Pre and Post Exposure Prophylaxis. Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018
|
|
|
- Simon Hall
- 5 years ago
- Views:
Transcription
1 Pre and Post Exposure Prophylaxis Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018
2 Indications for Pre and Post Exposure Prophylaxis: occupational and non-occupational exposure Legal aspects of occupational and non-occupational exposure And should it be mandatory for HCP? Is prophylaxis always justified? Updated guidelines: when to give, what to give, for how long and monitoring- Case scenarios Rashid Hospital data
3 The essence of ID and IC : how to prevent before exposure and how to control after exposure
4 Relevant factors when assessing for PrEP and PEP Immunity of exposed person:age,immunesupressing disease or medication Vaccine-preventable diseases vaccination history Specific immune globulin- Medical chemoprophylaxis-signs/symptoms of active infection Risk assessment /stratification /checklists Baseline tests ( active and latent infections, renal/hepatic profiles, pregnancy/breast feeding, concomitant medication ) Counseling
5 Non-occupational ( community) exposure Sexual: known or unknown partner Respiratory route ( airborne and droplet) Mucosal and Contact transmission Needle stick and sharp objects exposure Human and animals bites Spectrum: HIV, HBV,STD VZV, TB, meningococcal, influenza, measles, VHF, Rabies, Tetanus,
6 Occupational exposure Needle stick and sharp objects exposure Mucosal and Contact transmission Respiratory route ( airborne and droplet) Bites and scratches Spectrum: BBV: HBV/HCV/HIV VZV, TB-MDR TB, influenza,measles,meningococcal, Brucellosis VHF,
7 Pre and post exposure vaccines what is relevant to HCW BCG HAV Typhoid Cholera MMR Tetanus Meningococcal Pertussis Diphtheria HBV VZV Influenza
8 Specific immunoglobulin HAV HBV Rabies CMV VZV Tetanus German Measles (Rubella)
9 Efficacy and safety data Any form of PrEP or PEP is not 100% effective in preventing the development of active infection post exposure. Several factors are linked to efficacy like route of transmission, inoculum size, time to prophylaxis, PEP regimen potency, PrEP and PEP are not always safe and there can be drug-related SE and toxicities as in other situations
10
11 At Dubai Government level
12
13 Administrative support At DHA level Medical Fitness Department-DHA and community Preventive Medicine Department- community Occupational Health Department Central Infection Control and prevention committee Pharmacy, Laboratory, Quality offices, Staff clinics, employee health clinics, IDU in Rashid Hospital, IC teams, IPC committees in hospitals and Primary Health Care clinics with Policies and Procedures plus pathways in place.
14
15 RH data Staff clinic/quality office Type of injury NS and sharp object injury Mucous membrane exposure Other Infectious diseases exposure Number of exposed staff
16 Ward 4 ( Infectious Diseases Unit) data F: Blood splash from HIV pt. into her eyes PEP No conversions F:Needle prick from HIV pt. PEP No conversions M : NSI while inserting Central line PEP No conversion F: non bloody Secretion splash from HIV pt. on her hands M: Saliva from HIV positive on non intact skin No PEP No PEP No conversion No conversion M: Sneezing on face by MDR,PTB pt. No PEP Did not develop active disease 37/52 pregnant nurse exposed to H1N1 +VE case Female nurse exposed to VZV case M: nurse had a spit on his face by HIV/HBV positive patient F: nurse had a CCVHF patient vomitus on her hand Oseltamivir VZV vaccine series No PEP Ribavirin PEP Did not develop active disease Did not develop active disease No follow up No conversion
17 Most recent consults: 3 OB/GY young female doctors had emergency surgery for ovarian torsion case. After closure, they were informed that the patient was HIV positive A young CID police officer had a bite from an aggressive? HIV positive lady ( sex worker) A young UAE male with recent travel to Thailand had un-protected exposure while there to unknown sex worker
18 Scenario 1 A 39 yr old female, working in ward 4, and while collecting ABG samples at 1700 on Thursday for a newly diagnosed advanced AIDS patient with HIV VL of > 100,000 copies per ml and pending HIV genotype test, she had eye splashes with blood. She stopped immediately, washed her eyes and went to ER. The immediate action to be taken by ER physician would be to: 1- reassure her as the risk of mucosal transmission of HIV is very low and no need for Post Exposure Prophylaxis 2- check her baseline status and start PEP as standards immediately 3- ask her to go to staff clinic on Sunday 4- call ID on call immediately
19 Scenario 2 3 ob./gyn doctors were involved in emergency surgery in Dubai Hospital for an un-booked patient. They has variable degrees of undocumented exposure with one only wearing double gloves. After wound closure, they were told that she is HIV positive with high titers on ELISA test. The ID on call is contacted 33 hours after exposure. What would be the best action to take now? 1- Start PEP for all three pending WB confirmation and HIV PCR for the patient 2- Individualize PEP decision based on history of exposure and risk of transmission 3- Do not start PEP to any as it is too late to be effective ( more than 24 hrs) 4- council the doctors and reassure that risk of exposure is very low and her HIV is not confirmed yet
20 Scenario 4 A 32 year old lady is married to HIV positive patient, he is on ART for the last 3/12 and his HIV VL is zero on Rx. She is planning to become pregnant. What advise would you give her? 1- She should be on protected sex and start pre exposure prophylaxis till he is maintaining zero viremia for at least 6/12 2- She should be on life long prophylaxis plus protected sex as there is a risk of virologic failure in her husband 3- She can have un-protected sex and no need for PrEP as he has zero viremia 4- They should try IVF to avoid the risk of HIV transmission
21 HIV PrEP
22 HIV PrEP at IDU-RH Used in few discordant couples Main indication is for female partner planning for natural methods of pregnancy Majority of our discordant couples are not on PrEP: monitored every 6/12 and counseled about transmission reduction methods with maintenance of zero viremia in positive partner.
