Research Article Study of Serum Calcium, Magnesium And Phosphorous Levels In Patients With Thyroid Disorders
|
|
|
- Irma Mason
- 5 years ago
- Views:
Transcription
1 Research Article Study of Serum Calcium, Magnesium And Phosphorous Levels In Patients With Thyroid Disorders Dr. Shweta R. Hebbar*, Dr. Nagarajappa. K., Dr. Sushma B. J, Dr. C. R. Mallikarjun Department of Biochemistry, S.S. Institute of Medical Sciences and Research Centre, Davangere. Received 22 Feb 2014; Accepted 15 Mar 2014 Corresponding Author*: ABSTRACT Thyroid disorders are most common and prevalent conditions in India, incidence being 42 million. Thyroid hormones are central regulator of body s haemodynamics, thermoregulation and metabolism. They also determine the mineral pool in the blood. The aim of the study was to study Serum calcium, magnesium and phosphorous levels in patients with thyroid disorders. In this study we included 30 diagnosed cases of Hypothyroidism, 30 diagnosed cases of Hyperthyroidism and 30 healthy controls in the similar age group from whom 3 ml of blood was drawn under aseptic precautions to measure Serum calcium, magnesium and phosphorous levels by spectrophotometry method. Serum Ca 2+ and PO -4 levels were significantly elevated in hyperthyroid and significantly decreased in hypothyroid patients compared to healthy controls. Serum Mg 2+ level was significantly decreased in hyperthyroid and significantly elevated in hypothyroid patients compared to healthy controls. There was a significant negative correlation between serum TSH and Ca 2+ level. The study indicates the profound influence of thyroid hormone on mineral metabolism. A patient with thyroid disorder may also manifest the symptoms that reflect altered mineral levels. Hence it is necessary to evaluate the serum levels of calcium, magnesium and phosphorous in patients with thyroid disorder in order to prevent further bone complications. Key words: Thyroid hormones, calcium, magnesium, phosphorous. How to Cite this Article Dr.Shwetha R.Hebbar et al., Study of Serum Calcium, Magnesium and Phosphorous levels in patients with Thyroid disorders. Soushrutam Int.Res.J. Of Phar. & Plant sci., Vol 2(2), 2014:
2 INTRODUCTION The thyroid gland produces two related hormones, Thyroxin (T 4 ) and triiodothyronine (T 3 ). Acting through thyroid hormone receptors α and β, these hormones plays a critical role in cell differentiation during development and helps to maintain thermogenic and metabolic homeostasis in adults (Fauci AS et al, 2008). The term hyperthyroidism is reserved for disorders that result from sustained overproduction of hormone by the thyroid gland itself. Reduced production of thyroid hormone is the central feature of the clinical state termed hypothyroidism. Thyroid hormone is essential for normal growth and maturation of the skeleton. Before puberty, thyroid hormone plays a major role in the maturation of bone (Kronenberg HM et al, 2008). In India, 42 million people are suffering from thyroid diseases; hypothyroidism being the commonest thyroid disorder (Murgod R and Soans G, 2012). The mean annual incidence of hypothyroidism is up to 4 in 1000 females, 1 in 1000 males and 1 in 4000 newborns (Suneel B et al, 2011; Suneel B et al, 2012). Calcium (Ca 2+ ) and phosphorous (PO -4 ) are the principal constituents of bone and together they comprise 65% of its weight. The quantitatively minor amounts of each of these ions in the extracellular fluid and within cells play crucial roles in normal physiology (Kronenberg HM et al, 2008). The majority of the total body stores of Ca 2+ and PO -4 are located in bone in the form of hydroxyapatite. Magnesium (Mg 2+ ) is the second most abundant intracellular cation in the body after potassium (Moe MS, 2008). Most of the total body Mg 2+ (67%) are found in bones and soft tissues (Gilroy CV et al, 2006). Thyroid hormone determines the mineral pool in the blood by influencing mobilization of minerals like Ca 2+ and PO -4 into the blood and also by influencing their clearance through urinary excretion due to its effect on glomerular filtration rate (GFR) or renal plasma flow ( RPF) (Suneel B et al, 2011; Suneel B et al, 2012). Previous studies done on serum Ca 2+, PO - 4 and Mg 2+ levels in thyroid disorders have shown conflicting results. Even though thyroid disorders are most common and prevalent conditions in India, studies focusing on blood levels of minerals are sparse (Murgod R and Soans G, 2012; Suneel B et al, 2011; Suneel B et al, 2012; Shivaleela MB et al, 2012). AIMS AND OBJECTIVES The present study was undertaken to assess the serum levels of Ca 2+, PO -4 and Mg
3 levels in thyroid disorders. We also investigated the correlation of serum TSH with Ca 2+, Mg 2+ and PO -4 levels in hypo and hyperthyroidism. MATERIALS AND METHODS Study design A case control study was carried out and the study group was selected from patients attending Medicine OPD of S.S.Hospital attached to S. S. Institute of Medical Sciences & Research Centre (SSIMS & RC), Davangere. The study was approved by the institutional ethical committee. Written informed consent was taken from each subject. Inclusion criteria The study population included cases and healthy controls in the age group of years attending the medicine outpatient department of SS hospital attached to SSIMS & RC. Both males and females were included in the study. They were divided into 3 groups: a) Group 1 included 30 newly diagnosed and untreated cases of