Neurological and Neuromuscular Disorders. Elizabeth Papp, RN, MSN, CNS
|
|
|
- Cory Geoffrey Evans
- 5 years ago
- Views:
Transcription
1 Neurological and Neuromuscular Disorders Elizabeth Papp, RN, MSN, CNS June, 2018
2 Neuromuscular Birth Injuries: Overview Nerve damage caused by trauma during delivery Abnormal labor time (long or short) LGA CPD Abnormal presentation Instrument-assisted delivery Nerves most commonly implicated Cervical nerves 5, 6, 7, and 8 Thoracic nerve 1 Cranial nerve VII Phrenic nerve 2
3 Neuromuscular Birth Injuries: Brachial Plexus Injuries Presentation Erb s palsy: No spontaneous abduction or external rotation of affected arm (absent Moro) Hand function is often preserved (grasp reflex present) waiter s tip position Global plexus palsy (Erb-Duchenne-Klumpke): Flaccidity of affected arm and hand Absent Moro and grasp reflexes Klumpke palsy: Flaccidity of hand and fingers of affected arm (present Moro, absent grasp) claw-hand deformity 3
4 Neuromuscular Birth Injuries: Brachial Plexus Injuries Cause Erb s palsy: Most common, injury to nerve roots C5 and C6 Global plexus palsy (Erb-Duchenne- Klumpke): Second most common, injury to nerve roots C5 through T1 Klumpke palsy: Injury to nerve roots C8 and T1 only 4
5 Neuromuscular Birth Injuries: Brachial Plexus Injuries Management Physical examination to assess extent of neurological involvement X-ray if concern for fracture or shoulder dislocation Neurology, orthopedic, and PT consultation Passive ROM exercises when post-injury neuritis has resolved (7-10 days) Use of wrist and/or finger splints, if indicated Caregiver education regarding importance of passive exercise to maintain joint function Complications Contractures may develop without passive exercise Decreased sensation may lead to developmental deficits in affected arm Outcome Spontaneous resolution generally occurs within 12 months Best predictor of recovery is return of biceps function by 3 months of age 5
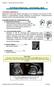
6 Neuromuscular Birth Injuries: Phrenic Nerve Injury Presentation Typically associated with brachial plexus injury, but can occur alone Respiratory distress often requiring oxygen and supportive ventilation Cause Difficult extraction, esp. breech Damage to phrenic nerve impairs nervous system stimulation of ipsilateral half of diaphragm; cervical nerves III, IV & V Management Diagnosed via US, NOT CXR Affected side down Supportive therapies including respiratory support Surgical plication of diaphragm, if indicated Complications Respiratory failure, pulmonary infection, growth failure, death Outcome Mortality rate is 10 15% Surviving infants generally recover within a year 6
7 Neuromuscular Birth Injuries: Facial Nerve Palsy Presentation Persistent open eye on affected side Suck with drooling on affected side Mouth drawn to normal side when crying Cause Trauma to nerve sheath (CN VII) during birth Associated with instrument-assisted deliveries (forceps) Management Provide artificial tears to open eye, a patch may be needed Family support Complications Feeding impairment Outcome Spontaneous resolution is common (> 90% recover without intervention) 7
8 Hypoxic Ischemic Encephalopathy (HIE): Overview Cerebral injury associated with hypoxia and ischemia Incidence: 1-2 cases per 1000 term births with a mortality rate of 10 20% Hypoxemia: decrease in amount of oxygen circulating in the blood Ischemia: decrease in blood flow to brain (decreased perfusion) Decreased glucose available Asphyxia: Impairment of oxygen and carbon dioxide exchange Initially causes increase in cerebral blood flow Increasing levels of carbon dioxide contribute to acidosis Associated with widespread systemic injury secondary to hypoxic-ischemic insult 8
9 Hypoxic Ischemic Encephalopathy (HIE): Overview Associated antepartum conditions (20% of cases): Maternal hypotension, placental vasculopathy Contribute to decreased fetal reserves Intrapartum events (35% of cases): Prolapsed cord, abruption, traumatic birth Combination of antepartum and intrapartum (35% of cases) Neonatal conditions (10% of cases): Severe pulmonary disease, recurrent apnea Congenital heart disease Preterm infant is at greater risk of HIE than term infant 9
10 HIE: Presentation Stage I (mild encephalopathy) Hyperalert, normal muscle tone, active suck, strong Moro reflex, (+) myoclonus, hyper-responsive to stimuli Stage II (moderate) Lethargy and hypotonic, (+) myoclonus, seizures common, weak reflexes with overall increased tendon reflexes, overactive Doll s eye Stage III (severe) Comatose, apnea and bradycardia, mechanical ventilation, seizures typical within 12 hours of birth, severe hypotonia and flaccidity, absent reflexes, pupils often unequal, variable reactivity, poor light reflex, Doll s eye weak or absent 10
11 HIE: Management Diagnostic testing: Neurologic examination (Sarnat criteria) Conventional EEG (ceeg) Amplitude-integrated EEG (aeeg) Neuroimaging Head ultrasound CT scan MRI Interventions: Resuscitation and stabilization Therapeutic hypothermia Family support and education Palliative care Treat seizures 11
12 HIE: Complications Multisystem disorders are common with stage II and III HIE Renal and cardiac abnormalities Pulmonary hypertension Liver function abnormalities Thrombocytopenia Disseminated intravascular coagulation (DIC) 12
13 HIE: Outcome Mild encephalopathy: Recovery expected Good outcome with very small risk of long-term disability Moderate encephalopathy (in absence of therapeutic hypothermia): 6% death, 30% disability Severe encephalopathy (in absence of therapeutic hypothermia): 60% death, 100% disability Early onset of seizures and ability to control szs are good predictors of outcome Rapid turnaround after initial insult also good predictor 13
