Autoimmune pancreatitis (AIP) can be defined as a
|
|
|
- Stewart Glenn
- 6 years ago
- Views:
Transcription
1 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4: Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI TAKAHASHI, LIZHI ZHANG, JONATHAN E. CLAIN,* RANDALL K. PEARSON,* BRET T. PETERSEN,* SANTHI SWAROOP VEGE,* and MICHAEL B. FARNELL *Division of Gastroenterology and Hepatology, Department of Pathology, Department of Radiology, and Division of Gastroenterologic and General Surgery, Mayo Clinic College of Medicine, Rochester, Minnesota See CME exam on page 934. Background & Aims: The Japan Pancreas Society criteria for diagnosis of autoimmune pancreatitis (AIP) mandate presence of characteristic imaging (diffuse pancreatic enlargement with diffusely irregular, narrow pancreatic duct). AIP has unique histologic features associated with infiltration of tissues of affected organs with abundant IgG4-positive cells. We propose expanded diagnostic criteria for AIP with a cohort of histologically confirmed AIP. Methods: We reviewed the pancreatic imaging findings on computed tomography scans, serum IgG4 levels, other organ involvement, and response to steroids in 29 consecutive patients who met histologic criteria for AIP. Results: Computed tomography scans (n 22) showed diffuse pancreatic enlargement in 6 (27%) patients; the rest had focal enlargement, distinct mass, normal pancreas, or focal acute pancreatitis. Serum IgG4 level was elevated in 15 of 21 (71%) patients, and other organ involvement (eg, intrahepatic biliary strictures) was noted in 11 of 29 (38%) patients. All 17 patients treated with steroids exhibited resolution/marked improvement of pancreatic/extrapancreatic manifestation. On the basis of this experience we propose that diagnosis of AIP can be made in patients with >1 of these criteria: (1) diagnostic histology, (2) characteristic imaging on computed tomography and pancreatography with elevated serum IgG4 level, or (3) response to steroid therapy of pancreatic/extrapancreatic manifestations of AIP. Twenty additional patients met expanded diagnostic criteria for AIP, and their demographic and clinical profile was similar to that of the 29 patients meeting histologic criteria. Conclusions: AIP defined by histological criteria shows a wide spectrum of radiologic features, with characteristic imaging seen only in a minority. Incorporation of additional features into current diagnostic criteria can identify the full spectrum of clinical presentations of AIP. Autoimmune pancreatitis (AIP) can be defined as a systemic fibroinflammatory disease that afflicts not only the pancreas but also a variety of other organs including bile duct, salivary glands, the retroperitoneum, and lymph nodes. Organs affected by AIP have a lymphoplasmacytic infiltrate rich in IgG4-positive cells. 1 The inflammatory process responds to steroid therapy. 2 The diagnosis of AIP currently rests on fulfilling the Japan Pancreas Society s minimal consensus criteria 3 (Table 1), which require the presence of characteristic imaging features, that is, a diffusely enlarged sausage-shaped gland and a diffusely irregular, attenuated pancreatic duct (Figure 1). Histopathologic features of chronic pancreatitis usually encountered in practice do not provide information about its etiology. However, recent studies have shown that pancreatic histology can distinguish AIP from usual chronic pancreatitis and obstructive pancreatitis. 4 6 The histology of AIP, termed lymphoplasmacytic sclerosing pancreatitis (LPSP), is characterized by a lymphoplasmacytic infiltrate around small-sized ducts, swirling fibrosis centered around ducts and veins (storiform fibrosis), and obliterative phlebitis wherein the infiltrate surrounds pancreatic venules while sparing arterioles In addition, pancreatic immunostaining is diagnostic of AIP when it shows abundant IgG4-positive cells, and it can distinguish AIP from alcoholic pancreatitis and inflammatory infiltrate surrounding pancreatic cancer. 14 Similarly, other organs involved in AIP also show abundant tissue infiltration with IgG4-positive cells. 1 Thus, histopathology and immunostaining can be used to diagnose AIP. Abbreviations used in this paper: AIP, autoimmune pancreatitis; CT, computed tomography; HPF, high-power field; LPSP, lymphoplasmacytic sclerosing pancreatitis by the American Gastroenterological Association Institute /06/$32.00 doi: /j.cgh
2 August 2006 DIAGNOSIS OF AUTOIMMUNE PANCREATITIS 1011 Table 1. Japanese Pancreas Society Criteria for AIP 3 Mandatory criteria Typical imaging: diffuse enlargement of pancreas along with diffuse ( 33%) main pancreatic duct narrowing with an irregular wall Supportive criteria (at least one) (1) Serology: autoantibodies, elevated -globulins or IgG (2) Histopathology: lymphoplasmacytic infiltrate and pancreatic fibrosis A review of literature reveals a number of additional features of AIP not included in the Japanese criteria. These include serologic features, other organ involvement, and response to steroids. Serologic abnormalities in AIP include elevated titers of -globulins, IgG, and elevated titers of a variety of antibodies including antinuclear antibody, rheumatoid factor, anti carbonic anhydrase antibody, and antilactoferrin antibody Recently Hamano et al 18 reported that elevated serum levels of the IgG4 subset of IgG were a sensitive and specific marker of AIP. AIP has been traditionally described as being associated with a number of disorders such as primary sclerosing cholangitis, Sjögren s syndrome, and retroperitoneal fibrosis. 