Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal Prolapse: A Series of 32 Cases
|
|
|
- Harold Gaines
- 5 years ago
- Views:
Transcription
1 ARS Medica Tomitana ; 2(77): /arsm Brătilă V. Elvira 1, Brătilă P.C. 2, Negroiu Andra-Teodora 3 Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal Prolapse: A Series of 32 Cases 1 Saint Pantelimon Clinical Emergency Hospital, Department of Obstetrics and Gynecology, Bucharest, Romania; Carol Davila University of Medicine and Pharmacy, Bucharest, Romania 2 Euroclinic Hospital, Department of Obstetrics and Gynecology, Bucharest, Romania; Carol Davila University of Medicine and Pharmacy, Bucharest, Romania 3 Carol Davila University of Medicine and Pharmacy, Bucharest, Romania ABSTRACT Advanced utero-vaginal prolapse is a frequent condition in the aging female population and several strategies aimed at its treatment have been developed. In order to demonstrate the importance of using the vaginal route in assistance to laparoscopic hysterosacropexy, a retrospective case series was designed, comparing thirty-two patients diagnosed with stage III-IV uterovaginal prolapse according to the POP-Q system. The patients were treated between using one of two methods of hysterosacropexy: vaginally assisted laparoscopic hysterosacropexy (VALHS) in 18 cases and total laparoscopic hysterosacropexy (LHS) in 14 cases. The choice of method was based on the primary mechanism of central compartment prolapse. The total operative time, the time required for mesh fixation at the cervix and sacrum, the cure rate of prolapse and the rate of re-operation for prolapse were statistically analyzed for both LHS and VALHS and compared between these two procedures by Student T-Test. The main outcome parameters were related to the operative method. The total operative time proved to be equal for both procedures, although the time necessary to attach the mesh to the cervical ring was shorter in Petre Cornel Brătilă, MD, PhD Postal address: Dionisie Lupu 74, N074, sector 1, Bucharest, Romania, Telephone number: address: pbratila49@yahoo.com VALHS. Therefore, the combination of the vaginal and laparoscopic routes yields a minimally invasive variant of sacropexy with as short an operative time as possible. The vaginal route offers a safe alternative for suturing the mesh and treating concurrent vaginal wall prolapse, while laparoscopy reduces the inherent risks of open abdominal surgery. Keywords: hysterosacropexy, utero-vaginal prolapse, vaginal assistance Introduction Despite recent advances in urogynecology, the surgical management of advanced uterine prolapse remains challenging. Uterine sacropexy, done by an open or laparoscopic route, represents a valuable alternative for the treatment of utero-vaginal prolapse in women who desire preservation of copulative function and an intact body image. The classical route carries all the risks of open surgery, while the laparoscopic alternative requires advanced surgical skills and is more time-consuming [1], especially when attaching the mesh to the cervical ring or the vaginal walls. The reappearance of prolapse at another compartment after apical correction is also discouraging, as the condition persists despite treating its cause. In this study, we used the cervix 63
2 first, cervix last concept to appreciate the primary mechanism involved in advanced uterovaginal prolapse and planned our operative strategy based on this finding. We hypothesized that these outcomes might be improved without increasing operative time or diminishing the quality of the suture by adding a transvaginal procedure to uterine sacropexy. The operative time and postoperative anatomical and functional outcome of each case were evaluated. Materials and methods This retrospective cohort study includes 32 patients with utero-vaginal prolapse, POP-Q stages three and four, on whom hysterosacropexy was performed after obtaining appropriate informed consent. The two groups of patients were matched according to their general characteristics, as illustrated by Table I. Table I - General and demographic characteristics of the patients LHS (n=14) Age (years) 59 (37-70) ± 10.1 VALHS (n=18) 57 (42-68) ± 8.1 BMI (kg/m2) Median parity 2 2 Vaginal delivery (%) Caesarean delivery (%) Menstrual status (%) Premenopausal Menopausal The patients were treated between at the same hospital and by the same surgical team. They were screened preoperatively for existing cervical and uterine pathology by Papanicolau smear and transvaginal ultrasound. Cervical elongation was identified in six cases by ultrasound measurement (i.e. length of cervix greater than length of uterine body or cervix longer than 4.5 cm). Each patient was examined clinically, focusing on pelvic organ prolapse quantification at maximum strain effort (POP-Q SYSTEM), as well as on urinary and prolapse-specific symptoms. The latter were quantified using the short form of the pelvic floor distress inventory (PFDI- 20). Urinary stress incontinence was identified by the clinical cough test on a full bladder after manually reducing and maintaining the prolapse intravaginally. The patients were divided into two groups based on the