Occult anal sphincter injuries myth or reality?
|
|
|
- Marianna Andrews
- 6 years ago
- Views:
Transcription
1 DOI: /j x Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones b a Mayday University Hospital, Croydon, Surrey, UK b School of Computing and Mathematics, Keele University, Stafforshire, UK Correspondence: AH Sultan, Mayday University Hospital, London Road, Croydon, Surrey CR7 7YE, UK. Accepted 28 September Objectives To establish the true prevalence of clinically recognisable and occult obstetric anal sphincter injuries (OASIS). Design Prospective interventional study. Setting Busy district general hospital. Sample Two hundred and fifty-four women having their first vaginal delivery over a 12-month period were invited. Two hundred and forty-one (95%) participated and 208 (86%) attended follow up. Methods Women had a clinical examination at delivery by the accoucheur and repeated by an experienced research fellow immediately after delivery. All identified OASIS were verified and repaired by the duty specialist registrar or consultant. Endoanal ultrasound was performed immediately postpartum prior to suturing and repeated seven weeks later. Main outcome measures Prevalence of recognised and occult anal sphincter injuries. Results Fifty-nine (24.5%) women sustained OASIS. The prevalence of OASIS increased significantly from 11% to 24.5% when women were re-examined. Of these, 30 occurred in deliveries by midwives who missed 26 (87%) and 29 following deliveries by doctors who missed 8 (28%) injuries. All clinically apparent OASIS were also identified on endoanal ultrasound. In addition, three (1.2%) women had an occult anal sphincter injury. Two of these occult sphincter injuries were isolated to the internal anal sphincter (IAS) and would not usually be clinically detectable. Conclusions OASIS occur more frequently than previously reported. Many remain undiagnosed and are subsequently classified as occult when identified on anal endosonography. Genuine occult injuries are rare. Training in perineal anatomy and recognition of OASIS needs to be enhanced in order to increase detection of OASIS and minimise the risk of consequent anal incontinence. Please cite this paper as: Andrews V, Sultan A, Thakar R, Jones P. Occult anal sphincter injuries myth or reality? BJOG 2006; 113: Introduction Obstetric trauma is the major cause of anal incontinence in women and is believed to affect 40,000 mothers (5%) annually in the UK. 1 However, it is largely under reported due to social stigma and embarrassment. Recognised obstetric anal sphincter injuries (OASIS) occur in % of vaginal deliveries in centres practising mediolateral and midline episiotomies, respectively. 2,3 Obstetric-related anal incontinence was previously believed to be largely due to pudendal neuropathy. 4,5 However, following the advent of anal endosonography most of these women demonstrated occult anal sphincter injuries (Fig. 1). A strong association has been shown between anal incontinence and occult anal sphincter injury diagnosed by ultrasound. 6 There are now nine prospective studies 6 14 showing that between 20% and 41% of women sustain occult sphincter injuries. However, it remains to be established whether these injuries are truly occult or represent overt anal sphincter injuries that have either been wrongly classified as a seconddegree tear 1,15 or missed. 16 Furthermore, as OASIS are scrutinised during risk management meetings, there is a disincentive to document these injuries accurately. Previous teaching caused confusion in classification 17 and a recent study by Fernando et al. 1 found that 33% of practising obstetric consultants in the United Kingdom were wrongly classifying external anal sphincter (EAS) tears as second-degree tears. Sultan et al. 15 interviewed 75 trainee doctors and 75 midwives and found that there was considerable inconsistency in their classification, and that most were unaware that anal incontinence was an important consequence of vaginal delivery. Consequently, a new classification was suggested 18 and this has now been accepted by the RCOG 19 and the International Consultation on Incontinence 20 (Table 1). OASIS therefore represent third or fourthdegree tears. Concern has also been raised that some anal ª RCOG 2006 BJOG An International Journal of Obstetrics and Gynaecology 195
2 Andrews et al. Figure 1. Endoanal scan demonstrating anal sphincter defect. Anal endosonographic image of the mid-anal canal demonstrating an anterior EAS defect between the arrows. The adjacent hypoechoic ring (l) is the IAS that also appears fragmented anteriorly. sphincter injuries are being missed at the time of delivery. This has been demonstrated at Queen Charlotte s Hospital, London, 16 where a clinical research fellow examined women who sustained perineal trauma and found that 40% of OASIS were being missed. In view of the anatomical confusion, inconsistency in classification of perineal tears and evidence that OASIS are being missed, we aimed to determine the true prevalence of clinically overt and occult anal sphincter trauma in women having their first vaginal delivery. Table 1. Classification of perineal tears Intact perineum First-degree tear Second-degree tear Third-degree tear Fourth-degree tear No visible tear Injury to skin only Injury to the perineum involving perineal muscles but not the anal sphincter Injury to the perineum involving the anal sphincter complex: 3a: less than 50% external sphincter thickness torn 3b: more than 50% external sphincter thickness torn 3c: IAS torn Injury to the perineum involving the anal sphincter and anal epithelium Methods Women having their first vaginal delivery over a 12-month period between February 2003 and January 2004 at Mayday University Hospital were invited to participate. A trained clinical research fellow (VA) recruited women prior to delivery during office hours, nights and weekends. All consenting women had a repeat perineal and rectal examination by the research fellow immediately after being examined by the accoucheur. In addition, when the delivery was conducted by a doctor, the midwife caring for the woman examined the perineum and her findings were noted. When OASIS were diagnosed they were confirmed by the on-call specialist registrar or consultant. Labour and delivery details were recorded prospectively. Endoanal ultrasound (Fig. 1) was performed in the left lateral position using a 10-MHz 360 rotating probe (B & K Naerum, Denmark). 