19 However, more recent studies suggest that these associations are in fact manifestations of AIP that mimic other well-described diseases. The common thread that links these manifestations is the finding of tissue infiltration with abundant IgG4-positive cells, 11,13,20 a characteristic that distinguishes them from the diseases they mimic. The pancreatic and extrapancreatic manifestations of AIP respond, often dramatically, to steroid therapy, whereas the Figure 1. Diagnostic group A: diagnostic histology. Low-density lesion is seen in the tail of the pancreas (A) with elevated serum IgG4 (450 mg/dl). A core biopsy of the pancreas shows lymphoplasmacytic infiltrate with abundant IgG4-positive cells on immunostaining (B). After prednisone therapy there is resolution of the changes in the pancreatic tail with development of mild atrophy (C). Table 2. Diagnostic Criteria for AIP (The HISORt Criteria): Definitions Histology Category Pancreatic imaging Criteria At least one of the following: (1) Periductal lymphoplasmacytic infiltrate with obliterative phlebitis and storiform fibrosis (LPSP) (2) Lymphoplasmacytic infiltrate with storiform fibrosis showing abundant ( 10 cells/hpf) IgG4-positive cells (Figure 1) Typical: diffusely enlarged gland with delayed (rim) enhancement; diffusely irregular, attenuated main pancreatic duct (Figure 2) Others a : Focal pancreatic mass/enlargement; focal pancreatic duct stricture; pancreatic atrophy; pancreatic calcification; or pancreatitis Serology Elevated serum IgG4 level (normal, mg/dl) Other organ Hilar/intrahepatic biliary strictures, persistent involvement b distal biliary stricture, parotid/lacrimal gland involvement, mediastinal lymphadenopathy, retroperitoneal fibrosis Response to steroid therapy c Resolution/marked improvement of pancreatic/ extrapancreatic manifestation with steroid therapy (Figure 3) a With negative work-up for known etiologies for pancreatic disease, especially pancreatic/biliary cancer. b Radiologic evidence of organ involvement can be confirmed by biopsy showing lymphoplasmacytic infiltrate with abundant IgG4-positive cells or its resolution/improvement with steroid therapy. c Steroid therapy should be given only to patients with negative work-up for known etiologies for pancreatic disease and only to those in whom response can be objectively assessed. It should not be used as a substitute for a thorough search for etiology. diseases they mimic do not. The typical example of this steroid responsiveness is seen in sclerosing cholangitis like biliary strictures in AIP, which respond to steroid therapy, 21,22 whereas typical primary sclerosing cholangitis does not. 23 Since 1999 we have maintained a prospective database of patients investigated for AIP. From this database we identified 29 patients who met histologic criteria for AIP. We describe the histologic, clinical, serologic, and imaging features of these patients and report their response to steroids. On the basis of this experience, we propose new diagnostic criteria for AIP and describe the features of 20 additional patients who met alternate (non-histologic) criteria for AIP. Methods The study was approved by the Mayo Foundation Institutional Review Board. Patients From a database of patients suspected or diagnosed to have AIP, prospectively maintained since 1999 by one of the
3 1012 CHARI ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 4, No. 8 authors (S.T.C.), we identified 29 patients who met histologic criteria for AIP (Table 2). We noted their demographic data and clinical presentation at onset and diagnosis. We also noted the presence of 5 criteria pertaining to histology, imaging, serology, other organ involvement, and response to steroid therapy as defined in Table 2 (the HISORt Criteria). Pancreatic Histology and Immunostaining The resection specimens and core biopsies of the 29 patients were reviewed by a single pathologist (T.C.S.). For tissue immunostaining, monoclonal anti-human IgG4 antibody (Zymed, San Francisco, CA) was applied to 4- m thick sections by using standard immunohistochemical techniques. Peroxidase activity was visualized by applying diaminobenzidine solution containing 0.05% H 2 O 2. Sections were then counterstained with hematoxylin, dehydrated, cleared, and mounted. Appropriate positive and negative controls were run with each batch. The number of immunohistochemically identified IgG4-positive plasma cells per high-power field (HPF) was counted in each specimen (Nikon E 600, field diameter mm; Nikon, Tokyo, Japan). Moderate (11 30 cells/ HPF) to severe ( 30 cells/hpf) infiltration with IgG4-positive cells 1 was considered diagnostic of AIP. Imaging Available pretreatment computed tomography (CT) scans (n 22) were reviewed by a single radiologist (N.T.) blinded to final diagnosis. Pancreatic enlargement was defined as an increase in size of the gland in the absence of a discrete mass. Mass was defined as a lesion that had different density compared with surrounding pancreatic tissue. Available endoscopic retrograde cholangiopancreatograms were reviewed. Serum Immunoglobulin G4 The concentrations of IgG and its subclasses in serum were measured in 21 patients by automated nephelometry. 24 Results are expressed as mean standard error of the mean. Other Organ Involvement Presence or history of other organ involvement (PSClike changes, Sjögren s syndrome like salivary gland disease, mediastinal adenopathy, tubulointerstitial nephritis, and retroperitoneal fibrosis) was noted. Response to Steroid Therapy A total of 17 patients with histologically confirmed AIP received steroids. The indications, dosage, and duration of therapy were noted. Biliary and pancreatic duct strictures were considered steroid-responsive if follow-up imaging showed normal biliary tree and pancreatic duct, respectively. Pancreatic mass/enlargement was considered steroid-responsive if the abnormality resolved, with post-therapy imaging showing normal-appearing pancreas or pancreatic atrophy. Marked improvement was defined as measurable reduction in size but not resolution of pancreatic mass or improvement in ductal irregularity, often permitting removal of stents. Diagnostic Groups On the basis of review of the performance of each of the 5 criteria, we identified combinations that were diagnostic of AIP. Patients who met alternate diagnostic criteria were identified, and their profile was noted and compared with that of patients with AIP meeting histologic criteria. Results Histologically Confirmed Autoimmune Pancreatitis Demographics and presentation. The mean age of the 29 patients was years (range, years), with 23 (79%) being 50 years of age; majority (83%) were male. Presentation at the onset of symptoms was with obstructive jaundice in 23 (73%) patients, with