Malignant Transformation of a Dysembryoplastic Neuroepithelial Tumor (DNET) Characterized by Genome-Wide Methylation Analysis
|
|
|
- Joel Lindsey
- 5 years ago
- Views:
Transcription
1 J Neuropathol Exp Neurol Vol. 75, No. 4, April 2016, pp doi: /jnen/nlw007 ORIGINAL ARTICLE Malignant Transformation of a Dysembryoplastic Neuroepithelial Tumor (DNET) Characterized by Genome-Wide Methylation Analysis Dieter Henrik Heiland, MD, Ori Staszewski, MD, Martin Hirsch, MD, Waseem Masalha, MD, Pamela Franco, MD, Jürgen Grauvogel, MD, David Capper, MD, Daniel Schrimpf, Dr. sci. hum., Horst Urbach, MD, and Astrid Weyerbrock, MD Abstract Dysembryoplastic neuroepithelial tumors (DNET) are considered to be rare, benign, and associated with chronic epilepsy. We present the case of a 28-year-old man with a history of epilepsy since age 12. Surgery of an occipital cortical lesion in 2009 revealed a DNET. Five years later, a recurrent tumor at the edge of the resection cavity was removed, and the tissue underwent an intensive diagnostic workup. The first tumor was unequivocally characterized as a DNET, but neuropathological diagnostics of the recurrent tumor revealed a glioblastoma. After 6 months, another recurrent tumor was detected next to the location of the original tumor, and this was also resected. An Illumina 450 K beadchip methylation array was performed to characterize all of the tumors. The methylation profile of these tumors significantly differed from other glioblastoma and epilepsy-associated tumor profiles and revealed a DNET-like methylation profile. Thus, molecular characterization of these recurrent tumors suggests malignant transformation of a previously benign DNET. We found increased copy number changes in the recurrent DNET tumors after malignant transformation. Modern high-throughput analysis adds essential molecular information in addition to standard histopathology for proper identification of rare brain tumors that present with an unusual clinical course. Key Words: Copy number changes, Dysembryoplastic neuroepithelial tumor (DNET), Epigenetic alteration, Illumina 450 K beadchip methylation array, Malignant DNET, Methylation. From the Department of Neurosurgery (DHH, WM, PF, JG, AW), Department of Pathology, Institute of Neuropathology (OS), Department of Neurosurgery, Epilepsy Center (MH), and Department of Neuroradiology (HU), Medical Center - University of Freiburg, Freiburg, Germany; and Department of Neuropathology, University Heidelberg, Im Neuenheimer Feld 224 and German Cancer Consortium (DKTK), CCU Neuropathology, German Cancer Research Center (DKFZ), Heidelberg, Germany (DC, DS). Send correspondence to: Astrid Weyerbrock, MD, Department of Neurosurgery, Medical Center - University of Freiburg, Breisacher Strasse 64, Freiburg, Germany; astrid.weyerbrock@uniklinik-freiburg.de This study was supported by the core facility of CCU Neuropathology, German Cancer Research Center, Heidelberg, Germany. INTRODUCTION Dysembryoplastic neuroepithelial tumors (DNETs) are classified as low-grade (World Health Organization [WHO] I) tumors with a good prognosis. If they are symptomatic, they can be treated successfully by surgery alone. Daumas-Duport et al first described DNETs as curable tumors of young patients; they are cortical lesions with multinodular architecture containing loci resembling diffuse oligodendroglioma, oligoastrocytoma, and astrocytoma elements with floating neurons (1). Kleihues et al described DNETs as slow-growing tumors that typically do not undergo malignant transformation to high-grade tumors (2). Moreover, 11 cases of suspected recurrent DNET were recently reanalyzed and reclassified as lowor high-grade astrocytoma or oligoastrocytoma based on histopathological and immunohistochemical features (3). Malignant transformation of DNET is not considered in the current version of the WHO classification of CNS tumors, and no information exists whether or not these tumors maintain their DNET characteristics upon malignant transformation. We report the case of a recurrent DNET with secondary malignant transformation mimicking histopathological features of a glioblastoma (GBM). Methylation analysis by Illumina 450 K beadchip methylation array and comparison with methylation patterns of glial tumors in The Cancer Genome Atlas and the German Cancer Research Center (DKFZ) databases allowed identification of the recurrent tumor as a DNET that had undergone malignant transformation with a methylation pattern distinct from that of malignant gliomas. MATERIALS AND METHODS Patient A 28-year-old man suffered from a seizure disorder since the age of 12. His disorder was described as structural epilepsy with visual aura followed by secondary bilateral tonic-clonic seizures. In 2009, an MRI brain scan revealed a cortical and subcortical occipital lesion localized next to the optical fiber tracts with low signal in T1-weighted images, high signal in T2-weighted images, and no contrast enhancement or mass effect (Fig. 1A). The tumor was identified as the epileptogenic focus by presurgical epilepsy diagnostics. 358 VC 2016 American Association of Neuropathologists, Inc. All rights reserved.
2 J Neuropathol Exp Neurol Volume 75, Number 4, April 2016 The patient underwent surgery, and the tumor was subtotally resected due to the proximity to the optic tract, which was successfully preserved. Histopathologically, the tumor was characterized as a DNET WHO grade I (Fig. 2). Yearly postoperative follow-up scans were performed (Fig. 1B, C). Five Malignant Transformation of a DNET years later, the patient developed deterioration of his overall clinical condition and an increase in the frequency of the epileptic seizures. An MRI brain scan revealed a new contrastenhancing lesion with slight mass effect but without extensive brain edema next to the cortical left occipital resection FIGURE 1. (A, B) Pre- and postoperative MRIs from 2009; T1-weighted images with contrast enhancement and T2-weighted images. (C) Follow-up MRIs from 2010 until tumor progression in (D) Preoperative tractography of the visual tracts. The tractography is superimposed on the MRI using white dots and marked with an arrow. (E) Preoperative T1-weighted images with contrast enhancement and T2-weighted images. (F) T1- and T2-weighted images of the first follow-up in (G) Preoperative T1-weighted images with contrast enhancement (arrow) and T2-weighted and diffusion images, May 2015 (arrowheads). (H) Postoperative MRIs from 2015: T1-weighted images with contrast enhancement and T2-weighted images. 359
3 Heiland et al J Neuropathol Exp Neurol Volume 75, Number 4, April 2016 FIGURE 2. Histopathology and immunostaining of samples in 2009, 2014, and (A) In 2009, hematoxylin and eosin (H&E) staining shows loss of oligodendroglia-like cells. The tumor of 2009 shows typical dysembryoplastic neuroepithelial tumor (DNET) morphology. (B) In the recurrent tumor (2014), microtubule-associated protein 2 (Map2) immunohistochemistry stains some tumor cells with prominent cellular processes; no neurons are stained. Ki67 immunostaining reveals a strongly increased proliferative activity with about 10% of cells staining positively in 2014 compared with <1% in 2009 (A). The histological and immunohistochemical findings of the recurrent tumor bear all hallmarks of a glioblastoma (WHO IV). (C) The histological and immunohistochemical findings of the recurrent malignant DNET show parts of GBM morphology but also DNET features. GFAP, glial fibrillary acidic protein. 360
