Staging of Bone Tumors: A Review with Illustrative Examples
|
|
|
- Marianna Booth
- 5 years ago
- Views:
Transcription
1 Staging one Tumors Musculoskeletal Imaging Review C D E M N E U T R Y L I M C I G O F I N G Staging of one Tumors: Review with Illustrative Examples Gregory S. Stacy 1 Ravinder S. Mahal 1,2 Terrance D. Peabody 3 Stacy GS, Mahal RS, Peabody TD OJECTIVE. The radiologist plays an important role in the workup and staging of bone tumors. The purpose of this article is to review that role and to discuss recent changes to the primary malignant bone tumor staging system developed by the merican Joint Committee on Cancer. CONCLUSION. Knowledge of staging parameters for the diagnosis and management of bone tumors will help the radiologist to generate meaningful reports for the referring physician. Keywords: bone cancer, musculoskeletal imaging, musculoskeletal system, oncologic imaging DOI: /JR Received pril 15, 2005; accepted after revision ugust 10, Department of Radiology, University of Chicago, 5841 S Maryland ve., MC2026, Chicago, IL ddress correspondence to G. S. Stacy. 2 Present address: Department of Radiology, Mayo Clinic, Scottsdale, Z. 3 Department of Orthodaedic Surgery, University of Chicago, Chicago, IL CME This article is available for CME credit. See supplemental data for this article at or visit for more information. JR 2006; 186: X/06/ merican Roentgen Ray Society wo systems are currently used T for staging malignant primary bone tumors: the Musculoskeletal Tumor Society (MSTS) system and the merican Joint Committee on Cancer (JCC) system. Recent revisions to the JCC system have received little attention in the radiology literature. We review the importance of proper selection of the appropriate imaging techniques for the evaluation of a patient with a suspected benign or malignant bone tumor and describe the radiologist s role in staging primary bone neoplasms, emphasizing recent changes to the JCC system. The Initial Evaluation of a one Lesion patient may seek treatment for a bone lesion because it is painful, it is associated with a palpable mass, it is associated with a pathologic fracture, or it is discovered incidentally on an imaging study. The ppropriateness Criteria [1], established by the merican College of Radiology, dictate that for the initial evaluation of a bone lesion, radiographs should be the first line of imaging (Table 1). Not only are radiographs relatively inexpensive, but the differential diagnosis of most primary bone tumors is generated based on features detected on radiographs [2, 3]. Such features suggest either benignity or malignancy and allow one to decide whether additional imaging examinations, if any, should be performed. The next imaging step generally depends on one of four clinical conditions: first, the radiograph shows normal findings, but the patient has persistent symptoms; second, the radiograph reveals abnormal findings and the clinician suspects metastatic disease or multiple myeloma on the basis of the patient s history, laboratory values, or both; third, the radiograph depicts abnormal findings, showing a nonaggressive-appearing tumor; or, fourth, the radiograph reveals abnormal findings, showing an aggressive-appearing primary bone tumor. n important role of the radiologist is to assist the clinician to ensure that imaging is performed in an appropriate manner. Lytic bone lesions are often not detectable on standard radiographs until the tumor has resulted in 30 50% loss of mineralization [4]. If the radiograph shows normal or indeterminate findings, but the patient has persistent localized symptoms, additional imaging studies are frequently required. MRI is the preferred imaging technique in this setting [1]. It is the most sensitive technique for detecting marrow-based lesions, and the anatomic detail seen on MRI is superior to that of radionuclide studies [5]. In addition, MRI may offer a specific diagnosis other than that of a bone tumor (e.g., occult fracture, osteonecrosis), whereas this is often not possible with skeletal scintigraphy. If the patient s pain is not localized, then a nuclear medicine bone scan may be indicated as a screening test for evaluating the entire skeleton. lesion seen on a radiograph may represent a focus of metastatic disease from a known or unknown primary tumor, particularly in older patients. In the setting of a known primary tumor, radionuclide bone scanning is the primary imaging examina- JR:186, pril
2 TLE 1: Summary of ppropriate Radiologic Examination Procedures for Evaluation of one Tumors Radiologic Examination Procedure and ppropriateness Rating Nuclear Medicine one Clinical Condition Routine Radiography MRI Scanning Screening, first study 9: bsolute requirement Persistent symptoms, but radiograph negative 9: Contrast may be useful: depends on expertise and institutional preference 4: Good option if patient cannot have MRI; nonspecific (MRI more specific and sensitive) Definitely benign on radiographs a Clinically suspected osteoid osteoma Suspicious for malignant characteristics on radiographs 9: Necessary; follow up with CT if positive 6: CT is more useful but diagnosis can often be made with MRI; contrast may improve nidus identification 9: Contrast can provide more information; useful for vascularity and necrotic areas 6: Very sensitive but nonspecific; good for localization if lesion is occult radiographically 3: Probably not indicated except to look for additional lesions CT 3: If MRI not available; useful to evaluate cortex and trabecular pattern 9: Contrast not needed 5: May be useful if MRI not available or possible; useful for evaluation of calcification, cortical breakthrough, and pathologic fractures Note Modified from the merican College of Radiology ppropriateness Criteria for one Tumors [1]. The appropriateness rating ranges from 1 (least appropriate) to 9 (most appropriate). a dditional studies (MRI or CT) may be needed if surgical intervention is contemplated and further anatomic information is required. Fig year-old girl with fibroxanthoma (i.e., nonossifying fibroma). Note benign characteristics of lesion: narrow zone of transition, intact cortex, lack of periostitis, and lack of soft-tissue mass. tion used to detect osseous metastases [6]. Patients presenting with a bone lesion on a radiograph who do not have a known primary tumor but are suspected of having metastatic disease based on data acquired through history and physical examination may also undergo bone scintigraphy to confirm whether there are multiple foci [7]. dditional imaging studies may be warranted in these cases to locate a primary tumor, including CT of the chest and abdomen, primarily to search for lung or renal carcinomas [8]. Mammography may be considered in women. Laboratory studies are also often performed, including a test to determine the prostate-specific antigen level in men. Protein electrophoresis is recommended to detect myeloma, in which case a radiographic skeletal survey is indicated for staging [9]. Solitary primary tumors and tumorlike lesions of bone are commonly encountered by radiologists. The radiologist should attempt to classify the lesion as either nonaggressive or aggressive on the basis of its radiographic characteristics. Nonaggressive characteristics include a narrow zone of transition between the lesion and the surrounding normal bone, an intact (although possibly thinned) cortex, mature periostitis, and lack of an associated soft-tissue mass [10] (Fig. 1). Such lesions are usually benign. If the radiograph shows a nonaggressive bone tumor, additional imaging studies may be required depending on the biologic behavior of the lesion suggested by the radiographic findings and the potential need for operative intervention. Chondroblastomas, for example, typically have a nonaggressive, benign appearance on radiographs; however, these le- Fig year-old girl with osteosarcoma. Note malignant characteristics of lesion: wide zone of transition, aggressive periostitis, and soft-tissue extension. 968 JR:186, pril 2006
3 Staging one Tumors sions show progressive growth and will need to be removed. MRI is usually the study of choice in these instances [11, 12] because it will often show marrow and softtissue involvement better than CT. CT remains of value, however, in assessing suspected cartilaginous neoplasms for the presence of intralesion mineralization and degree of cortical erosion. staging system of benign bone tumors is described later in this article. Radiographic characteristics of an aggressive bone lesion include a wide zone of transition between the tumor and the surrounding normal bone, cortical destruction, aggressive-appearing periosteal new bone formation (e.g., onionskin or sunburst appearance), and an associated soft-tissue mass (Fig. 2). Lesions with aggressive radiologic characteristics are often malignant, although certain benign entities, such as osteomyelitis and giant cell tumor, can also appear aggressive. These aggressive-appearing benign entities may be associated with additional radiographic or clinical features that will support the diagnosis of a nonmalignant lesion. For example, there is a good chance that a nonmineralized radiolucent metaepiphyseal lesion in a young adult that extends to the articular surface of the affected bone is a giant cell tumor, even if the margins of the lesion are poorly defined and there is limited cortical destruction. Similarly, an aggressive-appearing lesion with a central sequestrum in an IV drug abuser likely represents osteomyelitis. If there are no additional features to support benignity, however, then an aggressive-appearing lesion should be considered malignant until proven otherwise. If a malignant tumor is suspected, additional imaging is required. In most cases, MRI is the best imaging technique for local staging because it best shows features important for staging. lthough MRI is currently the best imaging technique for detecting marrow-based disease and for delineating the osseous and soft-tissue extent of a bone tumor, it is not as useful as conventional radiography for characterizing the aggressiveness of most bone lesions [1 3]; however, it