Comparison of three different volumes of mepivacaine in axillary plexus block using multiple nerve stimulation ²
|
|
|
- Hubert Poole
- 5 years ago
- Views:
Transcription
1 British Journal of Anaesthesia 91 (4): 519±24 (2003) DOI: /bja/aeg215 Comparison of three different volumes of mepivacaine in axillary plexus block using multiple nerve stimulation ² A. Serradell*, R. Herrero, J. A. Villanueva, J. A. Santos, J. M. Moncho and J. Masdeu Service of Anaesthesiology and Resuscitation, Hospital de la Creu Roja, Dos de Maig 301, E Barcelona, Spain *Corresponding author. Background. The multiple injection technique for axillary block, in which the four distal nerves of the plexus are located by a nerve stimulator and separately injected, has been shown to provide a high success rate and a short onset time. This randomized double-blind study was conducted to compare the effectiveness of three different volumes of mepivacaine 10 mg ml ±1 in patients undergoing elective distal upper limb surgery under axillary brachial plexus block with the four-nerve approach. The number of complete sensory blocks was the primary ef cacy variable. Methods. A total of 114 adult patients were randomly allocated to receive 36 (n=38), 28 (n=38), and 20 ml (n=38) of mepivacaine 10 mg ml ±1. In each group, volumes were equally distributed in the four nerve territories. In all patients, performance time, latency time, block characteristics, need of supplementary blocks, tourniquet tolerance, duration of analgesia, and complications were recorded. Results. Complete sensory block was obtained in 97% of patients receiving a volume of 36 ml, 97% of those receiving 28 ml, and 94% of those receiving 20 ml. One patient in the group of 28 ml and ve patients in the group of 20 ml experienced pain on in ation of the tourniquet. Two months after surgery, no case of postoperative neurological dysfunction was observed. Conclusions. The three volumes (38, 28, and 20 ml) of mepivacaine 10 mg ml ±1 ensured a similar and high percentage of complete sensory blocks in axillary brachial plexus anaesthesia with nerve stimulation involving the location of four motor responses. Br J Anaesth 2003; 91: 519±24 Keywords: anaesthetic techniques, regional, brachial plexus; anaesthetics local, mepivacaine Accepted for publication: May 28, 2003 Peripheral nerve blocks are widely used to provide anaesthesia for both upper and lower limb surgery. Success of plexus nerve block is dependent on the correct positioning of the local anaesthetic solution near the desired nerves. Demonstration of septa dividing incompletely the axillary sheath 12 refuted the concept of unicompartment structure 3 according to which the injected local anaesthetic solution spread easily by simple diffusion to all nerve components of the brachial plexus and constituted the anatomical basis for the single injection technique. A debate was subsequently initiated between authors advocating the single injection procedure and groups that proposed block with multiple injection techniques. Different studies have compared the results obtained with different methods of nerve location (search for paresthesia, transarterial injection, catheter insertion inside the sheath, neurostimulation) and showed that, independently of the technique used, a better success rate was obtained when dose of the anaesthetic agent was divided into two or more administrations. 45 Since the introduction of the nerve stimulation technique, different studies have compared the ef cacy of brachial plexus block after localization of one or various responses 6±9 and showed that multiple nerve stimulation had a higher success rate than single nerve stimulation procedures. Moreover, three or four nerve response techniques were those with the highest rate of complete sensory block. 10±12 ² Presented in part at the World Congress in Regional Anesthesia and Pain Therapy, Barcelona, Spain, May 29 to June 1, Ó The Board of Management and Trustees of the British Journal of Anaesthesia 2003
2 Serradell et al. Multiple nerve response techniques allow the volume of anaesthetic solution to be administered to be reduced 13 as a diffusion effect through the aponeurotic sheath to reach nerves located more distally from the injection point in axillary plexus block was not necessary. The use of the nerve stimulator and multiple injection technique allows smaller volumes of drugs to be placed closer to the nerves. We are not aware of previously published studies comparing the effectiveness of three different volumes of mepivacaine 10 mg ml ±1 for axillary block with nerve stimulation involving the location of four motor responses. Methods A double-blind, randomized, three-arm parallel study was designed. The study was approved by our hospital ethical committee and all patients gave written informed consent. We studied patients of both sexes (ASA I±III) who were aged 18±80 yr and undergoing elective or acute surgery of the hand, wrist, or forearm under brachial plexus block using the four-nerve stimulation technique. Exclusion criteria consisted of local or systemic disease that contraindicated regional anaesthesia and diseases affecting sensory or motor function of the upper extremity unrelated to the orthopaedic disorder. Patients in whom the arterial pulse was not palpated were excluded. Patients were allocated to one of three anaesthetic groups according to a table of random numbers. Patients in Group A received 36 ml of a plain solution of mepivacaine 10 mg ml ±1, patients in Group B received 28 ml of mepivacaine 10 mg ml ±1, and patients in Group C received 20 ml of mepivacaine 10 mg ml ±1. Patients were pre-medicated with oral lorazepam 1 mg the night before surgery and lorazepam 1 mg sublingually 1 h before operation. Before starting axillary brachial plexus block, midazolam, 1 or 2 mg according to the level of anxiety of the patient, was intravenously administered. The technique of axillary block was the same in all patients. The arm to be operated on was abducted to at least 90 and the forearm was in exion of 90. The arterial pulse was palpated at the level of the major pectoral muscle crossing the axilla and the s.c. tissue overlying the artery was in ltrated with lidocaine 10 mg ml ±1. A 21-gauge 50- mm Te on-coated needle (Locoplex â, Vygon, S.A., Barcelona, Spain) connected to the negative lead of the nerve stimulator (Plexival â, Medival, Italy), which was set to deliver 1 ma pulses at 2 Hz, was used. In all patients, a single puncture was performed. Nerves were located according to speci c twitches elicited by their stimulation (musculocutaneous nerve: forearm exion; median: radial exion of the wrist, 2nd and 3rd nger exion, pronation; ulnar: ulnar exion of the wrist, 4th and 5th nger exion, thumb adduction; radial: wrist and/or nger extension with or without forearm extension). Musculocutaneous and median nerves were located on the external aspect of the axillary artery, whereas ulnar and radial nerves were located on the internal aspect of the artery. This external-to-internal sequence of nerve location was consistently used in all patients. In each manoeuvre, needle position was optimized at the point of motor response when the current was decreased to equal to/less than 0.4 ma. When the location was considered adequate, predetermined volumes of mepivacaine 10 mg ml ±1 were then injected, that is, 36 ml divided into 9 ml for each nerve in patients assigned to Group A, 28 ml divided into 7 ml for each nerve in Group B, and 20 ml divided into 5 ml for each nerve in Group C. At the end of the procedure and in order to improve tourniquet tolerance, block of the intercostobrachial and accessory of the cutaneous brachii medialis nerves was performed by administering 4 ml of the local anaesthetic subcutaneously. The anaesthetist performing the block was aware of the site of surgery, but other staff members unaware of the patient's group evaluated the sensory and motor block. In all axillary plexus blocks performed, dif culties in location of each nerve were assessed by the anaesthetist and de ned as `easy' (one or two attempts), `dif cult' (more than two attempts), and `not localized'. The sensory block was assessed at 10-min intervals with a pinwheel in the skin areas supplied by the ve terminal nerves: musculocutaneous (lateral side of forearm), cutaneous brachii medialis (internal forearm), median (thenar eminence), ulnar (hypothenar eminence), and radial (radial dorsum of the hand). Complete sensory block at 40 min was the primary ef cacy variable. Sensory block was de ned as complete when analgesia and anaesthesia was present in the ve sensory areas 40 min after the end of the axillary block. The block was evaluated as incomplete when only analgesia or neither analgesia nor anaesthesia was present in any of the ve sensory areas evaluated. If pain and touch sensation were felt, patients received supplementary blocks by electrolocating the nerves at the elbow (median, radial) or mid-humerus (ulnar, musculocutaneous) and the sensory assessments continued 50 and 60 min after ending of the primary block. Degree of motor block was evaluated at the same time as sensory block and de ned as complete (absence of mobility) or incomplete (minor movements possible, but not against resistance, or no obvious relaxation) in relation to forearm exion (musculocutaneous), exion of the hand (median), abduction and adduction of the ngers (ulnar), and wrist extension (radial). The following parameters were recorded: block performance time (from insertion to removal of the neurostimulation needle); latency time (from end of axillary block to the time the patient was declared ready for surgery, that is, analgesia and/or anaesthesia in the ve sensory areas evaluated); initial tourniquet tolerance (in all cases, cuff of the tourniquet was in ated to 250 mm Hg); duration of analgesia (from end of axillary block to the start of pain sensation); and local adverse effects during block performance. Neurological sequelae (dysesthesia not related to surgery) were recorded 24 h after the operation and again 2 months later. Patient comfort during the anaesthetic 520
