Myopathy with anti-hmgcr antibodies: Perimysium and myofiber pathology
|
|
|
- Jodie Adams
- 5 years ago
- Views:
Transcription
1 Washington University School of Medicine Digital Open Access Publications 2015 Myopathy with anti-hmgcr antibodies: Perimysium and myofiber pathology Ali Alshehri Washington University School of Medicine Rati Choksi Washington University School of Medicine Robert Bucelli Washington University School of Medicine Alan Pestronk Washington University School of Medicine Follow this and additional works at: Recommended Citation Alshehri, Ali; Choksi, Rati; Bucelli, Robert; and Pestronk, Alan,,"Myopathy with anti-hmgcr antibodies: Perimysium and myofiber pathology." Neurol Neuroimmunol Neuroinflamm.2,4. e124. (2015). This Open Access Publication is brought to you for free and open access by Digital It has been accepted for inclusion in Open Access Publications by an authorized administrator of Digital For more information, please contact
2 Myopathy with anti-hmgcr antibodies Perimysium and myofiber pathology Ali Alshehri, MD Rati Choksi, MS Robert Bucelli, MD, PhD Alan Pestronk, MD Correspondence to Dr. Pestronk: ABSTRACT Objective: To analyze clinical features and myopathology changes in muscle fibers, connective tissue, and vessels in 3-hydroxy-3-methylglutaryl-coenzyme A reductase (HMGCR) antibody associated myopathies. Methods: Retrospective review of records and myopathologic features of 49 consecutive patients with myopathies and serum HMGCR antibodies. Results: Clinical features included onset age from 12 to 83 years, female predominance (67%), proximal, symmetric weakness (84%), muscle discomfort (78%), dysphagia (35%), systemic features, including skin rash and interstitial lung disease (37%), statin use (38%), and a high serum creatine kinase (83%). Myopathology included muscle fiber necrosis or regeneration (66%), myonuclear pathology (43%), perimysial connective tissue damage (61%), and lymphocytic foci (27%). Conclusions: Patients with HMGCR antibody associated myopathies present with weakness and muscle discomfort and often have damage to both perimysial connective tissue and muscle fibers, with necrosis and myonuclear pathology. Only a minority of patients with HMGCR antibody associated myopathies have a history of statin exposure. Neurol Neuroimmunol Neuroinflamm 2015;2:e124; doi: /NXI GLOSSARY CK 5 creatine kinase; HMGCR 5 3-hydroxy-3-methylglutaryl-coenzyme A reductase; IIM 5 immune and inflammatory myopathy; IMPP 5 immune myopathies with perimysial pathology; MHC 5 major histocompatibility complex; NGS 5 normal goat serum; PBS 5 phosphate-buffered saline. Serum autoantibodies and myopathology features are useful for characterization and classification of acquired immune and inflammatory myopathy (IIM) syndromes. 1 3 Serum IgG binding to 3-hydroxy-3-methylglutaryl-coenzyme A reductase (HMGCR) has been identified in patients with presumed immune myopathies that usually have no lymphocytic cell foci. 4,5 Myopathies with HMGCR antibodies have been suggested to be statin-induced, but statin histories are not universal and the strength of association with statin use varies among reports Previous pathologic descriptions of myopathies with HMGCR antibodies have noted active necrosis and regeneration of scattered muscle fibers without inflammation, 5 but some series mainly screened for HMGCR antibodies in groups of patients with necrotizing myopathies. 6 Involvement of other components of muscle tissue has not been systematically evaluated. We have found that IIM syndromes often have characteristic pathology that involves several tissues in muscle, including muscle fibers, connective tissue, and vessels, and patterns of humoral and cellular immunity. 3 In this study we evaluated clinical and pathologic features of 49 patients with acquired myopathies associated with serum IgG binding to HMGCR. Clinically, our patients had symmetric, proximal weakness and often had a high serum creatine kinase (CK). Only a minority had a history of statin use. Pathologic features in HMGCR antibody associated myopathies often include damage to both perimysial connective tissue and muscle fibers. From the Department of Neurology (A.A., R.C., R.B., A.P.) and Department of Pathology and Immunology (A.P.), Washington University School of Medicine, Saint Louis, MO. Funding information and disclosures are provided at the end of the article. Go to Neurology.org/nn for full disclosure forms. The Article Processing Charge was paid by the authors. This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivatives License 4.0 (CC BY- NC-ND), which permits downloading and sharing the work provided it is properly cited. The work cannot be changed in any way or used commercially. Neurology.org/nn 2015 American Academy of Neurology 1 ª 2015 American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
3 METHODS Patients. We retrospectively analyzed charts, laboratory records, and muscle biopsies from 49 patients with high levels of serum HMGCR antibodies (titers. 2,800). Muscle biopsies of 44 patients were evaluated at Washington University School of Medicine in Saint Louis. The presence and degree of myonuclear pathology were evaluated later by 2 different pathologists (A.P. and A.A.) in 40 available muscle biopsies. We tested 37 additional sera from patients with a definite diagnosis of inclusion body myositis. 11 Standard protocol approvals, registrations, and patient consents. The Human Studies Committee of Washington University in Saint Louis approved all procedures. Histochemical and immunohistochemical evaluation. Cryostat sections of rapidly frozen muscle were processed using the same methodology described in our previous studies. 12,13 Immunohistochemical stains for antibodies were performed on consecutive sections using muscle from patients and paired controls on the same glass slide. Primary antibodies used in this study were directed against HAM-56 (macrophages), CD8, CD4, CD20, C 5b-9 complement (membrane attack complex) (Sigma-Aldrich, St. Louis, MO), and class I human major histocompatibility complex (MHC) (US Biological, Swampscott, MA). Ulex Europaeus Agglutinin I lectin (Sigma-Aldrich) was used to visualize endothelium in vessels. Anti-HMGCR ELISA. HMGCR antigen (Sigma-H7039) (Sigma-Aldrich) was diluted to 2 mg/ml in 0.01 M phosphate-buffered saline (PBS). HMGCR 0.1 mg was placed in each well of Immulon 2 HB ELISA plates (Thermo Fisher Scientific, Waltham, MA) and incubated overnight at 4 C. After washing 3 times with PBS-0.05% Tween 20, residual nonspecific binding sites in ELISA wells were blocked with 1% normal goat serum in PBS (PBS-NGS) (100 ml per well) for 4 hours at room temperature and washed 3 times with PBS-NGS. Subsequent steps were performed at 4 C. Between steps, washing was performed 5 times using PBS-NGS without detergent. Patient sera were tested in duplicate at 1:3,000 dilution with overnight incubation in ELISA wells at 4 C. Binding of serum IgG to HMGCR was measured using a 4-hour exposure to goat anti-human IgG linked to horseradish peroxidase (Organon Teknika Cappel, West Chester, PA) in PBS with 1% bovine serum albumin (1:20,000). Color was developed with 100 ml substrate buffer (0.1 M citrate buffer, ph 4.5 with 0.004% H 2 O 2 and 0.1% phenylenediamine) for 30 minutes. Optical density was measured at 450 nm. Final anti-hmgcr antibody titers were calculated after subtracting levels of nonspecific serum IgG binding to sulfatide. A normal range of values was determined by analysis of sera from 85 adult patients with other immune or inflammatory neuromuscular disorders. Statistical analysis. Fisher exact test was used to compare categorical variables. Independent 2-tailed t test and mean 6 standard error were used to compare and report quantitative Figure 1 Muscle biopsy from a patient with a slowly progressive (24 years) HMGCR antibody associated myopathy syndrome (A) Hematoxylin & eosin stain, (B) Verhoeff-van Gieson stain. Muscle fiber size varies from very small to hypertrophied. Some small muscle fibers have mildly basophilic, or darkly stained, cytoplasm (white arrows). A few muscle fibers have internal nuclei. Endomysial connective tissue between muscle fibers is increased. (C) Alkaline phosphatase stains perimysial connective tissue and the cytoplasm of scattered small muscle fibers (white arrow). (D) Acid phosphatase stains scattered cells in the perimysium and cells associated with a necrotic muscle fiber (black arrow). Scale bar 5 50 mm for A, B, and D and 100 mm for C. HMGCR 5 3-hydroxy-3-methylglutaryl-coenzyme A reductase. 2 Neurology: Neuroimmunology & Neuroinflammation
4 Table Clinical features of HMGCR myopathy patients Table Continued Disease features Association Disease features Demographics Age at disease onset, y, mean 6 SE Association Perivascular Mononuclear cell foci 12/44 (27) B cells in foci 7/44 (16) Female 33/49 (67) Ethnicity Caucasian 37/49 (76) African 11/49 (22) Asian 1/49 (2) Clinical symptoms & signs Statin exposure 18/47 (38) Weakness, proximal 41/49 (84) Muscle discomfort 38/49 (78) Dysphagia 17/49 (35) Skin rash 12/49 (25) Dyspnea 15/49 (31) Interstitial lung disease 10/49 (20) Malignancy history 5/49 (10) Laboratory results Serum CK, mean 6 SE (% high) Serum aldolase, mean 6 SE (% high) HMGCR antibody titers, mean 6 SE 4, (83) (75) 12, ,367 ANA > 1:80 11/49 (23) Myositis-specific antibodies 16/49 (33) Synthetase 9/49 (18) Jo-1 7/49 (14) Other a 8/49 (16) EMG: Myopathic 32/43 (74) Irritable 28/43 (65) Muscle fibers Damage 32/44 (73) Necrosis 23/44 (52) C 5b-9 deposition (cytoplasm) 21/40 (53) Immaturity & regeneration 29/44 (66) Class I MHC upregulation (diffuse) 12/40 (30) Myonuclear pathology 17/40 (43) Perimysium Pathology 27/44 (61) Alkaline phosphatase staining Acid phosphatase & HAM56 cells 19/44 (43) 20/44 (45) Mononuclear cells 20/44 (45) C 5b-9 deposition 7/40 (18) Continued Abbreviations: ANA 5 antinuclear antibody; CK 5 creatine kinase; HMGCR 5 3-hydroxy-3-methylglutaryl-coenzyme A reductase; MHC 5 major histocompatibility complex. Data are n/n (%), unless otherwise indicated. a Signal recognition particle (#1), PM-Scl (#3), RNP (#5), Ku (#2), and SSA (#2). variables. A p value, 0.05 was considered a significant difference between groups. RESULTS Case report. A 26-year-old woman noted proximal weakness with onset shortly after the delivery of her first child that progressed over a few months to difficulty walking up and down stairs. There was no history of statin use or dyspnea. Examination showed symmetric, mild proximal weakness but no skin rash. Laboratory testing showed a myopathic EMG, a serum CK