Research Article Clinicopathologic Correlation of Oral Lichen Planus and Oral Lichenoid Lesions: A Preliminary Study
|
|
|
- Louisa Park
- 6 years ago
- Views:
Transcription
1 e Scientific World Journal, Article ID , 6 pages Research Article Clinicopathologic Correlation of Oral Lichen Planus and Oral Lichenoid Lesions: A Preliminary Study Marinka Mravak-StipetiT, 1 BoDana LonIar-Brzak, 1 Iva Bakale-Hodak, 1 Ivan Sabol, 2 Sven Seiwerth, 3 Martina MajstoroviT, 4 and Magdalena Grce 2 1 Department of Oral Medicine, Department of Oral Medicine, School of Dental Medicine, University of Zagreb, Zagreb, Croatia 2 Division of Molecular Medicine, Rudjer Boskovic Institute, Zagreb, Croatia 3 Department of Pediatric Dentistry, School of Dental Medicine, University of Zagreb, Zagreb, Croatia 4 School of Medicine, Institute of Pathology, University of Zagreb, Zagreb, Croatia Correspondence should be addressed to Marinka Mravak-Stipetić; mmstipetic@gmail.com Received 31 July 2014; Revised 8 September 2014; Accepted 17 September 2014; Published 29 October 2014 Academic Editor: Niroshani Soysa Copyright 2014 Marinka Mravak-Stipetić et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Oral lichen planus (OLP) and oral lichenoid lesions (OLL) are clinically and histologically similar lesions but their treatment planning and prognosis are different. The review of the literature indicates numerous criteria to distinguish these two lesions; however there is a lot of inconsistency. Thus, the aim of this study was to determine the correlation of histopathology and clinical OLP and OLL diagnosis and to clarify which histopathologic criteria could best distinguish these two diagnoses. A retrospective study showed that clinically diagnosed 92 OLPs and 14 OLLs have been confirmed histopathologically in 52.2% and 42.9% of cases, respectively. In addition, histopathology showed statistically significant more eosinophils (P < ), plasma cells (P < ), and granulocytes (P < 0.05) in OLL than OLP. To establish histopathological diagnosis of OLP and OLL it should be mandatory to define the type of cells in mononuclear infiltrate, which can be associated more accurately with clinical feature and patient history. Therefore, currently accepted diagnostic criteria for OLP and OLL should be modified and validated on a larger number of patients taking into account particular distinguishing histopathological features. 1. Introduction Oral lichen planus (OLP) is a chronic immunological mucocutaneous disorder of unknown etiology with prevalence in general population ranging from 0.2 to 2% [1, 2], whereas the prevalence of OLP found in our population was 4.3% [3]. Due to low [2, 4, 5] and rather questionable [6 8] risk for malignant transformation, OLP is classified as potentially malignant disorder [9]. Indeed, OLP has distinctive clinical features within the oral cavity with several characteristic morphological types and symmetrical distribution in oral mucosa [5, 6, 8]. These features facilitate clinical diagnosis. However, due to its premalignant potential, nonreticular types, unilateral presentation, or lesions present at the cancerrisk oral sites it requires histopathological confirmation as well. Histopathological criteria for OLP, which are currently accepted in clinical practice, are those given by WHO [10]. These criteria do not distinguish between the OLP and oral lichenoid lesions (OLL); therefore, several reports have suggested their modifications [8, 11, 12]. Van der Meij and van der Waal [11]proposedmodifiedWHOcriteriaaccording to which OLP could be diagnosed only in cases when both clinical and histopathological criteria are fulfilled, while in other cases, the disorder should be considered as OLL. It is accepted that OLL is clinically and histologically similar to OLP [11, 13] but has less characteristic morphology and distribution, whereas lichen planus-like lesions are described as oral lichenoid lesion (OLL), oral lichenoid tissue reaction (OLTR), or lichenoid contact stomatitis [14]. The etiology of OLL is usually identifiable: in case of topographically related lesions to amalgam fillings, intake of particular drugs, history
2 2 The Scientific World Journal of chronic graft versus host disease (cgvhd), or systemic diseases [4, 15].OLLisalsoconsideredaspotentiallymalignant disorder [4], although it is still unclear whether its malignant potential differs from OLP [16]. So far, various authors [1, 2, 14, 17] have suggested different parameters that might be indicative for OLP and OLL diagnosis (Table 1). Given that the approach to treatment planning and prognosis of both OLP and OLL usually differs, the suggested parameters define criteria that distinguish these lesions. AsopposedtoratherevidentclinicaldiagnosisofOLP, less obvious, imprecisely or incompletely defined histopathological findings often complicate the confirmation of final diagnosis. Therefore, the aim of this preliminary study was to determine the correlation of histopathological and clinical diagnosis of OLP and OLL and to clarify which histopathologicfeaturesdistinguishbestthesetwodiagnosesandcould improve differential histopathological diagnosis. 2. Materials and Methods The retrospective study group comprised 106 patients who were referred to the Department of Oral Medicine, School of Dental Medicine, University of Zagreb, in the period between January 1, 2012, and December 31, Diagnosis was based on clinical examination and medical and dental history, intake of drugs, and duration of the lesions. Clinical diagnoses were established by experienced (MMS) and trained clinicians (BLB, IB), specialist in oral medicine who usedthesameandconsistentcriteriainscoringlevelsof OLP and OLL. Histopathologic diagnosis was established at a single pathology service that is under supervision of an experienced pathologist (SS). In all patients with OLP and OLL oral mucosa swabs for yeast culture on Sabouraud Agar plates (Sabouraud Dextrose Agar (Becton Dickinson and Co., Cockeysville, USA) were taken, as a routine procedure in all patients with white oral lesions. Those who have had positive finding of yeast superinfection were excluded from the study. Only patients who underwent biopsy were included in the study. The clinical diagnosis of OLP was established in 92 patients (70 female; 22 male; ratio f/m = 3.18 : 1), while in 14 patients OLL was diagnosed (6 female; 8 male, ratio f/m = 0.75 : 1). The mean age of OLP and OLL patients was 56.1 and 64.9 years, respectively. OLP was diagnosed according to criteria described by Kramer et al. [10]: presence of white papules and/or striae usually with bilateral involvement and histopathological signs of liquefaction degeneration in the basal cell layer (degenerative changes to the basal cells) along with the presence of a well-defined band-like zone of inflammatory infiltrate confined to the superficial part of the connective tissue (this infiltrate being composed almost exclusively of lymphocytes and characterized by absence of epithelial dysplasia). Clinical diagnosis of OLL was established due to the presence of hyperkeratotic lesions adjacent to amalgam fillings with asymmetric and mainly unilateral distribution and a patient medical history related to drugs, which provoke lichenoid changes in oral mucosa [16]. Data were analyzed by using Chi-squared test (χ 2 )and differences at P < 0.05 were considered to be significant Histopathology Lichen planus (n =92) Oral lichenoid lesion (n =14) OLP OLL Some elements of OLP Clinical diagnosis SCC Inflammation and keratosis Other Figure 1: The distribution of clinical and histopathologic diagnoses among patients; OLP: oral lichen planus; OLL: oral lichenoid lesions; OSCC: oral squamous cell carcinoma. 3. Results The distribution of clinical and histopathological diagnoses is shown on Figure 1. In 52.2% (48/92) of patients, clinical diagnosis of OLP was histopathologically confirmed, while in 5.4% (5/92) of cases there was a partial confirmation and only some criteria were fulfilled. In 10.9% (10/92) of OLP patients, both clinical and histopathologic diagnosis were concordant, while in 26.1% (24/92) of patients histopathologic diagnosis was nonspecific, being described as inflammation and keratosis. Clinical and histopathological diagnoses coincide in 42.9% (6/14) of OLL patients. According to the histopathologic findings, in clinically diagnosed OLL, in one case the diagnosis of OLP was established, one have had some histopathological elements of OLP, and 4 (28.6%) cases had inflammation and keratosis, while in 2 (14.3%) cases squamous cell carcinoma (OSCC) was diagnosed. The distribution of histopathologic features between OLP and OLL with statistically significant differences between the parameters is indicated in Figure 2. Results showed significantly more eosinophils (P < ), plasma cells (P < ), and granulocytes (P < 0.05)inOLLthanOLP. Other observed parameters such as premature keratosis and inflammatory cell invasion through basal membrane were more frequently found in OLP and OLL in comparison with nonspecific clinical findings of inflammation and keratosis; the difference was significant (P < and P < , resp.). Abundant and diffuse mononuclear infiltration was more frequently found in cases of inflammation and keratosis than in OLP or OLL with statistically significant differences (P < 0.05, P < 0.005, orp < ), but between OLP andolldiagnosisstatisticallysignificantdifferenceinthese parameters was not found. 4. Discussion To establish and confirm OLP and OLL diagnosis by using methods such as clinical examination and histopathological analysis, which are available in everyday clinical practice and among wider population of patients, sometimes represents a diagnostic challenge. Earlier reports have shown that while 4 0