level of the initial injury that determined the primary mechanism of prolapse. This level was determined by inviting the patient to strain after reducing the prolapse. If the cervix appeared at the introitus before the vaginal walls (henceforth termed cervix-first type), the mechanism of prolapse involved the first level of suspension [2]. In these cases, restoration of the anatomy solely required the suspension of the vaginal apex by laparoscopic hysterosacropexy (LHS) without the further need to repair the fascial support of the vaginal walls. Conversely, if the cervix appeared after the vaginal walls bulged at the introitus (termed cervix-last type), the initial injury was considered to be located at the second or third level of vaginal suspension. In these cases, restoration of the fascial support of the vaginal walls was necessary, and was done in conjunction with hysterosacropexy by vaginallyassisted laparoscopic hysterosacropexy (VALHS). Follow-up took place at one month, three months and then yearly. Results were quantified anatomically and functionally. The short form of the questionnaire PFDI-20 was used to evaluate the symptoms and the POP-Q system was used to quantify the anatomical results (no prolapse beyond the hymen for the anterior and posterior walls and cervix above the level of the mid vagina: C < TVL / 2). The main outcomes related to operative time (total operative time, time required for mesh fixation to the uterus and total time for mesh fixation) were statistically analyzed for both LHS and VALHS and compared between these two procedures by Student T-Test (α=0.05). The clinical method that assesses the primary mechanism of prolapse (and thus, indirectly, the choice between the two aforementioned surgical 64
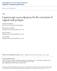
3 procedures) was analyzed according to the cure rate of prolapse and the rate of re-operation. Description of the operative technique of VALHS After proper placement, cleansing and draping of the patient, the operation begins vaginally with the fixation of the mesh to the cervical ring and the restoration of the support of the anterior and posterior vaginal walls. An anterior colpoceliotomy is carried out, anteverting the uterus in Döderlein manner and exposing the broad ligaments at the level of the isthmus (Figure 1). Figure 2 - Tailored Polypropillene Mesh The broad ligaments are perforated bilaterally and the short arms of the mesh are introduced from the posterior to the anterior aspect (Figures 3 & 4) and subsequently fixed posteriorly to the sacrouterine ligaments near their insertion in the uterus and anteriorly to the uterine isthmus by no. 0 polypropillene suture (Ethicon, Johnson&Johnson) (Figure 5). Figure 3 - Posterior Insertion of the Mesh Figure 1 - Anteversion of the Uterus in Döderlein Manner A soft polypropillene mesh with a macroporous structure (pore size > 70 μm) is tailored in tuning fork fashion, with long arms measuring 12 centimeters, short arms measuring six centimeters and a distance of five centimeters between the arms (Figure 2). 65
4 Figure 4 - Completely Inserted Mesh The uterus and mesh are then reintroduced into the peritoneal cavity and the colpoceliotomy is closed with one layer of absorbable sutures, leaving the short arms of the mesh extraperitoneally. The correction of large cystoceles could also be done at this time before closing the colpoceliotomy by a separate vertical incision at the level of the anterior vaginal wall. In this case series, the anterior transobturator mesh with four arms (A.T.O.M.) was routinely used after reducing the cystoceles by in situ vaginoplasty. The correction of large rectoceles was done using the posterior bridge procedure and perineoplasties were also done where necessary. Figure 5 - Anterior Fixation of the Mesh The second (laparoscopic) stage of the procedure begins with the creation of four ports: one transumbilical port (vision), two lateral ports at the level of the iliac spines and and one median port at half the distance between the pubic symphysis and umbilicus. Dissection of the presacral space at level L5-S1 is then carried out, thus creating a peritoneal tunnel to the right side of the sigmoid colon between the first sacral vertebra and the pouch of Douglas. The mesh is passed though the tunnel and fixed to the anterior longitudinal ligament of the spine by two polypropillene no.0 sutures (Ethicon, Johnson & Johnson). In seven cases, the mesh was left unburied inside the peritoneal cavity in order to reduce the laparoscopic operative time and the complications related to the retroperitonealization of the mesh (Figure 6). 66