of 6,270 IU/L, and an antinuclear antibody titer of 1:320. Muscle biopsies (figure 1) at presentation and 8 years later showed increased endomysial connective tissue, many small- and moderate-sized basophilic muscle fibers, scattered necrotic fibers, and no foci of lymphocytic inflammation. Alkaline phosphatase diffusely stained the perimysium (figure 1C). Dystrophy-related protein staining and blots were normal for dystrophin, sarcoglycans, a-dystroglycan, dysferlin, desmin, emerin, calpain-3, caveolin-3, and laminin-a2. Gene testing was not performed. Oral treatments with high-dose prednisone, methotrexate, cyclosporine, and azathioprine produced no functional benefit. Myositis-specific antibody panels were negative on several occasions. Anti-HMGCR antibody titers were 34,000 in a serum sample obtained in 1991 and 48,000 in Weakness was slowly progressive. Twenty-three years after disease onset she required a scooter for mobility and could only walk 3 m with help. Quantitative testing showed strength that was 50% 60% of normal in proximal muscles in the arms and legs and normal in distal muscles. HMGCR antibodies. HMGCR antibody titers in our initial 49 patients ranged from 2,800 to 80,000. In the few patients with serial sera available, as in our case report, antibody titers showed no clear changes over long periods of time. A second patient evaluated over a very long period had titers of 7,000 at presentation, which included rapidly progressive severe weakness with respiratory failure, and 12,000 7 years later after chronic corticosteroid treatment that was associated with improvement to near-normal strength. Neurology: Neuroimmunology & Neuroinflammation 3 ª 2015 American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
5 Figure 2 Clinical characteristics. Patients with HMGCR antibodies included 33 females (67%) and 16 males (33%) (table). Mean age at disease onset was 50 years (range years). Ethnicities were Caucasian (76%), African American (22%), and Asian (2%). Neuromuscular symptoms included myalgia (78%) and dysphagia (35%). Weakness was present on examination in 84%. The 8 patients (16%) with no weakness reported muscle discomfort, cramps, or fasciculations. On examination, weakness was generally symmetric (98%) and proximal-greater-than-distal (100%). The course of disease progression ranged from subacute (progression to respiratory failure over 2 months) to chronic (slow progression over decades mimicking limb-girdle muscular dystrophies; see case report). Systemic features (37%) included skin rash affecting the face, chest, and dorsum of the hands (22%); interstitial lung disease (by chest imaging) (20%); and associated malignancy (10%) (pancreatic [2], colon, prostate, and hematologic). Statin use was reported in 38% of patients. Statin users were older (p ; mean 58 years) than nonusers (mean 44 years). The frequency of a history of statin use in our cohort was somewhat higher than, but not statistically different from, patients in an age-matched concurrent group with other immune myopathies (38% vs 23%; p 5 0.2). There were no differences in any clinical features between patients with or without statin exposure (table). Abnormal myofiber nuclei in HMGCR antibody associated myopathy Myonuclei are often enlarged (dark arrow) with clear centers (dark arrowhead) or irregular shapes (light arrowhead). Internal nuclei are common. Some myonuclei are in abnormal clusters or clumps (light arrows). Scale bar 5 18 mm. HMGCR 5 3-hydroxy-3-methylglutarylcoenzyme A reductase. Laboratory data. Anti-HMGCR antibody titers ranged from 2,800 to 80,000 (mean 12,606) and were similar in patients with and without statin exposure (table). Serum CK was high in 83% of our patients (mean 4,232 IU/L; range 26 to 27,000). Fifty percent of patients with normal strength had high serum CK (mean 447 IU/L; range 48 1,846). Patients with very high titers of anti-hmgcr antibodies ($6,000) had higher levels of serum CK (p ). Serum aldolase was high in 75% (mean 38 U/L; range ). Three patients with normal serum CK levels had a high aldolase. Other serum antibodies included antinuclear (22%), anti-synthetase (18% [Jo-1, 14%]), signal recognition particle (2%), and connective tissue disease overlap antibodies (PM- Scl, SSA, or RNP) (16%). EMG was often myopathic (74%), with fibrillation potentials and/or positive sharp waves in many (65%). Myopathology. Common myopathic features involved muscle fibers and perimysial connective tissue (table; figures 1 3). Muscle fiber pathology included evidence of ongoing damage, with fibers in varied stages of necrosis (52%) and regeneration or immaturity (66%) (figure 1). C 5b-9 complement stained the cytoplasm of some necrotic muscle fibers but was not typically deposited on the surface of non-necrotic muscle fibers. Large clusters of contiguous damaged fibers were not present. In some muscles, immature fibers and necrosis were most prominent at the edge of fascicles near damaged or cellular perimysial connective tissue (figure 3, C and F). Focal invasion of muscle fibers by cells was present in a few patients (7%). Myonuclear pathology (43%) (figure 2) included enlargement, irregular shapes, empty central regions, and clusters. Perimysial connective tissue pathology was present in 61% of biopsies, with diffuse alkaline phosphatase staining (figure 1C), histiocytic (acid phosphataseand esterase-positive) cells (figure 3, B and E), or damaged structure (figure 3D). The most common general pathologic pattern (57%; 25/44) was for both muscle fiber and perimysial pathology to be present. Muscles with neither muscle fiber nor perimysial pathology occurred in 25% (11/44). Weakness was more common (p ) in patients with perimysial damage (100%) than in those without perimysial damage (77%). Anti-HMGCR antibody titers were higher in patients with muscle biopsies showing muscle fiber necrosis (19, ,509 vs 6, ,249; p ) and connective tissue damage (17, ,998 vs 6, ,027; p ). Some biopsies contained lymphocytic cell foci (27%), generally surrounding intermediate-sized perimysial vessels. MHC class I was diffusely upregulated by all muscle fibers in some biopsies (30%). In some cases MHC class I expression was 4 Neurology: Neuroimmunology & Neuroinflammation
6 Figure 3 Perimysial and muscle fiber pathology in HMGCR antibody associated myopathy (A) Perimysial pathology with histiocytic cells and widening (hematoxylin & eosin stain). (B) Most cells in the perimysium are histiocytic and stain for acid phosphatase. (C) Muscle fibers at the edge of some fascicles are small and may be dark-stained (immature) (nicotinamide adenine dinucleotide stain). (D) Fragmentation of perimysial connective tissue (Gomori trichrome stain). (E) Cells in perimysial connective tissue are scattered, large, and irregularly shaped (nonspecific esterase stain). (F) Necrotic (dark) muscle fibers, with C 5b-9 complement staining of cytoplasm, are scattered through the muscle but may have increased frequency at the edge of fascicles, a feature common in immune myopathies with perimysial pathology. C 5b-9 complement is also deposited in perimysial connective tissue, occasionally extending into the endomysium. Scale bar mm for A, B, and D and 50 mm for C, E, and F. HMGCR 5 3-hydroxy-3-methylglutaryl-coenzyme A reductase. more prominent on fibers at the edge of fascicles near perimysium. There were no differences in biopsy features between patients with or without statin use. Endomysial connective tissue was increased in a few biopsies (8%), mostly in patients with longer histories of disease (figure 1). Vacuoles in muscle fibers were not observed. HMGCR antibodies in patients with inclusion body myositis. To evaluate the specificity of HMGCR antibodies for the myopathologic features identified in this study, we tested sera from 37 patients with definite inclusion body myositis, a group in whom we did not expect to detect positive results. We found 2 sera with high HMGCR antibody titers (2,900 and 8,400). Both patients also had serum IgG binding to NT5C1A antigen. The muscle pathology in these 2 patients showed changes consistent with inclusion body myositis, including vacuoles containing basophilic debris, endomysial foci of CD4 and CD8 lymphocytes with focal invasion of muscle fibers, and diffuse upregulation of MHC class I by muscle fibers. However, there were also scattered necrotic muscle fibers and perimysial connective tissue pathology (alkaline phosphatase staining and acid phosphatase positive cells), as noted above in other HMGCR antibody positive patients. Similar changes were found in only 2 of the 35 HMGCR antibody negative inclusion body myositis patients (p ). DISCUSSION We retrospectively reviewed clinical and myopathology features of 49 patients with serum anti-hmgcr antibodies. Some clinical features in our patients with serum IgG binding to HMGCR Neurology: Neuroimmunology & Neuroinflammation 5
7 were similar to those in previous studies. 5,6 We observed a moderate female predominance. Onset ages varied widely from childhood to older adulthood. Presenting features often included proximal, symmetric weakness, myalgia, and a high serum CK. The disease course varied from acute to very chronic. Three patients with slowly progressive proximal weakness were initially thought to have limb-girdle muscular dystrophies but had no histologic or molecular diagnosis despite extensive testing. Patients with previous exposure to statin drugs were older, but clinical and laboratory findings were similar to those in patients without statin exposure. Differences in our cohort from prior studies included a small group of HMGCR antibody patients who presented with myalgia, cramps, and elevated CK but no weakness. 14,15 Systemic manifestations, including skin rash and interstitial lung disease, were more frequent than previously reported. Interstitial lung disease, ascertained by chest imaging, was found in 20% of our cohort. Other myositis-associated antibodies were identified in 33% of our patients. The wider spectrum of clinical and laboratory features seen in our series likely reflects our inclusive pattern of serum testing (i.e., most patients with acquired myopathies). The initial series of HMGCR antibody patients excluded patients with inflammation in the muscle biopsy and selectively studied patients referred to a myositis clinic. 4 Another series analyzed only patients who had noninflammatory biopsies with active and prominent muscle fiber necrosis and regeneration. 6 Our data suggest that myopathies associated with HMGCR antibodies should not be called statin myopathies. Statin-intolerant patients with a clear temporal association between statin intake and symptoms have a very low frequency of HMGCR antibodies. 