 104 Recipients
ANNALS OF SURGERY Vol. 232, No. 1, 104 111 2000 Lippincott Williams & Wilkins, Inc. Primary Living-Donor Liver Transplantation at the University of Chicago Technical Aspects of the First 104 Recipients
Liver Splitting During Normothermic Organ Preservation
 LETTERS FROM THE FRONTLINE Liver Splitting During Normothermic Organ Preservation TO THE EDITOR: Although widely established as a means to increase the number of patients who can benefit from transplantation,
LETTERS FROM THE FRONTLINE Liver Splitting During Normothermic Organ Preservation TO THE EDITOR: Although widely established as a means to increase the number of patients who can benefit from transplantation,
Technique of Split-Liver Transplant for Two Adult Recipients
 F'UJIUWA H.EAL,THCAREi, INC. PRESENTS IMAGES mljk?zr 3TUiVU?MAZ7ON Technique of Split-Liver Transplant for Two Adult Recipients Abhinuv Humur, KhuLid Khwuju> Timothy D. SieLu$'John R. Luke, und WiLLium
F'UJIUWA H.EAL,THCAREi, INC. PRESENTS IMAGES mljk?zr 3TUiVU?MAZ7ON Technique of Split-Liver Transplant for Two Adult Recipients Abhinuv Humur, KhuLid Khwuju> Timothy D. SieLu$'John R. Luke, und WiLLium
Tranjugular Intrahepatic Portosystemic Shunt
 Tranjugular Intrahepatic Portosystemic Shunt Christopher Selhorst July 25, 2005 BIDMC Radiology Overview Portal Hypertension Indications, Contraindications The Procedure Case Review Complications Outcomes
Tranjugular Intrahepatic Portosystemic Shunt Christopher Selhorst July 25, 2005 BIDMC Radiology Overview Portal Hypertension Indications, Contraindications The Procedure Case Review Complications Outcomes
Case Report Inferior Vena Cava Torsion and Stenosis Complicated by Compressive Pericaval Regional Ascites following Orthotopic Liver Transplantation
 Case Reports in Radiology Volume 2013, Article ID 576092, 4 pages http://dx.doi.org/10.1155/2013/576092 Case Report Inferior Vena Cava Torsion and Stenosis Complicated by Compressive Pericaval Regional
Case Reports in Radiology Volume 2013, Article ID 576092, 4 pages http://dx.doi.org/10.1155/2013/576092 Case Report Inferior Vena Cava Torsion and Stenosis Complicated by Compressive Pericaval Regional
Collateral Pathways in Budd Chiari Syndrome- MDCT Depiction
 Review Article imedpub Journals http://www.imedpub.com/ http://dx.doi.org/10.4172/ijdd.1000025 Collateral Pathways in Budd Chiari Syndrome- MDCT Depiction Abstract Budd Chiari syndrome (BCS) is a condition
Review Article imedpub Journals http://www.imedpub.com/ http://dx.doi.org/10.4172/ijdd.1000025 Collateral Pathways in Budd Chiari Syndrome- MDCT Depiction Abstract Budd Chiari syndrome (BCS) is a condition
Transplant Hepatology
 Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE
 ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
Value of CT and Doppler Sonography in the Evaluation of Hepatic Vein Stenosis After Dual-Graft Living Donor Liver Transplantation
 CT and Sonography After Liver Transplantation Hepatobiliary Imaging Original Research Seung Soo Lee 1 Kyoung Won Kim 1 Seong Ho Park 1 Yong Moon Shin 1 Pyo Nyun Kim 1 Sung Gyu Lee 2 Moon-Gyu Lee 1 Lee
CT and Sonography After Liver Transplantation Hepatobiliary Imaging Original Research Seung Soo Lee 1 Kyoung Won Kim 1 Seong Ho Park 1 Yong Moon Shin 1 Pyo Nyun Kim 1 Sung Gyu Lee 2 Moon-Gyu Lee 1 Lee
Classification of choledochal cyst with MR cholangiopancreatography in children and infants: special reference to type Ic and type IVa cyst
 Classification of choledochal cyst with MR cholangiopancreatography in children and infants: special reference to type Ic and type IVa cyst Poster No.: C-1333 Congress: ECR 2011 Type: Educational Exhibit
Classification of choledochal cyst with MR cholangiopancreatography in children and infants: special reference to type Ic and type IVa cyst Poster No.: C-1333 Congress: ECR 2011 Type: Educational Exhibit
AMR in Liver Transplantation: Incidence
 AMR in Liver Transplantation: Incidence Primary AMR 1/3 to 1/2 of ABO-incompatible transplants Uncommon with ABO-compatible transplant Secondary AMR Unknown incidence: rarely tested Why is AMR uncommon
AMR in Liver Transplantation: Incidence Primary AMR 1/3 to 1/2 of ABO-incompatible transplants Uncommon with ABO-compatible transplant Secondary AMR Unknown incidence: rarely tested Why is AMR uncommon
Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2003;1:183 188 Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation KAZUNORI HASEGAWA,* SHUJIRO YAZUMI,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2003;1:183 188 Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation KAZUNORI HASEGAWA,* SHUJIRO YAZUMI,*
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Interventional Radiology Rounds:
 1295 Interventional Radiology Rounds: University of California, San Francisco Percutaneous Biliary Drainage in the Management of Cholangiocarcinoma Robert K. Kerlan, Jr., Moderator1 Anton C. Pogany2 Henry
1295 Interventional Radiology Rounds: University of California, San Francisco Percutaneous Biliary Drainage in the Management of Cholangiocarcinoma Robert K. Kerlan, Jr., Moderator1 Anton C. Pogany2 Henry
Portal biliopathy from the image to the diagnostic: a systematic illustrated overview
 Portal biliopathy from the image to the diagnostic: a systematic illustrated overview Poster No.: C-1690 Congress: ECR 2018 Type: Educational Exhibit Authors: F. Stefan, M. D. M. Boros, E. M. Preda, I.
Portal biliopathy from the image to the diagnostic: a systematic illustrated overview Poster No.: C-1690 Congress: ECR 2018 Type: Educational Exhibit Authors: F. Stefan, M. D. M. Boros, E. M. Preda, I.
Intraoperative Stent Placement in the Portal Vein During or After Liver Transplantation
 LIVER TRANSPLANTATION 13:1145-1152, 2007 ORIGINAL ARTICLE Intraoperative Stent Placement in the Portal Vein During or After Liver Transplantation Yong-Jae Kim, Gi-Young Ko,* Hyun-Ki Yoon, Ji-Hoon Shin,
LIVER TRANSPLANTATION 13:1145-1152, 2007 ORIGINAL ARTICLE Intraoperative Stent Placement in the Portal Vein During or After Liver Transplantation Yong-Jae Kim, Gi-Young Ko,* Hyun-Ki Yoon, Ji-Hoon Shin,
Interesting Cases from Liver Tumor Board. Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine
 Interesting Cases from Liver Tumor Board Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Common Liver Diseases Hemangioma Cyst FNH Focal Fat/Sparing THID Non-Cirrhotic
Interesting Cases from Liver Tumor Board Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Common Liver Diseases Hemangioma Cyst FNH Focal Fat/Sparing THID Non-Cirrhotic