6,21 All women had endoanal ultrasound scans performed at delivery (prior to suturing) and repeated at seven weeks postpartum. All scans were video recorded and reviewed independently by two experts in endoanal ultrasonography (AHS & RT) who were blinded to the clinical diagnosis. Data were entered into a Microsoft Excel database and analysed by SPSS version 11.0 (Chicago, Illinois, USA). To investigate the change in dependent proportions a McNemar test was used, and to compare proportions in independent groups the x 2 test was used. Women were given written information about the study in the antenatal period and all gave written consent when admitted in labour. Results Over the study period there were a total of 1495 primiparous women who had a vaginal delivery of whom 254 were invited and 241 (16%) consented to participate in the study. Two hundred and thirty-two (96%) were nulliparous and nine (4%) had had a previous caesarean section (none in the second stage of labour). One hundred and seventy-three (72%) deliveries were conducted by midwives and 68 (28%) by doctors. Sixty-three (91%) of the deliveries by doctors were instrumental deliveries (40 vacuum extraction, 23 forceps deliveries). Ninety-eight (41%) had a mediolateral episiotomy performed. The comparable episiotomy and instrumental delivery rates in our institution during the same period were 39% and 21%, respectively. The prevalence of OASIS increased significantly from 11% to 24.5% (McNemar s test P < 0.000) when women were re-examined by the trained research fellow. One hundred and twenty-nine of the 173 (75%) deliveries were performed by midwives with at least five years experience. The diagnosis of injuries by the midwives and research 196 ª RCOG 2006 BJOG An International Journal of Obstetrics and Gynaecology
3 Occult anal sphincter injuries myth or reality? fellow are shown in Table 2. Of the 173 deliveries, midwives classified eight as OASIS of which only four had OASIS confirmed by the research fellow. In a further two cases, the midwife suspected OASIS and requested a doctor s opinion but neither of these were found to have OASIS. In total, 30 sustained OASIS but only 4 were correctly identified by the midwife. Of the remaining 26 OASIS, the midwife made a diagnosis of a second-degree tear in 25 and in one case classified it as a first-degree tear. All 30 women with OASIS had the diagnosis confirmed either by the on-call specialist registrar or consultant and their anal sphincter was repaired in theatre according to a standardised protocol. 22 The remaining 68 deliveries were performed by doctors, 14 by senior house officers under supervision and 54 by specialist registrars. None of the women delivered by doctors had an intact perineum and only one woman had a first-degree tear. Of the 68 deliveries, 22 (32%) had OASIS identified by the doctor performing the delivery and all were confirmed by the research fellow. In a further seven cases OASIS were missed by the doctor performing the delivery. In four cases, the career senior house officer conducting the delivery failed to identify the OASIS that were subsequently confirmed by the duty specialist registrar and research fellow. In three further cases the research fellow identified OASIS that were missed by the duty specialist registrar and these injuries were all confirmed by the on-call consultant. One woman with a second-degree tear was wrongly classified as third degree by a senior house officer. Specialist registrars missed 14% of OASIS, this being significantly less than the 67% missed by senior house officers (x 2 test, P = 0.016). The midwife caring for each woman delivered by a doctor was asked to examine the perineum in the same manner as they would normally do after delivery. Only 1 of the 29 (3.4%) OASIS was identified and no midwife performed a rectal examination. Twenty- seven were classified as second-degree tears and one as first degree. The classification of perineal trauma following deliveries performed by doctors is shown in Table 3. The results of the endoanal ultrasound scan are shown in Table 4. Two hundred and nine (87%) attended follow up at a mean of seven weeks and two days (SD = 16 days). There were 11 discrepancies on scan reports initially that were resolved on review. All women who had OASIS had a sonographic defect at delivery. In addition, there were three defects on ultrasound that were not seen clinically. Two of these involved the internal anal sphincter (IAS) alone and one was a combined defect of the IAS and EAS. No de novo defects were seen at follow up. Discussion Anal incontinence is a social stigma that can have a devastating effect on a woman s quality of life. Although anal sphincter injury remains the major aetiological factor, it was previously largely attributed to occult anal sphincter injuries. 6 Table 2. Rates of perineal trauma in deliveries conducted by midwives. The question mark (?) represents suspected anal sphincter injuries and details of these are given in the Results section Midwives diagnosis (%), n = 173 Research Fellow diagnosis (%), n = 173 Intact perineum 32 (18.5) Intact perineum 24 (13.9) First-degree tear 7 (4) Second-degree tear 1 (0.6) Third/fourth-degree tear 0 First-degree tear 20 (11.6) Intact perineum 5 (2.9) First-degree tear 5 (2.9) Second-degree tear 9 (5.2) Third/fourth-degree tear 1 (0.6) Second-degree tear 111 (64.2) Intact perineum 0 First-degree tear 4 (2.3) Second-degree tear 82 (47.4) Third/fourth-degree tear 25 (14.5) Third/fourth-degree tear 8 (4.6) Intact perineum 0 First-degree tear 0 Second-degree tear 4 (2.3) Third/fourth-degree tear 4 (2.3) Third-degree tear* 2 (1.2) Intact perineum 0 First-degree tear 0 Second-degree tear 2 (1.2) Third/fourth-degree tear 0 *Suspected anal sphincter injuries. See Results section for further details. ª RCOG 2006 BJOG An International Journal of Obstetrics and Gynaecology 197