14 Intraventricular Hemorrhage (IVH): Overview Significant injury in the preterm brain Germinal matrix hemorrhage: Germinal matrix is immature and highly vascularized area of preterm infant brain Site of neuron and glia development Poorly supported and fragile blood vessels, sensitive to blood pressure fluctuation and reperfusion injury Hypotension/hypertension, perinatal asphyxia, rapid volume infusions, myocardial failure, hypothermia, hyperosmolarity, etc. Involution of germinal matrix occurs with advancing gestational age, germinal matrix disappears by 36 weeks, GM hemorrhage less common in infants > 32 weeks Germinal matrix hemorrhage may extend to fill lateral ventricles and worsening IVH 14
15 Intraventricular Hemorrhage (IVH): Overview Incidence: 30 40% of infants <1500 grams or <30 weeks PMA <28 weeks PMA have a 3-fold higher risk than weeks PMA 2 3% in term infants Timing of onset: 50% by 24 hours 80% by 48 hours 90% by 72 hours 15
16 IVH: Presentation Presentation ranges from undetectable to dramatic Sudden deterioration: oxygen desaturation, bradycardia, metabolic acidosis, falling hematocrit, hypotonia, shock, hyperglycemia Symptoms of worsening hemorrhage: full or tense fontanelle, increased ventilator support, seizures, apnea, decreased activity, decreased level of consciousness Rapid and profound clinical decline associated with increased severity of IVH Grading of IVH 16
17 Neuroimaging IVH: Management Routine head ultrasound screening of infants born at < 30 weeks PMA Serial head ultrasounds to monitor progression MRI if parenchymal injury is suspected Supportive Care Minimize stimulation Avoid wide swings in blood pressure Closely monitor respiratory support Avoid acidosis, hypercarbia, fluid overload 17
18 IVH: Complications Neurodevelopmental disabilities Progressive hydrocephalus Seizures Death 18
19 Mild/small IVH IVH: Outcome Neurodevelopmental disabilities (NDD) similar to premature infants without hemorrhage, major NDD 10% Moderate IVH Major NDD in 40% Mortality rate 10% Progressive hydrocephalus in 20% Severe IVH Major NDD in 80% Mortality rate 50 60% Progressive hydrocephalus common 19
20 Periventricular Leukomalacia (PVL): Overview Severe white matter injury highly associated with preterm birth; HYPOTENSION Focal injury: cystic necrotic lesion found bilaterally Nonhemorrhagic and symmetric Caused by ischemia from fluctuations in arterial circulation Diffuse white matter injury Noncystic lesions associated with disturbances in myelinization Often associated with germinal matrix hemorrhages or IVH Leukomalacia: softening of white matter 20
21 Acute phase: Subtle PVL: Presentation Altered muscle tone in lower extremities, hypotension, lethargy 6 10 weeks after white matter injury Irritable, hypertonic, increased flexion of arms and extension of legs, frequent tremors and startles Moro reflex abnomalities 21
22 Diagnostic evaluation: Head ultrasound CT scan or MRI Interventions: Treat primary insult PVL: Management Supportive care to prevent further hypoxic-ischemic damage Treatment of hydrocephalus and associated neurological sequalea Family support and anticipatory guidance Developmental care, PT/OT, feeding support 22
23 Spastic diplegia PVL: Complications Intellectual deficits, learning disorders Hyperactivity disorders Visual impairment Lower limb weakness 23
24 PVL: Outcome Determined by location and extent of injury Spastic diplegia reported in as many as 50% of infants with PVL Neurodevelopmental follow-up and developmental support improve outcomes related to learning and behavioral disorders 24
25 Seizures: Overview Sign of malfunctioning neuronal system Excessive simultaneous electrical discharge Causes include: Metabolic encephalopathies Structural abnormalities Meningitis Drug withdrawal Genetic etiology 25
26 Seizures: Overview Metabolic encephalopathies: Hypoglycemia Ischemia Hypoxemia Hypo- or hypernatremia, Hypocalcemia Hypomagnesemia Inborn error of metabolism Pyridoxine deficiency Hyperammonemia 26
27 Structural abnormalities: HIE IVH Intrapartum trauma Perinatal stroke Cerebral dysgenesis Seizures: Overview 27
28 Other causes: Meningitis Group B streptococcus Listeria monocytogenes TORCH etiology Drug withdrawal Seizures: Overview Prenatal or postnatal exposure to opiates Genetic (familial) Self-limiting 28
29 Seizures: Presentation Subtle (motor automatisms) Rowing, stepping, pedaling movements, eye blinking/fluttering, staring, lacrimation, smacking of lips, salivation, sucking Clonic Rhythmic movements of muscle groups in a focal distribution Rapid phase followed by a slow return to movement Not stopped with flexion Tonic (postural) Sustained generalized tonic extension of all extremities or flexion of the upper limbs with extension of the lower extremities Characteristic of preterm infants with severe IVH May closely mimic decerebrate or decorticate posturing Multifocal clonic (generalized) Clonic movements that migrate from one limb to another without a specific pattern Associated with significant morbidity and mortality 29
30 Diagnostic evaluation: Seizures: Management Review perinatal/neonatal clinical course and family history Blood glucose immediately to rule out hypoglycemia Physical examination Lab studies (blood gas, electrolytes, CBC with differential) Septic workup if infectious etiology suspected Blood, urine, CSF cultures Nasal and rectal swabs if HSV suspected Metabolic studies Head ultrasound, CT, MRI EEG 30
31 Supportive care Seizures: Management Careful assessment of clinical seizure activity Medication management: Phenobarbitol Monitor respiratory status Fosphenytoin Monitor respiratory status and BP Levetiracetam Lorazepam 31
32 Seizures: Complications and Outcome Untreated sustained seizures exacerbate underlying pathology Outcome varies significantly based upon etiology: Familial seizures: often benign and self-limiting Refractory seizures associated with HIE: severe morbidity and mortality 32
