I mmune mediated and inflammatory myopathies are usually
|
|
|
- Mae Rice
- 5 years ago
- Views:
Transcription
1 420 PAPER Myopathy with antibodies to the signal recognition particle: clinical and pathological features T Miller, M T Al-Lozi, G Lopate, A Pestronk... J Neurol Neurosurg Psychiatry 2002;73: See end of article for authors affiliations... Correspondence to: Dr A Pestronk, Washington University School of Medicine, Department of Neurology, Box 8111, 660 South Euclid Ave, St Louis, MO 63110, USA; pestronk@kids.wustl.edu Received 15 April 2002 In revised form 19 June 2002 Accepted 21 June Objectives: To study myopathies with serum antibodies to the signal recognition particle (SRP), an unusual, myositis specific antibody associated syndrome that has not been well characterised pathologically. Methods: Clinical, laboratory, and myopathological features were evaluated in seven consecutive patients with a myopathy and serum anti-srp antibodies, identified over three years. The anti-srp myopathy was compared with myopathology in other types of inflammatory and immune myopathies. Results: The patients with anti-srp antibodies developed weakness at ages ranging from 32 to 70 years. Onset was seasonal (August to January). Weakness became severe and disability developed rapidly over a period of months. Muscle pain and fatigue were present in some patients. No patient had a dermatomyositis-like rash. Serum creatine kinase was very high (3000 to IU/l). Muscle biopsies showed an active myopathy, including muscle fibre necrosis and regeneration. There was prominent endomysial fibrosis, but little or no inflammation. Endomysial capillaries were enlarged, reduced in number, and associated with deposits of the terminal components of complement (C5b-9, membrane attack complex). Strength improved in several patients after corticosteroid treatment. Conclusions: Myopathies associated with anti-srp antibodies may produce severe and rapidly progressive weakness and disability. Muscle biopsies show active myopathy with pathological changes in endomysial capillaries but little inflammation. Corticosteroid treatment early in the course of the illness is often followed by improvement in strength. In patients with rapidly progressive myopathies and a high serum creatine kinase but little inflammation on muscle biopsy, measurement of anti-srp antibodies and pathological examination of muscle, including evaluation of endomysial capillaries, may provide useful information on diagnosis and treatment. I mmune mediated and inflammatory myopathies are usually classified according to their clinical, electrophysiological, serological, and pathological features. 1 3 Polymyositis is a group of disorders that have in common weakness (usually proximal), a raised serum creatine kinase, a myopathic and irritative pattern of changes on electrodiagnostic testing, and myopathic changes often associated with inflammation on pathological examination of muscle. Dermatomyositis has many features that are similar to polymyositis but is distinguished by skin involvement and by muscle pathology that usually includes perifascicular myopathic changes. Inclusion body myositis is distinguished from other inflammatory myopathies by its clinical pattern of patchy, asymmetrical, proximal and distal weakness and pathological changes that include vacuoles and focal invasion of muscle fibres by inflammatory cells. Polymyositis and dermatomyositis are generally thought to be immune mediated, but the pathogenic processes underlying inclusion body myositis are unclear. It now appears that subgroups of polymyositis and dermatomyositis can be delineated on the basis of clinical, serological, and pathological features of disease syndromes. Some of these myopathy syndromes are associated with characteristic myositis specific serum antibodies. 45 The best defined, and most common, of these syndromes is associated with serum antibodies to the Jo-1 antigen (histidyl t-rna synthetase). 4 6 Anti-Jo-1 antibodies are associated with a characteristic clinical syndrome that may include muscle weakness and pain, Raynaud s phenomenon, interstitial lung disease, arthritis, and skin disorders. Pathological features in muscle also distinguish the Jo-1 syndrome from other types of immune myopathy. 7 Characteristic histological features include prominent, but patchy, fragmentation and macrophage inflammation in perimysial connective tissue. Muscle fibre degeneration and regeneration are most marked in perifascicular regions neighbouring the connective tissue pathology. Another myopathy syndrome includes rapidly developing and often severe weakness, and a serum myositis specific antibody directed against the signal recognition particle (SRP). 58 The SRP, and its membrane associated receptor (SRPR or docking protein), catalyse the targeting of nascent secretory and membrane proteins to the protein translocation apparatus of the endoplasmic reticulum. 910 The role of anti-srp antibodies in the pathogenesis of the myopathy has not been defined. The anti-srp associated syndrome has been described clinically in fewer than 20 patients. 58 Pathological features of the myopathy have not been reported in detail. During the past three years we identified seven patients with myopathy syndromes and serum anti-srp antibodies. We report the features of these patients, who have a characteristic clinical and pathological syndrome. METHODS Clinical data Over a three year period, adult patients presenting to the neuromuscular service at Washington University School of Medicine in St Louis, Missouri, USA with acquired myopathies without other clear causes had serum evaluated for a panel of 12 myositis specific and myositis associated antibodies. Assays were performed by the Oklahoma Medical Research Foundation (Oklahoma City, Oklahama, USA) using immunoprecipitation methodology. Assays included studies for antibodies to Jo-1, PL-7, PL-12, EJ, OJ, Mi-2, SRP, PM-Scl, Ku, U1RNP, U2RNP, and Ro. Results are reported qualitatively as positive or negative. Our report includes the seven consecutive patients evaluated during this period in whom serum anti-srp antibodies
2 Myopathy with anti-srp antibodies 421 were detected and confirmed by serum immunoprecipitation and immunodiffusion methods. None of these patients had positive tests for antibodies to any of the other antigens studied. Anti-SRP antibodies were not detected in the serum of eight patients with dermatomyositis (five adults and three children) or in 31 patients with inflammatory myopathies tested during the same period. Physicians in our neuromuscular group examined the seven patients with myopathy and anti-srp antibodies. All had muscle biopsies that were evaluated in our neuromuscular pathology laboratory without knowledge of the antibody status of the patient. Clinical data were obtained from clinical examination and a review of the patients case notes. Strength was evaluated on the MRC scale, and was also measured quantitatively, in six proximal and three distal muscle groups bilaterally, using a hand held myometer (Chatillon, Champion Scale, St Louis, Missouri, USA) and a grip meter (Jaymar, Preston, New Jersey, USA). 11 We compared the myopathology in our seven patients with anti-srp antibodies with muscle changes in 42 patients with no antibodies to SRP in their serum. Thirty six patients had definite polymyositis, 12 definite dermatomyositis, 12 or other subgroups of immune myopathies diagnosed on clinical, serological, electrophysiological, and pathological grounds. 78 Specifically, for all these pathology control groups, we included only biopsies with myopathic, connective tissue, or vascular involvement. Serum anti-jo-1 antibodies were confirmed using immunoprecipitation, as enzyme linked immunosorbent assay (ELISA) methodology alone can give false positive results. Six control patients had biopsies with no morphological abnormalities. Laboratory data Muscles chosen for biopsy had 4/5 strength (MRC grade). Five of the seven muscle biopsies were obtained before treatment with corticosteroids or immunosuppressive agents. The initial muscle biopsies from patients 2 and 5 were obtained two to four days after the onset of treatment with corticosteroids. Cryostat sections of rapidly frozen muscle were processed for muscle histochemistry and immunocytochemistry in a standard fashion. 713 The evaluators (TM and AP) were blinded to the status of the anti-srp antibodies at the time of initial biopsy evaluation and subsequent quantitative analysis. Immunocytochemistry was performed on biopsies from the seven patients with anti-srp antibodies and paired normal tissue controls for each antibody using standard protocols. Primary antibodies used in this study were directed against CD68, CD3, and C5b-9 (membrane attack complex (MAC)) antigens (Sigma, St Louis, Missouri, USA) and human major histocompatibility complex class I antigen (MHC-1) (US Biological, Swampscott, Massachusetts, USA). Ulex europaeus agglutinin I (UEA-I) (Sigma), a lectin that binds to α-fucosyl residues on endothelial cells, was used as a marker for capillaries Antibody binding was visualised using peroxidase conjugated secondary antibodies (Sigma). Data analysis Light microscopic images from regions randomly chosen for quantitative analysis were stored digitally. Endomysial vessel (capillary) density was determined by quantitating the number of endomysial vessels per 1000 µm 2 of muscle fibre area (capillary index). The average endomysial capillary diameter was calculated from measurements of the smallest cross sectional diameters of endomysial vessels in randomly selected regions of digitally stored images of patient and control muscle biopsies. For analysis of C5b-9 deposition we evaluated only endomysial vessels, as antibodies to C5b-9 may stain the media of perimysial arterioles in normal muscle. Fisher s exact and Mann Whitney rank sum tests were used to calculate the statistical significance of differences between groups. CASE REPORTS Patient 1 A 32 year old man was admitted to the hospital with a five month history of rapidly progressive severe weakness in the trunk, arms, and legs leading to inability to stand or sit. He had also noted generalised myalgia, fatigue, dyspnoea, and weight loss. Neurological examination showed bifacial weakness and severe symmetrical proximal weakness, graded at 0/5 in the lower extremities and 2/5 in the proximal upper extremities. Sensory and skin examination was normal. Laboratory data included raised creatine kinase (CK) at 6204 IU/l and raised aldolase at 55 IU/l. Electromyography revealed fibrillations, positive sharp waves, and myopathic motor unit potentials in proximal and intermediate muscles. Nerve conduction studies were normal except for a mildly reduced tibial CMAP amplitude. A muscle biopsy showed an active myopathy with muscle fibre degeneration and regeneration, markedly increased connective tissue, and a few small foci of mononuclear inflammatory cells. High dose intravenous corticosteroid treatment produced no improvement in strength. Patient 2 A 35 year old woman developed weakness in the legs, and then in the arms, which progressed over 12 months. She also experienced myalgia, stiffness, and fatigue. Mild dysphagia was present initially but this did not persist. She was diagnosed as having polymyositis on clinical grounds, and treated using oral prednisone with symptomatic improvement in muscle strength. After two years, steroids were discontinued and the weakness and fatigue recurred. Reinstitution of prednisone and the addition of methotrexate and azathioprine were not effective. Over the next year, weakness progressed. Neurological examination showed symmetrical proximal weakness (3/5). Sensory and skin examination was normal. Laboratory data included a raised serum CK at 3064 IU/l. Electromyography revealed fibrillation potentials, positive sharp waves, and short duration, early recruited motor unit potentials in proximal muscles. Nerve conduction studies were normal. A muscle biopsy showed severe end stage pathology. Treatment with intravenous methylprednisolone (Solumedrol) (1 g/day for five days) followed by oral prednisone (60 mg/day for several months) produced mild improvement in functional abilities and proximal muscle strength. Patient 3 A 48 year old woman developed weakness in the arms and legs and generalised fatigue that rapidly progressed over three months to severe disability with inability to rise from a bed or chair. She denied significant myalgia, skin changes, or bulbar or respiratory dysfunction. Neurological examination showed severe, relatively symmetrical proximal extremity muscle weakness (0/5 to 1/5) and mild neck flexor weakness (4/5), but no facial weakness. Serum CK was IU/l. Electromyography revealed fibrillation potentials, positive sharp waves, and myopathic motor unit potentials in proximal muscles. A muscle biopsy showed an active myopathy with degenerating and regenerating muscle fibres, increased endomysial connective tissue, and no inflammation. The patient was treated with oral prednisone (60 mg/day) and azathioprine (50 mg/day) for two months with no change in symptoms. Drug doses were increased to 150 mg/day of azathioprine and 80 mg/day of prednisone. Quantitative muscle strength testing showed progressive improvement in proximal strength, reaching nearly normal values by 12 months, and continuing at those values over the next year with tapering doses of prednisone. Patient 4 A 46 year old man developed weakness in the arms and legs that progressed over eight months to severe disability, with need for
