Atypical ganglioneurocytoma: case report and review of literature
|
|
|
- Gwenda Prudence Evans
- 5 years ago
- Views:
Transcription
1 CASE REPORT Atypical ganglioneurocytoma: case report and review of literature Javed Khader Eliyas 1, Peter Pytel 2, Rimas V. Lukas 3, Patrik Gabikian 4 1. Section of Neurosurgery, University of Chicago, Chicago, IL, USA. 2. Departments of Pathology, University of Chicago, Chicago, IL, USA. 3. Department of Neurology, University of Chicago, Chicago, IL, USA. 4. Department of Neurosurgery, Kaiser Foundation Hospital, Los Angeles, CA, USA. Correspondence: Javed Khader Eliyas. Address: University of Chicago Medical Center, Section of Neurosurgery, 5841 S. Maryland Ave, MC 3026, Chicago, IL, USA. javkhel@gmail.com Received: January 28, 2015 Accepted: May 3, 2015 Online Published: May 28, 2015 DOI: /crcp.v2n4p7 URL: Abstract Extra-ventricular neurocytoma (EVN) is a distinct neuro-pathological entity that has received increasing attention as the routine use of immunohistochemical staining has helped to distinguish it from oligodendroglioma; its more common morphologic mimic. Ganglionic differentiation in parts of the tumor is common, hence lending the name of Ganglioneurocytoma. Generally considered as low-grade tumors, recent literature highlights clinical examples with atypical pathologic features that elevate the grade of these tumors to World Health Organization (WHO) grade III and portend a worse prognosis. Biological progression to a higher tumor grade, serially over time in the same patient, has not been previously described. We report a case of low-grade ganglioneurocytoma (WHO grade II) that recurred with increased proliferation index and atypical features (WHO grade III). This case illustrates the challenges involved in precise grading of these tumors. Also exemplified is the unpredictable potential of seemingly low-grade lesions. Gross total resection and routine follow-up are essential for optimum treatment, as EVNs are associated with worse prognosis than their intra-ventricular counterparts. Key words Cerebral neurocytoma, Extraventricular neurocytoma, Ganglioneurocytoma, Atypical extraventricular neurocytoma, MIB-1 proliferation index 1 Introduction Neurocytomas are rare brain tumors classically located in the vicinity of the foramen of Monro. Since their first intra-ventricular description by Hassoun et al. in 1982, these tumors have also been reported in many extraventricular and extra-axial sites [1]. EVNs may comprise as much as 10% of all neurocytomas, and unlike the central (intraventricular) variant, glial or ganglionic differentiation has been noted more frequently in them [2]. Ganglioneurocytoma, a subtype of neurocytoma with ganglionic differentiation, initially described by Nishio et al., is considered a low-grade tumor without reports of histopathological grade progression [3, 4]. In this report, we present a case of WHO grade II ganglioneurocytoma (with typical features) progressing into an atypical ganglioneurocytoma. Also reviewed is the relevant body of literature on ganglioneurocytoma with special emphasis on natural history and clinical progression. Published by Sciedu Press 7
2 2 Case history A 25-year-old right-handed gentleman presented with recurrent left frontal brain tumor. Five years prior to the current presentation, he was evaluated for headaches and new onset seizures at another institution. Magnetic resonance imaging (MRI) of the brain had revealed a cystic tumor in the left frontal lobe with a mural nodule (see Figure 1). At that time, he underwent gross total resection of this lesion. Pathological examination from the first surgery demonstrated well demarcated tumor consisting of small round or polygonal cells arranged in clusters and sheets (see Figure 2). Some of the more polygonal cells showed distinct ganglion cell differentiation on H&E stained sections. No areas of necrosis or vascular proliferation were noted. Only scattered mitotic figures were identified (< 1 per 20 high-powered fields), and the MIB-1 proliferation index was less than 4% focally. Immuno-histochemical staining was strongly positive for synaptophysin while Neuronal Nuclei (NeuN) was minimally reactive. Tumor cells were negative for Glial Fibrillary Acidic Protein (GFAP) and other glial markers. Final pathological diagnosis of ganglioneurocytoma WHO grade II was made based on these features. Figure 1. Pre-operative (A) and post-operative (B) MRI images, T1 with gadolinium contrast and FLAIR, respectively, in chronological order. The initial tumor in 2005 consisted of cystic lesion, an enhancing nodule with considerable surrounding edema (A1); immediate post-operative images show gross total resection (B1). In 2007, there was a small recurrence posterior to the surgical cavity (A1), which again underwent resection without complications (A2). For a second time the tumor recurred in 2010 (A3). We resected the tumor completely and irradiated the tumor bed. There has been no recurrence of tumor in 2.5 years since last resection (B3). Although the patient remained neurologically well, routine surveillance imaging two years later (three years prior to current presentation) revealed tumor recurrence in the left frontal lobe (see Figure 1). This prompted a second surgery with resection of the enhancing mass. The pathologic specimen obtained from second surgery again showed similar morphologic features to those observed from the initial surgical specimen. However, mitotic figures were more numerous 8 ISSN E-ISSN
