Generally, myopia is a condition of the eye that makes it
|
|
|
- Octavia Franklin
- 5 years ago
- Views:
Transcription
1 Glaucoma Effect of Myopia on the Progression of Primary Open- Angle Glaucoma Jin Young Lee, 1 Kyung Rim Sung, 1 Seungbong Han, 2 and Jung Hwa Na 1 1 Department of Ophthalmology, College of Medicine, University of Ulsan, Asan Medical Center, Seoul, Korea 2 Department of Applied Statistics, Gachon University, Seongnam-si, Gyeonggi-do, Korea Correspondence: Kyung Rim Sung, Department of Ophthalmology, University of Ulsan, College of Medicine, Asan Medical Center, Pungnap- 2-dong, Songpa-gu, Seoul, Korea ; sungeye@gmail.com. Submitted: November 4, 2014 Accepted: February 12, 2015 Citation: Lee JY, Sung KR, Han S, Na JH. Effect of myopia on the progression of primary open-angle glaucoma. Invest Ophthalmol Vis Sci. 2015;56: DOI: / iovs PURPOSE. To evaluate the effect of myopia on the progression of primary open-angle glaucoma. METHODS. In this retrospective cohort study, eyes were classified into nonmyopic (NMG, >0 diopters [D]), mild to moderate (MMG, 0 to 6 D), and highly myopic glaucoma (HMG, < 6 D) groups according to the level of spherical equivalent. Glaucoma progression was determined either by optic disc/retinal nerve fiber layer (RNFL) photographs or by serial visual field (VF) data. Cox s proportional hazard models were used to detect associations between potential risk factors and glaucoma progression. RESULTS. Among 369 eyes from 369 glaucoma patients (average follow-up, 4.4 years), 54 of 178 eyes (30.3%) in the NMG, 49 of 151 eyes (32.5%) in the MMG, and 8 of 40 eyes (20.0%) in the HMG showed progression. When VF was used as a progression criterion, thinner baseline RNFL (hazard ratio [HR]: 0.942, P < 0.001) was predictive of progression. When optic disc/ RNFL photographs were used, worse baseline visual field mean deviation (VF MD) and thinner RNFL were associated. The HMG category was a preventive factor for optic disc/rnfl photographic progression (HR: 0.323, P ¼ 0.031). CONCLUSIONS. No levels of myopia were associated with glaucoma progression in our study. High myopia was a protective factor for optic disc/rnfl progression. These results may be interpreted as a lower progression detection rate because of the difficulty in detecting changes in the optic disc/rnfl in HMG, or as a consequence of some of highly myopic eyes that may not be true cases of glaucoma. Keywords: glaucoma, progression, myopia Generally, myopia is a condition of the eye that makes it difficult to see objects that are far away without optical correction. Although myopia can be induced by lens or corneal curvature or by other factors, axially elongated eyes represent a major portion of all myopia cases. Axial elongation can affect the intraocular structure, such as the optic disc or macula, which are target sites for glaucomatous damage. Many studies have reported that myopia is a risk factor for glaucoma development. 1 3 Large-scale population-based studies have also reported that myopia is a risk factor for glaucoma development. 4 8 Whether myopia is a risk factor for glaucoma progression is still a subject of debate As already mentioned, some studies have reported that myopia is a risk factor for glaucoma progression. 13,14 However, another study on young Chinese myopic eyes with a glaucomatous optic disc that were followed for 7 years did not report progression in their optic discs, regardless of glaucoma treatment. 15 Moreover, two recent papers from Japan have reported that myopia is a preventive factor for glaucoma progression. 16,17 Thus, the association between glaucoma progression and myopia remains unresolved. Considering that myopia is a common condition and that its incidence is increasing in young people, a better understanding of the relationship between myopia and glaucoma progression is an important issue that will require more intensive investigations. 18,19 Hence, to explore the effect of myopia on glaucoma progression, we have here analyzed longitudinal cohort data of medically treated primary openangle glaucoma patients. Additionally, high myopia is thought to have a somewhat different pathology than mild to moderate myopia. Highly myopic eyes show more aggressive pathological changes in the posterior pole of the eye and tend to deteriorate, whereas myopic changes in cases of mild to moderate myopia usually remain stable after adolescence. 20,21 Because the posterior pole includes the optic disc and macula, which are target sites for glaucomatous damage, high myopia and glaucoma might be linked. 1,3,22 Some studies have reported different retinal nerve fiber layer (RNFL) involvement patterns in highly myopic glaucomatous eyes compared to nonhighly myopic glaucomatous eyes, suggesting that the pattern of glaucoma progression may be different in myopic cases of differing severity. 23 Hence, we categorized our participants into three subgroups based on the degree of refractive error as follows: nonmyopic, mildly to moderately myopic, and highly myopic. We also evaluated the risk factors for glaucoma progression in each subgroup. One possible reason for conflicting data regarding glaucoma progression and myopia may be the small number of myopic patients who were analyzed in previous longitudinal studies. In our present study, we intended to investigate this potential association with a relatively large number of participants. Copyright 2015 The Association for Research in Vision and Ophthalmology, Inc. j ISSN:
2 Myopia and the Progression of Glaucoma IOVS j March 2015 j Vol. 56 j No. 3 j 1776 METHODS Subjects We performed a retrospective review of the medical records of all subjects who were evaluated by a single glaucoma specialist (KRS) at the glaucoma clinic of the Asan Medical Center (Seoul, Korea) from March 2008 to April Subjects who met the inclusion criteria were consecutively enrolled. At the initial test, each participant received a comprehensive ophthalmological examination, including a review of the medical history, measurement of best-corrected visual acuity, slit-lamp biomicroscopy, Goldmann applanation tonometry, gonioscopy, central corneal thickness (CCT) measurement (DGH-550 instrument; DGH Technology, Inc., Exton, PA, USA), dilated fundoscopic examination using a 90- or 78-diopter (D) lens, stereoscopic optic disc photography, RNFL photography, a visual field (VF) test, and spectral-domain optical coherence tomography (SD-OCT). To be included in the study, participants had to meet the following criteria at their initial assessment: best-corrected visual acuity of 20/40 or better, the presence of a normal anterior chamber, an open angle on slit-lamp and gonioscopic examinations, glaucomatous optic nerve damage (the presence of focal thinning of the neuroretinal rim or notching and an RNFL defect) and glaucomatous VF defect. These findings were confirmed and agreed upon by two glaucoma specialists (KRS and JYL). Glaucomatous VF defects were defined as those with a cluster of three points with probabilities of <5% on the pattern deviation map in at least one hemifield, including at least one point with a probability of <1%; or a cluster of two points with a probability of <1% and a glaucoma hemifield test (GHT) result outside normal limits; or a pattern standard deviation (PSD) outside 95% of normal limits. We excluded participants with any other ophthalmic or neurological condition that could result in a VF defect or those who had a history of diabetes mellitus. Pseudophakic or aphakic eyes were also excluded. If both eyes of the same patient were found to be eligible, one eye was randomly selected for analysis. All of the subjects with glaucoma in our present study were followed up at 6-month intervals with stereoscopic optic disc photography, RNFL photography, VF testing, and SD-OCT scanning. All tests were performed at the same visit or within a 2-week period. To be included in the analyses, all subjects were followed up for at least 3 years. All participants underwent medical therapy during the follow-up period. If the subject underwent intraocular surgery or laser therapy during the follow-up period, only data obtained before such operations were included. The Institutional Review Board of the Asan Medical Center approved this study, and the study design followed the principles of the Declaration of Helsinki. VF Assessment Visual field tests were performed using a Humphrey field analyzer (Swedish Interactive Threshold Algorithm [SITA] 24-2; Carl Zeiss Meditec, Dublin, CA, USA). Only reliable VF test results (false-positive errors < 15%, false-negative errors < 15%, and fixation loss < 20%) were included in the analysis. The VF test was repeated within 2 weeks of the baseline measurement for confirmation. Patients were expected to come back approximately 1 month after baseline exam to check the response of the medication and underwent the third VF test at that time. Hence a total of three VF tests were performed within the first 6 weeks. The very first VF test data were excluded to obviate any learning effect. Therefore, the second and third VF results, which were obtained within 1 month, were incorporated into analysis as baseline exams. For inclusion in the study cohort, at least five reliable VF tests (except for the very first VF) that were taken at separate visits were required. Visual field progression was determined using commercial software (Humphrey Field Analyzer Guided Progression Analysis [GPA]; Carl Zeiss Meditec) and was defined as significant deterioration from the baseline pattern deviation at three or more of the same test points that