Jennifer Adams, MD Denver Health. September 28, 2010
|
|
|
- Agatha Horton
- 6 years ago
- Views:
Transcription
1 Jennifer Adams, MD Denver Health General Internal Medicine dii and HIV Primary Care September 28, 2010
2 HIV for PCP s PCP s often think they don t need to know much about HIV: it s managed by specialists Making the diagnosis and linkage to care is your job HIV patients will seek care in ER s s, urgent care, specialty care and other settings Incidence of new HIV infections in US unchanged in past decade but patients are living much longer so prevalence is increasing dramatically HIV workforce is decreasing so generalists will be caring for patients with HIV more and more Patients are developing chronic illnesses and complications of aging unrelated to their HIV The truth is, you need to know at least a little bit
3 Objectives Understand new HIV screening guidelines Correctly interpret the various HIV tests and know which one to order Recognize and diagnose acute HIV infection Counsel patients about appropriate post exposure prophylactic treatment Recognize common anti retroviral drug interactions We are not going to cover chronic management of HIV infection today
4 Case 52 year old woman presents for a PAP. Also wants to discuss her knee pain, insomnia, and needs refills of her anti hypertensive medications. You notice she s also due for diabetes and lipid screening, mammogram and colorectal cancer screening. Divorced mother of 2 teenagers. Monogamous with male partner for past 18 months. Denies recent STI s or drug use Has never been tested for HIV Is testing this woman for HIV a priority during this visit?
5 Screening HIV/AIDS is a leading cause of illness and death in the U.S million HIV infected persons live in the U.S. US 25% are unaware of their HIV infection HIV testing ti often is not done until late in the disease process: 39% of people are diagnosed with AIDS within 1 year of testing HIV+ Perinatal HIV transmission continues, usually in women not offered testing during pregnancy; sometimes as result of infection i during pregnancy Nakashima AK et al.,morbidity and Mortality Weekly Report, 2003.
6 Awareness of Serostatus Among People with HIV and Estimatesof Transmission ~25% Unaware of Infection Accounting for: ~54% of New Infections ~75% Aware of Infection Marks, et al AIDS 2006;20: ~46% of New Infections People Living with HIV/AIDS: 1,039,000-1,185,000 New Infections Each Year: ~32,000
7 September 22, 2006: CDC Recommends Routine Screening Rationale for change: Routine HIV screening will identify unrecognized HIV infection so that early treatment can be offered and interventions to reduce transmission can be implemented. HIV screening is cost effective, even in low prevalence settings. Among pregnant women, routine screening is much more effective than risk based testing for detecting unsuspected HIV infection. i Making testing routine reduces stigma.
8 AIDS Diagnoses by Transmission Category, United States, 1985 & 2008 Heterosexual 3% Other 13% IDU 19% MSM 64% Heterosexual 31% MSM 47% Other 6% IDU 16% NOTE: Data are estimates. MSM=Men who have sex with men (gay and bisexual men); IDU=Injection drug use. SOURCE: Kaiser Family Foundation, based on CDC, Presentation by Dr. Harold Jaffe, HIV/AIDS in America Today, National HIV Prevention Conference, 2003; CDC, HIV Surveillance Report, Vol. 20, 2010.
9 New Recommendations ROUTINE one time voluntary screening for patients age in all health care settings OPT OUT testing NO separate consent Pre test counseling NOT required (but it s still a good idea) Additional screening recommended for patients treated for TB or other STI s, pregnant women, patients with ongoing risk factors for new infection i Low prevalence areas should stop if < 1:1000 tests positive Colorado s rate of HIV infection is 1.3% 54.9% of patients diagnosed with HIV in Colorado live in Denver Remember, state laws and hospital policies trump guidelines Colorado does not require written consent Colorado Department of Public Health, STD surveillance report, 2008
10 Are the new recommendations working to identify new cases? Alternate 4 months sequences of opt out testing and physician directed d testing between in the DH ED In opt out phase, of approximately 28,000 eligible ER visits, 25% of patients were screened resulting in diagnosis of 25 infections (case rate of 0.15%) 10 of these infections were not new but allowed linkage to care In physician directed phase, of approximately 29,000 eligible ER visits, 0.8% of patients were tested resulting li in diagnosis i of 5 infections i (case rate of 0.01%) One of these infections was not new Non targeted opt out testing was associated with more new diagnoses but at a lower rate than expected (RR 3.6) Average CD4 in opt out group was 69, average CD4 in targeted testing group was 13 (p=0.02), only 4 cases in the opt out phase had a CD4 >350 Haukoos, et al. JAMA 2010
11 Percent of patients ages who have been tested for HIV, 2010 Same survey in 2006 found that only 42% had never been tested! Kaiser Family Foundation, Survey on HIV/AIDS, 2006 and 2010
12 Why aren t we doing a better job of screening? We don t have enough time We don t think our patients are at risk We don t think we re qualified to counsel patients about risks and benefits of screening We don t know what to do if someone tests positive! ii Back to our case
13 Back to our case should she be screened? Yes, she should be screened today! One approach: Normalize testing Obtain verbal consent Describe the possible test t results Make a plan to disclose results Now, what test are we going to use?
14 Complexities of HIV tests Different types of tests Standard d blood test: initial ELISA, confirmed with Western blot (sensitivity 99.3/specificity 99.7) Oral test: swab collects oral mucosal exudate, tested for antibody (not looking for Ab in the saliva). Positive tests must be confirmed. Higher false positive rate Rapid HIV antibody test: fingerstick or oral swab placed in developing solution. Results available in 20 minutes. Positive results must be confirmed. Home testing: Same technology as standard blood test. Mail kit to lab and results are given over the phone.
15 Testing Any positive EIA or rapid test needs to be confirmed with a western blot A positive EIA and negative WB = negative test False positives can occur and will become more common as we scale up testing What causes a false positive test? Cross reacting antibodies: pregnancy, other viral infections, collagen vascular diseases, autoimmune diseases, malignancy, recent influenza vaccination
16 The Indeterminate Test Back to our patient: She s back for a follow up of her hypertension and for test results You re 20 minutes behind, but glance through her labs before entering her room Her HIV antibody is positive and her Western Blot is positive for the p24 and G160 antigens Does she have HIV?