hypothyroidism. The diagnosis was based on decreased serum T 3 and T 4 levels associated with increased TSH levels. b) Group 2 included 30 newly diagnosed and untreated cases of hyperthyroidism. The diagnosis was based on increased serum T 3 and T 4 levels associated with decreased TSH levels. All patients suffering from thyroid disorders were diagnosed and confirmed by the physician based on T 3 (Normal: ng/ml), T 4 (Normal: μg/ dl) and TSH (Normal: μiu/ ml) levels of the patients. c) Group 3 included 30 healthy controls in the similar age group having normal thyroid profile. Exclusion criteria Paediatric age group (<18 yrs), elderly age group (>60 yrs), renal disorders, hepatic disorders, bone disorders, diabetes, hypertension or any other systemic illness that may affect the mineral status, patients on mineral supplementation, drugs for treatment of thyroid disorders or any other medications that might affect serum mineral concentration. Method of sample collection About 3 ml of venous blood was drawn using a disposable syringe under aseptic conditions in a sterile bulb from selected subjects. Blood was allowed to clot and serum was separated after min by Remicentrifuge machine at 3000 rpm, serial no: LMC
4 Analytical methods The serum was used for the analysis of calcium, magnesium and phosphorous by the spectrophotometric method on semi autoanalyzer using commercially available kits (Burtis and Ashwood, 2001). RESULTS Results of the present study are shown below. STATISTICAL ANALYSIS The data was expressed in terms of mean and standard deviation. The comparison among the groups was done using one way analysis of variance (ANOVA) and post hoc. Table 1: Age and sex distribution in cases and healthy controls Variable Hypothyroid Hyperthyroid Controls Age (Yrs) 35.4 ± ± ± 10.7 Gender (M/F) 05/25 08/22 07/23 The values are expressed as Mean ± SD * p value <0.05- significant compared with controls ** P value < highly significant compared controls Table 2: Comparison of serum calcium, magnesium and phosphorous levels in cases and healthy controls Group 1 (N=30) Hypothyroid Group 2 (N= 30) Hyperthyroid Group 3 (N= 30) Healthy controls T3 (ng/ml) 0.79 ± 0.39** 3.34 ± 2.46 ** 1.13 ± 0.31 T4 (μg/dl) 4.73 ± 2.51 ** 14.6 ± 2.76 ** 8.89 ± 2.03 TSH (μiu/ml) ± ** 0.15 ± ± 1.06 Calcium (mg/dl) 6.35 ± 1.20 ** ± 1.93** 9.97 ± 0.63 Magnesium (mg/dl) Phosphorous (mg/dl) 4.92 ± 1.02 ** 1.23 ± 0.29 ** 2.04 ± ± 0.42 ** 5.75 ± 0.69 ** 3.63 ± 0.57 The values are expressed as Mean ± SD; n= number of subjects * p value <0.05- significant compared with controls ** P value < highly significant compared with controls 151
5 Serum Ca 2+ and PO -4 levels were significantly elevated in hyperthyroid (14.48 ± 1.93 and 5.75 ± 0.69, respectively. p< 0.001) and significantly decreased in hypothyroid patients (6.35 ± 1.20 and 1.59 ± 0.42, respectively. p< 0.001) compared to healthy controls (9.97 ± 0.63 and 3.63 ± 0.57, respectively). Serum Mg 2+ levels were significantly decreased (1.23 ± 0.29) in hyperthyroid and significantly elevated (4.92 ± 1.02) in hypothyroid patients compared to healthy controls (2.04 ± 0.21). Fig. 1: Graph showing the comparison of Serum calcium, magnesium and phosphorous levels in groups 1 (Hypothyroid), 2 (Hyperthyroid) and 3 (Healthy controls) Group 1 mg/ dl Group 2 Group calcium magnesium phosphorous Table 3: Correlation of serum TSH with Calcium, Phosphorous and Magnesium Hypothyroid Hyperthyroid Relation between r value p value r value p value TSH & Calcium * TSH & Phosphorous TSH & Magnesium
6 There was significant negative correlation between serum TSH and calcium in hypothyroid cases. No other significant correlation was found in hypo and hyperthyroid cases. Fig. 2: Scatter plot showing correlation of serum TSH with Calcium in Hypothyroid cases Calcium (mg/ dl) TSH (μiu/ml) DISCUSSION The present study was taken to study the effect of thyroid hormones on mineral status (Ca +, PO -4 and Mg 2+ ). Taking the age, the peak incidence of thyroid disorder was observed between years. Taking sex incidence, women had higher incidence when compared to men. Previous studies done on serum calcium, phosphorous and magnesium levels in thyroid disorders have shown variable results. Most of the studies have shown hypercalcemia in hyperthyroidism and hypocalcemia in hypothyroidism (Murgod R and Soans G, 2012; Suneel B et al, 2011; Suneel B et al, 2012; Shivaleela MB et al 2012) which is consistent with the present study. Hyperthyroidism is characterized by accelerated bone turnover, which is caused from direct stimulation of bone cells by high thyroid hormone concentration leading to hypercalcemia (Shivaleela MB et al, 2012; Schwarz C et al, 2012; Pantazi H and Papapetrou PD, 2000). Thyroid hormones exert its effect on osteoblasts via nuclear receptors to stimulate osteoclastic bone resorption (Shivaleela MB et al, 2012). Patients with hyperthyroidism have a significantly decreased bone mineral density (BMD) (Feigerlova E et al, 2012). Thus hyperthyroidism is one of the major 153