3 Three different volumes of mepivacaine 10 mg ml ±1 Table 1 Patient characteristics and surgical data Variable Mepivacaine 10 mg ml ±1 36 ml 28 ml 20 ml P value Total patients Age, yr, mean (range) 49.7 (20±78) 55.7 (18±80) 57.2 (20±77) NS Sex % women NS Weight, kg, mean (SD) 71.2 (12.7) 73.8 (16.0) 74.8 (15.6) NS ASA status, number (%) NS I 17 (44.7) 12 (31.6) 12 (31.6) II 16 (42.1) 18 (47.4) 18 (47.4) III 5 (13.2) 8 (21.1) 8 (21.1) Localization of surgery, number (%) NS Forearm 4 (10.5) 2 (5.3) 2 (5.3) Wrist 15 (39.5) 16 (42.1) 21 (55.3) Hand 19 (50.0) 20 (52.6) 15 (39.5) Type of procedure NS Soft tissue 27 (71.1) 31 (81.6) 31 (81.6) Osteoarticular 11 (28.9) 7 (18.4) 7 (18.4) Table 2 Results of axillary plexus block with multiple nerve stimulation. *Venous puncture and accidental paresthesia in one patient Variable Mepivacaine 10 mg ml ±1 P value 36 ml 28 ml 20 ml Block performance time, min Mean (SD) 7.6 (2.3) 6.6 (1.6) 6.1 (1.7) Median (range) 7.5 (4±12) 6.0 (4±10) 6.0 (3±10) Local adverse effects, number (%) 9 (23.7) 8 (21.1) 10 (26.3)* NS Venous puncture Arterial puncture Accidental paresthesia during the block Latency time, min Mean (SD) 22.6 (10.9) 20.8 (9.1) 21.9 (11.6) NS Duration of analgesia, min Mean (SD) (39.4) (36.2) (45.0) NS procedure was evaluated on a VAS 0±10 scale before discharge. The patients were also asked to make a comparison between discomfort associated with insertion of the needle and use of the nerve stimulator, as well as if they would undergo the same anaesthetic procedure in the future. The sample size was calculated according to results of a pilot study carried out at our hospital, in which the number of patients with complete sensory block at 30 min was the primary ef cacy variable. Considering an alpha error of 0.05 and a beta error of 0.20, a total of 38 patients per group would be necessary to reject the null hypothesis of nonequivalence between two groups, de ned as a difference of 17.3% or higher and assuming a proportion of complete sensory blocks in one of group of 90%. Statistical analysis of data was performed with the SPSS/ PC+ (version 8.0, SPSS Inc., Chicago, IL) software program. Homogeneity of the three study groups at baseline with regard to age, sex, weight, ASA status, site of operation, and type of procedure was analysed. Quantitative variables in the three study groups were compared using one-way analysis of variance (ANOVA) with Bonferroni's correction in the post-hoc analyses. The Kruskal±Wallis test was used as a non-parametric alternative. Comparison of categorical variables was carried out with the c 2 test or the Fisher's exact test. Data are expressed as mean (SD) unless indicated otherwise. Results A total of 114 patients with a mean (range) age of 54 (18±80) yr were included in the study (60.5% women). There were no differences in patient characteristics, ASA status, and surgical procedures in the three study groups (Table 1). With regard to dif culties in location of each nerve, more than two attempts were required for the radial nerve in 66% of cases, musculocutaneous nerve in 45%, ulnar nerve in 41%, and median nerve in 36%. In no case could nerves not be localized. Results of axillary plexus block are shown in Table 2. There were no differences in relation to duration of analgesia and latency time. However, mean block performance time was signi cantly shorter in patients receiving 20 ml mepivacaine 10 mg ml ±1 compared with 521
4 Serradell et al. Table 3 Assessment of sensory and motor block. *Analgesia only. ² Minor movements possible, but not against resistance. ³ Two nerve territories in one patient Variable Mepivacaine 10 mg ml ±1 P value 36 ml 28 ml 20 ml Sensory block Complete, number (%) 37 (97.4) 37 (97.4) 36 (94.7) NS Incomplete, number (%)* 1 (2.6) 1 (2.6) 2 (5.3) Median nerve Ulnar nerve Radial nerve Musculocutaneous nerve Cutaneous brachii medialis Motor block Complete, number (%) 38 (100) 36 (94.7) 34 (89.5) NS Incomplete, number (%) ² 0 2 (5.3) 4 (10.5) ³ Median nerve Ulnar nerve Radial nerve Musculocutaneous nerve Fig 1 Number of complete sensory blocks obtained in each group at 10, 20, 30, and 40 min after the block (P=NS). 36 ml. Twenty episodes of vascular puncture were recorded during axillary plexus block (venous puncture in 19 cases and arterial puncture in one). The percentages of patients with complete sensory and motor blocks were similar in the three study groups (Table 3). The number of complete sensory blocks obtained in each group at 10, 20, 30, and 40 min was also similar (Fig. 1). In the four cases of incomplete sensory block (analgesia only), supplementary blocks were not performed and all patients were able to undergo surgery without the need of any additional anaesthetic technique. In four patients with complete sensory block at 40 min (ready for surgery), surgical procedures started later than arranged for unknown reasons. These four patients (one in the group of 36 ml, one in the group of 28 ml, and two in the group of 20 ml) experienced pain in the surgical site, 170, 180, 125, and 140 min after axillary plexus block, respectively. Therefore, in order to be able to nish operation, local anaesthetic in ltration was required in two cases and a dose of fentanyl 50±75 mg was given in the remaining two. Two patients required additional sedation with midazolam due to anxiety during surgery. Six patients had tourniquet pain. All these patients had complete sensory and motor block of the musculocutaneous nerve. As shown in Table 4, the percentage of patients experiencing tourniquet pain was higher in the 20 ml mepivacaine 10 mg ml ±1 group, and two patients received a dose of 50 mg fentanyl for pain relief. Another patient in the 20 ml group reported tourniquet pain 70 min after the end of axillary plexus block and was treated with an additional dose of fentanyl and propofol. The level of discomfort associated with the procedure was rated similarly in the three groups; however, most patients rated nerve stimulation worse than needle insertion (Table 4). At the 24-h postoperative assessment, ve cases of dysesthesia were recorded, although none of the patients required treatment and, in all cases, dysesthesia disappeared in about 2 weeks. At the 2-month assessment, three patients reported dysesthesia that had already disappeared at the time of the visit. None of these eight patients had experienced paresthesia whilst the block was performed. A venous puncture during axillary block had occurred in one of these patients. Symptoms of anaesthetic toxicity were not reported. Discussion Brachial plexus block via the axillary approach is widely used in upper extremity procedures. The present results give further evidence for the high success rate obtained with peripheral nerve block performed using the multiple twitches technique with a nerve stimulator. The nerve stimulator technique allows results to be individually evaluated because the same local anaesthetic volume is used for each nerve block. In addition, the multiple injection technique offers the advantage of using smaller doses of drug, which also reduces the risk of local anaesthetic toxicity. A consistent sequence of nerve location (from the external to the internal quadrants, i.e. musculocutaneous, median, ulnar, and radial nerves) was followed to minimize 522