3 (3-4 mitoses per 20 high-powered fields) and the MIB-1 proliferative index was elevated at 10% (see Figure 2). The final pathologic diagnosis remained ganglioneurocytoma. The patient recovered well from the second surgery, but despite the recurrence and increase in the proliferative index, he declined adjuvant treatment. Figure 2. Representative histopathological sections demonstrating tumor progression over time. H&E stain preparations show a cellular tumor consisting of numerous neurons and ganglion cells arranged in clusters, a hallmark of ganglioneurocytomas (A magnification 10 & B magnification 20). The tumor is strongly reactive for Synaptophysin (C magnification 20). MIB-1 staining of successive tumor resections shows progression of proliferative index over time from typical to atypical ganglioneurocytoma (D, E & F magnification 20). Over the succeeding years, he underwent serial clinical and imaging surveillance and transferred his care to our institution. Three years after his second surgery, a new recurrence was noted as a nodule of MRI contrast enhancement (see Figure 1); because of lack of clinical sequelae, the patient chose no treatment. Recurrent seizures prompted another brain MRI now four years after his second surgery and six years after initial presentation that revealed a larger nodular tumor growth and mass effect (see Figure 1). As a result, the patient underwent a third craniotomy where a complete resection of tumor was achieved. He developed transient supplementary motor area syndrome post-operatively, but made a complete neurologic recovery within weeks. Histopathological examination of the tumor again revealed sheet-like arrangement of neurocytic cells with variable degrees of ganglion-cell differentiation (see Figure 2). Synaptophysin and Protein Gene Product (PGP) 9.5 staining were strongly positive, while reaction to NeuN was again weak. Electron microscopic studies also confirmed neuronal differentiation of the lesional cells. No necrosis or vascular proliferation was apparent but mitotic figures (< 2 per 10 high-powered filed) were again noted. MIB-1 proliferation index was still elevated at 11%. The final histopathologic diagnosis of this tumor specimen was atypical ganglioneurocytoma. Considering the biologic progression of the tumor and repeated clinical recurrence, the patient then underwent intensity-modulated radiotherapy equaling 54 Gy to the tumor bed. At 2.5-year follow-up from his third surgery, the patient remains well without neurologic deficits or evidence of tumor recurrence on neuroimaging. Given the patient s clinical course and pathologic progression, we plan routine imaging surveillance at six-month intervals, for the time being. 3 Discussion Neurocytomas constitute less than 0.5% of all primary brain tumors but only a small subset are found in extraventricular locations (two-thirds of these are reported to be ganglioneurocytomas) [2, 5-7]. Extra-ventricular ganglioneurocytomas have been reported in various sites including cerebral hemispheres, diencephalon, brainstem, spinal cord and skull base [2, 8-10]. Within the cerebral hemispheres, they are more commonly found in the frontal lobe, similar to EVNs [11, 12]. Patients with Published by Sciedu Press 9
4 EVN usually present in middle age, especially in the third and fourth decades of life, while ganglioneurocytomas are often diagnosed in the second decade of life (see Table 1). No convincing sexual predilection exists though some series have reported slight female preponderance [11, 13]. Hydrocephalus is usually associated with central neurocytomas, while extraventricular counterparts present frequently with seizures. The preponderance of location in the fronto-temporal regions might explain the stronger correlation between seizure activity and ganglioneurocytomas (see Table 1). EVNs have rarely been reported to present with intra-tumoral hemorrhage [14]. The natural history is one of slow clinical progression, as in most low-grade primary brain tumors. Patients often present with symptoms of hemispheric space occupying lesions such as seizures and motor deficits [15, 16]. Table 1. List of ganglioneurocytomas reported in the literature References Age/Sex Presentation Location Nishio et al. [18] (1990) Nishio et al. [19] (1992) Nishio et al. [19] (1992) Nishio et al. [19] (1992) Funato et al. [7] (1997) Giangaspero et al. [10] (1997) Tortori-Donati et al. [28] Biernet et al. [12] (2000) [4] Brat et al. (2001) Shin et al. [25] (2002) Nishihara et al. [17] (2008) Chou et al. [5] (2010) Ghosal et al. [8] Agarwal et al. [2] Agarwal et al. [2] Agarwal et al. [2] Atypical Features Treatment Follow up Recurrence 30/F Seizures Left Frontal No STR + 45 Gy 7 Years None 2/F Seizures Left Frontal No STR 2 Years None 41/M Seizures Right Temporal No STR 2 Years None 3/M Seizures Right Frontal No STR 2 months None 11/F Hemiparesis Right Frontal No GTR 18 months None Ganglionic Differentiation In 6/6 40/F Hemiparesis Right Frontal Yes STR + 60Gy 30 months 24 months 31/M Seizures Right Fronto-Temporal No STR (95%) 6 Years In 4 Years 37/M Seizures Right Temporal No STR 4 Years In 2 Years 25/F Seizures Left Frontal Yes STR + 59 Gy + BCNU 13 months None 9/F Seizures Right Frontal No GTR 6 months None 12/M Seizures Left Frontal Yes GTR Not reported Unknown Ganglionic Differentiation 23/M Seizures in 23/35 Left Parieto-Occipital 32/F Seizures Right Parietal No No Not reported Not reported Not reported STR + RT (dose unknown) Not reported Not reported 34/M Seizures Right Frontal Yes GTR Not reported Not reported 9/M Headache Left Fronto-Parietal Yes STR Not reported Not reported 19/M Left Paraventricular No GTR + RT 36 months None 20/M Left Frontal Yes STR + RT 3 months Unknown 35/M Left Fronto-Parietal Yes STR + RT 5 months None Our Report 19/M Seizures Left Frontal Yes GTR Gy 7 Years 2 recurrences Note. GTR Gross total resection, STR Subtotal Resection, Gy Gray 10 ISSN E-ISSN
5 Imaging characteristics of ganglioneurocytomas consist of well-circumscribed cortical lesions with both solid and cystic components and occasional areas of calcification [17, 18]. On brain Computerized tomography (CT), lesions appear hyperdense with irregular calcifications. MR imaging reveals isointense to hypointense lesions on T1-weighed sequences with heterogenous gadolinium enhancement. On T2-weighed sequences, these tumors can be isointense to hyperintense, and peritumoral edema can be appreciated in fluid attenuation inversion recovery images [7, 17, 18]. Rarely, these are dural based and take up contrast homogenously similar to meningiomas [19]. In cases with ganglionic differentiation, a cystic mass may be found with a mural nodule (see Figure 1). The solid component can have varying MR features, based on the cellularity and differentiation of the tumor. In MR spectroscopy, EVNs show increased choline and decreased (or absent) N-acetyl aspartate, similar to intraventricular