7 causes of secondary osteoporosis (Shivaleela MB et al, 2012; Dhanwal DK, 2011). In hypothyroidism, there is depressed bone turnover due to impaired mobilization of calcium in to the bone that leads to decrease in the blood calcium level (Suneel B et al, 2011). Reduced bone turnover impairs bone formation and mineralization with a subsequent risk of bone fragility and increased fracture (Feigerlova E et al, 2012). Associated vitamin D deficiency may be the cause for hypocalcaemia in Indian hyperthyroid patients (Shivaleela MB et al, 2012; Dhanwal DK, 2011). There are variable reports on serum phosphorous levels in patients with thyroid disorders. Some studies reported hyperphosphatemia in hyperthyroidism and vice versa which is consistent with the present study (Shivaleela MB et al, 2012). The changes are due to suppressed parathyroid hormone (PTH) levels as well as direct effects of thyroid hormones on tissue PO -4 metabolism and renal PO -4 handling (Dhanwal DK, 2011). Thyroid hormones stimulate bone resorption directly thereby increasing serum Ca + and PO -4 levels and suppressing PTH. Opposite effects are seen in hypothyroidism (Shivaleela MB et al, 2012). Some studies reported hypophosphatemia in hyperthyroidism and vice versa (Murgod R and Soans G, 2012; Suneel B et al, 2011; Suneel B et al, 2012; Schwarz C et al, 2012). In hypothyroidism, increased production of thyroid calcitonin can promote the tubular reabsorption of phosphate. In hyperthyroidism, decreased production of thyroid calcitonin promotes the tubular excretion of phosphate (Suneel B et al, 2011; Suneel B et al, 2012). Studies regarding serum magnesium in thyroid disorders are also conflicting. Some studies reported hypermagnesaemia in hypothyroidism and vice versa which is consistent with the present study (Murgod R and Soans G, 2012; Schwarz C et al, 2012; Jones JE et al, 1966). Thyroid hormone has direct effect on the tubule, which if chronically absent, results in renal retention of magnesium (Murgod R and Soans G, 2012; Mc Caffrey C and Quamme GA, 1984). Hyperthyroidism can increase renal excretion of magnesium, thus leading to hypomagnesemia (Gilroy CV et al, 2006). Increased thyroid activity causes more magnesium to be consumed by the tissue, thus favouring hypomagnesemia (Swaminathan S et al, 2010). Some studies reported hypomagnesaemia in hypothyroidism and vice versa. In hypothyroidism there is increased renal plasma flow (RPF) leading 154
8 to high clearance of magnesium from kidneys leading to hypomagnesaemia. In hyperthyroidism there is hypermagnesaemia because of low clearance of magnesium from renal tubules (Suneel B et al, 2011; Suneel B et al, 2012). REFERENCES Burtis, A.C and Ashwood, E.R. (2001) Tietz Fundamentals of Clinical chemistry. 5th ed. Philadelphia: W B Saunders. Dhanwal, D.K. (2011) Thyroid disorders and bone mineral metabolism. Indian Journal of Endocrinology and Metabolism, 15 (2), pp. S Fauci, A.S. et al. (2008) Harrison s Principles of Internal medicine. 18 th edition. New York: McGraw Hill. Feigerlova, E. et al. (2012) Thyroid disorders and bone mineral homeostasis [Monograph on the Internet]. Vandoeuvre: InTech- Open Access Company. Available from: Gilroy C.V. et al. (2006) Evaluation of ionized and total serum magnesium concentrations in hyperthyroid cats. The Canadian Journal of Veterinary Research, 70, pp Jones, J.E. et al. (1966) Magnesium metabolism in hyperthyroidism and hypothyroidism. Journal of Clinical Investigation, 45 (6), pp CONCLUSION The present study indicates the profound influence of thyroid hormone on mineral metabolism and changes in these minerals may eventually lead to complications like decreased bone mineral density and secondary osteoporosis. Therefore, it is necessary to evaluate the serum levels of these minerals in all patients with thyroid disorders. Kronenberg, H.M. et al. (2008) William s Textbook of Endocrinology. 11th ed. Philadelphia: Saunders. Mc Caffrey C and Quamme G.A. (1984) Effects of Thyroid status on Renal calcium and magnesium handling. Canadian Journal of Comparative Medicine, 48, pp Moe, M.S. (2008) Disorders involving calcium, phosphorous, and magnesium. Prim Care, 35 (2), pp Murgod, R and Soans, G. (2012) Changes in electrolyte and lipid profile in hypothyroidism. International Journal of Life Science and Pharma Research, 2 (3), pp Pantazi, H and Papapetrou, P.D. (2000) Changes in parameters of bone and mineral metabolism during therapy for hyperthyroidism. The Journal of Clinical Endocrinology and Metabolism, 85 (3), pp Schwarz, C. et al. (2012) Thyroid function and serum electrolytes: Does an association really exist? Swiss Medical Weekly, 142(13669), pp
9 Shivaleela, M.B. Poornima, R.T. and Jayaprakash Murthy, D.S. (2012) Serum calcium and phosphorous levels in Thyroid dysfunction. Indian Journal of Fundamental and Applied Life Sciences, 2 (2), pp Suneel, B. et al. (2011) Mineral status in Thyroid disorders (hypo & hyper). International Journal of Applied Biology and Pharmaceutical Technology, 2 (4), pp Suneel, B. Naidu, J.N. and Aparna, R.R. (2012) Mineral metabolism in hyper thyroidism. International Journal of Pharma and Bio Sciences, 3 (2), pp. B Swaminathan, S. Priyaand, G. and Ghosh, M. (2010) Association between thyroid hormones and macro metals calcium and magnesium. Journal of Pharmaceutical and Biomedical Sciences, 4 (4), pp.1-5. Source of Support: Nil Conflict of Interest: None declared 156
SERUM CALCIUM AND PHOSPHOROUS LEVELS IN THYROID DYSFUNCTION
 SERUM CALCIUM AND PHOSPHOROUS LEVELS IN THYROID DYSFUNCTION *Shivaleela MB, Poornima RT and Jayaprakash Murthy DS Department of Biochemistry, J. J. M. Medical College, Davangere -577004, Karnataka, India.
SERUM CALCIUM AND PHOSPHOROUS LEVELS IN THYROID DYSFUNCTION *Shivaleela MB, Poornima RT and Jayaprakash Murthy DS Department of Biochemistry, J. J. M. Medical College, Davangere -577004, Karnataka, India.