5 Three different volumes of mepivacaine 10 mg ml ±1 Table 4 Assessment of tourniquet pain, comfort during the anaesthetic procedure and complications Variable Mepivacaine 10 mg ml ±1 36 ml 28 ml 20 ml P value Tourniquet pain, number (%) 0 1 (2.6) 5 (13.2) Tourniquet time, min Mean (SD) 34.0 (20.0) 31.6 (22.0) 30.1 (18.3) NS Median (range) 30 (10±100) 27.5 (10±100) 20 (15±90) Axillary block discomfort, VAS 0±10 Mean (SD) 6.3 (2.5) 7.2 (1.8) 5.7 (2.4) 0.20 Needle insertion vs nerve stimulation, number (%) Equal 19 (50.0) 22 (57.9) 20 (52.6) NS Needle insertion worse 2 (5.3) 4 (10.5) 3 (7.9) Nerve stimulation worse 17 (44.7) 12 (31.6) 15 (39.5) Do you would undergo the same procedure in the future? Yes (%) 38 (100) 36 (94.7) 36 (94.7) NS Dysesthesia at 24 h, number Assessment at 2 months Between 24 h and 2 months At the control visit the risk of passing through the same zone and trans xing a potentially blocked nerve. Barker and Coventry 14 also considered that the order in which the nerves are blocked is very important and have recommended the sequence of musculocutaneous, median, and radial, with no speci c localization for the ulnar nerve, providing that the radial is identi ed and blocked. However, accidental trans xion during location of another nerve is a criticized aspect of the multiple injection technique compared with the single injection technique. With regard to the optimal stimulating current, it has been recently suggested that a stimulating current less than 0.5 ma should be used in every patient Indeed, the lower the current, the closer the nerve, and the success rate should also be higher. In our study, needle position was considered adequate at the point of motor response when the current was decreased to equal to/less than 0.4 ma. However, a distance from the nerve that is too small may cause paresthesia during puncture. 16 In our study, accidental paresthesia occurred in eight cases, a number similar or less than that reported by other authors using the multiple or single 9 nerve stimulation techniques. The fact that all axillary plexus blocks were performed with nerve stimulation involving the four motor responses using the same concentration of a single anaesthetic agent allow comparison between groups in latency time, level of sensory and motor block achieved, tourniquet tolerance and duration of analgesia, with doses of the anaesthetic agent contained in the different volumes assigned to each group. With regard to the primary ef cacy variable (complete sensory block) it has generally been indicated that a better quality of sensory block is obtained with higher volumes. In the study of Vester-Andersen and colleagues, 19 perivascular axillary block was performed in 90 patients allocated to receive 40, 50, or 60 ml of mepivacaine 10 mg ml ±1 with epinephrine. Although no differences were found in sensory or motor block between the three groups, a better quality of sensory block was found in the groups given 50 and 60 ml than in the group given 40 ml. In the study of Rucci and colleagues 20 using the `orthogonal two-needle technique' and in which patients were randomly assigned to 20, 30, and 40 ml of bupivacaine with epinephrine, a better analgesic spread to all major branches of the plexus was obtained when increased volumes of anaesthetic solution were injected. Other studies have also shown that for the same amount of local anaesthetic, the larger volumes provided better quality sensory block than smaller ones. In addition, it has been demonstrated that small volume (5 ml) injections of mepivacaine 10 mg ml ±1 with epinephrine using the four terminal nerve technique reduced total anaesthetic time and provided better spread of analgesia in the hand than a single injection of 80 ml of the same anaesthetic solution into the neurovascular sheath. 13 In the present study, a high rate of complete sensory block was obtained, with a success rate higher than 94% in the three study groups, including patients assigned to the lowest volume of anaesthetic solution. However, duration of the study (40 min) may account in part for the favourable results. As shown in Figure 1, 10% of patients that had a complete sensory block at the end of the study, showed incomplete sensory block at the 30-min assessment. With regard to other variables, such as latency time, duration of analgesia, and motor block, there were no statistically signi cant differences among the three study groups. Six patients had tourniquet pain but, in all of them, complete sensory and motor block of the musculocutaneous nerve was recorded. The poor results obtained with this technique with respect to block of the axillary nerve may justify tourniquet pain. On the other hand, muscle pain and ischaemia may be more important than cutaneous pain. A high tourniquet will often encroach on deltoid as well as the proximal cutaneous area and this may be more relevant in causing tourniquet discomfort when the axillary nerve is not blocked. In our study, tourniquet tolerance was poorer in 523
6 Serradell et al. patients receiving 20 ml of mepivacaine 10 mg ml ±1. Koscielniak-Nielsen and colleagues 13 indicated that large dose and volume axillary injection provides better analgesia of the upper arm as a result of a higher incidence of block of the axillary nerve, which is responsible for sensory innervation of the external aspect of the arm. In our study, block of the intercostobrachial and accessory of the cutaneous brachii medialis nerves was performed at the end of the axillary brachial plexus block to improve tourniquet tolerance. Overall, the study group in which a volume of 7 ml of mepivacaine 10 mg ml ±1 was used to block each of the four motor responses (Group B), showed a success rate of complete sensory block, motor block, and tourniquet tolerance similar to the study group given a volume of 9 ml (Group A), with the further advantage of a lower risk of systemic toxicity associated with larger volumes of local anaesthetic agents. In the study of Bertini and colleagues 23 comparing the ef cacy of ropivacaine and bupivacaine, a dose equivalent to that given to our patients in Group B provided an excellent level of sensory block and no patient needed additional block for surgical or tourniquet pain. In summary, the three volumes (38 ml, 28 ml, 20 ml) of mepivacaine 10 mg ml ±1 ensured a similar and high percentage of complete sensory blocks in axillary brachial plexus anaesthesia with nerve stimulation involving the location of four motor responses. Axillary block using an adequate concentration of a local anaesthetic agent, and the approach of multiple injection sites with stimulation of all four major nerves of the brachial plexus, may contribute to minimize the importance of the injected volume of anaesthetic solution. Acknowledgements We thank the nurses of the surgical ward and the Department of Orthopaedic Surgery of our hospital for valuable help during the study, Montserrat MartõÂn, MD, from the Unit of Epidemiology of Consorcio Sanitario Creu Roja for statistical analysis, Vygon company for nancial support, and Marta Pulido, MD for editing the manuscript and editorial assistance. References 1 Thompson GE, Rorie DK. Functional anatomy of the brachial plexus sheaths. Anesthesiology 1983; 59: 117±22 2 Partridge BL, Katz J, Benirschke K. Functional anatomy of the brachial plexus sheath: implications for anesthesia. Anesthesiology 1987; 66: 743±7 3 Winnie AP, Radonjic R, Akkinemi SR, Durrani Z. Factors in uencing the distribution of local anesthetic injected into the brachial plexus sheath. Anesth Analg 1979; 58: 225±34 4 Baranowski AP, Pither CE. A comparison of three methods of axillary brachial plexus anaesthesia. Anaesthesia 1990; 45: 362±5 5 Koscielniak-Nielsen ZJ, Nielsen PR, Nielsen SL, Gardi T, Hermann C. Comparison of transarterial and multiple nerve stimulation techniques for axillary block using a high dose of mepivacaine with adrenaline. Acta Anaesthesiol Scand 1999; 43: 398±404 6 Lavoie J, Martin R, TeÂtrault JP, CoÃte DJ, Colas MJ. Axillary plexus block using a peripheral nerve stimulator: single or multiple injections. Can J Anaesth 1992; 39: 583±6 7 Inberg P, Annila I, Annila P. Double-injection method using peripheral nerve stimulator is superior to single injection in axillary plexus block. Reg Anesth Pain Med 1999; 24: 509±13 8 Bussac JJ, Akaga R, Lena P, Legre R, FrancËois G. Bloc du plexus brachial par voie axillaire: injections unique ou multiples? Ann Fr Anesth ReÂanim 1991; 10: R53 9 Koscielniak-Nielsen ZJ, Stens-Pedersen HL, Lippert FK. Readiness for surgery after axillary block: single or multiple injection techniques. Eur J Anaesthesiol 1997; 14: 164±71 10 Sia S, Bartoli M. Selective ulnar nerve localization is not essential for axillary brachial plexus block using a multiple nerve stimulation technique. Reg Anesth Pain Med 2001; 26: 12±16 11 Coventry DM, Barker KF, Thomson M. Comparison of two neurostimulation techniques for axillary brachial plexus blockade. Br J Anaesth 2001; 86: 80±3 12 Serradell Catalan A, Moncho Rodriguez JM, Santos Carnes J, et al. Anestesia de plexo braquial por võâa axilar. CuÂantas respuestas buscamos con neuroestimulacioân? Rev Esp Anestesiol Reanim 2001; 48: 356±63 13 Koscielniak-Nielsen ZJ, Rotboll-Nielsen P, Sùrensen T, Stenùr M. Low dose axillary block by targeted injections of the terminal nerves. Can J Anesth 1999; 46: 658±64 14 Baker KE, Coventry DM. Sequence of nerve blockade in brachial plexus anesthesiaðsafety before speed. Acta Anaesthesiol Scand 2000; 43: De AndreÂs J, Sala-Blanch X. Peripheral nerve stimulation in the practice of brachial