Generation of experimental allergic airways inflammation in the absence of draining lymph nodes
|
|
|
- Rosa Craig
- 5 years ago
- Views:
Transcription
1 Generation of experimental allergic airways inflammation in the absence of draining lymph nodes Beata U. Gajewska, 1 David Alvarez, 1 Mariana Vidric, 1 Susanna Goncharova, 1 Martin R. Stämpfli, 1 Anthony J. Coyle, 2 José-Carlos Gutierrez-Ramos, 2 and Manel Jordana 1 1 Department of Pathology and Molecular Medicine, and Division of Respiratory Diseases and Allergy, Centre for Gene Therapeutics, McMaster University, Hamilton, Ontario, Canada 2 Millennium Pharmaceuticals Inc., Cambridge, Massachusetts, USA Address correspondence to: Manel Jordana, Health Sciences Centre Room 4H17, Department of Pathology and Molecular Medicine, Centre for Gene Therapeutics, McMaster University, 1200 Main Street West, Hamilton, Ontario, Canada L8N 3Z5. Phone: (905) ext ; Fax: (905) ; jordanam@mcmaster.ca. Beata U. Gajewska and David Alvarez contributed equally to this work. Received for publication February 27, 2001, and accepted in revised form May 22, The objective of this study was to investigate the contribution of secondary lymphoid organs in the generation and maintenance of experimental allergic airway inflammation. We employed a previously reported murine model of respiratory mucosal allergic sensitization, induced by repeated aerosolizations of ovalbumin in the context of a GM-CSF airway environment. We executed this protocol in wildtype (WT) and lymphotoxin-α deficient mice (LTα-KO) mice, which are devoid of lymph nodes (LNs) and possess rudimentary spleen structures. Despite the lack of pulmonary LNs draining the airway compartment, LTα-KO mice were fully capable of mounting a robust inflammatory response in the airways, consisting of Th2 polarized CD4 + T cells and eosinophils. This was accompanied by IL-5, IL-13, and IFN-γ production by splenocytes and generation of ovalbumin-specific serum IgE. Exposure to the same antigen 7 weeks after complete resolution of airway inflammation once again induced a Th2 polarized infiltrate, demonstrating intact immunological memory. To investigate inherent plasticity in establishing antigen-specific immunity, mice were splenectomized before sensitization. Allergic sensitization was completely abrogated in splenectomized LTα-KO mice, compared with eusplenic LTα-KO controls. These data demonstrate that secondary lymphoid organs, either LN or spleen, are essential for the generation of allergic airway responses. J. Clin. Invest. 108: (2001). DOI: /JCI Introduction Current understanding is that antigens that penetrate the mucosae are taken up by antigen presenting cells (APCs), mainly dendritic cells (DCs), and transported to the regional lymph nodes (LNs). In the LNs, these antigens are presented in the context of MHC molecules to naive T cells that will, then, undergo differentiation (1). An extension of this notion with reference to allergic asthma would assume that allergen-specific T cells are generated in the LN compartment, undergo Th2 differentiation, and traffic to the airway, where they execute their effector function including, most notably, production of a distinct cytokine and chemokine program that results in eosinophilic inflammation, goblet cell hyperplasia, and bronchial hyperreactivity (2 4). Evidence that intranasal delivery of antigen leads to activation events in the cervical LNs (5, 6), and a recent elegant demonstration of DC migration from the lung to the thoracic LNs in response to allergen aerosolization (7), support a role of the regional LNs in the generation of immune responses to aeroallergens. Yet the functional requirement of the thoracic LNs in the generation of allergic responses has not been directly investigated. Lymphotoxin-α deficient mice (LTα-KO) are born without morphologically detectable LNs or Peyer s patches; in addition, they have an altered splenic architecture, with the loss of the typical T and B cell areas and deficient germinal center formation (8 10). Hence, LTα-KO mice provide a particularly suitable model to investigate the role of secondary lymphoid structures in the generation of mucosal immune responses. To investigate the role of LNs in this process, we used a murine model in which allergic sensitization is achieved by repeated aerosolizations of ovalbumin (OVA) in the context of a GM-CSF airway environment, which is established by gene transfer of a replicationdeficient adenovirus encoding murine GM-CSF (11). Our data show that, despite a complete deficiency of all peripheral LNs, LTα-KO mice subjected to this experimental protocol mount a robust airway inflammatory response that is qualitatively comparable and quantitatively greater than that observed in wild-type (WT) littermates. In vivo antigen recall responses, Th2-associated IgE synthesis, and in vitro cytokine production confirmed the establishment of antigen-specific immunity and memory. To investigate the site of allergic sen- The Journal of Clinical Investigation August 2001 Volume 108 Number 4 577
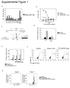
2 sitization in LTα-KO mice, we surgically removed the spleen. Splenectomy of LTα-KO mice before the initiation of our protocol prevented sensitization and airway inflammation, whereas splenectomy of WT littermates did not affect the generation of allergic sensitization. These data establish a critical requirement of secondary lymphoid organs in the generation of Th2 responses to aeroallergens and intimate the plasticity of the immune system in the generation of mucosal immunity. Methods Animals. C57BL/6 and LTα-KO mice (5 8 weeks old) were purchased from The Jackson Laboratory (Bar Harbor, Maine, USA). Mice were housed in a specific pathogen-free environment after a 12-hour light-dark cycle. All experiments performed were approved by the Animal Research Ethics Board of McMaster University. Model of respiratory mucosal allergic sensitization. Replication-deficient human type 5 adenoviral construct encoding murine GM-CSF cdna in the E1 region of the viral genome (Ad/GM-CSF) was delivered intranasally 24 hours before the first OVA exposure. Ad/GM-CSF was administered intranasally at a dose of pfu in 30 µl of PBS vehicle (two 15-µl administrations, 5 minutes apart) into anesthetized animals. Over a period of 10 consecutive days (days 0 9), mice were placed in a Plexiglas chamber (10 cm 15 cm 25 cm) and exposed for 20 minutes daily to aerosolized OVA (1% wt/vol in 0.9% saline). OVA aerosol was generated by a Bennet nebulizer (Puritan-Bennet Corp., Carlsbad, California, USA) at a flow rate of 10 l/min. For in vivo rechallenge with OVA, mice were reexposed to a 1% OVA aerosol for 20 minutes daily for 3 consecutive days, after complete resolution of initial airways inflammation. Collection and measurement of specimens. At various time points, mice were sacrificed and bronchoalveolar lavage (BAL) was performed according to standard protocol (11). Briefly, the lungs were dissected and the trachea was cannulated with a polyethylene tube (Becton Dickinson and Co., Sparks, Maryland, USA). The lungs were lavaged twice with PBS (0.25 ml followed by 0.2 ml); approximately 0.3 ml of the instilled fluid was consistently recovered. Total cell counts were determined using a hemocytometer. Cell pellets were resuspended in PBS, and smears were prepared by cytocentrifugation (Shandon Inc., Pittsburgh, Pennsylvania, USA) at g for 2 minutes. Hema 3 (Biochemical Sciences Inc., Swedesboro, New Jersey, USA) was used to stain all smears. Differential counts of BAL cells were determined from at least 500 leukocytes using standard hemocytological criteria to classify the cells as neutrophils, eosinophils, lymphocytes, or macrophages/monocytes. Additionally, blood was collected by retro-orbital bleeding. Serum was obtained by centrifugation after incubating whole blood for 30 minutes at 37 C. Finally, lung tissue was fixed in 10% formalin and embedded in paraffin. Sections (3-µm thick) were stained with hematoxylin and eosin (H&E). Splenocyte culture. Spleens were harvested into sterile tubes containing sterile HBSS (Life Technologies Inc., Burlington, Ontario, Canada). Tissue was triturated between the ends of sterile frosted slides, and the resulting cell suspension was filtered through nylon mesh (BSH Thompson, Scarborough, Ontario, Canada). Red blood cells were lysed with ACK lysis buffer (0.5 M NH 4 Cl, 10 mm KHCO 3, and 0.1 nm Na 2 EDTA [ph ]). Remaining splenocytes were washed twice with HBSS and then resuspended in RPMI supplemented with 10% FBS (Life Technologies Inc.), 1% L-glutamine, 1% penicillin/streptomycin. Cells were Figure 1 Airway eosinophilia in BAL of C57BL/6 (WT) and LT-α deficient (LTα-KO) mice exposed to aerosolized OVA in the context of GM-CSF expression. Over a period of 10 consecutive days, mice were exposed daily to OVA. Twenty-four hours before first exposure, mice were infected intranasally with adenoviral construct expressing GM-CSF. Data were obtained 48 hours after last exposure to OVA. (Mean ± SEM; n = 4 6; statistical analysis was performed using one-way ANOVA with Fisher s post hoc test; *P < 0.05.) 578 The Journal of Clinical Investigation August 2001 Volume 108 Number 4