5 Figure 6 - Intraperitoneal Mesh at 6 Months Postoperatively Of the 32 patients included in this study, eight cases (25%) had had previous surgeries for uterovaginal prolapse: eight anterior colporraphies, four posterior colporrahies and two McCall procedures were noted. Clinical examination revealed third-degree prolapse in 20 cases (62.5%) and fourth-degree prolapse in 12 cases (37.5%). Of these, there were 14 cases (43.7%) of cervix first prolapse and 18 cases (56.2%) of cervix last prolapse. Cervical elongation associated with cervix first prolapse was identified via ultrasound measurement in six cases (33.3%). The 14 cases (43.7%) with cervix first prolapse were treated with LHS, while the 18 cases (56.2%) with cervix last prolapse were treated with VALHS. In most of these cases, an additional vaginal procedure was performed alongside hysterosacropexy (Table III). Results Symptomatic stress urinary incontinence was present in seven patients (21,8%) from both groups three (21.4%) of the LHS group and four (22.2%) of the VALHS group. The symptoms of these patients are detailed in Table II and compared between the two study groups. Table II - Associated symptoms - The associated symptoms were evaluated using the PFDI-20 questionnaire in both groups: laparoscopic hysterosacropexy (LHS) versus vaginally-assisted laparoscopic hysterosacropexy (VALHS) Symptoms (n %) LHS (n=14) VALHS (n=18) Bulge 12 (85.7) 14 (77.7) Pressure 10 (71.4) 12 (66.6) Urinary urgency 2 (14.2) 11 (61.1) Urinary 3 (21.4) 4 (22.2) incontinence Difficult defecation 1 (7.14) 12 (66.6) Table III - Type of hysterosacropexy based on primary mechanism of prolapse and additional surgical procedures LHS ( cervix first prolapse) (n = 14) VALHS ( cervix last prolapse) (n = 18) Stage III (n = 20) 12 8 Stage IV (n = 12) 2 10 Trachelectomy 6 - ATOM - 8 TOT 3 4 PB - 8 PP 5 11 Abbreviations: LHS = laparoscopic hysterosacropexy; VALHS = vaginally assisted laparoscopic hysterosacropexy; ATOM = anterior transobturator mesh; PB = posterior bridge procedure; TOT = transobturator midurethral tape; PP = perineal plasty. The total operative time did not reflect an advantage of VALHS over other procedures, as the additional procedures performed vaginally are more time consuming than those performed with LHS. There was no difference between the total operative time of VALHS versus LHS (Table IV). The vaginal operative time of VALHS can be divided into the time necessary to fix the mesh to the 67
6 uterus and the time necessary to perform associated procedures to correct the fascial support of the vaginal walls and perineal body. The total time for mesh fixation (operative time for the attachment of the mesh to the cervical ring and to the sacrum) was shorter for VALHS than LHS (56.8 ± 10.8 (SD) vs ± 13.2 (SD) minutes, p=0.011). These differences result from the more facile attachment of the mesh by vaginal route. The operative time necessary to attach the mesh to the cervical ring for VALHS was half as long as that of LHS (34.1± 6.5 (SD) vs ± 8.3 (SD), p < 0.01). There was no statistically significant difference between the quantity of blood lost during either LHS or VALHS (115 ± 18.4 (SD) ml vs. 120 ± 20.6 (SD) ml). All patients had a hospital stay of one-two days and there were no intraoperative complications. The median follow-up time was 34 months (range: months). All patients attended their first follow-up visit and subsequent visits at three months and one year. There was no mesh erosion in any group. There was a 100% success rate in terms of uterine and upper vaginal support for both groups, as no patient required further surgery for recurrent uterine prolapse. Three cases (9.3%) treated with LHS developed second-degree cystoceles in the first year after the initial surgery. The cystoceles were treated with the A.T.O.M. procedure. No long-term (12-45 months) intestinal complications were registered in the seven cases where the mesh was left unburied. Table IV - Operative time description for VALHS and LHS Operative time (min) VALHS (mean ± SD, range) LHS(mean ± SD, range) Mean difference p Time for mesh fixation to ± 6.5 (24-45) ± 8.3 (45-73) < 0.01 cervical ring Time for mesh fixation to 26.1 ± 9.1 (15-42) 30.3 ± 13.6 (16-48) the sacrum Total time for mesh fixation ± 10.8 (45-78) ± 13.2 (71-111) Time for associated **44.5 ± 13.4 (25-60) ***18.5 ± 2.12 (17-20) - - procedures Total operative time ± 20.1 (77-138) ± 22.2 (60-144) ** = associated procedures, which included ATOM, PB and TOT *** = associated procedures, which included AC, TOT and PP Abbreviations: LHS = laparoscopic hysterosacropexy; VALHS = vaginally assisted laparoscopic hysterosacropexy; ATOM = anterior transobturator mesh; PB = posterior bridge procedure; TOT = transobturator midurethral tape; AC = anterior colporaphy; PP = perineal plasty. Discussions The clinical aspect of advanced uterovaginal prolapse ( cervix-first vs. cervix-last ) is determined by the level of the pelvic suspension and support system at which the main damage is located [3]. This observation allows the clinician to plan an operative strategy according to the presence or absence of major fascial defects at the second and third suspension levels of the vagina. The cervixfirst type of prolapse can therefore be treated as a central compartment defect, as first- and seconddegree prolapse associated with this type is cured by the simple suspension of the vaginal apex by LHS. However, most of these cases also require a supplementary vaginal procedure for the treatment of urinary incontinence or perineoplasty, allowing the surgeon to fix the mesh at the level of the cervical ring before proceeding with the laparoscopic step of the surgery. This allows the surgeon to have a short operative time even in LHS, where the attachment of the mesh is time-consuming compared to VALHS. In our opinion, hysterectomy for severe uterovaginal prolapse is unnecessary and the omission of this step has several advantages, because, as Bonney noted in 1934, uterine prolapse is not a cause but an effect, and hysterectomy is not a solution to restore 68