H 2 O, Electrolytes and Acid-Base Balance
 H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
David Bruyette, DVM, DACVIM
 VCAwestlaspecialty.com David Bruyette, DVM, DACVIM Disorders of calcium metabolism are common endocrine disorders in both dogs and cats. In this article we present a logical diagnostic approach to patients
VCAwestlaspecialty.com David Bruyette, DVM, DACVIM Disorders of calcium metabolism are common endocrine disorders in both dogs and cats. In this article we present a logical diagnostic approach to patients
The Parathyroid Glands Secrete Parathyroid Hormone, which Regulates Calcium, Magnesium, and Phosphate Ion Levels
 17.6 The Parathyroid Glands Secrete Parathyroid Hormone, which Regulates Calcium, Magnesium, and Phosphate Ion Levels Partially embedded in the posterior surface of the lateral lobes of the thyroid gland
17.6 The Parathyroid Glands Secrete Parathyroid Hormone, which Regulates Calcium, Magnesium, and Phosphate Ion Levels Partially embedded in the posterior surface of the lateral lobes of the thyroid gland
WATER, SODIUM AND POTASSIUM
 WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
Ca, Mg metabolism, bone diseases. Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary
 Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
The Parathyroid Glands
 The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
Major intra and extracellular ions Lec: 1
 Major intra and extracellular ions Lec: 1 The body fluids are solutions of inorganic and organic solutes. The concentration balance of the various components is maintained in order for the cell and tissue
Major intra and extracellular ions Lec: 1 The body fluids are solutions of inorganic and organic solutes. The concentration balance of the various components is maintained in order for the cell and tissue
Changes in the Electrolyte Profile of Patients having Hypothyroidism
 www.jmscr.igmpublication.org Impact Factcor-1.1147 ISSN (e)-2347-176x Changes in the Electrolyte Profile of Patients having Hypothyroidism Authors Jaskiran Kaur 1, Naved Ahmad 2, Akash Gupta 3* 1. Assistant
www.jmscr.igmpublication.org Impact Factcor-1.1147 ISSN (e)-2347-176x Changes in the Electrolyte Profile of Patients having Hypothyroidism Authors Jaskiran Kaur 1, Naved Ahmad 2, Akash Gupta 3* 1. Assistant
Amani Alghamdi. Slide 1
 Minerals in the body Amani Alghamdi Slide 1 The Minerals Small, naturally occurring, inorganic, chemical elements Serve as structural components Minerals classification The minerals present in the body
Minerals in the body Amani Alghamdi Slide 1 The Minerals Small, naturally occurring, inorganic, chemical elements Serve as structural components Minerals classification The minerals present in the body
Endocrine secretion cells secrete substances into the extracellular fluid
 Animal Hormones Concept 30.1 Hormones Are Chemical Messengers Endocrine secretion cells secrete substances into the extracellular fluid Exocrine secretion cells secrete substances into a duct or a body
Animal Hormones Concept 30.1 Hormones Are Chemical Messengers Endocrine secretion cells secrete substances into the extracellular fluid Exocrine secretion cells secrete substances into a duct or a body
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
OMICS Journals are welcoming Submissions
 OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
5/18/2017. Specific Electrolytes. Sodium. Sodium. Sodium. Sodium. Sodium
 Specific Electrolytes Hyponatremia Hypervolemic Replacing water (not electrolytes) after perspiration Freshwater near-drowning Syndrome of Inappropriate ADH Secretion (SIADH) Hypovolemic GI disease (decreased
Specific Electrolytes Hyponatremia Hypervolemic Replacing water (not electrolytes) after perspiration Freshwater near-drowning Syndrome of Inappropriate ADH Secretion (SIADH) Hypovolemic GI disease (decreased
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Head and Neck Endocrine Surgery
 Objectives Endocrine Physiology Risk factors for hypocalcemia Management strategies Passive vs. active Treatment of hypocalcemia Department of Head and Neck Management of Calcium in Thyroid and Parathyroid
Objectives Endocrine Physiology Risk factors for hypocalcemia Management strategies Passive vs. active Treatment of hypocalcemia Department of Head and Neck Management of Calcium in Thyroid and Parathyroid
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
Thyroid Function Test Ordering Pattern in a Tertiary Care Hospital in Western Uttar Pradesh, India.
 Research and Reviews: Journal of Medical and Health Sciences Thyroid Function Test Ordering Pattern in a Tertiary Care Hospital in Western Uttar Pradesh, India. Rajni Dawar Mahajan *, Tabassum Yasmin,
Research and Reviews: Journal of Medical and Health Sciences Thyroid Function Test Ordering Pattern in a Tertiary Care Hospital in Western Uttar Pradesh, India. Rajni Dawar Mahajan *, Tabassum Yasmin,
Bone Remodeling & Repair Pathologies
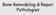 Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
GLOSSARY OF TERMS. produced in response to an antigen to bond with and neutralize that antigen / the body's way of destroying foreign invaders
 TERM 24-hour urine acidosis acquired aemia (prefix) albumin alkalosis anemia antibodies antigen autocrine autoimmune basal ganglion bone turnover calcilytic calcimimetic calcitonin Calcitriol Calcium carbonate
TERM 24-hour urine acidosis acquired aemia (prefix) albumin alkalosis anemia antibodies antigen autocrine autoimmune basal ganglion bone turnover calcilytic calcimimetic calcitonin Calcitriol Calcium carbonate
Calcium Nephrolithiasis and Bone Health. Noah S. Schenkman, MD
 Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Parathyroid hormone (serum, plasma)
 Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
Acid-Base Balance 11/18/2011. Regulation of Potassium Balance. Regulation of Potassium Balance. Regulatory Site: Cortical Collecting Ducts.