23 Occupational BBV: HIV,HBV,HCV
24 For transmission of blood borne pathogens (HIV, HBV and HCV) to occur, an exposure must include both of the following: Infectious body fluid Blood, semen, vaginal fluid, amniotic fluid, breast milk, cerebrospinal fluid, pericardial fluid, peritoneal fluid, pleural fluid and synovial fluid can transmit HIV, HBV and HCV. Saliva, vomitus, urine, feces, sweat, tears and respiratory secretions do not transmit HIV (unless visibly bloody). The risk of HBV and HCV transmission from non-bloody saliva is negligible. A portal of entry (percutaneous, mucous membrane, cutaneous with non-intact skin). If both of these factors are not present, there is no risk of transmission and further evaluation is not required.
25 Risk of HBV, HCV and HIV transmission after occupational percutaneous exposure Role of 30,3 and 0.3% HBV risk varies depending on e-antigen: If e-antigen positive, risk is up to 30% If e-antigen negative, risk is 1-6% HCV risk is 1.8% (range of 0-7%) HIV risk is 0.3% (range of %)
26 Average Risk of HIV Infection to Healthcare Personnel by Exposure Route
27 Occupations of US Healthcare Personnel with Documented/Possible Occupational AIDS/HIV Infection
28
29
30 What is the time frame for using PEP? Efficacy is time sensitive: first dose should be given as soon as possible. Optimal time to start PEP is within hours of exposure, rather than days. Do not wait for SP test results (unless results will be available within an hour or two) to proceed with a PEP decision and initiation, when indicated. 72 hours post-exposure as the outer limit of opportunity to initiate PEP; however, a delay of that scale is believed to compromise PEP efficacy. The 72-hour outside limit recommendation is based on animal studies; no human data are available.
31 SEXUAL ASSAULT? Yes No Assailant known? Yes No TESTING AND MEDICAL HISTORY Previous Baseline Following Current Exposure Condition Result Date Result Date Other results HIV +ve -ve +ve -ve Biochemistry/liver function tests Hepatitis C +ve -ve +ve -ve Pregnancy +ve -ve Syphilis +ve -ve +ve -ve Current and past medical history, e.g. renal disease: Other STIs +ve -ve +ve -ve HBsAg +ve -ve +ve -ve All medications and drug allergies: Anti-HBs +ve -ve +ve -ve Anti-HBc +ve -ve +ve -ve Psychiatric history: Hepatitis A IgG +ve -ve Drug and alcohol history: CHARACTERISTICS OF EXPOSURE Date of exposure / / Time of exposure am/pm Place of exposure: Sexual contact Sharps exposure Receptive anal sex: ejaculation withdrawal Occupational Non-occupational Insertive anal sex: circumcised uncircumcised Reuse of injecting equipment Other needle-stick injury Receptive vaginal sex Hollow bore needle Solid bore needle Solid sharp Insertive vaginal sex: circumcised uncircumcised Other exposure Receptive oral sex Insertive oral sex Mucous membrane: occupational non-occupational Other risks Blood splash: Condoms used? Yes No superficial non-intact skin mucous membrane Condom: broke slipped removed by source Under the influence of alcohol or drugs? Yes No RISK CHARACTERISTICS OF SOURCE Sex Male Female Non-binary HIV positive Antiretroviral use Source HIV risk Partner +ve -ve Unknown known no ARV MSM regular HBV suspected unknown Injecting drug use casual HCV unknown past ARV High prevalence other STIs Last viral load: Date: current ARV country Which STIs, if any: TRIAGE AND PEP ASSESSMENT Date / / Time am/pm Location Management Post exposure prophylaxis for HIV recommended? Yes No Hepatitis B immunoglobulin / / Regimen commenced? Yes No Hepatitis B vaccine / / Has patient taken PEP in the last 12 months? Yes No Was patient referred to counselling? Yes No Did patient consent to receive PEP? Yes No Reason not referred? Date PEP was received / / Time: am/pm Was PrEP discussed? Yes No Follow-up date / / & Location GP SHC Other Was PrEP recommended? Yes No Drug prescribed Dose Frequency Contraception given? Yes No I confirm that the above patient has had an exposure incident that may be a risk for HIV transmission. The result of the assessment for eligibility for HIV PEP is documented and drugs prescribed. Prescriber s signature Prescriber s name Provider number Contact details Telephone
32 Recommended PEP regimens 1- Emtricitabine/Tenofovir + Dolutegravir 2-Emtricitabine/Tenofovir + Raltegravir 3- Emtricitabine/Tenofovir + boosted Darunavir
33 Baseline tests and follow up Baseline Exposed staff HIV Ag/Ab, HBS Ag, HBS Ab, HCV Ab, CBC, LFT, renal profile Inform the lab that your sending post exposure samples for rapid TAT Exposure source HIV Ag/Ab-PCR if known HIV positive HBS Ag HCV Ab, PCR 72 hrs. Assessment for adherence and early SE Check lab results If HIV negative: stop PEP 14 days Assessment + blood tests Check lab results If HIV negative: stop PEP 28 days Assessment+ blood tests Check lab results If HIV negative: stop PEP 6-8 weeks HIV Ag/Ab-HIV PCR is not indicated Window period assessment in high risk groups only 16 weeks HIV Ag/Ab- stop if using COMBO test Check lab results if indicated 6 months HIV Ag/Ab, Check lab results if indicated 1 year HIV Ag/Ab- if HCV co-infection