3 The Scientific World Journal 3 Table 1: Histopathological criteria distinctive of OLP and OLL. Diagnosis Epithelium Subepithelium Authors Bilateral presentation of lesions Well-defined subepithelial band of chronic Hyperkeratosis inflammatory infiltrate composed predominantly of Juneja et al., Reduced epithelial thickness lymphocytes 2006 [14] Liquefactive degeneration Absence of eosinophils and neutrophils of the basal cell layer Band shaped inflammatory infiltrate in some or all areas Thornhill et al., 2006 [1] OLP Normal stratification and maturation Basal cell liquefaction is always present Atypia absent Dense band of inflammatory components, chiefly lymphocytes, in the juxtaepithelium Dyskeratotic epithelial cells Civatte bodies are usually found in subepithelial area, at the junction of the lamina propria and epithelial layer Ismail et al [22] OLL OLL related with amalgam filling Compact hyperorthokeratosis, seldom a moderate degree of parakeratosis Thickened stratum granulosum at acrosyringia and acrotrichia, irregular saw-tooth-like epidermal layers Unilateral presentation of lesions Focalparakeratosis,cytoidbodiesinthe cornified layer Thickened stratum granulosum possible, however, with focal interruption of the granular layer, cytoid bodies in the granular layer, necrotic keratinocytes scattered in all epidermal layers Normal stratification basal cell liquefaction may or may not be present Atypia absent Mostly a superficial dermal inflammatory infiltrate; seldom eosinophils acanthosis, necrotic keratinocytes in the lower epidermal layers Poorly differentiated lower border of the subepithelial inflammatory zone Presence of a substantial number of plasma cells in the lymphocytic infiltrate Perivascular infiltrate Increased number of colloid bodies Presence of acute inflammatory cells, such as eosinophils and neutrophils More often a deep dermal infiltrate, especially in nonphotodistributed lichenoid drug eruption; admixture of eosinophils and plasma cells possible (presence of plasma cells is a regular finding in biopsies from mucous membranes independently of the origin of dermatosis) Inflammatory infiltrate located deep to superficial infiltrate in some or all areas Focal perivascular infiltrate Plasma cells, eosinophils, and neutrophils in the connective tissue Lymphoid follicle formations, with mixed inflammatory cells consisting of plasma cells and neutrophils Ziemer, 2014 [17] Juneja et al., 2006 [14] Ziemer, 2014 [17] Thornhill et al., 2006 [1] Ismail et al [22] OLL related with drugs Basal cell liquefaction may not be present Extensive degeneration in the lower prickle cell layer, prompting spongiotic vesicle formation Basal cell liquefaction is usually present Atypia absent Apoptotic and colloid body formation are evident OLP: oral lichen planus; OLL: oral lichenoid lesions. Predominant formation of lymphoid follicles chiefly consisting of plasma cells and neutrophils Dense inflammatory cells in the stroma Infiltrate is not band-like but extends to the deeper stroma inflammatory cells predominated by plasma cells and eosinophils Perivascular cuffing of inflammatory cells is evident Infiltrate is often not band-like but extends to the deeper stroma, with plasma cells and eosinophils which predominate the inflammatory component Hiremath et al., 2011 [2] Ismail et al [22] Hiremath et al., 2011 [2]
4 4 The Scientific World Journal 32.7% 37.5% 35.7% 57.1% 75.0% 57.1% 16.3% 6.3% 25.0% 53.1% 37.5% 4.1% 77.6% 87.5% 60.7% 16.3% 3.6% 40.8% 31.3% 21.4% 91.8% 87.5% 5 6.1% 6.3% 46.4% 2.0% 12.5% 25.0% 4.1% 6.3% 17.9% 4.1% 62.5% 3.6% 2.0% 62.5% 17.9% 8.2% 37.5% 14.3% Hyperkeratosis Parakeratosis Orthokeratosis 79.6% 87.5% 21.4% Premature keratosis Keratinisation disorder Acanthosis of the spinous layer Vacuolisation Epithelial extensions Mononuclear cell infiltrate-abundant Mononuclear cell infiltrate-scarce Mononuclear cell infiltrate-diffuse Mononuclear cell infiltrate-focal Eosinophils Plasma cells Granulocytes Inflammatory cell invasion through basal membrane OLP OLL Inflammation and keratosis P 0.05 P P Figure 2: The distribution of histopathologic criteria between the diagnosis oral lichen planus (OLP) and oral lichenoid lesion (OLL). clinical diagnosis depends on a clinician interpretation [11, 14], histopathological diagnosis is strictly dependent on a pathologist interpretation as well [2, 12], but also the choice of biopsy area [18], clinical severity of the disease, activity or remission of the disease, and the clinical type of OLP (reticular lesions are considered easier for histopathological confirmation) [2, 19]. Pathologists lack of information on clinical features and distribution of lesions could also influence their judgment [11, 12, 20]. Having in mind these parameters, which could affect the final histopathologic interpretation, the results of our study could partially be explained by possible interobserver bias as the patients were examined by different clinicians, and histopathological diagnosis was done by different pathologists. This should be taken into account in the future prospective studies. Therefore, due to many variables affecting diagnosis, histopathological finding is insufficiently reproducible [2, 12]. Theresultsofthisstudyshowthatclinicaldiagnoses of OLP and OLL have been confirmed histopathologically in 52.2% patients with OLP and 42.9% patients with OLL. These results are similar to those shown by van der Meij and van der Waal [11] according to whom 42% of OLP clinically diagnosed cases were not confirmed by histopathology. Interestingly, authors also showed that a clinician s consensus in patients with clear histopathological confirmation of OLP was achieved in only 50% of cases. Thornhill et al. [1] showed an overall correlation of clinical and histopathologicaldiagnosesofolpandollbasedonthefindingsoffive different pathologists. Difficulties reported in distinguishing these lesions in histological features were related to amalgam fillings in only 36% of cases. These results are similar to those of Al-ani [20] who found clinical and pathological correlation ofolpinonly38.5%.radetal.[21]foundsignificantlyhigher clinical and pathological correlation of OLP (93.9%) in cases in which WHO modified criteria were applied. The results of Rad et al. [21]arepromisingbutshouldbevalidatedinalarger group of patients, applying strictly validated and reproducible criteria [11]. According to the literature review, there is a lack of studies, which applied WHO modified criteria in determining correlation of clinical and histopathological diagnosis of OLP. It would be reasonable to expect that the overall prevalence of OLP in the observed population would be lower andtheprevalenceofollhigherifwhomodifiedcriteria for establishing diagnosis were applied. This could possibly affect an expected malignant transformation rate in both