3 422 Miller, Al-Lozi, Lopate, et al Table 1 Clinical and laboratory characteristics of the patients Patient No Clinical features Age at onset (years) Sex M F F M F F F Weakness Proximal > distal Arms + legs Maximum severity 0% 20% 0% 0% 0% 20% 0% (% of normal strength) Time to maximum severity (months) Season of onset of weakness Autumn Autumn Summer Autumn Winter Autumn Autumn (August) (January) Muscle pain Fatigue Dysphagia Skin rash + Dyspnoea + + Palpitations Weight loss Steroid response Laboratory data Creatine kinase (maximum) (IU/l) Aldolase (IU/l) 55 ND ND ND ESR (mm/h) Antinuclear antibody 1:160 EMG ND, not determined;, negative or not present; +, present. EMG, electromyography; ESR, erythrocyte sedimentation rate; F, female; M, male; Myopathic, myopathic EMG with brief, small amplitude, polyphasic motor unit potentials;, spontaneous activity at rest, including fibrillations and positive sharp waves. a walking frame and inability to rise from the sitting position. He also experienced diffuse myalgia, fatigue, and a 13.5 kg (30 pound) weight loss. General examination was notable only for mild tachycardia. Neurological examination showed severe symmetrical weakness, proximal greater than distal (2/5 to 3/5 in the legs and 0/5 in the proximal arms). Bilateral moderate facial and neck weakness was also present. Sensory and skin examination was normal. Serum CK was 8940 IU/l. Electromyography showed fibrillation potentials, positive sharp waves, and myopathic motor unit potentials in proximal muscles. Nerve conduction studies were generally normal. A muscle biopsy revealed an active myopathy, with degenerating and regenerating muscle fibres, but no inflammation. Treatment with oral prednisone (60 mg/day) for three months produced no improvement. Intravenous methylprednisolone (Solumedrol), 1 g/day for five days, followed by weekly single doses of 1 g, was associated with reduced fatigue and gradual improvement in strength and walking over 10 months. Patient 5 A 39 year old woman presented with a two month history of progressive difficulty in climbing stairs and walking, falling, and a sense of generalised body heaviness. Serum CK was 7406 IU/l. Electrodiagnostic testing showed myopathic motor unit potentials in the biceps and early recruitment in the quadriceps muscles. Haematoxylin and eosin (H&E) stains of paraffin embedded muscle revealed scattered muscle fibre degeneration and regeneration but no inflammation. She was treated with a tapering dose of oral prednisone, beginning at 60 mg/day, and azathioprine 50 mg twice daily. Weakness continued to progress. Ten months after the onset of disease symptoms, general examination showed mild Cushingoid features and normal skin. On neurological examination there was symmetrical severe proximal weakness (0/5 to 1/5 in proximal arms and legs and 4/5 in the neck flexors). Facial strength was normal. Sensory examination was normal. Serum CK was 1950 IU/l. A second muscle biopsy showed an active myopathy with many degenerating and regenerating fibres and increased endomysial connective tissue. Treatment with weekly corticosteroids (0.75 to 1 g) for two years was associated with gradual and substantial improvement in strength, including 4/5 values in the proximal arms and legs and 5/5 in more distal muscles. Patient 6 A 70 year old woman presented with a two month history of progressive proximal weakness, more in the legs than the arms, and generalised fatigue. A scaly skin rash was noted on her hands, neck, and eyelids. Serum CK was IU/l. Treatment with oral prednisone, up to 80 mg/day, was followed by subjectively improved proximal strength. Tapering of the corticosteroid dose was associated with a moderate decline in proximal strength and increased disability. Neurological examination showed severe proximal weakness (0/5 to 3/5) in the arms and legs. Serum CK was mildly elevated at 473 IU/l. Electrodiagnostic testing was consistent with an irritable myopathy. A muscle biopsy revealed myopathic changes with many regenerating and some degenerating muscle fibres, but no inflammation. Increased doses of oral corticosteroids led to a subjective sense of increased strength. Patient 7 A 66 year old woman presented with a one month history of progressive proximal weakness, exercise induced myalgia, a 2.3 kg (5 pound) weight loss, and mild dyspnoea on exertion. On examination there was severe proximal weakness (1/5 to 2/5). Serum CK was IU/l. Electromyography showed fibrillation potentials and positive sharp waves with myopathic motor units in proximal and distal muscles. A muscle biopsy revealed an active myopathy with many degenerating and regenerating fibres but no inflammation. She was treated with corticosteroids, initially oral prednisone (60 mg/day), but when weakness progressed (to 0/5 in some muscles) this was
4 Myopathy with anti-srp antibodies 423 Table 2 Muscle pathology in patients with anti-srp antibodies Patient No Time from disease onset to muscle biopsy (months) Pathological features Lymphocytic inflammation Perimysial Endomysial ± + Perivascular + Muscle fibre size Variation + NA Bimodal + NA Hypertrophy + NA Hypercontracted fibres + NA + Grouped small round fibres + NA Perifascicular atrophy NA Muscle fibre pathology Necrosis Scattered + NA Regional (large groups) NA Regeneration + NA Coarse internal architecture + NA Immature (2C) fibres + NA Mitochondrial changes NA C5b-9 deposition ± NA Connective tissue features Endomysial Increased + NA Acid phosphatase+/cd68+ cells + NA Perimysial Fragmentation + Alkaline phosphatase staining Acid phosphatase+/cd68+ cells + + Vessels Capillaries Reduced number + NA Enlarged size + NA C5b-9 deposition NA, tissue type not present for evaluation in biopsy; +, present in biopsy;, not present in biopsy. changed to pulse dose intravenous, and then oral, methylprednisolone (Solumedrol). Methotrexate (15 mg/week) was also added. Improvement in strength and reduction in dyspnoea began after two months. Quantitative strength testing has shown mild progressive improvement in strength with residual severe weakness in proximal muscles. RESULTS Clinical characteristics of patients with anti-srp antibodies These data are shown in table 1. Our seven patients with myopathy and anti-srp antibodies ranged in age from 32 to 70 years, with a mean of 48 years, at the onset of weakness. The onset of weakness in all patients was between August and January, usually in the autumn. Five patients were women. All the patients had a history of proximal weakness that progressed relatively rapidly to severe disability. The time from onset to peak weakness ranged from two to 12 months, with a mean of five months. Six patients had a history of muscle discomfort, such as pain or fatigue, but this was never a primary complaint. Three patients noted dysphagia and two complained of dyspnoea. None had a history of palpitations or malignancy. On examination all patients had proximal, mostly symmetrical, weakness involving both upper and lower limbs. Weakness was very severe in some proximal muscles in all patients. MRC grades in the weakest muscles ranged from 0/5 in five patients to a maximum of 3/5 (quantitative strength testing reduced to a maximum of 20% of normal) in two patients. The weakest muscles were always the deltoid and psoas. Very distal muscles, such as the intrinsic muscles of the hands and feet, were often only mildly weak or normal. Sensation was normal. One patient had a scaly rash that was not typical of dermatomyositis. After treatment with corticosteroids, six of the seven patients showed improvement on quantitative strength testing. Three patients relapsed, with increased weakness, during steroid tapering. Reintroduction of corticosteroid treatment did not result in the same level of improved strength as was observed initially. Laboratory data Laboratory data are shown in table 1. Serum CK was markedly raised at presentation in all seven patients with anti-srp antibodies, ranging from 3064 to IU/l (normal < 170), with a mean of IU/l. Aldolase was raised in the four patients tested, ranging from 23 to 174 IU/l (normal < 8). Antinuclear antibodies were found in only one patient. The erythrocyte sedimentation rate (ESR) ranged from 1 to 42 (normal < 30), and was mildly raised in four of the seven patients. Electromyography in all seven patients was consistent with a myopathy, showing small amplitude, brief, polyphasic motor unit potentials. Features of muscle irritability, including spontaneous fibrillation potentials and positive sharp waves, were very prominent. Muscle pathology in patients with anti-srp antibodies These data are shown in tables 2 and 3 and fig 1. One muscle biopsy (from patient 2) was end stage, with muscle fibres largely replaced by fat. The few remaining muscle fibres were small, rounded, and embedded in abundant connective tissue. Muscle biopsies from the other six patients with anti-srp antibodies showed myopathic features including prominent variation of muscle fibre size (fig 1). None of
5 424 Miller, Al-Lozi, Lopate, et al Table 3 Muscle pathology in immune myopathies: comparative features Anti-SRP myopathy Polymyositis: Jo-1 antibody positive Polymyositis: Jo-1 antibody negative Dermatomyositis Fasciitis Paraneoplastic necrotic myopathy No of biopsies Inflammation (focal) 2 a Perimysial Endomysial Perivascular Muscle fibre features Enlarged muscle fibres 6* a Perifascicular myopathy 0 c Regional necrosis Perimysium Fragmentation 1 d Alkaline phosphatase Endomysium Diffusely increased 6 a Vessels Reduced number 4* b Enlarged size 6* b C5b-9 deposition 7 e *Based on six rather than seven anti-srp patients: one muscle biopsy (from patient No 2) had too few muscle fibres for determination of the capillary index. a Different from other forms of immune myopathy, p < b Different from myositis and fasciitis, p < c Different from dermatomyositis, p < d Different from Jo-1 myositis and fasciitis, p < e Different from polymyositis and fasciitis, p < ND, not determined; +, positive. the biopsies showed a perifascicular distribution of atrophic or myopathic changes. The distribution of muscle fibre sizes often appeared bimodal. One population of muscle fibres was hypertrophied (fig 1, panels A and B). Many dark, rounded, probably hypercontracted, muscle fibres were also observed in two biopsies. The other population of muscle fibres was small, rounded, and often occurred in clusters (fig 1B). Small regenerating muscle fibres (basophilic colour on H&E stain, or intermediate colour on ATPase, ph 4.3) were distributed randomly through most biopsies. Necrotic muscle fibres (diffuse pale staining and a hyaline appearance with H&E) often invaded by macrophage-like cells that stained with non-specific esterase, acid phosphatase, and anti-cd68 antibody were scattered through all six biopsies. Prominently increased endomysial connective tissue was a feature of five biopsies (fig 1C). In several, the marked increase in connective tissue was especially notable in the light of the short (two to five month) history of weakness. In all biopsies NADH stains showed coarse, irregular internal architecture in many muscle fibres scattered throughout the biopsy. Mononuclear inflammatory cells were uncommon. No biopsy had perimysial or perivascular accumulations of mononuclear cells. One biopsy showed a single focus of mononuclear cells in the endomysium. Focal cellular invasion of intact muscle fibres was not observed. Alkaline phosphatase staining of perimysial connective tissue was noted in three patients. Mitochondrial stains reflected the abnormal internal architecture of muscle fibres that was also noted on NADH, but these were otherwise unremarkable. No biopsies had any muscle fibres with vacuoles. Staining of muscle fibres for MHC-I was absent in three biopsies, present only on scattered regenerating fibres in two, and present in scattered fascicles in small amounts in one. Endomysial capillary changes in patients with anti-srp antibodies Endomysial capillary density was reduced in muscles from patients with anti-srp antibodies (fig 2). The mean endomysial capillary index was reduced in muscles from patients with Figure 1 Muscle pathology in patients with myopathy and anti-srp (signal recognition particle) antibodies. Early changes: (A) Muscle fibre necrosis. Scattered, pale, fragmented muscle fibres, some of which contain cells with large nuclei (macrophages). (Haematoxylin and eosin (H&E) stain, bar = 14 µm.) (B) Bimodal distribution of fibre sizes. The largest fibres are mildly hypertrophied. There is no inflammation. (H&E stain, bar = 18 µm.). Late changes: (C) Endomysial connective tissue is increased. Hypercontracted muscle fibres with abnormal internal architecture are present. (H&E stain, bar = 18 µm.)