pancreatic mass in 3, and with new-onset diabetes, steatorrhea, and pancreatitis in 1 each. Abdominal pain was present at onset in 10 of 29 (34.5%) patients but was mild in all, and none required narcotics for pain relief. At diagnosis, which was made weeks to years after onset of symptoms, 10 patients already had a resection for pancreatic mass, 7 had obstructive jaundice with distal bile duct stricture, 3 had persistent pancreatic mass, 4 had sclerosing cholangitis, 3 had nonspecific dyspeptic symptoms, and 1 each had weight loss caused by uncontrolled diabetes and steatorrhea. Pancreatic histology and immunostaining. Pancreatic resection specimens (n 13) showed features of LPSP in 12 of 13 patients, and 1 showed extensive fibrosis with intense lymphoplasmacytic infiltrate without obliterative phlebitis. IgG4 immunostaining was positive in 7 of 8 patients including the one who did not show full spectrum of changes of LPSP on histology; 1 patient had only a few IgG4-positive cells, despite showing LPSP on histology. Sixteen subjects underwent pancreatic core biopsy. In 7 of 16 (44%) the full spectrum of diagnostic changes of LPSP were seen. IgG4 immunostaining showed abundant IgG4-positive cells in 15 of 16 patients; 1 patient had only a few IgG4-positive cells, despite showing LPSP on histology. Imaging. Pretreatment CT scans of 22 patients with AIP were available for re-review. Six patients had diffuse pancreatic enlargement, 10 had focal enlargement, and 3 had a distinct mass, 2 were normal, and 1 had changes of acute pancreatitis. Four patients had pancreatic calcification noted on CT at diagnosis or follow-up. A pancreatogram was performed in 7 of 29 patients, 4 with diffuse gland enlargement, 2 with focal enlargement, and 1 with a normal-appearing gland on CT. There was no correlation between CT and pancreatographic findings. Of the 4 with diffuse pancreatic
4 August 2006 DIAGNOSIS OF AUTOIMMUNE PANCREATITIS 1013 Figure 2. Diagnostic group B: typical imaging features. Characteristic diffusely enlarged sausage-shaped gland (A) with pancreatogram showing diffusely irregular narrow pancreatic duct (B). enlargement on CT, 2 had focal strictures, and 2 had diffusely irregular duct on pancreatography. In the 2 with focal pancreatic enlargement on CT, 1 had diffuse irregularity and the other a focal stricture on pancreatography. The patient with a normal-appearing gland on CT had a diffusely irregular pancreatic duct. The wide spectrum of imaging findings in the pancreas is illustrated in Figure 4. Serology. IgG4 was more frequently elevated in AIP than total IgG (15/21 [71%] vs 8/21 [38%]; P.03). All patients with AIP who had elevated total IgG also had IgG4 elevation. Eleven of 12 patients with elevated serum IgG4 who had pancreatic tissue immunostaining showed abundant IgG4-positive cells. However, all 6 patients with normal serum IgG4 levels also had positive tissue immunostaining for IgG4-positive cells. Other organ involvement. Evidence of other organ involvement was seen in 11 of 29 (38%) patients. The organs involved (other than distal common bile duct) included the common hepatic and/or intrahepatic Figure 3. Diagnostic group C: response to steroid therapy. Endoscopic retrograde cholangiopancreatography shows diffuse stricturing of the intrahepatic biliary tree (A) and a diffusely irregular pancreatic duct (B). Serum IgG4 elevated at 870 mg/dl. After 12-week course of prednisone there is nearly complete resolution of intrahepatic strictures and normalization of serum IgG4 levels. Figure 4. Spectrum of CT appearances of the pancreas in AIP. (A) Left panel: diffuse swelling of pancreas, body/tail head with elevated serum IgG4 (351 mg/dl). Right panel: 6 months after completion of steroid course, multiple intraductal calculi (arrow) seen in the absence of pain or clinical pancreatitis. (B) Left panel: peripancreatic fluid collection (arrow) with elevated serum IgG4 (1710 mg/dl). Right panel: 10 months after steroid therapy there is marked pancreatic atrophy. (C) Left panel: unresectable pancreatic body mass with dilatation of duct in the tail with normal serum IgG4. Core biopsy of mass showed abundant IgG4-positive cells. Right panel: 6 weeks after steroid course, there is marked reduction in size of mass. bile duct (n 5), retroperitoneum (n 3), salivary gland (n 2), and mediastinal lymph nodes (n 1). The intrapancreatic portion of the bile duct was frequently involved, and the stricture was indistinguishable from malignant biliary obstruction. Involvement of proximal extrahepatic ducts and intrahepatic biliary tree raised suspicion of primary sclerosing cholangitis and/or cholangiocarcinoma. Response to steroids. A total of 17 patients received steroids. Indications for starting therapy included persistent pancreatic enlargement/mass (n 6), intrahepatic biliary strictures (n 3), obstructive jaundice with distal biliary stricture (n 5), and 1 each with retroperitoneal fibrosis, pancreatitis with pancreatic duct stricture, and uncontrolled diabetes and weight loss. All patients were treated with oral prednisone. The most common regimen involved an induction dose of 40 mg for 4 weeks followed by a taper (5 mg/week) during a period of 8 weeks. The patients have been followed for a median of 6.5 months (range, 2 56 months) after initiation of steroid treatment. All patients have shown complete resolution or marked improvement in the manifestations for which steroids were started. Diagnostic categories. On the basis of this experience we propose new criteria for diagnosis of AIP (Table 3). AIP can be diagnosed in subjects with characteristic histology (LPSP) and/or pancreatic IgG4 immunostaining (group A, Figure 1), in subjects who meet
