OPINION. Endocrine Journal 2015, 62 (8),
|
|
|
- Gerard Thomas
- 6 years ago
- Views:
Transcription
1 Endocrine Journal 2015, 62 (8), OPINION Pathogenesis and diagnostic criteria for rickets and osteomalacia Proposal by an expert panel supported by Ministry of Health, Labour and Welfare, Japan, The Japanese Society for Bone and Mineral Research and The Japan Endocrine Society Seiji Fukumoto 1), Keiichi Ozono 2), Toshimi Michigami 3), Masanori Minagawa 4), Ryo Okazaki 5), Toshitsugu Sugimoto 6), Yasuhiro Takeuchi 7) and Toshio Matsumoto 1) 1) Fujii Memorial Institute of Medical Sciences, Tokushima University, Tokushima , Japan 2) Department of Pediatrics, Osaka University Graduate School of Medicine, Suita , Japan 3) Department of Bone and Mineral Research, Research Institute, Osaka Medical Center for Maternal and Child Health, Izumi , Japan 4) Department of Endocrinology, Chiba Children s Hospital, Chiba , Japan 5) Third Department of Medicine, Teikyo University Chiba Medical Center, Ichihara , Japan 6) Internal Medicine 1, Shimane University Faculty of Medicine, Izumo , Japan 7) Division of Endocrinology, Toranomon Hospital Endocrine Center, Tokyo , Japan Abstract. Rickets and osteomalacia are diseases characterized by impaired mineralization of bone matrix. Recent investigations revealed that the causes for rickets and osteomalacia are quite variable. While these diseases can severely impair the quality of life of the affected patients, rickets and osteomalacia can be completely cured or at least respond to treatment when properly diagnosed and treated according to the specific causes. On the other hand, there are no standard criteria to diagnose rickets or osteomalacia nationally and internationally. Therefore, we summarize the definition and pathogenesis of rickets and osteomalacia, and propose the diagnostic criteria and a flowchart for the differential diagnosis of various causes for these diseases. We hope that these criteria and flowchart are clinically useful for the proper diagnosis and management of patients with these diseases. Key words: Vitamin D, Hypophosphatemia, Hyopcalcemia, FGF23 RICKETS and osteomalacia are diseases characterized by impaired mineralization of bone matrix [1, 2]. While rickets and osteomalacia are caused by the same etiologies, rickets develops before the closure of the growth plates. These diseases have been classified as metabolic bone diseases and endocrinologists have not considered these as endocrine diseases. Historically, nutritional vitamin D deficient rickets and osteomalacia were clinically very important [3]. Studies about this vitamin D deficient diseases led to the identification of 25-hydroxyvitain D [25(OH)D] and 1,25-dihydroxyvitamin D [1,25(OH) 2 D]. Since then, many causes of rickets and osteomalacia have been identified. Especially, Submitted May 19, 2015; Accepted Jun. 9, 2015 as EJ Released online in J-STAGE as advance publication Jul. 4, 2015 Correspondence to: Seiji Fukumoto, Fujii Memorial Institute of Medical Sciences, Tokushima University, Kuramoto-cho, Tokushima , Japan. fukumoto-tky@umin.ac.jp The Japan Endocrine Society recent studies established that fibroblast growth factor 23 (FGF23) is a phosphotropic hormone produced by bone and excessive actions of FGF23 cause several kinds of hypophosphatemic rickets and osteomalacia [4]. These results indicate that at least some kinds of hypophosphatemic rickets and osteomalacia are now considered to be endocrine diseases. Furthermore, it has been proposed that FGF23 measurement is useful for the differential diagnosis of hypophosphatemic diseases [5]. Therefore, it may be possible to newly classify causes of rickets and osteomalacia based on the pathophysiology utilizing these new findings. There are no standard criteria to diagnose rickets or osteomalacia nationally and internationally. Since rickets and osteomalacia are not common lifestyle diseases, it may be difficult for general health professionals to properly diagnose and manage patients with these diseases. As impaired mineralization results in
2 666 Fukumoto et al. is usually caused by impaired intestinal phosphate absorption and/or renal phosphate wasting. Phosphate is abundant in food and phosphate deficiency does not occur in healthy subjects taking usual food. Phosphate deficiency may be observed in some patients suffering from malnutrition, malabsorption syndrome and so on. 1,25(OH) 2 D enhances intestinal phosphate and calcium absorption, and impaired actions of vitamin D metabolites can result in hypophosphatemia and/ or hypocalcemia. Drugs such as diphenylhydantoin and rifampicin may cause impaired actions of vitamin D metabolites by altering vitamin D metabolism. Vitamin D-dependent rickets type 1 is caused by mutations in CYP27B1 encoding 25(OH)D-1α-hydroxylase [6]. This enzyme converts 25(OH)D into 1,25(OH) 2 D. Vitamin D receptor (VDR) is mutated in patients with vitamin D-dependent rickets type 2 [7]. In patients with these vitamin D-dependent rickets, both hypophosphatemia and hypocalcemia are observed. Because hypocalcemia causes secondary hyperparathyroidism resulting in reduced renal tubular phosphate reabsorplow bone mineral density measured by dual energy X-ray absorptiometry, osteomalacia must be discriminated from osteoporosis, a much commoner disease. Bone deformities observed in patients with rickets may lead to a wrong diagnosis like skeletal dysplasia. On the other hand, rickets and osteomalacia can severely impair the quality of life of the affected patients without proper diagnosis and management. From these backgrounds, it is clinically important to establish diagnostic criteria for rickets and osteomalacia that can be easily used by health professionals. In this review, we briefly summarize the definition and pathogenesis of rickets and osteomalacia, and propose the diagnostic criteria and investigation methods for the differential diagnosis of various causes for these diseases. Definition and Clinical Presentations Bone is a hard tissue created by deposition of hydroxyapatite crystals [Ca 10 (PO 4 ) 6 (OH) 2 ] on matrix proteins produced by osteoblasts. Because of the impairment of this mineralization of matrix proteins, unmineralized bone matrix (osteoid) increases in rickets and osteomalacia [1, 2]. Of these, rickets develops in children and osteomalacia is a disease in adulthood. Patients with rickets present several symptoms and signs including growth retardation, bone deformities such as genu valgum and varum, spinal curvature, craniotabes, open fontanels, rachitic rosary and joint swelling [1, 2]. Patients with osteomalacia may complain of bone pain and have muscle weakness, pigeon chest, spinal curvature and pseudofractures (Looser s zone) [1, 2]. Pathogenesis and Causes Several drugs such as aluminum and etidronate directly inhibit mineralization of bone matrix proteins. In most other cases with rickets or osteomalacia, chronic hypophosphatemia, hypocalcemia, or both are present (Table 1). Hydroxyapatite crystals are formed in matrix vesicles produced by osteoblasts from calcium ion and phosphate. Hypophosphatemia or hypocalcemia is believed to impair mineralization by decreasing calcium x phosphate product. Serum phosphate level is maintained by intestinal phosphate absorption, renal phosphate handling and phosphate movement between extracellular fluid and bone or intracellular fluid. Of these, chronic hypophosphatemia resulting in rickets and osteomalacia Table 1 Causes of rickets/osteomalacia Hypophosphatemia Impaired actions of vitamin D metabolites Vitamin D deficiency Drugs (Diphenylhydantoin, Rifampicin, etc.) Vitamin D-dependent rickets type 1 1) Vitamin D-dependent rickets type 2 2) Renal tubular dysfunction Hereditary hypophosphatemic rickets with hypercalciuria 3) Fanconi syndrome Dent disease 4) Renal tubular acidosis Drugs (Ifosfamide, Adefovir pivoxil, Valproic acid, etc.) FGF23-related hypophosphatemic rickets/osteomalacia (Table 2) Phosphate depletion Phosphate deficiency Malabsorption Hypocalcemia Some cases of vitamin D deficiency Vitamin D-dependent rickets type 1 1) Vitamin D-dependent rickets type 2 2) Impaired mineralization from other causes Drugs (Aluminum, Etidronate, etc.) 1) Mutations in CYP27B1 gene, autosomal recessive 2) Mutations in VDR gene, autosomal recessive 3) Mutations in SLC34A3 gene, autosomal recessive 4) Mutations in CLCN5 gene, X-linked recessive
