CEUS LI-RADS: algorithm, implementation, and key differences from CT/MRI
|
|
|
- Lucy Craig
- 6 years ago
- Views:
Transcription
1 Abdominal Radiology ª Springer Science+Business Media, LLC 2017 Abdom Radiol (2017) DOI: /s CEUS LI-RADS: algorithm, implementation, and key differences from CT/MRI Stephanie R. Wilson, 1 Andrej Lyshchik, 2 Fabio Piscaglia, 3 David Cosgrove, 4,5 Hyun-Jung Jang, 6 Claude Sirlin, 7 Christoph F. Dietrich, 8 Tae Kyoung Kim, 9 Juergen K. Willmann, 10 Yuko Kono 11 1 Department of Radiology, University of Calgary, Street NW, Calgary T2N 2T9, Canada 2 Department of Radiology, Thomas Jefferson University Hospital, 132 S. 10th Street, 763G Main Bldg, Philadelphia, PA 19107, USA 3 Unit of Internal Medicine, Department of Medical and Surgical Sciences, University of Bologna, S. Orsola-Malpighi Hospital, Bologna, Italy 4 Hammersmith hospital, London, UK 5 King s College Hospital, London, UK 6 Department of Medical Imaging, University of Toronto, 585 University Ave, Toronto, ON M5G 2N2, Canada 7 Department of Radiology, University of California, 9500 Gilman Dr, La Jolla, San Diego, CA 92093, USA 8 Caritas Krankenhaus Bad Mergentheim, Uhlandstraße 7, Bad Mergentheim, Germany 9 University of Toronto, Toronto, Canada 10 Stanford University, Stanford, USA 11 Division of Gastroenterology & Hepatology, University of California, 200 West Arbor Dr, San Diego, CA 92103, USA Abstract Deceased: David Cosgrove Correspondence to: Yuko Kono; ykono@ucsd.edu Contrast-enhanced ultrasound (CEUS) is a specialized form of ultrasound (US) performed with an intravenous injection of microbubble contrast agents. It has been successfully used for a variety of applications including characterization of liver tumors. In April 2014, the American College of Radiology (ACR) convened a working group of international experts to develop ACR CEUS Liver Imaging Reporting and Data System (CEUS LI-RADS). An initial version of CEUS LI- RADS was published in August Although the CEUS LI-RADS concept and principles for liver lesion characterization, using dynamic contrast enhancement features, are similar to those for CT or MRI, there are significant differences between CT/MRI and CEUS LI- RADS. Therefore, CEUS LI-RADS has different diagnostic features and a unique characterization algorithm. The size of a lesion, the type and degree of arterial phase enhancement, the presence of washout, and the timing and degree of washout are the major features used for categorization. This paper describes key differences between CT/MRI and CEUS, and provides a diagnostic algorithm of CEUS LI-RADS with detailed, step-by-step instructions and imaging examples of CEUS LI-RADS categories. Key words: CEUS HCC Diagnosis LI-RADS Abbreviations CEUS Contrast-enhanced ultrasound HCC Hepatocellular carcinoma LI-RADS Liver Imaging Reporting and Data System ICC Intrahepatic cholangiocarcinoma ACR American College of Radiology AASLD American Association for the Study of Liver Disease APHE Arterial phase hyperenhancement APS Arterioportal shunts TIV Tumor in vein MDD Multi-Disciplinary Discussion Contrast-enhanced ultrasound (CEUS) is a specialized form of ultrasound (US) performed with an intravenous injection of microbubble contrast agents. It is now a widely accepted imaging technique for many applications
2 including characterization of liver tumors. With recent FDA approval of the microbubble contrast agent Lumason (SonoVue outside of USA, Bracco Diagnostics Inc. Monroe Township, NJ) for liver lesion characterization, CEUS Liver Imaging Reporting and Data System (LI-RADS) was added to the American College of Radiology (ACR) LI-RADS in Although the CEUS LI-RADS concept and principles for liver lesion characterization, using dynamic contrast enhancement features, are similar to those for CT or MRI, there are significant differences between CT or MRI and CEUS LI-RADS. Therefore, CEUS LI-RADS has different diagnostic features and a unique characterization algorithm. Contrast agents for US are biodegradable microbubbles, measuring 3 5 lm in diameter. These microbubbles resonate under low-power US waves and generate harmonic signals. A contrast-specific US imaging mode is available on the majority of US scanners and utilizes this unique property of microbubbles, by highlighting signals from microbubbles while applying specific pulse sequences that suppress signals from tissues. Similar to CT and MRI, CEUS permits demonstration of a lesion and surrounding liver blood flow, including arterial phase hyperenhancement (APHE) and washout. Many studies, including several recent metaanalyses, have shown that CEUS has similar diagnostic performance to contrast-enhanced CT and MRI in focal liver lesion characterization [1 8]. The American Association for the Study of Liver Disease (AASLD) practice guidelines for HCC management initially included CEUS along with CT and MRI in an HCC diagnostic algorithm in 2005, but removed CEUS in a 2010 update due to the possibility of misdiagnosing intrahepatic cholangiocarcinoma (ICC) as HCC, an action based on one retrospective study [9]. Since then, there have been multiple studies investigating the accuracy of CEUS for focal liver lesion characterization. These studies have shown that ICCs often show arterial phase rim enhancement, unusual for HCC, and washout which tends to be much earlier than that of HCC, and of marked degree [10, 11]. In April 2014, the ACR convened a working group of international experts to develop ACR CEUS LI-RADS including radiologists and hepatologists from the United States, Canada, and Europe. Beta versions of the CEUS LI-RADS algorithm were presented at numerous national and international conferences in 2015 and 2016 [12 14]. Based on feedback from those presentations and through iterative refinement and consensus, the working group completed CEUS LI-RADS version 2016 on May 21, The algorithm was officially approved by the ACR LI-RADS Steering Committee on June 24, The system was published online in August Key differences of CEUS from CT and MRI The method of image acquisition Acquisition of images for CEUS utilizes dynamic realtime imaging performed at the frame rates of about 10/s, thus providing the highest temporal resolution available today in abdominal imaging. This compares with more static imaging protocols for CT and MRI which are performed according to a predetermined timing regime or related to timing from an aortic contrast bolus. Therefore, CEUS may detect both early and late APHE that might be missed on CT or MRI due to mistiming of the arterial phase. Additionally, a strength of CEUS is its ability to show the rapidly changing arterial phase enhancement patterns which typify many benign tumors and especially flash-filling hemangiomas. Despite the rapidity of its occurrence, CEUS will typically show discontinuous peripheral puddles of enhancement and centripetal filling of the lesion. CT and MRI, by comparison, may often fail to reveal these rapidly changing features, showing only an enhanced mass in the arterial phase without the typical diagnostic enhancing pattern. Contrast agent properties Differences in contrast agent properties lead to different enhancement patterns on CEUS as compared with CT and MRI especially in non-hepatocellular malignancies, such as ICC, with permeable vascular endothelium and fibrous stroma. This results in persistent or increasing enhancement of ICCs in the portal venous and late phases on CT and MRI as the contrast agent passes the permeable endothelium into the tumor interstitial space with accumulation in the stroma. Purely intravascular microbubble contrast agents for CEUS show instead rapid onset and a marked degree of washout of ICCs, occurring very early and often within the time frame defined as the arterial phase. This discordance is an additional important indicator in ICC diagnosis. Increasing enhancement of ICC on CT or MRI may infrequently be associated with misdiagnosis as a benign tumor, while enhancement features on CEUS have a typical appearance for a malignant tumor; thus, combining the observations from these modalities may be beneficial [15]. Terminology: observation or nodule On CT and MRI, there are many findings that may not represent true nodules, such as perfusion alterations; therefore, the terminology observations is used to describe focal signal abnormalities throughout their LI- RADS algorithm. On CEUS, most of the observations are true nodules, and the only exceptions are focal fatty
3 infiltration and sparing which would be categorized as CEUS LR-1 when findings are definite. Otherwise, the CEUS LI-RADS algorithm is used to categorize true liver nodules visible on pre-contrast ultrasound examination on patients at risk for HCC. It is recognized that nodules identified on the B-mode scan are a prerequisite for CEUS LI-RADS categorization at this time. CEUS technique Following careful determination of the optimal scanning plane, transducer location, and patient position and breathing, CEUS is performed with an intravenous injection of a microbubble contrast agent, ideally through an angiocath, preferably 20 gauge, placed in an antecubital vein of the left arm. There are two commercially available ultrasound contrast agents suitable for CEUS LI-RADS characterization of focal liver observations: Definity (Lantheus Medical Imaging, Billerica, MA) and recently FDA-approved Lumason (Bracco Diagnostics Inc., Monroe Township, NJ). The dose is 0.2 ml for Definity and ml for Lumason, injected as a bolus followed by a 5 10 ml saline flush. These are guidelines and there are equipment-, transducer-, and patient-specific demands which may alter these choices. A single injection generally focuses on a single nodule with maintenance of the transducer in a fixed location throughout at least the arterial phase and often the entire scan. Scanning the identified nodule in the plane of respiratory movement optimizes visualization by reducing out-of-plane motion from respiration. Frequently, multiple injections can be performed with Definity and up to 2 injections may be performed from a single vial of Lumason. Repeat injections may focus on the original nodule or other nodules as required. In the portal venous/late phase of enhancement, continuous sweeps to encompass the entire liver are invaluable to look for any regions of washout which may indicate additional pathology. The timer is started at the beginning of the saline flush to coincide with the actual injection of the contrast agent. As a minimum requirement, continuous imaging should be performed from the beginning of contrast flush through peak AP enhancement with image recording performed from the first bubble arrival through peak AP enhancement. Optionally, imaging and recording can be continued beyond the AP peak enhancement until 60 s after contrast flush, to fully evaluate APHE and document early washout, which occurs before 1 min. After 1 min, intermittent imaging at s intervals should be performed until there is unequivocal clearance of microbubbles from the circulation at about 4 6 min after contrast injection to detect mild and late washout, a major feature for LR-5 categorization. Intermittent imaging is important to minimize microbubble destruction and to have adequate late-phase enhancement. A still image should be acquired at 1 minute and at regular intervals following. Major features of CEUS LI-RADS Arterial phase hyperenhancement (APHE) Arterial phase hyperenhancement (APHE) refers to arterial phase enhancement that is unequivocally greater than the background liver and does not show rim-like or peripheral discontinuous globular morphology. This feature can be considered present if it is demonstrated in either the entire nodule or in only a portion of the nodule (Fig. 1). Regardless of the extent of enhancement, the interpreter must be 100% confident arterial phase hyperenhancement is present prior to using this feature to categorize a nodule. This feature should be evaluated during the arterial phase of contrast enhancement usually occurring approximately to s after injection. APHE on CT or MRI could be seen in a wide variety of both benign and malignant focal liver observations including a wide variety of liver masses and arterioportal shunts (APS). Accurate diagnosis of APS on CT and MRI commonly presents substantial diagnostic challenges. APS are commonly visualized on both contrastenhanced CT and MRI in at-risk patients as ill-defined areas of APHE with no other associated findings on nonenhanced scans and show no washout on later phase images. Their appearance, therefore, is non-specific and either follow-up or other types of contrast-enhanced imaging may be required to confirm their benign nature. By comparison, APS are not visualized on either precontrast or on CEUS. Therefore, when APS is suspected, a routine greyscale US will generally not show any abnormality or nodule to correspond with the APHE shown on CT/MRI. A negative US, therefore, supports the notion that the APHE on the CT or MRI is indeed related to shunting rather than a nodule. In other situations, where US/CEUS is performed following CT or MRI showing a positive observation with APHE, CEUS will only be performed if a true nodule is identified on US. As the vast majority of observations subjected to CEUS examination are true nodules, the observation of APHE on CEUS is of much greater significance than is APHE observation on a CT or MRI. As a result, a liver mass visible on precontrast demonstrating a typical APHE pattern (not rim or peripheral discontinuous globular) on CEUS should be characterized as a typical lesion of hepatocellular origin (CEUS LR-3, LR-4, or LR-5). An additional unique benefit of CEUS for the assessment of nodules in an at-risk liver is the exquisite demonstration of the morphology of the arteries in the nodule at the time of washin of contrast in the early arterial phase. This is optimized with the selection of a
4 Fig. 1. Major feature of CEUS LI-RADS, APHE. A Schematics and associated CEUS images show diffuse APHE, characteristic of a small HCC (arrows), and B a nodule-in-nodule APHE, also a characteristic of HCC. These are classic features for LR-5. C Rim enhancement in the arterial phase is one of the requirements for the designation of LR-M. bubble tracking option, available on many US systems. Dysmorphic vessel morphology (Fig. 2) and centripetal filling of a nodule are both associated with HCC. Washout Washout is the popular term for the visually assessed temporal reduction in enhancement of a nodule, in whole or in part, relative to the liver beginning in or after the arterial phase and resulting in portal venous or late phase hypoenhancement. Washout can be applied to any enhancing observation even in the absence of APHE. On CT or MRI, the presence of washout is one of the major features for LR-5. On the other hand, on CEUS, all malignant lesions including HCC, ICC, and metastases have a strong tendency to show washout. Differentiation on CEUS between typical hepatocellular lesions (CEUS LR-3, LR-4, and LR-5) and malignant tumors with enhancement characteristics not specific for HCC (CEUS LR-M) relies on the onset and the degree of washout. Washout onset: Onset refers to the time after contrast injection at which washout is first detected, recorded precisely in seconds, relative to liver. When initial washout onset is detected within 60 s of contrast injection, it is characterized as early onset. When initial This pattern is common for ICC and also metastases, both included within LR-M. D Peripheral discontinuous globular enhancement is the classic pattern for a hemangioma which requires additionally also demonstration of sustained enhancement (Image reproduced with permission from the ACR). wahsout onset is detected at or after 60 s, it is characterized as late onset (Fig. 3). Washout degree: The degree of nodule washout is assessed by comparing the degree of contrast enhancement of the nodule relative to the surrounding liver. Marked washout is diagnosed when the liver nodule becomes virtually devoid of contrast ( punched-out ) within 2 min after contrast injection. Marked washout suggests a probable categorization as LR-M. Mild washout is diagnosed when the liver nodule becomes less enhanced than the surrounding liver, but still demonstrates some degree of persistent contrast enhancement. Nodules initially demonstrating mild washout might eventually become virtually devoid of contrast ( punched-out ). If this occurs within the first 2 min after contrast injection, it should be characterized as marked washout and LR-M should be considered. If this occurs after 2 min, the lesion is still categorized as showing mild washout. Hepatocellular carcinoma typically shows washout with late onset ( 60 s) and of mild degree, while nonhepatocellular lesions, including ICC, show early onset
5 Fig. 2. Differences in CEUS from CT/MRI. Real-time imaging shows dysmorphic vessels in HCC in a 53-year-old male with HBV cirrhosis. A A greyscale image shows a mildly heterogeneous mass (arrows). B, C, D, and E Sequential frames in the arterial phase, taken with a bubble tracking technique, showing dysmorphic vessels and a centripetal filling pattern to complete fill-in (not shown). There is APHE. F Weak washout at 1 min 30 s (Image reproduced with permission from the ACR). Fig. 3. Major feature of CEUS LI-RADS, washout. Schematics and images show the major features related to washout: TIMING and INTENSITY. A, B, Images showing a classic CEUS LR-5 (arrows) with APHE and late and weak washout, occurring after 1 min and appearing faded more than washed out. C, D Images showing a classic CEUS LR- M, a probably malignant tumor, with AP rim enhancement and marked punched-out washout occurring rapidly at 1 min (Image reproduced with permission from the ACR).