3 cultured in medium alone or with 40 µg OVA per well at cells per well in a flat-bottom, 96-well plate (Becton Dickinson, Franklin Lakes, New Jersey, USA). After 5 days of culture, supernatants were harvested for cytokine measurements. Cytokine and Ig measurement. ELISA kits for murine IL-13, and IFN-γ, were purchased from R&D Systems Inc. (Minneapolis, Minnesota, USA), whereas the kit for murine IL-5 was obtained from Amersham Pharmacia Biotech (Buckinghamshire, United Kingdom). Each of these assays has a threshold of detection of 3 5 pg/ml. Levels of OVA-specific IgE were measured using an antigen-capture ELISA method described previously (11). Flow cytometric analysis. Flow cytometric analysis was performed on lung cells isolated as described previously with slight modifications (11). Briefly, total lung mononuclear cells were isolated by collagenase digestion (Collagenase type III; Life Technologies Inc., Rockville, Maryland, USA) followed by discontinuing gradient centrifugation in 30% and 60% Percoll (Pharmacia Biotech AB, Uppsala, Sweden). Interface containing mononuclear cells was collected, washed twice with PBS, and stained with a panel of antibodies. In addition, we performed flow cytometric analyses on white blood cells. To this end, blood was collected from the abdominal vein into 1-ml syringes coated with heparin. Red blood cells were lysed with lysing buffer (150 mm NH4Cl, 0.1 mm disodium EDTA, and 10 nm NaHCO3), and samples were subjected to three washes with PBS. Total white cell number in peripheral blood was counted with a hemocytometer, and cells were stained with appropriate antibodies. The following antibodies were purchased from PharMingen (Mississauga, Ontario, Canada): anti-cd3 (PEconjugated 145-2CII), anti-cd4 (biotin-conjugated L3T4), and anti-mhc class II (FITC-conjugated ). The T1/ST2 (3E10) antibody was provided by Millennium Pharmaceuticals Inc. (Cambridge, Massachusetts, USA), and FITC was labeled in-house according to a standard protocol (12). To minimize nonspecific binding, 106 cells were preincubated with FcBlock (CD16/CD32; PharMingen). For each antibody combination, 106 cells were incubated with mab s at 0 4 C for 30 minutes; the cells were then washed and treated with second-stage reagents. Streptavidin PerCP (Becton Dickinson Immunocytometry Systems, San Jose, California, USA) was used as a second-step reagent for detection of biotin-labeled antibodies. Titration was used to determine the optimal concentration for each antibody. Cells were fixed in 1% paraformaldehyde and counted on a FACScan (Becton Dickinson and Co.), and analyses were performed using WinMDI software (The Scripps Research Institute, La Jolla, California, USA). A total of 20,000 30,000 events were acquired. Surgical removal of spleen. Mice were anesthetized with isoflurane, and buprenorphine was administered subcutaneously. Splenectomy was preformed as described The Journal of Clinical Investigation previously (13). After surgical skin preparation, the spleen was exteriorized through a 1-cm left subcostal incision. The splenic artery and vein were double ligated and the spleen was removed. The peritoneum and skin were closed in separate layers using 4.0 absorbable suture. Mice were rested for 10 days before commencement of our allergic sensitization protocol. Data analysis. Data are expressed as mean ± SEM. Statistical interpretation was performed using ANOVA with Fisher s post hoc test or Student s t test. Differences were considered statistically significant when P < Results Immune-inflammatory responses in the airway. LTα-KO mice and WT littermates subjected to our protocol of respiratory mucosal allergic sensitization were sacrificed 48 hours after the last OVA aerosolization, and the BAL cellular profile was assessed (Figure 1). The BAL cellular content in naive mice from either strain was very similar. Compared with naive controls, both strains mounted an inflammatory response after sensitization. The extent of the response in WT mice was similar to that reported previously (11). Interestingly, the inflammatory response detected in the BAL of LTα-KO mice was approximately five times greater than that observed in sensitized WT mice. Owing to the unequal variance between strains, Figure 2 Light photomicrograph of paraffin-embedded sections of lung tissues. Over a period of 10 consecutive days, mice were exposed to OVA, and tissues were obtained 48 hours after last exposure. Sections were stained with H&E. Panels represent naive mice (a and b) and mice exposed to OVA in the context of GM-CSF expression (c f). 50 (a d); 200 (e and f). August 2001 Volume 108 Number 4 579
4 Figure 3 T1/ST2 expression on T cells obtained from lung tissues after exposure to OVA in the context of GM-CSF. Lungs were collected 48 hours after last exposure and subjected to enzymatic digestion. Cells were stained with mab s against CD3, CD4, and T1/ST2 and analyzed by flow cytometry. Histograms were gated on CD3 + /CD4 + T lymphocytes. Open histograms represent the background staining with the isotype control antibody. Data are representative of two independent experiments that yielded similar results. statistical significance between naive and OVA-treated WT mice was not reached, as assessed by one-way ANOVA. However, a t test conducted only on WT mice showed statistical significance. Proportionately, the percentage of eosinophils in LTα-KO and WT mice was similar (15.5 ± 2.0% vs ± 2.5%, respectively); in contrast, the percentage of lymphocytes in LTα-KO mice was considerably greater, 37 ± 5% vs. 5 ± 3% in WT mice. Histological examination of lung tissues paralleled the findings observed in the BAL (Figure 2). In agreement with our previous reports, sensitized WT mice showed a marked accumulation of inflammatory cells that was both perivascular and peribronchial; evidence of goblet cell hyperplasia and mucus production was readily apparent. In naive LTα-KO mice, there was no indication of peribronchial inflammation, but we observed scattered mild mononuclear perivascular infiltrates. The response to allergic sensitization was qualitatively similar in both strains, with extensive peribronchial inflammation characterized primarily by eosinophils and mononuclear cells. Of note, the perivascular infiltrate of LTα-KO mice was rather massive and consisted almost exclusively of mononuclear cells. To determine whether the considerable infiltration of mononuclear cells reflected an accumulation of Th2 cells, we examined the percentage of CD4 + T cells expressing T1/ST2, a putative marker of Th2 polarized cells (14). As indicated in the histograms shown in Figure 3, the percentage of CD3 + /CD4 + cells expressing this marker was similar in naive mice of both strains. This percentage increased approximately threefold in both WT and LTα-KO mice after OVA sensitization. Flow cytometric analysis of lung cells from naive C57BL/6 and LTα-KO mice. Given that the airway inflammatory response observed in LTα-KO mice was considerably greater than that observed in WT controls, we used flow cytometric analysis to investigate aspects of the immunological status of lungs from naive mice of both strains. Figure 4a shows the absolute number of lung Figure 4 Flow cytometric analysis of T cells (CD3 + /CD4 + ) and APC (MHC II + ) obtained from lungs of naive C57BL/6 and LTα-KO. (a) Lung mononuclear cell fraction was obtained by enzymatic digestion of whole lung. Lung cells from three to four mice were pooled for each group. Bars represent data obtained from three independent experiments. (Mean ± SEM; statistical analysis was performed using Student s t test; *P < 0.05.) (b) Cells were stained with indicated antibodies or alternatively with isotype controls, and 30,000 events were collected. Data are representative of three independent experiments that yielded similar results. 580 The Journal of Clinical Investigation August 2001 Volume 108 Number 4