14 In all but one study, a substantial proportion of HMGCR antibody positive patients (37% to 62%) have been statin-naive. 5,6,16 In some HMGCR antibody positive patients, the statin exposure was years prior to the onset of myopathy. An Australian report is an outlier, finding that 94% of HMGCR antibody positive patients had statin exposure. 9 In this study the clinical correlations, including myopathy type and sex predominance, also differed from other reports. The initial focus of our study was to analyze the myopathology features of HMGCR antibody patients. Our results show that 2 components of muscle tissue are commonly involved: muscle fibers and connective tissue. Muscle fibers showed 2 patterns of pathology. Non-necrotic muscle fibers often had nuclear pathology with irregular shapes, enlargement, and aggregation (figure 2). This pattern of myopathology of uncertain cause is not common in most other myopathies with prominent necrosis. A study of myopathies associated with Jo-1 antibodies found nuclear actin aggregates in many patients. 17 The relationship between these nuclear aggregates and the myonuclear pathology seen on histologic sections in our study is unclear because ultrastructural analysis was not available. A second pattern of myofiber pathology is the scattered fibers in different stages of necrosis and regeneration that has been described in all previous studies of HMGCR antibody patients. This general pattern of scattered, ongoing muscle fiber necrosis is not specific for HMGCR antibody syndromes and is common in many immune and hereditary myopathies. 18 One distinctive feature of the distribution of the muscle fiber necrosis in some of our HMGCR antibody patients was a tendency for necrotic and regenerating fibers to be more common at the edge of fascicles near the perimysium. This distribution of necrosis occurs in immune myopathies with perimysial pathology (IMPP), such as those seen with Jo-1 antibodies. 12,17 The patterns of scattered necrosis differ from the clusters of muscle fibers in similar stages of necrosis seen in regional ischemic immune myopathy, which is likely due to vascular pathology. 19 The second area of muscle commonly involved in HMGCR antibody patients is connective tissue, especially the perimysium. Perimysial pathology with scattered histiocytic cells, alkaline phosphatase staining, and damaged structure (figures 1 and 3) was as common as muscle fiber necrosis in our HMGCR antibody patients. HMGCR antibody associated myopathology is similar to disorders in the IMPP pathologic group. 3 Damage to both perimysial connective tissue and muscle fibers is the most common pattern of myopathology in IMPP, Jo-1 antibody associated myopathies, and our HMGCR patients. The common types of muscle fiber damage in IMPP syndromes are necrosis and regeneration, which are more prominent in perifascicular regions near perimysium and nuclear pathology. 3,12,17 There is also some clinical overlap of features between IMPP syndromes and our patients. Systemic features present in 37% of our patient series included interstitial lung disease or a skin rash. Our myopathology results differ from previous descriptions of HMGCR patients, which have mainly emphasized the myopathy as necrotic. 5,6,9,10 One reason for this discrepancy is that some studies have biased their results by selecting patients based on the presence of muscle fiber necrosis. Another issue reducing reporting of perimysial damage may be that our pathology laboratory routinely performs histochemical analysis of muscle biopsies that includes acid and alkaline phosphatase stains. Acid and alkaline phosphatase stains are especially sensitive for 6 Neurology: Neuroimmunology & Neuroinflammation
8 observing cellular and molecular pathology in perimysial connective tissue. 3 They are not routinely performed in many laboratories and were not reported in previous HMGCR series. The specificity of HMGCR antibodies in immune and other myopathies requires further study. One series reported that HMGCR antibodies occur in 10% of patients with an entirely different disorder, inclusion body myositis. 9 Our initial results, identifying 49 antibodypositive patients, were at least partly the result of clinicians with a suspicion of an HMGCR antibody associated syndrome ordering serum testing. Our follow-up review of patients diagnosed with inclusion body myositis suggested a prevalence of 5.4%. However, review of themusclebiopsiesinthe2positivepatientsshowed perimysial connective tissue damage in addition to the typical inclusion body myositis pathology. It is wellknown that there is an increased frequency of associated immune features in inclusion body myositis, including antinuclear antibodies, SSA, and M proteins. 20,21 Clinically, the patients had features that were somewhat atypical for inclusion body myositis, including younger onset in the fifth decade and prominent proximal weakness early in the disease course. This suggests that these patients may have had 2 concurrent myopathy syndromes, inclusion body myositis and HMGCR antibody associated myopathology. HMGCR antibodies may correlate better with specific pathology features than with general clinical diagnoses. HMGCR antibody associated myopathies can be considered in the context of the common clinical classification and our proposed pathologic groups of immune myopathies. 3 Polymyositis and inclusion body myositis can be ruled out because there are few lymphocytic inflammatory foci or inclusion bodies in HMGCR myopathies. Dermatomyositis is not a useful diagnosis because skin changes were present in only a minority of our patients. Necrotic myopathies are a possible class within which to group HMGCR patients, but such a classification is misleading and lacks pathologic specificity. The term necrotic myopathy can be applied equally well to rhabdomyolysis and a variety of hereditary, ischemic, and toxic disorders. 18 Denoting the HMGCR syndrome as a necrotic myopathy implies that myofiber necrosis is a constant feature and that the disorder involves mainly damage to muscle fibers. However, connective tissue in perimysium is also commonly damaged in HMGCR myopathies. The connective tissue damage includes distinctive cellular mechanisms with histiocytic, not lymphocytic, infiltration. In muscles in which necrosis is present, the myopathic features are often nonuniform and more prominent near the perimysium. An additional non-necrotic muscle fiber pathology, abnormal myonuclear morphology, was also observed in many biopsies. The therapeutic response of some patients with HMGCR antibodies to immunomodulation supports the idea that these myopathies are autoimmune disorders. 4,6,22 The absence of lymphocytic inflammation suggests that humoral mechanisms may be important. However, despite the presence of serum autoantibodies, intracellular molecules such as HMGCR have been difficult to implicate as pathogenic target antigens of humoral or cellular immune mechanisms in immune disorders. The specific molecular antigenic targets of the immune response in muscle and connective tissue in HMGCR antibody associated myopathy remain to be defined. AUTHOR CONTRIBUTIONS Ali Alshehri: obtaining, analysis, and interpretation of the data, drafting and revising the manuscript. Rati Choksi: obtaining the data. Robert Bucelli: obtaining and interpretation of the data, revising the manuscript. Alan Pestronk: study design, obtaining, analysis, and interpretation of the data, revising the manuscript. STUDY FUNDING No targeted funding reported. DISCLOSURE A. Alshehri and R. Choksi report no disclosures. R. Bucelli received a financial gift from a patient s family for Parsonage-Turner research. A. Pestronk is on the scientific advisory board for The Myositis Association; holds patents and receives payments for TS-HDS antibody, GALOP antibody, GM1 Ganglioside antibody, and Sulfatide antibody; received speaker honoraria from Athena; is on the speakers bureau for The Myositis Association; received research support from Genzyme, Insmed, Knopp, Ultragenyx, ISIS, Sanofi, Cytokinetics, GSK, Biogen, CSL Behring, NIH, Washington University Neuromuscular Research Fund, CINRG Children s Hospital Washington DC, and Muscular Dystrophy Association; holds stock in Johnson & Johnson; and receives payments for antibody testing from Athena. Go to Neurology.org/nn for full disclosure forms. Received February 23, Accepted in final form May 1, REFERENCES 1. Hoogendijk J, Amato A, Lecky B, et al. 119th ENMC international workshop: trial design in adult idiopathic inflammatory myopathies, with the exception of inclusion body myositis, October 2003, Naarden, The Netherlands. Neuromuscul Disord 2004;14: Gunawardena H, Betteridge ZE, McHugh NJ. Myositisspecific autoantibodies: their clinical and pathogenic significance in disease expression. Rheumatology (Oxford) 2009;48: Pestronk A. Acquired immune and inflammatory myopathies: pathologic classification. Curr Opin Rheumatol 2011;23: Christopher-Stine L, Casciola-Rosen LA, Hong G, Chung T, Corse AM, Mammen AL. A novel autoantibody recognizing 200-kd and 100-kd proteins is associated with an immune-mediated necrotizing myopathy. Arthritis Rheum 2010;62: Mammen AL, Chung T, Christopher-Stine L, et al. Autoantibodies against 3-hydroxy-3-methylglutarylcoenzyme a reductase (HMGCR) in patients with statin-associated autoimmune myopathy. Arthritis Rheum 2011;63: Neurology: Neuroimmunology & Neuroinflammation 7