neurocytomas [20]. Histopathologically, ganglioneurocytomas consist of small round or polygonal cells arranged in sheets, clusters, or ribbons. The nuclei are distinct and lack mitotic figures except in cases of atypical tumors while the cytoplasm is clear or eosinophilic. Frequently, these cells are embedded in a neuropil stroma that shows chicken-wire pattern of vascularization by hyalinised vessels [2, 21]. With these features, the histomorphology can be similar to oligodendrogliomas. Preparation techniques can produce halos around the nuclei simulating oligodendrogliomas, although 1p and/or 19q deletions associated with oligodendrogliomas are absent [2]. EVNs can differentiate into either glial and/or ganglionic forms, but ganglionic differentiation is more common, especially in cerebral tumors [7, 13]. Immunohistochemical staining often shows positivity for synaptophysin and NeuN while being negative for GFAP and p53. Occasional tumors with glial differentiation can be positive for GFAP or GFAP positivity could be due to entrapped astrocytes [22]. On electron microscopy, synapse-like structures are absent or sparsely distributed at the surface of tumor cell processes [23]. Atypical features, including nuclear pleomorphism, mitotic index > 3 per high-power field, areas of necrosis, and/or vascular proliferation, are occasionally seen [7, 19, 24]. Recently, proliferation index in the form of MIB-1 labeling has been used to delineate more aggressive tumors, with a MIB-1 index greater than 2%-5% conferring atypical status in these tumors [25, 26]. In the largest series on EVN by Brat et al., 31% of tumors were atypical, while Furtado et al. in their review found atypical features in 27% of these tumors [7, 11]. The current WHO classification of Central Nervous System (CNS) tumors recognizes neurocytomas as low grade (grade II) [5]. Correlation between ganglionic differentiation and atypicality of EVNs is inferable, due to clinical and pathological outcome such as in our patient. In the case series by Brat et al, 73% of atypical EVNs exhibited ganglionic differentiation [7]. Treatment is mainly surgical with good outcomes achieved after gross total resection. Post-operative radiation may reduce recurrences, especially in cases with atypical histopathology or residual tumor. Gross total resection (GTR) is an important factor in preventing or delaying recurrences. In the series by Brat et al., 11 out of 14 patients who underwent GTR developed no recurrence over a mean follow up period of 29 months [7]. In contrast, 10 out of 19 sub-total resection (STR) patients experienced tumor recurrence within 17 months [7]. Furtado et al. corroborate this finding in their review and further emphasize that atypical lesions manifested disease recurrence earlier than typical EVNs [11]. Adjuvant radiotherapy is generally advocated for residual disease and atypical tumors. Rades et al. in their meta-analysis of atypical neurocytomas found a better outcome for incompletely resected tumors radiated post-operatively compared with incomplete resections that were not irradiated. This increased benefit of improved overall survival and progression-free survival matched that of completely resected lesions (with or without radiation). The treatment dose ranges from Gy of fractionated irradiation, analogous to radiotherapy treatment for other glial neoplasms. Other forms of radiotherapy; brachytherapy, hypofractionated treatment schemes, and stereotactic radiosurgery to the tumor bed or residual mass as alternatives in select cases, have not been studied or reported. The role of adjuvant radiotherapy for a typical EVN after GTR is unknown. However, there can be progression of pathology toward a more malignant phenotype in recurrences, sometimes in spite of GTR [28]. Given the rare incidence of EVNs or ganglioneurocytomas, the definitive role and timing of chemotherapy is not well established, with a tendency to reserve chemotherapy as a salvage option. Numerous chemotherapy regimens have been evaluated in the adjuvant and salvage setting for central neurocytomas with suggestion of benefit. Commonly employed regimens are often cisplatin/carboplatin and etoposide based, with addition of cyclophosphamide or ifosfamide as a third agent [29, 30]. Published by Sciedu Press 11
6 4 Conclusions In the histopathologic spectrum of glioneuronal neoplasms, ganglioneurocytomas have been recognized as a subtype of neurocytomas with a predilection for extraventricular location, low-grade pathologic features, and generally good prognosis. However, because of limited long-term clinical data, potential for histopathologic uncertainty due to a lack of diagnostic markers, and recent reports indicating more aggressive clinical behavior, the presumed benign nature of these tumors is questionable. In this report, we present a detailed course of clinical and pathological progression observed in a ganglioneurocytoma patient over a seven-year period with serial histopathologic and imaging confirmation. This case presents a rare opportunity to study serial tumor progression in ganglioneurocytoma unaffected by adjuvant treatments over a long follow-up. In many brain tumors increased proliferative activity is a feature of higher WHO grade. In this case, the patient was recurrence free for three years after the second surgery, despite not receiving any adjuvant therapy. It is difficult to establish whether a ganglioneurocytoma with the described features to be regarded as anaplastic (WHO grade III). Alternatively one could argue that the behavior in this case was still more indolent than that typically observed in WHO grade III neoplasms and that the observed increased proliferative activity alone may not be a poor predictor of aggressive growth.. Nevertheless, we advocate maximal tumor resection for surgically accessible ganglioneurocytomas, as well as close imaging surveillance and clinical follow-up. In cases of STR or atypical features, adjuvant treatment with radiotherapy, and possibly chemotherapy, may be considered. Additional investigation into immunohistochemical and molecular markers that can refine pathological diagnosis of glioneuronal neoplasms is necessary to enable prospective evaluation of clinical outcomes and treatment effectiveness. References [1] Hassoun J, et al. Central neurocytoma. An electron-microscopic study of two cases. Acta Neuropathol. 