17 The indeterminate test WB very specific Band patterns evolves over weeks to months Need a full compliment of bands to diagnose HIV 20% of healthy h adults have an isolated p24 band Indeterminate test can indicate a false positive or early infection
18 Management of indeterminate results Back to our case. You need to tell her that she has an indeterminate result Bring her back for re testing of the HIV Antibody and Western Blot in 4 weeks OR, consider viral load testing now if risk factors present, pregnant, patient anxiety, provider anxiety, risk for loss to follow up
19 Primary HIV Infection? 37 yo MSM C/o 1 week of malaise, night sweats, rash Exam: afebrile, maculopapular rash, diffuse adenopathy By the way, had unprotected insertive i anal sex with ih an anonymous male partner 6 weeks ago. He s worried this is HIV. Acknowledgement: case adapted from NW AETC slide set
20 What is the chance this is PHI? <1% 1 5% 6 10% 11 20% 21 40% >40%
21 Exposure Risks (average, per episode, involving untreated HIV infected source patient) Percutaneous (blood) 1 0.3% Mucocutaneous (blood) (blood) % Receptive anal intercourse % Insertive anal li intercourse % 06% Receptive vaginal intercourse % Insertive vaginal intercourse %
22 Primary HIV Infection: Signs & Symptoms Up to 90% of patients will be symptomatic Signs and symptoms typically begin 1 6 weeks post exposure (2 weeks is most common) Cases outside of this range have been reported Non specific signs and symptoms: similar to EBV, influenza, hepatitis, streptococcal, syphilis High index of suspicion ii is critical ii Kahn JO, Walker BD. N Engl J Med. 1998;339: Schacker T, et al. Ann Intern Med. 1996;125:
23 Day 0 Day 0-2 Exposure to HIV at mucosal surface or blood Virus collected by dendritic cells, carried to lymph node Day 4-11 HIV replicates in CD4 cells, released into blood Day 11 on Kahn JO, Walker BD. N Engl J Med. 1998;339: Virus spreads to other organs
24 Primary HIV Infection: Common Signs & Symptoms fever 86 lethargy 74 myalgias rash headache pharyngitis N = 160 patients with PHI in Geneva, Seattle, and Sydney adenopathy % of patients Vanhems P et al. AIDS 2000; 14:
25 Primary HIV Infection: Other Signs & Symptoms aseptic meningitis 24 oral ulcers 15 genital ulcers 10 thrombocytopenia 45 leukopenia 40 transaminitis % of patients Kahn JO, Walker BD. N Engl J Med. 1998;339:33-39.
26 Primary HIV Infection Rash Mucosal Lesions Trunk and face > limbs Small pink macules Oral ulcers, thrush (Kahn, NEJM, 1998)
27 How often do patients with Primary HIV Infection seek care? Cohort of 46 adults with acute seroconversion 89% sought care in ER s, urgent cares, or primary care clinics i for symptoms consistent it t with HIV seroconversion Diagnosis of acute HIV considered in only 26% of these patients PHI often leads to medical evaluation, but HIV is under diagnosed Schacker T, et al. Clinical and epidemiologic features of primary HIV infection. Annals of Int Med, 1996.
28 Back to our Patient Exposure Risk: unprotected insertive anal intercourse, unknown HIV status Time Course: onset of symptoms 5 weeks after exposure Signs and Symptoms: malaise, night sweats, rash, adenopathy I would estimate his risk to be 1 5% What tests would be most appropriate now?
29 His test results HIV RNA: 437 copies/ml HIV antibody: negative Mono spot: negative RPR: pending AST 112, ALT 67 Normal CBC Does he have HIV? yes no unsure
30 Primary HIV Infection Plasm ma HIV RN NA (copies /ml) 10,000,000 1,000, ,000 10,000 1, Symptoms Plasma RNA Viral Load CD4 Cell Count CD4 Cell Cou unt (cells/mm m³) 1, Weeks Up to 12 Years 2-3 Years
31 Diagnostic Testing: Viral Load More sensitive than HIV antibody 3 for the diagnosis of PHI Positive one to three weeks before antibody test 1 Typically high level, e.g. greater than 50, ,000 copies/ml 2,3 False positives can occur Most false positives are low level (<10,000 copies/ml) HIV VL <10,000 copies/ml should probably be considered indeterminate 1. Busch MP, Satten GA. Am J Med 1997;102:Suppl 5B: Kahn JO, Walker BD. N Engl J Med. 1998;339: Daar ES et al. Ann Intern Med. 2001;134:25-29.
32 Follow up 6 weeks later HIV RNA <50 HIV Ab negative RPR 1:64
33 Why do we Care about Diagnosing PHI? Public Health: Patients with PHI are likely to be highly infectious given very high viral loads Diagnosis of HIV infection may lead to safer sex and needle practices Personal Health 40% of patients with HIV not diagnosed until they are within one year of AIDS diagnosis Antiretroviral therapy (ART) during PHI may alter the natural course of HIV disease
34 Linkage to Care Important next step for anyone diagnosed through screening, with primary infection, or known positive not currently in care Ideal if patient can be seen by HIV provider within hours of their diagnosis PCP s responsibility to know what resources are available to connect patients with appropriate p care
35 Post Exposure Prophylaxis (PEP) Case 1: 28 yo F, Ob/Gyn resident presents to the urgent care clinic after needlestick in the OR 30 minutes prior. Unknown HIV status of the source patient. Case 2: 24 yo M, scratched his arm on unidentified sharp object yesterday when reaching into a trash can at a night club and drew blood. Case 3: 36 yo M, unprotected sex last night ih with ih male partner, unknown HIV status. Should these patients be offered PEP?