were evaluated on three consecutive examinations, or as a significantly negative slope (P < 0.05) in a linear regression analysis using VF mean deviation (MD) data. 24 Optic Disc and RNFL Assessment The progression of optic disc and RNFL defects was determined by an evaluation of a whole series of stereoscopic optic disc and red-free RNFL photographs. Serial stereoscopic photographs were displayed on a liquid crystal display (LCD) monitor. Two glaucoma experts (KRS and JHN) independently assessed all photographs to estimate glaucoma progression. The most recent photograph was compared to the baseline photograph for each patient. The experts were not aware of each other s assessments, and were blind to all clinical, OCT, and VF information. Each grader reviewed all photographs of each eye before making an assessment and was asked to determine glaucomatous optic disc or RNFL progression, as revealed by an increase in the extent of neuroretinal rim thinning, the appearance of new disc hemorrhage, enhancement of disc excavation, and/or any widening or deepening or new appearance of an RNFL defect. Each grader classified each glaucomatous eye as either stable or progressing. If the RNFL photographs were difficult to evaluate because of diffuse atrophy or invisible RNFL resulting from lightly pigmented fundus, the progression determination was obtained by optic disc assessment. If the opinions of the two graders differed, that eye was excluded from subsequent analysis. SD-OCT Assessment Spectral-domain OCT images were obtained using a Cirrus HD OCT system (Carl Zeiss Meditec). The image acquisition procedure has been described in detail elsewhere Our Cirrus HD OCT system is regularly calibrated by a technician employed by the manufacturer. Circumpapillary RNFL (crnfl) thicknesses were measured using the optic disc cube mode, and ganglion cell inner plexiform complex (GCIPL) thicknesses were measured using the macular cube mode. Pupil dilation was performed when necessary. All accepted images exhibited a centered optic disc or fovea, were well focused with even and adequate illumination, exhibited no eye motion within the measurement circle, and had a signal strength of at least 7. Statistical Analysis The eyes of the study participants were divided into the following three groups according to the level of spherical equivalent: a nonmyopic group (>0 D, NMG), a mild to moderate myopic group (0 to 6 D, MMG), and a highly myopic group (< 6 D, HMG). Baseline and follow-up data were compared among these three groups by ANOVA test. Glaucomatous progression was defined based on two criteria, optic disc/rnfl progression and VF progression. We fitted univariate and multivariate Cox proportional hazard models to detect associations between potential risk factors, including the category of refractive error, baseline untreated intraocular pressure (IOP) and mean follow-up IOP, CCT, baseline average crnfl and GCIPL thicknesses, baseline visual field mean deviation (VF MD), and glaucoma progression time based on two different criteria. Furthermore, we conducted subgroup
3 Myopia and the Progression of Glaucoma IOVS j March 2015 j Vol. 56 j No. 3 j 1777 analysis for the three groups. Both univariate and multivariate analyses were performed separately for each group. Variables with a P value less than or equal to 0.20 in the univariate analyses were included as candidate variables for the multivariate regression analysis. A backward elimination process was used to develop the final multivariate model. Data are presented as adjusted hazard ratios (HRs) with 95% confidence intervals (CIs). The Schoenfeld residuals test was used to verify the proportional hazards assumption; no violations were detected during this analysis. All statistical analyses were performed using SPSS version 15.0 (SPSS, Inc., Chicago, IL, USA). RESULTS Twenty-nine eyes (7.3%) from 398 eyes that met other inclusion criteria were excluded due to disagreement between two graders regarding progression assessment. Hence, a total of 369 eyes from 369 subjects were included in our final study cohort. The mean follow-up period (6 standard deviation [SD]) was years, and the mean number of analyzed optic disc/rnfl photographs and VF was and per eye, respectively. Among the 369 subjects, 192 were men, 177 were women, and all were Koreans. Among the 369 eyes, we categorized 178 eyes as NMG, 151 eyes as MMG, and 40 eyes as HMG. Clinical characteristics were described and compared among the three groups (Table 1). The age at baseline was significantly different among the three groups: oldest in the NMG group and youngest in the HMG group ( , years, P < 0.001). The baseline RNFL was thinner in the HMG group than in the NMG group ( , lm, P ¼ 0.043, Table 1). Among the 369 eyes, progression was observed in 91 eyes (24.7%) by optic disc/rnfl photographic assessment, 46 eyes (12.5%) by VF analysis, and 111 eyes (30.1%) by either optic disc/rnfl or VF examination. Among 178 eyes in the NMG group, 45 eyes (25.3%) showed progression by optic disc/ RNFL photographic assessment, 24 eyes (13.5%) by VF analysis, and 54 eyes (30.3%) by either optic disc/rnfl or VF exams. Among the 151 eyes in the MMG group, 42 eyes (27.8%) showed progression by optic disc/rnfl photographic assessment, 18 eyes (11.8%) by VF analysis, and 49 eyes (32.5%) by either optic disc/rnfl or VF exams. Among the 40 eyes in the HMG group, 4 eyes (10.0%) showed progression by optic disc/rnfl photographic assessment, 4 eyes (10.0%) by VF analysis, and 8 eyes (20.0%) by either optic disc/rnfl or VF exams. Glaucoma filtering surgery was performed in 7, 8, and 2 eyes in the NMG, MMG, and HMG groups, respectively, during the follow-up period. Selective laser trabeculoplasty was performed in 7, 13, and 3 eyes in the NMG, MMG, and HMG groups, respectively, during the follow-up period. The univariate and multivariate HRs for each putative risk factor, including the three categories of refractive error in all study participants according to the Cox proportional hazard model, are listed in Table 2. Two types of criteria for glaucoma progression, optic disc/rnfl and VF assessments, were assessed independently. When VF was used as a progression criterion, thinner baseline RNFL (HR; 0.942, P < 0.001) was found to be significant. When the NMG category was used as a reference, neither the MMG (P ¼ 0.553) nor the HMG (P ¼ 0.794) category was a significant risk factor for progression. When optic disc/rnfl photographic assessment was used as a progression criterion, worse baseline VF MD (HR; 0.949, P ¼ 0.007) and thinner RNFL (HR; 0.971, P ¼ 0.004) were associated with progression. The HMG category (HR; 0.323, P ¼ 0.031) was a preventive factor for optic disc/rnfl photographic progression. TABLE 1. Clinical Characteristics of the Three Study Groups Based on Spherical Equivalent In our subgroup analysis, a higher baseline IOP (HR; 1.089, P ¼ 0.001) and thinner baseline RNFL (HR; 0.926, P < 0.001) were found to be associated with VF progression in the NMG group. When using optic disc/rnfl photographic assessment as a progression criterion, thinner baseline GCIPL thickness (HR; 0.939, P < 0.001) was associated with progression (Table 3). In the MMG cases, worse baseline VF MD (HR; 0.899, P < 0.001) was associated with VF progression, and thinner baseline RNFL (HR; 0.955, P < 0.001) was associated with optic disc/rnfl progression (Table 4). In the HMG group, thinner baseline GCIPL (HR; 0.845, P ¼ 0.003) was associated with VF progression, whereas worse baseline VF MD (HR; 0.718, P ¼ 0.008) was found to be associated with optic disc/ RNFL progression (Table 5). DISCUSSION NMG, n ¼ 178 MMG, n ¼ 151 HMG, n ¼ 40 P Value Age <0.002* <0.001 <0.001 Sex, male/ female 86/92 83/68 23/ SE <0.001* <0.001 <0.001 CCT * Baseline IOP * Mean followup IOP * DH occurrence, no/yes 166/12 144/7 39/1 Baseline VF MD Baseline RNFL thickness Baseline GCIPL thickness SE, spherical equivalent; DH, disc hemorrhage. * NMG versus MMG. NMG versus HMG. MMG versus HMG * * * * Myopia is extremely prevalent in Asian countries, especially in the young. 18,28,29 Our present study found that approximately 52% of all analyzed glaucomatous eyes were myopic, including 10.8% of the total eyes that were highly myopic (lower than 6 D). Thus, myopia presents as a frequent condition in Asian glaucomatous eyes. Considering this finding, a determination of whether myopia is a risk factor for glaucoma progression or not is of paramount importance for the management and care of affected individuals.
4 Myopia and the Progression of Glaucoma IOVS j March 2015 j Vol. 56 j No. 3 j 1778 TABLE 2. Univariate and Multivariate Cox Proportional Hazard Model With Backward Elimination for Predicting Glaucoma Progression Using VF and Optic Disc/RNFL Photographic Assessments, Respectively Age ( ) ( ) Sex, male ¼ ( ) ( ) CCT ( ) ( ) Baseline IOP ( ) ( ) Mean follow-up IOP ( ) ( ) Baseline VF MD ( ) < ( ) < ( ) Baseline RNFL thickness ( ) < ( ) < ( ) < ( ) Baseline GCIPL thickness ( ) < ( ) <0.001 *NMG Reference *MMG ( ) ( ) *HMG ( ) ( ) ( ) * Refractive error was analyzed as a categorical variable (NMG, MMG, and HMG), and HR was calculated as a relative HR when using NMG as a reference. TABLE 3. Univariate and Multivariate Cox Proportional Hazard Models With Backward Elimination for Predicting Glaucoma Progression in the NMG Patients Age ( ) ( ) Sex, male ¼ ( ) ( ) RE ( ) ( ) CCT ( ) ( ) Baseline IOP ( ) ( ) ( ) Mean follow-up IOP ( ) ( ) Baseline VF MD ( ) ( ) <0.001 Baseline RNFL thickness ( ) < ( ) < ( ) <0.001 Baseline GCIPL thickness ( ) ( ) < ( ) <0.001 RE, refractive error.