9 6. Allenbach Y, Drouot L, Rigolet A, et al. Anti-HMGCR autoantibodies in European patients with autoimmune necrotizing myopathies: inconstant exposure to statin. Medicine (Baltimore) 2014;93: Albayda J, Mammen AL. Is statin-induced myositis part of the polymyositis disease spectrum? Curr Rheumatol Rep 2014;16: Hamann PD, Cooper RG, McHugh NJ, Chinoy H. Statin-induced necrotizing myositis a discrete autoimmune entity within the statin-induced myopathy spectrum. Autoimmun Rev 2013;12: Limaye V, Bundell C, Hollingsworth P, et al. Clinical and genetic associations of autoantibodies to 3-hydroxy-3- methyl-glutaryl-coenzyme a reductase in patients with immune-mediated myositis and necrotizing myopathy. Muscle Nerve Epub 2014 Dec Watanabe Y, Suzuki S, Nishimura H, et al. Statins and myotoxic effects associated with anti-3-hydroxy-3- methylglutaryl-coenzyme a reductase autoantibodies: an observational study in Japan. Medicine (Baltimore) 2015;94:e Rose MR; ENMC IBM Working Group. 188th ENMC International Workshop: Inclusion Body Myositis, 2 4 December 2011, Naarden, The Netherlands. Neuromuscul Disord 2013;23: Mozaffar T, Pestronk A. Myopathy with anti-jo-1 antibodies: pathology in perimysium and neighbouring muscle fibres. J Neurol Neurosurg Psychiatry 2000;68: Miller T, Al-Lozi MT, Lopate G, Pestronk A. Myopathy with antibodies to the signal recognition particle: clinical and pathological features. J Neurol Neurosurg Psychiatry 2002;73: Mammen AL, Pak K, Williams EK, et al. Rarity of anti-3- hydroxy-3-methylglutaryl-coenzyme A reductase antibodies in statin users, including those with self-limited musculoskeletal side effects. Arthritis Care Res (Hoboken) 2012;64: Mohassel P, Mammen AL. The spectrum of statin myopathy. Curr Opin Rheumatol 2013;25: Drouot L, Allenbach Y, Jouen F, et al. Exploring necrotizing autoimmune myopathies with a novel immunoassay for anti-3-hydroxy-3-methyl-glutaryl-coa reductase autoantibodies. Arthritis Res Ther 2014;16:R Stenzel W, Preuße C, Allenbach Y, et al. Nuclear actin aggregation is a hallmark of anti-synthetase syndromeinduced dysimmune myopathy. Neurology 2015;84: Allenbach Y, Benveniste O. Acquired necrotizing myopathies. Curr Opin Neurol 2013;26: Cai C, Alshehri A, Choksi R, Pestronk A. Regional ischemic immune myopathy: a paraneoplastic dermatomyopathy. J Neuropathol Exp Neurol 2014;73: Koffman BM, Rugiero M, Dalakas MC. Immune-mediated conditions and antibodies associated with sporadic inclusion body myositis. Muscle Nerve 1998;21: Dalakas MC, Illa I, Gallardo E, Juarez C. Inclusion body myositis and paraproteinemia: incidence and immunopathologic correlations. Ann Neurol 1997;41: Werner JL, Christopher-Stine L, Ghazarian SR, et al. Antibody levels correlate with creatine kinase levels and strength in anti-hmg-coa reductase-associated autoimmune myopathy. Arthritis Rheum 2012;64: Neurology: Neuroimmunology & Neuroinflammation
10 Myopathy with anti-hmgcr antibodies: Perimysium and myofiber pathology Ali Alshehri, Rati Choksi, Robert Bucelli, et al. Neurol Neuroimmunol Neuroinflamm 2015;2; DOI /NXI This information is current as of June 4, 2015 Updated Information & Services References Subspecialty Collections Permissions & Licensing Reprints including high resolution figures, can be found at: This article cites 21 articles, 3 of which you can access for free at: This article, along with others on similar topics, appears in the following collection(s): Autoimmune diseases Muscle disease Information about reproducing this article in parts (figures,tables) or in its entirety can be found online at: Information about ordering reprints can be found online: Neurol Neuroimmunol Neuroinflamm is an official journal of the American Academy of Neurology. Published since April 2014, it is an open-access, online-only, continuous publication journal. Copyright 2015 American Academy of Neurology. All rights reserved. Online ISSN:
Idiopathic inflammatory myopathies excluding inclusion body myositis
 Idiopathic inflammatory myopathies excluding inclusion body myositis Marianne de Visser, Dept. of Neurology, Academic Medical Centre, Amsterdam, The Netherlands The idiopathic inflammatory myopathies (IIMs),
Idiopathic inflammatory myopathies excluding inclusion body myositis Marianne de Visser, Dept. of Neurology, Academic Medical Centre, Amsterdam, The Netherlands The idiopathic inflammatory myopathies (IIMs),
The many faces of myositis. Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands
 The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
 MURDOCH RESEARCH REPOSITORY This is the author s final version of the work, as accepted for publication following peer review but without the publisher s layout or pagination. The definitive version is
MURDOCH RESEARCH REPOSITORY This is the author s final version of the work, as accepted for publication following peer review but without the publisher s layout or pagination. The definitive version is
Identifying statin-associated autoimmune necrotizing myopathy
 REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will recognize autoimmune necrotizing myopathy if it occurs in their patients taking statins JEMIMA ALBAYDA, MD Division of Rheumatology, Department of
REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will recognize autoimmune necrotizing myopathy if it occurs in their patients taking statins JEMIMA ALBAYDA, MD Division of Rheumatology, Department of
Significance of antibody testing in idiopathic inflammatory myopathies
 2/0/20 Significance of antibody testing in idiopathic inflammatory myopathies Jiří Vencovský Institute of Rheumatology, Prague Diagnosis Polymyositis Juvenile DM (JPM) Paraneoplastic Myositis in overlap
2/0/20 Significance of antibody testing in idiopathic inflammatory myopathies Jiří Vencovský Institute of Rheumatology, Prague Diagnosis Polymyositis Juvenile DM (JPM) Paraneoplastic Myositis in overlap
Expression of anti-srp19 antibody in muscle tissues from patients with autoimmune necrotizing myopathy
 Expression of anti-srp19 antibody in muscle tissues from patients with autoimmune necrotizing myopathy Q. Wang 1, F. Duan 2, P. Liu 3, P.F. Wang 4 and M.X. Wang 5 1 EmergencyDepartment, General Hospital
Expression of anti-srp19 antibody in muscle tissues from patients with autoimmune necrotizing myopathy Q. Wang 1, F. Duan 2, P. Liu 3, P.F. Wang 4 and M.X. Wang 5 1 EmergencyDepartment, General Hospital
I mmune mediated and inflammatory myopathies are usually
 420 PAPER Myopathy with antibodies to the signal recognition particle: clinical and pathological features T Miller, M T Al-Lozi, G Lopate, A Pestronk... J Neurol Neurosurg Psychiatry 2002;73:420 428 See
420 PAPER Myopathy with antibodies to the signal recognition particle: clinical and pathological features T Miller, M T Al-Lozi, G Lopate, A Pestronk... J Neurol Neurosurg Psychiatry 2002;73:420 428 See
Case 1: History of J.H. Outside Evaluation. Outside Labs. Question #1
 Case 1: History of J.H. 64 yo man seen at UCSF 6-256 25-07. 9 months ago onset progressive weakness of arms and legs, with muscle atrophy in arms. 4 months ago red scaly rash on face, back of hands and
Case 1: History of J.H. 64 yo man seen at UCSF 6-256 25-07. 9 months ago onset progressive weakness of arms and legs, with muscle atrophy in arms. 4 months ago red scaly rash on face, back of hands and
Myopathy with anti-jo-1 antibodies: pathology in perimysium and neighbouring muscle fibres
 472 Department of Neurology, Washington University School of Medicine, St Louis, MO 63110, USA T MozaVar A Pestronk Correspondence to: Dr Alan Pestronk, Department of Neurology, Box 8111, 660 South Euclid
472 Department of Neurology, Washington University School of Medicine, St Louis, MO 63110, USA T MozaVar A Pestronk Correspondence to: Dr Alan Pestronk, Department of Neurology, Box 8111, 660 South Euclid
INCREASING INCIDENCE OF IMMUNE MEDIATED NECROTIZING MYOPATHY SINGLE CENTRE EXPERIENCE
 INCREASING INCIDENCE OF IMMUNE MEDIATED NECROTIZING MYOPATHY SINGLE CENTRE EXPERIENCE Martin Klein 1,2*, Heřman Mann 1,2*, Lenka Pleštilová 1,2, Josef Zámečník 3, Zoe Betteridge 4, Neil McHugh 4, Jiří
INCREASING INCIDENCE OF IMMUNE MEDIATED NECROTIZING MYOPATHY SINGLE CENTRE EXPERIENCE Martin Klein 1,2*, Heřman Mann 1,2*, Lenka Pleštilová 1,2, Josef Zámečník 3, Zoe Betteridge 4, Neil McHugh 4, Jiří
III./10.4. Diagnosis. Introduction. A.) Laboratory tests. Laboratory tests, electrophysiology, muscle biopsy, genetic testing, imaging techniques
 III./10.4. Diagnosis Laboratory tests, electrophysiology, muscle biopsy, genetic testing, imaging techniques After studying this chapter, you will become familiar with the most commonly used diagnostic
III./10.4. Diagnosis Laboratory tests, electrophysiology, muscle biopsy, genetic testing, imaging techniques After studying this chapter, you will become familiar with the most commonly used diagnostic
Autoantibodies andprognosis. Jiří Vencovský Institute of Rheumatology, Prague, Czech Republic
 Autoantibodies andprognosis Jiří Vencovský Institute of Rheumatology, Prague, Czech Republic HeterogeneityofIIMs Diagnosis Polymyositis Dermatomyositis IBM Necrotising myopathy Paraneoplastic Amyopathic
Autoantibodies andprognosis Jiří Vencovský Institute of Rheumatology, Prague, Czech Republic HeterogeneityofIIMs Diagnosis Polymyositis Dermatomyositis IBM Necrotising myopathy Paraneoplastic Amyopathic
This month, we are very pleased to introduce some new tests for Scleroderma as well as some test changes to our existing scleroderma tests/panels.
 February 20, 2017 Client Letter Test Update February 2017 Dear Colleague: This month, we are very pleased to introduce some new tests for Scleroderma as well as some test changes to our existing scleroderma
February 20, 2017 Client Letter Test Update February 2017 Dear Colleague: This month, we are very pleased to introduce some new tests for Scleroderma as well as some test changes to our existing scleroderma
IDIOPATHIC INFLAMMATORY MYOPATHIES AND RELATED DISORDERS. Franclo Henning Division of Neurology Tygerberg Hospital
 IDIOPATHIC INFLAMMATORY MYOPATHIES AND RELATED DISORDERS Franclo Henning Division of Neurology Tygerberg Hospital Classification systems Clinical (Bohan and Peter) Clinico-pathological (Dalakas & others)
IDIOPATHIC INFLAMMATORY MYOPATHIES AND RELATED DISORDERS Franclo Henning Division of Neurology Tygerberg Hospital Classification systems Clinical (Bohan and Peter) Clinico-pathological (Dalakas & others)
Autoantibodies in the Idiopathic Inflammatory Myopathies
 Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
4/16/2018. Demystifying weakness: how to approach refractory myositis. Objectives. Disclosures. Off-label uses for medications will be discussed
 Demystifying weakness: how to approach refractory myositis Jemima Albayda, MD Assistant Professor Johns Hopkins Myositis center Disclosures Off-label uses for medications will be discussed Objectives To
Demystifying weakness: how to approach refractory myositis Jemima Albayda, MD Assistant Professor Johns Hopkins Myositis center Disclosures Off-label uses for medications will be discussed Objectives To
UNICORNS, DRAGONS, POLYMYOSITIS AND OTHER MYTHOLOGICAL BEASTS: THE TRUTH ABOUT POLYMYOSITIS
 UNICORNS, DRAGONS, POLYMYOSITIS AND OTHER MYTHOLOGICAL BEASTS: THE TRUTH ABOUT POLYMYOSITIS Tahseen Mozaffar, MD University of California, Irvine Polymyositis is a commonly diagnosed condition in Neurology,
UNICORNS, DRAGONS, POLYMYOSITIS AND OTHER MYTHOLOGICAL BEASTS: THE TRUTH ABOUT POLYMYOSITIS Tahseen Mozaffar, MD University of California, Irvine Polymyositis is a commonly diagnosed condition in Neurology,
Muscle Pathology Surgical Pathology Unknown Conference. November, 2008 Philip Boyer, M.D., Ph.D.