6 Untreated observation visible on pre-contrast US and without pathologic proof in patients at high risk for HCC If cannot be categorized due to image degradation or omission If tumor in vein (TIV) If definitely benign If probably benign Probably or definitely malignant, not specific for HCC* CEUS LR-NC CEUS LR-TIV CEUS LR-1 CEUS LR-2 CEUS LR-M Otherwise, use CEUS diagnostic table below If intermediate malignancy probability If probably HCC If definitely HCC CEUS LR-3 CEUS LR-4 CEUS LR-5 CEUS Diagnostic Table Arterial phase hyperenhancement (APHE) No APHE APHE ** Nodule size (mm) < < No washout of any type CEUS LR-3 CEUS LR-3 CEUS LR-3 CEUS LR-4 Late and mild washout CEUS LR-3 CEUS LR-4 CEUS LR-4 CEUS LR-5 * CEUS LR-M criteria: If rim APHE OR early (<60s) washout OR marked washout ** APHE: Not rim (indicates LR-M) Not peripheral discontinuous globular (indicates hemangioma) If unsure about the presence of any major feature: characterize that feature as absent Fig. 4. CEUS LI-RADS algorithm (Image reproduced with permission from the ACR). (<60 s) and/or marked washout. Therefore, on CEUS, it is critical to carefully evaluate the timing of onset and the degree of washout. In order to reliably assess the timing of washout onset, we recommend initial real-time imaging and dynamic acquisition with low mechanical index (MI) up to 60 s after contrast injection, and intermittent imaging afterwards. Microbubble contrast agents are destroyed by even low-energy US. While real-time imaging is critical to assess arterial phase enhancement, continuous scanning of a large area of liver after 60 s will result in increased contrast agent destruction with no additional benefit. After an initial 60 s continuous recording, intermittent imaging for a few seconds every s is recommended until near all contrast agent has disappeared from the circulation (usually 4 6 min after injection). This prolonged intermittent scanning is critical to detect late and mild washout, one of the major features of LR-5 nodules on CEUS. Indications CEUS is a valuable contributor to multimodality imaging for characterizing nodules in a cirrhotic liver [16]. CEUS may be used to. Assess nodules 10 mm detected at surveillance US; Assess LR-3, LR-4, and LR-M observations detected on prior CT or MRI; Characterize APHE for observations in which mistiming is suspected as the reason for its absence on prior CT or MRI; Assess biopsied observations with inconclusive histology;
7 Guide biopsy or treatment of lesions that are difficult to visualize with pre-contrast US; Help select the most appropriate observation(s) or observation component(s) for biopsy; Monitor changes in enhancement pattern over time for selected LR-3 or LR-4 observations; Differentiate tumor in vein ( tumor thrombus ) from bland thrombus; and. Monitor therapy for treatment of HCC, both intraprocedural and following therapy (not addressed in the current version of CEUS LI-RADS). CEUS is a focused exam and is not suitable for screening or surveillance. Rather, it is used to characterize lesion(s) identified on a screening and surveillance ultrasound or on CT/MRI. CEUS is also not suitable for staging the entire liver. Once a patient is diagnosed with any malignant lesion(s), a CECT or CEMRI is necessary for staging disease. The CEUS LI-RADS algorithm The CEUS LI-RADS algorithm is applied in a step-bystep manner to encompass the interpretation and reporting of all variety of imaging findings in patients at high risk for HCC. The algorithm (Fig. 4) is intended to be used from the first option through to the last option or the option which fits the observations in the case at hand, whichever occurs first. The algorithm includes, therefore, benign and malignant possibilities and provides different confidence levels for suggested diagnoses. CEUS LR-NC The first step of the CEUS LI-RADS Algorithm deals with the quality of the scan and the ability to make appropriate interpretations leading to an assignment to a specific category. Shortcomings of the technique or equipment and failures related to patient body habitus or observation size may all lead to an ultimate CEUS examination technical failure. Therefore, appropriate diagnostic features might not be documented or the observation may not be assigned an appropriate category and, therefore, should be classified instead as LI-RADS not categorizable or LR-NC. These determinations must be relayed to the referring physician with suggestions for their resolution, which most often involves recommendation for either contrast-enhanced CT or MRI. CEUS LR-TIV The next step in the algorithm is to evaluate for the presence of thrombus within the portal and/or hepatic veins. Identification of a soft tissue mass within the vein lumen associated with its APHE and then washout is diagnostic of tumor thrombus (Fig. 5). Avascularity of the thrombus, throughout all phases of enhancement, suggests bland thrombus, revascularization of which emphasizes the necessity of correctly timing the demonstration of enhancement and also the presence of washout. When TIV is present, indicate its likely etiology and describe vessel(s) involved. The majority of CEUS LR- TIV are HCC associated, but some may be related to ICC, H-ChC (hepatocholangiocarcinoma), or other non- HCC malignancies. If TIV is contiguous with a CEUS LR-M lesion, describe it as may be due to non-hcc malignancy. If TIV is contiguous with a CEUS LR-5 lesion, then describe it as definitely due to HCC. If TIV is contiguous with a CEUS LR-4 lesion or associated with an infiltrative mass, then describe it as probably due to HCC. Otherwise, describe it as of unknown etiology. If unsure about the presence of TIV, do not categorize as TIV. Management implications CEUS LR-TIV cases are usually referred to multi-disciplinary discussion (MDD) for consensus management. It may include alternative or repeat imaging, biopsy, or treatment. CEUS LR-1 Fig. 5. CEUS LR-TIV. A 59-year-old male with HCV cirrhosis and new onset of ascites. A Sagittal greyscale US image shows a focal echogenic large liver mass (M). There is a soft tissue mass within the ascending left portal vein (arrow). B In the arterial phase, there is hyperenhancement of both the portal vein thrombus and the mass (Image reproduced with permission from the ACR). The next step in the algorithmic approach is to categorize all lesions which are definitely benign, CEUS LR-1.
8 Fig. 6. CEUS LR-1, a flash-filling hemangioma. A 59-yearold female with chronic HBV and a nodule on outside surveillance US. A Contrast-enhanced T1-weighted MR scan in the arterial phase shows a slightly heterogeneous hyperenhancing nodule (arrow) in the liver. B The nodule (arrow) is homogenously hyperintense in the delayed phase. MR findings are indeterminate as the arterial phase enhancement pattern is non-specific and there is no washout. C A greyscale US image confirms the right lobe focal liver nodule with an Hemangiomas are felt to be less common in the cirrhotic liver than the normal liver, but their presence in cirrhosis is indisputable. They have variable B-mode appearance and may appear echogenic, as they most often do in the non-cirrhotic liver, or they may also be hypoechoic or even mixed in echogenicity. Fortunately, on CEUS, their features are classic including discontinuous globular peripheral enhancement followed by variable fill-in, which is generally sustained (Fig. 6). They occur most often in the patient with chronic hepatitis B infection and no cirrhosis but may also occur in the liver with cirrhosis and may additionally co-exist with HCC. Fast-filling hemangioma variant, with an increased incidence in small nodules, is most optimally studied with CEUS where the rapidly changing arterial phase enhancement is detected by the excellent temporal resolution of real-time CEUS. echogenic rim. D, E and F Sequential frames in the arterial phase of CEUS showing progressive peripheral nodular enhancement with centripetal filling to complete fill-in. There is sustained enhancement to 5 min, not shown (Reproduced from: Kim TK, Jang HJ, Wilson SR. Ultrasound of Hepatocellular Carcinoma: The Important Contribution of Contrast Enhancement. Hepatocellular Carcinoma Diagnosis and Treatment (2016). Editors: Carr, Brian I. (Ed.) Humana Press, Springer Science.). Focal fat deposition and focal fat sparing may also occur within an at-risk liver. The former is characterized by an echogenic nonmasslike, nonspherical observation on precontrast US with isovascularity in both the arterial and portal venous phases on CEUS with no washout (Fig. 7). The latter is characterized alternately by a hypoechoic observation on baseline again with isoenhancement throughout all phases of CEUS imaging. As with hemangioma, if all features on greyscale and CEUS are in agreement, these fat-related lesions may also be confidently categorized as CEUS LR-1. Simple cysts with classic benign morphology on greyscale US can be diagnosed as simple cysts without CEUS although more complex appearing lesions on the greyscale scan may require CEUS showing complete avascularity to be classified as CEUS LR-1.