33 Subdural Hemorrhage: Overview Rupture of draining veins and sinuses that occupy the subdural space Due to molding and torsional forces on the head during birth Risk factors: Macrosomia, CPD, shoulder dystocia Traumatic birth Vaginal breech presentation Malpresentation Instrument-assisted vaginal birth 33
34 Subdural Hemorrhage: Presentation Subdural hemorrhage accounts for less than 10% of all intracranial bleeds Large hemorrhage: Nuchal rigidity, coma, abnormal respiratory pattern, unreactive pupils, signs of increased ICP, seizures, signs of hypovolemia and anemia Small hemorrhage: Subtle or few signs until hematoma presses on brain tissue or CSF starts to build up, may cause deterioration in mental status, development of hydrocephalus, seizures 34
35 Subdural Hemorrhage: Management Supportive care and seizure management Volume replacement, respiratory support, pressor support Close monitoring of neurologic status Subdural tap or subdural shunt in infants with increasing ICP Monitor and intervention for progressive hydrocephalus May occur weeks after the hemorrhage 35
36 Hydrocephalus Seizures Subdural Hemorrhage: Complications Neurodevelopmental impairment 36
37 Subdural Hemorrhage: Outcome Outcome dependent upon severity of hemorrhage Mortality rate may be as high as 45% 37
38 Hydrocephalus: Overview Excess of CSF in ventricular system Caused by inadequate reabsorption of CSF or overproduction Aqueductal outflow obstruction (non-communicating hydrocephalus) Dandy-Walker cyst, myelomeningocele with Arnold-Chiari malformation, infection, aqueductal stenosis, Post-hemorrhagic hydrocephalus Flow between lateral ventricles and subarachnoid space (communicating, non-obstructive hydrocephalus) 38
39 Hydrocephalus: Presentation Increasing head circumference Widened sutures Full, bulging, or tense fontanelles Setting-sun eyes Vomiting, lethargy, irritability 39
40 Hydrocephalus: Management Diagnostic testing: determine underlying cause, identify site of obstruction (if obstructive) Supportive care: decreased stimuli, minimal handling, monitor head circumference measurements, prone for feedings Mechanical CSF drainage: Short term: lumbar puncture or direct ventricular access Long term: ventriculo-peritoneal shunt Procedural and post-op care Medications: Lasix or Diamox (Acetazolamide) 40
41 Hydrocephalus: Complications Neurological deterioration associated with increased ICP Infection of VP shunt, infection associated with LP and ventricular access 41
42 Hydrocephalus: Outcome Determined by underlying cause 42
43 Neural Tube Defects: Overview Primary NTD Failure of neural tube closure or disruption of closed tube Occurs between days of gestation Location of neural tube failure determines presentation Anencephaly, encephalocele, myelomeningocele Secondary NTD Abnormal development of the lower sacral or coccygeal segments during secondary neurulation Defects present primarily in lumbosacral spinal region Skin typically intact over lesion Meningocele, lipomeningocele, sacral agenesis/dysgenesis 43
44 44
45 Presentation Etiology Management Complications Outcome Neural Tube Defects: Anencephaly 45
46 Neural Tube Defects: Anencephaly Presentation Etiology Management Complications Outcome Key Points: 1. Alpha-fetoprotein high in latter part of 1 st trimester 2. Higher risk if you are: Female, White, poor, affected sibling 3. Failure of anterior neural tube closure 4. Occurs in 1 st stage of neuro development; primary neurulation 46
47 Presentation Etiology Management Complications Outcome Neural Tube Defects: Encephalocele 47
48 Neural Tube Defects: Encephalocele Presentation Etiology Management Complications Outcome Key Points 1. May or may not contain meninges or brain parenchyma 2. Most occur in occipital region; most contain neural tissue 3. Treatment is surgical, 50% also have hydrocephalus 48
49 Neural Tube Defects: Myelomeningocele 49
50 Neural Tube Defects: Myelomeningocele Presentation Etiology Management Complications Outcome Key Points: 1. Spinal cord and meninges are exposed 2. 95% will have some degree of hydrocephalus 3. Almost all infants with MM ALSO have Chiari malformation 50
51 Chiari Malformation Brain tissue extends into the spinal canal Presents with reflux, laryngeal stridor and in severe forms, central apnea 51
52 Neural Tube Defects: Myelomeningocele Key Points: 1. Failure of posterior neural tube to close 2. 80% occur in lumbar region 3. At birth, wrap defect in gauze soaked with NS and sterile feeding tube 4. Prone, kneeling position 5. Drape over buttocks below the lesion 6. 80% with normal intelligence 7. 85% ambulatory (with or without aid); ability to be ambulatory depends on location of lesion. < = S1 walk unaided, L4/5 walk with aid, > L2 wheelchair 52
53 Recommended further study: General brain anatomy Brain physiology Neuro Assessment Disorders not covered: Microcephaly Craniosynostosis Birth Injuries not covered: Cephalohematoma and Caput Skull fractures 53
54 Recommended further study: Intracranial Hemorrhage not covered: Subarachnoid Intracerubellar Meningitis 54
55
Neurological and Neuromuscular Disorders. Elizabeth Papp, RN, MSN, CNS
 Neurological and Neuromuscular Disorders Elizabeth Papp, RN, MSN, CNS June, 2018 Neuromuscular Birth Injuries: Overview Nerve damage caused by trauma during delivery Prolonged labor LGA CPD Abnormal presentation
Neurological and Neuromuscular Disorders Elizabeth Papp, RN, MSN, CNS June, 2018 Neuromuscular Birth Injuries: Overview Nerve damage caused by trauma during delivery Prolonged labor LGA CPD Abnormal presentation
Neuro. Development. Judy Philbrook, NNP-BC. ! Primary neurulation! Prosencepahlic! Neuronal proliferation. ! 3-4 weeks! 2-3 months!
