Introduction. Kumar Prashant 1 Devendra Lakhotia. Anil Kumar Mahanta 3 Aakhil Ravoof
|
|
|
- Kory Caldwell
- 5 years ago
- Views:
Transcription
1 J Orthopaed Traumatol (2016) 17: DOI /s ORIGINAL ARTICLE A comparative study of two percutaneous pinning techniques (lateral vs medial lateral) for Gartland type III pediatric supracondylar fracture of the humerus Kumar Prashant 1 Devendra Lakhotia 2 Tulsi Das Bhattacharyya 3 Anil Kumar Mahanta 3 Aakhil Ravoof 4 Received: 28 August 2015 / Accepted: 29 April 2016 / Published online: 16 June 2016 The Author(s) This article is published with open access at Springerlink.com Abstract Background The management of displaced supracondylar fracture of the humerus with closed reduction and percutaneous pin fixation is the most widely accepted method of treatment, but controversy continues regarding the pin fixation techniques. A prospective randomized controlled study was undertaken to compare the stability, functional outcome and iatrogenic ulnar nerve injury between lateral pin fixation and medial lateral pin fixation. Material and method Sixty-two patients with Gartland type III supracondylar fracture of the humerus were randomized into two groups lateral pin fixation (n = 31) and medial lateral pin fixation (n = 31). Primary assessment was performed for major loss of reduction and iatrogenic ulnar nerve injury. Secondary assessment included clinical outcome, elbow range of motion, radiographic measurements, Flynn grade, and complications. Results There were two (6.5 %) iatrogenic ulnar nerve injury cases in the medial lateral entry group and two (6.5 %) cases with mild loss of reduction in the lateral entry group. No major loss of reduction was observed in either of the groups. There was no statistically significant difference in change of Baumann angle, metaphyseal & Kumar Prashant dr.kumarprashant83@gmail.com Trauma Centre, Banaras Hindu University, Varanasi, UP , India Institute of Medical Sciences and Research Center, Jagatpura, Jaipur, India Department of Orthopaedics, Gauhati Medical College and Hospital, Guwahati, Assam, India Mysore Medical College and Research Institute, Mysore, India diaphyseal angle, Flynn grade, carrying angle, and the total elbow range of motion (P \ 0.05) between the two groups. Conclusions Lateral pin fixation offers similar functional and radiological outcome and almost equal mechanical stability compared with medial lateral pinning without the risk of iatrogenic ulnar nerve injury. Level of evidence [OCEBM 2011] Level 2. Keywords Supracondylar fracture Humerus Percutaneous fixation Iatrogenic ulnar nerve injury Randomized controlled study Introduction Supracondylar humerus fractures constitute % of all the fractures around the elbow joint, with a peak incidence between 4 and 7 years of age in children [1]. The main complications associated with supracondylar fractures are malunion, ischemic contracture and neurovascular damage [2, 3]. Of the methods described for the treatment of displaced extension-type supracondylar humeral fractures, closed reduction with percutaneous pin stabilization is the current preferred method of treatment [1]. However, controversy persists between lateral or crossed medial and lateral pin fixation techniques [4]. Two major complications associated with percutaneous pinning are iatrogenic ulnar nerve palsy and loss of reduction, resulting in cubitus varus deformity [5, 6]. The optimal pin configuration that provides adequate stability of the fracture and minimizes the risk of iatrogenic neurovascular injury is still a matter of discussion. The advantage of medial-lateral entry pin fixation is probably increased biomechanical stability, although iatrogenic ulnar nerve injury may result from placement of
2 224 J Orthopaed Traumatol (2016) 17: the medial pin [2, 4, 7]. Conversely, the advantage of lateral entry pin fixation is avoidance of iatrogenic ulnar nerve injury, although the construct may be less stable biomechanically [2, 8 10]. A few studies reported that there is no significant advantage of cross pins in comparison to lateral pins [11, 12]. The aim of this study was to compare the efficacy in terms of stability, functional outcome and iatrogenic ulnar nerve injury between lateral entry pin fixation and medial lateral entry pin fixation of completely displaced (type-iii) extension supracondylar fractures of the humerus in children. The null hypothesis was that there would be no difference between the pin fixation techniques in terms of major loss of reduction or iatrogenic ulnar nerve injury. Materials and methods We conducted a prospective, single-blinded randomized control trial in the Department of Orthopaedics, Gauhati Medical College and Hospital, Guwahati, Assam, India for a period of one year, after obtaining ethical committee approval. Full written informed consent was taken from parents/legal guardian before participating in this study. Inclusion criteria for this study were aged between 3 and 12 years, closed Gartland type III supracondylar humeral fracture [13], duration of injury \4 days, and competent neurological and vascular status of the affected limb. Exclusion criteria were duration of injury [4 days, inability to take part in postoperative rehabilitation, open fractures, medical contraindications to surgery, fracture requiring open reduction or neurovascular exploration, previous ipsilateral elbow fracture, and floating elbow injury. A total of 216 patients with supracondylar humerus fractures were admitted to the orthopedic wards either through the outpatient department or emergency services. Of the 216 patients, 140 were excluded from the present study as they did not fulfill the inclusion criteria. These included compound fractures (10 cases), aged [12 years (12 cases), were not fit for surgery/refused surgery (15 cases), were associated with ipsilateral forearm fractures (6 cases), or were being treated conservatively for Gartland I and II fractures (46 cases). The remaining 76 patients were enrolled in the study. The method of patient selection for lateral entry or medial-lateral entry was random, using a computer-generated randomization table from The seed for the random number generator was obtained from the clock of the local computer and was printed at the bottom of the randomization plan. Fourteen patients were excluded from the final analysis because of lost to follow-up. Our analysis included 62 patients who were followed up for at least 6 months at 1, 3, 6, 14, 18, and 24 weeks and then at 3-month intervals. All the children with suspected supracondylar fractures of the elbow were assessed for vascular and neurological status. Anteroposterior and lateral radiographs were performed. All displaced supracondylar fractures were admitted and the injured elbow was immobilized in an above-elbow splint with the elbow at of flexion and limb elevation. Pulseless viable limbs [absent radial pulse because of complete transaction, intimal tear or compression (temporary compression or reversible spasm) of brachial artery, but hand viable because of good collaterals around elbow] were also included in the study. In all such cases a vascular surgeon was present for the surgery but radial pulsation appeared in all cases after close reduction and pinning. Therefore, brachial artery exploration was not needed for any of our cases. Surgical techniques were standardized in terms of pin location, pin size (weight\20 kg size 1.5 mm;[20 kg size 2 mm), stability on the table and the position of the elbow for pin placement. Surgery was performed by a senior orthopedic surgeon who was well trained in this technique. General anesthesia was used for all patients with the injured upper limb on the side of the table. The injured elbow was placed on the plate of the image intensifier which was adequate for the surgery due to the small size of the elbow. Closed reduction was performed and confirmed by the image intensifier. First, longitudinal traction was applied with the elbow in hyperextension and the forearm in supination (Fig. 1). While the traction was maintained, the medial or lateral displacement was corrected by Fig. 1 Close reduction technique
3 J Orthopaed Traumatol (2016) 17: applying a valgus or varus force at the fracture site. The posterior displacement of the distal fragment was then corrected by applying a force to the posterior aspect while the elbow was gently hyperflexed and the elbow was secured in hyperflexion, and the reduction was confirmed by the image intensifier. The medial pin was placed directly through the apex of the medial epicondyle. The lateral pin was placed at the center of the lateral epicondyle. For the lateral fixation technique, two or three pins were inserted from the lateral aspect of elbow across the lateral cortex to engage the medial cortex keeping the elbow in hyperflexion. Pins were placed either in parallel or divergent configuration with adequate separation at the fracture site. For the medial-lateral fixation technique, first the lateral pin was inserted from lateral cortex to engage the medial cortex keeping the elbow in hyperflexion. The elbow was then extended to\90 and the ulnar nerve rolled back with the opposite thumb and the medial pin was inserted to engage the lateral cortex with the elbow in\90 of flexion. The pin configuration was considered to be acceptable if one pin was placed in the lateral column and another in the central or medial column. If this was not achieved, we realigned the configuration by changing the pin placement. In the coronal plane, the pins were placed at an angle of 30 with the long axis of the humerus. After the pins were placed, the elbow was extended and the carrying angle was measured and compared with that on the nonaffected side. The adequacy and stability of the reduction were checked under image intensification (Figs. 2, 3). The pins were bent to prevent migration and cut off outside the skin to allow removal in the outpatient clinic. A single preoperative parenteral dose of cefuroxime was given at the time of induction and postoperatively, and oral cefuroxmime was given for three days at the time of discharge. Postoperatively, the extremity was placed in a wellpadded posterior splint with the elbow flexed to 90. Any patients with immediate postoperative ulnar nerve deficit were investigated and the pin was placed in another location. For all patients, immediate postoperative radiographs were taken to determine the maintenance of the reduction. The operated limb was elevated and carefully observed at regular intervals for any neurovascular deficit. During follow-up in the outpatient department, clinicalradiological evaluation was performed for maintenance of reduction (at first follow-up) and functional outcome, which included passive range of motion, measurement of carrying angle, Baumann angle, metaphyseal diaphyseal (MD) angle, neurovascular status, superficial and deep infection, and the necessity to re-operate. Clinical evaluation was graded according to carrying angle and elbow range of motion using the criteria of Flynn et al. [14]. Radiographic evaluation was performed by anteroposterior and true lateral view at 1, 3, and 6 weeks and at 3 and Fig. 2 Reduction confirmation in A/P view Fig. 3 Reduction confimation in Lat. view 6 months. In the third week, the pins were removed without anesthesia. At 3- and 6-month follow-up, the children were evaluated for full function, minor limitation of function and major loss of function. The final results were graded as excellent, good, fair and poor, according to the loss of range of motion and loss of carrying angle using the criteria of Flynn et al. Loss of reduction was graded by the loss of Baumann angle using the classification of Gordon et al. [5]. Statistical screening of treatment effects was measured by relative risk reduction, absolute risk reduction with adjustment for a small sample size and confounders in the study. The Fisher exact test and unpaired t test were applied to check for the presence of a significant difference in outcome variable between the two groups. The software InStat version 3.10, 32 bits from GraphPad was used in the statistical analysis. A P value of \0.005 % was considered significant.
