Glaucoma is the leading cause of irreversible blindness
|
|
|
- Magdalene Horton
- 6 years ago
- Views:
Transcription
1 Glaucoma Characteristics of Optic Disc Morphology in Glaucoma Patients with Parafoveal Scotoma Compared to Peripheral Scotoma Kyoung In Jung, Hae-Young L. Park, and Chan Kee Park PURPOSE. We investigated the amount and location of optic nerve head (ONH) abnormal points and the retinal nerve fiber layer (RNFL) thickness with paracentral scotoma compared to peripheral scotoma. METHODS. Totals of 35 normal tension glaucoma (NTG) patients with isolated parafoveal scotoma (PFS) within a 108 radius in one hemifield, and 35 patients with isolated peripheral nasal step (PNS) within the nasal periphery outside 108 of fixation in one hemifield were enrolled if their mean deviation was greater than 10 decibels (db). Global and sector optic disc stereometric parameters obtained by Heidelberg retina tomography and analyzed by Moorfields regression analysis (MRA), and retinal RNFL thickness measured using Cirrus spectral domain-optical coherence tomography were compared between the two groups. The percentages of superior and inferior field defects were evaluated. RESULTS. In PFS, superior field defects (82.9%) were found to be dominant, whereas PNS showed a predominance of inferior field defects (80.0%). The PFS group revealed smaller rim area, more glaucomatous cup shape than the PNS group (P ¼ 0.036, 0.012, respectively). In MRA classification, the percentage outside of normal limits (ONL) was greater in the PFS group (P ¼ 0.006). Compared to the PNS group, the PFS group exhibited more glaucomatous ONH morphology in the temporal and inferotemporal sectors in a sector analysis of optic disc parameters, and had thinner RNFLs in the inferior quadrant, and at 7 and 8 o clock (P ¼ 0.007, 0.003, 0.005, respectively). CONCLUSIONS. In early NTG, paracentral scotoma may be more significant than peripheral scotoma because of narrower optic disc rim and larger cup, especially inferotemporally. (Invest Ophthalmol Vis Sci. 2012;53: ) DOI: / iovs Glaucoma is the leading cause of irreversible blindness worldwide. 1 A wide range of racial variation in the prevalence of normal tension glaucoma (NTG) has been From the Department of Ophthalmology and Visual Science, Seoul St. Mary s Hospital, College of Medicine, The Catholic University of Korea, Seoul, Korea. Presented at a meeting of the European Association for Vision and Eye Research on October 6, Submitted for publication March 25, 2012; revised May 21, 2012; accepted June 9, Disclosure: K.I. Jung, None;H.-Y.L. Park, None;C.K. Park, None Corresponding author: Chan Kee Park, Department of Ophthalmology and Visual Science, Seoul St. Mary s Hospital, College of Medicine, The Catholic University of Korea, Seoul, Korea, 505 Banpo-dong, Seocho-ku, Seoul , Korea: ckpark@catholic.ac.kr. reported. 2 An epidemiologic study in Korea revealed a high prevalence (3.5%) of primary open-angle glaucoma, with a high percentage (77%) of NTG. 3 Many studies have reported that visual field defects are more likely to be deeper, steeper, and closer to fixation in NTG compared to HTG, although no significant difference has been noted in the pattern of visual field defects in a number of reports. 4 9 The characteristics of visual field change in NTG have been reported as the occurrence of dense scotomas close to fixation and often at low levels of total loss, whereas in primary open-angle glaucoma (POAG), similar paracentral scotomas tend to occur in association with more advanced field loss. 6 Recently, it has been reported that NTG patients with parafoveal scotoma have different risk factor profiles; for example, systemic hypotension was higher in patients with parafoveal scotoma compared to those with nasal step. 10 Preserving central vision is of paramount importance in treating glaucoma. A parafoveal visual field defect is significant because patients with central visual disturbance are at risk for losing visual acuity, leading to decreased driving performance The central and paracentral retina is highly populated by ganglion cells. Area of peak ganglion cell density, which averages 35,000 cells/mm 2, are found approximately 1 mm from the foveal center, with a higher concentration of retinal ganglion cells in the central/paracentral retina compared to the periphery. 14 We assumed that glaucoma subjects with isolated paracentral visual field defects may have more structural difference apparent in the optic nerve head (ONH). Therefore, we compared the optic disc parameters measured using confocal scanning laser ophthalmoscopy and the retinal nerve fiber layer (RNFL) thickness profile determined by Cirrus spectral domain-optical coherence tomography (SD-OCT) between subjects with parafoveal scotoma (PFS) and peripheral nasal step (PNS) in early NTG. METHODS Our retrospective observational study protocol was approved by the Institutional Review Board of the Catholic University of Korea, Seoul, Korea. The study design followed the tenets of the Declaration of Helsinki for biomedical research. Eyes with NTG and meeting the eligibility criteria were enrolled consecutively from a database of patients who were examined for glaucoma between March 1, 2009 and December 31, 2009 in the Department of Ophthalmology, Seoul St. Mary s Hospital. Inclusion criteria for all patients were best-corrected visual acuity of 20/40 or better, refractive error of greater than 6 spherical diopters (D) and 2 D cylinder, and transparent ocular medium (nuclear color or opalescence, cortical or posterior subcapsular lens opacity <1) according to the Lens Opacities Classification System III. 15 The inclusion criteria for early NTG were eyes with a normal open angle on gonioscopy, initial Investigative Ophthalmology & Visual Science, July 2012, Vol. 53, No. 8 Copyright 2012 The Association for Research in Vision and Ophthalmology, Inc. 4813
2 4814 Jung et al. IOVS, July 2012, Vol. 53, No. 8 untreated intraocular pressure (IOP) of <21 mm Hg, and the presence of a glaucomatous optic neuropathy (diffuse or focal rim thinning, cupping, notching, hemorrhage, RNFL defect) with a corresponding reproducibly reliable visual field defect coincident with our criteria for PFS or PNS. Subjects with a history of previous intraocular surgery, diseases that may affect the peripapillary area, or systemic disease or medication that may affect visual acuity were excluded. Each patient had undergone comprehensive ophthalmic examinations, including a best corrected visual acuity test, slit-lamp biomicroscopy, IOP measurement by Goldmann applanation tonometry, gonioscopy, central corneal thickness (CCT) measurements using ultrasonic pachymetry (SP-3000; Tomey Corp., Nagoya, Japan), and dilated funduscopic examination. Stereoscopic optic disc photography and monoscopic red-free digital fundus photography (Canon Cf-60 UW with Canon EOS D-6 CCD camera; Canon, Tokyo, Japan) were performed. Patients were re-examined usually at 6- to 12-month intervals; the same tests were performed with the exception of CCT measurements. Data regarding age at the time of study entry, visual acuity, maximum known untreated IOP from records, spherical equivalent, and disc hemorrhage detection during follow-up were collected. Confocal Scanning Laser Ophthalmoscopy Topographic analysis of the ONH was performed by confocal scanning laser ophthalmoscopy using a Heidelberg Retina Tomograph II (HRT II; Heidelberg Engineering, Heidelberg, Germany). The spherical equivalent refractive error of each eye was adjusted in the dioptric ring of the HRT. The topographic images were obtained through dilated pupils and were analyzed using Advanced Glaucoma Analysis 3.0 software (HRT II; Heidelberg Engineering). All scans were required to have an intrascan SD of <30 lm. In cases of poor centration (more than onequarter of the disc outside the target circle), the scans were excluded from the study. The margin of the optic disc was traced manually by experienced users while viewing the stereo photographs under a stereoscopic viewer, and the inner edge of Elschnig s ring was defined with at least a four-point contour line. This was reviewed by a glaucoma specialist (CKP) who was blinded to patient identity and clinical history. The HRT II software displays several windows in which the topographic results are detailed. Eleven global optic disc stereometric parameters (disc area, cup area, rim area, cup/disc area ratio, rim/disc area ratio, cup volume, rim volume, mean cup depth, maximum cup depth, height variation contour, and cup shape measure) and six sector parameters were obtained with the HRT. Following the convention of measuring angles around the ONH, temporal was defined as 08, superior as 908, nasal as 1808, and inferior as 2708 (regardless of whether a left or right eye was analyzed). Therefore, the angles increased clockwise for right eyes and counterclockwise for left eyes. The ONH was then divided into six sectors: temporal (T) with angular extension from 458 to þ458, temporal-superior (TS) from þ458 to þ908, temporal-inferior (TI) from þ2708 to þ3158, nasal (N) from þ1358 to þ2258, nasal-superior (NS) from þ908 to þ1358, and nasal-inferior (NI) from þ2258 to þ The global and six sector (T, TS, TI, N, NS, and NI) ONH classifications also were obtained by Moorfields regression analysis (MRA). ONHs were classified as outside of normal limits (ONL) when a parameter was outside of the 99.9% confidence interval (CI), borderline when a parameter was between the 95% and 99.9% CIs, and within normal limits (WNL) when a parameter was within the 95% CI. These classifications were made for the entire optic disc considering the global rim area, and for each separate sector considering the rim area of the relative segment. Optical Coherence Tomography (OCT) Scanning The Cirrus SD-OCT (software version ; Carl Zeiss Meditec, Dublin, CA) uses the spectral domain technology of an optic disc cube obtained from a three-dimensional dataset