5 Figure 5 In vivo rechallenge of C57BL/6 (WT) and LT-α deficient (LTα-KO) mice exposed to OVA in the context of GM-CSF. At day 60, after complete resolution of the airway inflammation, mice were reexposed to aerosolized OVA for 3 consecutive days. Data show total cell number and differential of cells obtained 72 hours after last challenge from BAL (mean ± SEM; n = 4 6; statistical analysis was performed using Student s t test; *P < 0.05). mononuclear cells isolated. In agreement with our histological observations, the number of mononuclear cells in LTα-KO mice was approximately 40% greater, although the percentage of CD3 + /CD4 + cells was similar in both strains, at approximately 14% (Figure 4b). In contrast, the percentage of cells expressing MHC II was greater in LTα-KO mice (29%) than in WT mice (7%), suggesting that LTα-KO mice may have intrinsically enhanced antigen-presenting capability. Long term in vivo OVA recall responses. Next, we examined the impact of LN deficiency on the generation of longterm antigen-specific memory. After complete resolution of the acute airway inflammatory response, mice were reexposed to OVA (day 60). Seventy-two hours after the last exposure, they were sacrificed and the BAL cellular response assessed. As shown in Figure 5, LTα-KO mice mounted a robust mononuclear and eosinophilic airway inflammatory response upon OVA reexposure. Cytokine production of cultured splenocytes and OVA-specific serum IgE. Effector cytokines were measured in the supernatant of splenocyte cultures. This was done for two reasons: first, our experience is that it is generally difficult to detect cytokines in the BAL of mice with a C57BL/6 background in our model; second, it was particularly important in these studies to obtain evidence of systemic Th effector activity. As shown in Table 1, the levels of IFN-γ, IL-5, and IL-13 detected in the supernatant of unstimulated splenocytes from either strain was very low. Splenocytes from sensitized mice of both strains produced considerably greater levels of these three cytokines. This response was three to four times greater in LTα-KO mice. Table 1 provides additional evidence with respect to levels of OVA-specific IgE in serum, indicating that the response was quantitatively similar in WT as in LTα-KO mice subjected to the protocol of allergic sensitization. Impact of splenectomy in the generation of allergic sensitization. We addressed the role of the spleen in the generation of allergic airway inflammation. To this end, we surgically removed spleens of both WT and LTα-KO mice and, after full recovery, subjected the mice to the respiratory mucosal allergic sensitization protocol. The airway inflammatory response in splenectomized WT mice was not significantly different from that observed in eusplenic sensitized control mice (Figure 6a). In contrast, splenectomized LTα-KO mice were unable to generate an airway inflammatory response. In fact, total and differential cell counts in the BAL were identical to those of naive LTα-KO mice (Figure 6b). The histological evaluation of lungs from these mice agreed with the BAL data (Figure 6c). Peripheral blood changes before and after splenectomy. To assess the impact of splenectomy on number and distribution of white blood cells (specifically T cells and B cells) in the peripheral blood, blood samples were collected before and 10 days after surgical removal of the spleen and subjected to flow cytometric analyses. Total white blood cell counts were greater in LTα-KO than in WT mice preceding and following splenectomy (Table 2). However, removal of the spleen did not result in significant changes in cell numbers in either WT or LTα- KO mice. In addition, although splenectomy in WT mice did not have an impact on T and B cells distribution, we observed an increase in both CD3 + /CD4 + and CD3 + /CD8 + cells in LTα-KO mice. Table 1 Antigen-specific cytokine and IgE production WT KO Medium OVA Medium OVA IFN-γ 14 ± ± ± ± 4967 IL-5 0 ± 0 82 ± 44 0 ± ± 121 IL ± ± ± ± 1037 Naive GM/OVA Naive GM/OVA IgE 2 ± ± 61 0 ± ± 32 For cytokine measurement, splenocytes were obtained from C57BL/6 (WT) or LTα-KO (KO) mice after nine OVA exposures. Cells were cultured for 5 days in medium alone or stimulated with OVA. Data represent picograms per milliliter, mean ± SEM; n = 4 per group. Levels of OVA-specific IgE were measured in serum of WT and KO mice obtained 48 hours after last OVA exposure. Data represent units per milliliter, mean ± SEM; n = 4 per group. The Journal of Clinical Investigation August 2001 Volume 108 Number 4 581
6 Figure 6 Impact of splenectomy on the generation of inflammation in airways of C57BL/6 and LTα-KO mice. Mice were splenectomized as described in Methods. Ten days after surgery, mice were infected intranasally with Ad/GM-CSF and subsequently exposed to OVA. BAL samples were obtained 48 hours after last OVA exposure from C57BL/6 (a) and LTα- KO (b) mice. (Mean ± SEM; n = 4; statistical analysis was performed using ANOVA with Fisher s post hoc test; *P < 0.05.) (c) Light photomicrograph of lung sections stained with H&E. 50. Discussion To our knowledge, this is the first demonstration of intact antigen-specific Th2 immunity upon mucosal sensitization of LTα-KO mice. Indeed, compared with WT mice, LTα-KO mice responded to OVA aerosolization in the context of GM-CSF with a similar pattern of T1/ST2 expression on Th2 cells and a robust Th2-associated inflammatory response characterized primarily by eosinophilia in the lung tissue. Moreover, after resolution of the initial response, OVA reexposure readily reconstituted airway eosinophilic inflammation, indicating antigen specificity and the persistence of immunological memory. As further evidence of Th2 immunity, LTα-KO mice were able to generate OVAspecific IgE responses. This is of particular interest in the light of previous data indicating the compromised ability of LTα-KO mice to generate antibody responses against KLH, HSV-1, and SRBC (9, 15). It is also of interest because germinal centers, which are considered to be essential for Ig isotype switching, are absent in these mutant mice. However, Matsumoto et al. (16) recently demonstrated near-normal affinity maturation and isotype switching in LTα-KO mice after repeated challenge with high doses of antigen (NP-OVA) together with an adjuvant. As suggested by Wang et al. (17) and illustrated by our experimental system, persistence of antigen in the context of adjuvant plausibly explains Ig affinity maturation of B cells outside germinal centers. The magnitude of the airway inflammatory response in LTα-KO mice exposed to aerosolized OVA in the context of GM-CSF was rather striking. Indeed, whether in terms of total number of cells or of differential cell counts, the degree of the inflammatory response in the mutant mice was four- to sixfold greater than that observed in WT controls. As documented histologically (Figure 2), and in agreement with Banks et al. (9), part of the reason may be that there is an increased number of mononuclear cells in the perivascular areas of naive mutant mice. However, this difference (Figure 4a) appears quantitatively insufficient to explain the changes documented after exposure to our allergic sensitization protocol. A contributing factor may be that, as a result of lacking lymphoid structures (other than the spleen), there is an increased number of immune cells circulating in LTα-KO mice, as described previously by De Togni et al. (8) and confirmed in our studies (Table 2). We provide evidence of an additional, potentially important mechanism underlying the enhanced immune responsiveness observed in the mutant mice: a dramatic increase in the number of MHCII + cells in the lung of naive mice: 29% in LTα-KO versus 7% in WT mice. That LTα-KO mice have an increased capacity for presenting antigen may also explain the very recent observation by Lee et al. (18) of enhanced immune responses of LTα-KO mice to murine gammaherpes virus 68. Compelled by the observation that mice lacking LN were able to generate Th2 immunity and airway eosinophilic inflammation, we investigated whether the spleen, albeit architecturally aberrant in LTα-KO mice, was able to compensate as the site of the primary immune response. The ability of splenocytes from LTα- KO mice subjected to repeated OVA aerosolizations in the context of GM-CSF to produce cytokines upon OVA recall in vitro argues for the role of the spleen in this Table 2 Changes in peripheral blood lymphocytes following splenectomy WBC CD3 + /CD4 + CD3 + /CD8 + B220 + (cells 10 6 /ml) (%) (%) (%) WT/+SP 5.8 ± ± ± ± 3.3 WT/ SP 8.6 ± ± ± ± 5.5 KO/+SP 33.2 ± 8.8 A 17.5 ± ± ± 2.0 KO/ SP 24.7 ± 3.6 B 27.7 ± 0.1 C 17.8 ± 1.4 C 59.8 ± 4.8 Changes in peripheral blood were collected from naive C57BL/6 (WT) and LTα-KO (KO) mice before (+SP) or after ( SP) splenectomy as described in Methods. Cells were stained with antibodies against indicated markers and subjected to flow cytometric analysis. A gate was set up for lymphocytes and 30,000 events were collected. A Statistically different from WT/+SP. B Statistically different from WT/ SP. C Statistically different from KO/+SP. 582 The Journal of Clinical Investigation August 2001 Volume 108 Number 4