4 226 J Orthopaed Traumatol (2016) 17: Result The mean age of the patients was 8.4 years. The mean age in the lateral pin group was 8.25 years and 8.55 years in the medial lateral pin fixation group. In the lateral entry group, 23 were male and 8 were female, whereas in the medial lateral entry group, 22 were male, and 9 were female. The commonest cause of injury was falling while playing (64.51 %), followed by fall from a tree (27.41 %) and fall from a bicycle (8.06 %). Involvement of the left side was 77.4 % and 22.6 % for the right side. Left and right side involvement was and % in the lateral entry group and 70.9 and 29.1 % in the medial-lateral entry group, respectively. At the time of presentation, the radial pulse was weak in %, normal in %, and absent with the viable hand in 8.06 %. In this study, the frequency of posteromedial and posterolateral injuries was % and %, respectively. The frequency in the lateral entry group was 87.1 and 12.9 %, respectively and 74.9 and % in the medial lateral entry group, respectively. The average delay in reporting the injury was 1.79 ± 0.54 days. The average delay between the day of injury and day of the operation was 2.3 days. In the lateral entry group, the average delay was 2.25 days and 2.35 days in the medial-lateral entry group. The average hospital stay was 2.41 days with a minimum and maximum duration of two and four days, respectively. In the lateral entry group, the average hospital stay was 2.32 days and 2.51 days in the medial-lateral entry group. Mean duration of follow-up was weeks with a minimum duration of 24 weeks and maximum duration of 64 weeks. In the lateral entry group, the mean duration of follow-up was weeks and weeks in the medial-lateral group. There were no significant differences (P [ 0.05) between groups with regard to any of these variables (Table 1). Postoperative complications like pin tract infection were found in four cases (three in the lateral entry group and one in the medial-lateral entry group) but all infections were superficial only (Fig. 4). There were two cases of iatrogenic ulnar nerve palsy following medial pinning (6.5 %) in the medial lateral entry group one case had paraesthesia along the ulnar nerve distribution, which subsided spontaneously within three weeks, and the other case had Fig. 4 Pin tract infection both motor and sensory deficits but complete neurological recovery occurred after four months. No patient in either group had a major loss of reduction. There was a mild loss of reduction in two cases and both were in the lateral entry group. Although radiological and clinical union occurred within a similar time period without any residual deformity, the loss of both the range of motion and the carrying angle was greater in these two patients compared to those without loss of reduction. However, there were no significant differences (P [ 0.05) between groups regarding change in the Baumann angle, MD angle, carrying angle, or total elbow motion (Table 1). According to Flynn criteria, the final result was excellent in % and good in % of cases. The result for the medial-lateral entry group was excellent in % and good in % cases, and the result for the lateral entry group was excellent in % and good in % (Table 2). Discussion The ideal treatment for completely displaced (type-iii) extension supracondylar fractures of the humerus in children is closed reduction and percutaneous pin fixation. Table 1 Analysis of carrying angle loss, Baumann angle loss, MD angle loss and range of motion loss at 6-month follow-up Parameters Lateral entry group (mean ± SD) Medial lateral entry group (mean ± SD) P value Loss of carrying angle a 4.12 ± ± Loss of Baumann angle a 4.74 ± ± Loss of MD angle a 2.34 ± ± Loss of range of motion a 8.03 ± ± a Values are given as the mean and SD
5 J Orthopaed Traumatol (2016) 17: Table 2 Comparison of variables Variables Lateral entry (n = 31) Medial-lateral entry (n = 31) P value Sex distribution a Male Female 8 9 Mean age of the patient (years) b 8.25 ± ± Side affected a Left 26 (83 %) 22 (71 %) Right 5 (17 %) 9 (29 %) Hospital stay (days) b 2.32 ± ± Fracture type a PM 25 (87 %) 23 (74 %) PL 6 (13 %) 8 (26 %) Average delay from injury to surgery (days) b 2.25 ± ± Average follow-up (weeks) b ± ± Pin tract infection a 3 (9.6 %) 1 (3.2 %) Iatrogenic ulnar nerve injury a 0 (0 %) 2 (6.5 %) Functional results (Flynn grading) a Excellent 23 (74.19 %) 26 (83.87 %) Good 8 (25.82 %) 5 (16.12 %) PM posteromedial, PL posterolateral, MD metaphysio-diaphyseal a Values are given as the number of patients b Values are given as the mean and SD However, controversy regarding the optimal technique, whether lateral or crossed medial lateral pin fixation is still debatable. According to earlier studies, the advantage of medial lateral entry pin fixation is increased biomechanical stability [7, 15], although iatrogenic ulnar nerve injury may result from placement of the medial pin [4]. Conversely, the advantage of lateral entry pin fixation is avoidance of iatrogenic ulnar nerve injury, although the construct may be less stable biomechanically [10, 11, 16, 17] and failure to provide torsional stability, for which some have suggested adding a third medial pin [11, 18]. A biomechanical study by Zionts et al. [7] demonstrated that crossed pinning is more stable than lateral pinning in rotational testing as well as varus and valgus loading. However, a study by Skaggs et al. [10] demonstrated no clinical difference in stability between crossed and lateral pins. The average loss of the carrying angle, Baumann angle, M D angle and range of motion in the lateral pinning cases in our study may be related to a comparatively less stable construct with two lateral pins compared to crossed medial lateral pins. According to the classification by Gordon et al. [5], the mild loss of reduction in two cases of lateral entry group in our study suggest that lateral entry is biomechanically weaker. Although radiological and clinical union occurred in a similar time period without any residual deformity, the loss of both the range of motion and the carrying angle was greater in these two patients, compared to those without loss of reduction. In a recent analysis of the two techniques by Lee et al. [19], the loss of reduction in the lateral entry group was %. An older study by Kallio et al. found a reduction of 14 % [12], a study by Davis et al. found 29 % [20], while a study by Skaggs et al. found 0 % [10]. The risk of loss of reduction after lateral entry pin fixation can be minimized by following proper pin placement technique, with divergent pins, pins that engage the lateral and central columns, and the use of a third lateral pin if needed. The reported risk of iatrogenic ulnar nerve injury from medial entry pin fixation has been found to range from % [6, 21], and depends on the technique of pin insertion. In a recent trial by Lee et al. [19], the risk of iatrogenic ulnar nerve injury was %. In our study, the risk was 6.5 % (2 cases) in the medial lateral entry group one case showed only paraesthesia along the ulnar nerve distribution, which subsided spontaneously within one week while the other case of nerve palsy with both motor and sensory deficits, showed complete neurological recovery after 4 months. The incidence of ulnar nerve injury in our study was low because of precautions such as inserting the lateral pin first, avoiding hyperflexion of the elbow during medial pin placement and by retracting the
6 228 J Orthopaed Traumatol (2016) 17: nerve more posteriorly by the digital method before medial pin insertion. The risk of iatrogenic ulnar nerve injury can be further reduced with a mini medial incision as reported by Kocher et al. [2] and with extension of the elbow during medial pin placement. Iatrogenic ulnar nerve injuries associated with medial pin fixation resolve after replacement of the medial pin at a new location [21], as occurred in our two cases. In our study, the difference with regard to the loss of range of movement between the two groups was statistically insignificant (P = 0.51), with both groups showing an excellent or good range of movements. The functional outcome following medial and lateral pinning was excellent in 83 % and good in 17 % of cases. There were no poor results, while cases treated with lateral pinning showed 74 % excellent and 26 % good results with no poor results. Similar results were shown by Kocher et al. [2], Mostafavi and Spero [22], and Aronson and Prager [23]. The difference in functional outcome between the two groups in our study was not statistically significant (P = 0.53). One of the strengths of this study was being a prospective randomized clinical trial with the patients randomized at the time of fracture treatment. Furthermore, both the lateral entry and the medial lateral entry techniques were standardized in terms of pin size, pin location, and the position of the elbow for medial pin placement. Full clinical and radiographic evaluation was performed at regular intervals. The major limitation of the study was the small number of cases in each group. A randomized controlled trial (possibly triple blind) involving a large number of patients with long-term follow-up is clearly needed to clarify the differences between the two techniques. Compliance with ethical standards Conflict of interest The authors declare that they have no conflict of interest. (1) All patients provided informed consent prior being included into the study. (2) All procedures involving human participants were in accordance with the 1964 Helsinki Declaration and its later amendments. (3) The study was approved by the Research Ethics Committee. Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( tivecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. References 1. Beaty JH, Kasser JR (1995) Fractures about the elbow. Instr Course Lect 44: Kocher MS, Kasser JR, Waters PM, Bae D, Snyder BD, Hresko MT et al (2007) Lateral entry compared with medial and lateral entry pin fixation for completely displaced supracondylar humeral fractures in children. A randomized clinical trial. J Bone Jt Surg Am 89(4): Ramachandran M, Skaggs DL, Crawford HA, Eastwood DM, Lalonde FD, Vitale MG et al (2008) Delaying treatment of supracondylar fractures in children: has the pendulum swung too far? J Bone Jt Surg Br 90(9): Brauer CA, Lee BM, Bae DS, Waters PM, Kocher MS (2007) A systematic review of medial and lateral entry pinning versus lateral entry pinning for supracondylar fractures of the humerus. J Pediatr Orthop 27(2): Gordon JE, Patton CM, Luhmann SJ, Bassett GS, Schoenecker PL (2001) Fracture stability after pinning of displaced supracondylar distal humerus fractures in children. J Pediatr Orthop 21(3): Kalenderer O, Reisoglu A, Surer L, Agus H (2008) How should one treat iatrogenic ulnar injury after closed reduction and percutaneous pinning of paediatric supracondylar humeral fractures? Injury 39(4): Zionts LE, McKellop HA, Hathaway R (1994) Torsional strength of pin configurations used to fix supracondylar fractures of the humerus in children. J Bone Jt Surg Am 76(2): Shannon FJ, Mohan P, Chacko J, D Souza LG (2004) Dorgan s percutaneous lateral cross-wiring of supracondylar fractures of the humerus in children. J Pediatr Orthop 24(4): Weinberg AM, Castellani C, Arzdorf M, Schneider E, Gasser B, Linke B (2007) Osteosynthesis of supracondylar humerus fractures in children: a biomechanical comparison of four techniques. Clin Biomech (Bristol, Avon) 22(5): Skaggs DL, Cluck MW, Mostofi A, Flynn JM, Kay RM (2004) Lateral-entry pin fixation in the management of supracondylar fractures in children. J Bone Jt Surg Am 86-A(4): Topping RE, Blanco JS, Davis TJ (1995) Clinical evaluation of crossed-pin versus lateral-pin fixation in displaced supracondylar humerus fractures. J Pediatr Orthop 15(4): Kallio PE, Foster BK, Paterson DC (1992) Difficult supracondylar elbow fractures in children: analysis of percutaneous pinning technique. J Pediatr Orthop 12(1): Gartland JJ (1959) Management of supracondylar fractures of the humerus in children. Surg Gynecol Obstet 109(2): Flynn JC, Matthews JG, Benoit RL (1974) Blind pinning of displaced supracondylar fractures of the humerus in children. Sixteen years experience with long-term follow-up. J Bone Jt Surg Am 56(2): Lee SS, Mahar AT, Miesen D, Newton PO (2002) Displaced pediatric supracondylar humerus fractures: biomechanical analysis of percutaneous pinning techniques. J Pediatr Orthop 22(4): Omid R, Choi PD, Skaggs DL (2008) Supracondylar humeral fractures in children. J Bone Jt Surg Am 90(5): Sibinski M, Sharma H, Sherlock DA (2006) Lateral versus crossed wire fixation for displaced extension supracondylar humeral fractures in children. Injury 37(10): Zenios M, Ramachandran M, Milne B, Little D, Smith N (2007) Intraoperative stability testing of lateral-entry pin fixation of pediatric supracondylar humeral fractures. J Pediatr Orthop 27(6): Lee KM, Chung CY, Gwon DK, Sung KH, Kim TW, Choi IH et al (2012) Medial and lateral crossed pinning versus lateral pinning for supracondylar fractures of the humerus in children: decision analysis. J Pediatr Orthop 32(2): Davis RT, Gorczyca JT, Pugh K (2000) Supracondylar humerus fractures in children. Comparison of operative treatment methods. Clin Orthop Relat Res 376:49 55
7 J Orthopaed Traumatol (2016) 17: Rasool MN (1998) Ulnar nerve injury after K-wire fixation of supracondylar humerus fractures in children. J Pediatr Orthop 18(5): Mostafavi HR, Spero C (2000) Crossed pin fixation of displaced supracondylar humerus fractures in children. Clin Orthop Relat Res 376: Aronson DD, Prager BI (1987) Supracondylar fractures of the humerus in children. A modified technique for closed pinning. Clin Orthop Relat Res 219:
Results of lateral pin fixation for the displaced supracondylar fracture of humerus in children
 Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-1,13-17 Original Article Results of lateral pin fixation for the displaced supracondylar fracture of humerus in children H.K. Gupta 1, K.D.
Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-1,13-17 Original Article Results of lateral pin fixation for the displaced supracondylar fracture of humerus in children H.K. Gupta 1, K.D.
Is Closed Manipulative Reduction and Percutaneous Kirschner Wiring of Supracondylar Humeral Fracture in Children as Day-Care Surgery a Safe Procedure?
 Doi:http://dx.doi.org/10.5704/MOJ.1307.006 Is Closed Manipulative Reduction and Percutaneous Kirschner Wiring of Supracondylar Humeral Fracture in Children as Day-Care Surgery a Safe Procedure? Ashok R
Doi:http://dx.doi.org/10.5704/MOJ.1307.006 Is Closed Manipulative Reduction and Percutaneous Kirschner Wiring of Supracondylar Humeral Fracture in Children as Day-Care Surgery a Safe Procedure? Ashok R
A clinical study of closed reduction and percutaneous Kirschner wire fixation of displaced supracondylar fractures of humerus in children
 International Journal of Research in Orthopaedics Asimuddin M et al. Int J Res Orthop. 2017 Mar;3(2):282-286 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20170787
International Journal of Research in Orthopaedics Asimuddin M et al. Int J Res Orthop. 2017 Mar;3(2):282-286 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20170787
Cross pinning versus lateral pinning in type III supracondylar fracture: a retrospective analysis
 International Journal of Research in Orthopaedics http://www.ijoro.org Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20162619 Cross pinning versus lateral pinning in type
International Journal of Research in Orthopaedics http://www.ijoro.org Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20162619 Cross pinning versus lateral pinning in type
Comparative Evaluation of Results of Cross Pin Fixation by Conventional Method with Dorgan s Method in Displaced Supracondylar Fracture in Children
 Original Article DOI: 10.17354/ijss/2015/409 Comparative Evaluation of Results of Cross Pin Fixation by Conventional Method with Dorgan s Method in Displaced Supracondylar Fracture in Children Prasanta
Original Article DOI: 10.17354/ijss/2015/409 Comparative Evaluation of Results of Cross Pin Fixation by Conventional Method with Dorgan s Method in Displaced Supracondylar Fracture in Children Prasanta
Iatrogenic or fracture-related nerve injuries in supracondylar humerus fracture: is treatment necessary for nerve injury?
 European Review for Medical and Pharmacological Sciences Iatrogenic or fracture-related nerve injuries in supracondylar humerus fracture: is treatment necessary for nerve injury? S. GUNER, N. GUVEN, S.
European Review for Medical and Pharmacological Sciences Iatrogenic or fracture-related nerve injuries in supracondylar humerus fracture: is treatment necessary for nerve injury? S. GUNER, N. GUVEN, S.
To Compare the Outcome of Patients with Supracondylar Fractures of Humerus Treated by Cross K-Wires and Lateral Entry K-Wires in Children
 ORIGINAL ARTICLE To Compare the Outcome of Patients with Supracondylar Fractures of Humerus Treated by Cross K-Wires and Lateral Entry K-Wires in Children SHAFI-UR-REHMAN 1, KHIZAR HAYAT 2, ABBAS BAJWA
ORIGINAL ARTICLE To Compare the Outcome of Patients with Supracondylar Fractures of Humerus Treated by Cross K-Wires and Lateral Entry K-Wires in Children SHAFI-UR-REHMAN 1, KHIZAR HAYAT 2, ABBAS BAJWA
Type III Supracondylar Fractures of the Humerus in Children Straight-Arm Treatment
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 11 Number 2 Type III Supracondylar Fractures of the Humerus in Children Straight-Arm Treatment J Gandhi, G Horne Citation J Gandhi, G Horne..
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 11 Number 2 Type III Supracondylar Fractures of the Humerus in Children Straight-Arm Treatment J Gandhi, G Horne Citation J Gandhi, G Horne..