 Influence of Other Hormones on Sodium Balance Acid-Base Balance Estrogens: Enhance NaCl reabsorption by renal tubules May cause water retention during menstrual cycles Are responsible for edema during
Influence of Other Hormones on Sodium Balance Acid-Base Balance Estrogens: Enhance NaCl reabsorption by renal tubules May cause water retention during menstrual cycles Are responsible for edema during
Instrumental determination of electrolytes in urine. Amal Alamri
 Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
CALCIUM AND THYROID METABOLISM. Westmead Primary Exam Group
 CALCIUM AND THYROID METABOLISM Westmead Primary Exam Group THYROID HORMONES Chemistry - principle hormones are: T3 (Triiodothyronine) Can be formed in peripheral tissues by de-iodination of T4 T3 is more
CALCIUM AND THYROID METABOLISM Westmead Primary Exam Group THYROID HORMONES Chemistry - principle hormones are: T3 (Triiodothyronine) Can be formed in peripheral tissues by de-iodination of T4 T3 is more
Hyperparathyroidism. There is however another more potent method to achieve the lowering of PTH in a more natural way.
 Hyperparathyroidism Old Theory The parathyroid glands maintain proper levels of both calcium and phosphorus in your body by turning the secretion of parathyroid hormone (PTH) off or on, much like a thermostat
Hyperparathyroidism Old Theory The parathyroid glands maintain proper levels of both calcium and phosphorus in your body by turning the secretion of parathyroid hormone (PTH) off or on, much like a thermostat
25/10/56. Hypothyroidism Myxedema in adults Cretinism congenital deficiency of thyroid hormone Hashimoto thyroiditis. Simple goiter (nontoxic goiter)
 THERAPEUTIC USES OF THYROID HORMONE Supeecha Wittayalertpunya Wannarasmi Ketchart Nov 2013 Hyperthyroidism (Thyrotoxicosis) Grave s disease (diffuse toxic goiter) Toxic uninodular & Toxic multinodular
THERAPEUTIC USES OF THYROID HORMONE Supeecha Wittayalertpunya Wannarasmi Ketchart Nov 2013 Hyperthyroidism (Thyrotoxicosis) Grave s disease (diffuse toxic goiter) Toxic uninodular & Toxic multinodular
Hyperparathyroidism. When to Suspect, How to Diagnose, When and How to Intervene. Johanna A. Pallotta, MD, FACP, FACE
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
Index. B BMC. See Bone mineral content BMD. See Bone mineral density Bone anabolic impact, Bone mass acquisition
 A Acid base balance dietary protein detrimental effects of, 19 Acid base balance bicarbonate effects, 176 in bone human studies, 174 mechanisms, 173 174 in muscle aging, 174 175 alkali supplementation
A Acid base balance dietary protein detrimental effects of, 19 Acid base balance bicarbonate effects, 176 in bone human studies, 174 mechanisms, 173 174 in muscle aging, 174 175 alkali supplementation
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE
 Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Skeletal. Parathyroid hormone-related protein Analyte Information
 Skeletal Parathyroid hormone-related protein Analyte Information 1 2012-04-04 Parathyroid hormone related protein (PTHrP) Introduction Parathyroid hormone-related protein (PTHrP) is actually a family of
Skeletal Parathyroid hormone-related protein Analyte Information 1 2012-04-04 Parathyroid hormone related protein (PTHrP) Introduction Parathyroid hormone-related protein (PTHrP) is actually a family of
Safety Profile of Viread and Truvada. Ian McGowan, MD PhD FRCP Cape Town MTN Regional Meeting September, 2008
 Safety Profile of Viread and Truvada Ian McGowan, MD PhD FRCP Cape Town MTN Regional Meeting September, 2008 Overview Safety assessment in drug development Physiology 101 Renal Bone Liver Safety profile
Safety Profile of Viread and Truvada Ian McGowan, MD PhD FRCP Cape Town MTN Regional Meeting September, 2008 Overview Safety assessment in drug development Physiology 101 Renal Bone Liver Safety profile
The Endocrine System
 The Endocrine System The nervous system allows the body to respond to various stimuli in a quick manner and this allows for homeostasis. The endocrine system, using hormones also allows the body to respond
The Endocrine System The nervous system allows the body to respond to various stimuli in a quick manner and this allows for homeostasis. The endocrine system, using hormones also allows the body to respond
CAYUGA COMMUNITY COLLEGE Division of Computer Science, Mechanical Technology, Electrical Technology, GIS, Math, Nursing, Science
 CAYUGA COMMUNITY COLLEGE Division of Computer Science, Mechanical Technology, Electrical Technology, GIS, Math, Nursing, Science Anatomy and Physiology II - Biology 204 4 Credit Hours CATALOG DESCRIPTION
CAYUGA COMMUNITY COLLEGE Division of Computer Science, Mechanical Technology, Electrical Technology, GIS, Math, Nursing, Science Anatomy and Physiology II - Biology 204 4 Credit Hours CATALOG DESCRIPTION
BEC FEED SOLUTIONS NEW ZEALAND Ltd
 BEC FEED SOLUTIONS NEW ZEALAND Ltd Proudly sponsor Dr Alessandro Mereu Yara Feed Phosphates July 2017 NZARN Meeting www.becfeed.co.nz Phosphorus metabolism in cattle: principles and interactions with Ca
BEC FEED SOLUTIONS NEW ZEALAND Ltd Proudly sponsor Dr Alessandro Mereu Yara Feed Phosphates July 2017 NZARN Meeting www.becfeed.co.nz Phosphorus metabolism in cattle: principles and interactions with Ca
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Inpatient Pediatric Endocrinology. Tala Dajani MD MPH Pediatric Endocrinology of Phoenix