6 Myopathy with anti-srp antibodies 425 Figure 2 Endomysial capillary pathology. Normal muscle (panels A and C): numerous small endomysial capillaries are present; each muscle fibre cross section borders on several capillaries. (A, bar = 40 µm; C, bar = 8 µm.) Anti-SRP muscle (panels B, D, and E): endomysial capillaries are enlarged and reduced in number; muscle fibre cross sections may have no neighbouring capillaries. (B, bar = 40 µm; D and E, bar = 8 µm; UEA-I stain.) anti-srp antibodies (p = 0.006), measuring 0.7 (0.1) (mean (SD)), compared with values in the normal controls of 1.2 (0.1). Muscle fibre profiles with no neighbouring capillaries were common (fig 2, panel E). Capillary density was uniformly reduced throughout the biopsies. In normal controls most muscle fibres had several neighbouring capillaries (fig 2, panels A and C). We have previously found in agreement with other studies that capillary density is normal in polymyositis and Jo-1 myositis, but reduced in dermatomyositis. 7 The mean diameter of endomysial capillaries was increased in muscle from patients with anti-srp antibodies (p = 0.001) (fig 2, panels B, D, and E), measuring 9.1 (0.3) µm compared with control values of 6.5 (0.4) µm (fig 2, panels A and C). Membrane attack complex, the terminal C5b-9 components of complement, was deposited irregularly in endomysial capillaries in all seven biopsies (fig 3). C5b-9 staining was present in capillaries in most endomysial regions of anti-srp muscles, in contrast to dermatomyositis in which deposition was usually patchy. No biopsy had diffuse staining of C5b-9 within muscle fibres. In one biopsy (patient 1) C5b-9 was deposited around the rim of scattered muscle fibres. Deposition of the terminal C5b-9 components of complement was not found in endomysial vessels in three control muscle biopsies without myopathy, or in the 19 patients with polymyositis. DISCUSSION Our study shows that myopathies associated with serum anti- SRP antibodies have characteristic clinical and pathological features. In previous studies anti-srp antibodies have been associated with a myopathy syndrome which includes onset in the autumn and a rapidly developing severe weakness. 58 Our results emphasise that severe weakness is a prominent clinical feature of the myopathy, occurring in all of our patients. The severity of weakness is often manifest as a complete loss of strength (0/5 on the MRC scale), which develops bilaterally in at least one muscle group. This occurred in five of our seven patients. In contrast, none of our 11 previously reported patients with myopathies associated with anti-jo-1 antibodies 7 had such severe weakness in any muscles (p = 0.003). Weakness in the anti-srp antibody patients developed rapidly, with the time from onset to the maximum severity of weakness averaging only five months. The distribution of the weakness, which was symmetrical and predominantly proximal, was similar in all the patients with anti-srp antibodies. After treatment with corticosteroids, weakness often improved, but only partially. Residual relatively disabling weakness in some muscle groups was the rule. As in other studies of individuals with anti-srp antibodies, 58 most of our patients complained of muscle discomfort, but the pain was never severe enough to require analgesic treatment. In contrast to previous series, none of our patients complained of palpitations or of other features suggesting cardiac involvement. The onset of weakness in all our patients fell during the period between August and January. This differs from the onset of the anti-jo-1 antibody related myopathy syndromes, which generally occurs in the spring. 7 A seasonal pattern of disease onset might suggest an antecedent infectious or other environmental trigger to the anti-srp antibody syndrome. However, no clear prodromal illness was identified in any of our patients. A notable laboratory feature in all our patients, which probably reflected the active myopathic process, was the very high serum CK at presentation, ranging from 3064 to IU/l, with a mean of Serum aldolase was also raised in the four patients who were tested, ranging from 23 to 174 IU/l (normal less than 8). The EMG suggested an active myopathy, showing myopathic motor unit potentials and prominent spontaneous activity in proximal muscles in all the patients. There were few laboratory signs of systemic disease in our patients: the ESR ranged from 1 to 42, with a mean of 27, while antinuclear antibodies were mildly raised in only one patient. Several different pathological patterns occur in immune and inflammatory myopathies In some polymyositis
7 426 Miller, Al-Lozi, Lopate, et al Figure 3 Terminal complement complex (C5b-9) in endomysial capillaries. C5b-9 is deposited in a patchy fashion in endothelial regions of scattered, enlarged endomysial capillaries (panel A). A high power image (panel B) shows C5b-9 deposition in four enlarged capillaries surrounding a single muscle fibre. A second high power image (panel C) illustrates the patchy nature of the C5b-9 deposition within the enlarged capillaries. (A, bar = 14 µm; B and C, bar = 7 µm). (D) Normal muscle shows no endomysial capillary staining for C5b-9 (bar = 12 µm). syndromes mononuclear cell infiltration of the endomysium and focal cellular invasion of muscle fibres are the rule. Specific pathological features may be more common in subgroups of inflammatory or immune myopathies. In Jo-1 antibody associated myositis a common feature is inflammation in, and fragmentation of, perimysial connective tissue. 7 Notable features in other syndromes include cytochrome oxidase negative muscle fibres in a group of patients with polymyositis unresponsive to corticosteroid treatment, 18 and inclusion bodies in inclusion body myositis. 19 In dermatomyositis and Jo-1 antibody associated myositis, a perifascicular localisation of muscle fibre pathology is common. Perivascular inflammation may be more prominent when immune myopathies occur in the setting of a systemic connective tissue disease, 20 but can also be found in disorders with no clear immune pathogenesis, such as inclusion body myositis and some muscular dystrophies. Capillary pathology somewhat similar to that in our patients with myopathy and anti-srp antibodies has been described in dermatomyositis 15 and in necrotising myopathy with pipestem capillaries. 21 Deposition of the complement component C5b-9 (membrane attack complex) in capillaries, a reduction in the capillary density (capillary index), and enlargement of endomysial capillaries is common to the anti- SRP syndrome and those other two disorders. Enlarged capillaries with thickened PAS positive walls and small lumens as described in the pipestem capillary syndrome were not present in muscles from patients with anti-srp antibodies. The capillary pathology in the anti-srp antibody syndrome with C5b-9 deposition and enlarged lumens and outside diameters is similar to the changes reported in dermatomyositis. However, the capillary pathology, enlarged size, and C5b-9 deposition in the anti-srp antibody syndrome occurred diffusely throughout the muscle rather than having a patchy distribution as is typical of dermatomyositis. 22 Other differences from dermatomyositis in patients with anti-srp antibody associated myopathies included the severe diffuse weakness, absence of rash, and, in the muscle biopsy, prominently increased endomysial connective tissue and relatively enlarged muscle fibres that often appeared hypertrophied or hypercontracted. Further, none of our control patients with typical dermatomyositis syndromes had serum anti-srp antibodies. Clinical, laboratory, and pathological features of the anti-srp syndrome also distinguish it from other immune myopathy syndromes (table 4). There are few of the systemic features such as skin disorders, arthritis, interstitial lung disease, or associated neoplasms that occur in other myositis syndromes. The anti-srp syndrome with rapidly progressive severe proximal weakness, occasionally associated with prominent weight loss has clinical similarities to paraneoplastic necrotic myopathies. 13 However, the syndromes differ in their pathology. In paraneoplastic necrotic myopathies, large regions of necrotic C5b-9 positive muscle fibres are typical features, 23 while prominently increased endomysial connective tissue or enlarged capillaries are not usually present (table 3). This differs from the muscle pathology in the anti-srp syndrome, with its appearance of a chronic active myopathy, including prominent endomysial connective tissue and scattered necrotic muscle fibres that are only rarely positive for C5b-9. The explanation for the prominently increased connective tissue in the anti-srp syndrome might be inhibition of muscle fibre regeneration, or stimulation of fibroblasts by antibodies, as is found in systemic sclerosis 24 or fibrogenic cytokines. 25 Another common feature of anti-srp myopathies that differs from many immune or inflammatory myopathies is the rarity, or absence, of foci of mononuclear inflammatory cells. Other than the CD68 and acid phosphatase positive cells associated with necrotic muscle fibres, anti-srp biopsies show few or no foci of perimysial or endomysial mononuclear cells, and no focal invasion of muscle fibres by mononuclear cells. Groups of CD3 positive inflammatory cells were only detected in one patient (patient 1). In contrast to inclusion body myositis and some types of polymyositis, 26 MHC-I antigen was not prominently expressed on muscle fibres, except in scattered regenerating fibres, in most of the biopsies. The improvement after corticosteroid treatment in patients with myopathies and anti-srp antibodies suggests that the syndrome may be immune mediated. Several features in muscle biopsies from patients with anti-srp antibodies support the idea that immune mechanisms, especially humoral factors, may play a role in the pathogenesis of the myopathy. First, perimysial connective tissue showed staining for alkaline phosphatase in biopsies from three anti-srp patients. In our experience, staining of perimysial connective tissue for alkaline phosphatase occurs commonly in immune mediated myopathies and rarely in muscular dystrophies or inclusion body myositis. 7 Second, the most consistent pathological feature suggesting the presence of a humoral immune disorder is the pattern of non-inflammatory capillary pathology in all anti-srp patients. This pathological pattern is similar to that found in dermatomyositis, a disorder in which humoral immune mechanisms are thought to play a prominent role. The pattern of prominent vascular pathology could suggest that muscle fibre damage in anti-srp antibody associated myopathies is related to ischaemia. The frequent finding of myopathic grouping multiple foci of small rounded, muscle fibres that
