The Thoracodorsal Artery Perforator Flap: Clinical Experience and Anatomic Study with Emphasis on Harvest Techniques
|
|
|
- Rosalind Fox
- 5 years ago
- Views:
Transcription
1 The Thoracodorsal Artery Perforator Flap: Clinical Experience and Anatomic Study with Emphasis on Harvest Techniques Aldo Benjamin Guerra, M.D., Stephen Eric Metzinger, M.D., Kiersten Maria Lund, M.D., Michelle Maria Cooper, M.D., Robert Johnson Allen, M.D., and Charles Louis Dupin, M.D. New Orleans, La. The thoracodorsal artery perforator flap is a relatively new flap that has yet to find its niche in reconstructive surgery. At the authors institution it has been used for limb salvage, head and neck reconstruction, and trunk reconstruction in cases related to trauma, burns, and malignancy. The authors have found the flap to be advantageous for cranial base reconstruction and for resurfacing the face and oral cavity. The flap has been used successfully for reconstruction of traumatic upper and lower extremity defects, and it can be used as a pedicled flap or as a free tissue transfer. The perforating branches of the thoracodorsal artery offer a robust blood supply to a skin soft-tissue paddle of 10 to 12 cm 25 cm, overlying the latissimus dorsi muscle. The average pedicle length is 20 cm (range, 16 to 23 cm), which allows for a safe anastomosis outside the zone of injury in traumatized extremities; the flap can be made sensate by neurorrhaphy with sensory branches of the intercostal nerves. Vascularized bone can be transferred with this flap by taking advantage of the inherent vascular anatomy of the subscapular artery. A total of 30 pedicled and free flap transfers were performed at the authors institution with an overall complication rate of 23 percent and an overall flap survival rate of 97 percent. Major complications, such as vascular thrombosis, return to the operating room, fistula formation, recurrence of tumor, and flap loss, occurred in 17 percent of the patients. Despite these drawbacks, the authors have found the thoracodorsal artery perforator flap to be a safe and extremely versatile flap that offers significant advantages in acute and delayed reconstruction cases. (Plast. Reconstr. Surg. 114: 32, 2004.) Initially described in 1995, 1 the thoracodorsal artery perforator flap is based on at least one perforating vessel from the thoracodorsal artery. 2 4 It was originally called the latissimus dorsi musculocutaneous flap without muscle, 1 and others refer to it as the thin latissimus dorsi perforator-based flap. 3,4 This nomenclature is confusing and incorrect. Because the flap derives its blood supply from the perforating vessels that originate from the lateral or medial branch of the thoracodorsal artery, its proper name is the thoracodorsal artery perforator flap. 5 The flap can be further classified as an indirect muscular perforator-type flap. 6,7 Like other perforator-based flaps, it can be raised with maximal preservation of donor-site structures. 1 4 Unlike perforator flaps from the buttocks and abdomen, 8,9 which are bulky, this flap provides a thin and pliable skin soft-tissue paddle, which can be used to resurface shallower defects. 3 Its pliability is advantageous, as it allows for greater manipulation and contouring in reconstruction of complex structures. An anatomic study of the thoracodorsal artery perforator flap focusing on bony and softtissue landmarks that aid the surgeon in dissection of this flap was performed. Our dissections focused on the topographical anatomy of the latissimus dorsi muscle, the anatomy of the main vascular tree, and the perforating vessels. The study spotlights the lateral branch of the thoracodorsal artery, which is known to have the largest and most reliable perforating vessels. The arc of rotation of the flap was also demonstrated. Our clinical experience with the thoracodorsal artery perforator flap in reconstruction of traumatic and postoncologic defects at the same institution is described. The location of From the Department of Surgery, Division of Plastic and Reconstructive Surgery, and the Department of Otolaryngology-Head and Neck Surgery, Louisiana State University Health Sciences Center. Received for publication June 11, 2002; revised August 15, DOI: /01.PRS C5 32
2 Vol. 114, No. 1 / THORACODORSAL ARTERY PERFORATOR FLAP 33 defects has been variable and includes the oral cavity, mandible, anterior and lateral cranial base, trunk, and upper and lower extremities. Our overall experience consists of 30 cases since ANATOMIC STUDY Methods and Materials Twenty cadavers were dissected for this anatomic study. A flap measuring 10 cm in width by 30 cm in length was diagrammed on each cadaver and was centered over a point 8 cm below the posterior axillary fold and 2 cm behind the anterior border of the latissimus dorsi muscle. It included skin that draped 2 cm anterior and 6 cm posterior to the anterior edge of the muscle. Based on previous anatomic studies, this flap would include perforators arising from the lateral branch of the thoracodorsal system. 1,5,10 A second reference point was chosen 2 cm behind the anterior border of the muscle and 4 cm below the tip of the scapula. According to Heitmann et al., 5 this is the location of the thoracodorsal hilus where the vessel bifurcates into the lateral and medial branches. Skin incisions were opened from the axilla to the posterior-lateral torso, leaving the flap undissected. The skin was elevated, thereby preserving the underlying latissimus dorsi muscle. This muscle is organized into large muscular bundles. It was noted that large perforating vessels would rise to the skin between and not through the muscle bundles. In the cadaver, the muscle bundles are thin and appear wasted compared with the live specimen, making it easier to separate them. At the distal end of the thoracodorsal artery perforator flap, we identified a cleavage plane between muscle bundles on the anterior-lateral portion of the latissimus dorsi muscle, where the lateral branch of the thoracodorsal artery was recognized. The inferior portion of the flap was elevated first, and then the flap was approached from medial and lateral directions. Dissection halted when a perforator was encountered. We observed perforating vessels capable of feeding the flap ascending from the lateral branch of the thoracodorsal artery in this muscle cleavage plane. All perforators greater than 0.5 mm ascended to the skin soft-tissue flap via separations between muscle bundles. Spreading the muscle apart allowed dissection below the main body of the latissimus dorsi muscle between two large muscle bellies. Dissection was continued into the axilla. Measurements of the perforators and arc of rotation were carried out. Results Seventeen of 20 cadavers (85 percent) were found to have at least one perforator from the lateral branch of the thoracodorsal artery, which supplied the skin soft-tissue paddle. The first perforator was always the largest from this vessel system, measuring between 0.5 and 0.6 mm in diameter, originating 2 to 4 cm distal to the bifurcation of the thoracodorsal artery, and measuring 4 to 6 cm in length. Twelve cadavers had a second perforator about 2 to 6 cm distal to the main perforating vessel. A third perforator was found in only 10 cadavers. All perforating vessels were found within 8 cm of the vascular hilus. The perforators were observed to penetrate the dorsal thoracic fascia and travel for a distance of 2 to 6 cm. The direction was quite variable. Importantly, the average distance from the axillary artery to the hilus was found to be 12 cm in length, making the average total length of the pedicle 20 cm. A line of cleavage where the perforator vessels ascend to the flap could be identified on all 20 latissimus dorsi muscles. Perforating vessels from the lateral branch were found on a line that begins 2 cm posterior to the anterior border of the latissimus dorsi muscle and travels along the muscle s anterior long axis. Identification of the cleavage plane that carries the neurovascular structures is facilitated by early identification of the thoracodorsal nerve in the distal portion of the latissimus dorsi muscle. The arc of rotation for the thoracodorsal artery perforator was defined (Fig. 1, above, left). The flap offers an arc of 90 degrees clockwise and counterclockwise. The flap was transposed onto the breast anterolateral and posterolateral chest wall (Fig. 1, above, right). This is not the extensive transposition seen with the musculocutaneous flap, because the radius of the thoracodorsal artery perforator arc is smaller. Rotation through 180 degrees clockwise to the head and neck was performed. The flap comfortably reaches the clavicle area (Fig. 1, below, left). Arc of rotation to the arm is accomplished with counterclockwise rotation 90 degrees (Fig. 1, below, right). In addition, the flap can be transposed easily to the axilla. With more extensive dissection, some flaps reached just beyond the elbow and the base of the neck. Further efforts to advance the flaps higher on