 Inpatient Pediatric Endocrinology Tala Dajani MD MPH Pediatric Endocrinology of Phoenix Objectives Identify calcium disorders in the hospital Distinguish between temporary versus permanent glucose problems
Inpatient Pediatric Endocrinology Tala Dajani MD MPH Pediatric Endocrinology of Phoenix Objectives Identify calcium disorders in the hospital Distinguish between temporary versus permanent glucose problems
9.2 Hormonal Regulation of Growth
 9.2 Hormonal Regulation of Growth Hormonal Regulation of Growth Pituitary gland regulates growth and development Thyroid gland regulates metabolic rate (exception: some hormones for growth and development)
9.2 Hormonal Regulation of Growth Hormonal Regulation of Growth Pituitary gland regulates growth and development Thyroid gland regulates metabolic rate (exception: some hormones for growth and development)
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance
 Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD
 The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
MINERAL IMBALANCE, ENDOCRINES AND HAIR TISSUE MINERAL ANALYSIS
 VOLUME 6 JUNE/JULY 1993 NUMBER 2 MINERAL IMBALANCE, ENDOCRINES AND HAIR TISSUE MINERAL ANALYSIS ----- David L. Watts, Ph.D., Director of Research ----------------------------------------------------------------------------------------
VOLUME 6 JUNE/JULY 1993 NUMBER 2 MINERAL IMBALANCE, ENDOCRINES AND HAIR TISSUE MINERAL ANALYSIS ----- David L. Watts, Ph.D., Director of Research ----------------------------------------------------------------------------------------
Water, Electrolytes, and Acid-Base Balance
 Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Drugs Affecting Bone. Rosa McCarty PhD. Department of Pharmacology & Therapeutics
 Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Electrolyte Disorders in ICU. Debashis Dhar
 Electrolyte Disorders in ICU Debashis Dhar INTRODUCTION Monovalent ions most important Na,K main cations and Cl &HCO - 3 main anions Mg,Ca & Phosphate are major divalent ions Normal Physiology Body tries
Electrolyte Disorders in ICU Debashis Dhar INTRODUCTION Monovalent ions most important Na,K main cations and Cl &HCO - 3 main anions Mg,Ca & Phosphate are major divalent ions Normal Physiology Body tries
Chapter 24 Water, Electrolyte and Acid-Base Balance
 Chapter 24 Water, Electrolyte and Acid-Base Balance Total body water for 150 lb. male = 40L 65% ICF 35% ECF 25% tissue fluid 8% blood plasma, lymph 2% transcellular fluid (CSF, synovial fluid) Water Movement
Chapter 24 Water, Electrolyte and Acid-Base Balance Total body water for 150 lb. male = 40L 65% ICF 35% ECF 25% tissue fluid 8% blood plasma, lymph 2% transcellular fluid (CSF, synovial fluid) Water Movement
Parathyoid glands and PTH
 Parathyoid glands and PTH They are four glands located behind the thyroid gland, each one from (20-50) mg in weight, and composed of two types of cells: 1. Cheif cells: that produces PTH. 2-oxyphil cells:
Parathyoid glands and PTH They are four glands located behind the thyroid gland, each one from (20-50) mg in weight, and composed of two types of cells: 1. Cheif cells: that produces PTH. 2-oxyphil cells:
Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis
 Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis Tutorial for Specialist Portfolio Biomedical Scientists 03/02/2014 Dr Petros Kampanis Clinical Scientist 1. Calcium Most abundant
Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis Tutorial for Specialist Portfolio Biomedical Scientists 03/02/2014 Dr Petros Kampanis Clinical Scientist 1. Calcium Most abundant
Thyroid Hormones and Lipid Profile Changes during Hemodialysis in CKD Cases of Libya
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. II (Nov. 2015), PP 73-81 www.iosrjournals.org Thyroid Hormones and Lipid Profile Changes
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. II (Nov. 2015), PP 73-81 www.iosrjournals.org Thyroid Hormones and Lipid Profile Changes
The Role of the Laboratory in Metabolic Bone Disease
 The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
JOURNAL OF INTERNATIONAL ACADEMIC RESEARCH FOR MULTIDISCIPLINARY Impact Factor 1.393, ISSN: , Volume 2, Issue 7, August 2014
 HYPOVITAMINOSIS D IN INDIAN FEMALES WITH POSTMENOPAUSAL OSTEOPOROSIS DR. SHAH WALIULLAH 1 DR. VINEET SHARMA 2 DR. R N SRIVASTAVA 3 DR. YASHODHARA PRADEEP 4 DR. A A MAHDI 5 DR. SANTOSH KUMAR 6 1 Research
HYPOVITAMINOSIS D IN INDIAN FEMALES WITH POSTMENOPAUSAL OSTEOPOROSIS DR. SHAH WALIULLAH 1 DR. VINEET SHARMA 2 DR. R N SRIVASTAVA 3 DR. YASHODHARA PRADEEP 4 DR. A A MAHDI 5 DR. SANTOSH KUMAR 6 1 Research
Renal Physiology. April, J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine.
 Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Therapeutic golas in the treatment of CKD-MBD
 Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients. Int.J.Curr.Res.Aca.Rev.2016; 4(11):
 Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
Osteoporosis. When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of.
 Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS
 OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
CALCIUM BALANCE. James T. McCarthy & Rajiv Kumar
 CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
CHAPTER 27 LECTURE OUTLINE
 CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Trebeculae. Step 4. compact bone. Diploë Pearson Education, Inc.
