CLINICAL VIGNETTES FOR A LIFETIME (I HOPE!!)
|
|
|
- Norma Shelton
- 5 years ago
- Views:
Transcription
1 CLINICAL VIGNETTES FOR A LIFETIME (I HOPE!!) As you near completion of this course I want you to begin to think in terms of Case Vignettes instead of facts. In the front of Module 3 I have included the 14 case scenarios listed below. They are: 1. Duschenne s Muscular Dystrophy 2. Guillain-Barre Syndrome 3. Spinal cord hemisection-brown Sequard Syndrome 4. Lateral Medullary (Wallenberg) Syndrome 5. Acoustic Neuroma 6. Weber Syndrome (Rostral Alternating Hemiplegia) 7. Cerebellar Cases (2) 8. Broca s Aphasia 9. Huntington s Disease 10. Cataract 11. Several Hearing Loss Cases 12. Thalamic Lesion-Pure Sensory Loss 13. Subdural Hematoma 14. David and Goliath (my favorite!!) There are nine more vignettes on this www. site that you should look over for Exam #3. While at first glance your cortisol and NE might go up, I think you will enjoy reviewing these cases since they are associated with material that we have covered this year. When the 9 scenarios below are added to the 14 above, you will have 23 neuro vignettes in your long-term memory (your blackboard can t hold them all long enough!). Please go for the on all of the Clinical Vignettes, as that is my goal in having you review them. I have given the for the 9 new vignettes discussed below, so I will leave the other 14 (above) up to you.
2 15. Clinical Vignette--ALZHEIMER S A 52 year-old man is noted to have memory difficulties. He forgets to pay several bills and forgets numerous business appointments. His wife reports that he appears depressed and is not his usually jovial self. He acts strangely and inappropriately and has an affair with a 15 year-old high school sophomore. Neurological examination shows the following abnormalities. 1. disorientation for year, month, and day 2. inability to remember 3 unrelated objects at 15 minutes 3. inability to accurately draw geometric shapes 4. inability to think abstractly. CT and MRI show no evidence of brain atrophy; MRI-SPECT (spectroscopy) shows reduced metabolism/blood flow in frontal, temporal and parietal regions bilaterally. This patient has dementia, most likely of the pre-senile Alzheimer type. In the early stages of this disorder there may be clinical evidence of cognitive or intellectual deterioration; however, CT and MRI may not yet show evidence of brain atrophy (shrinkage). In the later stages there should be anatomical evidence of brain atrophy and pathological studies would show loss of neurons. There are other pathological changes e.g. neurofibrillary tangles, amyloid deposits. MRI-SPECT shows physiological evidence of reduced perfusion and presumed reduced metabolism. This is more sensitive test than CT/MRI. Although there is reduced brain perfusion, techniques to increase cerebral blood flow will not enhance brain function. The reduced brain perfusion is a manifestation of primary neural depression; therefore as there is reduced brain mass, there is need for reduced blood flow. In Alzheimer dementia, there is a central cholinergic disorder. Drugs that enhance acetylcholine function are effective in enhancing memory (physostimine is an inhibitor of the catabolic enzyme of ACh and therefore increases the level of ACh; carbachol=cholinergic agonist).! DISORIENTATION FOR YEAR, MONTH AND DAY; ACTS STRANGELY: FORGETS; NEUROFIBRILLARY TANGLES AND SENILE PLAQUES; LOW ACETYLCHOLINE
3 16. Clinical Vignette--PARKINSON S Louise Bermel is a 60 year old female who presents to the office with difficulty using her right arm. Ms. Bermel states that the difficulty in using her right arm has occurred over the past 2 months. She is right-handed. The clumsiness and intermittent tremor have become progressively worse. No other symptoms are present. To direct questioning she says the right shoulder aches, "it may be bursitis," and that she has noted saliva on her pillow in the mornings. Her children feel she is slower and looks depressed. She denies any visual disturbances, vertigo, palpitations, sensory symptoms or unconsciousness. She denies headaches and there is no history of trauma. The problems with her shoulder and arm are making it more difficult for her to carry out her work. There is no history of neurological diseases in the family except for her mother who had a slight shake of her head in old age. There is no history of early cerebrovascular or coronary artery disease in the family. There is no family history of hypertension. Her father died of pneumonia and her mother died of cancer of the breast. Neurologic Exam: Normal cranial nerves II-XII and finger to finger and heel to shin on gait testing (cebellar). Her right arm swings less and on turns her neck looks stiff. Deep tendon reflexes, sensation, and fine coordination are almost normal. There is no significant weakness. Initiation of gait is slow (what is this called?) and a little unsteady, but when pulled from behind she does not lose her balance. There is a slight tremor of her right hand intermittently at rest that disappears when she reaches for something. It is also noted when she is walking. This is a case of Parkinson s.. It often begins unilaterally. An MRI could be done, but the presence of a tremor would interfere with getting a good exam. Treatment is designed to maintain normal function--the lifestyle to which she was accustomed--which has tremendous psychological benefit for her. The surgical possibilities are pallidotomy (lesion of Gpi), deep brain stimulation of the subthalamic nucleus (mess up its firing!) and fetal transplantation of cells that will produce DA.. SLOW INITIATION OF GAIT; SLOWER AND DEPRESSED; RESTING TREMOR; REFLEXES AND SENSATION NORMAL
4 17. Clinical Vignette LOW BACK PAIN A 45 year old delivery man comes to see you complaining of low back pain that has been intermittent for the past 6 months. The pain is in the middle of the lower back and usually radiates into the left buttock. The pain is made worse by sneezing, coughing, or when he hits a pothole while driving. In some cases these maneuvers cause the pain to radiate down the back of his left leg into the bottom lateral aspect of his foot (what a clue!!). Over the past 6 weeks, he has noted that it is difficult for him to stand on his tip toes (what a great second clue!!) and that this is primarily because of weakness in his left foot. On exam he has a normal neurological exam except that his left ankle jerk is absent and he has weakness of his left gastrocnemius. There is abnormal sensation over the lateral aspect of the left foot. He cannot stand on his toes of his left foot. When you have him lying down, you cannot elevate his left leg above 35 degrees because of shooting pain into his left buttock and down the back of his left leg. JKH Comment The clinical picture is compatible with a left S1 radiculopathy and most likely it is due to a L5-S1 herniated disc. The needle exam would reveal signs of denervation in the S1- innervated muscles, particularly the gastrocnemius, glutei, and the S1 paraspinous muscles. NCV (nerve conductin velocities) would probably be normal. To define a herniated disc and make sure that this was not some other problem, an MRI of the spine would be appropriate. Abnormal MRIs of the lumbosacral spine are common and must always be interpreted with respect to the clinical picture. Symptomatic medical treatment is probably as successful as surgical decompression and the patient s condition will improve. Surgery is favored when an active process associated with denervation and weakness is combined with disabling pain. If the EMG does not indicate active denervation (lower CMAP for instance), conservative medical therapy may be more reasonable. RADIATING PAIN IN DERMATOMAL DISTRIBUTION; WEAKNESS; HYPOTONIA OR ATONIA; ABNORMAL SENSATION
5 18. Clinical Vignette-Amyotropic Lateral Sclerosis A 65 year old man presents with a six month history of progressive fatigue, weakness and leg cramps. On a few occasions he choked on food. His wife noted diffuse twitching of muscles on his chest and upper back. Two months ago he developed a foot drop in his left leg. He has not complained of any sensory symptoms. There has been no cognitive decline. He has no difficulty with bowel or bladder function. His family history is noncontributory. Examination showed that the patient had normal mental status. Motor examination showed severe, bilateral diffuse muscle wasting in both upper and lower extremities. The most atrophied were the deltoid, triceps, biceps, hand muscles and quadriceps on either side and the left anterior tibialis. There were prominent fasciculations (WHAT ATE FIBRILLATIONS?) in all muscle groups. The muscle tone was increased in both upper and lower extremities. There was diffuse weakness in all 4 extremities with complete left foot drop. Neck extensors were profoundly weak so that the patient was barely able to keep his head up. The tendon reflexes were hyperactive in all four extremities. The plantar reflexes were extensor (Babinski sign). Sensory examination and coordination were normal. His gait was characterized by decreased arm swing and limping of the left leg. JKH Comment This is a case of amyotrophic lateral sclerosis. The increased muscle tone, hyperreflexia and positive Babinski sign indicate upper motor neuron (UMN) damage (lateral corticospinal tract). Severe, diffuse muscle wasting and fasciculations are suggestive of a lower motor neuron (LMN) involvement (anterior horn cells). In amyotrophic lateral sclerosis, not all of the LMNs die at the same time (the disease is progressive). Loss of anterior horn cells leads to atrophy of their target muscles (therefore no spasticity), while those ventral horn cells that are still functional will cause spasticity in their targeted muscles due to the loss of the LCST input, an upper motor neuron deficit. FASCICULATIONSAND ATROPHY (LMN PROBLEMS) COMBINED WITH UMN PROBLEMS LIKE A BABINSKI SIGN, SPASTICITY, INCREASED TENDON REFLEXES; NORMAL SENSATION AND COGNITION. DO YOU THINK THE PATIENT HAS CLONUS?