4 Andrews et al. Table 3. Rates of perineal trauma in deliveries conducted by doctors Delivering doctors diagnosis (%) Research fellow diagnosis (%) Intact perineum 0 0 First-degree tear 1 (1.5) 1 (1.5) Second-degree tear 45 (66.2) 38 (55.9) Third/Fourth-degree tear 22 (32.4) 29 (42.6) This is the first prospective study to accurately establish the prevalence of anal sphincter injury using the new internationally accepted classification of perineal trauma. 18,20 Secondly, this is the first study in which endoanal ultrasound was performed immediately postpartum and then repeated seven weeks later to establish the true prevalence of occult sphincter injuries. To avoid bias, all ultrasound images were reported independently by two clinicians who were blinded to the clinical diagnosis. We found that when a trained research fellow re-examined postpartum women before suturing of the perineum, the prevalence of OASIS increased significantly from 11% to 24.5%. This finding is consistent with another observational study in which the rate of OASIS doubled when women were re-examined. 16 Our findings indicate that the majority of midwives and junior doctors (senior house officers) were failing to identify OASIS. This is in keeping with questionnairebased studies in which the majority of practising doctors and midwives indicated that they were inadequately trained in diagnosing and repairing perineal trauma. 1,15 We therefore believe that our findings are not unique to local practice but probably reflect a more widespread phenomenon. Doctors and midwives were not blinded to the intent of the study because women subsequently found to have OASIS had to have their anal sphincter injury repaired in theatre with written consent. However, their prior knowledge of the study did not appear to affect their clinical practice as the rates of episiotomy and instrumental deliveries did not differ from that of other primiparous women delivering in this unit. All clinically diagnosed OASIS were identified by endoanal ultrasound. In three women, defects were identified by endoanal ultrasound but not seen clinically. Two of these were isolated IAS injuries. It is unclear whether these minor IAS defects were due to clinical disruption or whether they represent distortion of the IAS as a result of the shearing forces during delivery. 6 In practice, isolated IAS injuries would not normally be clinically apparent as the EAS would need to be torn as well. There was only one anal sphincter injury diagnosed by scan that was not recognised at delivery (involving both the IAS and EAS). This may therefore represent a genuine occult sphincter injury. No new defects were identified by ultrasound at follow up that were not seen on the first scan performed immediately after delivery, indicating that all anal sphincter injuries occur at the time of birth and not in the puerperium. This study also demonstrates that following appropriate training, clinical examination can be as accurate as anal endosonography in the immediate postpartum period. However, as postpartum anal endosonography is technically difficult, time consuming, expensive and requires additional expertise, it should not substitute accurate clinical examination. By performing anal endosonography in the immediate postpartum period and repeating it seven weeks later, we have demonstrated that genuine occult sphincter injuries are a rare occurrence. Therefore, almost all occult sphincter injuries described previously 6 14 probably represent missed tears. Although two other studies have shown that endoanal ultrasound is feasible in the postpartum period neither study had independent clinical verification nor were follow up scans performed. 23,24 Table 4. Endoanal ultrasound scan findings Type of injury No. of cases, n = 241 (%) Anal endosonographic defects prior to perineal repair, n = 241 (%) Anal endosonographic defects at follow up, n = 209 (%) Intact perineum 29 (12) 1/29 (3.4) 1/24 (4.2) First-degree tear 17 (7.1) 0/17 (0) 0/16 (0) Second-degree tear 136 (56) 2/136 (1.5) 2/111 (1.8) 3a tear 28 (11.6) 28/28 (100) 0/27 (0) 3b tear 30 (12.4) 30/30 (100) 6/30 (20) 3c tear 0 0/0 (0) 0/0 (0) Fourth-degree tear 1 (0.5) 1 (100) 0/1 (0) All third/fourth-degree tears (OASI) 59 (24.5) 59/59 (100) 6/58 (10) 198 ª RCOG 2006 BJOG An International Journal of Obstetrics and Gynaecology
5 Occult anal sphincter injuries myth or reality? We have also demonstrated that clinical examination at the time of delivery remains the cornerstone of diagnosis of anal sphincter damage. In each case, the research fellow performed a careful examination of the perineum and vagina. In keeping with previous recommendations, 25 he performed a rectal examination to exclude rectal or anal sphincter injury. Visual inspection combined with palpation by performing a pillrolling motion between the index finger in the rectum and the thumb over the anal sphincter 25 improved the detection rate of OASIS. Unfortunately, although most midwifery and obstetric textbooks recommend that a rectal examination should be performed after perineal repair, very few indicate the need for rectal examination before repair. Conclusions Our study has demonstrated that a large number of OASIS are missed at delivery. These injuries that have previously been classified as occult do have clinical relevance as it has been shown that 42% of women who have asymptomatic occult anal sphincter defects after their first vaginal delivery develop faecal incontinence after a subsequent vaginal delivery. 