Osteoarthritis of the Knee:
|
|
|
- Jeffery Baldwin
- 6 years ago
- Views:
Transcription
1 799 Osteoarthritis of the Knee: Comparison of Radiography, CT, and MR Imaging to Assess Extent and Severity Wing P. Chan1 Although conventional radiography is the method most frequently used for monitoring Philipp Lang1 progression of osteoarthritis, it may not show osteoarthritic changes of the knee until Michael P. Stevens2 late in the disease, and it may show involvement of only one or two compartments in Kenneth Sack2 patients who have tricompartmental disease. We compared radiography, CT, and MR Sharmila Maumdar1 imaging for assessing the extent and severity of osteoarthritis of the knee in 20 patients. r 1-i %Al Cf II 1 Radiography included posteroantenor weight-bearing, true lateral, and sunrise patellar avk vv. Louuer projections. Axial CT scans were reformatted in sagittal and coronal planes. MR imaging Chrlsta Basch consisted of spin-echo ( /20; 2000/60, 120 [TR/TE]), and gradient-echo (600/ Harry K. Genant 30, 0 = 30#{176}) sequences. The severity of osteoarthntic changes was graded from 0 to 3. MR frequently showed tricompartmental cartilage loss when radiography and CT showed only bicompartmental involvement in the medial and patellofemoral compartments. In the lateral compartment, MR showed a higher prevalence of cartilage loss (60%) than radiography (35%) and CT (25%) did. In the medial compartment, CT and MR showed osteophytes in 100% of the knees, whereas radiography showed osteophytes in only 60%. Notably, radiography often failed to show osteophytes in the posterior medial femoral condyle. On MR images, meniscal degeneration or tears were found in all 20 knees studied. Partial and complete tears of the anterior cruciate ligament were found in three and seven patients, respectively. MR is more sensitive than radiography and CT for assessing the extent and severity of osteoarthritic changes and frequently shows tricompartmental disease in patients in whom radiography and CT show only bicompartmental involvement. MR imaging is unique for evaluating meniscal and ligamentous disease related to osteoarthntis. AJR 157: , October 1991 Osteoarthritis frequently affects the knee and can cause profound changes in the surrounding bone and soft tissues. These changes include cartilage loss, subchondral sclerosis, osteophytosis, subchondral cysts, and meniscal degeneration [1-5]. Radiographs can show osteoarthritic changes of the bone; however, soft-tissue involvement may not be appreciated. CT is superior to conventional February. 20, ; accepted.. after. re- radiography osseous changes. because it provides a tomographic assessment of soft-tissue and Department of Radiology, University of Califor nia, San Francisco, 505 Parnassus Ave., San Fran- MR imaging has direct multiplanar imaging capability and provides a higher softcisco, CA Address reprint requests to H. K. tissue contrast than CT does. MR imaging is established as a noninvasive tool for Genant. evaluating pathologic changes in the articular cartilage, menisci, and ligaments of 2 Department of Medicine, University of Califor- the knee [6-13] nia, San Francisco, 505 Parnassus Ave., San Fran-.... cisco, CA In this study, we compared radiography, CT, and MR imaging for assessing the 3 Syntex Laboratories, Inc., 3401 Hillview Ave., extent and severity of osteoarthritis of the knee. Twenty consecutive patients with Palo Alto, CA osteoarthritis of the knee were examined prospectively with radiography, CT, and X/91/ MR imaging. The severity of the osteoarthritic changes was graded for each American Roentgen Ray Society imaging technique.
2 800 CHAN ET AL. AJA:157, October 1991 Materials and Methods Selection of Patients Twenty patients (1 1 women and nine men), 42 to 73 years old (mean, 58 years), with clinical and radiologic evidence of osteoarthritis of the knee were studied prospectively as part of a clinical drug trial to monitor the effects of nonsteroidal antiinflammatory drug therapy on osteoarthritis. In each patient, one knee was evaluated with radiography, CT, and MR imaging. A requirement for inclusion in the study was that patients had knee pain and knee joint effusion for at least 1 month. For patients with bilateral disease, the knee clinically determined to have the most severe disease was selected for study. Imaging Techniques Radiography of the knee consisted of posteroantenor weightbearing, true lateral non-weight-bearing, and sunrise patellar projections [1, 2, 1 4]. Posteroanterior weight-bearing radiographs were obtained with the knee in 20#{176} flexion to orient the tibial plateau orthogonal to the X-ray beam. Axial CT was performed with a GE CT/T 9800 unit. We used a scanning time of 2 sec, 1 40 kvp, 70 ma, and a vertical gantry. A 34.5-cm field of view (FOV) with a 512 x 51 2 matrix was used. Slice thickness was 3 mm. Scans were obtained contiguously. The patient was supine, with both extremities parallel and the ankles and the knees taped together. The knees were placed in 30#{176} flexion [5]. Images were reformatted in sagittal and coronal planes by using a slice thickness of 3 mm with no interslice gap. MR imaging was performed on a 1.5-T Signa system (General Electric, Milwaukee, WI) with a transmit-and-receive extremity coil. A spin-echo sequence was used to obtain images in three orthogonal planes. Repetition time (TR) varied from 600 to 800 msec, and echo time (TE) was 20 msec for all three planes. Axial images were generated also by using a spin-echo technique with a TR of 2000 msec and TEs of 60 and 120 msec. Additionally, gradient-echo images were obtained with a TA of 600 msec, a TE of 30 msec, and a flip angle 0 of 30#{176} in axial and sagittal planes. For all cases, the slice thickness was 5 mm, the image matrix varied from 256 x 192 to 256 x 256, and FOV ranged from 14 to 16 cm. Spin-echo and gradient-echo images were acquired with two excitations. The interval between radiography, CT, and MR did not exceed 2 weeks for any of the patients. Interpretation of the Images Image analysis included evaluation of four diagnostic parameters: cartilage loss, subchondral sclerosis, osteophytes, and subchondral cysts. MR also was used to evaluate the menisci and ligaments. The extent of the disease was evaluated separately for the medial, lateral, and patellofemoral compartments. The severity of the osteoarthritic changes of the knee was graded from 0 to 3. The seventy of cartilage loss was judged as 0 = normal; 1 = mild, or 1-33% decrease in cartilage thickness; 2 = moderate, or 34-66% decrease in cartilage thickness; and 3 = severe, or % decrease in cartilage thickness. Subchondral sclerosis was noted as 0 = absent; 1 = mild, or localized ebumation (or mild localized signal reduction on MR); 2 = moderate increase in density (or moderate localized signal reduction on MR); 3 = severe, widespread sclerosis (or severe extensive signal reduction on MR) [2]. Osteophytes were graded as 0 = absent; 1 = small beaklike osteophyte; 2 = intermediate-size osteophyte, between those of grades 1 and 3; 3 = proliferative or mushroomlike osteophyte [1 5]. Subchondral cysts were evaluated as 0 = absent; 1 = one to two small cysts; 2 = single large or multiple small cysts; or 3 = many large cysts [2]. In the event of nonuniform involvement of a single compartment, the most severe degree of change was used for grading. Meniscal changes were graded by MR as 0 = no tear; 1 = focal or globular intrasubstance increased signal intensity that did not extend to the articular surface; 2 = horizontal, linear intrasubstance increased signal intensity that extended from periphery of the meniscus but did not involve an articular surface; and 3 = increased signal intensity communicating or extending to at least one articular surface [7]. Ligamental changes were evaluated as no tear, partial tear, and complete tear. All images were assessed in a joint reading by three of the authors, and a consensus interpretation was reached. Twenty sets of radiographs; axial and reformatted coronal and sagittal CT scans; and axial, coronal, and sagittal MR images were interpreted in random patient sequence. First, 20 sets of radiographicfilms were interpreted, and the scoring forms were collected by another author. After 2 weeks, 20 sets of CT films were interpreted by the same readers. The readers had no knowledge of the radiographic scoring forms. Two weeks after the CT evaluation, MR images were interpreted by using the same method. Statistical Analysis Rank-order correlations were calculated by using Kendall s tau (r) for pairwise combinations: radiography vs CT, radiography vs MR, CT vs MR. Four diagnostic parameters were compared among the techniques. Kendall s correlation coefficients (r) were corrected for ties before the p values were obtained [1 6]. The null hypothesis was rejected at the 95% or 99% confidence level, and p values of.05 or less and.01 or less, respectively, were considered significant. Results Cartilage Loss Bicompartmental cartilage loss was seen frequently on radiographs (1 2 knees) and on CT (1 4 knees). On MR, however, tricompartmental cartilage loss predominated (nine knees)(fig. 1). This discrepancy was caused by cartilage loss in the lateral compartment, which was detected by MR imaging but not by radiography and CT (Fig. 1). In the medial compartment, the occurrence rate of grade 3 cartilage loss was higher on both radiography and MR (nine knees, 45%, each) than on CT (three knees, 1 5%; Table 1). In the lateral compartment, the overall occurrence rate of cartilage loss on MR (1 2 knees, 60%) was markedly greater than that on radiography (seven knees, 35%) and CT (five knees, 25%; Fig. 2). In the patellofemoral compartment, all techniques showed a similar occurrence rate and severity of cartilage loss (Table 1, Fig. 3). The correlation between radiography and CT reached statistical significance in the lateral (r , p.0003) and patellofemoral (r = , p.0007) compartments. Similarly, in the lateral and patellofemoral compartments, correlation between CT and MR was also significant (r , p =.0222 and r , p.01 4, respectively), although it was not as strong as that between radiography and CT. The correlation between radiography and MR was statistically significant in the medial (r , p.0001) and lateral compartments (r = , p.0136).