 Muscle Pathology Surgical Pathology Unknown Conference November, 2008 Philip Boyer, M.D., Ph.D. Etiologic Approach to Differential Diagnosis Symptoms / Signs / Imaging / Biopsy / CSF Analysis Normal Abnormal
Muscle Pathology Surgical Pathology Unknown Conference November, 2008 Philip Boyer, M.D., Ph.D. Etiologic Approach to Differential Diagnosis Symptoms / Signs / Imaging / Biopsy / CSF Analysis Normal Abnormal
Budsakorn Darawankul, MD. Maharat Nakhon Ratchasima Hospital
 Budsakorn Darawankul, MD. Maharat Nakhon Ratchasima Hospital Outline What is ANA? How to detect ANA? Clinical application Common autoantibody in ANA diseases Outline What is ANA? How to detect ANA? Clinical
Budsakorn Darawankul, MD. Maharat Nakhon Ratchasima Hospital Outline What is ANA? How to detect ANA? Clinical application Common autoantibody in ANA diseases Outline What is ANA? How to detect ANA? Clinical
POLYMYOSITIS (PM) DERMATOMYOSITIS (DM) Body myositis Eosinophilic myositis Giant cell myositis Focal / localised myositis Myopathies caused by
 POLYMYOSITIS (PM) DERMATOMYOSITIS (DM) Body myositis Eosinophilic myositis Giant cell myositis Focal / localised myositis Myopathies caused by infections, drugs, toxins Definition Epidemiology Pathogenesis
POLYMYOSITIS (PM) DERMATOMYOSITIS (DM) Body myositis Eosinophilic myositis Giant cell myositis Focal / localised myositis Myopathies caused by infections, drugs, toxins Definition Epidemiology Pathogenesis
Tools to Aid in the Accurate Diagnosis of. Connective Tissue Disease
 Connective Tissue Disease Tools to Aid in the Accurate Diagnosis of Connective Tissue Disease Connective Tissue Disease High quality assays and novel tests Inova offers a complete array of assay methods,
Connective Tissue Disease Tools to Aid in the Accurate Diagnosis of Connective Tissue Disease Connective Tissue Disease High quality assays and novel tests Inova offers a complete array of assay methods,
Genetics of Inclusion Body Myositis
 Genetics of Inclusion Body Myositis Thomas Lloyd, MD, PhD Associate Professor of Neurology and Neuroscience Co-director, Johns Hopkins Myositis Center Sporadic IBM (IBM) Age at onset usually > 50 Prevalence
Genetics of Inclusion Body Myositis Thomas Lloyd, MD, PhD Associate Professor of Neurology and Neuroscience Co-director, Johns Hopkins Myositis Center Sporadic IBM (IBM) Age at onset usually > 50 Prevalence
Myosites du sujet âgé
 Myosites du sujet âgé Olivier Benveniste Département de Médecine Interne Centre de Référence Maladies Neuro-Musculaires Equipe Muscle Inflammatoire U974 Groupe Hospitalier Pitié-Salpêtrière Myositis classification
Myosites du sujet âgé Olivier Benveniste Département de Médecine Interne Centre de Référence Maladies Neuro-Musculaires Equipe Muscle Inflammatoire U974 Groupe Hospitalier Pitié-Salpêtrière Myositis classification
Diseases of Muscle and Neuromuscular Junction
 Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
Inflammatory Myopathies 4 th year MBBS. Marwan Adwan MBChB, MSc, MRCPI, MRCP(rheum) Consultant Rheumatologist
 Inflammatory Myopathies 4 th year MBBS Marwan Adwan MBChB, MSc, MRCPI, MRCP(rheum) Consultant Rheumatologist Case A 64 woman presents with erythematous itchy rash over back of hands & forehead. For 1 month
Inflammatory Myopathies 4 th year MBBS Marwan Adwan MBChB, MSc, MRCPI, MRCP(rheum) Consultant Rheumatologist Case A 64 woman presents with erythematous itchy rash over back of hands & forehead. For 1 month
Clinical Laboratory. 14:41:00 Complement Component 3 50 mg/dl Oct-18
 Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Thyroid Peroxidase (TPO) Antibody 5.0 IU/mL [0.0-9.0] 18-289-900139 16-Oct-18 Complement Component 3 50 mg/dl 18-289-900139
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Thyroid Peroxidase (TPO) Antibody 5.0 IU/mL [0.0-9.0] 18-289-900139 16-Oct-18 Complement Component 3 50 mg/dl 18-289-900139
Clinical Laboratory. [None
 Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Double-Stranded DNA (dsdna) Ab IgG ELISA Detected * [None 18-289-900151 Detected] Double-Stranded DNA (dsdna) Ab IgG
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Double-Stranded DNA (dsdna) Ab IgG ELISA Detected * [None 18-289-900151 Detected] Double-Stranded DNA (dsdna) Ab IgG
An autoimmune perspective on neuromuscular diseases
 An autoimmune perspective on neuromuscular diseases Colin Chalk MD,CM FRCPC Montreal General Hospital McGill University Schlomchik 2001 The proportion of neuromuscular patients who have an autoimmune cause
An autoimmune perspective on neuromuscular diseases Colin Chalk MD,CM FRCPC Montreal General Hospital McGill University Schlomchik 2001 The proportion of neuromuscular patients who have an autoimmune cause
Autoantibodies in Idiopathic Inflammatory Myopathies. Vidya Limaye Rheumatology Department Royal Adelaide Hospital
 Autoantibodies in Idiopathic Inflammatory Myopathies Vidya Limaye Rheumatology Department Royal Adelaide Hospital Idiopathic Inflammatory Myopathies (IIM) Heterogeneous group of systemic autoimmune syndromes
Autoantibodies in Idiopathic Inflammatory Myopathies Vidya Limaye Rheumatology Department Royal Adelaide Hospital Idiopathic Inflammatory Myopathies (IIM) Heterogeneous group of systemic autoimmune syndromes
Paraneoplastic necrotizing myopathy in association with metastatic malignant melanoma: two case reports and a review of the literature
 CASE REPORT Paraneoplastic necrotizing myopathy in association with metastatic malignant melanoma: two case reports and a review of the literature Molly S Peterson 1, Bjoern Buehring 2, Patrick S Rush
CASE REPORT Paraneoplastic necrotizing myopathy in association with metastatic malignant melanoma: two case reports and a review of the literature Molly S Peterson 1, Bjoern Buehring 2, Patrick S Rush
Amyloid neuropathy: (A) scattered Congo Red positive material in endoneurium displays apple green birefringence under polarized light.
 Cơ vân Cơ vân Cơ vân (cắt dọc) Amyloid neuropathy: (A) scattered Congo Red positive material in endoneurium displays apple green birefringence under polarized light. (A, Congo Red). Amyloid neuropathy:
Cơ vân Cơ vân Cơ vân (cắt dọc) Amyloid neuropathy: (A) scattered Congo Red positive material in endoneurium displays apple green birefringence under polarized light. (A, Congo Red). Amyloid neuropathy:
Rituximab Therapy for Myopathy Associated With Anti Signal Recognition Particle Antibodies: A Case Series
 Arthritis Care & Research Vol. 62, No. 9, September 2010, pp 1328 1334 DOI 10.1002/acr.20219 2010, American College of Rheumatology ORIGINAL ARTICLE Rituximab Therapy for Myopathy Associated With Anti
Arthritis Care & Research Vol. 62, No. 9, September 2010, pp 1328 1334 DOI 10.1002/acr.20219 2010, American College of Rheumatology ORIGINAL ARTICLE Rituximab Therapy for Myopathy Associated With Anti
*Pari Basharat ABSTRACT OVERVIEW OF IDIOPATHIC INFLAMMATORY MYOPATHIES
 IDIOPATHIC INFLAMMATORY MYOPATHIES: ASSOCIATION WITH OVERLAP MYOSITIS AND SYNDROMES: CLASSIFICATION, CLINICAL CHARACTERISTICS, AND ASSOCIATED AUTOANTIBODIES *Pari Basharat University of Western Ontario,
IDIOPATHIC INFLAMMATORY MYOPATHIES: ASSOCIATION WITH OVERLAP MYOSITIS AND SYNDROMES: CLASSIFICATION, CLINICAL CHARACTERISTICS, AND ASSOCIATED AUTOANTIBODIES *Pari Basharat University of Western Ontario,
1 DOS CME Course 2011
 Statin Myopathy February 23, 2011 Jinny Tavee, MD Associate Professor Neurological Institute Cleveland Clinic Foundation 1 Case 1 50 y/o woman with hyperlipidemia presents with one year history of deep
Statin Myopathy February 23, 2011 Jinny Tavee, MD Associate Professor Neurological Institute Cleveland Clinic Foundation 1 Case 1 50 y/o woman with hyperlipidemia presents with one year history of deep
CLINICAL AND LABORATORY FEATURES OF NEUROPATHIES WITH SERUM IgM BINDING TO TS-HDS
 CLINICAL AND LABORATORY FEATURES OF NEUROPATHIES WITH SERUM IgM BINDING TO TS-HDS ALAN PESTRONK, MD, 1,2 ROBERT E. SCHMIDT, MD, PhD, 2 RATI M. CHOKSI, MS, 1 R. BRIAN SOMMERVILLE, MD, 1 and MUHAMMAD T.
CLINICAL AND LABORATORY FEATURES OF NEUROPATHIES WITH SERUM IgM BINDING TO TS-HDS ALAN PESTRONK, MD, 1,2 ROBERT E. SCHMIDT, MD, PhD, 2 RATI M. CHOKSI, MS, 1 R. BRIAN SOMMERVILLE, MD, 1 and MUHAMMAD T.