8 Myopathy with anti-srp antibodies 427 Table 4 Comparative features in selected immune myopathy syndromes Myopathy syndrome Clinical features Pathological features SRP antibodies Onset: autumn, acute, adult Muscle fibres: degeneration, regeneration. Endomysial Weakness: severe, proximal Serum CK: very high Steroid responsive connective tissue: increased. Endomysial capillaries: diffuse pathology, reduced number, enlarged, MAC deposition. Inflammation: minimal Jo-1 antibodies Onset: spring, adult Muscle fibres: perifascicular myopathy. Endomysial Weakness: moderate, proximal Features: interstitial pneumonitis, Raynaud s, arthritis Serum CK: high Steroid responsive capillaries: normal. Perimysium: fragmentation. Inflammation: perimysial, macrophage Paraneoplastic (necrotic) Onset: acute, older adult Muscle fibres: regional necrosis, MAC deposition in Weakness: severe, proximal Serum CK: very high Steroid responsive sarcoplasm. Inflammation: within muscle fibres; macrophage Dermatomyositis Onset age: child or adult Muscle fibres: perifascicular atrophy. Endomysial connective Weakness: proximal > distal Features: rash Serum CK: high Steroid responsive tissue: normal. Endomysial capillaries: regional pathology, reduced number, enlarged, MAC deposition. Inflammation: perivascular, lymphocytic Myositis + mitochondrial abnormalities Onset age: older adult Weakness: quadriceps, slowly progressive Serum CK: normal or mildly high Steroid resistant Muscle fibres: focal invasion by inflammatory cells; cytochrome oxidase negative fibres. Inflammation: endomysial, lymphocytic often appear to be immature or regenerating might support the idea of a multifocal ischaemic pathology. The relation of antibody binding to SRP, an intracellular antigen, to the pathogenesis of the associated myopathy syndrome is uncertain. It has been difficult to show that antibodies directed against intracellular antigens play a role in any neuromuscular disorder. 27 SRP is a ubiquitous protein complex in eukaryotic organisms that docks newly translated proteins at the endoplasmic reticulum. 910 This function involves binding of a hydrophobic signal sequence on nascent proteins and targeting of the ribosome nascent protein SRP complex to the membrane through a GTP dependent interaction with the SRP receptor. It will be interesting to study whether anti-srp antibodies, or other serum factors, from our patients with myopathies are capable of interfering with any phase of this process in cells, either in general or in muscle fibres in particular. Overall, characteristic clinical features of myopathies associated with anti-srp antibodies include rapid progression of weakness over a period of months, culminating in severe disability. The anti-srp syndrome may be more common than previously recognised. We identified seven patients with anti- SRP antibodies in a three year period, from a total of 95 patients diagnosed in our clinical and pathological service with immune or inflammatory myopathies. Further, the anti- SRP antibody has been detected in 14% of European patients with immune mediated myopathies. 4 Pathologically, the myopathy shows active muscle fibre degeneration and regeneration and a prominent increase in endomysial connective tissue, but little or no mononuclear cell inflammation. The pathological features suggesting an immune pathogenesis, including small vessels, with altered morphology and complement deposition, and perimysial connective tissue, with alkaline phosphatase staining, may be missed on routine muscle histochemistry. Clinically, the myopathy with anti-srp antibodies should be included in the differential diagnosis of syndromes with rapidly progressive weakness and a high serum CK, especially when the muscle biopsy shows some of the characteristic pathological features described here. Strength may improve when corticosteroid treatment is given early. However, confirmation of appropriate treatment strategies will require further study.... Authors affiliations T Miller, M T Al-Lozi, G Lopate, A Pestronk, Washington University School of Medicine, Department of Neurology, St Louis, Missouri, USA Competing interests: none declared REFERENCES 1 Dalakas MC. Polymyositis, dermatomyositis and inclusion-body myositis. N Engl J Med 1991;325: Targoff IN, Miller FW, Medsger TA, et al. Classification criteria for the idiopathic inflammatory myopathies. Curr Opin Rheumatol 1997;9: Hilton-Jones D. Inflammatory muscle diseases. Curr Opin Neurol 2001;14: Brouwer R, Hengstman GJ, Vree Egberts W, et al. Autoantibody profiles in the sera of European patients with myositis. Ann Rheum Dis 2001;60: Targoff IN. Update on myositis-specific and myositis associated autoantibodies. Curr Opin Rheumatol 2000;12: Schmidt WA, Wetzel W, Friedlander R, et al. Clinical and serological aspects of patients with anti-jo-1 antibodies an evolving spectrum of disease manifestations. Clin Rheumatol 2000;19: Mozaffar T, Pestronk A. Myopathy with anti-jo-1 antibodies: pathology in perimysium and neighbouring muscle fibers. J Neurol Neurosurg Psychiatry 2000;68: Targoff IN, Johnson AE, Miller FW. Antibody to signal recognition particle in polymyositis. Arthritis Rheum 1990;33: Grosshans H, Deinert K, Hurt E, et al. Biogenesis of the signal recognition particle (SRP) involves import of SRP proteins into the nucleolus, assembly with the SRP-RNA, and Xpo1p-mediated export. J Cell Biol 2001;153: Keenan RJ, Freymann DM, Stroud RM, et al. The signal recognition particle. Annu Rev Biochem 2001;70: Pestronk A, Lopate G, Kornberg AJ, et al. Distal lower motor neuron syndrome with high titer serum IgM anti-gm1 antibodies: Improvement following immunotherapy with monthly plasma exchange and intravenous cyclophosphamide. Neurology 1994;44: Levin MI, Mozaffar T, Al-Lozi MT, et al. Paraneoplastic necrotizing myopathy: clinical and pathological features. Neurology 1998;50: Bohan A, Peter JB, Bowman RL, et al. Computer-assisted analysis of 153 patients with polymyositis and dermatomyositis. Medicine (Baltimore) 1977;56: Arahata K, Engel AG. Monoclonal antibody analysis of mononuclear cells in myopathies. IV: cell-mediated cytotoxicity and muscle fiber necrosis. Ann Neurol 1988;23: Emslie-Smith AM, Engel AG. Microvascular changes in early and advanced dermatomyositis: a quantitative study. Ann Neurol 1990;27: Bertorini T. Histopathology of the inflammatory myopathies. In: Dalakas MC, ed. Polymyositis and dermatomyositis. Boston: Butterworths, 1988:
9 428 Miller, Al-Lozi, Lopate, et al 17 Carpenter S, Karpati G. Pathology of skeletal muscle, 2nd ed. New York: Oxford University Press, 2001: Blume G, Pestronk A, Frank B, et al. Polymyositis with cytochrome oxidase negative muscle fibers: early quadriceps weakness and poor response to immunosuppressive therapy. Brain 1997;120: Oldfors A, Fyhr IM. Inclusion body myositis: genetic factors, aberrant protein expression, and autoimmunity. Curr Opin Rheumatol 2001;13: Ringel SP, Carry MR, Aguilera AJ, et al. Quantitative histopathology of the inflammatory myopathies. Arch Neurol 1986;43: Emslie-Smith AM, Engel AG. Necrotizing myopathy with pipestem capillaries, microvascular deposition of the complement membrane attack complex (MAC), and minimal cellular infiltration. Neurology 1991;41: Kissel JT, Halterman RK, Rammohan KW, et al. The relationship of complement-mediated microvasculopathy to the histologic features and clinical duration of disease in dermatomyositis. Arch Neurol 1991;48: Pestronk A. Paraneoplastic necrotizing myopathy. In: Neuromuscular disease center [online]. Available at: neuromuscular/pathol/parneonec.htm (accessed June 10, 2002). 24 Chizzolini C, Raschi E, Rezzonico R, et al. Autoantibodies to fibroblasts induce a proadhesive and proinflammatory fibroblast phenotype in patients with systemic sclerosis. Arthritis Rheum 2002;46: Blobe GC, Schiemann WP, Lodish HF. Role of transforming growth factor β in human disease. N Engl J Med 2000;342: Englund P, Lindroos E, Nennesmo I, et al. Skeletal muscle fibers express major histocompatibility complex class II antigens independently of inflammatory infiltrates in inflammatory myopathies. Am J Pathol 2001;159: Posner JB. Anti-Hu autoantibody associated sensory neuropathy/ encephalomyelitis: a model of paraneoplastic syndrome. Perspect Biol Med 1995;38: NEUROLOGICAL PICTURE... Periodic limb movement syndrome P atients with periodic limb movement syndrome (PLMS) experience a series of involuntary leg movements at sleep onset and during sleep. The movements are rhythmic or jerky and range from simple extension of the big toe to movement of the whole leg, with flexion of the knee and hip. They generally occur every seconds and last seconds. A 65 year old woman was referred to our department for differential diagnosis of suspected sleep apnoea syndrome. At presentation she reported excessive daytime sleepiness and mild snoring. Polysomnography revealed PLMS of both legs, with an index score of 89 (fig 1). When the condition was explained to her, she reflected for a moment and said, now I know why I can always tell which way around my sheets go on my bed. The patient later brought in a fitted terry bedsheet with two well worn areas at one end, corresponding to the position of her feet in bed (fig 2). Ad hoc exmination of a new terry sheet showed that repeated rubbing rapidly causes noticeable roughening of the surface. With continuing wear the fabric gradually becomes threadbare and finally tears. Bedding in disarray is a well known feature of PLMS. The increased use of fitted terry sheets may offer a new diagnostic sign for this syndrome discrete areas of wear from foot movement in bed. A Knoblauch, JD Leuppi Center for Sleep Medicine and Home Ventilation, Kantonsspital St.Gallen, Switzerland Correspondence to: Dr A Knoblauch, Pulmonary Department and Center for Sleep Medicine, Kantonsspital St Gallen, CH-9007 St.Gallen, Switzerland; anknoblauch@kssg.ch Figure 1 Four minute section of polysomnograph tracing showing periodic movements of both legs (circle). Figure 2 The patient reported that she replaces about four bedsheets every year because they wear out near the bottom.