may occasionally help with the histologic diagnosis in certain situations (e.g., aneurysmal bone cyst, intraosseous lipoma). CT may be preferred over MRI for the evaluation of cortical involvement or cortically based lesions, such as osteoid osteoma, periosteal reaction, matrix mineralization, and lesions in flat bones. Furthermore, MDCT, with its multiplanar capability, is a reasonable substitute for those patients who cannot undergo MRI and can provide exquisite 3D reformations for volumetric and preoperative assessment [13]. Staging of Primary one Tumors Malignant Neoplasms In 1980, Enneking et al. [14] described a system for staging bone sarcomas that was adopted by the MSTS. Staging with the Enneking system is based on three criteria. The first criterion is that of the extent of the tumor: The tumor is designated T1 if it remains confined to a single anatomic compartment (intracompartmental) and is designated T2 if it spreads into an additional compartment or compartments (extracompartmental). The second criterion is that of metastasis: The tumor is designated M0 if there are no metastases and is designated M1 if there are either regional or distant metastases. The third criterion is that of the TLE 2: Enneking Staging System [14] for Primary Malignant Tumors of one Stage Tumor Metastases Grade I T1 M0 G1 I T2 M0 G1 II T1 M0 G2 II T2 M0 G2 III T1 or T2 M1 G1 or G2 Note T1 = tumor is intracompartmental, T2 = tumor is extracompartmental, M0 = no regional or distant metastasis, M1 = regional or distant metastasis, G1 = low grade, G2 = high grade. grade of the tumor, which is a histologic assessment of cellular atypia and is related to the tumor s tendency to metastasize. The estimated metastatic risk of low-grade (G1) tumors is less than 25%, whereas that of highgrade (G2) tumors is greater than 25%. This staging system is summarized in Table 2. In 1983, the JCC [15, 16] developed a slightly different system for the staging of malignant bone tumors. Until recently, staging with the JCC system was based on the following four criteria: first, the extent of the primary tumor, either confined by bone cortex (T1) or extending through cortex (T2); second, the absence (N0) or presence (N1) of regional lymph node metastases; third, the absence (M0) or presence (M1) of distant metastases; and, fourth, the histologic grade of the tumor. Low-grade tumors were designated either G1 (well differentiated) or G2 (moderately differentiated), whereas highgrade tumors were designated either G3 (poorly differentiated) or G4 (undifferentiated). Low-grade lesions generally are associated with a better prognosis than high-grade lesions. This staging system is summarized in Table 3. Note that this system did not have a defined stage III. The JCC system was recently revised [17], and for cases diagnosed beginning January 1, 2003, the extent (T) of the tumor now reflects the size of the tumor rather than its transcortical extension. Tumors 8 cm or less in the greatest dimension are designated T1, whereas those greater than 8 cm are designated T2. Patients with small tumors generally have a better prognosis than those with large tumors. new designation, T3, has been added to indicate skip metastases that TLE 3: merican Joint Committee on Cancer Staging System for Primary Malignant Tumors of one efore 2003 [16] Stage Tumor Lymph Node Metastases Grade I T1 N0 M0 G1 or G2 I T2 N0 M0 G1 or G2 II T1 N0 M0 G3 or G4 II T2 N0 M0 G3 or G4 III Not defined IV ny T N1 M0 ny G IV ny T ny N M1 ny G Note T1 = tumor confined to cortex, T2 = tumor extends beyond cortex; N0 = no regional lymph node metastasis, N1 = regional lymph node metastasis; M0 = no distant metastasis, M1 = distant metastasis; and G1 = well differentiated (low grade), G2 = moderately differentiated (low grade), G3 = poorly differentiated (high grade), G4 = undifferentiated (high grade). JR:186, pril
4 TLE 4: merican Joint Committee on Cancer Staging System for Primary Malignant Tumors of one for Those Tumors Diagnosed on or fter January 1, 2003 [17] Stage Tumor Lymph Node Metastases Grade I T1 N0 M0 G1 or G2 I T2 N0 M0 G1 or G2 II T1 N0 M0 G3 or G4 II T2 N0 M0 G3 or G4 III T3 N0 M0 ny G IV ny T N0 M1a ny G IV ny T N1 ny M ny G IV ny T ny N M1b ny G Note Tx = primary tumor cannot be assessed, T0 = no evidence of primary tumor, T1 = tumor 8 cm or less in greatest dimension; T2 = tumor more than 8 cm in greatest dimension, T3 = discontinuous tumors in the primary bone; Nx = regional lymph nodes not assessed, N0 = no regional lymph node metastases, N1 = regional lymph node metastasis; Mx = distant metastasis cannot be assessed, M0 = no distant metastasis, M1 = distant metastasis, M1a = lung, M1b = other distant sites; and Gx = grade cannot be assessed, G1 = well differentiated (low grade), G2 = moderately differentiated (low grade), G3 = poorly differentiated high grade), G4 = undifferentiated (high grade). is, discontinuous tumors in the primary bone site. Furthermore, M1 has been subdivided into M1a (lung-only metastases) and M1b Fig year-old man with osteosarcoma., Radiograph shows poorly defined radiolucency in proximal femoral diaphysis. ccurate measurement of lesion length is not possible., Fat-suppressed T2-weighted coronal MR image of proximal femur better reveals extent of lesion (arrowheads), which is well over 8 cm in length. This finding would be classified as T2 using revised merican Joint Committee on Cancer staging system [17]. (metastases to other distant sites, including distant lymph nodes). Lung-only metastases, particularly a solitary pulmonary metastasis, appear to convey a better prognosis than osseous or hepatic metastases. This new JCC staging system is summarized in Table 4. Note that there is now a defined stage III, representing a tumor without regional nodal (N0) or distant (M0) metastases, but with a skip metastasis (T3) in the affected bone. For high-grade tumors such as osteosarcoma, a skip lesion portends a poor prognosis. Determining the effect on survival of multifocal low-grade lesions, such as low-grade chondrosarcomas or low-grade vascular tumors, has proven to be more difficult [18]. This JCC staging system does not apply to primary malignant lymphoma of bone or multiple myeloma, but is used for all other primary malignant tumors of bone (e.g., osteosarcoma, Ewing s sarcoma). In addition to providing assistance to the clinician to ensure that imaging is performed in an appropriate manner, the radiologist has a role in evaluating each of the parameters of the bone sarcoma staging systems. For example, when assessing the primary tumor (T), reporting the size of the neoplasm, particularly its greatest dimension, is important for staging using the revised JCC system. s stated previously, MRI is best for evaluating tumor extent and therefore the size of the primary tumor [19 21], particularly if one cannot discern on radiographs whether the tumor is greater than 8 cm in greatest dimension (Fig. 3). On the other hand, the Enneking system does not consider the actual size tumor size, but rather whether the tumor is intra- or extracompartmental. Intracompartmental tumors are those that are entirely intraosseous or parosseous without intraosseous or extrafascial extension (Figs. 4 and 5). Extracompartmental tumors are those that are intraosseous with soft-tissue extension or parosseous with intraosseous or extrafascial extension (Figs. 6 and 7). Identification of skip metastases is also important. Hence, we recommend that the MRI protocol contain at least one coronal or sagittal sequence with a large field of view that includes the entire affected bone to search for skip metastases (Fig. 8). We use STIR images for this purpose at our institution, but others prefer using T1-weighted images; we are unaware of any prospective study comparing the relative sensitivity and specificity of T1- weighted versus STIR images for the diagnosis of skip metastases. We prefer MRI to bone scintigraphy for the evaluation of potential skip metastases 970 JR:186, pril 2006
5 Staging one Tumors Fig year-old woman with telangiectatic osteosarcoma., Radiograph shows poorly defined radiolucency in proximal tibia., T1-weighted coronal MR image shows hemorrhagic tumor (arrowheads) in proximal tibia without soft-tissue extension, making it intracompartmental; it would be classified as T1 using Enneking staging system [14]. Tumor is greater than 8 cm in length and would be classified as T2 using revised merican Joint Committee on Cancer staging system [17]. Fig year-old woman with parosteal osteosarcoma., Radiograph shows ossified mass along posterior aspect of distal femoral metadiaphysis., T2-weighted sagittal MR image shows low-signal-intensity mass (arrow) abutting posterior surface of distal femur. No intramedullary invasion is evident. This finding would be considered intracompartmental and classified as T1 using Enneking staging system [14]. because skip lesions that are close to the primary tumor may not be easily resolved with bone scintigraphy. The remaining MRI sequences should use a surface coil and the smallest field of view possible that includes the entire lesion; this provides optimal visualization of soft-tissue extension, including potential neurovascular and joint involvement. sample MRI protocol for assessing the primary tumor, therefore, would include, first, a large field-of-view coronal or sagittal sequence covering the entire bone and, second, several additional sequences with a small field of view to cover the primary tumor in its entirety for example, T1- and fat-suppressed T2-weighted sequences performed in the axial plane and T1- and fatsuppressed T2-weighted sequences performed in at least one orthogonal plane. s a general rule, IV gadolinium administration is of limited value in the evaluation of primary bone tumors because the contrast between the tumor and normal marrow is sufficient without it [22 24]. Occasionally, however, gadolinium will allow one to better identify areas of solid tumor amid necrosis and hemorrhage, which is important for biopsy planning, and joint involvement. Some investigators have shown encouraging results using dynamic postgadolinium imaging to distinguish tumor from reactive edema after chemotherapy and residual tumor from nontumor tissue postoperatively [25 29]; however, this technique currently does not have a role in the initial staging of the tumor. Lymphadenopathy accompanying primary bone sarcomas is rare, and a dedicated search for lymph node spread is thus rarely undertaken. However, after assessing the primary tumor using an MRI or CT examination, the radiologist should not forget to use the same study to search for any regional lymphadenopathy that would upstage the disease from N0 to N1. The lung is the most common site of distant metastasis from a primary bone sarcoma, and CT is currently the technique of choice for the detection of pulmonary metastases [15, 30] (Fig. 9). one metastases are uncommon at initial presentation of patients with primary bone sarcomas. However, the presence of osteosarcoma metastasis may affect treatment; therefore, skeletal scintigraphy is recommended for patients with osteosarcoma [31, 32] (Fig. 10). Identification of metastases would group the patient into stage III using the Enneking system and into stage IVa (lung-only metastases, M1a) or stage IVb (other distant metastases, M1b) us- JR:186, pril