composed of 200 A-scans from each of 200 B-scans. The software determines automatically the center of the disc and then extracts a circumpapillary circle (radius 1.73 mm) from the cube data set for RNFL thickness measurements. All subjects were measured through dilated pupils, using the Optic Disc Cube program (Carl Zeiss Meditec). Poor-quality scans were defined as those with a signal strength of <6, the presence of overt misalignment of the surface detection algorithm on 15% of consecutive A-scans or 20% of cumulative A-scans, or overt decentration of the measurement circle location as assessed subjectively. These were excluded. The RNFL thickness parameters evaluated in our study were temporal, superior, nasal, and inferior quadrant thicknesses, and thicknesses for all of the 12 clock-hour positions, with the 9 o clock (3 o clock for left eyes) position being temporal, 12 o clock position being superior, 3 o clock position being nasal, and 6 o clock position being inferior. Visual Field Testing Standard automated perimetry (SAP) was performed with a Humphrey field analyzer (Carl Zeiss Meditec), applying the Swedish interactive threshold algorithm (SITA) standard and program 24-2 test. Optical lens correction was placed in front of the tested eye, while the other eye was occluded with a patch. A reliable test was defined as <30% fixation losses, false-positives or false-negatives. When the test results did not meet the reliability criteria, the test was repeated. The visual field indices, expressed as mean deviation (MD) and pattern standard deviation (PSD), and the visual field index (VFI) from SAP were evaluated. All ophthalmic examinations, two consecutive perimetry tests performed on different days, and all topographic analyses were performed within 1 month from the subject s date of enrollment. Visual Field Criteria for PFS and PNS One experienced glaucoma specialist divided the patients into two groups based on pattern deviation probability plots. The PFS group included patients with isolated PFS within 12 points of a central 108 radius in one hemifield on the SITA 24-2 test (Fig. 1). The PNS group included those with isolated PNS within the nasal periphery outside 108 of fixation in one hemifield. Criteria for a PFS or PNS visual field defect were the presence of three or more points with a P value of <5%, one of which had a P value of <1%, among 12 points in each group on the pattern deviation plot. Patients with visual field defects in the central 108 and peripheral nasal visual fields, with visual field defects other than the central or nasal peripheral fields, or with visual field defects in the superior and inferior hemifields were excluded. When both eyes fulfilled the inclusion criteria, one eye per subject was chosen randomly for the study. Statistical Analysis Statistical analyses were performed with SPSS software (ver. 17.0; SPSS, Chicago, IL). Differences between the two groups were assessed by Student s t-test for continuous parameters and the v 2 test for numeric parameters. Each group was divided into superior and inferior field defect groups, and the percentage of these groups were compared between the PFS and PNS groups by the v 2 test. Global and sector optic disc stereometric parameters were compared between the two groups by Student s t-test. Global and sector MRA classification was compared between the two groups by the v 2 test. We considered this study as an exploratory analysis. Therefore, we did not adjust P value to control overall significance level to 5% in all statistical tests. RESULTS There was little difference in age, sex, IOP, visual acuity, or disc hemorrhage between the two groups (P ¼ 0.497, 0.236, 0.187,
3 IOVS, July 2012, Vol. 53, No. 8 Optic Disc Morphology in Parafoveal Scotoma 4815 Comparison of Topographic Optic Disc Parameters and MRA Classification between the PFS and PNS Groups Rim area measured using HRT was smaller in the PFS group than in the PNS group (P ¼ 0.036). Compared to the PNS group, the PFS group displayed more positive values for cup shape measurements (P ¼ 0.012, Table 2). There was a tendency that the cup/disc area ratio and cup volume was higher, and rim/disc area ratio was lower in the PFS group compared to the PNS group (P ¼ 0.052, 0.052, and 0.079, respectively). In the sector analysis of optic disc parameters, the cup area, rim area, cup/disc area ratio, rim/disc area ratio, cup volume, rim volume, and height variation contour revealed more glaucomatous ONH morphology in the temporal and inferotemporal quadrants in the PFS group compared to the PNS group, but there were no great differences in the other quadrants (Table 3). In terms of MRA classification, the percentage ONL was greater in the PFS group (85.7%) than in the PNS group (51.4%, P ¼ 0.006, Table 4). The PFS group also showed a greater percentage ONL (74.3%) compared to the PNS group (34.3%, P ¼ 0.003) in the temporal-inferior MRA classification. FIGURE 1. Pattern deviation plot divided into two subfields of the Humphrey visual field. The parafoveal scotoma group includes abnormal points within 12 points of a central 108 radius (dashed-line). The peripheral nasal step group has abnormal points within 12 nasal peripheral points (dotted-line) in one hemifield , and 0.617, respectively; Table 1). Spherical equivalent tended to be more myopic in the PFS group ( D) than in the PNS group ( D, P ¼ 0.035). Comparison of Visual Field Features between the PFS and PNS Groups Both groups had similar MD and PSD (MD P ¼ and PSD P ¼ 0.248, Table 1). VFI was 89.47% in the PFS group and 93.2% in the PNS group. Superior field defects were dominant (82.9%) in the PFS group, whereas inferior field defects were dominant (80.0%) in the PNS group (Fig. 2). Comparison of RNFL Thickness between the PFS and PNS Groups The RNFL thickness measurements are shown in Table 5 and Figure 3. The 3608 average RNFL showed no great difference between the PFS ( lm) and the PNS ( lm, P ¼ 0.625) groups. The inferior quadrant RNFL was thinner in the PFS group (P ¼ 0.007), while the superior quadrant RNFL was thinner in the PNS group (P ¼ 0.006). The RNFL thicknesses in the 7 and 8 o clock sectors were less in the PFS group (P ¼ and 0.005, respectively), and the RNFL thickness in the 11 o clock sector was less in the PNS group (P ¼ 0.008). DISCUSSION In our study, paracentral scotomas were associated with marked ONH abnormality in locations important for reading and seeing detail in glaucomatous optic neuropathy. A VFI that places greater weight on the location in the paracentral visual TABLE 1. Characteristics of Patients with Parafoveal Scotoma (PFS) and Peripheral Nasal Step (PNS) Parameter PFS Group (N ¼ 35) PNS Group (N ¼ 35) P Value* Age (y) Male/Female 14/21 18/ Right/left laterality 15/20 14/ Maximum untreated IOP (mm Hg) CCT (lm) Visual acuity (logmar) Spherical equivalent (D) Mean deviation (db) PSD (db) Visual field index 89.47% 93.26% Disc hemorrhage 7 (20.0) 7 (20.0) Follow-up period (mo) Interval between visits (mo) Continuous variables are expressed as N (percentage), mean 6 SD, or percentage. * Statistically significant differences between the PFS and PNS groups (P < 0.05) by Student s t-test for continuous variables or v 2 test for categorical data are indicated in bold.
4 4816 Jung et al. IOVS, July 2012, Vol. 53, No. 8 FIGURE 2. The parafoveal scotoma group showed a predominance of superior field defects (82.9%), whereas the peripheral nasal step group had a higher percentage of inferior field defects (80.0%). TABLE 2. Heidelberg Retina Tomography Parameters of Global and Sector (T, N) Parameters in the PFS and PNS Groups Parameter PFS Group (N ¼ 35) PNS Group (N ¼ 35) P Value* Global Disc area (mm 2 ) Cup area (mm 2 ) Rim area (mm 2 ) Cup/disc area ratio Rim/disc area ratio Cup volume (mm 3 ) Rim volume (mm 3 ) Mean cup depth (mm) Maximum cup depth (mm) Height variation contour Cup shape measure Temporal Disc area (mm 2 ) Cup area (mm 2 ) Rim area (mm 2 ) Cup/disc area ratio Rim/disc area ratio Cup volume (mm 3 ) Rim volume (mm 3 ) Mean cup depth (mm) Maximum cup depth (mm) Height variation contour Cup shape measure Nasal Disc area (mm 2 ) Cup area (mm 2 ) Rim area (mm 2 ) Cup/disc area ratio Rim/disc area ratio Cup volume (mm 3 ) Rim volume (mm 3 ) Mean cup depth (mm) Maximum cup depth (mm) Height variation contour Cup shape measure Continuous variables are expressed as mean 6 SD. * Statistically significant differences between the PFS and PNS groups (P < 0.05) by Student s t-test are indicated in bold.
5 IOVS, July 2012, Vol. 53, No. 8 Optic Disc Morphology in Parafoveal Scotoma 4817 TABLE 3. Heidelberg Retina Tomography Optic Disc Sector Stereometric Parameters (TS, TI, NS, NI sectors) in the PFS and PNS Groups Sector Optic Disc Stereometric Parameters PFS Group (N ¼ 35) PNS Group (N ¼ 35) P Value* Sector Optic Disc Stereometric Parameters PFS Group (N ¼ 35) PNS Group (N ¼ 35) P Value* Temporalsuperior sector Temporalinferior sector Disc area (mm 2 ) Nasalsuperior Disc area (mm 2 ) Cup area (mm 2 ) Cup area (mm 2 ) Rim area (mm 2 ) sector Rim area (mm 2 ) Cup/disc area ratio Cup/disc area ratio Rim/disc area ratio Rim/disc area ratio Cup volume (mm 3 ) Cup volume (mm 3 ) Rim volume (mm 3 ) Rim volume (mm 3 ) Mean cup depth (mm) Mean cup depth (mm) Maximum cup depth (mm) Maximum cup depth (mm) Height variation contour Height variation contour Cup shape measure Cup shape measure Disc area (mm 2 ) Nasalinferior Disc area (mm 2 ) Cup area (mm 2 ) Cup area (mm 2 ) Rim area (mm 2 ) sector Rim area (mm 2 ) Cup/disc area ratio Cup/disc area ratio Rim/disc area ratio Rim/disc area ratio Cup volume (mm 3 ) Cup volume (mm 3 ) Rim volume (mm 3 ) Rim volume (mm 3 ) Mean cup depth (mm) Mean cup depth (mm) Maximum cup depth (mm) Maximum cup depth (mm) Height variation contour Height variation contour Cup shape measure Cup shape measure * Statistically significant differences between the PFS and PNS groups (P < 0.05) by Student s t-test are indicated in bold.