3 34 PLASTIC AND RECONSTRUCTIVE SURGERY, July 2004 FIG. 1.(Above, left) The arc of rotation for the thoracodorsal artery perforator flap. (Above, right) The thoracodorsal artery perforator flap offers an arc of 90 degrees clockwise and counterclockwise. The flap was transposed onto the breast anterolateral and posterolateral chest wall. This is not the extensive transposition seen with the musculocutaneous flap, because the radius of the thoracodorsal artery perforator arc is smaller. (Below, left) Rotation through 180 degrees clockwise to the head and neck was performed. The flap comfortably reaches the clavicle area. (Below, right) Arc of rotation to the arm is accomplished with counterclockwise rotation of 90 degrees. The flap covers the upper arm comfortably. the neck and distal elbow caused perforating vessels to tear. TABLE I Anatomy Studies of the Thoracodorsal Artery Perforating Vessels First Perforator Second Perforator Third Perforator Angrigiani et al. 1 40/40 40/40 32/40 Van Landuyt et al /30 NA NA Heitmann et al. 5 20/20 13/20 2/20 This study 17/20 12/20 10/20 NA, not applicable. Discussion The reliability of the thoracodorsal artery perforator flap will depend on the presence and size of the perforating vessels. Injection studies focussing on the vascular anatomy of these vessels have been performed by other groups (Table I). Angrigiani et al. 1 were able to find at least one perforating vessel capable of supplying the flap in their anatomic study of 40 cadavers. His group used fresh cadavers with intravascular injection of colored latex, highlighting small vascular structures. A European study using similar methods found a reliablesize perforator in 29 of 30 cadaver dissections. 10 More recently, Heitmann et al. 5 reported their findings using injectable latex in 20 fresh cadavers. This detailed study demonstrated the presence of two or more perforating vessels per latissimus dorsi muscle. In accordance with our study, all the cutaneous perforators were within 8 cm of the hilus. Both the medial and lateral branches were observed to have perforators greater than 0.5 mm, but the largest vessels originated from the lateral branch of the thoracodorsal artery. In the same study, the
4 Vol. 114, No. 1 / THORACODORSAL ARTERY PERFORATOR FLAP 35 lateral branch showed a 100 percent rate of adequate perforators and averaged 1.8 perforators per vessel examined. 5 The cumulative results of these studies show that cutaneous perforating vessels in close proximity to the hilus of the thoracodorsal artery are reliable in presence and size. For our study, we did not have the advantage of using fresh cadavers, and this could have led to the lower number of vessels identified in our dissections. Identification of the vascular structures was important, but our focus was on obtaining a greater understanding of the relationship between neurovascular pedicle and muscle topography as it relates to the harvesting of the flap. In addition, we wished to identify certain landmarks that may help with localization of the perforators and flap elevation. Furthermore, primary interest was placed on the lateral branch of the thoracodorsal artery. We identified 17 of 20 cadavers (85 percent) with at least one perforator from the lateral branch of the thoracodorsal artery capable of supplying the skin soft-tissue paddle. In accordance with other studies, the first perforator was always the largest and most consistent. Second and third perforators were identified but were smaller and their presence was less consistent. Our failure to find more than 85 percent of the perforators may have been derived from the lack of fresh cadavers or injectable materials for this study. Regardless, three other studies using more sophisticated methods have demonstrated the consistency of the perforator anatomy over the latissimus dorsi muscle. In addition, other investigators of the thoracodorsal artery perforator flap have considered the perforator distribution over the entire latissimus dorsi muscle, while we focused only on the lateral branch. According to Heitmann et al., 5 we would miss 44 percent of the perforators studying only the lateral branch of the thoracodorsal artery. The lateral branch has been the nutrient source for the thoracodorsal artery perforator flap we have used at our institution for the past 11 years, and it made sense to direct attention to this important vessel. We have not attempted to raise a medial branch perforator-based flap. The lateral branch was found descending along a line at approximately 2.5 cm behind the anterior border of the latissimus dorsi muscle edge. In order for this vessel to nourish the skin, it must send perforators through the muscle. We found these vessels traveling between muscle bundles and infrequently through the bundles. Spinelli et al. 11 described this row of perforating vessels located directly over the lateral branch of the thoracodorsal artery in six fresh cadavers. Kim et al. 12 observed similar anatomy. This line is not imaginary, but occurs as a cleft between muscle bundles that allows the underlying vessels to nourish the skin softtissue envelope. Moreover, the line appears white because the lateral thoracodorsal pedicle is accompanied by the thoracodorsal nerve, which was found in a superficial location relative to the vascular structures. We observed this line in all 20 cadavers (100 percent). The first effort to locate the perforators by using topographical landmarks was performed using the posterior axillary fold and the anterior border of the latissimus dorsi muscle. Angrigiani et al. 1 first used these landmarks in their original description of the thoracodorsal artery perforator flap. In addition, as pointed out by Heitmann et al., 5 identification of the hilus by using the anterior border of the latissimus dorsi muscle and the lowest point of the scapula is useful. Using this method placed us within 2 cm or less of the actual hilus location in most cases. Identification of the line of cleavage adds a third topographic point. Using all three landmarks, we were able to triangulate on the location of the perforators. On the cadaver, transposition of the flap to the anterior chest wall, axilla, arm, and supraclavicular area was accomplished safely, establishing the arc of rotation for this flap. CLINICAL SERIES Patients and Materials The medical records of 32 patients involved in this study were reviewed for demographic information, operative time, operative technique, blood loss, and complications. This group included all thoracodorsal artery perforator flaps performed over an 11-year period, from March of 1992 to March of Two patients had the procedure aborted for lack of adequate perforators. Complications were divided into early and late. Early complications included vessel thrombosis, return to the operating room, flap loss, early débridement, seromas, and wound infections. Late complications included delayed wound healing, fat necrosis, and unexpected revision surgery.