5 1014 CHARI ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 4, No. 8 Table 3. Diagnostic Groups: Patients Meeting Criteria for 1 of the Groups Have AIP Group A: diagnostic pancreatic histology (Figure 2) Group B: typical imaging serology (Figure 1) Group C: response to steroids (Figure 3) Presence of one or both of the following criteria Resection specimen or core biopsy showing the full spectrum of changes of LPSP, ie, periductal lymphoplasmacytic infiltrate with obliterative phlebitis and storiform fibrosis. Presence of a lymphoplasmacytic infiltrate without other features of LPSP is not diagnostic of AIP. 10 IgG4-positive cells/hpf IgG4 on immunostain of pancreatic lymphoplasmacytic infiltrate. Presence of all the following criteria CT or magnetic resonance imaging scan showing diffusely enlarged pancreas with delayed and rim enhancement Pancreatogram showing diffusely irregular pancreatic duct Elevated serum IgG4 levels Presence of all the following criteria Unexplained pancreatic disease after negative work-up for known etiologies including cancer Elevated serum IgG4 levels and/or other organ involvement confirmed by presence of abundant IgG4-positive cells Resolution/marked improvement in pancreatic and/or extrapancreatic manifestations with steroid therapy Japanese imaging criteria and have elevated serum IgG4 levels (group B, Figure 2), and in subjects in whom their pancreatic/extrapancreatic disease responds to steroid therapy (group C, Figure 3). We reviewed our database and identified an additional 20 patients who met the expanded diagnostic criteria for AIP (Table 4). There was no difference in age distribution, gender, proportion with diffuse pancreatic enlargement, proportion with elevated serum IgG4, or response to steroids among the 3 groups. However, the proportion with other organ involvement was significantly greater in patients in group C, reflecting the fact that these patients were referred predominantly for extrapancreatic manifestations of AIP and often did not have a pancreatic lesion amenable to biopsy. Discussion Unlike usual chronic pancreatitis, AIP is a relatively painless disease, despite histology showing chronic pancreatic inflammation and evidence of pancreatic edema, peripancreatic inflammation, and in some cases pancreatic calculi. Although the most common acute presentation of AIP is with obstructive jaundice, it has protean other manifestations, both pancreatic and extrapancreatic. 1,13,25 29 Many patients present during the postacute phase, months to years after initial presentation, and some might seek medical attention for extrapancreatic disease. In such patients the pancreas might show persistent mass; however, it is more likely that the gland might be atrophic, show calcification, 30 or even be radiographically normal. The wide spectrum of changes on pancreatic imaging in AIP is shown in Figure 4. AIP should be suspected in patients with unexplained pancreatic disease presenting with or having history of obstructive jaundice, pancreatic mass/enlargement, pancreatitis, pancreatic atrophy, or exocrine insufficiency. However, our data suggest that search for AIP in patients with abdominal pain as the predominant symptom is likely to be low yield. In patients presenting with an extrapancreatic manifestation, presence or history of unexplained pancreatic disease or painless chronic pancreatitis might be an important diagnostic clue. In patients suspected to have AIP, the diagnosis can be made in 1 of 3 ways. Regardless of pancreatic imaging features, the diagnosis of AIP can be made if histology shows all features of LPSP (periductal lymphoplasmacytic infiltrate with storiform fibrosis and obliterative phlebitis) or by immunostaining, if the characteristic lymphoplasmacytic infiltrate has 10 IgG4-positive/ HPF (group A, Table 3). Thus, histologic criteria could be considered the gold standard for diagnosis of AIP. A combination of characteristic pancreatic imaging and elevation in serum IgG4 is also diagnostic (group B, Table 3); however, in our study these criteria lacked sensitivity because only 3 patients met these criteria (group C, Table 4). Finally, in patients with a strong suspicion of AIP (idiopathic pancreatic disease associated with elevated serum IgG4 level and/or other organ involvement), the diagnosis can be confirmed if the manifestations, pancreatic and/or extrapancreatic, resolve or markedly improve with steroid therapy (group C, Table 3). Crucial to preoperative identification of AIP is the question of whether the diagnosis of AIP can be made on pancreatic core biopsy specimens. We confirm findings of a recent study by Zamboni et al 5 that pancreatic core biopsies are often nondiagnostic by routine histology alone because they do not show the complete spectrum of diagnostic changes of LPSP due to small sample size and lack of a duct or vein in the biopsy specimen. We show that the diagnostic yield of core biopsies can be significantly enhanced by tissue immunostaining for
6 August 2006 DIAGNOSIS OF AUTOIMMUNE PANCREATITIS 1015 Table 4. Demographic and Clinical Profiles of the 3 Diagnostic Groups Diagnostic groups Median age (y) (range) Gender (% male) Histology Imaging (CT): diffuse pancreatic enlargement Serology: elevated serum IgG4 Other organ involvement Response to steroids Group A: diagnostic histology (n 29) Group B: characteristic imaging with elevated serum IgG4 (n 3) Group C: response to steroids (n 17) 72 a (14 85) 24/29 a (83%) Diagnostic 29/29 (100%) 6/22 (27%) a 15/21 a (71%) 11/29 b (38%) 17/17 a (100%) 59 (38 75) 3/3 (100%) Not done 3/3 (100%) 3/3 (100%) 1/3 (33%) 1/1 (100%) 60.5 (33 77) 14/17 (82%) Supportive (lymphoplasmacytic infiltrate fibrosis) (n 7), nondiagnostic (n 1) 9/17 (53%) 13/16 (81%) 12/17 (71%) 17/17 (100%) a P not significant vs group B or C. b P.03 vs group C. IgG4-positive cells. In our study, although only 7 of 16 (44%) core biopsies showed the full spectrum of diagnostic changes of LPSP, IgG4 immunostaining showed abundant IgG4-positive cells in 15 of 16 patients, and either histology or immunostain was diagnostic in all 16. Apart from histology and imaging, we used serum IgG4 levels and other organ involvement as clinical clues to suspect AIP. We confirm the observation by Hamano et al 18 that serum IgG4 is more sensitive than total serum IgG for diagnosis of AIP. However, we found a lower sensitivity for serum IgG4 compared with that reported by Hamano et al (78% vs 95%). Interestingly, tissue infiltration with IgG4-positive cells was seen even in the absence of elevation in serum levels of IgG4. We found other organ involvement in 24 of 49 (49%) patients with AIP. In patients presenting with jaundice, the presence of unusual extrapancreatic findings such as retroperitoneal fibrosis, intrahepatic biliary strictures, or salivary gland enlargement are important clues to the diagnosis of AIP. In patients with predominantly extrapancreatic disease, immunostaining the tissue from an involved organ to look for infiltration with IgG4-positive cells can provide supportive evidence. 