PATHOLOGY, EPIDEMIOLOGY. EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (1)
|
|
|
- Bertram Palmer
- 5 years ago
- Views:
Transcription
1 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (1) Extradural Spinal Tumors, Vertebral Tumors Last updated: September 5, 2017 PATHOLOGY, EPIDEMIOLOGY... 1 Metastases... 1 Primary Vertebral Tumors... 2 CLINICAL FEATURES... 2 DIAGNOSIS... 2 Serum... 2 Imaging... 2 Biopsy... 3 DIFFERENTIAL DIAGNOSIS... 4 TREATMENT... 4 Metastases, malignant tumors... 5 Benign tumors... 5 SEPARATION SURGERY... 5 PROGNOSIS... 5 SPECIFIC TUMOR TYPES... 5 Lymphoma... 6 Enostosis... 6 Osteoid osteoma... 6 Osteoblastoma... 6 Osteosarcoma (osteogenic sarcoma)... 6 Giant cell tumor (osteoclastoma)... 7 Osteochondroma (solitary osteocartilaginous exostosis)... 8 Chondrosarcoma... 9 Aneurysmal bone cyst... 9 Ewing sarcoma Multiple myeloma Solitary plasmacytoma Eosinophilic granuloma Hemangioma Angiolipoma TUMORS OF SKULL see p. Onc40 >> GENERAL FEATURES OF BONE, CARTILAGE, SOFT TISSUE TUMORS see p >> PATHOLOGY, EPIDEMIOLOGY usually involve only few spinal segments. occasionally, tumor extends through intervertebral foramina, lying partially within and partially outside of spinal canal ( dumbbell or hourglass tumor). epidural mass lesion can produce damage to spinal cord: a) mechanical distortion demyelination, axonal destruction. b) vascular compromise venous congestion and vasogenic edema ischemia, myelin loss. vast majority of metastases affecting spinal cord expand from vertebral body or paravertebral tissues into epidural space. METASTASES PATHOLOGY see p (9) >> 85% cases of epidural spinal cord compression arise from vertebral metastases! 10-15% - from tumors* spreading through intervertebral foramina. *typically lymphoma or renal cell cancers spine is 3 rd most common site for metastasis (after lung and liver): a) 94-98% - epidural and/or vertebrae isolated epidural involvement is particularly common in lymphoma and renal cell carcinoma. b) 5-6% - intradural extramedullary c) 0.5-1% - intramedullary 90% of all cancer patients have spinal metastasis at time of death (only 5-30% of these patients are symptomatic)! why metastases favor vertebrae: large volume of blood that slowly courses through bidirectional venous channels (Batson plexus) in epidural space. rich concentration of growth factors in bone marrow. most common tumors with predilection to metastasize to vertebrae: 1) prostate 2) breast 3) lung 4) renal cell 5) gastric primary sources for spinal metastases: 1) lung 15-31% 2) breast 22-24% 3) GI tract 9% 4) prostate 8-10% 5) lymphoma 6-10% 6) multiple myeloma 7) melanoma 4% 8) unknown 2% 9) kidney 1% 10) others 13% spread from primary tumors: a) arterial route b) retrograde spread through Batson plexus (during Valsalva maneuver) c) direct invasion through intervertebral foramina vertebral body is often involved first in metastasis; posterior elements are affected only one-fifth to one-seventh as often as vertebral bodies. 70% symptomatic lesions are found in thoracic region (small diameter of canal); 20% - lumbosacral, 10% - cervical. exceptions - prostate and ovarian cancers - metastases favor sacral and lumbar vertebrae (spread through Batson's plexus) > 50% cases have several levels of involvement (in 10-38% sites are noncontiguous).
2 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (2) PRIMARY VERTEBRAL TUMORS (3-25 times less common than metastatic tumors!) 1. BONE producing tumors 1) OSTEOID OSTEOMA 2) OSTEOBLASTOMA 3) OSTEOSARCOMA (OSTEOGENIC SARCOMA) about specific tumor features see below 2. CARTILAGE producing tumors 1) OSTEOCHONDROMA. 2) CHONDROSARCOMA. 3. LYMPHOPROLIFERATIVE tumors most common primary vertebral tumors! 1) MULTIPLE MYELOMA, PLASMACYTOMA 2) LYMPHOMA 4. Tumor of NOTOCHORDAL origin CHORDOMA. see p. Onc42 >> 5. Round cell tumor - EWING SARCOMA. - in course of hours, days or weeks: CLINICAL FEATURES 1. Most frequent initial symptom - gradually worsening constant focal back pain, unresponsive to rest (and may actually be most severe when recumbent at night* forcing some patients to sleep in sitting position); exacerbated by Valsalva maneuver; percussion tenderness; movement such as turning over in bed or rising from lying position may be painful; later radicular pain may develop; *vs. degenerative joint disease pain may improve with recumbent position N.B. neoplastic disease often presents with back pain indistinguishable from benign causes! 1) bone pain - bony destruction (stretching of periosteum), pathologic fractures (vertebral collapse mechanical instability). 2) neuropathic pain (root / meningeal irritation). 2. Neurologic complications - MYELOPATHY & RADICULOPATHY - Extramedullary Cord / Root Compression. see p. Spin1 >> pain typically precedes signs of cord compression by weeks months, but once cord compression occurs, it is always rapidly progressive (paraplegia may develop in hours or even minutes). RADICULOPATHY may appear before MYELOPATHY. 3. Constitutional symptoms (in malignant disease), hypercalcemia (polyuria, pre-renal failure). SERUM DIAGNOSIS ESR, anemia hypercalcemia, alkaline phosphatase - neoplastic bone processes. serum (or urine) electrophoresis - multiple myeloma, plasmacytoma. Best predictors of spinal level of abnormality: 1) focal pain 2) percussive tenderness 3) nerve root signs 4) LMN signs. IMAGING Plain X-ray of entire spine - what tumor is doing to bone and what bone is doing to tumor. N.B. 50% of vertebral cancellous bone mass needs to be destroyed before it becomes evident on plain X-rays! osteoblastic (osteosclerotic) changes: 1) prostate cancer 2) Hodgkin disease 3) osteomas 4) sarcomas 5) occasionally - breast cancer, lymphoma, hemangioma signs - pedicular erosion (enlarged intervertebral foramen), paraspinal soft tissue shadow, vertebral collapse, kyphoscoliosis. owl-eye erosion of pedicles in AP view of lumbar spine ( missing pedicle) - characteristic of metastatic disease! intervertebral space is usually not involved by tumors (if disk space is obliterated, infection is more likely). epidural disease cannot be confirmed or excluded by plain X-ray! Vertebral body collapse is highly specific indicator of epidural disease! epidural disease is found in 87% cases with > 50% collapse of vertebra, 31% cases with pedicle erosion without major vertebral collapse, 7% cases with tumor limited to vertebral body without collapse MRI of entire spine (sensitivity > 95%): on emergency basis if cord compression is present; radiculopathy without myelopathy - safe to defer imaging for h. vertebral metastases are T1 hypointense (relative to normal bone marrow); gadolinium contrast enhancement "normalizes" tumor appearance by increasing its intensity to that of normal bone marrow. contrast-enhanced fat-suppressed T1-MRI and especially STIR-sequence provide exquisite sensitivity for pathology within vertebral bodies. in contrast to infection, vertebral metastases do not cross disk space! CT delineates primary bone tumors better than MRI or plain X-ray. Myelography tumor displaces cord with narrowing of both ipsilateral and contralateral subarachnoid spaces. (vs. INTRADURAL EXTRAMEDULLARY tumor cord displacement with widening ipsilateral subarachnoid space while narrowing contralateral space). contrast outlines gentle curve around lesion. push technique may be necessary to overcome partial blocks. acute postmyelography decompensation may occur with compressive lesions emergency decompressive laminectomy. emergency myelography is still used if MRI is not available. Bone scans (technetium-99m) are positive in 60% vertebral METASTASES but are not specific. Spinal preoperative angiography: 1) localizing artery of Adamkiewicz