6 4818 Jung et al. IOVS, July 2012, Vol. 53, No. 8 TABLE 4. MRA of HRT: Global and Sector Analysis in the PFS and PNS Groups Sector Analysis MRA Classification PFS Group (N ¼ 35) PNS Group (N ¼ 35) P Value* Global WNL 3 (8.6%) 6 (17.1%) Borderline 2 (5.7%) 11 (31.4%) ONL 30 (85.7%) 18 (51.4%) Temporal WNL 18 (51.4%) 22 (62.9%) Borderline 7 (20.0%) 8 (22.9%) ONL 10 (28.6%) 5 (14.3%) Temporal-superior WNL 15 (42.9%) 18 (51.4%) Borderline 8 (22.9%) 6 (17.1%) ONL 12 (34.3%) 11 (31.4%) Temporal-inferior WNL 7 (20.0%) 16 (45.7%) Borderline 2 (5.7%) 7 (20.0%) ONL 26 (74.3%) 12 (34.3%) Nasal WNL 15 (42.9%) 22 (62.9%) Borderline 6 (17.1%) 7 (20.0%) ONL 14 (40.0%) 6 (17.1%) Nasal-superior WNL 16 (45.7%) 18 (51.4%) Borderline 7 (20.0%) 11 (31.4%) ONL 12 (34.3%) 6 (17.1%) Nasal-inferior WNL 13 (37.1%) 18 (51.4%) Borderline 8 (22.9%) 7 (20.0%) ONL 14 (40.0%) 10 (28.6%) * Statistically significant differences between the PFS and PNS groups (P < 0.05) by the v 2 test are indicated in bold. field arguably gives a more appropriate indication of small, but clinically important, losses in this area. The VFI clearly was lower in the PFS group than in the PNS group (P ¼ 0.008). Therefore, the PFS is located critically, although a paracentral scotoma does not necessarily mean a loss of functional vision. The most important finding of our study was the narrower optic disc rim and the larger cup, on a quantitative basis, in eyes with paracentral scotoma compared to peripheral scotoma. Before initiating the study, we predicted that given the large number of ganglion cells in the central and paracentral retina, subjects with PFS would have more glaucomatous optic disc morphology compared to subjects with PNS. 14 We observed the difference in global and sector optic disc parameters, and local RNFL thickness between eyes with PFS and eyes with PNS. The narrower neural rim and larger cup of the ONH in the PFS group compared to the PNS group also may be explained by the ratio of human midget to parasol ganglion cells, which changes from approximately 30:1 in the central retina to approximately 3:1 in the retinal periphery. 16 Midget ganglion cells, which are predominant in the central retina, generally are known to have very small receptive fields. 17 Even though one report suggests that the receptive field size shows no big difference between midget and parasol ganglion cells, receptive field radii become larger as the degree of eccentricity from fixation increases in small and large ganglion cells. 18 Therefore, glaucoma with PFS may involve a greater number of damaged ganglion cells than with PNS, at a similar level of visual field defect. The PFS group showed no big difference in average peripapillary RNFL thickness compared to the PNS group (P ¼ 0.625). We speculate that this may be related to the inconsistency of the mean axon diameter along the intraretinal axon length. Ganglion cell axon diameters increase by 20 40% over the first lm from the soma and then decrease with increasing distance from the soma. 19 Furthermore, the mean axon diameter at a location 50 lm from the soma was smaller in midget ganglion cells than in parasol ganglion cells, and it was similar between parasol and midget ganglion cells, within lm, closer to the optic disc. 19 Therefore, a marked loss of ganglion cells in the optic disc with PFS may not affect the RNFL thickness prominently because of the smaller mean axon diameter. Histologic studies investigating the distribution and function of ganglion cells in the human retina are required to determine the reasons for the structural differences in optic discs between the PFS and PNS groups. The PFS group revealed a predominance of superior field defects, which is in agreement with previous study results, and the frequent involvement of the superior hemifield our patients with PFS is consistent with previous reports. In one study, 10 of 11 eyes with arcuate glaucomatous visual field defects confined largely to the macula showed superior hemifield defects. 10 Another study found initial PFS predominantly in the superior hemifield. 10,20 However, to our TABLE 5. RNFL Thickness Measured Using HD-OCT in the PFS Group and PNS Groups Parameter PFS Group (N ¼ 35) PNS Group (N ¼ 35) P Value* Average thickness Superior thickness Nasal thickness Inferior thickness Temporal thickness Values are expressed in lm as mean 6 SD. * Statistically significant differences between the PFS and PNS groups (P < 0.05) by Student s t-test are indicated in bold.
7 IOVS, July 2012, Vol. 53, No. 8 Optic Disc Morphology in Parafoveal Scotoma 4819 FIGURE 3. The global and six sector (T, TS, TI, N, NS, and NI) classifications of the optic nerve head by MRA. Left: the eye with superior parafoveal scotoma was classified as outside normal limits by MRA. Sector analysis showed the TI sector to be outside normal limits and the T sector to be borderline. Right: the eye with inferior peripheral nasal step was classified as within normal limits by global and sector analyses of MRA. knowledge no studies have investigated the structural characteristics of ONH or the RNFL thickness to explain the superior dominance of visual field defects in PFS. Intriguingly, compared to the PNS group in our study, the PFS group showed generally smaller rim area and more glaucomatous cup shape in ONH parameters, as well as more glaucomatous ONH morphology in the TI sector, corresponding to superior hemifield defects. In addition, the PFS group had a thinner RNFL in the temporal sector, and in the 7 and 8 o clock sectors, compared to the PNS group. This may explain, at least in part, the predominance of superior visual field defects in the PFS group. Global and TI sector MRA classifications indicated more abnormal optic disc shape in the PFS group compared to the PNS group, with a comparable MD and higher PSD. Figure 4 illustrates representative cases: an eye (MD 1.68 decibels [db], PSD 2.05 db) with PFS classified as ONL by MRA, and another eye (MD 2.21 db, PSD 7.12 db) with PNS classified as WNL in global and sector MRA. The optic disc was more analogous to normal ONH form in eyes with PNS compared to PFS; thus, the MRA algorithm did not reveal optic disc abnormality in early NTG patients with PNS. In our study, we excluded patients with highly myopic eyes, as this condition frequently is associated with a tilted disc and peripapillary atrophy, which could have confounding effects on the optic disc analysis. Our result of a more myopic tendency in PFS differs from a previous finding of no significant difference in refractive error between PFS and PNS. 10 However, that study included highly myopic eyes, and the PNS group comprised only 15 patients. Limitations of our current study include its retrospective design and the relatively small number of patients. Nevertheless, we tried to elucidate the characteristics of glaucoma with PFS because to our knowledge there have been no reports comparing structural difference of ONH between PFS and PNS. Parafoveal visual field defects are important in the aspect of their location functionally because they have a greater influence on visual acuity and reading compared to peripheral visual field defects Therefore, fundamental information about the structural features of the ONH and RNFL in PFS is valuable. We tried to make as thorough an investigation of the diagnosis of glaucoma in the PFS group as possible to exclude other optic neuropathy or retinal disease that could cause central scotoma. To avoid the diagnostic bias in patients with FIGURE 4. Comparison of the RNFL thickness between the parafoveal scotoma and peripheral nasal step groups. The thicknesses at the 7, 8, and 11 o clock positions differed between the two groups (P < 0.05, by Student s t-test).