1982; 56(2): PMid: [2] Agarwal S, et al. Extraventricular neurocytomas: a morphological and histogenetic consideration. A study of six cases. Pathology. 2011; 43(4): PMid: [3] Nishio SI Takeshita, Fukui M. Primary cerebral ganglioneurocytoma in an adult. Cancer. 1990; 66(2): [4] Nishio S, et al. Cerebral neurocytoma. A new subset of benign neuronal tumors of the cerebrum. Cancer. 1992; 70(2): [5] Louis DN, et al. The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol. 2007; 114(2): PMid: [6] Kurose A, et al. Ganglioneurocytoma: distinctive variant of central neurocytoma. Pathol Int. 2007; 57(12): PMid: [7] Brat DJ, et al. Extraventricular neurocytomas: pathologic features and clinical outcome. Am J Surg Pathol. 2001; 25(10): PMid: [8] Shidoh S, et al. Extraaxial neurocytoma in the skull base. Brain Tumor Pathol. 2011; 28(3): PMid: [9] Swinson BM, Friedman WA, Yachnis AT. Pontine atypical neurocytoma: case report. Neurosurgery. 2006; 58(5): E990; discussion E990. [10] Sgouros S, Walsh AR, Barber P. Central neurocytoma of thalamic origin. Br J Neurosurg. 1994; 8(3): PMid: [11] Furtado A, et al. Comprehensive review of extraventricular neurocytoma with report of two cases, and comparison with central neurocytoma. Clin Neuropathol. 2010; 29(3): PMid: [12] Biernat W, Zakrzewski K, Liberski PP. January 2000: 12 year old boy with recent onset seizures. Brain Pathol. 2000; 10(2): 313-4, 319. PMid: [13] Giangaspero F, et al. Extraventricular neoplasms with neurocytoma features. A clinicopathological study of 11 cases. Am J Surg Pathol. 1997; 21(2): PMid: [14] Ritz R, et al. Extraventricular neurocytoma presenting with intratumoral hemorrhage. Clin Neuropathol. 2005; 24(3): PMid: ISSN E-ISSN
7 [15] Nishihara H, et al. A case of cerebral ganglioneuronal tumor in the parietal lobe of an adult. Brain Tumor Pathol. 2008; 25(1): PMid: [16] Tortori-Donati P, et al. Extraventricular neurocytoma with ganglionic differentiation associated with complex partial seizures. AJNR Am J Neuroradiol. 1999; 20(4): PMid: [17] Yang GF, et al. Imaging findings of extraventricular neurocytoma: report of 3 cases and review of the literature. AJNR Am J Neuroradiol. 2009; 30(3): PMid: [18] Shin JH, et al. Neuronal tumors of the central nervous system: radiologic findings and pathologic correlation. Radiographics. 2002; 22(5): PMid: [19] Moriguchi S, et al. Atypical extraventricular neurocytoma. Pathol Int. 2006; 56(1): PMid: [20] Moller-Hartmann W, et al. Proton magnetic resonance spectroscopy of neurocytoma outside the ventricular region--case report and review of the literature. Neuroradiology. 2002; 44(3): PMid: [21] Teo JG, et al. A distinctive glioneuronal tumor of the adult cerebrum with neuropil-like (including "rosetted") islands: report of 4 cases. Am J Surg Pathol. 1999; 23(5): PMid: [22] Mpairamidis E, et al. Extraventricular neurocytoma in a child: case report and review of the literature. J Child Neurol. 2009; 24(4): PMid: [23] Funato H, et al. Cystic ganglioneurocytoma outside the ventricular region. Acta Neuropathol. 1997; 94(1): PMid: [24] Chou S, et al. Extraventricular neurocytoma with atypical features and ganglionic differentiation. J Clin Neurosci. 2010; 17(7): PMid: [25] Rades D, Schild SE, Fehlauer F. Prognostic value of the MIB-1 labeling index for central neurocytomas. Neurology. 2004; 62(6): PMid: [26] Ghosal N, et al. Atypical extraventricular neurocytoma: a rare and challenging case diagnosed on intraoperative cytology. Cytopathology. 2012; 23(4): PMid: Rades D, Fehlauer F, Schild SE. Treatment of atypical neurocytomas. Cancer. 2004; 100(4): PMid: [28] Myung JK, et al. Clinicopathological and genetic characteristics of extraventricular neurocytomas. Neuropathology. 2013; 33(2): PMid: [29] Brandes AA, et al. Chemotherapy in patients with recurrent and progressive central neurocytoma. Cancer. 2000; 88(1): [30] Dodds D, et al. Central neurocytoma: a clinical study of response to chemotherapy. J Neurooncol. 1997; 34(3): PMid: Published by Sciedu Press 13
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
Case 7391 Intraventricular Lesion
 Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Case #3. USCAP Neuropathology Evening Seminar/Companion Meeting
 Case #3 USCAP Neuropathology Evening Seminar/Companion Meeting Clinical History A 71-year year-old man presented with a 4-4 week history of word finding difficulty. An initial screening head CT followed
Case #3 USCAP Neuropathology Evening Seminar/Companion Meeting Clinical History A 71-year year-old man presented with a 4-4 week history of word finding difficulty. An initial screening head CT followed
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution
 Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad
 Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases
 Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases Ho Sung Kim, MD 1 Ho Kyu Lee, MD 1 Ae Kyung Jeong, MD 1 Ji Hoon Shin, MD 1 Choong Gon Choi, MD 1 Shin Kwang Khang, MD 2 We
Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases Ho Sung Kim, MD 1 Ho Kyu Lee, MD 1 Ae Kyung Jeong, MD 1 Ji Hoon Shin, MD 1 Choong Gon Choi, MD 1 Shin Kwang Khang, MD 2 We
Joana Ramalho, MD C. Ryan Miller, MD, PhD
 Joana Ramalho, MD C. Ryan Miller, MD, PhD Case 1 3 month old baby girl Presented with new onset of seizures Newborn. Questionable blurring of the gray-white junction within the right occipital lobe. Findings
Joana Ramalho, MD C. Ryan Miller, MD, PhD Case 1 3 month old baby girl Presented with new onset of seizures Newborn. Questionable blurring of the gray-white junction within the right occipital lobe. Findings
Pleomorphic Xanthoastrocytoma
 Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum
 Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
In 1988 Dumas-Duport et al. first used
 Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Infratentorial and Intraparenchymal Subependymoma in the Cerebellum: Case Report
 Case Report Neuroimaging and Head and Neck http://dx.doi.org/10.3348/kjr.2014.15.1.151 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(1):151-155 Infratentorial and Intraparenchymal Subependymoma