1 We used this approach in the patient with renal failure in whom the kidney biopsy showed IgG4-positive interstitial nephritis. 31 Recent studies suggest that many other organs might be affected by this disease including breast, 32 kidney, 31 and stomach. 33 Future studies are likely to expand the spectrum of this disease considerably, which has appropriately been called systemic IgG4 disease. 13 Although pancreatic histology is the most definitive way to diagnose AIP, in some patients it might not be feasible to obtain pancreatic biopsy. In such patients, response to steroids is helpful in confirming the diagnosis of AIP because no other pancreaticobiliary disease, especially pancreatic cancer, is known to respond to steroids. All 35 patients treated with steroids in our study exhibited significant improvement or resolution of manifestations of AIP. AIP is a fibroinflammatory disorder. The inflammatory component consisting of a lymphoplasmacytic infiltrate resolves with steroid therapy. However, this is accompanied by intense fibrosis that is unaffected by therapy and might cause permanent damage to the affected organ. Therefore, restoration of normal structure and function does not occur in all patients with AIP despite steroid therapy. A note of caution needs to be sounded regarding use of steroid trial for diagnosis of AIP. Steroid trial should not be used as a substitute for a thorough search for etiology and should be given only to patients with negative work-up for known etiologies for pancreatic/biliary disease, especially cancer. Moreover, steroids should only be given to those in whom the response can be objectively assessed. In patients without pancreatic mass/enlargement or manifest extrapancreatic disease, it might be difficult to assess steroid response. In summary, in the absence of a diagnostic serologic test for AIP, its diagnosis rests on identifying unique patterns of abnormalities. The Japanese criteria for AIP focus heavily on characteristic pancreatic imaging and therefore lack sensitivity to diagnose the wide spectrum of manifestations of AIP. The proposed criteria reflect the current understanding of AIP as a systemic steroidresponsive disorder characterized by tissue infiltration with IgG4-positive cells and clearly identify a wider
7 1016 CHARI ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 4, No. 8 spectrum of manifestations of the disease than do the Japanese criteria. Improved understanding of the pathogenesis of AIP will help the development of better diagnostic biomarkers for AIP. References 1. Kamisawa T. IgG4-positive plasma cells specifically infiltrate various organs in autoimmune pancreatitis. Pancreas 2004;29: Kamisawa T, Yoshiike M, Egawa N, et al. Treating patients with autoimmune pancreatitis: results from a long-term follow-up study. Pancreatology 2005;5: Pearson RK, Longnecker DS, Chari ST, et al. Controversies in clinical pancreatology: autoimmune pancreatitis: does it exist? Pancreas 2003;27: Suda K, Takase M, Fukumura Y, et al. Histopathologic characteristics of autoimmune pancreatitis based on comparison with chronic pancreatitis. Pancreas 2005;30: Zamboni G, Luttges J, Capelli P, et al. Histopathological features of diagnostic and clinical relevance in autoimmune pancreatitis: a study on 53 resection specimens and 9 biopsy specimens. Virchows Arch 2004;445: Yadav D, Notahara K, Smyrk TC, et al. Idiopathic tumefactive chronic pancreatitis: clinical profile, histology, and natural history after resection. Clin Gastroenterol Hepatol 2003;1: Weber SM, Cubukcu-Dimopulo O, Palesty JA, et al. Lymphoplasmacytic sclerosing pancreatitis: inflammatory mimic of pancreatic carcinoma. J Gastrointest Surg 2003;7: Kloppel G, Luttges J, Lohr M, et al. Autoimmune pancreatitis: pathological, clinical, and immunological features. Pancreas 2003;27: Abraham SC, Wilentz RE, Yeo CJ, et al. Pancreaticoduodenectomy (Whipple resections) in patients without malignancy: are they all chronic pancreatitis? Am J Surg Pathol 2003;27: Notohara K, Burgart LJ, Yadav D, et al. Idiopathic chronic pancreatitis with periductal lymphoplasmacytic infiltration: clinicopathologic features of 35 cases. Am J Surg Pathol 2003;27: Kamisawa T, Funata N, Hayashi Y, et al. A new clinicopathological entity of IgG4-related autoimmune disease. J Gastroenterol 2003;38: Kamisawa T, Funata N, Hayashi Y, et al. Close relationship between autoimmune pancreatitis and multifocal fibrosclerosis. Gut 2003;52: Kamisawa T, Funata N, Hayashi Y. Lymphoplasmacytic sclerosing pancreatitis is a pancreatic lesion of IgG4-related systemic disease. Am J Surg Pathol 2004;28: Zhang L, Chari ST, Levy MJ, et al. Pancreatic IgG4 stain for diagnosing autoimmune pancreatitis (AIP) and for distinguishing AIP subtypes. Gastroenterology 2005;128:A Okazaki K, Chiba T. Autoimmune related pancreatitis. Gut 2002; 51: Yoshida K, Toki F, Takeuchi T, et al. Chronic pancreatitis caused by an autoimmune abnormality: proposal of the concept of autoimmune pancreatitis. Dig Dis Sci 1995;40: Kino-Ohsaki J, Nishimori I, Morita M, et al. Serum antibodies to carbonic anhydrase I and II in patients with idiopathic chronic pancreatitis and Sjogren s syndrome. Gastroenterology 1996; 110: Hamano H, Kawa S, Horiuchi A, et al. High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med 2001;344: Lara LP, Chari ST. Autoimmune pancreatitis. Curr Gastroenterol Rep 2005;7: Kamisawa T, Egawa N, Nakajima H. Autoimmune pancreatitis is a systemic autoimmune disease. Am J Gastroenterol 2003;98: Nishino T, Toki F, Oyama H, et al. Biliary tract involvement in autoimmune pancreatitis. Pancreas 2005;30: Kojima E, Kimura K, Noda Y, et al. Autoimmune pancreatitis and multiple bile duct strictures treated effectively with steroid. J Gastroenterol 