4 J Neuropathol Exp Neurol Volume 75, Number 4, April 2016 cavity. A preoperative MRI scan with tractography of the visual tracts was obtained for intraoperative navigation (Fig. 1D, E). The tumor was removed, and a comprehensive diagnostic and molecular analysis was performed. The patient underwent postoperative adjuvant radiotherapy. The 3-month follow-up scan showed no tumor progression (Fig. 1F). Six months after the surgery, new contrast enhancing lesions were detected around the resection cavity (Fig. 1G). Again, the tumor was removed, and intensive comprehensive diagnostic and molecular analysis was performed. The most recent 3- month follow-up in August 2015 showed no tumor progression (Fig. 1H). Histopathological and Immunohistochemical Analyses Standard histology was performed on paraffin-embedded tumor tissue after written informed consent of the patient. Retrieval and scientific analysis of patient-derived tissue was approved by the local ethics committee under protocol /09. Tissue samples were fixed using 4% phosphate-buffered formaldehyde and paraffin embedded with standard procedures. Hematoxylin and eosin stains were performed on 4-mm paraffin sections using standard protocols. Immunohistochemistry was performed using an autostainer (Dako, Glostrup, Denmark) after heat-induced epitope retrieval in citrate buffer. Primary antibodies used were to glial fibrillary acidic protein ([GFAP] 1:1000, Zytomed Systems, Berlin, Germany), NeuN (1:500, Millipore, Billerica, MA), Ki-67 (Mib1, 1:50, Dako), microtubule-associated protein 2 ([Map2] 1:10,000, Sigma-Aldrich, St Louis, MO), and synaptophysin (1:50, Dako). Diaminobenzidine DAB staining was performed using the Envision Flex High ph Kit (Dako). Isocitrate dehydrogenase IDH1 mutation was assessed by immunohistochemistry using an anti- IDH1-R123 antibody (1:20, Dianova, Hamburg, Germany). Methylation Analysis DNA was extracted from tumor tissue and underwent methylation analysis using the Infinium HumanMethylation450 BeadChip array ( at the DKFZ core facility (Heidelberg, Germany). All raw data of the Illumina 450 K beadchip methylation array were analyzed with R-software and available packages ( Data were imported and analyzed using the RnBeads pipeline (http// :rnbeads.mpi-inf.mpg.de). Quality control was done by major quality-control algorithms, including sample-independent controls. In a preprocessing Greedycut, 4713 CpG sites were removed because they overlap with single nucleotide polymorphisms and cause unreliable measurements. The background subtraction was performed using the methylumi package. We used the Beta-Mixture Quantile Normalization (BMIQ) method to normalize b-methylation values. In addition, we removed sex chromosomal probes (n ¼ 11,497). Methylation profiles were computed for the specific gene region types as whole gene regions, promoter region, and individual CpG islands. Differential methylation on gene regions was computed by t-testbased statistics (paired t test with false discovery rate (FDR)-adjusted p value) in the limma r-tool. Data visualization was done Malignant Transformation of a DNET in ggplot2 (r-based). Methylation data of the DNET and malignant DNETs were added to the DKFZ database and clustered by average-based unsupervised hierarchical cluster (Euclidean distance, complete linkage). Analysis of DKFZ Tumor Samples Tumor samples (n ¼ 116) from the DKFZ tumor database were used as reference samples. For further cluster analysis, we included 44 patients with a GBM. Fifteen out of 44 were classified as an H3.3 K27-mutated GBM; 14 patients had a G34 mutation. Methylation profiling grouped 15 patients into the receptor tyrosine kinase (RTK) I subgroup and 14 patients into the GBM classic (RTK II) subgroup. Fifteen patients had a R132H-mutated astrocytoma with a glioma CpG methylated phenotype (G-CIMP)-positive methylation pattern. In addition, typical epilepsy-associated tumors, including ganglioglioma (n ¼ 13), DNET (n ¼ 14), and pleomorphic xanthoastrocytoma (PXA) (n ¼ 15), were included in the cluster analysis. Raw data were processed as described above including agglomerative hierarchical clustering (median based). The clustering was performed at the DKFZ (Heidelberg, Germany). Copy Number Profile A copy number profile was done by R-software included in the conumee package (4) ( This tool allows performing copy number variation analysis on Infinium HumanMethylation450 BeadChip data. This function of detecting copy number alterations in HumanMethylation450 data was first described by Feber et al (5). Sturm et al used this tool to detect specific chromosomal aberrations in cancer samples (6). Copy number variation analysis was performed in a 2-step approach by combining methylated and unmethylated intensity values of each CpG probe and normalizing them with normal brain controls. In the next step, neighboring probes were combined by hybridization method. Finally, segmentation was performed by circular binary segmentation algorithm implemented in the DNAcopy package (5). Visualization included in the conumee package was performed at the DKFZ (Heidelberg, Germany). RESULTS Histopathology and Immunohistochemistry Hematoxylin-and-eosin-stained tissue sections obtained from the primary tumor in 2009 showed CNS tissue with sheaths and isolated nodules of monomorphic cells within a relatively sparse microcystic matrix. The tumor cells exhibited oligodendroglia-like morphology with monomorphic, small, round nuclei and optically clear perinuclear halos (Fig. 2A). Scattered isolated neurons were detected in NeuN immunostains. Synaptophysin immunohistochemistry showed a positively stained tumor matrix. Immunohistochemical staining for GFAP revealed weak GFAP-positive staining of the matrix with some activated astrocytes interspersed between the tumor cells; the tumor cells showed no GFAP expression. The scattered neurons were also 361
5 Heiland et al J Neuropathol Exp Neurol Volume 75, Number 4, April 2016 stained positively for Map2. The proliferation, marked by Ki- 67, was below 1% (Fig. 2A). In contrast to the primary lesion resected in 2009, the recurrent tumor in 2014 exhibited glial appearance with a lack of perinuclear halos and comparatively pleomorphic nuclei (Fig. 2B). The cell density was increased with areas of necrosis and microvascular proliferation. GFAP and Map2 immunostaining revealed fibrillary staining for GFAP in some tumor cells and strong staining for Map2. Notably, neuronal structures were absent, and NeuN and synaptophysin staining were negative. In the Ki67 immunostaining, positive staining of approximately 10% of the cells indicated increased tumor-cell proliferation. The histological and immunohistochemical findings of the recurrent tumor bear all hallmarks of GBM, WHO IV with an astroglial (GFAP-positive) component, necrosis, and microvascular proliferation. In addition, R123H-IDH1 mutation could be not detected in the original and recurrent DNET by immunostaining or Illumina 450 K beadchip methylation array (data not shown). The Illumina 450 K beadchip methylation array is a powerful tool to identify the IDH mutation by its epigenetic changes (G- CIMP) (7). Therefore, additional IDH-1 or IDH-2 sequencing was not necessary. The histological specimens were sent to 2 neuropathological reference centers (Heidelberg and Bonn, Germany) to obtain second opinions; both confirmed the histological features of a malignant glioma. The 1p19q-codeletion status was assessed by Illumina 450 K beadchip methylation array and additional copy number variation analysis. There were no typical gain and loss of 1p or 19q detected in the primary or recurrent tumors. The second recurrent malignant DNET showed a similar histological appearance as the first malignant DNET (Fig. 2C). Scattered neuronal structures were detected by NeuN staining, showing isolated neurons, and antisynaptophysin staining, showing positive reaction in parts of the tumor matrix. Increases of necrotic regions and nuclear pleomorphism were detected in the tumor. The second tumor recurrence tumor showed monomorphic cells within a relatively sparse microcystic matrix and areas of necrosis and microvascular proliferation. GFAP and Map2 immunostainings revealed strong fibrillary staining for GFAP and expression of Map2 in some of the tumor cells (Fig. 2C). In addition, the second recurrent malignant DNET was partly heterogeneous with parts of typical GBM morphology but also some areas of DNET morphology. Methylation Analysis Identifies Different Methylation Patterns Methylation data of the DNET samples (primary and 2 recurrences), GBM from the The Cancer Genome Atlas database (subgrouped in GBM-K27, GBM-G34, GBM-RTK-I, and GBM-RTK-II-Classical), and other epilepsy-associated tumors (ie, PXA and ganglioglioma) were clustered by Euclidean distance. The cluster analysis clearly showed distinct methylation patterns of the DNET WHO grade I and the malignant DNETs compared with GBM samples or other epilepsy-associated tumor types (Fig. 3A). Analysis of the original and the malignant DNET tumor revealed several genes 362 with methylation changes: 865 hypomethylated (> 0.2 methylation difference) and 76 hypermethylated genes in the malignant DNET (> 0.2 methylation difference) (Fig. 3B). Genes that are strongly demethylated in the malignant DNET included TRDD2 and TRDJ1, 2 genes that play a role in T- cell receptor binding, and IGHVIII-44, which is associated with the immune system. On the other hand, we found a loss of gene promoter methylation of oncogenes such as HULC, which is linked to hepatocellular cancer (8). Further analysis showed a genome-wide distribution of the methylation differences (Fig. 3C, D). These methylation patterns are only partially associated with copy number changes. In summary, there was a loss of methylation after malignant transformation resulting in a methylation pattern distinct from the typical pattern of the GBM samples (Fig. 3A). Most of the methylation changes were on chromosomes 1, 6, and 15. A detailed analysis of methylation changes in specific gene regions could not be performed (n ¼ 1). Multiple chromosomal aberrations were seen after malignant transformation. As shown in Fig. 4A, typical DNETs do not have any chromosomal aberrations. As expected, the copy number profile of the original DNET did not reveal any chromosomal aberrations. After malignant transformation, losses on chromosome 10, 14 19, and 22 were detected (Fig. 4B). Only chromosome 21 revealed a slight gain. In the recurrent malignant DNET, the chromosomal aberrations increased (Fig. 4C). Copy number changes were detected with a gain on chromosomes 5 7 and 21. A chromosomal loss was found on chromosomes 2, 9 11, 13 14, 16, 19, and 22 (Fig. 4C). DISCUSSION Here, we describe for the first time the malignant transformation of an initially benign DNET (confirmed by modern high-throughput analysis), the recurrence of which was initially classified as a malignant glioma based on standard neuropathological diagnostics. We introduce an Illumina 450 K beadchip methylation array as a diagnostic tool to characterize brain tumors and identify differences in their methylation profiles. The Illumina 450 K beadchip methylation array is widely used in research to analyze genome-wide methylation changes, for example, in IDH-mutated gliomas (9). A recent study showed different GBM subtypes that could be identified by methylation array (6). By unsupervised clustering of these GBM subtypes and other epilepsy-associated tumors, we identified individually clustered subgroups. Specific methylation profiles were representative for each tumor entity. This technique is new and not well established but adds valuable additional information to classic histopathological findings. Malignant transformation of a DNET is a rare phenomenon with few cases described in the literature; at this time, this is not considered in the WHO classification of tumors of the CNS (10). A recent literature review of malignant DNET cases identified 11 cases of malignant transformation of tumors primarily categorized as WHO grade I DNET. The recurrent tumors were most often classified as oligo- or astrocytomas ranging from grades II to IV or pilocytic astrocytomas. We report the transformation of a DNET WHO grade I into a high-grade DNET. Its methylation
6 J Neuropathol Exp Neurol Volume 75, Number 4, April 2016 Malignant Transformation of a DNET FIGURE 3. (A) Hierarchical cluster of different glioblastoma subtypes (G43, RTK-I, RTK-II, K27, IDH1-mutated) and other epilepsy-associated tumors (ganglioglioma, dysembryoplastic neuroepithelial tumor [DNET], PXA). The heatmap shows the 1000 most-variable CpG sites with low methylation values colored in blue, medium methylation level in white, and high methylation CpG in red. Samples of the origin DNET and the recurrent tumors are marked in black. (B) After malignant transformation of the original DNET, 754 gene promoters were strongly demethylated (mean methylation changes of CpG sites in gene promoter, p > 0.2); 74 showed increased methylation (p > 0.2). (C, D) Differential methylation of genes in DNET before and after malignant transformation. (E, F) Volcano and scatter plots of differential methylation of gene promoters. 363
7 Heiland et al J Neuropathol Exp Neurol Volume 75, Number 4, April 2016 FIGURE 4. Copy number variants (CNV) of the origin dysembryoplastic neuroepithelial tumor (DNET) and the recurrent tumors of 2014 and Increased numbers of CNVs with gene loss and gain were detected after malignant transformation. (A) Original DNET. (B) DNET after malignant transformation. (C) Recurrent malignant DNET. 364
8 J Neuropathol Exp Neurol Volume 75, Number 4, April 2016 pattern clearly differs from typical glioma methylation patterns that have been described (6, 11, 12). In particular, all specific GBM methylation subgroups were clearly distinct from the DNET and malignant DNET methylation patterns. Therefore, despite histological criteria of a malignant glioma (ie, staining for glial markers, high proliferation, necrosis, and angiogenesis), the recurrent tumor should be categorized as a malignant DNET with reference to its tumor of origin and the methylation pattern incompatible with established methylation patterns of GBM subtypes. Comparison of the methylation patterns of the original and recurrent malignant DNET indicates a loss of methylation of a variety of promoter regions after malignant transformation. These methylation changes lead to the massive chromosomal aberrations shown in Fig. 4. We performed differential methylation analysis to identify genes that potentially could play a role in the malignant transformation. On the basis of an individual case, further specific methylation and pathway analysis is not possible. Because of the low sample number of DNETs (n ¼ 13) and malignant DNETs (n ¼ 2 [of the same patient]), the results of this analysis are of interest but have low explanatory power. We found increased methylation in genes associated with the T-cell response and the immune system, whereas oncogenes such as HULC were demethylated (8). Another demethylated gene was VPS72, a gene that plays a role in hematopoietic stem cell development (13). These findings must be verified in a larger sample of malignant DNETs. In addition, we saw a gain on chromosome 21 and several chromosomal losses. These chromosomal aberrations are common in a variety of leukemias and thyroid cancers (14) and require further analysis of their biological relevance. Interestingly, chromosomal aberrations and instability were never described in DNET, whereas malignant gliomas show massive instabilities (15, 16). The recurrence of the malignant DNET emphasized its aggressive phenotype. We detected an increased number of chromosomal aberrations in the second recurrent malignant DNET, which represent an ongoing malignant transformation. Although our analysis includes 1 case of primary and malignant transformed DNET, it clearly points to the increasing importance of high-throughput molecular analysis of CNS tumors for proper identification of rare tumors with distinct marker profiles and unusual clinical courses. These results have to be reevaluated with more matched tumor samples of transformed tumors. This study describes for the first time the molecular subtype of a malignant DNET identified by Illumina 450 K beadchip methylation array. Adding molecular data to standard neuropathological analysis allows proper identification Malignant Transformation of a DNET of rare CNS tumors and identification of specific subtypes based on the pattern of molecular markers and may help delivering the adequate treatment to the affected patients. REFERENCES 1. Daumas-Duport C, Scheithauer BW, Chodkiewicz JP, et al. Dysembryoplastic neuroepithelial tumor: A surgically curable tumor of young patients with intractable partial seizures. Report of