5 The Scientific World Journal 5 OLP and OLL showing that OLL is more prone to malignant transformation than OLP as already documented by some authors [8, 22]andalsoshowninourresults. Van der Meij et al. [23, 24] havefoundinprolonged follow-up that patients with OLL have an increased risk for malignant transformation compared to OLP and that this is more likely to occur in erosive lesions. The malignant transformation could be attributable to the extrinsic factors [24], other than alcohol and tobacco, use of particular antihypertensive [25] and antiretroviraldrugs [26], andinfection with strains of Candida albicans [27], which all can enhance malignant transformation in oral lesions. In our two patients with oral SCC we did not found any of the listed risk factors. This finding emphasises the importance of regular followup of patients with oral lesions and eventually biopsies to confirm or refute clinical diagnosis of OLL or OLP. Gannot et al. [28]haveshownthattissuechangestowards malignancy had a distinct lymphocyte profile: the number of CD4, CD8, and B cells is significantly higher in inflammatory infiltrate in moderate and severe dysplasia and SCC, compared to mild dysplasia and hyperkeratosis. In addition, inflammatory cell infiltration has been considered in cancer progression. Particularly, CD8 and NK cell are increased in oral SCC since they have cytotoxic immune response against neoplastic cells [29]. Several authors so far have suggested histopathologic criteria, which should be distinctive in achieving both OLP and OLL diagnoses (Table 1). In their studies, they found differences in some parameters between OLP and OLL, but in order to accept these findings as a standard protocol, a larger number of patients should be examined as already suggested by some authors. All authors agree that findings of plasma cells, eosinophils, and neutrophils in inflammatory infiltrate can be distinctive for OLL compared to OLP, which is in consensus with our results (Figure 2). Therefore, we consider that this type of cells should be a certain diagnostic feature in histopathologic differentiation between OLP and OLL given that these cells are relevant in nonimmediate allergic reactions, particularly those induced by drugs [30, 31], where OLL is classified. Unlike other findings (Table 1), we did not observed statistically significant differences in other histopathological criteria between OLP and OLL. These results therefore may enhance a closer collaboration with pathologists in order to get a more precise description of histopathological features, particularly cellular composition of mononuclear infiltrate. This consequently should improve the list of parameters, which pathologists may consider relevant for either diagnosis, therefore avoiding misinterpretation due to different criteria, which usually affect the results. 5. Conclusion OLP and OLL are clinically similar but diagnostically insufficiently distinguished lesions. Their prognosis and treatment may vary. To achieve accurate histopathologic diagnosis it is mandatory to define the type of cells in mononuclear infiltrate, which can be interpreted in accordance with clinical findings and a patient history. Currently accepted diagnostic criteria in diagnosing OLP and OLL should be modified and modifications should be validated in a larger number of patients. The results of this study, which is in accordance with similar reports from the literature, have shown that histopathological findings coincide with clinical diagnosis in approximately only 50% of cases and as such cannot always be exclusive in the final interpretation. Based on the results of this study, prominent diagnostic histopathological features in distinguishing between OLP and OLL are the type of cells in the mononuclear cell infiltrate, that is, eosinophils, plasma cells, and granulocytes. Conflict of Interests The authors declare that there is no conflict of interests regarding the publication of this paper. Acknowledgment This research has been supported by the National Science Foundation of Croatia. References [1] M. H. Thornhill, V. Sankar, X.-J. Xu et al., The role of histopathological characteristics in distinguishing amalgamassociated oral lichenoid reactions and oral lichen planus, JournalofOralPathologyandMedicine,vol.35,no.4,pp , [2]S.K.S.Hiremath,A.D.Kale,andS.Charantimath, Oral lichenoid lesions: clinico-pathological mimicry and its diagnostic implications, IndianJournalofDentalResearch,vol.22,no. 6, pp , [3]B.L.Brzak,M.Mravak-Stipetić, I. Canjuga et al., The frequency and malignant transformation rate of oral lichen planus and leukoplakia a retrospective study, Collegium Antropologicum, vol. 36, no. 3, pp , [4] I. van der Waal, Oral lichen planus and oral lichenoid lesions; a critical appraisal with emphasis on the diagnostic aspects, Medicina Oral, Patologia Oral y Cirugia Bucal,vol.14,no.7,pp. E310 E314, [5] C. Scully and M. Carrozzo, Oral mucosal disease: Lichen planus, British Oral and Maxillofacial Surgery, vol. 46,no.1,pp.15 21,2008. [6]F.A.C.G.DeSousaandL.E.B.Rosa, Orallichenplanus: clinical and histopathological considerations, Brazilian Journal of Otorhinolaryngology,vol.74,no.2,pp ,2008. [7]D.J.Krutchkoff,L.Cutler,andS.Laskowski, Orallichen planus. The evidence regarding potential malignant transformation, JournalofOralPathology, vol. 7, no.1,pp. 1 7, [8] E. Eisenberg, Oral lichen planus: a benign lesion, OralandMaxillofacialSurgery,vol.58,no.11,pp , [9] I. van der Waal, Potentially malignant disorders of the oral and oropharyngeal mucosa; terminology, classification and present concepts of management, Oral Oncology, vol. 45, no. 4-5, pp , [10] I. R. H. Kramer, R. B. Lucas, J. J. Pindborg, and L. H. Sobin, Definition of leukoplakia and related lesions: an aid to
6 6 The Scientific World Journal studies on oral precancer, Oral Surgery Oral Medicine and Oral Pathology,vol.46,no.4,pp ,1978. [11] E. H. van der Meij and I. van der Waal, Lack of clinicopathologic correlation in the diagnosis of oral lichen planus based on thepresentlyavailablediagnosticcriteriaandsuggestionsfor modifications, JournalofOralPathologyandMedicine,vol.32, no. 9, pp , [12] S.-O. Piboonniyom, N. Treister, W. Pitiphat, and S.-B. Woo, Scoring system for monitoring oral lichenoid lesions: a preliminary study, Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology and Endodontology,vol.99,no.6,pp ,2005. [13] D.Eisen,M.Carrozzo,J.-V.B.Sebastian,andK.Thongprasom, Number V. Oral lichen planus: clinical features and management, Oral Diseases,vol. 11,no.6, pp , [14]M.Juneja,S.Mahajan,N.N.Rao,T.George,andK.Boaz, Histochemical analysis of pathological alterations in oral lichen planus and oral lichenoid lesions., oral science, vol.48,no.4,pp ,2006. [15] M.-J. Cobos-Fuentes, Á. Martínez-Sahuquillo-Márquez, I. Gallardo-Castillo, J.-R. Armas-Padrón, A. Moreno-Fernández, and P. Bullón-Fernández, Oral lichenoid lesions related to contact with dental materials: a literature review, Medicina Oral, Patologia Oral y Cirugia Bucal, vol.14,no.10,pp.e514 e520, [16] S. G. Fitzpatrick, S. A. Hirsch, and S. C. Gordon, The malignant transformation of oral lichen planus and oral lichenoid lesions: a systematic review, The the American Dental Association,vol.145,no.1,pp.45 56,2014. [17] M. Ziemer, Delayed-type cutaneous drug reactions. Pathogenesis, clinical features and histology, Der Hautarzt, vol. 65, no. 5, pp , May [18] G. W. Gynther, B. Rozell, and A. Heimdahl, Direct oral microscopy and its value in diagnosing mucosal lesions a pilot study, Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontics, vol. 90, no. 2, pp , [19] D. J. Zegarelli, Lichen planus: a simple and reliable biopsy technique, JournalofOralMedicine, vol. 36, no. 1, pp , [20] L. S. Al-ani, Oral lichen planus clinical study with the clinicopathological correlation in the diagnosis of O. L. P, College Dentistry,vol.17,no.1,pp.57 60,2005. [21] M. Rad, M. A. Hashemipoor, A. Mojtahedi et al., Correlation between clinical and histopathologic diagnoses of oral lichen planus based on modified WHO diagnostic criteria, Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology and Endodontology,vol.107,no.6,pp ,2009. [22] S. B. Ismail, S. K. S. Kumar, and R. B. Zain, Oral lichen planus and lichenoid reactions: etiopathogenesis, diagnosis, management and malignant transformation, Oral Science,vol.49,no.2,pp ,2007. [23] E. H. van der Meij, K.-P. Schepman, and I. van der Waal, The possible premalignant character of oral lichen planus and oral lichenoid lesions: a prospective study, Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontics,vol. 96,no.2,pp ,2003. [24] E. H. van der Meij, H. Mast, and I. van der Waal, The possible premalignant character of oral lichen planus and oral lichenoid lesions: A prospective five-year follow-up study of 192 patients, Oral Oncology,vol.43,no.8,pp ,2007. [25] G. D. Friedman, M. M. Asgari, E. M. Warton, J. Chan, and L. A. Habel, Antihypertensive drugs and lip cancer in non-hispanic whites, Archives of Internal Medicine,vol.172,no.16,pp , [26] P. Arirachakaran, M. Hanvanich, P. Kuysakorn, and K. Thongprasom, Antiretroviral drug-associated oral lichenoid reaction in HIV patient: a case report, International Dentistry, vol. 2010, Article ID , 4 pages, [27] P. Krogh, B. Hald, and P. Holmstrup, Possible mycological etiology of oral mucosal cancer: catalytic potential of infecting Candida albicans and other yeasts in production of N- nitrosobenzylmethylamine, Carcinogenesis, vol. 8, no. 10, pp , [28] G. Gannot, I. Gannot, H. Vered, A. Buchner, and Y. Keisari, Increase in immune cell infiltration with progression of oral epithelium from hyperkeratosis to dysplasia and carcinoma, British Cancer, vol. 86, no. 9, pp , [29] E. Zancope, N. L. Costa, A. P. Junqueira-Kipnis et al., Differential infiltration of CD8 + andnkcellsinlipandoral cavity squamous cell carcinoma, JournalofOralPathologyand Medicine, vol. 39, no. 2, pp , [30] W. J. Pichler and N. Yawalkar, Allergic reactions to drugs: involvement of T cells, Thorax, vol. 55, no. 2, pp. S61 S65, [31] M. J. Torres, C. Mayorga, and M. Blanca, Nonimmediate allergic reactions induced by drugs: pathogenesis and diagnostic tests, JournalofInvestigationalAllergologyandClinical Immunology,vol.19,no.2,pp.80 90,2009.