7 the normal anatomy of a prolapsed vagina [4]. Leaving the cervical ring in place offers the best support for the suspension of the vaginal apex and the atrophy of the already-weakened uterine ligaments as a consequence of poor vascular supply is thus avoided. Therefore, uterus-sparing surgery shortens the operative time for sacropexy and provides a good suspension for the vaginal apex. In 1999, Godin, Nissole and Donnez performed a colposacropexy for vaginal vault prolapse by transvaginally suturing a polypropillene mesh to the vaginal walls and fixing the mesh to the promontorium with titanium tacks [5]. The anatomical benefits of sacral colpopexy are well-documented in literature [6-8]. The recurrence of apical prolapse after sacropexy is rare, although it predisposes to another form of prolapse in other compartments at different periods of time after the initial surgery. According to the literature, the appearance of additional prolapse is either due to a redistribution of forces (thus weakening the anterior compartment) or to unidentified or unaddressed defects before the operation [9,10]. In this case series, given that cystocele was excluded upon initial evaluation, its postoperative appearance in 9.3% of the patients treated with LHS was probably due to the redistribution of forces in the anterior compartment after posterior suspension of the uterus to the promontory, There are numerous advantages to vaginallyassisted laparoscopic hysteropexy. It is a minimallyinvasive technique which preserves the uterus, allows for an easy suture of the mesh to the cervical ring and reduces blood loss. Furthermore, patients with multicompartment defects benefit from a reduction in operative time while avoiding the complications associated with the laparoscopic dissection of the bladder and rectum. The goals at the outset of this study were to shorten the total operative time and reduce the difficulty of the laparoscopic step. Several studies place the mean time for laparoscopic colposacropexy (LCS) between minutes [11-14]. In this case series, the total operative time for LHS was 93,2 minutes. Although vaginal assistance increases the total operative time when it is necessary to add associated procedures, it shortens the time for mesh attachment compared to an exclusively laparoscopic alternative in patients with multicompartment defects and offers the possibility to solve the defects of other pelvic compartments during the same procedure. Although the rate of complications of sacrocolpopexy is generally estimated at 15% [15], there were no perioperative complications related to bladder or rectal injuries in both patient groups. Open dissection by the vaginal route in VALHS offers the surgeon a more facile approach to the bladder and rectum and bypasses the pitfalls associated with laparoscopic electrosurgery. Mesh erosion or other related complications were not noted. The preservation of the uterus and the attachment of the mesh at the level of the uterine isthmus prevent mesh erosion at the level of the vaginal apex. Conclusions The present study suggests that the combination of the vaginal and laparoscopic routes is useful in obtaining a variant of sacropexy, which is as minimallyinvasive as possible and has a short operative time. The vaginal route offers a safe alternative for suturing the mesh and treating concurrent vaginal wall prolapse, while the laparoscopic route reduces the risks associated with open abdominal surgery. The election of the surgical procedure according to the clinical confirmation of the primary mechanism of advanced utero-vaginal prolapse is a valuable strategy which aims to reduce the rate of prolapse, relapse and the rate of intraoperative complications: VALHS is a multicompartment solution, while LHS is especially suitable for central compartment defects. 69
8 References 1. Pantazis, K., Freeman, R., Thomson, A., Frappell, J. & Bombieri, L. (2008). Results from the LAS Trial, an RCT comparing open abdominal to laparoscopic sacrocolpopexy for the treatment of post hysterectomy vault prolapse. International Urogynecology Journal. 19 Suppl 1, Abstract number Nichols, D.H. & Randal, C.L. (1989). Vaginal surgery. Third edition. Philadelphia, PA: Lippincott Williams&Wilkins 3. Porges, R. (2008). Abnormalities of pelvic support. Glob. libr. women's med. (ISSN: ); DOI /GLOWM Bonney, V. (1934). The principles that should underlie all operations for prolapse. J Obstet Gynaecol Br Emp. 41, Godin, P.A., Nisolle, M., Smets, M., Squifet, J. & and Donnez, J. (1999). Combined vaginal and laparoscopic sacrofxation for genital prolapse using a tacking technique: a series of 45 cases. Gynaecol Endosc. 8, Culligan, P.J., Murphy, M., Blackwell, L., Hammons, G., Graham, C. & Heit, M.H. (2002). Long-term success of abdominal sacral colpopexy using synthetic mesh. Am J Obstet Gynecol. 