9 Fig. 7. CEUS LR-1, a focal fat deposition. A 56-year-old male with alcohol cirrhosis. A A sagittal greyscale US image shows a severely fatty liver with a deep focal echogenic mass (arrow) measuring about 3 cm in diameter. B In the arterial phase of CEUS and C the portal venous phase, there is isovascularity of the mass with the adjacent liver. There is no APHE and there is no washout. This is diagnostic of focal fat (Image reproduced with permission from the ACR). Fig. 8. CEUS LR-2, a probably benign nodule. A 50-year-old female with HCV cirrhosis. A A greyscale US image of the left lobe of the liver shows at least 3-subcentimeter hypoechoic nodules (arrows). B AP shows isovascularity with no evidence of APHE. C An image from a sweep of the left lobe in the portal venous phase shows a homogeneous liver with no washout or other alteration. Frequently, CEUS will remove concern about nodules shown on the greyscale scan by its demonstration of homogeneously enhancing parenchyma in all phases of enhancement (Image reproduced with permission from the ACR). Management implications Patients with CEUS LR-1 may return to regular 6-month surveillance. CEUS LR-2 After the elimination from consideration of definitely benign lesions, the next step is to identify lesions which are probably benign, CEUS LR-2. Criteria for categorization as CEUS LR-2 are currently very stringent and require identification of the following: Distinct isoenhancing solid nodule <10 mm Nonmasslike isoenhancing observation of any size, not typical hepatic fat deposition/sparing LR-3 nodules with interval size stability for 2 years Since CEUS is generally recommended for characterization of definite nodules 10 mm, the vast majority of LR-2 nodules will be detected incidentally while performing CEUS for other observations. These small nodules are typical regenerative nodules and their probably benign categorization is useful and effective (Fig. 8). Nonmasslike isoenhancing observation of any size, not typical hepatic fat deposition/sparing would be categorized to LR-2. Additionally, any observation previously categorized as CEUS LR-3 with an interval size stability for 2 years may be categorized as CEUS LR-2. Observations that are not definitely benign (CEUS LR-1) and do not meet the above CEUS LR-2 criteria are categorized CEUS LR-3 or higher.
10 Fig. 9. CEUS LR-M, probably or definitely malignant nodule, not specific for HCC. A 78-year-old male with HBV and a growing nodule on MR, previously diagnosed 2 years earlier on MR as a hemangioma. Post-gadolinium MR images in A the arterial phase (arrow) and B the portal venous phase show obeservation with arterial phase enhancement with no washout in either the portal venous or the delayed Management implications Patients with CEUS LR-2 may return to regular 6-month surveillance. CEUS LR-M The next step is to identify CEUS LR-M, a probably or definitely malignant nodule, not necessarily HCC (Figs. 9). These observations show a distinct solid nodule on precontrast US, with at least some enhancement in the arterial phase. There is no size threshold for LR-M. Although CEUS is usually performed to assess nodules 10 mm detected on surveillance US, smaller nodules with LR-M features may be identified during CEUS and should be categorized LR-M. Any one of the following criteria mandates placement of the nodule in the CEUS LR-M category: Early washout relative to liver, within 60 s of contrast injection; Marked washout, resulting in a punched-out appearance within 2 min after contrast injection; Arterial phase rim enhancement, followed by washout (regardless of onset or degree). phase. C The hypoechoic mass is confirmed on greyscale US. D In the arterial phase of CEUS, the mass shows APHE. E There is rapid washout prior to 1 min, shown at 34 s. F The washout is marked at 4 min, discordant with the sustained enhancement on MRI. Biopsy following CEUS shows cholangiocarcinoma (Image reproduced with permission from the ACR). Management implications Management of CEUS LR- M nodules is variable, depending on the type of malignancy suspected. However, biopsy is frequently needed for a CEUS LR-M observation, as there is a lack of specificity for an imaging diagnosis. ICC, hepatocholangiocarcinoma, and metastases account for the majority of tumors characterized as CEUS LR-M. Some poorly differentiated HCCs may also show the enhancement pattern of CEUS LR-M, especially rapid washout (Fig. 10). It is unknown how many LR-M lesions are actually HCC. One retrospective study showed that 40% (6/15) of LR-M lesions were HCCs, 13% (2/15) were hepatocholangiocarcinomas, and 47% (7/15) were cholangiocarcinomas [17]. In our unpublished data, 35% (11/31) of LR-M lesions were HCCs. The CEUS LI-RADS diagnostic table The remaining considerations within the algorithm address identified nodules, which develop by the process of hepatocarcinogenesis in the at risk liver. There are three considerations for all of these nodules, which categorize them as follows:
11 Fig. 10. CEUS LR-M, biopsy-proven HCC. A 62-year-old male with HCV cirrhosis. A Surveillance US shows a focal hypoechoic nodule in segment 7 (arrows). B There is typical CEUS LR-3 intermediate malignancy probability, CEUS LR-4 probably HCC, and. CEUS LR-5 definitely HCC. This characterization is based on. Nodule size (<10, 10 20, and 20 mm), APHE (not rim or peripheral discontinuous globular), and. APHE at 25 s. C There is rapid mild washout at 35 s (Image reproduced with permission from the ACR). Washout, its presence, timing, and degree. Accurate assignment of nodules to the CEUS LR-3, LR-4, and LR-5 categories requires a constant familiarity and referral to the CEUS LI-RADS Diagnostic Table (Fig. 3), included within the algorithm. Fig. 11. CEUS LR-3, nodule 2 cm, no APHE, and no washout. A 64-yearold male with ethanolrelated cirrhosis. A A surveillance US scan shows an exophytic hypoechoic nodule measuring just over 2cm(arrows). B The nodule is isovascular at peak AP. C At 2 min and D at 4 min, the nodule remains isovascular with the adjacent parenchyma (Image reproduced with permission from the ACR).
12 CEUS LR-3 CEUS LR-3 nodules have an intermediate malignancy probability. They include nodules with a variety of sizes, with or without APHE, and with or without late and mild washout, making them a somewhat heterogeneous catch-all group intended to provide a conservative option which does not eliminate the possibility of malignancy. CEUS LR-3 includes distinct solid nodules 10 mm with isoenhancement in all phases, nodules <20 mm which do not show APHE but do show late washout onset ( 60 s) and mild degree of washout. CEUS LR-3 also includes nodules <10 mm which do show APHE (not rim or peripheral discontinuous globular) but no washout (Fig. 11). Management implications The suggested management of CT/MRI LR-3 observations is repeat imaging in 3 6 months or alternative imaging in 3 6 months. However, management implications for CEUS LR-3 nodules vary including alternative imaging, biopsy, or shorter interval surveillance. Additionally, they often require MDD. Two recent studies [18, 19] show that most LR-3 observations detected at CT or MRI are benign or indolent lesions that can be followed safely without requiring MDD in all cases. Less is known about the natural history of LR-3 observations detected at CEUS, but preliminary evidence suggests that such observations warrant closer scrutiny. By definition, all CEUS observations are distinctive nodules in a cirrhotic liver visible on pre-contrast B-mode images, which thus have high probability of being HCC, unless contrast enhancement features are diagnostic of a benign entity such as a hemangioma. A recent retrospective study [17] found that 60% (45/75) of CEUS LR-3 observations were HCC. Therefore, MDD should be considered for all CEUS LR-3 observations, because biopsy or alternative imaging in less than 3 months may be appropriate. CEUS LR-4 CEUS LR-4 nodules are probably HCC. They are highly suspicious for HCC but lack the precise requirements for this diagnosis. They include nodules with APHE (not rim or peripheral discontinuous globular) but no washout measuring 10 mm and those with APHE (not rim or peripheral discontinuous globular), late washout onset ( 60 s), and mild degree of washout but measuring <10 mm. Nodules 20 mm with no APHE but with late washout onset ( 60 s) and mild degree of washout may also be characterized as CEUS LR-4 (Fig. 12). Fig. 12. CEUS LR-4, probably HCC. A 27-yearold male with cryptogenic cirrhosis. A surveillance US shows two nodules between 10 and 20 mm. A The greyscale US confirming two hypoechoic nodules (arrows). B There is typical APHE. C At 2.5 min, the nodules remain hyperenhanced. D At 5 min, the liver is now poorly enhanced. The nodules remain slightly more enhanced than the parenchyma. There is no washout. Subsequent biopsy is negative for HCC and short interval surveillance has continued to show interval stability for over 1 year (Image reproduced with permission from the ACR).
13 Fig. 13. CEUS LR-5, definitely HCC. A 64-yearold male with HCV cirrhosis. A Surveillance US shows a focal hypoechoic nodule measuring 1.7 cm (arrows). B There is typical APHE. C There is mild washout at 1.5 min. D At 4.5 min, there is a marked washout which does not influence the categorization. Biopsy following CEUS shows HCC (Image reproduced with permission from the ACR). This category, CEUS LR-4, emphasizes the importance of typical APHE on CEUS, which is predominantly associated with nodules of hepatocellular origin, unlike CT or MRI where APHE is often detected in APS in the cirrhotic liver. On CT and MRI, observations with APHE often represent APS [20], and therefore it is essential to have portal venous phase washout for diagnosis of HCC. CEUS, by comparison, does not show abnormality in the presence of known APS. Therefore, the significance of identification of a nodule with typical APHE alone on CEUS as a predictor of HCC is high [2]. Management implications CEUS LR-4 nodules are probable HCC, but not with 100% probability; therefore, these nodules require either biopsy, treatment, or short interval follow-up. CEUS LR-5 CEUS LR-5 is definitely HCC with nearly 100% probability, and therefore confirmation with biopsy prior to treatment is deemed to be unnecessary. The diagnosis of HCC has rigorous criteria, all of which must be present for this categorization. There are three essential criteria including a size 10 mm, typical APHE (not rim or peripheral discontinuous globular), and late washout onset ( 60 s) with mild washout degree (Fig. 13). Management implications CEUS LR-5 nodules may undergo locoregional therapy, surgical resection, or transplantation without requirement for tissue diagnosis. Ancillary features and tie-breaking rules Upon completion of the algorithm categorization, ancillary features (Fig. 14) may be used at the interpreter s discretion to increase diagnostic confidence, or to adjust a LR category. Use of ancillary features may be used to upgrade or downgrade a category, but may not be used to upgrade any nodule to LR-5. Although ancillary features are applied less often on CEUS than on CT and MRI, they are nonetheless very important. Ancillary features favoring malignancy, without specificity for HCC, include definite interval size increase, whereas definite interval size reduction or stability 2 years favor benignancy. Features favoring HCC, in particular, include a mosaic appearance of the nodule and a nodule-in-nodule appearance in the arterial phase.