7 Advances in Preventive Medicine The Scientific World Journal Case Reports in Dentistry International Dentistry Scientifica Pain Research and Treatment International Biomaterials Environmental and Public Health Submit your manuscripts at Oral Implants Computational and Mathematical Methods in Medicine Advances in Oral Oncology Anesthesiology Research and Practice Orthopedics Drug Delivery Dental Surgery BioMed Research International International Oral Diseases Endocrinology Radiology Research and Practice
Oral Manifestations of Dermatologic Disease: A Focus on Lichenoid Lesions. Proceedings of the NASHNP Companion Meeting, March, 2011, San Antonio, TX
 1 Oral Manifestations of Dermatologic Disease: A Focus on Lichenoid Lesions Proceedings of the NASHNP Companion Meeting, March, 2011, San Antonio, TX Susan Müller, DMD, MS Professor Department of Pathology
1 Oral Manifestations of Dermatologic Disease: A Focus on Lichenoid Lesions Proceedings of the NASHNP Companion Meeting, March, 2011, San Antonio, TX Susan Müller, DMD, MS Professor Department of Pathology
A QUANTITATIVE EVALUATION OF EPITHELIUM AND INFLAMMATORY INFILTRATE OF LICHEN PLANUS AND LICHENOID REACTIONS
 A QUANTITATIVE EVALUATION OF EPITHELIUM AND INFLAMMATORY INFILTRATE OF LICHEN PLANUS AND LICHENOID REACTIONS 1 2 Usha Balan Nitin Gonsalves Maji Jose 1 Departments of Oral & Maxillofacial Pathology, KMCT
A QUANTITATIVE EVALUATION OF EPITHELIUM AND INFLAMMATORY INFILTRATE OF LICHEN PLANUS AND LICHENOID REACTIONS 1 2 Usha Balan Nitin Gonsalves Maji Jose 1 Departments of Oral & Maxillofacial Pathology, KMCT
A DIAGNOSTIC DILEMMA: ORAL LICHEN PLANUS OR LICHENOID REACTION - A SERIES OF CASE REPORTS
 CASE REPORT A DIAGNOSTIC DILEMMA: ORAL LICHEN PLANUS OR LICHENOID REACTION - A SERIES OF CASE REPORTS Chanchal Sareen 1, Aparna Pathak 2, Puneet Ahuja 3, Moulshree Kohli 4 1 Senior Lecturer, 3 Prof & Head,
CASE REPORT A DIAGNOSTIC DILEMMA: ORAL LICHEN PLANUS OR LICHENOID REACTION - A SERIES OF CASE REPORTS Chanchal Sareen 1, Aparna Pathak 2, Puneet Ahuja 3, Moulshree Kohli 4 1 Senior Lecturer, 3 Prof & Head,
04/09/2018. Squamous Cell Neoplasia and Precursor Lesions. Agenda. Squamous Dysplasia. Squamo-proliferative lesions. Architectural features
 Squamous Cell Neoplasia and Precursor Lesions Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical
Squamous Cell Neoplasia and Precursor Lesions Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical
Squamous Cell Neoplasia and Precursor Lesions
 Squamous Cell Neoplasia and Precursor Lesions Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical
Squamous Cell Neoplasia and Precursor Lesions Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical
Premalignant lesions may expose to a promoting. factor & may be induced to undergo malignant. Carcinoma in situ displays the cytologic features of
 بسم رلاهللا Def. Premalignant lesions may expose to a promoting factor & may be induced to undergo malignant transformation. Carcinoma in situ displays the cytologic features of malignancy without invasion
بسم رلاهللا Def. Premalignant lesions may expose to a promoting factor & may be induced to undergo malignant transformation. Carcinoma in situ displays the cytologic features of malignancy without invasion
Histopathological Findings in Oral Lichen Planus: A Three-Year Report from Western Iran
 Journal of Research in Medical and Dental Science 2018, Volume 6, Issue 1, Page No: 274-278 Copyright CC BY-NC-ND 4.0 Available Online at: www.jrmds.in eissn No. 2347-2367: pissn No. 2347-2545 Histopathological
Journal of Research in Medical and Dental Science 2018, Volume 6, Issue 1, Page No: 274-278 Copyright CC BY-NC-ND 4.0 Available Online at: www.jrmds.in eissn No. 2347-2367: pissn No. 2347-2545 Histopathological
Smoking Habits Among Patients Diagnosed with Oral Lichen Planus
 TOBACCO INDUCED DISEASES Vol. 2, No. 2: 103-108 (2004) PTID Society Smoking Habits Among Patients Diagnosed with Oral Lichen Planus Meir Gorsky, 1 Joel B. Epstein, 2 Haya Hasson-Kanfi, 1 Eliezer Kaufman
TOBACCO INDUCED DISEASES Vol. 2, No. 2: 103-108 (2004) PTID Society Smoking Habits Among Patients Diagnosed with Oral Lichen Planus Meir Gorsky, 1 Joel B. Epstein, 2 Haya Hasson-Kanfi, 1 Eliezer Kaufman
Quantification of Colloid Bodies in Oral Lichen Planus and Oral Lichenoid Reaction - A Histochemical Study
 Journal section: Oral Medicine and Pathology Publication Types: Research doi:0.437/jced.3.e207 Quantification of Colloid Bodies in Oral Lichen Planus and Oral Lichenoid Reaction - A Histochemical Study
Journal section: Oral Medicine and Pathology Publication Types: Research doi:0.437/jced.3.e207 Quantification of Colloid Bodies in Oral Lichen Planus and Oral Lichenoid Reaction - A Histochemical Study
JMSCR Vol 05 Issue 10 Page October 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i10.125 Histomorphological Study of Lichen Planus
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i10.125 Histomorphological Study of Lichen Planus
Clinical behaviour of malignant transforming oral lichen planus
 EJSO 2002; 28: 838±843 doi:10.1053/ejso.2002.1302, available online at http://www.idealibrary.com on 1 Clinical behaviour of malignant transforming oral lichen planus M. D. Mignogna*, L. Lo Russo*, S.
EJSO 2002; 28: 838±843 doi:10.1053/ejso.2002.1302, available online at http://www.idealibrary.com on 1 Clinical behaviour of malignant transforming oral lichen planus M. D. Mignogna*, L. Lo Russo*, S.
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more
 Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Dysplasia, Mimics and Other Controversies
 Dysplasia, Mimics and Other Controversies Mary S. Richardson, MD Dept. of Pathology Medical University of South Carolina Charleston, SC Notice of Faculty Disclosure In accordance with ACGME guidelines,
Dysplasia, Mimics and Other Controversies Mary S. Richardson, MD Dept. of Pathology Medical University of South Carolina Charleston, SC Notice of Faculty Disclosure In accordance with ACGME guidelines,
Epidemiology of Oral Lichen Planus in a Cohort of South Indian Population: A Retrospective Study
 JOURNAL OF CANCER PREVENTION Vol. 21, No. 1, March 2016 http://crossmark.crossref.org/dialog/?doi=10.15430/jcp.2016.21.1.55&domain=pdf&date_stamp=2016-3-30 http://dx.doi.org/10.15430/jcp.2016.21.1.55 pissn
JOURNAL OF CANCER PREVENTION Vol. 21, No. 1, March 2016 http://crossmark.crossref.org/dialog/?doi=10.15430/jcp.2016.21.1.55&domain=pdf&date_stamp=2016-3-30 http://dx.doi.org/10.15430/jcp.2016.21.1.55 pissn
Actinic keratosis (AK): Dr Sarma s simple guide
 Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
lichenoid lesions related to contact with dental materials: A literature review.
 Journal section: Oral Medicine and Pathology Publication Types: Review doi:10.4317/medoral.14.e514 Oral lichenoid lesions related to contact with dental materials: A literature review María-José Cobos-Fuentes
Journal section: Oral Medicine and Pathology Publication Types: Review doi:10.4317/medoral.14.e514 Oral lichenoid lesions related to contact with dental materials: A literature review María-José Cobos-Fuentes
الطلاوة = Leukoplakia LEUKOPLAKIA
 LEUKOPLAKIA Leukoplakia is a clinical term that refers to a predominantly white lesion of the oral mucosa that cannot be rubbed off or characterized by any other definable lesion or known disease. 130
LEUKOPLAKIA Leukoplakia is a clinical term that refers to a predominantly white lesion of the oral mucosa that cannot be rubbed off or characterized by any other definable lesion or known disease. 130
Histopathological evaluation of oral lichen planus
 Histopathological evaluation of oral lichen planus Layla S. Yas, B.D.S. M.Sc. (1) ABSTRACT Background: Oral lichen planus( OLP) is a chronic inflammatory disorder affecting mucosal surfaces, which can
Histopathological evaluation of oral lichen planus Layla S. Yas, B.D.S. M.Sc. (1) ABSTRACT Background: Oral lichen planus( OLP) is a chronic inflammatory disorder affecting mucosal surfaces, which can
American Journal of Cancer Science
 American Journal of Cancer Science http://ivyunion.org/index.php/ajcs/ Akerzoul N et al. American Journals of Cancer Science 2015, 5:63-77 Page 1 of 6 Case Report Malignant Transformation of Erosive Oral
American Journal of Cancer Science http://ivyunion.org/index.php/ajcs/ Akerzoul N et al. American Journals of Cancer Science 2015, 5:63-77 Page 1 of 6 Case Report Malignant Transformation of Erosive Oral
PACIFIC JOURNAL OF MEDICAL SCIENCES {Formerly: Medical Sciences Bulletin} ISSN:
 PACIFIC JOURNAL OF MEDICAL SCIENCES {Formerly: Medical Sciences Bulletin} ISSN: 2072 1625 Pac. J. Med. Sci. (PJMS) www.pacjmedsci.com. Email: pacjmedsci@gmail.com. EROSIVE LICHEN PLANUS A CASE REPORT *Prathima
PACIFIC JOURNAL OF MEDICAL SCIENCES {Formerly: Medical Sciences Bulletin} ISSN: 2072 1625 Pac. J. Med. Sci. (PJMS) www.pacjmedsci.com. Email: pacjmedsci@gmail.com. EROSIVE LICHEN PLANUS A CASE REPORT *Prathima
Original Article. Direct Immunofluorescence in Clinically Diagnosed Oral Lichen Planus
 JOMP Journal of Oral Medicine and Pain Original Article pissn 2288-9272 eissn 2383-8493 J Oral Med Pain 2016;41(1):16-20 http://dx.doi.org/10.14476/jomp.2016.41.1.16 Direct Immunofluorescence in Clinically
JOMP Journal of Oral Medicine and Pain Original Article pissn 2288-9272 eissn 2383-8493 J Oral Med Pain 2016;41(1):16-20 http://dx.doi.org/10.14476/jomp.2016.41.1.16 Direct Immunofluorescence in Clinically
IJCMR 1. Jay Ashokkumar Pandya, 1 Srikant Natarajan, 2 Karen Boaz, 3 Nidhi Manaktala, 4 Amitha J Lewis, 5 Supriya Nikita Kapila 1 ABSTRACT
 IJCMR 1 ORIGINAL RESEARCH Assessment And Comparison of Keratin, Epithelial And Inflammatory Thickness In Oral Lichen Planus And Oral Reaction Using Picrosirius Red Stain Jay Ashokkumar Pandya, 1 Srikant
IJCMR 1 ORIGINAL RESEARCH Assessment And Comparison of Keratin, Epithelial And Inflammatory Thickness In Oral Lichen Planus And Oral Reaction Using Picrosirius Red Stain Jay Ashokkumar Pandya, 1 Srikant
WHITE LESIONS OF THE ORAL CAVITY - diagnostic appraisal & management strategies
 WHITE LESIONS OF THE ORAL CAVITY - diagnostic appraisal & management strategies * Joshy V.R ** Hari.S * Reader, Dept of Oral Pathology, Yenepoya Dental College, Yenepoya University, Mangalore 575 018.