8 4820 Jung et al. IOVS, July 2012, Vol. 53, No. 8 parafoveal scotoma, we confirmed that there was no eye with decreased visual acuity and retinal diseases through fundus examination. In summary, patients with PFS, even in the early stage of NTG, appear to have more structural abnormality in the optic disc, especially in the TI sector, with thinner RNFL in the inferior quadrant. Therefore, the optic disc should be examined carefully in patients with PFS. Further studies will focus on the pattern of progression in the optic disc and visual field. References 1. Resnikoff S, Pascolini D, Etyáale D, et al. Global data on visual impairment in the year Bull World Health Organ. 2004; 82: Shields MB. Normal-tension glaucoma: is it different from primary open-angle glaucoma? Curr Opin Ophthalmol. 2008; 19: Kim CS, Seong GJ, Lee NH, Song KC. Prevalence of primary open-angle glaucoma in central South Korea the Namil study. Ophthalmology. 2011;118: Araie M. Pattern of visual field defects in normal-tension and high-tension glaucoma. Curr Opin Ophthalmol. 1995;6: Araie M, Yamagami J, Suziki Y. Visual field defects in normaltension and high-tension glaucoma. Ophthalmology. 1993; 100: Caprioli J, Spaeth GL. Comparison of visual field defects in the low-tension glaucomas with those in the high-tension glaucomas. Am J Ophthalmol. 1984;97: Chauhan BC, Drance SM, Douglas GR, Johnson CA. Visual field damage in normal-tension and high-tension glaucoma. Am J Ophthalmol. 1989;108: Hitchings RA, Anderton SA. A comparative study of visual field defects seen in patients with low-tension glaucoma and chronic simple glaucoma. Br J Ophthalmol. 1983;67: Thonginnetra O, Greenstein VC, Chu D, Liebmann JM, Ritch R, Hood DC. Normal versus high tension glaucoma: a comparison of functional and structural defects. J Glaucoma. 2010;19: Park SC, De Moraes CG, Teng CC, Tello C, Liebmann JM, Ritch R. Initial parafoveal versus peripheral scotomas in glaucoma: risk factors and visual field characteristics. Ophthalmology. 2011;118: Coeckelbergh TR, Brouwer WH, Cornelissen FW, Van Wolffelaar P, Kooijman AC. The effect of visual field defects on driving performance: a driving simulator study. Arch Ophthalmol. 2002;120: Fujita K, Yasuda N, Oda K, Yuzawa M. Reading performance in patients with central visual field disturbance due to glaucoma. Nippon Ganka Gakkai Zasshi. 2006;110: Kolker AE. Visual prognosis in advanced glaucoma: a comparison of medical and surgical therapy for retention of vision in 101 eyes with advanced glaucoma. Trans Am Ophthalmol Soc. 1977;75: Curcio CA, Allen KA. Topography of ganglion cells in human retina. J Comp Neurol. 1990;300: Iester M, Perdicchi A, Capris E, Siniscalco A, Calabria G, Recupero SM. Comparison between discriminant analysis models and glaucoma probability score for the detection of glaucomatous optic nerve head changes. J Glaucoma. 2008;17: Dacey DM, Petersen MR. Dendritic field size and morphology of midget and parasol ganglion cells of the human retina. Proc Natl Acad Sci U S A. 1992;89: De Monasterio FM, Gouras P. Functional properties of ganglion cells of the rhesus monkey retina. J Physiol. 1975;251: Lee BB. Paths to colour in the retina. Clin Exp Optom. 2004; 87: Walsh N, Fitzgibbon T, Ghosh KK. Intraretinal axon diameter: a single cell analysis in the marmoset (Callithrix jacchus). J Neurocytol. 1999;28: Hood DC, Raza AS, de Moraes CG, et al. Initial arcuate defects within the central 10 degrees in glaucoma. Invest Ophthalmol Vis Sci. 2011;52:
Research Article The Pattern of Retinal Nerve Fiber Layer and Macular Ganglion Cell-Inner Plexiform Layer Thickness Changes in Glaucoma
 Hindawi Ophthalmology Volume 2017, Article ID 78365, 8 pages https://doi.org/10.1155/2017/78365 Research Article The Pattern of Retinal Nerve Fiber Layer and Macular Ganglion Cell-Inner Plexiform Layer
Hindawi Ophthalmology Volume 2017, Article ID 78365, 8 pages https://doi.org/10.1155/2017/78365 Research Article The Pattern of Retinal Nerve Fiber Layer and Macular Ganglion Cell-Inner Plexiform Layer
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma
 Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma.
 Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma. Donald C. Hood 1,2,* and Ali S. Raza 1 1 Department of Psychology, Columbia
Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma. Donald C. Hood 1,2,* and Ali S. Raza 1 1 Department of Psychology, Columbia
Noel de Jesus Atienza, MD, MSc and Joseph Anthony Tumbocon, MD
 Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
 Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients
 Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients Yoshio Yamazaki, Kenji Mizuki, Fukuko Hayamizu and Chizuru Tanaka Department of Ophthalmology, Nihon
Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients Yoshio Yamazaki, Kenji Mizuki, Fukuko Hayamizu and Chizuru Tanaka Department of Ophthalmology, Nihon
Seiji T. Takagi, Yoshiyuki Kita, Asuka Takeyama, and Goji Tomita. 1. Introduction. 2. Subjects and Methods
 Ophthalmology Volume 2011, Article ID 914250, 5 pages doi:10.1155/2011/914250 Clinical Study Macular Retinal Ganglion Cell Complex Thickness and Its Relationship to the Optic Nerve Head Topography in Glaucomatous
Ophthalmology Volume 2011, Article ID 914250, 5 pages doi:10.1155/2011/914250 Clinical Study Macular Retinal Ganglion Cell Complex Thickness and Its Relationship to the Optic Nerve Head Topography in Glaucomatous
Clinical Study Visual Field Loss Morphology in High- and Normal-Tension Glaucoma
 Journal of Ophthalmology Volume 2012, Article ID 327326, 8 pages doi:10.1155/2012/327326 Clinical Study Visual Field Loss Morphology in High- and Normal-Tension Glaucoma Michele Iester, 1, 2 Fabio De Feo,
Journal of Ophthalmology Volume 2012, Article ID 327326, 8 pages doi:10.1155/2012/327326 Clinical Study Visual Field Loss Morphology in High- and Normal-Tension Glaucoma Michele Iester, 1, 2 Fabio De Feo,
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Structural examina.on: Imaging
 ManaMa: Glaucoma Structural examina.on: Imaging Luís Abegão Pinto, MD, PhD Department of Ophthalmology CHLC Lisbon Faculty of Medicine, Lisbon University 1 11-10- 2013 Structural changes Qualitative changes
ManaMa: Glaucoma Structural examina.on: Imaging Luís Abegão Pinto, MD, PhD Department of Ophthalmology CHLC Lisbon Faculty of Medicine, Lisbon University 1 11-10- 2013 Structural changes Qualitative changes
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
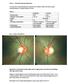 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Differences between Non-arteritic Anterior Ischemic Optic Neuropathy and Open Angle Glaucoma with Altitudinal Visual Field Defect
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
Retinal nerve fiber layer thickness in Indian eyes with optical coherence tomography
 Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Ganglion cell complex scan in the early prediction of glaucoma
 Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
OCT in the Diagnosis and Follow-up of Glaucoma
 OCT in the Diagnosis and Follow-up of Glaucoma Karim A Raafat MD. Professor Of Ophthalmology Cairo University Hmmmm! Do I have Glaucoma or not?! 1 Visual Function 100% - N Gl Structure : - 5000 axon /
OCT in the Diagnosis and Follow-up of Glaucoma Karim A Raafat MD. Professor Of Ophthalmology Cairo University Hmmmm! Do I have Glaucoma or not?! 1 Visual Function 100% - N Gl Structure : - 5000 axon /
Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography
 Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Jong Chul Han, Da Ye Choi, and Changwon Kee. 1. Introduction
 Ophthalmology Volume 2015, Article ID 641204, 7 pages http://dx.doi.org/10.1155/2015/641204 Clinical Study The Different Characteristics of Cirrus Optical Coherence Tomography between Superior Segmental
Ophthalmology Volume 2015, Article ID 641204, 7 pages http://dx.doi.org/10.1155/2015/641204 Clinical Study The Different Characteristics of Cirrus Optical Coherence Tomography between Superior Segmental
Diagnostic Accuracy of OCT with a Normative Database to Detect Diffuse Retinal Nerve Fiber Layer Atrophy: Diffuse Atrophy Imaging Study METHODS
 Glaucoma Diagnostic Accuracy of OCT with a Normative Database to Detect Diffuse Retinal Nerve Fiber Layer Atrophy: Diffuse Atrophy Imaging Study Jin Wook Jeoung, 1,2 Seok Hwan Kim, 1,3 Ki Ho Park, 1,2
Glaucoma Diagnostic Accuracy of OCT with a Normative Database to Detect Diffuse Retinal Nerve Fiber Layer Atrophy: Diffuse Atrophy Imaging Study Jin Wook Jeoung, 1,2 Seok Hwan Kim, 1,3 Ki Ho Park, 1,2
Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements
 Original article Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements Dewang Angmo, 1 Shibal Bhartiya, 1 Sanjay K Mishra,
Original article Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements Dewang Angmo, 1 Shibal Bhartiya, 1 Sanjay K Mishra,
Comparison of Retinal Nerve Fiber Layer Thickness between Stratus and Spectralis OCT
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(3):166-173 DOI: 10.3341/kjo.2011.25.3.166 Original Article Comparison of Retinal Nerve Fiber Layer Thickness between Stratus and Spectralis
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(3):166-173 DOI: 10.3341/kjo.2011.25.3.166 Original Article Comparison of Retinal Nerve Fiber Layer Thickness between Stratus and Spectralis
Optical coherence tomography (OCT) is a noninvasive,
 Ability of Stratus OCT to Detect Progressive Retinal Nerve Fiber Layer Atrophy in Glaucoma Eun Ji Lee, 1,2 Tae-Woo Kim, 1,2 Ki Ho Park, 2 Mincheol Seong, 3 Hyunjoong Kim, 4 and Dong Myung Kim 2 PURPOSE.