thirty-nine cases. Neurosurgery 1988;23: Kleihues P, Burger PC, Scheithauer BW. The new WHO classification of brain tumours. Brain Pathol 1993;3: Moazzam AA, Wagle N, Shiroishi MS. Malignant transformation of DNETs: A case report and literature review. Neuroreport 2014;25: Hovestadt V, Zapatka M. Conumee: Enhanced copy-number variation analysis using Illumina 450k methylation arrays. Available at: Feber A, Guilhamon P, Lechner M, et al. Using high-density DNA methylation arrays to profile copy number alterations. Genome Biol 2014; 15:R30 6. Sturm D, Witt H, Hovestadt V, et al. Hotspot mutations in H3F3A and IDH1 define distinct epigenetic and biological subgroups of glioblastoma. Cancer Cell 2012;22: Wiestler B, Capper D, Hovestadt V, et al. Assessing CpG island methylator phenotype, 1p/19q codeletion, and MGMT promoter methylation from epigenome-wide data in the biomarker cohort of the NOA-04 trial. Neuro Oncol 2014;16: Peng W, Gao W, Feng J. Long noncoding RNA HULC is a novel biomarker of poor prognosis in patients with pancreatic cancer. Med Oncol 2014;31: Noushmehr H, Weisenberger DJ, Diefes K, et al. Identification of a CpG island methylator phenotype that defines a distinct subgroup of glioma. Cancer Cell 2010;17: Louis DN, Ohgaki H, Wiestler OD, et al. The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol 2007; 114: Verhaak RG, Hoadley KA, Purdom E, et al. Integrated genomic analysis identifies clinically relevant subtypes of glioblastoma characterized by abnormalities in PDGFRA, IDH1, EGFR, and NF1. Cancer Cell 2010; 17: Wagner DE, Ho JJ, Reddien PW. Genetic regulators of a pluripotent adult stem cell system in planarians identified by RNAi and clonal analysis. Cell Stem Cell 2012;10: Umemoto T, Yamato M, Ishihara J, et al. Integrin-avb3 regulates thrombopoietin-mediated maintenance of hematopoietic stem cells. Blood 2012;119: Fröhling S, Döhner H. Chromosomal abnormalities in cancer. N Engl J Med 2008;359: Brat DJ, Verhaak RG, Cancer Genome Atlas Research Network, et al. Comprehensive, integrative genomic analysis of diffuse lower-grade gliomas. N Engl J Med 2015;372: Brennan CW, Verhaak RG, McKenna A, et al. The somatic genomic landscape of glioblastoma. Cell 2013;155:
2017 Diagnostic Slide Session Case 3
 2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad
 Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas
 The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas Stefan Prokop, MD Neuropathology Fellow Hospital of the University of Pennsylvania Background
The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas Stefan Prokop, MD Neuropathology Fellow Hospital of the University of Pennsylvania Background
MOLECULAR DIAGNOSTICS OF GLIOMAS
 MOLECULAR DIAGNOSTICS OF GLIOMAS Arie Perry, M.D. Director, Neuropathology Division DIFFUSE GLIOMAS Cell types Astrocytomas (A) Oligodendrogliomas (O) Mixed oligoastrocytoma (MOA) Three WHO grades: II,
MOLECULAR DIAGNOSTICS OF GLIOMAS Arie Perry, M.D. Director, Neuropathology Division DIFFUSE GLIOMAS Cell types Astrocytomas (A) Oligodendrogliomas (O) Mixed oligoastrocytoma (MOA) Three WHO grades: II,
Morphological features and genetic alterations
 Morphological features and genetic alterations Tutor : Audrey Rousseau Caget Lise: Université d Angers Iorio Vittoria: Seconda Università degli studi di Napoli Manaila Roxana: Iuliu Hatieganu University
Morphological features and genetic alterations Tutor : Audrey Rousseau Caget Lise: Université d Angers Iorio Vittoria: Seconda Università degli studi di Napoli Manaila Roxana: Iuliu Hatieganu University
Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls. Rob Macaulay Neuropathologist, MCC October 21, 2017
 Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls Rob Macaulay Neuropathologist, MCC October 21, 2017 Objectives Explain why the designation high grade glioma is preferable to GBM for intraoperative
Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls Rob Macaulay Neuropathologist, MCC October 21, 2017 Objectives Explain why the designation high grade glioma is preferable to GBM for intraoperative
Case Presentation: USCAP Jason T. Huse, MD, PhD Assistant Member Department of Pathology Memorial Sloan Kettering Cancer Center
 Case Presentation: USCAP 2016 Jason T. Huse, MD, PhD Assistant Member Department of Pathology Memorial Sloan Kettering Cancer Center Case History 53 year old female with a long standing history of migraines
Case Presentation: USCAP 2016 Jason T. Huse, MD, PhD Assistant Member Department of Pathology Memorial Sloan Kettering Cancer Center Case History 53 year old female with a long standing history of migraines
Neuropathology Evening Session: Case 3
 Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Gliomas in the 2016 WHO Classification of CNS Tumors
 Gliomas in the 2016 WHO Classification of CNS Tumors Hindi N Al-Hindi, MD, FCAP Consultant Neuropathologist and Head Section of Anatomic Pathology Department of Pathology and Laboratory Medicine King Faisal
Gliomas in the 2016 WHO Classification of CNS Tumors Hindi N Al-Hindi, MD, FCAP Consultant Neuropathologist and Head Section of Anatomic Pathology Department of Pathology and Laboratory Medicine King Faisal
In 1988 Dumas-Duport et al. first used
 Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Radioterapia no Tratamento dos Gliomas de Baixo Grau
 Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
Nature Methods: doi: /nmeth.3115
 Supplementary Figure 1 Analysis of DNA methylation in a cancer cohort based on Infinium 450K data. RnBeads was used to rediscover a clinically distinct subgroup of glioblastoma patients characterized by
Supplementary Figure 1 Analysis of DNA methylation in a cancer cohort based on Infinium 450K data. RnBeads was used to rediscover a clinically distinct subgroup of glioblastoma patients characterized by
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
Examining large groups of cancer patients to identify ways of predicting which therapies cancers might respond to.
 Stratified Medicine Examining large groups of cancer patients to identify ways of predicting which therapies cancers might respond to. Looking in detail at cancer cells and their genetic make up. Permit
Stratified Medicine Examining large groups of cancer patients to identify ways of predicting which therapies cancers might respond to. Looking in detail at cancer cells and their genetic make up. Permit
Chapter 1 Introduction
 Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
Gliomatosis cerebri: no evidence for a separate brain tumor entity
 DOI 10.1007/s00401-015-1495-z ORIGINAL PAPER Gliomatosis cerebri: no evidence for a separate brain tumor entity Ulrich Herrlinger 1 David T. W. Jones 2,3 Martin Glas 1,4 Elke Hattingen 5 Dorothee Gramatzki
DOI 10.1007/s00401-015-1495-z ORIGINAL PAPER Gliomatosis cerebri: no evidence for a separate brain tumor entity Ulrich Herrlinger 1 David T. W. Jones 2,3 Martin Glas 1,4 Elke Hattingen 5 Dorothee Gramatzki
Five Most Common Problems in Surgical Neuropathology
 Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
DNA methylation signatures for 2016 WHO classification subtypes of diffuse gliomas
 Paul et al. Clinical Epigenetics (2017) 9:32 DOI 10.1186/s13148-017-0331-9 RESEARCH Open Access DNA methylation signatures for 2016 WHO classification subtypes of diffuse gliomas Yashna Paul, Baisakhi
Paul et al. Clinical Epigenetics (2017) 9:32 DOI 10.1186/s13148-017-0331-9 RESEARCH Open Access DNA methylation signatures for 2016 WHO classification subtypes of diffuse gliomas Yashna Paul, Baisakhi
SUPPLEMENTARY FIGURES: Supplementary Figure 1
 SUPPLEMENTARY FIGURES: Supplementary Figure 1 Supplementary Figure 1. Glioblastoma 5hmC quantified by paired BS and oxbs treated DNA hybridized to Infinium DNA methylation arrays. Workflow depicts analytic
SUPPLEMENTARY FIGURES: Supplementary Figure 1 Supplementary Figure 1. Glioblastoma 5hmC quantified by paired BS and oxbs treated DNA hybridized to Infinium DNA methylation arrays. Workflow depicts analytic
IDH1 R132H/ATRX Immunohistochemical validation
 IDH1 R132H/ATRX Immunohistochemical validation CIQC/DSM 2016 12 June 2016 0835-0905 Stephen Yip, M.D., Ph.D., FRCPC University of British Columbia Disclosure Statement I have nothing to disclose I will