WHITE LESIONS OF THE ORAL CAVITY - diagnostic appraisal & management strategies * Joshy V.R ** Hari.S * Reader, Dept of Oral Pathology, Yenepoya Dental College, Yenepoya University, Mangalore 575 018.
Histopathology: skin pathology
 Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
buccal mucosa is well maintained without a recurrence (Fig. (Fig. 1A). The tentative diagnosis was oral lichenoid lesion
 JOMP Journal of Oral Medicine and Pain Case Report pissn 2288-9272 eissn 2383-8493 J Oral Med Pain 2015;40(4):163-168 http://dx.doi.org/10.14476/jomp.2015.40.4.163 Lichenoid Dysplasia Misdiagnosed as Oral
JOMP Journal of Oral Medicine and Pain Case Report pissn 2288-9272 eissn 2383-8493 J Oral Med Pain 2015;40(4):163-168 http://dx.doi.org/10.14476/jomp.2015.40.4.163 Lichenoid Dysplasia Misdiagnosed as Oral
Oral lichenoid disease as a premalignant condition: The controversies and the unknown
 Journal section: Oral Medicine and Pathology Publication Types: Review as a premalignant condition: The controversies and the unknown Dionisio-Alejandro Cortés-Ramírez 1, Maria-Luisa Gainza-Cirauqui 1,
Journal section: Oral Medicine and Pathology Publication Types: Review as a premalignant condition: The controversies and the unknown Dionisio-Alejandro Cortés-Ramírez 1, Maria-Luisa Gainza-Cirauqui 1,
UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA FACULTY OF MEDICINE DOCTORAL THESIS SUMMARY
 UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA FACULTY OF MEDICINE DOCTORAL THESIS SUMMARY CLINICAL, HISTOPATHOLOGICAL AND IMMUNOHISTOCHEMICAL STUDY OF THE EPITHELIAL PRECANCEROUS LESIONS PRECURSORS OF
UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA FACULTY OF MEDICINE DOCTORAL THESIS SUMMARY CLINICAL, HISTOPATHOLOGICAL AND IMMUNOHISTOCHEMICAL STUDY OF THE EPITHELIAL PRECANCEROUS LESIONS PRECURSORS OF
Kharidi U.A, Kodgi A, Biradar A, Kulkarni A
 Case Report Malignant Conversion of Oral Lichen Planus - A Case Report 1 2 3 4 Kharidi U.A, Kodgi A, Biradar A, Kulkarni A Kharidi U.A, Kodgi A, Biradar A, Kulkarni A. Malignant Conversion of Oral Lichen
Case Report Malignant Conversion of Oral Lichen Planus - A Case Report 1 2 3 4 Kharidi U.A, Kodgi A, Biradar A, Kulkarni A Kharidi U.A, Kodgi A, Biradar A, Kulkarni A. Malignant Conversion of Oral Lichen
Pathology of the skin. 2nd Department of Pathology, Semmelweis University
 Pathology of the skin 2nd Department of Pathology, Semmelweis University Histology of the skin Epidermis: Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis: papillary and reticular
Pathology of the skin 2nd Department of Pathology, Semmelweis University Histology of the skin Epidermis: Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis: papillary and reticular
Clinically Microscopically Pathogenesis: autoimmune not lifetime
 Vulvar Diseases: Can be divided to non-neoplastic and neoplastic diseases. The neoplastic diseases are much less common. Of those, squamous cell carcinoma is the most common. most common in postmenopausal
Vulvar Diseases: Can be divided to non-neoplastic and neoplastic diseases. The neoplastic diseases are much less common. Of those, squamous cell carcinoma is the most common. most common in postmenopausal
Case No. 5; Slide No. B13/8956/2
 Interface diseases Case No. 5; Slide No. B13/8956/2 Histological findings Severe hydropic vacuolation of epidermal and follicular basal cells/ interface dermatitis Multifocally apoptotic keratinocytes
Interface diseases Case No. 5; Slide No. B13/8956/2 Histological findings Severe hydropic vacuolation of epidermal and follicular basal cells/ interface dermatitis Multifocally apoptotic keratinocytes
Basal cell carcinoma 5/28/2011
 Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
Original Research Article
 ASSESSMENT OF HUMAN PAPILLOMA VIRUS SUBTYPES BY POLYMERASE CHAIN REACTION AND THEIR IMPACT ON THE DEGREE OF DYSPLASIA IN ORAL LEUKOPLAKIA Submitted on: XXXX Dr. N. Kannan, Dr Teja Srinivas, Dr. Rakesh
ASSESSMENT OF HUMAN PAPILLOMA VIRUS SUBTYPES BY POLYMERASE CHAIN REACTION AND THEIR IMPACT ON THE DEGREE OF DYSPLASIA IN ORAL LEUKOPLAKIA Submitted on: XXXX Dr. N. Kannan, Dr Teja Srinivas, Dr. Rakesh
Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor
 Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Pathology of the skin. Dr Fónyad László, 1sz. Patológiai és Kísérleti Rákkutató Intézet, SE
 Pathology of the skin Dr Fónyad László, 1sz. Patológiai és Kísérleti Rákkutató Intézet, SE The skin Biggest organ Kb. 1.8 nm Kb. 10 kg Most frequent site for tumor development (BCC) Pathology of the skin
Pathology of the skin Dr Fónyad László, 1sz. Patológiai és Kísérleti Rákkutató Intézet, SE The skin Biggest organ Kb. 1.8 nm Kb. 10 kg Most frequent site for tumor development (BCC) Pathology of the skin
Diagnostic difficulties with lesions of the oral mucosa
 BDIAP London, November 2010 School of Clinical Dentistry University of Sheffield Diagnostic difficulties with lesions of the oral mucosa Paul M Speight Dept Oral & Maxillofacial Pathology University of
BDIAP London, November 2010 School of Clinical Dentistry University of Sheffield Diagnostic difficulties with lesions of the oral mucosa Paul M Speight Dept Oral & Maxillofacial Pathology University of
LARYNGEAL DYSPLASIA. Tomas Fernandez M; 3 rd year ENT resident, Son Espases University Hospital
 LARYNGEAL DYSPLASIA Tomas Fernandez M; 3 rd year ENT resident, Son Espases University Hospital INTRODUCTION Laryngeal cancer constitutes 1-2% of all malignancies diagnosed worldwide Survival is related
LARYNGEAL DYSPLASIA Tomas Fernandez M; 3 rd year ENT resident, Son Espases University Hospital INTRODUCTION Laryngeal cancer constitutes 1-2% of all malignancies diagnosed worldwide Survival is related
Histochemical analysis of pathological alterations in oral lichen planus and oral lichenoid lesions
 185 Journal of Oral Science, Vol. 48, No. 4, 185-193, 2006 Original Histochemical analysis of pathological alterations in oral lichen planus and oral lichenoid lesions Manish Juneja, Sumita Mahajan, Nirmala
185 Journal of Oral Science, Vol. 48, No. 4, 185-193, 2006 Original Histochemical analysis of pathological alterations in oral lichen planus and oral lichenoid lesions Manish Juneja, Sumita Mahajan, Nirmala
NEOPLASMS OF THE SURFACE EPITHELIUM (KERATINOCYTES)
 NEOPLASMS OF THE SURFACE EPITHELIUM (KERATINOCYTES) Papillary Lesions Precancerous Lesions Keratinocyte Proliferations Carcinomas Melanotic Lesions Melanomas Normal Mucosa Keratin layer Spinous layer Basal
NEOPLASMS OF THE SURFACE EPITHELIUM (KERATINOCYTES) Papillary Lesions Precancerous Lesions Keratinocyte Proliferations Carcinomas Melanotic Lesions Melanomas Normal Mucosa Keratin layer Spinous layer Basal
Childhood Oral Lichen Planus: Report of Two Cases
 Case Report Sageena George 1, Sheen Ann John 2, Anandaraj S 3, Jyoti Sumi Issac 4, Anoop Harris 5, Reshmi J 6 1 Professor, Department of Pedodontics and Preventive Dentistry, PMS College of Dental Science
Case Report Sageena George 1, Sheen Ann John 2, Anandaraj S 3, Jyoti Sumi Issac 4, Anoop Harris 5, Reshmi J 6 1 Professor, Department of Pedodontics and Preventive Dentistry, PMS College of Dental Science
Oral Lichen Planus A Case Report with Current Trends Review of Literature
 ISSN 2455-4499; Vol.05, Issue 01 (2016) Institute of Research Advances Pg. no. 6-17 http://research-advances.org/index.php/irajas Oral Lichen Planus A Case Report with Current Trends Review of Literature
ISSN 2455-4499; Vol.05, Issue 01 (2016) Institute of Research Advances Pg. no. 6-17 http://research-advances.org/index.php/irajas Oral Lichen Planus A Case Report with Current Trends Review of Literature
Benign Lichenoid Keratosis
 Benign Lichenoid Keratosis ALAN F. FRIGY, M.D. AND PHILIP H. COOPER, M.D. The microscopic spectrum of benign lichenoid keratosis (BLK) was studied by examination of 30 examples. BLK consists of a segment
Benign Lichenoid Keratosis ALAN F. FRIGY, M.D. AND PHILIP H. COOPER, M.D. The microscopic spectrum of benign lichenoid keratosis (BLK) was studied by examination of 30 examples. BLK consists of a segment
Research Article Quantitative Analysis of Salivary TNF-α in Oral Lichen Planus Patients
 International Dentistry Volume 2015, Article ID 283465, 5 pages http://dx.doi.org/10.1155/2015/283465 Research Article Quantitative Analysis of Salivary TNF-α in Oral Lichen Planus Patients T. Malarkodi
International Dentistry Volume 2015, Article ID 283465, 5 pages http://dx.doi.org/10.1155/2015/283465 Research Article Quantitative Analysis of Salivary TNF-α in Oral Lichen Planus Patients T. Malarkodi
Clinical profile of 108 cases of oral lichen planus
 43 Journal of Oral Science, Vol. 58, No. 1, 43-47, 2016 Original Clinical profile of 108 cases of oral lichen planus Pritam K. Mankapure, Jayanti G. Humbe, Mandakini S. Mandale, and Jyoti D. Bhavthankar
43 Journal of Oral Science, Vol. 58, No. 1, 43-47, 2016 Original Clinical profile of 108 cases of oral lichen planus Pritam K. Mankapure, Jayanti G. Humbe, Mandakini S. Mandale, and Jyoti D. Bhavthankar
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB. Friday, February 12, :30 am 11:00 am
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 12, 2012 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 12, 2012 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
Salivary Glands 3/7/2017
 Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
LEUKOPLAKIA Definition Epidemiology Clinical presentation