36 Possible HIV Exposures Potentially infectious: Blood Cerebrospinal fluid Synovial fluid Pleural fluid Pericardial fluid Peritoneal fluid Amniotic fluid Semen or vaginal secretions NOT infectious unless visibly bloody Feces Nasal secretions Saliva Sputum Sweat Tears Urine Vomitus
37 Risk of HIV Infection following Occupational Exposure to HIV Infected Blood Approximately 0.3% following percutaneous exposure Approximately 0.09% following mucous membrane exposure As of 2004, only 57 documented d cases in the US of occupational transmission Last reported case of occupational transmission in 2001 Huge emotional impact of an occupational exposure
38 Risk of Other Blood Borne Infections from a Needlestick HIV 0.3% Hepatitis C 1.8% Hepatitis B (if not immunized) Source EAg negative: 1 6% clinical hepatitis, 23 37% serologic infection Source EAg positive: 22 31% clinical hepatitis, 37 62% serologic infection
39 NEJM, 1997: A CASE CONTROL STUDY OF HIV SEROCONVERSION IN HEALTH CARE WORKERS AFTER PERCUTANEOUS EXPOSURE 33 case patients tested positive for HIV after occupational exposure, 665 patients tested negative for HIV after occupational exposure Enrolled patients reported to national surveillance databases between in US, UK, France and Italy Case patients significantly less likely to have taken PEP 80% reduction in transmission if any PEP regimen given within 2 hours of exposure Most common PEP regimen was mono therapy with AZT for a month
40 Factors Associated with Increased Risk of Transmission Deep injury (OR 15) Visible contamination of device with patient s blood (OR 6.2) Needle having been placed directly into vein or artery (OR 43) 4.3) Source patient with terminal illness who died of AIDS within 2 months of the exposure (OR 5.6) Interpreted now as VL >1500 Cardo, et al. NEJM, 1997
41 Initiating PEP PEP should be started within hours of exposure Monkey studies have shown no benefit if treated >72 hours after exposure PEP should be administered for 4 weeks, if tolerated Reevaluate within ihi 72 hours of exposure, especially ill as additional information about the exposure or source patient becomes available If the source is found to be HIV negative, PEP should be discontinued Window period with current HIV Ab assays is <3 weeks for most patients; 90% within 1 month; 95% within 3 months Most acute HIV identifiable by symptoms Never been a case of occupational transmission in the US involving a source patient in the window period
42 Which Drugs to Use? Consultation with an expert is recommended Regimens should be chosen to minimize potential drug toxicities and maximize the likelihood of adherence. Consider pregnancy in all women of child bearing age. Consideration should be given to the history of the source person, including history of and response to ART, resistance tests, and disease stage If information on possible resistance is not immediately available, PEP (if indicated) should not be delayed; changes can be made later
43 Non Occupational lexposures Testing of source usually not possible CDC guidelines: recommend PEP if source known to be HIV+ and within 72 hours of exposure. Case by case decision i if HIV status of source is unknown Never been a documented case in US of transmission from a needle found in the community (2 cases of injuries from needles found in hospitals) HIV thought to degenerate very quickly outside of the body Unclear how to manage people with ongoing risky exposures
44 Follow Up of Exposed Patient All exposed patients should receive the following, regardless of whether they receive PEP: Advise to use precautions (eg, avoid blood or tissue donations, breast feeding, pregnancy, unprotected sex) to prevent secondary transmission HIV antibody testing (EIA) to monitor for seroconversion: at baseline, 6 weeks, 12 weeks, and 6 months after exposure; HIV testing (what test?) if develops illness compatible with acute retroviral syndrome
45 Resources for Consultation Local experts National Clinicians Postexposure Prophylaxis Hotline (PEPline) 24 hour telephone consultation service:
46 What do you want to do? Case 1: 28 yo F, OB/Gyn resident presents to the ER after needlestick in the OR 30 min prior. Unknown HIV status of the source patient. Case 2: 24 yo M, yesterday scratched his arm on unidentified sharp object when reaching into a trash can. Case 3: 36 yo M, unprotected receptive anal intercourse last night with male partner, unknown HIV status.
47 Our next case 38 yo F with well controlled HIV, seen in urgent care for 1 week of epigastric pain and symptoms of reflux Current medications: i OCP s, HAART (FTC/TDF, Atazanavir, Ritonavir) Labs are within normal limits Diagnosed with dyspepsia and GERD Prescribed Omeprazole and sent home, told to follow up with her PCP in a week 2 days later, you get a call from her HIV provider
48 What went wrong? Drug interaction! PPI s significantly ifi decrease serum levels l of Protease Inhibitors and are contraindicated in treatment experienced patients Many of the commonly used drugs in primary care have significant interactions with antiretroviral therapy Reported in 14 41% 41% of patients on ARV s Can cause lower ARV concentration (ie. Resistance), or higher ARV concentration (ie. Toxicity) Can also effect efficacy and toxicity in the other drugs you re prescribing You need to look it up! CROI 2007, abstract 573
49 Some common drugs to be aware of: PPI s Inhaled/Nasal Steroids Statins Antifungals Antibiotics Oral contraceptives Warfarin Anticonvulsants Antidepressants Benzodiazepines Calcium channel blockers Alpha blockers Phosphodiesterase inhibitors Many herbals
50 Take Home Points for the HIV savvy PCP Make screening for HIV routine in your practice Recognize symptoms that could be consistent with primary HIV and don t miss an opportunity to make the diagnosis Linkage to care is a priority for newly diagnosed patients with HIV Be prepared to discuss post exposure prophylaxis with your patients Always consider drug interactions in patients on ARV s
51 Thank You
HIV and PEP. LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED
 HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
Blood-Borne Pathogens and Post-Exposure Prophylaxis
 Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
0% 0% 0% Parasite. 2. RNA-virus. RNA-virus
 HIV/AIDS and Treatment Manado, Indonesia 16 november HIV [e] EDUCATION HIV is a 1. DNA-virus 2. RNA-virus 3. Parasite 0% 0% 0% DNA-virus RNA-virus Parasite HIV HIV is a RNA-virus. HIV is an RNA virus which
HIV/AIDS and Treatment Manado, Indonesia 16 november HIV [e] EDUCATION HIV is a 1. DNA-virus 2. RNA-virus 3. Parasite 0% 0% 0% DNA-virus RNA-virus Parasite HIV HIV is a RNA-virus. HIV is an RNA virus which
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Post-Exposure Prophylaxis Review for International Visitors
 Post-Exposure Prophylaxis Review for International Visitors Case Presentation 27 yo nurse presents to Urgent Care for a needlestick 2 days ago from a diabetic lancet. Source patient (SP): 35 yo male known
Post-Exposure Prophylaxis Review for International Visitors Case Presentation 27 yo nurse presents to Urgent Care for a needlestick 2 days ago from a diabetic lancet. Source patient (SP): 35 yo male known
Didactic Series. Primary HIV Infection. Greg Melcher, M.D. UC Davis AETC 8 Nov 2012
 Didactic Series Primary HIV Infection Greg Melcher, M.D. UC Davis AETC 8 Nov 2012 ACCREDITATION STATEMENT: University of California, San Diego School of Medicine is accredited by the Accreditation Council
Didactic Series Primary HIV Infection Greg Melcher, M.D. UC Davis AETC 8 Nov 2012 ACCREDITATION STATEMENT: University of California, San Diego School of Medicine is accredited by the Accreditation Council
43. Guidelines on Needle stick Injury
 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