3 AJR:157, October1991 OSTEOARTHRITIS OF KNEE 801 Radiography CT Cartilage M L M L M L (;7\\ K) knees without subchondral cyars) Subchondrai loss MR without cartilage PF loss ) PF Osteophtes Subchondrai sclerosis cysts knees knees without 1 without subchondral subchondrul cysts ) cysts Fig. 1.-Compartmental distribution of changes in knee as determined by radiography, CT, and MR in 20 patients with osteoarthritis of the knee. Overlapping portions of circles indicate number of knees in which more than one compartment was abnormal. Note that for cartilage loss, MR imaging frequently shows tricompartmental involvement when radiography and CT show primarily bicompartmentai disease. Similarly, in detecting osteophytes, both CT and MR show tricompartmental involvement more often than radiography does. Unicompartmentai distribution predominates for both subchondral sclerosis and subchondrai cysts. M = medial compartment, L = lateral compartment, PF = pateilofemorai compartment. Fig. 2.-A, Conventional radiograph of knee shows mild widening of joint space in lateral compartment (arrows). B, MR image (SE 600/20) shows focal grade 3 cartilage defect in lateral compartment (arrow). Note that width of joint space in A does not provide accurate information on cartilage loss. A Subchondral B Sclerosis Unicompartmental subchondral sclerosis was seen frequently on radiography (1 0 knees), CT (1 1 knees), and MR (1 2 knees; Figs. 1 and 4). In the medial and lateral compartments, both radiography and CT showed a higher occurrence rate of subchondral sclerosis than MR did. In the patellofemoral compartment, subchondral sclerosis was observed more frequently on MR (1 3 knees, 65%) than on radiography (nine knees, 45%) and on CT (nine knees, 45%; Table 1). The correlation between radiography and CT, radiography and MR, and CT and MR was statistically significant (p.05) for subchondral sclerosis in all compartments. Osteophytes With radiography, both bicompartmental and tricompartmental osteophytosis was observed frequently (eight knees). With CT and MR imaging, however, tricompartmental osteophytosis predominated (1 6 and 1 5 knees, respectively; Figs. 1 and 5). In the medial compartment, both CT and MR showed a markedly higher occurrence rate (20 knees, 1 00%) of osteophytes than radiography did (1 2 knees, 60%). In the lateral compartment, the occurrence rate of osteophytes on CT and MR (1 7 knees, 85%) was also greater than on radiography (1 2 knees, 60%). In the patellofemoral compartment, however, radiography showed a higher occurrence rate (1 9 knees, 95%) of osteophytes than CT (1 6 knees, 80%) and MR (15 knees, 75%) did (Table 1). The correlation between radiography and CT, radiography and MR, and CT and MR was statistically significant (p.05) for osteophytes in all compartments. Subchondral Cysts Unicompartmental formation of subchondral cysts was observed frequently on radiography (four knees), CT (eight knees), and MR (1 2 knees; Fig. 1). In all compartments, both CT and MR showed a higher occurrence rate of subchondral cysts than radiography did (Table 1, Fig. 6). The correlation between CT and MR was statistically significant for subchondral cysts in the medial (r , p.0001 ) and the patellofemoral compartments (r , p =.0001).
4 802 CHAN ET AL. AJR:157, October 1991 TABLE 1: Occurrence Rates and Severity of Osteoarthntic Changes on Radiographs (RG), CT Scans, and MR Images of the Knee in 20 Patients Grade RG M edial CT MR AG Lateral CT MA Pate Ilofem oral Cartilage loss Subchondral sclerosis Osteophytes Subchondral cysts RG CT MR Meniscal Abnormalities In the anterior horn of the medial meniscus, MR showed grade 1 meniscal pathologic changes in three patients, grade 2 changes in one, and grade 3 changes in 16. In the posterior horn of the medial meniscus, grade 1 changes were seen in one knee and grade 3 changes in 1 9 knees (Fig. 7). In the lateral meniscus, grade 1, 2, and 3 changes in the anterior horn were shown in four, six, and 1 0 knees, respectively. In the posterior horn of the lateral meniscus, grade 1 changes were shown in two knees, grade 2 changes in three, and grade 3 changes in 15. Ligamentous Changes For the anterior cruciate ligament, MR showed no tears in 1 0 knees, partial tears in three, and complete tears in seven. For the posterior cruciate ligament, partial tears were found in two knees and a complete tear in one knee. No tears were detected in the medial or lateral collateral ligaments. Discussion Osteoarthritis is characterized pathologically by cartilage loss, subchondral sclerosis and cyst formation, and osteo- Fig. 3.-A, Conventional radiograph (sunrise pateilar projection) of knee does not show joint-space narrowing in patellofemoral compartment. Note incidental small, radiolucent area at apex of patella (arrow). B, Axial CT scan shows thickness of cartilage is difficult to evaluate on CT. Note small cyst at patellar apex (arrow). C and D, Ti-weighted (C, SE 600/ 20) and T2-weighted (D, SE 2000/60) MR images. On T2-weighting (D), cartilage denudation and grade 3 cartilage loss at pateilar apex are shown (arrow), which cannot be detected on radiography and CT. Note, small cyst at pateliar apex is seen as low-intensity area on Ti-weighted image (arrows in C).