Bioscience Research Print ISSN: Online ISSN:
 Available online freely at www.isisn.org Bioscience Research Print ISSN: 1811-9506 Online ISSN: 2218-3973 Journal by Innovative Scientific Information & Services Network RESEARCH ARTICLE BIOSCIENCE RESEARCH,201815(2):1409-1414
Available online freely at www.isisn.org Bioscience Research Print ISSN: 1811-9506 Online ISSN: 2218-3973 Journal by Innovative Scientific Information & Services Network RESEARCH ARTICLE BIOSCIENCE RESEARCH,201815(2):1409-1414
Treatment of Displaced Supracondylar Fracture of Humerus in Children by Lateral Entry Pinning versus Cross Pinning
 Original Article DOI: 10.17354/ijss/2016/190 Treatment of Displaced Supracondylar Fracture of Humerus in Children by Lateral Entry Pinning versus (Maj Gen) V P Pathania 1, Nishant Dubey 2, Sanjay Gupta
Original Article DOI: 10.17354/ijss/2016/190 Treatment of Displaced Supracondylar Fracture of Humerus in Children by Lateral Entry Pinning versus (Maj Gen) V P Pathania 1, Nishant Dubey 2, Sanjay Gupta
PERCUTANEOUS FIXATION OF DISPLACED SUPRACONDYLAR FRACTURE IN CHILDREN COMPARING LATERAL WITH MEDIAL AND LATERAL PIN
 1 PERCUTANEOUS FIXATION OF DISPLACED SUPRACONDYLAR FRACTURE IN CHILDREN COMPARING LATERAL WITH MEDIAL AND LATERAL PIN A THESIS SUBMITTED TO UNIVERSITY OF SEYCHELLES American Institute of medicine In fulfillment
1 PERCUTANEOUS FIXATION OF DISPLACED SUPRACONDYLAR FRACTURE IN CHILDREN COMPARING LATERAL WITH MEDIAL AND LATERAL PIN A THESIS SUBMITTED TO UNIVERSITY OF SEYCHELLES American Institute of medicine In fulfillment
Percutaneous pinning in displaced supracondylar fracture of humerus in children
 2017; 3(3): 156-160 ISSN: 2395-1958 IJOS 2017; 3(3): 156-160 2017 IJOS www.orthopaper.com Received: 25-05-2017 Accepted: 26-06-2017 Dr. Anvesh Gattu Assistant Professor, Dr. BLS Kumar Babu Associate Professor,
2017; 3(3): 156-160 ISSN: 2395-1958 IJOS 2017; 3(3): 156-160 2017 IJOS www.orthopaper.com Received: 25-05-2017 Accepted: 26-06-2017 Dr. Anvesh Gattu Assistant Professor, Dr. BLS Kumar Babu Associate Professor,
Crossed Versus Lateral Pinning In The Treatment Of Displaced Extension-Type Supracondylar Fractures Of The Humerus: A Prospective Study
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 21 Number 2 Crossed Versus Lateral Pinning In The Treatment Of Displaced Extension-Type Supracondylar Fractures Of The Humerus: A Prospective
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 21 Number 2 Crossed Versus Lateral Pinning In The Treatment Of Displaced Extension-Type Supracondylar Fractures Of The Humerus: A Prospective
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 50/ June 22, 2015 Page 8632
 MANAGEMENT OF DISPLACED SUPRACONDYLAR FRACTURES OF THE HUMERUS IN CHILDREN BY CLOSED REDUCTION AND PERCUTANEOUS PINNING P. L. Srinivas 1, K. Jagadish 2, B. Mahesh 3 HOW TO CITE THIS ARTICLE: P. L. Srinivas,
MANAGEMENT OF DISPLACED SUPRACONDYLAR FRACTURES OF THE HUMERUS IN CHILDREN BY CLOSED REDUCTION AND PERCUTANEOUS PINNING P. L. Srinivas 1, K. Jagadish 2, B. Mahesh 3 HOW TO CITE THIS ARTICLE: P. L. Srinivas,
We report the results of 116 consecutive displaced
 Systematic pinning of displaced extension-type supracondylar fractures of the humerus in children A PROSPECTIVE STUDY OF 116 CONSECUTIVE PATIENTS K. Mazda, C. Boggione, F. Fitoussi, G. F. Penneçot From
Systematic pinning of displaced extension-type supracondylar fractures of the humerus in children A PROSPECTIVE STUDY OF 116 CONSECUTIVE PATIENTS K. Mazda, C. Boggione, F. Fitoussi, G. F. Penneçot From
Surgical Complications
 Surgical Complications Complications are common even with ideal management. Recently, Bashyal performed a retrospective review of 622 patients treated for supracondylar fractures and evaluated the complications
Surgical Complications Complications are common even with ideal management. Recently, Bashyal performed a retrospective review of 622 patients treated for supracondylar fractures and evaluated the complications
Or thopaedic Surger y
 Article Treatment of displaced flexion-type pediatric supracondylar humeral fractures in the prone position Journal of Or thopaedic Surger y Journal of Orthopaedic Surgery Volume: 25(1) 1 6 ª Journal of
Article Treatment of displaced flexion-type pediatric supracondylar humeral fractures in the prone position Journal of Or thopaedic Surger y Journal of Orthopaedic Surgery Volume: 25(1) 1 6 ª Journal of
Surgical Treatment of Supracondylar Humerus Fractures in Children
 519/, p. 519 523 Surgical Treatment of Supracondylar Humerus Fractures in Children Chirurgická léčba suprakondylických zlomenin humeru u dětí K. REISING, H. SCHMAL, M. KOHR, K. KUMINACK, N. P. SÜDKAMP,
519/, p. 519 523 Surgical Treatment of Supracondylar Humerus Fractures in Children Chirurgická léčba suprakondylických zlomenin humeru u dětí K. REISING, H. SCHMAL, M. KOHR, K. KUMINACK, N. P. SÜDKAMP,
Outcomes of Percutaneous Medial-Lateral Cross Pinning of the Pediatric Supracondylar Fractures of the Humerus
 Original Article DOI: 10.17354/ijss/2015/458 Outcomes of Percutaneous Medial-Lateral Cross Pinning of the Pediatric Supracondylar Fractures of the Humerus M Julfiqar 1, Ajay Pant 2, Najmul Huda 3, Mohammed
Original Article DOI: 10.17354/ijss/2015/458 Outcomes of Percutaneous Medial-Lateral Cross Pinning of the Pediatric Supracondylar Fractures of the Humerus M Julfiqar 1, Ajay Pant 2, Najmul Huda 3, Mohammed
--Manuscript Draft-- the Humerus in Children in the Hands of Junior Trainees. Walid A Elnahal, M.Sc Tr & Orth
 Journal of Orthopaedic Trauma Crossed Wires versus Two Lateral Wires in Management of Supracondylar Fracture of the Humerus in Children in the Hands of Junior Trainees --Manuscript Draft-- Manuscript Number:
Journal of Orthopaedic Trauma Crossed Wires versus Two Lateral Wires in Management of Supracondylar Fracture of the Humerus in Children in the Hands of Junior Trainees --Manuscript Draft-- Manuscript Number:
Type-III supracondylar fracture humerus: results 0f open reduction and internal fixation after failed closed reduction
 Original Article Type-III supracondylar fracture humerus: results 0f open reduction and internal fixation after failed closed reduction ABSTARCT Objective Naji ullah Khan, Zahid Askar, Faheem ullah Department
Original Article Type-III supracondylar fracture humerus: results 0f open reduction and internal fixation after failed closed reduction ABSTARCT Objective Naji ullah Khan, Zahid Askar, Faheem ullah Department
A study of biplanar crossed pin construct in the management of displaced pediatric supracondylar humeral fractures
 J Child Orthop (2014) 8:435 441 DOI 10.1007/s11832-014-0607-y ORIGINAL CLINICAL ARTICLE A study of biplanar crossed pin construct in the management of displaced pediatric supracondylar humeral fractures
J Child Orthop (2014) 8:435 441 DOI 10.1007/s11832-014-0607-y ORIGINAL CLINICAL ARTICLE A study of biplanar crossed pin construct in the management of displaced pediatric supracondylar humeral fractures
Functional and radiological outcome after closed reduction and percutaneous pinning versus open reduction and
 Original Article Functional and radiological outcome after closed reduction and percutaneous pinning versus open reduction and children Amin Kumar Shrestha 1, Suresh Uprety 2, Govinda K.C. 2, Sharma Paudel