FAMILY HIV CENTER NJ CARES SANE
 HIV, Hepatitis B & C Postexposure Prophylaxis for Sexual Assault Victims Update for Case Managers Susan Burrows-Clark, RN, MSN, CNS, C. 10/17/11 Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug
HIV, Hepatitis B & C Postexposure Prophylaxis for Sexual Assault Victims Update for Case Managers Susan Burrows-Clark, RN, MSN, CNS, C. 10/17/11 Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug
MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE
 Sandyford Protocols MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE www.hiv-druginteractions.org If you require information on occupational exposure to blood borne viruses, including HIV, please refer to the
Sandyford Protocols MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE www.hiv-druginteractions.org If you require information on occupational exposure to blood borne viruses, including HIV, please refer to the
Post-Sexual Exposure Prophylaxis (npep)
 Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft:
 Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft: 10-2-2015 Clinical studies demonstrate that when a person without HIV infection takes
Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft: 10-2-2015 Clinical studies demonstrate that when a person without HIV infection takes
INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
PREVENTION OF HIV IN THE TIMES OF PREP. Daniela Chiriboga, MD Florida Department of Health in Polk County
 PREVENTION OF HIV IN THE TIMES OF PREP Daniela Chiriboga, MD Florida Department of Health in Polk County MAKING THE CASE FOR PREVENTION The Epidemic in Florida Population in 2014: 19.6 million (3 rd in
PREVENTION OF HIV IN THE TIMES OF PREP Daniela Chiriboga, MD Florida Department of Health in Polk County MAKING THE CASE FOR PREVENTION The Epidemic in Florida Population in 2014: 19.6 million (3 rd in
The Latest on HIV Testing. Dominika Seidman, MD MAS
 The Latest on HIV Testing Dominika Seidman, MD MAS Disclosures none 2 Learning objectives At the conclusion of this session, participants should be able to Define the window periods for various HIV tests
The Latest on HIV Testing Dominika Seidman, MD MAS Disclosures none 2 Learning objectives At the conclusion of this session, participants should be able to Define the window periods for various HIV tests
Diagnosis and Management of Acute HIV
 Diagnosis and Management of Acute HIV A New HIV Diagnosis is a Call to Action In support of the NYSDOH AIDS Institute s January 2018 call to action for patients newly diagnosed with HIV, this committee
Diagnosis and Management of Acute HIV A New HIV Diagnosis is a Call to Action In support of the NYSDOH AIDS Institute s January 2018 call to action for patients newly diagnosed with HIV, this committee
HIV Lecture. Anucha Apisarnthanarak, MD Division of Infectious Diseases Thammasart University Hospital
 HIV Lecture Anucha Apisarnthanarak, MD Division of Infectious Diseases Thammasart University Hospital End-2001 global estimates for children and adults People living with HIV/AIDS New HIV infections in
HIV Lecture Anucha Apisarnthanarak, MD Division of Infectious Diseases Thammasart University Hospital End-2001 global estimates for children and adults People living with HIV/AIDS New HIV infections in
SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison
 SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
HIV Occupational Transmission and Exposure. Marsh Gelbart 2010
 HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
Objectives. HIV in the Trenches HIV Update for the Primary Care Provider, An Overview The HIV Continuum of Care.
 1:30 2:30pm HIV Update SPEAKER Gordon Dickinson, MD Presenter Disclosure Information The following relationships exist related to this presentation: Gordon Dickinson, MD, has no financial relationships
1:30 2:30pm HIV Update SPEAKER Gordon Dickinson, MD Presenter Disclosure Information The following relationships exist related to this presentation: Gordon Dickinson, MD, has no financial relationships
determine need but regimen does not change based on risk factor ED medicine attending meets
 HIV PEP Guidelines after Sexual Assault Harborview Medical Center January 2015 Initial risk assessment and discussion with patient about risk and PEP is by clinician who does exam (SANE, Ob-Gyn resident,
HIV PEP Guidelines after Sexual Assault Harborview Medical Center January 2015 Initial risk assessment and discussion with patient about risk and PEP is by clinician who does exam (SANE, Ob-Gyn resident,
Practice Steps for Implementation of Guidelines Recommendations The guideline recommendations are shown schematically -
 ASK SCREEN Test for HIV and STI Practice Steps for Implementation of Guidelines Recommendations The guideline recommendations are shown schematically - Routinely obtain a thorough sexual history from all
ASK SCREEN Test for HIV and STI Practice Steps for Implementation of Guidelines Recommendations The guideline recommendations are shown schematically - Routinely obtain a thorough sexual history from all
HIV Testing. ECHO Hep C. Judith Feinberg, MD June 22, 2017
 HIV Testing ECHO Hep C Judith Feinberg, MD June 22, 2017 Overview A few basics HIV epidemiology in the US HIV testing Time course of HIV-1 infection symptoms HIV proviral DNA symptoms window period HIV
HIV Testing ECHO Hep C Judith Feinberg, MD June 22, 2017 Overview A few basics HIV epidemiology in the US HIV testing Time course of HIV-1 infection symptoms HIV proviral DNA symptoms window period HIV
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS
 STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
PrEP in the Real World: Clinical Case Studies
 PrEP in the Real World: Clinical Case Studies Kevin L. Ard, MD, MPH April 30, 2015 Massachusetts General Hospital, National LGBT Health Education Center Continuing Medical Education Disclosure Program
PrEP in the Real World: Clinical Case Studies Kevin L. Ard, MD, MPH April 30, 2015 Massachusetts General Hospital, National LGBT Health Education Center Continuing Medical Education Disclosure Program
Nursing Interventions
 Chapter 16 H I Human Immunodeficiency V Virus A Acquired I Immuno D Deficiency S Syndrome Slide 1 Nursing Interventions Duty to treat Health care professionals may not pick and choose their patients Rehabilitation
Chapter 16 H I Human Immunodeficiency V Virus A Acquired I Immuno D Deficiency S Syndrome Slide 1 Nursing Interventions Duty to treat Health care professionals may not pick and choose their patients Rehabilitation
Welcome to Your Reading Assignment
 Welcome to Your Reading Assignment This workbook contains four reading assignments. It is filled with easy-to-read articles you can use to help keep yourself and those you care about safe. After each reading
Welcome to Your Reading Assignment This workbook contains four reading assignments. It is filled with easy-to-read articles you can use to help keep yourself and those you care about safe. After each reading
Non-Occupational Post-Exposure HIV Prophylaxis npep
 Non-Occupational Post-Exposure HIV Prophylaxis npep Peter Meacher MD (Chief Medical Officer) Anthony Vavasis MD (Director of Medicine) Callen-Lorde Community Health Center Objectives - at the end of the
Non-Occupational Post-Exposure HIV Prophylaxis npep Peter Meacher MD (Chief Medical Officer) Anthony Vavasis MD (Director of Medicine) Callen-Lorde Community Health Center Objectives - at the end of the
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
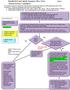 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
INTEGRATING HIV INTO PRIMARY CARE
 INTEGRATING HIV INTO PRIMARY CARE ADELERO ADEBAJO, MD, MPH, AAHIVS, FACP NO DISCLOSURE 1.2 million people in the United States are living with HIV infection and 1 in 5 are unaware of their infection.