34 Occupational HBV exposure
35 Concentration of HBV in Body Fluids
36 PEP for Exposure to HBV Unvaccinated Previously vaccinated Antibody response unknown HBIG x 1 and initiate hepatitis B vaccine series Test exposed person for anti-hbs 1. If adequate, no treatment 2. If inadequate, HBIG x 1 and vaccine booster
37 Efficacy of HBV PEP Regimen Multiple doses of HBIG alone when 1st dose initiated within 1 week Prevention of HBV Infection 70-75% Hepatitis B vaccine series alone Combination of HBIG and vaccine series 70-75% 85-95%
38 HCV work up and? PEP
39 Occupational Transmission of HCV Inefficiently transmitted by occupational exposures Average incidence 1.8% (range 0-7%) following percutaneous exposure from HCV-positive source Case reports of transmission from blood splash to mucous membrane
40 Recommendations Baseline testing Initial follow-up Final follow-up HCV+ SP or SP has potential HCV risk factors 6 weeks HCV RNA (HCV viral load) PEPline 2017 SP HCV status unknown or SP is known and has no known HCV risk factors HCV Ab Optional: 6 week HCV RNA 6 months HCV Ab CDC 2016 All source persons HCV Ab 3 weeks HCV RNA Optional: 6 month HCV Ab
41 CCVHF PEP Exposure assessment Baseline blood tests ( Pregnancy test if indicated) Ribavirin for 10-14? 21 days at 400 mg bd dose Check CCVHF PCR on day 5-if asymptomatic and negative PCR- stop ribavirin prophylaxis
42 Counselling Avoid blood /organ donation until informed that no active infection occurred Protected sex or refrain till advised Discuss pregnancy plans No job restrictions for occupational exposure while on PEP or under follow up
43 Process map mucosal exposure from viremic HIV/HBV/HCV positive + MDR-TB patient into unprotected eyes Exposure at 0830 Incident report in AMAN at minutes Staff clinic Registration and evaluation 0900 Lab for baseline test 1045
44 Challenges Lack of awareness in both occupational and community exposure on importance of PrEP and PEP whenever applicable Taking occupational exposure too easy or too serious to the degree on denial ( no tests done, delay in initialing PEP, not complaint with PrEP, no compliance with PEP, no time) Fear of stigma and legal consequences if diagnosed with serious infectious diseases ( TB, HIV) Lack of timely reporting and incidence documentation ( can have legal consequences) No access to PrEP or PEP including vaccines and immunoglobulin (availability, cost, no system in place)
45 In summary Assess exposure with understanding of core transmission principles Perform baseline tests- exposed and exposure source if available Decide if prophylaxis is indicated or not Decide what to give and for how long Follow up on prophylaxis and post completion In case of occupational exposure: timely reporting is crucial
46 Thank you
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Revised April WGH ER #5 Hospital Rd. Whitehorse Phone: (867) Outside of Whitehorse: Local Community Health Centre/Clinic/ER
 Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
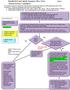 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS
 STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
Blood-Borne Pathogens and Post-Exposure Prophylaxis
 Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
HIV and PEP. LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED
 HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
PEDIATRIC EMERGENCY DEPARTMENT CLINICAL GUIDELINE: NON- OCCUPATIONAL EXPOSURE TO BLOOD-BORNE PATHOGENS (HIV, Hepatitis B, AND Hepatitis C)
 General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Management
 01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
43. Guidelines on Needle stick Injury
 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
Contamination Incidents Frequently Asked Questions
 Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK)
 POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Non-occupational HIV Post Exposure Prophylaxis (npep)
 Mountain West AIDS Education and Training Center Non-occupational HIV Post Exposure Prophylaxis (npep) Robert Harrington, M.D. This presentation is intended for educational use only, and does not in any
Mountain West AIDS Education and Training Center Non-occupational HIV Post Exposure Prophylaxis (npep) Robert Harrington, M.D. This presentation is intended for educational use only, and does not in any
El Paso - Ambulatory Clinic Policy and Procedure
 Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: F:
 University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
Introduction to Blood Borne Pathogens
 Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison
 SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
Post Exposure Prophylaxis (PEP)
 Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
An International Antiviral Society-USA
 Doug Campos-Outcalt, MD, MPA University of Arizona, Phoenix dougco@email.arizona. edu A look at new guidelines for HIV treatment and prevention Start antiretroviral therapy as soon as possible after HIV
Doug Campos-Outcalt, MD, MPA University of Arizona, Phoenix dougco@email.arizona. edu A look at new guidelines for HIV treatment and prevention Start antiretroviral therapy as soon as possible after HIV
HCW & OCCUPATIONAL INFECTIOUS HAZARDS
 HCW & OCCUPATIONAL INFECTIOUS HAZARDS Dr Sheela Mathew 4 ways infections are transmitted Contact Direct transmission through touch (staph) Vehicle sexual intercourse(gonnerhia,hiv), Fecal oral transmission
HCW & OCCUPATIONAL INFECTIOUS HAZARDS Dr Sheela Mathew 4 ways infections are transmitted Contact Direct transmission through touch (staph) Vehicle sexual intercourse(gonnerhia,hiv), Fecal oral transmission
Clinical management of non-occupational and occupational exposure to blood borne pathogens. - A Pocket Reference -
 Pocket P.E.P. Clinical management of non-occupational and occupational eposure to blood borne pathogens Development Team: Deborah Yoong, PharmD 1 1, 2, 3 Kevin Gough, MD, MEd 1 Positive Care Clinic, Toronto,
Pocket P.E.P. Clinical management of non-occupational and occupational eposure to blood borne pathogens Development Team: Deborah Yoong, PharmD 1 1, 2, 3 Kevin Gough, MD, MEd 1 Positive Care Clinic, Toronto,
Blood Borne Pathogens. Becky Walch, R.N. Micheel Valdez, L.V.N.
 Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
HIV Occupational Transmission and Exposure. Marsh Gelbart 2010
 HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital
 HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE
 Sandyford Protocols MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE www.hiv-druginteractions.org If you require information on occupational exposure to blood borne viruses, including HIV, please refer to the
Sandyford Protocols MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE www.hiv-druginteractions.org If you require information on occupational exposure to blood borne viruses, including HIV, please refer to the
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses
 Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Infection Control Standard Precautions. CDC Recommendations: Application of Standard Precautions for All Patients
 Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Bloodborne Pathogens: Recognition and Treatment 2011
 Bloodborne Pathogens: Recognition and Treatment 2011 Occupational Health Services at The Summit Rita M. Lopez, APRN-BC, MSN 751-4189 rlopez@krmc.org OBJECTIVES DEFINE Bloodborne Pathogen Exposure WHO must
Bloodborne Pathogens: Recognition and Treatment 2011 Occupational Health Services at The Summit Rita M. Lopez, APRN-BC, MSN 751-4189 rlopez@krmc.org OBJECTIVES DEFINE Bloodborne Pathogen Exposure WHO must
Post-Sexual Exposure Prophylaxis (npep)
 Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
TRANSMISSION OF BLOODBORNE PATHOGENS: HIV,HBV,HCV. Dr Daniel Kimani HIV Prevention Medical Transmission CDC, Kenya.
 TRANSMISSION OF BLOODBORNE PATHOGENS: HIV,HBV,HCV Dr Daniel Kimani HIV Prevention Medical Transmission CDC, Kenya. Nevada Hepatitis C Outbreak Tied to Las Vegas Clinic. Thousands Now At Risk for Hepatitis,
TRANSMISSION OF BLOODBORNE PATHOGENS: HIV,HBV,HCV Dr Daniel Kimani HIV Prevention Medical Transmission CDC, Kenya. Nevada Hepatitis C Outbreak Tied to Las Vegas Clinic. Thousands Now At Risk for Hepatitis,
Non-Occupational Post-Exposure HIV Prophylaxis npep
 Non-Occupational Post-Exposure HIV Prophylaxis npep Peter Meacher MD (Chief Medical Officer) Anthony Vavasis MD (Director of Medicine) Callen-Lorde Community Health Center Objectives - at the end of the
Non-Occupational Post-Exposure HIV Prophylaxis npep Peter Meacher MD (Chief Medical Officer) Anthony Vavasis MD (Director of Medicine) Callen-Lorde Community Health Center Objectives - at the end of the
Definitions. Appendix A
 Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
TO DECREASE THE CHANCE OF GETTING
 POST ASSAULT MEDICATIONS Terri Stewart RN Naomi Sugar MD TO DECREASE THE CHANCE OF GETTING Pregnant STDs Chlamydia Gonorrhea Trichomonas Hep B HIV EMERGENCY CONTRACEPTION Plan B Levonorgestrel PLAN B Plan
POST ASSAULT MEDICATIONS Terri Stewart RN Naomi Sugar MD TO DECREASE THE CHANCE OF GETTING Pregnant STDs Chlamydia Gonorrhea Trichomonas Hep B HIV EMERGENCY CONTRACEPTION Plan B Levonorgestrel PLAN B Plan
Hepatitis B Control. Table of Contents
 Control Table of Contents 1.0 INTRODUCTION... 1 2.0 GOALS... 1 3.0 DEFINITIONS... 1 4.0 CASE MANAGEMENT... 3 5.0 HEPATITIS B POST- EXPOSURE MANAGEMENT... 4 TABLE 1: HEPATITIS B POST EXPOSURE PROPHYLAXIS...