Original Article Functional and radiological outcome after closed reduction and percutaneous pinning versus open reduction and children Amin Kumar Shrestha 1, Suresh Uprety 2, Govinda K.C. 2, Sharma Paudel
1/19/2018. Winter injuries to the shoulder and elbow. Highgate Private Hospital (Whittington Health NHS Trust)
 Winter injuries to the shoulder and elbow Omar Haddo Consultant Orthopaedic Surgeon, Shoulder, Elbow, Hand & Wrist Specialist MBBS, BmedSci, FRCS(Orth) Highgate Private Hospital (Whittington Health NHS
Winter injuries to the shoulder and elbow Omar Haddo Consultant Orthopaedic Surgeon, Shoulder, Elbow, Hand & Wrist Specialist MBBS, BmedSci, FRCS(Orth) Highgate Private Hospital (Whittington Health NHS
Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini
 Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Study of type-iii supracondylar humerus fractures in children treated by closed reduction with percutaneous crossed pin fixation
 Al Am een J Med Sci 2016; 9(4):241-247 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G Study of type-iii supracondylar humerus fractures in children
Al Am een J Med Sci 2016; 9(4):241-247 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G Study of type-iii supracondylar humerus fractures in children
Consensus and Different Perspectives on Treatment of Supracondylar Fractures of the Humerus in Children
 Original Article Clinics in Orthopedic Surgery 212;4:91-97 http://dx.doi.org/1.455/cios.212.4.1.91 Consensus and Different Perspectives on Treatment of Supracondylar Fractures of the Humerus in Children
Original Article Clinics in Orthopedic Surgery 212;4:91-97 http://dx.doi.org/1.455/cios.212.4.1.91 Consensus and Different Perspectives on Treatment of Supracondylar Fractures of the Humerus in Children
Analysis of displaced supracondylar fractures in children treated with closed reduction and percutaneous pinning
 International Journal of Research in Medical Sciences Sakthivel RN et al. Int J Res Med Sci. 2016 May;4(5):1590-1596 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20161232
International Journal of Research in Medical Sciences Sakthivel RN et al. Int J Res Med Sci. 2016 May;4(5):1590-1596 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20161232
Treatment approaches and outcomes in childhood supracondylar humerus fractures
 European Review for Medical and Pharmacological Sciences Treatment approaches and outcomes in childhood supracondylar humerus fractures B.Y. UÇAR, A. DEMIRTAŞ, D.E. UÇAR* 2012; 16: 936-941 Department of
European Review for Medical and Pharmacological Sciences Treatment approaches and outcomes in childhood supracondylar humerus fractures B.Y. UÇAR, A. DEMIRTAŞ, D.E. UÇAR* 2012; 16: 936-941 Department of
Percutaneous pinning after closed reduction of supracondylar
 ORIGINAL ARTICLE Complications After Pinning of Supracondylar Distal Humerus Fractures Ravi K. Bashyal, MD,*w z Jennifer Y. Chu, MD,* Perry L. Schoenecker, MD,*w z Matthew B. Dobbs, MD,*w z Scott J. Luhmann,
ORIGINAL ARTICLE Complications After Pinning of Supracondylar Distal Humerus Fractures Ravi K. Bashyal, MD,*w z Jennifer Y. Chu, MD,* Perry L. Schoenecker, MD,*w z Matthew B. Dobbs, MD,*w z Scott J. Luhmann,
Pin tract infection of operatively treated supracondylar fractures in children: long-term functional outcomes and anatomical study
 J Child Orthop (2015) 9:295 302 DOI 10.1007/s11832-015-0674-8 ORIGINAL CLINICAL ARTICLE Pin tract infection of operatively treated supracondylar fractures in children: long-term functional outcomes and
J Child Orthop (2015) 9:295 302 DOI 10.1007/s11832-015-0674-8 ORIGINAL CLINICAL ARTICLE Pin tract infection of operatively treated supracondylar fractures in children: long-term functional outcomes and
Safe Cross-Pinning of Pediatric Supracondylar Humerus Fractures With a Flexion-Extension External Rotation Technique AJO DO NOT COPY
 An Original Study Safe Cross-Pinning of Pediatric Supracondylar Humerus Fractures With a Flexion-Extension External Rotation Technique Andrew G. Georgiadis, MD, and Jeffrey J. Settecerri, MD Abstract The
An Original Study Safe Cross-Pinning of Pediatric Supracondylar Humerus Fractures With a Flexion-Extension External Rotation Technique Andrew G. Georgiadis, MD, and Jeffrey J. Settecerri, MD Abstract The
Fractures of the shoulder girdle, elbow and fractures of the humerus. H. Sithebe 2012
 Fractures of the shoulder girdle, elbow and fractures of the humerus H. Sithebe 2012 Fractures of the Clavicle (mid-shaft). Fractures of the clavicle Fractures of the clavicle Treatment- conservative.
Fractures of the shoulder girdle, elbow and fractures of the humerus H. Sithebe 2012 Fractures of the Clavicle (mid-shaft). Fractures of the clavicle Fractures of the clavicle Treatment- conservative.
Gartland type III supracondylar humerus fractures: outcome and complications as related to operative timing and pin configuration
 J Child Orthop (2014) 8:473 477 DOI 10.1007/s11832-014-0624-x ORIGINAL CLINICAL ARTICLE Gartland type III supracondylar humerus fractures: outcome and complications as related to operative timing and pin
J Child Orthop (2014) 8:473 477 DOI 10.1007/s11832-014-0624-x ORIGINAL CLINICAL ARTICLE Gartland type III supracondylar humerus fractures: outcome and complications as related to operative timing and pin
Outcome of surgically treated displaced medial epicondyle fracture of humerus in children: A prospective study
 2017; 3(3): 287-291 ISSN: 2395-1958 IJOS 2017; 3(3): 287-291 2017 IJOS www.orthopaper.com Received: 08-05-2017 Accepted: 10-06-2017 Sahu RL M.S. Orthopaedics, Professor, Dr. Nadeem Ahmad Outcome of surgically
2017; 3(3): 287-291 ISSN: 2395-1958 IJOS 2017; 3(3): 287-291 2017 IJOS www.orthopaper.com Received: 08-05-2017 Accepted: 10-06-2017 Sahu RL M.S. Orthopaedics, Professor, Dr. Nadeem Ahmad Outcome of surgically
Controversies in Pediatric Supracondylar Humerus Fractures. No disclosures for this presentation 10/29/18. Agenda
 Doernbecher Children s Hospital Controversies in Pediatric Supracondylar Humerus PRESENTED BY: Scott Yang MD, Assistant Professor, Pediatric Orthopaedic Surgery Doernbecher Children s Hospital, OHSU No
Doernbecher Children s Hospital Controversies in Pediatric Supracondylar Humerus PRESENTED BY: Scott Yang MD, Assistant Professor, Pediatric Orthopaedic Surgery Doernbecher Children s Hospital, OHSU No
Elevated, straight-arm traction for supracondylar fractures of the humerus in children
 Children s orthopaedics Elevated, straight-arm traction for supracondylar fractures of the humerus in children A. Gadgil, C. Hayhurst, N. Maffulli, J. S. M. Dwyer From University Hospital of North Staffordshire
Children s orthopaedics Elevated, straight-arm traction for supracondylar fractures of the humerus in children A. Gadgil, C. Hayhurst, N. Maffulli, J. S. M. Dwyer From University Hospital of North Staffordshire
THE FLOATING ELBOW IN CHILDREN
 THE FLOATING ELBOW IN CHILDREN SIULTANEOUS SUPRACONDYLAR FRACTURES OF THE HUERUS AND OF THE FOREAR IN THE SAE UPPER LIB PETER A. TEPLETON. H. KERR GRAHA From the Royal Belfast Hospital for Sick Children,
THE FLOATING ELBOW IN CHILDREN SIULTANEOUS SUPRACONDYLAR FRACTURES OF THE HUERUS AND OF THE FOREAR IN THE SAE UPPER LIB PETER A. TEPLETON. H. KERR GRAHA From the Royal Belfast Hospital for Sick Children,
Displaced Supracondylar Humerus Fractures in Children Are They All Identical?