3 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (3) 2) delineation & embolization of vascular tumors (e.g. METASTATIC renal cell carcinoma, HEMANGIOMA, HEMANGIOBLASTOMA, ANEURYSMAL BONE CYST) BIOPSY (open or percutaneous image-guided) - ultimate way to make diagnosis (unnecessary in patients with known preexisting cancer). biopsy tract should be placed in line with future incision site (can be excised with specimen en bloc). biopsy should not be performed when suspected tumor is CHORDOMA (or other aggressive primary spine tumor that spreads via direct extension). meticulous hemostasis (blood can dissect soft tissue planes and contaminate adjacent compartments); drain must be placed to prevent hematoma (drain should exit skin in line with incision). N.B. CSF removal (lumbar puncture) in presence of spinal tumor may worsen cord compression! Thoracic vertebral metastasis (T1-MRI): normally bright signal of fatty marrow completely replaced by tumor of intermediate signal intensity; tumor extension into spinal canal with compression of spinal cord. Metastases of renal carcinoma: A. T1-MRI - multiple levels of spinal involvement; L 2 vertebra (arrow) is collapsed with epidural extension. B. CT - degree of bone destruction at L 2 level; note retropulsion of bone fragments into epidural space (arrow): Liposarcoma metastatic to L4 and L5: A. T1-MRI low-signal-intensity marrow in L4 and L5 bodies and ventral epidural soft-tissue mass of similar signal intensity at L5. B. FSE-STIR tumor is much more conspicuous; L3-L4 and L4-L5 discs are degenerated, but inversion recovery image clearly excludes disc as source of epidural soft-tissue mass; additional sacral metastases. Epidural spinal cord compression due to metastatic breast carcinoma: A (T1-MRI), B (T2-MRI) - compression fracture of T2 vertebral body with posterior displacement and compression of upper thoracic spinal cord; low-intensity bone marrow signal in A signifies replacement by tumor. C (T1-MRI through T2 vertebral body) - soft tissue mass (arrow) extending posteriorly and laterally from vertebral body into epidural space. Metastases from prostate cancer (radioisotope bone scan) - increased radiotracer uptake throughout skeleton, particularly in cervical spine: Multiple areas of increased uptake (darker foci):
4 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (4) Extradural lymphoma (CT myelogram): anterior and rightward displacement of cord and contrast-enhanced cerebrospinal fluid space (arrowhead) caused by posterolateral epidural soft-tissue mass (arrow): Metastatic breast carcinoma (MRI) - three contiguous thoracic vertebral segments with vertebral marrow replacement, compression fracture, spinal angulation, and epidural spinal cord compression: DIFFERENTIAL DIAGNOSIS 1. Herniated disc material or degenerative spinal stenosis - most common cause of epidural mass! 2. Epidural abscess / hematoma 3. Epidural lipomatosis TREATMENT Spinal cord compression is emergency! (therapy will not reverse fixed paralysis of > 48 h duration) 1. Steroids (DEXAMETHASONE mg IV 4-24 mg q6h or METHYLPREDNISOLONE in Bracken protocol) - give immediately prior to imaging study if clinical suspicion is strong (may help to preserve spinal cord function!) steroid is continued until radiotherapy is completed. 2. Emergency radiotherapy (combined with high-dose steroids): 30 Gy in 10 fractions. immediate salutary effect of radiotherapy may be seen in h, at best. 3. If effective chemotherapeutic agents are available, they should be used with radiotherapy. 4. Indications for surgical decompression: 1) cord compression worsens despite radiotherapy 2) maximum tolerated dose of radiotherapy has been delivered previously to site 3) bony compression (e.g. vertebral fracture) contributes to cord compression. approach must be tailored to anatomical site of compression within spinal canal (e.g. indiscriminate use of laminectomy in all patients frequent surgical failures; anterior approach is now used for many cases of vertebral body lesions). see p. Op220 >>
5 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (5) METASTASES, MALIGNANT TUMORS No treatment increases life expectancy in spinal metastasis! 1. Bone pain control: 1) NSAIDs 2) steroids (DEXAMETHASONE 10 mg loading dose 4 mg q6h). 3) spinal orthotics and physiotherapy 4) irradiation (for bone pain due to stretching of periosteum). 2. Neuropathic pain control: antiepileptics (e.g. GABAPENTIN), tricyclic antidepressants, lidocaine patch, opioid analgesics. neurosurgical ablations (rhizotomy, spinothalamic tractotomy, cordotomy) are not commonly used in spinal metastases. 3. Hypercalcemia: rehydration, steroid, bisphosphonate (inhibits osteoclast function). 4. Control of local disease: a) radiotherapy (procedure of choice in most patients!) improves neurologic function, pain. 30 Gy in daily fractions. traditional treatment plan is to include 2 vertebral bodies above and 2 below lesion. b) early radical* surgical resection (spondylectomy) stereotactic radiotherapy. *goal is always palliative (rather than curative) - pain relief, improved mobility indications for surgery: 1) single lesion 2) radiotherapy-resistant tumor (e.g. melanoma) 3) spinal instability 4) spinal compression (with bone or disk fragments) 5) progressive neurologic deterioration 6) previous radiation exposure 7) uncertain diagnosis (that requires tissue diagnosis) 8) life expectancy > 6 months. tumor in posterior epidural space or posterior bony elements is best treated by posterior decompression (laminectomy); laminectomy is not good solution for anteriorly based lesions (posterior decompression may further destabilize spine). anterior approaches: 1) cervicomedullary junction - transoral or transcervical retro-parapharyngeal approach 2) lower in neck - anterolateral cervical approach. 3) thoracic - thoracotomy 4) abdominal - retroperitoneal approach. for some vascularized tumors may need embolize preoperatively to decrease intraoperative blood loss (usually liters of blood loss). anterior stabilization is achieved with polymethylmethacrylate (PMMA) or hardware. at least part of, if not entire, vertebral body must be removed to approach spinal canal. modern minimally invasive approaches - endoscopy-assisted spinal-cord decompression, percutaneous vertebroplasty / kyphoplasty, minimally invasive imageguided tumoral resection and spinal reconstruction, percutaneous approach to place pedicle screws. BENIGN TUMORS surgery. steroids in perioperative period. see p. Onc50 >> SEPARATION SURGERY (SS) - moving cord away from SRS target. posterior approach just to decompress cord. SRS is done 2-3 weeks after SS. PROGNOSIS Pretreatment neurological status is one of most important prognostic factor affecting outcome (importance of early diagnosis!!!) rapidly progressing deficits carry worse prognosis (than slowly evolving ones). loss of bowel / bladder function is usually irreversible. Median survival: spinal metastatic disease - 10 months SPECIFIC TUMOR TYPES about analogous tumors in SKULL see p. Onc40 >>