 Neuro Judy Philbrook, NNP-BC Microsoft clip art Development! Primary neurulation! Prosencepahlic! Neuronal proliferation! Neuronal migration! Organization! Myelination! 3-4 weeks! 2-3 months! 3-4 months!
Neuro Judy Philbrook, NNP-BC Microsoft clip art Development! Primary neurulation! Prosencepahlic! Neuronal proliferation! Neuronal migration! Organization! Myelination! 3-4 weeks! 2-3 months! 3-4 months!
NEONATAL SEIZURE. IAP UG Teaching slides
 NEONATAL SEIZURE 1 INTRODUCTION One of the important neonatal neurological emergencies requiring immediate medical care. Contribute to significant morbidity and mortality Incidence is around 0.5 to 0.8%
NEONATAL SEIZURE 1 INTRODUCTION One of the important neonatal neurological emergencies requiring immediate medical care. Contribute to significant morbidity and mortality Incidence is around 0.5 to 0.8%
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Neonatal Seizure. Dr.Nawar Yahya. Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan. Supervised by:
 Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Surgical Options in Post Haemorrhagic Ventricular Dilation
 Surgical Options in Post Haemorrhagic Ventricular Dilation Benedetta Pettorini Consultant Paediatric Neurosurgeon Alder Hey Childrens Hospital Liverpool, UK Risk Factors for IVH 1. Prematurity: Occurs
Surgical Options in Post Haemorrhagic Ventricular Dilation Benedetta Pettorini Consultant Paediatric Neurosurgeon Alder Hey Childrens Hospital Liverpool, UK Risk Factors for IVH 1. Prematurity: Occurs
PEDIATRIC BRAIN CARE
 PEDIATRIC BRAIN CARE The brain matters most! OVERVIEW OF NEURO ASSESSMENT 1. Overall responsiveness/activity 2. The eyes 3.? Increased ICP 4. Movements 5.? Seizures 6. Other OVERALL RESPONSIVENESS/ ACTIVITY
PEDIATRIC BRAIN CARE The brain matters most! OVERVIEW OF NEURO ASSESSMENT 1. Overall responsiveness/activity 2. The eyes 3.? Increased ICP 4. Movements 5.? Seizures 6. Other OVERALL RESPONSIVENESS/ ACTIVITY
The high risk neonate
 The high risk neonate Infant classification by gestational (postmenstrual) age Preterm. Less than 37 completed weeks (259 days). Term. Thirty-seven to 416/7 weeks (260-294 days). Post-term. Forty-two weeks
The high risk neonate Infant classification by gestational (postmenstrual) age Preterm. Less than 37 completed weeks (259 days). Term. Thirty-seven to 416/7 weeks (260-294 days). Post-term. Forty-two weeks
NEONATAL SEIZURES-PGPYREXIA REVIEW
 NEONATAL SEIZURES-PGPYREXIA REVIEW This is a very important Postgraduate topics will few Q asked in undergraduation also. Lets see them in detail. References: 1.Volpe s Neurology of newborn 2.Nelson s
NEONATAL SEIZURES-PGPYREXIA REVIEW This is a very important Postgraduate topics will few Q asked in undergraduation also. Lets see them in detail. References: 1.Volpe s Neurology of newborn 2.Nelson s
Birth Asphyxia. Perinatal Depression. Birth Asphyxia. Risk Factors maternal. Risk Factors fetal. Risk Factors Intrapartum 2/12/2011
 Birth Asphyxia Perinatal Depression Sara Brown, ARNP Children s Hospital and Regional Medical Center May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood
Birth Asphyxia Perinatal Depression Sara Brown, ARNP Children s Hospital and Regional Medical Center May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
These signs should lead to the administration of high concentrations of
 Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Neonatal infections and neonatal seizures. Mohamed Waheed Elsharief Dept. of paediatrics Faculty of medicine Jazan University KSA
 Neonatal infections and neonatal seizures Mohamed Waheed Elsharief Dept. of paediatrics Faculty of medicine Jazan University KSA objectives By the end of this lecture the student should Define neonatal
Neonatal infections and neonatal seizures Mohamed Waheed Elsharief Dept. of paediatrics Faculty of medicine Jazan University KSA objectives By the end of this lecture the student should Define neonatal
Intraventricular Hemorrhage and Periventricular Leukomalacia
 Intraventricular Hemorrhage and Periventricular Leukomalacia Intraventricular Hemorrhage Intraventricular hemorrhage (IVH) is bleeding inside the lateral ventricles. Bleeding frequently occurs in areas
Intraventricular Hemorrhage and Periventricular Leukomalacia Intraventricular Hemorrhage Intraventricular hemorrhage (IVH) is bleeding inside the lateral ventricles. Bleeding frequently occurs in areas
NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY
 Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
Perinatal Depression. Lauren Sacco DNP, ARNP Seattle Children s
 Perinatal Depression Lauren Sacco DNP, ARNP Seattle Children s Birth Asphyxia May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood gas exchange that leads
Perinatal Depression Lauren Sacco DNP, ARNP Seattle Children s Birth Asphyxia May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood gas exchange that leads
Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound
 Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound Robert H. Debbs, D.O.,F.A.C.O.O.G. Professor of OB-GYN Perelman School of Medicine, University of Pennsylvania Director, Pennsylvania
Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound Robert H. Debbs, D.O.,F.A.C.O.O.G. Professor of OB-GYN Perelman School of Medicine, University of Pennsylvania Director, Pennsylvania
DISORDERS OF THE NERVOUS SYSTEM
 DISORDERS OF THE NERVOUS SYSTEM Bell Work What s your reaction time? Go to this website and check it out: https://www.justpark.com/creative/reaction-timetest/ Read the following brief article and summarize
DISORDERS OF THE NERVOUS SYSTEM Bell Work What s your reaction time? Go to this website and check it out: https://www.justpark.com/creative/reaction-timetest/ Read the following brief article and summarize
Supplemental Digital Content: Definitions Based on the International Classification of Diseases, Ninth Revision, Clinical Modification
 Supplemental Digital Content: Definitions Based on the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) Diagnose and Procedures Codes 1. ICD-9-CM definition of
Supplemental Digital Content: Definitions Based on the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) Diagnose and Procedures Codes 1. ICD-9-CM definition of
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised by P.
 TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised 05-13-13 by P. Joe SCREENING FOR POTENTIAL COOLING PATIENTS Patients who are >
TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised 05-13-13 by P. Joe SCREENING FOR POTENTIAL COOLING PATIENTS Patients who are >
Admission/Discharge Form for Infants Born in Please DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012
 Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Clinical Guidance. Neonatal Manual Chapter 10: Musculoskeletal problems
 Clinical Guidance Neonatal Manual Chapter 10: Musculoskeletal problems Summary This manual contains clinical guidelines developed by the Neonatal Unit multidisciplinary team over recent years. This chapter
Clinical Guidance Neonatal Manual Chapter 10: Musculoskeletal problems Summary This manual contains clinical guidelines developed by the Neonatal Unit multidisciplinary team over recent years. This chapter
The Neurologic Examination. John W. Engstrom, M.D. University of California San Francisco School of Medicine
 The Neurologic Examination John W. Engstrom, M.D. University of California San Francisco School of Medicine Overview The Neurologic Examination Mental status demonstration/questions Cranial nerves demonstration/questions
The Neurologic Examination John W. Engstrom, M.D. University of California San Francisco School of Medicine Overview The Neurologic Examination Mental status demonstration/questions Cranial nerves demonstration/questions
Babies First and CaCoon Risk Factors (A Codes and B Codes)
 Babies First and Risk Factors (A Codes and B Codes) (Birth through 4 years of age) Medical Risk Factors A1. Drug exposed infant (See A29) A2. Infant HIV positive A3. Maternal PKU or HIV positive A4. Intracranial
Babies First and Risk Factors (A Codes and B Codes) (Birth through 4 years of age) Medical Risk Factors A1. Drug exposed infant (See A29) A2. Infant HIV positive A3. Maternal PKU or HIV positive A4. Intracranial
COMPLICATIONS OF PREMATURITY
 ا د. نعمان نافع الحمداني Professor Numan Nafie Hameed COMPLICATIONS OF PREMATURITY Early: RDS, Jaundice, PDA, IVH, Early anemia of prematurity. These occur while the patient in hospital. Late: ROP, BPD
ا د. نعمان نافع الحمداني Professor Numan Nafie Hameed COMPLICATIONS OF PREMATURITY Early: RDS, Jaundice, PDA, IVH, Early anemia of prematurity. These occur while the patient in hospital. Late: ROP, BPD
Complex Hydrocephalus
 2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
Neurologic Examination
 John W. Engstrom, MD October 16, 2015 Neurologic Examination Overview The Neurologic Examination Neurologic Examination John W. Engstrom, M.D. Dept. of Neurology University of California, San Francisco
John W. Engstrom, MD October 16, 2015 Neurologic Examination Overview The Neurologic Examination Neurologic Examination John W. Engstrom, M.D. Dept. of Neurology University of California, San Francisco
TLC March 27, Shawn Hollinger-Neonatal Fellow CHEO
 TLC March 27, 2013 Presented/Prepared by: Shawn Hollinger, PGY5 Neonatal-Perinatal Medicine Resident - University of Ottawa With slides/images from Dr. Brigitte Lemyre Associate Professor of Pediatrics
TLC March 27, 2013 Presented/Prepared by: Shawn Hollinger, PGY5 Neonatal-Perinatal Medicine Resident - University of Ottawa With slides/images from Dr. Brigitte Lemyre Associate Professor of Pediatrics
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Birth injuries may result from :
 Birth Trauma ( Birth Injuries) avoidable and unavoidable mechanical, hypoxic and ischemic injury affecting the infant during labor and delivery. Birth injuries may result from : 1. Inappropriate or deficient
Birth Trauma ( Birth Injuries) avoidable and unavoidable mechanical, hypoxic and ischemic injury affecting the infant during labor and delivery. Birth injuries may result from : 1. Inappropriate or deficient
Traumatic brain Injury- An open eye approach
 Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
The two most common forms of brain injury noted in preterm neonates are intraventricular hemorrhage (IVH) and 1
 9 The two most common forms of brain injury noted in preterm neonates are intraventricular hemorrhage (IVH) and 1 periventricular leukomalacia (PVL). These lesions are more common in the smallest and most
9 The two most common forms of brain injury noted in preterm neonates are intraventricular hemorrhage (IVH) and 1 periventricular leukomalacia (PVL). These lesions are more common in the smallest and most
Hypoxic-Ischemic Encephalopathy. TW de Witt University of Pretoria Department of Paediatrics Neonatology
 Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Intraventricular Hemorrhage in the Neonate
 Intraventricular Hemorrhage in the Neonate Angela Forbes, RN, MN, ARNP Seattle Children s Hospital Division of Pediatric Neurosurgery Seattle, Washington, U.S.A. Intraventricular Hemorrhage Who Premature
Intraventricular Hemorrhage in the Neonate Angela Forbes, RN, MN, ARNP Seattle Children s Hospital Division of Pediatric Neurosurgery Seattle, Washington, U.S.A. Intraventricular Hemorrhage Who Premature
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
NEONATOLOGY Healthy newborn. Neonatal sequelaes
 NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
Fetal Medicine. Case Presentations. Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital. October 2003
 Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
CNS Embryology 5th Menstrual Week (Dorsal View)