6 Fig. 6 6-year-old girl with Ewing s sarcoma., Radiograph shows aggressive lesion of distal femur., T2-weighted MR image with fat suppression shows abnormal hyperintense signal in marrow of femur with associated soft-tissue mass (arrowhead); such extension constitutes extracompartmental spread and would be classified as T2 using Enneking staging system [14]. Fig year-old boy with parosteal osteosarcoma., Radiograph shows ossified mass along distal femoral diaphysis., T1-weighted sagittal MR image shows tumor abutting posterior surface of distal femur (white arrow) with extension into medullary cavity (black arrow); such extension constitutes extracompartmental spread and would be classified as T2 using Enneking staging system [14]. Fig year-old boy with osteosarcoma. Fatsuppressed T2-weighted coronal image with wide field of view shows primary tumor in proximal tibia (arrow). Note skip metastasis (arrowhead) in tibial diaphysis distally. This finding would be classified as T3 using revised merican Joint Committee on Cancer staging system [17]. 972 JR:186, pril 2006
7 Staging one Tumors Fig year-old boy with metastatic osteosarcoma., rm radiograph shows osteosarcoma of proximal humerus with large soft-tissue mass., xial CT image through thorax shows multiple pulmonary metastases, some with mineralization (arrow). ing the JCC system. PET has yet to find a place in the algorithm of primary staging; however, it has shown promise in the evaluation of chemotherapy response and posttreatment evaluation for recurrence and residual tumor [33 35]. The radiologist also plays an important role in imaging-guided biopsies. Obtaining an adequate specimen for microscopic analysis completes the staging process and allows a histologic grade (G) to be assigned. The biopsy should be performed after all imaging studies that might otherwise become compromised by postbiopsy edema and hemorrhage have been obtained. The biopsy should be attempted only after consultation with the surgeon who plans to operate on the tumor because the biopsy track must be excised with the tumor and hence must not contaminate additional compartments, neurovascular structures, or areas that may be used for reconstruction. enign Neoplasms lthough not routinely used by radiologists, a staging system for benign bone tumors that is based on the biologic behavior of the tumors as suggested by the radiographic findings has been described by Enneking [36]. Stage 1 tumors are latent benign bone neoplasms that remain static or heal spontaneously. n example of such a lesion is a fibroxanthoma (nonossifying fibroma, Fig. 1). Further radiographic and clinical observation is usually not required, nor is treatment for lesions that are not at risk for or have not undergone fracture. Stage 2 tumors are active benign bone tumors; their behavior shows progressive growth, but extension is limited by natural barriers. n example of such a lesion is a chondroblastoma (Fig. 11). These tumors are typically treated via curettage, and therefore additional imaging studies may be required preoperatively to assess the tumor extent. MRI is generally the preferred technique for assessing marrow extension, although CT may be warranted in certain instances as described earlier. Stage 3 tumors are locally invasive benign bone tumors; their behavior shows progressive growth not limited by natural barriers. n example of such a lesion is a giant cell tumor (Fig. 12). These tumors are typically treated via extended curettage or marginal resection with or without adjuvant therapy, and therefore additional imaging is usually required preoperatively. MRI is generally the preferred technique for assessing osseous and soft-tissue extension. JR:186, pril
8 C Fig year-old girl with metastatic osteosarcoma., Forearm radiograph shows osteosarcoma of ulnar diaphysis (arrowhead)., Skeletal scintigram shows increased radiotracer activity in ulnar diaphysis (white arrowhead), corresponding to primary tumor, and increased activity in contralateral distal femur (black arrowhead) adjacent to physis. C, Knee radiograph shows histologically confirmed osteosarcoma metastasis (arrowhead) in distal femoral metaphysis. Conclusion Proper selection of the appropriate imaging techniques for the evaluation of a patient with a suspected bone tumor is crucial for successful diagnosis and management; radiologists should work closely with the orthopedic oncologists for optimal management of patients with primary bone tumors. Recent changes to the JCC staging system emphasize the importance of tumor size over transcortical extension. Transcompartmental extension, however, remains an important feature of the Enneking system. The new JCC system also addresses skip metastases. These features, which are important for staging, should be evaluated by the radiologist and mentioned in his or her report. It is not necessary for most radiologists to be intimately familiar with the details of the two staging systems. In fact, if the radiologist is accustomed to producing complete and descriptive reports when evaluating bone tumors, then the recent changes to the JCC system will probably not affect his or her dic- 974 JR:186, pril 2006
9 Staging one Tumors Fig year-old boy with chondroblastoma., Knee radiograph shows radiolucent lesion with sclerotic margins (white arrowheads) in epiphysis of distal femur and with probable extension into metaphysis (black arrowhead)., T1-weighted coronal MR image of knee better depicts transphyseal extension of chondroblastoma (arrow). tations. ll radiologists, however, should be aware that imaging factors heavily in the staging of bone tumors, and a basic knowledge of bone tumor staging parameters will help the radiologist produce meaningful reports. Fig year-old man with giant cell tumor of bone., Wrist radiograph shows slightly expansile radiolucent lesion of distal radius extending to articular surface., Fat-suppressed T1-weighted coronal MR image of wrist after IV administration of gadolinium chelate shows giant cell tumor with soft-tissue extension (arrow). References 1. Morrison W, Dalinka MK, Daffner RH, et al. one tumors. In: CR appropriateness criteria. Reston, V: merican College of Radiology, 2005: Sundaram M, McLeod R. MR imaging of tumor and tumorlike lesions of bone and soft tissue. JR 1990; 155: Resnick D. Tumors and tumor-like lesions of bone: radiographic principles. In: Resnick D, ed. Diagnosis of bone and joint disorders. Philadelphia, P: Saunders, 2002: rdran GM. one destruction not demonstrable by radiography. r J Radiol 1951; 24: Frank J, Ling, Patronas NJ, et al. Detection of malignant bone tumors: MR imaging vs scintigraphy. JR 1990; 155: El-Khoury GY, ennett DL, Dalinka MK, et al. Metastatic bone disease. In: CR appropriateness criteria. Reston, V: merican College of Radiology, 2005: Deely D, Schwietzer M. Imaging evaluation of the patient with suspected bone tumor. In: Taveras JM, Ferrucci JT, ed. Radiology, vol. 5. Philadelphia, P: Lippincott Williams & Wilkins, 1998: chapter 74, pp Rougraff T, Kneisl JS, Simon M. Skeletal metastases of unknown origin: a prospective study of a diagnostic strategy. J one Joint Surg m 1993; 75: ngtuaco EJC, Fassas T, Walker R, Sethi R, arlogie. Multiple myeloma: clinical review and diagnostic imaging. Radiology 2004; 231: Lodwick GS, Wilson J, Farrell C, Virtama P, Dittrich F. Determining growth rates of focal lesions of bone from radiographs. Radiology 1980; 134: Zimmer WD, erquist TH, McLeod R, et al. one tumors: magnetic resonance imaging versus CT. Radiology 1985; 155: Hogeboom WR, Hoekstra HJ, Mooyart EL, et al. MRI or CT in the preoperative diagnosis of bone tumors. Eur J Surg Oncol 1992; 18: Salamipour H, Jimenez RM, rec SL, Chapman VM, Kalra MK, Jaramillo D. Multidetector row CT in pediatric musculoskeletal imaging. Pediatr Radiol 2005; 35: Enneking WF, Spanier SS, Goodman M. system for the surgical staging of musculoskeletal sarcoma. Clin Orthop 1980; 153: Peabody TD, Gibbs CP Jr, Simon M. Evaluation and staging of musculoskeletal neoplasms. J one Joint Surg m 1998; 80: merican Joint Committee on Cancer. one. In: Fleming ID, Cooper JS, Henson DE, et al., eds. JCC cancer staging manual. Philadelphia, P: Lippincott-Raven, 1997: merican Joint Committee on Cancer. one. In: Greene FL, Page DL, Fleming ID, et al., eds. JCC cancer staging manual. New York, NY: Springer- Verlag, 2002: Heck RK, Stacy GS, Flaherty MJ, Montag G, Peabody TD, Simon M. comparison study of stag- JR:186, pril