plexus anesthesia: a review. Reg Anesth Pain Med 2001; 26: 478±83 16 Benhamou D. Axillary plexus block using multiple nerve stimulation: a European view. Reg Anesth Pain Med 2001; 26: 495±8 17 Sia S, Bartoli M, Lepri A, Marchini O, Ponsecchi P. Multipleinjection axillary brachial plexus block: a comparison of two methods of nerve localization±nerve stimulation versus paresthesia. Anesth Analg 2000; 91: 647±51 18 Fanelli G, Casati A, Garancini P, Torri G for the Study Group on Regional Anesthesia. Nerve stimulator and multiple injection technique for upper and lower limb blockade: failure rate, patient acceptance, and neurologic complications. Anesth Analg 1999; 88: 847±52 19 Vester-Andersen T, Husum B, Lindeburg T, Borritis L, Gothgen I. Perivascular axillary block IV: blockade following 40, 50 or 60 ml of mepivacaine 1% with adrenaline. Acta Anaesthesiol Scand 1984; 28: 99± Rucci FS, Barbagli R, Pippa P, Boccaccini A. The optimal dose of local anaesthetic in the orthogonal two-needle technique. Extent of sensory block after the injection of 20, 30 and 40 ml of anaesthetic solution. Eur J Anaesthesiol 1997; 14: 281±6 21 Vester-Andersen T, Christiansen C, Sorensen M, Kaalund- Jorgensen HO, Saugbjerg P, Schultz-Moller K. Perivascular axillary block II: in uence of injected volume of local anaesthetic on neural blockade. Acta Anaesthesiol Scand 1983; 27: 95±8 22 Martin R, Dumais R, Cinq-Mars S, TeÂtrault JP. Bloc axillaire par blocage simultaneâ de plusieurs nefrs. IÐIn uence du volume de la solution anestheâsique. Ann Fr Anesth Reanim 1993; 12: 229±32 23 Bertini L, Tagariello V, Mancini S, et al. 0.75% and 0.5% ropivacaine for axillary brachial plexus block: a clinical comparison with 0.5% bupivacaine. Reg Anesth Pain Med 1999; 24: 514±8 524
The relationship of the musculocutaneous nerve to the brachial plexus evaluated by MRI
 DOI 10.1007/s10877-015-9807-3 ORIGINAL RESEARCH The relationship of the musculocutaneous nerve to the brachial plexus evaluated by MRI Trygve Kjelstrup 1,2 Axel R. Sauter 3 Per K. Hol 2,4 Received: 23
DOI 10.1007/s10877-015-9807-3 ORIGINAL RESEARCH The relationship of the musculocutaneous nerve to the brachial plexus evaluated by MRI Trygve Kjelstrup 1,2 Axel R. Sauter 3 Per K. Hol 2,4 Received: 23
Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block
 Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Tanta Medical Journal Vol. (6), April 2008 Original Article ABSTRACT Dexamethasone Improves Outcome Of Infraclavicular Brachial Plexus Block Mohamed Samy Seddik Department of Anesthesia & Intensive Care,
Distribution of Local Anesthetic in Axillary Brachial Plexus Block
 Anesthesiology 2002; 96:1315 24 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Distribution of Local Anesthetic in Axillary Brachial Plexus Block A Clinical and Magnetic
Anesthesiology 2002; 96:1315 24 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Distribution of Local Anesthetic in Axillary Brachial Plexus Block A Clinical and Magnetic
Comparison Of 0.5%Bupivacaine And 0.5% Bupivacaine Plus Buprenorphine in Brachial Plexus Block
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 1 Ver. VIII (Jan. 2016), PP 01-08 www.iosrjournals.org Comparison Of 0.5%Bupivacaine And 0.5%
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 1 Ver. VIII (Jan. 2016), PP 01-08 www.iosrjournals.org Comparison Of 0.5%Bupivacaine And 0.5%
Comparison of Success Rate of Classical Supraclavicular Brachial Plexus Block with and without Nerve Stimulator
 MVP Journal of Medical Sciences, Vol 4(2), 135 140, July-December 2017 ISSN (Print) : 2348 263X ISSN (Online) : 2348-2648 DOI: 10.18311/mvpjms/2017/v4i2/11033 Comparison of Success Rate of Classical Supraclavicular
MVP Journal of Medical Sciences, Vol 4(2), 135 140, July-December 2017 ISSN (Print) : 2348 263X ISSN (Online) : 2348-2648 DOI: 10.18311/mvpjms/2017/v4i2/11033 Comparison of Success Rate of Classical Supraclavicular
British Journal of Anaesthesia 98 (6): (2007) doi: /bja/aem100 Advance Access publication May 3, 2007 REGIONAL ANAESTHESIA Effects of ultr
 British Journal of Anaesthesia 98 (6): 823 7 (2007) doi:10.1093/bja/aem100 Advance Access publication May 3, 2007 REGIONAL ANAESTHESIA Effects of ultrasound guidance on the minimum effective anaesthetic
British Journal of Anaesthesia 98 (6): 823 7 (2007) doi:10.1093/bja/aem100 Advance Access publication May 3, 2007 REGIONAL ANAESTHESIA Effects of ultrasound guidance on the minimum effective anaesthetic
Regional Anaesthesia of the Thoracic Limb
 Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
ASSESSMENT OF THE ROLE OF DEXAMETHASONE AS AN ADJUVANT IN SUPRACLAVICULAR BLOCK FOR UPPER LIMB SURGERIES
 ORIGINAL ARTICLE ASSESSMENT OF THE ROLE OF DEXAMETHASONE AS AN ADJUVANT IN SUPRACLAVICULAR BLOCK FOR UPPER LIMB SURGERIES Priyesh Bhaskar, Mamta Harjai (e) ISSN Online: 2321-9599 (p) ISSN Print: 2348-6805
ORIGINAL ARTICLE ASSESSMENT OF THE ROLE OF DEXAMETHASONE AS AN ADJUVANT IN SUPRACLAVICULAR BLOCK FOR UPPER LIMB SURGERIES Priyesh Bhaskar, Mamta Harjai (e) ISSN Online: 2321-9599 (p) ISSN Print: 2348-6805
The infraclavicular brachial plexus block by the coracoid approach is clinically effective: an observational study of 150 patients
 253 Regional Anesthesia and Pain The infraclavicular brachial plexus block by the coracoid approach is clinically effective: an observational study of 150 patients [Le bloc infraclaviculaire du plexus
253 Regional Anesthesia and Pain The infraclavicular brachial plexus block by the coracoid approach is clinically effective: an observational study of 150 patients [Le bloc infraclaviculaire du plexus
Continuous interscalene infusion and single injection using levobupivacaine for analgesia after surgery of the shoulder
 Upper limb Continuous interscalene infusion and single injection using levobupivacaine for analgesia after surgery of the shoulder A DOUBLE-BLIND, RANDOMISED CONTROLLED TRIAL J. Kean, C. A. Wigderowitz,
Upper limb Continuous interscalene infusion and single injection using levobupivacaine for analgesia after surgery of the shoulder A DOUBLE-BLIND, RANDOMISED CONTROLLED TRIAL J. Kean, C. A. Wigderowitz,
Plantar Flexion Seems More Reliable than Dorsiflexion with Labat s Sciatic Nerve Block: A Prospective, Randomized Comparison
 Plantar Flexion Seems More Reliable than Dorsiflexion with Labat s Sciatic Nerve Block: A Prospective, Randomized Comparison Manuel Taboada, MD*, Peter G. Atanassoff, MD, Jaime Rodríguez, MD, PhD*, Joaquín
Plantar Flexion Seems More Reliable than Dorsiflexion with Labat s Sciatic Nerve Block: A Prospective, Randomized Comparison Manuel Taboada, MD*, Peter G. Atanassoff, MD, Jaime Rodríguez, MD, PhD*, Joaquín
Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven
 Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven 55 years old woman Latarjetprocedure ASA-1, 49 kg. NKDA Informed consent for RA ISB with catheter uneventful throughout, rate 4/4/60 according
Dr. Georgi Valchev Fellow in regional anaesthesia UZ Leuven 55 years old woman Latarjetprocedure ASA-1, 49 kg. NKDA Informed consent for RA ISB with catheter uneventful throughout, rate 4/4/60 according
Original article: Supraclavicular block with 0.5% levobupivacaine and 0.5% ropivacainecomparative
 Original article: Supraclavicular block with 0.5% levobupivacaine and 0.5% ropivacainecomparative study Dr.V.Sai Dilip 1, Dr.G.Chandra Sekhar 1, Dr.Gopala Krishna Murthy 1, Dr.A.S.Kameswara Rao 1, Dr.K.Sivaji
Original article: Supraclavicular block with 0.5% levobupivacaine and 0.5% ropivacainecomparative study Dr.V.Sai Dilip 1, Dr.G.Chandra Sekhar 1, Dr.Gopala Krishna Murthy 1, Dr.A.S.Kameswara Rao 1, Dr.K.Sivaji
COMPARATIVE ANAESTHETIC PROPERTIES OF VARIOUS LOCAL ANAESTHETIC AGENTS IN EXTRADURAL BLOCK FOR LABOUR
 Br.J. Anaesth. (1977), 49, 75 COMPARATIVE ANAESTHETIC PROPERTIES OF VARIOUS LOCAL ANAESTHETIC AGENTS IN EXTRADURAL BLOCK FOR LABOUR D. G. LITTLEWOOD, D. B. SCOTT, J. WILSON AND B. G. COVINO SUMMARY Various
Br.J. Anaesth. (1977), 49, 75 COMPARATIVE ANAESTHETIC PROPERTIES OF VARIOUS LOCAL ANAESTHETIC AGENTS IN EXTRADURAL BLOCK FOR LABOUR D. G. LITTLEWOOD, D. B. SCOTT, J. WILSON AND B. G. COVINO SUMMARY Various
WITH ISOBARIC BUPIVACAINE (5 MG/ML)
 , 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
, 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
Interscalene brachial plexus blocks in the management of shoulder dislocations
 Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Intraneural injection during nerve stimulator-guided sciatic nerve block at the popliteal fossa
 British Journal of Anaesthesia 102 (6): 855 61 (2009) doi:10.1093/bja/aep097 Advance Access publication May 6, 2009 Intraneural injection during nerve stimulator-guided sciatic nerve block at the popliteal
British Journal of Anaesthesia 102 (6): 855 61 (2009) doi:10.1093/bja/aep097 Advance Access publication May 6, 2009 Intraneural injection during nerve stimulator-guided sciatic nerve block at the popliteal
S Kannan, Prem Kumar. Assistant Professor, Saveetha Medical College and Hospital, Chennai.