187, Benson, J.T., Lucente, V. & McClellen, E. (1996). Vaginal versus abdominal reconstructive surgery for the treatment of pelvic support defects: a prospective randomized study with long-term outcome evaluation. Am J Obstet Gynecol. 175, Diwadkar, G.B., Barber, M.D., Feiner, B., Maher, C. & Jelovsek, J.E. (2009). Complication and reoperation rates after apical vaginal prolapse surgical repair: a systematic review. Obstet Gynecol. 113, Cosson, M., Occelli, B., Narducci, F., Ego, A., Querleu, D. & Crepin, G. (2000). Causes of Failure of Abdominal Colposacropexy for the Treatment of Genital and Vaginal Vault Prolapse. J Gynecol Surg. 16, Rooney, K., Kenton, K., Mueller, E.R., FitzGerald, M.P. & Brubaker, L. (2006). Advanced anterior vaginal wall prolapse is highly correlated with apical prolapse. Am J Obstet Gynecol. 195, Paraiso, M.F.R., Walters, M.D., Rackley, R.R., Melek, S. & Hugney, C. (2005). Laparoscopic and open sacral colpopexies: a cohort study. Am J Obstet Gynecol. 192, Hsiao, K.C., Latchamsetty, K., Govier, F.E., Kozlowski, P. & Kobashi, K.C. (2007). Comparison of laparoscopic and abdominal sacrocolpopexy for the treatment of vaginal vault prolapse. J Endourol. 21, Ross, J.W. & Preston, M. (2005). Laparoscopic sacrocolpopexy for severe vaginal vault prolapse: five-year outcome. J Minim Invasive Gynecol. 12, Sarlos, D., Brandner, S., Kots, L., Gygax, N. & Schaer, G. (2008). Laparoscopic sacrocolpopexy for uterine and posthysterectomy prolapse: anatomical results, quality of life and perioperative outcome - a prospective study with 101 cases. Int Urogynecol J Pelvic Floor Dysfunct. 19: Leron, E. & Stanton, S.L. (2001). Sacrohysteropexy with synthetic mesh for the management of uterovaginal prolapse. Brit J Obstet Gynecol. 108,
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
ORIGINAL ARTICLE. Alper Biler 1, I. Egemen Ertas 1, Gokhan Tosun 1, Ismet Hortu 2, Unal Turkay 3, Ozge E. Gultekin 4, Gulfem Igci 3 ABSTRACT
 ORIGINAL ARTICLE Vol. 44 (5): 996-1004, September - October, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0692 Perioperative complications and short-term outcomes of abdominal, laparoscopic, and laparoscopic
ORIGINAL ARTICLE Vol. 44 (5): 996-1004, September - October, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0692 Perioperative complications and short-term outcomes of abdominal, laparoscopic, and laparoscopic
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Surgery for women with apical vaginal prolapse(review)
 Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
Laparoscopic sacrocolpopexy: how low does the mesh go?
 Ultrasound Obstet Gynecol 2017; 49: 404 408 Published online 7 February 2017 in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.15882 Laparoscopic sacrocolpopexy: how low does the mesh
Ultrasound Obstet Gynecol 2017; 49: 404 408 Published online 7 February 2017 in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.15882 Laparoscopic sacrocolpopexy: how low does the mesh
Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes
 DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
The UK National Prolapse Survey: 10 years on
 Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Laparoscopic Uterine Conservation in Uterovaginal Prolapse
 SMGr up Laparoscopic Uterine Conservation in Uterovaginal Prolapse Hasan Cilgin Medicine Faculty of Kafkas University, Kars, Turkey *Corresponding author: Hasan Cilgin, Medicine Faculty of Kafkas University,
SMGr up Laparoscopic Uterine Conservation in Uterovaginal Prolapse Hasan Cilgin Medicine Faculty of Kafkas University, Kars, Turkey *Corresponding author: Hasan Cilgin, Medicine Faculty of Kafkas University,
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic mesh pectopexy for apical prolapse of the uterus or vagina Apical
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic mesh pectopexy for apical prolapse of the uterus or vagina Apical
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
Medium-term follow-up on use of freeze-dried, irradiated donor fascia for sacrocolpopexy and sling procedures
 Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy
 Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Long-term follow-up of sacrocolpopexy mesh implants at two time intervals at least 1 year apart using 4D transperineal ultrasound
 Ultrasound Obstet Gynecol 2017; 49: 398 403 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.15891 Long-term follow-up of sacrocolpopexy mesh implants at two time intervals
Ultrasound Obstet Gynecol 2017; 49: 398 403 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.15891 Long-term follow-up of sacrocolpopexy mesh implants at two time intervals
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of uterine suspension using mesh (including sacrohysteropexy) to repair uterine prolapse
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of uterine suspension using mesh (including sacrohysteropexy) to repair uterine prolapse
SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Effects of uterus-preserving surgical modalities on sexual functions in total prolapsus cases.