INTEGRATING HIV INTO PRIMARY CARE ADELERO ADEBAJO, MD, MPH, AAHIVS, FACP NO DISCLOSURE 1.2 million people in the United States are living with HIV infection and 1 in 5 are unaware of their infection.
Definitions. Appendix A
 Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
HIV: What Every Clinician Needs to Know ARIZONA STATE ASSOCIATION OF PHYSICIAN ASSISTANTS SPRING CONFERENCE BETTIE COPLAN MARCH 2018
 HIV: What Every Clinician Needs to Know ARIZONA STATE ASSOCIATION OF PHYSICIAN ASSISTANTS SPRING CONFERENCE BETTIE COPLAN MARCH 2018 Overview Overview recent trends in HIV incidence in the U.S. HIV screening
HIV: What Every Clinician Needs to Know ARIZONA STATE ASSOCIATION OF PHYSICIAN ASSISTANTS SPRING CONFERENCE BETTIE COPLAN MARCH 2018 Overview Overview recent trends in HIV incidence in the U.S. HIV screening
Non-occupational HIV Post Exposure Prophylaxis (npep)
 Mountain West AIDS Education and Training Center Non-occupational HIV Post Exposure Prophylaxis (npep) Robert Harrington, M.D. This presentation is intended for educational use only, and does not in any
Mountain West AIDS Education and Training Center Non-occupational HIV Post Exposure Prophylaxis (npep) Robert Harrington, M.D. This presentation is intended for educational use only, and does not in any
OR: Steps you can take in the clinic to prevent HIV infections
 Implementing Changes to Reduce HIV Incidence: Synergies between Public Health and Primary Care Kevin Ard, MD, MPH Brigham and Women s Hospital, Massachusetts General Hospital, and the Fenway Institute
Implementing Changes to Reduce HIV Incidence: Synergies between Public Health and Primary Care Kevin Ard, MD, MPH Brigham and Women s Hospital, Massachusetts General Hospital, and the Fenway Institute
Diagnosis and Initial Management of HIV/AIDS: What the Primary Care Provider Should Know
 Diagnosis and Initial Management of HIV/AIDS: What the Primary Care Provider Should Know Carolyn K. Burr, EdD, RN Co-Clinical Director Deputy Director François-Xavier Bagnoud Center December 17 th, 2013
Diagnosis and Initial Management of HIV/AIDS: What the Primary Care Provider Should Know Carolyn K. Burr, EdD, RN Co-Clinical Director Deputy Director François-Xavier Bagnoud Center December 17 th, 2013
Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
 PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
TALKING TO YOUR. DOCTOR ABOUT npep
 TALKING TO YOUR DOCTOR ABOUT npep Please share this with your health provider. If your doctor does not have a great deal of HIV experience, he or she may want to contact a more experienced provider to
TALKING TO YOUR DOCTOR ABOUT npep Please share this with your health provider. If your doctor does not have a great deal of HIV experience, he or she may want to contact a more experienced provider to
Exposure. Blood. Department of Health & Human Services
 Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Pre-exposure Prophylaxis and Primary Care
 Pre-exposure Prophylaxis and Primary Care National Latino HIV and Hepatitis C Conference June 7 th, 2016 Allison Finkenbinder, MSN, WHNP-BC Denver Prevention Training Center Who s in the audience? Disclosures
Pre-exposure Prophylaxis and Primary Care National Latino HIV and Hepatitis C Conference June 7 th, 2016 Allison Finkenbinder, MSN, WHNP-BC Denver Prevention Training Center Who s in the audience? Disclosures
HIV and Public Health: the Basics
 HIV and Public Health: the Basics Joy Zeh, RN, MS, Family Nurse Practitioner VCU HIV/AIDS Center HIV and Public Health: the Basics Epidemiology Related Infections and Co-Morbidities Spectrum of HIV Infection
HIV and Public Health: the Basics Joy Zeh, RN, MS, Family Nurse Practitioner VCU HIV/AIDS Center HIV and Public Health: the Basics Epidemiology Related Infections and Co-Morbidities Spectrum of HIV Infection
SFAF CLINICAL PROTOCOLS
 SFAF CLINICAL PROTOCOLS Page 1 of Supersedes Date: December 31, 2016 Original Date: August 20, 2014 Version: 03 Policy Section: Patient Care Non-Occupational Post Exposure Prophylaxis Program Back ground:
SFAF CLINICAL PROTOCOLS Page 1 of Supersedes Date: December 31, 2016 Original Date: August 20, 2014 Version: 03 Policy Section: Patient Care Non-Occupational Post Exposure Prophylaxis Program Back ground:
Arizona State Office of Rural Health Webinar Series
 Arizona State Office of Rural Health Webinar Series Mute your phone &/or computer microphone Time is reserved at the end for Q&A Please fill out the post-webinar survey Webinar is being recorded Recording
Arizona State Office of Rural Health Webinar Series Mute your phone &/or computer microphone Time is reserved at the end for Q&A Please fill out the post-webinar survey Webinar is being recorded Recording
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
HIV Basics for the Family Practitioner Olha Smolynets, DO
 HIV BASICS FOR FAMILY PRACTITIONER, MS DISCLOSURES Dr. Smolynets has provided no disclosures. OBJECTIVES Indications for HIV screening Prevention counseling Prophylaxis: PrEP, PEP and npep Diagnosis Basic
HIV BASICS FOR FAMILY PRACTITIONER, MS DISCLOSURES Dr. Smolynets has provided no disclosures. OBJECTIVES Indications for HIV screening Prevention counseling Prophylaxis: PrEP, PEP and npep Diagnosis Basic
What Are HIV & AIDS? Together, we can change the course of the HIV epidemic one woman at a time.