14 CEUS ancillary features may be used Increased confidence or category adjustment for: For category adjustment (upgrade or downgrade), apply CEUS AF as follows 1 AF favoring malignancy: upgrade by 1 category up to LR-4 (Absence of these AFs should not be used to downgrade) CEUS LR-1 CEUS LR-2 CEUS LR-3 CEUS LR-4 LR-5CEUS 1 AF favoring benignity: downgrade by 1 category If there are conflicting AFs (i.e., 1 AF favoring malignancy and 1 AF favoring benignity): Do not change category AFs cannot be be used to upgrade to LR-5 CEUS AF favoring malignancy Favoring malignancy in general, not HCC in particular Definite growth Favoring HCC in particular Nodule-in-nodule architecture Mosaic architecture CEUS AF favoring benignity Size stability 2 years Size reduction If unsure about presence of any ancillary feature: characterize that feature as absent Fig. 14. Ancillary features and tie-breaking rules of CEUS LI-RADS (Image reproduced with permission from the ACR). Tie-breaking rules If after full categorization there is a dilemma between two categories, always choose the category reflecting lower certainty as below (Fig. 15). Final check Upon completion of the categorization of the nodule, consider its reasonability and accuracy. If the category seems appropriate, then you are done. If not, reevaluate. Discussion CEUS is a new addition to LI-RADS. Although it is very similar to the original LI-RADS for CT and MRI, CEUS has distinct differences. It is important to understand the difference of CEUS from CT and MRI, and its advantages and limitations not only to interpret and use CEUS correctly, but also to take advantage of the unique capabilities of CEUS. Key differences of CEUS from CT and MRI are summarized in this article. In a meta-analysis evaluating the test performance of imaging modalities for HCC, Chou et al. concluded that there were no differences in sensitivity among CEUS, CT, and MRI [6]. In a meta-analysis assessing the accuracy of diagnosis of small HCC by CEUS [21], we evaluated 6 references which had less stringent criteria than current CEUS LI-RADS, as they included only identification of washout, without consideration of timing or degree. However, these less stringent criteria still provided high specificity (99%) and PPV (97%) for 1- to 2-cm HCC. Sensitivity for smaller HCC was 62%. Falsepositive diagnosis of ICC as HCC was rare. However, the described studies include only 2 ICCs. The data from Terzi, E., et al., suggest that the probability of HCC for each CEUS LR category fits
15 Fig. 15. Ancillary Feature of CEUS LI-RADS, nodule-innodule architecture. A 54-year-old male with HCV cirrhosis. A A surveillance US shows an exophytic nodule (arrow) at the tip of the left lobe. B In the early AP of CEUS, there is a small hypervascular nodule (arrow) within a larger hypoechoic nodule, appearing black. C By 23 s, the entire nodule is hyperenhanced. D At 5 min, there is washout corresponding with the initial hypervascular nodule. The remainder of the nodule remains isoenhanced. Although the area of initial hyperenhancement and late and mild washout is small and less than 1 cm, the entire nodule is greater than 1 cm. This is APHE in part, as well as washout in part, major features for LR-5. Therefore, this is a CEUS LI-RADS 5 lesion, confirmed HCC by biopsy at RFA (Image reproduced with permission from the ACR). within the intended probability of HCC: LR-1 0%, LR-2 <20%, LR %, LR %, and LR-5 100% [17]. Management suggestions for CEUS are the same in all categories with CT and MRI except for the category CEUS LR-3. Currently, HCC probability of CEUS LR- 3 seems to be higher than that of CT and MRI, with LR- 3, 45/75 (60%) in the Terzi study. When nodules are seen by ultrasound, they are true nodules and, therefore, the pretest probability of HCC is high. Multicenter, prospective studies are needed to validate CEUS LI- RADS criteria. We present several important indications of CEUS for characterizing nodules in a cirrhotic liver. CEUS can be used as the first step to characterize nodule(s) detected on HCC surveillance US, which will allow prompt evaluation of the nodule(s), avoiding misregistration. Further, it will avoid unnecessary further imaging for benign lesions. CEUS will also add complementary or additional information to CT or MRI for suspect APS, and CEUS, performed for negative or indeterminate nodules from CT or MR imaging, provides more noninvasive diagnoses prior to consideration of biopsy [22]. Limitations of CEUS include unsuitability for HCC staging. Therefore, once a patient is diagnosed with a malignant lesion(s), either HCC or other malignancy, a CECT or CEMRI is necessary for staging disease. Further, inaccessibility of subdiaphragmatic or deep lesions, limited penetration in large patients, and signal attenuation in patients with severe hepatic steatosis, and infrequent interference of bowel or gastric gas may also limit the success of CEUS. Although CEUS has been used for liver lesion characterization and for other indications for many years
16 worldwide, it is fairly new in the United States. CEUS LI-RADS will improve the integration of CEUS into the multimodality approach for the study of the liver at risk for HCC, providing unique and complimentary information to CT and MRI. Acknowledgement Images are from the University of Calgary using the contrast agent Definity (Lantheus Medical Imaging, Billerica MA). References 1. Wilson SR, Jang HJ, Kim TK, Burns PN (2007) Diagnosis of focal liver masses on ultrasonography: comparison of unenhanced and contrast-enhanced scans. J Ultrasound Med 26(6): Jang HJ, Kim TK, Wilson SR (2009) Small nodules (1-2 cm) in liver cirrhosis: characterization with contrast-enhanced ultrasound. Eur J Radiol 72(3): doi: /j.ejrad Strobel D, Seitz K, Blank W, et al. (2009) Tumor-specific vascularization pattern of liver metastasis, hepatocellular carcinoma, hemangioma and focal nodular hyperplasia in the differential diagnosis of 1,349 liver lesions in contrast-enhanced ultrasound (CEUS). Ultraschall Med 30(4): doi: /s Niu Y, Huang T, Lian F, Li F (2013) Contrast-enhanced ultrasonography for the diagnosis of small hepatocellular carcinoma: a meta-analysis and meta-regression analysis. Tumour Biol 34(6): doi: /s z 5. Hanna RF, Miloushev VZ, Tang A, et al. (2016) Comparative 13-year meta-analysis of the sensitivity and positive predictive value of ultrasound, CT, and MRI for detecting hepatocellular carcinoma. Abdom Radiol 41(1):71 90 ((NY)). doi: /s Chou R, Cuevas C, Fu R, et al. (2015) Imaging techniques for the diagnosis of hepatocellular carcinoma: a systematic review and meta-analysis. Ann Intern Med 162(10): doi: /M Guang Y, Xie L, Ding H, Cai A, Huang Y (2011) Diagnosis value of focal liver lesions with SonoVue(R)-enhanced ultrasound compared with contrast-enhanced computed tomography and contrastenhanced MRI: a meta-analysis. J Cancer Res Clin Oncol 137(11): doi: /s Xie L, Guang Y, Ding H, Cai A, Huang Y (2011) Diagnostic value of contrast-enhanced ultrasound, computed tomography and magnetic resonance imaging for focal liver lesions: a meta-analysis. Ultrasound Med Biol 37(6): doi: /j.ultrasmedbio Vilana R, Forner A, Bianchi L, et al. (2010) Intrahepatic peripheral cholangiocarcinoma in cirrhosis patients may display a vascular pattern similar to hepatocellular carcinoma on contrast-enhanced ultrasound. Hepatology 51(6): doi: /hep Li R, Yuan MX, Ma KS, et al. (2014) Detailed analysis of temporal features on contrast enhanced ultrasound may help differentiate intrahepatic cholangiocarcinoma from hepatocellular carcinoma in cirrhosis. PLoS One 9(5):e doi: /journal.pone Wildner D, Bernatik T, Greis C, et al. (2015) CEUS in hepatocellular carcinoma and intrahepatic cholangiocellular carcinoma in 320 patients early or late washout matters: a subanalysis of the DEGUM multicenter trial. Ultraschall Med 36(2): doi: /s Kono Y, Cosgrove D, Dietrich C, Jang HJ, Kim TK, Lyshchik A, Piscaglia F, Sirlin C, Willmann JK, Wilson S (2016) Contrast-enhanced ultrasound liver imaging reporting and data system for diagnosis of hepatocellular carcinoma: initial proposal. In: American Institute of Ultrasound in Medicine, New York. 16 Mar Mar vol suppl. p S Jang HJ, Kono Y, Sirlin C, et al. (2015) Incorporation of CEUS into LI-RADS for diagnosis of hepatocellular carcinoma (HCC): a work in progress. In: Radiological Society of North America, Chicago, 29 Nov Dec Piscaglia F (2016) The new American CEUS LI-RADS classification of focal lesions in cirrhosis. In: Euroson Congress of the EF- SUMB, Leipsig, Germany, Oct Wilson SR, Kim TK, Jang HJ, Burns PN (2007) Enhancement patterns of focal liver masses: discordance between contrast-enhanced sonography and contrast-enhanced CT and MRI. AJR Am J Roentgenol 189(1):W7 W12. doi: /ajr Claudon M, Dietrich CF, Choi BI, et al. (2013) Guidelines and good clinical practice recommendations for Contrast Enhanced Ultrasound (CEUS) in the liver update 2012: a WFUMB-EF- SUMB initiative in cooperation with representatives of AFSUMB, AIUM, ASUM, FLAUS and ICUS. Ultrasound Med Biol 39(2): doi: /j.ultrasmedbio Terzi E, De Bonis L, Leoni S, et al. (2017) CEUS LI-RADS are effective in predicting the risk hepatocellular carcinoma of liver nodules. Dig Liver Dis 49(Suppl 1):e Choi J-Y, Cho HC, Sun M, Kim HC, Sirlin CB (2013) Indeterminate observations (liver imaging reporting and data system category 3) on MRI in the cirrhotic liver: fate and clinical implications. AJR Am J Roentgenol 201(5): Tanabe M, Kanki A, Wolfson T, et al. (2016) Imaging outcomes of liver imaging reporting and data system version 2014 category 2, 3, and 4 observations detected at CT and MR imaging. Radiology 281(1): Galia M, Taibbi A, Marin D, et al. (2014) Focal lesions in cirrhotic liver: what else beyond hepatocellular carcinoma? Diagn Interv Radiol 20(3): doi: /dir Kono Y, Cosgrove D, Dietrich CF, Jang HJ, Kim TK, Lyshchik A, Piscaglia F, Sirlin CB, Vezeridis A, Willmann JK, Wilson SR (2016) Metaanalysis of diagnostic performance of CEUS LI-RADS Ò criteria for diagnosis of 2 cm hepatocellular carcinoma. In: AASLD Annual Meeting 2016, Boston 22. Jo PC, Jang HJ, Burns PN, et al. (2017) Integration of contrastenhanced US into a multimodality approach to imaging of nodules in a cirrhotic liver: how i do it. Radiology 282(2):
LI-RADS v2016 Key Dates
 Key Dates April 2014: ACR CEUS LI-RADS working group was formed Chair: Yuko Kono, Co-chair: Andrej Lyshchik Members: David Cosgrove, Christoph Dietrich, Hyun-Jung Jang, Tae Kim, Fabio Piscaglia, Claude
Key Dates April 2014: ACR CEUS LI-RADS working group was formed Chair: Yuko Kono, Co-chair: Andrej Lyshchik Members: David Cosgrove, Christoph Dietrich, Hyun-Jung Jang, Tae Kim, Fabio Piscaglia, Claude
Management. Chapter 11. Primary Author. Contributing Authors. University of Toronto & University of Ottawa. Illustrators & figure contributors
 Chapter 11 Primary Author Donald G. Mitchell Thomas Jefferson University Contributing Authors Victoria Chernyak Ania Z. Kielar Yuko Kono Claude B. Sirlin Montefiore Medical Center University of Toronto
Chapter 11 Primary Author Donald G. Mitchell Thomas Jefferson University Contributing Authors Victoria Chernyak Ania Z. Kielar Yuko Kono Claude B. Sirlin Montefiore Medical Center University of Toronto
Objectives. LI-RADS v2017. Working Groups. Cynthia Santillan. Released October 2014 Diagnosis. Screening/ Surveillance. Diagnosis
 LR-NC Cynthia Santillan LR-TIV Objectives 1. To teach participants how to apply the Liver Imaging Reporting and Data System () to their interpretation of imaging studies for the evaluation of hepatocellular