3 Diagnosis of rickets and osteomalacia 667 Table 2 FGF23-related hypophosphatemic rickets/osteomalacia X-linked dominant hypophosphatemic rickets/osteomalacia (XLH) Mutations in PHEX gene Autosomal dominant hypophosphatemic rickets/osteomalacia (ADHR) Mutations in FGF23 gene Autosomal recessive hypophosphatemic rickets/osteomalacia 1 (ARHR1) Mutations in DMP1 gene Autosomal recessive hypophosphatemic rickets/osteomalacia 2 (ARHR2) Mutations in ENPP1 gene Hypophosphatemic disease with dental anomalies and ectopic calcification Mutations in FAM20C gene McCune-Albright syndrome/fibrous dysplasia Linear sebaceous nevus syndrome Tumor-induced rickets/osteomalacia Hypophosphatemic rickets/osteomalacia by saccharated ferric oxide or iron polymaltose PHEX, phosphate-regulating gene with homologies to endopeptidases on the X chromosome; DMP1, dentin matrix protein 1; ENPP1, ectonucleotide pyrophosphatase/phosphodiesterase 1; FAM20C, family with sequence similarity 20, member C tion, both impaired intestinal phosphate absorption and increased renal phosphate excretion contribute to the development of hypophosphatemia in these patients. Vitamin D deficiency is diagnosed by low serum 25(OH)D levels. Some patients with vitamin D deficiency also present secondary hyperparathyroidism. Because parathyroid hormone (PTH) stimulates conversion of 25(OH)D into 1,25(OH) 2 D, patients with vitamin D deficiency can present various levels of 1,25(OH) 2 D. Therefore, vitamin D deficiency cannot be diagnosed by 1,25(OH) 2 D levels. Gastrectomy or enterectomy can cause osteomalacia [8]. It is possible that patients with osteomalacia after these surgeries are not properly diagnosed and treated. The causes for osteomalacia in these patients may be multifactorial including vitamin D deficiency and impaired mineral absorption. While liver cirrhosis or chronic liver disease was described as one of causes for osteomalacia, osteoporosis seems to be much commoner than osteomalacia in these patients [9]. There are many causes for renal phosphate wasting. About 80-90% phosphate filtered from glomeruli is absorbed in renal proximal tubules. Type 2a and 2c sodium-phosphate cotransporters mediate physiological phosphate reabsorption in proximal tubules [10]. Renal phosphate wasting can be observed in patients with Fanconi syndrome and some form of renal tubular acidosis. In addition, hereditary hypophosphatemic rickets with hypercalciuria is caused by mutations in SLC34A3 which encodes type 2c sodium-phosphate cotransporter [11, 12]. Dent disease is characterized by low molecular weight proteinuria, hypophosphatemia and nephrolithiasis. This disease is caused by mutations in CLC5 encoding a chloride channel [13]. In addition to these intrinsic renal tubular defect, excessive actions of FGF23 cause hypophosphatemia with enhanced renal phosphate excretion. FGF23 suppresses renal tubular phosphate reabsorption by reducing the expression of type 2a and 2c sodiumphosphate cotransporters [14]. In addition, FGF23 decreases serum 1,25(OH) 2 D level by altering the expression levels of vitamin D-metabolizing enzymes [14]. Therefore, FGF23 reduces serum phosphate by suppressing renal phosphate reabsorption and inhibiting intestinal phosphate absorption through lowering 1,25(OH) 2 D. After the identification of FGF23, it became clear that patients with some kinds of hypophosphatemic rickets/osteomalacia such as X-linked hypophosphatemic rickets (XLH) and tumor-induced osteomalacia (TIO), a rare paraneoplastic syndrome, show high circulatory levels of FGF23 [15, 16]. In contrast, FGF23 levels in patients suffering from other causes for rickets/osteomalacia including vitamin D deficiency were rather low [5]. Together with the biological activities of FGF23 as mentioned above, these results indicated that FGF23 is the humoral factor that causes hypophosphatemia in patients with several diseases including XLH and TIO. Since then, other hypophosphatemic diseases have also been shown to be associated with high FGF23 levels [17] (Table 2). It is believed that FGF23 production in bone is enhanced in most patients with these FGF23-related hypophosphatemic diseases except for TIO. However, the precise mechanisms of overproduction of FGF23 and the actions of gene products responsible for genetic FGF23-related hypophosphatemic diseases are largely unknown. Diagnostic Criteria (Table 3) Because the clinical presentations of rickets and osteomalacia are quite different, it is not practical to prepare one kind of diagnostic criteria for both of these diseases. Therefore, we propose the following diagnostic criteria (Table 3). Rickets is basically diagnosed by the presence of rachitic changes of bones such as cupping and fraying of metaphysis, and widening of epiphyseal plate observed by X-ray. In addition, high
4 668 Fukumoto et al. alkaline phosphatase is characteristic for diseases with impaired mineralization. We believe that these two laboratory findings are essential to make a diagnosis of rickets or suspect the presence of this disease. In addition, patients with rickets usually show hypophosphatemia or hypocalcemia, and some clinical signs. However, it is possible that patients show no clinical signs especially when the diagnosis of rickets is established in the early phase of the disease. This can happen in family members of affected patients with rickets from genetic causes. Therefore, we propose that patients with all these four findings (a to d in Table 3A) are regarded to have definite rickets, and subjects who lack either hypophosphatemia or hypocalcemia, or clinical signs (c or d) as possible rickets. In contrast to rickets, there is no single laboratory test which strongly suggests the presence of osteomalacia. However, patients with osteomalacia usually show either hypophosphatemia or hypocalcemia. High alkaline phosphatase is also seen in patients with osteomalacia. While almost all alkaline phosphatase activity in blood derives from bone in children, there is significant contribution from liver and other organs in adults. We believe that either hypophosphatemia or hypocalcemia, and high bone alkaline phosphatase are essential to make a diagnosis of osteomalacia or suspect this disease. In addition, patients with osteomalacia may show some clinical symptoms, low bone mineral density (BMD), multiple uptakes by bone scintigraphy or Looser s zone. However, patients may not show these findings when osteomalacia is suspected early in the course of the disease as in the case of rickets. Therefore, we propose that patients with all these five findings (a to e in Table 3B) are regarded to have definite osteomalacia, and subjects who lack either clinical symptoms, low BMD or abnormal imaging findings (c to e) as possible osteomalacia. Drugs that inhibit mineralization can induce rickets or osteomalacia without changing serum calcium or phosphate levels. In addition, several diseases need to be discriminated form rickets/osteomalacia (Table 4). Diseases shown in Table 4 can mimic some features of rickets or osteomalacia. On the other hand, most of these diseases cannot be diagnosed as rickets or osteomalacia using the diagnostic criteria shown in Table 3. The exceptions are multiple metastases, primary hyperparathyroidism and renal osteodystrophy. Osteoblastic bone metastases can cause either hypocalcemia or hypophosphatemia, high bone alkaline phos- Table 3 Diagnostic criteria for rickets and osteomalacia A. Rickets a) Rachitic changes in X-ray (Cupping and fraying of metaphysis, widening of epiphyseal plate) b) High alkaline phosphatase c) Hypophosphatemia or hypocalcemia 1) d) Clinical signs Bone deformities such as genu varum and valgum, abnormal spinal curvature, craniotabes, open