10 Myopathy with antibodies to the signal recognition particle: clinical and pathological features T Miller, M T Al-Lozi, G Lopate and A Pestronk J Neurol Neurosurg Psychiatry : doi: /jnnp Updated information and services can be found at: References alerting service These include: This article cites 24 articles, 5 of which you can access for free at: Receive free alerts when new articles cite this article. Sign up in the box at the top right corner of the online article. Topic Collections Articles on similar topics can be found in the following collections Muscle disease (257) Musculoskeletal syndromes (537) Neuromuscular disease (1311) Radiology (1747) Surgical diagnostic tests (401) Immunology (including allergy) (1943) Pain (neurology) (763) Notes To request permissions go to: To order reprints go to: To subscribe to BMJ go to:
Myopathy with anti-jo-1 antibodies: pathology in perimysium and neighbouring muscle fibres
 472 Department of Neurology, Washington University School of Medicine, St Louis, MO 63110, USA T MozaVar A Pestronk Correspondence to: Dr Alan Pestronk, Department of Neurology, Box 8111, 660 South Euclid
472 Department of Neurology, Washington University School of Medicine, St Louis, MO 63110, USA T MozaVar A Pestronk Correspondence to: Dr Alan Pestronk, Department of Neurology, Box 8111, 660 South Euclid
Case 1: History of J.H. Outside Evaluation. Outside Labs. Question #1
 Case 1: History of J.H. 64 yo man seen at UCSF 6-256 25-07. 9 months ago onset progressive weakness of arms and legs, with muscle atrophy in arms. 4 months ago red scaly rash on face, back of hands and
Case 1: History of J.H. 64 yo man seen at UCSF 6-256 25-07. 9 months ago onset progressive weakness of arms and legs, with muscle atrophy in arms. 4 months ago red scaly rash on face, back of hands and
The many faces of myositis. Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands
 The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
Idiopathic inflammatory myopathies excluding inclusion body myositis
 Idiopathic inflammatory myopathies excluding inclusion body myositis Marianne de Visser, Dept. of Neurology, Academic Medical Centre, Amsterdam, The Netherlands The idiopathic inflammatory myopathies (IIMs),
Idiopathic inflammatory myopathies excluding inclusion body myositis Marianne de Visser, Dept. of Neurology, Academic Medical Centre, Amsterdam, The Netherlands The idiopathic inflammatory myopathies (IIMs),
Autoantibodies in the Idiopathic Inflammatory Myopathies
 Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
IDIOPATHIC INFLAMMATORY MYOPATHIES AND RELATED DISORDERS. Franclo Henning Division of Neurology Tygerberg Hospital
 IDIOPATHIC INFLAMMATORY MYOPATHIES AND RELATED DISORDERS Franclo Henning Division of Neurology Tygerberg Hospital Classification systems Clinical (Bohan and Peter) Clinico-pathological (Dalakas & others)
IDIOPATHIC INFLAMMATORY MYOPATHIES AND RELATED DISORDERS Franclo Henning Division of Neurology Tygerberg Hospital Classification systems Clinical (Bohan and Peter) Clinico-pathological (Dalakas & others)
EDX in Myopathies Limitations. EDX in Myopathies Utility Causes of Myopathy. Myopathy: Issues for Electromyographers
 Electrodiagnostic Assessment of Myopathy Myopathy: Issues for Electromyographers Often perceived as challenging Ian Grant Division of Neurology QEII Health Sciences Centre Halifax NS CNSF EMG Course June
Electrodiagnostic Assessment of Myopathy Myopathy: Issues for Electromyographers Often perceived as challenging Ian Grant Division of Neurology QEII Health Sciences Centre Halifax NS CNSF EMG Course June
An autoimmune perspective on neuromuscular diseases
 An autoimmune perspective on neuromuscular diseases Colin Chalk MD,CM FRCPC Montreal General Hospital McGill University Schlomchik 2001 The proportion of neuromuscular patients who have an autoimmune cause
An autoimmune perspective on neuromuscular diseases Colin Chalk MD,CM FRCPC Montreal General Hospital McGill University Schlomchik 2001 The proportion of neuromuscular patients who have an autoimmune cause
Muscle Pathology Surgical Pathology Unknown Conference. November, 2008 Philip Boyer, M.D., Ph.D.
 Muscle Pathology Surgical Pathology Unknown Conference November, 2008 Philip Boyer, M.D., Ph.D. Etiologic Approach to Differential Diagnosis Symptoms / Signs / Imaging / Biopsy / CSF Analysis Normal Abnormal
Muscle Pathology Surgical Pathology Unknown Conference November, 2008 Philip Boyer, M.D., Ph.D. Etiologic Approach to Differential Diagnosis Symptoms / Signs / Imaging / Biopsy / CSF Analysis Normal Abnormal
Inflammatory Myopathies 4 th year MBBS. Marwan Adwan MBChB, MSc, MRCPI, MRCP(rheum) Consultant Rheumatologist
 Inflammatory Myopathies 4 th year MBBS Marwan Adwan MBChB, MSc, MRCPI, MRCP(rheum) Consultant Rheumatologist Case A 64 woman presents with erythematous itchy rash over back of hands & forehead. For 1 month
Inflammatory Myopathies 4 th year MBBS Marwan Adwan MBChB, MSc, MRCPI, MRCP(rheum) Consultant Rheumatologist Case A 64 woman presents with erythematous itchy rash over back of hands & forehead. For 1 month
POLYMYOSITIS (PM) DERMATOMYOSITIS (DM) Body myositis Eosinophilic myositis Giant cell myositis Focal / localised myositis Myopathies caused by
 POLYMYOSITIS (PM) DERMATOMYOSITIS (DM) Body myositis Eosinophilic myositis Giant cell myositis Focal / localised myositis Myopathies caused by infections, drugs, toxins Definition Epidemiology Pathogenesis
POLYMYOSITIS (PM) DERMATOMYOSITIS (DM) Body myositis Eosinophilic myositis Giant cell myositis Focal / localised myositis Myopathies caused by infections, drugs, toxins Definition Epidemiology Pathogenesis
Chronic focal polymyositis in the adult
 Journal of Neurology, Neurosurgery, and Psychiatry, 1981, 44, 419-425 Chronic focal polymyositis in the adult N E BHARUCHA AND J A MORGAN-HUGHES From the Institute of Neurology, Queen Square, London S
Journal of Neurology, Neurosurgery, and Psychiatry, 1981, 44, 419-425 Chronic focal polymyositis in the adult N E BHARUCHA AND J A MORGAN-HUGHES From the Institute of Neurology, Queen Square, London S
Answers to Self Assessment Questions
 Answers to Self Assessment Questions 1. Which of the following findings is supportive of the diagnosis of multifocal motor neuropathy (MMN): A. Absence of conduction block (CB) on nerve conduction studies
Answers to Self Assessment Questions 1. Which of the following findings is supportive of the diagnosis of multifocal motor neuropathy (MMN): A. Absence of conduction block (CB) on nerve conduction studies
Myopathy with anti-hmgcr antibodies: Perimysium and myofiber pathology
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Myopathy with anti-hmgcr antibodies: Perimysium and myofiber pathology Ali Alshehri Washington University School
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Myopathy with anti-hmgcr antibodies: Perimysium and myofiber pathology Ali Alshehri Washington University School
Rheumatology E-learning. University of Szeged Department of Rheumatology and Immunology
 Rheumatology E-learning University of Szeged Department of Rheumatology and Immunology Introduction Idiopathic inflammatory myopathies (IIM) are a group of systemic diseases characterized by an immune
Rheumatology E-learning University of Szeged Department of Rheumatology and Immunology Introduction Idiopathic inflammatory myopathies (IIM) are a group of systemic diseases characterized by an immune
Autoantibodies andprognosis. Jiří Vencovský Institute of Rheumatology, Prague, Czech Republic
 Autoantibodies andprognosis Jiří Vencovský Institute of Rheumatology, Prague, Czech Republic HeterogeneityofIIMs Diagnosis Polymyositis Dermatomyositis IBM Necrotising myopathy Paraneoplastic Amyopathic
Autoantibodies andprognosis Jiří Vencovský Institute of Rheumatology, Prague, Czech Republic HeterogeneityofIIMs Diagnosis Polymyositis Dermatomyositis IBM Necrotising myopathy Paraneoplastic Amyopathic
Myositis and Your Lungs
 Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Diseases of Muscle and Neuromuscular Junction
 Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
CLINICAL AND LABORATORY FEATURES OF NEUROPATHIES WITH SERUM IgM BINDING TO TS-HDS
 CLINICAL AND LABORATORY FEATURES OF NEUROPATHIES WITH SERUM IgM BINDING TO TS-HDS ALAN PESTRONK, MD, 1,2 ROBERT E. SCHMIDT, MD, PhD, 2 RATI M. CHOKSI, MS, 1 R. BRIAN SOMMERVILLE, MD, 1 and MUHAMMAD T.
CLINICAL AND LABORATORY FEATURES OF NEUROPATHIES WITH SERUM IgM BINDING TO TS-HDS ALAN PESTRONK, MD, 1,2 ROBERT E. SCHMIDT, MD, PhD, 2 RATI M. CHOKSI, MS, 1 R. BRIAN SOMMERVILLE, MD, 1 and MUHAMMAD T.