LR-NC Cynthia Santillan LR-TIV Objectives 1. To teach participants how to apply the Liver Imaging Reporting and Data System () to their interpretation of imaging studies for the evaluation of hepatocellular
Modern liver imaging techniques - A new era in liver ultrasound
 Modern liver imaging techniques - A new era in liver ultrasound Yuko Kono, M.D., Ph.D. Clinical Professor Departments of Medicine and Radiology University of California, San Diego San Diego, USA How to
Modern liver imaging techniques - A new era in liver ultrasound Yuko Kono, M.D., Ph.D. Clinical Professor Departments of Medicine and Radiology University of California, San Diego San Diego, USA How to
Mædica - a Journal of Clinical Medicine
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS How Often Hepatocellular Carcinoma Has a Typical Pattern in Contrast Enhanced Ultrasound? Alina MARTIE, MD; Ioan SPOREA, MD, PhD; Roxana SIRLI, MD,
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS How Often Hepatocellular Carcinoma Has a Typical Pattern in Contrast Enhanced Ultrasound? Alina MARTIE, MD; Ioan SPOREA, MD, PhD; Roxana SIRLI, MD,
The Contribution of Contrast Enhanced Ultrasound for the characterization of benign liver lesions in clinical practice a monocentric experience
 Original papers Med Ultrason 2012, Vol. 14, no. 4, 283-287 The Contribution of Contrast Enhanced Ultrasound for the characterization of benign liver lesions in clinical practice a monocentric experience
Original papers Med Ultrason 2012, Vol. 14, no. 4, 283-287 The Contribution of Contrast Enhanced Ultrasound for the characterization of benign liver lesions in clinical practice a monocentric experience
HCC e CEUS. Prof. A. Giorgio. Direttore IX UOC di Malattie Infettive ad Indirizzo Ecointerventistico
 HCC e CEUS Prof. A. Giorgio Direttore IX UOC di Malattie Infettive ad Indirizzo Ecointerventistico The natural history of compensated cirrhosis due to hepatitis C virus: a 17 year cohort study of 214 patients
HCC e CEUS Prof. A. Giorgio Direttore IX UOC di Malattie Infettive ad Indirizzo Ecointerventistico The natural history of compensated cirrhosis due to hepatitis C virus: a 17 year cohort study of 214 patients
INTRODUCTION. Key Words: Contrast enhanced ultrasonography; Liver masses. ORiginal Article
 Gut and Liver, Vol. 8, No. 3, May 2014, pp. 292-297 ORiginal Article Clinically Useful Diagnostic Tool of Contrast Enhanced Ultrasonography for Focal Liver Masses: Comparison to Computed Tomography and
Gut and Liver, Vol. 8, No. 3, May 2014, pp. 292-297 ORiginal Article Clinically Useful Diagnostic Tool of Contrast Enhanced Ultrasonography for Focal Liver Masses: Comparison to Computed Tomography and
Contrast Enhanced Ultrasound of Parenchymal Masses in Children
 Contrast Enhanced Ultrasound of Parenchymal Masses in Children Sue C Kaste, DO On behalf of Beth McCarville, MD St. Jude Children s Research Hospital Memphis, TN Overview Share St. Jude experience with
Contrast Enhanced Ultrasound of Parenchymal Masses in Children Sue C Kaste, DO On behalf of Beth McCarville, MD St. Jude Children s Research Hospital Memphis, TN Overview Share St. Jude experience with
US LI-RADS v2017 CORE
 US LI-RADS v2017 CORE Screening or surveillance US in patient at high risk for HCC US category US-1 US-2 US-3 Negative Subthreshold Positive Category Concept Definition US-1 Negative US-2 Subthreshold
US LI-RADS v2017 CORE Screening or surveillance US in patient at high risk for HCC US category US-1 US-2 US-3 Negative Subthreshold Positive Category Concept Definition US-1 Negative US-2 Subthreshold
CT/MRI LI-RADS v2017 CORE
 CT/MRI LI-RADS v2017 CORE Untreated observation without pathologic proof in patient at high risk for HCC If cannot be categorized due to image degradation or omission If definite tumor in vein (TIV) If
CT/MRI LI-RADS v2017 CORE Untreated observation without pathologic proof in patient at high risk for HCC If cannot be categorized due to image degradation or omission If definite tumor in vein (TIV) If
Talking To Your Hepatologists & Colleagues About LI-RADS. Joseph Yacoub MD & Claude Sirlin MD SCBT-MR 2017 Workshop
 Talking To Your Hepatologists & Colleagues About LI-RADS Joseph Yacoub MD & Claude Sirlin MD SCBT-MR 2017 Workshop What is LI-RADS? System for standardizing technique, interpretation, and reporting For
Talking To Your Hepatologists & Colleagues About LI-RADS Joseph Yacoub MD & Claude Sirlin MD SCBT-MR 2017 Workshop What is LI-RADS? System for standardizing technique, interpretation, and reporting For
Objectives. HCC Incidence and Mortality. Disclosure Statement HCC. Imaging of Hepatocellular Carcinoma. Treatment of Hepatocellular Carcinoma
 Imaging of Hepatocellular Carcinoma and the use of LI RADS Treatment of Hepatocellular Carcinoma Aaron D. Anderson, D.O. AOCR April 2015 Objectives Show how the use of LI RADS can simplify the diagnosis
Imaging of Hepatocellular Carcinoma and the use of LI RADS Treatment of Hepatocellular Carcinoma Aaron D. Anderson, D.O. AOCR April 2015 Objectives Show how the use of LI RADS can simplify the diagnosis
LIVER IMAGING TIPS IN VARIOUS MODALITIES. M.Vlychou, MD, PhD Assoc. Professor of Radiology University of Thessaly
 LIVER IMAGING TIPS IN VARIOUS MODALITIES M.Vlychou, MD, PhD Assoc. Professor of Radiology University of Thessaly Hepatocellular carcinoma is a common malignancy for which prevention, screening, diagnosis,
LIVER IMAGING TIPS IN VARIOUS MODALITIES M.Vlychou, MD, PhD Assoc. Professor of Radiology University of Thessaly Hepatocellular carcinoma is a common malignancy for which prevention, screening, diagnosis,
Simplifying liver assessment in internal medicine
 Ultrasound Customer story Simplifying liver assessment in internal medicine Philips Affiniti ultrasound for elastography and contrast-enhanced ultrasound (CEUS) Where Sonography Institute, Uster, Switzerland
Ultrasound Customer story Simplifying liver assessment in internal medicine Philips Affiniti ultrasound for elastography and contrast-enhanced ultrasound (CEUS) Where Sonography Institute, Uster, Switzerland
Imaging-Based Diagnostic Systems for Hepatocellular Carcinoma
 Gastrointestinal Imaging Review Cruite et al. Imaging-Based Diagnosis of Hepatocellular Carcinoma Gastrointestinal Imaging Review FOCUS ON: Irene Cruite 1 An Tang 2 Claude B. Sirlin 3 Cruite I, Tang A,
Gastrointestinal Imaging Review Cruite et al. Imaging-Based Diagnosis of Hepatocellular Carcinoma Gastrointestinal Imaging Review FOCUS ON: Irene Cruite 1 An Tang 2 Claude B. Sirlin 3 Cruite I, Tang A,
RICCARDO LENCIONI,CLOTILDE DELLA PINA, LAURA CROCETTI,DANIA CIONI. Chapter 1
 RICCARDO LENCIONI,CLOTILDE DELLA PINA, LAURA CROCETTI,DANIA CIONI Chapter 1 Impact of European Federation of Societies for Ultrasound in Medicine and Biology (EFSUMB) Guidelines on the Use of Contrast
RICCARDO LENCIONI,CLOTILDE DELLA PINA, LAURA CROCETTI,DANIA CIONI Chapter 1 Impact of European Federation of Societies for Ultrasound in Medicine and Biology (EFSUMB) Guidelines on the Use of Contrast
Alice Fung, MD Oregon Health and Science University
 Alice Fung, MD Oregon Health and Science University Disclosure Comments The speaker Alice Fung, MD Has relevant financial relationships to disclose. Received honorarium from (Guerbet). This individual
Alice Fung, MD Oregon Health and Science University Disclosure Comments The speaker Alice Fung, MD Has relevant financial relationships to disclose. Received honorarium from (Guerbet). This individual
LI-RADS Reporting. Chapter 14. Primary Authors. Contributing Authors. Memorial Sloan Kettering Cancer Center
 Chapter 14 LI-RADS Primary Authors Victoria Chernyak Mustafa R. Bashir Montefiore Medical Center Duke University Medical Center Contributing Authors Richard K. Do Aya Kamaya Ania Z. Kielar Donald G. Mitchell
Chapter 14 LI-RADS Primary Authors Victoria Chernyak Mustafa R. Bashir Montefiore Medical Center Duke University Medical Center Contributing Authors Richard K. Do Aya Kamaya Ania Z. Kielar Donald G. Mitchell
Innovations in HCC Imaging: MDCT/MRI
 Innovations in HCC Imaging: MDCT/MRI Anthony E. Cheng, M.D. Cardinal MRI Center Cardinal Santos Medical Center, Wilson Street, San Juan Innovations in HCC Imaging: Goals/Objectives MDCT/MRI Learn the diagnostic
Innovations in HCC Imaging: MDCT/MRI Anthony E. Cheng, M.D. Cardinal MRI Center Cardinal Santos Medical Center, Wilson Street, San Juan Innovations in HCC Imaging: Goals/Objectives MDCT/MRI Learn the diagnostic
Hepatic Imaging: What Every Practitioner Should Know
 Hepatic Imaging: What Every Practitioner Should Know Shuchi K. Rodgers, MD Section Chief, Abdominal Imaging Director of Ultrasound Department of Radiology Einstein Medical Center rodgerss@einstein.edu
Hepatic Imaging: What Every Practitioner Should Know Shuchi K. Rodgers, MD Section Chief, Abdominal Imaging Director of Ultrasound Department of Radiology Einstein Medical Center rodgerss@einstein.edu
The UGent Institutional Repository is the electronic archiving and dissemination platform for
 biblio.ugent.be The UGent Institutional Repository is the electronic archiving and dissemination platform for all UGent research publications. Ghent University has implemented a mandate stipulating that
biblio.ugent.be The UGent Institutional Repository is the electronic archiving and dissemination platform for all UGent research publications. Ghent University has implemented a mandate stipulating that
Liver Imaging Reporting and Data System LI-RADS v A Pictorial Review of the Categories on CT and MRI
 Liver Imaging Reporting and Data System LI-RADS v2014 - A Pictorial Review of the Categories on CT and MRI Poster No.: C-1584 Congress: ECR 2017 Type: Educational Exhibit Authors: M. El Hawari, K. Ali,
Liver Imaging Reporting and Data System LI-RADS v2014 - A Pictorial Review of the Categories on CT and MRI Poster No.: C-1584 Congress: ECR 2017 Type: Educational Exhibit Authors: M. El Hawari, K. Ali,
The Focal Hepatic Lesion: Radiologic Assessment
 The Focal Hepatic Lesion: Radiologic Assessment Kevin Kuo, Harvard Medical School Year III Our Patient: PS 67 y/o female w/ long history of alcohol use Drinking since age 18, up to one bottle of wine/day
The Focal Hepatic Lesion: Radiologic Assessment Kevin Kuo, Harvard Medical School Year III Our Patient: PS 67 y/o female w/ long history of alcohol use Drinking since age 18, up to one bottle of wine/day
Characterization of Focal Liver Lesions using Contrast Enhanced Ultrasound as a First Line Method: a Large Monocentric Experience
 ORIGINAL PAPER Characterization of Focal Liver Lesions using Contrast Enhanced Ultrasound as a First Line Method: a Large Monocentric Experience Ioan Sporea, Alina Martie, Simona Bota, Roxana Șirli, Alina
ORIGINAL PAPER Characterization of Focal Liver Lesions using Contrast Enhanced Ultrasound as a First Line Method: a Large Monocentric Experience Ioan Sporea, Alina Martie, Simona Bota, Roxana Șirli, Alina
Fusion Ultrasound: Characterization of Abdominal Masses with MR, CT, PET, and Contrast Ultrasound
 Fusion Ultrasound: Characterization of Abdominal Masses with MR, CT, PET, and Contrast Ultrasound Mollie Rashid, MD Corinne Deurdulian, MD Hisham Tchelepi, MD Keck School of Medicine, University of Southern
Fusion Ultrasound: Characterization of Abdominal Masses with MR, CT, PET, and Contrast Ultrasound Mollie Rashid, MD Corinne Deurdulian, MD Hisham Tchelepi, MD Keck School of Medicine, University of Southern
HCC and mass effect. Hepatocellular cancer: what if the AFP is rising but no lesion seen on imaging? What you need to know about AFP.