fontanels, rachitic rosary, joint swelling Definite rickets Patients who have a) to d) Possible rickets Patients who show a), b) and one of c) or d) B. Osteomalacia a) Hypophosphatemia or hyocalcemia 1) b) High bone alkaline phosphatase c) Clinical symptoms Muscle weakness or bone pain d) Low BMD Less than 80% of YAM e) Abnormal imaging findings Multiple uptakes by bone scintigraphy or Looser s zone by X-ray Definite osteomalacia Patients who have a) to e) Possible osteomalacia Patients who show a), b) and two of c) to e) 1) Does not apply to patients with inhibitors of mineralization Table 4 Diseases that need to be discriminated form rickets/ osteomalacia Low BMD Osteoporosis, Renal osteodystrophy, Primary hyperparathyroidism Bone deformity Skeletal dysplasia Bone pain Polymyalgia rheumatica, Ankylosing spondylitis Muscle weakness Neuromuscular diseases Multiple uptakes by bone scintigraphy Multiple metastases Rachitic change Hypophosphatasia High bone alkaline phosphatase Primary hyperparathyroidism, Renal osteodystrophy, Multiple metastases phatase, bone pain and multiple uptakes by bone scintigraphy. This possibility need to be considered before finalizing the diagnosis of osteomalacia. Patients with primary hyperparathyroidism may also show hypophosphatemia, high bone alkaline phosphatase, bone pain, low BMD and multiple uptakes by bone scintigraphy. However, hypercalcemia which is rare in
5 Diagnosis of rickets and osteomalacia 669 patients with osteomalacia is usually present in patients with primary hyperparathyroidism. Patients with renal osteodystrophy may show hypocalcemia, high bone alkaline phosphatase, bone pain, low BMD and multiple uptakes by bone scintigraphy. On the other hand, hyperphosphatemia rather than hypophosphatemia is usually observed in patients with renal osteodystrophy. Hypophosphatasia is caused by mutations in TNALP which encodes tissue-nonspecific alkaline phosphatase [18]. This disease is also characterized by impaired mineralization because alkaline phosphatase converts pyrophosphate with potent inhibitory effects on mineralization into phosphate. In this sense, hypophosphatasia can be regarded as one cause for rickets. However, patients with hypophosphatasia show low alkaline phosphatase levels in contrast to those with rickets from other causes. Therefore, hypophosphatasia was treated as a disease that should be discriminated from rickets rather than a cause for rickets to avoid confusion in this proposal. Differential Diagnosis of Causes for Rickets/Osteomalacia (Table 5, Fig. 1) After establishing the diagnosis of rickets or osteomalacia, it is necessary to find the exact cause for these diseases. Table 5 summarizes typical biochemical changes observed in patients with various causes for rickets and osteomalacia. Vitamin D deficiency is defined by low 25(OH)D levels as mentioned before. Therefore, patients with low 25(OH)D levels are theoretically considered to have vitamin D deficient rickets or osteomalacia. However, vitamin D deficiency or insufficiency is quite common even in general population [19] and it is possible that low 25(OH)D levels can be observed in patients with other causes for rickets or osteomalacia. Actually, investigation of 25(OH)D levels in patients with vitamin D deficient rickets and XLH indicated that there was overlap of serum 25(OH)D levels in these patients. In contrast, FGF23 completely discriminated patients with vitamin D deficient rickets and XLH [20]. From these results, we propose a flowchart for differentiating various causes for rickets and osteomalacia (Fig. 1). In patients with hypophosphatemic rickets/osteomalacia, high FGF23 levels indicate FGF23-related hypophosphatemic diseases (Table 2). Vitamin D deficient rickets/osteomalacia is diagnosed after ruling out FGF23-related hypophosphatemic diseases, phosphate depletion and other causes of renal tubular phosphate wasting. Vitamin D-dependent rickets 1 and 2 can be differentiated by 1,25(OH) 2 D levels. HHRH is also characterized by high 1,25(OH) 2 D levels. In normophosphatemic patients, drugs that inhibit mineralization and vitamin D deficiency should be considered. It should be also noted that patients with vitamin D deficiency may not show frank hypophosphatemia or hypocalcemia. It is possible that serum phosphate and calcium remain in the low normal range in these patients. Discussion Rickets and osteomalacia are not common diseases. However, quality of life of the affected patients can be severely compromised. For example, some untreated patients with TIO can become completely bedridden because of severe muscle weakness and bone pain. Short stature and bone deformities are big problems for patients with rickets. However, patients with rickets or osteomalacia can be completely cured or at least Table 5 Typical biochemical findings in patient with various causes of rickets/osteomalacia Serum Ca Serum Pi TmP/ GFR BAP 1,25(OH) 2 D 25(OH)D FGF23 FGF23-related hypophosphatemic disease Phosphate depletion Fanconi syndrome Vitamin D-dependent rickets type 1 Vitamin D-dependent rickets type 2 HHRH Vitamin D deficiency Drugs that inhibit mineralization : Specific laboratory tests for each category. Pi, phosphate; TmP/GFR, tubular maximum transport of phosphate per glomerular filtration rate; BAP, bone alkaline phosphatase; 1,25(OH) 2 D, 1,25-dihydroxyvitamin D; 25(OH)D, 25-hydroxyvitamin D; HHRH, hereditary hypophosphatemic rickets with hypercalciuria
6 670 Fukumoto et al. Fig. 1 A flowchart for the differential diagnosis of causes for rickets/osteomalacia The causes for rickets and osteomalacia can be identified by several clinical findings and laboratory tests. respond to treatment when properly diagnosed and treated according to the specific causes. Therefore, we here listed causes for rickets and osteomalacia, and proposed the diagnostic criteria and a flowchart for the differential diagnosis of various causes for these diseases. There are several limitations in the proposed diagnostic criteria. These criteria are not created by retrospective review of clinical presentations of a large number of patients, but proposed by several researchers and clinicians based on their experiences. Therefore, the validity of these criteria and the flowchart needs to be examined in the future studies. However, without any diagnostic criteria, it would be difficult for general medical professionals to correctly diagnose not-so-common illnesses. We hope that this proposal will become a momentum for propagation of proper knowledge about rickets and osteomalacia, and for accumulation of more clinical data for future revision of the criteria. In addition, there was a discussion about hypophosphatasia among us. This disease can be considered to be one cause of rickets. However, if hypophosphatasia is included in the causes for rickets, high alkaline phosphatase cannot be used as one of criteria for the diagnosis of rickets, and the flowchart for the differential diagnosis of various causes needs to be more complex. Because hypophosphatasia is rarer than other causes for rickets such as vitamin D deficiency and XLH, and the easily usable diagnostic criteria for rickets and osteomalacia were planned, hypophosphatasia was not included as a cause for rickets in this proposal. Finally, measurements of FGF23 and 25(OH)D are not covered by medical insurance in Japan now and are not routine laboratory tests. In contrast, these measurements are available in several commercial and research laboratories. We hope that this proposal will contribute to some extent to the future coverage of these measurements by medical insurance in Japan. In summary, we have created a diagnostic criteria and a flowchart for the differential diagnosis of various causes for rickets/osteomalacia. We hope that these criteria and flowchart are clinically useful for the proper diagnosis and management of patients with these diseases. Acknowledgements This study was supported in part by a grant from Ministry of Health, Labour and Welfare of Japan. Disclosure The authors declare no conflicts of interest.