26 It is therefore important that doctors and midwives undergo more focussed and intensive training to recognise these tears at delivery. Recent innovations such as using a specially designed latex model and fresh animal anal sphincters in dedicated hands-on workshops 22 (www. perineum.net) are proving very popular. These hands-on workshops have been shown to change clinical practice of doctors 27 and midwives. 28 Consequently, a fourfold change of practice was noted among midwives who began performing rectal examinations prior to and after perineal repair. Recognition of the deficiencies of current training and more widespread implementation of re-education programmes need reappraisal so as to improve identification of OASIS. Only then can we minimise the risk of developing anal incontinence a physically and socially devastating affliction. Acknowledgements We would like to thank B & K Medical for loaning the scanner to perform this project. Competing interests Mayday University Hospital provides training courses for doctors and midwives in perineal repair. Funding Mayday Childbirth Charity Fund. Ethical approval The study was approved by the Croydon Ethics and Research Committee. j References 1 Fernando RJ, Sultan AH, Radley S, Jones PW, Johanson RB. Management of obstetric anal sphincter injury: a systematic review and national practice survey. BMC Health Serv Res 2002;2:9. 2 Sultan AH, Kamm MA, Hudson CN, Bartram CI. Third degree obstetric anal sphincter tears: risk factors and outcome of primary repair. BMJ 1994;308: Fenner DE, Genberg B, Brahma P, Marek L, DeLancey JOL. Am J Obstet Gynecol 2003;189(6): Snooks SJ, Setchell M, Swash M, Henry MM. Injury to innervation of pelvic floor sphincter musculature in childbirth. Lancet 1984;2: Allen RE, Hosker GL, Smith ARB, Warrell DW. Pelvic floor damage and childbirth: a neurophysiological study. Br J Obstet Gynaecol 1990; 97: Sultan AH, Kamm MA, Hudson CN, Thomas JM, Bartram CI. Anal sphincter disruption during vaginal delivery. N Engl J Med 1993; 329: Donnelly V, Fynes M, Campbell D, Johnson H, O Connell PR, O Herlihy C. Obstetric events leading to anal sphincter damage. Obstet Gynecol 1998;92: Rieger N, Schloithe A, Saccone G, Wattchow D. A prospective study of anal sphincter injury due to childbirth. Scand J Gastroenterol 1998;33: Zetterstrom J, Mellgren A, Jensen LJ, et al. Effect of delivery on anal sphincter morphology and function. Dis Colon Rectum 1999;42: Chaliha C, Sultan AH, Kalia V, Monga AK, Stanton SL. Anal function: effect of pregnancy and delivery. Am J Obstet Gynecol 2001;185: Abramowitz L, Sobhani I, Ganasia R, et al. Are sphincter defects the cause of anal incontinence after vaginal delivery? Results of a prospective study. Dis Colon Rectum 2000;43: Faltin D, Boulvain M, Irion O, Bretones S, Catalin S, Weil A. Diagnosis of anal sphincter tears by postpartum endosonography to predict fecal incontinence. Obstet Gynecol 2000;95(5): Nazir M, Carlsen E, Nesheim B. Do occult anal sphincter injuries, vector volume manometry and delivery variables have any predictive value for bowel symptoms after first time vaginal delivery without third and fourth degree rupture? A prospective study. Acta Obstet Gynecol Scand 2002;81(8): Belmonte-Montes C, Hagerman G, Vega-Yepez PA, Hernandez-de- Anda E, Fonseca-Morales V. Anal sphincter injury after vaginal delivery in primiparous females. Dis Colon Rectum 2001;44(9): Sultan AH, Kamm MA, Hudson CN. Obstetric perineal trauma: an audit of training. J Obstet Gynaecol 1995;15: Groom KM, Paterson-Brown S. Can we improve the diagnosis of third degree tears? Eur J Obstet Gynecol Reprod Biol 2002;101: Sultan AH, Thakar R. Lower genital tract and anal sphincter trauma. Bailliere s Best Pract Res Clin Obstet Gynaecol 2002;16: Sultan AH. Obstetric perineal injury and anal incontinence. Clin Risk 1999;5: Royal College of Obstetricians and Gynaecologists. Management of Third and Fourth Degree Perineal Tears Following Vaginal Delivery. London: RCOG Press, 2001 [RCOG Guideline No. 29]. ª RCOG 2006 BJOG An International Journal of Obstetrics and Gynaecology 199
6 Andrews et al. 20 Norton C, Christiansen J, Butler U, et al. Anal Incontinence. In: Abrams P, Cardozo L, Khoury, Wein A, editors. Incontinence, 2nd edition. Plymouth: Health Publication Ltd, 2002: Thakar R, Sultan AH. Anal endosonography and its role in assessing the incontinent patient. Bailliere s Best Pract Res Clin Obstet Gynaecol 2004;28(1): Thakar R, Sultan AH. Management of obstetric anal sphincter injury. Obstet Gynaecol 2003;5(2): Pretlove SJ, Thompson PJ, Guest P, Toozs-Hobson P, Radley S. Detecting anal sphincter injury: acceptability and feasibility of endo- anal ultrasound immediately post partum. Ultrasound Obstet Gynecol 2003;22: Faltin DL, Boulvain M, Stan C, Epiney M, Weil A, Irion O. Intra- observer and interobserver agreement in the diagnosis of anal sphincter tears by postpartum endosonography. Ultrasound Obstet Gynecol 2003;21: Andrews V, Thakar R, Sultan AH. Management of third and fourth degree tears. Rev Gynaecol Pract 2003;3: Fynes M, Donnelly V, Behan M, O Connell PR, O Herlihy C. Effect of second vaginal delivery on anorectal physiology and faecal incontinence: a prospective study. Lancet 1999;354: Thakar R, Sultan AH, Fernando R, Monga A, Stanton SL. Can workshops on obstetric anal sphincter rupture change practice? Int Urogynecol J Pelvic Floor Dysfunction 2001;12(3):S5. 28 Andrews V, Thakar R, Kettle C, Sultan AH. Do Hands-On training workshops change practice? Proceedings of the XVII European Congress of Obstetrics and Gynaecology, :P ª RCOG 2006 BJOG An International Journal of Obstetrics and Gynaecology
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship?
 DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial
 DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
Clinical Guideline for: The Management of Perineal Trauma following Childbirth
 For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Post-partum Anal Incontinence in SA: A myth or reality?
 Post-partum Anal Incontinence in SA: A myth or reality? TD Naidoo Consultant and Honorary Lecturer, Department of Obstetrics and Gynaecology, Grey s Hospital, Pietermaritzburg Metropolitan Hospitals Complex,
Post-partum Anal Incontinence in SA: A myth or reality? TD Naidoo Consultant and Honorary Lecturer, Department of Obstetrics and Gynaecology, Grey s Hospital, Pietermaritzburg Metropolitan Hospitals Complex,
Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women who sustained a previous obstetric anal sphincter injury
 International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
K. Jundt 1, I. scheer 2, v. von Bodungen 1, F. Krumbachner 1, K. Friese 1, U. M. Peschers 3
 362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
Hands-on Workshop. Cape Town, South Africa 3 August Chairpersons
 Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA
 AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
Anal incontinence after childbirth is more common than was previously believed. Anal incontinence after childbirth. Methods
 Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Obstetric anal sphincter injury is the most common
 Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Ultrasound Imaging of the Anal Sphincter Complex: A Review
 Ultrasound Imaging of the Anal Sphincter Complex: A Review Authors: 1. Zeelha Abdool, FCOG (SA) Consultant Obstetrician & Gynaecologist, University of Pretoria Pretoria, South Africa, 0002 2. Abdul H Sultan
Ultrasound Imaging of the Anal Sphincter Complex: A Review Authors: 1. Zeelha Abdool, FCOG (SA) Consultant Obstetrician & Gynaecologist, University of Pretoria Pretoria, South Africa, 0002 2. Abdul H Sultan
anal incontinence; endoanal ultrasonography; grading systems; obstetric sphincter tears; three-dimensional
 Ultrasound Obstet Gynecol 2012; 40: 207 214 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10154 Incontinence after primary repair of obstetric anal sphincter tears
Ultrasound Obstet Gynecol 2012; 40: 207 214 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10154 Incontinence after primary repair of obstetric anal sphincter tears
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Natural progression of anal incontinence after childbirth
 Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Risk factors and management of obstetric perineal injury
 Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Perineal and Anal Sphincter Trauma
 Perineal and Anal Sphincter Trauma Abdul H. Sultan, Ranee Thakar and Dee E. Fenner (Eds) Perineal and Anal Sphincter Trauma Diagnosis and Clinical Management Abdul H. Sultan, MB ChB, MD, FRCOG Consultant
Perineal and Anal Sphincter Trauma Abdul H. Sultan, Ranee Thakar and Dee E. Fenner (Eds) Perineal and Anal Sphincter Trauma Diagnosis and Clinical Management Abdul H. Sultan, MB ChB, MD, FRCOG Consultant
Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial*
 DOI: 10.1111/j.1471-0528.2008.01726.x www.blackwellpublishing.com/bjog General obstetrics Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial* J Nordenstam, a,b
DOI: 10.1111/j.1471-0528.2008.01726.x www.blackwellpublishing.com/bjog General obstetrics Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial* J Nordenstam, a,b
Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases
 CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Midline episiotomy and anal incontinence: retrospective cohort study
 Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Pregnancy and childbirth: the effects on pelvic floor muscles
 Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Repair of vaginal tears and episiotomy guidelines
 Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?
 DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?.* Mohamed El-Negeri', Mohamed Eltotongy \ Maged Elshamy AbdA. Yasser Abdel Dayem'", waleed Omar \ Waleed Thabet Elrefaei, Department
DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?.* Mohamed El-Negeri', Mohamed Eltotongy \ Maged Elshamy AbdA. Yasser Abdel Dayem'", waleed Omar \ Waleed Thabet Elrefaei, Department
Guideline for Management and Repair of Perineal Trauma
 Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
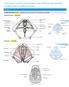 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Obstetric pelvic floor and anal sphincter injuries
 DOI: 10.1111/j.1744-4667.2012.00133.x The Obstetrician & Gynaecologist http://onlinetog.org 2012;14:257 66 Review Obstetric pelvic floor and anal sphincter injuries Farah Lone MBBS MRCOG, a Abdul Sultan
DOI: 10.1111/j.1744-4667.2012.00133.x The Obstetrician & Gynaecologist http://onlinetog.org 2012;14:257 66 Review Obstetric pelvic floor and anal sphincter injuries Farah Lone MBBS MRCOG, a Abdul Sultan
Pregnancy and delivery: a urodynamic viewpoint
 British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
Introduction. A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus.