5 Myopia and the Progression of Glaucoma IOVS j March 2015 j Vol. 56 j No. 3 j 1779 TABLE 4. Univariate and Multivariate Cox Proportional Hazard Models With Backward Elimination for Predicting Glaucoma Progression in the MMG Patients Age ( ) ( ) Sex, male ¼ ( ) ( ) RE ( ) ( ) CCT ( ) ( ) Baseline IOP ( ) ( ) Mean follow-up IOP ( ) ( ) Baseline VF MD ( ) < ( ) < ( ) <0.001 Baseline RNFL thickness ( ) ( ) < ( ) <0.001 Baseline GCIPL thickness ( ) ( ) TABLE 5. Univariate and Multivariate Cox Proportional Hazard Models With Backward Elimination for Predicting Glaucoma Progression in the HMG Patients Age ( ) ( ) Sex, male ¼ ( ) ( ) RE ( ) ( ) CCT ( ) ( ) Baseline IOP ( ) ( ) Mean follow-up IOP ( ) ( ) Baseline VF MD ( ) ( ) ( ) Baseline RNFL thickness ( ) ( ) Baseline GCIPL thickness ( ) ( ) ( ) 0.522
6 Myopia and the Progression of Glaucoma IOVS j March 2015 j Vol. 56 j No. 3 j 1780 According to longitudinal follow-up results for our current glaucoma cohort, myopia was not associated with glaucoma progression. We categorized our glaucoma patients into three groups based on the spherical equivalent. Neither the MMG nor the HMG categorization was a significant covariate for progression. Because glaucomatous damage is assessed based on structural changes in the optic disc/rnfl or functional changes in the VF, and as these structural and functional changes may not occur simultaneously in some eyes, 30 we independently used both optic disc/rnfl photographic assessments and VF exams as progression criteria. The refractive error category was found not to be a risk factor for either criterion. Interestingly, high myopia was observed to be a significant preventive factor for progression when using optic disc/rnfl photographic assessment as a criterion. This correlation may be explained by the increased difficulty in detecting progression by optic disc/rnfl photographs in highly myopic glaucomatous eyes. Highly myopic eyes have a tendency to show a tilted optic disc with large peripapilllary atrophy, which makes it difficult to assess glaucomatous neuroretinal rim changes. 31 A lightly pigmented fundus also obscures the detection of changes in the RNFL. Hence, when adopting optic disc or RNFL photographic change as a criterion for glaucoma progression, prevalence of glaucoma progression may appear to be low because the detection rate is low. Another possible explanation is that glaucomatous structural progression per se is lower in highly myopic eyes. A myopic optic disc/rnfl change may mimic the glaucomatous optic disc/rnfl appearance. Therefore, myopic eyes that show a glaucomatous optic disc appearance may not be true glaucoma cases. 32 Hence, these eyes would not show glaucomatous progression. In other words, the HMG group may be mixed, with eyes that mimic glaucomatous optic disc and true glaucomatous eyes; this heterogeneity may lead to the lower prevalence of structural progression in HMG. This is speculation, however, and thus warrants further investigation. Additionally, the HMG group was the youngest among three groups, which may affect the outcome. However, our observation that the category of refractive error was not a significant risk factor when using the VF criterion may suggest that no level of myopia is associated with glaucoma progression in our study. Because refractive errors are based on a numerical scale, they could be analyzed as a continuous variable rather than by the categorization into groups in our current analysis. However, we assumed that the MMG and the HMG cases may have different characteristics in which the use of the refractive error as a continuous variable may bias the result. Hence, we included the categorical covariate as a refractive error in our present analysis. However, we also performed analysis that included the refractive error as a continuous variable, and we again found that this parameter was not a significant factor for progression using either optic disc/rnfl or VF assessment as the progression criterion (data not shown). We characterized the risk factors for glaucoma progression in each of the three groups separately with the assumption that the characteristics of glaucoma may differ among different refractive error groups. Kimura et al. 23 compared highly myopic and nonhighly myopic glaucomatous eyes for RNFL defect location and reported that high myopia is significantly associated with the nearest RNFL defect involving the papillomacular bundle. Considering that typical glaucomatous RNFL changes start at inferotemporal locations in the optic disc, this pattern of central involvement in highly myopic glaucoma is different from the usual glaucomatous pattern. Consequently, we explored whether risk factors for progression would differ among nonmyopic, mild to moderate, and highly myopic eyes. Our findings demonstrated that the risk factors for glaucoma progression are not significantly different among these subgroups. The baseline glaucoma severity, which was assessed by VF MD or OCT RNFL/GCIPL thickness, was found in our current analyses to be associated with glaucoma progression in all three study groups. Optic disc hemorrhage has been reported to be a strong risk factor for glaucoma progression by many publications However, since we included the occurrence of disc hemorrhage as a criterion for optic disc/rnfl progression according to the collaborative normal-tension glaucoma study criterion, 36 we did not include the occurrence of disc hemorrhage in risk factor analysis. Whether optic disc hemorrhage is a sign of glaucoma progression or a risk factor for this progression remains a subject of debate. 37,38 Our current study has several limitations to note. We included and categorized our participants according to the refractive error. Axial length measurement may be a more direct assessment of the degree of myopia, as myopia can be induced by lens changes or other events. However, axial length is strongly associated with refractive error, and eyes with visually significant lens changes were excluded from our analysis, so those effects might not be great. Since this study was a retrospective one, there is a possibility that subjects were treated with different degrees of aggressiveness with respect to their target pressures. Thus, this should be considered in the interpretation of our results. However, as reported in previous studies, most Korean glaucoma patients have a low baseline IOP. 39,40 Consistently, approximately 80% of our current study cases had a baseline IOP of less than 21 mm Hg. And most of our patients had well-controlled IOP during the follow-up period. Relatively shorter follow-up period should be acknowledged as another limitation. In conclusion, our results showed that no level of myopia was associated with glaucoma progression using either the VF or optic disc/rnfl criterion. High myopia was a preventive factor for glaucoma progression when using optic disc/rnfl criteria. This may be interpreted as a lower progression detection rate when using structural criteria that occurs because of a difficulty in detecting changes in the optic disc/ RNFL in highly myopic eyes, or may mean that some highly myopic glaucomatous eyes are not true cases of glaucoma. Acknowledgments Supported by a Grant ( ) from the Asan Medical Center, Seoul, Korea. The authors alone are responsible for the content and writing of the paper. The authors have no proprietary interest or financial involvement in the development or marketing of instruments or equipment mentioned in this article or any competing instruments or pieces of equipment. Disclosure: J.Y. Lee, None; K.R. Sung, None; S. Han, None; J.H. Na, None References 1. Marcus MW, de Vries MM, Junoy Montolio FG, et al. Myopia as a risk factor for open-angle glaucoma: a systematic review and meta-analysis. Ophthalmology. 2011;118: Wong TY, Foster PJ, Hee J, et al. Prevalence and risk factors for refractive errors in adult Chinese in Singapore. Invest Ophthalmol Vis Sci. 2000;41: Chon B, Qiu M, Lin SC. Myopia and glaucoma in the South Korean population. Invest Ophthalmol Vis Sci. 2013;54: Wu SY, Nemesure B, Leske MC. Refractive errors in a black adult population: the Barbados Eye Study. Invest Ophthalmol Vis Sci. 1999;40:
7 Myopia and the Progression of Glaucoma IOVS j March 2015 j Vol. 56 j No. 3 j Mitchell P, Hourihan F, Sandbach J, et al. The relationship between glaucoma and myopia: the Blue Mountains Eye Study. Ophthalmology. 1999;106: Ramakrishnan R, Nirmalan PK, Krishnadas R, et al. Glaucoma in a rural population of southern India: the Aravind comprehensive eye survey. Ophthalmology. 2003;110: Suzuki Y, Iwase A, Araie M, et al. Risk factors for open-angle glaucoma in a Japanese population: the Tajimi Study. Ophthalmology. 2006;113: Xu L, Wang Y, Wang S. High myopia and glaucoma susceptibility the Beijing Eye Study. Ophthalmology. 2007; 114: Bengtsson B, Heijl A. A long-term prospective study of risk factors for glaucomatous visual field loss in patients with ocular hypertension. J Glaucoma. 2005;14: Heijl A, Leske MC, Bengtsson B, et al. Reduction of intraocular pressure and glaucoma progression: results from the Early Manifest Glaucoma Trial. Arch Ophthalmol. 2002;120: Kim YJ, Yun SC, Na JH, et al. Glaucoma progression in eyes with a history of refractive corneal surgery. Invest Ophthalmol Vis Sci. 2012;53: Sohn SW, Song JS, Kee C. Influence of the extent of myopia on the progression of normal-tension glaucoma. Am J Ophthalmol. 2010;149: Chihara E, Liu X, Dong J, et al. Severe myopia as a risk factor for progressive visual field loss in primary open-angle glaucoma. Ophthalmologica. 1997;211: Perdicchi A, Iester M, Scuderi G, et al. Visual field damage and progression in glaucomatous myopic eyes. Eur J Ophthalmol. 2007;17: Doshi A, Kreidl KO, Lombardi L, et al. Nonprogressive glaucomatous cupping and visual field abnormalities in young Chinese males. Ophthalmology. 2007;114: Sakata R, Aihara M, Murata H, et al. Contributing factors for progression of visual field loss in normal-tension glaucoma patients with medical treatment. J Glaucoma. 2013;22: Araie M, Shirato S, Yamazaki Y, et al. Risk factors for progression of normal-tension glaucoma under b-blocker monotherapy. Acta Ophthalmol. 2012;90: Morgan RK. How genetic is school myopia? Prog Retin Eye Res. 2005;24: Pan CW, Ramamurthy D, Saw SM. Worldwide prevalence and risk factors for myopia. Ophthalmic Physiol Opt. 2012;32: Bell GR. Biomechanical considerations of high myopia: part I physiological characteristics. J Am Optom Assoc. 1993;64: Saw SM, Gazzard G, Shih-Yen EC, et al. Myopia and associated pathological complications. Ophthalmic Physiol Opt. 2005; 25: Chen SJ, Lu P, Zhang WF, et al. High myopia as a risk factor in primary open angle glaucoma. Int J Ophthalmol. 2012;5: Kimura Y, Hangai M, Morooka S, et al. Retinal nerve fiber layer defects in highly myopic eyes with early glaucoma. Invest Ophthalmol Vis Sci. 2012;53: Heijl A, Leske MC, Bengtsson B, et al.; EMGT Group. Measuring visual field progression in the Early Manifest Glaucoma Trial. Acta Ophthalmol Scand. 2003;81: Sung KR, Sun JH, Na JH, et al. Progression detection capability of macular thickness in advanced glaucomatous eyes. Ophthalmology. 2012;119: Sung KR, Kim DY, Park SB, Kook MS. Comparison of retinal nerve fiber layer thickness measured by Cirrus HD and Stratus optical coherence tomography. Ophthalmology. 2009;116: Na JH, Sung KR, Lee JR, et al. Detection of glaucomatous progression by spectral-domain optical coherence tomography. Ophthalmology. 2013;120: Lee JH, Jee D, Kwon JW, Lee WK. Prevalence and risk factors for myopia in a rural Korean population. Invest Ophthalmol Vis Sci. 2013;54: Lin LL, Shih YF, Hsiao CK, Chen CJ. Prevalence of myopia in Taiwanese school children: 1983 to Ann Acad Med Singapore. 2004;33: Leung CK, Choi N, Weinreb RN, et al. Retinal nerve fiber layer imaging with spectral-domain optical coherence tomography: pattern of RNFL defects in glaucoma. Ophthalmology. 2010; 117: Kim TW, Kim M, Weinreb RN, et al. Optic disc change with incipient myopia of childhood. Ophthalmology. 2012;119: Chang RT, Singh K. Myopia and glaucoma: diagnostic and therapeutic challenges. Curr Opin Ophthalmol. 2013;24: Leske MC, Heijl A, Hyman L, Bengtsson B, Dong L, Yang Z; EMGT Group. Predictors of long-term progression in the early manifest glaucoma trial. Ophthalmology. 2007;114: Medeiros FA, Alencar LM, Sample PA, et al. The relationship between intraocular pressure reduction and rates of progressive visual field loss in eyes with optic disc hemorrhage. Ophthalmology. 2010;117: Nitta K, Sugiyama K, Higashide T, et al. Does the enlargement of retinal nerve fiber layer defects relate to disc hemorrhage or progressive visual field loss in normal-tension glaucoma? J Glaucoma. 2011;20: Drance S, Anderson DR, Schulzer M; Collaborative Normal- Tension Glaucoma Study Group. Risk factors for progression of visual field abnormalities in normal-tension glaucoma. Am J Ophthalmol. 2001;131: Sung KR. Disc hemorrhage: is that a risk factor or sign of progression? J Glaucoma. 2012;21: Nitta K. Disc hemorrhage is a sign of progression in normaltension glaucoma. J Glaucoma. 2012;21: Sung KR, Lee S, Park SB, et al. Twenty-four hour ocular perfusion pressure fluctuation and risk of normal-tension glaucoma progression. Invest Ophthalmol Vis Sci. 2009;50: Kim CS, Seong GJ, Lee NH, Song KC; Namil Study Group, Korean Glaucoma Society. Prevalence of primary open-angle glaucoma in central South Korea the Namil study. Ophthalmology. 2011;118:
Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach
 ORIGINAL STUDY Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach Joong Won Shin, MD, Kyung Rim Sung, MD, PhD, Jiyun
ORIGINAL STUDY Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach Joong Won Shin, MD, Kyung Rim Sung, MD, PhD, Jiyun
Refractive corneal surgery (RCS) using a laser, such as. Glaucoma Progression in Eyes with a History of Refractive Corneal Surgery.
 Glaucoma Glaucoma Progression in Eyes with a History of Refractive Corneal Surgery Yoon Jeon Kim, 1 Sung-Cheol Yun, 2 Jung Hwa Na, 3 Hung Won Tchah, 1 Jong Jin Jung, 3 and Kyung Rim Sung 1 PURPOSE. To
Glaucoma Glaucoma Progression in Eyes with a History of Refractive Corneal Surgery Yoon Jeon Kim, 1 Sung-Cheol Yun, 2 Jung Hwa Na, 3 Hung Won Tchah, 1 Jong Jin Jung, 3 and Kyung Rim Sung 1 PURPOSE. To
Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography
 Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Jong Chul Han, Da Ye Choi, and Changwon Kee. 1. Introduction
 Ophthalmology Volume 2015, Article ID 641204, 7 pages http://dx.doi.org/10.1155/2015/641204 Clinical Study The Different Characteristics of Cirrus Optical Coherence Tomography between Superior Segmental
Ophthalmology Volume 2015, Article ID 641204, 7 pages http://dx.doi.org/10.1155/2015/641204 Clinical Study The Different Characteristics of Cirrus Optical Coherence Tomography between Superior Segmental
A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT) Retinal Nerve Fiber Layer Measurements Based on Time Domain OCT Measurements
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(5):369-377 http://dx.doi.org/10.3341/kjo.2012.26.5.369 Original Article A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT)
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(5):369-377 http://dx.doi.org/10.3341/kjo.2012.26.5.369 Original Article A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT)
Research Article The Pattern of Retinal Nerve Fiber Layer and Macular Ganglion Cell-Inner Plexiform Layer Thickness Changes in Glaucoma
 Hindawi Ophthalmology Volume 2017, Article ID 78365, 8 pages https://doi.org/10.1155/2017/78365 Research Article The Pattern of Retinal Nerve Fiber Layer and Macular Ganglion Cell-Inner Plexiform Layer
Hindawi Ophthalmology Volume 2017, Article ID 78365, 8 pages https://doi.org/10.1155/2017/78365 Research Article The Pattern of Retinal Nerve Fiber Layer and Macular Ganglion Cell-Inner Plexiform Layer
Noel de Jesus Atienza, MD, MSc and Joseph Anthony Tumbocon, MD
 Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
 Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma.
 Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma. Donald C. Hood 1,2,* and Ali S. Raza 1 1 Department of Psychology, Columbia
Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma. Donald C. Hood 1,2,* and Ali S. Raza 1 1 Department of Psychology, Columbia
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial
 Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience
 Hindawi Ophthalmology Volume 2017, Article ID 2651645, 6 pages https://doi.org/10.1155/2017/2651645 Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience Sang Wook
Hindawi Ophthalmology Volume 2017, Article ID 2651645, 6 pages https://doi.org/10.1155/2017/2651645 Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience Sang Wook
Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements
 Original article Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements Dewang Angmo, 1 Shibal Bhartiya, 1 Sanjay K Mishra,
Original article Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements Dewang Angmo, 1 Shibal Bhartiya, 1 Sanjay K Mishra,
Rates of Abnormal Retinal Nerve Fiber Layer and Ganglion Cell Layer OCT Scans in Healthy Myopic Eyes: Cirrus Versus RTVue
 CLINICAL SCIENCE Rates of Abnormal Retinal Nerve Fiber Layer and Ganglion Cell Layer OCT Scans in Healthy Myopic Eyes: Cirrus Versus RTVue Jean-Claude Mwanza, MD, MPH, PhD; Fouad E. Sayyad, MD; Ahmad A.
CLINICAL SCIENCE Rates of Abnormal Retinal Nerve Fiber Layer and Ganglion Cell Layer OCT Scans in Healthy Myopic Eyes: Cirrus Versus RTVue Jean-Claude Mwanza, MD, MPH, PhD; Fouad E. Sayyad, MD; Ahmad A.