Ability of Stratus OCT to Detect Progressive Retinal Nerve Fiber Layer Atrophy in Glaucoma Eun Ji Lee, 1,2 Tae-Woo Kim, 1,2 Ki Ho Park, 2 Mincheol Seong, 3 Hyunjoong Kim, 4 and Dong Myung Kim 2 PURPOSE.
Relationship Between Structure
 Original Article Relationship Between Structure and Function of the Optic Nerve Head-Glaucoma versus Normal Dr Savita Bhat, Dr Anna Elias, Dr Siddharth Pawar, Dr S.J. Saikumar, Dr Alpesh Rajput, superior,
Original Article Relationship Between Structure and Function of the Optic Nerve Head-Glaucoma versus Normal Dr Savita Bhat, Dr Anna Elias, Dr Siddharth Pawar, Dr S.J. Saikumar, Dr Alpesh Rajput, superior,
Patterns of Subsequent Progression of Localized Retinal Nerve Fiber Layer Defects on Red-free Fundus Photographs in Normal-tension Glaucoma
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):330-336 http://dx.doi.org/10.3341/kjo.2014.28.4.330 Original Article Patterns of Subsequent Progression of Localized Retinal Nerve Fiber
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):330-336 http://dx.doi.org/10.3341/kjo.2014.28.4.330 Original Article Patterns of Subsequent Progression of Localized Retinal Nerve Fiber
Evaluating Optic Nerve Damage: Pearls and Pitfalls
 54 The Open Ophthalmology Journal, 9, 3, 54-58 Evaluating Optic Nerve Damage: Pearls and Pitfalls Open Access Paul J. Mackenzie * and Frederick S. Mikelberg Division of Glaucoma, Department of Ophthalmology
54 The Open Ophthalmology Journal, 9, 3, 54-58 Evaluating Optic Nerve Damage: Pearls and Pitfalls Open Access Paul J. Mackenzie * and Frederick S. Mikelberg Division of Glaucoma, Department of Ophthalmology
Scanning Laser Tomography to Evaluate Optic Discs of Normal Eyes
 Scanning Laser Tomography to Evaluate Optic Discs of Normal Eyes Hiroshi Nakamura,* Toshine Maeda,* Yasuyuki Suzuki and Yoichi Inoue* *Eye Division of Olympia Medical Clinic, Tokyo, Japan; Department of
Scanning Laser Tomography to Evaluate Optic Discs of Normal Eyes Hiroshi Nakamura,* Toshine Maeda,* Yasuyuki Suzuki and Yoichi Inoue* *Eye Division of Olympia Medical Clinic, Tokyo, Japan; Department of
Glaucoma: Diagnostic Modalities
 Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT) Retinal Nerve Fiber Layer Measurements Based on Time Domain OCT Measurements
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(5):369-377 http://dx.doi.org/10.3341/kjo.2012.26.5.369 Original Article A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT)
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(5):369-377 http://dx.doi.org/10.3341/kjo.2012.26.5.369 Original Article A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT)
Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach
 ORIGINAL STUDY Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach Joong Won Shin, MD, Kyung Rim Sung, MD, PhD, Jiyun
ORIGINAL STUDY Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach Joong Won Shin, MD, Kyung Rim Sung, MD, PhD, Jiyun
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD
 New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
CLINICAL SCIENCES. Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography
 CLINICAL SCIENCES Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography Seong Bae Park, MD; Kyung Rim Sung, MD, PhD; Sung Yong Kang, MD; Kyung Ri Kim, BS;
CLINICAL SCIENCES Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography Seong Bae Park, MD; Kyung Rim Sung, MD, PhD; Sung Yong Kang, MD; Kyung Ri Kim, BS;
Advances in OCT Murray Fingeret, OD
 Disclosures Advances in OCT Murray Fingeret, OD Consultant Alcon, Allergan, Bausch & Lomb, Carl Zeiss Meditec, Diopsys, Heidelberg Engineering, Reichert, Topcon Currently Approved OCT Devices OCT Devices
Disclosures Advances in OCT Murray Fingeret, OD Consultant Alcon, Allergan, Bausch & Lomb, Carl Zeiss Meditec, Diopsys, Heidelberg Engineering, Reichert, Topcon Currently Approved OCT Devices OCT Devices
CLINICAL SCIENCES. Felipe A. Medeiros, MD; Linda M. Zangwill, PhD; Christopher Bowd, PhD; Robert N. Weinreb, MD
 CLINICAL SCIENCES Comparison of the GDx VCC Scanning Laser Polarimeter, HRT II Confocal Scanning Laser Ophthalmoscope, and Stratus OCT Optical Coherence Tomograph for the Detection of Glaucoma Felipe A.
CLINICAL SCIENCES Comparison of the GDx VCC Scanning Laser Polarimeter, HRT II Confocal Scanning Laser Ophthalmoscope, and Stratus OCT Optical Coherence Tomograph for the Detection of Glaucoma Felipe A.
EXPERIMENTAL AND THERAPEUTIC MEDICINE 6: , 2013
 268 Comparison of optic nerve morphology in eyes with glaucoma and eyes with non-arteritic anterior ischemic optic neuropathy by Fourier domain optical coherence tomography YUXIN YANG 1, HAITAO ZHANG 1,
268 Comparison of optic nerve morphology in eyes with glaucoma and eyes with non-arteritic anterior ischemic optic neuropathy by Fourier domain optical coherence tomography YUXIN YANG 1, HAITAO ZHANG 1,
To assess the glaucoma diagnostic ability of Fourier Domain Optical Coherence Tomography
 American Journal of Engineering Research (AJER) e-issn : 2320-0847 p-issn : 2320-0936 Volume-02, Issue-11, pp-104-110 www.ajer.org Research Paper Open Access To assess the glaucoma diagnostic ability of
American Journal of Engineering Research (AJER) e-issn : 2320-0847 p-issn : 2320-0936 Volume-02, Issue-11, pp-104-110 www.ajer.org Research Paper Open Access To assess the glaucoma diagnostic ability of
CLINICAL SCIENCES. optic neuropathy characterized
 CLINICAL SCIENCES Spectral-Domain Optical Coherence Tomography for Detection of Localized Retinal Nerve Fiber Layer Defects in Patients With Open-Angle Glaucoma Na Rae Kim, MD; Eun Suk Lee, MD, PhD; Gong
CLINICAL SCIENCES Spectral-Domain Optical Coherence Tomography for Detection of Localized Retinal Nerve Fiber Layer Defects in Patients With Open-Angle Glaucoma Na Rae Kim, MD; Eun Suk Lee, MD, PhD; Gong
The optic nerve head ONH) is an important anatomic
 Glaucoma Deep Optic Nerve Head Morphology Is Associated With Pattern of Glaucomatous Visual Field Defect in Open-Angle Glaucoma Jong Chul Han, Jae Hwan Choi, Do Young Park, Eun Jung Lee, and Changwon Kee
Glaucoma Deep Optic Nerve Head Morphology Is Associated With Pattern of Glaucomatous Visual Field Defect in Open-Angle Glaucoma Jong Chul Han, Jae Hwan Choi, Do Young Park, Eun Jung Lee, and Changwon Kee
Influence of Myopic Disc Shape on the Diagnostic Precision of the Heidelberg Retina Tomograph
 Influence of Myopic Disc Shape on the Diagnostic Precision of the Heidelberg Retina Tomograph Yoshio Yamazaki,* Keiji Yoshikawa, Shiho Kunimatsu, Nobuyuki Koseki, Yasuyuki Suzuki, Shun Matsumoto and Makoto
Influence of Myopic Disc Shape on the Diagnostic Precision of the Heidelberg Retina Tomograph Yoshio Yamazaki,* Keiji Yoshikawa, Shiho Kunimatsu, Nobuyuki Koseki, Yasuyuki Suzuki, Shun Matsumoto and Makoto
Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
 Romanian Journal of Ophthalmology, Volume 60, Issue 3, July-September 2016. pp:158-164 GENERAL ARTICLE Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
Romanian Journal of Ophthalmology, Volume 60, Issue 3, July-September 2016. pp:158-164 GENERAL ARTICLE Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
Available online at Pelagia Research Library. Advances in Applied Science Research, 2013, 4(6):
 Available online at www.pelagiaresearchlibrary.com Advances in Applied Science Research, 2013, 4(6):201-206 ISSN: 0976-8610 CODEN (USA): AASRFC Comparison of glaucoma diagnostic ability of retinal nerve
Available online at www.pelagiaresearchlibrary.com Advances in Applied Science Research, 2013, 4(6):201-206 ISSN: 0976-8610 CODEN (USA): AASRFC Comparison of glaucoma diagnostic ability of retinal nerve
21st Century Visual Field Testing
 Supplement to Supported by an educational grant from Carl Zeiss Meditec, Inc. Winter 2011 21st Century Visual Field Testing the Evolution Continues 21st Century Visual Field Testing 21st Century Visual
Supplement to Supported by an educational grant from Carl Zeiss Meditec, Inc. Winter 2011 21st Century Visual Field Testing the Evolution Continues 21st Century Visual Field Testing 21st Century Visual
The Role of the RNFL in the Diagnosis of Glaucoma
 Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
RETINAL NERVE FIBER LAYER
 CLINICAL SCIENCES The Effect of Scan Diameter on Retinal Nerve Fiber Layer Thickness Measurement Using Stratus Optic Coherence Tomography Giacomo Savini, MD; Piero Barboni, MD; Michele Carbonelli, MD;
CLINICAL SCIENCES The Effect of Scan Diameter on Retinal Nerve Fiber Layer Thickness Measurement Using Stratus Optic Coherence Tomography Giacomo Savini, MD; Piero Barboni, MD; Michele Carbonelli, MD;
International Journal of Scientific & Engineering Research, Volume 4, Issue 12, December ISSN
 International Journal of Scientific & Engineering Research, Volume 4, Issue 12, December-2013 108 Name of Chief and Corresponding Author : Dr Chandrima Paul TITLE : Comparison of glaucoma diagnostic ability
International Journal of Scientific & Engineering Research, Volume 4, Issue 12, December-2013 108 Name of Chief and Corresponding Author : Dr Chandrima Paul TITLE : Comparison of glaucoma diagnostic ability
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma. Module 3a GDx
 STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
Science & Technologies
 STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
Relationship between the GDx VCC and Stratus OCT in Primary Open Angle Glaucoma
 Relationship between the GDx VCC and Stratus OCT in Primary Open Angle Glaucoma Reza Zarei, MD 1 Mohammad Soleimani, MD 2 Sasan Moghimi, MD 3 Mohammad Yaser Kiarudi, MD 2 Mahmoud Jabbarvand, MD 1 Yadollah
Relationship between the GDx VCC and Stratus OCT in Primary Open Angle Glaucoma Reza Zarei, MD 1 Mohammad Soleimani, MD 2 Sasan Moghimi, MD 3 Mohammad Yaser Kiarudi, MD 2 Mahmoud Jabbarvand, MD 1 Yadollah
Financial Disclosure. Visual Field Interpretation RELIABILITY VISUAL FIELD INTERPRETATION IN GLAUCOMA METHODS OF DATA PRESENTATION
 VISUAL FIELD INTERPRETATION IN GLAUCOMA Danica J. Marrelli, OD, FAAO University of Houston College of Optometry Financial Disclosure I have received speaking and/or consulting fees from: Aerie Pharmaceutical
VISUAL FIELD INTERPRETATION IN GLAUCOMA Danica J. Marrelli, OD, FAAO University of Houston College of Optometry Financial Disclosure I have received speaking and/or consulting fees from: Aerie Pharmaceutical
Confocal Adaptive Optics Imaging of Peripapillary Nerve Fiber Bundles: Implications for Glaucomatous Damage Seen on Circumpapillary OCT Scans
 Article DOI: 10.1167/tvst.4.2.12 Confocal Adaptive Optics Imaging of Peripapillary Nerve Fiber Bundles: Implications for Glaucomatous Damage Seen on Circumpapillary OCT Scans Donald C. Hood 1, Monica F.