 TD Naidoo J Moodley Introduction A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus. Faecal incontinence is a complaint of involuntary loss
TD Naidoo J Moodley Introduction A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus. Faecal incontinence is a complaint of involuntary loss
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
for a review under the Accident Compensation Act
 FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence
 American Journal of Obstetrics and Gynecology (2005) 193, 512 8 www.ajog.org The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence Vikki McKinnie, MD, a Steven
American Journal of Obstetrics and Gynecology (2005) 193, 512 8 www.ajog.org The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence Vikki McKinnie, MD, a Steven
In healthy young women, anal sphincter tear at
 Risk Factors for Anal Sphincter Tear During Vaginal Delivery Mary P. FitzGerald, MD, Anne M. Weber, MD, MS, Nancy Howden, MD, MS, Geoffrey W. Cundiff, MD, and Mort B. Brown, PhD, for the Pelvic Floor Disorders
Risk Factors for Anal Sphincter Tear During Vaginal Delivery Mary P. FitzGerald, MD, Anne M. Weber, MD, MS, Nancy Howden, MD, MS, Geoffrey W. Cundiff, MD, and Mort B. Brown, PhD, for the Pelvic Floor Disorders
Title: A modified surgical approach to women with obstetric anal sphincter tears
 Reviewer's report Title: A modified surgical approach to women with obstetric anal sphincter tears Version: 3 Date: 27 January 2010 Reviewer: Stig S Norderval Reviewer's report: Review on manuscript entitled:
Reviewer's report Title: A modified surgical approach to women with obstetric anal sphincter tears Version: 3 Date: 27 January 2010 Reviewer: Stig S Norderval Reviewer's report: Review on manuscript entitled:
Does delayed child-bearing increase the risk of levator injury in labour?
 Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem
 Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England,
 DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
Guide to Pelvic Floor Multicompartment Scanning
 Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
PREPARED FOR: U.S. Army Medical Research and Materiel Command Fort Detrick, Maryland
 AD Cooperative Agreement DAMD17-95-2-5003 TITLE: The Non-Invasive Detection and Characterization of Anal Incontinence in the Parous Soldier Robert L. Hays COL Scott Benjamin PRINCIPAL INVESTIGATOR: Hugh
AD Cooperative Agreement DAMD17-95-2-5003 TITLE: The Non-Invasive Detection and Characterization of Anal Incontinence in the Parous Soldier Robert L. Hays COL Scott Benjamin PRINCIPAL INVESTIGATOR: Hugh
CURRICULUM VITAE. Fida F Asali. M.B, B.S, MSc, MRCOG, DFSRH
 CURRICULUM VITAE Fida F Asali M.B, B.S, MSc, MRCOG, DFSRH Assistant Professor in Obstetrics and Gynaecology Consultant in Obstetrics and Gynaecology Faculty of Medicine The Hashemite University 1 Personal
CURRICULUM VITAE Fida F Asali M.B, B.S, MSc, MRCOG, DFSRH Assistant Professor in Obstetrics and Gynaecology Consultant in Obstetrics and Gynaecology Faculty of Medicine The Hashemite University 1 Personal
Correlation of three dimensional anorectal manometry and three dimensional endoanal ultrasound findings in primi gravida: a cross sectional study
 DOI 10.1186/s13104-015-1346-y RESEARCH ARTICLE Open Access Correlation of three dimensional anorectal manometry and three dimensional endoanal ultrasound findings in primi gravida: a cross sectional study
DOI 10.1186/s13104-015-1346-y RESEARCH ARTICLE Open Access Correlation of three dimensional anorectal manometry and three dimensional endoanal ultrasound findings in primi gravida: a cross sectional study
Interventions METHODS
 Prevention of postpartum stress incontinence PREVENTION OF POSTPARTUM STRESS INCONTINENCE 69 There is good evidence that postnatal pelvic floor exercises are effective in the treatment of postpartum stress
Prevention of postpartum stress incontinence PREVENTION OF POSTPARTUM STRESS INCONTINENCE 69 There is good evidence that postnatal pelvic floor exercises are effective in the treatment of postpartum stress
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention
 Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention Katariina Laine, MD PhD thesis 2013 Katariina Laine, MD Department of Obstetrics Oslo University Hospital, Ullevål
Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention Katariina Laine, MD PhD thesis 2013 Katariina Laine, MD Department of Obstetrics Oslo University Hospital, Ullevål
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION. Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital
 ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Repair of Perineal trauma, including 3 rd and 4 th degree tear
 MATERNITY GUIDELINES Repair of Perineal trauma, including 3 rd and 4 th degree tear Navigation Guidance document in the contents page the Press Ctrl on your keyboard and click on a heading to navigate
MATERNITY GUIDELINES Repair of Perineal trauma, including 3 rd and 4 th degree tear Navigation Guidance document in the contents page the Press Ctrl on your keyboard and click on a heading to navigate
Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor parameters
 British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1360-1365 Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor
British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1360-1365 Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 5, Issue 1 2015 Article 4 The Effect Of Lateral Sphincterotomy On The Anal Sphincter Complex In Chronic Anal Fissure Assesed By Perioperative Transperineal Ultrasonography
World Journal of Colorectal Surgery Volume 5, Issue 1 2015 Article 4 The Effect Of Lateral Sphincterotomy On The Anal Sphincter Complex In Chronic Anal Fissure Assesed By Perioperative Transperineal Ultrasonography
SAUGA WORKSHOP DURBAN 2009
 SAUGA WORKSHOP DURBAN 2009 6 MARCH 2009: Inkosi Albert Luthuli Central Hospital 7 MARCH 2009: Sun Coast Casino INVITATION 2 ND ANNOUNCEMENT A warm welcome to the third biennial symposium of the South African
SAUGA WORKSHOP DURBAN 2009 6 MARCH 2009: Inkosi Albert Luthuli Central Hospital 7 MARCH 2009: Sun Coast Casino INVITATION 2 ND ANNOUNCEMENT A warm welcome to the third biennial symposium of the South African
Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula
 BJOG: an International Journal of Obstetrics and Gynaecology July 2002, Vol. 109, pp. 828 832 Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula Christine Murray,
BJOG: an International Journal of Obstetrics and Gynaecology July 2002, Vol. 109, pp. 828 832 Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula Christine Murray,
Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair
 SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
Abstract. Introduction
 Original article doi:10.1111/codi.12740 Assessment of pubovisceral muscle defects and levator hiatal dimensions in women with faecal incontinence after vaginal delivery: is there a correlation with severity
Original article doi:10.1111/codi.12740 Assessment of pubovisceral muscle defects and levator hiatal dimensions in women with faecal incontinence after vaginal delivery: is there a correlation with severity
Impact of Delivery Types on Women s Postpartum Sexual Health
 Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May Dr. Annie Leong MBBS, FRANZCOG, CU
 EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or???
 Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS
 P.L. Chou, et al ORIGINAL ARTICLE FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS Pei-Ling Chou, Fang-Ping Chen*, Li-Fen Teng Department of Obstetrics and Gynecology, Keelung Chang Gung
P.L. Chou, et al ORIGINAL ARTICLE FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS Pei-Ling Chou, Fang-Ping Chen*, Li-Fen Teng Department of Obstetrics and Gynecology, Keelung Chang Gung
A scoring system for the assessment of bowel and lower urinary tract symptoms in women
 BJOG: an International Journal of Obstetrics and Gynaecology April 2002, Vol. 109, pp. 424 430 A scoring system for the assessment of bowel and lower urinary tract symptoms in women L. Hiller a, H.D. Bradshaw
BJOG: an International Journal of Obstetrics and Gynaecology April 2002, Vol. 109, pp. 424 430 A scoring system for the assessment of bowel and lower urinary tract symptoms in women L. Hiller a, H.D. Bradshaw
Papers. Abstract. Introduction. Methods
 Conservative management of persistent postnatal urinary and faecal incontinence: randomised controlled trial Topic: 66;68;159;161 Cathryn M A Glazener, G Peter Herbison, P Don Wilson, Christine MacArthur,
Conservative management of persistent postnatal urinary and faecal incontinence: randomised controlled trial Topic: 66;68;159;161 Cathryn M A Glazener, G Peter Herbison, P Don Wilson, Christine MacArthur,
Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes?
 Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes? Lawrence M. Leeman, MD, Rebecca G. Rogers, MD, Betsy Greulich, CNM, and Leah L. Albers, DrPH Background: To compare
Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes? Lawrence M. Leeman, MD, Rebecca G. Rogers, MD, Betsy Greulich, CNM, and Leah L. Albers, DrPH Background: To compare
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
ENTRY INTO SPECIALTY TRAINING USING THE CESR (CP) ROUTE DETAILS OF PREVIOUS POSTS IN OBSTETRICS & GYNAECOLOGY PRIOR TO APPOINTMENT TO NTN
 ENTRY INTO SPECIALTY TRAINING USING THE CESR (CP) ROUTE DETAILS OF PREVIOUS POSTS IN OBSTETRICS & GYNAECOLOGY PRIOR TO APPOINTMENT TO NTN PERSONAL DETAILS Trainee name Surname Forename(s) NTN Details NTN
ENTRY INTO SPECIALTY TRAINING USING THE CESR (CP) ROUTE DETAILS OF PREVIOUS POSTS IN OBSTETRICS & GYNAECOLOGY PRIOR TO APPOINTMENT TO NTN PERSONAL DETAILS Trainee name Surname Forename(s) NTN Details NTN
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Endoanal MR Imaging of the Anal Sphincter in Fecal Incontinence 1 Elena Rociu, MD Jaap Stoker, MD Andries W. Zwamborn Johan S.