 Hepatocellular cancer: what if the AFP is rising but no lesion seen on imaging? Arun J Sanyal M.B.B.S., M.D. Charles Caravati Professor of Medicine Virginia Commonwealth University Imaging features used
Hepatocellular cancer: what if the AFP is rising but no lesion seen on imaging? Arun J Sanyal M.B.B.S., M.D. Charles Caravati Professor of Medicine Virginia Commonwealth University Imaging features used
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Report for Guidance Executive
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Centre for Health Technology Evaluation Report for Guidance Executive Review of DG5: SonoVue (sulphur hexafluoride microbubbles) - contrast agent for contrast
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Centre for Health Technology Evaluation Report for Guidance Executive Review of DG5: SonoVue (sulphur hexafluoride microbubbles) - contrast agent for contrast
Jesse Civan, M.D. Medical Director, Jefferson Liver Tumor Center
 Liver Tumors Jesse Civan, M.D. Medical Director, Jefferson Liver Tumor Center Differential Diagnosis Malignant Metastatic from non-hepatic primary Hepatocellular carcinoma Cholangiocarcinoma Biliary cystcarcinoma
Liver Tumors Jesse Civan, M.D. Medical Director, Jefferson Liver Tumor Center Differential Diagnosis Malignant Metastatic from non-hepatic primary Hepatocellular carcinoma Cholangiocarcinoma Biliary cystcarcinoma
Liver imaging takes a step forward with Ingenia
 Publication for the Philips MRI Community ISSUE 49 2013 / 2 Liver imaging takes a step forward with Ingenia Lyon South Hospital strives to move from several studies first CT, then MR or PET to using just
Publication for the Philips MRI Community ISSUE 49 2013 / 2 Liver imaging takes a step forward with Ingenia Lyon South Hospital strives to move from several studies first CT, then MR or PET to using just
Hepatocellular Carcinoma. Markus Heim Basel
 Hepatocellular Carcinoma Markus Heim Basel Outline 1. Epidemiology 2. Surveillance 3. (Diagnosis) 4. Staging 5. Treatment Epidemiology of HCC Worldwide, liver cancer is the sixth most common cancer (749
Hepatocellular Carcinoma Markus Heim Basel Outline 1. Epidemiology 2. Surveillance 3. (Diagnosis) 4. Staging 5. Treatment Epidemiology of HCC Worldwide, liver cancer is the sixth most common cancer (749
U ltrasonography (US) is reported to be the primary
 401 LIVER Improved characterisation of histologically proven liver tumours by contrast enhanced ultrasonography during the portal venous and specific late phase of SHU 508A C F Dietrich, A Ignee, J Trojan,
401 LIVER Improved characterisation of histologically proven liver tumours by contrast enhanced ultrasonography during the portal venous and specific late phase of SHU 508A C F Dietrich, A Ignee, J Trojan,
Guideline 11. Content. Abstract! List of abbreviations
 Guideline 11 Guidelines and Good Clinical Practice Recommendations for Contrast Enhanced Ultrasound (CEUS) in the Liver Update 2012 A WFUMB-EFSUMB Initiative in Cooperation With Representatives of AFSUMB,
Guideline 11 Guidelines and Good Clinical Practice Recommendations for Contrast Enhanced Ultrasound (CEUS) in the Liver Update 2012 A WFUMB-EFSUMB Initiative in Cooperation With Representatives of AFSUMB,
Evaluation of contrast-enhanced ultrasound for diagnosis of dysplastic nodules with a focus of hepatocellular carcinoma in liver cirrhosis patients
 Original Article Evaluation of contrast-enhanced ultrasound for diagnosis of dysplastic nodules with a focus of hepatocellular carcinoma in liver cirrhosis patients Wei Wu, Minhua Chen, Kun Yan, Yin Dai,
Original Article Evaluation of contrast-enhanced ultrasound for diagnosis of dysplastic nodules with a focus of hepatocellular carcinoma in liver cirrhosis patients Wei Wu, Minhua Chen, Kun Yan, Yin Dai,
*, Meng-Xia Yuan, Kuan-sheng Ma, Xiao-Wu Li, Chun-Lin Tang, Xiao-Hang Zhang, De-Yu Guo, Xiao-Chu Yan. Abstract. Introduction
 Detailed Analysis of Temporal Features on Contrast Enhanced Ultrasound May Help Differentiate Intrahepatic Cholangiocarcinoma from Hepatocellular Carcinoma in Cirrhosis Rui Li 1 1 2 2 1 1 *, Meng-Xia Yuan,
Detailed Analysis of Temporal Features on Contrast Enhanced Ultrasound May Help Differentiate Intrahepatic Cholangiocarcinoma from Hepatocellular Carcinoma in Cirrhosis Rui Li 1 1 2 2 1 1 *, Meng-Xia Yuan,
With the widespread use of hepatic imaging, liver masses
 2B: Liver Assessment of the Liver Mass: What Do You Need to Know? With the widespread use of hepatic imaging, liver masses are detected either unexpectedly or in the course of screening for liver cancer
2B: Liver Assessment of the Liver Mass: What Do You Need to Know? With the widespread use of hepatic imaging, liver masses are detected either unexpectedly or in the course of screening for liver cancer
Analysis of only 0-1 min clip or 1-4 min Clip for focal liver lesions during contrast-enhanced ultrasonography
 Tropical Journal of Pharmaceutical Research April 2016; 15 (4): 833-839 ISSN: 1596-5996 (print); 1596-9827 (electronic) Pharmacotherapy Group, Faculty of Pharmacy, University of Benin, Benin City, 300001
Tropical Journal of Pharmaceutical Research April 2016; 15 (4): 833-839 ISSN: 1596-5996 (print); 1596-9827 (electronic) Pharmacotherapy Group, Faculty of Pharmacy, University of Benin, Benin City, 300001
 116 ( 3. 0 cm), 146 ( 3. 0 cm) 42 48 ; 48, 5 CT 38 (79. 2 %),, ;6 ;4 3 1. 5 cm, 1 2. 2 cm 27 (56. 0 %) ; 14 (29. 0 %) 2 4,17 1 2, 4, 42, 87. 5 %(42/ 48 ), ; CT, ; ; ; Early diagnosis of small hepatocellular
116 ( 3. 0 cm), 146 ( 3. 0 cm) 42 48 ; 48, 5 CT 38 (79. 2 %),, ;6 ;4 3 1. 5 cm, 1 2. 2 cm 27 (56. 0 %) ; 14 (29. 0 %) 2 4,17 1 2, 4, 42, 87. 5 %(42/ 48 ), ; CT, ; ; ; Early diagnosis of small hepatocellular
Integration of Contrastenhanced. Multimodality Approach to Imaging of Nodules in a Cirrhotic Liver: How I Do It 1
 This copy is for personal use only. To order printed copies, contact reprints@rsna.org Integration of Contrastenhanced US into a Multimodality Approach to Imaging of Nodules in a Cirrhotic Liver: How I
This copy is for personal use only. To order printed copies, contact reprints@rsna.org Integration of Contrastenhanced US into a Multimodality Approach to Imaging of Nodules in a Cirrhotic Liver: How I
Contrast-enhanced ultrasound for assessing focal liver lesions.
 Contrast-enhanced ultrasound for assessing focal liver lesions. Poster No.: C-1455 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Garcia Etxebarria, L. Atilano, M. Bringas veiga, A. Mera 1 3
Contrast-enhanced ultrasound for assessing focal liver lesions. Poster No.: C-1455 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Garcia Etxebarria, L. Atilano, M. Bringas veiga, A. Mera 1 3
MRI for HCC surveillance and reporting: LI-RADS. Donald G. Mitchell, M.D. Thomas Jefferson University Philadelphia, PA
 MRI for HCC surveillance and reporting: LI-RADS Donald G. Mitchell, M.D. Thomas Jefferson University Philadelphia, PA Cirrhotic Nodules Regenerative Nodule Atypical Nodule Hyperplastic Nodule Dysplastic
MRI for HCC surveillance and reporting: LI-RADS Donald G. Mitchell, M.D. Thomas Jefferson University Philadelphia, PA Cirrhotic Nodules Regenerative Nodule Atypical Nodule Hyperplastic Nodule Dysplastic
The role of contrast enhanced ultrasound (ceus) in the assessment of liver nodules in patients with cirrhosis
 Review Medical Ultrasonography 2010, Vol. 12, no. 2, 145-149 The role of contrast enhanced ultrasound (ceus) in the assessment of liver nodules in patients with cirrhosis Mirela Dănilă, Ioan Sporea, Roxana
Review Medical Ultrasonography 2010, Vol. 12, no. 2, 145-149 The role of contrast enhanced ultrasound (ceus) in the assessment of liver nodules in patients with cirrhosis Mirela Dănilă, Ioan Sporea, Roxana
HEPATO-BILIARY IMAGING
 HEPATO-BILIARY IMAGING BY MAMDOUH MAHFOUZ MD PROF.OF RADIOLOGY CAIRO UNIVERSITY mamdouh.m5@gmail.com www.ssregypt.com CT ABDOMEN Indications Patient preparation Patient position Scanogram Fasting 4-6 hours
HEPATO-BILIARY IMAGING BY MAMDOUH MAHFOUZ MD PROF.OF RADIOLOGY CAIRO UNIVERSITY mamdouh.m5@gmail.com www.ssregypt.com CT ABDOMEN Indications Patient preparation Patient position Scanogram Fasting 4-6 hours
Radiation burden of hepatocellular carcinoma screening program in hepatitis B virus patients should we recommend magnetic resonance imaging instead?
 Radiation burden of hepatocellular carcinoma program in hepatitis B virus patients should we recommend magnetic resonance imaging instead? Background: Current Hepatocellular Carcinoma (HCC) surveillance
Radiation burden of hepatocellular carcinoma program in hepatitis B virus patients should we recommend magnetic resonance imaging instead? Background: Current Hepatocellular Carcinoma (HCC) surveillance
Liver imaging reporting and data system (LI-RADS) version 2014: understanding and application of the diagnostic algorithm
 pissn 2287-2728 eissn 2287-285X Liver Imaging Clinical and Molecular Hepatology 2016;22:296-307 Liver imaging reporting and data system (LI-RADS) version 2014: understanding and application of the diagnostic
pissn 2287-2728 eissn 2287-285X Liver Imaging Clinical and Molecular Hepatology 2016;22:296-307 Liver imaging reporting and data system (LI-RADS) version 2014: understanding and application of the diagnostic
S th US Contrast
 S3-1 Comparison of CEUS and CECT or CEMRI in Assessment of Tumor Vascularity and Response to Thermal Ablation in Patients with Hepatocellular Carcinoma: A Multi-centre Study in China Ming-De LU, 1 Xiao-Ling
S3-1 Comparison of CEUS and CECT or CEMRI in Assessment of Tumor Vascularity and Response to Thermal Ablation in Patients with Hepatocellular Carcinoma: A Multi-centre Study in China Ming-De LU, 1 Xiao-Ling
Liver Perfusion Analysis New Frontiers in Dynamic Volume Imaging. Case Study Brochure Chang Gung Memorial Hospital.
 New Frontiers in Dynamic Volume Imaging dynamic volume CT Case Study Brochure Chang Gung Memorial Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2010-2011. All rights
New Frontiers in Dynamic Volume Imaging dynamic volume CT Case Study Brochure Chang Gung Memorial Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2010-2011. All rights
Evangelos Chartampilas Bioclinic Hospital Thessaloniki, Greece
 Evangelos Chartampilas Bioclinic Hospital Thessaloniki, Greece Hepatospecificcontrast agents Gadobenate dimeglumine (Multihance) Gadoxeticacid (Primovist) 3-5% liver uptake 50% liver uptake Hepatobiliary
Evangelos Chartampilas Bioclinic Hospital Thessaloniki, Greece Hepatospecificcontrast agents Gadobenate dimeglumine (Multihance) Gadoxeticacid (Primovist) 3-5% liver uptake 50% liver uptake Hepatobiliary
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary)
 Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary) Staff Reviewers: Dr. Yoo Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary) Staff Reviewers: Dr. Yoo Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer
Detection and Characterization of Hepatocellular Carcinoma by Imaging
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S136 S140 Detection and Characterization of Hepatocellular Carcinoma by Imaging OSAMU MATSUI Department of Imaging Diagnosis and Interventional Radiology,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S136 S140 Detection and Characterization of Hepatocellular Carcinoma by Imaging OSAMU MATSUI Department of Imaging Diagnosis and Interventional Radiology,
HEPATOCYTE SPECIFIC CONTRAST MEDIA: WHERE DO WE STAND?
