METABOLISM, INCLUDING CALCIUM/PHOSPHATE METABOLISM
|
|
|
- Cameron Marsh
- 6 years ago
- Views:
Transcription
1 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 12. Disorders of bone metabolism, including calcium/phosphate metabolism. Horm Res 2007;68(suppl 2):87 90 ESPE Code Diagnosis OMIM ICD10 12 DISORDERS OF BONE METABOLISM, INCLUDING CALCIUM/PHOSPHATE METABOLISM 12A TRANSIENT HYPOCALCAEMIA (NEONATAL) E A.1 Early neonatal 1 P A.1a Prematurity 2 12A.1b Asphyxia 12A.1c Infant of diabetic mother 12A.1d Perinatal stress or trauma 12A.2 Late neonatal 3 P A.2a Disorders classified elsewhere: Conditions classified under permanent hypocalcaemia, hypomagnesaemia 12A.2b High milk phosphate load P71.0, P A.2c Parenteral nutrition 12A.2d Exchange transfusions 12A.2e Chronic alkalosis or bicarbonate treatment 12A.2f Maternal hypercalcaemia 12A.2g Maternal vitamin D deficiency 12A.2h Transient hypoparathyroidism P B PERMANENT HYPOCALCAEMIA 12B.1 Genetic disorders of the calcium-sensing receptor 12B.1a Autosomal-dominant hypocalcaemia # B.1b Autosomal-dominant hypocalcaemia with Bartter-like features B.2 Hypoparathyroidism E B.2a Disorders classified elsewhere: E20.8 DiGeorge syndrome types 1 and 2 (14B.10) Autoimmune polyglandular syndrome type 1 (APECED syndrome) (14C.4a) 12B.2b X-linked hypoparathyroidism % E20.8 Disorders of Bone Metabolism, Including Calcium/Phosphate Metabolism 87
2 ESPE Code Diagnosis OMIM ICD10 12B.2c Mitochondrial disorders 12B.2c.1 Kearns-Sayre # B.2c.2 MELAS # B.2c.3 Pearson marrow-pancreas syndrome # B.2c.4 trna-leu mutation * B.2c.9 Other 12B.2d Hypoparathyroidism, deafness and renal anomalies (Barakat # syndrome) 12B.2e Long-chain hydroxyacyl-coa dehydrogenase deficiency (LCHAD deficiency) [primary 11B.5d] * B.2f Other familial syndromes E B.2f.1 Kenny-Caffey syndrome type 1 # B.2f.2 Sanjad-Sakati # B.2f.9 Other specified syndromes 12B.2g Acquired hypoparathyroidism 12B.2g.1 Parathyroid surgery 12B.2g.2 Isolated autoimmune hypoparathyroidism 12B.2g.3 Iron overload 12B.2g.4 Other specified acquired forms 12B.2z Idiopathic E B.3 PTH defects (autosomal-dominant or autosomal-recessive familial isolated hypoparathyroidism) # E B.4 PTH/PTHrP receptor defects 4 12B.4a Pseudohypoparathyroidism type 1b # B.4z Other PTH/PTHrP receptor defects, unspecified 12B.5 Post-receptor defects 12B.5a Classified elsewhere: Pseudohypoparathyroidism type Ia (Albright s hereditary osteodystrophy, 14B.2) 12B.5b Pseudohypoparathyroidism type Ic # E B.5c Pseudohypoparathyroidism type II % E B.5d Pseudohypoparathyroidism with testotoxicosis # E B.6 Magnesium deficiency 5 E B.6a Familial primary hypomagnesaemia # B.6b Familial hypomagnesaemia with hypercalciuria, # nephrocalcinosis, and severe ocular involvement 12B.6c Isolated renal magnesium wasting # B.6d Hypomagnesaemia with secondary hypocalcemia # E20.1 ESPE Classification of Paediatric Endocrine Diagnoses 88
3 ESPE Code Diagnosis OMIM ICD10 12B.6e Gitelman syndrome [primary 14B.15] # B.7 Calciopenic rickets (see 12C.1) 12B.8 Systemic conditions associated with hypocalcaemia 12B.8a Tumour lysis syndrome 12B.8b Renal osteodystrophy 6 N B.8c AIDS 12B.8y Other specified conditions 12B.8z Other conditions, unspecified 12C RICKETS 12C.1 Calciopenic rickets E C.1a Nutritional (vitamin D deficiency) 12C.1a.1 Malabsorption 12C.1a.2 Liver disease 12C.1a.3 Anticonvulsant treatment (phenobarbital, phenytoin) 12C.1a.4 Renal osteodystrophy 6 N C.1a.5 Calcium deficiency rickets 7 12C.1b Genetic 12C.1b.1 Vitamin D 1 -hydroxylase deficiency (formerly known as # E83.3 pseudo-vitamin D-deficiency rickets, vitamin D-dependent rickets type I) 12C.1b.2 Hereditary 1,25(OH) 2 D-resistant rickets (formerly known as pseudo-vitamin D-deficiency rickets type II, vitamin D-dependent rickets type II, calcitriol-resistant rickets) # E C.2 Phosphopenic rickets E C.2a Classified elsewhere: McCune-Albright syndrome (14B.22) Renal tubular disorders Fanconi renotubular syndrome (14B.13) 12C.2b Familial hypophosphataemic rickets 12C.2b.1 X-linked hypophosphataemic rickets 8 # C.2b.2 Autosomal-dominant hypophosphataemic rickets 9 # C.2b.3 Hereditary hypophosphataemic rickets with hypercalciuria 10 # C.2b.4 Hypophosphataemic nonrachitic bone disease % C.2c Tumour-induced osteomalacia 11 12C.2d Decreased phosphate intake 12 12C.3 Hypopophosphatasia (if not associated with rickets, classify under 12E.5l) # # E83.3 Disorders of Bone Metabolism, Including Calcium/Phosphate Metabolism 89
4 ESPE Code Diagnosis OMIM ICD10 12D OSTEOPOROSIS M D.1 Genetic defects 12D.1a Classified elsewhere: Ehlers-Danlos syndrome (14B.11) Marfan syndrome [primary 14B.20, other secondary 2A.2a] 12D.1b Osteogenesis imperfecta (types I VII) # # # # # D.1c Homocystinuria [if tall, classify also as 2A.2c] D.1d Other genetic defects 12D.2 Chromosomal defects M D.3 Endocrine disorders M D.4 Iatrogenic causes M D.5 Nutritional disorders M D.6 Chronic diseases M D.7 Malignancies M D.8 Disuse M D.9 Other specified disorders, e.g. muscle and neuromuscular disorders M D.10 Idiopathic juvenile osteoporosis 13 M E HYPERCALCAEMIA E E.1 Disorders of the calcium-sensing receptor 12E.1a Familial benign hypercalcaemia (familial hypocalciuric # hypercalcaemia) 12E.1b Neonatal severe primary hyperparathyroidism # E.1c Calcium-sensing receptor blocking antibodies ESPE Classification of Paediatric Endocrine Diagnoses 90
5 ESPE Code Diagnosis OMIM ICD10 12E.2 Disorders of the parathyroid glands/pth oversecretion E21 12E.2a Disorders classified elsewhere: Multiple endocrine neoplasia type 1 (14C.5a) Multiple endocrine neoplasia type 2a (14C.5b) Multiple endocrine neoplasia type 2b (14C.5c) 12E.2b Familial isolated hyperparathyroidism, type 1 # E E.2c Familial isolated hyperparathyroidism, type 2 (jaw tumour) # E E.2d Sporadic parathyroid adenomas E E.2e Parathyroid carcinomas E E.2f Tertiary hyperparathyroidism E E.2y Other PTH abnormalities (specified) E E.3 PTH/PTHrP Receptor abnormalities 12E.3a Metaphyseal chondrodysplasia, Jansen type # Q E.4y Other PTH/PTHrP receptor abnormalities (specified) 12E.4 Abnormal vitamin D metabolism 12E.4a Disorders classified elsewhere: Williams-Beuren syndrome (14B.37) 12E.4b Idiopathic infantile hypercalcaemia 14 # E.5 Miscellaneous causes of hypercalcaemia in childhood E E.5a Vitamin D (or vitamin D metabolite) intoxication 15 E E.5b Sarcoidosis, other granulomatous diseases D E.5c Immobilisation 16 E E.5d Hypercalcaemia of malignancy E E.5e Subcutaneous fat necrosis 12E.5f Excessive calcium supplementation 12E.5g Congenital lactase deficiency # E.5h Disaccharidase deficiency # E.5i Endocrine forms (adrenal insufficiency, severe congenital hypothyroidism, thyrotoxicosis) (primarily classified elsewhere) 12E.5j Down syndrome # Q90 12E.5k AIDS B24 12E.5l IMAGe syndrome E.5m Hypophosphatasia # E E.5y Other specified disorders 12E.5z Other disorders (unspecified) Disorders of Bone Metabolism, Including Calcium/Phosphate Metabolism 91