 LEUKOPLAKIA Definition Leukoplakia is the most common premalignant or "potentially malignant" lesion of the oral mucosa. Leukoplakia is a predominantly white lesion of the oral mucosa than cannot be clinicopathologically
LEUKOPLAKIA Definition Leukoplakia is the most common premalignant or "potentially malignant" lesion of the oral mucosa. Leukoplakia is a predominantly white lesion of the oral mucosa than cannot be clinicopathologically
Chapter 6 Squamous Cell Carcinoma: Variants and Challenges
 Chapter 6 Squamous Cell Carcinoma: Variants and Challenges Michael B. Morgan EPIDEMIOLOGY: Second most common skin cancer, rare in the dark-skinned races. ETIOLOGY: Ultraviolet light, HPV infection. PATHOGENESIS:
Chapter 6 Squamous Cell Carcinoma: Variants and Challenges Michael B. Morgan EPIDEMIOLOGY: Second most common skin cancer, rare in the dark-skinned races. ETIOLOGY: Ultraviolet light, HPV infection. PATHOGENESIS:
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation. Dermatopathology Specialists Needed. Changing Trends
 Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Gastrooesophageal reflux disease. Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia
 Gastrooesophageal reflux disease Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia Reflux esophagitis (RE) GERD: a spectrum of clinical conditions and histologic alterations resulting
Gastrooesophageal reflux disease Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia Reflux esophagitis (RE) GERD: a spectrum of clinical conditions and histologic alterations resulting
Malignant Transformation in Leukoplakia and its Associated Factors in Southern Iran: A Hospital Based Experience
 Iran J Public Health, Vol. 46, No.8, Aug 2017, pp.1110-1117 Original Article Malignant Transformation in Leukoplakia and its Associated Factors in Southern Iran: A Hospital Based Experience Alireza BARFI
Iran J Public Health, Vol. 46, No.8, Aug 2017, pp.1110-1117 Original Article Malignant Transformation in Leukoplakia and its Associated Factors in Southern Iran: A Hospital Based Experience Alireza BARFI
Autoimmune Diseases with Oral Manifestations
 Autoimmune Diseases with Oral Manifestations Martin S. Greenberg DDS, FDS RCSEd Professor Emeritus Department of Oral Medicine University of Pennsylvania Disclosure Statement I have no actual or potential
Autoimmune Diseases with Oral Manifestations Martin S. Greenberg DDS, FDS RCSEd Professor Emeritus Department of Oral Medicine University of Pennsylvania Disclosure Statement I have no actual or potential
LESIONS OF THE ORAL CAVITY ORAL CAVITY. Oral Cavity Subsites 4/10/2013 LIPS TEETH GINGIVA ORAL MUCOUS MEMBRANES PALATE TONGUE ORAL LYMPHOID TISSUES
 LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
Squamous Cell Carcinoma of the Head and Neck (SCCHN)
 Squamous Cell Carcinoma of the Head and Neck (SCCHN) Part 1 Bruce M. Wenig, M.D. Dept. of Pathology & Laboratory Medicine Continuum Health Partners New York, NY College of American Pathologists 2004. Materials
Squamous Cell Carcinoma of the Head and Neck (SCCHN) Part 1 Bruce M. Wenig, M.D. Dept. of Pathology & Laboratory Medicine Continuum Health Partners New York, NY College of American Pathologists 2004. Materials
IN THE NAME OF GOD. Dr.kheirandish DDS,MSC Oral and maxillofacial pathology
 IN THE NAME OF GOD Dr.kheirandish DDS,MSC Oral and maxillofacial pathology Dermatologic Diseases Chapter 16 ECTODERMAL DYSPLASIA o Two or more ectodermally derived anatomic structures fail to develop o
IN THE NAME OF GOD Dr.kheirandish DDS,MSC Oral and maxillofacial pathology Dermatologic Diseases Chapter 16 ECTODERMAL DYSPLASIA o Two or more ectodermally derived anatomic structures fail to develop o
Histopathology: Cervical HPV and neoplasia
 Histopathology: Cervical HPV and neoplasia These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about
Histopathology: Cervical HPV and neoplasia These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about
Case Report Supernumerary Teeth in Primary Dentition and Early Intervention: A Series of Case Reports
 Case Reports in Dentistry Volume 2012, Article ID 614652, 4 pages doi:10.1155/2012/614652 Case Report Supernumerary Teeth in Primary Dentition and Early Intervention: A Series of Case Reports Rakesh N.
Case Reports in Dentistry Volume 2012, Article ID 614652, 4 pages doi:10.1155/2012/614652 Case Report Supernumerary Teeth in Primary Dentition and Early Intervention: A Series of Case Reports Rakesh N.
Histopathology of Melanoma
 THE YALE JOURNAL OF BIOLOGY AND MEDICINE 48, 409-416 (1975) Histopathology of Melanoma G. J. WALKER SMITH Department ofpathology, Yale University School ofmedicine, 333 Cedar Street, New Haven, Connecticut
THE YALE JOURNAL OF BIOLOGY AND MEDICINE 48, 409-416 (1975) Histopathology of Melanoma G. J. WALKER SMITH Department ofpathology, Yale University School ofmedicine, 333 Cedar Street, New Haven, Connecticut
DERMATITIS CHRONICA HELICIS
 J. clin. Path. (1957), 10, 46. THE HISTOLOGICAL APPEARANCES OF CHONDRO- DERMATITIS CHRONICA HELICIS BY E. M. McCONNELL From the Department of Pathology, Liverpool Radium Institute, Liverpool (RECEIVED
J. clin. Path. (1957), 10, 46. THE HISTOLOGICAL APPEARANCES OF CHONDRO- DERMATITIS CHRONICA HELICIS BY E. M. McCONNELL From the Department of Pathology, Liverpool Radium Institute, Liverpool (RECEIVED
Premalignant Nature of Oral Lichen Planus
 Acta Derm Venereol, February 2005; 85: 516 520 CLINICAL REPORT Premalignant Nature of Oral Lichen Planus Ronald LAEIJENDECKER 1, Theodoor Van JOOST 2, Marti C. KUIZINGA 3, Bhupendra TANK 2 and H. A. Martino
Acta Derm Venereol, February 2005; 85: 516 520 CLINICAL REPORT Premalignant Nature of Oral Lichen Planus Ronald LAEIJENDECKER 1, Theodoor Van JOOST 2, Marti C. KUIZINGA 3, Bhupendra TANK 2 and H. A. Martino
Scientific Dental Journal
 Scientific Dental Journal Pigmented Oral Lichen Planus: A Case Report Firstine Kelsi Hartanto 1, Thomas George Kallarakal 2 1 Department of Oral Medicine, Faculty of Dentistry, Trisakti University Indonesia
Scientific Dental Journal Pigmented Oral Lichen Planus: A Case Report Firstine Kelsi Hartanto 1, Thomas George Kallarakal 2 1 Department of Oral Medicine, Faculty of Dentistry, Trisakti University Indonesia
Immunohistochemical study of lichen planus
 Immunohistochemical study of lichen planus SAI SHOUSHA AND JOHN SVIRBELY1 rom the Department of Histopathology, Royal ree Hospital, London NW3 2QG J. clin. Path., 1977, 30, 569-574 SUARY The distribution
Immunohistochemical study of lichen planus SAI SHOUSHA AND JOHN SVIRBELY1 rom the Department of Histopathology, Royal ree Hospital, London NW3 2QG J. clin. Path., 1977, 30, 569-574 SUARY The distribution
Case Report Treatment of Two Canals in All Mandibular Incisor Teeth in the Same Patient
 Case Reports in Dentistry, Article ID 893980, 4 pages http://dx.doi.org/10.1155/2014/893980 Case Report Treatment of Two Canals in All Mandibular Incisor Teeth in the Same Patient Vandana B. Kokane, Swapnil
Case Reports in Dentistry, Article ID 893980, 4 pages http://dx.doi.org/10.1155/2014/893980 Case Report Treatment of Two Canals in All Mandibular Incisor Teeth in the Same Patient Vandana B. Kokane, Swapnil
Research Article Oral Health Status and Oromucosal Lesions in Patients Living with HIV/AIDS in India: A Comparative Study
 AIDS Research and Treatment, Article ID 480247, 4 pages http://dx.doi.org/10.1155/2014/480247 Research Article Oral Health Status and Oromucosal Lesions in Patients Living with HIV/AIDS in India: A Comparative
AIDS Research and Treatment, Article ID 480247, 4 pages http://dx.doi.org/10.1155/2014/480247 Research Article Oral Health Status and Oromucosal Lesions in Patients Living with HIV/AIDS in India: A Comparative
INFLAMMATORY DISEASES PART I. Immunopathology Part I
 INFLAMMATORY DISEASES PART I Immunopathology Part I Nonspecific & T Cell Mediated Mucosal Inflammatory Lesions Nonspecific and Idiopathic Mucositis Hypersensitivity and Autoimmune T cell mediated Immunoglobulin
INFLAMMATORY DISEASES PART I Immunopathology Part I Nonspecific & T Cell Mediated Mucosal Inflammatory Lesions Nonspecific and Idiopathic Mucositis Hypersensitivity and Autoimmune T cell mediated Immunoglobulin
MAST CELLS IN ORAL LICHEN PLANUS
 MAST CELLS IN ORAL LICHEN PLANUS Mahija Janardhanan* V.Ramesh. ** *Reader, Department of Oral Pathology & Microbiology, Amrita school of Dentistry, Kochi. **Professor & HOD, Department of Oral Pathology
MAST CELLS IN ORAL LICHEN PLANUS Mahija Janardhanan* V.Ramesh. ** *Reader, Department of Oral Pathology & Microbiology, Amrita school of Dentistry, Kochi. **Professor & HOD, Department of Oral Pathology
Histopathologic analysis of gingival lesions: A 20-year retrospective study at one academic dental center
 Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/jced.54766 http://dx.doi.org/10.4317/jced.54766 Histopathologic analysis of gingival lesions: A 20-year retrospective
Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/jced.54766 http://dx.doi.org/10.4317/jced.54766 Histopathologic analysis of gingival lesions: A 20-year retrospective
Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report
 Case Reports in Oncological Medicine, Article ID 206260, 4 pages http://dx.doi.org/10.1155/2014/206260 Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report Sharad P. Paul 1,2,3 1 Skin
Case Reports in Oncological Medicine, Article ID 206260, 4 pages http://dx.doi.org/10.1155/2014/206260 Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report Sharad P. Paul 1,2,3 1 Skin