5 AJR:157, October 1991 OSTEOARTHRITIS OF KNEE 803 Fig. 4.-A, Conventional radiograph shows subchondral sclerosis, narrowing of joint space, and osteophytosis. B, MR image (SE 600/20) shows subchondrai sclerosis as an area of low signal intensity (arrow) in medial compartment extending into high-signal-intensity marrow space. Fig. 5.-A, Conventional radiograph shows formation of osteophytes (arrows) in medial and lateral compartments. B, CT scan shows marked osteophytosis in both medial and lateral compartments. Osteophytosis is particularly accentuated in posterior femoral condyles. C, MR image (SE 600/20) confirms advanced osteophytosis in medial and lateral femoral condyles and in tibial plateau (thick arrows). Note beaklike intercondylar osteophyte (thin arrow) at medial femoral condyle, which was not detected by radiography. phytosis [1-5]. Radiography has been the primary method for monitoring the progression of these changes in the knee [1 7]. Unfortunately, osteoarthritic changes may not be detected on radiographs until late in the disease. The use of radiography is limited in clinical drug trials designed to assess the influence of therapies on the progression of osteoarthritis. Similar to previous animal studies [3], the results of our in vivo investigation in humans indicate that MR imaging is more sensitive than radiography and CT for detecting osteoarthritic joint changes and is unique for assessing soft-tissue changes related to osteoarthritis. Cartilage Cartilage loss appeared frequently and to a severe degree in the medial compartment (Table 1 ). The occurrence rate of grade 3 medial cartilage loss was markedly lower on CT than that observed on radiography and MR (Table 1). With radiography, cartilage is assessed indirectly by evaluating the width of the joint space on weight-bearing projections [1, 2, 14]. With MR, the cartilage is evaluated directly. Cartilage appears as an intermediate to high-signal-intensity line next to the lowintensity subchondral bone [3, 1 2, 1 3]. CT does not provide a direct assessment of cartilage [1 8] because soft-tissue contrast is not as great as that seen on MR. CT also is limited in the accurate evaluation of the width of the joint space as an indirect sign of cartilage thickness because the patient is not in weight-bearing position during the study. These differences may explain the lower sensitivity of CT compared with radiography and MR in detecting cartilage loss. In the lateral compartment, MR was more sensitive than radiography or CT in showing cartilage loss (Table 1). Our MR findings correspond with pathologic studies that report abnormal cartilage not only in the medial but also in the lateral compartments of the knees of patients with osteoarthritis [1, 2]. Radiography primarily detects cartilage loss in the medial compartment. This may be because cartilage loss in the medial compartment causes the lateral joint space to open 1-2 mm as weight is shifted medially [1 4]. Joint-space widening in the lateral compartment as seen on radiographs, therefore, does not necessarily reflect the actual thickness of the cartilage (Fig. 2). This may account for the lower frequency and severity of cartilage loss in the lateral compartment
6 804 CHAN ET AL. AJA:1 57, October 1991 Fig. 6.-A, Conventional radiograph does not show any signs of subchondral cyst formation. B, CT scan shows a small subchondral cyst (arrow) in medial femoral condyle, which is surrounded by a thin sclerotic halo. C, On T2-weighted gradient-echo MR image (600/30/300), subchondral cyst (arrow) has high signal intensity. Cyst can be differentiated easily from surrounding normal marrow, which has low signal intensity. Fig. 7.-MR image (SE 600/20) shows marked osteophytosis (straight arrows) and subchondral sclerosis (arrowhead) corresponding to osteoarthritic changes. Posterior horn of medial meniscus has a grade 3 tear with macoration (curved arrow). discernible on radiography, and it also may explain the higher occurrence rate of tricompartmental cartilage loss on MR compared with radiography (Fig. 1). Detection of cartilage loss in the lateral compartment on MR imaging may have a direct impact on surgical treatment. Among patients in whom radiography showed cartilage loss only in the medial compartment, a unicompartmental prosthetic device has been used in many centers for surgical treatment [1 9]. However, when cartilage loss is detected in both the medial and lateral compartments on MR imaging, a total knee joint prosthesis appears preferable [20]. Subchondral Sclerosis Radiography and CT show subchondral sclerosis as areas of increased density and attenuation. On MR, these areas of increased bone density have low signal intensity on all sequences because of the lack of resonating protons. Because both subchondral sclerosis and subchondral bone are characterized by low signal intensity, delineation of sclerotic regions that were located immediately adjacent to the subchondral bone was sometimes difficult on MR. This may explain why MR had less sensitivity than radiography and CT in detecting early grade 1 subchondral sclerosis (Table 1). However, once sclerotic areas extended deeper from the joint margin into the high-signal-intensity marrow cavity on Ti - weighted images, detection was facilitated on MR (Fig. 4). Because marrow fat has a short Ti -relaxation time and resultant high signal intensity on short TR/TE sequences, detection of low-intensity sclerotic areas within the bone marrow was best on these imaging sequences. In the patellofemoral compartment, radiography and CT were limited for assessing subchondral sclerosis. Osteophytes that project over the patellofemoral compartment and overlapping parts of the patella and femur may make radiographic evaluation of this area difficult [1]. Osteophytes Osteophytosis is thought to be a reparative response associated with early osteoarthritis [5]. Osteophytes were the most prevalent CT and MR abnormalities. This suggests that osteophytosis is a valuable diagnostic sign for osteoarthritis of the knee. Osteophytes were not detected on radiographs in eight knees (40%) in the medial compartment and in eight knees (40%) in the lateral compartment. In many cases, osteophytes were overlapped by adjacent anterior and postenor bony Structures evident on radiographs (Fig. 5).