 Original Article CLINICAL COMPARISON OF TWO DIFFERENT VOLUMES OF 0.5% BUPIVACAINE FOR CLAVICULAR SURGERIES USING COMBINED INTERSCALENE AND SUPERFICIAL CERVICAL PLEXUS BLOCK 2 S Kannan, Prem Kumar,2 Assistant
Original Article CLINICAL COMPARISON OF TWO DIFFERENT VOLUMES OF 0.5% BUPIVACAINE FOR CLAVICULAR SURGERIES USING COMBINED INTERSCALENE AND SUPERFICIAL CERVICAL PLEXUS BLOCK 2 S Kannan, Prem Kumar,2 Assistant
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Brachial Plexus Block, a Comparison of Nerve Locator versus Paresthesia Technique
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. X. (Feb. 2014), PP 06-10 Brachial Plexus Block, a Comparison of Nerve Locator versus
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. X. (Feb. 2014), PP 06-10 Brachial Plexus Block, a Comparison of Nerve Locator versus
Gross Anatomy Questions That Should be Answerable After October 27, 2017
 Gross Anatomy Questions That Should be Answerable After October 27, 2017 1. The inferior angle of the scapula of a woman who was recently in an automobile accident seems to protrude making a ridge beneath
Gross Anatomy Questions That Should be Answerable After October 27, 2017 1. The inferior angle of the scapula of a woman who was recently in an automobile accident seems to protrude making a ridge beneath
BJA Advance Access published January 26, British Journal of Anaesthesia Page 1 of 10 doi: /bja/aen384
 BJA Advance Access published January 26, 2009 British Journal of Anaesthesia Page 1 of 10 doi:10.1093/bja/aen384 Ultrasound guidance compared with electrical neurostimulation for peripheral nerve block:
BJA Advance Access published January 26, 2009 British Journal of Anaesthesia Page 1 of 10 doi:10.1093/bja/aen384 Ultrasound guidance compared with electrical neurostimulation for peripheral nerve block:
Deltoid, triceps, or both responses improve the success rate of the interscalene catheter surgical block compared with the biceps response
 British Journal of Anaesthesia 109 (6): 975 80 (2012) Advance Access publication 8 August 2012. doi:10.1093/bja/aes296 REGIONAL ANAESTHESIA Deltoid, triceps, or both responses improve the success rate
British Journal of Anaesthesia 109 (6): 975 80 (2012) Advance Access publication 8 August 2012. doi:10.1093/bja/aes296 REGIONAL ANAESTHESIA Deltoid, triceps, or both responses improve the success rate
CARPAL TUNNEL RELEASE BLOCK Author John Hyndman
 Questions CARPAL TUNNEL RELEASE BLOCK Author John Hyndman Web Editor Kirsten Fehrmann - kirstenfehrmann@hotmail.com 1) Why does a LA solution containing Epinephrine cause pain on injection and what can
Questions CARPAL TUNNEL RELEASE BLOCK Author John Hyndman Web Editor Kirsten Fehrmann - kirstenfehrmann@hotmail.com 1) Why does a LA solution containing Epinephrine cause pain on injection and what can
Pre-operative Care For Surgery of Forearm Fracture. WONG Mei Chee OT (CMC)
 Pre-operative Care For Surgery of Forearm Fracture WONG Mei Chee OT (CMC) Pre-operative Nursing Considerations for Surgery of Forearm Fracture 1. Patient s problems - Diagnosis: Clinical features, x-ray
Pre-operative Care For Surgery of Forearm Fracture WONG Mei Chee OT (CMC) Pre-operative Nursing Considerations for Surgery of Forearm Fracture 1. Patient s problems - Diagnosis: Clinical features, x-ray
Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries
 Cronicon OPEN ACCESS ANAESTHESIA Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries Susmita Bhattacharyya, KalyanBrata Mandal,
Cronicon OPEN ACCESS ANAESTHESIA Research Article A Comparative Study of Interscalene and Supraclavicular Approach of Brachial Plexus Block on Upper Limb Surgeries Susmita Bhattacharyya, KalyanBrata Mandal,
COMPARISON OF EXTRADURAL ROPIVACAINE AND BUPIVACAINE
 British Journal of Anaesthesia 99; : -7 COMPARISON OF EXTRADURAL ROPIVACAINE AND BUPIVACAINE M. S. BROCKWAY, J. BANNISTER, J. H. McCLURE, D. McKEOWN AND J. A. W. WILDSMITH SUMMARY Ropivacaine, a new long
British Journal of Anaesthesia 99; : -7 COMPARISON OF EXTRADURAL ROPIVACAINE AND BUPIVACAINE M. S. BROCKWAY, J. BANNISTER, J. H. McCLURE, D. McKEOWN AND J. A. W. WILDSMITH SUMMARY Ropivacaine, a new long
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Assessment of topographic brachial plexus nerves variations at the axilla using ultrasonography
 BJA Advance Access published August, 00 British Journal of Anaesthesia Page of doi:./bja/aep0 Assessment of topographic brachial plexus nerves variations at the axilla using ultrasonography J.-L. Christophe,
BJA Advance Access published August, 00 British Journal of Anaesthesia Page of doi:./bja/aep0 Assessment of topographic brachial plexus nerves variations at the axilla using ultrasonography J.-L. Christophe,
The Arm and Cubital Fossa
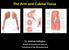 The Arm and Cubital Fossa Dr. Andrew Gallagher School of Anatomical Sciences University of the Witwatersrand Introduction The ARM (BRACHIUM) is the most proximal segment of the upper limb musculoskeletal
The Arm and Cubital Fossa Dr. Andrew Gallagher School of Anatomical Sciences University of the Witwatersrand Introduction The ARM (BRACHIUM) is the most proximal segment of the upper limb musculoskeletal
An evaluation of brachial plexus block using a nerve stimulator versus ultrasound guidance: A randomized controlled trial
 Original Article An evaluation of brachial plexus block using a nerve versus ultrasound guidance: A randomized controlled trial Shivinder Singh, Rakhee Goyal, Kishan Kumar Upadhyay, Navdeep Sethi, Ram
Original Article An evaluation of brachial plexus block using a nerve versus ultrasound guidance: A randomized controlled trial Shivinder Singh, Rakhee Goyal, Kishan Kumar Upadhyay, Navdeep Sethi, Ram
Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical Trial
 J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
prilocaine hydrochloride 2% hyperbaric solution for injection (Prilotekal ) SMC No. (665/10) Goldshield Group
 prilocaine hydrochloride 2% hyperbaric solution for injection (Prilotekal ) SMC No. (665/10) Goldshield Group 17 December 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the
prilocaine hydrochloride 2% hyperbaric solution for injection (Prilotekal ) SMC No. (665/10) Goldshield Group 17 December 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the
region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla.
 1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
The arm: *For images refer back to the slides
 The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
DOI: / Page. 1 Dr. Seetharamaiah.S., 2 Dr. G.R.Santhilatha, 3 Dr. T.Venugopala rao, 4 Dr. Venugopalan.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. VII (Sep. 2015), PP 44-48 www.iosrjournals.org To evaluate the efficacy of Inj. Dexmedetomidine
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. VII (Sep. 2015), PP 44-48 www.iosrjournals.org To evaluate the efficacy of Inj. Dexmedetomidine
Comparison of ultrasound-guided supraclavicular block according to the various volumes of local anesthetic
 Clinical Research Article Korean J Anesthesiol 2013 June 64(6): 494-499 http://dx.doi.org/10.4097/kjae.2013.64.6.494 Comparison of ultrasound-guided supraclavicular block according to the various volumes
Clinical Research Article Korean J Anesthesiol 2013 June 64(6): 494-499 http://dx.doi.org/10.4097/kjae.2013.64.6.494 Comparison of ultrasound-guided supraclavicular block according to the various volumes
Review Article Axillary Brachial Plexus Block
 Anesthesiology Research and Practice Volume 2011, Article ID 173796, 5 pages doi:10.1155/2011/173796 Review Article Axillary Brachial Plexus Block Ashish R. Satapathy and David M. Coventry Department of
Anesthesiology Research and Practice Volume 2011, Article ID 173796, 5 pages doi:10.1155/2011/173796 Review Article Axillary Brachial Plexus Block Ashish R. Satapathy and David M. Coventry Department of
Maaike G. E. Fenten 3, Karin P. W. Schoenmakers 3, Petra J. C. Heesterbeek 2, Gert Jan Scheffer 3 and Rudolf Stienstra 1*
 Fenten et al. BMC Anesthesiology (2015) 15:130 DOI 10.1186/s12871-015-0110-0 RESEARCH ARTICLE Open Access Effect of local anesthetic concentration, dose and volume on the duration of single-injection ultrasound-guided
Fenten et al. BMC Anesthesiology (2015) 15:130 DOI 10.1186/s12871-015-0110-0 RESEARCH ARTICLE Open Access Effect of local anesthetic concentration, dose and volume on the duration of single-injection ultrasound-guided
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone
 *the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
*the Arm* -the arm extends from the shoulder joint (proximal), to the elbow joint (distal) - it has one bone ; the humerus which is a long bone - muscles in the arm : *brachialis muscle *Biceps brachii
AXILLARY BRACHIAL PLEXUS BLOCK: METHOD OF CHOICE?