Article DOI: 10.1167/tvst.4.2.12 Confocal Adaptive Optics Imaging of Peripapillary Nerve Fiber Bundles: Implications for Glaucomatous Damage Seen on Circumpapillary OCT Scans Donald C. Hood 1, Monica F.
The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation
 C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
Glaucoma: a disease of the macula?
 Glaucoma: a disease of the macula? Derek MacDonald, OD, FAAO Waterloo, Ontario, Canada Please silence all mobile devices and remove items from chairs so others can sit. Unauthorized recording of this session
Glaucoma: a disease of the macula? Derek MacDonald, OD, FAAO Waterloo, Ontario, Canada Please silence all mobile devices and remove items from chairs so others can sit. Unauthorized recording of this session
Generally, myopia is a condition of the eye that makes it
 Glaucoma Effect of Myopia on the Progression of Primary Open- Angle Glaucoma Jin Young Lee, 1 Kyung Rim Sung, 1 Seungbong Han, 2 and Jung Hwa Na 1 1 Department of Ophthalmology, College of Medicine, University
Glaucoma Effect of Myopia on the Progression of Primary Open- Angle Glaucoma Jin Young Lee, 1 Kyung Rim Sung, 1 Seungbong Han, 2 and Jung Hwa Na 1 1 Department of Ophthalmology, College of Medicine, University
Comparison of Optic Disc Topography Measured by Retinal Thickness Analyzer with Measurement by Heidelberg Retina Tomograph II
 Comparison of Optic Disc Topography Measured by Retinal Analyzer with Measurement by Heidelberg Retina Tomograph II Noriko Itai*, Masaki Tanito*, and Etsuo Chihara* *Senshokai Eye Institute, Uji, Kyoto,
Comparison of Optic Disc Topography Measured by Retinal Analyzer with Measurement by Heidelberg Retina Tomograph II Noriko Itai*, Masaki Tanito*, and Etsuo Chihara* *Senshokai Eye Institute, Uji, Kyoto,
S Morishita, T Tanabe, S Yu, M Hangai, T Ojima, H Aikawa, N Yoshimura. Clinical science
 Department of Ophthalmology and Visual Sciences, Kyoto University Graduate School of Medicine, Kyoto, Japan Correspondence to: Dr T Tanabe, Department of Ophthalmology, The Tazuke Kofukai Medical Institute,
Department of Ophthalmology and Visual Sciences, Kyoto University Graduate School of Medicine, Kyoto, Japan Correspondence to: Dr T Tanabe, Department of Ophthalmology, The Tazuke Kofukai Medical Institute,
Correspondence should be addressed to Kui Dong Kang;
 Journal of Ophthalmology, Article ID 931738, 9 pages http://dx.doi.org/10.1155/2014/931738 Clinical Study Correlation between Optic Nerve Parameters Obtained Using 3D Nonmydriatic Retinal Camera and Optical
Journal of Ophthalmology, Article ID 931738, 9 pages http://dx.doi.org/10.1155/2014/931738 Clinical Study Correlation between Optic Nerve Parameters Obtained Using 3D Nonmydriatic Retinal Camera and Optical
Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic Syndrome
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Research Article Repeatability of Perimacular Ganglion Cell Complex Analysis with Spectral-Domain Optical Coherence Tomography
 Ophthalmology Volume 2015, Article ID 605940, 5 pages http://dx.doi.org/10.1155/2015/605940 Research Article Repeatability of Perimacular Ganglion Cell Complex Analysis with Spectral-Domain Optical Coherence
Ophthalmology Volume 2015, Article ID 605940, 5 pages http://dx.doi.org/10.1155/2015/605940 Research Article Repeatability of Perimacular Ganglion Cell Complex Analysis with Spectral-Domain Optical Coherence
Introduction. Hemma Resch, Gabor Deak, Ivania Pereira and Clemens Vass. e225. Acta Ophthalmologica 2012
 Comparison of optic disc parameters using spectral domain cirrus high-definition optical coherence tomography and confocal scanning laser ophthalmoscopy in normal eyes Hemma Resch, Gabor Deak, Ivania Pereira
Comparison of optic disc parameters using spectral domain cirrus high-definition optical coherence tomography and confocal scanning laser ophthalmoscopy in normal eyes Hemma Resch, Gabor Deak, Ivania Pereira
Elevated intraocular pressure (IOP) is a major risk factor for
 Glaucoma The Association between Retinal Vessel Diameter and Retinal Nerve Fiber Layer Thickness in Asymmetric Normal Tension Glaucoma Patients Joon Mo Kim, 1 Mo Sae Kim, 2 Hyo Ju Jang, 1 Ki Ho Park, 3
Glaucoma The Association between Retinal Vessel Diameter and Retinal Nerve Fiber Layer Thickness in Asymmetric Normal Tension Glaucoma Patients Joon Mo Kim, 1 Mo Sae Kim, 2 Hyo Ju Jang, 1 Ki Ho Park, 3
Heidelberg Retina Tomography Analysis in Optic Disks with Anatomic Particularities
 Journal of Medicine and Life Vol. 3, No.4, October December 2010, pp.359 364 Heidelberg Retina Tomography Analysis in Optic Disks with Anatomic Particularities A. M. Dascalu*, C. Alexandrescu*, R. Pascu*,
Journal of Medicine and Life Vol. 3, No.4, October December 2010, pp.359 364 Heidelberg Retina Tomography Analysis in Optic Disks with Anatomic Particularities A. M. Dascalu*, C. Alexandrescu*, R. Pascu*,
THE BASIC PATHOLOGIC CHANGE IN GLAUCOMA IS
 Quantitative Assessment of Atypical Birefringence Images Using Scanning Laser Polarimetry With Variable Corneal Compensation HARMOHINA BAGGA, MD, DAVID S. GREENFIELD, MD, AND WILLIAM J. FEUER, MS PURPOSE:
Quantitative Assessment of Atypical Birefringence Images Using Scanning Laser Polarimetry With Variable Corneal Compensation HARMOHINA BAGGA, MD, DAVID S. GREENFIELD, MD, AND WILLIAM J. FEUER, MS PURPOSE:
Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed?
 Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed? Jody Piltz-Seymour, M.D. Clinical Professor Perelman School of Medicine University of Pennsylvania Wills Glaucoma Service Valley
Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed? Jody Piltz-Seymour, M.D. Clinical Professor Perelman School of Medicine University of Pennsylvania Wills Glaucoma Service Valley
Evolving glaucoma management True diagnostic integration for the preservation of vision
 Evolving glaucoma management True diagnostic integration for the preservation of vision // GLAUCOMA MANAGEMENT MADE BY ZEISS The moment you are certain it is glaucoma. This is the moment we work for. There
Evolving glaucoma management True diagnostic integration for the preservation of vision // GLAUCOMA MANAGEMENT MADE BY ZEISS The moment you are certain it is glaucoma. This is the moment we work for. There
Linking structure and function in glaucoma
 CET CONTINUING Sponsored by 1 CET POINT Linking structure and function in glaucoma 50 Dr Samantha McGinnigle PhD, BSc (Hons), MCOptom, AHEA This article will give an overview of the latest imaging technology
CET CONTINUING Sponsored by 1 CET POINT Linking structure and function in glaucoma 50 Dr Samantha McGinnigle PhD, BSc (Hons), MCOptom, AHEA This article will give an overview of the latest imaging technology
Il contributo dell'angio-oct: valutazione integrata della componente nervosa e vascolare della malattia glaucomatosa
 SIMPOSIO G.O.A.L. - LE NUOVE FRONTIERE DIAGNOSTICHE E LE LINEE DI INDIRIZZO AMBULATORIALI DEL GLAUCOMA Coordinatore e moderatore: D. Mazzacane Presidente: L. Rossetti Il contributo dell'angio-oct: valutazione
SIMPOSIO G.O.A.L. - LE NUOVE FRONTIERE DIAGNOSTICHE E LE LINEE DI INDIRIZZO AMBULATORIALI DEL GLAUCOMA Coordinatore e moderatore: D. Mazzacane Presidente: L. Rossetti Il contributo dell'angio-oct: valutazione
Discriminating between Normal and Glaucoma-Damaged Eyes with the Heidelberg Retina Tomograph 3
 Discriminating between Normal and Glaucoma-Damaged Eyes with the Heidelberg Retina Tomograph 3 Antonio Ferreras, MD, PhD, 1 Luís E. Pablo, MD, PhD, 1 José M. Larrosa, MD, PhD, 1 Vicente Polo, MD, PhD,
Discriminating between Normal and Glaucoma-Damaged Eyes with the Heidelberg Retina Tomograph 3 Antonio Ferreras, MD, PhD, 1 Luís E. Pablo, MD, PhD, 1 José M. Larrosa, MD, PhD, 1 Vicente Polo, MD, PhD,
A comparison of HRT II and GDx imaging for glaucoma detection in a primary care eye clinic setting
 (2007) 21, 1050 1055 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye CLINICAL STUDY A comparison of HRT II and GDx imaging for glaucoma detection in a primary
(2007) 21, 1050 1055 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye CLINICAL STUDY A comparison of HRT II and GDx imaging for glaucoma detection in a primary
Scanning Laser Polarimetry and Optical Coherence Tomography for Detection of Retinal Nerve Fiber Layer Defects
 접수번호 : 2008-105 Korean Journal of Ophthalmology 2009;23:169-175 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.169 Scanning Laser Polarimetry and Optical Coherence Tomography for Detection of Retinal Nerve
접수번호 : 2008-105 Korean Journal of Ophthalmology 2009;23:169-175 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.169 Scanning Laser Polarimetry and Optical Coherence Tomography for Detection of Retinal Nerve
Optic nerve head morphometry in healthy adults using confocal laser scanning tomography
 761 SCIENTIFIC REPORT Optic nerve head morphometry in healthy adults using confocal laser scanning tomography M M Hermann, I Theofylaktopoulos, N Bangard, C Jonescu-Cuypers, S Coburger, M Diestelhorst...
761 SCIENTIFIC REPORT Optic nerve head morphometry in healthy adults using confocal laser scanning tomography M M Hermann, I Theofylaktopoulos, N Bangard, C Jonescu-Cuypers, S Coburger, M Diestelhorst...
CHAPTER 13 CLINICAL CASES INTRODUCTION
 2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
Study of correlation of cup disc ratio with visual field loss in primary open angle glaucoma
 Original Research Article DOI: 10.18231/2395-1451.2017.0003 Study of correlation of cup disc ratio with visual field loss in primary open angle glaucoma Pankaj Soni 1,*, Ashwani Srivastava 2, Akash Srivastava
Original Research Article DOI: 10.18231/2395-1451.2017.0003 Study of correlation of cup disc ratio with visual field loss in primary open angle glaucoma Pankaj Soni 1,*, Ashwani Srivastava 2, Akash Srivastava
G laucoma is a progressive optic neuropathy in which
 1135 EXTENDED REPORT The correlation between optic nerve head topographic measurements, peripapillary nerve fibre layer thickness, and visual field indices in glaucoma Y-W Lan, D B Henson, A J Kwartz...
1135 EXTENDED REPORT The correlation between optic nerve head topographic measurements, peripapillary nerve fibre layer thickness, and visual field indices in glaucoma Y-W Lan, D B Henson, A J Kwartz...
1/25/2019 OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! THE ORIGINAL RAGING GLAUCOMA OCT RETINAL IMAGING OPTIC NERVE HEAD EXAMINATION
 OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com THE ORIGINAL RAGING GLAUCOMA 47-year-old Black
OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com THE ORIGINAL RAGING GLAUCOMA 47-year-old Black
Reproducibility of Bruch Membrane Opening-Minimum Rim Width Measurements With Spectral Domain Optical Coherence Tomography
 ORIGINAL STUDY Reproducibility of Bruch Membrane Opening-Minimum Rim Width Measurements With Spectral Domain Optical Coherence Tomography Keunheung Park, MD,* Jinmi Kim, PhD, and Jiwoong Lee, MD, PhD*
ORIGINAL STUDY Reproducibility of Bruch Membrane Opening-Minimum Rim Width Measurements With Spectral Domain Optical Coherence Tomography Keunheung Park, MD,* Jinmi Kim, PhD, and Jiwoong Lee, MD, PhD*
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL SCIENCES. (FDP) was designed to emphasize the response characteristics of the parasol
 CLINICAL SCIENCES Detecting Visual Function Abnormalities Using the Swedish Interactive Threshold Algorithm and Matrix Perimetry in Eyes With Glaucomatous Appearance of the Optic Disc Lisandro M. Sakata,
CLINICAL SCIENCES Detecting Visual Function Abnormalities Using the Swedish Interactive Threshold Algorithm and Matrix Perimetry in Eyes With Glaucomatous Appearance of the Optic Disc Lisandro M. Sakata,
NIH Public Access Author Manuscript Arch Ophthalmol. Author manuscript; available in PMC 2010 November 18.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Ophthalmol. 2009 July ; 127(7): 875 881. doi:10.1001/archophthalmol.2009.145. Measurement of Local Retinal Ganglion Cell Layer
NIH Public Access Author Manuscript Published in final edited form as: Arch Ophthalmol. 2009 July ; 127(7): 875 881. doi:10.1001/archophthalmol.2009.145. Measurement of Local Retinal Ganglion Cell Layer
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1
 Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
T he lamina cribrosa is a sieve-like membrane in the
 1299 EXTENDED REPORT Three dimensional analysis of the lamina cribrosa in glaucoma J Morgan-Davies, N Taylor, A R Hill, P Aspinall, CJ O Brien, A Azuara-Blanco... See end of article for authors affiliations...
1299 EXTENDED REPORT Three dimensional analysis of the lamina cribrosa in glaucoma J Morgan-Davies, N Taylor, A R Hill, P Aspinall, CJ O Brien, A Azuara-Blanco... See end of article for authors affiliations...