6 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (6) LYMPHOMA tends to spread in epidural space, through foramina (but not destroying the bone) biopsy only ENOSTOSIS mass of proliferating bone tissue within bone (i.e. calcified medullary defects of lamellar compact bone with haversian systems found within cancellous portion of bone). one of most common spine lesions (found in 14% autopsies). most frequent in thoracic and lumbar spine. remain stable (some may slowly increase in size). discovered incidentally: X-ray circular or oblong osteoblastic lesions with spiculated margin; abrupt transition from normal to sclerotic bone. bone scan normal (vs. osteoblastic metastases!). MRI low signal intensity with normal surrounding intensity. if exhibits diameter increase > 25% in 6 months biopsy. OSTEOID OSTEOMA histologically identical to OSTEOBLASTOMA* - microscopic well-organized trabecular bone with vascular fibrous connective tissue stroma surrounded by reactive cortical bone. *but behaviorally very different osteoid osteoma is locally self-limited. diameter < 1.5 cm (vs. OSTEOBLASTOMA - typically > 2.0 cm). only 10% of body osteoid osteomas involve axial skeleton. 59% spinal osteoid osteomas are found in lumbar region. 75% occur in posterior elements (pedicles, facets, laminae), 18% - in transverse and spinous processes, 7% - in vertebral body. present in children years. actively symptomatic - painful scoliosis (60%), radicular pain, muscular atrophy. N.B. nocturnal pain is classically relieved with NSAIDs or salicylates! X-ray - round or oval radiolucent nidus, with surrounding rim of sclerotic bone (classic area of central calcification may be obscured by complex spinal architecture). bone scan - marked increased uptake by nidus (central lucent nidus is "cold" and sclerotic rim "hot") - allows confirmation of complete removal intraoperatively (with radioactive counter). CT (criterion standard for radiographic diagnosis) - well-defined low attenuation nidus with or without central calcification surrounded by area of sclerosis. MRI - vividly enhanced nidus. treatment complete nidus resection (open surgery or percutaneous CT-guided resection or percutaneous radiofrequency ablation); scoliosis resolves spontaneously with time. CT of thoracic vertebra: OSTEOBLASTOMA histologically similar (but not so well organized) as OSTEOID OSTEOMA* - expansile lesion with interconnecting trabecular bone and fibrovascular stroma, multiple small calcifications and peripheral scalloped and sclerotic rim. *but behaviorally very different osteoblastoma is locally aggressive (bone destruction, infiltration of surrounding tissue) Histology at low and high magnification: 10-15% have ANEURYSMAL BONE CYST component. can attain considerable size, typically > cm. (vs. OSTEOID OSTEOMA). 35% of all body osteoblastomas occur in spine. equal distribution throughout spinal column. 55% cases involve posterior spinal elements; 42% - vertebral bodies. 2-3 rd decade of life (i.e. peak incidence below 30 years). 2:1 male-to-female predominance. dull aching pains (neither nocturnal nor relieved by aspirin), local scoliosis, spinal stiffness; if tumor is large enough encroaching on spinal cord! X-ray: central radiolucent area surrounded by sclerotic rim. CT - areas of mineralization, expansile bone remodeling, and sclerosis or thin osseous shell at its margins. MRI (nonspecific enhancement). bone scan - marked radionucleotide uptake. treatment of choice - wide local resection with spine stabilization; both anterior and posterior procedures may be required for total removal. not radiosensitive + irradiation may cause malignant transformation % recurrence rate. Osteoblastoma in posterior elements of C3 and C4 (X-ray, MRI): OSTEOSARCOMA (OSTEOGENIC SARCOMA)
7 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (7) commonly associated with Paget's disease, previous irradiation. blastic malignant spindle cell lesion which produces osteoid % of all body osteosarcomas occur in spine (50% represent metastases); most common in lumbosacral segments. eccentric involvement of vertebral body with extension into posterior elements is common. median age of presentation - 40 years; slight male predominance. pain and palpable mass; neurologic symptoms are found in 70-80% patients. X-ray - densely mineralized matrix ( ivory vertebrae ); loss of vertebral height with sparing of adjacent disc. MRI if large amount of mineralized matrix is present, lesion may appear with low signal intensity on all sequences. treatment: surgical resection is rule (in spine often incomplete) adjuvant chemotherapy and radiotherapy. deaths usually within first year of diagnosis. Chondroblastic osteosarcoma T2 MRI (20 yo M patient underwent thoracic laminectomy; resistant to chemotherapy; eventually developed paraplegia not operative candidate): Source of pictures: Viktoras Palys, MD >> GIANT CELL TUMOR (OSTEOCLASTOMA) benign highly vascular (5% malignant - related to previous irradiation), but locally aggressive. multinucleated giant cells with fibrous stroma consisting of mononuclear cells; no active matrix production. 7% of all GCTs in body (spine is 4 th most common site). most occur in sacrum, thoracic spine. occur in 3-5 th decades of life; more common in women. can dramatically increase during pregnancy (hormonal influences). pain with neurologic impingement. X-ray - large osteolytic expansile lesions soap bubbles (in sacrum - destruction of sacral foraminal lines, can extend past sacroiliac joints bilaterally). bone scan - diffuse radionucleotide uptake with areas of central photopenia and increased peripheral uptake. angiography - hypervascular lesions. CT - soft tissue attenuation with well-defined margins and thin rim of sclerotic bone. MRI - heterogeneous low-to-intermediate signal intensity (on both T1 and T2). treatment: (arterial embolization +) complete resection (better en bloc); radiation reserved for surgically inaccessible tumors. recurrence rates 40-60%.
8 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (8) Contrast T1-MRI - C2 is replaced by tumor and large extraosseous mass is compressing spinal cord: OSTEOCHONDROMA (SOLITARY OSTEOCARTILAGINOUS EXOSTOSIS) etiology - trapping of physeal cartilage outside growth plate during skeletal development. 7-9% patients with multiple hereditary exostoses (MHE) have multiple spinal lesions. pathology - benign lesion pedicle of normal bone (protruding from cortex) with proliferating cartilaginous cap (bone is normal, but abnormal growth occurs at and as result of cartilage cap; continuity of lesion with marrow and cortex of underlying bone is present); may be sessile or pedunculated; typically do not increase in size after skeletal maturity occurs (growth after skeletal maturity, especially when accompanied by pain and bony destruction on imaging should prompt concern for malignant transformation). 4% of all solitary spine tumors. more common in cervical spine (esp. C2). posterior elements usually are involved. typically in males < 30 years (younger in MHE). neurologic deficits are more frequent in MHE (77% vs. 34%). X-ray (normal in 15%) - round bony exostosis with radiolucent cartilaginous cap protruding posteriorly from spinous process. CT - study of choice: calcified mass, often attached to a bony surface via a bony pedicle; typically no bony destruction unless malignant transformation has occurred (a rare finding). T1-MRI - central area of high signal intensity represents marrow (intermediate intensity on T2); cortex of exostosis - low signal intensity; hyaline cartilage cap - low signal intensity (high intensity on T2); post-contrast enhancement usually spares the cartilaginous cap; if cartilage cap is > 2 cm - suspect malignant transformation to CHONDROSARCOMA (very rarely, OSTEOSARCOMA). treatment: complete surgical resection without radiation is curative.