 British Journal of Anaesthesia 1990; 64: 224-231 AXILLARY BRACHIAL PLEXUS BLOCK: METHOD OF CHOICE? M. S. BROCKWAY AND J. A. W. WILDSMITH The first brachial plexus block is said to have been performed by
British Journal of Anaesthesia 1990; 64: 224-231 AXILLARY BRACHIAL PLEXUS BLOCK: METHOD OF CHOICE? M. S. BROCKWAY AND J. A. W. WILDSMITH The first brachial plexus block is said to have been performed by
Block of the sacral segments in lumbar epidural anaesthesia
 British Journal of Anaesthesia 90 (2): 173±8 (2003) DOI: 10.1093/bja/aeg045 Block of the sacral segments in lumbar epidural anaesthesia M. Arakawa*, Y. Aoyama and Y. Ohe Second Department of Anaesthesiology,
British Journal of Anaesthesia 90 (2): 173±8 (2003) DOI: 10.1093/bja/aeg045 Block of the sacral segments in lumbar epidural anaesthesia M. Arakawa*, Y. Aoyama and Y. Ohe Second Department of Anaesthesiology,
Nerve Injury. 1) Upper Lesions of the Brachial Plexus called Erb- Duchene Palsy or syndrome.
 Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
Bier s block is a frequently used intravenous regional. Original Article Journal of Kathmandu Medical College, Vol. 2, No. 1, Issue 3, Jan.-Mar.
 Original Article, Vol. 2, No. 1, Issue 3, Jan.-Mar., 2013 Tabdar S 1, Lama S 2, Kadariya ER 3 1 Assistant Professor, 2 Lecturer, Department of Anaesthesiology and Intensive Care Kathmandu Medical College
Original Article, Vol. 2, No. 1, Issue 3, Jan.-Mar., 2013 Tabdar S 1, Lama S 2, Kadariya ER 3 1 Assistant Professor, 2 Lecturer, Department of Anaesthesiology and Intensive Care Kathmandu Medical College
Comparison of clonidine adjuvants to ropivacaine in subclavian perivascular approach of supra clavicular brachial plexus block
 Original Research Article Comparison of clonidine adjuvants to ropivacaine in subclavian perivascular approach of supra clavicular brachial plexus block S. Arul Rajan 1, N. Sathyan 2*, T. Murugan 3 1 Assistant
Original Research Article Comparison of clonidine adjuvants to ropivacaine in subclavian perivascular approach of supra clavicular brachial plexus block S. Arul Rajan 1, N. Sathyan 2*, T. Murugan 3 1 Assistant
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Induction position for spinal anaesthesia: Sitting versus lateral position
 11 ORIGINAL ARTICLE Induction position for spinal anaesthesia: Sitting versus lateral position Khurrum Shahzad, Gauhar Afshan Abstract Objective: To compare the effect of induction position on block characteristics
11 ORIGINAL ARTICLE Induction position for spinal anaesthesia: Sitting versus lateral position Khurrum Shahzad, Gauhar Afshan Abstract Objective: To compare the effect of induction position on block characteristics
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi. E. mail:
 Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
JOURNAL OF PHARMACEUTICAL AND BIOMEDICAL SCIENCES
 JOURNAL OF PHARMACEUTICAL AND BIOMEDICAL SCIENCES Singh R, Bisoi P, Mohanty SN, Debata PC. Study On Effect of Dexmedetomidine When Added To Bupivacaine On The Onset Time And Duration Of Block In Supraclavicular
JOURNAL OF PHARMACEUTICAL AND BIOMEDICAL SCIENCES Singh R, Bisoi P, Mohanty SN, Debata PC. Study On Effect of Dexmedetomidine When Added To Bupivacaine On The Onset Time And Duration Of Block In Supraclavicular
Comparison between ultrasound-guided sciatic femoral nerve block and unilateral spinal anaesthesia for outpatient knee arthroscopy
 Research Report Comparison between ultrasound-guided sciatic femoral nerve block and unilateral spinal anaesthesia for outpatient knee arthroscopy Journal of International Medical Research 41(5) 1639 1647!
Research Report Comparison between ultrasound-guided sciatic femoral nerve block and unilateral spinal anaesthesia for outpatient knee arthroscopy Journal of International Medical Research 41(5) 1639 1647!
Nerves of Upper limb. Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh
 Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Assistant Professor, Anaesthesia Department, Govt. General Hospital / Guntur Medical College, Guntur, Andhra Pradesh, India.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. I (August. 2016), PP 87-91 www.iosrjournals.org A Comparative Study of 0.25% Ropivacaine
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. I (August. 2016), PP 87-91 www.iosrjournals.org A Comparative Study of 0.25% Ropivacaine
Fascial Compartments of the Upper Arm
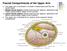 Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Fascial Compartments of the Upper Arm The upper arm is enclosed in a sheath of deep fascia and has two fascial septa: 1- Medial fascial septum (medial intermuscular septum): attached to the medial supracondylar
Efficacy Of Ropivacaine - Fentanyl In Comparison To Bupivacaine - Fentanyl In Epidural Anaesthesia
 ISPUB.COM The Internet Journal of Anesthesiology Volume 33 Number 1 Efficacy Of Ropivacaine - Fentanyl In Comparison To Bupivacaine - Fentanyl In Epidural Anaesthesia S Gautam, S Singh, R Verma, S Kumar,
ISPUB.COM The Internet Journal of Anesthesiology Volume 33 Number 1 Efficacy Of Ropivacaine - Fentanyl In Comparison To Bupivacaine - Fentanyl In Epidural Anaesthesia S Gautam, S Singh, R Verma, S Kumar,
International Journal of Clinical And Diagnostic Research ISSN Volume 3, Issue 2, Mar-Apr 2015.
 Anesthesiology Original Research International Journal of Clinical And Diagnostic Research ISSN 2395-3403 Volume 3, Issue 2, Mar-Apr 2015. Glorigin Lifesciences Private Limited. COMPARISON OF DEXMEDETOMIDINE
Anesthesiology Original Research International Journal of Clinical And Diagnostic Research ISSN 2395-3403 Volume 3, Issue 2, Mar-Apr 2015. Glorigin Lifesciences Private Limited. COMPARISON OF DEXMEDETOMIDINE
Citation for published version (APA): Wegener, J. T. (2013). Educational and clinical aspects of peripheral nerve blockade
 UvA-DARE (Digital Academic Repository) Educational and clinical aspects of peripheral nerve blockade Wegener, Jessica Link to publication Citation for published version (APA): Wegener, J. T. (2013). Educational
UvA-DARE (Digital Academic Repository) Educational and clinical aspects of peripheral nerve blockade Wegener, Jessica Link to publication Citation for published version (APA): Wegener, J. T. (2013). Educational
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR
 GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR INTRODUCTION Regional block provides superior pain relief, compared
GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR INTRODUCTION Regional block provides superior pain relief, compared
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
Key Relationships in the Upper Limb
 Key Relationships in the Upper Limb This list contains some of the key relationships that will help you identify structures in the lab. They are organized by dissection assignment as defined in the syllabus.
Key Relationships in the Upper Limb This list contains some of the key relationships that will help you identify structures in the lab. They are organized by dissection assignment as defined in the syllabus.