 Doi: http://dx.doi.org/10.5704/moj.1707.017 Displaced Supracondylar Humerus Fractures in Children Are They All Identical? Gera SK, MS Orth, Tan MCH, MBBS, Lim YG, MRCS Ed, Lim KBL, FRCSEd Orth Department
Doi: http://dx.doi.org/10.5704/moj.1707.017 Displaced Supracondylar Humerus Fractures in Children Are They All Identical? Gera SK, MS Orth, Tan MCH, MBBS, Lim YG, MRCS Ed, Lim KBL, FRCSEd Orth Department
Clinical Study Open Reduction and Internal Fixation of Displaced Supracondylar Fracture of Late Presentation in Children: A Preliminary Report
 Advances in Orthopedic Surgery Volume 2016, Article ID 9256540, 6 pages http://dx.doi.org/10.1155/2016/9256540 Clinical Study Open Reduction and Internal Fixation of Displaced Supracondylar Fracture of
Advances in Orthopedic Surgery Volume 2016, Article ID 9256540, 6 pages http://dx.doi.org/10.1155/2016/9256540 Clinical Study Open Reduction and Internal Fixation of Displaced Supracondylar Fracture of
Original Research Article. ISSN (Online) ISSN (Print) DOI: /sajb
 DOI: 10.21276/sajb.2016.4.10.22 Scholars Academic Journal of Biosciences (SAJB) Sch. Acad. J. Biosci., 2016; 4(10B):934-951 Scholars Academic and Scientific Publisher (An International Publisher for Academic
DOI: 10.21276/sajb.2016.4.10.22 Scholars Academic Journal of Biosciences (SAJB) Sch. Acad. J. Biosci., 2016; 4(10B):934-951 Scholars Academic and Scientific Publisher (An International Publisher for Academic
International Journal of Research and Review E-ISSN: ; P-ISSN:
 International Journal of Research and Review www.gkpublication.in E-ISSN: 2349-9788; P-ISSN: 2454-2237 Original Research Article Prospective Observational Study of Management of Supracondylar Fracture
International Journal of Research and Review www.gkpublication.in E-ISSN: 2349-9788; P-ISSN: 2454-2237 Original Research Article Prospective Observational Study of Management of Supracondylar Fracture
Posterolateral dislocation of the elbow with concomitant fracture. of the lateral humeral condyle in a five year old child
 Posterolateral dislocation of the elbow with concomitant fracture of the lateral humeral condyle in a five year old child H Sharma ( ), L Al-badran, S Bhagat, R Sharma, M Naik Department of Trauma and
Posterolateral dislocation of the elbow with concomitant fracture of the lateral humeral condyle in a five year old child H Sharma ( ), L Al-badran, S Bhagat, R Sharma, M Naik Department of Trauma and
Comparative study between two patterns of percutaneous K- wire fixation of supracondylar fracture of the humerus in children
 Research Article Comparative study between two patterns of percutaneous K- wire fixation of supracondylar fracture of the humerus in children Mushtaq Talib Hussein F.I.B.M.S,C.A.B.O Date Submitted: 5/1/2016
Research Article Comparative study between two patterns of percutaneous K- wire fixation of supracondylar fracture of the humerus in children Mushtaq Talib Hussein F.I.B.M.S,C.A.B.O Date Submitted: 5/1/2016
THE EXPERIENCE OF A SPECIALIST REFERRAL CENTRE
 Trauma Clinical outcome of nerve injuries associated with supracondylar fractures of the humerus in children THE EXPERIENCE OF A SPECIALIST REFERRAL CENTRE M. Ramachandran, R. Birch, D. M. Eastwood From
Trauma Clinical outcome of nerve injuries associated with supracondylar fractures of the humerus in children THE EXPERIENCE OF A SPECIALIST REFERRAL CENTRE M. Ramachandran, R. Birch, D. M. Eastwood From
Prospective study of cubitus varus deformity, its etiopathology, clinical study and treatment
 International Journal of Research in Medical Sciences Dudhekar U. Int J Res Med Sci. 2017 Jan;5(1):201-205 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20164549
International Journal of Research in Medical Sciences Dudhekar U. Int J Res Med Sci. 2017 Jan;5(1):201-205 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20164549
Distance of translation as a predictor of failure of fixation in paediatric supracondylar fractures
 TRAUMA AND ORTHOPAEDIC SURGERY Ann R Coll Surg Engl 2017; 99: 524 528 doi 10.1308/rcsann.2017.0040 Distance of translation as a predictor of failure of fixation in paediatric supracondylar fractures P
TRAUMA AND ORTHOPAEDIC SURGERY Ann R Coll Surg Engl 2017; 99: 524 528 doi 10.1308/rcsann.2017.0040 Distance of translation as a predictor of failure of fixation in paediatric supracondylar fractures P
1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint
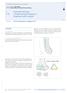 1 Executive Editor: Chris Colton Authors: Mariusz Bonczar, Daniel Rikli, David Ring 1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint Indication All 13-A type fractures, excluding
1 Executive Editor: Chris Colton Authors: Mariusz Bonczar, Daniel Rikli, David Ring 1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint Indication All 13-A type fractures, excluding
SUPRACONDYLAR HUMERUS FRACTURE FIXATION IN CHILDREN WITH CROSS K-WIRES VS TWO LATERAL K-WIRES
 SUPRACONDYLAR HUMERUS FRACTURE FIXATION IN CHILDREN WITH CROSS K-WIRES VS TWO LATERAL K-WIRES Syed Dil Bagh Ali Shah 1, Syeda um-e-habiba Gillani 2, Sameer Khan Kabir 3, Prof. Zaffar Durrani 4 ABSTRACT
SUPRACONDYLAR HUMERUS FRACTURE FIXATION IN CHILDREN WITH CROSS K-WIRES VS TWO LATERAL K-WIRES Syed Dil Bagh Ali Shah 1, Syeda um-e-habiba Gillani 2, Sameer Khan Kabir 3, Prof. Zaffar Durrani 4 ABSTRACT
Elbow fractures account for approximately 5% to
 Common Pediatric Elbow Fractures Erin S. Hart Allison Turner Maurice Albright Brian E. Grottkau Fractures of the elbow are a very common injury in children. The most common mechanism of injury is a fall
Common Pediatric Elbow Fractures Erin S. Hart Allison Turner Maurice Albright Brian E. Grottkau Fractures of the elbow are a very common injury in children. The most common mechanism of injury is a fall
Tuomilehto, N
 https://helda.helsinki.fi Postponing surgery of paediatric supracondylar humerus fractures to office hours increases consultant attendance in operations and saves operative room time Tuomilehto, N. 2018-06
https://helda.helsinki.fi Postponing surgery of paediatric supracondylar humerus fractures to office hours increases consultant attendance in operations and saves operative room time Tuomilehto, N. 2018-06
STUDY OF RESULTS OF PERCUTANEOUS PARALLEL LATERAL AND CROSS PINNING IN TYPE III SUPRACONDYLAR FRACTURES OF HUMERUS IN CHILDREN. Dr.K.
 STUDY OF RESULTS OF PERCUTANEOUS PARALLEL LATERAL AND CROSS PINNING IN TYPE III SUPRACONDYLAR FRACTURES OF HUMERUS IN CHILDREN BY Dr.K.SARAVANAN A Dissertation submitted to the BOOLEAN EDUCATION In partial
STUDY OF RESULTS OF PERCUTANEOUS PARALLEL LATERAL AND CROSS PINNING IN TYPE III SUPRACONDYLAR FRACTURES OF HUMERUS IN CHILDREN BY Dr.K.SARAVANAN A Dissertation submitted to the BOOLEAN EDUCATION In partial
Posteromedial approach to the distal humerus for fracture fixation
 Acta Orthop. Belg., 2006, 72, 395-399 ORIGINAL STUDY Posteromedial approach to the distal humerus for fracture fixation Cédric LAPORTE, Maurice THIONGO, Dominique JEGOU From the General Hospital of Meaux,
Acta Orthop. Belg., 2006, 72, 395-399 ORIGINAL STUDY Posteromedial approach to the distal humerus for fracture fixation Cédric LAPORTE, Maurice THIONGO, Dominique JEGOU From the General Hospital of Meaux,
SUPRACONDYLAR HUMERUS FRACTURE (SCH FX)
 SUPRACONDYLAR HUMERUS FRACTURE (SCH FX) ALGORITHM. Supracondylar Humerus Fracture Page 1 of 12 Algorithm: Vascular Injury 5 Yes, well perfused Supracondylar Humerus Fracture Pulseless (undopplerable) Consult
SUPRACONDYLAR HUMERUS FRACTURE (SCH FX) ALGORITHM. Supracondylar Humerus Fracture Page 1 of 12 Algorithm: Vascular Injury 5 Yes, well perfused Supracondylar Humerus Fracture Pulseless (undopplerable) Consult
Anterior Displacement of Ulnar Nerve at the Elbow in Children Based on Ultrasonography
 108472 NV-OA8 pg29-33.qxd 11/05/2007 05:05 PM Page 29 (Black plate) Anterior Displacement of Ulnar Nerve at the Elbow in Children Based on Ultrasonography H Shamsul, MS (Ortho)*, A Saw, FRCS*, G John,
108472 NV-OA8 pg29-33.qxd 11/05/2007 05:05 PM Page 29 (Black plate) Anterior Displacement of Ulnar Nerve at the Elbow in Children Based on Ultrasonography H Shamsul, MS (Ortho)*, A Saw, FRCS*, G John,
(Un)importance of physical therapy in treatment of displaced supracondylar humerus fractures in children
 Acta Orthop. Belg., 2015, 81, 368-374 ORIGINAL STUDY (Un)importance of physical therapy in treatment of displaced supracondylar humerus fractures in children Sinisa Ducic, Marko Bumbasirevic, Vladimir
Acta Orthop. Belg., 2015, 81, 368-374 ORIGINAL STUDY (Un)importance of physical therapy in treatment of displaced supracondylar humerus fractures in children Sinisa Ducic, Marko Bumbasirevic, Vladimir
Proximal radioulnar translocation associated with elbow dislocation and radial neck fracture in child: a case report and review of literature
 DOI 10.1007/s00402-013-1820-8 TRAUMA SURGERY Proximal radioulnar translocation associated with elbow dislocation and radial neck fracture in child: a case report and review of literature Hong Kee Yoon
DOI 10.1007/s00402-013-1820-8 TRAUMA SURGERY Proximal radioulnar translocation associated with elbow dislocation and radial neck fracture in child: a case report and review of literature Hong Kee Yoon
PEDIATRIC ELBOW FRACTURES.
 PEDIATRIC ELBOW FRACTURES www.fisiokinesiterapia.biz INCIDENCE SECOND MOST COMMON PEDIATRIC INJURY OSSIFICATION 1. CAPITELLUM (6 mo. - 2 yrs.) 2. MED. EPICONDYLE (5-9 yrs.) 3. TROCHLEA (7-13 yrs.) 4. LAT.
PEDIATRIC ELBOW FRACTURES www.fisiokinesiterapia.biz INCIDENCE SECOND MOST COMMON PEDIATRIC INJURY OSSIFICATION 1. CAPITELLUM (6 mo. - 2 yrs.) 2. MED. EPICONDYLE (5-9 yrs.) 3. TROCHLEA (7-13 yrs.) 4. LAT.