6 19. Clinical Vignette--Syringomyelia A 56-year old woman has a long history of numbness in and clumsiness of her hands. Initially the numbness started in her right hand but progressed slowly to include both hands and both arms. Over the past year the numbness has actually included the shoulders, neck, scalp and most recently the area of the face next to the hairline and the angle of the jaw on the right. Besides the numbness, she has noted increasing difficulty in opening jars and over the past 2-3 years has had trouble brushing her hair. Most recently she has begun to have trouble with slurred speech, swallowing, and a hoarse voice. Her other complaints include trouble with walking. It seems that she is having trouble with tripping over her toes. She has smoked cigarettes for many years and recently stopped because she has burned her fingers a number of times and did not feel the pain (big clue!). She had to have a skin graft of her right hand because of a severe burn she sustained from a stove. Her exam revealed a normal mental status. Cranial nerve exam showed a bilateral decrease in pin prick sensation at the hair line and angle of the jaw. The palate moved poorly and her voice had a nasal characteristic. Her gag reflex was depressed. There was some atrophy of the left side of her tongue with fasciculations noted. The motor exam revealed diffuse weakness and atrophy of the upper extremities. There were some fasciculations noted in the biceps bilaterally. The reflexes in the upper extremities were barely obtained. In the lower extremities there was mild weakness and increased tone and reflexes. Bilateral Babinski signs were noted. The patient s gait was stiff and she could not walk on her heels. The sensory exam in the lower extremities was normal. The sensation in the upper extremities was intact to vibration and joint position sense but she could not feel pin prick in either upper extremity or across the shoulders, the neck or the scalp. This is a case of syringomyelia, which is a cavitation/gliosis in the central canal (and interruption of the crossing dorsal horn fibers headed into the ALSs or lateral spinothalamic fibers; LSTT) of the spinal cord. The destructive process has obviously moved rostrally into the brain stem. The tongue findings suggest a lower motor neuron lesion on the right (either nerve or nucleus) and the decrease gag, nasal speech, and hoarseness point to a medullary lesion (remember nucleus ambiguous??). The weakness in the upper extremities is consistent with a lower motor lesion; however, in the lower extremities the findings suggest an upper motor lesion. The sensory findings point to a lesion affecting the crossing fibers of the spinothalamic pathway (ALS) in the spinal cord and the right spinal nucleus V.
7 CAPE-LIKE DISTRIBUTION OF PAIN (PIN PRICK) AND TEMPERATURE LOSS DUE TO DAMAGE TO CROSSING ALS/SPINOTHALAMIC FIBERS IN THE SPINAL CORD. ALSO CAN SPREAD INTO THE BRAINSTEM WHERE THERE IS LMN AND OTHER DAMAGE. DON T CONFUSE THIS WITH GLOVE AND STOCKING DISTRIBUTION SEEN IN NEUROPATHIES. 20. Clinical Vignette--Wernicke-Korsakoff Syndrome A 50 year-old CEO develops abdominal pain and is found to have a tender abdomen on examination. Liver function studies are markedly abnormal and serum amylase is markedly elevated. An abdominal CT shows a mass. At surgery, he is found to have a pancreatic pseudocyst. (The pseudocyst is, by far, the most common cystic mass of the pancreas. Approximately 10% of patients develop pseudocysts following several episodes of alcohol induced pancreatitis [severe complications of pancreatitis are more common when alcohol induced]). These cysts are usually noncomplicated. If complicated, and there is no history of pancreatitis, the diagnosis of mucinous cystic neoplasm must be entertained. This may seem to be an obvious distinction, but many mucinous cystic neoplasms carry a diagnosis of pseudocyst before the correct diagnosis is made.. In the surgical recovery room, he awakens and is delirious and tremulous. He is treated with CNS tranquilizers and this calms him. Two days later, he awakens but his recent memory is quite poor but remote (past) memory is intact. He can not remember any of three unrelated objects at 10 minutes. Based upon the clinical features, this patient most likely has alcohol-induced damage even though no statement is made to suggest "chronic alcoholism." Initially, he is "delirious" and "tremulous" and this suggest major alcoholic withdrawal syndrome which occurs after abrupt cessation of alcohol. As the patient awakens and shows poor recent memory (like H.M.), this is consistent with Wernicke-Korsakoff Syndrome. One way of telling this disease from anoxia of the hippocampi (both exhibit the absence of new memories) is that in the Korsakoff s there is confabulation, that is, the patient tries to cover his memory loss by making up stories. Pathological changes include necrotic and hemorrhagic microscopic lesions involving the mammillary bodies (memory problem due to connections with hippocampus via fornix) periaqueductal midbrain, paraventricular thalamus, and hypothalamus. This disorder
8 results from specific deficiency of vitamin B-1 (thiamine). This is an essential cofactor for decarboxylation of pyruvate and alpha-ketoglutarate. Replacement therapy with thiamine should cause improvement in memory function. TOO MUCH ALCOHOL!! (DON T FORGET ABOUT ALCOHOL S EFFECT ON THE MEDIAL ZONE (VERMIS) OF CEREBELLUM). PATIENT HAS SIMILAR MEMORY PROBLEMS AS H.M AFTER HIS BILATERAL HIPPOCAMPAL REMOVAL BUT IN ADDITION EXHIBITS CONFABULATION. LESION INVOLVES MAMMILLARY BODIES AND PERHAPS ADJACENT HYPOTHALAMUS AND THALAMUS. 21. Clinical Vignette-Multiple Sclerosis Leslie Biggins, a twenty-eight year old, male, graduate student presents complaining of double vision when he looks to the right for the past three days. Mr. Biggins states that the double vision was first noticed upon awakening three days ago. He feels fine and has no other complaints. He has never been ill with the exception of an occasional upper respiratory infection and the usual childhood diseases of measles, chickenpox and mumps. His family history is negative except for hypertension in his father, which is well controlled with medication. His maternal grandmother was afflicted with "rheumatism" and was in a wheel chair for many years before her death. He reports no headaches, muscle weakness, dizziness or sensory anomalies. He sleeps poorly and is up most of the night because of a need to urinate frequently. He feels that this is a direct consequence of caffeine intake. Two months ago he became incontinent of urine in bed, and he has cut off coffee altogether. He feels that this has improved matters somewhat, but not entirely. He has noticed an inability to concentrate and fatigue has become an inordinate problem. He is not currently taking any medication and does not smoke or drink. He is a graduate student in clinical psychology and is under much pressure to finish his dissertation. His wife is anxious to start a family. He admits to being "stressed out" and depressed. This has had a significant negative impact regarding his relationship with his wife and recently he has had problems with impotence. Neurological Examination: (I have noted only important ones!)