 HEPATOCYTE SPECIFIC CONTRAST MEDIA: WHERE DO WE STAND? Andrew T. Trout, MD @AndrewTroutMD Disclosures No relevant disclosures Outline Review of hepatocyte specific contrast media Review of hepatocellular
HEPATOCYTE SPECIFIC CONTRAST MEDIA: WHERE DO WE STAND? Andrew T. Trout, MD @AndrewTroutMD Disclosures No relevant disclosures Outline Review of hepatocyte specific contrast media Review of hepatocellular
Technological advancements improve the sensitivity of CEUS diagnostics
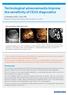 Technological advancements improve the sensitivity of CEUS diagnostics. Martegani, MD, L. iani, MD Department of Diagnostic Imaging, Valduce Hospital, Como, Italy Characterization with Ultrasound B C D
Technological advancements improve the sensitivity of CEUS diagnostics. Martegani, MD, L. iani, MD Department of Diagnostic Imaging, Valduce Hospital, Como, Italy Characterization with Ultrasound B C D
Radiological Reasoning: Incidentally Discovered Liver Mass
 AJR Integrative Imaging LIFELONG LEARNING FOR RADIOLOGY This Radiological Reasoning article is available for SAM credit and CME credits when completed with the additional educational material provided
AJR Integrative Imaging LIFELONG LEARNING FOR RADIOLOGY This Radiological Reasoning article is available for SAM credit and CME credits when completed with the additional educational material provided
Financial Disclosure
 Benign Liver Masses Adil Abdalla, MBBS Creighton University-CHI Health August 25, 2018 Financial Disclosure Nothing to disclose Financial Disclosure 1 Objectives To assess patients with benign liver tumors
Benign Liver Masses Adil Abdalla, MBBS Creighton University-CHI Health August 25, 2018 Financial Disclosure Nothing to disclose Financial Disclosure 1 Objectives To assess patients with benign liver tumors
Diagnostics guidance Published: 29 August 2012 nice.org.uk/guidance/dg5
 SonoVue (sulphur hexafluoride microbubbles) contrast agent for contrast-enhanced ultrasound imaging of the liver Diagnostics guidance Published: 29 August 2012 nice.org.uk/guidance/dg5 NICE 2018. All rights
SonoVue (sulphur hexafluoride microbubbles) contrast agent for contrast-enhanced ultrasound imaging of the liver Diagnostics guidance Published: 29 August 2012 nice.org.uk/guidance/dg5 NICE 2018. All rights
Zoltan Harkanyi M.D., Ph.D. Department of Radiology, Heim Pal Children s Hospital, Budapest, Hungary
 Zoltan Harkanyi M.D., Ph.D. Department of Radiology, Heim Pal Children s Hospital, Budapest, Hungary CEUS expereince 10 years Department of Radiology, Heim Pal Children s Hospital, Budapest US N o 1 study
Zoltan Harkanyi M.D., Ph.D. Department of Radiology, Heim Pal Children s Hospital, Budapest, Hungary CEUS expereince 10 years Department of Radiology, Heim Pal Children s Hospital, Budapest US N o 1 study
ACG Clinical Guideline: Diagnosis and Management of Focal Liver Lesions
 ACG Clinical Guideline: Diagnosis and Management of Focal Liver Lesions Jorge A. Marrero, MD, 1 Joseph Ahn, MD, FACG, 2 K. Rajender Reddy, MD, FACG 3 1 University of Texas at Southwestern, Dallas, Texas,
ACG Clinical Guideline: Diagnosis and Management of Focal Liver Lesions Jorge A. Marrero, MD, 1 Joseph Ahn, MD, FACG, 2 K. Rajender Reddy, MD, FACG 3 1 University of Texas at Southwestern, Dallas, Texas,
LUNG NODULES: MODERN MANAGEMENT STRATEGIES
 Department of Radiology LUNG NODULES: MODERN MANAGEMENT STRATEGIES Christian J. Herold M.D. Department of Biomedical Imaging and Image-guided Therapy Medical University of Vienna Vienna, Austria Pulmonary
Department of Radiology LUNG NODULES: MODERN MANAGEMENT STRATEGIES Christian J. Herold M.D. Department of Biomedical Imaging and Image-guided Therapy Medical University of Vienna Vienna, Austria Pulmonary
Newcastle HPB MDM updated radiology imaging protocol recommendations. Author Dr John Scott. Consultant Radiologist Freeman Hospital
 Newcastle HPB MDM updated radiology imaging protocol recommendations Author Dr John Scott. Consultant Radiologist Freeman Hospital This document is intended as a guide to aid radiologists and clinicians
Newcastle HPB MDM updated radiology imaging protocol recommendations Author Dr John Scott. Consultant Radiologist Freeman Hospital This document is intended as a guide to aid radiologists and clinicians
Contrast-enhanced ultrasound (CEUS) of focal liver lesions. A useful, rapid and accessible tool.
 Contrast-enhanced ultrasound (CEUS) of focal liver lesions. A useful, rapid and accessible tool. Poster No.: C-2329 Congress: ECR 2012 Type: Educational Exhibit Authors: S. Santamaria Jareño, J. Carrero
Contrast-enhanced ultrasound (CEUS) of focal liver lesions. A useful, rapid and accessible tool. Poster No.: C-2329 Congress: ECR 2012 Type: Educational Exhibit Authors: S. Santamaria Jareño, J. Carrero
Essentials of Clinical MR, 2 nd edition. 65. Benign Hepatic Masses
 65. Benign Hepatic Masses Pulse sequences acquired for abdominal MRI typically consist of fast acquisition schemes such as single-shot turbo spin echo (i.e. HASTE) and gradient echo schemes such as FLASH
65. Benign Hepatic Masses Pulse sequences acquired for abdominal MRI typically consist of fast acquisition schemes such as single-shot turbo spin echo (i.e. HASTE) and gradient echo schemes such as FLASH
Interesting Cases from Liver Tumor Board. Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine
 Interesting Cases from Liver Tumor Board Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Common Liver Diseases Hemangioma Cyst FNH Focal Fat/Sparing THID Non-Cirrhotic
Interesting Cases from Liver Tumor Board Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Common Liver Diseases Hemangioma Cyst FNH Focal Fat/Sparing THID Non-Cirrhotic
MRI of Small Hepatocellular Carcinoma: Typical Features Are Less Frequent Below a Size Cutoff of 1.5 cm
 Gastrointestinal Imaging Original Research Choi et al. MRI of Small HCC Gastrointestinal Imaging Original Research Moon Hyung Choi 1 Joon-Il Choi 1 Young Joon Lee 1 Michael Yong Park 1 Sung Eun Rha 1 Chandana
Gastrointestinal Imaging Original Research Choi et al. MRI of Small HCC Gastrointestinal Imaging Original Research Moon Hyung Choi 1 Joon-Il Choi 1 Young Joon Lee 1 Michael Yong Park 1 Sung Eun Rha 1 Chandana
Use of Ultrasound in NAFLD
 Institute for Liver and Digestive Health Use of Ultrasound in NAFLD Dr. Davide Roccarina Specialist in General Medicine Specialist Doctor in Clinical Ultrasound and non-invasive liver assessment Hepatology
Institute for Liver and Digestive Health Use of Ultrasound in NAFLD Dr. Davide Roccarina Specialist in General Medicine Specialist Doctor in Clinical Ultrasound and non-invasive liver assessment Hepatology
Impact of reader's experience in contrast-enhanced ultrasonography (CEUS) management of patients with indeterminate liver lesions
 Impact of reader's experience in contrast-enhanced ultrasonography (CEUS) management of patients with indeterminate liver lesions Poster No.: C-1699 Congress: ECR 2011 Type: Scientific Paper Authors: E.
Impact of reader's experience in contrast-enhanced ultrasonography (CEUS) management of patients with indeterminate liver lesions Poster No.: C-1699 Congress: ECR 2011 Type: Scientific Paper Authors: E.
Focal Hypoechoic Tumors of Fatty Liver
 Article Focal Hypoechoic Tumors of Fatty Liver Characterization of Conventional and Contrast-Enhanced Ultrasonography Li-Ping Liu, MD, Bao-Wei Dong, MD, Xiao-Ling Yu, MD, Ping Liang, MD, Da-Kun Zhang,
Article Focal Hypoechoic Tumors of Fatty Liver Characterization of Conventional and Contrast-Enhanced Ultrasonography Li-Ping Liu, MD, Bao-Wei Dong, MD, Xiao-Ling Yu, MD, Ping Liang, MD, Da-Kun Zhang,
Contrast Enhanced US
 Contrast Enhanced US c/o Dr Stephanie Wilson Deborah Rubens MD Professor of Imaging Sciences, Biomedical Engineering and Oncology University of Rochester Medical Center None Disclosures Thank You Dr Stephanie
Contrast Enhanced US c/o Dr Stephanie Wilson Deborah Rubens MD Professor of Imaging Sciences, Biomedical Engineering and Oncology University of Rochester Medical Center None Disclosures Thank You Dr Stephanie
Hepatocellular Carcinoma: Diagnosis and Management
 Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Gastrointestinal Imaging Original Research
 Gastrointestinal Imaging Original Research Jang et al. Multiphase CT in HCC Gastrointestinal Imaging Original Research Hyun-Jung Jang 1 Tae Kyoung Kim 1 Korosh Khalili 1 Leyla Yazdi 1 Ravi Menezes 1 Seong
Gastrointestinal Imaging Original Research Jang et al. Multiphase CT in HCC Gastrointestinal Imaging Original Research Hyun-Jung Jang 1 Tae Kyoung Kim 1 Korosh Khalili 1 Leyla Yazdi 1 Ravi Menezes 1 Seong
Common Occurrence of Benign Liver Lesions in Patients With Newly Diagnosed Breast Cancer Investigated by MRI for Suspected Liver Metastases
 JOURNAL OF MAGNETIC RESONANCE IMAGING 10:165 169 (1999) Original Research Common Occurrence of Benign Liver Lesions in Patients With Newly Diagnosed Breast Cancer Investigated by MRI for Suspected Liver
JOURNAL OF MAGNETIC RESONANCE IMAGING 10:165 169 (1999) Original Research Common Occurrence of Benign Liver Lesions in Patients With Newly Diagnosed Breast Cancer Investigated by MRI for Suspected Liver
The role for contrast-enhanced ultrasonography outside of focal liver lesions
 The role for contrast-enhanced ultrasonography outside of focal liver lesions Paul S. Sidhu King s College Hospital, London, UK Introduction Contrast-enhanced ultrasonography (US) of focal liver lesions
The role for contrast-enhanced ultrasonography outside of focal liver lesions Paul S. Sidhu King s College Hospital, London, UK Introduction Contrast-enhanced ultrasonography (US) of focal liver lesions
CT-MRI LI-RADS v2017: A Comprehensive Guide for Beginners
 Review Article CT-MRI LI-RADS v2017: A Comprehensive Guide for Beginners Francesca Patella 1, Filippo Pesapane* 1, Enrico Maria Fumarola 1, Ilaria Emili 1, Riccardo Spairani 1, Salvatore Alessio Angileri
Review Article CT-MRI LI-RADS v2017: A Comprehensive Guide for Beginners Francesca Patella 1, Filippo Pesapane* 1, Enrico Maria Fumarola 1, Ilaria Emili 1, Riccardo Spairani 1, Salvatore Alessio Angileri
Impact of a Structured Report Template on the Quality of CT and MRI Reports for Hepatocellular Carcinoma Diagnosis
 Impact of a Structured Report Template on the Quality of CT and MRI Reports for Hepatocellular Carcinoma Diagnosis Jeremy Ganeles 1, Tulay Ekinci 1, Milana Flusberg 1, Viktoriya Paroder 1, Mariya Kobi
Impact of a Structured Report Template on the Quality of CT and MRI Reports for Hepatocellular Carcinoma Diagnosis Jeremy Ganeles 1, Tulay Ekinci 1, Milana Flusberg 1, Viktoriya Paroder 1, Mariya Kobi
Enhancing diagnostic confidence in the technically difficult patient
 Ultrasound Customer story Enhancing diagnostic confidence in the technically difficult patient Philips Affiniti 70 with PureWave technology Putting Affiniti to the test A study of abdominal exams at Freeman
Ultrasound Customer story Enhancing diagnostic confidence in the technically difficult patient Philips Affiniti 70 with PureWave technology Putting Affiniti to the test A study of abdominal exams at Freeman