 PELVIC IMAGING Endoanal MR Imaging of the Anal Sphincter in Fecal Incontinence 1 Elena Rociu, MD Jaap Stoker, MD Andries W. Zwamborn Johan S. Laméris, MD Fecal incontinence is a major medical and social
PELVIC IMAGING Endoanal MR Imaging of the Anal Sphincter in Fecal Incontinence 1 Elena Rociu, MD Jaap Stoker, MD Andries W. Zwamborn Johan S. Laméris, MD Fecal incontinence is a major medical and social
A systematic review of etiological factors for postpartum fecal incontinence
 Acta Obstetricia et Gynecologica. 2010; 89: 302 314 ACTA REVIEW A systematic review of etiological factors for postpartum fecal incontinence ESTHER M.J. BOLS 1,2, ERIK J.M. HENDRIKS 1,2, BARY C.M. BERGHMANS
Acta Obstetricia et Gynecologica. 2010; 89: 302 314 ACTA REVIEW A systematic review of etiological factors for postpartum fecal incontinence ESTHER M.J. BOLS 1,2, ERIK J.M. HENDRIKS 1,2, BARY C.M. BERGHMANS
Traumatic injury to the anal sphincter sustained in a thirdor
 Obstetric Anal Sphincter Injuries: A Survey of Clinical Practice Among Canadian Obstetricians Carolyn Best, BSc, MD, FRCSC, Harold P. Drutz, MD, FRCSC, May Alarab, MBChB, MRCOG, MRCPI, MSc Division of
Obstetric Anal Sphincter Injuries: A Survey of Clinical Practice Among Canadian Obstetricians Carolyn Best, BSc, MD, FRCSC, Harold P. Drutz, MD, FRCSC, May Alarab, MBChB, MRCOG, MRCPI, MSc Division of
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
SUTURING AN EPISIOTOMY/GENITAL LACERATION
 WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
Screening, Diagnosis and Management of Gestational Diabetes in New Zealand: A Clinical Practice Guideline
 Screening, Diagnosis and Management of Gestational Diabetes in New Zealand: A Clinical Practice Guideline 6 November 2014 Gary Tonkin Today Process to develop the guideline What the guideline recommends
Screening, Diagnosis and Management of Gestational Diabetes in New Zealand: A Clinical Practice Guideline 6 November 2014 Gary Tonkin Today Process to develop the guideline What the guideline recommends
(UI Urine incontinence)! " # $% &'! ( ) * " " +, -. &/ !!" # $%& /'0 = ='' &!( )'*(" &%: "## $ "% % &' ( )* .!
 39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
Episiotomy and obstetric outcomes among women living with type 3 female genital mutilation: a secondary analysis
 Rodriguez et al. Reproductive Health (2016) 13:131 DOI 10.1186/s12978-016-0242-9 RESEARCH Open Access Episiotomy and obstetric outcomes among women living with type 3 female genital mutilation: a secondary
Rodriguez et al. Reproductive Health (2016) 13:131 DOI 10.1186/s12978-016-0242-9 RESEARCH Open Access Episiotomy and obstetric outcomes among women living with type 3 female genital mutilation: a secondary
A retrospective postal survey of women s experiences of physiotherapy management following a third- or fourth-degree perineal tear
 Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 25 35 CLINICAL PAPER A retrospective postal survey of women s experiences of physiotherapy management following
Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 25 35 CLINICAL PAPER A retrospective postal survey of women s experiences of physiotherapy management following
Care of your Perineum following 3 rd and 4 th degree tears
 Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Until very recently, imaging of the external and internal anal
 PICTORIAL ESSAY Exoanal Imaging of the Anal Sphincters Hans Peter Dietz, MD, PhD, FRANZCOG, DDU, CU Since its introduction in the early 1990s, endoanal sonography has become the mainstay of morphologic
PICTORIAL ESSAY Exoanal Imaging of the Anal Sphincters Hans Peter Dietz, MD, PhD, FRANZCOG, DDU, CU Since its introduction in the early 1990s, endoanal sonography has become the mainstay of morphologic
Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse
 DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
A Clinical Guideline for Bladder Care in Labour and Postnatally
 For Use in: Maternity department By: Clinical staff caring for women during pregnancy, labour and postnatally For: Obstetric patients Division responsible for document: Division 3- Women and Children s
For Use in: Maternity department By: Clinical staff caring for women during pregnancy, labour and postnatally For: Obstetric patients Division responsible for document: Division 3- Women and Children s
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
Faecal incontinence persisting after childbirth: a 12 year longitudinal
 Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
period, cesarean delivery is thought to protect against anal incontinence, 3 albeit incompletely. In this study, we investigated anal incontinence
 Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
The Prevention of Early-onset Neonatal Group B Streptococcal Disease in UK Obstetric Units
 Royal College of Obstetricians and Gynaecologists and London School of Hygiene and Tropical Medicine The Prevention of Early-onset Neonatal Group B Streptococcal Disease in UK Obstetric Units An audit
Royal College of Obstetricians and Gynaecologists and London School of Hygiene and Tropical Medicine The Prevention of Early-onset Neonatal Group B Streptococcal Disease in UK Obstetric Units An audit
RANZCOG Advanced Training Modules
 RANZCOG Advanced Training Modules Generalist Obstetrics ATM and Generalist Gynaecology ATM The Generalist ATMs in each of Obstetrics and Gynaecology provide a framework for trainees to consolidate and
RANZCOG Advanced Training Modules Generalist Obstetrics ATM and Generalist Gynaecology ATM The Generalist ATMs in each of Obstetrics and Gynaecology provide a framework for trainees to consolidate and
Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery
 WOMEN'S HEALTH WOMEN'S HEALTH Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery Sandra A. Baydock, MD, 1 Catherine Flood, MD, 1 Jane A. Schulz, MD, 1 Dianna
WOMEN'S HEALTH WOMEN'S HEALTH Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery Sandra A. Baydock, MD, 1 Catherine Flood, MD, 1 Jane A. Schulz, MD, 1 Dianna
Bladder care postpartum including bladder care for women with epidural analgesia (GL792)
 Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
The Pelvic Floor: Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology
 The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
Perineal Trauma Assessment, Repair and Safe Practice
 1. Purpose This document outlines the guideline and the procedure details for the assessment and repair of perineal trauma in postpartum women. Genital tract trauma can occur spontaneously during a vaginal
1. Purpose This document outlines the guideline and the procedure details for the assessment and repair of perineal trauma in postpartum women. Genital tract trauma can occur spontaneously during a vaginal