 Research Article http://www.alliedacademies.org/research-and-reports-in-gynecology-and-obstetrics Effects of uterus-preserving surgical modalities on sexual functions in total prolapsus cases. Hasan Çılgın*
Research Article http://www.alliedacademies.org/research-and-reports-in-gynecology-and-obstetrics Effects of uterus-preserving surgical modalities on sexual functions in total prolapsus cases. Hasan Çılgın*
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery
 Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Randomized trial of fascia lata and polypropylene mesh for abdominal sacrocolpopexy: 5-year follow-up
 DOI 10.1007/s00192-010-1249-3 ORIGINAL ARTICLE Randomized trial of fascia lata and polypropylene mesh for abdominal sacrocolpopexy: 5-year follow-up Susan B. Tate & Linda Blackwell & Douglas J. Lorenz
DOI 10.1007/s00192-010-1249-3 ORIGINAL ARTICLE Randomized trial of fascia lata and polypropylene mesh for abdominal sacrocolpopexy: 5-year follow-up Susan B. Tate & Linda Blackwell & Douglas J. Lorenz
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
9/24/2015. Pelvic Floor Disorders. Agenda. What is the Pelvic Floor? Pelvic Floor Problems
 Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair uterine prolapse Uterine prolapse
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair uterine prolapse Uterine prolapse
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks
 T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
High success rate and considerable adverse events of pelvic prolapse surgery with Prolift: A single center experience
 Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh
 DOI 10.1007/s00192-013-2265-x ORIGINAL ARTICLE Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh Patrick J. Culligan & Emil Gurshumov & Christa Lewis & Jennifer
DOI 10.1007/s00192-013-2265-x ORIGINAL ARTICLE Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh Patrick J. Culligan & Emil Gurshumov & Christa Lewis & Jennifer
American Journal of Obstetrics and Gynecology
 American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
12/1/13. What are Pelvic Floor Disorders? What is the Pelvic Floor? Facts. Prevalence of Urinary InconOnence. What s New in Pelvic Floor Disorders?
 What are Pelvic Floor Disorders? Urinary Control Problems - InconOnence or leakage of urine Prolapse of pelvic organs - Vagina, bladder, rectum What s New in Pelvic Floor Disorders? Kimberly Kenton MD,
What are Pelvic Floor Disorders? Urinary Control Problems - InconOnence or leakage of urine Prolapse of pelvic organs - Vagina, bladder, rectum What s New in Pelvic Floor Disorders? Kimberly Kenton MD,
An Unusual Case of Prolapse Uterus
 An Unusual Case of Prolapse Uterus Sarita Channawar*, Nagendra Sardesh Pande** Abstract A 12 year old girl, operated earlier for ectopia vesica, pubic diathesis and vaginal at - resia presented to us with
An Unusual Case of Prolapse Uterus Sarita Channawar*, Nagendra Sardesh Pande** Abstract A 12 year old girl, operated earlier for ectopia vesica, pubic diathesis and vaginal at - resia presented to us with
Management of Vaginal Prolapse
 Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications
 Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Female Urology. Young-Suk Lee, Deok Hyun Han, Ji Youl Lee 1, Joon Chul Kim 2, Myung-Soo Choo 3, Kyu-Sung Lee
 www.kjurology.org DOI:1.4111/kju.21.51.3.187 Female Urology Anatomical and Functional Outcomes of Posterior Intravaginal Slingplasty for the Treatment of Vaginal Vault or Uterine Prolapse: A Prospective,
www.kjurology.org DOI:1.4111/kju.21.51.3.187 Female Urology Anatomical and Functional Outcomes of Posterior Intravaginal Slingplasty for the Treatment of Vaginal Vault or Uterine Prolapse: A Prospective,
Three-dimensional transperineal ultrasound for imaging mesh implants following sacrocolpopexy
 Ultrasound Obstet Gynecol 2014; 43: 459 465 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.13303 Three-dimensional transperineal ultrasound for imaging mesh implants
Ultrasound Obstet Gynecol 2014; 43: 459 465 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.13303 Three-dimensional transperineal ultrasound for imaging mesh implants
Scottish Clinical Coding Standards
 Scottish Clinical Coding Standards Number 16 October 2017 Scottish Clinical Coding Standards ICD-10 Sepsis Sepsis is a serious condition which must always be coded when documented in the medical record.