ORIGINAL ARTICLE. Abdulkadir Dost, 1 Baris Yilmaz, 2 Baran Kömür, 3 Serhat Mutlu, 4 Harun Mutlu, 5 Korhan Özkan, 6 Abdullah Eren 7
 393 ORIGINAL ARTICLE Middle and long term radiologic and functional results of childhood supracondylar humeral fractures operated in first 24 hours with limited medial approach Abdulkadir Dost, 1 Baris
393 ORIGINAL ARTICLE Middle and long term radiologic and functional results of childhood supracondylar humeral fractures operated in first 24 hours with limited medial approach Abdulkadir Dost, 1 Baris
SUPRACONDYLAR HUMERUS FRACTURE (SCH FX)
 SUPRACONDYLAR HUMERUS FRACTURE (SCH FX) ALGORITHM. Supracondylar Humerus Fracture Page 1 of 12 Algorithm: Vascular Injury 5 Supracondylar Humerus Fracture Pulseless (undopplerable) Consult Orthopedics
SUPRACONDYLAR HUMERUS FRACTURE (SCH FX) ALGORITHM. Supracondylar Humerus Fracture Page 1 of 12 Algorithm: Vascular Injury 5 Supracondylar Humerus Fracture Pulseless (undopplerable) Consult Orthopedics
Upper Extremity Injury Management. Jonathan Pirie MD, Med, FRCPC, FAAP
 Upper Extremity Injury Management Jonathan Pirie MD, Med, FRCPC, FAAP Learning Objectives At the end of this session, you will be able to manage common fractures of the: 1. Humerus 2. Elbow 3. Forearm
Upper Extremity Injury Management Jonathan Pirie MD, Med, FRCPC, FAAP Learning Objectives At the end of this session, you will be able to manage common fractures of the: 1. Humerus 2. Elbow 3. Forearm
Open reduction; plate fixation 1 Principles
 Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
ORIGINAL ARTICLE ABSTRACT INTRODUCTION MIAN MUHAMMAD AZHAR
 ORIGINAL ARTICLE Close Reduction and Percutaneous Pin Fixation in Displaced (Type-III) Supracondylar Fractures of Humerus in Children Surgical Outcomes and Comparison with other study MIAN MUHAMMAD AZHAR
ORIGINAL ARTICLE Close Reduction and Percutaneous Pin Fixation in Displaced (Type-III) Supracondylar Fractures of Humerus in Children Surgical Outcomes and Comparison with other study MIAN MUHAMMAD AZHAR
E ORIGINAL ARTICLE Low extra-articular (transcondylar) fractures of the distal humerus
 Shoulder & Elbow. ISSN 1758-5732 E ORIGINAL ARTICLE Low extra-articular (transcondylar) fractures of the distal humerus Alexander A. Weening, Kim M. Brouwer, Margaritha Adams & David Ring Orthopaedic Hand
Shoulder & Elbow. ISSN 1758-5732 E ORIGINAL ARTICLE Low extra-articular (transcondylar) fractures of the distal humerus Alexander A. Weening, Kim M. Brouwer, Margaritha Adams & David Ring Orthopaedic Hand
Paediatric fractures in the Emergency Department. October 2012
 Paediatric fractures in the Emergency Department October 2012 Victorian Paediatric Orthopaedic Network What this presentation covers Paediatric bone anatomy Buckle injury of distal radius Supracondylar
Paediatric fractures in the Emergency Department October 2012 Victorian Paediatric Orthopaedic Network What this presentation covers Paediatric bone anatomy Buckle injury of distal radius Supracondylar
Case Report Successful Closed Reduction of a Lateral Elbow Dislocation
 Case Reports in Orthopedics Volume 2016, Article ID 5934281, 5 pages http://dx.doi.org/10.1155/2016/5934281 Case Report Successful Closed Reduction of a Lateral Elbow Dislocation Kenya Watanabe, Takuma
Case Reports in Orthopedics Volume 2016, Article ID 5934281, 5 pages http://dx.doi.org/10.1155/2016/5934281 Case Report Successful Closed Reduction of a Lateral Elbow Dislocation Kenya Watanabe, Takuma
Orthopedics in Motion Tristan Hartzell, MD January 27, 2016
 Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Case Report Medial Condyle Fracture (Kilfoyle Type III) of the Distal Humerus with Transient Fishtail Deformity after Surgery
 Hindawi Case Reports in Orthopedics Volume 2017, Article ID 9053949, 4 pages https://doi.org/10.1155/2017/9053949 Case Report Medial Condyle Fracture (Kilfoyle Type III) of the Distal Humerus with Transient
Hindawi Case Reports in Orthopedics Volume 2017, Article ID 9053949, 4 pages https://doi.org/10.1155/2017/9053949 Case Report Medial Condyle Fracture (Kilfoyle Type III) of the Distal Humerus with Transient
Outcome of displaced supracondylar fractures of humerus in children treated by closed reduction and percutaneous K-wire fixation
 Original article: Outcome of displaced supracondylar fractures of humerus in children treated by closed reduction and percutaneous K-wire fixation Dr. Prashanth P, Dr. Srinivasan S, Dr. Arunprasath C,
Original article: Outcome of displaced supracondylar fractures of humerus in children treated by closed reduction and percutaneous K-wire fixation Dr. Prashanth P, Dr. Srinivasan S, Dr. Arunprasath C,
Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture Dislocation of the Elbow in an Adult
 Hindawi Case Reports in Orthopedics Volume 2018, Article ID 5401634, 6 pages https://doi.org/10.1155/2018/5401634 Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture
Hindawi Case Reports in Orthopedics Volume 2018, Article ID 5401634, 6 pages https://doi.org/10.1155/2018/5401634 Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture
Abd Ali Muhsin FICMS.
 Comparative study between close reductions versus close reduction with K-Wire fixation in completely dorsally displaced distal radial metaphyseal fracture, in children and adolescent. Abd Ali Muhsin FICMS.
Comparative study between close reductions versus close reduction with K-Wire fixation in completely dorsally displaced distal radial metaphyseal fracture, in children and adolescent. Abd Ali Muhsin FICMS.
FLOATING ELBOW IN CHILDREN: A DESCRIPTIVE STUDY OF 31 CASES ATTENDED IN A REFERENCE CENTER FOR PEDIATRIC TRAUMA
 original article FLOATING ELBOW IN CHILDREN: A DESCRIPTIVE STUDY OF 31 CASES ATTENDED IN A REFERENCE CENTER FOR PEDIATRIC TRAUMA Dorotea Starling Malheiros 1, Gustavo Henrique Silva Bárbara 2, Leandro
original article FLOATING ELBOW IN CHILDREN: A DESCRIPTIVE STUDY OF 31 CASES ATTENDED IN A REFERENCE CENTER FOR PEDIATRIC TRAUMA Dorotea Starling Malheiros 1, Gustavo Henrique Silva Bárbara 2, Leandro
Sports Medicine Unit 16 Elbow
 Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Recurrent subluxation or dislocation after surgical
 )263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
)263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
Comparison of Below The Elbow Cast with Above The Elbow Cast in Treating Distal Third Forearm Fractures in Children
 ORIGINAL ARTICLE ABSTRACT Comparison of Below The Elbow Cast with Above The Elbow Cast in Treating Distal Third Forearm Fractures in Children Noor Rahman, Wasim Anwar, Malik Javed Iqbal, Israr Ahmad, Mohammad
ORIGINAL ARTICLE ABSTRACT Comparison of Below The Elbow Cast with Above The Elbow Cast in Treating Distal Third Forearm Fractures in Children Noor Rahman, Wasim Anwar, Malik Javed Iqbal, Israr Ahmad, Mohammad
DISPLACED SUPRACONDYLAR FRACTURES OF HUMERUS IN CHILDREN TREATED WITH OPEN REDUCTION AND CROSS K-WIRE FIXATION
 ORIGINAL ARTICLE DISPLACED SUPRACONDYLAR FRACTURES OF HUMERUS IN CHILDREN TREATED WITH OPEN REDUCTION AND CROSS K-WIRE FIXATION Shakir Hussain, Malik Faiz Ahmad, Khalid, Waqas Orthopaedics Unit District
ORIGINAL ARTICLE DISPLACED SUPRACONDYLAR FRACTURES OF HUMERUS IN CHILDREN TREATED WITH OPEN REDUCTION AND CROSS K-WIRE FIXATION Shakir Hussain, Malik Faiz Ahmad, Khalid, Waqas Orthopaedics Unit District
The Outcome of Supracondyler Fractures of Elbow Joint Treated during Different Periods of Time by Different Techniques in District Population
 ORIGINAL ARTICLE The Outcome of Supracondyler Fractures of Elbow Joint Treated during Different Periods of Time by Different Techniques in District Population MIAN MUHAMMAD AZHAR ABSTRACT Objective: To
ORIGINAL ARTICLE The Outcome of Supracondyler Fractures of Elbow Joint Treated during Different Periods of Time by Different Techniques in District Population MIAN MUHAMMAD AZHAR ABSTRACT Objective: To
Biomechanical analysis between Orthofix external fixator and different K-wire configurations for pediatric supracondylar humerus fractures
 Li et al. Journal of Orthopaedic Surgery and Research (2018) 13:188 https://doi.org/10.1186/s13018-018-0893-z RESEARCH ARTICLE Biomechanical analysis between Orthofix external fixator and different K-wire
Li et al. Journal of Orthopaedic Surgery and Research (2018) 13:188 https://doi.org/10.1186/s13018-018-0893-z RESEARCH ARTICLE Biomechanical analysis between Orthofix external fixator and different K-wire
Follow-up and evaluation