9 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (9) CHONDROSARCOMA malignant (but low-grade) cartilage producing tumors (round cellular stroma in chondroid matrix). lungs are most frequent sites of metastasis. Histology at 40 times magnification: second most common nonlymphoproliferative tumor of spine (7-12% of all spine tumors); spine is primary site in 3-12% of all body chondrosarcomas. thoracic spine is most common site. typically involve vertebral bodies. 35% tumors involve adjacent vertebral levels (by extension through disc). men : women = 2-4 : 1. mean age of presentation - 45 years. pain is frequent and constant finding. X-ray - bone destruction; mineralization in soft tissue component of lesion; characteristic chondroid matrix in form of rings and arcs (70%). tumors that arise from malignant transformation of osteochondromas are observed as thickening of cartilaginous cap. bone scan - intense heterogeneous uptake. angiography - very vascular tumor. treatment: surgical resection (vertebral corpectomy and strut bone grafting sometimes may be necessary for complete excision). adjunctive radiotherapy is controversial. if wide marginal resection cannot be achieved tumor recurrence and death in 74% cases. mean survival years. X-ray, CT, MRI of same patient: Recurrent chondrosarcoma of C4 (A - T1; B - T2-MRI): large mixed signal mass invading spinal canal; previous laminectomy: ANEURYSMAL BONE CYST etiology: Primary ABC (65-95%) - result from micro-trauma to bone with local circulatory disturbance. Secondary ABC - result from underlying neoplasms (giant cell tumors, osteoblastomas, chondroblastomas, osteosarcomas) - neoplasms produce venous obstruction and possible arteriovenous malformations and set stage for ABC formation. macro - expansile (locally aggressive) area of bone remodeling, septations within mass, thin outer periosteal rim of bone. micro - multiloculated blood-filled cystic spaces not lined by endothelium (i.e. not vascular channels):
10 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (10) may extend into adjacent vertebrae, discs, ribs, and paravertebral soft tissues. typically affect young patients (80% < 20 years) % of all body ABCs occur in spine; thoracic and lumbar spine are affected most commonly. predilection for posterior elements; 75% extend into vertebral body. painful scoliosis; 60% cause neurologic deficits. X-ray - honeycomb trabeculated pattern with eggshell-thin cortical margin. bone scan - peripheral uptake with central "cold area" ( doughnut sign). angiography - hypervascular mass (multiple vascular "lakes"). CT / MRI - cystic lesion with internal septations and lakes containing fluid levels (visualized on MRI); enhancement of periosteal rim and septations but not cystic spaces. Picture source: VCU treatment - embolization + radiation (or postoperative) complete resection. recurrence rate 20-30%. EWING SARCOMA etiology - 11;12 chromosomal translocation. malignant round cell tumor (large sheet of homogenous small, round, blue cells divided by septa; abundant collagen); areas of osteonecrosis are found. most common nonlymphoproliferative primary malignant tumor of spine in children. 3-10% of all body Ewing sarcomas occur in spine (most commonly metastatic foci than primary lesions). most commonly sacrococcygeal region. centered primarily in vertebral body. patients years. X-ray - permeative bone lysis, osseous expansion; diffuse sclerosis (69%) is associated with osteonecrosis. treatment - radiation & chemotherapy - almost 100% local control with 86% long-term survival rate (but sacral tumors have 62% local control and only 25% long-term survival rate - because of tendency for delayed clinical presentation and larger tumor size). MULTIPLE MYELOMA systemic disease with areas of local bone destruction (diffuse multifocal involvement of hematopoietic bone marrow). malignant plasma cells produce abnormal quantities of immunoglobulins. most common primary malignancy of spine! compared with metastases, posterior elements are involved less frequently. peak incidence in 6-8 th decade. blood - total protein with albumin, hypercalcemia, ESR ; Bence Jones monoclonal antibody protein in urine. serum / urine protein electrophoresis. bone scan in 33% cases, uptake may be decreased ("cold" spots); skeletal survey with plain X- rays is more helpful* for detecting occult lesions multiple round, "punched-out" or "moth-eaten" appearances (osteolysis) with pathological fractures. *MRI is even more sensitive! treatment - radiation to affected spine & chemotherapy; surgery for spine stabilization may be necessary ( adjuvant radiotherapy once healing of surgical site has been obtained). 5-yr survival - 30%. SOLITARY PLASMACYTOMA solitary lesion that usually affects vertebral body.
11 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (11) self-limited, but 10-20% dedifferentiate into MULTIPLE MYELOMA (monitor for 20 years following original diagnosis). patients younger than in MULTIPLE MYELOMA. X-ray - single lytic lesion. treatment: radiation and bracing (if pathologic fracture surgical vertebrectomy and stabilization adjuvant radiotherapy). 5-year survival > 60%. EOSINOPHILIC GRANULOMA one end of spectrum of systemic diseases, including Letterer-Siwe and Hand-Schiller-Christian disease. micro - bone is infiltrated and destroyed by histiocytes and eosinophils. most common benign bone tumor of children. vertebral involvement occurs in 10-15% cases. frequently in thoracic spine. peak incidence 5-10 years. acute onset of chest or back pain, focal sprain, torticollis, kyphoscoliosis, and, rarely, neurological compromise. X-ray - classic vertebra plana (symmetrically flattened and thinned vertebral body). treatment: curettage low-dose radiotherapy; multiregimen chemotherapy for systemic eosinophilic granulomas. HEMANGIOMA benign tumor of newly formed blood vessels within vertebral body and arch. most common benign bone tumor (9-13% autopsies). in 33% cases, multiple vertebra are involved. confined to vertebral bodies but can extend into neural arches. usually* do not produce symptoms - usually discovered incidentally. *pathologic vertebral fractures or epidural extension can occur - most frequently in thoracic region of teenaged girls. X-ray - coarse vertical striations or trabeculae ("corduroy cloth" impression). CT - dilated vascular spaces are easily seen (characteristic spotted appearance). MRI - bright high-intensity signals (on both T1 and T2). angiography - vascular lacunae and multiple feeding vessels (readily amenable to embolization). treatment - low-dose radiotherapy and external bracing; asymptomatic hemangiomas are left untreated. spinal cord compression vertebrectomy and spine stabilization (preoperative embolization* of tumor feeders is recommended). *percutaneously puncturing vertebral body and injecting acrylic within it (vertebroplasty). Capillary angioma of T8 involving vertebral body, transverse process and epidural space (A T2-MRI, B contrast T1- MRI): ANGIOLIPOMA - very rare congenital vascular tumor. mature lipocytes and angiomatous proliferation, with or without other mesenchymal elements (e.g. muscles, cartilage). predominantly in thoracic spine. commonly, multiple, cystic, and encapsulated; less commonly, infiltrate entire vertebral body and epidural space. X-ray - coarse trabecular pattern (as HEMANGIOMA). MRI - high-signal intensity in vertebral body, consistent with fatty infiltration. treatment: total excision (anterior vertebrectomy or posterior laminectomy). angiolipomas do not undergo malignant transformation - no role for radiotherapy. Source of picture: Frank H. Netter Clinical Symposia ; Ciba Pharmaceutical Company; Saunders >> BIBLIOGRAPHY for ch. Neuro-Oncology follow this LINK >>
12 EXTRADURAL SPINAL TUMORS, VERTEBRAL TUMORS Onc56 (12) Viktor s Notes for the Neurosurgery Resident Please visit website at
1/9/2013 EXTRAMEDULLARY TUMORS OF THE PEDIATRIC SPINE. Introduction. Classification for Extramedullary Tumors
 EXTRAMEDULLARY TUMORS OF THE PEDIATRIC SPINE Eugene Wang 1/20/12 Dent Neurologic Institute Introduction 2/3 of all intraspinal tumors of childhood are extramedullary 50% Extradural 10-15% Intradural Back
EXTRAMEDULLARY TUMORS OF THE PEDIATRIC SPINE Eugene Wang 1/20/12 Dent Neurologic Institute Introduction 2/3 of all intraspinal tumors of childhood are extramedullary 50% Extradural 10-15% Intradural Back