9 Mental status: Mr. Biggins is cooperative and is oriented as to place and time. He has appropriate memory for immediate (working), recent (hippocampal) and past events. He is able to compute arithmetically and can attend to similarities and differences. Eyes: On right gaze the right eye abducts but the left eye cannot pass the midline. Nystagmus is present in the right (good) eye during right lateral gaze. On left gaze both eyes turn left normally without nystagmus or diplopia. Motor System--Upper and lower limbs are strong. Tone in both lower extremities is elevated. Clonus is elicited in the left ankle. Sensation: Proprioception, vibration, pain, and temperature are all normal, as is stereognosis and two-point-discrimination. DTR (deep tendopn reflexes): Symmetrical and 3+. Babinski + Bilaterally. Cerebellar funct.: Gait, toe-heel, finger-nose, rapid alternating movement are normal and symmetric. The MRI shows multiple high signal (white) white-matter lesions. The lesions are mostly around the lateral ventricles. A number of the lesions are oval in shape and some lesions also appear as dark "holes" in the T 1 images (sequences when the ventricles are dark). JKH Comment This is multiple sclerosis. Mr. Biggins was placed on prednisone, 60 mg per day. The diplopia resolved by the tenth day of treatment and the dose was tapered and discontinued. Hopefully you remember what happens with a lesion (demyelination) of the left MLF (can t turn left eye medially to the right). Moreover, both LCSTs (increased reflexes, clonus, and Babinskis) are exhibiting demyelination. THE KEY HERE IS MULTIFOCAL LESIONS. WE HAVE EMPHASIZED IN THE PROBLEM SOLVINGS SINGLE LESIONS THAT ACCOUNT FOR NUMEROUS CLINICAL DEFICITS. MS HITS ALL OVER THE PLACE AND COMMONLY AFFECTS THE MLF, LCSTS AND OPTIC NERVES.
10 22. Clinical Vignette--EPILEPSY A two-year-old boy presents to the ER. Just after awakening, the mother noticed that his right arm, then leg, began to shake. He was also "out of it" but not unconscious; he would not respond to her. This continued while she brought the child to the ER. He had been fine that day except for feeling "warm." On arrival to the ER, the right-sided rhythmic jerking movements continued. The rest of the exam was significant for a temperature of and a left otitis media. Past medical history was significant for speech delay, as he did not yet have any words beside "mama" and "dada." The two-year-old boy presented above has a simple partial seizure involving predominantly the left hemisphere (right sided jerking movements). The MRI showed a subependymal heterotopia on the left. Gray matter heterotopias are collections of normal neurons in an unusual location, due to an arrest in fetal neuronal migration. Because of its localization, these neurons have escaped the cortical GABA-ergic inhibition that normally prevents over excitation. Because of this lack of inhibition, these misplaced neurons are highly epileptogenic. Increased body temperature, such as one sees during a fever, increases the excitability and can provoke a seizure. THE KEY HERE IS THE MAINTENANCE OF CONSCIOUSNESS WITH THE RHYTHMIC JERKING OF THE CONTRALATERAL LIMBS. 23. Clinical Vignette Myasthenia Gravis A 25 year old woman came to your office complaining of intermittent double vision for the last three weeks. She also has complained of fatigue. She has felt best during the early morning hours, but later, during the course of the day, she gradually develops double vision and diffuse weakness. Her boy friend has observed that her right eyelid has been drooping frequently. She used to play competitive basketball while in college, but now she has been short of breath after climbing only 2 flights of stairs. Also, on a few occasions, she choked on food and her friends noted that her speech was slurred or thick. On examination her mental status was normal. She had marked ptosis on the right side. Eye movement examination showed decreased movement in all directions in the right
11 eye. There was also slightly decreased abduction in the left eye. On repetitive blinking she developed ptosis of the left eyelid and her right-sided ptosis got much worse. Motor examination showed normal muscle bulk and tone. Muscle testing revealed that she was initially strong, but rapidly became tired or weak with repeated effort. She was unable to hold her arms abducted at 90 degrees for more than 30 seconds. All sensory modalities, reflexes, coordination and gait examination were normal. Plantar reflexes were flexor. Myasthenia gravis is an immune mediated disorder of neuromuscular transmission. This condition is characterized by fluctuating weakness and fatigability of voluntary muscles. In the vast majority of cases, extraocular muscles are involved. Some patients may also have involvement of the muscles of the tongue, pharynx, and soft palate (dysphagia; difficulty swallowing and dysarthria; slurred speech). Weakness gets worse with any sustained activity and improves after a period of rest. MG is caused by immune mediated destruction of acetylcholine receptors at the postsynaptic membrane and in some patients it may be associated with a thymoma (tumor) of the thyroid gland (about one in ten MG patients). THE KEY HERE IS FATIGUE, EYE MUSCLE(S) WEAKNESS THAT GETS WORSE AS THE DAY PROGRESSES, DECREMENTAL CMAP and NORMAL SENSATION
BRAIN STEM CASE HISTORIES CASE HISTORY VII
 463 Brain stem Case history BRAIN STEM CASE HISTORIES CASE HISTORY VII A 60 year old man with hypertension wakes one morning with trouble walking. He is feeling dizzy and is sick to his stomach. His wife
463 Brain stem Case history BRAIN STEM CASE HISTORIES CASE HISTORY VII A 60 year old man with hypertension wakes one morning with trouble walking. He is feeling dizzy and is sick to his stomach. His wife
High Yield Neurological Examination
 High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
A Hypothesis Driven Approach to the Neurological Exam
 A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
The Neurologic Examination: High-Yield Strategies
 The Neurologic Examination: High-Yield Strategies S. Andrew Josephson, MD Examination Approach Two types of neurologic examinations 1. Screening Examination 2. Testing Hypotheses Select high-yield tests
The Neurologic Examination: High-Yield Strategies S. Andrew Josephson, MD Examination Approach Two types of neurologic examinations 1. Screening Examination 2. Testing Hypotheses Select high-yield tests
Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of
 Peripheral Nervous System Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of non-insulin dependent diabetes
Peripheral Nervous System Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of non-insulin dependent diabetes
The NIHSS score is 4 (considering 2 pts for the ataxia involving upper and lower limbs.