R. Diagnostic criteria in proliferative verrucous leukoplakia: Evaluation.
 Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/medoral.19424 http://dx.doi.org/doi:10.4317/medoral.19424 Diagnostic criteria in proliferative verrucous leukoplakia:
Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/medoral.19424 http://dx.doi.org/doi:10.4317/medoral.19424 Diagnostic criteria in proliferative verrucous leukoplakia:
Disorders of Cell Growth & Neoplasia. Histopathology Lab
 Disorders of Cell Growth & Neoplasia Histopathology Lab Paul Hanna April 2010 Case #84 Clinical History: 5 yr-old, West Highland White terrier. skin mass from axillary region. has been present for the
Disorders of Cell Growth & Neoplasia Histopathology Lab Paul Hanna April 2010 Case #84 Clinical History: 5 yr-old, West Highland White terrier. skin mass from axillary region. has been present for the
International Journal of Scientific Research and Innovative Technology ISSN: Vol. 4 No. 12; December 2017
 THE FREQUENCY OF ORAL LICHEN PLANUS IN SAMPLES SENT TO PATHOLOGY DEPARTMENT OF TABRIZ DENTAL SCHOOL (2006-2016) AND ITS RELATION WITH AGE, SEX, LESION TYPE AND LOCATION Farzaneh Pakdel 1, Parya Emamverdizadeh
THE FREQUENCY OF ORAL LICHEN PLANUS IN SAMPLES SENT TO PATHOLOGY DEPARTMENT OF TABRIZ DENTAL SCHOOL (2006-2016) AND ITS RELATION WITH AGE, SEX, LESION TYPE AND LOCATION Farzaneh Pakdel 1, Parya Emamverdizadeh
Chapter 5. Oxygenated Hemoglobin Diffuse Reflectance Ratio for In Vivo Detection of oral Pre-cancer
 Chapter 5 Oxygenated Hemoglobin Diffuse Reflectance Ratio for In Vivo Detection of oral Pre-cancer This work is published in: JB0 (SPIE) 13(4):041306 (1-10), 2008 Oxygenated Hemoglobin Diffuse Reflectance
Chapter 5 Oxygenated Hemoglobin Diffuse Reflectance Ratio for In Vivo Detection of oral Pre-cancer This work is published in: JB0 (SPIE) 13(4):041306 (1-10), 2008 Oxygenated Hemoglobin Diffuse Reflectance
Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease:
 Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease: Hematological GIT Behcet s HIV 5. Associated with dermatological diseases:
Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease: Hematological GIT Behcet s HIV 5. Associated with dermatological diseases:
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB. Friday, February 13, :30 am 11:00 am
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 13, 2009 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 13, 2009 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
IJPCDR ORIGINAL RESEARCH ABSTRACT INTRODUCTION /jp-journals
 ORIGINAL RESEARCH 10.5005/jp-journals-00000-0000 Histopathological Assessment of Fungal Infection in the Biopsies of Oral Squamous Cell Carcinoma, Oral Lichen Planus, and Leukoplakia Using Hematoxylin
ORIGINAL RESEARCH 10.5005/jp-journals-00000-0000 Histopathological Assessment of Fungal Infection in the Biopsies of Oral Squamous Cell Carcinoma, Oral Lichen Planus, and Leukoplakia Using Hematoxylin
IMMUNOPATHOLOGY OF ORAL LEUKOPLAKIA
 442 IMMUNOPATHOLOGY OF ORAL LEUKOPLAKIA T. LEHNER From the Department of Oral Medicine and Pathology, Guy's Hospital Medical School, London, S.E.1 Received for publication April 17, 197 SUMMARY.-The lymphocyte
442 IMMUNOPATHOLOGY OF ORAL LEUKOPLAKIA T. LEHNER From the Department of Oral Medicine and Pathology, Guy's Hospital Medical School, London, S.E.1 Received for publication April 17, 197 SUMMARY.-The lymphocyte
Citation The Journal of Dermatology, 37(8), available at
 NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
A five year study on differential diagnosis of verruciform penile lesions
 Original Research Article A five year study on differential diagnosis of verruciform penile lesions S. Sujatha 1, V. Srinivas Kumar 2*, K. Durga 3 1 Associate Professor, 2 Assistant Professor, 3 Professor
Original Research Article A five year study on differential diagnosis of verruciform penile lesions S. Sujatha 1, V. Srinivas Kumar 2*, K. Durga 3 1 Associate Professor, 2 Assistant Professor, 3 Professor
Clinical Study Conservative Approach in Patients with Pemphigus Gingival Vulgaris: A Pilot Study of Five Cases
 International Dentistry, Article ID 747506, 4 pages http://dx.doi.org/10.1155/2014/747506 Clinical Study Conservative Approach in Patients with Pemphigus Gingival Vulgaris: A Pilot Study of Five Cases
International Dentistry, Article ID 747506, 4 pages http://dx.doi.org/10.1155/2014/747506 Clinical Study Conservative Approach in Patients with Pemphigus Gingival Vulgaris: A Pilot Study of Five Cases
CINtec p16 INK4a Staining Atlas
 CINtec p16 INK4a Staining Atlas Rating Rating Positive The rating positive will be assigned if the p16 INK4a -stained slide shows a continuous staining of cells of the basal and parabasal cell layers of
CINtec p16 INK4a Staining Atlas Rating Rating Positive The rating positive will be assigned if the p16 INK4a -stained slide shows a continuous staining of cells of the basal and parabasal cell layers of
Lichenoid Tissue Reaction in Malignant Melanoma A Potential Diagnostic Pitfall
 natomic Pathology / LICHENOID TISSUE RECTION IN MLIGNNT MELNOM Lichenoid Tissue Reaction in Malignant Melanoma Potential Diagnostic Pitfall CPT Scott R. Dalton, MC, US, 1,3 Capt Matt. aptista, USF, MC,
natomic Pathology / LICHENOID TISSUE RECTION IN MLIGNNT MELNOM Lichenoid Tissue Reaction in Malignant Melanoma Potential Diagnostic Pitfall CPT Scott R. Dalton, MC, US, 1,3 Capt Matt. aptista, USF, MC,
The Prevalence of Oral Leukoplakia: Results From a Romanian Medical Center
 The Prevalence of Oral Leukoplakia: Results From a Romanian Medical Center Ramona Vlad, DMD Department of Odontology and Oral Pathology, Faculty of Dental Medicine, University of Medicine and Pharmacy
The Prevalence of Oral Leukoplakia: Results From a Romanian Medical Center Ramona Vlad, DMD Department of Odontology and Oral Pathology, Faculty of Dental Medicine, University of Medicine and Pharmacy
A Clinicohistopathologic Study and Probable Mechanism of Pigmentation in Oral Lichen Planus
 10.5005/jp-journals-10015-1184 Rubina Anjum et al ORIGINAL RESEARCH A Clinicohistopathologic Study and Probable Mechanism of Pigmentation in Oral Lichen Planus Rubina Anjum, Jasmin Singh, Shailesh Kudva
10.5005/jp-journals-10015-1184 Rubina Anjum et al ORIGINAL RESEARCH A Clinicohistopathologic Study and Probable Mechanism of Pigmentation in Oral Lichen Planus Rubina Anjum, Jasmin Singh, Shailesh Kudva
Case Report Maintenance of Increased Mouth Opening in Oral Submucous Fibrosis Patient Treated with Nasolabial Flap Technique
 Case Reports in Dentistry, Article ID 842578, 4 pages http://dx.doi.org/10.1155/2014/842578 Case Report Maintenance of Increased Mouth Opening in Oral Submucous Fibrosis Patient Treated with Nasolabial
Case Reports in Dentistry, Article ID 842578, 4 pages http://dx.doi.org/10.1155/2014/842578 Case Report Maintenance of Increased Mouth Opening in Oral Submucous Fibrosis Patient Treated with Nasolabial
Journal of International Academy of Forensic Science & Pathology (JIAFP)
 Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
A Speckled Lesion. Angela C. Chi, DMD; Michele Carter Ravenel, DMD