Control Table of Contents 1.0 INTRODUCTION... 1 2.0 GOALS... 1 3.0 DEFINITIONS... 1 4.0 CASE MANAGEMENT... 3 5.0 HEPATITIS B POST- EXPOSURE MANAGEMENT... 4 TABLE 1: HEPATITIS B POST EXPOSURE PROPHYLAXIS...
Greenwood School District 50 OSHA UPDATE BLOODBORNE PATHOGENS
 Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Post Blood & Body Fluid Exposure Checklist
 Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
3/23/2016. Managing Bloodborne Pathogen Exposures. Managing Bloodborne Pathogen Exposures
 This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
Healthcare Personnel Immunization Recommendations
 Healthcare Personnel Immunization Recommendations Kathleen Harriman, PhD, MPH, RN California Department of Public Health Immunization Branch Vaccine Preventable Disease Epidemiology Section kathleen.harriman@cdph.ca.gov
Healthcare Personnel Immunization Recommendations Kathleen Harriman, PhD, MPH, RN California Department of Public Health Immunization Branch Vaccine Preventable Disease Epidemiology Section kathleen.harriman@cdph.ca.gov
Module 1: HIV epidemiology, transmission and prevention
 Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
2017 BLOODBORNE PATHOGENS
 2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
PrEP for HIV Prevention. Adult Clinical Guideline from the New York State Department of Health AIDS Institute
 PrEP for HIV Prevention Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the PrEP Guideline Raise awareness of PrEP among healthcare
PrEP for HIV Prevention Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the PrEP Guideline Raise awareness of PrEP among healthcare
POLICY, PROCEDURE & GUIDELINES FOR POST EXPOSURE PROPHYLAXIS IN CUHG.
 POLICY, PROCEDURE & GUIDELINES FOR POST EXPOSURE PROPHYLAXIS IN CUHG. Reference Number: PPG CUH CUH Revision No: 1 Review Cycle: 2 Years Author (Lead): Dr Colm Kerr, Infectious Owner: Dr A Jackson, Infectious
POLICY, PROCEDURE & GUIDELINES FOR POST EXPOSURE PROPHYLAXIS IN CUHG. Reference Number: PPG CUH CUH Revision No: 1 Review Cycle: 2 Years Author (Lead): Dr Colm Kerr, Infectious Owner: Dr A Jackson, Infectious
Bloodborne Pathogens Across the Continuum of Care Sue Sebazco, Arlington, Texas A Webber Training Teleclass
 Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Chapter 2 Hepatitis B Overview
 Chapter 2 Hepatitis B Overview 23 24 This page intentionally left blank. HEPATITIS B OVERVIEW Hepatitis B Virus The hepatitis B virus (HBV) belongs to the Hepadnaviridae family and is known to cause both
Chapter 2 Hepatitis B Overview 23 24 This page intentionally left blank. HEPATITIS B OVERVIEW Hepatitis B Virus The hepatitis B virus (HBV) belongs to the Hepadnaviridae family and is known to cause both
Blood-borne Pathogens Exposure Policy
 Blood-borne Pathogens Exposure Policy Contents Blood Borne Pathogen(s) Exposure (BBPE) -Post-Exposure Prophylaxis... 1 STUDENT CHECKLIST... 3 PROGRAM CHECKLIST... 4 PROVIDER CHECKLIST... 5 POST-EXPOSURE
Blood-borne Pathogens Exposure Policy Contents Blood Borne Pathogen(s) Exposure (BBPE) -Post-Exposure Prophylaxis... 1 STUDENT CHECKLIST... 3 PROGRAM CHECKLIST... 4 PROVIDER CHECKLIST... 5 POST-EXPOSURE
People who experience gender based violence are more at risk of HIV.