 Neuroscience case 5 1. Speech comprehension, ability to speak, and word use were normal in Mr. Washburn, indicating that aphasia (cortical language problem) was not involved. However, he did have a problem
Neuroscience case 5 1. Speech comprehension, ability to speak, and word use were normal in Mr. Washburn, indicating that aphasia (cortical language problem) was not involved. However, he did have a problem
How to Think like a Neurologist Review of Exam Process and Assessment Findings
 Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
The High-Yield Neurologic Examination
 The High-Yield Neurologic Examination S. Andrew Josephson MD Carmen Castro Franceschi and Gladyne K. Mitchell Neurohospitalist Distinguished Professor Chair, Department of Neurology Director, Neurohospitalist
The High-Yield Neurologic Examination S. Andrew Josephson MD Carmen Castro Franceschi and Gladyne K. Mitchell Neurohospitalist Distinguished Professor Chair, Department of Neurology Director, Neurohospitalist
Spinal Cord: Clinical Applications. Dr. Stuart Inglis
 Spinal Cord: Clinical Applications Dr. Stuart Inglis Tabes dorsalis, also known as syphilitic myelopathy, is a slow degeneration (specifically, demyelination) of the nerves in the dorsal funiculus of the
Spinal Cord: Clinical Applications Dr. Stuart Inglis Tabes dorsalis, also known as syphilitic myelopathy, is a slow degeneration (specifically, demyelination) of the nerves in the dorsal funiculus of the
Upper and Lower Motoneurons for the Head Objectives
 Upper and Lower Motoneurons for the Head Objectives Know the locations of cranial nerve motor nuclei Describe the effects of motor cranial nerve lesions Describe how the corticobulbar tract innervates
Upper and Lower Motoneurons for the Head Objectives Know the locations of cranial nerve motor nuclei Describe the effects of motor cranial nerve lesions Describe how the corticobulbar tract innervates
The Neurologic Examination: High-Yield Strategies
 The Neurologic Examination: High-Yield Strategies S. Andrew Josephson, MD Assistant Professor, Department of Neurology Divisions of Neurovascular and Behavioral Neurology University of California San Francisco
The Neurologic Examination: High-Yield Strategies S. Andrew Josephson, MD Assistant Professor, Department of Neurology Divisions of Neurovascular and Behavioral Neurology University of California San Francisco
Movement Disorders. Psychology 372 Physiological Psychology. Background. Myasthenia Gravis. Many Types
 Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
Power Line to your Line to your Circuit Line to the station neighborhood house breaker living room. Outlet lamp Lamp with socket, Light bulb
 IMC 606 Neuroscience and Behavior Module Dr. Margaret Paroski Analysis of Sensory Lesions You walk into your living room and turn on the lamp. But no light comes on. What would you do? You would probably
IMC 606 Neuroscience and Behavior Module Dr. Margaret Paroski Analysis of Sensory Lesions You walk into your living room and turn on the lamp. But no light comes on. What would you do? You would probably
Anatomy of the Spinal Cord
 Spinal Cord Anatomy of the Spinal Cord Anatomy of the Spinal Cord Posterior spinal arteries Lateral corticospinal tract Dorsal column Spinothalamic tract Anterior spinal artery Anterior white commissure
Spinal Cord Anatomy of the Spinal Cord Anatomy of the Spinal Cord Posterior spinal arteries Lateral corticospinal tract Dorsal column Spinothalamic tract Anterior spinal artery Anterior white commissure
UF NEUROLOGY HISTORY AND PHYSICAL GUIDELINES
 UF NEUROLOGY HISTORY AND PHYSICAL GUIDELINES HISTORY Chief Complaint A maximally succinct statement of the patient age, handedness, gender, main problem, and its duration (e.g. 56 year old right-handed
UF NEUROLOGY HISTORY AND PHYSICAL GUIDELINES HISTORY Chief Complaint A maximally succinct statement of the patient age, handedness, gender, main problem, and its duration (e.g. 56 year old right-handed
The Cerebellum. Physiology #13 #CNS1
 Physiology #13 #CNS1 The cerebellum consists of cortex and deep nuclei, it is hugely condensed with gray mater (condensed with neurons (1/3 of the neurons of the brain)). Cerebellum contains 30 million
Physiology #13 #CNS1 The cerebellum consists of cortex and deep nuclei, it is hugely condensed with gray mater (condensed with neurons (1/3 of the neurons of the brain)). Cerebellum contains 30 million
e) None of the above e) None of the above
 Neurology 1) For the management of an acute delirium acquired in the hospital, which one of the following options would be least appropriate? a) Treating the underlying cause b) Promptly increasing antibiotic
Neurology 1) For the management of an acute delirium acquired in the hospital, which one of the following options would be least appropriate? a) Treating the underlying cause b) Promptly increasing antibiotic
OBJECTIVES. Unit 7:5 PROPERTIES OR CHARACTERISTICS OF MUSCLES. Introduction. 3 Kinds of Muscles. 3 Kinds of Muscles 4/17/2018 MUSCULAR SYSTEM
 OBJECTIVES Unit 7:5 MUSCULAR SYSTEM Compare the three main kinds of muscles by describing the action of each Differentiate between voluntary and involuntary muscles List at least three functions of muscles
OBJECTIVES Unit 7:5 MUSCULAR SYSTEM Compare the three main kinds of muscles by describing the action of each Differentiate between voluntary and involuntary muscles List at least three functions of muscles
Neurological Assessment
 Neurological Assessment Name: Age: Gender: Date: History Review of history related to neurological system YES/NO If YES, provide details: General Neurological Mental Illness Neurological disease Severe
Neurological Assessment Name: Age: Gender: Date: History Review of history related to neurological system YES/NO If YES, provide details: General Neurological Mental Illness Neurological disease Severe
Slide 1. Slide 2. Slide 3. Intro to Physical Therapy for Neuromuscular Conditions. PT Evaluation. PT Evaluation
 Slide 1 Intro to Physical Therapy for Neuromuscular Conditions PTA 103 Introduction to Clinical Practice 2 Slide 2 Mental status: consciousness, attention, orientation, cognition Communication: speech
Slide 1 Intro to Physical Therapy for Neuromuscular Conditions PTA 103 Introduction to Clinical Practice 2 Slide 2 Mental status: consciousness, attention, orientation, cognition Communication: speech
The Neurologic Examination. John W. Engstrom, M.D. University of California San Francisco School of Medicine
 The Neurologic Examination John W. Engstrom, M.D. University of California San Francisco School of Medicine Overview The Neurologic Examination Mental status demonstration/questions Cranial nerves demonstration/questions
The Neurologic Examination John W. Engstrom, M.D. University of California San Francisco School of Medicine Overview The Neurologic Examination Mental status demonstration/questions Cranial nerves demonstration/questions
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
3) Approach to Ataxia - Dr. Zana
 3) Approach to Ataxia - Dr. Zana Introduction Ataxia is derived from Greek word a -not, taxis -orderly, (not orderly/ not in order) Ataxia is the inability to make smooth, accurate and coordinated movements
3) Approach to Ataxia - Dr. Zana Introduction Ataxia is derived from Greek word a -not, taxis -orderly, (not orderly/ not in order) Ataxia is the inability to make smooth, accurate and coordinated movements
Examination Approach. Examination Approach. Case 1: Mental Status. The Neurological Exam In the ICU: High Yield Techniques 5/8/2015
 The Neurological Exam In the ICU: High Yield Techniques Examination Approach Two types of neurologic examinations 1. Screening Examination 2. Testing Hypotheses Select high-yield tests and techniques S.
The Neurological Exam In the ICU: High Yield Techniques Examination Approach Two types of neurologic examinations 1. Screening Examination 2. Testing Hypotheses Select high-yield tests and techniques S.