7 Diagnosis of rickets and osteomalacia 671 References 1. Reginato AJ, Coquia JA (2003) Musculoskeletal manifestations of osteomalacia and rickets. Best Pract Res Clin Rheumatol 17: Whyte MP, Thakker RV (2009) Rickets and osteomalacia. Medicine 37: Prentice A (2013) Nutritional rickets around the world. J Steroid Biochem Mol Biol 136: Fukumoto S, Martin TJ (2009) Bone as an endocrine organ. Trends Endocrinol Metab 20: Endo I, Fukumoto S, Ozono K, Namba N, Tanaka H, et al. (2008) Clinical usefulness of measurement of fibroblast growth factor 23 (FGF23) in hypophosphatemic patients: proposal of diagnostic criteria using FGF23 measurement. Bone 42: Kitanaka S, Takeyama K, Murayama A, Sato T, Okumura K, et al. (1998) Inactivating mutations in the 25-hydroxyvitamin D3 1alpha-hydroxylase gene in patients with pseudovitamin D-deficiency rickets. N Engl J Med 338: Hughes MR, Malloy PJ, Kieback DG, Kesterson RA, Pike JW, et al. (1988) Point mutations in the human vitamin D receptor gene associated with hypocalcemic rickets. Science 242: Tovey FI, Hall ML, Ell PJ, Hobsley M (1992) A review of postgastrectomy bone disease. J Gastroenterol Hepatol 7: Collier J (2007) Bone disorders in chronic liver disease. Hepatology 46: Blaine J, Chonchol M, Levi M (2015) Renal control of calcium, phosphate, and magnesium homeostasis. Clin J Am Soc Nephrol 10: Bergwitz C, Roslin NM, Tieder M, Loredo-Osti JC, Bastepe M, et al. (2006) SLC34A3 mutations in patients with hereditary hypophosphatemic rickets with hypercalciuria predict a key role for the sodium-phosphate cotransporter NaPi-IIc in maintaining phosphate homeostasis. Am J Hum Genet 78: Lorenz-Depiereux B, Benet-Pages A, Eckstein G, Tenenbaum-Rakover Y, Wagenstaller J, et al. (2006) Hereditary hypophosphatemic rickets with hypercalciuria is caused by mutations in the sodium-phosphate cotransporter gene SLC34A3. Am J Hum Genet 78: Lloyd SE, Pearce SH, Fisher SE, Steinmeyer K, Schwappach B, et al. (1996) A common molecular basis for three inherited kidney stone diseases. Nature 379: Shimada T, Hasegawa H, Yamazaki Y, Muto T, Hino R, et al. (2004) FGF-23 is a potent regulator of vitamin D metabolism and phosphate homeostasis. J Bone Miner Res 19: Jonsson KB, Zahradnik R, Larsson T, White KE, Sugimoto T, et al. (2003) Fibroblast growth factor 23 in oncogenic osteomalacia and X-linked hypophosphatemia. N Engl J Med 348: Yamazaki Y, Okazaki R, Shibata M, Hasegawa Y, Satoh K, et al. (2002) Increased circulatory level of biologically active full-length FGF-23 in patients with hypophosphatemic rickets/osteomalacia. J Clin Endocrinol Metab 87: Fukumoto S (2014) Anti-fibroblast growth factor 23 antibody therapy. Curr Opin Nephrol Hypertens 23: Weiss MJ, Cole DE, Ray K, Whyte MP, Lafferty MA, et al. (1988) A missense mutation in the human liver/ bone/kidney alkaline phosphatase gene causing a lethal form of hypophosphatasia. Proc Natl Acad Sci U S A 85: Bendik I, Friedel A, Roos FF, Weber P, Eggersdorfer M (2014) Vitamin D: a critical and essential micronutrient for human health. Front Physiol 5: Kubota T, Kitaoka T, Miura K, Fujiwara M, Ohata Y, et al. (2014) Serum fibroblast growth factor 23 is a useful marker to distinguish vitamin D-deficient rickets from hypophosphatemic rickets. Horm Res Paediatr 81:
Sachin Soni DNB Pediatrics
 Sachin Soni DNB Pediatrics Vitamin D physiology Introduction Etiology Clinical feature Radiology Diagnosis Lab Treatment Source: -Fish, liver and oil, - Human milk (30-40 IU/L) - Exposure to sun light
Sachin Soni DNB Pediatrics Vitamin D physiology Introduction Etiology Clinical feature Radiology Diagnosis Lab Treatment Source: -Fish, liver and oil, - Human milk (30-40 IU/L) - Exposure to sun light
Hypophosphatemic rickets: new treatments
 Hypophosphatemic rickets: new treatments Gema Ariceta Pediatric Nephrology, University Hospital Vall d Hebron, Barcelona 1 11.06.18 Tubulopathies Disclosures Lectures and educational activities sponsored
Hypophosphatemic rickets: new treatments Gema Ariceta Pediatric Nephrology, University Hospital Vall d Hebron, Barcelona 1 11.06.18 Tubulopathies Disclosures Lectures and educational activities sponsored
DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS
 DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS XLH IS CHARACTERIZED BY CHRONIC HYPOPHOSPHATEMIA XLH is a hereditary, progressive, lifelong disorder. In children and adults,
DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS XLH IS CHARACTERIZED BY CHRONIC HYPOPHOSPHATEMIA XLH is a hereditary, progressive, lifelong disorder. In children and adults,
Review Article Fibroblast Growth Factor 23 (FGF23) and Disorders of Phosphate Metabolism
 Hindawi Publishing Corporation International Journal of Pediatric Endocrinology Volume 2009, Article ID 496514, 6 pages doi:10.1155/2009/496514 Review Article Fibroblast Growth Factor 23 (FGF23) and Disorders
Hindawi Publishing Corporation International Journal of Pediatric Endocrinology Volume 2009, Article ID 496514, 6 pages doi:10.1155/2009/496514 Review Article Fibroblast Growth Factor 23 (FGF23) and Disorders
University of Zurich. What goes in must come out - the small intestine modulates renal phosphate excretion. Zurich Open Repository and Archive
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2007 What goes in must come out - the small intestine modulates renal phosphate
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2007 What goes in must come out - the small intestine modulates renal phosphate
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
OPINION. Definition and Significance
 2017, 64 (1), 1-10 OPINION Advance Publication doi: 10.1507/endocrj.EJ16-0548 Assessment criteria for vitamin D deficiency/insufficiency in Japan proposal by an expert panel supported by Research Program
2017, 64 (1), 1-10 OPINION Advance Publication doi: 10.1507/endocrj.EJ16-0548 Assessment criteria for vitamin D deficiency/insufficiency in Japan proposal by an expert panel supported by Research Program
Case Report ANovelPHEX Mutation in Japanese Patients with X-Linked Hypophosphatemic Rickets
 Case Reports in Genetics Volume 2015, Article ID 301264, 5 pages http://dx.doi.org/10.1155/2015/301264 Case Report ANovelPHEX Mutation in Japanese Patients with X-Linked Hypophosphatemic Rickets Tetsuya
Case Reports in Genetics Volume 2015, Article ID 301264, 5 pages http://dx.doi.org/10.1155/2015/301264 Case Report ANovelPHEX Mutation in Japanese Patients with X-Linked Hypophosphatemic Rickets Tetsuya
Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes.
 Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B.
 Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B. Increased concentration of proteins in foods C. Decreasing
Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B. Increased concentration of proteins in foods C. Decreasing
Approach to a child presenting with rickets
 Current Practice Approach to a child presenting with rickets Navoda Atapattu 1 Sri Lanka Journal of Child Health, 2013; 42(1): 40-44 (Key words: Rickets; vitamin D; children) Introduction Rickets is a
Current Practice Approach to a child presenting with rickets Navoda Atapattu 1 Sri Lanka Journal of Child Health, 2013; 42(1): 40-44 (Key words: Rickets; vitamin D; children) Introduction Rickets is a
X-linked hypophosphatemic rickets across the lifespan
 X-linked hypophosphatemic rickets across the lifespan AACE Midwest Regional Meeting Erik A. Imel, M.D. Associate Professor of Medicine and Pediatrics Indiana Center for Musculoskeletal Health July 28,
X-linked hypophosphatemic rickets across the lifespan AACE Midwest Regional Meeting Erik A. Imel, M.D. Associate Professor of Medicine and Pediatrics Indiana Center for Musculoskeletal Health July 28,
Emerging Concepts in Pediatric Bone Disease
 Volume 10 Supplement 2, June 2013 Emerging Concepts in Pediatric Bone Disease Guest Editor: Francis H. Glorieux, MD, OC, PhD Y.S. Medical Media Ltd. 3 Forword Francis H. Glorieux...346 Nutritional Rickets:
Volume 10 Supplement 2, June 2013 Emerging Concepts in Pediatric Bone Disease Guest Editor: Francis H. Glorieux, MD, OC, PhD Y.S. Medical Media Ltd. 3 Forword Francis H. Glorieux...346 Nutritional Rickets:
Hypophosphatasia. Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX
 Hypophosphatasia Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX Hypophosphatasia Case Teeth 57 y/o male with a hyperlipidemia and hypogonadism. Noted to have an alkaline phosphatase of
Hypophosphatasia Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX Hypophosphatasia Case Teeth 57 y/o male with a hyperlipidemia and hypogonadism. Noted to have an alkaline phosphatase of
FGF-23 Is a Potent Regulator of Vitamin D Metabolism and Phosphate Homeostasis
 JOURNAL OF BONE AND MINERAL RESEARCH Volume 19, Number 3, 2004 Published online on December 29, 2003; doi: 10.1359/JBMR.0301264 2004 American Society for Bone and Mineral Research FGF-23 Is a Potent Regulator
JOURNAL OF BONE AND MINERAL RESEARCH Volume 19, Number 3, 2004 Published online on December 29, 2003; doi: 10.1359/JBMR.0301264 2004 American Society for Bone and Mineral Research FGF-23 Is a Potent Regulator
Case 4 Generalised bone pain
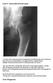 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Renal Tubular Acidosis
 1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
X-linked hypophosphatemic rickets across the lifespan
 X-linked hypophosphatemic rickets across the lifespan AACE Midwest Regional Meeting Erik A. Imel, M.D. Associate Professor of Medicine and Pediatrics Indiana Center for Musculoskeletal Health July 28,
X-linked hypophosphatemic rickets across the lifespan AACE Midwest Regional Meeting Erik A. Imel, M.D. Associate Professor of Medicine and Pediatrics Indiana Center for Musculoskeletal Health July 28,
A case of hereditary hypophosphataemic rickets with hypercalciuria (HHRH)
 Case Reports A case of hereditary hypophosphataemic rickets with hypercalciuria (HHRH) M N Lucas 1, Savithri Dias 2 Sri Lanka Journal of Child Health, 2006; 35:141-3 (Key words: hereditary hypophosphataemic
Case Reports A case of hereditary hypophosphataemic rickets with hypercalciuria (HHRH) M N Lucas 1, Savithri Dias 2 Sri Lanka Journal of Child Health, 2006; 35:141-3 (Key words: hereditary hypophosphataemic
Thomas Carpenter Yale University School of Medicine New Haven, Connecticut, USA
 A Randomized, Open-label Phase 2 Study of, a Fully Human Anti-FGF23 Monoclonal Antibody, in 52 Children with X-linked Hypophosphatemia (XLH): 40-Week Results Thomas Carpenter Yale University School of
A Randomized, Open-label Phase 2 Study of, a Fully Human Anti-FGF23 Monoclonal Antibody, in 52 Children with X-linked Hypophosphatemia (XLH): 40-Week Results Thomas Carpenter Yale University School of
Magnesium Homeostasis
 ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
Fibroblast Growth Factor-23 (FGF23) in Patients with Transient Hypoparathyroidism: Its Important Role in Serum Phosphate Regulation
 Endocrine Journal 2007, 54 (3), 465 470 Fibroblast Growth Factor-23 (FGF23) in Patients with Transient Hypoparathyroidism: Its Important Role in Serum Phosphate Regulation HIROYUKI YAMASHITA, YUJI YAMAZAKI*,
Endocrine Journal 2007, 54 (3), 465 470 Fibroblast Growth Factor-23 (FGF23) in Patients with Transient Hypoparathyroidism: Its Important Role in Serum Phosphate Regulation HIROYUKI YAMASHITA, YUJI YAMAZAKI*,
The hart and bone in concert
 The hart and bone in concert Piotr Rozentryt III Department of Cardiology, Silesian Centre for Heart Disease, Silesian Medical University, Zabrze, Poland Disclosure Research grant, speaker`s fee, travel
The hart and bone in concert Piotr Rozentryt III Department of Cardiology, Silesian Centre for Heart Disease, Silesian Medical University, Zabrze, Poland Disclosure Research grant, speaker`s fee, travel
Factors Affecting Calcium Metabolism in Disorders of the Kidney*
 ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 11, No. 4 Copyright 1981, Institute for Clinical Science, Inc. Factors Affecting Calcium Metabolism in Disorders of the Kidney* MURRAY J. FAVUS, M.D. Departm
ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 11, No. 4 Copyright 1981, Institute for Clinical Science, Inc. Factors Affecting Calcium Metabolism in Disorders of the Kidney* MURRAY J. FAVUS, M.D. Departm
STRENSIQ (asfotase alfa)
 STRENSIQ (asfotase alfa) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
STRENSIQ (asfotase alfa) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
Hypophosphatemia An Evidence-based Problem-Solving Approach to Clinical Cases
 Kidney Diseases Hypophosphatemia An Evidence-based Problem-Solving Approach to Clinical Cases Section of Pediatric Nephrology, Rush University Medical Center, Chicago, Illinois, USA Keywords. hypophosphatemia,
Kidney Diseases Hypophosphatemia An Evidence-based Problem-Solving Approach to Clinical Cases Section of Pediatric Nephrology, Rush University Medical Center, Chicago, Illinois, USA Keywords. hypophosphatemia,
Hereditary hypophosphataemic rickets: experience from a paediatric nephrology unit
 ORIGINAL ARTICLE Advance Access publication 22 November 2012 Hereditary hypophosphataemic rickets: experience from a paediatric nephrology unit Joana S. Caetano, Carolina Cordinhã, Clara Gomes, António
ORIGINAL ARTICLE Advance Access publication 22 November 2012 Hereditary hypophosphataemic rickets: experience from a paediatric nephrology unit Joana S. Caetano, Carolina Cordinhã, Clara Gomes, António
Agents that Affect Bone & Mineral Homeostasis
 Agents that Affect Bone & Mineral Homeostasis 1 Agents that Affect Bone & Mineral Homeostasis Calcium and phosphate are the major mineral constituents of bone. They are also two of the most important minerals
Agents that Affect Bone & Mineral Homeostasis 1 Agents that Affect Bone & Mineral Homeostasis Calcium and phosphate are the major mineral constituents of bone. They are also two of the most important minerals
Fibroblast growth factor 23 and bone metabolism in children with chronic kidney disease
 http://www.kidney-international.org & 21 International Society of Nephrology Fibroblast growth factor 23 and bone metabolism in children with chronic kidney disease Michael van Husen 1, Ann-Katrin Fischer