2003;38: Chen W, Gluud C. Glucocorticosteroids for primary sclerosing cholangitis. Cochrane Database Syst Rev 2004;3:CD Vlug A, Nieuwenhuys EJ, van Eijk RV, et al. Nephelometric measurements of human IgG subclasses and their reference ranges. Ann Biol Clin (Paris) 1994;52: Chutaputti A, Burrell MI, Boyer JL. Pseudotumor of the pancreas associated with retroperitoneal fibrosis: a dramatic response to corticosteroid therapy. Am J Gastroenterol 1995;90: Colaut F, Toniolo L, Sperti C, et al. Autoimmune-like pancreatitis in thymoma with myasthenia gravis. Chir Ital 2002;54: Duvic C, Desrame J, Leveque C, et al. Retroperitoneal fibrosis, sclerosing pancreatitis and bronchiolitis obliterans with organizing pneumonia. Nephrol Dial Transplant 2004;19: Eerens I, Vanbeckevoort D, Vansteenbergen W, et al. Autoimmune pancreatitis associated with primary sclerosing cholangitis: MR imaging findings. Eur Radiol 2001;11: Kamisawa T, Matsukawa M, Ohkawa M. Autoimmune pancreatitis associated with retroperitoneal fibrosis. JOP 2005;6: Takayama M, Hamano H, Ochi Y, et al. Recurrent attacks of autoimmune pancreatitis result in pancreatic stone formation. Am J Gastroenterol 2004;99: Takeda S, Haratake J, Kasai T, et al. IgG4-associated idiopathic tubulointerstitial nephritis complicating autoimmune pancreatitis. Nephrol Dial Transplant 2004;19: Zen Y, Kasahara Y, Horita K, et al. Inflammatory pseudotumor of the breast in a patient with a high serum IgG4 level: histologic similarity to sclerosing pancreatitis. Am J Surg Pathol 2005;29: Shinji A, Sano K, Hamano H, et al. Autoimmune pancreatitis is closely associated with gastric ulcer presenting with abundant IgG4-bearing plasma cell infiltration. Gastrointest Endosc 2004; 59: Address requests for reprints to: Suresh T. Chari, MD, 200 First Street SW, Mayo Clinic, Rochester, Minnesota chari. suresh@mayo.edu; fax: (507)
The most common presentation of autoimmune pancreatitis. A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
Autoimmune Pancreatitis: A Great Imitator
 Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
Overview of Diagnostic Criteria for Autoimmune Pancreatitis
 2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic Pancreatitis of Other Etiology
 94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
IgG4-related sclerosing disease
 IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
Autoimmune pancreatitis (AIP) was described more than a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy
 ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
Diagnostic Algorithm for Autoimmune Pancreatitis in Korea
 Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Review Article The Utility of Serum IgG4 Concentrations as a Biomarker
 International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
Immunoglobulin G4-Related Disease with Several Inflammatory Foci
 CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma
 Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
An Autopsy Case of Autoimmune Pancreatitis
 MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA. Dr. Tejaswi Sindhiya Ragni
 AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
Autoimmune pancreatitis
 Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
IgG4 Disease. General Principles of IgG4-related disease. EL Cluvar, AC Bateman
 IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis
 CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Renal manifestations of IgG4-related systemic disease
 Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Autoimmune Pancreatitis and Retroperitoneal Fibrosis
 Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Renal Pathology Case Conference. Case 2
 Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4
 238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease
 Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Strategy to differentiate autoimmune pancreatitis from pancreas cancer
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction
 Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Ulcerative Colitis and Immunoglobulin G4
 Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management
 Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
Histological diagnosis of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study with EUS-FNA
 J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
Autoimmune pancreatitis (AIP), a clinical entity originally
 Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Autoimmune pancreatitis (AIP) is a chronic fibroinflammatory
 Review Article Autoimmune Pancreatitis More Than Just a Pancreatic Disease? A Contemporary Review of Its Pathology Vikram Deshpande, MD; Mari Mino-Kenudson, MD; William Brugge, MD; Gregory Y. Lauwers,
Review Article Autoimmune Pancreatitis More Than Just a Pancreatic Disease? A Contemporary Review of Its Pathology Vikram Deshpande, MD; Mari Mino-Kenudson, MD; William Brugge, MD; Gregory Y. Lauwers,
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings
 Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Type 2 Autoimmune Pancreatitis with Crohn s Disease
 doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
IgG4-related Sclerosing Disease: Autoimmune Pancreatitis and Extrapancreatic
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
IgG4-related systemic disease (ISD) is a multisystem
 Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Overview of the Immunoglobulin G4-related Disease Spectrum
 Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Autoimmune pancreatitis: the classification puzzle
 Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
IgG4-Related Sclerosing Cholangitis
 REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
How 5 Diseases Became One. Moez Tajdin R3 McGill University
 How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
Autoimmune Pancreatitis & Cholangiopathy. Goal and Objectives
 Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis
 Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
 Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Autoimmune Pancreatitis: A Succinct Overview
 REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
Tratamiento endoscópico de la CEP. En quien como y cuando?
 Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Autoimmune Pancreatitis: Pathological Findings
 AISP - 28th National Congress. Verona (Italy). October 28-30, 2004. Autoimmune Pancreatitis: Pathological Findings Günter Klöppel 1, Jutta Lüttges 1, Bence Sipos 1, Paola Capelli 2, Giuseppe Zamboni 2
AISP - 28th National Congress. Verona (Italy). October 28-30, 2004. Autoimmune Pancreatitis: Pathological Findings Günter Klöppel 1, Jutta Lüttges 1, Bence Sipos 1, Paola Capelli 2, Giuseppe Zamboni 2
Hideaki Miura, Yasutaka Miyachi. Department of Internal Medicine, Social Insurance Central General Hospital. Tokyo, Japan
 CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features.
 'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features. Poster No.: C-2649 Congress: ECR 2013 Type: Educational Exhibit Authors: R. P. Patel, T. M. Chandler, S. Barrett, J.
'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features. Poster No.: C-2649 Congress: ECR 2013 Type: Educational Exhibit Authors: R. P. Patel, T. M. Chandler, S. Barrett, J.
Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related Disease
 Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Case Report IgG4-Related Nasal Pseudotumor
 Case Reports in Otolaryngology Volume 2015, Article ID 749890, 4 pages http://dx.doi.org/10.1155/2015/749890 Case Report IgG4-Related Nasal Pseudotumor L. K. Døsen, 1 P. Jebsen, 2 B. Dingsør, 3 and R.
Case Reports in Otolaryngology Volume 2015, Article ID 749890, 4 pages http://dx.doi.org/10.1155/2015/749890 Case Report IgG4-Related Nasal Pseudotumor L. K. Døsen, 1 P. Jebsen, 2 B. Dingsør, 3 and R.
FOR PUBLIC CONSULTATION ONLY. Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD)
 Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD) NHS England FOR PUBLIC CONSULTATION ONLY Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4- RD) First published:
Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD) NHS England FOR PUBLIC CONSULTATION ONLY Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4- RD) First published:
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid
 The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review
 Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Pancreatic Cancer Masquerading as Pancreatitis
 Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term Follow-Up Study of 73 Japanese Patients
 International Rheumatology Volume 2013, Article ID 272595, 8 pages http://dx.doi.org/10.1155/2013/272595 Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term
International Rheumatology Volume 2013, Article ID 272595, 8 pages http://dx.doi.org/10.1155/2013/272595 Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term
University of Texas-MD Anderson Cancer Center, Houston, Texas, USA. University of Medicine and Pharmacy Craiova, Romania
 Case Report A Diagnostic Challenge: Pancreatic Cancer or Autoimmune Pancreatitis? IRINA MIHAELA CAZACU 1,2, ADRIANA ALEXANDRA LUZURIAGA CHAVEZ 1, ADRIAN SAFTOIU 2, TONYA G. WHITLOW 1, PRIYA BHOSALE 3,
Case Report A Diagnostic Challenge: Pancreatic Cancer or Autoimmune Pancreatitis? IRINA MIHAELA CAZACU 1,2, ADRIANA ALEXANDRA LUZURIAGA CHAVEZ 1, ADRIAN SAFTOIU 2, TONYA G. WHITLOW 1, PRIYA BHOSALE 3,
IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal
 CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones
 MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
Calcifying Obstructive Pancreatitis: A Study of Intraductal Papillary Mucinous Neoplasm Associated With Pancreatic Calcification
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:57 63 Calcifying Obstructive Pancreatitis: A Study of Intraductal Papillary Mucinous Neoplasm Associated With Pancreatic Calcification MAURICIO ZAPIACH,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:57 63 Calcifying Obstructive Pancreatitis: A Study of Intraductal Papillary Mucinous Neoplasm Associated With Pancreatic Calcification MAURICIO ZAPIACH,*
Autoimmune Pancreatitis: Case Series and Review of the Literature.
 Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 39, no. 2, 2009 167 Autoimmune Pancreatitis: Case Series and Review of the Literature. Rada Shakov, 1 Joseph R. DePasquale,
Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 39, no. 2, 2009 167 Autoimmune Pancreatitis: Case Series and Review of the Literature. Rada Shakov, 1 Joseph R. DePasquale,
Chronic Sclerosing Dacryoadenitis
 The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Autoimmune Liver Diseases
 2nd Pannonia Congress of pathology Hepato-biliary pathology Autoimmune Liver Diseases Vera Ferlan Marolt Institute of pathology, Medical faculty, University of Ljubljana Slovenia Siofok, Hungary, May 2012
2nd Pannonia Congress of pathology Hepato-biliary pathology Autoimmune Liver Diseases Vera Ferlan Marolt Institute of pathology, Medical faculty, University of Ljubljana Slovenia Siofok, Hungary, May 2012
IgG4 cholangitis Case Report: Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam.