 Trebeculae compact bone Step 4 Diploë Abnormalities in bone growth Fibrodysplasia ossificans progressiva (FOP) autosomal dominant, Codon 206: Arg à Hist 1 : 2, 000, 000 endothelial cells à mesenchymal
Trebeculae compact bone Step 4 Diploë Abnormalities in bone growth Fibrodysplasia ossificans progressiva (FOP) autosomal dominant, Codon 206: Arg à Hist 1 : 2, 000, 000 endothelial cells à mesenchymal
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Serum and urinary calcium levels in Type 2 diabetes mellitus
 Original article: Serum and urinary calcium levels in Type 2 diabetes mellitus Goutam Chakraborti 1, Sandip Chakraborti 2 * 1 Associate Professor, Biochemistry, Murshidabad medical college and hospital,
Original article: Serum and urinary calcium levels in Type 2 diabetes mellitus Goutam Chakraborti 1, Sandip Chakraborti 2 * 1 Associate Professor, Biochemistry, Murshidabad medical college and hospital,
Research Article. Study of serum apolipoprotein A1 and HDL cholesterol in subclinical hypothyroidism
 Available online www.jocpr.com Journal of Chemical and Pharmaceutical Research, 216, 8(7):767-771 Research Article ISSN : 975-7384 CODEN(USA) : JCPRC5 Study of serum apolipoprotein A1 and HDL cholesterol
Available online www.jocpr.com Journal of Chemical and Pharmaceutical Research, 216, 8(7):767-771 Research Article ISSN : 975-7384 CODEN(USA) : JCPRC5 Study of serum apolipoprotein A1 and HDL cholesterol
Thyroid Function Abnormalities in Patients with Chronic Kidney Disease - A Prospective Study
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/338 Thyroid Function Abnormalities in Chronic Kidney Disease - A Prospective Study Aarathy Kannan 1, V Sriramakrishnan
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/338 Thyroid Function Abnormalities in Chronic Kidney Disease - A Prospective Study Aarathy Kannan 1, V Sriramakrishnan
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
POLYTECHNIC OF NAMIBIA SCHOOL OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES BIOMEDICAL SCIENCES PROGRAMME
 セ @セ @ POLYTECHNIC OF NAMIBIA SCHOOL OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES BIOMEDICAL SCIENCES PROGRAMME QUALIFICATION(S): Bachelor Of Biomedical Sciences QUALIFICATION CODE: 50BBMS
セ @セ @ POLYTECHNIC OF NAMIBIA SCHOOL OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES BIOMEDICAL SCIENCES PROGRAMME QUALIFICATION(S): Bachelor Of Biomedical Sciences QUALIFICATION CODE: 50BBMS
Elecsys bone marker panel. Optimal patient management starts in the laboratory
 bone marker panel Optimal patient management starts in the laboratory Complete solution for osteoporosis The most complete bone metabolism panel on a single platform bone marker assays are important diagnostic
bone marker panel Optimal patient management starts in the laboratory Complete solution for osteoporosis The most complete bone metabolism panel on a single platform bone marker assays are important diagnostic
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
SKELETAL SYSTEM CHAPTER 07. Bone Function BIO 211: ANATOMY & PHYSIOLOGY I. Body Movement interacts with muscles bones act as rigid bar of a lever
 Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
SKELETAL SYSTEM CHAPTER 07 BIO 211: ANATOMY & PHYSIOLOGY I
 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI Page 1 Page 2 syndrome of inappropriate secretion of antidiuretic hormone in malignancy
DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI Page 1 Page 2 syndrome of inappropriate secretion of antidiuretic hormone in malignancy
Body water content. Fluid compartments. Regulation of water output. Water balance and ECF osmolallty. Regulation of water intake
 Body water content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; females 50% This difference reflects
Body water content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; females 50% This difference reflects
Thyroid dysfunctions in patients with chronic renal failure
 International Journal of Research in Medical Sciences Pakhle K et al. Int J Res Med Sci. 2017 Jun;5(6):2773-2778 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20172485
International Journal of Research in Medical Sciences Pakhle K et al. Int J Res Med Sci. 2017 Jun;5(6):2773-2778 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20172485
TOMOFUSA USUI M.D.* information has been available on zinc status in. thyroid disease. The present study was undertaken
 Postgraduate Medical Journal (December 198) 56, 833-837 YOSHIKAZU NISHI M.D.* Zinc metabolism in thyroid disease TOMOFUSA USUI M.D.* RYOSO KAWATE M.D.t *Department of Pediatrics, and tdepartment of Internal
Postgraduate Medical Journal (December 198) 56, 833-837 YOSHIKAZU NISHI M.D.* Zinc metabolism in thyroid disease TOMOFUSA USUI M.D.* RYOSO KAWATE M.D.t *Department of Pediatrics, and tdepartment of Internal
1. remove: waste products: urea, creatinine, and uric acid foreign chemicals: drugs, water soluble vitamins, and food additives, etc.
 Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Regulation of the skeletal mass through the life span
 Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD
 Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD Reprinted with permission from: E-Medicine: Instant Access to the Minds of Medicine http://www.emedicine.com/emerg/topic276.htm
Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD Reprinted with permission from: E-Medicine: Instant Access to the Minds of Medicine http://www.emedicine.com/emerg/topic276.htm
Thyroid, antithyroid, parathyroid & Calcium metabolism. Suharti K Suherman Dept. of Pharmacology & Therapeutic Medical Faculty, Univ.