http://www.kidney-international.org & 21 International Society of Nephrology Fibroblast growth factor 23 and bone metabolism in children with chronic kidney disease Michael van Husen 1, Ann-Katrin Fischer
Calcium, phosphate & magnesium regulation
 Calcium, phosphate & magnesium regulation Tim Arnett Department of Cell and Developmental Biology University College London Bone composition Treated with hydrochloric acid to dissolve mineral leaves organic
Calcium, phosphate & magnesium regulation Tim Arnett Department of Cell and Developmental Biology University College London Bone composition Treated with hydrochloric acid to dissolve mineral leaves organic
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Cholecalciferol (D3) - sources Vitamin D. Endogenous - synthesis in the skin
 Department of Pediatrics and Developmental Disorders Medical University of Bialystok Vitamin D metabolism and clinical manifestation of its deficit Pawel Abramowicz M.D., Ph.D. Jerzy Konstantynowicz MD,
Department of Pediatrics and Developmental Disorders Medical University of Bialystok Vitamin D metabolism and clinical manifestation of its deficit Pawel Abramowicz M.D., Ph.D. Jerzy Konstantynowicz MD,
Approach to hypophosphataemia
 Approach to hypophosphataemia A/Prof Roderick Clifton-Bligh Kolling Institute of Medical Research, University of Sydney Department of Endocrinology Royal North Shore Hospital, St Leonards, NSW Royal North
Approach to hypophosphataemia A/Prof Roderick Clifton-Bligh Kolling Institute of Medical Research, University of Sydney Department of Endocrinology Royal North Shore Hospital, St Leonards, NSW Royal North
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Endocrine functions of bone in mineral metabolism regulation
 Amendment history: Corrigendum (February 2009) Endocrine functions of bone in mineral metabolism regulation L. Darryl Quarles J Clin Invest. 2008;118(12):3820-3828. https://doi.org/10.1172/jci36479. Science
Amendment history: Corrigendum (February 2009) Endocrine functions of bone in mineral metabolism regulation L. Darryl Quarles J Clin Invest. 2008;118(12):3820-3828. https://doi.org/10.1172/jci36479. Science
CKD-Mineral Bone Disorder (MBD) Pathogenesis of Metabolic Bone Disease. Grants: NIH, Abbott, Amgen, OPKO, Shire
 Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Failure to thrive (faltering growth) Dr. Khalid
 Failure to thrive (faltering growth) Dr. Khalid FTT (faltering growth) The term 'failure to thrive' is a clinical state of growth failure due to any causes, characterized by any one or more of the following
Failure to thrive (faltering growth) Dr. Khalid FTT (faltering growth) The term 'failure to thrive' is a clinical state of growth failure due to any causes, characterized by any one or more of the following
Pseudohypoparathyroidism Showing Positive Phosphaturic and Negative Cyclic AMP Excretion Response to Parathyroid Hormone
 Pseudohypoparathyroidism Showing Positive Phosphaturic and Negative Cyclic AMP Excretion Response to Parathyroid Hormone KIICHIRO HIGASHI, KENICHI HONDA*, MITSUO MORITA*, TERUHISA UMEDA*, TATSUYA SHIMADA,
Pseudohypoparathyroidism Showing Positive Phosphaturic and Negative Cyclic AMP Excretion Response to Parathyroid Hormone KIICHIRO HIGASHI, KENICHI HONDA*, MITSUO MORITA*, TERUHISA UMEDA*, TATSUYA SHIMADA,
Inherited Calcium and Magnesium Disorders
 Inherited Calcium and Magnesium Disorders Martin Konrad University Children s Hospital Münster, Germany IPNA / ESPN Master Class, Leuven, Sep 2nd 2015 Outline Hypercalcemia Hypomagnesemia Outline Hypercalcemia
Inherited Calcium and Magnesium Disorders Martin Konrad University Children s Hospital Münster, Germany IPNA / ESPN Master Class, Leuven, Sep 2nd 2015 Outline Hypercalcemia Hypomagnesemia Outline Hypercalcemia
chapter 1 & 2009 KDIGO
 http://www.kidney-international.org chapter 1 & 2009 DIGO Chapter 1: Introduction and definition of CD MBD and the development of the guideline statements idney International (2009) 76 (Suppl 113), S3
http://www.kidney-international.org chapter 1 & 2009 DIGO Chapter 1: Introduction and definition of CD MBD and the development of the guideline statements idney International (2009) 76 (Suppl 113), S3
بسم هللا الرحمن الرحيم. Rickets
 بسم هللا الرحمن الرحيم Rickets 1 Rickets IS defined as failure of mineralization of growing bone or osteoid tissue due to vitamin D deficiency. Vitamin D appear as rickets in children and as oteomalacia
بسم هللا الرحمن الرحيم Rickets 1 Rickets IS defined as failure of mineralization of growing bone or osteoid tissue due to vitamin D deficiency. Vitamin D appear as rickets in children and as oteomalacia
Index. B BMC. See Bone mineral content BMD. See Bone mineral density Bone anabolic impact, Bone mass acquisition
 A Acid base balance dietary protein detrimental effects of, 19 Acid base balance bicarbonate effects, 176 in bone human studies, 174 mechanisms, 173 174 in muscle aging, 174 175 alkali supplementation
A Acid base balance dietary protein detrimental effects of, 19 Acid base balance bicarbonate effects, 176 in bone human studies, 174 mechanisms, 173 174 in muscle aging, 174 175 alkali supplementation
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
CALCIUM BALANCE. James T. McCarthy & Rajiv Kumar
 CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
Magnesium deficiency increases serum fibroblast growth factor-23 levels in rats
 Magnesium Research 2013; 26 (1): 18-23 ORIGINAL ARTICLE Magnesium deficiency increases serum fibroblast growth factor-23 levels in rats Hiroshi Matsuzaki 1, Yasutaka Kajita 2, Misao Miwa 1 1 Department
Magnesium Research 2013; 26 (1): 18-23 ORIGINAL ARTICLE Magnesium deficiency increases serum fibroblast growth factor-23 levels in rats Hiroshi Matsuzaki 1, Yasutaka Kajita 2, Misao Miwa 1 1 Department
National University Faculty of Medicine RICKETS. Dr. Gehan M. Osman MBBS, MD Pediatrics Jaffar Ibn Auf Specialized Hospital
 National University Faculty of Medicine RICKETS Dr. Gehan M. Osman MBBS, MD Pediatrics Jaffar Ibn Auf Specialized Hospital DEFINITION o Rickets is consequence of the vitamin D deficit and may occur
National University Faculty of Medicine RICKETS Dr. Gehan M. Osman MBBS, MD Pediatrics Jaffar Ibn Auf Specialized Hospital DEFINITION o Rickets is consequence of the vitamin D deficit and may occur
Hypophosphatemic Rickets with Hypercalciuria
 REFERENCES 1. Hasselbach H. Idiopathic myelo-fibrosis. A clinical study of 80 patients. Am J Hematol 1990, 34: 291-300. 2. McCarthy DM. Fibrosis of the bone marrow: content and cause. Br J Hematol 1985,
REFERENCES 1. Hasselbach H. Idiopathic myelo-fibrosis. A clinical study of 80 patients. Am J Hematol 1990, 34: 291-300. 2. McCarthy DM. Fibrosis of the bone marrow: content and cause. Br J Hematol 1985,
Conventional Therapy in Adults With X-Linked Hypophosphatemia: Effects on Enthesopathy and Dental Disease
 ORIGINAL ARTICLE Conventional Therapy in Adults With X-Linked Hypophosphatemia: Effects on Enthesopathy and Dental Disease Jessica Connor,* Elizabeth A. Olear,* Karl L. Insogna, Lee Katz, Suher Baker,
ORIGINAL ARTICLE Conventional Therapy in Adults With X-Linked Hypophosphatemia: Effects on Enthesopathy and Dental Disease Jessica Connor,* Elizabeth A. Olear,* Karl L. Insogna, Lee Katz, Suher Baker,
The Parathyroid Glands
 The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
Skeletal Manifestations
 Skeletal Manifestations of Metabolic Bone Disease Mishaela R. Rubin, MD February 21, 2008 The Three Ages of Women Gustav Klimt 1905 1 Lecture Outline Osteoporosis epidemiology diagnosis secondary causes