 Know the HIV risk People who experience gender based violence are more at risk of HIV. HIV Human Immunodeficiency Virus is the virus that causes AIDS by interfering with the body s ability to fight off
Know the HIV risk People who experience gender based violence are more at risk of HIV. HIV Human Immunodeficiency Virus is the virus that causes AIDS by interfering with the body s ability to fight off
Healthcare Professionals
 EMPLOYEE HEALTH Employee Health: Screening and immunization programs Counseling, follow up work restrictions Analysis and trending of occupational exposure incidents Assess risk for occupational exposure
EMPLOYEE HEALTH Employee Health: Screening and immunization programs Counseling, follow up work restrictions Analysis and trending of occupational exposure incidents Assess risk for occupational exposure
Infection/Disease Control HEPATITIS CONTROL PROGRAM
 OPERATING PROCEDURE NO. 153-29 Florida State Hospital Chattahoochee, Florida July 8, 2009 Infection/Disease Control HEPATITIS CONTROL PROGRAM 1. Purpose: To establish consistent surveillance, reporting,
OPERATING PROCEDURE NO. 153-29 Florida State Hospital Chattahoochee, Florida July 8, 2009 Infection/Disease Control HEPATITIS CONTROL PROGRAM 1. Purpose: To establish consistent surveillance, reporting,
Infection Prevention and Control - General Orientation
 Infection Prevention and Control - General Orientation Hand Hygiene-CDC Isolation Precautions - CDC Medical Waste - OSHA Environmental Cleaning - CDC Safe Injection Practices - CDC Bloodborne Pathogens
Infection Prevention and Control - General Orientation Hand Hygiene-CDC Isolation Precautions - CDC Medical Waste - OSHA Environmental Cleaning - CDC Safe Injection Practices - CDC Bloodborne Pathogens
determine need but regimen does not change based on risk factor ED medicine attending meets
 HIV PEP Guidelines after Sexual Assault Harborview Medical Center January 2015 Initial risk assessment and discussion with patient about risk and PEP is by clinician who does exam (SANE, Ob-Gyn resident,
HIV PEP Guidelines after Sexual Assault Harborview Medical Center January 2015 Initial risk assessment and discussion with patient about risk and PEP is by clinician who does exam (SANE, Ob-Gyn resident,
Controlling Infection. Madeleine Myers FNP-BC
 Controlling Infection Madeleine Myers FNP-BC Core Curriculum Elements Professional Responsibilities Infection Cycle Barriers and PPE Safe Client Care Environment Work Practice Controls Prevention and Control
Controlling Infection Madeleine Myers FNP-BC Core Curriculum Elements Professional Responsibilities Infection Cycle Barriers and PPE Safe Client Care Environment Work Practice Controls Prevention and Control
EQuIP 5 - This version June 2011 Revision Due June 2014
 Preamble Rockingham Peel Group Non-Occupational Post-Exposure Prophylaxis (NPEP) To Prevent HIV in Western Australia Protocol The purpose of this protocol is to clarify the appropriate use and methods
Preamble Rockingham Peel Group Non-Occupational Post-Exposure Prophylaxis (NPEP) To Prevent HIV in Western Australia Protocol The purpose of this protocol is to clarify the appropriate use and methods
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Prophylaxis
 01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Establish protocol for management of occupational exposures to blood or potentially infectious materials. All employees of
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Establish protocol for management of occupational exposures to blood or potentially infectious materials. All employees of
Hepatitis STARS Program. Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003
 Hepatitis 2003 STARS Program Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003 Outline n Hepatitis A Epidemiology and screening Transmission n Hepatitis B Epidemiology
Hepatitis 2003 STARS Program Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003 Outline n Hepatitis A Epidemiology and screening Transmission n Hepatitis B Epidemiology
EMPLOYEE HEALTH TABLE OF CONTENTS
 EMPLOYEE HEALTH TABLE OF CONTENTS PHYSICAL ASSESSMENT.2 REPORTING EMPLOYEE INFECTIONS...3 SUMMARY OF IMPORTANT RECOMMENDATIONS AND WORK RESTRICTIONS FOR PERSONNEL WITH INFECTIOUS DISEASES.4 HEPATITIS B
EMPLOYEE HEALTH TABLE OF CONTENTS PHYSICAL ASSESSMENT.2 REPORTING EMPLOYEE INFECTIONS...3 SUMMARY OF IMPORTANT RECOMMENDATIONS AND WORK RESTRICTIONS FOR PERSONNEL WITH INFECTIOUS DISEASES.4 HEPATITIS B
HIV: Pregnancy in Serodiscordant Couple. Dr Chow TS ID Clinic HPP
 HIV: Pregnancy in Serodiscordant Couple Dr Chow TS ID Clinic HPP Sexual Reproductive Health and Rights The recognition of the sexual and reproductive health and rights (SRHR) of all individuals and couples