P1: OTA/XYZ P2: ABC c01 BLBK231-Ginsberg December 23, :43 Printer Name: Yet to Come. Part 1. The Neurological Approach COPYRIGHTED MATERIAL
 Part 1 The Neurological Approach COPYRIGHTED MATERIAL 1 2 Chapter 1 Neurological history-taking The diagnosis and management of diseases of the nervous system have been revolutionized in recent years by
Part 1 The Neurological Approach COPYRIGHTED MATERIAL 1 2 Chapter 1 Neurological history-taking The diagnosis and management of diseases of the nervous system have been revolutionized in recent years by
FILED: NEW YORK COUNTY CLERK 04/12/ :57 PM INDEX NO /2011 NYSCEF DOC. NO RECEIVED NYSCEF: 04/12/2018
 ' NYNeurological.- 't Associates, P.C. e 3He e a David Dc vld Snyder, M.D. Emilio Oribe, M.D., F.A.C.P Tonya FOtiml, M.D. Yvonne Zoharckis, M,b. www.nynapc.com July 3, 2017 Sabatini 4 Associates 237 West
' NYNeurological.- 't Associates, P.C. e 3He e a David Dc vld Snyder, M.D. Emilio Oribe, M.D., F.A.C.P Tonya FOtiml, M.D. Yvonne Zoharckis, M,b. www.nynapc.com July 3, 2017 Sabatini 4 Associates 237 West
Problems of Neurological Function. Unit 10
 Problems of Neurological Function Unit 10 Independent Student Review Brain Anatomy and physiology of cerebral hemispheres, diencephalon, brain stem, and cerebellum Meninges, ventricles, flow of CSF Blood
Problems of Neurological Function Unit 10 Independent Student Review Brain Anatomy and physiology of cerebral hemispheres, diencephalon, brain stem, and cerebellum Meninges, ventricles, flow of CSF Blood
GENERAL PRINCIPLES OF NEUROLOGY- John W. Day, M.D., Ph.D.
 I. TAKE HOME POINTS FOR THIS LECTURE A. Localizing the disease is the first step in diagnosing a neurological disorder. B. Time course of the disease (acute, subacute, or chronic) indicates the pathophysiological
I. TAKE HOME POINTS FOR THIS LECTURE A. Localizing the disease is the first step in diagnosing a neurological disorder. B. Time course of the disease (acute, subacute, or chronic) indicates the pathophysiological
Functional Distinctions
 Functional Distinctions FUNCTION COMPONENT DEFICITS Start Basal Ganglia Spontaneous Movements Move UMN/LMN Cerebral Cortex Brainstem, Spinal cord Roots/peripheral nerves Plan Cerebellum Ataxia Adjust Cerebellum
Functional Distinctions FUNCTION COMPONENT DEFICITS Start Basal Ganglia Spontaneous Movements Move UMN/LMN Cerebral Cortex Brainstem, Spinal cord Roots/peripheral nerves Plan Cerebellum Ataxia Adjust Cerebellum
Neurological Examination
 Neurological Examination Charles University in Prague 1st Medical Faculty and General University Hospital Neurological examination: Why important? clinical history taking and bedside examination: classical
Neurological Examination Charles University in Prague 1st Medical Faculty and General University Hospital Neurological examination: Why important? clinical history taking and bedside examination: classical
Physical Assessment Class 3
 Physical Assessment Class 3 Daily Tasks **Spot Test and assessment 1 (Class materials from1 2)** Goals: Understand significant features of a neurological history Know the complete sequence of cranial nerve
Physical Assessment Class 3 Daily Tasks **Spot Test and assessment 1 (Class materials from1 2)** Goals: Understand significant features of a neurological history Know the complete sequence of cranial nerve
Unit VIII Problem 5 Physiology: Cerebellum
 Unit VIII Problem 5 Physiology: Cerebellum - The word cerebellum means: the small brain. Note that the cerebellum is not completely separated into 2 hemispheres (they are not clearly demarcated) the vermis
Unit VIII Problem 5 Physiology: Cerebellum - The word cerebellum means: the small brain. Note that the cerebellum is not completely separated into 2 hemispheres (they are not clearly demarcated) the vermis
NS201C Anatomy 1: Sensory and Motor Systems
 NS201C Anatomy 1: Sensory and Motor Systems 25th January 2017 Peter Ohara Department of Anatomy peter.ohara@ucsf.edu The Subdivisions and Components of the Central Nervous System Axes and Anatomical Planes
NS201C Anatomy 1: Sensory and Motor Systems 25th January 2017 Peter Ohara Department of Anatomy peter.ohara@ucsf.edu The Subdivisions and Components of the Central Nervous System Axes and Anatomical Planes
X-Plain Muscles Reference Summary
 X-Plain Reference Summary Introduction are very important elements of the human body. They account for about half of a person s weight. Understanding how muscles work and how they can be injured is necessary
X-Plain Reference Summary Introduction are very important elements of the human body. They account for about half of a person s weight. Understanding how muscles work and how they can be injured is necessary
MOTOR NEURONE DISEASE
 MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
Assignment 4: An Introduction to Functional Neuroanatomy.
 Assignment 4: An Introduction to Functional Neuroanatomy. Neurons are organized into functional regions of the brain that work together to produce complete behaviors. This process is called distributive
Assignment 4: An Introduction to Functional Neuroanatomy. Neurons are organized into functional regions of the brain that work together to produce complete behaviors. This process is called distributive
Clinical Learning Exercise #1
 Clinical Learning Exercise #1 Exercise: We are going to assume nothing is wrong with the peripheral nervous system and attempt to identify the central nervous system anatomical location for the following
Clinical Learning Exercise #1 Exercise: We are going to assume nothing is wrong with the peripheral nervous system and attempt to identify the central nervous system anatomical location for the following
NEUROLOGY CLERKSHIP CORE CURRICULUM GUIDELINES
 NEUROLOGY CLERKSHIP CORE CURRICULUM GUIDELINES Endorsed by the following organizations - October 2000: American Academy of Neurology Association of University Professors of Neurology American Neurological
NEUROLOGY CLERKSHIP CORE CURRICULUM GUIDELINES Endorsed by the following organizations - October 2000: American Academy of Neurology Association of University Professors of Neurology American Neurological
Neurologic Examination
 John W. Engstrom, MD October 16, 2015 Neurologic Examination Overview The Neurologic Examination Neurologic Examination John W. Engstrom, M.D. Dept. of Neurology University of California, San Francisco
John W. Engstrom, MD October 16, 2015 Neurologic Examination Overview The Neurologic Examination Neurologic Examination John W. Engstrom, M.D. Dept. of Neurology University of California, San Francisco
Approach to a Neurologic Diagnosis
 Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Anatomy of Nervous System. Neurological Assessment. Brain. Brain. Spinal Cord. Spinal Cord 03/23/2010. Central. Peripheral
 Anatomy of Nervous System Neurological Assessment Central Brain Spinal cord Peripheral Spinal Nerves Brain Cerebral cortex ( rind ) gray matter Frontal Parietal Temporal Occipital Wernicke s area receptive
Anatomy of Nervous System Neurological Assessment Central Brain Spinal cord Peripheral Spinal Nerves Brain Cerebral cortex ( rind ) gray matter Frontal Parietal Temporal Occipital Wernicke s area receptive
Pain and Temperature Objectives
 Pain and Temperature Objectives 1. Describe the types of sensory receptors that transmit pain and temperature. 2. Understand how axon diameter relates to transmission of pain and temp information. 3. Describe
Pain and Temperature Objectives 1. Describe the types of sensory receptors that transmit pain and temperature. 2. Understand how axon diameter relates to transmission of pain and temp information. 3. Describe
HEAD AND NECK PART 2
 HEAD AND NECK PART 2 INTEGRATED CURRICULUM = Integrate Basic Science and Clinical Training 1- ENT PATIENT EXAM IN ICS COURSE - Today and next week - Review/Preview Anatomy underlying ENT exam 2- NEUROANATOMY/NEUROLOGY
HEAD AND NECK PART 2 INTEGRATED CURRICULUM = Integrate Basic Science and Clinical Training 1- ENT PATIENT EXAM IN ICS COURSE - Today and next week - Review/Preview Anatomy underlying ENT exam 2- NEUROANATOMY/NEUROLOGY
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
QUESTIONS CASE HISTORY XII
 615 Case History XII A 80 year old ex-president of the United States was out riding his horse when the horse stumbled and the ex-president fell off the horse hitting his head on the ground. He did not
615 Case History XII A 80 year old ex-president of the United States was out riding his horse when the horse stumbled and the ex-president fell off the horse hitting his head on the ground. He did not
PAGE 1 NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only)
 PAGE 1 NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only) 1. What is the main problem that you are having? (If additional space is required, please use the back of this
PAGE 1 NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only) 1. What is the main problem that you are having? (If additional space is required, please use the back of this
How to Do the EDSS. Stephen S. Kamin, MD New Jersey Medical School
 How to Do the EDSS Stephen S. Kamin, MD New Jersey Medical School John F. Kurtzke, MD 1926-2015 EDSS Expanded Disability Status Scale Devised by John Kurtzke in the 1960s and modified in the 1980s EDSS
How to Do the EDSS Stephen S. Kamin, MD New Jersey Medical School John F. Kurtzke, MD 1926-2015 EDSS Expanded Disability Status Scale Devised by John Kurtzke in the 1960s and modified in the 1980s EDSS
It s Always a Stroke; Except For When It s Not..