Disorders of Muscle. Disorders of Muscle. Muscle Groups Involved in Myopathy. Needle Examination of EMG. History. Muscle Biopsy
 Disorders of Muscle Disorders of Muscle Zakia Bell, M.D. Associate Professor of Neurology and Physical Medicine & Rehabilitation Virginia Commonwealth University Cardinal symptom of diseases of the muscle
Disorders of Muscle Disorders of Muscle Zakia Bell, M.D. Associate Professor of Neurology and Physical Medicine & Rehabilitation Virginia Commonwealth University Cardinal symptom of diseases of the muscle
The spectrum of elderly myopathies in an Asian population
 Neurology Asia 2013; 18(2) : 177 181 The spectrum of elderly myopathies in an Asian population Shereen Ng, *Kum-Thong Wong FRCPath MD, Khean-Jin Goh FRCP Division of Neurology, Department of Medicine and
Neurology Asia 2013; 18(2) : 177 181 The spectrum of elderly myopathies in an Asian population Shereen Ng, *Kum-Thong Wong FRCPath MD, Khean-Jin Goh FRCP Division of Neurology, Department of Medicine and
Pathology of Neuromuscular Disease Part 1: muscle
 Pathology of Neuromuscular Disease Part 1: muscle Zarife Sahenk, MD. PhD. Research Institute at Nationwide Children s Hospital Center for gene therapy, Neuromuscular Program Experimental & Clinical Neuromuscular
Pathology of Neuromuscular Disease Part 1: muscle Zarife Sahenk, MD. PhD. Research Institute at Nationwide Children s Hospital Center for gene therapy, Neuromuscular Program Experimental & Clinical Neuromuscular
CLASSIFICATION OF PERIPHERAL NERVE DISEASES
 DIFFERENTIAL DIAGNOSIS OF NEUROGENIC DISORDERS & MYOPATHIES NEUROPATHY MYOPATHY Weakness distal proximal Sensory loss + 0 Loss of reflexes early late CSF protein elevated normal Electromyography neurogenic
DIFFERENTIAL DIAGNOSIS OF NEUROGENIC DISORDERS & MYOPATHIES NEUROPATHY MYOPATHY Weakness distal proximal Sensory loss + 0 Loss of reflexes early late CSF protein elevated normal Electromyography neurogenic
Electron microscopy in the investigation and diagnosis of muscle disease
 Electron microscopy in the investigation and diagnosis of muscle disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Muscle Normal Muscle The Sarcomere The names
Electron microscopy in the investigation and diagnosis of muscle disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Muscle Normal Muscle The Sarcomere The names
Rheumatology E-learning. University of Szeged Department of Rheumatology and Immunology
 Rheumatology E-learning University of Szeged Department of Rheumatology and Immunology Introduction Idiopathic inflammatory myopathies (IIM) are a group of systemic diseases characterized by an immune
Rheumatology E-learning University of Szeged Department of Rheumatology and Immunology Introduction Idiopathic inflammatory myopathies (IIM) are a group of systemic diseases characterized by an immune
Medicine. Observational Study OPEN
 Observational Study Medicine Atorvastatin-induced necrotizing autoimmune myositis An emerging dominant entity in patients with autoimmune myositis presenting with a pure polymyositis phenotype Yves Troyanov,
Observational Study Medicine Atorvastatin-induced necrotizing autoimmune myositis An emerging dominant entity in patients with autoimmune myositis presenting with a pure polymyositis phenotype Yves Troyanov,
CURRENT ESSENTIALS IN INFLAMMATORY MYOPATHIES
 CURRENT ESSENTIALS IN INFLAMMATORY MYOPATHIES Maren Breithaupt, 1 Jens Schmidt 1,2 1. Clinic for Neurology, University Medical Center Göttingen, Göttingen, Germany 2. Department of Neuroimmunology, Institute
CURRENT ESSENTIALS IN INFLAMMATORY MYOPATHIES Maren Breithaupt, 1 Jens Schmidt 1,2 1. Clinic for Neurology, University Medical Center Göttingen, Göttingen, Germany 2. Department of Neuroimmunology, Institute
Inflammatory muscle diseases.
 Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology 4-30-2015 Inflammatory muscle diseases. Marinos C Dalakas Department of Neurology, Neuromuscular
Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology 4-30-2015 Inflammatory muscle diseases. Marinos C Dalakas Department of Neurology, Neuromuscular
SCLERODERMA OVERLAP SYNDROME: A CASE REPORT Diwakar K. Singh 1, Nataraju H. V 2
 SCLERODERMA OVERLAP SYNDROME: A Diwakar K. Singh 1, Nataraju H. V 2 HOW TO CITE THIS ARTICLE: Diwakar K. Singh, Nataraju H. V. Scleroderma Overlap Syndrome: A Case Report. Journal of Evolution of Medical
SCLERODERMA OVERLAP SYNDROME: A Diwakar K. Singh 1, Nataraju H. V 2 HOW TO CITE THIS ARTICLE: Diwakar K. Singh, Nataraju H. V. Scleroderma Overlap Syndrome: A Case Report. Journal of Evolution of Medical
Long-term follow-up of sporadic inclusion body myositis treated with intravenous immunoglobulin: a retrospective study of 16 patients
 Long-term follow-up of sporadic inclusion body myositis treated with intravenous immunoglobulin: a retrospective study of 16 patients C. Dobloug, R. Walle-Hansen, J.T. Gran, Ø. Molberg Section of Rheumatology,
Long-term follow-up of sporadic inclusion body myositis treated with intravenous immunoglobulin: a retrospective study of 16 patients C. Dobloug, R. Walle-Hansen, J.T. Gran, Ø. Molberg Section of Rheumatology,
Myositis 101. Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic, Rochester, MN
 Myositis 101 Steven R. Ytterberg, M.D. Rheumatology Mayo Clinic, Rochester, MN Myositis Association Annual Conference Louisville, KY Sept. 6 & 7, 2018 Disclosures Consulting: Dynavax Pfizer Off-label use:
Myositis 101 Steven R. Ytterberg, M.D. Rheumatology Mayo Clinic, Rochester, MN Myositis Association Annual Conference Louisville, KY Sept. 6 & 7, 2018 Disclosures Consulting: Dynavax Pfizer Off-label use:
Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18
![Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18 Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18](/thumbs/95/125595183.jpg) Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Rheumatoid Factor
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Rheumatoid Factor
The Power of the ANA. April 2018 Emily Littlejohn, DO MPH
 Emergent Rheumatologic Diseases and Disorders for Primary Care. The Power of the ANA April 2018 Emily Littlejohn, DO MPH Question 1: the ANA test is: A) A screening test with high specificity to diagnose
Emergent Rheumatologic Diseases and Disorders for Primary Care. The Power of the ANA April 2018 Emily Littlejohn, DO MPH Question 1: the ANA test is: A) A screening test with high specificity to diagnose
SUPPLEMENTARY MATERIALS
 SUPPLEMENTARY MATERIALS Supplementary Table 1. Demographic and clinical characteristics of the primary Sjögren's syndrome patient cohort Number % Females/males 73/5 93.6/6.4 Age, median (range) years 65
SUPPLEMENTARY MATERIALS Supplementary Table 1. Demographic and clinical characteristics of the primary Sjögren's syndrome patient cohort Number % Females/males 73/5 93.6/6.4 Age, median (range) years 65
Contributed equally. Columbia, Vancouver BC, Canada. Hacettepe University Faculty of Medicine, Ankara, Turkey.
 DR PETER SCHUTZ (Orcid ID : 0000-0001-7962-1560) PROFESSOR THOMAS S JACQUES (Orcid ID : 0000-0002-7833-2158) Article type : Original Article HISTOLOGICAL HETEROGENEITY IN A LARGE CLINICAL COHORT OF JUVENILE
DR PETER SCHUTZ (Orcid ID : 0000-0001-7962-1560) PROFESSOR THOMAS S JACQUES (Orcid ID : 0000-0002-7833-2158) Article type : Original Article HISTOLOGICAL HETEROGENEITY IN A LARGE CLINICAL COHORT OF JUVENILE
Discovery, Understanding, and Progress in Myositis
 Discovery, Understanding, and Progress in Myositis Steven Ytterberg, M.D. TMA Annual Patient Conference New Orleans, LA Sept. 2, 2016 Disclosures Financial: Dynavax Corp. Pfizer Mallinckrodt American Board
Discovery, Understanding, and Progress in Myositis Steven Ytterberg, M.D. TMA Annual Patient Conference New Orleans, LA Sept. 2, 2016 Disclosures Financial: Dynavax Corp. Pfizer Mallinckrodt American Board
myopathy and interstitial lung dise
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case of primary Sjögren's syndrom myopathy and interstitial lung dise Koga, Tomohiro; Kouhisa, Yukiko; Na Akinari; Motomura, Masakatsu; Kawak
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case of primary Sjögren's syndrom myopathy and interstitial lung dise Koga, Tomohiro; Kouhisa, Yukiko; Na Akinari; Motomura, Masakatsu; Kawak
TMA San Diego September 7, 2017
 Myositis 101: Clinical Features, Diagnosis and Management Namita Goyal, MD Associate Professor of Neurology Director, Neuromuscular Medicine Fellowship Director, Neuromuscular Diagnostic Laboratory Associate
Myositis 101: Clinical Features, Diagnosis and Management Namita Goyal, MD Associate Professor of Neurology Director, Neuromuscular Medicine Fellowship Director, Neuromuscular Diagnostic Laboratory Associate
muscle biopsy How to do it
 How to do it muscle biopsy Gillian Hall Department of Clinical Neurosciences, Western General Hospital, Edinburgh EH4 2XU. Email: ghall@skull.dcn.ed.ac.uk INTRODUCTION Good clinical evaluation remains
How to do it muscle biopsy Gillian Hall Department of Clinical Neurosciences, Western General Hospital, Edinburgh EH4 2XU. Email: ghall@skull.dcn.ed.ac.uk INTRODUCTION Good clinical evaluation remains
Magnetic resonance imaging changes of thigh muscles in myopathy with antibodies to signal recognition particle
 RHEUMATOLOGY Rheumatology 2015;54:1017 1024 doi:10.1093/rheumatology/keu422 Advance Access publication 21 November 2014 Original article Magnetic resonance imaging changes of thigh muscles in myopathy
RHEUMATOLOGY Rheumatology 2015;54:1017 1024 doi:10.1093/rheumatology/keu422 Advance Access publication 21 November 2014 Original article Magnetic resonance imaging changes of thigh muscles in myopathy
Overview of Diagnostic Autoantibodies in Inflammatory Myopathy
 Overview of Diagnostic Autoantibodies in Inflammatory Myopathy Minoru Satoh, M.D., Ph.D. Research Associate Professor of Medicine Division of Rheumatology and Clinical Immunology University of Florida
Overview of Diagnostic Autoantibodies in Inflammatory Myopathy Minoru Satoh, M.D., Ph.D. Research Associate Professor of Medicine Division of Rheumatology and Clinical Immunology University of Florida
Idiopathic inflammatory myopathies
 Myositis and cancer Idiopathic inflammatory myopathies Primary idiopathic polymyositis Primary idiopathic dermatomyositis Juvenile poly/dermatomyositis Myositis associated with another CTD Myositis associated
Myositis and cancer Idiopathic inflammatory myopathies Primary idiopathic polymyositis Primary idiopathic dermatomyositis Juvenile poly/dermatomyositis Myositis associated with another CTD Myositis associated
Comparison of Performance of ELISA with Indirect Immunofluoresence for the Testing of Antinuclear Antibodies
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 12 (2016) pp. 423-427 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.512.046
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 12 (2016) pp. 423-427 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.512.046
Complex repetitive discharge on electromyography as a risk factor for malignancy in idiopathic inflammatory myopathy
 ORIGINAL ARTICLE Korean J Intern Med 2014;29:814-821 Complex repetitive discharge on electromyography as a risk factor for malignancy in idiopathic inflammatory myopathy Na Ri Kim 1, Eon Jeong Nam 1, Jong
ORIGINAL ARTICLE Korean J Intern Med 2014;29:814-821 Complex repetitive discharge on electromyography as a risk factor for malignancy in idiopathic inflammatory myopathy Na Ri Kim 1, Eon Jeong Nam 1, Jong
Chapter 5 Inclusion Body Myositis
 Chapter 5 Inclusion Body Myositis Lawrence J. Kagen Abstract Inclusion body myositis is an insidious, slowly progressive myopathy of middle-aged and older individuals. Because of these characteristics,
Chapter 5 Inclusion Body Myositis Lawrence J. Kagen Abstract Inclusion body myositis is an insidious, slowly progressive myopathy of middle-aged and older individuals. Because of these characteristics,
HUNGARIAN MYOSITIS COHORT
 CLINICAL ADVANCES OF ANTI- TIF1Γ AUTOANTIBODY IN A HUNGARIAN MYOSITIS COHORT Melinda Nagy-Vincze 1, Zoltán Griger 1, Levente Bodoki 1, Zsuzsa Szankai 1, Zoe E. Betteridge 2, Katalin Dankó 1 1 University
CLINICAL ADVANCES OF ANTI- TIF1Γ AUTOANTIBODY IN A HUNGARIAN MYOSITIS COHORT Melinda Nagy-Vincze 1, Zoltán Griger 1, Levente Bodoki 1, Zsuzsa Szankai 1, Zoe E. Betteridge 2, Katalin Dankó 1 1 University
Myositis and Your Lungs
 Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Citation The Journal of dermatology, 37(1), available at
 NAOSITE: Nagasaki University's Ac Title Author(s) Case of localized scleroderma assoc Muroi, Eiji; Ogawa, Fumihide; Yamao Sato, Shinichi Citation The Journal of dermatology, 37(1), Issue Date 2010-01 URL
NAOSITE: Nagasaki University's Ac Title Author(s) Case of localized scleroderma assoc Muroi, Eiji; Ogawa, Fumihide; Yamao Sato, Shinichi Citation The Journal of dermatology, 37(1), Issue Date 2010-01 URL
What your autoantibodies tell us about your disease. Mark Gourley, MD
 What your autoantibodies tell us about your disease Mark Gourley, MD The Importance of the Immune System Defends us against foreign invaders Self (cancer) and Nonself (virus, bacteria, etc.) But, if the
What your autoantibodies tell us about your disease Mark Gourley, MD The Importance of the Immune System Defends us against foreign invaders Self (cancer) and Nonself (virus, bacteria, etc.) But, if the
Case Report J Clin Med Res. 2015;7(6): ress. Elmer. John O Grady a, c, Len Harty a, Nick Mayer b, Val Critcher b, John Ryan b.