 IgG4 cholangitis New Perspectives on Biliary Tract Disease Case Report: male, 64 yrs, truck driver and car industry worker Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam
IgG4 cholangitis New Perspectives on Biliary Tract Disease Case Report: male, 64 yrs, truck driver and car industry worker Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico
 Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
CME/SAM. Increased Immunoglobulin (Ig) G4 Positive Plasma Cell Density and IgG4/IgG Ratio Are Not Specific for IgG4- Related Disease in the Skin
 Increased Immunoglobulin (Ig) G4 Positive Plasma Cell Density and IgG4/IgG Ratio Are Not Specific for IgG4- Related Disease in the Skin Julia S. Lehman, MD, 1,2 Thomas C. Smyrk, MD, 1 and Mark R. Pittelkow,
Increased Immunoglobulin (Ig) G4 Positive Plasma Cell Density and IgG4/IgG Ratio Are Not Specific for IgG4- Related Disease in the Skin Julia S. Lehman, MD, 1,2 Thomas C. Smyrk, MD, 1 and Mark R. Pittelkow,
Key Points: Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective. Jenny Heathcote, MD. University of Toronto
 Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
Diseases of pancreas - Chronic pancreatitis
 Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids. Cholestasis
 Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
Incidence of Malignancy in Type 1 Autoimmune Pancreatitis
 ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus
 Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus Omar Abu Suliman, MBBS, SB-ORL Senior Registrar, otolaryngology Head & neck surgery King Abdullah Medical City, Makkah,
Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus Omar Abu Suliman, MBBS, SB-ORL Senior Registrar, otolaryngology Head & neck surgery King Abdullah Medical City, Makkah,
IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT
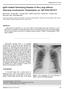 J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
An Intraductal Papillary Neoplasm of the Bile Duct at the Duodenal Papilla
 Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Autoimmune pancreatitis can transform into chronic features similar to advanced
 Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers
 Case Reports in Medicine Volume 2015, Article ID 832463, 4 pages http://dx.doi.org/10.1155/2015/832463 Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers Alessandro
Case Reports in Medicine Volume 2015, Article ID 832463, 4 pages http://dx.doi.org/10.1155/2015/832463 Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers Alessandro
Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor
 International Rheumatology Volume 2012, Article ID 139409, 6 pages doi:10.1155/2012/139409 Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor Arezou Khosroshahi,
International Rheumatology Volume 2012, Article ID 139409, 6 pages doi:10.1155/2012/139409 Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor Arezou Khosroshahi,
IgG4-related hypophysitis presenting as a pituitary adenoma with systemic disease
 Asian Journal of Surgery (2013) 36, 93e97 Available online at www.sciencedirect.com journal homepage: www.e-asianjournalsurgery.com CASE REPORT IgG4-related hypophysitis presenting as a pituitary adenoma
Asian Journal of Surgery (2013) 36, 93e97 Available online at www.sciencedirect.com journal homepage: www.e-asianjournalsurgery.com CASE REPORT IgG4-related hypophysitis presenting as a pituitary adenoma
Evaluation and Management of Refractory Biliary Stricture. J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc.
 Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore
 IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore W. Fong 1,2,3, I. Liew 1, D. Tan 2,3,4, K.H. Lim 5, A. Low 6, Y.Y. Leung 1,2 1 Department of Rheumatology and
IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore W. Fong 1,2,3, I. Liew 1, D. Tan 2,3,4, K.H. Lim 5, A. Low 6, Y.Y. Leung 1,2 1 Department of Rheumatology and
Kazuichi Okazaki 1 and Hisanori Umehara Introduction. 2. The Concept of IgG4-Related Disease
 Hindawi Publishing Corporation International Journal of Rheumatology Volume 2012, Article ID 357071, 9 pages doi:10.1155/2012/357071 Review Article Are Classification Criteria for IgG4-RD Now Possible?
Hindawi Publishing Corporation International Journal of Rheumatology Volume 2012, Article ID 357071, 9 pages doi:10.1155/2012/357071 Review Article Are Classification Criteria for IgG4-RD Now Possible?
LIVER SPECIALTY CONFERENCE USCAP Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA
 LIVER SPECIALTY CONFERENCE USCAP 2016 Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA Nothing to disclose Case History 47-year-old male, long standing ileal
LIVER SPECIALTY CONFERENCE USCAP 2016 Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA Nothing to disclose Case History 47-year-old male, long standing ileal
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine
 Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
IgG4-Related Disease: Dataset of 235 Consecutive Patients
 IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
Title. CitationHepato-Gastroenterology, 61(135): Issue Date Doc URL. Type. File Information. IgG4-Related Sclerosing Cholangitis
 Title Difference from Bile Duct Cancer and Relationship be IgG4-Related Sclerosing Cholangitis Kuwatani, Masaki; Kawakami, Hiroshi; Zen, Yoh; Kawak Author(s) Sakamoto, Naoya CitationHepato-Gastroenterology,
Title Difference from Bile Duct Cancer and Relationship be IgG4-Related Sclerosing Cholangitis Kuwatani, Masaki; Kawakami, Hiroshi; Zen, Yoh; Kawak Author(s) Sakamoto, Naoya CitationHepato-Gastroenterology,
Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Immunoglobulin G4 (IgG4)-related disease, a systemic,
 IgG4-Related Disease of the Gastrointestinal Tract A 21st Century Chameleon Vikram Deshpande, MD Context. Immunoglobulin G4 (IgG4) related disease is a systemic fibroinflammatory disease capable of affecting
IgG4-Related Disease of the Gastrointestinal Tract A 21st Century Chameleon Vikram Deshpande, MD Context. Immunoglobulin G4 (IgG4) related disease is a systemic fibroinflammatory disease capable of affecting
Pediatric Primary Sclerosing Cholangitis and Potential Therapies
 Pediatric Primary Sclerosing Cholangitis and Potential Therapies Philip Rosenthal, M.D. Professor of Pediatrics & Surgery University of California, San Francisco DISCLOSURE I have the following financial
Pediatric Primary Sclerosing Cholangitis and Potential Therapies Philip Rosenthal, M.D. Professor of Pediatrics & Surgery University of California, San Francisco DISCLOSURE I have the following financial
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Personal Profile. Name: 劉 XX Gender: Female Age: 53-y/o Past history. Hepatitis B carrier
 Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