SRS for Spinal Tumors
 SRS for Spinal Tumors I. Introduction: This white paper will focus on spinal radiosurgery - with sections one though five (I-V) comprising a general review of spinal tumors from emedicine.com, more information
SRS for Spinal Tumors I. Introduction: This white paper will focus on spinal radiosurgery - with sections one though five (I-V) comprising a general review of spinal tumors from emedicine.com, more information
MARK D. MURPHEY MD, FACR. Physician-in-Chief, AIRP. Chief, Musculoskeletal Imaging
 ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE MARK D. MURPHEY MD, FACR Physician-in-Chief, AIRP Chief, Musculoskeletal Imaging ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE Giant cell tumor (GCT) Unicameral
ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE MARK D. MURPHEY MD, FACR Physician-in-Chief, AIRP Chief, Musculoskeletal Imaging ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE Giant cell tumor (GCT) Unicameral
Primary bone tumors > metastases from other sites Primary bone tumors widely range -from benign to malignant. Classified according to the normal cell
 Primary bone tumors > metastases from other sites Primary bone tumors widely range -from benign to malignant. Classified according to the normal cell counterpart and line of differentiation. Among the
Primary bone tumors > metastases from other sites Primary bone tumors widely range -from benign to malignant. Classified according to the normal cell counterpart and line of differentiation. Among the
Malignant bone tumors. Incidence Myeloma 45% Osteosarcoma 24% Chondrosarcoma 12% Lyphoma 8% Ewing s Sarcoma 7%
 Malignant bone tumors Incidence Myeloma 45% Osteosarcoma 24% Chondrosarcoma 12% Lyphoma 8% Ewing s Sarcoma 7% Commonest primary bone sarcoma is osteosarcoma X ray Questions to ask 1. Solitary or Multiple
Malignant bone tumors Incidence Myeloma 45% Osteosarcoma 24% Chondrosarcoma 12% Lyphoma 8% Ewing s Sarcoma 7% Commonest primary bone sarcoma is osteosarcoma X ray Questions to ask 1. Solitary or Multiple
Bone Tumors Clues and Cues
 William Herring, M.D. 2002 Bone Tumors Clues and Cues In Slide Show mode, advance the slides by pressing the spacebar All Photos Retain the Copyright of their Authors Clues by Appearance of Lesion Patterns
William Herring, M.D. 2002 Bone Tumors Clues and Cues In Slide Show mode, advance the slides by pressing the spacebar All Photos Retain the Copyright of their Authors Clues by Appearance of Lesion Patterns
Spinal Neoplasms. First Things First!! Localize the Lesion!! Ependymomas. Common Intramedullary Lesions
 Acta Radiológica Portuguesa, Vol.XXIII, nº 90, pág. 101-114, Abr.-Jun., 2011 Spinal Neoplasms Bruno A Policeni University of Iowa Hospitals and Clinics Assistant Professor of Radiology Disclosure of Commercial
Acta Radiológica Portuguesa, Vol.XXIII, nº 90, pág. 101-114, Abr.-Jun., 2011 Spinal Neoplasms Bruno A Policeni University of Iowa Hospitals and Clinics Assistant Professor of Radiology Disclosure of Commercial
Spine. Neuroradiology. Spine. Spine Pathology. Distribution of fractures. Radiological algorithm. Role of radiology 18/11/2015
 Spine Neuroradiology Spine Prof.Dr.Nail Bulakbaşı X Ray: AP/L/Oblique Vertebra & disc spaces CT & CTA Vertebra, discs, vessels MRI & MRA Vertebra, disc, vessels, meninges Spinal cord & nerves Myelography
Spine Neuroradiology Spine Prof.Dr.Nail Bulakbaşı X Ray: AP/L/Oblique Vertebra & disc spaces CT & CTA Vertebra, discs, vessels MRI & MRA Vertebra, disc, vessels, meninges Spinal cord & nerves Myelography
The Radiology Assistant : Bone tumor - ill defined osteolytic tumors and tumor-like lesions
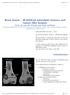 Bone tumor - ill defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
Bone tumor - ill defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
The Radiology Assistant : Bone tumor - well-defined osteolytic tumors and tumor-like lesions
 Bone tumor - well-defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
Bone tumor - well-defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Focal Sclerosis in a Vertebra: Differential Diagnosis of a Solitary Osteoblastic Metastasis
 July 2001 Focal Sclerosis in a Vertebra: Differential Diagnosis of a Solitary Osteoblastic Metastasis Alice L. Fisher, Harvard Medical School Year IV Review of the Normal Anatomy of a Lumbar Vertebra:
July 2001 Focal Sclerosis in a Vertebra: Differential Diagnosis of a Solitary Osteoblastic Metastasis Alice L. Fisher, Harvard Medical School Year IV Review of the Normal Anatomy of a Lumbar Vertebra:
Essentials of Clinical MR, 2 nd edition. 51. Primary Neoplasms
 51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
A Journey Down The Canal
 A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2
 Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2 Case 79 yo M with hx of T3N0 colon cancer diagnosed in 2008 metastatic liver disease s/p liver segmentectomy 2009
Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2 Case 79 yo M with hx of T3N0 colon cancer diagnosed in 2008 metastatic liver disease s/p liver segmentectomy 2009
ESSENTIALS OF PLAIN FILM INTERPRETATION: SPINE DR ASIF SAIFUDDIN
 ESSENTIALS OF PLAIN FILM INTERPRETATION: SPINE DR ASIF SAIFUDDIN Consultant Musculoskeletal Radiologist Royal National Orthopaedic Hospital Stanmore,UK. INTRODUCTION 2 INTRODUCTION 3 INTRODUCTION Spinal
ESSENTIALS OF PLAIN FILM INTERPRETATION: SPINE DR ASIF SAIFUDDIN Consultant Musculoskeletal Radiologist Royal National Orthopaedic Hospital Stanmore,UK. INTRODUCTION 2 INTRODUCTION 3 INTRODUCTION Spinal
MRI Findings of Giant Cell Tumors of the Spine
 MRI of Spinal Tumors Musculoskeletal Imaging Clinical Observations Jong Won Kwon 1 Hye Won Chung 1,2 Eun Yoon Cho 3 Sung Hwan Hong 4 Sang-Hee Choi 1 Young Cheol Yoon 1 Sang Kyu Yi 1 Kwon JW, Chung HW,
MRI of Spinal Tumors Musculoskeletal Imaging Clinical Observations Jong Won Kwon 1 Hye Won Chung 1,2 Eun Yoon Cho 3 Sung Hwan Hong 4 Sang-Hee Choi 1 Young Cheol Yoon 1 Sang Kyu Yi 1 Kwon JW, Chung HW,
Pediatric Spine Tumors (and other masses)
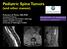 Pediatric Spine Tumors (and other masses) Francisco A Perez, MD, PhD Assistant Professor Neuroradiology and Pediatric Radiology Seattle Children s Hospital University of Washington, Seattle Commercial
Pediatric Spine Tumors (and other masses) Francisco A Perez, MD, PhD Assistant Professor Neuroradiology and Pediatric Radiology Seattle Children s Hospital University of Washington, Seattle Commercial
MRI XR, CT, NM. Principal Modality (2): Case Report # 2. Date accepted: 15 March 2013
 Radiological Category: Musculoskeletal Principal Modality (1): Principal Modality (2): MRI XR, CT, NM Case Report # 2 Submitted by: Hannah Safia Elamir, D.O. Faculty reviewer: Naga R. Chinapuvvula, M.D.
Radiological Category: Musculoskeletal Principal Modality (1): Principal Modality (2): MRI XR, CT, NM Case Report # 2 Submitted by: Hannah Safia Elamir, D.O. Faculty reviewer: Naga R. Chinapuvvula, M.D.
Benign tumors tumors K 01
 A tumor or suspected tumor diagnosis is a major setback in any person s life. Right from the start - in the initial phase of the patient s personal confrontation with the disease, possibly characterized
A tumor or suspected tumor diagnosis is a major setback in any person s life. Right from the start - in the initial phase of the patient s personal confrontation with the disease, possibly characterized
Vertebral and Paravertebral Diseases
 Department of Radiology University of California San Diego Vertebral and Paravertebral Diseases John R. Hesselink, M.D. Vertebral / Paravertebral Disease (Extradural) Metastatic disease Primary bone tumors
Department of Radiology University of California San Diego Vertebral and Paravertebral Diseases John R. Hesselink, M.D. Vertebral / Paravertebral Disease (Extradural) Metastatic disease Primary bone tumors
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION
 CLINICAL VIGNETTE 2017; 3:2 SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION Editor-in-Chief: Idowu, Olufemi E. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria.
CLINICAL VIGNETTE 2017; 3:2 SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION Editor-in-Chief: Idowu, Olufemi E. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria.