10 ing systems for bone sarcomas. Clin Orthop Relat Res 2003; 415: loem JL, Taminiau H, Eulderink F, Hermans J, Pauwels EK. Radiologic staging of primary bone sarcoma: MRI, scintigraphy, angiography and CT correlated with pathologic examination. Radiology 1988; 169: oyko O, Cory D, Cohen MD, Provisor, Mirkin D, DeRosa GP. MR imaging of osteogenic and Ewing s sarcoma. JR 1987; 148: Simon M, Kirchner PT. Scintigraphic evaluation of primary bone tumors: comparison of technetium- 99m phosphonate and gallium citrate imaging. J one Joint Surg m 1980; 62: Sundaram M. The use of gadolinium in the MR imaging of bone tumors. Semin Ultrasound CT MR 1997; 18: May D, Good R, Smith DK, Parsons TW. MR imaging of musculoskeletal tumors and tumor mimickers with intravenous gadolinium: experience with 242 patients. Skeletal Radiol 1997; 26: Verstraete KL, Lang P. one and soft tissue tumors: the role of contrast agents for MR imaging. Eur J Radiol 2000; 34: risse H, Ollivier L, Edeline V, et al. Imaging of malignant tumours of the long bones in children: monitoring response to neoadjuvant chemotherapy and preoperative assessment. Pediatr Radiol 2004; 34: Reddick WE, Wang S, Xiong X, et al. Dynamic magnetic resonance imaging of regional contrast access as an additional prognostic factor in pediatric osteosarcoma. Cancer 2001; 91: Egmont-Petersen M, Hogendoorn PCW, van der Geest RJ, et al. Detection of areas with viable remnant tumor in postchemotherapy patients with Ewing s sarcoma by dynamic contrast-enhanced MRI using pharmacokinetic modeling. Magn Reson Imaging 2000; 18: Ongolo-Zogo P, Thiesse P, Sau J, et al. ssessment of osteosarcoma response to neoadjuvant chemotherapy: comparative usefulness of dynamic gadolinium-enhanced spin-echo magnetic resonance imaging and technetium-99m skeletal angioscintigraphy. Eur Radiol 1999; 9: El Khadrawy M, Hoffer F, Reddick W. Ewing sarcoma recurrence vs radiation necrosis in dynamic contrast-enhanced MR imaging: a case report. Pediatr Radiol 1999; 29: Franzius C, Daldrup-Link HE, Sciuk J, et al. FDG- PET for detection of pulmonary metastases from malignant primary bone tumors: comparison with spiral CT. nn Oncol 2001; 12: McKillop JH, Etcubanas E, Goris ML. The indications for and limitations of bone scintigraphy in osteogenic sarcoma: a review of 55 patients. Cancer 1981; 48: Goldstein G, McNeil J, Zufall E, Jaffe N, Treves S. Changing indications for bone scintigraphy in patients with osteosarcoma. Radiology 1980; 135: Hawkins DS, Rajendran JG, Conrad EU, ruckner JD, Eary JF. Evaluation of chemotherapy response in pediatric bone sarcomas by [F-18]-fluorodeoxy- D-glucose positron emission tomography. Cancer 2002; 94: Franzius C, Schulte M, Hillmann, et al. Clinical value of positron emission tomography (PET) in the diagnosis of bone and soft-tissue tumors. 3rd Interdisciplinary Consensus Conference PET in oncology : results of the one and Soft-Tissue Study Group [in German]. Chirurg 2001; 72: Franzius C, Sciuk J, rinkschmidt C, Jurgens H, Schober O. Evaluation of chemotherapy response in primary bone tumors with F-18 FDG positron emission tomography compared with histologically assessed tumor necrosis. Clin Nucl Med 2000; 25: Enneking WF. Staging musculoskeletal tumors. In: Enneking WF, ed. Musculoskeletal tumor surgery. New York, NY: Churchill Livingstone, 1983:87 88 FOR YOUR INFORMTION This article is available for CME credit. See supplemental data for this article at or visit for more information. 976 JR:186, pril 2006
Staging of Bone Tumors: A Review with Illustrative Examples
 Staging one Tumors Musculoskeletal Imaging Review C D E M N E U T R Y L I M C I G O F I N G Gregory S. Stacy 1 Ravinder S. Mahal 1,2 Terrance D. Peabody 3 Stacy GS, Mahal RS, Peabody TD Keywords: bone
Staging one Tumors Musculoskeletal Imaging Review C D E M N E U T R Y L I M C I G O F I N G Gregory S. Stacy 1 Ravinder S. Mahal 1,2 Terrance D. Peabody 3 Stacy GS, Mahal RS, Peabody TD Keywords: bone
The Radiology Assistant : Bone tumor - ill defined osteolytic tumors and tumor-like lesions
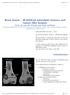 Bone tumor - ill defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
Bone tumor - ill defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
General Approach to Lytic Bone Lesions D. Lee Bennett, MD, MA, Georges Y. El Khoury, MD Appl Radiol. 2004;33(5)
 General Approach to Lytic Bone Lesions D. Lee Bennett, MD, MA, Georges Y. El Khoury, MD Appl Radiol. 2004;33(5) www.medscape.com Abstract and Introduction Abstract When interpreting musculoskeletal radiographs,
General Approach to Lytic Bone Lesions D. Lee Bennett, MD, MA, Georges Y. El Khoury, MD Appl Radiol. 2004;33(5) www.medscape.com Abstract and Introduction Abstract When interpreting musculoskeletal radiographs,
MRI XR, CT, NM. Principal Modality (2): Case Report # 2. Date accepted: 15 March 2013
 Radiological Category: Musculoskeletal Principal Modality (1): Principal Modality (2): MRI XR, CT, NM Case Report # 2 Submitted by: Hannah Safia Elamir, D.O. Faculty reviewer: Naga R. Chinapuvvula, M.D.
Radiological Category: Musculoskeletal Principal Modality (1): Principal Modality (2): MRI XR, CT, NM Case Report # 2 Submitted by: Hannah Safia Elamir, D.O. Faculty reviewer: Naga R. Chinapuvvula, M.D.
Bone Tumors Clues and Cues
 William Herring, M.D. 2002 Bone Tumors Clues and Cues In Slide Show mode, advance the slides by pressing the spacebar All Photos Retain the Copyright of their Authors Clues by Appearance of Lesion Patterns
William Herring, M.D. 2002 Bone Tumors Clues and Cues In Slide Show mode, advance the slides by pressing the spacebar All Photos Retain the Copyright of their Authors Clues by Appearance of Lesion Patterns
COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED
 84 COPYRIGHT 2004 BY THE JOURNAL BONE AND JOINT SURGERY, INCORPORATED Radiographic Evaluation of Pathological Bone Lesions: Current Spectrum of Disease and Approach to Diagnosis BY BENJAMIN G. DOMB, MD,
84 COPYRIGHT 2004 BY THE JOURNAL BONE AND JOINT SURGERY, INCORPORATED Radiographic Evaluation of Pathological Bone Lesions: Current Spectrum of Disease and Approach to Diagnosis BY BENJAMIN G. DOMB, MD,
Mark D. Murphey, MD, FACR
 Fundamental Concepts of Musculoskeletal Neoplasm: CT and MRI Mark D. Murphey, MD, FACR Important Features in Evaluation of Musculoskeletal Masses Differential diagnosis Preoperative assessment and staging
Fundamental Concepts of Musculoskeletal Neoplasm: CT and MRI Mark D. Murphey, MD, FACR Important Features in Evaluation of Musculoskeletal Masses Differential diagnosis Preoperative assessment and staging
MARK D. MURPHEY MD, FACR. Physician-in-Chief, AIRP. Chief, Musculoskeletal Imaging
 ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE MARK D. MURPHEY MD, FACR Physician-in-Chief, AIRP Chief, Musculoskeletal Imaging ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE Giant cell tumor (GCT) Unicameral
ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE MARK D. MURPHEY MD, FACR Physician-in-Chief, AIRP Chief, Musculoskeletal Imaging ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE Giant cell tumor (GCT) Unicameral
A Modified Lodwick-Madewell Grading System for the Evaluation of Lytic Bone Lesions
 Musculoskeletal Imaging Original Research Caracciolo et al. Evaluation of Lytic one Lesions Musculoskeletal Imaging Original Research Jamie T. Caracciolo 1 H. Thomas Temple 2 G. Douglas Letson 3 Mark J.
Musculoskeletal Imaging Original Research Caracciolo et al. Evaluation of Lytic one Lesions Musculoskeletal Imaging Original Research Jamie T. Caracciolo 1 H. Thomas Temple 2 G. Douglas Letson 3 Mark J.
ARTICLE. MR imaging in staging of bone tumors
 Cancer Imaging (2006) 6, 158 162 DOI: 10.1102/1470-7330.2006.0026 CI ARTICLE MR imaging in staging of bone tumors Shigeru Ehara Department of Radiology, Iwate Medical University School of Medicine, Morioka
Cancer Imaging (2006) 6, 158 162 DOI: 10.1102/1470-7330.2006.0026 CI ARTICLE MR imaging in staging of bone tumors Shigeru Ehara Department of Radiology, Iwate Medical University School of Medicine, Morioka
Radiography in the Initial Diagnosis of Primary Bone Tumors
 Residents Section Structured Review Costelloe and Madewell Radiography of Primary Bone Tumors Residents Section Structured Review Colleen M. Costelloe 1 John E. Madewell Costelloe CM, Madewell JE Keywords:
Residents Section Structured Review Costelloe and Madewell Radiography of Primary Bone Tumors Residents Section Structured Review Colleen M. Costelloe 1 John E. Madewell Costelloe CM, Madewell JE Keywords:
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Musculoskeletal tumours Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary bone tumours 3 Clinical
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Musculoskeletal tumours Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary bone tumours 3 Clinical
Review Course «Musculoskeletal Oncology» October 6, 2011 UNIKLINIK BALGRIST. Imaging of Bone and Soft Tissue. Tumors
 Imaging of Bone and Soft Tissue Tumors Approach from a radiologist s point of view Florian Buck Radiology Radio- Radio- Oncologist Oncologist Orthopedist Orthopedist Patient Management Oncologist Oncologist
Imaging of Bone and Soft Tissue Tumors Approach from a radiologist s point of view Florian Buck Radiology Radio- Radio- Oncologist Oncologist Orthopedist Orthopedist Patient Management Oncologist Oncologist
Downloaded from by on 11/21/17 from IP address Copyright ARRS. For personal use only; all rights reserved
 Downloaded from www.ajronline.org by 46.3.196.1 on 11/21/17 from IP address 46.3.196.1. opyright RRS. For personal use only; all rights reserved T he scapula is a small bone in which many neoplasms can
Downloaded from www.ajronline.org by 46.3.196.1 on 11/21/17 from IP address 46.3.196.1. opyright RRS. For personal use only; all rights reserved T he scapula is a small bone in which many neoplasms can
The Radiology Assistant : Bone tumor - well-defined osteolytic tumors and tumor-like lesions
 Bone tumor - well-defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
Bone tumor - well-defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
Radiologic Pathologic Correlation of Intraosseous Lipomas. Tim Propeck 1, Mary Anne Bullard 1, John Lin 1, Kei Doi 2, William Martel 1
 Downloaded from www.ajronline.org by 148.251.232.83 on 04/10/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Radiologic Pathologic orrelation of Intraosseous
Downloaded from www.ajronline.org by 148.251.232.83 on 04/10/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Radiologic Pathologic orrelation of Intraosseous
APMA 2018 Radiology Track Bone Tumors When to say Gulp!