7 AJA:157, October 1991 OSTEOARTHRITIS OF KNEE 805 Osteophytosis appeared frequently and to a severe degree in the posterior femoral condyle of the medial compartment. When osteophytes were present in only one condyle, it was almost always the posterior medial femoral condyle. This suggests that osteophytosis of the knee may begin at this site [1 5]. A small osteophyte in that location usually remains undetected on radiography, but it is detected easily on transaxial CT and MR (Fig. 5), indicating that tomographic, thinsection imaging techniques with multiplanar imaging capability significantly improve the diagnostic sensitivity. Interestingly, in the patellofemoral compartment, CT and MR were less sensitive than radiography (Table 1 ). On radiography, the lateral projection provided more information for detecting osteophytes than the sunrise patellar projection did. Osteophytes usually were found in the superior and inferior margins of the patellar facets on lateral radiographs. Sagittal CT reformations and sagittal MR images were difficult to evaluate for the presence of osteophytes in the patella. This may be due to the lower spatial resolution of CT in the reformatted sagittal plane as compared with the original axial plane. In addition, a prominent partial volume effect in the sagittal plane on both CT and MR may contribute to the difficulties Subchondral in interpretation. Cysts Subchondral cysts result from focal bone resorption in an area of high intraarticular pressure that is frequently associated with cartilage loss [5]. In all imaging techniques, subchondral cysts were shown most often in the medial compartment (Table i). On radiographs, subchondral cysts frequently were missed. This may be related to local osteopenia or sparse trabeculae producing radiolucent areas below the articular surface and thereby obscuring the cysts. Many small subchondral cysts were detected by CT and MR because of the techniques tomographic nature and multiplanar imaging capability. The value of MR imaging was enhanced further by using T2*weighted gradient-echo sequences (Fig. 6). Subchondral cysts showed high signal intensity when these pulse Sequences were used, and differentiation from adjacent lowsignal-intensity normal marrow and subchondral bone was good (Fig. 6). The high signal intensity of subchondral cysts on this imaging sequence may be caused by joint fluid filling the defect. The low signal intensity of the surrounding normal marrow may be related to inhomogeneous magnetic susceptibility at the interface of bone marrow and trabecular bone [21]. In some cases, MR showed the synovial fluid tract leading to the cysts (Fig. 6). This correlates with the hypothesis by Freund that intrusion of synovial fluid is an important pathogenetic factor in the formation of subchondral cysts [5]. Meniscal Abnormalities MR showed a high prevalence of meniscal degeneration (Fig. 7) in osteoarthritis, similar to findings in earlier animal studies [3]. This suggests a strong relationship between meniscal abnormalities and degenerative joint disease. In the standing adult, the weight-bearing line normally passes from the center of femoral head through the center of both knees and ankles. Any condition that leads to angular deformity will result in a shift of force per unit area in the knee [5]. A varus angulation of the knee, for example, will increase the weightbearing load across the medial compartment, thereby intensifying the biomechanical stress on the cartilage there [1, 5]. In our study, degeneration of the medial meniscus was seen more often than lateral meniscal degeneration. This may explain the frequent finding of varus deformity seen in osteoarthritis of the knee. Further studies including pathologicanatomic correlation are needed to determine whether meniscal degeneration is (1) the underlying pathogenetic principle of osteoarthritis or (2) a result of changes in the joint related to osteoarthritis. Ligaments The prevalence of tears of the anterior cruciate ligament (1 0 knees) on MR imaging was greater than that of tears of the posterior cruciate ligament (three knees). Tears and resultant insufficiency of the anterior cruciate ligament are known to cause osteoarthritic changes in the affected knee [22]. Anterior cruciate ligament tears frequently were associated with medial compartmental disease. This association may result from increased mechanical stresses in the medial compartment of the unstable knee. Study Limitations Our investigation was limited by the relatively small number of patients. Study of larger populations is desirable to determine the prevalence of osteoarthritic changes for each technique more precisely. Arthroscopic or surgical confirmation of the imaging results was not available in any of the patients. The high diagnostic yield of MR imaging in detecting osteoarthritic changes may be limited, therefore, by false-positive and false-negative results that cannot be reliably excluded in the absence of a gold standard. However, surgery and arthroscopy could not be performed in our volunteer subjects because of the invasiveness of the procedures. In addition, surgery and arthroscopy can be used as a gold standard for cartilage loss, osteophytosis, and meniscal and ligamentous disorders only. Subchondral cysts and subchondral sclerosis as well as grade 1 and 2 meniscal degeneration cannot be detected arthroscopically and surgically. With respect to cartilage loss and soft-tissue changes, previous studies have emphasized the high correlation between MR and arthroscopy [3, 6-8, 11-13]. Our data may overestimate the sensitivity of radiography for detecting osteoarthritic changes, because patients were selected on the basis of both clinical and radiologic findings. However, the clinician responsible for the selection of patients was not involved in the interpretation of the different imaging studies. The sensitivity of radiography in detecting intercondylar changes, in turn, may be improved when tunnel views are added. In general, better results on radiographs can be
8 806 CHAN ET AL. AJR:157, October 1991 expected when additional projections are obtained to supplement the standard views. Conclusions On the basis of this preliminary cross-sectional investigation, MR imaging is more sensitive than conventional radiography and CT in showing the joint changes caused by osteoarthritis. We conclude the following: (1) MR frequently detects tricompartmental disease when radiography and CT show only bicompartmental involvement. (2) The finding of normaljoint spaces on radiographs does not exclude cartilage loss, which can be shown by MR. (3) Osteoarthritis frequently is associated with meniscal pathologic changes and tears of the anterior cruciate ligament. Both may be contributing causes of osteoarthritis. MR imaging is the only noninvasive diagnostic tool that can be used to evaluate meniscal and ligamentous abnormalities related to osteoarthritis. (4) MR is a sensitive tool for detecting early osteoarthritic changes. MR appears to be particularly useful for noninvasive longitudinal monitoring of osteoarthritis in studies that assess the efficacy of treatments for osteoarthritis. REFERENCES 1. Ahlback S. Osteoarthritis of the knee: a radiographic investigation. Acta Radiol Suppl (Stockh) 1968:277: Thomas RH, Aesnick D, Alazraki NP, Daniel D, Greenfield A. Compartmental evaluation of osteoarthritis of the knee: comparative study of available diagnostic modalities. Radiology 1975:116: Sabiston CP, Adams ME, Li DKB. Magnetic resonance imaging of osteoarthritis: correlation with gross pathology using an experimental model. J Orthop Res 1987;5: Pataki A, Fries A, Ochsner K, Witzemann E. Qualitative radiographic diagnosis of osteoarthritis of the knee joint in the C57BL mouse. Agents Actions 1987:22: Aesnick D, Niwayama G. Degenerative disease. In: Aesnick D, Niwayama G, eds. Diagnosis of bone and joint disorders, 2nd ed. Philadelphia: Saunders, 1988: Braunstein EM, Grandt KD, Albrecht M. MAI demonstration of hypertrophic articular cartilage repair in osteoarthritis. Ske!eta!Radio! 1990:19: Stoller DW, Martin C, Crues JV Ill, Kaplan L, Mink JH. Meniscal tears: pathologic correlation with MA imaging. Radiology 1987:164: Crues JV ill, Mink JH, Levy TL, Lotysch M, Stoller DW. Meniscal tears of the knee: accuracy of MA imaging of the knee: first 144 cases. Radiology 1987:164: Aeicher MA, Aauschning W, Gold RH, et al. Magnetic resonance imaging of the knee joint. Clinical update I. Injuries to menisci, patellar tendon and cruciate ligaments. Radiology 1987:162: Mink JH, Levy T, Crues JV lii. Tears of the anterior cruciate ligament and menisci of the knee: MR imaging evaluation. Radiology 1988:167: Lee JK, Yao L, Phelps CT, et al. Anterior cruciate ligament tears: MA imaging compared with arthroscopy and clinical tests. Radiology 1988:166: Konig H, Sauter A, Deimling M, Vogt M. Cartilage disorders: comparison of spin-echo CHESS, and FLASH sequence MA images. Radiology 1987:164: Aeiser MF, Bongartz G, Erlemann A, et al. Magnetic resonance in cartilaginous lesions of the knee joint with three-dimensional gradient-echo imaging. Skeletal Radio! 1988;17: Leach RE, Gregg T, Siber FJ. Weighted-bearing radiography in osteoarthritis of the knee. Radiology 1970:97: Kindynis P, HaIler J. Kang HS, et al. Osteophytosis of the knee: anatomic, radiographic, and pathologic investigation. Radiology 1990;1 74: Kendall MG, Stuart A. The advanced theory of statistics, vol 2. New York: Hafner, 1967: Altman AD, Fries JF, Gloch DA, et al. Radiographic assessment of progression in osteoarthritis. Arthritis Rheum 1987:30: Hemandez AJ, Poznanski AK. CT evaluation of pediatric hip disorders. Orthop C/in North Am 1985:16: Macintosh DL. Hemiarthroplasty of the knee using a space occupying prosthesis for painful varus and valgus deformities. J Bone Joint Surg [Br] 1958:48-B: Goldberg VM, Figgie MP, Figgie HE Ill, Heiple KG, Sobel M. Use of a total condylar knee prosthesis for treatment of osteoarthritis and rheumatoid arthritis. J Bone Joint Surg [Am] 1988;70-A: Davis CA, Genant HK, Dunham JS. The effects of bone on proton NMA relaxation times of surrounding liquids. Invest Radiol 1986:21 : Kannus P, Jarvinen M. Posttraumatic anterior cruciate ligament insufticiency as a cause of osteoarthntis in a knee joint. C/in Rheumatol 1989:8:
MR imaging of the knee in marathon runners before and after competition
 Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Meniscal Tears: Role of Axial MRI Alone and in Combination with Other Imaging Planes
 Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Arthrographic study of the rheumatoid knee.