5 36 PLASTIC AND RECONSTRUCTIVE SURGERY, July 2004 Results Thirty thoracodorsal artery perforator flap procedures were performed over an 11-year period (Table II). Thirteen flaps were pedicled and 17 were free tissue transfers. Twenty-nine of 30 flaps survived. Major complications occurred in 17 percent of patients. One flap was lost to arterial thrombosis. One venous thrombosis occurred, but the flap was salvaged. This salvaged flap experienced fat necrosis. Fat necrosis was seen in one pedicled breast flap and in a free flap used to reconstruct a composite mandibular defect after a fistula developed requiring débridement. Both flaps survived. The same patient later developed recurrence of his primary tumor and subsequently died. Fewer complications were seen in the pedicled group. One donor-site wound-healing delay occurred and two donor scar revisions were performed. Only one flap was debulked with suctionassisted lipectomy at a second stage. Operative Technique The patient is marked in the sitting position. An area 2 cm behind the anterior border of the latissimus dorsi muscle and 4 cm inferior to the tip of the scapula is marked in an attempt to locate the hilus of the vessel. A point 8 cm below the posterior axillary fold and centered 2 cm behind the anterior edge of the latissimus dorsi muscle is mapped out with a hand-held Doppler (Koven, Inc., St. Louis, Mo.) device (Fig. 2). Surgery is performed with the patient in the lateral decubitus position under loupe magnification. The inferior portion of the flap is raised first. The neurovascular bundle is identified. Subsequently, the posterior-dorsal edge of the flap is elevated. We begin dissection above the dorsal thoracic fascia and descend below the fascia when we get within 2 cm of the perforating row of vessels. The surgeon enters a bloodless plane, which facilitates dissection toward the anterior edge. Visualization is maximized in this plane. Dissection should be done carefully as one approaches the meridian of the flap, which is reached by dissecting parallel to the direction of the muscle bundles. Dissection continues by peeling the perimysium off the muscle bundles until the perforator cleavage line is identified on the TABLE II Thoracodorsal Artery Perforator Flaps at LSUHSC Location Defect Etiology Outcome and Complications Pedicled TDAP flaps 1 Trunk Clavicle Gunshot blast Healed 2 Axilla Contracture Burn Healed 3 Axilla Contracture Burn Healed 4 Axilla Contracture Hydradenitis Healed 5 Axilla Hydradenitis Hydradenitis Skin graft donor site, revision 6 Axilla Hydradenitis Hydradenitis Healed 7 Breast Mastectomy Carcinoma Healed 8 Breast Mastectomy Carcinoma Fat necrosis 9 Breast Mastectomy Carcinoma Healed 10 Breast Mastectomy Carcinoma Healed 11 Breast Mastectomy Carcinoma Healed 12 Breast Mastectomy Carcinoma Healed 13 Breast Mastectomy Carcinoma Healed Free TDAP flaps 14 L. skull base Temporal Carcinoma Healed 15 L. skull base Temporal Carcinoma Healed 16 Orbital Exenteration Carcinoma Healed 17 Orbital Exenteration Carcinoma Healed 18 A. skull base Frontal MVA Healed 19 Maxilla Palate Carcinoma Healed 20 Maxilla Palate Carcinoma Fat necrosis 21 Mandible Multiple Carcinoma Fistula, partial flap necrosis, recurrent tumor 22 Elbow Dorsal MVA Healed 23 Forearm Volar Degloving Delayed site scar revision 25 Forearm Volar Degloving Healed 26 Leg Lateral Shotgun blast Arterial thrombosis, flap loss 27 Leg Medial Open tibia Venous thrombosis, flap salvage, fat necrosis 28 Leg Anterior Open tibia Healed 29 Leg Anterior Open tibia Healed 30 Foot Dorsal Degloving Healed LSUHSC, Louisiana State University Health Science Center; TDAP, thoracodorsal artery perforator; L., left; A., anterior; MVA, motor vehicle accident.
6 Vol. 114, No. 1 / THORACODORSAL ARTERY PERFORATOR FLAP 37 muscle. This line appears white due to the presence of the lateral thoracodorsal nerve and vascular bundle. The perforating vessels will be found along this line as the dissection proceeds proximally. Once a perforator vessel is visualized and found to be adequate, the anterior-lateral edge of the flap can then be elevated in a similar fashion toward the meridian. Dissection proceeds until all the perforators are identified. The space between two large muscle bundles where the perforator vessels ascend toward the skin flap can be further dissected until the underlying structures are identified. The thoracodorsal nerve can be separated from the vessels so that it can be preserved. The distal end of the thoracodorsal vessels, close to the origin of the muscle, is ligated and dissected toward the axilla. The most delicate part of the operation occurs when the perforators are separated from the muscle as dissection descends toward the main pedicle. Care is used in order not to damage the delicate venae comitantes that accompany the perforating artery. Once the perforator is released, retractors are placed on the proximal latissimus dorsi muscle to continue dissection into and eventually under the muscle. Dissection can usually proceed more rapidly at this point and includes ligation of the major branches of the thoracodorsal and subscapular vessels until one reaches the axillary artery and vein. Case 1 CASE REPORTS A 28-year-old man presented to our clinic 2 years after undergoing excision of hidradenitis suppurativa and skin grafting at the axilla. He developed a scar contracture that had been present for 13 months. He was unable to abduct the arm more than 85 degrees (Fig. 3, left). A thoracodorsal artery perforator flap was pedicled into the axillary defect after scar release, with restoration of joint motion (Fig. 3, right). The donor site required skin grafting for closure. Secondary scar revision was carried out 8 months later. FIG. 2. The patient is marked in the sitting position. An area 2 cm behind the anterior border of the latissimus dorsi muscle and 4 cm inferior to the tip of the scapula is marked in an attempt to locate the hilus of the vessel. A point 8 cm below the posterior axillary fold and centered 2 cm behind the anterior edge of the latissimus dorsi muscle is mapped out with a hand-held Doppler device. Case 2 A 39-year-old man was transferred to our service after several attempts at closure of an anterior skull defect over a period of 18 months. Earlier he had sustained a crush injury to the frontal sinus and anterior skull complicated by a subdural hematoma and skull flap infection. On presentation, dural exposure was noted along with persistent deep bone infection (Fig. 4, above). The pedicle measured 23 cm, allowing an easier anastomosis (Fig. 4, center). Fourteen months after surgery, the patient had no evidence of recurrent infection and was fully healed (Fig. 4, below). DISCUSSION Perforator-based flaps have allowed surgeons to provide vascularized tissue transfers while minimizing donor-site morbidity. 13,14 The thoracodorsal artery perforator flap allows for preservation of the muscle unit and is advantageous for several reasons (Table III). Dissection through the muscle results in a much longer pedicle (Fig. 4, center). In traumatized extremities, the long pedicle is advantageous, allowing for safe anastomosis outside the zone of injury. A flow-through vascular anastomosis is an option with this flap. 4 A lengthy pedicle is of great advantage in head and neck reconstruction, as it allows for anastomosis to any vessel in the neck without vein grafts. Postoperative magnetic resonance imaging facilitates cranial base oncologic follow-up, with T1- weighted images demonstrating a distinct plane between fat and any potential tumor recurrence (Fig. 5). The sparing of innervated muscle minimizes functional loss in those who require trunk stabilization or muscle use in the early postoperative period. Thoracodorsal nerves were routinely spared in this series (Fig. 6). This maintains the contour of the back unaltered.