 APMA 2018 Radiology Track Bone Tumors When to say Gulp! DANIEL P. EVANS, DPM, FACFAOM Professor, Department of Podiatric Medicine and Radiology Dr. Wm. Scholl College of Podiatric Medicine Conflict of
APMA 2018 Radiology Track Bone Tumors When to say Gulp! DANIEL P. EVANS, DPM, FACFAOM Professor, Department of Podiatric Medicine and Radiology Dr. Wm. Scholl College of Podiatric Medicine Conflict of
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Disclosures. Giant Cell Rich Tumors of Bone. Outline. The osteoclast. Giant cell rich tumors 5/21/11
 Disclosures Giant Cell Rich Tumors of Bone Andrew Horvai, MD, PhD Associate Clinical Professor, Pathology This lecture discusses "off label" uses of a number of pharmaceutical agents. The speaker is describing
Disclosures Giant Cell Rich Tumors of Bone Andrew Horvai, MD, PhD Associate Clinical Professor, Pathology This lecture discusses "off label" uses of a number of pharmaceutical agents. The speaker is describing
Fluid-fluid levels in bone tumors: A pictorial review
 Fluid-fluid levels in bone tumors: A pictorial review Poster No.: C-578 Congress: ECR 2009 Type: Educational Exhibit Topic: Musculoskeletal Authors: L. Figueroa Nasra, C. Martín Hervás, M. Tapia-Viñé,
Fluid-fluid levels in bone tumors: A pictorial review Poster No.: C-578 Congress: ECR 2009 Type: Educational Exhibit Topic: Musculoskeletal Authors: L. Figueroa Nasra, C. Martín Hervás, M. Tapia-Viñé,
Typical skeletal location and differential diagnosis of bone tumors.
 Typical skeletal location and differential diagnosis of bone tumors. Poster No.: C-2418 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Barros, L. A. Ferreira, Y. Costa, P. J. V. Coelho, F. Caseiro
Typical skeletal location and differential diagnosis of bone tumors. Poster No.: C-2418 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Barros, L. A. Ferreira, Y. Costa, P. J. V. Coelho, F. Caseiro
Evaluation of Bone tumors with Magnetic Resonance Imaging and correlation with surgical and gross pathological findings.
 9-137 611 Evaluation of Bone tumors with Magnetic Resonance Imaging and correlation with surgical and gross pathological findings. S BAWEJA, R ARORA, S SINGH, A SHARMA, P NARANG, S GHUMAN, SK KAPOOR, S
9-137 611 Evaluation of Bone tumors with Magnetic Resonance Imaging and correlation with surgical and gross pathological findings. S BAWEJA, R ARORA, S SINGH, A SHARMA, P NARANG, S GHUMAN, SK KAPOOR, S
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Musculoskeletal Sarcomas
 Musculoskeletal Sarcomas Robert C. Orth, M.D., Ph.D. Edward B. Singleton Department of Pediatric Radiology Texas Children s Hospital Page 0 xxx00.#####.ppt 9/23/2012 9:01:18 AM No disclosures Page 1 xxx00.#####.ppt
Musculoskeletal Sarcomas Robert C. Orth, M.D., Ph.D. Edward B. Singleton Department of Pediatric Radiology Texas Children s Hospital Page 0 xxx00.#####.ppt 9/23/2012 9:01:18 AM No disclosures Page 1 xxx00.#####.ppt
SICOT Online Report E057 Accepted April 23th, in Fibula and Rib
 Metachronous, multicentric giant cell tumors in Fibula and Rib Toshihiro Akisue, Tetsuji Yamamoto ( ), Teruya Kawamoto, Toshiaki Hitora, Takashi Marui, Tetsuya Nakatani, Takafumi Onga, and Masahiro Kurosaka
Metachronous, multicentric giant cell tumors in Fibula and Rib Toshihiro Akisue, Tetsuji Yamamoto ( ), Teruya Kawamoto, Toshiaki Hitora, Takashi Marui, Tetsuya Nakatani, Takafumi Onga, and Masahiro Kurosaka
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010
 Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Introduction to Musculoskeletal Tumors. James C. Wittig, MD Orthopedic Oncologist Sarcoma Surgeon
 Introduction to Musculoskeletal Tumors James C. Wittig, MD Orthopedic Oncologist Sarcoma Surgeon www.tumorsurgery.org Definitions Primary Bone / Soft tissue tumors Mesenchymally derived tumors (Mesodermal)
Introduction to Musculoskeletal Tumors James C. Wittig, MD Orthopedic Oncologist Sarcoma Surgeon www.tumorsurgery.org Definitions Primary Bone / Soft tissue tumors Mesenchymally derived tumors (Mesodermal)
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Skeletal Radiology. Solitary (unicameral) bone cyst. The fallen fragment sign revisited
 Skeletal Radiol (1989) 18:261-265 Skeletal Radiology Solitary (unicameral) bone cyst The fallen fragment sign revisited S. Struhl, M.D., C. Edelson, M.D., H. Pritzker, M.D., L.P. Seimon, M.D., and H.D.
Skeletal Radiol (1989) 18:261-265 Skeletal Radiology Solitary (unicameral) bone cyst The fallen fragment sign revisited S. Struhl, M.D., C. Edelson, M.D., H. Pritzker, M.D., L.P. Seimon, M.D., and H.D.
Primary bone tumors > metastases from other sites Primary bone tumors widely range -from benign to malignant. Classified according to the normal cell
 Primary bone tumors > metastases from other sites Primary bone tumors widely range -from benign to malignant. Classified according to the normal cell counterpart and line of differentiation. Among the
Primary bone tumors > metastases from other sites Primary bone tumors widely range -from benign to malignant. Classified according to the normal cell counterpart and line of differentiation. Among the
Musculoskeletal Radiology
 Musculoskeletal Radiology Hong Kong College of Radiologists MS 1 Acute osteomyelitis Acute osteomyelitis Plain radiographs reviewed Spine Other bones MRI Acute osteomyelitis diagnosed Acute osteomyelitis
Musculoskeletal Radiology Hong Kong College of Radiologists MS 1 Acute osteomyelitis Acute osteomyelitis Plain radiographs reviewed Spine Other bones MRI Acute osteomyelitis diagnosed Acute osteomyelitis
Publication for the Philips MRI Community
 FieldStrength Publication for the Philips MRI Community Issue 38 Summer 2009 Pediatric MSK imaging benefits from tailored scan protocols Vanderbilt University Children s Hospital builds dedicated scans
FieldStrength Publication for the Philips MRI Community Issue 38 Summer 2009 Pediatric MSK imaging benefits from tailored scan protocols Vanderbilt University Children s Hospital builds dedicated scans
Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C.
 Role of Whole-body Diffusion MR in Detection of Metastatic lesions Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C. Cancer is a potentially life-threatening disease,
Role of Whole-body Diffusion MR in Detection of Metastatic lesions Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C. Cancer is a potentially life-threatening disease,
Effective local and systemic therapy is necessary for the cure of Ewing tumor Most chemotherapy regimens are a combination of cyclophosphamide,
 Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
Malignant bone tumors. Incidence Myeloma 45% Osteosarcoma 24% Chondrosarcoma 12% Lyphoma 8% Ewing s Sarcoma 7%
 Malignant bone tumors Incidence Myeloma 45% Osteosarcoma 24% Chondrosarcoma 12% Lyphoma 8% Ewing s Sarcoma 7% Commonest primary bone sarcoma is osteosarcoma X ray Questions to ask 1. Solitary or Multiple
Malignant bone tumors Incidence Myeloma 45% Osteosarcoma 24% Chondrosarcoma 12% Lyphoma 8% Ewing s Sarcoma 7% Commonest primary bone sarcoma is osteosarcoma X ray Questions to ask 1. Solitary or Multiple
STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD
 STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD WHAT DO YOU DO WHEN THIS SHOWS UP IN YOUR OFFICE? besides panicking KEY PRINCIPLE!!! Reactive zone is the edema, neovascularity and inflammation
STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD WHAT DO YOU DO WHEN THIS SHOWS UP IN YOUR OFFICE? besides panicking KEY PRINCIPLE!!! Reactive zone is the edema, neovascularity and inflammation
Bone Tumours - a synopsis. Dr Zena Slim SpR in Histopathology QAH 2009
 Bone Tumours - a synopsis Dr Zena Slim SpR in Histopathology QAH 2009 Aims General approach to diagnosis Common entities.and not so common ones. Mini quiz Challenge of bone tumour diagnosis Bone tumours
Bone Tumours - a synopsis Dr Zena Slim SpR in Histopathology QAH 2009 Aims General approach to diagnosis Common entities.and not so common ones. Mini quiz Challenge of bone tumour diagnosis Bone tumours
MRI and CT Evaluation of Primary Bone and Soft- Tissue Tumors
 749 Alex M. Aisen1 William Martel1 Ethan M. Braunstein1 Kim I. McMillin1 William A. Phillips2 Thomas F. KIing2 Received June 10, 1985; accepted after revision December 23, 1985. Presented at the annu meeting
749 Alex M. Aisen1 William Martel1 Ethan M. Braunstein1 Kim I. McMillin1 William A. Phillips2 Thomas F. KIing2 Received June 10, 1985; accepted after revision December 23, 1985. Presented at the annu meeting
Guidelines for Specialist Referral for Newly Identified Bone Lesions
 MSTS Evidence Based Medicine Committee: Eric R. Henderson MD (Lead Author) Patrick J. Getty, MD Lawrence R. Menendez, MD Benjamin J. Miller, MD Christian M. Ogilvie, MD Rajiv Rajani, MD Steven W. Thorpe,
MSTS Evidence Based Medicine Committee: Eric R. Henderson MD (Lead Author) Patrick J. Getty, MD Lawrence R. Menendez, MD Benjamin J. Miller, MD Christian M. Ogilvie, MD Rajiv Rajani, MD Steven W. Thorpe,
Department of Radiology, University of Szeged. Imaging of the skeleton
 Imaging of the skeleton Methods of examination: plain x-ray (radiography, densitometry) x-ray with contrast material (fistulography, angiography) ultrasound (b-mode, Doppler, color, duplex) computed tomography
Imaging of the skeleton Methods of examination: plain x-ray (radiography, densitometry) x-ray with contrast material (fistulography, angiography) ultrasound (b-mode, Doppler, color, duplex) computed tomography
What s new in bone and soft tissue sarcoma Treatment and Guidelines 2012? Rob Grimer
 What s new in bone and soft tissue sarcoma Treatment and Guidelines 2012? Rob Grimer ESMO conference 2012 Top Oncologists in world (~ 400) Lots of sarcoma basic science key messages: 40% of STS diagnoses
What s new in bone and soft tissue sarcoma Treatment and Guidelines 2012? Rob Grimer ESMO conference 2012 Top Oncologists in world (~ 400) Lots of sarcoma basic science key messages: 40% of STS diagnoses
Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage
 Accepted February 13th, 2004 Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage Ludwig Schwering¹, Markus Uhl² and Georg W. Herget( )¹ ¹ Department of Orthopaedics and Traumatology,
Accepted February 13th, 2004 Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage Ludwig Schwering¹, Markus Uhl² and Georg W. Herget( )¹ ¹ Department of Orthopaedics and Traumatology,
Disseminated Primary Non-Hodgkin s Lymphoma of Bone : A Case Re p o r t 1
 Disseminated Primary Non-Hodgkin s Lymphoma of Bone : A Case Re p o r t 1 Hee-Jin Park, M.D., Sung-Moon Lee, M.D., Hee-Jung Lee, M.D., Jung-Sik Kim, M.D., Hong Kim, M.D. Primary lymphoma of bone is uncommon
Disseminated Primary Non-Hodgkin s Lymphoma of Bone : A Case Re p o r t 1 Hee-Jin Park, M.D., Sung-Moon Lee, M.D., Hee-Jung Lee, M.D., Jung-Sik Kim, M.D., Hong Kim, M.D. Primary lymphoma of bone is uncommon
Radiologic approach to pediatric lytic bone lesions
 Radiologic approach to pediatric lytic bone lesions Poster No.: C-1177 Congress: ECR 2016 Type: Educational Exhibit Authors: J. L. LERMA GALLARDO, I. de la Pedraja, A. Lancharro 1 1 1 2 1 1 Zapata, J.