jorapain Original Article ABSTRACT
 Original Article Comparison of Clonidine and Dexmedetomidine 10.5005/jp-journals-10046-0015 as an Adjuvant to 0.5% Ropivacaine Comparison of Clonidine and Dexmedetomidine as an Adjuvant to 0.5% Ropivacaine
Original Article Comparison of Clonidine and Dexmedetomidine 10.5005/jp-journals-10046-0015 as an Adjuvant to 0.5% Ropivacaine Comparison of Clonidine and Dexmedetomidine as an Adjuvant to 0.5% Ropivacaine
Increased body mass index and ASA physical status IV are risk factors for block failure in ambulatory surgery - an analysis of 9,342 blocks
 810 Regional Anesthesia and Pain Increased body mass index and ASA physical status IV are risk factors for block failure in ambulatory surgery - an analysis of 9,342 blocks [Un indice de masse corporelle
810 Regional Anesthesia and Pain Increased body mass index and ASA physical status IV are risk factors for block failure in ambulatory surgery - an analysis of 9,342 blocks [Un indice de masse corporelle
Page 1. Results: Both the ultrasound techniques are comparable and better than paracetamol
 ISSN- O: 2458-868X, ISSN P: 2458 8687 Index Copernicus Value: 49. 23 PubMed - National Library of Medicine - ID: 101731606 SJIF Impact Factor: 4.956 International Journal of Medical Science and Innovative
ISSN- O: 2458-868X, ISSN P: 2458 8687 Index Copernicus Value: 49. 23 PubMed - National Library of Medicine - ID: 101731606 SJIF Impact Factor: 4.956 International Journal of Medical Science and Innovative
Anesthetic Efficacy of Different Ropivacaine Concentrations for Inferior Alveolar Nerve Block
 SCIENTIFIC REPORT Anesthetic Efficacy of Different Ropivacaine Concentrations for Inferior Alveolar Nerve Block Eman El-Sharrawy, MBBCh, MSc, MD,* and John A. Yagiela, DDS, PhD *Faculty of Dentistry, Tanta
SCIENTIFIC REPORT Anesthetic Efficacy of Different Ropivacaine Concentrations for Inferior Alveolar Nerve Block Eman El-Sharrawy, MBBCh, MSc, MD,* and John A. Yagiela, DDS, PhD *Faculty of Dentistry, Tanta
Slides of Anatomy. Spring Dr. Maher Hadidi, University of Jordan
 Slides of Anatomy Please note : These slides are Dr. Maher Hadidi s slides of spring 2016 and were edited by the Premed Academic Team to fit the slides of spring 2019. Spring 2019 Dr. Maher Hadidi, University
Slides of Anatomy Please note : These slides are Dr. Maher Hadidi s slides of spring 2016 and were edited by the Premed Academic Team to fit the slides of spring 2019. Spring 2019 Dr. Maher Hadidi, University
Continuous axillary brachial plexus block
 201 Tsuneo Sada r~d, Tsutomu Kobayashi MD, Seiitsu Murakami MD Continuous axillary brachial plexus block Continuous axiftary brachial plexus block was performed M 597 patients undergoing prolonged operations
201 Tsuneo Sada r~d, Tsutomu Kobayashi MD, Seiitsu Murakami MD Continuous axillary brachial plexus block Continuous axiftary brachial plexus block was performed M 597 patients undergoing prolonged operations
Sign up to receive ATOTW weekly
 PERIPHERAL NERVE BLOCKS GETTING STARTED ANAESTHESIA TUTORIAL OF THE WEEK 134 PUBLICATION DATE 18/05/09 Dr Kim Russon, Consultant Anaesthetist Dr Helen Findley, ST3 Anaesthetics Dr Zoe Harclerode, ST3 Anaesthetics
PERIPHERAL NERVE BLOCKS GETTING STARTED ANAESTHESIA TUTORIAL OF THE WEEK 134 PUBLICATION DATE 18/05/09 Dr Kim Russon, Consultant Anaesthetist Dr Helen Findley, ST3 Anaesthetics Dr Zoe Harclerode, ST3 Anaesthetics
MUSCLES. Anconeus Muscle
 LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
LAB 7 UPPER LIMBS MUSCLES Anconeus Muscle anconeus origin: distal end of dorsal surface of humerus insertion: lateral surface of ulna from distal margin of the semilunar notch to proximal end of the olecranon
The use of a muscle relaxant to supplement local anaesthetics for Bier's
 Archives of mergency Medicine, 1988, 5, 79-85 The use of a muscle relaxant to supplement local anaesthetics for Bier's blocks R. McGLON,1 F. HYS2 & P. HARRIS3 'The General Infirmary, Leeds, 2Accident and
Archives of mergency Medicine, 1988, 5, 79-85 The use of a muscle relaxant to supplement local anaesthetics for Bier's blocks R. McGLON,1 F. HYS2 & P. HARRIS3 'The General Infirmary, Leeds, 2Accident and
Hyperbaric 2% Lignocaine In Spinal Anaesthesia An Excellent Option For Day Care Surgeries
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 2 Ver. III. (Feb. 2014), PP 09-13 Hyperbaric 2% Lignocaine In Spinal Anaesthesia An Excellent
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 2 Ver. III. (Feb. 2014), PP 09-13 Hyperbaric 2% Lignocaine In Spinal Anaesthesia An Excellent
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Australian and New Zealand Registry of Regional Anaesthesia (AURORA)
 Australian and New Zealand Registry of Regional Anaesthesia (AURORA) Overview of Results First 4000 procedures recorded to - www.anaesthesiaregistry.org June 1st 2011 to February 2012 Background Australian
Australian and New Zealand Registry of Regional Anaesthesia (AURORA) Overview of Results First 4000 procedures recorded to - www.anaesthesiaregistry.org June 1st 2011 to February 2012 Background Australian
Intravenous Regional Anesthesia with Drug Combinations of Lidocaine, Ketamine, and Atracurium
 ISPUB.COM The Internet Journal of Anesthesiology Volume 18 Number 1 Intravenous Regional Anesthesia with Drug Combinations of Lidocaine, Ketamine, and Atracurium G Mir, A Naqeeb, T Waani, A Shora Citation
ISPUB.COM The Internet Journal of Anesthesiology Volume 18 Number 1 Intravenous Regional Anesthesia with Drug Combinations of Lidocaine, Ketamine, and Atracurium G Mir, A Naqeeb, T Waani, A Shora Citation
(Senior Resident, Dept of Anaesthesia, Dr. D. Y. Patil Medical College, Dr. D. Y. Patil Vidyapeeth [DPU], Pune)
![(Senior Resident, Dept of Anaesthesia, Dr. D. Y. Patil Medical College, Dr. D. Y. Patil Vidyapeeth [DPU], Pune) (Senior Resident, Dept of Anaesthesia, Dr. D. Y. Patil Medical College, Dr. D. Y. Patil Vidyapeeth [DPU], Pune)](/thumbs/82/85649280.jpg) IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 25-29 www.iosrjournals.org To Compare the Efficacy of Dexamethasone
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 25-29 www.iosrjournals.org To Compare the Efficacy of Dexamethasone
Single-cuff forearm tourniquet in intravenous regional anaesthesia results in less pain and fewer sedation requirements than upper arm tourniquet
 British Journal of Anaesthesia 111 (2): 271 5 (2013) Advance Access publication 18 March 2013. doi:10.1093/bja/aet032 Single-cuff forearm tourniquet in intravenous regional anaesthesia results in less
British Journal of Anaesthesia 111 (2): 271 5 (2013) Advance Access publication 18 March 2013. doi:10.1093/bja/aet032 Single-cuff forearm tourniquet in intravenous regional anaesthesia results in less
DORIS DUKE MEDICAL STUDENTS JOURNAL Volume V,
 Continuous Femoral Perineural Infusion (CFPI) Using Ropivacaine after Total Knee Arthroplasty and its Effect on Postoperative Pain and Early Functional Outcomes Eric Lloyd Scientific abstract Total Knee
Continuous Femoral Perineural Infusion (CFPI) Using Ropivacaine after Total Knee Arthroplasty and its Effect on Postoperative Pain and Early Functional Outcomes Eric Lloyd Scientific abstract Total Knee
A comparative study of Ropivacaine and Bupivacaine in combined spinal epidural anaesthesia and Post- operative analgesia
 Original article: A comparative study of Ropivacaine and Bupivacaine in combined spinal epidural anaesthesia and Post- operative analgesia Dr. K. Hemnath Babu 1, Dr. Shashikanth G. Somani 2, Dr. (Col)
Original article: A comparative study of Ropivacaine and Bupivacaine in combined spinal epidural anaesthesia and Post- operative analgesia Dr. K. Hemnath Babu 1, Dr. Shashikanth G. Somani 2, Dr. (Col)
Regional Anaesthesia for Children
 Regional Anaesthesia for Children Indispensable! but also safe? PD Dr. med. Jacqueline Mauch Outline Significance of regional anaesthesia in paediatric surgery Risks and complications of regional anaesthesia
Regional Anaesthesia for Children Indispensable! but also safe? PD Dr. med. Jacqueline Mauch Outline Significance of regional anaesthesia in paediatric surgery Risks and complications of regional anaesthesia
Upper Extremity Fractures
 Upper Extremity Fractures Ranie Whatley, RN,FNP-C David W. Gray, MD Skeletal Trauma 10 to 15 % of all Childhood Injuries Physeal (Growth Plate) Injuries are ~ 15% of all Skeletal Injuries Orthopaedic Assessment
Upper Extremity Fractures Ranie Whatley, RN,FNP-C David W. Gray, MD Skeletal Trauma 10 to 15 % of all Childhood Injuries Physeal (Growth Plate) Injuries are ~ 15% of all Skeletal Injuries Orthopaedic Assessment
A new brachial plexus block technique in dogs
 Veterinary Anaesthesia and Analgesia, 2002, 29, 133^139 A new brachial plexus block technique in dogs Fa bio Futema DVM, MS, DeniseTabacchiFantoniDVM, PhD, Jose Ota vio Costa Auler Jr MD, PhD, Silvia Renata
Veterinary Anaesthesia and Analgesia, 2002, 29, 133^139 A new brachial plexus block technique in dogs Fa bio Futema DVM, MS, DeniseTabacchiFantoniDVM, PhD, Jose Ota vio Costa Auler Jr MD, PhD, Silvia Renata
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
Wrist Block For Dupuytren s Fasciectomies -Is This A Viable Option Of Regional Anaesthesia?