HIV: Pregnancy in Serodiscordant Couple Dr Chow TS ID Clinic HPP Sexual Reproductive Health and Rights The recognition of the sexual and reproductive health and rights (SRHR) of all individuals and couples
MANAGEMENT OF OCCUPATIONAL AND NON-OCCUPATIONAL EXPOSURES TO BLOODBORNE VIRUSES INCLUDING NEEDLESTICK INJURIES & SEXUAL EXPOSURES
 NHS GREATER GLASGOW CONTROL OF INFECTION COMMITTEE GUIDELINE MANAGEMENT OF OCCUPATIONAL AND NON-OCCUPATIONAL EXPOSURES TO BLOODBORNE VIRUSES INCLUDING NEEDLESTICK INJURIES & SEXUAL EXPOSURES Effective
NHS GREATER GLASGOW CONTROL OF INFECTION COMMITTEE GUIDELINE MANAGEMENT OF OCCUPATIONAL AND NON-OCCUPATIONAL EXPOSURES TO BLOODBORNE VIRUSES INCLUDING NEEDLESTICK INJURIES & SEXUAL EXPOSURES Effective
HEPATITIS B INFECTION and Pregnancy. Caesar Mensah Communicable Diseases & Infection Control Specialist, UK June 2011
 HEPATITIS B INFECTION and Pregnancy Caesar Mensah Communicable Diseases & Infection Control Specialist, UK June 2011 HEPATITIS B 26/07/2011 What is Hepatitis B? It is inflammation (infection) of the liver
HEPATITIS B INFECTION and Pregnancy Caesar Mensah Communicable Diseases & Infection Control Specialist, UK June 2011 HEPATITIS B 26/07/2011 What is Hepatitis B? It is inflammation (infection) of the liver
Occupational Health Update: Extended Care Facilities
 Occupational Health Update: Extended Care Facilities James J. Hill III, MD MPH FACOEM Associate Professor & Vice Chair Department of Physical Medicine & Rehabilitation University of North Carolina School
Occupational Health Update: Extended Care Facilities James J. Hill III, MD MPH FACOEM Associate Professor & Vice Chair Department of Physical Medicine & Rehabilitation University of North Carolina School
Infectious Disease Control Oi Orientation. Providence Health & Services
 Infectious Disease Control Oi Orientation ti Providence Health & Services Infection Control Who is at risk of infection & why? Exposures and Outcomes What tools do we use to reduce risk? Surveillance Analysis
Infectious Disease Control Oi Orientation ti Providence Health & Services Infection Control Who is at risk of infection & why? Exposures and Outcomes What tools do we use to reduce risk? Surveillance Analysis
Bloodborne Pathogens. Exposure Control Plan
 Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
Information for Health Care Workers
 Information for Health Care Workers This Bulletin highlights precautions to be taken by health care workers who may be exposed to blood and body fluids. In general, workers should minimize direct contact
Information for Health Care Workers This Bulletin highlights precautions to be taken by health care workers who may be exposed to blood and body fluids. In general, workers should minimize direct contact
Hepatitis C Virus (HCV)
 Clinical Practice Guidelines Hepatitis C Virus (HCV) OBJECTIVE The purpose is to guide the appropriate diagnosis and management of Hepatitis C Virus (HCV). GUIDELINE These are only guidelines, and are
Clinical Practice Guidelines Hepatitis C Virus (HCV) OBJECTIVE The purpose is to guide the appropriate diagnosis and management of Hepatitis C Virus (HCV). GUIDELINE These are only guidelines, and are
Bloodborne Pathogens. By Deborah Massarella RN, MSN
 Bloodborne Pathogens By Deborah Massarella RN, MSN 2010, 2014 Objectives At conclusion of in-service learners will: 1. Identify two types of personal protective equipment. 2. Identify two prevention measures
Bloodborne Pathogens By Deborah Massarella RN, MSN 2010, 2014 Objectives At conclusion of in-service learners will: 1. Identify two types of personal protective equipment. 2. Identify two prevention measures
Drew University Bloodborne Pathogens Exposure Control Plan and Procedures
 PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
Occupational Exposure to Blood Borne Viruses
 Occupational Exposure to Blood Borne Viruses Marissa Herron Occupational Health Support Nurse [BBV] 2014 Aim To raise awareness of the key information and procedures in NHS Lanarkshire's Control of Infection
Occupational Exposure to Blood Borne Viruses Marissa Herron Occupational Health Support Nurse [BBV] 2014 Aim To raise awareness of the key information and procedures in NHS Lanarkshire's Control of Infection
Hepatitis B at a Glance
 Return completed form, preferably within 30 days of U.S. date of arrival, to address on reverse side of this form. Review overseas medical exam if available and document immunization dates. Indicate if
Return completed form, preferably within 30 days of U.S. date of arrival, to address on reverse side of this form. Review overseas medical exam if available and document immunization dates. Indicate if
Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
 PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
Training for Employees of Taylor Special Care Services, Inc.
 Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
For. Correctional. Officers. Your. Health Risks. in Correctional Settings. Facts. About HIV
 For Correctional Officers Your Health Risks in Correctional Settings Facts About HIV Working in close quarters with inmates in a correctional facility puts correctional officers (COs) at increased risk
For Correctional Officers Your Health Risks in Correctional Settings Facts About HIV Working in close quarters with inmates in a correctional facility puts correctional officers (COs) at increased risk
Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV
 Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties An exposure that might place health
Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties An exposure that might place health
A. Background for Trainer: B. What OSHA Requires: Bloodborne Pathogens. Lesson Plan 6080a
 Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
HIV Prevention Pearls
 HIV Prevention Pearls Meghan Rothenberger, MD Assistant Professor Division of Infectious Diseases University of Minnesota Director, Youth and AIDS Projects October 27, 2017 Disclosure Information I have
HIV Prevention Pearls Meghan Rothenberger, MD Assistant Professor Division of Infectious Diseases University of Minnesota Director, Youth and AIDS Projects October 27, 2017 Disclosure Information I have
Bloodborne Pathogen Exposure STUDENT. Blood Borne Pathogen Exposure. Student. Rev:
 Blood Borne Pathogen Exposure Student INSTRUCTIONS 1. Student: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Blood Borne Pathogen Exposure Student INSTRUCTIONS 1. Student: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Bloodborne Pathogen Module. Chelmsford Public Schools September, 2016
 Bloodborne Pathogen Module Chelmsford Public Schools September, 2016 Why is this important? v OSHA BB Pathogen Standard anyone whose job requires exposure to BB pathogens is required to complete training
Bloodborne Pathogen Module Chelmsford Public Schools September, 2016 Why is this important? v OSHA BB Pathogen Standard anyone whose job requires exposure to BB pathogens is required to complete training
Vaccine preventable health associated infections (HAI) Entesar Husain BM BCH, FRCPC
 Vaccine preventable health associated infections (HAI) Entesar Husain BM BCH, FRCPC Assistant Professor, Department of Pediatrics Faculty of Medicine Consultant Pediatric Infectious Diseases NBK Hospital
Vaccine preventable health associated infections (HAI) Entesar Husain BM BCH, FRCPC Assistant Professor, Department of Pediatrics Faculty of Medicine Consultant Pediatric Infectious Diseases NBK Hospital
Hepatitis B and C Overview, Outbreaks, and Recommendations. Viral Hepatitis Language. Types of Viral Hepatitis 7/1/2013
 Hepatitis B and C Overview, Outbreaks, and Recommendations Elizabeth Lawlor, MS Healthy Kansans living in safe and sustainable environments. Viral Hepatitis Language Acute infection is when the infection
Hepatitis B and C Overview, Outbreaks, and Recommendations Elizabeth Lawlor, MS Healthy Kansans living in safe and sustainable environments. Viral Hepatitis Language Acute infection is when the infection
PrEP and npep for HIV Prevention. Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine
 PrEP and npep for HIV Prevention Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine Case Study A 26 y/o M presents for routine asymptomatic screening for sexually transmitted infections
PrEP and npep for HIV Prevention Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine Case Study A 26 y/o M presents for routine asymptomatic screening for sexually transmitted infections
Undergraduate Medical Education
 Undergraduate Medical Education Communicable Disease Screening Protocol Student Conduct Component: Procedure #SC 08P Corresponding Policy: Policy #SC-08 Supersedes: none Lead Writer: Communicable Disease
Undergraduate Medical Education Communicable Disease Screening Protocol Student Conduct Component: Procedure #SC 08P Corresponding Policy: Policy #SC-08 Supersedes: none Lead Writer: Communicable Disease
Management of sharps injuries in the healthcare setting
 Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
INFECTION PREVENTION AND CONTROL POLICY AND PROCEDURES Sussex Partnership NHS Foundation Trust (The Trust)
 A member of: Association of UK University Hospitals INFECTION PREVENTION AND CONTROL POLICY AND PROCEDURES Sussex Partnership NHS Foundation Trust (The Trust) IPC20 VACCINATION PROGRAMME FOR STAFF AND
A member of: Association of UK University Hospitals INFECTION PREVENTION AND CONTROL POLICY AND PROCEDURES Sussex Partnership NHS Foundation Trust (The Trust) IPC20 VACCINATION PROGRAMME FOR STAFF AND
Student Immunisation Record Faculty of Medicine. Section 1: Information. Notes
 Student Immunisation Record Faculty of Section 1: Information Students enrolled in programs offered by the Faculty of are REQUIRED to provide evidence of their immunisation status for the diseases listed
Student Immunisation Record Faculty of Section 1: Information Students enrolled in programs offered by the Faculty of are REQUIRED to provide evidence of their immunisation status for the diseases listed
PrEP Home Checklist v1.0
 PrEP Home Checklist v1.0 Every Visit o Risk Reduction Counseling o Appropriate referrals and follow-ups (SW, Pharmacy, et al.) o For those on PrEP: o Assessment of PrEP adherence, side effects, ongoing
PrEP Home Checklist v1.0 Every Visit o Risk Reduction Counseling o Appropriate referrals and follow-ups (SW, Pharmacy, et al.) o For those on PrEP: o Assessment of PrEP adherence, side effects, ongoing
Blood Borne Pathogen Exposure Employee
 Blood Borne Pathogen Exposure Employee INSTRUCTIONS 1. Employee: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Blood Borne Pathogen Exposure Employee INSTRUCTIONS 1. Employee: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Confirmed (Laboratory Tests) Serum positive for IgM anti-hbc or, hepatitis B surface antigen (HbsAg).
 Hepatitis B Hepatitis B is a liver disease that results from infection with the Hepatitis B virus. It can range in severity from a mild illness lasting a few weeks to a serious, lifelong illness. Hepatitis
Hepatitis B Hepatitis B is a liver disease that results from infection with the Hepatitis B virus. It can range in severity from a mild illness lasting a few weeks to a serious, lifelong illness. Hepatitis
Modernization of North Carolina s HIV control measures
 Modernization of North Carolina s HIV control measures North Carolina Division of Public Health Victoria Mobley, MD MPH Evelyn Foust, MPH CPM Agenda Introduction Summary of scientific evidence used to
Modernization of North Carolina s HIV control measures North Carolina Division of Public Health Victoria Mobley, MD MPH Evelyn Foust, MPH CPM Agenda Introduction Summary of scientific evidence used to