IDH1 R132H/ATRX Immunohistochemical validation CIQC/DSM 2016 12 June 2016 0835-0905 Stephen Yip, M.D., Ph.D., FRCPC University of British Columbia Disclosure Statement I have nothing to disclose I will
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
A clinical perspective on neuropathology and molecular genetics in brain tumors
 A clinical perspective on neuropathology and molecular genetics in brain tumors M.J. van den Bent Erasmus MC Cancer Institute Rotterdam, the Netherlands Disclosures Member speakersbureau: MSD Consultancy:
A clinical perspective on neuropathology and molecular genetics in brain tumors M.J. van den Bent Erasmus MC Cancer Institute Rotterdam, the Netherlands Disclosures Member speakersbureau: MSD Consultancy:
What yield in the last decade about Molecular Diagnostics in Neuro
 What yield in the last decade about Molecular Diagnostics in Neuro Oncology? Raphael Salles S.Medeiros Neuropathologist at HC FMUSP Clinical Research Project Manager at Oncology department at Hospital
What yield in the last decade about Molecular Diagnostics in Neuro Oncology? Raphael Salles S.Medeiros Neuropathologist at HC FMUSP Clinical Research Project Manager at Oncology department at Hospital
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
Clinical significance of genetic analysis in glioblastoma treatment
 Clinical significance of genetic analysis in glioblastoma treatment Department of Neurosurgery, Graduate School of Medical Sciences, Kyushu University, Fukuoka, Japan Koji Yoshimoto Can we get prognostic
Clinical significance of genetic analysis in glioblastoma treatment Department of Neurosurgery, Graduate School of Medical Sciences, Kyushu University, Fukuoka, Japan Koji Yoshimoto Can we get prognostic
21/03/2017. Disclosure. Practice Changing Articles in Neuro Oncology for 2016/17. Gliomas. Objectives. Gliomas. No conflicts to declare
 Practice Changing Articles in Neuro Oncology for 2016/17 Disclosure No conflicts to declare Frances Cusano, BScPharm, ACPR April 21, 2017 Objectives Gliomas To describe the patient selection, methodology
Practice Changing Articles in Neuro Oncology for 2016/17 Disclosure No conflicts to declare Frances Cusano, BScPharm, ACPR April 21, 2017 Objectives Gliomas To describe the patient selection, methodology
Supplemental Information. Molecular, Pathological, Radiological, and Immune. Profiling of Non-brainstem Pediatric High-Grade
 Cancer Cell, Volume 33 Supplemental Information Molecular, Pathological, Radiological, and Immune Profiling of Non-brainstem Pediatric High-Grade Glioma from the HERBY Phase II Randomized Trial Alan Mackay,
Cancer Cell, Volume 33 Supplemental Information Molecular, Pathological, Radiological, and Immune Profiling of Non-brainstem Pediatric High-Grade Glioma from the HERBY Phase II Randomized Trial Alan Mackay,
Genomic analysis of childhood High grade glial (HGG) brain tumors
 Genomic analysis of childhood High grade glial (HGG) brain tumors Linda D Cooley Children s Mercy, Kansas City The Children s Mercy Hospital, 2017 Genomic analysis of childhood High grade glial (HGG) brain
Genomic analysis of childhood High grade glial (HGG) brain tumors Linda D Cooley Children s Mercy, Kansas City The Children s Mercy Hospital, 2017 Genomic analysis of childhood High grade glial (HGG) brain
Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum
 Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
CHINESE MEDICAL ASSOCIATION
 Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Case #3. USCAP Neuropathology Evening Seminar/Companion Meeting
 Case #3 USCAP Neuropathology Evening Seminar/Companion Meeting Clinical History A 71-year year-old man presented with a 4-4 week history of word finding difficulty. An initial screening head CT followed
Case #3 USCAP Neuropathology Evening Seminar/Companion Meeting Clinical History A 71-year year-old man presented with a 4-4 week history of word finding difficulty. An initial screening head CT followed
5-hydroxymethylcytosine loss is associated with poor prognosis for
 5-hydroxymethylcytosine loss is associated with poor prognosis for patients with WHO grade II diffuse astrocytomas Feng Zhang 1,*, Yifan Liu 2, Zhiwen Zhang 1, Jie Li 1, Yi Wan 3, Liying Zhang 1, Yangmei
5-hydroxymethylcytosine loss is associated with poor prognosis for patients with WHO grade II diffuse astrocytomas Feng Zhang 1,*, Yifan Liu 2, Zhiwen Zhang 1, Jie Li 1, Yi Wan 3, Liying Zhang 1, Yangmei
Gliomatosis cerebri: no evidence for a separate brain tumor entity
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2016 Gliomatosis cerebri: no evidence for a separate brain tumor entity Herrlinger,
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2016 Gliomatosis cerebri: no evidence for a separate brain tumor entity Herrlinger,
Dysembryoplastic Neuroepithelial Tumor (DNT): Morphological and Immunohistochemical Features
 JKAU: Med. Sci., Vol. 14 No. 3, pp: 45-54 (2007 A.D. / 1428 A.H.) Dysembryoplastic Neuroepithelial Tumor (DNT): Morphological and Immunohistochemical Features Jaudah A. Al-Maghrabi 1,2 (MD, FRCPC) Department
JKAU: Med. Sci., Vol. 14 No. 3, pp: 45-54 (2007 A.D. / 1428 A.H.) Dysembryoplastic Neuroepithelial Tumor (DNT): Morphological and Immunohistochemical Features Jaudah A. Al-Maghrabi 1,2 (MD, FRCPC) Department
Title. CitationBrain Tumor Pathology, 34(4): Issue Date Doc URL. Rights. Type. Additional There Information.
 Title Diencephalic pediatric low-grade glioma harboring th sequential biopsy specimens Ishi, Yukitomo; Hatanaka, Kanako C.; Yamaguchi, Shig Author(s) Terasaka, Shunsuke; Houkin, Kiyohiro CitationBrain
Title Diencephalic pediatric low-grade glioma harboring th sequential biopsy specimens Ishi, Yukitomo; Hatanaka, Kanako C.; Yamaguchi, Shig Author(s) Terasaka, Shunsuke; Houkin, Kiyohiro CitationBrain
Corporate Medical Policy
 Corporate Medical Policy Analysis of MGMT Promoter Methylation in Malignant Gliomas File Name: Origination: Last CAP Review: Next CAP Review: Last Review: analysis_of_mgmt_promoter_methylation_in_malignant_gliomas
Corporate Medical Policy Analysis of MGMT Promoter Methylation in Malignant Gliomas File Name: Origination: Last CAP Review: Next CAP Review: Last Review: analysis_of_mgmt_promoter_methylation_in_malignant_gliomas
Pleomorphic Xanthoastrocytoma
 Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
I have no conflicts of interest in relation to this presentation. Vogel FS & Burger PC 3/28/2016
 IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
In 2005, Wang and coworkers 1 described a report of 8
 Angiocentric Glioma A Clinicopathologic Review of 5 Tumors With Identification of Associated Cortical Dysplasia Trent Marburger, MD; Richard Prayson, MD N Context. Angiocentric glioma is a rare, epilepsy-associated,
Angiocentric Glioma A Clinicopathologic Review of 5 Tumors With Identification of Associated Cortical Dysplasia Trent Marburger, MD; Richard Prayson, MD N Context. Angiocentric glioma is a rare, epilepsy-associated,
WHO 2016 CNS Tumor Classification Update. DISCLOSURES (Arie Perry, MD) PATTERN RECOGNITION. Arie Perry, M.D. Director, Neuropathology
 WHO 2016 CNS Tumor Classification Update Arie Perry, M.D. Director, Neuropathology DISCLOSURES (Arie Perry, MD) I have no financial relationships to disclose. - and - I will not discuss off label use or
WHO 2016 CNS Tumor Classification Update Arie Perry, M.D. Director, Neuropathology DISCLOSURES (Arie Perry, MD) I have no financial relationships to disclose. - and - I will not discuss off label use or
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature10866 a b 1 2 3 4 5 6 7 Match No Match 1 2 3 4 5 6 7 Turcan et al. Supplementary Fig.1 Concepts mapping H3K27 targets in EF CBX8 targets in EF H3K27 targets in ES SUZ12 targets in ES
doi:10.1038/nature10866 a b 1 2 3 4 5 6 7 Match No Match 1 2 3 4 5 6 7 Turcan et al. Supplementary Fig.1 Concepts mapping H3K27 targets in EF CBX8 targets in EF H3K27 targets in ES SUZ12 targets in ES
Dual-Genotype Diffuse Low-Grade Glioma: Is It Really Time to Abandon Oligoastrocytoma As a Distinct Entity?