6 1 Early neonatal hypocalcemia (ENH) (<72 h) Phenotype: Specific signs: tetany, generalised or focal clonic seizures, frequent twitches or jerking of limbs, hyperacusis, laringospasm, jitteriness, irritability; nonspecific signs: apnoea, tachycardia, tachypnoea, cyanosis, oedema; may be asymptomatic. Serum-Ca ( ), P (+), Mg ( ), PTH (+), CT (+), 25-OHD ( ), 1,25(OH) 2 D ( ). Comments: The mechanism(s) of ENH is uncertain; possible pathogenetic factors are exaggerated postnatal depression of circulating Ca levels, transient pseudohypoparathyroid-like state probably due to an immaturity of renal and bone response to PTH, and exaggerated rise in CT levels. Reduced 25-OHD and 1,25(OH) 2 D levels may be contributing factors. Conditions at risk to develop ENH: diabetes in the mother, pre-eclampsia, perinatal asphyxia, and prematurity. 2 Metabolic bone disease (MBD) of prematurity Synonym: Rickets of prematurity, osteopenia of prematurity. Phenotype: Asymptomatic, or hypotonia, signs of rickets and/or osteopenia, fractures of the ribs or long bones, skeletal deformities (rib cage softening, altered head shape), respiratory distress syndrome, growth delay. Serum-Ca ( /N), P ( /N), alkaline phosphatase (+/N), PTH (+/N), 25-OHD ( /N), 1,25(OH) 2 D (+ if Ca and P are reduced, in case of substrate deficiency), urine-ca (+ in phosphate depletion syndrome), urine-p (+ in secondary hyperparathyroidism, in phosphate depletion syndrome or normal). Hormonal findings may vary on the basis of the amount of Ca and P supplied by the preterm formula, fortified human milk, or parenteral nutrition, the degree of vitamin D deficiency, and the adaptative mechanisms in response to the dietary mineral insufficiency. Comments: MBD of prematurity mainly arises from insufficient dietary minerals (Ca and P). Copper deficiency, as a result of abnormal collagen metabolism, has also been implicated in this condition. Phosphate depletion syndrome mainly occurs in preterm neonates who are fed unfortified human milk or during parenteral nutrition. 3 Late neonatal hypocalcemia (> 72 h) Phenotype: Asymptomatic, or symptoms similar to those of early neonatal hypocalcaemia. Serum- Ca ( ), P (+), Mg ( ), PTH ( /+), CT (N), 25-OHD ( ), 1,25(OH) 2 D ( ). Comments: Possible pathogenetic factors seem to be excessive dietary P load in neonates fed cow s milk or cow s milk based formula with Ca/P molar ratio 3 4 times that of human milk, inability of the immature kidney to excrete P efficiently, insufficient PTH response to hypocalcaemia, and materno-foetal vitamin D deficiency. Late neonatal hypocalcaemia is less frequent than early neonatal hypocalcaemia. The incidence of late neonatal hypocalcaemia is greater in full term than in preterm infants. Infants of diabetic mother and infants with transient hypoparathyroidism due to maternal hypercalcaemia secondary to primary hyperparathyroidism may be at risk for late neonatal hypocalcaemia. 4 PTH/PTHrP receptor defects Comment: A congenital defect of the PTH/PTHrP receptor is Blomstrand chondrodysplasia, a perinatally lethal condition, that does not present with hypocalcaemia. 5 Magnesium deficiency Comment: Only some conditions, such as familial primary hypomagnesaemia and hypomagnesaemia with secondary hypocalcaemia, show hypocalcaemia. ESPE Classification of Paediatric Endocrine Diagnoses 92
7 6 Renal osteodystrophy (ROD) Phenotype: Growth failure, bone pain, muscle weakness, skeletal deformities (scoliosis, kyphosis, genu valgum, distorsion of the thoracic cage), bone fractures (ribs, hips, vertebral bodies), extraskeletal calcifications (periarticular, vascular, subcutaneous, and visceral). Serum-P (+), Ca ( ), Mg (+), alkaline phosphatase (+), PTH (+), 25-OHD ( /N), 1,25(OH) 2 D ( ). Osteitis fibrosa (subperiosteal erosions, osteosclerosis, slipped epiphyses), rickets-like lesions. Comments: ROD is determined by the skeletal effect of secondary hyperparathyroidism associated with a reduced 1,25(OH) 2 D production. Reduced GFR ] decreased urinary loss of P ] mild hyperphosphataemia ] hypocalcaemia ] secondary hyperparathyroidism. As renal function continues to decline, hypocalcaemia is further aggravated by a resistance to the action of PTH on bone. In addition, the set-point for the inhibition of PTH secretion by extracellular calcium is raised in chronic renal failure, making it more difficult to turn off the secondary hyperparathyroidism. Reduced 1,25(OH) 2 D production derives from a decline in the functioning renal mass available to perform 1 -hydroxylation of 25-OHD, hyperphosphataemia suppressing renal 1 -hydroxylase activity, and metabolic acidosis. The signs and symptoms of ROD are rather nonspecific, and laboratory and radiological abnormalities often do not correspond to the severity of the clinical manifestations. 7 Calcium deficiency rickets Phenotype: Clinical features are identical to those observed in patients with vitamin D deficiency rickets. Calcium deficiency rickets usually occurs after the age of 18 months. Serum-Ca ( /N), P ( /N), alkaline phosphatase (+), PTH (N/+), 25-OHD (N/ ), 1,25(OH) 2 D (+). Comments: Low dietary calcium intake, often exacerbated by a high oxalate and phytate content in the diet that impairs intestinal calcium absorption, is not able to ensure calcium demand for growth plate mineralisation. Reduced calcium intake ] hypocalcaemia ] secondary hyperparathyroidism ] increased 1,25(OH) 2 D production. Reduced 25-OH-D levels due to increased catabolism. 