Case Report Neuroimaging and Head and Neck http://dx.doi.org/10.3348/kjr.2014.15.1.151 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(1):151-155 Infratentorial and Intraparenchymal Subependymoma
Five Most Common Problems in Surgical Neuropathology
 Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Chapter 1 Introduction
 Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
Liponeurocytoma of Cerebellum: rare entity, case based study
 182 Satyarthee et al Liponeurocytoma Liponeurocytoma of Cerebellum: rare entity, case based study Guru Dutta Satyarthee 1, A.K. Mahapatra 2 Department of Neurosurgery 1 All India Institute of Medical sciences,
182 Satyarthee et al Liponeurocytoma Liponeurocytoma of Cerebellum: rare entity, case based study Guru Dutta Satyarthee 1, A.K. Mahapatra 2 Department of Neurosurgery 1 All India Institute of Medical sciences,
CHINESE MEDICAL ASSOCIATION
 Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Pediatric Brain Tumors: Updates in Treatment and Care
 Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma
 From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma Marcus C de Jong, Annette C Moll, Sophia Göricke, Paul van der Valk, Wijnanda A Kors, Jonas A
From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma Marcus C de Jong, Annette C Moll, Sophia Göricke, Paul van der Valk, Wijnanda A Kors, Jonas A
Symtomatic Subependymoma Of The Lateral Ventricle: A Rare Entity A Case report and review of literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Symtomatic Subependymoma Of The Lateral Ventricle: A Rare Entity A Case report and review of M Sharma, V Velho, P Ghodgaonkar, D Palande
ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Symtomatic Subependymoma Of The Lateral Ventricle: A Rare Entity A Case report and review of M Sharma, V Velho, P Ghodgaonkar, D Palande
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017
 AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017 SYLLABUS Papillary Tumor of the Pineal Region and the Differential
AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017 SYLLABUS Papillary Tumor of the Pineal Region and the Differential
Rapid recurrence of a malignant meningioma: case report
 Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Neurocytoma a Rare Intraventricular Tumor
 Neurocytoma a Rare Intraventricular Tumor J. A. Mallick,S. A. Ali ( Department of Oncology, Liaquat National Postgraduate Medical Centre, Karachi. ) Introduction Central neurocytoma was first recognized
Neurocytoma a Rare Intraventricular Tumor J. A. Mallick,S. A. Ali ( Department of Oncology, Liaquat National Postgraduate Medical Centre, Karachi. ) Introduction Central neurocytoma was first recognized
General Identification. Name: 江 X X Age: 29 y/o Gender: Male Height:172cm, Weight: 65kg Date of admission:95/09/27
 General Identification Name: 江 X X Age: 29 y/o Gender: Male Height:172cm, Weight: 65kg Date of admission:95/09/27 Chief Complaint Sudden onset of seizure for several minutes Present illness This 29-year
General Identification Name: 江 X X Age: 29 y/o Gender: Male Height:172cm, Weight: 65kg Date of admission:95/09/27 Chief Complaint Sudden onset of seizure for several minutes Present illness This 29-year
Supratentorial multiple little meningiomas with transitory stroke symptoms like. MRI case presentation
 114 Romanian Neurosurgery (2010) XVII 1: 114-121 Supratentorial multiple little meningiomas with transitory stroke symptoms like. MRI case presentation E. Moldovanu 1,2, Adriana Moldovanu 1,2, Carmen Gherman
114 Romanian Neurosurgery (2010) XVII 1: 114-121 Supratentorial multiple little meningiomas with transitory stroke symptoms like. MRI case presentation E. Moldovanu 1,2, Adriana Moldovanu 1,2, Carmen Gherman
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
ADSS Case 1. A 31-year-old male with a seizure. Se-Hoon Kim
 ADSS Case 1 A 31-year-old male with a seizure Se-Hoon Kim Department of Pathology, Yonsei University College of Medicine, Severance Hospital, Seoul, Korea A 31-year-old male patient without specific medical
ADSS Case 1 A 31-year-old male with a seizure Se-Hoon Kim Department of Pathology, Yonsei University College of Medicine, Severance Hospital, Seoul, Korea A 31-year-old male patient without specific medical
CASE OF THE WEEK PROFESSOR YASSER METWALLY
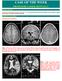 CASE OF THE WEEK PROFESSOR YASSER METWALLY CLINICAL PICTURE CLINICAL PICTURE: CLINICAL PICTURE: A 6 years old male patient presented clinically with intractable complex partial seizure. The child is mentally
CASE OF THE WEEK PROFESSOR YASSER METWALLY CLINICAL PICTURE CLINICAL PICTURE: CLINICAL PICTURE: A 6 years old male patient presented clinically with intractable complex partial seizure. The child is mentally
SPECIAL SLIDE SEMINAR CASE 3
 SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
Understanding general brain tumor pathology, Part I: The basics. Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky
 Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Rosette-forming glioneuronal tumor in the pineal gland and the third ventricle: a case with radiological and clinical implications
 Case Report Rosette-forming glioneuronal tumor in the pineal gland and the third ventricle: a case with radiological and clinical implications Junqing Xu 1, Yong Yang 1, Ying Liu 1, Mengqi Wei 1, Jing
Case Report Rosette-forming glioneuronal tumor in the pineal gland and the third ventricle: a case with radiological and clinical implications Junqing Xu 1, Yong Yang 1, Ying Liu 1, Mengqi Wei 1, Jing
Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child
 Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
Brain Tumors. Medulloblastoma. Pilocytic astrocytoma: Ahmed Koriesh, MD. Pathological finding
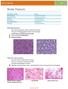 NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors
 Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors Poster No.: C-2652 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: M. Gavrilov, T.
Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors Poster No.: C-2652 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: M. Gavrilov, T.