 Journal of Neuropatholgy & Experimental Neurology Vol. 0, No. 0, 2017, pp. 1 5 doi: 10.1093/jnen/nlx024 BRIEF REPORT Dual-Genotype Diffuse Low-Grade Glioma: Is It Really Time to Abandon Oligoastrocytoma
Journal of Neuropatholgy & Experimental Neurology Vol. 0, No. 0, 2017, pp. 1 5 doi: 10.1093/jnen/nlx024 BRIEF REPORT Dual-Genotype Diffuse Low-Grade Glioma: Is It Really Time to Abandon Oligoastrocytoma
Dysembryoplastic neuroepithelial tumor with atypical presentation: MRI and diffusion tensorcharacteristics
 Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons Radiology Faculty Publications Radiology 2013 Dysembryoplastic neuroepithelial tumor with atypical
Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons Radiology Faculty Publications Radiology 2013 Dysembryoplastic neuroepithelial tumor with atypical
Understanding general brain tumor pathology, Part I: The basics. Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky
 Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Results and Discussion of Receptor Tyrosine Kinase. Activation
 Results and Discussion of Receptor Tyrosine Kinase Activation To demonstrate the contribution which RCytoscape s molecular maps can make to biological understanding via exploratory data analysis, we here
Results and Discussion of Receptor Tyrosine Kinase Activation To demonstrate the contribution which RCytoscape s molecular maps can make to biological understanding via exploratory data analysis, we here
Molecular Classification Defines 4 Prognostically Distinct Glioma Groups Irrespective of Diagnosis and Grade
 J Neuropathol Exp Neurol Copyright Ó 2015 by the American Association of Neuropathologists, Inc. Vol. 74, No. 3 March 2015 pp. 241Y249 ORIGINAL ARTICLE Molecular Classification Defines 4 Prognostically
J Neuropathol Exp Neurol Copyright Ó 2015 by the American Association of Neuropathologists, Inc. Vol. 74, No. 3 March 2015 pp. 241Y249 ORIGINAL ARTICLE Molecular Classification Defines 4 Prognostically
Adult IDH wild type astrocytomas biologically and clinically resolve into other tumor entities
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2015 Adult IDH wild type astrocytomas biologically and clinically resolve into
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2015 Adult IDH wild type astrocytomas biologically and clinically resolve into
Advances in Brain Tumor Research: Leveraging BIG data for BIG discoveries
 Advances in Brain Tumor Research: Leveraging BIG data for BIG discoveries Jill Barnholtz-Sloan, PhD Associate Professor & Associate Director for Bioinformatics and Translational Informatics jsb42@case.edu
Advances in Brain Tumor Research: Leveraging BIG data for BIG discoveries Jill Barnholtz-Sloan, PhD Associate Professor & Associate Director for Bioinformatics and Translational Informatics jsb42@case.edu
성균관대학교삼성창원병원신경외과학교실신경종양학 김영준. KNS-MT-03 (April 15, 2015)
 성균관대학교삼성창원병원신경외과학교실신경종양학 김영준 INTRODUCTIONS Low grade gliomas (LGG) - heterogeneous group of tumors with astrocytic, oligodendroglial, ependymal, or mixed cellular histology - In adults diffuse, infiltrating
성균관대학교삼성창원병원신경외과학교실신경종양학 김영준 INTRODUCTIONS Low grade gliomas (LGG) - heterogeneous group of tumors with astrocytic, oligodendroglial, ependymal, or mixed cellular histology - In adults diffuse, infiltrating
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
R1601 Essential Immunohistochemical and Molecular Markers for General CNS Glial Tumors
 October 22, 2018 12:00-1:00 PM Background The World Health Organization Classification of tumors of the Central Nervous System has recently been revised. There is now greater emphasis on molecular phenotype
October 22, 2018 12:00-1:00 PM Background The World Health Organization Classification of tumors of the Central Nervous System has recently been revised. There is now greater emphasis on molecular phenotype
Review: Diagnostic, prognostic and predictive relevance of molecular markers in gliomas
 Review: Diagnostic, prognostic and predictive relevance of molecular markers in gliomas Sebastian Brandner MD FRCPath 1 and Andreas von Deimling 2 MD 1) Division of Neuropathology, The National Hospital
Review: Diagnostic, prognostic and predictive relevance of molecular markers in gliomas Sebastian Brandner MD FRCPath 1 and Andreas von Deimling 2 MD 1) Division of Neuropathology, The National Hospital
Gangliogliomas: A Report of Five Cases
 Case Report Gangliogliomas: A Report of Five Cases Nair V, Suri VS, Tatke M, Saran RK, Malhotra V, Singh D* Departments of Pathology and *Neurosurgery, G. B. Pant Hospital, New Delhi, India. Correspondence
Case Report Gangliogliomas: A Report of Five Cases Nair V, Suri VS, Tatke M, Saran RK, Malhotra V, Singh D* Departments of Pathology and *Neurosurgery, G. B. Pant Hospital, New Delhi, India. Correspondence
Dysembryoplastic neuroepithelial tumor is a benign,
 J Neurosurg Pediatrics 11:518 525, 2013 AANS, 2013 Dynamic changes in magnetic resonance imaging appearance of dysembryoplastic neuroepithelial tumor with or without malignant transformation Report of
J Neurosurg Pediatrics 11:518 525, 2013 AANS, 2013 Dynamic changes in magnetic resonance imaging appearance of dysembryoplastic neuroepithelial tumor with or without malignant transformation Report of
Diagnostic implications of IDH1-R132H and OLIG2 expression patterns in rare and challenging glioblastoma variants
 & 2012 USCAP, Inc. All rights reserved 0893-3952/12 $32.00 1 Diagnostic implications of IDH1-R132H and OLIG2 expression patterns in rare and challenging glioblastoma variants Nancy M Joseph 1, Joanna Phillips
& 2012 USCAP, Inc. All rights reserved 0893-3952/12 $32.00 1 Diagnostic implications of IDH1-R132H and OLIG2 expression patterns in rare and challenging glioblastoma variants Nancy M Joseph 1, Joanna Phillips
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
Contemporary Management of Glioblastoma
 Contemporary Management of Glioblastoma Incidence Rates of Primary Brain Tumors Central Brain Tumor Registry of the United States, 1992-1997 100 Number of Cases per 100,000 Population 10 1 0.1 x I x I
Contemporary Management of Glioblastoma Incidence Rates of Primary Brain Tumors Central Brain Tumor Registry of the United States, 1992-1997 100 Number of Cases per 100,000 Population 10 1 0.1 x I x I
Pathological spectrum in recurrences of glioblastoma multiforme
 pathologica 2015;107:1-8 Original article Pathological spectrum in recurrences of glioblastoma multiforme G. MARUCCI 1, P.V. FABBRI 1, L. MORANDI 1, D. DE BIASE 2, E. DI OTO 1, G. TALLINI 2, C. STURIALE
pathologica 2015;107:1-8 Original article Pathological spectrum in recurrences of glioblastoma multiforme G. MARUCCI 1, P.V. FABBRI 1, L. MORANDI 1, D. DE BIASE 2, E. DI OTO 1, G. TALLINI 2, C. STURIALE
Neurocytoma a Rare Intraventricular Tumor
 Neurocytoma a Rare Intraventricular Tumor J. A. Mallick,S. A. Ali ( Department of Oncology, Liaquat National Postgraduate Medical Centre, Karachi. ) Introduction Central neurocytoma was first recognized
Neurocytoma a Rare Intraventricular Tumor J. A. Mallick,S. A. Ali ( Department of Oncology, Liaquat National Postgraduate Medical Centre, Karachi. ) Introduction Central neurocytoma was first recognized
Detection of IDH1 mutation in human gliomas: comparison of immunohistochemistry and sequencing
 DOI.7/s4--3-7 ORIGINAL ARTICLE Detection of IDH mutation in human gliomas: comparison of immunohistochemistry and sequencing Shingo Takano Wei Tian Masahide Matsuda Tetsuya Yamamoto Eiichi Ishikawa Mika