8 X-linked hypophosphataemic rickets (XLH) Synonyms: Hypophosphataemic vitamin D-resistant rickets. Phenotype: Growth failure with disproportionate short stature, lower limbs deformities, dental and periodontal lesions. Serum-P ( ), alkaline phosphatase (+), PTH (N), 25-OHD (N), 1,25(OH) 2 D ( or inappropriately normal relative to hypophosphataemia), TmP/GFR ( ), urine-p (+), urine-ca (N). Osteomalacia in both cortical and trabecular bone, increase in osteoid volume, areas of hypomineralisation around osteocytes in the lamellar cortical bone. Comment: Defective tubular reabsorption of P associated with abnormal renal vitamin D metabolism caused by mutations in the PHEX (phosphate-regulating gene with homology to endopeptidases) gene, which is located on Xp Autosomal-dominant hypophosphataemic rickets (ADHR) Synonym: Vitamin D-resistant rickets. Phenotype: Clinical features are similar to those observed in patients with XLH. In contrast to XLH, ADHR shows incomplete penetrance, variable age at onset (childhood to adult), and resolution of the phosphate-wasting defect in rare cases. Comments: Autosomal dominant. It is caused by mutation in a gene encoding a member of the fibroblast growth factor family (FGF23). Disorders of Bone Metabolism, Including Calcium/Phosphate Metabolism 93
8 10 Hereditary hypophosphataemic rickets with hypercalciuria (HHRH) Synonym: Hypercalciuric hypophosphataemic rickets. Phenotype: Stunted growth, lower limbs deformities. Serum-P ( ), PTH (N), 25-OHD (N), 1,25(OH) 2 D (+), TmP/GFR ( ), urine-p (+), urine-ca (+). Comments: Defective tubular reabsorption of P ] hypophosphataemia ] increased 1,25(OH) 2 D production ] increased intestinal calcium absorption ] hypercalcaemia ] increased calcium filtered load and PTH suppression ] hypercalciuria. A significant number of asymptomatic family members showed idiopathic hypercalciuria alone without associated bone disease. Complete remission of the disease on P therapy alone. 11 Tumour rickets and osteomalacia Synonyms: Tumour-associated rickets and osteomalacia, tumour-induced rickets, oncogenic hypophosphataemic osteomalacia (OHO), oncogenic rickets and osteomalacia. Phenotype: Stunted growth, bone and muscle pain, muscle weakness, fatigue, gait disturbances, skeletal abnormalities (bowing of the lower limbs), recurrent fractures of long bones (occasionally). The majority of patients have benign or malignant tumours of mesenchymal origin of either soft tissues or bone, carcinomas of epidermal or endodermal origin; occasionally, epidermal naevus, von Recklinghausen neurofibromatosis. Serum-P ( ), 25-OHD (N), 1,25(OH) 2 D ( or inappropriately normal relative to hypophosphatemia), TmP/GFR ( ), urine-p (+). Occasionally glycinuria, glucosuria, and hyperaminoaciduria. Comments: Production of a humoral factor(s) known as phosphatonin (FGF-23, matrix extracellular phosphoglycoprotein, frizzled-related protein 4), that may affect multiple functions of the proximal renal tubule, including P reabsorption. Complete resection of the tumour restores normophosphataemia. 12 Decreased phosphate intake Synonyms: Dietary phosphate deficiency, nutritional phosphate deficiency. Phenotype: Severe serum-p ( ): red cell dysfunction (haemolytic anaemia), leukocyte dysfunction [chemotaxis ( ), phagocytosis ( ), bacterial killing ( )]; platelet dysfunction (thrombocytopenia); musculo-skeletal: rhabdomyolysis, reversible cardiomyopathy and myopathy; CNS: metabolic encephalopathy; metabolic acidosis, rickets/osteomalacia/osteopenia. Serum-P ( ). Comments: The signs and symptoms of severe hypophosphataemia may be related to a decrease in 2,3-diphosphoglycerate and/or ATP content in tissues. Main causes: total parenteral nutrition (nutritional recovery syndrome) in which aluminium loading may be a complicating factor, low-phosphate feedings in low-birthweight infants (phosphate depletion syndrome), malabsorption. 13 Idiopathic juvenile osteoporosis Phenotype: Diffuse bone pain, mainly in the back, hips, and feet, and a characteristic gait with difficulty in walking, associated with radiological evidence of osteoporosis and fractures of the vertebrae and long bones, mostly at metaphyseal sites. Idiopathic juvenile osteoporosis may have a spontaneous recovery, usually within 3 5 years. Comments: The diagnosis of idiopathic juvenile osteoporosis is based on the exclusion of the other known causes of osteoporosis. It may be difficult to distinguish from mild forms of osteogenesis imperfecta. Bone biopsy may be useful for the correct diagnosis. ESPE Classification of Paediatric Endocrine Diagnoses 94
9 14 Idiopathic infantile hypercalcaemia Synonyms: Lightwood type (mild form) and Fanconi-Schlesinger type (severe forms). Phenotype: Similar to patients with Williams-Beuren syndrome; the distinction between the two syndromes remains problematic. Comment: A disorder in vitamin D metabolism with increased vitamin D sensitivity with respect to gastrointestinal transport of Ca has been postulated in some cases. Elevated serum PTHrP levels at the time of hypercalcaemia have been reported. 15 Vitamin D intoxication Synonym: Hypervitaminosis D. Phenotype: Asymptomatic or symptoms of hypercalcaemia/hypercalciuria. Excessive storage of vitamin D in adipose tissue and voluntary muscle. Serum-Ca (+), P (N/+), PTH ( ), 25-OHD (+ if vitamin D or 25-OHD is ingested), 1,25(OH) 2 D (N), urine-ca (+). Comment: Increased action of vitamin D metabolites on intestinal Ca absorption and Ca mobilisation from bone. 16 Immobilisation Synonyms: Immobilisation-induced hypercalciuria, immobilisation-induced hypercalcaemia and osteopenia. Phenotype: Asymptomatic or symptoms related to hypercalcaemia/hypercalciuria. Osteopenia. Serum-Ca (N/+), alkaline phosphatase (N/+), PTH (N), 1,25(OH) 2 D ( ), urine-ca (+), urine-p (+), GFR ( ), metabolic alkalosis. Comment: Uncoupling of bone cells activity for increased osteoclastic bone resorption and decreased osteoblastic bone formation. Disorders of Bone Metabolism, Including Calcium/Phosphate Metabolism 95
Sachin Soni DNB Pediatrics
 Sachin Soni DNB Pediatrics Vitamin D physiology Introduction Etiology Clinical feature Radiology Diagnosis Lab Treatment Source: -Fish, liver and oil, - Human milk (30-40 IU/L) - Exposure to sun light
Sachin Soni DNB Pediatrics Vitamin D physiology Introduction Etiology Clinical feature Radiology Diagnosis Lab Treatment Source: -Fish, liver and oil, - Human milk (30-40 IU/L) - Exposure to sun light
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Magnesium Homeostasis
 ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes.
 Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis
 Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis Tutorial for Specialist Portfolio Biomedical Scientists 03/02/2014 Dr Petros Kampanis Clinical Scientist 1. Calcium Most abundant
Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis Tutorial for Specialist Portfolio Biomedical Scientists 03/02/2014 Dr Petros Kampanis Clinical Scientist 1. Calcium Most abundant
DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS
 DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS XLH IS CHARACTERIZED BY CHRONIC HYPOPHOSPHATEMIA XLH is a hereditary, progressive, lifelong disorder. In children and adults,
DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS XLH IS CHARACTERIZED BY CHRONIC HYPOPHOSPHATEMIA XLH is a hereditary, progressive, lifelong disorder. In children and adults,
CKD-MBD CKD mineral bone disorder
 CKD Renal bone disease Dr Mike Stone University Hospital Llandough Affects 5 10 % of population Increasingly common Ageing, diabetes, undetected hypertension Associated with: Cardiovascular disease Premature
CKD Renal bone disease Dr Mike Stone University Hospital Llandough Affects 5 10 % of population Increasingly common Ageing, diabetes, undetected hypertension Associated with: Cardiovascular disease Premature
Approach to a child presenting with rickets
 Current Practice Approach to a child presenting with rickets Navoda Atapattu 1 Sri Lanka Journal of Child Health, 2013; 42(1): 40-44 (Key words: Rickets; vitamin D; children) Introduction Rickets is a
Current Practice Approach to a child presenting with rickets Navoda Atapattu 1 Sri Lanka Journal of Child Health, 2013; 42(1): 40-44 (Key words: Rickets; vitamin D; children) Introduction Rickets is a
A case of hereditary hypophosphataemic rickets with hypercalciuria (HHRH)
 Case Reports A case of hereditary hypophosphataemic rickets with hypercalciuria (HHRH) M N Lucas 1, Savithri Dias 2 Sri Lanka Journal of Child Health, 2006; 35:141-3 (Key words: hereditary hypophosphataemic
Case Reports A case of hereditary hypophosphataemic rickets with hypercalciuria (HHRH) M N Lucas 1, Savithri Dias 2 Sri Lanka Journal of Child Health, 2006; 35:141-3 (Key words: hereditary hypophosphataemic
CALCIUM BALANCE. James T. McCarthy & Rajiv Kumar
 CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
Inherited Calcium and Magnesium Disorders
 Inherited Calcium and Magnesium Disorders Martin Konrad University Children s Hospital Münster, Germany IPNA / ESPN Master Class, Leuven, Sep 2nd 2015 Outline Hypercalcemia Hypomagnesemia Outline Hypercalcemia
Inherited Calcium and Magnesium Disorders Martin Konrad University Children s Hospital Münster, Germany IPNA / ESPN Master Class, Leuven, Sep 2nd 2015 Outline Hypercalcemia Hypomagnesemia Outline Hypercalcemia
Hypophosphatemic rickets: new treatments
 Hypophosphatemic rickets: new treatments Gema Ariceta Pediatric Nephrology, University Hospital Vall d Hebron, Barcelona 1 11.06.18 Tubulopathies Disclosures Lectures and educational activities sponsored
Hypophosphatemic rickets: new treatments Gema Ariceta Pediatric Nephrology, University Hospital Vall d Hebron, Barcelona 1 11.06.18 Tubulopathies Disclosures Lectures and educational activities sponsored
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
DISEASES WITH ABNORMAL MATRIX
 DISEASES WITH ABNORMAL MATRIX MSK-1 FOR 2 ND YEAR MEDICAL STUDENTS Dr. Nisreen Abu Shahin CONGENITAL DISEASES WITH ABNORMAL MATRIX OSTEOGENESIS IMPERFECTA (OI): also known as "brittle bone disease" a group
DISEASES WITH ABNORMAL MATRIX MSK-1 FOR 2 ND YEAR MEDICAL STUDENTS Dr. Nisreen Abu Shahin CONGENITAL DISEASES WITH ABNORMAL MATRIX OSTEOGENESIS IMPERFECTA (OI): also known as "brittle bone disease" a group
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B.
 Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B. Increased concentration of proteins in foods C. Decreasing
Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B. Increased concentration of proteins in foods C. Decreasing
Parathyroid hormone (serum, plasma)
 Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Hypophosphatasia. Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX
 Hypophosphatasia Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX Hypophosphatasia Case Teeth 57 y/o male with a hyperlipidemia and hypogonadism. Noted to have an alkaline phosphatase of
Hypophosphatasia Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX Hypophosphatasia Case Teeth 57 y/o male with a hyperlipidemia and hypogonadism. Noted to have an alkaline phosphatase of
PARATHYROID, VITAMIN D AND BONE
 PARATHYROID, VITAMIN D AND BONE G M Kellerman Pathology North Hunter Service 30/01/2015 BIOLOGY OF BONE Bone consists of protein, polysaccharide components and mineral matrix. The mineral is hydroxylapatite,
PARATHYROID, VITAMIN D AND BONE G M Kellerman Pathology North Hunter Service 30/01/2015 BIOLOGY OF BONE Bone consists of protein, polysaccharide components and mineral matrix. The mineral is hydroxylapatite,
National University Faculty of Medicine RICKETS. Dr. Gehan M. Osman MBBS, MD Pediatrics Jaffar Ibn Auf Specialized Hospital
 National University Faculty of Medicine RICKETS Dr. Gehan M. Osman MBBS, MD Pediatrics Jaffar Ibn Auf Specialized Hospital DEFINITION o Rickets is consequence of the vitamin D deficit and may occur
National University Faculty of Medicine RICKETS Dr. Gehan M. Osman MBBS, MD Pediatrics Jaffar Ibn Auf Specialized Hospital DEFINITION o Rickets is consequence of the vitamin D deficit and may occur
Clinical biochemistry of calcium and vitamin D
 Clinical biochemistry of calcium and vitamin D Dr Andrew Day Consultant in Clinical Biochemistry and Metabolic Medicine University Hospitals Bristol NHS Trust e-mail: andrew.day@uhbristol.nhs.uk A 48-year
Clinical biochemistry of calcium and vitamin D Dr Andrew Day Consultant in Clinical Biochemistry and Metabolic Medicine University Hospitals Bristol NHS Trust e-mail: andrew.day@uhbristol.nhs.uk A 48-year
Agents that Affect Bone & Mineral Homeostasis
 Agents that Affect Bone & Mineral Homeostasis 1 Agents that Affect Bone & Mineral Homeostasis Calcium and phosphate are the major mineral constituents of bone. They are also two of the most important minerals
Agents that Affect Bone & Mineral Homeostasis 1 Agents that Affect Bone & Mineral Homeostasis Calcium and phosphate are the major mineral constituents of bone. They are also two of the most important minerals
BALANCE 13 DISORDERS OF WATER DISORDERS CHARACTERISED BY POLYDIPSIA AND POLYURIA. (vasopressin deficiency) 1 [primary] [secondary 6C] insipidus
![BALANCE 13 DISORDERS OF WATER DISORDERS CHARACTERISED BY POLYDIPSIA AND POLYURIA. (vasopressin deficiency) 1 [primary] [secondary 6C] insipidus BALANCE 13 DISORDERS OF WATER DISORDERS CHARACTERISED BY POLYDIPSIA AND POLYURIA. (vasopressin deficiency) 1 [primary] [secondary 6C] insipidus](/thumbs/80/80940031.jpg) Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 13. Disorders of water balance. Horm Res 2007;68(suppl 2):96 97 ESPE Code Diagnosis OMIM ICD10 13 DISORDERS OF
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 13. Disorders of water balance. Horm Res 2007;68(suppl 2):96 97 ESPE Code Diagnosis OMIM ICD10 13 DISORDERS OF
= Developmental disorders of chondro-osseous tissue
 = Developmental disorders of chondro-osseous tissue Common Orthopedic Problems Dwarfism Short Stature Pathologic Short Stature Normal Variant Short Stature Proportionate Short Stature Midget Endocrine/nutritional
= Developmental disorders of chondro-osseous tissue Common Orthopedic Problems Dwarfism Short Stature Pathologic Short Stature Normal Variant Short Stature Proportionate Short Stature Midget Endocrine/nutritional
Disorders of calcium homeostasis. FRACP part 1 lecture 2012 Peter Simm
 Disorders of calcium homeostasis FRACP part 1 lecture 2012 Peter Simm Calcium metabolism PTH bone osteoclast (resorption) Ca kidney 1 hydroxylation of Vitamin D Ca absorption from gut 25 OH Vit D Ca from
Disorders of calcium homeostasis FRACP part 1 lecture 2012 Peter Simm Calcium metabolism PTH bone osteoclast (resorption) Ca kidney 1 hydroxylation of Vitamin D Ca absorption from gut 25 OH Vit D Ca from
Case 4 Generalised bone pain
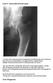 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case Reports. A Rare Cause of Symptomatic Neonatal Hypocalcaemia EKC YAU, AWF CHENG, SY LEE, CB CHOW. Abstract. Key words.
 HK J Paediatr (new series) 2003;8:121-125 Case Reports A Rare Cause of Symptomatic Neonatal Hypocalcaemia EKC YAU, AWF CHENG, SY LEE, CB CHOW Abstract Key words Neonatal hypocalcaemia due to maternal hyperparathyroidism
HK J Paediatr (new series) 2003;8:121-125 Case Reports A Rare Cause of Symptomatic Neonatal Hypocalcaemia EKC YAU, AWF CHENG, SY LEE, CB CHOW Abstract Key words Neonatal hypocalcaemia due to maternal hyperparathyroidism
بسم هللا الرحمن الرحيم. Rickets
 بسم هللا الرحمن الرحيم Rickets 1 Rickets IS defined as failure of mineralization of growing bone or osteoid tissue due to vitamin D deficiency. Vitamin D appear as rickets in children and as oteomalacia
بسم هللا الرحمن الرحيم Rickets 1 Rickets IS defined as failure of mineralization of growing bone or osteoid tissue due to vitamin D deficiency. Vitamin D appear as rickets in children and as oteomalacia
Osteoporosis, Osteomalasia & rickets. Bone disorders
 Osteoporosis, Osteomalasia & rickets Bone disorders Thank You for Your comments Voice--- Ok Lecture too long--- this is in schedule??? More interaction--- I can do that inshalla Slides are crowded--- but
Osteoporosis, Osteomalasia & rickets Bone disorders Thank You for Your comments Voice--- Ok Lecture too long--- this is in schedule??? More interaction--- I can do that inshalla Slides are crowded--- but
Normal Bone Health and Bone Disease. Mr Ryan Trickett Consultant Hand and Wrist Surgeon 6 th February 2017
 Normal Bone Health and Bone Disease Mr Ryan Trickett Consultant Hand and Wrist Surgeon 6 th February 2017 Learning outcomes Understand the structure and function of bone and articular cartilage Explain
Normal Bone Health and Bone Disease Mr Ryan Trickett Consultant Hand and Wrist Surgeon 6 th February 2017 Learning outcomes Understand the structure and function of bone and articular cartilage Explain
BMD: A Continuum of Risk WHO Bone Density Criteria
 Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
OSTEOMALACIA UPDATE. Nothing to Disclose. Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco
 OSTEOMALACIA UPDATE Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco Nothing to Disclose 1 Case History 59 YO WM referred for evaluation of diffuse
OSTEOMALACIA UPDATE Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco Nothing to Disclose 1 Case History 59 YO WM referred for evaluation of diffuse