Role of Diffusion weighted Imaging in the Evaluation of Intracranial Tumors
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 12 Ver. IX (December. 2016), PP 99-104 www.iosrjournals.org Role of Diffusion weighted Imaging
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 12 Ver. IX (December. 2016), PP 99-104 www.iosrjournals.org Role of Diffusion weighted Imaging
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Posterior fossa tumors: clues to differential diagnosis with case-based review
 Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
ISSN X (Print) Case Report
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(1A):128-132 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(1A):128-132 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
A case of multinodular high-grade neuroepithelial tumor
 Brain Tumor Pathol (2011) 28:253 257 DOI 10.1007/s10014-011-0032-6 CASE REPORT A case of multinodular high-grade neuroepithelial tumor with ependymal differentiation Kensaku Kamada Yuko Tanaka Takayuki
Brain Tumor Pathol (2011) 28:253 257 DOI 10.1007/s10014-011-0032-6 CASE REPORT A case of multinodular high-grade neuroepithelial tumor with ependymal differentiation Kensaku Kamada Yuko Tanaka Takayuki
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Supratentorial extraventricular anaplastic ependymoma in an adult with repeated intratumoral hemorrhage
 Brain Tumor Pathol (2014) 31:138 143 DOI 10.1007/s10014-013-0146-0 CASE REPORT Supratentorial extraventricular anaplastic ependymoma in an adult with repeated intratumoral hemorrhage Naotaka Iwamoto Yasuo
Brain Tumor Pathol (2014) 31:138 143 DOI 10.1007/s10014-013-0146-0 CASE REPORT Supratentorial extraventricular anaplastic ependymoma in an adult with repeated intratumoral hemorrhage Naotaka Iwamoto Yasuo
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Case Report Spinal pleomorphic xanthoastrocytoma companied with periventricular tumor
 Int J Clin Exp Pathol 2015;8(1):1036-1040 www.ijcep.com /ISSN:1936-2625/IJCEP0003595 Case Report Spinal pleomorphic xanthoastrocytoma companied with periventricular tumor Xintong Zhao 1, Xiaochun Jiang
Int J Clin Exp Pathol 2015;8(1):1036-1040 www.ijcep.com /ISSN:1936-2625/IJCEP0003595 Case Report Spinal pleomorphic xanthoastrocytoma companied with periventricular tumor Xintong Zhao 1, Xiaochun Jiang
RING ENCHANCING LESION BY M.S. HEMHNATH
 RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
MOLECULAR DIAGNOSTICS OF GLIOMAS
 MOLECULAR DIAGNOSTICS OF GLIOMAS Arie Perry, M.D. Director, Neuropathology Division DIFFUSE GLIOMAS Cell types Astrocytomas (A) Oligodendrogliomas (O) Mixed oligoastrocytoma (MOA) Three WHO grades: II,
MOLECULAR DIAGNOSTICS OF GLIOMAS Arie Perry, M.D. Director, Neuropathology Division DIFFUSE GLIOMAS Cell types Astrocytomas (A) Oligodendrogliomas (O) Mixed oligoastrocytoma (MOA) Three WHO grades: II,
Meningioma tumor. Meningiomas are named according to their location (Fig. 1) and cause various symptoms: > 1
 Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Case 2. Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset
 Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
MRI Findings Of An Atypical Cystic Meningioma A Rare Case
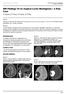 ISPUB.COM The Internet Journal of Radiology Volume 14 Number 1 MRI Findings Of An Atypical Cystic Meningioma A Rare Case D Saxena, P Rout, K Pavan, B Philip Citation D Saxena, P Rout, K Pavan, B Philip.
ISPUB.COM The Internet Journal of Radiology Volume 14 Number 1 MRI Findings Of An Atypical Cystic Meningioma A Rare Case D Saxena, P Rout, K Pavan, B Philip Citation D Saxena, P Rout, K Pavan, B Philip.
Pediatric and Adolescent Oligodendrogliomas
 Pediatric and Adolescent Oligodendrogliomas Harold Tice, 1 Patrick D. Barnes, 1 Liliana Goumnerova, 2 R. Michael Scott, 2 and Nancy J. Tarbell 3 PURPOSE: To review the clinical and imaging findings in
Pediatric and Adolescent Oligodendrogliomas Harold Tice, 1 Patrick D. Barnes, 1 Liliana Goumnerova, 2 R. Michael Scott, 2 and Nancy J. Tarbell 3 PURPOSE: To review the clinical and imaging findings in
Structural and functional imaging for the characterization of CNS lymphomas
 Structural and functional imaging for the characterization of CNS lymphomas Cristina Besada Introduction A few decades ago, Primary Central Nervous System Lymphoma (PCNSL) was considered as an extremely
Structural and functional imaging for the characterization of CNS lymphomas Cristina Besada Introduction A few decades ago, Primary Central Nervous System Lymphoma (PCNSL) was considered as an extremely
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Chordoid glioma: CT and MR features
 Chin J Radiol 2005; 30: 225-229 225 Chordoid glioma: CT and MR features YI-CHIH HSU HUNG-WEN KAO CHUNG-PING LO CHUN-JUNG JUAN SHY-CHYI CHIN CHENG-YU CHEN Department of Radiology, Tri-Service General Hospital
Chin J Radiol 2005; 30: 225-229 225 Chordoid glioma: CT and MR features YI-CHIH HSU HUNG-WEN KAO CHUNG-PING LO CHUN-JUNG JUAN SHY-CHYI CHIN CHENG-YU CHEN Department of Radiology, Tri-Service General Hospital
Masses of the Corpus Callosum
 Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
A Stable Secondary Gliosarcoma with Extensive Systemic Metastases: A Case Report
 CASE REPORT Brain Tumor Res Treat 2016;4(2):133-137 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2016.4.2.133 A Stable Secondary Gliosarcoma with Extensive Systemic Metastases: A
CASE REPORT Brain Tumor Res Treat 2016;4(2):133-137 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2016.4.2.133 A Stable Secondary Gliosarcoma with Extensive Systemic Metastases: A
Pathologic features and clinical outcome of central neurocytoma: analysis of 15 cases
 Original Article Pathologic features and clinical outcome of central neurocytoma: analysis of 15 cases Yu Li, Xiu-Feng Ye, Guo Qian, Yu Yin, Qian-Guan Pan Institute of Neuroscience, Department of Pathology,
Original Article Pathologic features and clinical outcome of central neurocytoma: analysis of 15 cases Yu Li, Xiu-Feng Ye, Guo Qian, Yu Yin, Qian-Guan Pan Institute of Neuroscience, Department of Pathology,
Gangliogliomas: A Report of Five Cases
 Case Report Gangliogliomas: A Report of Five Cases Nair V, Suri VS, Tatke M, Saran RK, Malhotra V, Singh D* Departments of Pathology and *Neurosurgery, G. B. Pant Hospital, New Delhi, India. Correspondence