Assessment of Retinal Nerve Fiber Layer Changes by Cirrus High-definition Optical Coherence Tomography in Myopia
 Divya Singh et al Original REASEARCH 10.5005/jp-journals-10028-1223 Assessment of Retinal Nerve Fiber Layer Changes by Cirrus High-definition Optical Coherence Tomography in Myopia 1 Divya Singh, 2 Sanjay
Divya Singh et al Original REASEARCH 10.5005/jp-journals-10028-1223 Assessment of Retinal Nerve Fiber Layer Changes by Cirrus High-definition Optical Coherence Tomography in Myopia 1 Divya Singh, 2 Sanjay
STANDARD AUTOMATED PERIMETRY IS A GENERALLY
 Comparison of Long-term Variability for Standard and Short-wavelength Automated Perimetry in Stable Glaucoma Patients EYTAN Z. BLUMENTHAL, MD, PAMELA A. SAMPLE, PHD, LINDA ZANGWILL, PHD, ALEXANDER C. LEE,
Comparison of Long-term Variability for Standard and Short-wavelength Automated Perimetry in Stable Glaucoma Patients EYTAN Z. BLUMENTHAL, MD, PAMELA A. SAMPLE, PHD, LINDA ZANGWILL, PHD, ALEXANDER C. LEE,
Parafoveal Scanning Laser Polarimetry for Early Glaucoma Detection
 Yamanashi Med. J. 18(1), 15~ 20, 2003 Original Article Parafoveal Scanning Laser Polarimetry for Early Glaucoma Detection Satoshi KOGURE, Yoshiki TODA, Hiroyuki IIJIMA and Shigeo TSUKAHARA Department of
Yamanashi Med. J. 18(1), 15~ 20, 2003 Original Article Parafoveal Scanning Laser Polarimetry for Early Glaucoma Detection Satoshi KOGURE, Yoshiki TODA, Hiroyuki IIJIMA and Shigeo TSUKAHARA Department of
OPTOMETRY RESEARCH PAPER
 C L I N I C A L A N D E X P E R I M E N T A L OPTOMETRY RESEARCH PAPER Interocular symmetry of retinal nerve fibre layer thickness in healthy eyes: a spectral-domain optical coherence tomographic study
C L I N I C A L A N D E X P E R I M E N T A L OPTOMETRY RESEARCH PAPER Interocular symmetry of retinal nerve fibre layer thickness in healthy eyes: a spectral-domain optical coherence tomographic study
Retinal Nerve Fiber Layer Measurement Variability with Spectral Domain Optical Coherence Tomography
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(1):32-38 http://dx.doi.org/10.3341/kjo.2012.26.1.32 Retinal Nerve Fiber Layer Measurement Variability with Spectral Domain Optical Coherence
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(1):32-38 http://dx.doi.org/10.3341/kjo.2012.26.1.32 Retinal Nerve Fiber Layer Measurement Variability with Spectral Domain Optical Coherence
Glaucoma is a chronic progressive optic neuropathy,
 ORIGINAL STUDY Comparison of Neuroretinal Rim Area Measurements Made by the Heidelberg Retina Tomograph I and the Heidelberg Retina Tomograph II Ya Xing Wang, MD,*w Neil O Leary, MSc,zy Nicholas G. Strouthidis,
ORIGINAL STUDY Comparison of Neuroretinal Rim Area Measurements Made by the Heidelberg Retina Tomograph I and the Heidelberg Retina Tomograph II Ya Xing Wang, MD,*w Neil O Leary, MSc,zy Nicholas G. Strouthidis,
3/16/2018. Perimetry
 Perimetry The normal visual field extends further away from fixation temporally and inferiorly than superiorly and nasally. From the center of the retina this sensitivity decreases towards the periphery,
Perimetry The normal visual field extends further away from fixation temporally and inferiorly than superiorly and nasally. From the center of the retina this sensitivity decreases towards the periphery,
MATERIALS AND METHODS
 Glaucoma Analysis of Peripapillary Retinal Nerve Fiber Distribution in Normal Young Adults Seung Woo Hong, 1,2 Myung Douk Ahn, 2 Shin Hee Kang, 1,3 and Seong Kyu Im 1,4 PURPOSE. To determine the anatomic
Glaucoma Analysis of Peripapillary Retinal Nerve Fiber Distribution in Normal Young Adults Seung Woo Hong, 1,2 Myung Douk Ahn, 2 Shin Hee Kang, 1,3 and Seong Kyu Im 1,4 PURPOSE. To determine the anatomic
Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC)
 Dada T et al Original article Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC) Dada T1, Aggarwal A1, Bali SJ2, Sharma A1, Shah
Dada T et al Original article Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC) Dada T1, Aggarwal A1, Bali SJ2, Sharma A1, Shah
Peripapillary Retinal Thickness. Maps in the Evaluation of Glaucoma Patients: A Novel Concept.
 Peripapillary Retinal Thickness Maps in the Evaluation of Glaucoma Patients: A Novel Concept The Harvard community has made this article openly available. Please share how this access benefits you. Your
Peripapillary Retinal Thickness Maps in the Evaluation of Glaucoma Patients: A Novel Concept The Harvard community has made this article openly available. Please share how this access benefits you. Your
Scanning laser polarimetry (SLP) provides real-time, objective
 The Effect of Atypical Birefringence Patterns on Glaucoma Detection Using Scanning Laser Polarimetry with Variable Corneal Compensation Christopher Bowd, Felipe A. Medeiros, Robert N. Weinreb, and Linda
The Effect of Atypical Birefringence Patterns on Glaucoma Detection Using Scanning Laser Polarimetry with Variable Corneal Compensation Christopher Bowd, Felipe A. Medeiros, Robert N. Weinreb, and Linda
Reproducibility of Nerve Fiber Layer Thickness Measurements by Use of Optical Coherence Tomography
 Reproducibility of Nerve Fiber Layer Thickness Measurements by Use of Optical Coherence Tomography Eytan Z. Blumenthal, MD, 1 Julia M. Williams, BS, 1 Robert N. Weinreb, MD, 1 Christopher A. Girkin, MD,
Reproducibility of Nerve Fiber Layer Thickness Measurements by Use of Optical Coherence Tomography Eytan Z. Blumenthal, MD, 1 Julia M. Williams, BS, 1 Robert N. Weinreb, MD, 1 Christopher A. Girkin, MD,
Comparison of macular GCIPL and peripapillary RNFL deviation maps for detection of glaucomatous eye with localized RNFL defect
 Comparison of macular GCIPL and peripapillary RNFL deviation maps for detection of glaucomatous eye with localized RNFL defect Mi Jeung Kim, 1,2 Ki Ho Park, 1,2 Beong Wook Yoo, 3 Jin Wook Jeoung, 1,2 Hee
Comparison of macular GCIPL and peripapillary RNFL deviation maps for detection of glaucomatous eye with localized RNFL defect Mi Jeung Kim, 1,2 Ki Ho Park, 1,2 Beong Wook Yoo, 3 Jin Wook Jeoung, 1,2 Hee
Thickness Changes in the Fovea and Peripapillary Retinal Nerve Fiber Layer Depend on the Degree of Myopia
 Thickness Changes in the Fovea and Peripapillary Retinal Nerve Fiber Layer Depend on the Degree of Myopia Sung-Won Choi, MD, Seok-Joon Lee, MD Department of Ophthalmology, Wonju Christian Hospital. Yonsei
Thickness Changes in the Fovea and Peripapillary Retinal Nerve Fiber Layer Depend on the Degree of Myopia Sung-Won Choi, MD, Seok-Joon Lee, MD Department of Ophthalmology, Wonju Christian Hospital. Yonsei
Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India
 Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Is NTG different from POAG?
 Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
R&M Solutions
 Mohamed Hosny El-Bradey, MD., Assistant Professor of Ophthalmology, Tanta University. Wael El Haig, MD., Professor of Ophthalmology. Zagazeeg University. 1 Myopic CNV is considered the most common vision
Mohamed Hosny El-Bradey, MD., Assistant Professor of Ophthalmology, Tanta University. Wael El Haig, MD., Professor of Ophthalmology. Zagazeeg University. 1 Myopic CNV is considered the most common vision
Glaucoma Evaluation. OCT Pearls for Glaucoma. OCT: Retinal Nerve Fiber Layer. Financial Disclosures. OCT: Macula. Case Example
 OCT Pearls for Glaucoma using OCT of the macula for glaucoma Glaucoma Evaluation Right eye Visual Acuity 20/25 20/25 IOP 13 13 Central corneal 530 530 thickness Anterior exam Normal with PCIOL Normal with
OCT Pearls for Glaucoma using OCT of the macula for glaucoma Glaucoma Evaluation Right eye Visual Acuity 20/25 20/25 IOP 13 13 Central corneal 530 530 thickness Anterior exam Normal with PCIOL Normal with
* Şükrü Bayraktar, MD, Zerrin Bayraktar, MD, and Ömer Faruk Yilmaz, MD
 Journal of Glaucoma 10:163 169 2001 Lippincott Williams & Wilkins, Inc. Influence of Scan Radius Correction for Ocular Magnification and Relationship Between Scan Radius With Retinal Nerve Fiber Layer
Journal of Glaucoma 10:163 169 2001 Lippincott Williams & Wilkins, Inc. Influence of Scan Radius Correction for Ocular Magnification and Relationship Between Scan Radius With Retinal Nerve Fiber Layer
Research Article Assessment of the Optic Disc Morphology Using Spectral-Domain Optical Coherence Tomography and Scanning Laser Ophthalmoscopy
 BioMed Research International, Article ID 275654, 6 pages http://dx.doi.org/10.1155/2014/275654 Research Article Assessment of the Optic Disc Morphology Using Spectral-Domain Optical Coherence Tomography
BioMed Research International, Article ID 275654, 6 pages http://dx.doi.org/10.1155/2014/275654 Research Article Assessment of the Optic Disc Morphology Using Spectral-Domain Optical Coherence Tomography
The Optic Nerve Head In Glaucoma. Clinical Pearl #1. Characteristics of Normal Disk 9/26/2017. Initial detectable damage Structure vs function
 The Optic Nerve Head In Glaucoma Clinical Pearl #1 Eric E. Schmidt, O.D., F.A.A.O. Omni Eye Specialists Wilmington,NC schmidtyvision@msn.com Glaucoma is an optic neuropathy Initial detectable damage Structure
The Optic Nerve Head In Glaucoma Clinical Pearl #1 Eric E. Schmidt, O.D., F.A.A.O. Omni Eye Specialists Wilmington,NC schmidtyvision@msn.com Glaucoma is an optic neuropathy Initial detectable damage Structure
Determinants of Optical Coherence Tomography Derived Minimum Neuroretinal Rim Width in a Normal Chinese Population
 Glaucoma Determinants of Optical Coherence Tomography Derived Minimum Neuroretinal Rim Width in a Normal Chinese Population Tin A. Tun, 1 Chen-Hsin Sun, 2,3 Mani Baskaran, 1,2,4 Michael J. A. Girard, 1,5
Glaucoma Determinants of Optical Coherence Tomography Derived Minimum Neuroretinal Rim Width in a Normal Chinese Population Tin A. Tun, 1 Chen-Hsin Sun, 2,3 Mani Baskaran, 1,2,4 Michael J. A. Girard, 1,5