Hypercalcemia. Hypercalcemia: When to Worry, When to Treat! Mineral Metabolism : A Short Course
 Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Southern Derbyshire Shared Care Pathology Guidelines. Primary Hyperparathyroidism
 Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
LRI Children s Hospital
 Calcium Disorders in Children LRI Children s Hospital Staff relevant to: Medical & Nursing staff caring for Children identified with having a Calcium disorder Team approval date: January 2019 Version:
Calcium Disorders in Children LRI Children s Hospital Staff relevant to: Medical & Nursing staff caring for Children identified with having a Calcium disorder Team approval date: January 2019 Version:
PROTOCOLS. Osteogenesis imperfecta. Principal investigator. Co-investigators. Background
 Osteogenesis imperfecta Principal investigator Leanne M. Ward, MD, FRCPC, paediatric endocrinologist Division of Endocrinology and Metabolism, Children s Hospital of Eastern Ontario, 401 Smyth Rd., Ottawa
Osteogenesis imperfecta Principal investigator Leanne M. Ward, MD, FRCPC, paediatric endocrinologist Division of Endocrinology and Metabolism, Children s Hospital of Eastern Ontario, 401 Smyth Rd., Ottawa
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium Nephrolithiasis and Bone Health. Noah S. Schenkman, MD
 Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Colecalciferol Meda 800 IU tablet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains colecalciferol (vitamin D 3 ) 800 IU
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Colecalciferol Meda 800 IU tablet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains colecalciferol (vitamin D 3 ) 800 IU
David Bruyette, DVM, DACVIM
 VCAwestlaspecialty.com David Bruyette, DVM, DACVIM Disorders of calcium metabolism are common endocrine disorders in both dogs and cats. In this article we present a logical diagnostic approach to patients
VCAwestlaspecialty.com David Bruyette, DVM, DACVIM Disorders of calcium metabolism are common endocrine disorders in both dogs and cats. In this article we present a logical diagnostic approach to patients
An unusual cause of hypocalcemia in a toddler
 An unusual cause of hypocalcemia in a toddler הכנס ה 13 ע"ש ד"ר חנוך האגר ז "ל מרץ 2017 ד"ר שירה לונדון המכון האנדוקריני לילדים, מרכז רפואי העמק, עפולה Case Presentation-History 3 years old male Family:
An unusual cause of hypocalcemia in a toddler הכנס ה 13 ע"ש ד"ר חנוך האגר ז "ל מרץ 2017 ד"ר שירה לונדון המכון האנדוקריני לילדים, מרכז רפואי העמק, עפולה Case Presentation-History 3 years old male Family:
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
The Parathyroid Glands
 The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
MEDICAL POLICY Vitamin D Testing
 POLICY: PG0433 ORIGINAL EFFECTIVE: 05/24/18 LAST REVIEW: MEDICAL POLICY Vitamin D Testing GUIDELINES This policy does not certify benefits or authorization of benefits, which is designated by each individual
POLICY: PG0433 ORIGINAL EFFECTIVE: 05/24/18 LAST REVIEW: MEDICAL POLICY Vitamin D Testing GUIDELINES This policy does not certify benefits or authorization of benefits, which is designated by each individual
Section 7. Metabolic and hematological disorders
 Section 7 Metabolic and hematological disorders 28. Hypocalcemia 29. Hypoglycemia 30. Inborn errors of metabolism 31. Congenital hypothyroidism 32. Bleeding neonate 33. Polycythemia 28 Hypocalcemia Hypocalcemia
Section 7 Metabolic and hematological disorders 28. Hypocalcemia 29. Hypoglycemia 30. Inborn errors of metabolism 31. Congenital hypothyroidism 32. Bleeding neonate 33. Polycythemia 28 Hypocalcemia Hypocalcemia
BIOL 2457 CHAPTER 6 SI 1. irregular ectopic: sutural (Wormian) The is between the shaft and end. It contains cartilage that is
 BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
Inpatient Pediatric Endocrinology. Tala Dajani MD MPH Pediatric Endocrinology of Phoenix
 Inpatient Pediatric Endocrinology Tala Dajani MD MPH Pediatric Endocrinology of Phoenix Objectives Identify calcium disorders in the hospital Distinguish between temporary versus permanent glucose problems
Inpatient Pediatric Endocrinology Tala Dajani MD MPH Pediatric Endocrinology of Phoenix Objectives Identify calcium disorders in the hospital Distinguish between temporary versus permanent glucose problems
Hyper and hypocalcaemia. Prof Tricia Tan
 Hyper and hypocalcaemia Prof Tricia Tan Learning Objectives Basic physiology of Ca regulation Case presentations Take home messages Calcium Total body calcium content ~1300g 99% in bone 1% intracellular
Hyper and hypocalcaemia Prof Tricia Tan Learning Objectives Basic physiology of Ca regulation Case presentations Take home messages Calcium Total body calcium content ~1300g 99% in bone 1% intracellular
Calcium, phosphate & magnesium regulation
 Calcium, phosphate & magnesium regulation Tim Arnett Department of Cell and Developmental Biology University College London Bone composition Treated with hydrochloric acid to dissolve mineral leaves organic
Calcium, phosphate & magnesium regulation Tim Arnett Department of Cell and Developmental Biology University College London Bone composition Treated with hydrochloric acid to dissolve mineral leaves organic
The Role of the Laboratory in Metabolic Bone Disease
 The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
1. Adults; a. Risk factors. b. Who should be tested for vitamin D deficiency? c. Investigations. d. Who do we treat and how do we treat? 2.
 Vitamin D and Bone Health: A Practical Clinical Guideline for Patient Management For Adults and Children Adapted from existing local guidance, National Osteoporosis Society Practical Guides and from Royal
Vitamin D and Bone Health: A Practical Clinical Guideline for Patient Management For Adults and Children Adapted from existing local guidance, National Osteoporosis Society Practical Guides and from Royal
Renal Tubular Acidosis
 1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
Research Article Effects of 1,25-Dihydroxycholecalciferol on Recovery and Resolution of Late Transient Neonatal Hypocalcemia
 Hindawi Publishing Corporation International Journal of Pediatric Endocrinology Volume 2010, Article ID 409670, 5 pages doi:10.1155/2010/409670 Research Article Effects of 1,25-Dihydroxycholecalciferol
Hindawi Publishing Corporation International Journal of Pediatric Endocrinology Volume 2010, Article ID 409670, 5 pages doi:10.1155/2010/409670 Research Article Effects of 1,25-Dihydroxycholecalciferol
Disclosure. Topic Outline. Calcium, Vitamin D, PTH Disorders. PTH/Calcium-Normal Physiology. I have nothing to disclose
 Disclosure Calcium, Vitamin D, PTH Disorders I have nothing to disclose Chienying Liu MD Associate Clinical Professor Division of Endocrinology & Metabolism UCSF Topic Outline Calcium/Vitamin D/PTH physiology
Disclosure Calcium, Vitamin D, PTH Disorders I have nothing to disclose Chienying Liu MD Associate Clinical Professor Division of Endocrinology & Metabolism UCSF Topic Outline Calcium/Vitamin D/PTH physiology
Dr Seeta Durvasula.