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 Wrist Block For Dupuytren s Fasciectomies -Is This A Viable Option Of Regional Anaesthesia? S Giri, M Kyi, M Thibbiah, G Krishnamurthy
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 Wrist Block For Dupuytren s Fasciectomies -Is This A Viable Option Of Regional Anaesthesia? S Giri, M Kyi, M Thibbiah, G Krishnamurthy
COMPARISON OF INCREMENTAL SPINAL ANAESTHESIA USING A 32-GAUGE CATHETER WITH EXTRADURAL ANAESTHESIA FOR ELECTIVE CAESAREAN SECTION
 British Journal of Anaesthesia 1991; 66: 232-236 COMPARISON OF INCREMENTAL SPINAL ANAESTHESIA USING A 32-GAUGE CATHETER WITH EXTRADURAL ANAESTHESIA FOR ELECTIVE CAESAREAN SECTION I. G. KESTIN, A. P. MADDEN,
British Journal of Anaesthesia 1991; 66: 232-236 COMPARISON OF INCREMENTAL SPINAL ANAESTHESIA USING A 32-GAUGE CATHETER WITH EXTRADURAL ANAESTHESIA FOR ELECTIVE CAESAREAN SECTION I. G. KESTIN, A. P. MADDEN,
Mr David A McDonald Service Improvement Manager Whole System patient Flow Improvement Programme Scottish Government
 Mr David A McDonald Service Improvement Manager Whole System patient Flow Improvement Programme Scottish Government Introduction Brief update Two main topics Use of Gabapentin Local Infiltration Analgesia
Mr David A McDonald Service Improvement Manager Whole System patient Flow Improvement Programme Scottish Government Introduction Brief update Two main topics Use of Gabapentin Local Infiltration Analgesia
Ultrasound-guided supraclavicular block
 THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
British Journal of Anaesthesia 103 (3): (2009) doi: /bja/aep173 Advance Access publication July 8, 2009
 REGIONAL ANAESTHESIA Comparison of economical aspects of interscalene brachial plexus blockade and general anaesthesia for arthroscopic shoulder surgery C. Gonano, S. C. Kettner, M. Ernstbrunner, K. Schebesta,
REGIONAL ANAESTHESIA Comparison of economical aspects of interscalene brachial plexus blockade and general anaesthesia for arthroscopic shoulder surgery C. Gonano, S. C. Kettner, M. Ernstbrunner, K. Schebesta,
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology University of Washington, Seattle, WA
 ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
perivascular, sensory and motor effects, 62, side effects, 64 and subfascial hematoma, 221 axillary plexus, 6 7 axonotmesis, 221, 222
 249 Index A abscess, and continuous peripheral nerve block, 244 Achilles tendon rupture, 173 and saphenous nerve block, 208 and sural nerve block, 209 and tibial nerve block, 203, 204, 210, 211 acromion,
249 Index A abscess, and continuous peripheral nerve block, 244 Achilles tendon rupture, 173 and saphenous nerve block, 208 and sural nerve block, 209 and tibial nerve block, 203, 204, 210, 211 acromion,
BILATERAL RARE NEURO VASCULAR VARIATIONS OF UPPER LIMB A CASE REPORT
 BILATERAL RARE NEURO VASCULAR VARIATIONS OF UPPER LIMB A CASE REPORT *N. B. S. Parimala Department of Anatomy, Dr. Pinnamaneni Siddhartha Institute of Medical Sciences & Research Foundation, Chinnaoutpalli,
BILATERAL RARE NEURO VASCULAR VARIATIONS OF UPPER LIMB A CASE REPORT *N. B. S. Parimala Department of Anatomy, Dr. Pinnamaneni Siddhartha Institute of Medical Sciences & Research Foundation, Chinnaoutpalli,
Minimum Effective Volume of Lidocaine for Ultrasound-Guided Infraclavicular Block
 ULTRASOUND ARTICLE Minimum Effective Volume of Lidocaine for Ultrasound-Guided Infraclavicular Block De Q.H. Tran, MD, FRCPC,* Shubada Dugani, MBBS, FRCA,* Alina Dyachenko, MSc,Þ José A. Correa, PhD,þ
ULTRASOUND ARTICLE Minimum Effective Volume of Lidocaine for Ultrasound-Guided Infraclavicular Block De Q.H. Tran, MD, FRCPC,* Shubada Dugani, MBBS, FRCA,* Alina Dyachenko, MSc,Þ José A. Correa, PhD,þ
Case Report THE COMBINATION OF ULTRASOUND-GUIDED PECTORAL NERVES II AND PARA-
 Case Report Interventional Pain Management Reports Volume 1, Number 4, pp175-179 2017, American Society of Interventional Pain Physicians THE COMBINATION OF ULTRASOUND-GUIDED PECTORAL NERVES II AND PARA-
Case Report Interventional Pain Management Reports Volume 1, Number 4, pp175-179 2017, American Society of Interventional Pain Physicians THE COMBINATION OF ULTRASOUND-GUIDED PECTORAL NERVES II AND PARA-
BRACHIAL PLEXUS 11/12/2014 كيف تتكون الضفيرة FORMATION ENLARGEMENT (INTUMESCENCE) OF THE SPINAL CORD. Grey matter. Cervical intumescence - C 6 - T 2
 BRACHIAL PLEXUS Prof. Fawzy Elnady ENLARGEMENT (INTUMESCENCE) OF THE SPINAL CORD Grey matter Cervical intumescence - C 6 - T 2 Lumbar intumescence - L 4 S 2 كيف تتكون الضفيرة FORMATION The ventral rami
BRACHIAL PLEXUS Prof. Fawzy Elnady ENLARGEMENT (INTUMESCENCE) OF THE SPINAL CORD Grey matter Cervical intumescence - C 6 - T 2 Lumbar intumescence - L 4 S 2 كيف تتكون الضفيرة FORMATION The ventral rami
A COMPARATIVE STUDY OF LIGNOCAINE 0.5% AND ROPIVACAINE 0.2% FOR INTRAVENOUS REGIONAL ANESTHESIA FOR ELECTIVE UPPER LIMB SURGERY
 A COMPARATIVE STUDY OF LIGNOCAINE 0.5% AND ROPIVACAINE 0.2% FOR INTRAVENOUS REGIONAL ANESTHESIA FOR ELECTIVE UPPER LIMB SURGERY S. Asrar 1, Devesh S 2, Vidushi S 3, Meenaxi S 4*, Anumeha J 5 Department
A COMPARATIVE STUDY OF LIGNOCAINE 0.5% AND ROPIVACAINE 0.2% FOR INTRAVENOUS REGIONAL ANESTHESIA FOR ELECTIVE UPPER LIMB SURGERY S. Asrar 1, Devesh S 2, Vidushi S 3, Meenaxi S 4*, Anumeha J 5 Department
Regional Anaesthesia: Minimizing risk and complications. Mafeitzeral Mamat Anaesthesiology & Critical Care Faculty of Medicine UiTM Sg Buloh
 Regional Anaesthesia: Minimizing risk and complications Mafeitzeral Mamat Anaesthesiology & Critical Care Faculty of Medicine UiTM Sg Buloh Regional anesthesia is an art. Remembering that even experts
Regional Anaesthesia: Minimizing risk and complications Mafeitzeral Mamat Anaesthesiology & Critical Care Faculty of Medicine UiTM Sg Buloh Regional anesthesia is an art. Remembering that even experts
Upper limb Arm & Cubital region 黃敏銓
 Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries and Perineal Surgeries
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/229 Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/229 Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries
Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report
 SHORT REPORT Eur J Anat, 10 (3): 61-66 (2006) Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report K. Ramachandran, I. Kanakasabapathy and
SHORT REPORT Eur J Anat, 10 (3): 61-66 (2006) Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report K. Ramachandran, I. Kanakasabapathy and
Repair of Severe Traction Lesions of the Brachial Plexus
 Repair of Severe Traction Lesions of the Brachial Plexus LAURENT SEDEL, M.D. Since 1972, the author has performed 259 brachial plexus repairs and various associated secondary procedures. The best results
Repair of Severe Traction Lesions of the Brachial Plexus LAURENT SEDEL, M.D. Since 1972, the author has performed 259 brachial plexus repairs and various associated secondary procedures. The best results
REGIONAL ANALGESIA FOR POST-OPERATIVE PAIN MANAGEMENT INITIAL EXPERIENCE IN A LOW RESOURCE SETTING
 1 Ea s t Af r i c a n Me d i c a l Jo u r n a l March 212 East African Medical Journal Vol. 89 No. 3 March 212 REGIONAL ANALGESIA FOR POST-OPERATIVE PAIN MANAGEMENT INITIAL EXPERIENCE IN A LOW RESOURCE
1 Ea s t Af r i c a n Me d i c a l Jo u r n a l March 212 East African Medical Journal Vol. 89 No. 3 March 212 REGIONAL ANALGESIA FOR POST-OPERATIVE PAIN MANAGEMENT INITIAL EXPERIENCE IN A LOW RESOURCE