Radiologic approach to pediatric lytic bone lesions Poster No.: C-1177 Congress: ECR 2016 Type: Educational Exhibit Authors: J. L. LERMA GALLARDO, I. de la Pedraja, A. Lancharro 1 1 1 2 1 1 Zapata, J.
F NaF PET/CT in the Evaluation of Skeletal Malignancy
 F NaF PET/CT in the Evaluation of Skeletal Malignancy Andrei Iagaru, MD September 26, 2013 School of of Medicine Ø Introduction Ø F NaF PET/CT in Primary Bone Cancers Ø F NaF PET/CT in Bone Metastases
F NaF PET/CT in the Evaluation of Skeletal Malignancy Andrei Iagaru, MD September 26, 2013 School of of Medicine Ø Introduction Ø F NaF PET/CT in Primary Bone Cancers Ø F NaF PET/CT in Bone Metastases
Disclosure. Acknowledgement. What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Rectal cancer imaging. None
 What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Zhen Jane Wang, MD Assistant Professor in Residence UC SF Department of Radiology Disclosure None Acknowledgement Hueylan Chern, MD, Department
What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Zhen Jane Wang, MD Assistant Professor in Residence UC SF Department of Radiology Disclosure None Acknowledgement Hueylan Chern, MD, Department
Chealon Miller, HMS IV Gillian Lieberman, MD. November Stress Fractures. Chealon Miller, Harvard Medical School Year IV Gillian Lieberman, MD
 November 2005 Stress Fractures Chealon Miller, Harvard Medical School Year IV Our Patient G.F. 29 year old female runner c/o left shin pain and swelling Evaluated at OSH with MRI showing a mass Referred
November 2005 Stress Fractures Chealon Miller, Harvard Medical School Year IV Our Patient G.F. 29 year old female runner c/o left shin pain and swelling Evaluated at OSH with MRI showing a mass Referred
MRI of Pediatric Ankle and Foot. Mahesh Thapa, MD Associate Professor Seattle Children s University of Washington School of Medicine
 MRI of Pediatric Ankle and Foot Mahesh Thapa, MD Associate Professor Seattle Children s University of Washington School of Medicine Disclosures Under contract with Lippincott Williams and Wilkins (LWW)
MRI of Pediatric Ankle and Foot Mahesh Thapa, MD Associate Professor Seattle Children s University of Washington School of Medicine Disclosures Under contract with Lippincott Williams and Wilkins (LWW)
Guidelines for Specialist Referral in Newly Identified Bone Lesions
 Evidence Based Medicine Committee: Patrick J. Getty, MD Eric R. Henderson MD (Lead Author) Lawrence R. Menendez, MD Benjamin J. Miller, MD (Chair) Christian M. Ogilvie, MD Rajiv Rajani, MD Felasfa Wodajo,
Evidence Based Medicine Committee: Patrick J. Getty, MD Eric R. Henderson MD (Lead Author) Lawrence R. Menendez, MD Benjamin J. Miller, MD (Chair) Christian M. Ogilvie, MD Rajiv Rajani, MD Felasfa Wodajo,
SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, :00 12:10 p.m.
 SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, 2018 10:00 12:10 p.m. Staging Susan E. Sharp, MD 1. In the International Neuroblastoma Risk Group Staging
SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, 2018 10:00 12:10 p.m. Staging Susan E. Sharp, MD 1. In the International Neuroblastoma Risk Group Staging
Screening for and Assessment of Osteonecrosis in Oncology Patients. Sue C. Kaste, DO SPR Postgraduate Course 2015
 Screening for and Assessment of Osteonecrosis in Oncology Patients Sue C. Kaste, DO SPR Postgraduate Course 2015 The author declares no potential conflicts of interest or financial disclosures Osteonecrosis
Screening for and Assessment of Osteonecrosis in Oncology Patients Sue C. Kaste, DO SPR Postgraduate Course 2015 The author declares no potential conflicts of interest or financial disclosures Osteonecrosis
Original Report. Sacral Fractures: A Potential Pitfall of FDG Positron Emission Tomography
 Downloaded from www.ajronline.org by 37.44.199.199 on 12/24/17 from IP address 37.44.199.199. opyright RRS. For personal use only; all rights reserved Laura M. Fayad 1 hristian ohade Richard L. Wahl Elliot
Downloaded from www.ajronline.org by 37.44.199.199 on 12/24/17 from IP address 37.44.199.199. opyright RRS. For personal use only; all rights reserved Laura M. Fayad 1 hristian ohade Richard L. Wahl Elliot
Chondrosarcoma with a late local relapse
 Chondrosarcoma with a late local relapse J. Shinoda, T. Ozaki, T. Oka, T. Kunisada, H. Inoue Department of Orthopaedic Surgery, Okayama University Medical School, Okayama, 700-8558, Japan Correspondence:
Chondrosarcoma with a late local relapse J. Shinoda, T. Ozaki, T. Oka, T. Kunisada, H. Inoue Department of Orthopaedic Surgery, Okayama University Medical School, Okayama, 700-8558, Japan Correspondence:
Imaging Findings Of Bone Tumors: A Pictorial Review
 Imaging Findings Of Bone Tumors: A Pictorial Review Poster No.: C-2511 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Limeme, N. Benzina, A. BelKhiria, H. Zaghouani, S. Majdoub, N. Mallat, H.
Imaging Findings Of Bone Tumors: A Pictorial Review Poster No.: C-2511 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Limeme, N. Benzina, A. BelKhiria, H. Zaghouani, S. Majdoub, N. Mallat, H.
FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION
 FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION CPT/HCPCS Codes 78300 Bone and/or joint imaging; limited area 78305 multiple areas 78306 whole body 78315 three phase study
FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION CPT/HCPCS Codes 78300 Bone and/or joint imaging; limited area 78305 multiple areas 78306 whole body 78315 three phase study
University Journal of Surgery and Surgical Specialities
 University Journal of Surgery and Surgical Specialities Volume 1 Issue 1 2015 EXTRA SKELETAL MESENCHYMAL CHONDROSARCOMA :A CASE REPORT Rajaraman R Subbiah S Navin Naushad Kilpaulk Medical College Abstract:
University Journal of Surgery and Surgical Specialities Volume 1 Issue 1 2015 EXTRA SKELETAL MESENCHYMAL CHONDROSARCOMA :A CASE REPORT Rajaraman R Subbiah S Navin Naushad Kilpaulk Medical College Abstract:
Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation
 Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Solitary Bone Cyst of the Lunate: A Case Report
 Cronicon OPEN ACCESS ORTHOPAEDICS Case Report Solitary Bone Cyst of the Lunate: A Case Report MihirDesai* and Shivanand Bandekar Department of Orthopedics, Goa Medical College, Goa, India *Corresponding
Cronicon OPEN ACCESS ORTHOPAEDICS Case Report Solitary Bone Cyst of the Lunate: A Case Report MihirDesai* and Shivanand Bandekar Department of Orthopedics, Goa Medical College, Goa, India *Corresponding
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR MAGNETIC RESONANCE IMAGING:
 National Imaging Associates, Inc. Clinical guidelines BONE MARROW MRI Original Date: July 2008 Page 1 of 5 CPT Codes: 77084 Last Review Date: September 2014 NCD 220.2 MRI Last Effective Date: July 2011
National Imaging Associates, Inc. Clinical guidelines BONE MARROW MRI Original Date: July 2008 Page 1 of 5 CPT Codes: 77084 Last Review Date: September 2014 NCD 220.2 MRI Last Effective Date: July 2011
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
GIANT CELL-RICH OSTEOSARCOMA: A CASE REPORT
 Nagoya J. Med. Sci. 59. 151-157, 1996 CASE REPORTS GIANT CELL-RICH OSTEOSARCOMA: A CASE REPORT KEIJI SATO!, SHIGEKI YAMAMURA!, HISASHI IWATA!, HIDESHI SUGIURA 2, NOBUO NAKASHIMA 3 and TETSURO NAGASAKA
Nagoya J. Med. Sci. 59. 151-157, 1996 CASE REPORTS GIANT CELL-RICH OSTEOSARCOMA: A CASE REPORT KEIJI SATO!, SHIGEKI YAMAMURA!, HISASHI IWATA!, HIDESHI SUGIURA 2, NOBUO NAKASHIMA 3 and TETSURO NAGASAKA
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD
 Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Bone tumors. RMG: jan
 Bone tumors RMG: jan 217. @Kijohs KIZZA JOHN KIJOHS Diseases arising in bone Lipoma Fibrous cortical defects Non-ossifying fibroma Bone island Benign simple cysts Enchondroma Osteochondroma Osteoid osteoma
Bone tumors RMG: jan 217. @Kijohs KIZZA JOHN KIJOHS Diseases arising in bone Lipoma Fibrous cortical defects Non-ossifying fibroma Bone island Benign simple cysts Enchondroma Osteochondroma Osteoid osteoma
Bone PET/MRI : Diagnostic yield in bone metastases and malignant primitive bone tumors
 Bone PET/MRI : Diagnostic yield in bone metastases and malignant primitive bone tumors Lars Stegger, Benjamin Noto Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to
Bone PET/MRI : Diagnostic yield in bone metastases and malignant primitive bone tumors Lars Stegger, Benjamin Noto Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to
Case 8 Soft tissue swelling
 Case 8 Soft tissue swelling 26-year-old female presented with a swelling on the back of the left knee joint since the last 6 months and chronic pain in the calf and foot since the last 2 months. Pain in
Case 8 Soft tissue swelling 26-year-old female presented with a swelling on the back of the left knee joint since the last 6 months and chronic pain in the calf and foot since the last 2 months. Pain in
FDG PET/CT STAGING OF LUNG CANCER. Dr Shakher Ramdave
 FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
International Journal of Research in Health Sciences ISSN: Available online at: Case Study
 International Journal of Research in Health Sciences ISSN: 2321-7251 Available online at: http://www.ijrhs.org/ Case Study Foreign body granuloma mimicking a soft tissue neoplasm *Rohan Sawant, Abhishek
International Journal of Research in Health Sciences ISSN: 2321-7251 Available online at: http://www.ijrhs.org/ Case Study Foreign body granuloma mimicking a soft tissue neoplasm *Rohan Sawant, Abhishek
Clinical indications for positron emission tomography
 Clinical indications for positron emission tomography Oncology applications Brain and spinal cord Parotid Suspected tumour recurrence when anatomical imaging is difficult or equivocal and management will
Clinical indications for positron emission tomography Oncology applications Brain and spinal cord Parotid Suspected tumour recurrence when anatomical imaging is difficult or equivocal and management will
Focal Sclerosis in a Vertebra: Differential Diagnosis of a Solitary Osteoblastic Metastasis
 July 2001 Focal Sclerosis in a Vertebra: Differential Diagnosis of a Solitary Osteoblastic Metastasis Alice L. Fisher, Harvard Medical School Year IV Review of the Normal Anatomy of a Lumbar Vertebra:
July 2001 Focal Sclerosis in a Vertebra: Differential Diagnosis of a Solitary Osteoblastic Metastasis Alice L. Fisher, Harvard Medical School Year IV Review of the Normal Anatomy of a Lumbar Vertebra:
We have studied 560 patients with osteosarcoma of a
 Osteosarcoma of the limb AMPUTATION OR LIMB SALVAGE IN PATIENTS TREATED BY NEOADJUVANT CHEMOTHERAPY G. Bacci, S. Ferrari, S. Lari, M. Mercuri, D. Donati, A. Longhi, C. Forni, F. Bertoni, M. Versari, E.
Osteosarcoma of the limb AMPUTATION OR LIMB SALVAGE IN PATIENTS TREATED BY NEOADJUVANT CHEMOTHERAPY G. Bacci, S. Ferrari, S. Lari, M. Mercuri, D. Donati, A. Longhi, C. Forni, F. Bertoni, M. Versari, E.
PET IMAGING (POSITRON EMISSION TOMOGRAPY) FACT SHEET
 Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
SMALL ROUND BLUE CELL LESION OF BONE
 DISCLOSURE SMALL ROUND BLUE CELL LESION OF BONE Dr. Alistair Jordan University of South Alabama No financial support or endorsement OBJECTIVES Describe the more common small round cell lesions of bone
DISCLOSURE SMALL ROUND BLUE CELL LESION OF BONE Dr. Alistair Jordan University of South Alabama No financial support or endorsement OBJECTIVES Describe the more common small round cell lesions of bone
Precursor B-Lymphoblastic Lymphoma Presenting as a Solitary Bone Tumor Mimicking Osteomyelitis on MRI
 ISPUB.COM The Internet Journal of Pathology Volume 5 Number 1 Precursor B-Lymphoblastic Lymphoma Presenting as a Solitary Bone Tumor Mimicking Osteomyelitis on J Mika, L Culton, C Adler, M Uhl, A Kersten,
ISPUB.COM The Internet Journal of Pathology Volume 5 Number 1 Precursor B-Lymphoblastic Lymphoma Presenting as a Solitary Bone Tumor Mimicking Osteomyelitis on J Mika, L Culton, C Adler, M Uhl, A Kersten,
Unusual location of bone sarcoma in children
 Unusual location of bone sarcoma in children Poster No.: C-1517 Congress: ECR 2014 Type: Educational Exhibit Authors: S. JERBI, A. Khalfalli, G. Abid, O. Bradai, N. chouchane, H. HAMZA; Mahdia/TN Keywords:
Unusual location of bone sarcoma in children Poster No.: C-1517 Congress: ECR 2014 Type: Educational Exhibit Authors: S. JERBI, A. Khalfalli, G. Abid, O. Bradai, N. chouchane, H. HAMZA; Mahdia/TN Keywords:
Case Report Giant Cell Tumor of Bone: Documented Progression over 4 Years from Its Origin at the Metaphysis to the Articular Surface
 Volume 2016, Article ID 9786925, 5 pages http://dx.doi.org/10.1155/2016/9786925 Case Report Giant Cell Tumor of Bone: Documented Progression over 4 Years from Its Origin at the Metaphysis to the Articular
Volume 2016, Article ID 9786925, 5 pages http://dx.doi.org/10.1155/2016/9786925 Case Report Giant Cell Tumor of Bone: Documented Progression over 4 Years from Its Origin at the Metaphysis to the Articular
Clinical Study Primary Malignant Tumours of Bone Following Previous Malignancy
 Sarcoma Volume 2008, Article ID 418697, 4 pages doi:10.1155/2008/418697 Clinical Study Primary Malignant Tumours of Bone Following Previous Malignancy J. T. Patton, S. M. M. Sommerville, and R. J. Grimer
Sarcoma Volume 2008, Article ID 418697, 4 pages doi:10.1155/2008/418697 Clinical Study Primary Malignant Tumours of Bone Following Previous Malignancy J. T. Patton, S. M. M. Sommerville, and R. J. Grimer
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Malignant Bone Tumors - Part I: a brief revision of diagnostic aspects with conventional radiology
 Malignant Bone Tumors - Part I: a brief revision of diagnostic aspects with conventional radiology Poster No.: C-2473 Congress: ECR 2013 Type: Educational Exhibit Authors: I. Candelaria, L. B. Barbosa,
Malignant Bone Tumors - Part I: a brief revision of diagnostic aspects with conventional radiology Poster No.: C-2473 Congress: ECR 2013 Type: Educational Exhibit Authors: I. Candelaria, L. B. Barbosa,
OSSEOUS INVASION IN ALVEOLAR SARCOMA OF SOFT TISSUES: A HEALING APPROACH AND LIMB-SALVAGING SURGERY. Summary
 Kovachev V. et. al. Osseous invasion in alveolar sarcoma of soft tissues: Case report OSSEOUS INVASION IN ALVEOLAR SARCOMA OF SOFT TISSUES: A HEALING APPROACH AND LIMB-SALVAGING SURGERY Vihar Ì. Kovachev,
Kovachev V. et. al. Osseous invasion in alveolar sarcoma of soft tissues: Case report OSSEOUS INVASION IN ALVEOLAR SARCOMA OF SOFT TISSUES: A HEALING APPROACH AND LIMB-SALVAGING SURGERY Vihar Ì. Kovachev,
Granulocyte-Stimulating Factor-Induced Bone Marrow Reconversion Simulating Neuroblastoma Metastases on MRI: Case Report and Literature Review
 Radiology Case Reports Volume II, Issue 1, 2007 Granulocyte-Stimulating Factor-Induced Bone Marrow Reconversion Simulating Neuroblastoma Metastases on MRI: Case Report and Literature Review Jason C. Naples,
Radiology Case Reports Volume II, Issue 1, 2007 Granulocyte-Stimulating Factor-Induced Bone Marrow Reconversion Simulating Neuroblastoma Metastases on MRI: Case Report and Literature Review Jason C. Naples,
I have no financial relationships to disclose. I WILL NOT include discussion of investigational or off-label use of a product in my presentation.