 Annals of the Rheumatic Diseases, 1981, 40, 344-349 Arthrographic study of the rheumatoid knee. Part 2. Articular cartilage and menisci KYOSUKE FUJIKAWA, YOSHINORI TANAKA, TSUNEYO MATSUBAYASHI, AND FUJIO
Annals of the Rheumatic Diseases, 1981, 40, 344-349 Arthrographic study of the rheumatoid knee. Part 2. Articular cartilage and menisci KYOSUKE FUJIKAWA, YOSHINORI TANAKA, TSUNEYO MATSUBAYASHI, AND FUJIO
Arthritis & Rheumatism
 ~ Arthritis & Rheumatism Official Journal of the American College of Rheumatology RELATIONSHIP BETWEEN ARTHROSCOPIC EVIDENCE OF CARTILAGE DAMAGE AND RADIOGRAPHIC EVIDENCE OF JOINT SPACE NARROWING IN EARLY
~ Arthritis & Rheumatism Official Journal of the American College of Rheumatology RELATIONSHIP BETWEEN ARTHROSCOPIC EVIDENCE OF CARTILAGE DAMAGE AND RADIOGRAPHIC EVIDENCE OF JOINT SPACE NARROWING IN EARLY
Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings
 Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries
 Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
Magnetic resonance imaging of femoral head development in roentgenographically normal patients
 Skeletal Radiol (1985) 14:159-163 Skeletal Radiology Magnetic resonance imaging of femoral head development in roentgenographically normal patients Peter J. Littrup, M.D. 1, Alex M. Aisen, M.D. 2, Ethan
Skeletal Radiol (1985) 14:159-163 Skeletal Radiology Magnetic resonance imaging of femoral head development in roentgenographically normal patients Peter J. Littrup, M.D. 1, Alex M. Aisen, M.D. 2, Ethan
BRIEF REPORT. KENNETH D. BRANDT, ROSE S. FIFE, ETHAN M. BRAUNSTEIN, and BARRY KATZ. From the Department of Medicine, the Department of
 1381 BRIEF REPORT RADIOGRAPHIC GRADING OF THE SEVERITY OF KNEE OSTEOARTHRITIS: RELATION OF THE KELLGREN AND LAWRENCE GRADE TO A GRADE BASED ON JOINT SPACE NARROWING, AND CORRELATION WITH ARTHROSCOPIC EVIDENCE
1381 BRIEF REPORT RADIOGRAPHIC GRADING OF THE SEVERITY OF KNEE OSTEOARTHRITIS: RELATION OF THE KELLGREN AND LAWRENCE GRADE TO A GRADE BASED ON JOINT SPACE NARROWING, AND CORRELATION WITH ARTHROSCOPIC EVIDENCE
Prevalence of Meniscal Radial Tears of the Knee Revealed by MRI After Surgery
 Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration
 Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
JMSCR Vol 05 Issue 01 Page January
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
UCLA UCLA Previously Published Works
 UCLA UCLA Previously Published Works Title MR-IMAGING OF TIBIAL COLLATERAL LIGAMENT INJURY - COMPARISON WITH CLINICAL EXAMINATION Permalink https://escholarship.org/uc/item/2bs9g934 Journal SKELETAL RADIOLOGY,
UCLA UCLA Previously Published Works Title MR-IMAGING OF TIBIAL COLLATERAL LIGAMENT INJURY - COMPARISON WITH CLINICAL EXAMINATION Permalink https://escholarship.org/uc/item/2bs9g934 Journal SKELETAL RADIOLOGY,
Meniscal Tears with Fragments Displaced: What you need to know.
 Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
Comparative study of imaging at 3.0 T versus 1.5 T of the knee
 Skeletal Radiol (2009) 38:761 769 DOI 10.1007/s00256-009-0683-0 SCIENTIFIC ARTICLE Comparative study of imaging at 3.0 T versus 1.5 T of the knee Scott Wong & Lynne Steinbach & Jian Zhao & Christoph Stehling
Skeletal Radiol (2009) 38:761 769 DOI 10.1007/s00256-009-0683-0 SCIENTIFIC ARTICLE Comparative study of imaging at 3.0 T versus 1.5 T of the knee Scott Wong & Lynne Steinbach & Jian Zhao & Christoph Stehling
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
MY PATIENT HAS KNEE PAIN. David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging
 MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
Accuracy of SPECT bone scintigraphy in diagnosis of meniscal tears ABSTRACT
 1 Iran J Nucl Med 2005; 23 Accuracy of SPECT bone scintigraphy in diagnosis of meniscal tears M. Saghari 1, M. Moslehi 1, J. Esmaeili 2, M.N. Tahmasebi 3, A. Radmehr 4, M. Eftekhari 1,2, A. Fard-Esfahani
1 Iran J Nucl Med 2005; 23 Accuracy of SPECT bone scintigraphy in diagnosis of meniscal tears M. Saghari 1, M. Moslehi 1, J. Esmaeili 2, M.N. Tahmasebi 3, A. Radmehr 4, M. Eftekhari 1,2, A. Fard-Esfahani
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
MRI of Bucket-Handle Te a rs of the Meniscus of the Knee 1
 MRI of ucket-handle Te a rs of the Meniscus of the Knee 1 Joon Yong Park, M.D., Young-uk Lee M.D., Eun-Chul Chung M.D., Hae-Won Park M.D., E u n - Kyung Youn M.D., Shin Ho Kook, M.D., Young Rae Lee, M.D.
MRI of ucket-handle Te a rs of the Meniscus of the Knee 1 Joon Yong Park, M.D., Young-uk Lee M.D., Eun-Chul Chung M.D., Hae-Won Park M.D., E u n - Kyung Youn M.D., Shin Ho Kook, M.D., Young Rae Lee, M.D.
Role of Magnetic Resonance Imaging in Patients with Knee Trauma
 Original Research Article Role of Magnetic Resonance Imaging in Patients with Knee Trauma Bhautik Kapadia 1, Bhumika Suthar 2* 1 Associate Professor, 2 Assistant Professor, Department of Radiodiagnosis,
Original Research Article Role of Magnetic Resonance Imaging in Patients with Knee Trauma Bhautik Kapadia 1, Bhumika Suthar 2* 1 Associate Professor, 2 Assistant Professor, Department of Radiodiagnosis,
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT. Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology
 PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A
 Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
MENISCAL INJURY. Meniscus. Anterior Roots. Medial Meniscus. Lateral Meniscus. Posterior Roots. MRI and Arthroscopic Findings
 Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
of the lumbar facet joints there
 Skeletal Radiol (1999) 28:215±219 International Skeletal Society 1999 A R T I C L E Dominik Weishaupt Marco Zanetti Norbert Boos Juerg Hodler MR imaging and CT in osteoarthritis of the lumbar facet joints
Skeletal Radiol (1999) 28:215±219 International Skeletal Society 1999 A R T I C L E Dominik Weishaupt Marco Zanetti Norbert Boos Juerg Hodler MR imaging and CT in osteoarthritis of the lumbar facet joints
Chronic knee pain in adults - a multimodality approach or which modality to choose and when?
 Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
Modified Oblique Sagittal Magnetic Resonance Imaging of Rotator Cuff Tears: Comparison with Standard Oblique Sagittal Images
 Journal of Magnetics 22(3), 519-524 (2017) ISSN (Print) 1226-1750 ISSN (Online) 2233-6656 https://doi.org/10.4283/jmag.2017.22.3.519 Modified Oblique Sagittal Magnetic Resonance Imaging of Rotator Cuff
Journal of Magnetics 22(3), 519-524 (2017) ISSN (Print) 1226-1750 ISSN (Online) 2233-6656 https://doi.org/10.4283/jmag.2017.22.3.519 Modified Oblique Sagittal Magnetic Resonance Imaging of Rotator Cuff
Radiologic Pathologic Correlation of Intraosseous Lipomas. Tim Propeck 1, Mary Anne Bullard 1, John Lin 1, Kei Doi 2, William Martel 1
 Downloaded from www.ajronline.org by 148.251.232.83 on 04/10/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Radiologic Pathologic orrelation of Intraosseous
Downloaded from www.ajronline.org by 148.251.232.83 on 04/10/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Radiologic Pathologic orrelation of Intraosseous
Imaging of Articular Cartilage
 Clinical Imaging of Articular Cartilage Imaging of Articular Cartilage Prof. Dr. K. Verstraete Ghent University Introduction : Articular Cartilage Histology and biochemical composition Review of Imaging
Clinical Imaging of Articular Cartilage Imaging of Articular Cartilage Prof. Dr. K. Verstraete Ghent University Introduction : Articular Cartilage Histology and biochemical composition Review of Imaging
Post-injury painful and locked knee
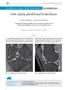 H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
Knee Joint Anatomy 101
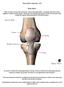 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies
 Original article: Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies Dr. Rakesh Gujjar*, Dr. R. P. Bansal, Dr. Sandeep
Original article: Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies Dr. Rakesh Gujjar*, Dr. R. P. Bansal, Dr. Sandeep
Priorities Forum Statement GUIDANCE
 Priorities Forum Statement Number 21 Subject Knee Arthroscopy including arthroscopic knee washouts Date of decision November 2016 Date refreshed March 2017 Date of review November 2018 Osteoarthritis of
Priorities Forum Statement Number 21 Subject Knee Arthroscopy including arthroscopic knee washouts Date of decision November 2016 Date refreshed March 2017 Date of review November 2018 Osteoarthritis of
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Osteoarthritis. Dr Anthony Feher. With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides
 Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Imaging Modalities: Clinical Reasoning and Key Instructional Elements: Radiography
 Imaging Modalities: Clinical Reasoning and Key Instructional Elements: Radiography Michael D. Ross, PT, DHSc, OCS mross@daemen.edu Disclosure No relevant financial relationship exists Objectives Determine
Imaging Modalities: Clinical Reasoning and Key Instructional Elements: Radiography Michael D. Ross, PT, DHSc, OCS mross@daemen.edu Disclosure No relevant financial relationship exists Objectives Determine
2 A B Fig. 1. Lateral tibial condyle fracture with joint effusion in a 35-year-old man. Sagittal T2-weighted MRI shows a large amount of effusion
 1 2 1 1 1 2 A B Fig. 1. Lateral tibial condyle fracture with joint effusion in a 35-year-old man. Sagittal T2-weighted MRI shows a large amount of effusion (between arrowheads) in the suprapatellar pouch,
1 2 1 1 1 2 A B Fig. 1. Lateral tibial condyle fracture with joint effusion in a 35-year-old man. Sagittal T2-weighted MRI shows a large amount of effusion (between arrowheads) in the suprapatellar pouch,
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
The mandibular condyle fracture is a common mandibular
 ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
IMAGING TECHNIQUES CHAPTER 4. Imaging techniques
 IMAGING TECHNIQUES Imaging techniques 23 4.1. Conventional radiographic findings Conventional radiography, tomography, arthrography and stress views have traditionally been used for imaging the ankle and
IMAGING TECHNIQUES Imaging techniques 23 4.1. Conventional radiographic findings Conventional radiography, tomography, arthrography and stress views have traditionally been used for imaging the ankle and
Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2, Patrick Smith, M.D. 2, and Larry S. Matthews, M.D. 2
 Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Magnetic resonance imaging in osteoarthritis of the
 14 Rheumatology Unit, Bristol Royal Infirmary, Bristol BS2 8HW T E M McAlindon I Watt F McCrae Goddard P A Dieppe Correspondence to: Dr McAlindon. Accepted for publication 2 February 1990 Annals of the
14 Rheumatology Unit, Bristol Royal Infirmary, Bristol BS2 8HW T E M McAlindon I Watt F McCrae Goddard P A Dieppe Correspondence to: Dr McAlindon. Accepted for publication 2 February 1990 Annals of the
OSTEOPHYTOSIS OF THE FEMORAL HEAD AND NECK
 908 RDIOLOGIC VIGNETTE OSTEOPHYTOSIS OF THE FEMORL HED ND NECK DONLD RESNICK Osteophytes are frequently considered the most characteristic abnormality of degenerative joint disease. In patients with osteoarthritis,
908 RDIOLOGIC VIGNETTE OSTEOPHYTOSIS OF THE FEMORL HED ND NECK DONLD RESNICK Osteophytes are frequently considered the most characteristic abnormality of degenerative joint disease. In patients with osteoarthritis,
FieldStrength. Achieva 3.0T enables cutting-edge applications, best-in-class MSK images
 FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
Are radiographs needed when MR imaging is performed for non-acute knee symptoms in patients younger than 45 years of age?
 Skeletal Radiol (2007) 36:1129 1139 DOI 10.1007/s00256-007-0384-5 SCIENTIFIC ARTICLE Are radiographs needed when MR imaging is performed for non-acute knee symptoms in patients younger than 45 years of
Skeletal Radiol (2007) 36:1129 1139 DOI 10.1007/s00256-007-0384-5 SCIENTIFIC ARTICLE Are radiographs needed when MR imaging is performed for non-acute knee symptoms in patients younger than 45 years of
Why Talk About Technique? MRI of the Knee:
 Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques
 Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques R O B E R T N A S C I M E N TO, M D, M S C H I E F OF S P O RT S M E D I C I N E & SH O U L D E R S U R G E RY N E W TO N- W E L L E S L
Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques R O B E R T N A S C I M E N TO, M D, M S C H I E F OF S P O RT S M E D I C I N E & SH O U L D E R S U R G E RY N E W TO N- W E L L E S L
Knee: Cruciate Ligaments
 72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
MRI of Osteochondral Defects of the Lateral Femoral Condyle: Incidence and Pattern of Injury After Transient Lateral Dislocation of the Patella
 Sanders et al. MRI of Osteochond ral Defects of the Lateral Femoral Condyle Musculoskeletal Imaging Clinical Observations A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:1332 1337 0361 803X/06/1875
Sanders et al. MRI of Osteochond ral Defects of the Lateral Femoral Condyle Musculoskeletal Imaging Clinical Observations A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:1332 1337 0361 803X/06/1875
HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE?
 HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE? To help horse owners better understand the tools we routinely use at VetweRx to evaluate their horse s soundness, the following section of this website reviews
HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE? To help horse owners better understand the tools we routinely use at VetweRx to evaluate their horse s soundness, the following section of this website reviews
MRI versus clinical examination for the diagnosis of meniscal and ligamentous injuries of kneee
 Original Research Article MRI versus clinical examination for the diagnosis of meniscal and ligamentous injuries of kneee Rakesh Gujjar *, R. P. Bansal, L. K. Gotecha, Raja Kollu Department of Radio-diagnosis
Original Research Article MRI versus clinical examination for the diagnosis of meniscal and ligamentous injuries of kneee Rakesh Gujjar *, R. P. Bansal, L. K. Gotecha, Raja Kollu Department of Radio-diagnosis
Posttraumatic subchondral bone contusions and fractures of the talotibial joint: Occurrence of kissing lesions
 KISSING CONTUSIONS CHAPTER 7 Posttraumatic subchondral bone contusions and fractures of the talotibial joint: Occurrence of kissing lesions Elizabeth S. Sijbrandij 1, Ad P.G. van Gils 1, Jan Willem K.