III./10.4. Diagnosis. Introduction. A.) Laboratory tests. Laboratory tests, electrophysiology, muscle biopsy, genetic testing, imaging techniques
 III./10.4. Diagnosis Laboratory tests, electrophysiology, muscle biopsy, genetic testing, imaging techniques After studying this chapter, you will become familiar with the most commonly used diagnostic
III./10.4. Diagnosis Laboratory tests, electrophysiology, muscle biopsy, genetic testing, imaging techniques After studying this chapter, you will become familiar with the most commonly used diagnostic
4/16/2018. Demystifying weakness: how to approach refractory myositis. Objectives. Disclosures. Off-label uses for medications will be discussed
 Demystifying weakness: how to approach refractory myositis Jemima Albayda, MD Assistant Professor Johns Hopkins Myositis center Disclosures Off-label uses for medications will be discussed Objectives To
Demystifying weakness: how to approach refractory myositis Jemima Albayda, MD Assistant Professor Johns Hopkins Myositis center Disclosures Off-label uses for medications will be discussed Objectives To
What your autoantibodies tell us about your disease. Mark Gourley, MD
 What your autoantibodies tell us about your disease Mark Gourley, MD The Importance of the Immune System Defends us against foreign invaders Self (cancer) and Nonself (virus, bacteria, etc.) But, if the
What your autoantibodies tell us about your disease Mark Gourley, MD The Importance of the Immune System Defends us against foreign invaders Self (cancer) and Nonself (virus, bacteria, etc.) But, if the
Rituximab Therapy for Myopathy Associated With Anti Signal Recognition Particle Antibodies: A Case Series
 Arthritis Care & Research Vol. 62, No. 9, September 2010, pp 1328 1334 DOI 10.1002/acr.20219 2010, American College of Rheumatology ORIGINAL ARTICLE Rituximab Therapy for Myopathy Associated With Anti
Arthritis Care & Research Vol. 62, No. 9, September 2010, pp 1328 1334 DOI 10.1002/acr.20219 2010, American College of Rheumatology ORIGINAL ARTICLE Rituximab Therapy for Myopathy Associated With Anti
L. Nandini Moorthy, MD MS 2012
 L. Nandini Moorthy, MD MS 2012 L Nandini Moorthy, MD MS 09 17 yo Ashkenazi male with proximal muscle pain and weakness, mild malar erythema and erythema over knees and dorsal aspect of PIPs Mild tenderness
L. Nandini Moorthy, MD MS 2012 L Nandini Moorthy, MD MS 09 17 yo Ashkenazi male with proximal muscle pain and weakness, mild malar erythema and erythema over knees and dorsal aspect of PIPs Mild tenderness
Treatment of multifocal motor neuropathy with interferon-β1a
 Treatment of multifocal motor neuropathy with interferon-β1a 12 MMN RM Van den Berg-Vos, LH Van den Berg, H Franssen, PA Van Doorn, ISJ Martina, JHJ Wokke Adapted from Neurology 2000; 54: 1518-1521. Chapter
Treatment of multifocal motor neuropathy with interferon-β1a 12 MMN RM Van den Berg-Vos, LH Van den Berg, H Franssen, PA Van Doorn, ISJ Martina, JHJ Wokke Adapted from Neurology 2000; 54: 1518-1521. Chapter
Two simple, reliable and valid tests of proximal muscle function, and their application to the management of idiopathic inflammatory myositis
 Rheumatology 26;45:874 879 Advance Access publication 31 January 26 Two simple, reliable and valid tests of proximal muscle function, and their application to the management of idiopathic inflammatory
Rheumatology 26;45:874 879 Advance Access publication 31 January 26 Two simple, reliable and valid tests of proximal muscle function, and their application to the management of idiopathic inflammatory
Myosites du sujet âgé
 Myosites du sujet âgé Olivier Benveniste Département de Médecine Interne Centre de Référence Maladies Neuro-Musculaires Equipe Muscle Inflammatoire U974 Groupe Hospitalier Pitié-Salpêtrière Myositis classification
Myosites du sujet âgé Olivier Benveniste Département de Médecine Interne Centre de Référence Maladies Neuro-Musculaires Equipe Muscle Inflammatoire U974 Groupe Hospitalier Pitié-Salpêtrière Myositis classification
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM. Andrzej Sladkowski
 Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies
 Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
Distal chronic spinal muscular atrophy involving the hands
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Clinical Laboratory. 14:41:00 Complement Component 3 50 mg/dl Oct-18
 Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Thyroid Peroxidase (TPO) Antibody 5.0 IU/mL [0.0-9.0] 18-289-900139 16-Oct-18 Complement Component 3 50 mg/dl 18-289-900139
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Thyroid Peroxidase (TPO) Antibody 5.0 IU/mL [0.0-9.0] 18-289-900139 16-Oct-18 Complement Component 3 50 mg/dl 18-289-900139
Clinical Laboratory. [None
 Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Double-Stranded DNA (dsdna) Ab IgG ELISA Detected * [None 18-289-900151 Detected] Double-Stranded DNA (dsdna) Ab IgG
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Double-Stranded DNA (dsdna) Ab IgG ELISA Detected * [None 18-289-900151 Detected] Double-Stranded DNA (dsdna) Ab IgG
SCLERODERMA OVERLAP SYNDROME: A CASE REPORT Diwakar K. Singh 1, Nataraju H. V 2
 SCLERODERMA OVERLAP SYNDROME: A Diwakar K. Singh 1, Nataraju H. V 2 HOW TO CITE THIS ARTICLE: Diwakar K. Singh, Nataraju H. V. Scleroderma Overlap Syndrome: A Case Report. Journal of Evolution of Medical
SCLERODERMA OVERLAP SYNDROME: A Diwakar K. Singh 1, Nataraju H. V 2 HOW TO CITE THIS ARTICLE: Diwakar K. Singh, Nataraju H. V. Scleroderma Overlap Syndrome: A Case Report. Journal of Evolution of Medical
Idiopathic inflammatory myopathies
 Myositis and cancer Idiopathic inflammatory myopathies Primary idiopathic polymyositis Primary idiopathic dermatomyositis Juvenile poly/dermatomyositis Myositis associated with another CTD Myositis associated
Myositis and cancer Idiopathic inflammatory myopathies Primary idiopathic polymyositis Primary idiopathic dermatomyositis Juvenile poly/dermatomyositis Myositis associated with another CTD Myositis associated
Citation The Journal of dermatology, 37(1), available at
 NAOSITE: Nagasaki University's Ac Title Author(s) Case of localized scleroderma assoc Muroi, Eiji; Ogawa, Fumihide; Yamao Sato, Shinichi Citation The Journal of dermatology, 37(1), Issue Date 2010-01 URL
NAOSITE: Nagasaki University's Ac Title Author(s) Case of localized scleroderma assoc Muroi, Eiji; Ogawa, Fumihide; Yamao Sato, Shinichi Citation The Journal of dermatology, 37(1), Issue Date 2010-01 URL
Idiopathic inflammatory muscle diseases. Dr. Paul Etau Ekwom MBChB, MMED Kenyatta National Hospital, Nairobi-Kenya
 Idiopathic inflammatory muscle diseases. Dr. Paul Etau Ekwom MBChB, MMED Kenyatta National Hospital, Nairobi-Kenya I.W, 28 YRS, FEMALE SHOP STEWARD Referred to KNH on 16/06/09 from Thika Nursing Home Weakness
Idiopathic inflammatory muscle diseases. Dr. Paul Etau Ekwom MBChB, MMED Kenyatta National Hospital, Nairobi-Kenya I.W, 28 YRS, FEMALE SHOP STEWARD Referred to KNH on 16/06/09 from Thika Nursing Home Weakness
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Enterprise Interest Nothing to declare
 Enterprise Interest Nothing to declare A rare cause of myopathy in adults Jorge Pinheiro MD, José Manuel Lopes MD, PhD Joint Slide Seminar Electron Microscopy and Trainees: Understanding diseases through
Enterprise Interest Nothing to declare A rare cause of myopathy in adults Jorge Pinheiro MD, José Manuel Lopes MD, PhD Joint Slide Seminar Electron Microscopy and Trainees: Understanding diseases through
Budsakorn Darawankul, MD. Maharat Nakhon Ratchasima Hospital
 Budsakorn Darawankul, MD. Maharat Nakhon Ratchasima Hospital Outline What is ANA? How to detect ANA? Clinical application Common autoantibody in ANA diseases Outline What is ANA? How to detect ANA? Clinical
Budsakorn Darawankul, MD. Maharat Nakhon Ratchasima Hospital Outline What is ANA? How to detect ANA? Clinical application Common autoantibody in ANA diseases Outline What is ANA? How to detect ANA? Clinical
Chapter 5 Inclusion Body Myositis
 Chapter 5 Inclusion Body Myositis Lawrence J. Kagen Abstract Inclusion body myositis is an insidious, slowly progressive myopathy of middle-aged and older individuals. Because of these characteristics,
Chapter 5 Inclusion Body Myositis Lawrence J. Kagen Abstract Inclusion body myositis is an insidious, slowly progressive myopathy of middle-aged and older individuals. Because of these characteristics,
Tools to Aid in the Accurate Diagnosis of. Connective Tissue Disease
 Connective Tissue Disease Tools to Aid in the Accurate Diagnosis of Connective Tissue Disease Connective Tissue Disease High quality assays and novel tests Inova offers a complete array of assay methods,
Connective Tissue Disease Tools to Aid in the Accurate Diagnosis of Connective Tissue Disease Connective Tissue Disease High quality assays and novel tests Inova offers a complete array of assay methods,
The Internist s Approach to Neuropathy
 The Internist s Approach to Neuropathy VOLKAN GRANIT, MD, MSC ASSISTANT PROFESSOR OF NEUROLOGY NEUROMUSCU LAR DIVISION UNIVERSITY OF MIAMI, MILLER SCHOOL OF MEDICINE RELEVANT DECLARATIONS Financial disclosures:
The Internist s Approach to Neuropathy VOLKAN GRANIT, MD, MSC ASSISTANT PROFESSOR OF NEUROLOGY NEUROMUSCU LAR DIVISION UNIVERSITY OF MIAMI, MILLER SCHOOL OF MEDICINE RELEVANT DECLARATIONS Financial disclosures:
Genetics of Inclusion Body Myositis
 Genetics of Inclusion Body Myositis Thomas Lloyd, MD, PhD Associate Professor of Neurology and Neuroscience Co-director, Johns Hopkins Myositis Center Sporadic IBM (IBM) Age at onset usually > 50 Prevalence
Genetics of Inclusion Body Myositis Thomas Lloyd, MD, PhD Associate Professor of Neurology and Neuroscience Co-director, Johns Hopkins Myositis Center Sporadic IBM (IBM) Age at onset usually > 50 Prevalence
Disorders of Muscle. Disorders of Muscle. Muscle Groups Involved in Myopathy. Needle Examination of EMG. History. Muscle Biopsy
 Disorders of Muscle Disorders of Muscle Zakia Bell, M.D. Associate Professor of Neurology and Physical Medicine & Rehabilitation Virginia Commonwealth University Cardinal symptom of diseases of the muscle
Disorders of Muscle Disorders of Muscle Zakia Bell, M.D. Associate Professor of Neurology and Physical Medicine & Rehabilitation Virginia Commonwealth University Cardinal symptom of diseases of the muscle
Novel Classification of Idiopathic Inflammatory Myopathies Based on Overlap Syndrome Features and Autoantibodies
 Novel Classification of Idiopathic Inflammatory Myopathies Based on Overlap Syndrome Features and Autoantibodies Analysis of 100 French Canadian Patients Yves Troyanov, MD, Ira N. Targoff, MD, Jean-Luc
Novel Classification of Idiopathic Inflammatory Myopathies Based on Overlap Syndrome Features and Autoantibodies Analysis of 100 French Canadian Patients Yves Troyanov, MD, Ira N. Targoff, MD, Jean-Luc
Case Report Development of Eosinophilic Fasciitis during Infliximab Therapy for Psoriatic Arthritis
 Case Reports in Rheumatology Volume 2016, Article ID 7906013, 4 pages http://dx.doi.org/10.1155/2016/7906013 Case Report Development of Eosinophilic Fasciitis during Infliximab Therapy for Psoriatic Arthritis
Case Reports in Rheumatology Volume 2016, Article ID 7906013, 4 pages http://dx.doi.org/10.1155/2016/7906013 Case Report Development of Eosinophilic Fasciitis during Infliximab Therapy for Psoriatic Arthritis
myopathy and interstitial lung dise
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case of primary Sjögren's syndrom myopathy and interstitial lung dise Koga, Tomohiro; Kouhisa, Yukiko; Na Akinari; Motomura, Masakatsu; Kawak
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case of primary Sjögren's syndrom myopathy and interstitial lung dise Koga, Tomohiro; Kouhisa, Yukiko; Na Akinari; Motomura, Masakatsu; Kawak
Test Name Results Units Bio. Ref. Interval
 LL - LL-ROHINI (NATIONAL REFERENCE 135091593 Age 25 Years Gender Male 30/8/2017 91600AM 30/8/2017 93946AM 31/8/2017 84826AM Ref By Final COLLAGEN DISEASES ANTIBODY ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF),
LL - LL-ROHINI (NATIONAL REFERENCE 135091593 Age 25 Years Gender Male 30/8/2017 91600AM 30/8/2017 93946AM 31/8/2017 84826AM Ref By Final COLLAGEN DISEASES ANTIBODY ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF),
Inclusion body myositis: an underdiagnosed
 Department of Immunology, University Hospital, Queen's Medical Centre, Nottingham NG7 2UH, United Kingdom N D Hopkinson R J Powell Department of Histopathology, University Hospital, Queen's Medical Centre,
Department of Immunology, University Hospital, Queen's Medical Centre, Nottingham NG7 2UH, United Kingdom N D Hopkinson R J Powell Department of Histopathology, University Hospital, Queen's Medical Centre,
Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18
![Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18 Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18](/thumbs/95/125595183.jpg) Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Rheumatoid Factor
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Rheumatoid Factor
Anesthesia recommendations for patients suffering from Welander distal myopathy
 orphananesthesia Anesthesia recommendations for patients suffering from Welander distal myopathy Disease name: Welander distal myopathy ICD 10: G71.0 Synonyms: late adult onset type 1 distal myopathy;
orphananesthesia Anesthesia recommendations for patients suffering from Welander distal myopathy Disease name: Welander distal myopathy ICD 10: G71.0 Synonyms: late adult onset type 1 distal myopathy;
Medicine. Observational Study OPEN
 Observational Study Medicine Atorvastatin-induced necrotizing autoimmune myositis An emerging dominant entity in patients with autoimmune myositis presenting with a pure polymyositis phenotype Yves Troyanov,
Observational Study Medicine Atorvastatin-induced necrotizing autoimmune myositis An emerging dominant entity in patients with autoimmune myositis presenting with a pure polymyositis phenotype Yves Troyanov,
British Journal of Rheumatology 1991; 30:
 British Journal of Rheumatology 1991; 30:468-470 CASE REPORT CARPAL TUNNEL SYNDROME COMPLICATED BY REFLEX SYMPATHETIC DYSTROPHY SYNDROME BY M.-A. FITZCHARLES AND J.M. ESDAILE Rheumatic Disease Unit, McGill
British Journal of Rheumatology 1991; 30:468-470 CASE REPORT CARPAL TUNNEL SYNDROME COMPLICATED BY REFLEX SYMPATHETIC DYSTROPHY SYNDROME BY M.-A. FITZCHARLES AND J.M. ESDAILE Rheumatic Disease Unit, McGill
PRACTICAL ROADMAP. MUSCLE WJ van der Spuy
 PRACTICAL ROADMAP MUSCLE WJ van der Spuy MUSCLE Skeletal (striated) Cardiac (striated) Smooth Identification based on Fiber size, shape and presence/absence of branching Number, shape and position of nuclei
PRACTICAL ROADMAP MUSCLE WJ van der Spuy MUSCLE Skeletal (striated) Cardiac (striated) Smooth Identification based on Fiber size, shape and presence/absence of branching Number, shape and position of nuclei
Objectives. Non-Traumatic Muscle Pathologies. Abnormal Muscle Signal Intensity. Inflammatory Myositis. Polymyostis / Dermatomyositis.