22110 vertebral segment; cervical vertebral segment; thoracic vertebral segment; lumbar
 The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
Diagnostic Imaging of Solitary Tumors of the Spine: What to Do and Say 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. EDUCATION EXHIBIT
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. EDUCATION EXHIBIT
Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine
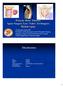 Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine Christopher Ames MD Professor of Neurosurgery and Orthopedic Surgery Director of Spine Tumor And Deformity Surgery UCSF Department
Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine Christopher Ames MD Professor of Neurosurgery and Orthopedic Surgery Director of Spine Tumor And Deformity Surgery UCSF Department
APPROPRIATE USE GUIDELINES
 APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Neck Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Updated June, 2017 Contents
APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Neck Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Updated June, 2017 Contents
Skeletal metastases are the most common variety of bone tumors and should always be considered in the differential diagnosis, particularly in older
 Dr Brajesh Nandan Skeletal metastases are the most common variety of bone tumors and should always be considered in the differential diagnosis, particularly in older patients. Cancers of the breast, prostate,
Dr Brajesh Nandan Skeletal metastases are the most common variety of bone tumors and should always be considered in the differential diagnosis, particularly in older patients. Cancers of the breast, prostate,
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Imaging Findings Of Bone Tumors: A Pictorial Review
 Imaging Findings Of Bone Tumors: A Pictorial Review Poster No.: C-2511 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Limeme, N. Benzina, A. BelKhiria, H. Zaghouani, S. Majdoub, N. Mallat, H.
Imaging Findings Of Bone Tumors: A Pictorial Review Poster No.: C-2511 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Limeme, N. Benzina, A. BelKhiria, H. Zaghouani, S. Majdoub, N. Mallat, H.
Primary Tumors of Ribs
 Primary Tumors of Ribs Frank E. Schmidt, M.D., and Max J. Trummer, Capt, MC, USN ABSTRACT An analysis of 50 consecutive patients with primary rib tumors operated on at the U.S. Naval Hospital, San Diego,
Primary Tumors of Ribs Frank E. Schmidt, M.D., and Max J. Trummer, Capt, MC, USN ABSTRACT An analysis of 50 consecutive patients with primary rib tumors operated on at the U.S. Naval Hospital, San Diego,
Bone/Osteoid Producing Lesions
 Chapter 2 Bone/Osteoid Producing Lesions Introduction There are many lesions that are associated with reactive new bone formation; this chapter predominantly covers those in which deposition of osteoid/bone
Chapter 2 Bone/Osteoid Producing Lesions Introduction There are many lesions that are associated with reactive new bone formation; this chapter predominantly covers those in which deposition of osteoid/bone
Brain Tumors. What is a brain tumor?
 Scan for mobile link. Brain Tumors A brain tumor is a collection of abnormal cells that grows in or around the brain. It poses a risk to the healthy brain by either invading or destroying normal brain
Scan for mobile link. Brain Tumors A brain tumor is a collection of abnormal cells that grows in or around the brain. It poses a risk to the healthy brain by either invading or destroying normal brain
APMA 2018 Radiology Track Bone Tumors When to say Gulp!
 APMA 2018 Radiology Track Bone Tumors When to say Gulp! DANIEL P. EVANS, DPM, FACFAOM Professor, Department of Podiatric Medicine and Radiology Dr. Wm. Scholl College of Podiatric Medicine Conflict of
APMA 2018 Radiology Track Bone Tumors When to say Gulp! DANIEL P. EVANS, DPM, FACFAOM Professor, Department of Podiatric Medicine and Radiology Dr. Wm. Scholl College of Podiatric Medicine Conflict of
1105 two (2) vertebrae... 1, add on per additional vertebra
 SPINE STAGE OPERATIONS Staged operations shall be paid at 100% for the first stage and 85% for the second stage. Where the second stage pays a higher fee 100% shall be paid and the first stage shall be
SPINE STAGE OPERATIONS Staged operations shall be paid at 100% for the first stage and 85% for the second stage. Where the second stage pays a higher fee 100% shall be paid and the first stage shall be
Managing Bone Pain in Metastatic Disease. Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018
 Managing Bone Pain in Metastatic Disease Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018 None Disclosures Managing Bone Pain in Metastatic Disease This lecture will
Managing Bone Pain in Metastatic Disease Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018 None Disclosures Managing Bone Pain in Metastatic Disease This lecture will
A Patient s Guide to Spinal Tumors
 A Patient s Guide to Spinal Tumors 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Spinal Tumors 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A PATIENT WITH TWO EPISODES OF THORACIC SPINAL CORD COMPRESSION CAUSED BY PRIMARY LYMPHOMA AND METASTATIC CARCINOMA OF THE PROSTATE, 11 YEARS APART
 A PATIENT WITH TWO EPISODES OF THORACIC SPINAL CORD COMPRESSION CAUSED BY PRIMARY LYMPHOMA AND METASTATIC CARCINOMA OF THE PROSTATE, 11 YEARS APART Shih-Huang Tai, 1 Yu-Chang Hung, 1 Jian-Chin Chen, 2
A PATIENT WITH TWO EPISODES OF THORACIC SPINAL CORD COMPRESSION CAUSED BY PRIMARY LYMPHOMA AND METASTATIC CARCINOMA OF THE PROSTATE, 11 YEARS APART Shih-Huang Tai, 1 Yu-Chang Hung, 1 Jian-Chin Chen, 2
Suspecting Tumors, or Could it be cancer?
 Suspecting Tumors, or Could it be cancer? Donna E. Reece, M.D. Princess Margaret Cancer Centre University Health Network Toronto, ON CANADA 07 February 2018 Background Low back pain is common However,
Suspecting Tumors, or Could it be cancer? Donna E. Reece, M.D. Princess Margaret Cancer Centre University Health Network Toronto, ON CANADA 07 February 2018 Background Low back pain is common However,
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
Metastatic Spinal Disease
 Metastatic Spinal Disease Mr Neil Chiverton Consultant Spinal Surgeon, Sheffield Objectives The scale and nature of the problem NICE recommendations Surgical decision making Case illustrations Incidence
Metastatic Spinal Disease Mr Neil Chiverton Consultant Spinal Surgeon, Sheffield Objectives The scale and nature of the problem NICE recommendations Surgical decision making Case illustrations Incidence
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Disclosures. Giant Cell Rich Tumors of Bone. Outline. The osteoclast. Giant cell rich tumors 5/21/11
 Disclosures Giant Cell Rich Tumors of Bone Andrew Horvai, MD, PhD Associate Clinical Professor, Pathology This lecture discusses "off label" uses of a number of pharmaceutical agents. The speaker is describing
Disclosures Giant Cell Rich Tumors of Bone Andrew Horvai, MD, PhD Associate Clinical Professor, Pathology This lecture discusses "off label" uses of a number of pharmaceutical agents. The speaker is describing
The surgical treatment of metastatic disease of the spine
 The surgical treatment of metastatic disease of the spine Péter Banczerowski National Institute of Neurosurgery, Budapest Spine tumours 15% of the primary tumours of the CNS affect the spine The spine
The surgical treatment of metastatic disease of the spine Péter Banczerowski National Institute of Neurosurgery, Budapest Spine tumours 15% of the primary tumours of the CNS affect the spine The spine
SMALL ROUND BLUE CELL LESION OF BONE
 DISCLOSURE SMALL ROUND BLUE CELL LESION OF BONE Dr. Alistair Jordan University of South Alabama No financial support or endorsement OBJECTIVES Describe the more common small round cell lesions of bone
DISCLOSURE SMALL ROUND BLUE CELL LESION OF BONE Dr. Alistair Jordan University of South Alabama No financial support or endorsement OBJECTIVES Describe the more common small round cell lesions of bone
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Bone Tumours - a synopsis. Dr Zena Slim SpR in Histopathology QAH 2009
 Bone Tumours - a synopsis Dr Zena Slim SpR in Histopathology QAH 2009 Aims General approach to diagnosis Common entities.and not so common ones. Mini quiz Challenge of bone tumour diagnosis Bone tumours
Bone Tumours - a synopsis Dr Zena Slim SpR in Histopathology QAH 2009 Aims General approach to diagnosis Common entities.and not so common ones. Mini quiz Challenge of bone tumour diagnosis Bone tumours
SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES Author : RITA GONÇALVES Categories : Vets Date : April 7, 2014 RITA
Vet Times The website for the veterinary profession https://www.vettimes.co.uk SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES Author : RITA GONÇALVES Categories : Vets Date : April 7, 2014 RITA
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