 A Speckled Lesion Angela C. Chi, DMD; Michele Carter Ravenel, DMD The following Case Challenge is provided in conjunction with the American Academy of Oral and Maxillofacial Pathology. Case Summary This
A Speckled Lesion Angela C. Chi, DMD; Michele Carter Ravenel, DMD The following Case Challenge is provided in conjunction with the American Academy of Oral and Maxillofacial Pathology. Case Summary This
Research Article A Structured Assessment to Decrease the Amount of Inconclusive Endometrial Biopsies in Women with Postmenopausal Bleeding
 International Surgical Oncology Volume 2016, Article ID 3039261, 5 pages http://dx.doi.org/10.1155/2016/3039261 Research Article A Structured Assessment to Decrease the Amount of Inconclusive Endometrial
International Surgical Oncology Volume 2016, Article ID 3039261, 5 pages http://dx.doi.org/10.1155/2016/3039261 Research Article A Structured Assessment to Decrease the Amount of Inconclusive Endometrial
CURRENT ASSESSMENTS REGARDING THE PATHOGENESIS AND TREATMENT STRATEGIES OF ORAL LICHEN PLANUS A REVIEW
 CURRENT ASSESSMENTS REGARDING THE PATHOGENESIS AND TREATMENT STRATEGIES OF ORAL LICHEN PLANUS A REVIEW Pratyush Singh 1, Pratik Patel 1, Raghu AR 2, Ankur Kaur Shergill 3, Monica Charlotte. Solomon* 4
CURRENT ASSESSMENTS REGARDING THE PATHOGENESIS AND TREATMENT STRATEGIES OF ORAL LICHEN PLANUS A REVIEW Pratyush Singh 1, Pratik Patel 1, Raghu AR 2, Ankur Kaur Shergill 3, Monica Charlotte. Solomon* 4
Newcastle University eprints
 Newcastle University eprints Diajil A, Robinson CM, Sloan P, Thomson PJ. (23) Clinical Outcome Following Oral Potentially malignant Disorder Treatment: A patient Cohort Study. International Dentistry Volume
Newcastle University eprints Diajil A, Robinson CM, Sloan P, Thomson PJ. (23) Clinical Outcome Following Oral Potentially malignant Disorder Treatment: A patient Cohort Study. International Dentistry Volume
Oral lichenoid lesions: distinguishing the benign from the deadly
 S54 2017 USCAP, Inc All rights reserved 0893-3952/17 $32.00 Oral lichenoid lesions: distinguishing the benign from the deadly Susan Müller Professor Emeritus, Emory University School of Medicine: Atlanta
S54 2017 USCAP, Inc All rights reserved 0893-3952/17 $32.00 Oral lichenoid lesions: distinguishing the benign from the deadly Susan Müller Professor Emeritus, Emory University School of Medicine: Atlanta
Epithelial tumors. Dr. F.F. Khuzin, PhD Dr. M.O. Mavlikeev
 Epithelial tumors Dr. F.F. Khuzin, PhD Dr. M.O. Mavlikeev Epithelial tumors Tumors from the epithelium are the most frequent among tumors. There are 2 group features of these tumors: The presence in most
Epithelial tumors Dr. F.F. Khuzin, PhD Dr. M.O. Mavlikeev Epithelial tumors Tumors from the epithelium are the most frequent among tumors. There are 2 group features of these tumors: The presence in most
THERE IS A GROUP OF PAtients. Defining Urticarial Dermatitis. A Subset of Dermal Hypersensitivity Reaction Pattern
 STUDY Defining Urticarial Dermatitis A Subset of Dermal Hypersensitivity Reaction Pattern Steven Kossard, FACD; Ian Hamann, FACD; Barbara Wilkinson, BSc Background: Urticarial dermatitis may represent
STUDY Defining Urticarial Dermatitis A Subset of Dermal Hypersensitivity Reaction Pattern Steven Kossard, FACD; Ian Hamann, FACD; Barbara Wilkinson, BSc Background: Urticarial dermatitis may represent
A retrospective clinicopathological study on oral lichen planus and malignant transformation: Analysis of 518 cases
 Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/medoral.17778 http://dx.doi.org/doi:10.4317/medoral.17778 A retrospective clinicopathological study on oral lichen planus
Journal section: Oral Medicine and Pathology Publication Types: Research doi:10.4317/medoral.17778 http://dx.doi.org/doi:10.4317/medoral.17778 A retrospective clinicopathological study on oral lichen planus
Case Report Typical Radiographic Findings of Dentin Dysplasia Type 1b with Dental Fluorosis
 Case Reports in Dentistry Volume 2013, Article ID 902861, 4 pages http://dx.doi.org/10.1155/2013/902861 Case Report Typical Radiographic Findings of Dentin Dysplasia Type 1b with Dental Fluorosis S. Venkata
Case Reports in Dentistry Volume 2013, Article ID 902861, 4 pages http://dx.doi.org/10.1155/2013/902861 Case Report Typical Radiographic Findings of Dentin Dysplasia Type 1b with Dental Fluorosis S. Venkata
ISPUB.COM. Seborrheic Keratosis: A Pictorial Review of the Histopathologic Variations. D Sarma, S Repertinger
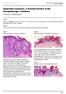 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 2 Seborrheic Keratosis: A Pictorial Review of the Histopathologic Variations D Sarma, S Repertinger Citation D Sarma, S Repertinger.. The Internet
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 2 Seborrheic Keratosis: A Pictorial Review of the Histopathologic Variations D Sarma, S Repertinger Citation D Sarma, S Repertinger.. The Internet
Lymphomatoid Papulosis 3 Case Reports
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. III (July. 2015), PP 31-35 www.iosrjournals.org Lymphomatoid Papulosis 3 Case Reports
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. III (July. 2015), PP 31-35 www.iosrjournals.org Lymphomatoid Papulosis 3 Case Reports
CS05 NEW DEVELOPMENTS IN GASTROINTESTINAL PATHOLOGY-GIPS FUNNY FORMS OF ESOPHAGITIS: BEYOND GERD AND EOSINOPHILIC ESOPHAGITIS
 CS05 NEW DEVELOPMENTS IN GASTROINTESTINAL PATHOLOGY-GIPS FUNNY FORMS OF ESOPHAGITIS: BEYOND GERD AND EOSINOPHILIC ESOPHAGITIS Rhonda K. Yantiss, M.D. Professor of Pathology and Laboratory Medicine Weill
CS05 NEW DEVELOPMENTS IN GASTROINTESTINAL PATHOLOGY-GIPS FUNNY FORMS OF ESOPHAGITIS: BEYOND GERD AND EOSINOPHILIC ESOPHAGITIS Rhonda K. Yantiss, M.D. Professor of Pathology and Laboratory Medicine Weill
Morsicatio Mucosae Oris A Chronic Oral Frictional Keratosis, Not a Leukoplakia
 J Oral Maxillofac Surg 67:140-146, 2009 Morsicatio Mucosae Oris A Chronic Oral Frictional Keratosis, Not a Leukoplakia Sook-Bin Woo, DMD,* and Dorothy Lin Purpose: Morsicatio mucosae oris (MMO) presents
J Oral Maxillofac Surg 67:140-146, 2009 Morsicatio Mucosae Oris A Chronic Oral Frictional Keratosis, Not a Leukoplakia Sook-Bin Woo, DMD,* and Dorothy Lin Purpose: Morsicatio mucosae oris (MMO) presents
Case Report A Case of Cystic Basal Cell Carcinoma Which Shows a Homogenous Blue/Black Area under Dermatoscopy
 Volume 20, Article ID 450472, 4 pages doi:0.55/20/450472 Case Report A Case of Cystic Basal Cell Carcinoma Which Shows a Homogenous Blue/Black Area under Dermatoscopy Akihiro Yoneta, Kohei Horimoto, Keiko
Volume 20, Article ID 450472, 4 pages doi:0.55/20/450472 Case Report A Case of Cystic Basal Cell Carcinoma Which Shows a Homogenous Blue/Black Area under Dermatoscopy Akihiro Yoneta, Kohei Horimoto, Keiko
IMMUNOPHENOTYPING OF THE INFLAMMATORY RESPONSE OF POTENTIALLY PRECANCEROUS ORAL MUCOSAL LESIONS. Andres David Flores Hidalgo
 IMMUNOPHENOTYPING OF THE INFLAMMATORY RESPONSE OF POTENTIALLY PRECANCEROUS ORAL MUCOSAL LESIONS Andres David Flores Hidalgo A thesis submitted to the faculty of the University of North Carolina at Chapel
IMMUNOPHENOTYPING OF THE INFLAMMATORY RESPONSE OF POTENTIALLY PRECANCEROUS ORAL MUCOSAL LESIONS Andres David Flores Hidalgo A thesis submitted to the faculty of the University of North Carolina at Chapel