 Dr Seeta Durvasula seeta.durvasula@sydney.edu.au 1 Avoid sun skin cancer risk Australia has highest rates of skin cancer in the world Epidemic of Vitamin D deficiency Lack of Vitamin D increases risk of
Dr Seeta Durvasula seeta.durvasula@sydney.edu.au 1 Avoid sun skin cancer risk Australia has highest rates of skin cancer in the world Epidemic of Vitamin D deficiency Lack of Vitamin D increases risk of
DISORDERS OF THE PARATHYROID GLANDS. Mona Fouda Neel MBBS,FRCPEdin.,FACE Professor of medicine and Endocrinology Consultant Endocrinologist
 DISORDERS OF THE PARATHYROID GLANDS Mona Fouda Neel MBBS,FRCPEdin.,FACE Professor of medicine and Endocrinology Consultant Endocrinologist Disorders of the Parathyroid Glands Maintenance of calcium, phosphate
DISORDERS OF THE PARATHYROID GLANDS Mona Fouda Neel MBBS,FRCPEdin.,FACE Professor of medicine and Endocrinology Consultant Endocrinologist Disorders of the Parathyroid Glands Maintenance of calcium, phosphate
Table of Contents Section I Pituitary and Hypothalamus 1. Development of the Pituitary Gland 2. Divisions of the Pituitary Gland and Relationship to
 Table of Contents Section I Pituitary and Hypothalamus 1. Development of the Pituitary Gland 2. Divisions of the Pituitary Gland and Relationship to the Hypothalamus 3. Blood Supply of the Pituitary Gland
Table of Contents Section I Pituitary and Hypothalamus 1. Development of the Pituitary Gland 2. Divisions of the Pituitary Gland and Relationship to the Hypothalamus 3. Blood Supply of the Pituitary Gland
Vitamin D: Is it a superhero??
 Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD
 The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
Drugs Affecting Bone. Rosa McCarty PhD. Department of Pharmacology & Therapeutics
 Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
DISORDERS OF MALE GENITALS
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Factors Affecting Calcium Metabolism in Disorders of the Kidney*
 ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 11, No. 4 Copyright 1981, Institute for Clinical Science, Inc. Factors Affecting Calcium Metabolism in Disorders of the Kidney* MURRAY J. FAVUS, M.D. Departm
ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 11, No. 4 Copyright 1981, Institute for Clinical Science, Inc. Factors Affecting Calcium Metabolism in Disorders of the Kidney* MURRAY J. FAVUS, M.D. Departm
Metabolic Bone Disease (Past, Present and Future Challenges in the Management)
 Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
Agent(s) FDA Labeled Indications Dosage and Administration. Perinatal/Infantile-onset hypophosphatasia. Juvenile-onset hypophosphatasia
 Strensiq (asfotase alfa) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE Agent(s) FDA Labeled Indications Dosage and Administration Strensiq (asfotase alfa) injection Perinatal/Infantile-onset
Strensiq (asfotase alfa) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE Agent(s) FDA Labeled Indications Dosage and Administration Strensiq (asfotase alfa) injection Perinatal/Infantile-onset
Package Insert. D-Bright
 Package Insert D-Bright Product Summary 1. Name of the medicinal product D-Bright 2. Qualitative and quantitative composition Each ml contains Cholecalciferol (Vitamin D3) IP 400 IU in a flavoured syrupy
Package Insert D-Bright Product Summary 1. Name of the medicinal product D-Bright 2. Qualitative and quantitative composition Each ml contains Cholecalciferol (Vitamin D3) IP 400 IU in a flavoured syrupy
Endocrine Quiz / overview. Endocrine Quiz. Pituitary insufficiency. Genetic causes of hypopituitarism. Acquired MPHD Order of hormone loss..
 Endocrine Quiz / overview Michele O Connell Pituitary insufficiency Endocrine Quiz Congenital Causes. Acquired Causes. Genetic causes of hypopituitarism PROP1 POU1F1 (previously called Pit 1) Hesx1 Lhx3/Lhx4.
Endocrine Quiz / overview Michele O Connell Pituitary insufficiency Endocrine Quiz Congenital Causes. Acquired Causes. Genetic causes of hypopituitarism PROP1 POU1F1 (previously called Pit 1) Hesx1 Lhx3/Lhx4.
Rahaf AL-Jafari. Marah Qaddourah. Rahmeh Abdullah. Saleem. 1 P a g e
 15 Rahaf AL-Jafari Marah Qaddourah Rahmeh Abdullah Saleem 1 P a g e If you are following with the record you may notice a little bit difference in information sequences. Hormones that function on growth
15 Rahaf AL-Jafari Marah Qaddourah Rahmeh Abdullah Saleem 1 P a g e If you are following with the record you may notice a little bit difference in information sequences. Hormones that function on growth
CHAPTER 18 - CALCIUM CALCIUM HOMEOSTASIS
 CHAPTER 18 - CALCIUM CALCIUM HOMEOSTASIS CALCIUM BALANCE Normal total plasma Ca++ (bound and free) = 2.1-2.5 mmol/l. Calcium Balance Input Normal diet contains 20-25 mmol calcium of which about half is
CHAPTER 18 - CALCIUM CALCIUM HOMEOSTASIS CALCIUM BALANCE Normal total plasma Ca++ (bound and free) = 2.1-2.5 mmol/l. Calcium Balance Input Normal diet contains 20-25 mmol calcium of which about half is
SUMMARY OF PRODUCT CHARACTERISTICS. A 2.5ml single-dose bottle containing IU Cholecalciferol (equivalent to 625 micrograms vitamin D 3 )
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Fultium 25 000 IU Oral Solution 2 QUALITATIVE AND QUANTITATIVE COMPOSITION A 2.5ml single-dose bottle containing 25 000 IU Cholecalciferol
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Fultium 25 000 IU Oral Solution 2 QUALITATIVE AND QUANTITATIVE COMPOSITION A 2.5ml single-dose bottle containing 25 000 IU Cholecalciferol
Bone Remodeling & Repair Pathologies
 Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION
 DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
Failure to thrive (faltering growth) Dr. Khalid
 Failure to thrive (faltering growth) Dr. Khalid FTT (faltering growth) The term 'failure to thrive' is a clinical state of growth failure due to any causes, characterized by any one or more of the following
Failure to thrive (faltering growth) Dr. Khalid FTT (faltering growth) The term 'failure to thrive' is a clinical state of growth failure due to any causes, characterized by any one or more of the following
Parathyoid glands and PTH
 Parathyoid glands and PTH They are four glands located behind the thyroid gland, each one from (20-50) mg in weight, and composed of two types of cells: 1. Cheif cells: that produces PTH. 2-oxyphil cells:
Parathyoid glands and PTH They are four glands located behind the thyroid gland, each one from (20-50) mg in weight, and composed of two types of cells: 1. Cheif cells: that produces PTH. 2-oxyphil cells:
Notes to/6 4- ( ea/2
 Notes to/6 4- ( 0 1 -. ea/2 PART Two FACTORS AFFECTING BONE DEVELOPMENT & GROWTH Nutrition There must be adequate intake of certain nutrients, such as: 1. Calcium 2. Vitamin C : Necessary for collagen
Notes to/6 4- ( 0 1 -. ea/2 PART Two FACTORS AFFECTING BONE DEVELOPMENT & GROWTH Nutrition There must be adequate intake of certain nutrients, such as: 1. Calcium 2. Vitamin C : Necessary for collagen
Ca, Mg metabolism, bone diseases. Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary
 Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
AACE Southern States Chapter Lecture. Basics
 AACE Southern States Chapter Lecture Unusual Bone Cases Basics Osteoporosis Osteomalacia Renal Osteodystrophy Multiple Myeloma 1 Osteoporosis Definition Modeling, Bone Remodeling Bone Resorption > Bone
AACE Southern States Chapter Lecture Unusual Bone Cases Basics Osteoporosis Osteomalacia Renal Osteodystrophy Multiple Myeloma 1 Osteoporosis Definition Modeling, Bone Remodeling Bone Resorption > Bone
Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD
 Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD Reprinted with permission from: E-Medicine: Instant Access to the Minds of Medicine http://www.emedicine.com/emerg/topic276.htm
Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD Reprinted with permission from: E-Medicine: Instant Access to the Minds of Medicine http://www.emedicine.com/emerg/topic276.htm
CKD-Mineral Bone Disorder (MBD) Pathogenesis of Metabolic Bone Disease. Grants: NIH, Abbott, Amgen, OPKO, Shire
 Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Osteoporosis. When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of.
 Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
X-linked hypophosphatemic rickets across the lifespan
 X-linked hypophosphatemic rickets across the lifespan AACE Midwest Regional Meeting Erik A. Imel, M.D. Associate Professor of Medicine and Pediatrics Indiana Center for Musculoskeletal Health July 28,
X-linked hypophosphatemic rickets across the lifespan AACE Midwest Regional Meeting Erik A. Imel, M.D. Associate Professor of Medicine and Pediatrics Indiana Center for Musculoskeletal Health July 28,
X-linked hypophosphatemic rickets across the lifespan
 X-linked hypophosphatemic rickets across the lifespan AACE Midwest Regional Meeting Erik A. Imel, M.D. Associate Professor of Medicine and Pediatrics Indiana Center for Musculoskeletal Health July 28,
X-linked hypophosphatemic rickets across the lifespan AACE Midwest Regional Meeting Erik A. Imel, M.D. Associate Professor of Medicine and Pediatrics Indiana Center for Musculoskeletal Health July 28,
Approach to hypophosphataemia
 Approach to hypophosphataemia A/Prof Roderick Clifton-Bligh Kolling Institute of Medical Research, University of Sydney Department of Endocrinology Royal North Shore Hospital, St Leonards, NSW Royal North
Approach to hypophosphataemia A/Prof Roderick Clifton-Bligh Kolling Institute of Medical Research, University of Sydney Department of Endocrinology Royal North Shore Hospital, St Leonards, NSW Royal North
Safety Profile of Viread and Truvada. Ian McGowan, MD PhD FRCP Cape Town MTN Regional Meeting September, 2008
 Safety Profile of Viread and Truvada Ian McGowan, MD PhD FRCP Cape Town MTN Regional Meeting September, 2008 Overview Safety assessment in drug development Physiology 101 Renal Bone Liver Safety profile
Safety Profile of Viread and Truvada Ian McGowan, MD PhD FRCP Cape Town MTN Regional Meeting September, 2008 Overview Safety assessment in drug development Physiology 101 Renal Bone Liver Safety profile
GLOSSARY OF TERMS. produced in response to an antigen to bond with and neutralize that antigen / the body's way of destroying foreign invaders
 TERM 24-hour urine acidosis acquired aemia (prefix) albumin alkalosis anemia antibodies antigen autocrine autoimmune basal ganglion bone turnover calcilytic calcimimetic calcitonin Calcitriol Calcium carbonate
TERM 24-hour urine acidosis acquired aemia (prefix) albumin alkalosis anemia antibodies antigen autocrine autoimmune basal ganglion bone turnover calcilytic calcimimetic calcitonin Calcitriol Calcium carbonate
Metabolic, Endocrine, and Hematologic disease 주선영 가톨릭대학교인천성모병원
 Metabolic, Endocrine, and Hematologic disease 주선영 가톨릭대학교인천성모병원 1 Metabolic disease Ca, P metabolism Vit D metabolism Rickets Nutritional Hypophosphatemic Renal osteodystrophy Hypophosphatasia Hypervitaminosis
Metabolic, Endocrine, and Hematologic disease 주선영 가톨릭대학교인천성모병원 1 Metabolic disease Ca, P metabolism Vit D metabolism Rickets Nutritional Hypophosphatemic Renal osteodystrophy Hypophosphatasia Hypervitaminosis
SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over 3 Weeks. A SEPARATE WORKSHEET WILL BE PROVIDED.
 BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE
 HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
25/10/56. Hypothyroidism Myxedema in adults Cretinism congenital deficiency of thyroid hormone Hashimoto thyroiditis. Simple goiter (nontoxic goiter)
 THERAPEUTIC USES OF THYROID HORMONE Supeecha Wittayalertpunya Wannarasmi Ketchart Nov 2013 Hyperthyroidism (Thyrotoxicosis) Grave s disease (diffuse toxic goiter) Toxic uninodular & Toxic multinodular
THERAPEUTIC USES OF THYROID HORMONE Supeecha Wittayalertpunya Wannarasmi Ketchart Nov 2013 Hyperthyroidism (Thyrotoxicosis) Grave s disease (diffuse toxic goiter) Toxic uninodular & Toxic multinodular
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS. BY: Shifaa Qa qa
 NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: testing_serum_vitamin_d_levels 9/2015 2/2017 2/2018 2/2017 Description of Procedure or Service Vitamin D,
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: testing_serum_vitamin_d_levels 9/2015 2/2017 2/2018 2/2017 Description of Procedure or Service Vitamin D,
The Parathyroid Glands Secrete Parathyroid Hormone, which Regulates Calcium, Magnesium, and Phosphate Ion Levels
 17.6 The Parathyroid Glands Secrete Parathyroid Hormone, which Regulates Calcium, Magnesium, and Phosphate Ion Levels Partially embedded in the posterior surface of the lateral lobes of the thyroid gland
17.6 The Parathyroid Glands Secrete Parathyroid Hormone, which Regulates Calcium, Magnesium, and Phosphate Ion Levels Partially embedded in the posterior surface of the lateral lobes of the thyroid gland
HYPERCALCAEMIA 101 FOR THE INTERNIST
 HYPERCALCAEMIA 101 FOR THE INTERNIST Dr Chionh Siok Bee Dept of Medicine, National University Hospital siok_bee_chionh@nuhs.edu.sg Medicine Review Course 18/09/2011 Outline of Talk Definition of hypercalcaemia
HYPERCALCAEMIA 101 FOR THE INTERNIST Dr Chionh Siok Bee Dept of Medicine, National University Hospital siok_bee_chionh@nuhs.edu.sg Medicine Review Course 18/09/2011 Outline of Talk Definition of hypercalcaemia
BONE REMODELLING. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