Introduction to Musculoskeletal Tumors. James C. Wittig, MD Orthopedic Oncologist Sarcoma Surgeon
 Introduction to Musculoskeletal Tumors James C. Wittig, MD Orthopedic Oncologist Sarcoma Surgeon www.tumorsurgery.org Definitions Primary Bone / Soft tissue tumors Mesenchymally derived tumors (Mesodermal)
Introduction to Musculoskeletal Tumors James C. Wittig, MD Orthopedic Oncologist Sarcoma Surgeon www.tumorsurgery.org Definitions Primary Bone / Soft tissue tumors Mesenchymally derived tumors (Mesodermal)
Review Article Chondrosarcoma of the Mobile Spine and Sacrum
 Sarcoma Volume 2011, Article ID 274281, 4 pages doi:10.1155/2011/274281 Review Article Chondrosarcoma of the Mobile Spine and Sacrum Ryan M. Stuckey and Rex A. W. Marco Department of Orthopaedics, University
Sarcoma Volume 2011, Article ID 274281, 4 pages doi:10.1155/2011/274281 Review Article Chondrosarcoma of the Mobile Spine and Sacrum Ryan M. Stuckey and Rex A. W. Marco Department of Orthopaedics, University
Epidemiology of Low back pain
 Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
The role of CT and MRI in evaluation of Osteoid Oteoma
 The role of CT and MRI in evaluation of Osteoid Oteoma Elene Iordanishvili Tbilisi Sate Medical University Instructor: Prof. Dr. Ketevan Kotetishvili Department of Physics Georgian Technical University
The role of CT and MRI in evaluation of Osteoid Oteoma Elene Iordanishvili Tbilisi Sate Medical University Instructor: Prof. Dr. Ketevan Kotetishvili Department of Physics Georgian Technical University
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Imaging of bone metastases
 Imaging of bone metastases Antoine Feydy Service de Radiologie B Hôpital Cochin APHP Université Paris Descartes antoine.feydy@aphp.fr MEXICO 2016 INTRODUCTION Diagnostic Imaging Imaging Modalities Strengths,
Imaging of bone metastases Antoine Feydy Service de Radiologie B Hôpital Cochin APHP Université Paris Descartes antoine.feydy@aphp.fr MEXICO 2016 INTRODUCTION Diagnostic Imaging Imaging Modalities Strengths,
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
The Role of Radiotherapy in Metastatic Breast Cancer. Shilpen Patel MD, FACRO Associate Professor Departments of Radiation Oncology and Global Health
 The Role of Radiotherapy in Metastatic Breast Cancer Shilpen Patel MD, FACRO Associate Professor Departments of Radiation Oncology and Global Health Indications for Palliative Pain Control Radiation Bone
The Role of Radiotherapy in Metastatic Breast Cancer Shilpen Patel MD, FACRO Associate Professor Departments of Radiation Oncology and Global Health Indications for Palliative Pain Control Radiation Bone
BACK PAIN. Disclaimer. Integrated web marketing. Multimedia Health Education
 BACK PAIN Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or a licensed healthcare
BACK PAIN Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or a licensed healthcare
Typical skeletal location and differential diagnosis of bone tumors.
 Typical skeletal location and differential diagnosis of bone tumors. Poster No.: C-2418 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Barros, L. A. Ferreira, Y. Costa, P. J. V. Coelho, F. Caseiro
Typical skeletal location and differential diagnosis of bone tumors. Poster No.: C-2418 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Barros, L. A. Ferreira, Y. Costa, P. J. V. Coelho, F. Caseiro
National Imaging Associates, Inc. Clinical guidelines
 National Imaging Associates, Inc. Clinical guidelines Original Date: September 1997 THORACIC SPINE CT Page 1 of 5 CPT Codes: 72128, 72129, 72130 Last Review Date: May 2013 Guideline Number: NIA_CG_043
National Imaging Associates, Inc. Clinical guidelines Original Date: September 1997 THORACIC SPINE CT Page 1 of 5 CPT Codes: 72128, 72129, 72130 Last Review Date: May 2013 Guideline Number: NIA_CG_043
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED
 84 COPYRIGHT 2004 BY THE JOURNAL BONE AND JOINT SURGERY, INCORPORATED Radiographic Evaluation of Pathological Bone Lesions: Current Spectrum of Disease and Approach to Diagnosis BY BENJAMIN G. DOMB, MD,
84 COPYRIGHT 2004 BY THE JOURNAL BONE AND JOINT SURGERY, INCORPORATED Radiographic Evaluation of Pathological Bone Lesions: Current Spectrum of Disease and Approach to Diagnosis BY BENJAMIN G. DOMB, MD,
Introduction to Neuroimaging spine. John J. McCormick MD
 Introduction to Neuroimaging spine John J. McCormick MD Neuroanatomy Netter drawings Radiographic Anatomy Cervical Spine Cervical Spine Oblique View Cervical Spine Dens View Thoracic Spine Lumbar Spine
Introduction to Neuroimaging spine John J. McCormick MD Neuroanatomy Netter drawings Radiographic Anatomy Cervical Spine Cervical Spine Oblique View Cervical Spine Dens View Thoracic Spine Lumbar Spine
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours. Colin Kennedy March 2015
 Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
The use of surgery in the elderly. for management of metastatic epidural spinal cord compression
 The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
Bone Metastases. Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital
 Bone Metastases Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital 1 Outline Pathophysiology Signs & Symptoms Diagnosis Treatment Spinal Cord Compression 2 General Information
Bone Metastases Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital 1 Outline Pathophysiology Signs & Symptoms Diagnosis Treatment Spinal Cord Compression 2 General Information
Revised Dec Spine MR Protocols
 Spine MR Protocols Sp 1: Cervical spine MRI without contrast Sp 2: Pre- and post-contrast cervical spine MRI Sp 3: Pre- and post-contrast cervical spine MRI (multiple sclerosis protocol) Sp 4: Thoracic
Spine MR Protocols Sp 1: Cervical spine MRI without contrast Sp 2: Pre- and post-contrast cervical spine MRI Sp 3: Pre- and post-contrast cervical spine MRI (multiple sclerosis protocol) Sp 4: Thoracic
Modern management in vertebral metastasis
 43 B. Costachescu, C.E. Popescu Modern management in vertebral metastasis Modern management in vertebral metastasis B. Costachescu, C.E. Popescu Department of Neurosurgery, Division of Spine Surgery, University
43 B. Costachescu, C.E. Popescu Modern management in vertebral metastasis Modern management in vertebral metastasis B. Costachescu, C.E. Popescu Department of Neurosurgery, Division of Spine Surgery, University
DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL
 SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT
 Nagoya J. Med. Sci. 73. 197 ~ 203, 2011 CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT NORIMITSU WAKAO 1, SHIRO IMAGAMA 1, ZENYA ITO 1, KEI ANDO 1, KENICHI HIRANO 1, RYOJI TAUCHI
Nagoya J. Med. Sci. 73. 197 ~ 203, 2011 CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT NORIMITSU WAKAO 1, SHIRO IMAGAMA 1, ZENYA ITO 1, KEI ANDO 1, KENICHI HIRANO 1, RYOJI TAUCHI
A rare case of cervical epidural extramedullary plasmacytoma presenting with monoparesis
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article A rare case of cervical epidural extramedullary plasmacytoma presenting with monoparesis Okan Turk, Ibrahim Burak Atci, Hakan Yilmaz,
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article A rare case of cervical epidural extramedullary plasmacytoma presenting with monoparesis Okan Turk, Ibrahim Burak Atci, Hakan Yilmaz,
* I have no disclosures or any
 Howard Rosenthal, M.D. Associate Professor of Orthopedic Surgery University of Kansas Sarcoma Center I have no disclosures or any conflicts related to the content of this presentation. Objectives 1. Describe
Howard Rosenthal, M.D. Associate Professor of Orthopedic Surgery University of Kansas Sarcoma Center I have no disclosures or any conflicts related to the content of this presentation. Objectives 1. Describe
Imaging of Sacral Masses: Self-Assessment Module
 1.5 CME AJR Integrative Imaging LIFELONG LEARNING FOR RADIOLOGY Imaging of Sacral Masses: Self-Assessment Module Alice S. Ha 1, Felix S. Chew ABSTRACT The educational objectives for this self-assessment
1.5 CME AJR Integrative Imaging LIFELONG LEARNING FOR RADIOLOGY Imaging of Sacral Masses: Self-Assessment Module Alice S. Ha 1, Felix S. Chew ABSTRACT The educational objectives for this self-assessment
Giant Cell Tumor of the Thoracic Spine Presenting as a Posterior Mediastinal Tumor with Benign Pulmonary Metastases: A Case Report 1
 Giant Cell Tumor of the Thoracic Spine Presenting as a Posterior Mediastinal Tumor with Benign Pulmonary Metastases: A Case Report 1 Tae Hun Kim, M.D., Byung Hak Rho, M.D. 2, Young Eun Bahn, M.D. 2, Won
Giant Cell Tumor of the Thoracic Spine Presenting as a Posterior Mediastinal Tumor with Benign Pulmonary Metastases: A Case Report 1 Tae Hun Kim, M.D., Byung Hak Rho, M.D. 2, Young Eun Bahn, M.D. 2, Won
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Bony framework of the vertebral column Structure of the vertebral column
 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D.