 What Are HIV & AIDS? Together, we can change the course of the HIV epidemic one woman at a time. #onewomanatatime #thewellproject What Is HIV? HIV stands for: Human Immunodeficiency Virus HIV is the virus
What Are HIV & AIDS? Together, we can change the course of the HIV epidemic one woman at a time. #onewomanatatime #thewellproject What Is HIV? HIV stands for: Human Immunodeficiency Virus HIV is the virus
Fertility Desires/Management of Serodiscordant HIV + Couples
 Fertility Desires/Management of Serodiscordant HIV + Couples William R. Short, MD, MPH Assistant Professor of Medicine Division Of Infectious Diseases Jefferson Medical College of Thomas Jefferson University
Fertility Desires/Management of Serodiscordant HIV + Couples William R. Short, MD, MPH Assistant Professor of Medicine Division Of Infectious Diseases Jefferson Medical College of Thomas Jefferson University
TO DECREASE THE CHANCE OF GETTING
 POST ASSAULT MEDICATIONS Terri Stewart RN Naomi Sugar MD TO DECREASE THE CHANCE OF GETTING Pregnant STDs Chlamydia Gonorrhea Trichomonas Hep B HIV EMERGENCY CONTRACEPTION Plan B Levonorgestrel PLAN B Plan
POST ASSAULT MEDICATIONS Terri Stewart RN Naomi Sugar MD TO DECREASE THE CHANCE OF GETTING Pregnant STDs Chlamydia Gonorrhea Trichomonas Hep B HIV EMERGENCY CONTRACEPTION Plan B Levonorgestrel PLAN B Plan
Disclosure. Learning Objectives. Epidemiology. Transmission. Risk of Transmission PRE-EXPOSURE PROPHYLAXIS (PREP) FOR HIV PREVENTION 50,000.
 Disclosure PRE-EXPOSURE PROPHYLAXIS (PREP) FOR HIV PREVENTION I have no financial interest in and/or affiliation with any external organizations in relation to this CE program. DaleMarie Vaughan, PharmD
Disclosure PRE-EXPOSURE PROPHYLAXIS (PREP) FOR HIV PREVENTION I have no financial interest in and/or affiliation with any external organizations in relation to this CE program. DaleMarie Vaughan, PharmD
Revised April WGH ER #5 Hospital Rd. Whitehorse Phone: (867) Outside of Whitehorse: Local Community Health Centre/Clinic/ER
 Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
ONLY IN HUMANS! CAN GET SICK FASTER. What is HIV? NO CURE. Human Immunodeficiency Virus. HIV ATTACKS your T-cells. And uses them to of itself
 The 411: HIV ONLY IN HUMANS! CAN GET SICK FASTER What is HIV? NO CURE Human Immunodeficiency Virus HIV ATTACKS your T-cells And uses them to of itself HIV Progression Acute Infection Stage Clinical Latency
The 411: HIV ONLY IN HUMANS! CAN GET SICK FASTER What is HIV? NO CURE Human Immunodeficiency Virus HIV ATTACKS your T-cells And uses them to of itself HIV Progression Acute Infection Stage Clinical Latency
Commonly Asked Questions About Chronic Hepatitis C
 Commonly Asked Questions About Chronic Hepatitis C From the American College of Gastroenterology 1. How common is the hepatitis C virus? The hepatitis C virus is the most common cause of chronic viral
Commonly Asked Questions About Chronic Hepatitis C From the American College of Gastroenterology 1. How common is the hepatitis C virus? The hepatitis C virus is the most common cause of chronic viral
Billing and Coding for HIV Services
 Billing and Coding for HIV Services Financial Disclosure This speaker does not have any financial relationships with commercial entities to disclose. This speaker will not discuss any off-label use or
Billing and Coding for HIV Services Financial Disclosure This speaker does not have any financial relationships with commercial entities to disclose. This speaker will not discuss any off-label use or
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
HIV Reproductive Health: Conception Options in the Era of PrEP
 HIV Reproductive Health: Conception Options in the Era of PrEP Meg Sullivan, MD Director, HIV Clinical Programs, Section of Infectious Diseases Boston Medical Center Boston University School of Medicine
HIV Reproductive Health: Conception Options in the Era of PrEP Meg Sullivan, MD Director, HIV Clinical Programs, Section of Infectious Diseases Boston Medical Center Boston University School of Medicine
Pre and Post Exposure Prophylaxis. Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018
 Pre and Post Exposure Prophylaxis Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018 Indications for Pre and Post Exposure Prophylaxis: occupational and non-occupational
Pre and Post Exposure Prophylaxis Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018 Indications for Pre and Post Exposure Prophylaxis: occupational and non-occupational
Introduction to Blood Borne Pathogens
 Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Importance of Viral Suppression to Reduce HIV Transmission: Recent Evidence
 Importance of Viral Suppression to Reduce HIV Transmission: Recent Evidence Toye Brewer, MD Co-Director, Fogarty International Training Program University of Miami Miller School of Medicine Viral suppression
Importance of Viral Suppression to Reduce HIV Transmission: Recent Evidence Toye Brewer, MD Co-Director, Fogarty International Training Program University of Miami Miller School of Medicine Viral suppression
Are You Positive You re Negative?
 Are You Positive You re Negative? [Myths] and [Truths] About HIV Testing www.amfar.org 2013. amfar, The Foundation for AIDS Research. [myth] I don t need an HIV test. There s no way I could be infected.
Are You Positive You re Negative? [Myths] and [Truths] About HIV Testing www.amfar.org 2013. amfar, The Foundation for AIDS Research. [myth] I don t need an HIV test. There s no way I could be infected.