DOI.7/s4--3-7 ORIGINAL ARTICLE Detection of IDH mutation in human gliomas: comparison of immunohistochemistry and sequencing Shingo Takano Wei Tian Masahide Matsuda Tetsuya Yamamoto Eiichi Ishikawa Mika
Supplementary Note. Nature Genetics: doi: /ng.2928
 Supplementary Note Loss of heterozygosity analysis (LOH). We used VCFtools v0.1.11 to extract only singlenucleotide variants with minimum depth of 15X and minimum mapping quality of 20 to create a ped
Supplementary Note Loss of heterozygosity analysis (LOH). We used VCFtools v0.1.11 to extract only singlenucleotide variants with minimum depth of 15X and minimum mapping quality of 20 to create a ped
Modeling origin and natural evolution of low-grade gliomas
 Modeling origin and natural evolution of low-grade gliomas Mathilde Badoual Paris Diderot University, IMNC lab 2nd HTE workshop: Mathematical & Computer Modeling to study tumors heterogeneity in its ecosystem,
Modeling origin and natural evolution of low-grade gliomas Mathilde Badoual Paris Diderot University, IMNC lab 2nd HTE workshop: Mathematical & Computer Modeling to study tumors heterogeneity in its ecosystem,
Integrating molecular markers into the World Health Organization classification of CNS tumors: a survey of the neuro-oncology community
 Integrating molecular markers into the World Health Organization classification of CNS tumors: a survey of the neuro-oncology community The Harvard community has made this article openly available. Please
Integrating molecular markers into the World Health Organization classification of CNS tumors: a survey of the neuro-oncology community The Harvard community has made this article openly available. Please
Nature Genetics: doi: /ng.2995
 Supplementary Figure 1 Kaplan-Meier survival curves of patients with brainstem tumors. (a) Comparison of patients with PPM1D mutation versus wild-type PPM1D. (b) Comparison of patients with PPM1D mutation
Supplementary Figure 1 Kaplan-Meier survival curves of patients with brainstem tumors. (a) Comparison of patients with PPM1D mutation versus wild-type PPM1D. (b) Comparison of patients with PPM1D mutation
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Imaging for suspected glioma
 Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Assessment performed on Friday, September 18, 2015, at Vancouver General Hospital
 Assessors report for ciqc Run 49: ATRX (June 2015) Assessors: S Yip and J Won (recorder) Assessment performed on Friday, September 18, 2015, at Vancouver General Hospital Background The combined application
Assessors report for ciqc Run 49: ATRX (June 2015) Assessors: S Yip and J Won (recorder) Assessment performed on Friday, September 18, 2015, at Vancouver General Hospital Background The combined application
AD (Leave blank) TITLE: Genomic Characterization of Brain Metastasis in Non-Small Cell Lung Cancer Patients
 AD (Leave blank) Award Number: W81XWH-12-1-0444 TITLE: Genomic Characterization of Brain Metastasis in Non-Small Cell Lung Cancer Patients PRINCIPAL INVESTIGATOR: Mark A. Watson, MD PhD CONTRACTING ORGANIZATION:
AD (Leave blank) Award Number: W81XWH-12-1-0444 TITLE: Genomic Characterization of Brain Metastasis in Non-Small Cell Lung Cancer Patients PRINCIPAL INVESTIGATOR: Mark A. Watson, MD PhD CONTRACTING ORGANIZATION:
Precision medicine for gliomas
 Precision medicine for YAZMIN ODIA, MD MS LEAD PHYSICIAN OF MEDICAL NEURO-ONCOLOGY DISCLOSURES Novocure: Advisory Board for Optune in No other financial conflicts of interest Glioma OVERVIEW INFILTRATIVE,
Precision medicine for YAZMIN ODIA, MD MS LEAD PHYSICIAN OF MEDICAL NEURO-ONCOLOGY DISCLOSURES Novocure: Advisory Board for Optune in No other financial conflicts of interest Glioma OVERVIEW INFILTRATIVE,
SUPPLEMENTARY INFORMATION
 VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
Integrated genomic analysis of human osteosarcomas
 Integrated genomic analysis of human osteosarcomas Leonardo A. Meza-Zepeda Project Leader Genomic Section Department of Tumor Biology The Norwegian Radium Hospital Head Microarray Core Facility Norwegian
Integrated genomic analysis of human osteosarcomas Leonardo A. Meza-Zepeda Project Leader Genomic Section Department of Tumor Biology The Norwegian Radium Hospital Head Microarray Core Facility Norwegian
CASE OF THE WEEK PROFESSOR YASSER METWALLY
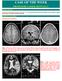 CASE OF THE WEEK PROFESSOR YASSER METWALLY CLINICAL PICTURE CLINICAL PICTURE: CLINICAL PICTURE: A 6 years old male patient presented clinically with intractable complex partial seizure. The child is mentally
CASE OF THE WEEK PROFESSOR YASSER METWALLY CLINICAL PICTURE CLINICAL PICTURE: CLINICAL PICTURE: A 6 years old male patient presented clinically with intractable complex partial seizure. The child is mentally
Histopathological Study and Categorisation of Brain Tumors
 Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
Karl Kashofer, Phd Institut für Pathologie Medizinische Universität Graz
 Expanding on WHO guideline compliant molecular testing of central nervous system tumors by low density whole genome sequencing. Karl Kashofer, Phd Institut für Pathologie Medizinische Universität Graz
Expanding on WHO guideline compliant molecular testing of central nervous system tumors by low density whole genome sequencing. Karl Kashofer, Phd Institut für Pathologie Medizinische Universität Graz
Characterizing invading glioma cells based on IDH1-R132H and Ki-67 immunofluorescence
 DOI 10.1007/s10014-013-0172-y ORIGINAL ARTICLE Characterizing invading glioma cells based on IDH1-R132H and Ki-67 immunofluorescence Hemragul Sabit Mitsutoshi Nakada Takuya Furuta Takuya Watanabe Yutaka
DOI 10.1007/s10014-013-0172-y ORIGINAL ARTICLE Characterizing invading glioma cells based on IDH1-R132H and Ki-67 immunofluorescence Hemragul Sabit Mitsutoshi Nakada Takuya Furuta Takuya Watanabe Yutaka
SALSA MLPA probemix P315-B1 EGFR
 SALSA MLPA probemix P315-B1 EGFR Lot B1-0215 and B1-0112. As compared to the previous A1 version (lot 0208), two mutation-specific probes for the EGFR mutations L858R and T709M as well as one additional
SALSA MLPA probemix P315-B1 EGFR Lot B1-0215 and B1-0112. As compared to the previous A1 version (lot 0208), two mutation-specific probes for the EGFR mutations L858R and T709M as well as one additional
UPDATES ON CHEMOTHERAPY FOR LOW GRADE GLIOMAS
 UPDATES ON CHEMOTHERAPY FOR LOW GRADE GLIOMAS Antonio M. Omuro Department of Neurology Memorial Sloan-Kettering Cancer Center II International Neuro-Oncology Congress Sao Paulo, 08/17/12 CHALLENGES IN
UPDATES ON CHEMOTHERAPY FOR LOW GRADE GLIOMAS Antonio M. Omuro Department of Neurology Memorial Sloan-Kettering Cancer Center II International Neuro-Oncology Congress Sao Paulo, 08/17/12 CHALLENGES IN
ASMS 2015 ThP 459 Glioblastoma Multiforme Subtype Classification: Integrated Analysis of Protein and Gene Expression Data
 ASMS 2015 ThP 459 Glioblastoma Multiforme Subtype Classification: Integrated Analysis of Protein and Gene Expression Data Durairaj Renu 1, Vadiraja Bhat 2, Mona Al-Gizawiy 3, Carolina B. Livi 2, Stephen
ASMS 2015 ThP 459 Glioblastoma Multiforme Subtype Classification: Integrated Analysis of Protein and Gene Expression Data Durairaj Renu 1, Vadiraja Bhat 2, Mona Al-Gizawiy 3, Carolina B. Livi 2, Stephen
Brain Tumors. Medulloblastoma. Pilocytic astrocytoma: Ahmed Koriesh, MD. Pathological finding
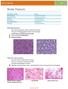 NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
2018 Diagnostic Slide Session Case #8
 2018 Diagnostic Slide Session Case #8 Angela N. Viaene, MacLean P. Nasrallah, and Zissimos Mourelatos Hospital of the University of Pennsylvania AANP June 9, 2018 Disclosures: none Clinical History Healthy,