7 38 PLASTIC AND RECONSTRUCTIVE SURGERY, July 2004 FIG. 3.(Left) A 28-year-old man with scar contracture of the axilla after failed reconstruction for hidradenitis suppurativa. (Right) At 3 months after surgery the patient had regained full use of the joint. Muscle origins are left undisturbed, producing less pain and no dead space. Seroma formation, a frequent complication of the latissimus dorsi muscle flap, 15,16 was avoided in our series (Table III). Bulky muscle flaps frequently have to be thinned out at a second stage, whereas the thoracodorsal artery perforator is a thin flap that is good for resurfacing and can achieve reconstruction of shallow defects in a more elegant manner. 3 We debulked only one flap at a second stage. The thoracodorsal artery perforator flap has a reliable blood supply and can be made as large as cm. 1,4,5,10 If one requires a flap larger than this, a different donor site should be used. The thoracodorsal artery perforator s arc of rotation allows for coverage of wounds on the anterior chest wall, clavicle, axilla, and proximal arm. A small radius on the arc of rotation limits the reach of the flap, although the arc itself is comparable to that of the latissimus dorsi musculocutaneous flap. 17 Care should be taken not to exceed the reach of the flap, as this may lead to rupture of the delicate perforating vessels and the flap failure that other groups have experienced. 18 Thicker flaps in obese patients provide excellent tissue bulk for breast reconstruction. 19 Surgeons are already familiar with the vasculature that nourishes the latissimus dorsi muscle. Large vessel diameter is an advantage in microsurgery (Table III). Multiple flaps have been raised from the subscapular system, including bone, muscle, musculocutaneous, and osteocutaneous flaps. This makes the subscapular territory one of the most versatile in plastic surgery. 20 The thoracodorsal artery perforator flap is an extension of this vascular pedicle that minimizes donor-site morbidity and can be safely combined with the above-mentioned tissues to create a variety of composite flaps. Disadvantages with this flap have been encountered (Table IV). Patient positioning and dissection of the perforator can increase operative time. The learning curve for this flap is steep. Careful planning and patient markings are required in order not to place the flap outside the realm of adequate perforators, and this takes experience and skill. Early in our series using Angrigiani et al. s 1 marking method, we failed to find vessels adequate to carry the flap for two cases. Marking the patient while sitting and operating in the decubitus position, with the arm elevated, shifts the location and direction of the perforators, an experience that other groups have shared. 18 In the first case, presurgical markings were made too low to include the major perforating vessel from the lateral branch of the thoracodorsal artery. In the second case, two small perforators were identified during the dissection of the flap. These were judged to be inadequate
8 Vol. 114, No. 1 / THORACODORSAL ARTERY PERFORATOR FLAP 39 TABLE III Advantages of the Thoracodorsal Artery Perforator Flap Aesthetic Musculature Vasculature Anastomosis Follow-up Pedicle Sensation Seroma Improved aesthetic appearance with intact muscle Preservation of function aids with rehabilitation Possibility of flow-through anastomosis Reliable, wide diameter subscapular artery and vein T1-weighted magnetic resonance images facilitate postoncologic follow-up Average 20-cm pedicle (range, cm); anastomosis out of zone of injury or radiation damage increases safety and patency Neurorrhaphy for sensation with intercostal nerves No dead space; incidence of seroma is zero FIG. 5. Postoperative magnetic resonance imaging facilitates cranial base oncologic follow-up, with T1-weighted images demonstrating a distinct plane between fat and any potential tumor recurrence. FIG. 4.(Above) A 39-year-old man with exposed dura and deep bone infection of the frontal skull after multiple attempts at closure of the anterior skull defect over a period of 18 months. (Center) The pedicle length of 23 cm is highly advantageous in head and neck and extremity reconstruction. (Below) Fourteen months after surgery, the patient is without evidence of recurrent infection and is fully healed. for flap transfer. Since then, we have noted that these perforators experience prolonged vasospasm as they are dissected. Patience is needed to allow the vasospasm to resolve. In retrospect, these perforators would likely have performed well. These events early in our experience were critical steps in the learning curve of this procedure. However, if the surgeon encounters similar situations, he or she should keep in mind the multiple flaps that can be based on the subscapular artery, such as the scapular, parascapular, latissimus dorsi, and serratus anterior muscle flaps, to salvage the reconstruction. Our anatomic study was completed in an effort to overcome these challenges. The addition of a second topographic reference point has helped tremendously. This reference point suggests the location of the thoracodorsal hi-
9 40 PLASTIC AND RECONSTRUCTIVE SURGERY, July 2004 FIG. 6. The preservation of the thoracodorsal nerve is straightforward and can be accomplished while minimizing functional loss. All 27 thoracodorsal nerves were spared in this series. TABLE IV Disadvantages of the Thoracodorsal Artery Perforator Flap Size Perforators Experience Positioning Timing Neurorrhaphy Limited to cm cm Variability of perforators Steep learning curve Requires lateral decubitus position for harvest Because of positioning requirements may not be able to have two teams working at the same time Interposition nerve grafts frequently required lus, a key landmark, as the first perforating vessel will be 2 to 4 cm from this location and all perforators are within an 8-cm radius of this point. 5 In addition, by elevating the inferior portion of the flap early and identifying the line of cleavage in the muscle, the surgeon is able to use a third topographic landmark and thus can triangulate the location of the perforators with reliability. Since the addition of multiple topographic landmarks, we have had a 100 percent success rate in harvesting the thoracodorsal artery perforator flap. Other groups have identified preoperative Doppler studies as being helpful in planning this flap. 3,18 We do not believe preoperative Doppler ultrasound modalities to be helpful. Blondeel et al. 21 found the sensitivity and positive predictive value of unidirectional Doppler flowmetry too low to be of any value in planning the thoracodorsal artery perforator flap. This is due to the basic anatomy of the flap. 1,5,10 After the perforators penetrate the muscle, they will likely travel on top of the fascia for 2 to 6 cm, but the actual distance and direction are extremely variable. 