Patterns of Subsequent Progression of Localized Retinal Nerve Fiber Layer Defects on Red-free Fundus Photographs in Normal-tension Glaucoma
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):330-336 http://dx.doi.org/10.3341/kjo.2014.28.4.330 Original Article Patterns of Subsequent Progression of Localized Retinal Nerve Fiber
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):330-336 http://dx.doi.org/10.3341/kjo.2014.28.4.330 Original Article Patterns of Subsequent Progression of Localized Retinal Nerve Fiber
Optical coherence tomography (OCT) is a noninvasive,
 Ability of Stratus OCT to Detect Progressive Retinal Nerve Fiber Layer Atrophy in Glaucoma Eun Ji Lee, 1,2 Tae-Woo Kim, 1,2 Ki Ho Park, 2 Mincheol Seong, 3 Hyunjoong Kim, 4 and Dong Myung Kim 2 PURPOSE.
Ability of Stratus OCT to Detect Progressive Retinal Nerve Fiber Layer Atrophy in Glaucoma Eun Ji Lee, 1,2 Tae-Woo Kim, 1,2 Ki Ho Park, 2 Mincheol Seong, 3 Hyunjoong Kim, 4 and Dong Myung Kim 2 PURPOSE.
Retinal Nerve Fiber Layer Measurement Variability with Spectral Domain Optical Coherence Tomography
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(1):32-38 http://dx.doi.org/10.3341/kjo.2012.26.1.32 Retinal Nerve Fiber Layer Measurement Variability with Spectral Domain Optical Coherence
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(1):32-38 http://dx.doi.org/10.3341/kjo.2012.26.1.32 Retinal Nerve Fiber Layer Measurement Variability with Spectral Domain Optical Coherence
Retinal nerve fiber layer thickness in Indian eyes with optical coherence tomography
 Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Thickness Changes in the Fovea and Peripapillary Retinal Nerve Fiber Layer Depend on the Degree of Myopia
 Thickness Changes in the Fovea and Peripapillary Retinal Nerve Fiber Layer Depend on the Degree of Myopia Sung-Won Choi, MD, Seok-Joon Lee, MD Department of Ophthalmology, Wonju Christian Hospital. Yonsei
Thickness Changes in the Fovea and Peripapillary Retinal Nerve Fiber Layer Depend on the Degree of Myopia Sung-Won Choi, MD, Seok-Joon Lee, MD Department of Ophthalmology, Wonju Christian Hospital. Yonsei
CLINICAL SCIENCES. Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography
 CLINICAL SCIENCES Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography Seong Bae Park, MD; Kyung Rim Sung, MD, PhD; Sung Yong Kang, MD; Kyung Ri Kim, BS;
CLINICAL SCIENCES Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography Seong Bae Park, MD; Kyung Rim Sung, MD, PhD; Sung Yong Kang, MD; Kyung Ri Kim, BS;
Seiji T. Takagi, Yoshiyuki Kita, Asuka Takeyama, and Goji Tomita. 1. Introduction. 2. Subjects and Methods
 Ophthalmology Volume 2011, Article ID 914250, 5 pages doi:10.1155/2011/914250 Clinical Study Macular Retinal Ganglion Cell Complex Thickness and Its Relationship to the Optic Nerve Head Topography in Glaucomatous
Ophthalmology Volume 2011, Article ID 914250, 5 pages doi:10.1155/2011/914250 Clinical Study Macular Retinal Ganglion Cell Complex Thickness and Its Relationship to the Optic Nerve Head Topography in Glaucomatous
OPTOMETRY RESEARCH PAPER
 C L I N I C A L A N D E X P E R I M E N T A L OPTOMETRY RESEARCH PAPER Interocular symmetry of retinal nerve fibre layer thickness in healthy eyes: a spectral-domain optical coherence tomographic study
C L I N I C A L A N D E X P E R I M E N T A L OPTOMETRY RESEARCH PAPER Interocular symmetry of retinal nerve fibre layer thickness in healthy eyes: a spectral-domain optical coherence tomographic study
To assess the glaucoma diagnostic ability of Fourier Domain Optical Coherence Tomography
 American Journal of Engineering Research (AJER) e-issn : 2320-0847 p-issn : 2320-0936 Volume-02, Issue-11, pp-104-110 www.ajer.org Research Paper Open Access To assess the glaucoma diagnostic ability of
American Journal of Engineering Research (AJER) e-issn : 2320-0847 p-issn : 2320-0936 Volume-02, Issue-11, pp-104-110 www.ajer.org Research Paper Open Access To assess the glaucoma diagnostic ability of
Il contributo dell'angio-oct: valutazione integrata della componente nervosa e vascolare della malattia glaucomatosa
 SIMPOSIO G.O.A.L. - LE NUOVE FRONTIERE DIAGNOSTICHE E LE LINEE DI INDIRIZZO AMBULATORIALI DEL GLAUCOMA Coordinatore e moderatore: D. Mazzacane Presidente: L. Rossetti Il contributo dell'angio-oct: valutazione
SIMPOSIO G.O.A.L. - LE NUOVE FRONTIERE DIAGNOSTICHE E LE LINEE DI INDIRIZZO AMBULATORIALI DEL GLAUCOMA Coordinatore e moderatore: D. Mazzacane Presidente: L. Rossetti Il contributo dell'angio-oct: valutazione
Available online at Pelagia Research Library. Advances in Applied Science Research, 2013, 4(6):
 Available online at www.pelagiaresearchlibrary.com Advances in Applied Science Research, 2013, 4(6):201-206 ISSN: 0976-8610 CODEN (USA): AASRFC Comparison of glaucoma diagnostic ability of retinal nerve
Available online at www.pelagiaresearchlibrary.com Advances in Applied Science Research, 2013, 4(6):201-206 ISSN: 0976-8610 CODEN (USA): AASRFC Comparison of glaucoma diagnostic ability of retinal nerve
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
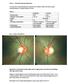 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
 Romanian Journal of Ophthalmology, Volume 60, Issue 3, July-September 2016. pp:158-164 GENERAL ARTICLE Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
Romanian Journal of Ophthalmology, Volume 60, Issue 3, July-September 2016. pp:158-164 GENERAL ARTICLE Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
Differences between Non-arteritic Anterior Ischemic Optic Neuropathy and Open Angle Glaucoma with Altitudinal Visual Field Defect
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
C-reactive Protein and Lipid Profiles in Korean Patients With Normal Tension Glaucoma
 접수번호 : 2008-099 Korean Journal of Ophthalmology 2009;23:193-197 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.193 C-reactive Protein and Lipid Profiles in Korean Patients With Normal Tension Glaucoma Jaewan
접수번호 : 2008-099 Korean Journal of Ophthalmology 2009;23:193-197 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.193 C-reactive Protein and Lipid Profiles in Korean Patients With Normal Tension Glaucoma Jaewan
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
Primary angle closure glaucoma (PACG) is one of the leading
 Glaucoma Comparison of Anterior Segment Parameters Between the Acute Primary Angle Closure Eye and the Fellow Eye Jong Rak Lee, 1 Kyung Rim Sung, 1 and Seungbong Han 2 1 Department of Ophthalmology, University
Glaucoma Comparison of Anterior Segment Parameters Between the Acute Primary Angle Closure Eye and the Fellow Eye Jong Rak Lee, 1 Kyung Rim Sung, 1 and Seungbong Han 2 1 Department of Ophthalmology, University
International Journal of Scientific & Engineering Research, Volume 4, Issue 12, December ISSN
 International Journal of Scientific & Engineering Research, Volume 4, Issue 12, December-2013 108 Name of Chief and Corresponding Author : Dr Chandrima Paul TITLE : Comparison of glaucoma diagnostic ability
International Journal of Scientific & Engineering Research, Volume 4, Issue 12, December-2013 108 Name of Chief and Corresponding Author : Dr Chandrima Paul TITLE : Comparison of glaucoma diagnostic ability
The Role of the RNFL in the Diagnosis of Glaucoma
 Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
21st Century Visual Field Testing
 Supplement to Supported by an educational grant from Carl Zeiss Meditec, Inc. Winter 2011 21st Century Visual Field Testing the Evolution Continues 21st Century Visual Field Testing 21st Century Visual
Supplement to Supported by an educational grant from Carl Zeiss Meditec, Inc. Winter 2011 21st Century Visual Field Testing the Evolution Continues 21st Century Visual Field Testing 21st Century Visual
Assessment of Retinal Nerve Fiber Layer Changes by Cirrus High-definition Optical Coherence Tomography in Myopia