 Non-Traumatic Muscle Pathologies Ali Naraghi Division of Musculoskeletal Radiology Joint Department of Medical Imaging University of Toronto Objectives Define the range of non-traumatic pathologies affecting
Non-Traumatic Muscle Pathologies Ali Naraghi Division of Musculoskeletal Radiology Joint Department of Medical Imaging University of Toronto Objectives Define the range of non-traumatic pathologies affecting
Evolving Uses of IVIG in myositis
 Evolving Uses of IVIG in myositis Rossitza I. Chichkova, MD, MS Associate Professor Depts of Neurology and Internal Medicine University of South Florida, Tampa, FL Immune Function In Normal State: Protects
Evolving Uses of IVIG in myositis Rossitza I. Chichkova, MD, MS Associate Professor Depts of Neurology and Internal Medicine University of South Florida, Tampa, FL Immune Function In Normal State: Protects
Functional outcome of myositis patients: Can a low-dose glucocorticoid regimen achieve good functional results?
 Hypothalamus-pituitary-adrenocortical and -gonadal axis in Endothelial RA / M. Cutolo cell activation induced by ANCA? / A.C. Muller EDITORIAL Kobold et al. Functional outcome of myositis patients: Can
Hypothalamus-pituitary-adrenocortical and -gonadal axis in Endothelial RA / M. Cutolo cell activation induced by ANCA? / A.C. Muller EDITORIAL Kobold et al. Functional outcome of myositis patients: Can
Pedro A. Mendez-Tellez, MD
 Critical Illness Polyneuropathy and Myopathy: Epidemiology and Risk Factors Pedro A. Mendez-Tellez, MD Johns Hopkins University Baltimore, Maryland, USA pmendez@jhmi.edu Conflict of Interest I have no
Critical Illness Polyneuropathy and Myopathy: Epidemiology and Risk Factors Pedro A. Mendez-Tellez, MD Johns Hopkins University Baltimore, Maryland, USA pmendez@jhmi.edu Conflict of Interest I have no
Pulmonary And Central Nervous System Involvement In Juvenile Dermatomyositis: Vasculopathy And/Or Steroids As Causative Agents - A Case Report
 ISPUB.COM The Internet Journal of Radiology Volume 4 Number 1 Pulmonary And Central Nervous System Involvement In Juvenile Dermatomyositis: Vasculopathy And/Or Steroids As Causative Agents - A Case Report
ISPUB.COM The Internet Journal of Radiology Volume 4 Number 1 Pulmonary And Central Nervous System Involvement In Juvenile Dermatomyositis: Vasculopathy And/Or Steroids As Causative Agents - A Case Report
Essentials of Human Anatomy & Physiology. The Muscular System
 Essentials of Human Anatomy & Physiology The Muscular System The Muscular System Muscles are responsible for all types of body movement they contract or shorten and are the machine of the body Three basic
Essentials of Human Anatomy & Physiology The Muscular System The Muscular System Muscles are responsible for all types of body movement they contract or shorten and are the machine of the body Three basic
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Myositis 101. Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic, Rochester, MN
 Myositis 101 Steven R. Ytterberg, M.D. Rheumatology Mayo Clinic, Rochester, MN Myositis Association Annual Conference Louisville, KY Sept. 6 & 7, 2018 Disclosures Consulting: Dynavax Pfizer Off-label use:
Myositis 101 Steven R. Ytterberg, M.D. Rheumatology Mayo Clinic, Rochester, MN Myositis Association Annual Conference Louisville, KY Sept. 6 & 7, 2018 Disclosures Consulting: Dynavax Pfizer Off-label use:
This month, we are very pleased to introduce some new tests for Scleroderma as well as some test changes to our existing scleroderma tests/panels.
 February 20, 2017 Client Letter Test Update February 2017 Dear Colleague: This month, we are very pleased to introduce some new tests for Scleroderma as well as some test changes to our existing scleroderma
February 20, 2017 Client Letter Test Update February 2017 Dear Colleague: This month, we are very pleased to introduce some new tests for Scleroderma as well as some test changes to our existing scleroderma
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
UNICORNS, DRAGONS, POLYMYOSITIS AND OTHER MYTHOLOGICAL BEASTS: THE TRUTH ABOUT POLYMYOSITIS
 UNICORNS, DRAGONS, POLYMYOSITIS AND OTHER MYTHOLOGICAL BEASTS: THE TRUTH ABOUT POLYMYOSITIS Tahseen Mozaffar, MD University of California, Irvine Polymyositis is a commonly diagnosed condition in Neurology,
UNICORNS, DRAGONS, POLYMYOSITIS AND OTHER MYTHOLOGICAL BEASTS: THE TRUTH ABOUT POLYMYOSITIS Tahseen Mozaffar, MD University of California, Irvine Polymyositis is a commonly diagnosed condition in Neurology,
Enzyme histochemistry of skeletal muscle
 J. Neurol. Neurosurg. Psychiat., 1966, 29, 23 Enzyme histochemistry of skeletal muscle Part III Neurogenic muscular atrophies VICTOR DUBOWITZ From the Department of Child Health, University of Sheffield
J. Neurol. Neurosurg. Psychiat., 1966, 29, 23 Enzyme histochemistry of skeletal muscle Part III Neurogenic muscular atrophies VICTOR DUBOWITZ From the Department of Child Health, University of Sheffield
Case Report Repository Corticotropin Injection for Treatment of Idiopathic Inflammatory Myopathies
 Case Reports in Rheumatology Volume 2016, Article ID 9068061, 4 pages http://dx.doi.org/10.1155/2016/9068061 Case Report Repository Corticotropin Injection for Treatment of Idiopathic Inflammatory Myopathies
Case Reports in Rheumatology Volume 2016, Article ID 9068061, 4 pages http://dx.doi.org/10.1155/2016/9068061 Case Report Repository Corticotropin Injection for Treatment of Idiopathic Inflammatory Myopathies
How to assess myositis disease activity in a busy general rheumatology clinic
 How to assess myositis disease activity in a busy general rheumatology clinic Patrick Gordon Consultant Rheumatologist / Honorary Senior Lecturer King s Health Partners Email: patrick.gordon2@nhs.net Many
How to assess myositis disease activity in a busy general rheumatology clinic Patrick Gordon Consultant Rheumatologist / Honorary Senior Lecturer King s Health Partners Email: patrick.gordon2@nhs.net Many
Identifying statin-associated autoimmune necrotizing myopathy
 REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will recognize autoimmune necrotizing myopathy if it occurs in their patients taking statins JEMIMA ALBAYDA, MD Division of Rheumatology, Department of
REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will recognize autoimmune necrotizing myopathy if it occurs in their patients taking statins JEMIMA ALBAYDA, MD Division of Rheumatology, Department of
PRIMARY DISEASES OF MYELIN. By: Shifaa Al Qa qa
 PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
Multidisciplinary Diagnosis in Action: Challenging Case Presentations
 Multidisciplinary Diagnosis in Action: Challenging Case Presentations Interstitial Lung Disease: Advances in Diagnosis and Management UCSF CME November 8, 2014 Case 1 69 yo M 3 year history of intermittent
Multidisciplinary Diagnosis in Action: Challenging Case Presentations Interstitial Lung Disease: Advances in Diagnosis and Management UCSF CME November 8, 2014 Case 1 69 yo M 3 year history of intermittent
Expression of anti-srp19 antibody in muscle tissues from patients with autoimmune necrotizing myopathy
 Expression of anti-srp19 antibody in muscle tissues from patients with autoimmune necrotizing myopathy Q. Wang 1, F. Duan 2, P. Liu 3, P.F. Wang 4 and M.X. Wang 5 1 EmergencyDepartment, General Hospital
Expression of anti-srp19 antibody in muscle tissues from patients with autoimmune necrotizing myopathy Q. Wang 1, F. Duan 2, P. Liu 3, P.F. Wang 4 and M.X. Wang 5 1 EmergencyDepartment, General Hospital
CLASSIFICATION OF PERIPHERAL NERVE DISEASES
 DIFFERENTIAL DIAGNOSIS OF NEUROGENIC DISORDERS & MYOPATHIES NEUROPATHY MYOPATHY Weakness distal proximal Sensory loss + 0 Loss of reflexes early late CSF protein elevated normal Electromyography neurogenic
DIFFERENTIAL DIAGNOSIS OF NEUROGENIC DISORDERS & MYOPATHIES NEUROPATHY MYOPATHY Weakness distal proximal Sensory loss + 0 Loss of reflexes early late CSF protein elevated normal Electromyography neurogenic
DOWNLOAD OR READ : MYOPATHIES AND MUSCLE DISEASES HANDBOOK OF CLINICAL NEUROLOGY PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : MYOPATHIES AND MUSCLE DISEASES HANDBOOK OF CLINICAL NEUROLOGY PDF EBOOK EPUB MOBI Page 1 Page 2 myopathies and muscle diseases handbook of clinical neurology myopathies and muscle diseases
DOWNLOAD OR READ : MYOPATHIES AND MUSCLE DISEASES HANDBOOK OF CLINICAL NEUROLOGY PDF EBOOK EPUB MOBI Page 1 Page 2 myopathies and muscle diseases handbook of clinical neurology myopathies and muscle diseases
Complex repetitive discharge on electromyography as a risk factor for malignancy in idiopathic inflammatory myopathy
 ORIGINAL ARTICLE Korean J Intern Med 2014;29:814-821 Complex repetitive discharge on electromyography as a risk factor for malignancy in idiopathic inflammatory myopathy Na Ri Kim 1, Eon Jeong Nam 1, Jong
ORIGINAL ARTICLE Korean J Intern Med 2014;29:814-821 Complex repetitive discharge on electromyography as a risk factor for malignancy in idiopathic inflammatory myopathy Na Ri Kim 1, Eon Jeong Nam 1, Jong
Patogenesi e terapia della Neuropatia Motoria Multifocale
 26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
Human Anatomy and Physiology - Problem Drill 09: The Muscular System
 Human Anatomy and Physiology - Problem Drill 09: The Muscular System Question No. 1 of 10 The muscular system of the human body fulfills many different roles. Which of the following statements about the
Human Anatomy and Physiology - Problem Drill 09: The Muscular System Question No. 1 of 10 The muscular system of the human body fulfills many different roles. Which of the following statements about the
A Tale of Five Demyelinating Neuropathies
 Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
Arthritis Superspeciality Center, Hubli, Karnataka and 2 Department of Rheumatology, SDM Medical College, Dharwad, Karnataka, India.