10 Schwabegger et al. 18 stated that relying solely on ultrasound images of the vessels can lead to failure when planning for these flaps. Visual confirmation of the perforators before finalizing the skin incisions is mandatory. However, use of topographic landmarks with identification of the line of cleavage in the muscle will help pinpoint where the perforating vessels are arising out of the muscle with accuracy, making expensive ultrasound studies obsolete. Alternative donor sites, such as the anterolateral thigh flap and radial forearm, can provide tissue with similar characteristics that can be harvested in the supine position. 22 These flaps have proven to be reliable and can be easier to dissect than the thoracodorsal artery perforator flap. 22 However, both of these flaps suffer from having donor sites in areas of high visibility. 23 In addition, tendon exposure can be problematic with the radial forearm flap donor site. Donor-site problems with the thoracodorsal artery perforator flap can occur. Tight closure can be problematic with wide flaps. 18 There is more tension on the skin at closure because the latissimus dorsi muscle remains in place. This led to delayed healing in one of our patients. Widening scars led to revision surgery in a second patient. However, the donor site remains well hidden in the posterior axillary fold. CONCLUSIONS The thoracodorsal artery perforator flap is not a well-known flap. Recent publications have outlined the anatomy and experience with this flap, but these accounts are limited in number. Over the past 11 years, we have obtained a relatively large amount of experience using this flap as a free or pedicled transfer. We have found the vascular anatomy of the perforator vessels to be dependable. The reliability of the thoracodorsal artery perforator flap may have been tainted by the inconstant presence of a direct cutaneous branch arising from the thoracodorsal artery and traveling anterior to the muscle edge. 24,25 This vessel is the basis for the thoracodorsal axillary flap described by Cabanie et al., 24 but it is not a perforator because it does not travel through the latissimus dorsi muscle. The thoracodorsal artery perforator flap receives its blood supply from indirect muscular perforators, has an arc of rotation similar to that of the latissimus dorsi musculo-
10 Vol. 114, No. 1 / THORACODORSAL ARTERY PERFORATOR FLAP 41 cutaneous flap, and has proven to be very versatile with a relatively low rate of complications. Aldo Benjamin Guerra, M.D. Department of Surgery Division of Plastic and Reconstructive Surgery Louisiana State University Health Sciences Cent 1542 Tulane Avenue, Room 701 New Orleans, La REFERENCES 1. Angrigiani, C., Grilli, D., and Siebert, J. W. Latissimus dorsi musculocutaneous flap without muscle. Plast. Reconstr. Surg. 96: 1608, Khoobehi, K., Allen, R. J., and Montegut, W. J. Thoracodorsal artery perforator flap for reconstruction (Abstract). South. Med. J. 89 (Suppl.): S110, Kim, J. T., Koo, B. S., and Kim, S. K. The thin latissimus dorsi perforator-based free flap for resurfacing. Plast. Reconstr. Surg. 107: 374, Koshima, I., Saisho, H., Kawada, S., Hamanaka, T., Umeda, N., and Moriguchi, T. Flow-through thin latissimus dorsi perforator flap for repair of soft-tissue defects in the legs. Plast. Reconstr. Surg. 103: 1483, Heitmann, C., Guerra, A., Metzinger, S. W., Levin, S. L., and Allen, R. J. The thoracodorsal artery perforator flap: Anatomical basis and clinical application. Ann. Plast. Surg. 51: 23, Hallock, G. G. Direct and indirect perforator flaps: The history and the controversy. Plast. Reconstr. Surg. 111: 855, Wei, F. C., Jain, V., Suominem, S., and Chen, H. C. Confusion among perforator flaps: What is a true perforator flap? Plast. Reconstr. Surg. 107: 874, Allen, R. J., and Treece, P. Deep inferior epigastric perforator flap for breast reconstruction. Ann. Plast. Surg. 32: 32, Allen, R., and Tucker, C., Jr. Superior gluteal artery perforator free flap for breast reconstruction. Plast. Reconstr. Surg. 95: 1207, Van Landuyt, K. Experience with the thoracodorsal artery perforator (TAP) flap. Presented at the Second International Course on Perforator Flaps, New Orleans, La., November 5-7, Spinelli, H. M., Fink, J. A., and Muzaffar, A. R. The latissimus dorsi perforator-based fasciocutaneous flap. Ann. Plast. Surg. 37: 500, Kim, D. Y., Cho, S. Y., Kim, K. S. Lee, S. Y., and Cho, B. H. Correction of axillary burn scar contracture with the thoracodorsal perforator-based cutaneous island flap. Ann. Plast. Surg. 44: 181, Blondeel, P. N., Vanderstraeten, G. G., Monstrey, S. J., et al. The donor site morbidity of free DIEP flaps and free TRAM flaps for breast reconstruction. Br. J. Plast. Surg. 53: 322, Kroll, S. S., Sharma, S., Koutz, C., et al. Postoperative morphine requirement of free TRAM and DIEP flaps. Plast. Reconstr. Surg. 107: 338, Schwabegger, A., Ninkovic, M., Brenner, F., and Anderl, H. Seroma as a common donor site morbidity after harvesting the latissimus dorsi flap: Observations on cause and prevention. Ann. Plast. Surg. 38: 594, Titley, O. G., Spyrou, G. E., and Fatah, M. F. Preventing seroma in the latissimus dorsi flap donor site. Br. J. Plast. Surg. 50: 106, Dinner, M. I., and Peters, C. R. The arc of rotation of the latissimus dorsi myocutaneous flap. Ann. Plast. Surg. 3: 425, Schwabegger, A. H., Bodner, G., Ninkovic, M., and Piza- Katzer, H. Thoracodorsal artery perforator (TAP) flap: Report of our experience and review of the literature. Br. J. Plast. Surg. 55: 390, Allen, R. J. Perforator flaps in breast reconstruction. In S. L. Spear, J. W. Little, M. E. Lippman, and W. C. Woods (Eds.), Surgery of the Breast: Principles and Art. Philadelphia: Lippincott-Raven, Germann, G., Bickert, B., Steinau, H. U., Wagner, H., and Sauerbier, M. Versatility and reliability of combined flaps of the subscapular system. Plast. Reconstr. Surg. 103: 1386, Blondeel, P. N., Beyens, G., Verhaeghe, R., et al. Doppler flowmetry in the planning of perforator flaps. Br. J. Plast. Surg. 51: 202, Wei, F. C., Jain, V., Celik, N., Chen, H. C., Chuang, D. C., and Lin, C. H. Have we found the ideal soft-tissue flap? An experience with 672 anterolateral thigh flaps. Plast. Reconstr. Surg. 111: 2481, Kimata, Y., Uchiyama, K., Ebihara, S., et al. Anterolateral thigh flap donor-site complications and morbidity. Plast. Reconstr. Surg. 106: 584, Cabanie, H., Garbe, J., and Guimberteau, J. C. Anatomical bases of the thoracodorsal axillary flap with respect to its transfer by means of microvascular surgery. Anat. Clin. 2: 65, Rowsell, A. R., Eisenberg, D. N., and Taylor, G. I. The anatomy of the subscapular-thoracodorsal arterial system: A study of 100 cadaver dissections. Br. J. Plast. Surg. 37: 574, 1984.
The free thoracodorsal artery perforator flap in head and neck reconstruction
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Scapular & Parascapular flap FLAP TERRITORY ANATOMY. is normally accompanied by two venae comitantes.