 Elmer ress Case Report J Clin Med Res. 2015;7(6):490-494 Immune-Mediated Necrotizing Myopathy, Associated With Antibodies to Signal Recognition Particle, Together With Lupus Nephritis: Case Presentation
Elmer ress Case Report J Clin Med Res. 2015;7(6):490-494 Immune-Mediated Necrotizing Myopathy, Associated With Antibodies to Signal Recognition Particle, Together With Lupus Nephritis: Case Presentation
Granulomatous Myositis Clinicopathologic Study of 12 Cases
 Anatomic Pathology / GRANULOMATOUS MYOSITIS Granulomatous Myositis Clinicopathologic Study of 12 Cases Richard A. Pray son, MD Key Words: Granulomas; Granulomatous myositis; Myositis; Granulomatous inflammation
Anatomic Pathology / GRANULOMATOUS MYOSITIS Granulomatous Myositis Clinicopathologic Study of 12 Cases Richard A. Pray son, MD Key Words: Granulomas; Granulomatous myositis; Myositis; Granulomatous inflammation
Idiopathic inflammatory muscle diseases. Dr. Paul Etau Ekwom MBChB, MMED Kenyatta National Hospital, Nairobi-Kenya
 Idiopathic inflammatory muscle diseases. Dr. Paul Etau Ekwom MBChB, MMED Kenyatta National Hospital, Nairobi-Kenya I.W, 28 YRS, FEMALE SHOP STEWARD Referred to KNH on 16/06/09 from Thika Nursing Home Weakness
Idiopathic inflammatory muscle diseases. Dr. Paul Etau Ekwom MBChB, MMED Kenyatta National Hospital, Nairobi-Kenya I.W, 28 YRS, FEMALE SHOP STEWARD Referred to KNH on 16/06/09 from Thika Nursing Home Weakness
Limb girdle muscular dystrophy type 2B masquerading as inflammatory myopathy: case report
 Jethwa et al. Pediatric Rheumatology 2013, 11:19 CASE REPORT Limb girdle muscular dystrophy type 2B masquerading as inflammatory myopathy: case report Hannah Jethwa 1, Thomas S Jacques 2, Roxanna Gunny
Jethwa et al. Pediatric Rheumatology 2013, 11:19 CASE REPORT Limb girdle muscular dystrophy type 2B masquerading as inflammatory myopathy: case report Hannah Jethwa 1, Thomas S Jacques 2, Roxanna Gunny
Immunohistochemical Study of Dystrophin Associated Glycoproteins in Limb-girdle Muscular Dystrophies
 Dystrophin Immunohistochemical Study of Dystrophin Associated Glycoproteins in Limb-girdle Muscular Dystrophies NSC 89-2314-B-002-111 88 8 1 89 7 31 ( Peroxidase -AntiPeroxidase Immnofluorescence) Abstract
Dystrophin Immunohistochemical Study of Dystrophin Associated Glycoproteins in Limb-girdle Muscular Dystrophies NSC 89-2314-B-002-111 88 8 1 89 7 31 ( Peroxidase -AntiPeroxidase Immnofluorescence) Abstract
Disclosures. Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies. None
 Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies Sarah Goglin MD Assistant Professor of Medicine Division of Rheumatology Disclosures None 1 [footer
Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies Sarah Goglin MD Assistant Professor of Medicine Division of Rheumatology Disclosures None 1 [footer
Polymyositis, a very uncommon isolated disease: clinical and histological re evaluation after long term follow up
 Rheumatol Int (2015) 35:915 920 DOI 10.1007/s00296-014-3198-5 Rheumatology INTERNATIONAL ORIGINAL ARTICLE - CASES WITH A MESSAGE Polymyositis, a very uncommon isolated disease: clinical and histological
Rheumatol Int (2015) 35:915 920 DOI 10.1007/s00296-014-3198-5 Rheumatology INTERNATIONAL ORIGINAL ARTICLE - CASES WITH A MESSAGE Polymyositis, a very uncommon isolated disease: clinical and histological
Is it Autoimmune or NOT! Presented to AONP! October 2015!
 Is it Autoimmune or NOT! Presented to AONP! October 2015! Four main jobs of immune system Detects Contains and eliminates Self regulates Protects Innate Immune System! Epithelial cells, phagocytic cells
Is it Autoimmune or NOT! Presented to AONP! October 2015! Four main jobs of immune system Detects Contains and eliminates Self regulates Protects Innate Immune System! Epithelial cells, phagocytic cells
RSR RSR RSR RSR RSR. ElisaRSR AQP4 Ab RSR. Aquaporin-4 Autoantibody Assay Kit
 To aid diagnosis of Neuromyelitis Optica (NMO) and NMO spectrum disorder (NMOSD) To confirm diagnosis before initial treatment of patients with demyelinating inflammatory disease NMO, NMOSD and AQP4 Elisa
To aid diagnosis of Neuromyelitis Optica (NMO) and NMO spectrum disorder (NMOSD) To confirm diagnosis before initial treatment of patients with demyelinating inflammatory disease NMO, NMOSD and AQP4 Elisa
Diagnosis of McArdle's disease in an elderly patient: Case report and review of literature
 ISPUB.COM The Internet Journal of Neurology Volume 9 Number 1 Diagnosis of McArdle's disease in an elderly patient: Case report and review of literature R Makary, A Berger, N Talpur, S Shuja Citation R
ISPUB.COM The Internet Journal of Neurology Volume 9 Number 1 Diagnosis of McArdle's disease in an elderly patient: Case report and review of literature R Makary, A Berger, N Talpur, S Shuja Citation R
Proceedings des 36èmes Journées Annuelles de l Association Vétérinaire Equine Française
 Close this window to return to IVIS www.ivis.org Proceedings des 36èmes Journées Annuelles de l Association Vétérinaire Equine Française 9-11 Octobre 2008 - Reims, France Reprinted in IVIS with the Permission
Close this window to return to IVIS www.ivis.org Proceedings des 36èmes Journées Annuelles de l Association Vétérinaire Equine Française 9-11 Octobre 2008 - Reims, France Reprinted in IVIS with the Permission
Explain the laboratory diagnosis of Rabies?