Scottish Clinical Coding Standards Number 16 October 2017 Scottish Clinical Coding Standards ICD-10 Sepsis Sepsis is a serious condition which must always be coded when documented in the medical record.
Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy
 Int Urogynecol J (2011) 22:205 212 DOI 10.1007/s00192-010-1265-3 ORIGINAL ARTICLE Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy Jasmine Tan-Kim & Shawn A. Menefee
Int Urogynecol J (2011) 22:205 212 DOI 10.1007/s00192-010-1265-3 ORIGINAL ARTICLE Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy Jasmine Tan-Kim & Shawn A. Menefee
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Tian-Ni Kuo 1, Ming-Ping Wu 1,2 *
 RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Infracoccygeal sacropexy using mesh for uterine prolapse repair
 Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Laparoscopic pectopexy: initial experience of single center with a new technique for apical prolapse surgery
 ORIGINAL ARTICLE Vol. 43 (5): 903-909, September - October, 2017 doi: 10.1590/S1677-5538.IBJU.2017.0070 Laparoscopic pectopexy: initial experience of single center with a new technique for apical surgery
ORIGINAL ARTICLE Vol. 43 (5): 903-909, September - October, 2017 doi: 10.1590/S1677-5538.IBJU.2017.0070 Laparoscopic pectopexy: initial experience of single center with a new technique for apical surgery
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October :00-12:00
 W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
ARTICLE IN PRESS. FDA approval through the 510(k) process. 2 Therefore, any clinical information
 Evaluation of a transvaginal mesh delivery system for the correction of pelvic organ prolapse: subjective and objective findings at least 1 year after surgery Patrick J. Culligan, MD; Paul M. Littman,
Evaluation of a transvaginal mesh delivery system for the correction of pelvic organ prolapse: subjective and objective findings at least 1 year after surgery Patrick J. Culligan, MD; Paul M. Littman,
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Pelvic Floor. Reimbursement & Coding Guide
 Pelvic Floor Reimbursement & Coding Guide Pelvic Floor Reimbursement and Coding Guide ACell Pelvic Floor Matrix products are biologically-derived devices comprised of porcine Urinary Bladder Matrix (UBM),
Pelvic Floor Reimbursement & Coding Guide Pelvic Floor Reimbursement and Coding Guide ACell Pelvic Floor Matrix products are biologically-derived devices comprised of porcine Urinary Bladder Matrix (UBM),
Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation in Treatment of Vaginal Vault Prolapse
 ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
FDA & Transvaginal Mesh: What Happened? What s Next?
 FDA & Transvaginal Mesh: What Happened? What s Next? Matthew D. Barber, MD MHS Professor & Vice Chair for Clinical Research Obstetrics Gynecology & Women s Health Institute Disclosures I receive no grants,
FDA & Transvaginal Mesh: What Happened? What s Next? Matthew D. Barber, MD MHS Professor & Vice Chair for Clinical Research Obstetrics Gynecology & Women s Health Institute Disclosures I receive no grants,
Laparoscopic Compared With Robotic Sacrocolpopexy for Vaginal Prolapse A Randomized Controlled Trial
 Compared With for Vaginal Prolapse A Randomized Controlled Trial Marie Fidela R. Paraiso, MD, J. Eric Jelovsek, MD, Anna Frick, MD, MPH, Chi Chung Grace Chen, MD, and Matthew D. Barber, MD, MHS OBJECTIVE:
Compared With for Vaginal Prolapse A Randomized Controlled Trial Marie Fidela R. Paraiso, MD, J. Eric Jelovsek, MD, Anna Frick, MD, MPH, Chi Chung Grace Chen, MD, and Matthew D. Barber, MD, MHS OBJECTIVE:
Complications from permanent synthetic mesh
 Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal mesh background of, 84 85 Age as factor in PFDs, 8 Anal plugs in FI management in women, 107 Anterior compartment native tissue
Index Note: Page numbers of article titles are in boldface type. A Abdominal mesh background of, 84 85 Age as factor in PFDs, 8 Anal plugs in FI management in women, 107 Anterior compartment native tissue
Laparoscopic Hysteropexy
 Page 1 of 10 Laparoscopic Hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
Page 1 of 10 Laparoscopic Hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
University College Hospital
 University College Hospital Surgery for prolapse Helping you to make the right choice Urogynaecology and Pelvic Floor Unit, Women s Health Contents Page 1. What type of surgery should I choose? 2 2. What
University College Hospital Surgery for prolapse Helping you to make the right choice Urogynaecology and Pelvic Floor Unit, Women s Health Contents Page 1. What type of surgery should I choose? 2 2. What
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy
 Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Study of correlation between symptoms and signs in women with anterior vaginal wall prolapse
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Bijwe SA et al. Int J Reprod Contracept Obstet Gynecol. 2017 Jul;6(7):3155-3159 www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20172953
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Bijwe SA et al. Int J Reprod Contracept Obstet Gynecol. 2017 Jul;6(7):3155-3159 www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20172953
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after vaginal hysterectomy
 Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Posterior vaginal compartment repairs: Where are the main anatomical defects?