 Thyroid, antithyroid, parathyroid & Calcium metabolism Suharti K Suherman Dept. of Pharmacology & Therapeutic Medical Faculty, Univ. of Indonesia Thyroid secreted by thyroid gland source of 2 different
Thyroid, antithyroid, parathyroid & Calcium metabolism Suharti K Suherman Dept. of Pharmacology & Therapeutic Medical Faculty, Univ. of Indonesia Thyroid secreted by thyroid gland source of 2 different
Journal of Medical Science & Technology
 Journal of Medical Science & Technology Original research Reference Intervals For Serum Creatinine In Nepal. Open Access Sushil Kumar 1, Roshan Takhelmayum 2, Athokpam Rajendra Singh 3, Jitendra Narayan
Journal of Medical Science & Technology Original research Reference Intervals For Serum Creatinine In Nepal. Open Access Sushil Kumar 1, Roshan Takhelmayum 2, Athokpam Rajendra Singh 3, Jitendra Narayan
Associations Between Liver Function, Bone Turnover Biomarkers and Adipokines in Older Patients With Hip Fracture
 Elmer ress Original Article J Endocrinol Metab. 2014;4(5-6):121-135 Associations Between Liver Function, Bone Turnover Biomarkers and Adipokines in Older Patients With Hip Fracture Leon Fisher a, d, Alexander
Elmer ress Original Article J Endocrinol Metab. 2014;4(5-6):121-135 Associations Between Liver Function, Bone Turnover Biomarkers and Adipokines in Older Patients With Hip Fracture Leon Fisher a, d, Alexander
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Hypercalcemia. Hypercalcemia: When to Worry, When to Treat! Mineral Metabolism : A Short Course
 Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
SERUM PHOSPHORUS TESTING
 MEDICAL POLICY For use with the UnitedHealthcare Laboratory Benefit Management Program, administered by BeaconLBS SERUM PHOSPHORUS TESTING Policy Number: CMP - 035 Effective Date: January 21, 2017 Table
MEDICAL POLICY For use with the UnitedHealthcare Laboratory Benefit Management Program, administered by BeaconLBS SERUM PHOSPHORUS TESTING Policy Number: CMP - 035 Effective Date: January 21, 2017 Table
DR. SHAMSUL AZAHARI ZAINAL BADARI DEPARTMENT OF RESOURCES MANAGEMENT AND CONSUMER STUDIES FACULTY OF HUMAN ECOLOGY UPM
 DR. SHAMSUL AZAHARI ZAINAL BADARI DEPARTMENT OF RESOURCES MANAGEMENT AND CONSUMER STUDIES FACULTY OF HUMAN ECOLOGY UPM Mineral nutrients are inorganic elements found in food which the body cannot synthesis.
DR. SHAMSUL AZAHARI ZAINAL BADARI DEPARTMENT OF RESOURCES MANAGEMENT AND CONSUMER STUDIES FACULTY OF HUMAN ECOLOGY UPM Mineral nutrients are inorganic elements found in food which the body cannot synthesis.
THE RENAL HANDLING OF PHOSPHATE IN THYROID DISEASE
 THE RENAL HANDLING OF PHOSPHATE IN THYROID DISEASE B. MALAMOS, P. SFIKAKIS and P. PANDOS Department of Clinical Therapeutics of the Athens Medical School, Alexandra Hospital, Athens, Greece (Received 18
THE RENAL HANDLING OF PHOSPHATE IN THYROID DISEASE B. MALAMOS, P. SFIKAKIS and P. PANDOS Department of Clinical Therapeutics of the Athens Medical School, Alexandra Hospital, Athens, Greece (Received 18
Chapter 6: SKELETAL SYSTEM
 Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
PARATHYROID, VITAMIN D AND BONE
 PARATHYROID, VITAMIN D AND BONE G M Kellerman Pathology North Hunter Service 30/01/2015 BIOLOGY OF BONE Bone consists of protein, polysaccharide components and mineral matrix. The mineral is hydroxylapatite,
PARATHYROID, VITAMIN D AND BONE G M Kellerman Pathology North Hunter Service 30/01/2015 BIOLOGY OF BONE Bone consists of protein, polysaccharide components and mineral matrix. The mineral is hydroxylapatite,
REGULATION OF CALCIUM AND PHOSPHATE HOMEOSTASIS
 REGULATION OF CALCIUM AND PHOSPHATE HOMEOSTASIS Linda S. Costanzo Virginia Commonwealth University, Medical College of Virginia, Richmond, Virginia 23298 Teaching Ca 2 and phosphate homeostasis in a physiology
REGULATION OF CALCIUM AND PHOSPHATE HOMEOSTASIS Linda S. Costanzo Virginia Commonwealth University, Medical College of Virginia, Richmond, Virginia 23298 Teaching Ca 2 and phosphate homeostasis in a physiology
Endocrine System. Modified by M. Myers
 Endocrine System Modified by M. Myers 1 The Endocrine System 2 Endocrine Glands The endocrine system is made of glands & tissues that secrete hormones. Hormones are chemicals messengers influencing a.
Endocrine System Modified by M. Myers 1 The Endocrine System 2 Endocrine Glands The endocrine system is made of glands & tissues that secrete hormones. Hormones are chemicals messengers influencing a.
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues
 An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
Lab 14 Endocrine System
 Lab 14 Endocrine System Laboratory Objectives Identify the location of the primary endocrine organs. List the hormones produced by the endocrine organs. Relate the mechanisms of up-regulation and down-regulation
Lab 14 Endocrine System Laboratory Objectives Identify the location of the primary endocrine organs. List the hormones produced by the endocrine organs. Relate the mechanisms of up-regulation and down-regulation
Rahaf AL-Jafari. Marah Qaddourah. Rahmeh Abdullah. Saleem. 1 P a g e
 15 Rahaf AL-Jafari Marah Qaddourah Rahmeh Abdullah Saleem 1 P a g e If you are following with the record you may notice a little bit difference in information sequences. Hormones that function on growth
15 Rahaf AL-Jafari Marah Qaddourah Rahmeh Abdullah Saleem 1 P a g e If you are following with the record you may notice a little bit difference in information sequences. Hormones that function on growth