7 process. That cytokine content in splenocyte cultures supernatant was, in fact, two to three times greater in LTα-KO mice than in WT control mice suggests an immune response of greater strength in the mutant mice. A decisive functional role for the spleen in allergic sensitization was provided by the splenectomy experiments. Indeed, splenectomy of LTα-KO mice fully prevented the development of airway inflammation. Our data are different from those of Davis et al. (13), who demonstrated that removal of the spleen in LTα-KO mice decreased, but did not abrogate, humoral responses to Salmonella in intestines. In our experiments, mice were subjected to allergic sensitization protocol 10 days after splenectomy; at this time, the peripheral cell counts of LTα-KO mice before and after splenectomy were not significantly different, indicating that the absence of sensitization and airway inflammation was not due to depletion of circulatory leukocytes and, specifically, of T cells (CD3 + /CD4 + and CD3 + /CD8 + ) or B cells (Table 2). Although these data demonstrate that the spleen indeed supplanted the role of the regional LN in LTα-KO mice, splenectomy of WT mice had no impact on the ability of asplenic mice to generate allergic sensitization and airway inflammation. Our current understanding of the generation of mucosal immunity is that antigens penetrating mucosae are captured by DCs and transported to the draining LNs to initiate immune responses (7). The data presented here indicate that the spleen can facilitate allergic sensitization to antigens introduced into the respiratory mucosae. This observation evokes an important question: How does aerosolized OVA reach the spleen to initiates allergic immunity? Wolvers et al. (5) have demonstrated that after OVA delivery to the nasal mucosae, there is evidence of APCs transporting this antigen to the spleen. This DC migration may occur via the bloodstream or, presumably, through the lymphatic system, which, importantly, remains intact in LTα-KO mice. In our experimental system, OVA aerosolization leads to eosinophilic airway inflammation only in the context of GM-CSF transgene expression. Such expression is compartmentalized within the lung/airway, as GM-CSF cannot be detected in the circulation. Therefore, we surmise that it is very unlikely that exogenous GM-CSF expression in the spleen contributed to the ability of LTα-KO mice to generate allergic sensitization. Thus, our data intimate that the generation of allergic priming in the spleen of mice lacking LNs may be the result of mobilization of OVA-carrying DC from the respiratory mucosae. In short, our data show that allergic sensitization and airway inflammation take place in the absence of thoracic (and other) LNs. That these responses are abrogated in splenectomized mice establishes the essential requirement of secondary lymphoid organs and implies that the lung does not possess the intrinsic capability to generate allergic sensitization. That the spleen can supplant the role of the draining LNs illustrates the plasticity of the immune system and highlights the systemic nature of allergic sensitization. What is the potential clinical significance of these findings? The current emphasis of the pharmacological management of asthma rests on local treatment, which effectively inhibits inflammatory processes that take place in the airway itself. However, one would argue that processes that are generated, and probably maintained, outside the airway will likely evade this treatment strategy. Thus, attempts to ultimately cure, rather than control, allergic airway inflammation may need to incorporate a systemic dimension. Acknowledgments This research has been supported by grants from the Canadian Institutes of Health Research (CIHR). We also acknowledge the support of the Hamilton Health Science Corp. and the St. Joseph Hospital Foundation. B.U. Gajewska and D. Alvarez hold CIHR doctoral fellowships. M.R. Stämpfli holds a Parker B. Francis Fellowship. We are grateful to Monika Cwiartka for technical support, Mary Kiriakopoulos for secretarial assistance, and Ryan E. Wiley for critical review of the manuscript. 1. Banchereau, J., and Steinman, R.M Dendritic cells and control of immunity. Nature. 392: Lambrecht, B.N., et al Myeloid dendritic cells induce Th2 responses to inhaled antigen leading to eosinophilic airway inflammation. J. Clin. Invest. 106: Lambrecht, B.N., Pauwels, R.A., and Fazekas De St. Groth, B Induction of rapid T cell activation, division, and recirculation by intratracheal injection of dendritic cells in a TCR transgenic model. J. Immunol. 164: Xia, W., Pinto, C.E., and Kradin, R.L The antigen-presenting activities of Ia + dendritic cells shift dynamically from lung to lymph node after an airway challenge with soluble antigen. J. Exp. Med. 181: Wolvers, D.D., et al Intranasally induced immunological tolerance is determined by characteristics of the draining lymph nodes: studies with OVA and human cartilage gp-39. J. Immunol. 162: Hoyne, G.F., Askonas, B.A., Hetzel, C., Thomas, W.R., and Lamb, J.R Regulation of house dust mite responses by intranasally administered peptide: transient activation of CD4+ T cells precedes the development of tolerance in vivo. Int. Immunol. 8: Vermaelen, K.Y., Carro-Muino, I., Lambrecht, B.N., and Pauwels, R.A Specific migratory dendritic cells rapidly transport antigen from the airways to the thoracic lymph nodes. J. Exp. Med. 193: De Togni, P., et al Abnormal development of peripheral lymphoid organs in mice deficient in lymphotoxin. Science. 264: Fu, Y.X., et al Lymphotoxin-alpha (LTalpha) supports development of splenic follicular structure that is required for IgG responses. J. Exp. Med. 185: Ruddle, N.H Lymphoid neo-organogenesis: lymphotoxin s role in inflammation and development. Immunol. Res. 19: Stämpfli, M.R., et al GM-CSF transgene expression in the airway allows aerosolized ovalbumin to induce allergic sensitization in mice. J. Clin. Invest. 102: Golding, J.W Conjugation of antibodies with fluorochromes: modification of the standard method. J. Immunol. Methods. 13: Davis, I.A., Knight, K.A., and Rouse, B.T The spleen and organized lymph nodes are not essential for the development of gut-induced mucosal immune responses in lymphotoxin-alpha deficient mice. Clin. Immunol. Immunopathol. 89: Lohning, M., et al T1/ST2 is preferentially expressed on murine Th2 cells, independent of interleukin 4, interleukin 5, and interleukin 10, and important for Th2 effector function. Proc. Natl. Acad. Sci. USA. 95: Banks, T.A., et al Lymphotoxin-alpha-deficient mice. Effects on secondary lymphoid organ development and humoral immune responsiveness. J. Immunol. 155: Matsumoto, M., et al Affinity maturation without germinal centres in lymphotoxin-alpha-deficient mice. Nature. 382: Wang, Y., et al Antigen persistence is required for somatic mutation and affinity maturation of immunoglobulin. Eur. J. Immunol. 30: Lee, B.J., Santee, S., Von Gejsen, S., Ware, C.F., and Sarawar, S.R Lymphotoxin-alpha-deficient mice can clear a productive infection with murine gammaherpesvirus 68 but fail to develop splenomegaly or lymphocytosis. J. Virol. 74: The Journal of Clinical Investigation August 2001 Volume 108 Number 4 583
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
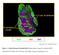 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
Rapid antigen-specific T cell enrichment (Rapid ARTE)
 Direct ex vivo characterization of human antigen-specific CD154+CD4+ T cell Rapid antigen-specific T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central role
Direct ex vivo characterization of human antigen-specific CD154+CD4+ T cell Rapid antigen-specific T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central role
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary Figures
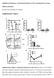 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
SUPPLEMENTARY INFORMATION
 Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Supplementary Information:
 Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
METHODS Penh. Measurements and ribonuclease protection assay. Intracellular cytokine staining. ELISAs RT-PCR. Lung morphometry.
 METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
SUPPLEMENTARY INFORMATION
 doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE)
 Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central
Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central
Supplementary Figure 1. Characterization of basophils after reconstitution of SCID mice
 Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Myeloid dendritic cells induce Th2 responses to inhaled antigen, leading to eosinophilic airway inflammation
 Myeloid dendritic cells induce Th2 responses to inhaled antigen, leading to eosinophilic airway inflammation Bart N. Lambrecht, 1,2 Marijke De Veerman, 3 Anthony J. Coyle, 4 Jose-Carlos Gutierrez-Ramos,
Myeloid dendritic cells induce Th2 responses to inhaled antigen, leading to eosinophilic airway inflammation Bart N. Lambrecht, 1,2 Marijke De Veerman, 3 Anthony J. Coyle, 4 Jose-Carlos Gutierrez-Ramos,
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
SUPPLEMENTARY INFORMATION
 Supplemental Figure 1. Furin is efficiently deleted in CD4 + and CD8 + T cells. a, Western blot for furin and actin proteins in CD4cre-fur f/f and fur f/f Th1 cells. Wild-type and furin-deficient CD4 +
Supplemental Figure 1. Furin is efficiently deleted in CD4 + and CD8 + T cells. a, Western blot for furin and actin proteins in CD4cre-fur f/f and fur f/f Th1 cells. Wild-type and furin-deficient CD4 +
Sipper BK Experimental Animal Co. (Shanghai, China) and bred in a specific. pathogen-free environment. The animal study protocol was approved by the
 Supplementary information, Data S1 Materials and Methods Mice, Ad vectors and reagents Female C57BL/6 mice, 8-10 weeks of age, were purchased from Joint Ventures Sipper BK Experimental Animal Co. (Shanghai,
Supplementary information, Data S1 Materials and Methods Mice, Ad vectors and reagents Female C57BL/6 mice, 8-10 weeks of age, were purchased from Joint Ventures Sipper BK Experimental Animal Co. (Shanghai,
Supporting Online Material for
 www.sciencemag.org/cgi/content/full/1175194/dc1 Supporting Online Material for A Vital Role for Interleukin-21 in the Control of a Chronic Viral Infection John S. Yi, Ming Du, Allan J. Zajac* *To whom
www.sciencemag.org/cgi/content/full/1175194/dc1 Supporting Online Material for A Vital Role for Interleukin-21 in the Control of a Chronic Viral Infection John S. Yi, Ming Du, Allan J. Zajac* *To whom
The Effect of BTP on the Development of Allergic Asthma in Mice
 93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD-
 Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Introduction to Immunology Part 2 September 30, Dan Stetson
 Introduction to Immunology Part 2 September 30, 2016 Dan Stetson stetson@uw.edu 441 Lecture #2 Slide 1 of 26 CLASS ANNOUNCEMENT PLEASE NO TREE NUTS IN CLASS!!! (Peanuts, walnuts, almonds, cashews, etc)
Introduction to Immunology Part 2 September 30, 2016 Dan Stetson stetson@uw.edu 441 Lecture #2 Slide 1 of 26 CLASS ANNOUNCEMENT PLEASE NO TREE NUTS IN CLASS!!! (Peanuts, walnuts, almonds, cashews, etc)
IMMUNOLOGICAL MEMORY. CD4 T Follicular Helper Cells. Memory CD8 T Cell Differentiation
 IMMUNOLOGICAL MEMORY CD4 T Follicular Helper Cells Memory CD8 T Cell Differentiation CD4 T Cell Differentiation Bcl-6 T-bet GATA-3 ROR t Foxp3 CD4 T follicular helper (Tfh) cells FUNCTION Provide essential
IMMUNOLOGICAL MEMORY CD4 T Follicular Helper Cells Memory CD8 T Cell Differentiation CD4 T Cell Differentiation Bcl-6 T-bet GATA-3 ROR t Foxp3 CD4 T follicular helper (Tfh) cells FUNCTION Provide essential
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Evaluation of directed and random motility in microslides Assessment of leukocyte adhesion in flow chambers
 Evaluation of directed and random motility in microslides Motility experiments in IBIDI microslides, image acquisition and processing were performed as described. PMN, which ended up in an angle < 180
Evaluation of directed and random motility in microslides Motility experiments in IBIDI microslides, image acquisition and processing were performed as described. PMN, which ended up in an angle < 180
Putting it Together. Stephen Canfield Secondary Lymphoid System. Tonsil Anterior Cervical LN s
 Putting it Together Stephen Canfield smc12@columbia.edu Secondary Lymphoid System Tonsil Anterior Cervical LN s Axillary LN s Mediastinal/Retroperitoneal LN s Thoracic Duct Appendix Spleen Inguinal LN
Putting it Together Stephen Canfield smc12@columbia.edu Secondary Lymphoid System Tonsil Anterior Cervical LN s Axillary LN s Mediastinal/Retroperitoneal LN s Thoracic Duct Appendix Spleen Inguinal LN
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic
 Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Detailed step-by-step operating procedures for NK cell and CTL degranulation assays
 Supplemental methods Detailed step-by-step operating procedures for NK cell and CTL degranulation assays Materials PBMC isolated from patients, relatives and healthy donors as control K562 cells (ATCC,
Supplemental methods Detailed step-by-step operating procedures for NK cell and CTL degranulation assays Materials PBMC isolated from patients, relatives and healthy donors as control K562 cells (ATCC,
Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice
 Supplementary Methods: Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice and gently meshed in DMEM containing 10% FBS to prepare for single cell suspensions. CD4 + CD25
Supplementary Methods: Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice and gently meshed in DMEM containing 10% FBS to prepare for single cell suspensions. CD4 + CD25
Supporting Information
 Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Krishnamoorthy et al.,
 Krishnamoorthy et al., c d e ND ND Supplementary Figure 1 RSV-induces inflammation even in the asence of allergen. Tolerized pups were either infected with RSV or not. The mice were sacrificed a week following
Krishnamoorthy et al., c d e ND ND Supplementary Figure 1 RSV-induces inflammation even in the asence of allergen. Tolerized pups were either infected with RSV or not. The mice were sacrificed a week following
Interferon γ regulates idiopathic pneumonia syndrome, a. Th17 + CD4 + T-cell-mediated GvH disease
 Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
PBS Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs , 27-30
 PBS 803 - Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs. 15-25, 27-30 Learning Objectives Compare and contrast the maturation of B and T lymphocytes Compare and contrast
PBS 803 - Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs. 15-25, 27-30 Learning Objectives Compare and contrast the maturation of B and T lymphocytes Compare and contrast
Th2 responses induced by epicutaneous or inhalational protein exposure are differentially dependent on IL-4
 Th2 responses induced by epicutaneous or inhalational protein exposure are differentially dependent on IL-4 Christina A. Herrick, 1,2 Heather MacLeod, 2 Earl Glusac, 1,3 Robert E. Tigelaar, 1,2 and Kim
Th2 responses induced by epicutaneous or inhalational protein exposure are differentially dependent on IL-4 Christina A. Herrick, 1,2 Heather MacLeod, 2 Earl Glusac, 1,3 Robert E. Tigelaar, 1,2 and Kim
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
Measuring Dendritic Cells
 Measuring Dendritic Cells A.D. Donnenberg, V.S. Donnenberg UNIVERSITY of PITTSBURGH CANCER INSTITUTE CCS Longbeach 10_04 Measuring DC Rare event detection The basics of DC measurement Applications Cancer
Measuring Dendritic Cells A.D. Donnenberg, V.S. Donnenberg UNIVERSITY of PITTSBURGH CANCER INSTITUTE CCS Longbeach 10_04 Measuring DC Rare event detection The basics of DC measurement Applications Cancer
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
SUPPLEMENTARY FIGURE 1
 SUPPLEMENTARY FIGURE 1 A LN Cell count (1 ) 1 3 1 CD+ 1 1 CDL lo CD hi 1 CD+FoxP3+ 1 1 1 7 3 3 3 % of cells 9 7 7 % of cells CD+ 3 1 % of cells CDL lo CD hi 1 1 % of CD+ cells CD+FoxP3+ 3 1 % of CD+ T
SUPPLEMENTARY FIGURE 1 A LN Cell count (1 ) 1 3 1 CD+ 1 1 CDL lo CD hi 1 CD+FoxP3+ 1 1 1 7 3 3 3 % of cells 9 7 7 % of cells CD+ 3 1 % of cells CDL lo CD hi 1 1 % of CD+ cells CD+FoxP3+ 3 1 % of CD+ T
Organic dust-induced interleukin-12 production activates T- and natural killer cells
 Eur Respir J 22; 2: 686 69 DOI:.1183/931936.2.222 Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Organic dust-induced interleukin-12 production
Eur Respir J 22; 2: 686 69 DOI:.1183/931936.2.222 Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Organic dust-induced interleukin-12 production
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation
 Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Interleukin-2-Dependent Allergen-Specific Tissue-Resident Memory Cells Drive Asthma
 Immunity Supplemental Information Interleukin-2-Dependent Allergen-Specific Tissue-Resident Memory Cells Drive Asthma Brian D. Hondowicz, Dowon An, Jason M. Schenkel, Karen S. Kim, Holly R. Steach, Akshay
Immunity Supplemental Information Interleukin-2-Dependent Allergen-Specific Tissue-Resident Memory Cells Drive Asthma Brian D. Hondowicz, Dowon An, Jason M. Schenkel, Karen S. Kim, Holly R. Steach, Akshay
MagniSort Mouse CD4 Naive T cell Enrichment Kit Catalog Number: RUO: For Research Use Only. Not for use in diagnostic procedures.