 It s Always a Stroke; Except For When It s Not.. TREVOR PHINNEY, D.O. Disclosures No Relevant Disclosures 1 Objectives Discuss variables of differential diagnosis for stroke Review when to TPA and when
It s Always a Stroke; Except For When It s Not.. TREVOR PHINNEY, D.O. Disclosures No Relevant Disclosures 1 Objectives Discuss variables of differential diagnosis for stroke Review when to TPA and when
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
CN V! touch! pain! Touch! P/T!
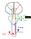 CN V! touch! pain! Touch! P/T! Visual Pathways! L! R! B! A! C! D! LT! E! F! RT! G! hypothalamospinal! and! ALS! Vestibular Pathways! 1. Posture/Balance!!falling! 2. Head Position! 3. Eye-Head Movements
CN V! touch! pain! Touch! P/T! Visual Pathways! L! R! B! A! C! D! LT! E! F! RT! G! hypothalamospinal! and! ALS! Vestibular Pathways! 1. Posture/Balance!!falling! 2. Head Position! 3. Eye-Head Movements
Neuro Exam Explained
 Neuro Exam Explained Michael Nelson M.D. Providence Neurological Specialties East Primary Care Conference October 26 rd, 2017 Michael Nelson M.D. Medical School: University of Missouri-Columbia Residency:
Neuro Exam Explained Michael Nelson M.D. Providence Neurological Specialties East Primary Care Conference October 26 rd, 2017 Michael Nelson M.D. Medical School: University of Missouri-Columbia Residency:
Reflexes. Dr. Baizer
 Reflexes Dr. Baizer 1 Learning objectives: reflexes Students will be able to describe: 1. The clinical importance of testing reflexes. 2. The essential components of spinal reflexes. 3.The stretch reflex.
Reflexes Dr. Baizer 1 Learning objectives: reflexes Students will be able to describe: 1. The clinical importance of testing reflexes. 2. The essential components of spinal reflexes. 3.The stretch reflex.
Lecturer. Prof. Dr. Ali K. Al-Shalchy MBChB/ FIBMS/ MRCS/ FRCS 2014
 Lecturer Prof. Dr. Ali K. Al-Shalchy MBChB/ FIBMS/ MRCS/ FRCS 2014 Dorsal root: The dorsal root carries both myelinated and unmyelinated afferent fibers to the spinal cord. Posterior gray column: Long
Lecturer Prof. Dr. Ali K. Al-Shalchy MBChB/ FIBMS/ MRCS/ FRCS 2014 Dorsal root: The dorsal root carries both myelinated and unmyelinated afferent fibers to the spinal cord. Posterior gray column: Long
Distal chronic spinal muscular atrophy involving the hands
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
TOXIC AND NUTRITIONAL DISORDER MODULE
 TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
Painless, progressive weakness Could this be Motor Neurone Disease?
 Painless, progressive weakness Could this be Motor Neurone Disease? The importance of early diagnosis removal of uncertainty for the person experiencing symptoms allowing for care and support to start
Painless, progressive weakness Could this be Motor Neurone Disease? The importance of early diagnosis removal of uncertainty for the person experiencing symptoms allowing for care and support to start
Problems of Neurological Function
 Problems of Neurological Function Unit 10 Independent Student Review Brain Anatomy and physiology of cerebral hemispheres, diencephalon, brain stem, and cerebellum Meninges, ventricles, flow of CSF Blood
Problems of Neurological Function Unit 10 Independent Student Review Brain Anatomy and physiology of cerebral hemispheres, diencephalon, brain stem, and cerebellum Meninges, ventricles, flow of CSF Blood
Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology
 Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology Activity Everyone stand up, raise your right hand, tell your neighbors your name 1 What part of the brain
Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology Activity Everyone stand up, raise your right hand, tell your neighbors your name 1 What part of the brain
5.1 Alex.
 5.1 Alex http://tinyurl.com/neuromakessense Alex is a 20-year-old full-time national serviceman. His only past medical history is asthma, presents to A&E with a 4-day history of bilateral finger weakness
5.1 Alex http://tinyurl.com/neuromakessense Alex is a 20-year-old full-time national serviceman. His only past medical history is asthma, presents to A&E with a 4-day history of bilateral finger weakness
Year 2 MBChB Clinical Skills Session Examination of the Motor System
 Year 2 MBChB Clinical Skills Session Examination of the Motor System Reviewed & ratified by: o o o o Dr D Smith Consultant Neurologist Dr R Davies Consultant Neurologist Dr B Michael Neurology Clinical
Year 2 MBChB Clinical Skills Session Examination of the Motor System Reviewed & ratified by: o o o o Dr D Smith Consultant Neurologist Dr R Davies Consultant Neurologist Dr B Michael Neurology Clinical
HISTORY TAKING ON NERVOUS SYSTEM. Dr. Amitesh Aggarwal
 HISTORY TAKING ON NERVOUS SYSTEM Dr. Amitesh Aggarwal General points History of neurological symptoms should also be taken from patient and close relative or friend Memory loss, intoxication, aphasia Patient
HISTORY TAKING ON NERVOUS SYSTEM Dr. Amitesh Aggarwal General points History of neurological symptoms should also be taken from patient and close relative or friend Memory loss, intoxication, aphasia Patient
The Physiology of the Senses Chapter 8 - Muscle Sense
 The Physiology of the Senses Chapter 8 - Muscle Sense www.tutis.ca/senses/ Contents Objectives... 1 Introduction... 2 Muscle Spindles and Golgi Tendon Organs... 3 Gamma Drive... 5 Three Spinal Reflexes...
The Physiology of the Senses Chapter 8 - Muscle Sense www.tutis.ca/senses/ Contents Objectives... 1 Introduction... 2 Muscle Spindles and Golgi Tendon Organs... 3 Gamma Drive... 5 Three Spinal Reflexes...