 Divya Singh et al Original REASEARCH 10.5005/jp-journals-10028-1223 Assessment of Retinal Nerve Fiber Layer Changes by Cirrus High-definition Optical Coherence Tomography in Myopia 1 Divya Singh, 2 Sanjay
Divya Singh et al Original REASEARCH 10.5005/jp-journals-10028-1223 Assessment of Retinal Nerve Fiber Layer Changes by Cirrus High-definition Optical Coherence Tomography in Myopia 1 Divya Singh, 2 Sanjay
Relationship Between Structure
 Original Article Relationship Between Structure and Function of the Optic Nerve Head-Glaucoma versus Normal Dr Savita Bhat, Dr Anna Elias, Dr Siddharth Pawar, Dr S.J. Saikumar, Dr Alpesh Rajput, superior,
Original Article Relationship Between Structure and Function of the Optic Nerve Head-Glaucoma versus Normal Dr Savita Bhat, Dr Anna Elias, Dr Siddharth Pawar, Dr S.J. Saikumar, Dr Alpesh Rajput, superior,
Diagnostic Accuracy of OCT with a Normative Database to Detect Diffuse Retinal Nerve Fiber Layer Atrophy: Diffuse Atrophy Imaging Study METHODS
 Glaucoma Diagnostic Accuracy of OCT with a Normative Database to Detect Diffuse Retinal Nerve Fiber Layer Atrophy: Diffuse Atrophy Imaging Study Jin Wook Jeoung, 1,2 Seok Hwan Kim, 1,3 Ki Ho Park, 1,2
Glaucoma Diagnostic Accuracy of OCT with a Normative Database to Detect Diffuse Retinal Nerve Fiber Layer Atrophy: Diffuse Atrophy Imaging Study Jin Wook Jeoung, 1,2 Seok Hwan Kim, 1,3 Ki Ho Park, 1,2
Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India
 Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Glaucoma Clinical Update. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma
 Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
CLINICAL SCIENCES. optic neuropathy characterized
 CLINICAL SCIENCES Spectral-Domain Optical Coherence Tomography for Detection of Localized Retinal Nerve Fiber Layer Defects in Patients With Open-Angle Glaucoma Na Rae Kim, MD; Eun Suk Lee, MD, PhD; Gong
CLINICAL SCIENCES Spectral-Domain Optical Coherence Tomography for Detection of Localized Retinal Nerve Fiber Layer Defects in Patients With Open-Angle Glaucoma Na Rae Kim, MD; Eun Suk Lee, MD, PhD; Gong
Scanning Laser Polarimetry and Optical Coherence Tomography for Detection of Retinal Nerve Fiber Layer Defects
 접수번호 : 2008-105 Korean Journal of Ophthalmology 2009;23:169-175 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.169 Scanning Laser Polarimetry and Optical Coherence Tomography for Detection of Retinal Nerve
접수번호 : 2008-105 Korean Journal of Ophthalmology 2009;23:169-175 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.169 Scanning Laser Polarimetry and Optical Coherence Tomography for Detection of Retinal Nerve
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma. Module 3a GDx
 STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
OtticaFisiopatologica
 Anno quindicesimo dicembre 2010 How to assess the retinal nerve fiber layer thickness Antonio Ferreras Miguel Servet University Hospital, Zaragoza. Aragón Health Sciences Institute University of Zaragoza
Anno quindicesimo dicembre 2010 How to assess the retinal nerve fiber layer thickness Antonio Ferreras Miguel Servet University Hospital, Zaragoza. Aragón Health Sciences Institute University of Zaragoza
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma
 Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Comparison of macular GCIPL and peripapillary RNFL deviation maps for detection of glaucomatous eye with localized RNFL defect
 Comparison of macular GCIPL and peripapillary RNFL deviation maps for detection of glaucomatous eye with localized RNFL defect Mi Jeung Kim, 1,2 Ki Ho Park, 1,2 Beong Wook Yoo, 3 Jin Wook Jeoung, 1,2 Hee
Comparison of macular GCIPL and peripapillary RNFL deviation maps for detection of glaucomatous eye with localized RNFL defect Mi Jeung Kim, 1,2 Ki Ho Park, 1,2 Beong Wook Yoo, 3 Jin Wook Jeoung, 1,2 Hee
Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC)
 Dada T et al Original article Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC) Dada T1, Aggarwal A1, Bali SJ2, Sharma A1, Shah
Dada T et al Original article Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC) Dada T1, Aggarwal A1, Bali SJ2, Sharma A1, Shah
CLINICAL SCIENCES. (FDP) was designed to emphasize the response characteristics of the parasol
 CLINICAL SCIENCES Detecting Visual Function Abnormalities Using the Swedish Interactive Threshold Algorithm and Matrix Perimetry in Eyes With Glaucomatous Appearance of the Optic Disc Lisandro M. Sakata,
CLINICAL SCIENCES Detecting Visual Function Abnormalities Using the Swedish Interactive Threshold Algorithm and Matrix Perimetry in Eyes With Glaucomatous Appearance of the Optic Disc Lisandro M. Sakata,
Glaucoma Diagnosis. Definition of Glaucoma. Diagnosing Glaucoma. Vision Institute Annual Fall Conference
 Glaucoma Diagnosis Vision Institute Annual Fall Conference Mitchell W. Dul, OD, MS, FAAO mdul@sunyopt.edu Richard J. Madonna, MA, OD, FAAO rmadonna@sunyopt.edu Definition of Glaucoma Glaucoma can be regarded
Glaucoma Diagnosis Vision Institute Annual Fall Conference Mitchell W. Dul, OD, MS, FAAO mdul@sunyopt.edu Richard J. Madonna, MA, OD, FAAO rmadonna@sunyopt.edu Definition of Glaucoma Glaucoma can be regarded
Detection of Progressive Retinal Nerve Fiber Layer Loss in Glaucoma Using Scanning Laser Polarimetry with Variable Corneal Compensation
 Detection of Progressive Retinal Nerve Fiber Layer Loss in Glaucoma Using Scanning Laser Polarimetry with Variable Corneal Compensation Felipe A. Medeiros, Luciana M. Alencar, Linda M. Zangwill, Christopher
Detection of Progressive Retinal Nerve Fiber Layer Loss in Glaucoma Using Scanning Laser Polarimetry with Variable Corneal Compensation Felipe A. Medeiros, Luciana M. Alencar, Linda M. Zangwill, Christopher
Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients
 Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients Yoshio Yamazaki, Kenji Mizuki, Fukuko Hayamizu and Chizuru Tanaka Department of Ophthalmology, Nihon
Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients Yoshio Yamazaki, Kenji Mizuki, Fukuko Hayamizu and Chizuru Tanaka Department of Ophthalmology, Nihon
Collaboration in the care of glaucoma patients and glaucoma suspects. Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012
 Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Glaucoma is the leading cause of irreversible blindness
 Glaucoma Characteristics of Optic Disc Morphology in Glaucoma Patients with Parafoveal Scotoma Compared to Peripheral Scotoma Kyoung In Jung, Hae-Young L. Park, and Chan Kee Park PURPOSE. We investigated
Glaucoma Characteristics of Optic Disc Morphology in Glaucoma Patients with Parafoveal Scotoma Compared to Peripheral Scotoma Kyoung In Jung, Hae-Young L. Park, and Chan Kee Park PURPOSE. We investigated
Joon Mo Kim 1, Ki Ho Park 2*, Seon Jeong Kim 2, Hyo Ju Jang 1, Eun Noh 3, Mi Jeung Kim 2, Tae Woo Kim 4, Dong Myung Kim 2 and Joseph Caprioli 5
 Kim et al. BMC Ophthalmology 2013, 13:67 RESEARCH ARTICLE Open Access Comparison of localized retinal nerve fiber layer defects in highly myopic, myopic, and non-myopic patients with normal-tension glaucoma:
Kim et al. BMC Ophthalmology 2013, 13:67 RESEARCH ARTICLE Open Access Comparison of localized retinal nerve fiber layer defects in highly myopic, myopic, and non-myopic patients with normal-tension glaucoma:
Elevated intraocular pressure (IOP) is a major risk factor for
 Glaucoma The Association between Retinal Vessel Diameter and Retinal Nerve Fiber Layer Thickness in Asymmetric Normal Tension Glaucoma Patients Joon Mo Kim, 1 Mo Sae Kim, 2 Hyo Ju Jang, 1 Ki Ho Park, 3
Glaucoma The Association between Retinal Vessel Diameter and Retinal Nerve Fiber Layer Thickness in Asymmetric Normal Tension Glaucoma Patients Joon Mo Kim, 1 Mo Sae Kim, 2 Hyo Ju Jang, 1 Ki Ho Park, 3
Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic Syndrome