 Prostate t Cancer MR Report Disclosure Information Vikas Kundra, M.D, Ph.D. I have no financial relationships to disclose. I WILL NOT include discussion of investigational or off-label use of a g product
Prostate t Cancer MR Report Disclosure Information Vikas Kundra, M.D, Ph.D. I have no financial relationships to disclose. I WILL NOT include discussion of investigational or off-label use of a g product
PET-MRI in malignant bone tumours. Lars Stegger Department of Nuclear Medicine University Hospital Münster, Germany
 PET-MRI in malignant bone tumours Lars Stegger Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to PET/MRI General considerations Bone metastases Primary bone tumours
PET-MRI in malignant bone tumours Lars Stegger Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to PET/MRI General considerations Bone metastases Primary bone tumours
Paediatric post-traumatic osseous cystic lesion following a distal radial fracture
 Paediatric post-traumatic osseous cystic lesion following a distal radial fracture Joey Chan Yiing Beh 1*, Ehab Shaban Mahmoud Hamouda 1 1. Department of Diagnostic Imaging, KK Women's and Children's Hospital,
Paediatric post-traumatic osseous cystic lesion following a distal radial fracture Joey Chan Yiing Beh 1*, Ehab Shaban Mahmoud Hamouda 1 1. Department of Diagnostic Imaging, KK Women's and Children's Hospital,
Special Imaging MUSCULOSKELETAL INFECTION. Special Imaging. Special Imaging. 18yr old male pt What is it? Additional Imaging
 MUSCULOSKELETAL INFECTION Additional Imaging May assist in diagnosis and, possibly, treatment Help create the picture May help differentiate from neoplasia 18yr old male pt What is it? Lymphoma Ewings
MUSCULOSKELETAL INFECTION Additional Imaging May assist in diagnosis and, possibly, treatment Help create the picture May help differentiate from neoplasia 18yr old male pt What is it? Lymphoma Ewings
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Staging Colorectal Cancer
 Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Topics. Musculoskeletal Infection Extremities. Detection of Infection. Role of Imaging in Extremity Infection. Detection of Infection
 Topics Musculoskeletal Infection Extremities Nuttaya Pattamapaspong M.D. Department of Radiology, Faculty of Medicine, Chiang Mai University, Chiang Mai, Thailand Role of imaging in extremity infection
Topics Musculoskeletal Infection Extremities Nuttaya Pattamapaspong M.D. Department of Radiology, Faculty of Medicine, Chiang Mai University, Chiang Mai, Thailand Role of imaging in extremity infection
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 4/30/2011 Radiology Quiz of the Week # 18 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 4/30/2011 Radiology Quiz of the Week # 18 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Prevalence of Meniscal Radial Tears of the Knee Revealed by MRI After Surgery
 Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Incidental Enchondromas of the Knee
 Musculoskeletal Imaging Original Research Musculoskeletal Imaging Original Research Michael J. Walden 1 Mark D. Murphey 1,2,3 Jorge. Vidal 1,2 Walden MJ, Murphey MD, Vidal J Keywords: appendicular musculoskeletal
Musculoskeletal Imaging Original Research Musculoskeletal Imaging Original Research Michael J. Walden 1 Mark D. Murphey 1,2,3 Jorge. Vidal 1,2 Walden MJ, Murphey MD, Vidal J Keywords: appendicular musculoskeletal
Invasive Ductal Carcinoma with Fibrotic Focus: Mammographic and Sonographic Findings with Histopathologic Correlation
 Mammograp hy and Sonography of Invasive Ductal arcinoma reast Imaging linical Observations Shara Millman Oken 1 ecilia L. Mercado 2 Lorenzo Memeo 3 Hanina Hibshoosh 3 Oken SM, Mercado L, Memeo L, Hibshoosh
Mammograp hy and Sonography of Invasive Ductal arcinoma reast Imaging linical Observations Shara Millman Oken 1 ecilia L. Mercado 2 Lorenzo Memeo 3 Hanina Hibshoosh 3 Oken SM, Mercado L, Memeo L, Hibshoosh
Preoperative MR Imaging Assessment of Osteosarcoma: A Radiological - Surgical Correlation
 Chin J Radiol 2001; 26: 9-16 9 ORIGINAL ARTICLE Preoperative MR Imaging Assessment of Osteosarcoma: A Radiological - Surgical Correlation HUNG-TA HONDAR WU 1 CHENG- YEN CHANG 1 JEFF LIN 2 TAIN-HSIUNG CHEN
Chin J Radiol 2001; 26: 9-16 9 ORIGINAL ARTICLE Preoperative MR Imaging Assessment of Osteosarcoma: A Radiological - Surgical Correlation HUNG-TA HONDAR WU 1 CHENG- YEN CHANG 1 JEFF LIN 2 TAIN-HSIUNG CHEN
Primary Intraosseus Xanthoma Involving the Proximal Femur in a Normolipidemic Patient: A Case Report
 CASE REPORT Hip Pelvis 28(3): 182-186, 2016 http://dx.doi.org/10.5371/hp.2016.28.3.182 Print ISSN 2287-3260 Online ISSN 2287-3279 Primary Intraosseus Xanthoma Involving the Proximal Femur in a Normolipidemic
CASE REPORT Hip Pelvis 28(3): 182-186, 2016 http://dx.doi.org/10.5371/hp.2016.28.3.182 Print ISSN 2287-3260 Online ISSN 2287-3279 Primary Intraosseus Xanthoma Involving the Proximal Femur in a Normolipidemic
ORTHOPAEDIC TUMOURS DJM FRANTZEN 2012 AUGUST TUMOURS 1
 ORTHOPAEDIC TUMOURS DJM FRANTZEN 2012 AUGUST TUMOURS 1 PRINCIPLES STAGING WORKUP RADIOLOGY BIOPSY PROCEDURES CHEMOTHERAPY RADIOTHERAPY 2012 AUGUST TUMOURS 2 STAGING ENNEKING'S SURGICAL STAGES (ENNEKING)
ORTHOPAEDIC TUMOURS DJM FRANTZEN 2012 AUGUST TUMOURS 1 PRINCIPLES STAGING WORKUP RADIOLOGY BIOPSY PROCEDURES CHEMOTHERAPY RADIOTHERAPY 2012 AUGUST TUMOURS 2 STAGING ENNEKING'S SURGICAL STAGES (ENNEKING)
Chondroblastoma of bone
 Chronology Chondroblastoma of bone LONG-TERM RESULTS AND FUNCTIONAL OUTCOME AFTER INTRALESIONAL CURETTAGE R. Suneja, R. J. Grimer, M. Belthur, L. Jeys, S. R. Carter, R. M. Tillman, A. M. Davies From The
Chronology Chondroblastoma of bone LONG-TERM RESULTS AND FUNCTIONAL OUTCOME AFTER INTRALESIONAL CURETTAGE R. Suneja, R. J. Grimer, M. Belthur, L. Jeys, S. R. Carter, R. M. Tillman, A. M. Davies From The
Original Report. Nontraumatic Avulsions of the Pelvis. Liem T. Bui-Mansfield 1 3 Felix S. Chew 2 Leon Lenchik 2 Mitch J. Kline 4 Carol A.
 Downloaded from www.ajronline.org by 148.251.232.83 on 05/12/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Liem T. ui-mansfield 1 3 Felix S. hew 2 Leon Lenchik
Downloaded from www.ajronline.org by 148.251.232.83 on 05/12/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Liem T. ui-mansfield 1 3 Felix S. hew 2 Leon Lenchik
The role of Imaging in Ewing sarcoma
 The role of Imaging in Ewing sarcoma Poster No.: P-0109 Congress: ESSR 2014 Type: Educational Poster Authors: D. Beomonte Zobel, C. Dell'atti, M. Bartocci, V. Martinelli, N. 1 2 2 2 1 1 1 2 Magarelli,
The role of Imaging in Ewing sarcoma Poster No.: P-0109 Congress: ESSR 2014 Type: Educational Poster Authors: D. Beomonte Zobel, C. Dell'atti, M. Bartocci, V. Martinelli, N. 1 2 2 2 1 1 1 2 Magarelli,
Ewing sarcoma family of tumors: a pictorial educational review
 Ewing sarcoma family of tumors: a pictorial educational review Poster No.: C-2039 Congress: ECR 2014 Type: Educational Exhibit Authors: F. Moloney, M. Twomey, P. Nicholson, K. O'Regan ; Cork/IE, 1 2 2
Ewing sarcoma family of tumors: a pictorial educational review Poster No.: C-2039 Congress: ECR 2014 Type: Educational Exhibit Authors: F. Moloney, M. Twomey, P. Nicholson, K. O'Regan ; Cork/IE, 1 2 2
Unusual Osteoblastic Secondary Lesion as Predominant Metastatic Disease Spread in Two Cases of Uterine Leiomyosarcoma
 49 Unusual Osteoblastic Secondary Lesion as Predominant Metastatic Disease Spread in Two Cases of Uterine Leiomyosarcoma Loredana Miglietta a Maria Angela Parodi b Luciano Canobbio b Luca Anselmi c a Medical
49 Unusual Osteoblastic Secondary Lesion as Predominant Metastatic Disease Spread in Two Cases of Uterine Leiomyosarcoma Loredana Miglietta a Maria Angela Parodi b Luciano Canobbio b Luca Anselmi c a Medical