 Page 1 of 2 MagniSort Mouse CD4 Naive T cell Enrichment Kit RUO: For Research Use Only. Not for use in diagnostic procedures. Mouse splenocytes were unsorted (left) or sorted with the MagniSort Mouse CD4
Page 1 of 2 MagniSort Mouse CD4 Naive T cell Enrichment Kit RUO: For Research Use Only. Not for use in diagnostic procedures. Mouse splenocytes were unsorted (left) or sorted with the MagniSort Mouse CD4
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
Mouse Total IgA Antibody Detection Kit
 Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs
 Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs (idcs) and mature DCs (mdcs). A myeloma cell line expressing
Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs (idcs) and mature DCs (mdcs). A myeloma cell line expressing
Supplementary Figures
 Supplementary Figures Supplementary Fig. 1. Surface thiol groups and reduction of activated T cells. (a) Activated CD8 + T-cells have high expression levels of free thiol groups on cell surface proteins.
Supplementary Figures Supplementary Fig. 1. Surface thiol groups and reduction of activated T cells. (a) Activated CD8 + T-cells have high expression levels of free thiol groups on cell surface proteins.
Lecture 9: T-cell Mediated Immunity
 Lecture 9: T-cell Mediated Immunity Questions to Consider How do T cells know where to go? Questions to Consider How do T cells know where to go? How does antigen get targeted to a T cell expressing the
Lecture 9: T-cell Mediated Immunity Questions to Consider How do T cells know where to go? Questions to Consider How do T cells know where to go? How does antigen get targeted to a T cell expressing the
LDL Uptake Flow Cytometry Assay Kit
 LDL Uptake Flow Cytometry Assay Kit Item No. 601470 www.caymanchem.com Customer Service 800.364.9897 Technical Support 888.526.5351 1180 E. Ellsworth Rd Ann Arbor, MI USA TABLE OF CONTENTS GENERAL INFORMATION
LDL Uptake Flow Cytometry Assay Kit Item No. 601470 www.caymanchem.com Customer Service 800.364.9897 Technical Support 888.526.5351 1180 E. Ellsworth Rd Ann Arbor, MI USA TABLE OF CONTENTS GENERAL INFORMATION
W/T Itgam -/- F4/80 CD115. F4/80 hi CD115 + F4/80 + CD115 +
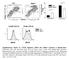 F4/8 % in the peritoneal lavage 6 4 2 p=.15 n.s p=.76 CD115 F4/8 hi CD115 + F4/8 + CD115 + F4/8 hi CD115 + F4/8 + CD115 + MHCII MHCII Supplementary Figure S1. CD11b deficiency affects the cellular responses
F4/8 % in the peritoneal lavage 6 4 2 p=.15 n.s p=.76 CD115 F4/8 hi CD115 + F4/8 + CD115 + F4/8 hi CD115 + F4/8 + CD115 + MHCII MHCII Supplementary Figure S1. CD11b deficiency affects the cellular responses
B6/COLODR/SPL/11C/83/LAP/#2.006 B6/COLODR/SPL/11C/86/LAP/#2.016 CD11C B6/COLODR/SPL/11C/80/LAP/#2.011 CD11C
 CD3-specific antibody-induced immune tolerance and suppression of autoimmune encephalomyelitis involves TGF-β production through phagocytes digesting apoptotic T cells Sylvain Perruche 1,3, Pin Zhang 1,
CD3-specific antibody-induced immune tolerance and suppression of autoimmune encephalomyelitis involves TGF-β production through phagocytes digesting apoptotic T cells Sylvain Perruche 1,3, Pin Zhang 1,
Comprehensive evaluation of human immune system reconstitution in NSG. and NSG -SGM3 mouse models toward the development of a novel ONCO-HU
 Comprehensive evaluation of human immune system reconstitution in NSG and NSG -SGM3 mouse models toward the development of a novel ONCO-HU xenograft model Aaron Middlebrook, 1 Eileen Snowden, 2 Warren
Comprehensive evaluation of human immune system reconstitution in NSG and NSG -SGM3 mouse models toward the development of a novel ONCO-HU xenograft model Aaron Middlebrook, 1 Eileen Snowden, 2 Warren
Natural Killer T Cells Are Critical for Dendritic Cells to Induce Immunity in Chlamydial Pneumonia
 Natural Killer T Cells Are Critical for Dendritic Cells to Induce Immunity in Chlamydial Pneumonia Antony George Joyee 1, Hongyu Qiu 1, Yijun Fan 1, Shuhe Wang 1, and Xi Yang 1 1 Laboratory for Infection
Natural Killer T Cells Are Critical for Dendritic Cells to Induce Immunity in Chlamydial Pneumonia Antony George Joyee 1, Hongyu Qiu 1, Yijun Fan 1, Shuhe Wang 1, and Xi Yang 1 1 Laboratory for Infection
% of live splenocytes. STAT5 deletion. (open shapes) % ROSA + % floxed
 Supp. Figure 1. a 14 1 1 8 6 spleen cells (x1 6 ) 16 % of live splenocytes 5 4 3 1 % of live splenocytes 8 6 4 b 1 1 c % of CD11c + splenocytes (closed shapes) 8 6 4 8 6 4 % ROSA + (open shapes) % floxed
Supp. Figure 1. a 14 1 1 8 6 spleen cells (x1 6 ) 16 % of live splenocytes 5 4 3 1 % of live splenocytes 8 6 4 b 1 1 c % of CD11c + splenocytes (closed shapes) 8 6 4 8 6 4 % ROSA + (open shapes) % floxed
Mouse Anti-OVA IgM Antibody Assay Kit
 Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Resolution of a chronic viral infection after interleukin-10 receptor blockade
 ARTICLE Resolution of a chronic viral infection after interleukin-10 receptor blockade Mette Ejrnaes, 1 Christophe M. Filippi, 1 Marianne M. Martinic, 1 Eleanor M. Ling, 1 Lisa M. Togher, 1 Shane Crotty,
ARTICLE Resolution of a chronic viral infection after interleukin-10 receptor blockade Mette Ejrnaes, 1 Christophe M. Filippi, 1 Marianne M. Martinic, 1 Eleanor M. Ling, 1 Lisa M. Togher, 1 Shane Crotty,
Dendritic cells in cancer immunotherapy Aimin Jiang
 Dendritic cells in cancer immunotherapy Aimin Jiang Feb. 11, 2014 Dendritic cells at the interface of innate and adaptive immune responses Dendritic cells: initiators of adaptive immune responses Dendritic
Dendritic cells in cancer immunotherapy Aimin Jiang Feb. 11, 2014 Dendritic cells at the interface of innate and adaptive immune responses Dendritic cells: initiators of adaptive immune responses Dendritic
Supplemental Table I.
 Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
Efficient Isolation of Mouse Liver NKT Cells by Perfusion
 Efficient Isolation of Mouse Liver NKT Cells by Perfusion Xianfeng Fang 1,2, Peishuang Du 1, Yang Liu 3 *, Jie Tang 1 * 1 Center for Infection and Immunity, Institute of Biophysics, Chinese Academy of
Efficient Isolation of Mouse Liver NKT Cells by Perfusion Xianfeng Fang 1,2, Peishuang Du 1, Yang Liu 3 *, Jie Tang 1 * 1 Center for Infection and Immunity, Institute of Biophysics, Chinese Academy of
Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder I Nakaya, Kousik
 SUPPLEMENTARY FIGURES 1-19 T H 2 response to cysteine-proteases requires dendritic cell-basophil cooperation via ROS mediated signaling Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder
SUPPLEMENTARY FIGURES 1-19 T H 2 response to cysteine-proteases requires dendritic cell-basophil cooperation via ROS mediated signaling Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder
Immunology 2017: Lecture 12 handout. Secondary lymphoid organs. Dr H Awad
 Immunology 2017: Lecture 12 handout Secondary lymphoid organs Dr H Awad INTRODUCTION So far we discussed the cells of the immune system and how they recognize their antigens and get stimulated. The number
Immunology 2017: Lecture 12 handout Secondary lymphoid organs Dr H Awad INTRODUCTION So far we discussed the cells of the immune system and how they recognize their antigens and get stimulated. The number
Online Data Supplement. Induction of Pulmonary Granuloma Formation by Propionibacterium acnes is regulated by. MyD88 and Nox2
 Online Data Supplement Induction of Pulmonary Granuloma Formation by Propionibacterium acnes is regulated by MyD88 and Nox2 Jessica L. Werner *, Sylvia G. Escolero *, Jeff T. Hewlett *, Tim N. Mak *3,
Online Data Supplement Induction of Pulmonary Granuloma Formation by Propionibacterium acnes is regulated by MyD88 and Nox2 Jessica L. Werner *, Sylvia G. Escolero *, Jeff T. Hewlett *, Tim N. Mak *3,
Endogenous TNFα orchestrates the trafficking of neutrophils into and within lymphatic vessels during acute inflammation
 SUPPLEMENTARY INFORMATION Endogenous TNFα orchestrates the trafficking of neutrophils into and within lymphatic vessels during acute inflammation Samantha Arokiasamy 1,2, Christian Zakian 1, Jessica Dilliway
SUPPLEMENTARY INFORMATION Endogenous TNFα orchestrates the trafficking of neutrophils into and within lymphatic vessels during acute inflammation Samantha Arokiasamy 1,2, Christian Zakian 1, Jessica Dilliway
Supporting Information
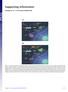 Supporting Information Aldridge et al. 10.1073/pnas.0900655106 Fig. S1. Flow diagram of sublethal (a) and lethal (b) influenza virus infections. (a) Infection of lung epithelial cells by influenza virus
Supporting Information Aldridge et al. 10.1073/pnas.0900655106 Fig. S1. Flow diagram of sublethal (a) and lethal (b) influenza virus infections. (a) Infection of lung epithelial cells by influenza virus
Integrin v 3 targeted therapy for Kaposi s sarcoma with an in vitro evolved antibody 1
 Integrin v 3 targeted therapy for Kaposi s sarcoma with an in vitro evolved antibody 1 CHRISTOPH RADER, 2 MIKHAIL POPKOV, JOHN A. NEVES, AND CARLOS F. BARBAS III 2 Department of Molecular Biology and The
Integrin v 3 targeted therapy for Kaposi s sarcoma with an in vitro evolved antibody 1 CHRISTOPH RADER, 2 MIKHAIL POPKOV, JOHN A. NEVES, AND CARLOS F. BARBAS III 2 Department of Molecular Biology and The
Adaptive Immunity: Humoral Immune Responses
 MICR2209 Adaptive Immunity: Humoral Immune Responses Dr Allison Imrie 1 Synopsis: In this lecture we will review the different mechanisms which constitute the humoral immune response, and examine the antibody
MICR2209 Adaptive Immunity: Humoral Immune Responses Dr Allison Imrie 1 Synopsis: In this lecture we will review the different mechanisms which constitute the humoral immune response, and examine the antibody
The Immune Response in Time and Space
 The Immune Response in Time and Space Chapters 14 & 4 Sharon S. Evans, Ph.D. Department of Immunology 845-3421 sharon.evans@roswellpark.org September 18 & 23, 2014 Inflammation Inflammation Complex response
The Immune Response in Time and Space Chapters 14 & 4 Sharon S. Evans, Ph.D. Department of Immunology 845-3421 sharon.evans@roswellpark.org September 18 & 23, 2014 Inflammation Inflammation Complex response
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Examples of questions for Cellular Immunology/Cellular Biology and Immunology
 Examples of questions for Cellular Immunology/Cellular Biology and Immunology Each student gets a set of 6 questions, so that each set contains different types of questions and that the set of questions
Examples of questions for Cellular Immunology/Cellular Biology and Immunology Each student gets a set of 6 questions, so that each set contains different types of questions and that the set of questions
NK cell flow cytometric assay In vivo DC viability and migration assay
 NK cell flow cytometric assay 6 NK cells were purified, by negative selection with the NK Cell Isolation Kit (Miltenyi iotec), from spleen and lymph nodes of 6 RAG1KO mice, injected the day before with
NK cell flow cytometric assay 6 NK cells were purified, by negative selection with the NK Cell Isolation Kit (Miltenyi iotec), from spleen and lymph nodes of 6 RAG1KO mice, injected the day before with
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Hematopoiesis. Hematopoiesis. Hematopoiesis
 Chapter. Cells and Organs of the Immune System Hematopoiesis Hematopoiesis- formation and development of WBC and RBC bone marrow. Hematopoietic stem cell- give rise to any blood cells (constant number,
Chapter. Cells and Organs of the Immune System Hematopoiesis Hematopoiesis- formation and development of WBC and RBC bone marrow. Hematopoietic stem cell- give rise to any blood cells (constant number,
Supplemental Figure 1
 Supplemental Figure 1 1a 1c PD-1 MFI fold change 6 5 4 3 2 1 IL-1α IL-2 IL-4 IL-6 IL-1 IL-12 IL-13 IL-15 IL-17 IL-18 IL-21 IL-23 IFN-α Mut Human PD-1 promoter SBE-D 5 -GTCTG- -1.2kb SBE-P -CAGAC- -1.kb
Supplemental Figure 1 1a 1c PD-1 MFI fold change 6 5 4 3 2 1 IL-1α IL-2 IL-4 IL-6 IL-1 IL-12 IL-13 IL-15 IL-17 IL-18 IL-21 IL-23 IFN-α Mut Human PD-1 promoter SBE-D 5 -GTCTG- -1.2kb SBE-P -CAGAC- -1.kb
CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma
 Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
The Adaptive Immune Response. B-cells
 The Adaptive Immune Response B-cells The innate immune system provides immediate protection. The adaptive response takes time to develop and is antigen specific. Activation of B and T lymphocytes Naive
The Adaptive Immune Response B-cells The innate immune system provides immediate protection. The adaptive response takes time to develop and is antigen specific. Activation of B and T lymphocytes Naive
Chapter 24 The Immune System
 Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Chapter 16 Lymphatic System and Immunity. Lymphatic Pathways. Lymphatic Capillaries. network of vessels that assist in circulating fluids
 Chapter 16 Lymphatic System and Immunity network of vessels that assist in circulating fluids closely associated with the cardiovascular system transports excess fluid away from interstitial spaces transports
Chapter 16 Lymphatic System and Immunity network of vessels that assist in circulating fluids closely associated with the cardiovascular system transports excess fluid away from interstitial spaces transports
The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF
 CORRECTION NOTICE Nat.Immunol. 12, 568 575 (2011) The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF Mohamed El-Behi, Bogoljub Ciric, Hong
CORRECTION NOTICE Nat.Immunol. 12, 568 575 (2011) The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF Mohamed El-Behi, Bogoljub Ciric, Hong
Chapter 2 (pages 22 33): Cells and Tissues of the Immune System. Prepared by Kristen Dazy, MD, Scripps Clinic Medical Group
 Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS; Andrew H. H. Lichtman, MD, PhD; and Shiv Pillai, MBBS, PhD. Chapter 2 (pages 22 33): Cells and
Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS; Andrew H. H. Lichtman, MD, PhD; and Shiv Pillai, MBBS, PhD. Chapter 2 (pages 22 33): Cells and
General Biology. A summary of innate and acquired immunity. 11. The Immune System. Repetition. The Lymphatic System. Course No: BNG2003 Credits: 3.