Skeletal Manifestations of Metabolic Bone Disease Mishaela R. Rubin, MD February 21, 2008 The Three Ages of Women Gustav Klimt 1905 1 Lecture Outline Osteoporosis epidemiology diagnosis secondary causes
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Phosphatonins a new perspective on mineral metabolism
 Mædica - a Journal of Clinical Medicine STATE TE-OF OF-THE THE-AR ART Phosphatonins a new perspective on mineral metabolism Irinel-Doina MAFTEI, MD; Adrian COVIC, MD, PhD Nephrology Clinic, C.I. Parhon
Mædica - a Journal of Clinical Medicine STATE TE-OF OF-THE THE-AR ART Phosphatonins a new perspective on mineral metabolism Irinel-Doina MAFTEI, MD; Adrian COVIC, MD, PhD Nephrology Clinic, C.I. Parhon
A Clinical and Molecular Genetic Study of Hypophosphatemic Rickets in Children
 0031-3998/05/5802-0329 PEDIATRIC RESEARCH Vol. 58, No. 2, 2005 Copyright 2005 International Pediatric Research Foundation, Inc. Printed in U.S.A. A Clinical and Molecular Genetic Study of Hypophosphatemic
0031-3998/05/5802-0329 PEDIATRIC RESEARCH Vol. 58, No. 2, 2005 Copyright 2005 International Pediatric Research Foundation, Inc. Printed in U.S.A. A Clinical and Molecular Genetic Study of Hypophosphatemic
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Osteoporosis, Osteomalasia & rickets. Bone disorders
 Osteoporosis, Osteomalasia & rickets Bone disorders Thank You for Your comments Voice--- Ok Lecture too long--- this is in schedule??? More interaction--- I can do that inshalla Slides are crowded--- but
Osteoporosis, Osteomalasia & rickets Bone disorders Thank You for Your comments Voice--- Ok Lecture too long--- this is in schedule??? More interaction--- I can do that inshalla Slides are crowded--- but
X-Linked Hypophosphatemia in Adults New Biology, New Therapies
 X-Linked Hypophosphatemia in Adults New Biology, New Therapies September 16, 2016 Karl L. Insogna, MD Ensign Professor of Medicine/Endocrinology Yale School of Medicine CONFLICT OF INTEREST Karl Insogna
X-Linked Hypophosphatemia in Adults New Biology, New Therapies September 16, 2016 Karl L. Insogna, MD Ensign Professor of Medicine/Endocrinology Yale School of Medicine CONFLICT OF INTEREST Karl Insogna
REVIEWS. The FGF23 Klotho axis: endocrine regulation of phosphate homeostasis. M. Shawkat Razzaque
 The FGF23 Klotho axis: endocrine regulation of phosphate homeostasis M. Shawkat Razzaque Abstract Appropriate levels of phosphate in the body are maintained by the coordinated regulation of the bone-derived
The FGF23 Klotho axis: endocrine regulation of phosphate homeostasis M. Shawkat Razzaque Abstract Appropriate levels of phosphate in the body are maintained by the coordinated regulation of the bone-derived
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
METABOLISM, INCLUDING CALCIUM/PHOSPHATE METABOLISM
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 12. Disorders of bone metabolism, including calcium/phosphate metabolism. Horm Res 2007;68(suppl 2):87 90 ESPE
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 12. Disorders of bone metabolism, including calcium/phosphate metabolism. Horm Res 2007;68(suppl 2):87 90 ESPE
Targeted ablation of Fgf23 demonstrates an essential physiological role of FGF23 in phosphate and vitamin D metabolism
 Targeted ablation of Fgf23 demonstrates an essential physiological role of FGF23 in phosphate and vitamin D metabolism Takashi Shimada, 1 Makoto Kakitani, 1 Yuji Yamazaki, 1 Hisashi Hasegawa, 1 Yasuhiro
Targeted ablation of Fgf23 demonstrates an essential physiological role of FGF23 in phosphate and vitamin D metabolism Takashi Shimada, 1 Makoto Kakitani, 1 Yuji Yamazaki, 1 Hisashi Hasegawa, 1 Yasuhiro
The phosphatonin pathway: New insights in phosphate homeostasis.
 Kidney International, Vol. 65 (2004), pp. 1 14 The phosphatonin pathway: New insights in phosphate homeostasis PERSPECTIVES IN BASIC SCIENCE SUSAN C. SCHIAVI and RAJIV KUMAR Genzyme Corporation, Framingham,
Kidney International, Vol. 65 (2004), pp. 1 14 The phosphatonin pathway: New insights in phosphate homeostasis PERSPECTIVES IN BASIC SCIENCE SUSAN C. SCHIAVI and RAJIV KUMAR Genzyme Corporation, Framingham,
Osteopetrosis, Hypophosphatemia, and Phosphaturia in a Young Man: A Case Presentation and Differential Diagnosis
 Osteopetrosis, Hypophosphatemia, and Phosphaturia in a Young Man: A Case Presentation and Differential Diagnosis Zahi Mitri, Emory University Vin Tangpricha, Emory University Journal Title: Case Reports
Osteopetrosis, Hypophosphatemia, and Phosphaturia in a Young Man: A Case Presentation and Differential Diagnosis Zahi Mitri, Emory University Vin Tangpricha, Emory University Journal Title: Case Reports
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
Vitamin D Hormone Du Jour
 Vitamin D Hormone Du Jour J R Minkoff MD, FACP Endocrinology Clinical Professor of Family and Community Medicine UCSF Why Is Vitamin D Important? Musculo-skeletal effects Possible other effects Immunomodulatory
Vitamin D Hormone Du Jour J R Minkoff MD, FACP Endocrinology Clinical Professor of Family and Community Medicine UCSF Why Is Vitamin D Important? Musculo-skeletal effects Possible other effects Immunomodulatory
A Novel PHEX Gene Mutation in a Patient with Sporadic Hypophosphatemic Rickets
 Case Report Endocrinol Metab 2014;29:195-201 http://dx.doi.org/10.3803/enm.2014.29.2.195 pissn 2093-596X eissn 2093-5978 A Novel PHEX Gene Mutation in a Patient with Sporadic Hypophosphatemic Rickets Yea
Case Report Endocrinol Metab 2014;29:195-201 http://dx.doi.org/10.3803/enm.2014.29.2.195 pissn 2093-596X eissn 2093-5978 A Novel PHEX Gene Mutation in a Patient with Sporadic Hypophosphatemic Rickets Yea
A case of X-linked hypophosphatemic rickets: complications and the therapeutic use of cinacalcet
 European Journal of Endocrinology (2008) 159 S101 S105 ISSN 0804-4643 A case of X-linked hypophosphatemic rickets: complications and the therapeutic use of cinacalcet Helge Ræder 1,2, Nick Shaw 3, Coen
European Journal of Endocrinology (2008) 159 S101 S105 ISSN 0804-4643 A case of X-linked hypophosphatemic rickets: complications and the therapeutic use of cinacalcet Helge Ræder 1,2, Nick Shaw 3, Coen
H 2 O, Electrolytes and Acid-Base Balance
 H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
FGF23 in CKD and ESRD Regulator of phosphorus balance, or much more than that?
 FGF23 in CKD and ESRD Regulator of phosphorus balance, or much more than that? Csaba P Kovesdy MD University of Tennessee Health Science Center Memphis, TN USA Learning Objectives Review the pathogenesis
FGF23 in CKD and ESRD Regulator of phosphorus balance, or much more than that? Csaba P Kovesdy MD University of Tennessee Health Science Center Memphis, TN USA Learning Objectives Review the pathogenesis
PARATHYROID, VITAMIN D AND BONE
 PARATHYROID, VITAMIN D AND BONE G M Kellerman Pathology North Hunter Service 30/01/2015 BIOLOGY OF BONE Bone consists of protein, polysaccharide components and mineral matrix. The mineral is hydroxylapatite,
PARATHYROID, VITAMIN D AND BONE G M Kellerman Pathology North Hunter Service 30/01/2015 BIOLOGY OF BONE Bone consists of protein, polysaccharide components and mineral matrix. The mineral is hydroxylapatite,
L EVIEW. Fibroblast Growth Factor (FGF)-23 and Hypophosphatemic. rickets/osteomalacia. Endocrine Journal 2001, 48 (6),
 Endocrine Journal 2001, 48 (6), 603-610 R L EVIEW Fibroblast Growth Factor (FGF)-23 and Hypophosphatemic Rickets/Osteomalacia SEIJI FUKUMOTO AND TAKEYOSHI YAMASHITA* Department of Laboratory Medicine,
Endocrine Journal 2001, 48 (6), 603-610 R L EVIEW Fibroblast Growth Factor (FGF)-23 and Hypophosphatemic Rickets/Osteomalacia SEIJI FUKUMOTO AND TAKEYOSHI YAMASHITA* Department of Laboratory Medicine,
Vitamin D: Is it a superhero??
 Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Natpara (parathyroid hormone) Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Natpara (parathyroid hormone) Prime Therapeutics will review Prior Authorization
Natpara (parathyroid hormone) Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Natpara (parathyroid hormone) Prime Therapeutics will review Prior Authorization
OSTEOMALACIA UPDATE. Nothing to Disclose. Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco
 OSTEOMALACIA UPDATE Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco Nothing to Disclose 1 Case History 59 YO WM referred for evaluation of diffuse
OSTEOMALACIA UPDATE Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco Nothing to Disclose 1 Case History 59 YO WM referred for evaluation of diffuse
Agent(s) FDA Labeled Indications Dosage and Administration. Perinatal/Infantile-onset hypophosphatasia. Juvenile-onset hypophosphatasia
 Strensiq (asfotase alfa) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE Agent(s) FDA Labeled Indications Dosage and Administration Strensiq (asfotase alfa) injection Perinatal/Infantile-onset
Strensiq (asfotase alfa) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE Agent(s) FDA Labeled Indications Dosage and Administration Strensiq (asfotase alfa) injection Perinatal/Infantile-onset
David Bruyette, DVM, DACVIM
 VCAwestlaspecialty.com David Bruyette, DVM, DACVIM Disorders of calcium metabolism are common endocrine disorders in both dogs and cats. In this article we present a logical diagnostic approach to patients
VCAwestlaspecialty.com David Bruyette, DVM, DACVIM Disorders of calcium metabolism are common endocrine disorders in both dogs and cats. In this article we present a logical diagnostic approach to patients
Vitamin D. Vitamin functioning as hormone. Todd A Fearer, MD FACP
 Vitamin D Vitamin functioning as hormone Todd A Fearer, MD FACP Vitamin overview Vitamins are organic compounds that are essential in small amounts for normal metabolism They are different from minerals
Vitamin D Vitamin functioning as hormone Todd A Fearer, MD FACP Vitamin overview Vitamins are organic compounds that are essential in small amounts for normal metabolism They are different from minerals
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
burosumab (Crysvita )
 burosumab (Crysvita ) Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ),
burosumab (Crysvita ) Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ),
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Osteomalacia in a young adult
 82 Alonso G 1, Varsavsky M 2 1 Servicio de Endocrinología - Humane Especialidades Médicas - Río Cuarto (Argentina) 2 Servicio de Endocrinología - Hospital Italiano de Buenos Aires - Buenos Aires (Argentina)
82 Alonso G 1, Varsavsky M 2 1 Servicio de Endocrinología - Humane Especialidades Médicas - Río Cuarto (Argentina) 2 Servicio de Endocrinología - Hospital Italiano de Buenos Aires - Buenos Aires (Argentina)
FGF23 parathyroid interaction: implications in chronic kidney disease
 http://www.kidney-international.org & 2010 International Society of Nephrology FGF23 parathyroid interaction: implications in chronic kidney disease Hirotaka Komaba 1 and Masafumi Fukagawa 1,2 1 Division
http://www.kidney-international.org & 2010 International Society of Nephrology FGF23 parathyroid interaction: implications in chronic kidney disease Hirotaka Komaba 1 and Masafumi Fukagawa 1,2 1 Division
OMICS Journals are welcoming Submissions
 OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
Bone Remodeling & Repair Pathologies
 Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
38 year old Male with Ankylosing Spondylitis. Olesya Krivospitskaya, MD April,
 38 year old Male with Ankylosing Spondylitis Olesya Krivospitskaya, MD April, 11 2013 HPI (Letter from the patient): Diagnosed with Ankylosing Spondylitis and prescribed a Sulfa drug to help with my back
38 year old Male with Ankylosing Spondylitis Olesya Krivospitskaya, MD April, 11 2013 HPI (Letter from the patient): Diagnosed with Ankylosing Spondylitis and prescribed a Sulfa drug to help with my back
Tumor-induced Osteomalacia Caused by a Parotid Tumor
 CASE REPORT Tumor-induced Osteomalacia Caused by a Parotid Tumor Yuichi Takashi 1, Yuka Kinoshita 1, Nobuaki Ito 1, Manabu Taguchi 1, Masaaki Takahashi 2, Naoya Egami 2, Shogo Tajima 3, Masaomi Nangaku
CASE REPORT Tumor-induced Osteomalacia Caused by a Parotid Tumor Yuichi Takashi 1, Yuka Kinoshita 1, Nobuaki Ito 1, Manabu Taguchi 1, Masaaki Takahashi 2, Naoya Egami 2, Shogo Tajima 3, Masaomi Nangaku
Biochemistry #01 Bone Formation Dr. Nabil Bashir Farah Banyhany
 Biochemistry #01 Bone Formation Dr. Nabil Bashir Farah Banyhany Greetings This lecture is quite detailed, but I promise you will make it through, it just requires your 100% FOCUS! Let s begin. Today s
Biochemistry #01 Bone Formation Dr. Nabil Bashir Farah Banyhany Greetings This lecture is quite detailed, but I promise you will make it through, it just requires your 100% FOCUS! Let s begin. Today s
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A A Diabetes Outcome Progression Trial (ADOPT), 194 Adaptive immunity, 129 131 ADOPT (A Diabetes Outcome Progression Trial), 194 Aging, vitamin
Note: Page numbers of article titles are in boldface type. A A Diabetes Outcome Progression Trial (ADOPT), 194 Adaptive immunity, 129 131 ADOPT (A Diabetes Outcome Progression Trial), 194 Aging, vitamin
The Role of the Laboratory in Metabolic Bone Disease
 The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
BMD: A Continuum of Risk WHO Bone Density Criteria
 Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
CKD-MBD CKD mineral bone disorder
 CKD Renal bone disease Dr Mike Stone University Hospital Llandough Affects 5 10 % of population Increasingly common Ageing, diabetes, undetected hypertension Associated with: Cardiovascular disease Premature
CKD Renal bone disease Dr Mike Stone University Hospital Llandough Affects 5 10 % of population Increasingly common Ageing, diabetes, undetected hypertension Associated with: Cardiovascular disease Premature
Vitamin D Deficiency. Decreases renal calcium excretion. Increases intestinal absorption Calcium. Increases bone resorption of calcium
 Vitamin D Deficiency Deborah Gordish, MD Assistant Professor of Clinical Internal Medicine Lead Physician Lewis Center Primary Care Associate Division Director General Internal Medicine The Ohio State
Vitamin D Deficiency Deborah Gordish, MD Assistant Professor of Clinical Internal Medicine Lead Physician Lewis Center Primary Care Associate Division Director General Internal Medicine The Ohio State
Nuclear receptors. Lecture 4. VDR: Not bones only
 Nuclear receptors Lecture 4 VDR: Not bones only Bones - During embryogenesis development of bones is a late event it is the last stage of skeleton formation. - Bone is a strongly metabolizing tissue, regulating
Nuclear receptors Lecture 4 VDR: Not bones only Bones - During embryogenesis development of bones is a late event it is the last stage of skeleton formation. - Bone is a strongly metabolizing tissue, regulating
Ca, Mg metabolism, bone diseases. Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary
 Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Clinical Policy: Measurement of Serum 1,25-dihydroxyvitamin D
 Clinical Policy: Reference Number: CP.MP.152 Last Review Date: 12/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Clinical Policy: Reference Number: CP.MP.152 Last Review Date: 12/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Impact of serum FGF23 levels on blood pressure of patients with chronic kidney disease
 European Review for Medical and Pharmacological Sciences 2018; 22: 721-725 Impact of serum FGF23 levels on blood pressure of patients with chronic kidney disease J.-X. LI, G.-Q. YU, Y.-Z. ZHUANG Department
European Review for Medical and Pharmacological Sciences 2018; 22: 721-725 Impact of serum FGF23 levels on blood pressure of patients with chronic kidney disease J.-X. LI, G.-Q. YU, Y.-Z. ZHUANG Department
AACE Southern States Chapter Lecture. Basics
 AACE Southern States Chapter Lecture Unusual Bone Cases Basics Osteoporosis Osteomalacia Renal Osteodystrophy Multiple Myeloma 1 Osteoporosis Definition Modeling, Bone Remodeling Bone Resorption > Bone
AACE Southern States Chapter Lecture Unusual Bone Cases Basics Osteoporosis Osteomalacia Renal Osteodystrophy Multiple Myeloma 1 Osteoporosis Definition Modeling, Bone Remodeling Bone Resorption > Bone