Case Report Gangliogliomas: A Report of Five Cases Nair V, Suri VS, Tatke M, Saran RK, Malhotra V, Singh D* Departments of Pathology and *Neurosurgery, G. B. Pant Hospital, New Delhi, India. Correspondence
Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence
 PEDIATRIC RHABDOID MENINGIOMA Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence CLINICAL HISTORY A 3-year-old boy, with a recent history of seizures, was admitted to the Neurosurgery
PEDIATRIC RHABDOID MENINGIOMA Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence CLINICAL HISTORY A 3-year-old boy, with a recent history of seizures, was admitted to the Neurosurgery
Neuropathology Evening Session: Case 3
 Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
NON MALIGNANT BRAIN TUMOURS Facilitator. Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol
 NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
Radioterapia no Tratamento dos Gliomas de Baixo Grau
 Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
No financial or other disclosures
 Case 2014-5 Esther N. Bit-Ivan, DO Northwestern University Jason Wang, MD Jason Park, MD Korgun Koral, MD Children s Medical Center Charles Timmons, MD Veena Rajaram, MD No financial or other disclosures
Case 2014-5 Esther N. Bit-Ivan, DO Northwestern University Jason Wang, MD Jason Park, MD Korgun Koral, MD Children s Medical Center Charles Timmons, MD Veena Rajaram, MD No financial or other disclosures
Rhabdoid Meningioma In A Background Of Atypical Meningioma With Lipomatous Metaplasia: Case Report And Review Of Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Rhabdoid Meningioma In A Background Of Atypical Meningioma With Lipomatous Metaplasia: Case Report And Review Of Literature S Shuja, T Lucey,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Rhabdoid Meningioma In A Background Of Atypical Meningioma With Lipomatous Metaplasia: Case Report And Review Of Literature S Shuja, T Lucey,
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
2017 Diagnostic Slide Session Case 3
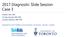 2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
BAH1 - Primary Glioblastoma
 BAH1 - Primary Glioblastoma R frontal tumour for frozen section. No known primary. Contrast enhancing lesion. Cholecystectomy. FROZEN SECTION REPORT Right frontal tumour: The specimen consists of multiple
BAH1 - Primary Glioblastoma R frontal tumour for frozen section. No known primary. Contrast enhancing lesion. Cholecystectomy. FROZEN SECTION REPORT Right frontal tumour: The specimen consists of multiple
Pediatric primary anaplastic ganglioglioma with malignant neuronal component
 The Turkish Journal of Pediatrics 2018; 60: 102-106 DOI: 10.24953/turkjped.2018.01.017 Case Report Pediatric primary anaplastic ganglioglioma with malignant neuronal component Meriç Kaymak-Cihan 1, Eda
The Turkish Journal of Pediatrics 2018; 60: 102-106 DOI: 10.24953/turkjped.2018.01.017 Case Report Pediatric primary anaplastic ganglioglioma with malignant neuronal component Meriç Kaymak-Cihan 1, Eda
CNS SESSION 3/8/ th Multidisciplinary Management of Cancers: A Case based Approach
 CNS SESSION Chair: Ruben Fragoso, MD/PhD UC Davis Fellow: Michael Cardenas, MD UC Davis Panel: Gordon Li, MD Stanford Seema Nagpal, MD Stanford Jennie Taylor, MD UCSF HPI: 46 yo right handed woman who
CNS SESSION Chair: Ruben Fragoso, MD/PhD UC Davis Fellow: Michael Cardenas, MD UC Davis Panel: Gordon Li, MD Stanford Seema Nagpal, MD Stanford Jennie Taylor, MD UCSF HPI: 46 yo right handed woman who
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy
 AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
Chordoid Meningioma in a Pediatric Patient with Tuberous Sclerosis Complex
 The Korean Journal of Pathology 2014; 48: 302-306 BRIEF CASE REPORT Chordoid Meningioma in a Pediatric Patient with Tuberous Sclerosis Complex Jiwon Lee Hee Joon Yu Jeehun Lee Ji Hye Kim 1 Hyung Jin Shin
The Korean Journal of Pathology 2014; 48: 302-306 BRIEF CASE REPORT Chordoid Meningioma in a Pediatric Patient with Tuberous Sclerosis Complex Jiwon Lee Hee Joon Yu Jeehun Lee Ji Hye Kim 1 Hyung Jin Shin
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
International Journal of Pharma and Bio Sciences CHROMOPHOBE VARIANT OF RENAL CELL CARCINOMA MASQUARDING AS RENAL ONCOCYTOMA ON CYTOLOGY.
 Case Report Pathology International Journal of Pharma and Bio Sciences ISSN 0975-6299 CHROMOPHOBE VARIANT OF RENAL CELL CARCINOMA MASQUARDING AS RENAL ONCOCYTOMA ON CYTOLOGY. DR.MAMATHA K*, DR. ARAKERI
Case Report Pathology International Journal of Pharma and Bio Sciences ISSN 0975-6299 CHROMOPHOBE VARIANT OF RENAL CELL CARCINOMA MASQUARDING AS RENAL ONCOCYTOMA ON CYTOLOGY. DR.MAMATHA K*, DR. ARAKERI
Hamartomas and epilepsy: clinical and imaging characteristics
 Seizure 2003; 12: 307 311 doi:10.1016/s1059 1311(02)00272-8 Hamartomas and epilepsy: clinical and imaging characteristics B. DIEHL, R. PRAYSON, I. NAJM & P. RUGGIERI Departments of Neurology, Pathology
Seizure 2003; 12: 307 311 doi:10.1016/s1059 1311(02)00272-8 Hamartomas and epilepsy: clinical and imaging characteristics B. DIEHL, R. PRAYSON, I. NAJM & P. RUGGIERI Departments of Neurology, Pathology
Cross sectional imaging of Intracranial cystic lesions Abdel Razek A
 Cross sectional imaging of Intracranial cystic lesions Abdel Razek A Department of Radiology. Mansoura Faculty of Medicine, Mansoura. Egypt. arazek@mans.edu.eg Introduction Intracranial cystic lesions
Cross sectional imaging of Intracranial cystic lesions Abdel Razek A Department of Radiology. Mansoura Faculty of Medicine, Mansoura. Egypt. arazek@mans.edu.eg Introduction Intracranial cystic lesions
Case Report Tackling a Recurrent Pinealoblastoma
 Case Reports in Oncological Medicine, Article ID 135435, 4 pages http://dx.doi.org/10.1155/2014/135435 Case Report Tackling a Recurrent Pinealoblastoma Siddanna Palled, 1 Sruthi Kalavagunta, 1 Jaipal Beerappa
Case Reports in Oncological Medicine, Article ID 135435, 4 pages http://dx.doi.org/10.1155/2014/135435 Case Report Tackling a Recurrent Pinealoblastoma Siddanna Palled, 1 Sruthi Kalavagunta, 1 Jaipal Beerappa
Brief History. Identification : Past History : HTN without regular treatment.