 JOURNAL OF CASE REPORTS 2015;5(1):147-151 A Rare Case of Juvenile Dermatomyositis Vikram Haridas 1,2, Kiran Haridas 1 1,2 Arthritis Superspeciality Center, Hubli, Karnataka and 2 Department of Rheumatology,
JOURNAL OF CASE REPORTS 2015;5(1):147-151 A Rare Case of Juvenile Dermatomyositis Vikram Haridas 1,2, Kiran Haridas 1 1,2 Arthritis Superspeciality Center, Hubli, Karnataka and 2 Department of Rheumatology,
The Role of Electron Microscopy in the Assessment of Dermatomyositis: A Retrospective Pilot Study on Skeletal Muscle Biopsies
 British Journal of Medicine & Medical Research 3(4): 962-970, 2013 SCIENCEDOMAIN international www.sciencedomain.org The Role of Electron Microscopy in the Assessment of : A Retrospective Pilot Study on
British Journal of Medicine & Medical Research 3(4): 962-970, 2013 SCIENCEDOMAIN international www.sciencedomain.org The Role of Electron Microscopy in the Assessment of : A Retrospective Pilot Study on
ELEVATION OF CREATINE KINASE IN AMYOTROPHIC LATERAL SCLEROSIS
 20 1 ELEVATION OF CREATINE KINASE IN AMYOTROPHIC LATERAL SCLEROSIS Po ten tial Confusion with Pol y m y osi ti s THOMAS M. HARRINGTON, MARC D. COHEN, JOHN D. BARTLESON, and WILLIAM W. GINSBURG Serum creatine
20 1 ELEVATION OF CREATINE KINASE IN AMYOTROPHIC LATERAL SCLEROSIS Po ten tial Confusion with Pol y m y osi ti s THOMAS M. HARRINGTON, MARC D. COHEN, JOHN D. BARTLESON, and WILLIAM W. GINSBURG Serum creatine
Types of osteoarthritis
 ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
Overview of Diagnostic Autoantibodies in Inflammatory Myopathy
 Overview of Diagnostic Autoantibodies in Inflammatory Myopathy Minoru Satoh, M.D., Ph.D. Research Associate Professor of Medicine Division of Rheumatology and Clinical Immunology University of Florida
Overview of Diagnostic Autoantibodies in Inflammatory Myopathy Minoru Satoh, M.D., Ph.D. Research Associate Professor of Medicine Division of Rheumatology and Clinical Immunology University of Florida
Magnetic resonance imaging changes of thigh muscles in myopathy with antibodies to signal recognition particle
 RHEUMATOLOGY Rheumatology 2015;54:1017 1024 doi:10.1093/rheumatology/keu422 Advance Access publication 21 November 2014 Original article Magnetic resonance imaging changes of thigh muscles in myopathy
RHEUMATOLOGY Rheumatology 2015;54:1017 1024 doi:10.1093/rheumatology/keu422 Advance Access publication 21 November 2014 Original article Magnetic resonance imaging changes of thigh muscles in myopathy
Symptomatic pain treatments (carbamazepine and gabapentin) were tried and had only a transient and incomplete effect on the severe pain syndrome.
 Laurencin 1 Appendix e-1 Supplementary Material: Clinical observations Patient 1 (48-year-old man) This patient, who was without a notable medical history, presented with thoracic pain and cough, which
Laurencin 1 Appendix e-1 Supplementary Material: Clinical observations Patient 1 (48-year-old man) This patient, who was without a notable medical history, presented with thoracic pain and cough, which
HASPI Medical Anatomy & Physiology 09a Lab Activity
 HASPI Medical Anatomy & Physiology 09a Lab Activity Name(s): Period: Date: http://www.fallingpixel.com/products/33817/mains/0000-malemuscular_1.jpg The Muscular System The main function of the muscular
HASPI Medical Anatomy & Physiology 09a Lab Activity Name(s): Period: Date: http://www.fallingpixel.com/products/33817/mains/0000-malemuscular_1.jpg The Muscular System The main function of the muscular
Clinical Commissioning Policy Proposition:
 Clinical Commissioning Policy Proposition: Rituximab for chronic inflammatory demyelinating polyradiculoneuropathy (CIDP), multifocal motor neuropathy (MMN), vasculitis of the peripheral nervous system
Clinical Commissioning Policy Proposition: Rituximab for chronic inflammatory demyelinating polyradiculoneuropathy (CIDP), multifocal motor neuropathy (MMN), vasculitis of the peripheral nervous system
Differential Diagnosis of Neuropathies and Compression. Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre
 Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
APPROACH TO PATIENTS WITH POLYARTHRALGIA
 APPROACH TO PATIENTS WITH POLYARTHRALGIA Scott Vogelgesang, MD Division of Immunology University of Iowa No conflicts of interest DEFINITIONS Arthralgia joint pain with no evidence of inflammation Arthritis
APPROACH TO PATIENTS WITH POLYARTHRALGIA Scott Vogelgesang, MD Division of Immunology University of Iowa No conflicts of interest DEFINITIONS Arthralgia joint pain with no evidence of inflammation Arthritis
 MURDOCH RESEARCH REPOSITORY This is the author s final version of the work, as accepted for publication following peer review but without the publisher s layout or pagination. The definitive version is
MURDOCH RESEARCH REPOSITORY This is the author s final version of the work, as accepted for publication following peer review but without the publisher s layout or pagination. The definitive version is
Diagnosis of McArdle's disease in an elderly patient: Case report and review of literature
 ISPUB.COM The Internet Journal of Neurology Volume 9 Number 1 Diagnosis of McArdle's disease in an elderly patient: Case report and review of literature R Makary, A Berger, N Talpur, S Shuja Citation R
ISPUB.COM The Internet Journal of Neurology Volume 9 Number 1 Diagnosis of McArdle's disease in an elderly patient: Case report and review of literature R Makary, A Berger, N Talpur, S Shuja Citation R
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Atlas of Antinuclear Antibodies
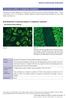 Fluorescence patterns of cytoplasmic autoantigens There are many important organelles in the cytoplasm which fulfill various functions of the cell as described in section 1. Various autoantibodies, known
Fluorescence patterns of cytoplasmic autoantigens There are many important organelles in the cytoplasm which fulfill various functions of the cell as described in section 1. Various autoantibodies, known
Profile, types, duration and severity of muscular dystrophy: a clinical study at a tertiary care hospital
 International Journal of Advances in Medicine Viswajyothi P et al. Int J Adv Med. 2018 Jun;5(3):700-704 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20182126
International Journal of Advances in Medicine Viswajyothi P et al. Int J Adv Med. 2018 Jun;5(3):700-704 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20182126
Test Name Results Units Bio. Ref. Interval
 135091660 Age 44 Years Gender Male 29/8/2017 120000AM 29/8/2017 100219AM 29/8/2017 105510AM Ref By Final EXTRACTABLENUCLEAR ANTIGENS (ENA), QUANTITATIVE ROFILE CENTROMERE ANTIBODY, SERUM 20-30 Weak ositive
135091660 Age 44 Years Gender Male 29/8/2017 120000AM 29/8/2017 100219AM 29/8/2017 105510AM Ref By Final EXTRACTABLENUCLEAR ANTIGENS (ENA), QUANTITATIVE ROFILE CENTROMERE ANTIBODY, SERUM 20-30 Weak ositive
Introduction and aims of the study
 Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment
 Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment 11 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, LH Van den Berg
Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment 11 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, LH Van den Berg
CIDP + MMN - how to diagnose and treat. Dr Hadi Manji
 CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
Discovery, Understanding, and Progress in Myositis
 Discovery, Understanding, and Progress in Myositis Steven Ytterberg, M.D. TMA Annual Patient Conference New Orleans, LA Sept. 2, 2016 Disclosures Financial: Dynavax Corp. Pfizer Mallinckrodt American Board
Discovery, Understanding, and Progress in Myositis Steven Ytterberg, M.D. TMA Annual Patient Conference New Orleans, LA Sept. 2, 2016 Disclosures Financial: Dynavax Corp. Pfizer Mallinckrodt American Board