HIV: Pregnancy in Serodiscordant Couple. Dr Chow TS ID Clinic HPP
 HIV: Pregnancy in Serodiscordant Couple Dr Chow TS ID Clinic HPP Sexual Reproductive Health and Rights The recognition of the sexual and reproductive health and rights (SRHR) of all individuals and couples
HIV: Pregnancy in Serodiscordant Couple Dr Chow TS ID Clinic HPP Sexual Reproductive Health and Rights The recognition of the sexual and reproductive health and rights (SRHR) of all individuals and couples
Sexually Transmissible Infections (STI) and Blood-borne Viruses (BBV) A guide for health promotion workers
 Sexually Transmissible Infections (STI) and Blood-borne Viruses (BBV) A guide for health promotion workers Sexual & Reproductive Health Western Australia Chlamydia (bacterial infection) Unprotected vaginal
Sexually Transmissible Infections (STI) and Blood-borne Viruses (BBV) A guide for health promotion workers Sexual & Reproductive Health Western Australia Chlamydia (bacterial infection) Unprotected vaginal
El Paso - Ambulatory Clinic Policy and Procedure
 Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
PrEP and npep for HIV Prevention. Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine
 PrEP and npep for HIV Prevention Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine Case Study A 26 y/o M presents for routine asymptomatic screening for sexually transmitted infections
PrEP and npep for HIV Prevention Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine Case Study A 26 y/o M presents for routine asymptomatic screening for sexually transmitted infections
HIV Prevention Pearls
 HIV Prevention Pearls Meghan Rothenberger, MD Assistant Professor Division of Infectious Diseases University of Minnesota Director, Youth and AIDS Projects October 27, 2017 Disclosure Information I have
HIV Prevention Pearls Meghan Rothenberger, MD Assistant Professor Division of Infectious Diseases University of Minnesota Director, Youth and AIDS Projects October 27, 2017 Disclosure Information I have
I M ENDING HIV PATIENT INFORMATION. endinghiv.org.au/prep
 I M ENDING HIV PrEP PATIENT INFORMATION endinghiv.org.au/prep THIS BOOKLET PROVIDES YOU WITH INFORMATION ABOUT Pre-Exposure Prophylaxis (PrEP) for HIV. CONTENTS 06 Who will benefit from PrEP? 04 What is
I M ENDING HIV PrEP PATIENT INFORMATION endinghiv.org.au/prep THIS BOOKLET PROVIDES YOU WITH INFORMATION ABOUT Pre-Exposure Prophylaxis (PrEP) for HIV. CONTENTS 06 Who will benefit from PrEP? 04 What is
Case Studies in PrEP Management. Kevin L. Ard, MD, MPH Massachusetts General Hospital, National LGBT Health Education Center April 15, 2016
 Case Studies in PrEP Management Kevin L. Ard, MD, MPH Massachusetts General Hospital, National LGBT Health Education Center April 15, 2016 Continuing Medical Education Disclosure Program Faculty: Kevin
Case Studies in PrEP Management Kevin L. Ard, MD, MPH Massachusetts General Hospital, National LGBT Health Education Center April 15, 2016 Continuing Medical Education Disclosure Program Faculty: Kevin
Post Blood & Body Fluid Exposure Checklist
 Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
Bloodborne Pathogens Across the Continuum of Care Sue Sebazco, Arlington, Texas A Webber Training Teleclass
 Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
10/17/2015. Chapter 55. Care of the Patient with HIV/AIDS. History of HIV. HIV Modes of Transmission
 Chapter 55 Care of the Patient with HIV/AIDS All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. History of HIV Remains somewhat obscure The earlier
Chapter 55 Care of the Patient with HIV/AIDS All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. History of HIV Remains somewhat obscure The earlier
People who experience gender based violence are more at risk of HIV.
 Know the HIV risk People who experience gender based violence are more at risk of HIV. HIV Human Immunodeficiency Virus is the virus that causes AIDS by interfering with the body s ability to fight off
Know the HIV risk People who experience gender based violence are more at risk of HIV. HIV Human Immunodeficiency Virus is the virus that causes AIDS by interfering with the body s ability to fight off
What Women Need to Know: The HIV Treatment Guidelines for Pregnant Women
 : The HIV Treatment Guidelines for Pregnant Women : The HIV Treatment Guidelines for Pregnant Women What Women Need to Know: Prepared by Elaine Gross, RN, MS, CNS-C National Pediatric & Family HIV Resource
: The HIV Treatment Guidelines for Pregnant Women : The HIV Treatment Guidelines for Pregnant Women What Women Need to Know: Prepared by Elaine Gross, RN, MS, CNS-C National Pediatric & Family HIV Resource
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Safety Tips from the WorkSafe People
 Blood Borne Pathogens Training HIV/AIDS Hepatitis B Determining Exposure Protecting Yourself Preventing Exposure during an Emergency HIV/AIDS Definition: AIDS stands for Acquired Immune Deficiency Syndrome.
Blood Borne Pathogens Training HIV/AIDS Hepatitis B Determining Exposure Protecting Yourself Preventing Exposure during an Emergency HIV/AIDS Definition: AIDS stands for Acquired Immune Deficiency Syndrome.
Lisa K. Fitzpatrick, MD, MPH Associate Professor of Medicine Howard University School of Medicine
 Lisa K. Fitzpatrick, MD, MPH Associate Professor of Medicine Howard University School of Medicine HIV Testing Missed Opportunities Acute Retroviral Syndrome Opportunistic Infections Treatment Reminders
Lisa K. Fitzpatrick, MD, MPH Associate Professor of Medicine Howard University School of Medicine HIV Testing Missed Opportunities Acute Retroviral Syndrome Opportunistic Infections Treatment Reminders
Hepatitis STARS Program. Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003
 Hepatitis 2003 STARS Program Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003 Outline n Hepatitis A Epidemiology and screening Transmission n Hepatitis B Epidemiology
Hepatitis 2003 STARS Program Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003 Outline n Hepatitis A Epidemiology and screening Transmission n Hepatitis B Epidemiology
Chapter 2 Hepatitis B Overview
 Chapter 2 Hepatitis B Overview 23 24 This page intentionally left blank. HEPATITIS B OVERVIEW Hepatitis B Virus The hepatitis B virus (HBV) belongs to the Hepadnaviridae family and is known to cause both
Chapter 2 Hepatitis B Overview 23 24 This page intentionally left blank. HEPATITIS B OVERVIEW Hepatitis B Virus The hepatitis B virus (HBV) belongs to the Hepadnaviridae family and is known to cause both