 Original Article Comparison of Medial and Posterior Surgical Approaches in Pediatric Supracondylar Humerus Fractures E Şahin, S Zehir 1, S Sipahioglu 2 Department of Orthopedics and Traumatology, Faculty
Original Article Comparison of Medial and Posterior Surgical Approaches in Pediatric Supracondylar Humerus Fractures E Şahin, S Zehir 1, S Sipahioglu 2 Department of Orthopedics and Traumatology, Faculty
CiSE. New Fixation Method Using Two Crossing Screws and Locking Plate for Cubitus Varus Deformity in Young Adult Elbow: Case Report CASE REPORT
 SE REPORT linics in Shoulder and Elbow Vol. 19, No. 1, March, 2016 http://dx.doi.org/10.5397/cise.2016.19.1.43 ise linics in Shoulder and Elbow New Fixation Method Using Two rossing Screws and Locking
SE REPORT linics in Shoulder and Elbow Vol. 19, No. 1, March, 2016 http://dx.doi.org/10.5397/cise.2016.19.1.43 ise linics in Shoulder and Elbow New Fixation Method Using Two rossing Screws and Locking
Common Limb Fractures. Mr Sheraz Malik MB BS MRCS Instructor Mr Paul Ofori-Atta Mb ChB FRCS President Motc Life UK April 2009
 Common Limb Fractures Mr Sheraz Malik MB BS MRCS Instructor Mr Paul Ofori-Atta Mb ChB FRCS President Motc Life UK April 2009 Objectives To be able to describe all characteristics of a fracture Describe
Common Limb Fractures Mr Sheraz Malik MB BS MRCS Instructor Mr Paul Ofori-Atta Mb ChB FRCS President Motc Life UK April 2009 Objectives To be able to describe all characteristics of a fracture Describe
Compared outcomes after percutaneous pinning versus open reduction in paediatric supracondylar elbow fractures
 Orthopaedics & Traumatology: Surgery & Research (2012) 98, 645 651 Available online at www.sciencedirect.com ORIGINAL ARTICLE Compared outcomes after percutaneous pinning versus open reduction in paediatric
Orthopaedics & Traumatology: Surgery & Research (2012) 98, 645 651 Available online at www.sciencedirect.com ORIGINAL ARTICLE Compared outcomes after percutaneous pinning versus open reduction in paediatric
Elbow, forearm injuries. K. Fekete
 Elbow, forearm injuries K. Fekete 1. Outline: Fractures of the elbow Dislocation of the elbow Fractures of the forearm Special injuries 2. ANATOMY 3. Lennard Funk Anatomical reminder Three joints: Humero-ulnar
Elbow, forearm injuries K. Fekete 1. Outline: Fractures of the elbow Dislocation of the elbow Fractures of the forearm Special injuries 2. ANATOMY 3. Lennard Funk Anatomical reminder Three joints: Humero-ulnar
TENS in paediatrics both bone forearm fractures
 TENS in paediatrics both bone forearm fractures Dr.Ajit Singh, Associate Professor, Department of orthopedics, IMS, BHU, Varanasi. Abstract Context: Diaphyseal fractures of the radius and ulna are common
TENS in paediatrics both bone forearm fractures Dr.Ajit Singh, Associate Professor, Department of orthopedics, IMS, BHU, Varanasi. Abstract Context: Diaphyseal fractures of the radius and ulna are common
The study of distal ¼ diaphyseal extra articular fractures of humerus treated with antegrade intramedullary interlocking nailing
 2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
Fractures of the Radial and Ulnar Shafts In the Pediatric Patient
 Fractures of the Radial and Ulnar Shafts In the Pediatric Patient Kaye E Wilkins DVM, MD Professor of Orthopedics and Pediatrics Departments of Orthopedics and Pediatrics University of Texas Health Science
Fractures of the Radial and Ulnar Shafts In the Pediatric Patient Kaye E Wilkins DVM, MD Professor of Orthopedics and Pediatrics Departments of Orthopedics and Pediatrics University of Texas Health Science
Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4)
 AO Manual of ESIN in children s fractures Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4) Title AO Manual of ESIN in children Subtitle Elastic stable intramedullary nailing (ESIN) Author
AO Manual of ESIN in children s fractures Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4) Title AO Manual of ESIN in children Subtitle Elastic stable intramedullary nailing (ESIN) Author
THE NANCY NAIL. The End Caps ADVANTAGES OF NANCY NAIL
 NANCY NAIL THE NANCY NAIL Nancy nails are manufactured from a specific titanyum alloy with proprietary surface treatment, which provides increased fatigue resistance. Six nail diameters (1.5 mm 2.0 mm
NANCY NAIL THE NANCY NAIL Nancy nails are manufactured from a specific titanyum alloy with proprietary surface treatment, which provides increased fatigue resistance. Six nail diameters (1.5 mm 2.0 mm
Closed reduction and internal fixation of fractures of the shaft of the femur by the Titanium Elastic Nailing System in children.
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 1 Closed reduction and internal fixation of fractures of the shaft of the femur by the Titanium Elastic Nailing System in children.
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 1 Closed reduction and internal fixation of fractures of the shaft of the femur by the Titanium Elastic Nailing System in children.
A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report
 CASE REPORT 41 OPEN ACCESS A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report Aysha Rajeev, John Harrison ABSTRACT Introduction: The phalangeal
CASE REPORT 41 OPEN ACCESS A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report Aysha Rajeev, John Harrison ABSTRACT Introduction: The phalangeal
Pediatric Tibia Fractures Key Points. Christopher Iobst, MD
 Pediatric Tibia Fractures Key Points Christopher Iobst, MD Goals Bone to heal Return to full weight bearing Acceptable alignment rule of 10s 10 degrees of varus 8 degrees of valgus 12 degrees of procurvatum
Pediatric Tibia Fractures Key Points Christopher Iobst, MD Goals Bone to heal Return to full weight bearing Acceptable alignment rule of 10s 10 degrees of varus 8 degrees of valgus 12 degrees of procurvatum
HUMERAL SHAFT FRACTURES: ORIF, IMN, NONOP What to do?
 HUMERAL SHAFT FRACTURES: ORIF, IMN, NONOP What to do? TRAUMA 101 2018 FRACTURE CARE FOR THE COMMUNITY ORTHOPEDIST William W. Cross III, MD Assistant Professor Division of Orthopaedic Trauma Chair, Division
HUMERAL SHAFT FRACTURES: ORIF, IMN, NONOP What to do? TRAUMA 101 2018 FRACTURE CARE FOR THE COMMUNITY ORTHOPEDIST William W. Cross III, MD Assistant Professor Division of Orthopaedic Trauma Chair, Division
Surgical Management of Paediatric Humerus Fractures with Tens - A Retrospective Analysis.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 11 Ver. IX (Nov. 2017), PP 82-86 www.iosrjournals.org Surgical Management of Paediatric Humerus
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 11 Ver. IX (Nov. 2017), PP 82-86 www.iosrjournals.org Surgical Management of Paediatric Humerus
Other Upper Extremity Trauma. Inje University Sanggye Paik Hospital Yong-Woon Shin
 Other Upper Extremity Trauma Inje University Sanggye Paik Hospital Yong-Woon Shin Forearm Fractures Forearm fractures - the most common orthopaedic injuries in children - 30-50% of all pediatric fractures
Other Upper Extremity Trauma Inje University Sanggye Paik Hospital Yong-Woon Shin Forearm Fractures Forearm fractures - the most common orthopaedic injuries in children - 30-50% of all pediatric fractures
Pediatric Elbow Radiology. Seema Awatramani, MD Friday, April 5, 2018 ACOEP Spring Seminar
 Pediatric Elbow Radiology Seema Awatramani, MD Friday, April 5, 2018 ACOEP Spring Seminar Disclosure I have no relevant financial relationships with the manufacturer(s) of any commercial product(s) and/or
Pediatric Elbow Radiology Seema Awatramani, MD Friday, April 5, 2018 ACOEP Spring Seminar Disclosure I have no relevant financial relationships with the manufacturer(s) of any commercial product(s) and/or
PEDIATRIC UPPER EXTREMITY FRACTURE MANAGEMENT JULIA RAWLINGS, MD SPORTS MEDICINE SYMPOSIUM: THE PEDIATRIC ATHLETE 2 MARCH 2018
 PEDIATRIC UPPER EXTREMITY FRACTURE MANAGEMENT JULIA RAWLINGS, MD SPORTS MEDICINE SYMPOSIUM: THE PEDIATRIC ATHLETE 2 MARCH 2018 DISCLOSURE I have nothing to disclose. 2 OBJECTIVES Discuss the diagnosis,
PEDIATRIC UPPER EXTREMITY FRACTURE MANAGEMENT JULIA RAWLINGS, MD SPORTS MEDICINE SYMPOSIUM: THE PEDIATRIC ATHLETE 2 MARCH 2018 DISCLOSURE I have nothing to disclose. 2 OBJECTIVES Discuss the diagnosis,
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Elbow. Chapter 2 LISTEN. Mechanism of Injury (If Applicable) Pain
 Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
MEDIAL EPICONDYLE FRACTURES
 MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