 Int Urogynecol J (2016) 27:741 745 DOI 10.1007/s00192-015-2874-7 ORIGINAL ARTICLE Posterior vaginal compartment repairs: Where are the main anatomical defects? Bernard T. Haylen 1 & Sushen Naidoo 2 & Stephen
Int Urogynecol J (2016) 27:741 745 DOI 10.1007/s00192-015-2874-7 ORIGINAL ARTICLE Posterior vaginal compartment repairs: Where are the main anatomical defects? Bernard T. Haylen 1 & Sushen Naidoo 2 & Stephen
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
With our aging population, the rate of pelvic
 Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
Laparoscopic hysteropexy
 Page 1 of 10 Laparoscopic hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
Page 1 of 10 Laparoscopic hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy
 Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
Comparison of sexual function between sacrocolpopexy and sacrocervicopexy
 Original Article Obstet Gynecol Sci 2017;60(2):207-212 https://doi.org/10.5468/ogs.2017.60.2.207 pissn 2287-8572 eissn 2287-8580 Comparison of sexual function between sacrocolpopexy and sacrocervicopexy
Original Article Obstet Gynecol Sci 2017;60(2):207-212 https://doi.org/10.5468/ogs.2017.60.2.207 pissn 2287-8572 eissn 2287-8580 Comparison of sexual function between sacrocolpopexy and sacrocervicopexy
Management of Urogenital Prolapse of Women in Primary Care. Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner
 Management of Urogenital Prolapse of Women in Primary Care Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner Primary Care Womens Health Forum www.pcwhf.org.uk Useful websites RCN genital
Management of Urogenital Prolapse of Women in Primary Care Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner Primary Care Womens Health Forum www.pcwhf.org.uk Useful websites RCN genital
Original article J Bas Res Med Sci 2015; 2(2): The incidence of recurrent pelvic organ prolapse: A cross sectional study
 The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
JMSCR Volume 03 Issue 03 Page March 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
Guide to Pelvic Floor Multicompartment Scanning
 Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Total vs Subtotal Hysterectomy
 Total vs Subtotal Hysterectomy AN UNSOLVED PROBLEM? G Centini, E Zupi, A Wattiez 153 patient with 15 years of follow-up The Timeline The first successful hysterectomy (Subtotal)! First Laparoscopic Hysterectomy!
Total vs Subtotal Hysterectomy AN UNSOLVED PROBLEM? G Centini, E Zupi, A Wattiez 153 patient with 15 years of follow-up The Timeline The first successful hysterectomy (Subtotal)! First Laparoscopic Hysterectomy!
Reconstructive Pelvic Floor Surgery: Sacrocolpopexy W43, 16 October :00-18:00
 Reconstructive Pelvic Floor Surgery: Sacrocolpopexy W43, 16 October 2012 14:00-18:00 Start End Topic Speakers 14:00 14:30 Introduction, Evidence and Applied Anatomy Salma Kayani 14:30 14:50 Applied Anatomy
Reconstructive Pelvic Floor Surgery: Sacrocolpopexy W43, 16 October 2012 14:00-18:00 Start End Topic Speakers 14:00 14:30 Introduction, Evidence and Applied Anatomy Salma Kayani 14:30 14:50 Applied Anatomy
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of sacrocolpopexy with hysterectomy using mesh to repair uterine prolapse Uterine
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of sacrocolpopexy with hysterectomy using mesh to repair uterine prolapse Uterine
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