 Explain the laboratory diagnosis of Rabies? The standard test for rabies testing is dfa. This test has been thoroughly evaluated for more than 40 years, and is recognized as the most rapid and reliable
Explain the laboratory diagnosis of Rabies? The standard test for rabies testing is dfa. This test has been thoroughly evaluated for more than 40 years, and is recognized as the most rapid and reliable
EDX in Myopathies Limitations. EDX in Myopathies Utility Causes of Myopathy. Myopathy: Issues for Electromyographers
 Electrodiagnostic Assessment of Myopathy Myopathy: Issues for Electromyographers Often perceived as challenging Ian Grant Division of Neurology QEII Health Sciences Centre Halifax NS CNSF EMG Course June
Electrodiagnostic Assessment of Myopathy Myopathy: Issues for Electromyographers Often perceived as challenging Ian Grant Division of Neurology QEII Health Sciences Centre Halifax NS CNSF EMG Course June
Evaluation and construction of diagnostic criteria for inclusion body myositis
 Evaluation and construction of diagnostic criteria for inclusion body myositis Thomas E. Lloyd, MD, PhD Andrew L. Mammen, MD, PhD Anthony A. Amato, MD Michael D. Weiss, MD Merrilee Needham, MBBS Steven
Evaluation and construction of diagnostic criteria for inclusion body myositis Thomas E. Lloyd, MD, PhD Andrew L. Mammen, MD, PhD Anthony A. Amato, MD Michael D. Weiss, MD Merrilee Needham, MBBS Steven
바터팽대부의신경내분비종양환자에서발생한피부근염
 대한내과학회지 : 제 92 권제 6 호 2017 https://doi.org/10.3904/kjm.2017.92.6.552 바터팽대부의신경내분비종양환자에서발생한피부근염 1 건국대학교의과대학건국대학교충주병원류마티스내과, 연세대학교원주의과대학원주세브란스기독병원 2 류마티스내과, 3 내과, 4 한림대학교의과대학춘천성심병원류마티스내과 박정은 1 ㆍ강태영 2 ㆍ유진세
대한내과학회지 : 제 92 권제 6 호 2017 https://doi.org/10.3904/kjm.2017.92.6.552 바터팽대부의신경내분비종양환자에서발생한피부근염 1 건국대학교의과대학건국대학교충주병원류마티스내과, 연세대학교원주의과대학원주세브란스기독병원 2 류마티스내과, 3 내과, 4 한림대학교의과대학춘천성심병원류마티스내과 박정은 1 ㆍ강태영 2 ㆍ유진세
Case Report Development of Eosinophilic Fasciitis during Infliximab Therapy for Psoriatic Arthritis
 Case Reports in Rheumatology Volume 2016, Article ID 7906013, 4 pages http://dx.doi.org/10.1155/2016/7906013 Case Report Development of Eosinophilic Fasciitis during Infliximab Therapy for Psoriatic Arthritis
Case Reports in Rheumatology Volume 2016, Article ID 7906013, 4 pages http://dx.doi.org/10.1155/2016/7906013 Case Report Development of Eosinophilic Fasciitis during Infliximab Therapy for Psoriatic Arthritis
Two simple, reliable and valid tests of proximal muscle function, and their application to the management of idiopathic inflammatory myositis
 Rheumatology 26;45:874 879 Advance Access publication 31 January 26 Two simple, reliable and valid tests of proximal muscle function, and their application to the management of idiopathic inflammatory
Rheumatology 26;45:874 879 Advance Access publication 31 January 26 Two simple, reliable and valid tests of proximal muscle function, and their application to the management of idiopathic inflammatory
Sawada J, Orimoto R, Misu T, Katayama T, Aizawa H, Asanome A, Takahashi K, Saito T, Anei R, Kamada K, Miyokawa N, Takahashi T, Fujihara K, Hasebe N.
 Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
The Role of Electron Microscopy in the Assessment of Dermatomyositis: A Retrospective Pilot Study on Skeletal Muscle Biopsies
 British Journal of Medicine & Medical Research 3(4): 962-970, 2013 SCIENCEDOMAIN international www.sciencedomain.org The Role of Electron Microscopy in the Assessment of : A Retrospective Pilot Study on
British Journal of Medicine & Medical Research 3(4): 962-970, 2013 SCIENCEDOMAIN international www.sciencedomain.org The Role of Electron Microscopy in the Assessment of : A Retrospective Pilot Study on
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies
 Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
Research Article Soluble IL-2 Receptor: A Biomarker for Assessing Myositis Activity
 Disease Markers, Article ID 76, 6 pages http://dx.doi.org/1.1155/1/76 Research Article Soluble IL- Receptor: A Biomarker for Assessing Myositis Activity Anne Tournadre, 1 Jean-Jacques Dubost, 1 Martin
Disease Markers, Article ID 76, 6 pages http://dx.doi.org/1.1155/1/76 Research Article Soluble IL- Receptor: A Biomarker for Assessing Myositis Activity Anne Tournadre, 1 Jean-Jacques Dubost, 1 Martin
L. Nandini Moorthy, MD MS 2012
 L. Nandini Moorthy, MD MS 2012 L Nandini Moorthy, MD MS 09 17 yo Ashkenazi male with proximal muscle pain and weakness, mild malar erythema and erythema over knees and dorsal aspect of PIPs Mild tenderness
L. Nandini Moorthy, MD MS 2012 L Nandini Moorthy, MD MS 09 17 yo Ashkenazi male with proximal muscle pain and weakness, mild malar erythema and erythema over knees and dorsal aspect of PIPs Mild tenderness
Enterprise Interest Nothing to declare
 Enterprise Interest Nothing to declare A rare cause of myopathy in adults Jorge Pinheiro MD, José Manuel Lopes MD, PhD Joint Slide Seminar Electron Microscopy and Trainees: Understanding diseases through
Enterprise Interest Nothing to declare A rare cause of myopathy in adults Jorge Pinheiro MD, José Manuel Lopes MD, PhD Joint Slide Seminar Electron Microscopy and Trainees: Understanding diseases through
Screening of Auto Antibodies using Indirect Immunofluorescence in Auto Immune Disease Patients
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 02 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.702.386
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 02 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.702.386
CNEMG. Myopathy, Stålberg. At rest denervation and spec spontaneous activity (myotonia, CRD, neuromyotonia) MUP number of fibres in recorded area
 clincial heredity biochem MYOPATHY biopsy Erik Stålberg Uppsala, Sweden imaging genetics Electrodes A B C MU D E Conc EMG signals from 2-15 muscle fibres CNEMG At rest denervation and spec spontaneous
clincial heredity biochem MYOPATHY biopsy Erik Stålberg Uppsala, Sweden imaging genetics Electrodes A B C MU D E Conc EMG signals from 2-15 muscle fibres CNEMG At rest denervation and spec spontaneous
Willcocks et al.,
 ONLINE SUPPLEMENTAL MATERIAL Willcocks et al., http://www.jem.org/cgi/content/full/jem.20072413/dc1 Supplemental materials and methods SLE and AASV cohorts The UK SLE cohort (n = 171) was obtained from
ONLINE SUPPLEMENTAL MATERIAL Willcocks et al., http://www.jem.org/cgi/content/full/jem.20072413/dc1 Supplemental materials and methods SLE and AASV cohorts The UK SLE cohort (n = 171) was obtained from
Chronic focal polymyositis in the adult
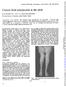 Journal of Neurology, Neurosurgery, and Psychiatry, 1981, 44, 419-425 Chronic focal polymyositis in the adult N E BHARUCHA AND J A MORGAN-HUGHES From the Institute of Neurology, Queen Square, London S
Journal of Neurology, Neurosurgery, and Psychiatry, 1981, 44, 419-425 Chronic focal polymyositis in the adult N E BHARUCHA AND J A MORGAN-HUGHES From the Institute of Neurology, Queen Square, London S
Inclusion body myositis
 Pathology Feature William R. Hart, M.D. Section Editor Inclusion body myositis A possible chronic persistent muscle infection mumps virus 1 Samuel M. Chou, M.D., Ph.D. Inclusion body myositis was diagnosed
Pathology Feature William R. Hart, M.D. Section Editor Inclusion body myositis A possible chronic persistent muscle infection mumps virus 1 Samuel M. Chou, M.D., Ph.D. Inclusion body myositis was diagnosed
Rare myositis-specific autoantibody associations among Hungarian patients with idiopathic inflammatory myopathy
 ARTIGO ORIGINAL Rare myositis-specific autoantibody associations among Hungarian patients with idiopathic inflammatory myopathy Bodoki L, Nagy-Vincze M, Griger Z, Betteridge Z, Szöllösi L, Jobanputra R,
ARTIGO ORIGINAL Rare myositis-specific autoantibody associations among Hungarian patients with idiopathic inflammatory myopathy Bodoki L, Nagy-Vincze M, Griger Z, Betteridge Z, Szöllösi L, Jobanputra R,
Histopathology: granulomatous inflammation, including tuberculosis
 Histopathology: granulomatous inflammation, including tuberculosis These presentations are to help you identify basic histopathological features. They do not contain the additional factual information
Histopathology: granulomatous inflammation, including tuberculosis These presentations are to help you identify basic histopathological features. They do not contain the additional factual information
9/15/11. Dr. Vivien Hsu Director, UMDNJ Scleroderma Program New Brunswick, NJ September Scleroderma. Hard skin
 Dr. Vivien Hsu Director, UMDNJ Scleroderma Program New Brunswick, NJ September 2011 Scleroderma Hard skin 1 No diagnostic test for scleroderma Pathogenesis is unknown prominent features of disease reflect
Dr. Vivien Hsu Director, UMDNJ Scleroderma Program New Brunswick, NJ September 2011 Scleroderma Hard skin 1 No diagnostic test for scleroderma Pathogenesis is unknown prominent features of disease reflect
Clinical features of seven Japanese patients with anti-pl- antibody frequent positivity for anti-cyclic citrullinated peptide antibody
 Cace report Clinical features of seven Japanese patients with anti-pl- antibody frequent positivity for anti-cyclic citrullinated peptide antibody Yoichiro Akiyama 1, Takao Nagashima 1, Masahiro Iwamoto
Cace report Clinical features of seven Japanese patients with anti-pl- antibody frequent positivity for anti-cyclic citrullinated peptide antibody Yoichiro Akiyama 1, Takao Nagashima 1, Masahiro Iwamoto
PRACTICAL ROADMAP. MUSCLE WJ van der Spuy
 PRACTICAL ROADMAP MUSCLE WJ van der Spuy MUSCLE Skeletal (striated) Cardiac (striated) Smooth Identification based on Fiber size, shape and presence/absence of branching Number, shape and position of nuclei
PRACTICAL ROADMAP MUSCLE WJ van der Spuy MUSCLE Skeletal (striated) Cardiac (striated) Smooth Identification based on Fiber size, shape and presence/absence of branching Number, shape and position of nuclei
Autoantibodies Against 3-Hydroxy-3-Methylglutaryl-Coenzyme A Reductase in Patients With Statin-Associated Autoimmune Myopathy
 ARTHRITIS & RHEUMATISM Vol. 63, No. 3, March 2011, pp 713 721 DOI 10.1002/art.30156 2011, American College of Rheumatology Autoantibodies Against 3-Hydroxy-3-Methylglutaryl-Coenzyme A Reductase in Patients
ARTHRITIS & RHEUMATISM Vol. 63, No. 3, March 2011, pp 713 721 DOI 10.1002/art.30156 2011, American College of Rheumatology Autoantibodies Against 3-Hydroxy-3-Methylglutaryl-Coenzyme A Reductase in Patients
Histopathology of Wooden Breast
 Histopathology of Wooden Breast Canadian Poultry and Egg Processors Council Aviagen Frederic J. Hoerr, DVM, PhD June 10, 2016 Halifax, Nova Scotia FJ Hoerr 1 Normal Veterinary Diagnostic Pathology, LLC
Histopathology of Wooden Breast Canadian Poultry and Egg Processors Council Aviagen Frederic J. Hoerr, DVM, PhD June 10, 2016 Halifax, Nova Scotia FJ Hoerr 1 Normal Veterinary Diagnostic Pathology, LLC