 Imaging of the Fetal Brain; Normal & Abnormal Alfred Abuhamad, M.D. Eastern Virginia Medical School CNS Embryology 5th Menstrual Week (Dorsal View) Day 20 from fertilization Neural plate formed in ectoderm
Imaging of the Fetal Brain; Normal & Abnormal Alfred Abuhamad, M.D. Eastern Virginia Medical School CNS Embryology 5th Menstrual Week (Dorsal View) Day 20 from fertilization Neural plate formed in ectoderm
Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1
 Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1 Therapeutic Hypothermia for Neonatal Encephalopathy: Preparation for Transport to Cooling Center Teresa Z. Baker, DNP-S Annie L. Addison, FNP-S NURS
Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1 Therapeutic Hypothermia for Neonatal Encephalopathy: Preparation for Transport to Cooling Center Teresa Z. Baker, DNP-S Annie L. Addison, FNP-S NURS
Neonatal Hypotonia. Encephalopathy acute No encephalopathy. Neurology Chapter of IAP
 The floppy infant assumes a frog legged position. On ventral suspension, the baby can not maintain limb posture against gravity and assumes the position of a rag doll. Encephalopathy acute No encephalopathy
The floppy infant assumes a frog legged position. On ventral suspension, the baby can not maintain limb posture against gravity and assumes the position of a rag doll. Encephalopathy acute No encephalopathy
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound
 Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound Priyanka Upadhyay *, Ketki U Patil 1, Rajesh Kuber 2, Vilas Kulkarni 3, Amarjit Singh 4 * Chief
Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound Priyanka Upadhyay *, Ketki U Patil 1, Rajesh Kuber 2, Vilas Kulkarni 3, Amarjit Singh 4 * Chief
Child Neurology Elective PL1 Rotation
 PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
State of Florida Hypothermia Protocol. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Hypothermia Protocol Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. Entry Criteria 1. Gestational Age greater than or equal to 35 weeks gestation
State of Florida Hypothermia Protocol Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. Entry Criteria 1. Gestational Age greater than or equal to 35 weeks gestation
Approach to a Neurologic Diagnosis
 Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Malformations of the Nervous System November 10, Dr. Peter Ostrow
 Malformations of the Nervous System November 10, 2016 Dr. Peter Ostrow Malformations of the Nervous System 1. Abnormal closure of the neural tube 1. Disorders of forebrain formation 1. Cortical anomalies
Malformations of the Nervous System November 10, 2016 Dr. Peter Ostrow Malformations of the Nervous System 1. Abnormal closure of the neural tube 1. Disorders of forebrain formation 1. Cortical anomalies
Neonatal Hypoglycemia. Presented By : Kamlah Olaimat 25\7\2010
 Neonatal Hypoglycemia Presented By : Kamlah Olaimat 25\7\2010 Definition The S.T.A.B.L.E. Program defines hypoglycemia as: Glucose delivery or availability is inadequate to meet glucose demand (Karlsen,
Neonatal Hypoglycemia Presented By : Kamlah Olaimat 25\7\2010 Definition The S.T.A.B.L.E. Program defines hypoglycemia as: Glucose delivery or availability is inadequate to meet glucose demand (Karlsen,
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Lecture 3. Professor Dr Numan Nafie Hameed Al-Hamdani االستاذ الدكتور نعمان نافع حميد الحمداني
 Lecture 3 Professor Dr Numan Nafie Hameed Al-Hamdani االستاذ الدكتور نعمان نافع حميد الحمداني Neonatal Birth Traumas or injuries: These are avoidable and unavoidable injuries to the NB that occurs during
Lecture 3 Professor Dr Numan Nafie Hameed Al-Hamdani االستاذ الدكتور نعمان نافع حميد الحمداني Neonatal Birth Traumas or injuries: These are avoidable and unavoidable injuries to the NB that occurs during
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Birth injuries. Dr. Nihad Al Doori 3 rd lecture
 Birth injuries Dr. Nihad Al Doori 3 rd lecture Birth injuries are injuries that occur during the birth process. They are most likely to occur when the infant is : large, the presentation is breech, forceful
Birth injuries Dr. Nihad Al Doori 3 rd lecture Birth injuries are injuries that occur during the birth process. They are most likely to occur when the infant is : large, the presentation is breech, forceful
Epilepsy CASE 1 Localization Differential Diagnosis
 2 Epilepsy CASE 1 A 32-year-old man was observed to suddenly become unresponsive followed by four episodes of generalized tonic-clonic convulsions of the upper and lower extremities while at work. Each
2 Epilepsy CASE 1 A 32-year-old man was observed to suddenly become unresponsive followed by four episodes of generalized tonic-clonic convulsions of the upper and lower extremities while at work. Each
D is for Disability Altered Mental Status in Children
 D is for Disability Altered Mental Status in Children Joshua Ross, MD, FAAP Pediatric Emergency Medicine Emergency Care and Trauma Symposium June 22, 2015 Objectives Describe a basic approach to evaluating
D is for Disability Altered Mental Status in Children Joshua Ross, MD, FAAP Pediatric Emergency Medicine Emergency Care and Trauma Symposium June 22, 2015 Objectives Describe a basic approach to evaluating
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Hypoxic Ischemic Encephalopathy. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Hypoxic Ischemic Encephalopathy. These podcasts are designed to give medical students an overview of key topics in pediatrics.