2018 Diagnostic Slide Session Case #8 Angela N. Viaene, MacLean P. Nasrallah, and Zissimos Mourelatos Hospital of the University of Pennsylvania AANP June 9, 2018 Disclosures: none Clinical History Healthy,
LOW GRADE ASTROCYTOMAS
 LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
Epigenetic programming in chronic lymphocytic leukemia
 Epigenetic programming in chronic lymphocytic leukemia Christopher Oakes 10 th Canadian CLL Research Meeting September 18-19 th, 2014 Epigenetics and DNA methylation programming in normal and tumor cells:
Epigenetic programming in chronic lymphocytic leukemia Christopher Oakes 10 th Canadian CLL Research Meeting September 18-19 th, 2014 Epigenetics and DNA methylation programming in normal and tumor cells:
The recently updated World Health Organization (WHO)
 REVIEW ARTICLE The Expanding Family of Glioneuronal Tumors Daniela S. Allende, MD and Richard A. Prayson, MD Abstract: Three new entities have been recently added to the group of glioneuronal tumors in
REVIEW ARTICLE The Expanding Family of Glioneuronal Tumors Daniela S. Allende, MD and Richard A. Prayson, MD Abstract: Three new entities have been recently added to the group of glioneuronal tumors in
FOLLICULAR LYMPHOMA- ILLUMINA METHYLATION. Jude Fitzgibbon
 FOLLICULAR LYMPHOMA- ILLUMINA METHYLATION Jude Fitzgibbon j.fitzgibbon@qmul.ac.uk Molecular Predictors of Clinical outcome Responders Alive Non-responders Dead TUMOUR GENETICS Targeted therapy, Prognostic
FOLLICULAR LYMPHOMA- ILLUMINA METHYLATION Jude Fitzgibbon j.fitzgibbon@qmul.ac.uk Molecular Predictors of Clinical outcome Responders Alive Non-responders Dead TUMOUR GENETICS Targeted therapy, Prognostic
Detection of Anaplastic Lymphoma Kinase (ALK) gene in Non-Small Cell lung Cancer (NSCLC) By CISH Technique
 Cancer and Clinical Oncology; Vol. 7, No. 1; 2018 ISSN 1927-4858 E-ISSN 1927-4866 Published by Canadian Center of Science and Education Detection of Anaplastic Lymphoma Kinase (ALK) gene in Non-Small Cell
Cancer and Clinical Oncology; Vol. 7, No. 1; 2018 ISSN 1927-4858 E-ISSN 1927-4866 Published by Canadian Center of Science and Education Detection of Anaplastic Lymphoma Kinase (ALK) gene in Non-Small Cell
Asma Bashir, MD, 1 Jannick Brennum, MD, DMSc, 2 Helle Broholm, MD, 3 and Ian Law, MD, PhD, DMSc 1
 CLINICAL ARTICLE The diagnostic accuracy of detecting malignant transformation of low-grade glioma using O-(2-[ 18 F]fluoroethyl)-l-tyrosine positron emission tomography: a retrospective study Asma Bashir,
CLINICAL ARTICLE The diagnostic accuracy of detecting malignant transformation of low-grade glioma using O-(2-[ 18 F]fluoroethyl)-l-tyrosine positron emission tomography: a retrospective study Asma Bashir,
Prognostic or predictive value of MGMT promoter methylation in gliomas depends on IDH1 mutation
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2013 Prognostic or predictive value of MGMT promoter methylation in gliomas
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2013 Prognostic or predictive value of MGMT promoter methylation in gliomas
Pathologic features and clinical outcome of central neurocytoma: analysis of 15 cases
 Original Article Pathologic features and clinical outcome of central neurocytoma: analysis of 15 cases Yu Li, Xiu-Feng Ye, Guo Qian, Yu Yin, Qian-Guan Pan Institute of Neuroscience, Department of Pathology,
Original Article Pathologic features and clinical outcome of central neurocytoma: analysis of 15 cases Yu Li, Xiu-Feng Ye, Guo Qian, Yu Yin, Qian-Guan Pan Institute of Neuroscience, Department of Pathology,
Accepted: 13 June 2018
 Received: 26 February 2018 Revised: 12 June 2018 DOI: 10.1002/cam4.1666 Accepted: 13 June 2018 ORIGINAL RESEARCH The TERT promoter mutation status and MGMT promoter methylation status, combined with dichotomized
Received: 26 February 2018 Revised: 12 June 2018 DOI: 10.1002/cam4.1666 Accepted: 13 June 2018 ORIGINAL RESEARCH The TERT promoter mutation status and MGMT promoter methylation status, combined with dichotomized
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Expert-guided Visual Exploration (EVE) for patient stratification. Hamid Bolouri, Lue-Ping Zhao, Eric C. Holland
 Expert-guided Visual Exploration (EVE) for patient stratification Hamid Bolouri, Lue-Ping Zhao, Eric C. Holland Oncoscape.sttrcancer.org Paul Lisa Ken Jenny Desert Eric The challenge Given - patient clinical
Expert-guided Visual Exploration (EVE) for patient stratification Hamid Bolouri, Lue-Ping Zhao, Eric C. Holland Oncoscape.sttrcancer.org Paul Lisa Ken Jenny Desert Eric The challenge Given - patient clinical
Data Mining for Research and Diagnostics
 UCL DEPARTMENT OF GEOGRAPHY UCL INSTITUTE OF NEUROLOGY Data Mining for Research and Diagnostics Sebastian Brandner, UCL Institute of Neurology, London Data mining for Research and Diagnostics Our setup
UCL DEPARTMENT OF GEOGRAPHY UCL INSTITUTE OF NEUROLOGY Data Mining for Research and Diagnostics Sebastian Brandner, UCL Institute of Neurology, London Data mining for Research and Diagnostics Our setup
Characterization and significance of MUC1 and c-myc expression in elderly patients with papillary thyroid carcinoma
 Characterization and significance of MUC1 and c-myc expression in elderly patients with papillary thyroid carcinoma Y.-J. Hu 1, X.-Y. Luo 2, Y. Yang 3, C.-Y. Chen 1, Z.-Y. Zhang 4 and X. Guo 1 1 Department
Characterization and significance of MUC1 and c-myc expression in elderly patients with papillary thyroid carcinoma Y.-J. Hu 1, X.-Y. Luo 2, Y. Yang 3, C.-Y. Chen 1, Z.-Y. Zhang 4 and X. Guo 1 1 Department
Systemic Treatment. Third International Neuro-Oncology Course. 23 May 2014
 Low-Grade Astrocytoma of the CNS: Systemic Treatment Third International Neuro-Oncology Course São Paulo, Brazil 23 May 2014 John de Groot, MD Associate Professor, Neuro-Oncology UT MD Anderson Cancer
Low-Grade Astrocytoma of the CNS: Systemic Treatment Third International Neuro-Oncology Course São Paulo, Brazil 23 May 2014 John de Groot, MD Associate Professor, Neuro-Oncology UT MD Anderson Cancer
Epidemiology and Semiology of Tumor-based Epilepsy December 2, 2012
 Epidemiology and Semiology of Tumor-based Epilepsy December 2, 2012 Charles J. Vecht, MD, PhD Medical Center The Hague SEIN Epilepsy Foundation, The Netherlands CHU Pitié-Salpêtrière, Paris, France American
Epidemiology and Semiology of Tumor-based Epilepsy December 2, 2012 Charles J. Vecht, MD, PhD Medical Center The Hague SEIN Epilepsy Foundation, The Netherlands CHU Pitié-Salpêtrière, Paris, France American
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Rapid recurrence of a malignant meningioma: case report
 Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Molecular diagnostics of gliomas: state of the art
 Acta Neuropathol (2010) 120:567 584 DOI 10.1007/s00401-010-0736-4 REVIEW Molecular diagnostics of gliomas: state of the art Markus J. Riemenschneider Judith W. M. Jeuken Pieter Wesseling Guido Reifenberger
Acta Neuropathol (2010) 120:567 584 DOI 10.1007/s00401-010-0736-4 REVIEW Molecular diagnostics of gliomas: state of the art Markus J. Riemenschneider Judith W. M. Jeuken Pieter Wesseling Guido Reifenberger
BAH1 - Primary Glioblastoma
 BAH1 - Primary Glioblastoma R frontal tumour for frozen section. No known primary. Contrast enhancing lesion. Cholecystectomy. FROZEN SECTION REPORT Right frontal tumour: The specimen consists of multiple
BAH1 - Primary Glioblastoma R frontal tumour for frozen section. No known primary. Contrast enhancing lesion. Cholecystectomy. FROZEN SECTION REPORT Right frontal tumour: The specimen consists of multiple