PrEP for HIV Prevention. Adult Clinical Guideline from the New York State Department of Health AIDS Institute
 PrEP for HIV Prevention Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the PrEP Guideline Raise awareness of PrEP among healthcare
PrEP for HIV Prevention Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the PrEP Guideline Raise awareness of PrEP among healthcare
PEDIATRIC EMERGENCY DEPARTMENT CLINICAL GUIDELINE: NON- OCCUPATIONAL EXPOSURE TO BLOOD-BORNE PATHOGENS (HIV, Hepatitis B, AND Hepatitis C)
 General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: F:
 University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
EDMA HIV-AIDS TEAM Fact Sheet November 2007
 EDMA HIV-AIDS TEAM Fact Sheet November 2007 1. HIV Facts AIDS epidemic update UNAIDS Epidemic Update, November 2007 (1) 760,000 people to be living with HIV in Western and Central Europe in 2007. 31,000
EDMA HIV-AIDS TEAM Fact Sheet November 2007 1. HIV Facts AIDS epidemic update UNAIDS Epidemic Update, November 2007 (1) 760,000 people to be living with HIV in Western and Central Europe in 2007. 31,000
GAY MEN/MSM AND STD S IN NJ: TAKE BETTER CARE OF YOUR PATIENTS! STEVEN DUNAGAN SPECIAL PROJECTS COORDINATOR NJ DOH STD PROGRAM SEPTEMBER 27, 2016
 GAY MEN/MSM AND STD S IN NJ: TAKE BETTER CARE OF YOUR PATIENTS! STEVEN DUNAGAN SPECIAL PROJECTS COORDINATOR NJ DOH STD PROGRAM SEPTEMBER 27, 2016 TOPICS FOR DISCUSSION What medical providers should know
GAY MEN/MSM AND STD S IN NJ: TAKE BETTER CARE OF YOUR PATIENTS! STEVEN DUNAGAN SPECIAL PROJECTS COORDINATOR NJ DOH STD PROGRAM SEPTEMBER 27, 2016 TOPICS FOR DISCUSSION What medical providers should know
Obstetrics and HIV An Update. Jennifer Van Horn MD University of Utah
 Obstetrics and HIV An Update Jennifer Van Horn MD University of Utah Obstetrics and HIV Perinatal transmission Testing Antiretroviral therapy Antepartum management Intrapartum management Postpartum management
Obstetrics and HIV An Update Jennifer Van Horn MD University of Utah Obstetrics and HIV Perinatal transmission Testing Antiretroviral therapy Antepartum management Intrapartum management Postpartum management
Biomedical Prevention in HIV
 Biomedical Prevention in HIV CHART - CCAS-CDC 3 RD Joint Meeting Montego Bay, Jamaica August 21-26,2011 Presented by Tina Hylton-Kong, ERTU-CHART Some Slides from Impact of ART on HIV Transmission Wafaa
Biomedical Prevention in HIV CHART - CCAS-CDC 3 RD Joint Meeting Montego Bay, Jamaica August 21-26,2011 Presented by Tina Hylton-Kong, ERTU-CHART Some Slides from Impact of ART on HIV Transmission Wafaa
Answering basic questions about HIV
 Answering basic questions about HIV Sixth Edition This booklet is for you if you have basic questions about HIV such as what it is, how it is transmitted and how it affects the body. If you have HIV and
Answering basic questions about HIV Sixth Edition This booklet is for you if you have basic questions about HIV such as what it is, how it is transmitted and how it affects the body. If you have HIV and
PREP IN PRIMARY CARE TRACY SALAMEH RN, BSN, ACRN HIV CLINICAL SPECIALIST DAKOTA AIDS EDUCATION AND TRAINING CENTER
 PREP IN PRIMARY CARE TRACY SALAMEH RN, BSN, ACRN HIV CLINICAL SPECIALIST DAKOTA AIDS EDUCATION AND TRAINING CENTER THE NEED FOR CONTINUED HIV PREVENTION Estimated new HIV infections in the US for the most
PREP IN PRIMARY CARE TRACY SALAMEH RN, BSN, ACRN HIV CLINICAL SPECIALIST DAKOTA AIDS EDUCATION AND TRAINING CENTER THE NEED FOR CONTINUED HIV PREVENTION Estimated new HIV infections in the US for the most
Module 1: HIV epidemiology, transmission and prevention
 Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses
 Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
HIV Update Objectives. Epidemiology. Epidemiology, Transmission and Natural History. Transmission Risk by Exposure. Transmission 9/29/2014
 Objectives HIV Update 2014 Jay Sizemore, MD, MPH Medical Director Chattanooga CARES Assistant Professor UTCOM Chattanooga 2October 2014 Review HIV epidemiology and screening/testing guidelines Discuss
Objectives HIV Update 2014 Jay Sizemore, MD, MPH Medical Director Chattanooga CARES Assistant Professor UTCOM Chattanooga 2October 2014 Review HIV epidemiology and screening/testing guidelines Discuss
Michigan Guidelines: HIV, Syphilis, HBV in Pregnancy
 Michigan Guidelines: HIV, Syphilis, HBV in Pregnancy Presenter: Theodore B. Jones, MD Maternal Fetal Medicine Wayne State University School of Medicine Beaumont Dearborn Hospital HIV, Syphilis, HBV in
Michigan Guidelines: HIV, Syphilis, HBV in Pregnancy Presenter: Theodore B. Jones, MD Maternal Fetal Medicine Wayne State University School of Medicine Beaumont Dearborn Hospital HIV, Syphilis, HBV in
The how and why of Acute HIV Infection 1. How do we best diagnosis patients with acute HIV?
 Acute HIV infection Eric Rosenberg, MD Associate Professor of Pathology Director, Clinical Microbiology Laboratory Massachusetts General Hospital Harvard Medical School The how and why of Acute HIV Infection
Acute HIV infection Eric Rosenberg, MD Associate Professor of Pathology Director, Clinical Microbiology Laboratory Massachusetts General Hospital Harvard Medical School The how and why of Acute HIV Infection
HIV/AIDS MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: HIV/AIDS MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN HIV/AIDS MEASURES GROUP: #159. HIV/AIDS: CD4+ Cell Count or CD4+ Percentage Performed #160. HIV/AIDS: Pneumocystis
2014 PQRS OPTIONS F MEASURES GROUPS: HIV/AIDS MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN HIV/AIDS MEASURES GROUP: #159. HIV/AIDS: CD4+ Cell Count or CD4+ Percentage Performed #160. HIV/AIDS: Pneumocystis
General HIV/AIDS Information
 General HIV/AIDS Information The History of HIV In the summer of 1981, physicians in San Francisco observed that young, previously healthy homosexual men were developing an unusual type of pneumonia which
General HIV/AIDS Information The History of HIV In the summer of 1981, physicians in San Francisco observed that young, previously healthy homosexual men were developing an unusual type of pneumonia which
Hepatitis C Best Practice Guidelines For Local Health Departments
 Hepatitis C Best Practice Guidelines For Local Health Departments LHDs are responsible for investigating and reporting all physician reported cases of acute hepatitis C (HCV). For clients known to have
Hepatitis C Best Practice Guidelines For Local Health Departments LHDs are responsible for investigating and reporting all physician reported cases of acute hepatitis C (HCV). For clients known to have