KISSING CONTUSIONS CHAPTER 7 Posttraumatic subchondral bone contusions and fractures of the talotibial joint: Occurrence of kissing lesions Elizabeth S. Sijbrandij 1, Ad P.G. van Gils 1, Jan Willem K.
Pre-operative clinical and radiological
 Pre-operative clinical and radiological assessment of the patellofemoral joint in unicompartmental knee replacement and its influence on outcome D. J. Beard, H. Pandit, S. Ostlere, C. Jenkins, C. A. F.
Pre-operative clinical and radiological assessment of the patellofemoral joint in unicompartmental knee replacement and its influence on outcome D. J. Beard, H. Pandit, S. Ostlere, C. Jenkins, C. A. F.
Lesions of the Menisci of the Knee: Value of MR Imaging Criteria for Recognition of Unstable Lesions
 B. C. Vande Berg 1 P. Poilvache 2 F. Duchateau 1 F. E. Lecouvet 1 J. E. Dubuc 2 B. Maldague 1 J. Malghem 1 Received June 12, 2000; accepted after revision August 24, 2000. 1 Department of Radiology, Cliniques
B. C. Vande Berg 1 P. Poilvache 2 F. Duchateau 1 F. E. Lecouvet 1 J. E. Dubuc 2 B. Maldague 1 J. Malghem 1 Received June 12, 2000; accepted after revision August 24, 2000. 1 Department of Radiology, Cliniques
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Sensitivity and Specificity in Detection of Labral Tears with 3.0-T MRI of the Shoulder
 Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
The Meniscus. History. Anatomy. Anatomy. Blood Supply. Attachments
 History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
Case 27 Clinical Presentation
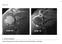 53 Case 27 Clinical Presentation 40-year-old man presents with acute shoulder pain and normal findings on radiographs. 54 RadCases Musculoskeletal Radiology Imaging Findings (,) Coronal images of the shoulder
53 Case 27 Clinical Presentation 40-year-old man presents with acute shoulder pain and normal findings on radiographs. 54 RadCases Musculoskeletal Radiology Imaging Findings (,) Coronal images of the shoulder
MRI of Cartilage. D. BENDAHAN (PhD)
 MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
"BONE BRUISES" OF THE KNEE: A REVIEW
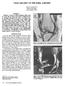 "BONE BRUISES" OF THE KNEE: A REVIEW Chad E. Mathis, M.D. Ken Noonan, M.D. Kosmas Kayes, M.D. ABSTRACT Magnetic resonance (MR) imaging is often used - to assess the location and degree of ligamentous wm.
"BONE BRUISES" OF THE KNEE: A REVIEW Chad E. Mathis, M.D. Ken Noonan, M.D. Kosmas Kayes, M.D. ABSTRACT Magnetic resonance (MR) imaging is often used - to assess the location and degree of ligamentous wm.
Patella position in the trochlea groove: comparison between supine and standing radiographs
 Patella position in the trochlea groove: comparison between supine and standing radiographs Award: Winner Poster No.: P-0098 Congress: ESSR 2014 Type: Authors: Keywords: DOI: Scientific Poster N. Skou,
Patella position in the trochlea groove: comparison between supine and standing radiographs Award: Winner Poster No.: P-0098 Congress: ESSR 2014 Type: Authors: Keywords: DOI: Scientific Poster N. Skou,
Available online at
 Original Research Article Evaluation of knee joint by MRI in 65 patients Gulamus sibtain asad *, Himanshu Singla, Ankit vasoya, P. J. Jhala 2 2 nd year Resident, 2 Professor Radiology Department, SBKS
Original Research Article Evaluation of knee joint by MRI in 65 patients Gulamus sibtain asad *, Himanshu Singla, Ankit vasoya, P. J. Jhala 2 2 nd year Resident, 2 Professor Radiology Department, SBKS
Differential Diagnosis
 Case 31yo M who sustained an injury to L knee while playing Basketball approximately 2 weeks ago. He describes pivoting and hyperextending his knee, which swelled over the next few days. He now presents
Case 31yo M who sustained an injury to L knee while playing Basketball approximately 2 weeks ago. He describes pivoting and hyperextending his knee, which swelled over the next few days. He now presents
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
IAIABC 2003 Lower Extremity Impairment Guides Part 4 of the Supplemental Impairment Rating Guides
 IAIABC 2003 Lower Extremity Impairment Guides Part 4 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 24 Madison, WI 53719 Phone: (608) 663-6355
IAIABC 2003 Lower Extremity Impairment Guides Part 4 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 24 Madison, WI 53719 Phone: (608) 663-6355
Evaluation of Role of Magnetic Resonance Imaging in Knee Joint Injuries in Correlation with Arthroscopy
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/442 Evaluation of Role of Magnetic Resonance Imaging in Knee Joint Injuries in Correlation with Arthroscopy T Sundara
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/442 Evaluation of Role of Magnetic Resonance Imaging in Knee Joint Injuries in Correlation with Arthroscopy T Sundara
Spontaneous osteonecrosis of the knee. Treatment and evolution.
 Spontaneous osteonecrosis of the knee. Treatment and evolution. J. R. Valentí Nín; M. Leyes; D. Schweitzer ABSTRACT We performed a retrospective study on 21 patients affected by unilateral spontaneous
Spontaneous osteonecrosis of the knee. Treatment and evolution. J. R. Valentí Nín; M. Leyes; D. Schweitzer ABSTRACT We performed a retrospective study on 21 patients affected by unilateral spontaneous
Original Research Article
 ROLE OF IN INTERNAL DERANGEMENT OF KNEE JOINT IN CORRELATION WITH ARTHROSCOPY Onteddu Joji Reddy 1, Jamkhana Abdul Gafoor 2, Balla Suresh 3, Polysetty Obuleswar Prasad 4 1Professor and HOD, Department
ROLE OF IN INTERNAL DERANGEMENT OF KNEE JOINT IN CORRELATION WITH ARTHROSCOPY Onteddu Joji Reddy 1, Jamkhana Abdul Gafoor 2, Balla Suresh 3, Polysetty Obuleswar Prasad 4 1Professor and HOD, Department
THE KNEE SOCIETY VIRTUAL FELLOWSHIP
 THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER 2: RADIOGRAPHIC EVALUATION OF THE KNEE Radiographic Evaluation of the Knee Presented by: R. Michael Meneghini, MD COPYRIGHT 2016 THE KNEE SOCIETY Disclosures
THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER 2: RADIOGRAPHIC EVALUATION OF THE KNEE Radiographic Evaluation of the Knee Presented by: R. Michael Meneghini, MD COPYRIGHT 2016 THE KNEE SOCIETY Disclosures
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/28/2012 Radiology Quiz of the Week # 83 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/28/2012 Radiology Quiz of the Week # 83 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
dgemric Effectively Predicts Cartilage Damage Associated with Femoroacetabular Impingement
 Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Meniscal tears on 3T MR: Patterns, pearls and pitfalls
 Meniscal tears on 3T MR: Patterns, pearls and pitfalls Poster No.: C-2221 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: J. C. Kandathil; Singapore/SG Keywords: Knee injuries,
Meniscal tears on 3T MR: Patterns, pearls and pitfalls Poster No.: C-2221 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: J. C. Kandathil; Singapore/SG Keywords: Knee injuries,
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE
 THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
Why the dog? Analogy of the anatomy
 Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Brain Atrophy. Brain Atrophy
 Aging Central Nervous System Processes Age related brain atrophy Non-age related brain atrophy Cerebrovascular disease Cerebral infarction Hypertensive hemorrhage Carotid artery stenosis and occlusion
Aging Central Nervous System Processes Age related brain atrophy Non-age related brain atrophy Cerebrovascular disease Cerebral infarction Hypertensive hemorrhage Carotid artery stenosis and occlusion
The Unispacer TM unicompartmental knee implant: Its outcomes in medial compartment knee osteoarthritis
 Orthopaedics & Traumatology: Surgery & Research (2011) 97, 410 417 ORIGINAL ARTICLE The Unispacer TM unicompartmental knee implant: Its outcomes in medial compartment knee osteoarthritis C. Catier, M.