 A summary of innate and acquired immunity General iology INNATE IMMUNITY Rapid responses to a broad range of microbes Course No: NG00 Credits:.00 External defenses Invading microbes (pathogens). The Immune
A summary of innate and acquired immunity General iology INNATE IMMUNITY Rapid responses to a broad range of microbes Course No: NG00 Credits:.00 External defenses Invading microbes (pathogens). The Immune
Immunology 2011 Lecture 17 Lymphoid Tissue Architecture 13 October
 Immunology 2011 Lecture 17 Lymphoid Tissue Architecture 13 October TODAY Lymphoid Tissue Architecture, Chap. 16 APC Antigen processing (dendritic cells, MΦ et al.) Antigen "presentation" Ag/Ab complexes
Immunology 2011 Lecture 17 Lymphoid Tissue Architecture 13 October TODAY Lymphoid Tissue Architecture, Chap. 16 APC Antigen processing (dendritic cells, MΦ et al.) Antigen "presentation" Ag/Ab complexes
Supporting Information
 Supporting Information lpek et al. 1.173/pnas.1121217 SI Materials and Methods Mice. cell knockout, inos / (Taconic arms), Rag1 /, INγR /, and IL-12p4 / mice (The Jackson Laboratory) were maintained and/or
Supporting Information lpek et al. 1.173/pnas.1121217 SI Materials and Methods Mice. cell knockout, inos / (Taconic arms), Rag1 /, INγR /, and IL-12p4 / mice (The Jackson Laboratory) were maintained and/or
TCR, MHC and coreceptors
 Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
General Overview of Immunology. Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center
 General Overview of Immunology Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center Objectives Describe differences between innate and adaptive immune responses
General Overview of Immunology Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center Objectives Describe differences between innate and adaptive immune responses
Increased IL-12 induced STAT-4 signaling in CD8 T cells. from aged mice
 Increased IL-2 induced STAT-4 signaling in CD8 T cells from aged mice Erin Rottinghaus * Abstract: Aging is associated with poor immune function leading to increased susceptibility to infectious diseases
Increased IL-2 induced STAT-4 signaling in CD8 T cells from aged mice Erin Rottinghaus * Abstract: Aging is associated with poor immune function leading to increased susceptibility to infectious diseases
MagniSort Mouse CD4 T cell Enrichment Kit Catalog Number: RUO: For Research Use Only. Not for use in diagnostic procedures.
 Page 1 of 2 MagniSort Mouse CD4 T cell Enrichment Kit RUO: For Research Use Only. Not for use in diagnostic procedures. Mouse splenocytes were unsorted (left) or sorted with the MagniSort Mouse CD4 T cell
Page 1 of 2 MagniSort Mouse CD4 T cell Enrichment Kit RUO: For Research Use Only. Not for use in diagnostic procedures. Mouse splenocytes were unsorted (left) or sorted with the MagniSort Mouse CD4 T cell
COMPONENT NAME COMPONENT # QUANTITY STORAGE SHELF LIFE FORMAT. Store at 2-8 C. Do not freeze. Store at 2-8 C. Do not freeze.
 This document is available at www.stemcell.com/pis Catalog #18765 EasySep Mouse CD4+CD62L+ T Cell Isolation Kit For processing 1x 10^9 cells Description Isolate highly purified naïve CD4+ T cells (CD4+CD62L+)
This document is available at www.stemcell.com/pis Catalog #18765 EasySep Mouse CD4+CD62L+ T Cell Isolation Kit For processing 1x 10^9 cells Description Isolate highly purified naïve CD4+ T cells (CD4+CD62L+)
IOM Immunization Safety Review 11/12/2001. Immunological Competition and the Infant Immune Response to Vaccines
 IOM Immunization Safety Review 11/12/2001 Immunological Competition and the Infant Immune Response to Vaccines Richard Insel University of Rochester Goals Neonatal and Infant Immune System Broad Effects
IOM Immunization Safety Review 11/12/2001 Immunological Competition and the Infant Immune Response to Vaccines Richard Insel University of Rochester Goals Neonatal and Infant Immune System Broad Effects
Principles of Adaptive Immunity
 Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
T Cell Effector Mechanisms I: B cell Help & DTH
 T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
Nishino, Tomoya; Fukushima, Chizu; Asthma and Immunology, 113, 2, (201
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Clearance of Aspergillus fumigatus inflammation Fukahori, Susumu; Matsuse, Hiroto; Nishino, Tomoya; Fukushima, Chizu; Annals of Allergy, Asthma
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Clearance of Aspergillus fumigatus inflammation Fukahori, Susumu; Matsuse, Hiroto; Nishino, Tomoya; Fukushima, Chizu; Annals of Allergy, Asthma
In vitro human regulatory T cell expansion
 - 1 - Human CD4 + CD25 + regulatory T cell isolation, Workflow in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation of T
- 1 - Human CD4 + CD25 + regulatory T cell isolation, Workflow in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation of T
Prepared by Cyrus H. Nozad, MD, University of Tennessee and John Seyerle, MD, Ohio State University
 Allergy and Immunology Review Corner: Chapter 21 of Middleton s Allergy Principles and Practice, Seventh Edition, edited by N. Franklin Adkinson, et al. Chapter 21: Antigen-Presenting Dendritic Cells (Pages
Allergy and Immunology Review Corner: Chapter 21 of Middleton s Allergy Principles and Practice, Seventh Edition, edited by N. Franklin Adkinson, et al. Chapter 21: Antigen-Presenting Dendritic Cells (Pages
Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained
 1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained jejunum sections ( 200 magnification;
1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained jejunum sections ( 200 magnification;
The Immune System. These are classified as the Innate and Adaptive Immune Responses. Innate Immunity
 The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
Adaptive immune responses: T cell-mediated immunity
 MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
In vitro human regulatory T cell suppression assay
 Human CD4 + CD25 + regulatory T cell isolation, in vitro suppression assay and analysis In vitro human regulatory T cell suppression assay Introduction Regulatory T (Treg) cells are a subpopulation of
Human CD4 + CD25 + regulatory T cell isolation, in vitro suppression assay and analysis In vitro human regulatory T cell suppression assay Introduction Regulatory T (Treg) cells are a subpopulation of
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA
 AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
In vitro human regulatory T cell expansion
 - 1 - Human CD4 + CD25 + CD127 dim/- regulatory T cell Workflow isolation, in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation
- 1 - Human CD4 + CD25 + CD127 dim/- regulatory T cell Workflow isolation, in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation
Mon, Wed, Fri 11:00 AM-12:00 PM. Owen, Judy, Jenni Punt, and Sharon Stranford Kuby-Immunology, 7th. Edition. W.H. Freeman and Co., New York.
 Course Title: Course Number: Immunology Biol-341/541 Semester: Fall 2013 Location: HS 268 Time: Instructor: 8:00-9:30 AM Tue/Thur Dr. Colleen M. McDermott Office: Nursing Ed 101 (424-1217) E-mail*: mcdermot@uwosh.edu
Course Title: Course Number: Immunology Biol-341/541 Semester: Fall 2013 Location: HS 268 Time: Instructor: 8:00-9:30 AM Tue/Thur Dr. Colleen M. McDermott Office: Nursing Ed 101 (424-1217) E-mail*: mcdermot@uwosh.edu
Innate immunity (rapid response) Dendritic cell. Macrophage. Natural killer cell. Complement protein. Neutrophil
 1 The immune system The immune response The immune system comprises two arms functioning cooperatively to provide a comprehensive protective response: the innate and the adaptive immune system. The innate
1 The immune system The immune response The immune system comprises two arms functioning cooperatively to provide a comprehensive protective response: the innate and the adaptive immune system. The innate