 J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
Giant invasive spinal schwannomas: definition and surgical management
 J Neurosurg (Spine 2) 94:210 215, 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D.,
J Neurosurg (Spine 2) 94:210 215, 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D.,
University Journal of Surgery and Surgical Specialities
 University Journal of Surgery and Surgical Specialities Volume 1 Issue 1 2015 EXTRA SKELETAL MESENCHYMAL CHONDROSARCOMA :A CASE REPORT Rajaraman R Subbiah S Navin Naushad Kilpaulk Medical College Abstract:
University Journal of Surgery and Surgical Specialities Volume 1 Issue 1 2015 EXTRA SKELETAL MESENCHYMAL CHONDROSARCOMA :A CASE REPORT Rajaraman R Subbiah S Navin Naushad Kilpaulk Medical College Abstract:
Synovial cyst of spinal facet
 Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Bone tumors. RMG: jan
 Bone tumors RMG: jan 217. @Kijohs KIZZA JOHN KIJOHS Diseases arising in bone Lipoma Fibrous cortical defects Non-ossifying fibroma Bone island Benign simple cysts Enchondroma Osteochondroma Osteoid osteoma
Bone tumors RMG: jan 217. @Kijohs KIZZA JOHN KIJOHS Diseases arising in bone Lipoma Fibrous cortical defects Non-ossifying fibroma Bone island Benign simple cysts Enchondroma Osteochondroma Osteoid osteoma
Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management
 THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
Grading of Bone Tumors
 Grading of Bone Tumors Joon Hyuk Choi, M.D. Department of Pathology College of Medicine, Yeungnam University Introduction to grading system of bone tumor used at Mayo Clinic WHO Histologic Classification
Grading of Bone Tumors Joon Hyuk Choi, M.D. Department of Pathology College of Medicine, Yeungnam University Introduction to grading system of bone tumor used at Mayo Clinic WHO Histologic Classification
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Surgery. Conus medullaris and Cauda Equina Syndromes. Anatomy. See online here
 Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Anterior Cervical Discectomy and Fusion Surgery
 Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Imaging Findings of Sacral Tumors 1
 Imaging Findings of Sacral Tumors 1 Seung Ho Kim, M.., Sung Hwan Hong, M.., Ja-Young hoi, M.., Sung Hye Koh, M.., Hye Won hung, M.., Jung-h hoi, M.., Heung Sik Kang, M.. The various pathologic conditions
Imaging Findings of Sacral Tumors 1 Seung Ho Kim, M.., Sung Hwan Hong, M.., Ja-Young hoi, M.., Sung Hye Koh, M.., Hye Won hung, M.., Jung-h hoi, M.., Heung Sik Kang, M.. The various pathologic conditions
Bubbly Lesions of Bone
 Residents Section Pattern of the Month w79 08.18.09 Eisenberg Residents Section Pattern of the Month Residents inradiology Ronald L. Eisenberg 1 Eisenberg RL Keywords: bubbly lesions, fegnomashic, skeletal
Residents Section Pattern of the Month w79 08.18.09 Eisenberg Residents Section Pattern of the Month Residents inradiology Ronald L. Eisenberg 1 Eisenberg RL Keywords: bubbly lesions, fegnomashic, skeletal
Properties of Purdue. Anatomy. Positioning AXIAL SKELETAL RADIOLOGY FOR PRIVATE PRACTITIONERS 11/30/2018
 AXIAL SKELETAL RADIOLOGY FOR PRIVATE PRACTITIONERS Anatomy Complex Text book is needed Species Contrast Positioning Painful/ non cooperative Sedation General anesthesia Species Contrast 1 Slightly oblique
AXIAL SKELETAL RADIOLOGY FOR PRIVATE PRACTITIONERS Anatomy Complex Text book is needed Species Contrast Positioning Painful/ non cooperative Sedation General anesthesia Species Contrast 1 Slightly oblique
Liver Tumors. Prof. Dr. Ahmed El - Samongy
 Liver Tumors Prof. Dr. Ahmed El - Samongy Objective 1. Identify the most important features of common benign liver tumors 2. Know the risk factors, diagnosis, and management of hepatocellular carcinoma
Liver Tumors Prof. Dr. Ahmed El - Samongy Objective 1. Identify the most important features of common benign liver tumors 2. Know the risk factors, diagnosis, and management of hepatocellular carcinoma
Common Thoraco- Lumbar Problems in the Mature Athlete
 Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Endovascular and surgical treatment of giant pelvic tumor
 Endovascular and surgical treatment of giant pelvic tumor Mitrev Z., MD FETCS; Anguseva T., MD; Milev I., MD; Zafiroski G., PhD MD Center for Cardiosurgery, Filip the II, Skopje, Macedonia Background Giant
Endovascular and surgical treatment of giant pelvic tumor Mitrev Z., MD FETCS; Anguseva T., MD; Milev I., MD; Zafiroski G., PhD MD Center for Cardiosurgery, Filip the II, Skopje, Macedonia Background Giant
Imaging of sacral tumors
 Neurosurg Focus 15 (2):Article 2, 2003, Click here to return to Table of Contents Imaging of sacral tumors BETTY JEAN MANASTER, M.D., PH.D., AND TRAVIS GRAHAM, M.D. Department of Radiology, University
Neurosurg Focus 15 (2):Article 2, 2003, Click here to return to Table of Contents Imaging of sacral tumors BETTY JEAN MANASTER, M.D., PH.D., AND TRAVIS GRAHAM, M.D. Department of Radiology, University
Imaging in breast cancer. Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since
 Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
PRIMARY STUDIES EN BLOC VERSUS DEBULKING
 PRIMARY STUDIES EN BLOC VERSUS DEBULKING I Study ID II Method III Patient characteristics IV Intervention(s) V Results primary outcome VI Results secondary and other outcome(s) VII Critical appraisal of
PRIMARY STUDIES EN BLOC VERSUS DEBULKING I Study ID II Method III Patient characteristics IV Intervention(s) V Results primary outcome VI Results secondary and other outcome(s) VII Critical appraisal of