 Scapular & Parascapular flap FLAP TERRITORY This is a composite flap that is situated over the scapula with various incisional arrangements. It can be harvested as a skin and subcutaneous tissue flap,
Scapular & Parascapular flap FLAP TERRITORY This is a composite flap that is situated over the scapula with various incisional arrangements. It can be harvested as a skin and subcutaneous tissue flap,
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects
 Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study
 Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
The lumbar artery perforator based island flap: anatomical study and case reports
 British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION. Adequate speech and swallowing are dependent
 ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
ORIGINAL ARTICLE MEDIAL SURAL ARTERY PERFORATOR FLAP FOR TONGUE AND FLOOR OF MOUTH RECONSTRUCTION Shao-Liang Chen, MD, 1 Tim-Mo Chen, MD, 1 Niann-Tzyy Dai, MD, 1 Yi-Jan Hsia, DDS, MDSC, 2 Yaoh-Shiang Lin,
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints
 Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
Gastrocnemius Muscle Flap Coverage of Chronically= Infected Knee Joints ABSTRACT Chronically infected open knee joints present dif cult problem. Aggressive debridement of chronically infected soft tissue
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction
 A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
INTRODUCTION. Jong Gyu Kim, Soo Hyang Lee. Original Article
 Comparison of the Multidetector-row Computed Tomographic ngiography xial and Coronal Planes Usefulness for Detecting Thoracodorsal rtery Perforators Original rticle Jong Gyu Kim, Soo Hyang Lee Department
Comparison of the Multidetector-row Computed Tomographic ngiography xial and Coronal Planes Usefulness for Detecting Thoracodorsal rtery Perforators Original rticle Jong Gyu Kim, Soo Hyang Lee Department
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
COMBINED ABDOMINAL FLAP FOR MAJOR HAND RECONSTRUCTION
 Int. J. Pharm. Med. & Bio. Sc. 2013 2014 Srinivas Somashekar et al., 2014 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 3, No. 1, January 2014 2014 IJPMBS. All Rights Reserved COMBINED ABDOMINAL FLAP
Int. J. Pharm. Med. & Bio. Sc. 2013 2014 Srinivas Somashekar et al., 2014 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 3, No. 1, January 2014 2014 IJPMBS. All Rights Reserved COMBINED ABDOMINAL FLAP
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
The progress in microsurgical procedures has led
 Original Article Breast reconstruction with free anterolateral thigh flap Ranjit Raje, Ramesh Chepauk, Kanti Shetty, Rajendra Prasad J. S. Plastic & Reconstructive Services, Department of Surgical Oncology,
Original Article Breast reconstruction with free anterolateral thigh flap Ranjit Raje, Ramesh Chepauk, Kanti Shetty, Rajendra Prasad J. S. Plastic & Reconstructive Services, Department of Surgical Oncology,
The most common type of breast reconstruction
 BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
A review of the advantages of the anterolateral thigh flap in head and neck reconstruction
 The British Association of Plastic Surgeons (2004) 57, 603 609 A review of the advantages of the anterolateral thigh flap in head and neck reconstruction Jagdeep S. Chana, Fu-chan Wei* Department of Plastic
The British Association of Plastic Surgeons (2004) 57, 603 609 A review of the advantages of the anterolateral thigh flap in head and neck reconstruction Jagdeep S. Chana, Fu-chan Wei* Department of Plastic
Tor Chiu. Deep Inferior Epigastric Artery Perforator Flap 161
 18 Deep Inferior Epigastric Artery Perforator Flap Tor Chiu Deep Inferior Epigastric Artery Perforator Flap 161 Deep Inferior Epigastric Artery Perforator Flap FLAP TERRITORY The deep inferior epigastric
18 Deep Inferior Epigastric Artery Perforator Flap Tor Chiu Deep Inferior Epigastric Artery Perforator Flap 161 Deep Inferior Epigastric Artery Perforator Flap FLAP TERRITORY The deep inferior epigastric
JMSCR Vol 07 Issue 01 Page January 2019
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.36 Original Article A Study on the
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.36 Original Article A Study on the
MUSCLES. Anconeus Muscle
 LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
The gluteal perforator-based flap in repair of pressure sores
 The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Septic Bone and Joint Surgery
 Septic Bone and Joint Surgery Bearbeitet von Reinhard Schnettler 1. Auflage 2010. Buch. 328 S. Hardcover ISBN 978 3 13 149031 5 Format (B x L): 19,5 x 27 cm Weitere Fachgebiete > Medizin > Chirurgie >
Septic Bone and Joint Surgery Bearbeitet von Reinhard Schnettler 1. Auflage 2010. Buch. 328 S. Hardcover ISBN 978 3 13 149031 5 Format (B x L): 19,5 x 27 cm Weitere Fachgebiete > Medizin > Chirurgie >
ORIGINAL ARTICLE. The Thoracoacromial/Cephalic Vascular System for Microvascular Anastomoses in the Vessel-Depleted Neck
 ORIGINAL ARTICLE The Thoracoacromial/Cephalic Vascular System for Microvascular Anastomoses in the Vessel-Depleted Neck Jeffrey R. Harris, MD; E. Lueg, MD; E. Genden, MD; M. L. Urken, MD Objective: To
ORIGINAL ARTICLE The Thoracoacromial/Cephalic Vascular System for Microvascular Anastomoses in the Vessel-Depleted Neck Jeffrey R. Harris, MD; E. Lueg, MD; E. Genden, MD; M. L. Urken, MD Objective: To
Anatomical relationship between arteries and veins in the paraumbilical region q
 The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps
 CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
Primary closure of the deltopectoral flap-donor site without skin grafting
 Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction
 Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction Fu-chan Wei, M.D., Sinikka Suominen, M.D., Ph.D., Ming-huei Cheng, M.D., Naci Celik, M.D., and Yung-lung Lai, M.D. Taipei, Taiwan Most
Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction Fu-chan Wei, M.D., Sinikka Suominen, M.D., Ph.D., Ming-huei Cheng, M.D., Naci Celik, M.D., and Yung-lung Lai, M.D. Taipei, Taiwan Most
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap
 Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
Medical Journal of the Volume 20 Islamic Republic of Iran Number 3 Fall 1385 November Original Articles
 Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Sensate First Dorsal Metacarpal Artery Flap for Resurfacing Extensive Pulp Defects of the Thumb
 ORIGINAL ARTICLE Sensate First Dorsal Metacarpal Artery Flap for Resurfacing Extensive Pulp Defects of the Thumb Shun-Cheng Chang, MD, Shao-Liang Chen, MD, Tim-Mo Chen, MD, Chia-Jueng Chuang, MD, Tian-Yeu
ORIGINAL ARTICLE Sensate First Dorsal Metacarpal Artery Flap for Resurfacing Extensive Pulp Defects of the Thumb Shun-Cheng Chang, MD, Shao-Liang Chen, MD, Tim-Mo Chen, MD, Chia-Jueng Chuang, MD, Tian-Yeu
Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps
 BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
Pedicled medial sural perforator flap for the reconstruction of knee defects
 International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Pedicled medial sural perforator flap for the reconstruction of knee defects I-Han Chiang 1, Chia-Chun Wu 2, Shyi-Gen Chen 1 & Chih-Hsin Wang
International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Pedicled medial sural perforator flap for the reconstruction of knee defects I-Han Chiang 1, Chia-Chun Wu 2, Shyi-Gen Chen 1 & Chih-Hsin Wang
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
VENOUS DRAINAGE O US F UPPER UPPER LIM B BY dr.fahad Ullah
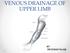 VENOUS DRAINAGE OF UPPER LIMB BY dr.fahad Ullah Venous drainage of the supper limb The venous system of the upper limb drains deoxygenated blood from the arm, forearm and hand It can anatomically be divided
VENOUS DRAINAGE OF UPPER LIMB BY dr.fahad Ullah Venous drainage of the supper limb The venous system of the upper limb drains deoxygenated blood from the arm, forearm and hand It can anatomically be divided
Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps
 e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
Progressive Tension Sutures to Prevent Seroma Formation after Latissimus Dorsi Harvest
 Progressive Tension Sutures to Prevent Seroma Formation after Latissimus Dorsi Harvest Jose L. Rios, M.D., Todd Pollock, M.D., and William P. Adams, Jr., M.D. Dallas, Texas The latissimus dorsi muscle
Progressive Tension Sutures to Prevent Seroma Formation after Latissimus Dorsi Harvest Jose L. Rios, M.D., Todd Pollock, M.D., and William P. Adams, Jr., M.D. Dallas, Texas The latissimus dorsi muscle
Flaps vs Grafts. Ronen Avram, MD MSc FRCSC
 Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Management of Brachial Plexus & Peripheral Nerves Blast Injuries. First Global Conflict Medicine Congress
 Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
ORIGINAL ARTICLE DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS
 DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
DISTALLY BASED PERONEUS BREVIS MUSCLE FLAP FOR DISTAL LEG DEFECTS Peddi Manjunath 1, Ramesha K.T 2, Smitha S Segu 3, Jainath 4, Shankarappa M 5 HOW TO CITE THIS ARTICLE: Peddi Manjunath, Ramesha KT, Smitha
The fibula osteoseptocutaneous flap with a RECONSTRUCTIVE
 RECONSTRUCTIVE Use of the Soleus Musculocutaneous Perforator for Skin Paddle Salvage of the Fibula Osteoseptocutaneous Flap: Anatomical Study and Clinical Confirmation Chin-Ho Wong, M.R.C.S. Bien-Keem
RECONSTRUCTIVE Use of the Soleus Musculocutaneous Perforator for Skin Paddle Salvage of the Fibula Osteoseptocutaneous Flap: Anatomical Study and Clinical Confirmation Chin-Ho Wong, M.R.C.S. Bien-Keem
ABSTRACT. Key words: Flaps, Adipofascial, Lower limb reconstruction. Khaldoun J. Haddadin, MD*, Samer Y. Haddad, MD. Introduction.
 DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
DISTALLY BASED ADIPOFASCIAL FLAPS: A VERSATILE FLAP FOR THE RECONSTRUCTION OF LOWER LEG AND PROXIMAL FOOT DEFECTS AT THE ROYAL JORDANIAN REHABILITATION CENTER Khaldoun J. Haddadin, MD*, Samer Y. Haddad,
Cour. 5 th - 7 th April 2018 RECONSTRUCTION COURSE ON CADAVER. Theoretical introduction to the basic concepts of microsurgery
 RECONSTRUCTION COURSE ON CADAVER Theoretical introduction to the basic concepts of microsurgery 5 th - 7 th April 2018 сh Cadavр F p s c Cour Head and neck: Submental flap Supraclavicular flap Free Helix
RECONSTRUCTION COURSE ON CADAVER Theoretical introduction to the basic concepts of microsurgery 5 th - 7 th April 2018 сh Cadavр F p s c Cour Head and neck: Submental flap Supraclavicular flap Free Helix
Few would deny that lower abdominal tissue BREAST. An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction.
 BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
The distally-based island ulnar artery perforator flap for wrist defects
 Free full text on www.ijps.org Original Article The distally-based island ulnar artery perforator flap for wrist defects Durga Karki, A. K. Singh Post Graduate Department of Plastic and Reconstructive
Free full text on www.ijps.org Original Article The distally-based island ulnar artery perforator flap for wrist defects Durga Karki, A. K. Singh Post Graduate Department of Plastic and Reconstructive
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
The anterolateral thigh perforator flap is RECONSTRUCTIVE
 RECONSTRUCTIVE The Extended Approach to the Vascular Pedicle of the Anterolateral Thigh Perforator Flap: Anatomical and Clinical Study Petros K. Spyriounis, M.D., Ph.D. Athens, Greece Background: The anterolateral
RECONSTRUCTIVE The Extended Approach to the Vascular Pedicle of the Anterolateral Thigh Perforator Flap: Anatomical and Clinical Study Petros K. Spyriounis, M.D., Ph.D. Athens, Greece Background: The anterolateral
Soft tissue reconstruction with the superior gluteal artery perforator f lap
 Clin Plastic Surg 30 (2003) 371 382 Soft tissue reconstruction with the superior gluteal artery perforator f lap Phillip N. Blondeel, MD, PhD*, Koenraad Van Landuyt, MD, Moustapha Hamdi, MD, Stan J. Monstrey,
Clin Plastic Surg 30 (2003) 371 382 Soft tissue reconstruction with the superior gluteal artery perforator f lap Phillip N. Blondeel, MD, PhD*, Koenraad Van Landuyt, MD, Moustapha Hamdi, MD, Stan J. Monstrey,
Kuwabara, Kaoru; Nonaka, Takashi; H. Citation Journal of Clinical Urology, 7(5),
 NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
The gastrocnemius with soleus bi-muscle flap
 The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications
 Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report
 Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION
 CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery
 Original Article Page 1 of 8 Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery Yuanbo Liu, Mengqing Zang, Shan Zhu, Bo Chen, Shanshan Li, Bingjian
Original Article Page 1 of 8 Distally based anterolateral thigh flap pedicled on the oblique branch of the lateral circumflex femoral artery Yuanbo Liu, Mengqing Zang, Shan Zhu, Bo Chen, Shanshan Li, Bingjian
Role of Latissimus Dorsi Island Flap in Coverage of Mutilating Upper Limb Injuries in Pediatric Age Group
 Original Article Annals of Pediatric Surgery Vol. 6, No 3,4 July, October 2010, PP 154-160 Role of Latissimus Dorsi Island Flap in Coverage of Mutilating Upper Limb Injuries in Pediatric Age Group Ahmed
Original Article Annals of Pediatric Surgery Vol. 6, No 3,4 July, October 2010, PP 154-160 Role of Latissimus Dorsi Island Flap in Coverage of Mutilating Upper Limb Injuries in Pediatric Age Group Ahmed
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps
 Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps Pierre M. Chevray, M.D., Ph.D. 1 ABSTRACT Breast reconstruction using autologous tissue is commonly accomplished using the transverse
Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps Pierre M. Chevray, M.D., Ph.D. 1 ABSTRACT Breast reconstruction using autologous tissue is commonly accomplished using the transverse
Key Relationships in the Upper Limb
 Key Relationships in the Upper Limb This list contains some of the key relationships that will help you identify structures in the lab. They are organized by dissection assignment as defined in the syllabus.
Key Relationships in the Upper Limb This list contains some of the key relationships that will help you identify structures in the lab. They are organized by dissection assignment as defined in the syllabus.
Surgical Anatomy of the Medial Sural Artery Perforator Flap
 555 Surgical Anatomy of the Medial Sural Artery Perforator Flap Man-Zhi Wong, M.B.B.S., M.R.C.S., M.Med. 1 Chin-Ho Wong, M.B.B.S., M.R.C.S., M.Med., F.A.M.S. 2 Bien-Keem Tan, M.B.B.S., F.R.C.S., F.A.M.S.
555 Surgical Anatomy of the Medial Sural Artery Perforator Flap Man-Zhi Wong, M.B.B.S., M.R.C.S., M.Med. 1 Chin-Ho Wong, M.B.B.S., M.R.C.S., M.Med., F.A.M.S. 2 Bien-Keem Tan, M.B.B.S., F.R.C.S., F.A.M.S.
Samer Saour, Guido Libondi, Venkat Ramakrishnan. Introduction
 Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity
 Original Article Page 1 of 7 A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity Limin Qing, Panfeng Wu, Zhouzheng Bing, Fang Yu,
Original Article Page 1 of 7 A new operative technique for dissecting perforator vessel in perforator flap: a better way to minimize donor-site morbidity Limin Qing, Panfeng Wu, Zhouzheng Bing, Fang Yu,
T. Rapis, S.N. Zanakis, I.F. Letsa, A.P. Karamanos CLINICAL CASE. Summary. Introduction
 Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Day 5 Respiratory & Cardiovascular: Respiratory System
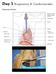 Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
Microvascular Free Flaps: Experience in Kwong Wah Hospital
 VOL. VOL.NO. NO. MAYNOVEMBER Microvascular Free Flaps: Experience in Kwong Wah Hospital Dr. Chiu-ming Ho, Dr. Vana SH Chan, Dr. Ming-shiaw Cheng, Dr. Wing-yung Cheung Division of Plastic Surgery, Department
VOL. VOL.NO. NO. MAYNOVEMBER Microvascular Free Flaps: Experience in Kwong Wah Hospital Dr. Chiu-ming Ho, Dr. Vana SH Chan, Dr. Ming-shiaw Cheng, Dr. Wing-yung Cheung Division of Plastic Surgery, Department
Disclosures. The Expanding Role of Microvascular Reconstruction. Overview. Things they are a Changing. Surgical Advisory Board, Genentech Corp
 Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
The arm: *For images refer back to the slides
 The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta.
 Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta. Fig-3: Showing high formation of Median nerve. Fig-1: Showing atypical formation of cords of Brachial plexus. 1 = Upper
Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta. Fig-3: Showing high formation of Median nerve. Fig-1: Showing atypical formation of cords of Brachial plexus. 1 = Upper
Microvascular reconstruction of traumatic defects requires
 The Journal of TRAUMA Injury, Infection, and Critical Care The Utility of the Anterolateral Thigh Donor Site in Reconstructing the United States Trauma Patient Eduardo D. Rodriguez, DDS, MD, Gedge D. Rosson,
The Journal of TRAUMA Injury, Infection, and Critical Care The Utility of the Anterolateral Thigh Donor Site in Reconstructing the United States Trauma Patient Eduardo D. Rodriguez, DDS, MD, Gedge D. Rosson,
Reconstruction of an extensive scalp defect using the split latissimus dorsi flap in combination with the serratus anterior musculo-osseous flap
 British Journal of Plastic Surgery (1998), 51,250-254 1998 The British Association of Plastic Surgeons BRITISH JOURNAL OF PLASTIC SURGERY Reconstruction of an extensive scalp defect using the split latissimus
British Journal of Plastic Surgery (1998), 51,250-254 1998 The British Association of Plastic Surgeons BRITISH JOURNAL OF PLASTIC SURGERY Reconstruction of an extensive scalp defect using the split latissimus
Breast Restoration Surgery After a mastectomy
 UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography
 BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function
 Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Forelimb Amputation. Indications. Pre operatively 11/12/2008. Technique Preparing for surgery. Bone neoplasia. Severe trauma/paralysis
 Forelimb Amputation January 10, 2007 Amy Bringardner Becky Pentecost Indications Bone neoplasia Osteosarcoma Fibrosarcoma Chondrosarcoma Severe trauma/paralysis Brachial plexus avulsion Infection Congenital
Forelimb Amputation January 10, 2007 Amy Bringardner Becky Pentecost Indications Bone neoplasia Osteosarcoma Fibrosarcoma Chondrosarcoma Severe trauma/paralysis Brachial plexus avulsion Infection Congenital
FREE DIEP-FLAP RECONSTRUCTION OF TUMOUR RELATED DEFECTS IN HEAD AND NECK
 JOURNAL OF PHYSIOLOGY AND PHARMACOLOGY 2008, 59, Suppl 5, 59 67 www.jpp.krakow.pl H. LEONHARDT 1, R. MAI 1, W. PRADEL 1, J. MARKWARDT 1, T. PINZER 2, A. SPASSOV 3, G. LAUER 1 FREE DIEP-FLAP RECONSTRUCTION
JOURNAL OF PHYSIOLOGY AND PHARMACOLOGY 2008, 59, Suppl 5, 59 67 www.jpp.krakow.pl H. LEONHARDT 1, R. MAI 1, W. PRADEL 1, J. MARKWARDT 1, T. PINZER 2, A. SPASSOV 3, G. LAUER 1 FREE DIEP-FLAP RECONSTRUCTION
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects
 Open Access Original Article DOI: 10.7759/cureus.2356 Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects Rhorie P. Kerr 1, Andrea Hanick 1, Michael A. Fritz 1 1. Head and Neck Institute,
Open Access Original Article DOI: 10.7759/cureus.2356 Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects Rhorie P. Kerr 1, Andrea Hanick 1, Michael A. Fritz 1 1. Head and Neck Institute,
Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps
 Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
SET - SNOMED Plastic Surgery (Aus.)
 NAME: Trainee Logbooks RACS ID: 18214 NOMINATED SUPERVISOR(S): Supervisor Logbooks ALTERNATE SUPERVISOR(S): Fellow Logbooks HOSPITAL(S): Flinders Medical Centre ROTATION PERIOD: T2 216 SET LEVEL: Year
NAME: Trainee Logbooks RACS ID: 18214 NOMINATED SUPERVISOR(S): Supervisor Logbooks ALTERNATE SUPERVISOR(S): Fellow Logbooks HOSPITAL(S): Flinders Medical Centre ROTATION PERIOD: T2 216 SET LEVEL: Year
Clinical teaching/experi ence. Lectures/semina rs/conferences Self-directed. learning. Clinical teaching/experi ence
 Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION
 Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
Interesting Case Series. Reconstruction of Dorsal Wrist Defects
 Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
FOLLOWING INTRODUCTION OF
 ORIGINAL ARTICLE Alternative 1-Step Nasal Reconstruction Technique Kazuo Kishi, MD, PhD; Nobuaki Imanishi, MD, PhD; Yusuke Shimizu, MD; Ruka Shimizu, MD, PhD; Keisuke Okabe, MD; Hideo Nakajima, MD, PhD
ORIGINAL ARTICLE Alternative 1-Step Nasal Reconstruction Technique Kazuo Kishi, MD, PhD; Nobuaki Imanishi, MD, PhD; Yusuke Shimizu, MD; Ruka Shimizu, MD, PhD; Keisuke Okabe, MD; Hideo Nakajima, MD, PhD
Anatomical Study of Pectoral Nerves and its Implications in Surgery
 DOI: 10.7860/JCDR/2014/8631.4545 Anatomy Section Original Article Anatomical Study of Pectoral Nerves and its Implications in Surgery Prakash KG 1, Saniya K 2 ABSTRACT Introduction: This anatomical study
DOI: 10.7860/JCDR/2014/8631.4545 Anatomy Section Original Article Anatomical Study of Pectoral Nerves and its Implications in Surgery Prakash KG 1, Saniya K 2 ABSTRACT Introduction: This anatomical study
Fascial Compartments of the Upper Arm
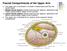 Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Modified Radical Mastectomy
 Modified Radical Mastectomy Valerie L. Staradub, MD, and Monica Morrow, MD S urgical management options for breast cancer include modified radical mastectomy (MRM), MRM with immediate reconstruction, and
Modified Radical Mastectomy Valerie L. Staradub, MD, and Monica Morrow, MD S urgical management options for breast cancer include modified radical mastectomy (MRM), MRM with immediate reconstruction, and
Scapular and Deltoid Regions
 M1 Gross and Developmental Anatomy Scapular and Deltoid Regions Dr. Peters 1 Outline I. Skeleton of the Shoulder and Attachment of the Upper Extremity to Trunk II. Positions and Movements of the Scapula
M1 Gross and Developmental Anatomy Scapular and Deltoid Regions Dr. Peters 1 Outline I. Skeleton of the Shoulder and Attachment of the Upper Extremity to Trunk II. Positions and Movements of the Scapula