Medical Follow-up of the High-Risk NICU Graduate
 Medical Follow-up of the High-Risk NICU Graduate Silvia Fajardo-Hiriart, M.D. Medical Director High-Risk Infant Follow-Up/Early Intervention Program University of Miami Miller School of Medicine Department
Medical Follow-up of the High-Risk NICU Graduate Silvia Fajardo-Hiriart, M.D. Medical Director High-Risk Infant Follow-Up/Early Intervention Program University of Miami Miller School of Medicine Department
Central nervous system
 Central nervous system By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 7 th Lecture Lecture outline Review of structure & function. Symptoms, signs & tests. Specific diseases. Review of structure
Central nervous system By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 7 th Lecture Lecture outline Review of structure & function. Symptoms, signs & tests. Specific diseases. Review of structure
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
This lecture will provide an overview of the neurologic exam of a neonate in the context of clinical cases.
 A11a Neuro Nuggets from the Trenches Michael D. Weiss, MD Associate Professor Department of Pediatrics, Division of Neonatology University of Florida, Gainesville, FL The speaker has signed a disclosure
A11a Neuro Nuggets from the Trenches Michael D. Weiss, MD Associate Professor Department of Pediatrics, Division of Neonatology University of Florida, Gainesville, FL The speaker has signed a disclosure
The Child with Alterations in Cerebral Function
 The Child with Alterations in Cerebral Function Neurologic Assessment VS HR, BP, Respirations, Temperature LOC Orientation Pediatric Glasgow Coma Scale Eyes Pupillary response and movement, extraoccular
The Child with Alterations in Cerebral Function Neurologic Assessment VS HR, BP, Respirations, Temperature LOC Orientation Pediatric Glasgow Coma Scale Eyes Pupillary response and movement, extraoccular
There are several types of epilepsy. Each of them have different causes, symptoms and treatment.
 1 EPILEPSY Epilepsy is a group of neurological diseases where the nerve cell activity in the brain is disrupted, causing seizures of unusual sensations, behavior and sometimes loss of consciousness. Epileptic
1 EPILEPSY Epilepsy is a group of neurological diseases where the nerve cell activity in the brain is disrupted, causing seizures of unusual sensations, behavior and sometimes loss of consciousness. Epileptic
NYEIS Version 4.3 (ICD) ICD - 10 Codes Available in NYEIS at time of version launch (9/23/2015)
 D82.1 Di George's syndrome E63.9 Nutritional deficiency, unspecified E70.21 Tyrosinemia E70.29 Other disorders of tyrosine metabolism E70.30 Albinism, unspecified E70.5 Disorders of tryptophan metabolism
D82.1 Di George's syndrome E63.9 Nutritional deficiency, unspecified E70.21 Tyrosinemia E70.29 Other disorders of tyrosine metabolism E70.30 Albinism, unspecified E70.5 Disorders of tryptophan metabolism
Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ٢ Level of consciousness is depressed Stuporous patients respond only to repeated
Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ٢ Level of consciousness is depressed Stuporous patients respond only to repeated
Provide specific counseling to parents and patients with neurological disorders, addressing:
 Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Blue Babies, Twitchy Toddlers, and Kool Kids. By Beth Paton, MSN, RN, PNP, CEN, CPEN, FAEN
 Blue Babies, Twitchy Toddlers, and Kool Kids By Beth Paton, MSN, RN, PNP, CEN, CPEN, FAEN I have no disclosures OBJECTIVES By the end of this presentation, the learner will Discuss etiologies of cyanosis
Blue Babies, Twitchy Toddlers, and Kool Kids By Beth Paton, MSN, RN, PNP, CEN, CPEN, FAEN I have no disclosures OBJECTIVES By the end of this presentation, the learner will Discuss etiologies of cyanosis
Experiences as a Donation Support Physician. Dead or not Dead? Are the following statements consistent with neurological
 Experiences as a Donation Support Physician Dead or not Dead? Are the following statements consistent with neurological determination of death (dead)? or not (not dead)? With thanks to Drs. Alex Manara,
Experiences as a Donation Support Physician Dead or not Dead? Are the following statements consistent with neurological determination of death (dead)? or not (not dead)? With thanks to Drs. Alex Manara,
intracranial anomalies
 Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Obstetric Brachial Plexus Injuries. Surgery department grand rounds Bassam MJ Addas, FRCSC Neurological Surgery, KAUH
 Obstetric Brachial Plexus Injuries. Surgery department grand rounds Bassam MJ Addas, FRCSC Neurological Surgery, KAUH Definition Obstetric versus birth palsy Obstetric versus congenital palsy Not all birth
Obstetric Brachial Plexus Injuries. Surgery department grand rounds Bassam MJ Addas, FRCSC Neurological Surgery, KAUH Definition Obstetric versus birth palsy Obstetric versus congenital palsy Not all birth
Yorkshire and Humber Neonatal ODN (South) Clinical Guideline
 Yorkshire and Humber Neonatal ODN (South) Clinical Guideline Title: Author: NEONATAL BRACHIAL PLEXUS INJURY Rebecca Musson Date written: January 2011, reviewed January 2016 Review date: January 2019 This
Yorkshire and Humber Neonatal ODN (South) Clinical Guideline Title: Author: NEONATAL BRACHIAL PLEXUS INJURY Rebecca Musson Date written: January 2011, reviewed January 2016 Review date: January 2019 This
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Management of Pregestational and Gestational Diabetes Mellitus
 Background and Prevalence Management of Pregestational and Gestational Diabetes Mellitus Pregestational Diabetes - 8 million women in the US are affected, complicating 1% of all pregnancies. Type II is
Background and Prevalence Management of Pregestational and Gestational Diabetes Mellitus Pregestational Diabetes - 8 million women in the US are affected, complicating 1% of all pregnancies. Type II is
Pediatric Learning Solutions A clinical education program exclusively for pediatric professionals
 Pediatric Learning Solutions A clinical education program exclusively for pediatric professionals The following Pediatric Learning Solutions courses align to focus areas of the Neonatal CCRN Exam Content