Differentiation Between Benign and Malignant Hepatic Lesions
 Article Differentiation Between Benign and Malignant Hepatic Lesions Utility of Color Stimulated Acoustic Emission With the Microbubble Contrast Agent Levovist Alexandra von Herbay, MD, Christoph Vogt,
Article Differentiation Between Benign and Malignant Hepatic Lesions Utility of Color Stimulated Acoustic Emission With the Microbubble Contrast Agent Levovist Alexandra von Herbay, MD, Christoph Vogt,
Surveillance for HCC Who, how Diagnosis of HCC Surveillance for HCC in Practice
 Surveillance for Hepatocellular Carcinoma Hashem B. El-Serag, MD, MPH Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Houston VA & Baylor College of Medicine Houston, TX Outline
Surveillance for Hepatocellular Carcinoma Hashem B. El-Serag, MD, MPH Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Houston VA & Baylor College of Medicine Houston, TX Outline
Sulfur hexafluoride-filled microbubbles SonoVue 3-7microns diameter Blood pool agent
 Sulfur hexafluoride-filled microbubbles SonoVue 3-7microns diameter Blood pool agent Extremely good tolerance in clinical practice - No nephrotoxicity, - No thyroid interaction - No need of Blood test
Sulfur hexafluoride-filled microbubbles SonoVue 3-7microns diameter Blood pool agent Extremely good tolerance in clinical practice - No nephrotoxicity, - No thyroid interaction - No need of Blood test
US-Guided Radiofrequency Ablation of Hepatic Focal Lesions
 US-Guided Radiofrequency Ablation of Hepatic Focal Lesions Poster No.: C-2219 Congress: ECR 2011 Type: Scientific Exhibit Authors: D. Armario Bel, A. PLA, F. TERREL, X. Serres; BARCELONA/ES Keywords: Neoplasia,
US-Guided Radiofrequency Ablation of Hepatic Focal Lesions Poster No.: C-2219 Congress: ECR 2011 Type: Scientific Exhibit Authors: D. Armario Bel, A. PLA, F. TERREL, X. Serres; BARCELONA/ES Keywords: Neoplasia,
Contrast-enhanced small bowel ultrasound in the assessment of the small bowel in patients with Crohn s Disease
 Contrast-enhanced small bowel ultrasound in the assessment of the small bowel in patients with Crohn s Disease C.F. Healy 1, D. Ferguson 1, S. Jepson 1, B. Salh 2, F. Donnellan 2, N. Chatur 2, A. C. Harris
Contrast-enhanced small bowel ultrasound in the assessment of the small bowel in patients with Crohn s Disease C.F. Healy 1, D. Ferguson 1, S. Jepson 1, B. Salh 2, F. Donnellan 2, N. Chatur 2, A. C. Harris
Contrast-Enhanced Ultrasound in Assessing Therapeutic Response in Ablative Treatments of Hepatocellular Carcinoma
 Contrast-Enhanced Ultrasound in Assessing Therapeutic Response in Ablative Treatments of Hepatocellular Carcinoma Zeno Sparchez 1, Pompilia Radu 1, Ofelia Anton 1, Mihai Socaciu 2, Radu Badea 1 1) 3 rd
Contrast-Enhanced Ultrasound in Assessing Therapeutic Response in Ablative Treatments of Hepatocellular Carcinoma Zeno Sparchez 1, Pompilia Radu 1, Ofelia Anton 1, Mihai Socaciu 2, Radu Badea 1 1) 3 rd
Imaging techniques to characterize spleen involvement in patients with Hodgkin lymphoma
 Imaging techniques to characterize spleen involvement in patients with Hodgkin lymphoma Marco Picardi, MD Ematologia, Azienda Ospedaliera Universitaria Federico II, Naples, Italy 5th International Workshop
Imaging techniques to characterize spleen involvement in patients with Hodgkin lymphoma Marco Picardi, MD Ematologia, Azienda Ospedaliera Universitaria Federico II, Naples, Italy 5th International Workshop
Byung Ihn Choi, M.D. Department of Radiology Seoul National University Hospital
 Byung Ihn Choi, M.D. Department of Radiology Seoul National University Hospital CEUS & US Elastography : Contents CEUS Introduction Contrast agents & imaging Clinical application US Video WS Summary US
Byung Ihn Choi, M.D. Department of Radiology Seoul National University Hospital CEUS & US Elastography : Contents CEUS Introduction Contrast agents & imaging Clinical application US Video WS Summary US
CTA/MRA of Pediatric Hepatic Masses Radiology-Pathology Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº70, pág. 41-50, Abr.-Jun., 2006 CTA/MRA of Pediatric Hepatic Masses Radiology-Pathology Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº70, pág. 41-50, Abr.-Jun., 2006 CTA/MRA of Pediatric Hepatic Masses Radiology-Pathology Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Focal Hepatic Lesions: Contrast- Enhancement Patterns at Pulse-Inversion Harmonic US using a Microbubble Contrast Agent
 Focal Hepatic Lesions: Contrast- Enhancement Patterns at Pulse-Inversion Harmonic US using a Microbubble Contrast Agent Eun-A Kim, MD Kwon-Ha Yoon, MD Young Hwan Lee, MD Hye Won Kim, MD Seon Kwan Juhng,
Focal Hepatic Lesions: Contrast- Enhancement Patterns at Pulse-Inversion Harmonic US using a Microbubble Contrast Agent Eun-A Kim, MD Kwon-Ha Yoon, MD Young Hwan Lee, MD Hye Won Kim, MD Seon Kwan Juhng,
Radiation reduction in the follow-up of abdominal trauma imaging using contrast-enhanced ultrasound
 Radiation reduction in the follow-up of abdominal trauma imaging using contrast-enhanced ultrasound Poster No.: B-0892 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Paper A. Deganello, E.
Radiation reduction in the follow-up of abdominal trauma imaging using contrast-enhanced ultrasound Poster No.: B-0892 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Paper A. Deganello, E.
Københavns Universitet. International guidelines for contrast-enhanced ultrasonography Nolsøe, Christian; Lorentzen, Torben
 university of copenhagen Københavns Universitet International guidelines for contrast-enhanced ultrasonography Nolsøe, Christian; Lorentzen, Torben Published in: Ultrasonography DOI: 10.14366/usg.15057
university of copenhagen Københavns Universitet International guidelines for contrast-enhanced ultrasonography Nolsøe, Christian; Lorentzen, Torben Published in: Ultrasonography DOI: 10.14366/usg.15057
Liver imaging reporting and data system: An expert consensus statement
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Liver imaging reporting and data system: An expert consensus statement Khaled M. Elsayes The University of
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Liver imaging reporting and data system: An expert consensus statement Khaled M. Elsayes The University of
Does elastography change the indication to biopsy? IBDC
 Does elastography change the indication to biopsy? A LEXANDRA A THANASIOU, M D DEPARTMENT OF RADIOLOGY CURIE INSTITUTE PARIS, FRANCE IBDC Ultrasound Detected Cancers Physician-performed ultrasound increases
Does elastography change the indication to biopsy? A LEXANDRA A THANASIOU, M D DEPARTMENT OF RADIOLOGY CURIE INSTITUTE PARIS, FRANCE IBDC Ultrasound Detected Cancers Physician-performed ultrasound increases
Case Report Contrast Enhanced Ultrasound of a Gallbladder Lesion in a Patient with a History of Renal Cell and Rectal Cancer
 Case Reports in Gastrointestinal Medicine Volume 2013, Article ID 538534, 4 pages http://dx.doi.org/10.1155/2013/538534 Case Report Contrast Enhanced Ultrasound of a Gallbladder Lesion in a Patient with
Case Reports in Gastrointestinal Medicine Volume 2013, Article ID 538534, 4 pages http://dx.doi.org/10.1155/2013/538534 Case Report Contrast Enhanced Ultrasound of a Gallbladder Lesion in a Patient with
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Portal Venous Thrombosis: Tumor VS Bland Thrombus
 June 2015 Portal Venous Thrombosis: Tumor VS Bland Thrombus SERGIO ALFARO, HARVARD MEDICAL SCHOOL YEAR III GILLIAN LIEBERMAN, MD Overview 2 Index Patient History Portal Venous Thrombosis (PVT) Imaging
June 2015 Portal Venous Thrombosis: Tumor VS Bland Thrombus SERGIO ALFARO, HARVARD MEDICAL SCHOOL YEAR III GILLIAN LIEBERMAN, MD Overview 2 Index Patient History Portal Venous Thrombosis (PVT) Imaging
Malignant Focal Liver Lesions
 Malignant Focal Liver Lesions Other Than HCC Pablo R. Ros, MD, MPH, PhD Departments of Radiology and Pathology University Hospitals Cleveland Medical Center Case Western Reserve University Pablo.Ros@UHhospitals.org
Malignant Focal Liver Lesions Other Than HCC Pablo R. Ros, MD, MPH, PhD Departments of Radiology and Pathology University Hospitals Cleveland Medical Center Case Western Reserve University Pablo.Ros@UHhospitals.org
Complete Summary GUIDELINE TITLE. Liver lesion characterization. BIBLIOGRAPHIC SOURCE(S)
 Complete Summary GUIDELINE TITLE Liver lesion characterization. BIBLIOGRAPHIC SOURCE(S) Foley WD, Bree RL, Gay SB, Glick SN, Heiken JP, Huprich JE, Levine MS, Ros PR, Rosen MP, Shuman WP, Greene FL, Rockey
Complete Summary GUIDELINE TITLE Liver lesion characterization. BIBLIOGRAPHIC SOURCE(S) Foley WD, Bree RL, Gay SB, Glick SN, Heiken JP, Huprich JE, Levine MS, Ros PR, Rosen MP, Shuman WP, Greene FL, Rockey
Hepatocellular carcinoma (HCC) is a malignant liver neoplasm
 Diagn Interv Radiol 2011; 17:328 333 Turkish Society of Radiology 2011 ABDOMINAL IMAGING ORIGINAL ARTICLE Correlation of dynamic multidetector CT findings with pathological grades of hepatocellular carcinoma
Diagn Interv Radiol 2011; 17:328 333 Turkish Society of Radiology 2011 ABDOMINAL IMAGING ORIGINAL ARTICLE Correlation of dynamic multidetector CT findings with pathological grades of hepatocellular carcinoma
THYROID NODULES: THE ROLE OF ULTRASOUND
 THYROID NODULES: THE ROLE OF ULTRASOUND NOVEMBER 2017 DR. DEAN DURANT DEFINITION Thyroid nodule: Focal area within the thyroid gland with echogenicity different from surrounding parenchyma. THYROID NODULES
THYROID NODULES: THE ROLE OF ULTRASOUND NOVEMBER 2017 DR. DEAN DURANT DEFINITION Thyroid nodule: Focal area within the thyroid gland with echogenicity different from surrounding parenchyma. THYROID NODULES
Liver Cancer (Hepatocellular Carcinoma or HCC) Overview
 Liver Cancer (Hepatocellular Carcinoma or HCC) Overview Recent advances in liver cancer care seek to address the rising incidence of liver cancer, which has steadily increased over the past three decades.
Liver Cancer (Hepatocellular Carcinoma or HCC) Overview Recent advances in liver cancer care seek to address the rising incidence of liver cancer, which has steadily increased over the past three decades.
AMSER Case of the Month: June 2018
 AMSER Case of the Month: June 2018 64 year old male undergoing evaluation for liver transplant By Timothy Morgan, MS IV Lake Erie College of Osteopathic Medicine Jonathan Potts, MD Interventional Radiology,
AMSER Case of the Month: June 2018 64 year old male undergoing evaluation for liver transplant By Timothy Morgan, MS IV Lake Erie College of Osteopathic Medicine Jonathan Potts, MD Interventional Radiology,
Effective Health Care Program
 Comparative Effectiveness Review Number 143 Effective Health Care Program Techniques for the Diagnosis and Staging of Hepatocellular Carcinoma Executive Background and Objectives Hepatocellular carcinoma
Comparative Effectiveness Review Number 143 Effective Health Care Program Techniques for the Diagnosis and Staging of Hepatocellular Carcinoma Executive Background and Objectives Hepatocellular carcinoma