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
 Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Clinical and Anterior Segment Anatomical Features in Primary Angle Closure Subgroups Based on Configurations of Iris Root Insertion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(3):206-213 http://dx.doi.org/10.3341/kjo.2016.30.3.206 Original Article Clinical and Anterior Segment Anatomical Features in Primary Angle
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(3):206-213 http://dx.doi.org/10.3341/kjo.2016.30.3.206 Original Article Clinical and Anterior Segment Anatomical Features in Primary Angle
Financial Disclosure. Visual Field Interpretation RELIABILITY VISUAL FIELD INTERPRETATION IN GLAUCOMA METHODS OF DATA PRESENTATION
 VISUAL FIELD INTERPRETATION IN GLAUCOMA Danica J. Marrelli, OD, FAAO University of Houston College of Optometry Financial Disclosure I have received speaking and/or consulting fees from: Aerie Pharmaceutical
VISUAL FIELD INTERPRETATION IN GLAUCOMA Danica J. Marrelli, OD, FAAO University of Houston College of Optometry Financial Disclosure I have received speaking and/or consulting fees from: Aerie Pharmaceutical
MATERIALS AND METHODS
 Glaucoma Analysis of Peripapillary Retinal Nerve Fiber Distribution in Normal Young Adults Seung Woo Hong, 1,2 Myung Douk Ahn, 2 Shin Hee Kang, 1,3 and Seong Kyu Im 1,4 PURPOSE. To determine the anatomic
Glaucoma Analysis of Peripapillary Retinal Nerve Fiber Distribution in Normal Young Adults Seung Woo Hong, 1,2 Myung Douk Ahn, 2 Shin Hee Kang, 1,3 and Seong Kyu Im 1,4 PURPOSE. To determine the anatomic
S Morishita, T Tanabe, S Yu, M Hangai, T Ojima, H Aikawa, N Yoshimura. Clinical science
 Department of Ophthalmology and Visual Sciences, Kyoto University Graduate School of Medicine, Kyoto, Japan Correspondence to: Dr T Tanabe, Department of Ophthalmology, The Tazuke Kofukai Medical Institute,
Department of Ophthalmology and Visual Sciences, Kyoto University Graduate School of Medicine, Kyoto, Japan Correspondence to: Dr T Tanabe, Department of Ophthalmology, The Tazuke Kofukai Medical Institute,
Glaucoma Evaluation. OCT Pearls for Glaucoma. OCT: Retinal Nerve Fiber Layer. Financial Disclosures. OCT: Macula. Case Example
 OCT Pearls for Glaucoma using OCT of the macula for glaucoma Glaucoma Evaluation Right eye Visual Acuity 20/25 20/25 IOP 13 13 Central corneal 530 530 thickness Anterior exam Normal with PCIOL Normal with
OCT Pearls for Glaucoma using OCT of the macula for glaucoma Glaucoma Evaluation Right eye Visual Acuity 20/25 20/25 IOP 13 13 Central corneal 530 530 thickness Anterior exam Normal with PCIOL Normal with
EXPERIMENTAL AND THERAPEUTIC MEDICINE 6: , 2013
 268 Comparison of optic nerve morphology in eyes with glaucoma and eyes with non-arteritic anterior ischemic optic neuropathy by Fourier domain optical coherence tomography YUXIN YANG 1, HAITAO ZHANG 1,
268 Comparison of optic nerve morphology in eyes with glaucoma and eyes with non-arteritic anterior ischemic optic neuropathy by Fourier domain optical coherence tomography YUXIN YANG 1, HAITAO ZHANG 1,
The optic nerve head ONH) is an important anatomic
 Glaucoma Deep Optic Nerve Head Morphology Is Associated With Pattern of Glaucomatous Visual Field Defect in Open-Angle Glaucoma Jong Chul Han, Jae Hwan Choi, Do Young Park, Eun Jung Lee, and Changwon Kee
Glaucoma Deep Optic Nerve Head Morphology Is Associated With Pattern of Glaucomatous Visual Field Defect in Open-Angle Glaucoma Jong Chul Han, Jae Hwan Choi, Do Young Park, Eun Jung Lee, and Changwon Kee
Evaluating Optic Nerve Damage: Pearls and Pitfalls
 54 The Open Ophthalmology Journal, 9, 3, 54-58 Evaluating Optic Nerve Damage: Pearls and Pitfalls Open Access Paul J. Mackenzie * and Frederick S. Mikelberg Division of Glaucoma, Department of Ophthalmology
54 The Open Ophthalmology Journal, 9, 3, 54-58 Evaluating Optic Nerve Damage: Pearls and Pitfalls Open Access Paul J. Mackenzie * and Frederick S. Mikelberg Division of Glaucoma, Department of Ophthalmology
Advances in OCT Murray Fingeret, OD
 Disclosures Advances in OCT Murray Fingeret, OD Consultant Alcon, Allergan, Bausch & Lomb, Carl Zeiss Meditec, Diopsys, Heidelberg Engineering, Reichert, Topcon Currently Approved OCT Devices OCT Devices
Disclosures Advances in OCT Murray Fingeret, OD Consultant Alcon, Allergan, Bausch & Lomb, Carl Zeiss Meditec, Diopsys, Heidelberg Engineering, Reichert, Topcon Currently Approved OCT Devices OCT Devices
Comparison of Retinal Nerve Fiber Layer Thickness between Stratus and Spectralis OCT
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(3):166-173 DOI: 10.3341/kjo.2011.25.3.166 Original Article Comparison of Retinal Nerve Fiber Layer Thickness between Stratus and Spectralis
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(3):166-173 DOI: 10.3341/kjo.2011.25.3.166 Original Article Comparison of Retinal Nerve Fiber Layer Thickness between Stratus and Spectralis
Optical coherence tomography (OCT) is a new noninvasive
 Use of Optical Coherence Tomography to Assess Variations in Macular Retinal Thickness in Myopia Marcus C. C. Lim, 1 Sek-Tien Hoh, 1 Paul J. Foster, 1,2 Tock-Han Lim, 3,4 Sek-Jin Chew, 1 Steve K. L. Seah,
Use of Optical Coherence Tomography to Assess Variations in Macular Retinal Thickness in Myopia Marcus C. C. Lim, 1 Sek-Tien Hoh, 1 Paul J. Foster, 1,2 Tock-Han Lim, 3,4 Sek-Jin Chew, 1 Steve K. L. Seah,
Measurement of Choroidal Thickness in Normal Eyes Using 3D OCT-1000 Spectral Domain Optical Coherence Tomography
 pissn: 111-8942 eissn: 292-9382 Korean J Ophthalmol 212;26(4):255-259 http://dx.doi.org/1.3341/kjo.212.26.4.255 Original Article Measurement of Choroidal Thickness in Normal Eyes Using 3D OCT-1 Spectral
pissn: 111-8942 eissn: 292-9382 Korean J Ophthalmol 212;26(4):255-259 http://dx.doi.org/1.3341/kjo.212.26.4.255 Original Article Measurement of Choroidal Thickness in Normal Eyes Using 3D OCT-1 Spectral
Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID
 Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID Glaucoma is one of the major causes of visual loss worldwide. The philosophy of glaucoma management is to preserve the visual
Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID Glaucoma is one of the major causes of visual loss worldwide. The philosophy of glaucoma management is to preserve the visual
Relationship between the GDx VCC and Stratus OCT in Primary Open Angle Glaucoma
 Relationship between the GDx VCC and Stratus OCT in Primary Open Angle Glaucoma Reza Zarei, MD 1 Mohammad Soleimani, MD 2 Sasan Moghimi, MD 3 Mohammad Yaser Kiarudi, MD 2 Mahmoud Jabbarvand, MD 1 Yadollah
Relationship between the GDx VCC and Stratus OCT in Primary Open Angle Glaucoma Reza Zarei, MD 1 Mohammad Soleimani, MD 2 Sasan Moghimi, MD 3 Mohammad Yaser Kiarudi, MD 2 Mahmoud Jabbarvand, MD 1 Yadollah
FORUM Glaucoma Workplace from ZEISS Clinical Interpretation Guide
 FORUM Glaucoma Workplace from ZEISS Clinical Interpretation Guide ZEISS FORUM Glaucoma Workplace.0 For years, doctors have asked for the operational capability to analyze data from their Humphrey Field
FORUM Glaucoma Workplace from ZEISS Clinical Interpretation Guide ZEISS FORUM Glaucoma Workplace.0 For years, doctors have asked for the operational capability to analyze data from their Humphrey Field
Early detection and control of disease progression or
 Glaucoma Agreement Among Spectral-Domain Optical Coherence Tomography, Standard Automated Perimetry, and Stereophotography in the Detection of Glaucoma Progression Sebastián A. Banegas, 1 Alfonso Antón,
Glaucoma Agreement Among Spectral-Domain Optical Coherence Tomography, Standard Automated Perimetry, and Stereophotography in the Detection of Glaucoma Progression Sebastián A. Banegas, 1 Alfonso Antón,
Present relevant clinical findings of four landmark glaucoma trials OHTS, EMGT, CNTGS and CIGTS.
 Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Characterization of Peripapillary Atrophy Using Spectral Domain Optical Coherence Tomography
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(6):353-359 DOI: 10.3341/kjo.2010.24.6.353 Characterization of Peripapillary trophy Using Spectral Domain Optical Coherence Tomography Original
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(6):353-359 DOI: 10.3341/kjo.2010.24.6.353 Characterization of Peripapillary trophy Using Spectral Domain Optical Coherence Tomography Original
Research Article Repeatability of Perimacular Ganglion Cell Complex Analysis with Spectral-Domain Optical Coherence Tomography
 Ophthalmology Volume 2015, Article ID 605940, 5 pages http://dx.doi.org/10.1155/2015/605940 Research Article Repeatability of Perimacular Ganglion Cell Complex Analysis with Spectral-Domain Optical Coherence
Ophthalmology Volume 2015, Article ID 605940, 5 pages http://dx.doi.org/10.1155/2015/605940 Research Article Repeatability of Perimacular Ganglion Cell Complex Analysis with Spectral-Domain Optical Coherence
Ability of Scanning Laser Polarimetry (GDx) to Discriminate among Early Glaucomatous, Ocular Hypertensive and Normal Eyes in the Korean Population
 Korean J Ophthalmol Vol. 18:1-8, 2004 Ability of Scanning Laser Polarimetry (GDx) to Discriminate among Early Glaucomatous, Ocular Hypertensive and Normal Eyes in the Korean Population Sun Young Lee, MD,
Korean J Ophthalmol Vol. 18:1-8, 2004 Ability of Scanning Laser Polarimetry (GDx) to Discriminate among Early Glaucomatous, Ocular Hypertensive and Normal Eyes in the Korean Population Sun Young Lee, MD,
Snellen VA 2 IOP 3 Ocular Examination * Only dilate if repeat photos required
 Page 1 of 7 Visit Date: Check Completed Modules Page Number Snellen VA 2 IOP 3 Ocular Examination * Only dilate if repeat photos required Humphrey VFs (if required) 5 Disc Photography (if required) 6 OCT
Page 1 of 7 Visit Date: Check Completed Modules Page Number Snellen VA 2 IOP 3 Ocular Examination * Only dilate if repeat photos required Humphrey VFs (if required) 5 Disc Photography (if required) 6 OCT
Ganglion cell complex scan in the early prediction of glaucoma
 Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
R&M Solutions
 Mohamed Hosny El-Bradey, MD., Assistant Professor of Ophthalmology, Tanta University. Wael El Haig, MD., Professor of Ophthalmology. Zagazeeg University. 1 Myopic CNV is considered the most common vision
Mohamed Hosny El-Bradey, MD., Assistant Professor of Ophthalmology, Tanta University. Wael El Haig, MD., Professor of Ophthalmology. Zagazeeg University. 1 Myopic CNV is considered the most common vision
1/25/2019 OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! THE ORIGINAL RAGING GLAUCOMA OCT RETINAL IMAGING OPTIC NERVE HEAD EXAMINATION
 OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com THE ORIGINAL RAGING GLAUCOMA 47-year-old Black
OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com THE ORIGINAL RAGING GLAUCOMA 47-year-old Black
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1
 Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
OCT in the Diagnosis and Follow-up of Glaucoma
 OCT in the Diagnosis and Follow-up of Glaucoma Karim A Raafat MD. Professor Of Ophthalmology Cairo University Hmmmm! Do I have Glaucoma or not?! 1 Visual Function 100% - N Gl Structure : - 5000 axon /
OCT in the Diagnosis and Follow-up of Glaucoma Karim A Raafat MD. Professor Of Ophthalmology Cairo University Hmmmm! Do I have Glaucoma or not?! 1 Visual Function 100% - N Gl Structure : - 5000 axon /
Detection of Glaucoma Using Scanning Laser Polarimetry with Enhanced Corneal Compensation
 Detection of Glaucoma Using Scanning Laser Polarimetry with Enhanced Corneal Compensation Felipe A. Medeiros, Christopher Bowd, Linda M. Zangwill, Chirag Patel, and Robert N. Weinreb From the Hamilton
Detection of Glaucoma Using Scanning Laser Polarimetry with Enhanced Corneal Compensation Felipe A. Medeiros, Christopher Bowd, Linda M. Zangwill, Chirag Patel, and Robert N. Weinreb From the Hamilton
The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
 European Journal of Ophthalmology / Vol. 13 no. 4, 2003 / pp. 377-382 The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
European Journal of Ophthalmology / Vol. 13 no. 4, 2003 / pp. 377-382 The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
Peripapillary Retinal Thickness. Maps in the Evaluation of Glaucoma Patients: A Novel Concept.
 Peripapillary Retinal Thickness Maps in the Evaluation of Glaucoma Patients: A Novel Concept The Harvard community has made this article openly available. Please share how this access benefits you. Your
Peripapillary Retinal Thickness Maps in the Evaluation of Glaucoma Patients: A Novel Concept The Harvard community has made this article openly available. Please share how this access benefits you. Your
Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure Glaucoma
 Original Article DOI 10.3349/ymj.2009.50.2.206 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(2):206-210, 2009 Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure
Original Article DOI 10.3349/ymj.2009.50.2.206 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(2):206-210, 2009 Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure
STANDARD AUTOMATED PERIMETRY IS A GENERALLY
 Comparison of Long-term Variability for Standard and Short-wavelength Automated Perimetry in Stable Glaucoma Patients EYTAN Z. BLUMENTHAL, MD, PAMELA A. SAMPLE, PHD, LINDA ZANGWILL, PHD, ALEXANDER C. LEE,
Comparison of Long-term Variability for Standard and Short-wavelength Automated Perimetry in Stable Glaucoma Patients EYTAN Z. BLUMENTHAL, MD, PAMELA A. SAMPLE, PHD, LINDA ZANGWILL, PHD, ALEXANDER C. LEE,
Influence of cataract on image quality and macular thickness measured using spectral domain optical coherence tomography: a prospective cohort study
 International Journal of Advances in Medicine Lathika VK et al. Int J Adv Med. 2017Apr;4(2):546-550 http://www.ijmedicine.com pissn2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20171058
International Journal of Advances in Medicine Lathika VK et al. Int J Adv Med. 2017Apr;4(2):546-550 http://www.ijmedicine.com pissn2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20171058
Glaucoma at a tertiary referral eye hospital in Nepal
 Original article Glaucoma at a tertiary referral eye hospital in Nepal Paudyal I 1,Thapa S S 1, Paudyal G 2, Gurung R 2, Ruit S 2 1 Nepal Glaucoma Eye Clinic, Tilganga Institute of Ophthalmology, Kathmandu,
Original article Glaucoma at a tertiary referral eye hospital in Nepal Paudyal I 1,Thapa S S 1, Paudyal G 2, Gurung R 2, Ruit S 2 1 Nepal Glaucoma Eye Clinic, Tilganga Institute of Ophthalmology, Kathmandu,
RETINAL NERVE FIBER LAYER
 CLINICAL SCIENCES The Effect of Scan Diameter on Retinal Nerve Fiber Layer Thickness Measurement Using Stratus Optic Coherence Tomography Giacomo Savini, MD; Piero Barboni, MD; Michele Carbonelli, MD;
CLINICAL SCIENCES The Effect of Scan Diameter on Retinal Nerve Fiber Layer Thickness Measurement Using Stratus Optic Coherence Tomography Giacomo Savini, MD; Piero Barboni, MD; Michele Carbonelli, MD;
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD
 New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
도시초등학교 4 학년의굴절이상과안계측치변화
 도시초등학교 4 학년의굴절이상과안계측치변화 1119 1120 Table 1. Comparison of uncorrected visual acuity using logmar between March and December [No. of eyes (%)] March December Difference p-value Total Uncorrected visual acuity
도시초등학교 4 학년의굴절이상과안계측치변화 1119 1120 Table 1. Comparison of uncorrected visual acuity using logmar between March and December [No. of eyes (%)] March December Difference p-value Total Uncorrected visual acuity
Scanning laser polarimetry (SLP) provides real-time, objective
 The Effect of Atypical Birefringence Patterns on Glaucoma Detection Using Scanning Laser Polarimetry with Variable Corneal Compensation Christopher Bowd, Felipe A. Medeiros, Robert N. Weinreb, and Linda
The Effect of Atypical Birefringence Patterns on Glaucoma Detection Using Scanning Laser Polarimetry with Variable Corneal Compensation Christopher Bowd, Felipe A. Medeiros, Robert N. Weinreb, and Linda
Clinical Study Visual Field Loss Morphology in High- and Normal-Tension Glaucoma
 Journal of Ophthalmology Volume 2012, Article ID 327326, 8 pages doi:10.1155/2012/327326 Clinical Study Visual Field Loss Morphology in High- and Normal-Tension Glaucoma Michele Iester, 1, 2 Fabio De Feo,
Journal of Ophthalmology Volume 2012, Article ID 327326, 8 pages doi:10.1155/2012/327326 Clinical Study Visual Field Loss Morphology in High- and Normal-Tension Glaucoma Michele Iester, 1, 2 Fabio De Feo,
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Glaucoma: Diagnostic Modalities
 Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Scanning Laser Tomography to Evaluate Optic Discs of Normal Eyes
 Scanning Laser Tomography to Evaluate Optic Discs of Normal Eyes Hiroshi Nakamura,* Toshine Maeda,* Yasuyuki Suzuki and Yoichi Inoue* *Eye Division of Olympia Medical Clinic, Tokyo, Japan; Department of
Scanning Laser Tomography to Evaluate Optic Discs of Normal Eyes Hiroshi Nakamura,* Toshine Maeda,* Yasuyuki Suzuki and Yoichi Inoue* *Eye Division of Olympia Medical Clinic, Tokyo, Japan; Department of
Central Corneal Thickness and its Association with Ocular Parameters
 Central Corneal Thickness and its Association with Ocular Parameters Authors: An-Fei Li 1,2 Mei-Ju Chen 1,2 Affiliations: 1 Department of Ophthalmology, Taipei Veterans General Hospital 2 National Yang-Ming
Central Corneal Thickness and its Association with Ocular Parameters Authors: An-Fei Li 1,2 Mei-Ju Chen 1,2 Affiliations: 1 Department of Ophthalmology, Taipei Veterans General Hospital 2 National Yang-Ming