Pediatric Learning Solutions A clinical education program exclusively for pediatric professionals The following Pediatric Learning Solutions courses align to focus areas of the Neonatal CCRN Exam Content
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY
 ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
Hypoglycemia. Objectives. Glucose Metabolism
 Hypoglycemia Instructor: Janet Mendis, MSN, RNC-NIC, CNS Outline: Janet Mendis, MSN, RNC-NIC, CNS Summer Morgan, MSN, RNC-NIC, CPNP UC San Diego Health System Objectives State the blood glucose level at
Hypoglycemia Instructor: Janet Mendis, MSN, RNC-NIC, CNS Outline: Janet Mendis, MSN, RNC-NIC, CNS Summer Morgan, MSN, RNC-NIC, CPNP UC San Diego Health System Objectives State the blood glucose level at
Status Epilepticus in Children
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on Needed to be resuscitated at birth
 No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
Chapter 13: The Spinal Cord and Spinal Nerves
 Chapter 13: The Spinal Cord and Spinal Nerves Spinal Cord Anatomy Protective structures: Vertebral column and the meninges protect the spinal cord and provide physical stability. a. Dura mater, b. Arachnoid,
Chapter 13: The Spinal Cord and Spinal Nerves Spinal Cord Anatomy Protective structures: Vertebral column and the meninges protect the spinal cord and provide physical stability. a. Dura mater, b. Arachnoid,
Organic Mental Disorders. Organic Mental Disorders. Axes. Damrongsak Bulyalert Department of Internal Medicine
 Organic Mental Disorders Damrongsak Bulyalert Department of Internal Medicine www.metadon.net 1 Organic Mental Disorders In DSM (Diagnostic and Statistical Manual of Mental Disorders), OMD includes Delirium,
Organic Mental Disorders Damrongsak Bulyalert Department of Internal Medicine www.metadon.net 1 Organic Mental Disorders In DSM (Diagnostic and Statistical Manual of Mental Disorders), OMD includes Delirium,
Neonatal Resuscitation. Dustin Coyle, M.D. Anesthesiology
 Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Difficulties at Birth: Long Term Developmental Outcomes
 Difficulties at Birth: Long Term Developmental Outcomes Alan D. Bedrick MD Division of Neonatology and Developmental Biology Department of Pediatrics University of Arizona Tucson, Arizona DISCLOSURE I
Difficulties at Birth: Long Term Developmental Outcomes Alan D. Bedrick MD Division of Neonatology and Developmental Biology Department of Pediatrics University of Arizona Tucson, Arizona DISCLOSURE I
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries. Goes to 6N
 Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Reflexes. Dr. Baizer
 Reflexes Dr. Baizer 1 Learning objectives: reflexes Students will be able to describe: 1. The clinical importance of testing reflexes. 2. The essential components of spinal reflexes. 3.The stretch reflex.
Reflexes Dr. Baizer 1 Learning objectives: reflexes Students will be able to describe: 1. The clinical importance of testing reflexes. 2. The essential components of spinal reflexes. 3.The stretch reflex.
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes
 Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Neurological Determination of Death Adult
 Approved by: Vice President and Chief Medical Officer Neurological Determination of Death Adult Corporate Policy & Procedures Manual Number: VII-B-400 Date Approved June 9, 2015 Next Review (3 years from
Approved by: Vice President and Chief Medical Officer Neurological Determination of Death Adult Corporate Policy & Procedures Manual Number: VII-B-400 Date Approved June 9, 2015 Next Review (3 years from
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level
 Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
Images have been removed from the PowerPoint slides in this handout due to copyright restrictions.
 Seizures Seizures & Status Epilepticus Seizures are episodes of disturbed brain activity that cause changes in attention or behavior. Donna Lindsay, MN RN, CNS-BC, CCRN, CNRN Neuroscience Clinical Nurse
Seizures Seizures & Status Epilepticus Seizures are episodes of disturbed brain activity that cause changes in attention or behavior. Donna Lindsay, MN RN, CNS-BC, CCRN, CNRN Neuroscience Clinical Nurse
Severity of Hypoxic Ischaemic Encephalopathy in Neonates with Birth Asphyxia
 Journal of Rawalpindi Medical College (JRMC); 2007; (): 8-22 Severity of Hypoxic Ischaemic Encephalopathy in Neonates with Birth Asphyxia Rubina Zulfiqar, Samiya Naeemullah Department of Paediatrics, Holy
Journal of Rawalpindi Medical College (JRMC); 2007; (): 8-22 Severity of Hypoxic Ischaemic Encephalopathy in Neonates with Birth Asphyxia Rubina Zulfiqar, Samiya Naeemullah Department of Paediatrics, Holy
Neurodevelopment. Checkpoints in children with congenital heart disease
 Neurodevelopment Checkpoints in children with congenital heart disease Jeehun Lee, M.D., PhD. Pediatric Neurology Samsung Medical Center Sungkyunkwan University, School of Medicine Heart and Brain : Why
Neurodevelopment Checkpoints in children with congenital heart disease Jeehun Lee, M.D., PhD. Pediatric Neurology Samsung Medical Center Sungkyunkwan University, School of Medicine Heart and Brain : Why
Traumatic Brain Injury
 Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy
 Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
Dr. Dafalla Ahmed Babiker Jazan University
 Dr. Dafalla Ahmed Babiker Jazan University change in motor activity and/or behaviour due to abnormal electrical activity in the brain. seizures in children either - provoked by somatic disorders originating
Dr. Dafalla Ahmed Babiker Jazan University change in motor activity and/or behaviour due to abnormal electrical activity in the brain. seizures in children either - provoked by somatic disorders originating
The NeuroNICU From Concept to Clinical Service. MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego
 The NeuroNICU From Concept to Clinical Service MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego What is a NeuroNICU? Collaboration between Neonatology and Neurology Neonatal
The NeuroNICU From Concept to Clinical Service MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego What is a NeuroNICU? Collaboration between Neonatology and Neurology Neonatal