Orthopaedics & Traumatology: Surgery & Research (2011) 97, 410 417 ORIGINAL ARTICLE The Unispacer TM unicompartmental knee implant: Its outcomes in medial compartment knee osteoarthritis C. Catier, M.
a - CM EARTICLE Clinics in diagnostic imaging (139) !Medical Education Singapore Med J 2012; 53(4) CASE PRESENTATION
 !Medical Education Singapore Med J 2012; 53(4) 283 CM EARTICLE Clinics in diagnostic imaging (139) Wei Yang Liml, MBBS, FRCR, Nor Azam Mahmud2, MD, MMed, Wilfred CG Peh3, FRCP, FRCR a - - - Fig. 1 Sagittal
!Medical Education Singapore Med J 2012; 53(4) 283 CM EARTICLE Clinics in diagnostic imaging (139) Wei Yang Liml, MBBS, FRCR, Nor Azam Mahmud2, MD, MMed, Wilfred CG Peh3, FRCP, FRCR a - - - Fig. 1 Sagittal
Conservative surgical treatments for osteoarthritis: A Finite Element Study
 Conservative surgical treatments for osteoarthritis: A Finite Element Study Diagarajen Carpanen, BEng (Hons), Franziska Reisse, BEng(Hons), Howard Hillstrom, PhD, Kevin Cheah, FRCS, Rob Walker, PhD, Rajshree
Conservative surgical treatments for osteoarthritis: A Finite Element Study Diagarajen Carpanen, BEng (Hons), Franziska Reisse, BEng(Hons), Howard Hillstrom, PhD, Kevin Cheah, FRCS, Rob Walker, PhD, Rajshree
A comparative study of MRI versus arthroscopic findings in ACL and meniscal injuries of the knee
 International Journal of Research in Orthopaedics Kulkarni OP et al. Int J Res Orthop. 2018 Mar;4(2):198-202 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180123
International Journal of Research in Orthopaedics Kulkarni OP et al. Int J Res Orthop. 2018 Mar;4(2):198-202 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180123
Partial Knee Replacement
 Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Dimensions of the intercondylar notch and the distal femur throughout life
 Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year
 Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year H. Pandit, C. Jenkins, D. J. Beard, J. Gallagher, A. J. Price, C. A. F. Dodd, J. W. Goodfellow, D. W. Murray From
Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year H. Pandit, C. Jenkins, D. J. Beard, J. Gallagher, A. J. Price, C. A. F. Dodd, J. W. Goodfellow, D. W. Murray From
Anterior Cruciate Ligament Surgery
 Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Unlocking the locked Knee
 Unlocking the locked Knee Poster No.: P-0027 Congress: ESSR 2013 Type: Scientific Exhibit Authors: J. P. SINGH, S. Srivastava, S. S. BAIJAL ; Gurgaon, Delhi 1 1 2 1 2 NCR/IN, LUCKNOW, UTTAR PRADESH/IN
Unlocking the locked Knee Poster No.: P-0027 Congress: ESSR 2013 Type: Scientific Exhibit Authors: J. P. SINGH, S. Srivastava, S. S. BAIJAL ; Gurgaon, Delhi 1 1 2 1 2 NCR/IN, LUCKNOW, UTTAR PRADESH/IN
Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping
 TR_002 Technical Reports Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping Min A Yoon 1,*, Suk-Joo Hong 1, Chang Ho Kang 2, Baek Hyun Kim 3 1 Korea University
TR_002 Technical Reports Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping Min A Yoon 1,*, Suk-Joo Hong 1, Chang Ho Kang 2, Baek Hyun Kim 3 1 Korea University
LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION
 LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION R. ŚMIGIELSKI, B. DOMINIK, U, ZDANOWICZ, Z. GAJEWSKI, K. SKIERBISZEWSKA, K. SIEWRUK,
LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION R. ŚMIGIELSKI, B. DOMINIK, U, ZDANOWICZ, Z. GAJEWSKI, K. SKIERBISZEWSKA, K. SIEWRUK,
Acute Elbow Trauma in Children: Spectrum of Injury Revealed by MR Imaging Not Apparent on Radiographs
 James F. Griffith 1 Derek J. Roebuck 1,2 Jack C. Y. Cheng 3 Yu Leung Chan 1 Timothy H. Rainer 4 Bobby K. W. Ng 3 Constantine Metreweli 1 Received December 14, 1999; accepted after revision June 8, 2000.
James F. Griffith 1 Derek J. Roebuck 1,2 Jack C. Y. Cheng 3 Yu Leung Chan 1 Timothy H. Rainer 4 Bobby K. W. Ng 3 Constantine Metreweli 1 Received December 14, 1999; accepted after revision June 8, 2000.
The Characteristic Findings to Assess Meniscal Healing Status After Meniscal Repair on MRI-T2 Mapping
 The Characteristic Findings to Assess Meniscal Healing Status After Meniscal Repair on MRI-T2 Mapping Shinya Yamasaki, MD, PhD 1,2, Yusuke Hashimoto, MD, PhD 2, Takuya Kinoshita, MD 2, Kazuya Nishino,
The Characteristic Findings to Assess Meniscal Healing Status After Meniscal Repair on MRI-T2 Mapping Shinya Yamasaki, MD, PhD 1,2, Yusuke Hashimoto, MD, PhD 2, Takuya Kinoshita, MD 2, Kazuya Nishino,
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
Disclosures. Background. Background
 Kinematic and Quantitative MR Imaging Evaluation of ACL Reconstructions Using the Mini-Two Incision Method Compared to the Anteromedial Portal Technique Drew A. Lansdown, MD Christina Allen, MD Samuel
Kinematic and Quantitative MR Imaging Evaluation of ACL Reconstructions Using the Mini-Two Incision Method Compared to the Anteromedial Portal Technique Drew A. Lansdown, MD Christina Allen, MD Samuel
TOTAL KNEE ARTHROPLASTY (TKA)
 TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
MRI of LEFT KNEE. There is a fluid collection seen anterior to and inferior to the superiorly displaced patella.
 MRI of LEFT KNEE Protocol: Multiplanar MRI of the left knee joint performed in the sagittal, coronal and transverse planes using T1 weighted spin echo, T2 and proton-density weighted fast spin echo, fatsaturated
MRI of LEFT KNEE Protocol: Multiplanar MRI of the left knee joint performed in the sagittal, coronal and transverse planes using T1 weighted spin echo, T2 and proton-density weighted fast spin echo, fatsaturated