 Brief History Identification : Name : 陳 x - Admission : 94/10/06 Gender : male Age : 75 y/o Chief Complaint : Urinary difficulty for months. Past History : HTN without regular treatment. Brief History
Brief History Identification : Name : 陳 x - Admission : 94/10/06 Gender : male Age : 75 y/o Chief Complaint : Urinary difficulty for months. Past History : HTN without regular treatment. Brief History
Spinal Meningeal Melanocytoma with Benign Histology Showing Leptomeningeal Spread: Case Report
 Case Report Musculoskeletal Imaging A 37-year-old previously healthy man presented with a 2 months history of increasing posterior neck pain and radiating pain to the right upper extremity. Neurological
Case Report Musculoskeletal Imaging A 37-year-old previously healthy man presented with a 2 months history of increasing posterior neck pain and radiating pain to the right upper extremity. Neurological
Laura Tormoehlen, M.D. Neurology and EM-Toxicology Indiana University
 Laura Tormoehlen, M.D. Neurology and EM-Toxicology Indiana University Disclosures! No conflicts of interest to disclose Neuroimaging 101! Plain films! Computed tomography " Angiography " Perfusion! Magnetic
Laura Tormoehlen, M.D. Neurology and EM-Toxicology Indiana University Disclosures! No conflicts of interest to disclose Neuroimaging 101! Plain films! Computed tomography " Angiography " Perfusion! Magnetic
Cerebral Parenchymal Lesions: I. Metastatic Neoplasms
 Chapter 4 Cerebral Parenchymal Lesions: I. Metastatic Neoplasms After one has reasonably ruled out the possibility of a nonneoplastic diagnosis (see Chap. 3), one is left with considering a diagnosis of
Chapter 4 Cerebral Parenchymal Lesions: I. Metastatic Neoplasms After one has reasonably ruled out the possibility of a nonneoplastic diagnosis (see Chap. 3), one is left with considering a diagnosis of
The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease
 AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
SUPPLEMENTARY INFORMATION
 VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
American Journal of. Medical Case Reports. CAM5.2 Expression in Metastatic Tumours of CNS: A Diagnostic Tool
 American Journal of American Journals of Medical Case Reports http://ivyunion.org/index.php/ajmcr/index Medical Case Reports Mathur SK et al. American Journal of Medical Case Reports 2014, 2:1-8 Vol 2,
American Journal of American Journals of Medical Case Reports http://ivyunion.org/index.php/ajmcr/index Medical Case Reports Mathur SK et al. American Journal of Medical Case Reports 2014, 2:1-8 Vol 2,
Primary Central Nervous System Lymphoma with Lateral Ventricle Involvement
 The Open Medical Imaging Journal, 2012, 6, 103-107 103 Open Access Primary Central Nervous System Lymphoma with Lateral Ventricle Involvement Yumi Oie 1,*, Kazuhiro Murayama 1, Shinya Nagahisa 2, Masato
The Open Medical Imaging Journal, 2012, 6, 103-107 103 Open Access Primary Central Nervous System Lymphoma with Lateral Ventricle Involvement Yumi Oie 1,*, Kazuhiro Murayama 1, Shinya Nagahisa 2, Masato
Intramedullary central neurocytoma of the thoracic spinal cord: A case report and literature review
 MOLECULAR AND CLINICAL ONCOLOGY 8: 539-543, 2018 Intramedullary central neurocytoma of the thoracic spinal cord: A case report and literature review ZHIMIN LI, JUN GAO, TIANYU WANG, XIANGYI KONG, JIAN
MOLECULAR AND CLINICAL ONCOLOGY 8: 539-543, 2018 Intramedullary central neurocytoma of the thoracic spinal cord: A case report and literature review ZHIMIN LI, JUN GAO, TIANYU WANG, XIANGYI KONG, JIAN
ASJ. Myxopapillary Ependymoma of the Cauda Equina in a 5-Year-Old Boy. Asian Spine Journal. Introduction
 Asian Spine Journal 846 Masashi Case Uehara Report et al. Asian Spine J 2014;8(6):846-851 http://dx.doi.org/10.4184/asj.2014.8.6.846 Asian Spine J 2014;8(6):846-851 Myxopapillary Ependymoma of the Cauda
Asian Spine Journal 846 Masashi Case Uehara Report et al. Asian Spine J 2014;8(6):846-851 http://dx.doi.org/10.4184/asj.2014.8.6.846 Asian Spine J 2014;8(6):846-851 Myxopapillary Ependymoma of the Cauda
Case 1. Maysa Al-Hussaini MD FRCPath
 Case 1 Maysa Al-Hussaini MD FRCPath MAYSA King AL-HUSSAINI Hussein Cancer MD Center MRCPATH KING HUSSEIN Amman CANCER Jordan CENTER Clinical history 4 year old boy History of frontal headache, sleepiness.
Case 1 Maysa Al-Hussaini MD FRCPath MAYSA King AL-HUSSAINI Hussein Cancer MD Center MRCPATH KING HUSSEIN Amman CANCER Jordan CENTER Clinical history 4 year old boy History of frontal headache, sleepiness.
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT
 SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
Case Report Intraparenchymal frontal lobe ependymoma without rosettes: a case report
 Int J Clin Exp Med 2018;11(9):10111-10115 www.ijcem.com /ISSN:1940-5901/IJCEM0070674 Case Report Intraparenchymal frontal lobe ependymoma without rosettes: a case report Qianlei Liang 1*, Xin Chen 2*,
Int J Clin Exp Med 2018;11(9):10111-10115 www.ijcem.com /ISSN:1940-5901/IJCEM0070674 Case Report Intraparenchymal frontal lobe ependymoma without rosettes: a case report Qianlei Liang 1*, Xin Chen 2*,
The recently updated World Health Organization (WHO)
 REVIEW ARTICLE The Expanding Family of Glioneuronal Tumors Daniela S. Allende, MD and Richard A. Prayson, MD Abstract: Three new entities have been recently added to the group of glioneuronal tumors in
REVIEW ARTICLE The Expanding Family of Glioneuronal Tumors Daniela S. Allende, MD and Richard A. Prayson, MD Abstract: Three new entities have been recently added to the group of glioneuronal tumors in
Case Presentation. Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD. Department of Pathology Jordan University Hospital Amman, Jordan
 Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE
 THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