Biological Bases of Behavior. 8: Control of Movement
 Biological Bases of Behavior 8: Control of Movement m d Skeletal Muscle Movements of our body are accomplished by contraction of the skeletal muscles Flexion: contraction of a flexor muscle draws in a
Biological Bases of Behavior 8: Control of Movement m d Skeletal Muscle Movements of our body are accomplished by contraction of the skeletal muscles Flexion: contraction of a flexor muscle draws in a
Pain Drawing. Name: Today s Date: How were you referred to the office: Visual Analog Scale
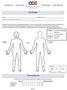 Pain Drawing Name: Today s Date: How were you referred to the office: Please be sure to fill this out as accurately as possible. This will become part of your permanent medical record and will be used
Pain Drawing Name: Today s Date: How were you referred to the office: Please be sure to fill this out as accurately as possible. This will become part of your permanent medical record and will be used
Neurology Clerkship Learning Objectives
 Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
Questionnaire for Lipedema Patients
 Questionnaire for Lipedema Patients Name Date of diagnosis Date Name of physician making diagnosis Do you also have lymphedema? What areas of the body are affected? Outside of thighs Inner thighs Knees
Questionnaire for Lipedema Patients Name Date of diagnosis Date Name of physician making diagnosis Do you also have lymphedema? What areas of the body are affected? Outside of thighs Inner thighs Knees
View the ventral side of the brain: o. Locate the optic nerve, optic chiasm, olfactory bulb
 BRAIN DISSECTION Identify External Structures: Cerebral hemispheres, brain stem, cerebellum Gyri, sulci, fissures (longitudinal and transverse fissures) Locate lobes of the cerebrum View the ventral side
BRAIN DISSECTION Identify External Structures: Cerebral hemispheres, brain stem, cerebellum Gyri, sulci, fissures (longitudinal and transverse fissures) Locate lobes of the cerebrum View the ventral side
First described by James Parkinson in his classic 1817 monograph, "An Essay on the Shaking Palsy"
 Parkinson's Disease First described by James Parkinson in his classic 1817 monograph, "An Essay on the Shaking Palsy" Parkinson s disease (PD) is a neurological disorder characterized by a progressive
Parkinson's Disease First described by James Parkinson in his classic 1817 monograph, "An Essay on the Shaking Palsy" Parkinson s disease (PD) is a neurological disorder characterized by a progressive
NEW PATIENT QUESTIONNAIRE For Dr Benoy Benny. Section 1: Today s Date: Date of Birth: Age:
 Baylor Physical Medicine and Rehabilitation NEW PATIENT QUESTIONNAIRE For Dr Benoy Benny Dear Patient: Please complete this questionnaire before you come for your appointment. Be sure to call us as soon
Baylor Physical Medicine and Rehabilitation NEW PATIENT QUESTIONNAIRE For Dr Benoy Benny Dear Patient: Please complete this questionnaire before you come for your appointment. Be sure to call us as soon
Chapter 8. Control of movement
 Chapter 8 Control of movement 1st Type: Skeletal Muscle Skeletal Muscle: Ones that moves us Muscles contract, limb flex Flexion: a movement of a limb that tends to bend its joints, contraction of a flexor
Chapter 8 Control of movement 1st Type: Skeletal Muscle Skeletal Muscle: Ones that moves us Muscles contract, limb flex Flexion: a movement of a limb that tends to bend its joints, contraction of a flexor
Done By: manar aljebreen Abdulrahman alsharidah
 Female Side Male side Done By: manar aljebreen Abdulrahman alsharidah Revised By: Nour Al-Khawajah Mohammed Asiri 2 Slide No.( 1 ) Slide No.( 2 ) 3 Slide No.( 3 ) Slide No.( 4 ) Upper motor neurons are
Female Side Male side Done By: manar aljebreen Abdulrahman alsharidah Revised By: Nour Al-Khawajah Mohammed Asiri 2 Slide No.( 1 ) Slide No.( 2 ) 3 Slide No.( 3 ) Slide No.( 4 ) Upper motor neurons are
NMH happens when there is an abnormal reflex interaction between the heart and the brain, although both are structurally normal.
 Neurally mediated hypotension: is also known as: the fainting reflex, neurocardiogenic syncope, vasodepressor syncope, the vaso-vagal reflex, and autonomic dysfunction. (Hypotension= low blood pressure,
Neurally mediated hypotension: is also known as: the fainting reflex, neurocardiogenic syncope, vasodepressor syncope, the vaso-vagal reflex, and autonomic dysfunction. (Hypotension= low blood pressure,
New Patient Pain Evaluation
 New Patient Pain Evaluation Name: Date: Using the following symbols, mark the areas of the body diagrams which are affected by your pain: \\ = Stabbing * = Electrical X = Aching N = Numbness 0 = Dull S
New Patient Pain Evaluation Name: Date: Using the following symbols, mark the areas of the body diagrams which are affected by your pain: \\ = Stabbing * = Electrical X = Aching N = Numbness 0 = Dull S
The Neurological System. Neurological Exam 5 Components. Mental Status Examination
 The Neurological System 1 Neurological Exam 5 Components Mental status Cranial nerves Reflexes Motor- includes Cerebellar function Sensory 2 Mental Status Examination Examination - ABCT Appearance Behavior
The Neurological System 1 Neurological Exam 5 Components Mental status Cranial nerves Reflexes Motor- includes Cerebellar function Sensory 2 Mental Status Examination Examination - ABCT Appearance Behavior
A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL
 A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL CASE HISTORY Nine year old male child Second born Born
A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL CASE HISTORY Nine year old male child Second born Born
COMPREHENSIVE HEALTH & WELLNESS PROFILE
 Patient Name DOB COMPREHENSIVE HEALTH & WELLNESS PROFILE The human body is designed to be healthy. Throughout life, events occur which damage your natural health expression. As a full spectrum Chiropractic
Patient Name DOB COMPREHENSIVE HEALTH & WELLNESS PROFILE The human body is designed to be healthy. Throughout life, events occur which damage your natural health expression. As a full spectrum Chiropractic
Diseases of Muscle and Neuromuscular Junction
 Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
General Sensory Pathways of the Trunk and Limbs
 General Sensory Pathways of the Trunk and Limbs Lecture Objectives Describe gracile and cuneate tracts and pathways for conscious proprioception, touch, pressure and vibration from the limbs and trunk.
General Sensory Pathways of the Trunk and Limbs Lecture Objectives Describe gracile and cuneate tracts and pathways for conscious proprioception, touch, pressure and vibration from the limbs and trunk.
HISTORY OF PRESENT ILLNESS A. TELL US ABOUT YOUR PAIN PROBLEM
 1 UT Health Austin Comprehensive Pain Management New Patient Questionnaire Thank you for scheduling a visit with the Comprehensive Pain Management Care Team. The responses you provide to these questions
1 UT Health Austin Comprehensive Pain Management New Patient Questionnaire Thank you for scheduling a visit with the Comprehensive Pain Management Care Team. The responses you provide to these questions
The Neurologic Examination
 The Neurologic Examination Cheryl L. Chrisman, DVM, MS, EdS, DACVIM (Neurology) The neurologic examination is a series of observations and tests done to answer the following four questions: h Is a lesion
The Neurologic Examination Cheryl L. Chrisman, DVM, MS, EdS, DACVIM (Neurology) The neurologic examination is a series of observations and tests done to answer the following four questions: h Is a lesion
Neuroanatomy of a Stroke. Joni Clark, MD Professor of Neurology Barrow Neurologic Institute
 Neuroanatomy of a Stroke Joni Clark, MD Professor of Neurology Barrow Neurologic Institute No disclosures Stroke case presentations Review signs and symptoms Review pertinent exam findings Identify the
Neuroanatomy of a Stroke Joni Clark, MD Professor of Neurology Barrow Neurologic Institute No disclosures Stroke case presentations Review signs and symptoms Review pertinent exam findings Identify the
Misdiagnosis in cervical spondylosis myelopathy.
 Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
The Nervous System: Sensory and Motor Tracts of the Spinal Cord
 15 The Nervous System: Sensory and Motor Tracts of the Spinal Cord PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction Millions of sensory
15 The Nervous System: Sensory and Motor Tracts of the Spinal Cord PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction Millions of sensory
ND Lesson 2.5 Jigsaw Case Study #1
 ND Lesson 2.5 Jigsaw Case Study #1 Gabby Gabby is 5 years old. Her parents have consulted with many specialists throughout their daughter s life in hopes of finding an explanation for why their daughter
ND Lesson 2.5 Jigsaw Case Study #1 Gabby Gabby is 5 years old. Her parents have consulted with many specialists throughout their daughter s life in hopes of finding an explanation for why their daughter
SENSORY PLASTICITY. Sensory Plasticity
 801 Sensory Plasticity SENSORY PLASTICITY You may have the idea that the visual, auditory and somatosensory systems are static pathways (i.e., the neural wiring is in place and simply does its job). To
801 Sensory Plasticity SENSORY PLASTICITY You may have the idea that the visual, auditory and somatosensory systems are static pathways (i.e., the neural wiring is in place and simply does its job). To
1. The cerebellum coordinates fine movement through interactions with the following motor-associated areas:
 DENT/OBHS 131 2009 Take-home test 4 Week 6: Take-home test (2/11/09 close 2/18/09) 1. The cerebellum coordinates fine movement through interactions with the following motor-associated areas: Hypothalamus
DENT/OBHS 131 2009 Take-home test 4 Week 6: Take-home test (2/11/09 close 2/18/09) 1. The cerebellum coordinates fine movement through interactions with the following motor-associated areas: Hypothalamus
Cerebrum. Impulses transmitted by:
 Sharon Niggemeier RN MSN Victoria Siegel RN, MSN, EdD Myung-Hee Pak, RN, MSN, CCRN Nervous system- divided into 2 structural parts Central Nervous System (CNS)- brain & spinal cord Peripheral Nervous System
Sharon Niggemeier RN MSN Victoria Siegel RN, MSN, EdD Myung-Hee Pak, RN, MSN, CCRN Nervous system- divided into 2 structural parts Central Nervous System (CNS)- brain & spinal cord Peripheral Nervous System
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012
 Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
NEW PATIENT INFORMATION FORM
 NEW PATIENT INFORMATION FORM Name: LAST FIRST MIDDLE Date of Birth: Sex: Marital Status: SS Number: Address: City: State: Zip Phone: Home Cell Work Email: Communication Preference: Patient Portal Phone
NEW PATIENT INFORMATION FORM Name: LAST FIRST MIDDLE Date of Birth: Sex: Marital Status: SS Number: Address: City: State: Zip Phone: Home Cell Work Email: Communication Preference: Patient Portal Phone
Dr. Gary Malstrom B.Sc.(Hon.), D.C., C.Ac Brant Street, Burlington, Ontario L7R 2J9 (905) Fax (905)
 Dr. Gary Malstrom B.Sc.(Hon.), D.C., C.Ac. Personal History: Name: Address: City: Province: Postal Code: Birth date: day /month /year Age: Sex: M F Home Phone: Business Phone: Cell Phone: E-mail: Health
Dr. Gary Malstrom B.Sc.(Hon.), D.C., C.Ac. Personal History: Name: Address: City: Province: Postal Code: Birth date: day /month /year Age: Sex: M F Home Phone: Business Phone: Cell Phone: E-mail: Health
Neurological Assessment. Lecture 8
 Neurological Assessment Lecture 8 Nervous System Central Nervous System Brain Spinal cord Peripheral Nervous System Cranial nerves Spinal nerves Central Nervous System-Brain Central Nervous System-Spinal
Neurological Assessment Lecture 8 Nervous System Central Nervous System Brain Spinal cord Peripheral Nervous System Cranial nerves Spinal nerves Central Nervous System-Brain Central Nervous System-Spinal
1/28/2019. OSF HealthCare INI Care Center Team. Neuromuscular Disease: Muscular Dystrophy. OSF HealthCare INI Care Center Team: Who are we?
 Neuromuscular Disease: Muscular Dystrophy Muscular Dystrophy Association (MDA) and OSF HealthCare Illinois Neurological Institute (INI) Care Center Team The Neuromuscular clinic is a designated MDA Care
Neuromuscular Disease: Muscular Dystrophy Muscular Dystrophy Association (MDA) and OSF HealthCare Illinois Neurological Institute (INI) Care Center Team The Neuromuscular clinic is a designated MDA Care
Biology 3201 Nervous System # 7: Nervous System Disorders
 Biology 3201 Nervous System # 7: Nervous System Disorders Alzheimer's Disease first identified by German physician, Alois Alzheimer, in 1906 most common neurodegenerative disease two thirds of cases of
Biology 3201 Nervous System # 7: Nervous System Disorders Alzheimer's Disease first identified by German physician, Alois Alzheimer, in 1906 most common neurodegenerative disease two thirds of cases of
ID # COMPLETED: YES.. 1 DATE NO... 5 NEUROLOGICAL EXAM
 ID # COMPLETED: YES.. 1 DATE NO... 5 NEUROLOGICAL EXAM VIDEOTAPED: YES.. 1 NO... 5 COMMENT: NEUROLOGICAL EXAM "Normal, Abnormal, Other, Can't execute or Missing for each question. Always complete specify
ID # COMPLETED: YES.. 1 DATE NO... 5 NEUROLOGICAL EXAM VIDEOTAPED: YES.. 1 NO... 5 COMMENT: NEUROLOGICAL EXAM "Normal, Abnormal, Other, Can't execute or Missing for each question. Always complete specify
Assessing the Stroke Patient. Arlene Boudreaux, MSN, RN, CCRN, CNRN
 Assessing the Stroke Patient Arlene Boudreaux, MSN, RN, CCRN, CNRN Cincinnati Pre-Hospital Stroke Scale May be done by EMS o One of many o F facial droop on one side o A arm drift (hold a pizza box, close
Assessing the Stroke Patient Arlene Boudreaux, MSN, RN, CCRN, CNRN Cincinnati Pre-Hospital Stroke Scale May be done by EMS o One of many o F facial droop on one side o A arm drift (hold a pizza box, close
PRACTICE EXAM QUESTIONS
 PRACTICE EXAM QUESTIONS 1. A patient presents with muscle weakness. To assess his condition, you test his knee-jerk reflex by tapping his patella tendon with your hammer. Next you examine the jaw-jerk
PRACTICE EXAM QUESTIONS 1. A patient presents with muscle weakness. To assess his condition, you test his knee-jerk reflex by tapping his patella tendon with your hammer. Next you examine the jaw-jerk
Sheet lab 3. Page 8B Section1 of medulla at pyramidal {motor} decussation:
 Sheet lab 3 Page 8B Section1 of medulla at pyramidal {motor} decussation: This section is at lower third of medulla and is the most close part to spinal cord and it has some characteristic of spinal cord
Sheet lab 3 Page 8B Section1 of medulla at pyramidal {motor} decussation: This section is at lower third of medulla and is the most close part to spinal cord and it has some characteristic of spinal cord
Gary Rea MD PhD Medical Director OSU Comprehensive Spine Center
 Gary Rea MD PhD Medical Director OSU Comprehensive Spine Center 1. The less specific the patient is about symptoms and pain, the less likely a specific diagnosis will be made and the less likely the patient
Gary Rea MD PhD Medical Director OSU Comprehensive Spine Center 1. The less specific the patient is about symptoms and pain, the less likely a specific diagnosis will be made and the less likely the patient
