TW Case Discussion Guide Key Learning Objectives
|
|
|
- Diane Sanders
- 5 years ago
- Views:
Transcription
1 TW Case Discussion Guide Key Learning Objectives Construct a differential diagnosis for a systemic disease presentation with primarily cutaneous manifestations. Summarize barriers that impede patient follow-up. Describe the complications of pregnancy associated with systemic lupus erythematosus (SLE), and how these are evaluated and managed. Discuss the uses of relevant medications in the context of SLE and pregnancy. Summarize the importance of a multidisciplinary team approach when caring for patients with SLE. 1
2 History of Present Illness The patient is an 18-year-old White, pregnant female, at 12-weeks gestation, admitted for evaluation of a diffuse skin rash. She was diagnosed with systemic lupus erythematosus (SLE) 4 years ago at the age of 14. Her original manifestations included positive antinuclear antibodies (ANA), oral ulcers, rash, leukopenia, and swollen fingers. She was followed and treated by a pediatric rheumatologist. Her disease had been under good control with hydroxychloroquine and prednisone. Three months ago, she became pregnant. As a result, her pediatric rheumatologist felt it was more appropriate for her to be followed by adult physicians. He began the process of transitioning her care to adult rheumatology and high-risk obstetrics. Several referrals were made; however, the patient was reluctant to establish care with new doctors and never made an appointment with either obstetrics or adult rheumatology. She continued to take prednisone but stopped the hydroxychloroquine out of concern for toxicity to the baby. Four weeks ago, at 8-weeks gestation, she began feeling fatigued and run down. She developed oral ulcers typical of her SLE. She decided on her own to increase her prednisone dose in response, from 5 mg/day to eventually 35 mg/day. In spite of this, the ulcers continued to expand. Over about a 10-day period, she developed swollen, puffy lips and an erythematous rash over her cheeks, hands, chest, and feet. She began to feel feverish. Her symptoms continued to the point that oral intake was severely limited due to odynophagia. She presented to the hospital with weight loss, odynophagia, low-grade fever, and diffuse rash. What are your concerns regarding her new symptoms? What is your differential diagnosis for what might be causing these new symptoms? This is a complicated patient with many issues that need to be considered in order to optimize her care. She is a pediatric patient, lost to follow-up care, and now pregnant with fever and mucocutaneous symptoms. One of the largest causes of morbidity in SLE patients is infection, and this should be at the top of their differential. Additionally, a flare of SLE prompted by both the patient s pregnancy and her selfdiscontinuation of medications should be considered. It is important to recognize that the initial presentation of a lupus flare can be very similar to that of infection (fever, malaise, fatigue, rash) and similar to many of the symptoms that occur in some women as a result of pregnancy. What is known about pediatric-onset SLE that may make us more concerned about this patient? A significant portion of SLE patients (15%, predominantly female) present in childhood, usually during adolescence. This patient 2
3 certainly fits into that category. Children with SLE are significantly more likely to have a more severe course of disease. Other important issues for consideration are the psychosocial issues stemming from childhood illness, including missed school, altered family dynamics, and compliance, all of which factor into SLE outcomes. Additional Medical History Past Medical History: SLE, diagnosed at age 14, with manifestations of oral ulcers, malar rash, arthritis, leukopenia, and positive ANA. No other past medical history. No prior pregnancies. No history of blood clots. Family History: Mother with type 2 diabetes mellitus; no family history of autoimmune disease. Her father s medical history is unknown, as she has had no contact with him since the age of 5. Social History: Lives with grandparents and boyfriend. Stopped attending high school when she became pregnant but was previously in her junior year. She intends to resume school after pregnancy. She does not smoke, drink alcohol, or use illicit drugs. Neither she nor her boyfriend is employed. Her mother works as a waitress. No other family members or close contacts have been ill. How do you think her transition from pediatric to adult caregivers could have contributed to her illness? How might that have been improved? Poor outcomes in SLE are influenced more by poverty and lack of education than genetics. Two important concepts for consideration are: First is the concept of self-efficacy, or the patient s confidence in his or her success in managing a complicated, chronic disease. Selfefficacy is lower in less educated individuals and those with lower socioeconomic status, and this alone is related to outcomes in SLE. The second important concept is the role of the physician in understanding social and economic factors that impact a patient s ability to adhere to a therapeutic plan. In this case, the patient s young age, lack of education, and pregnancy likely impeded appropriate care and management of her SLE. Her physician might have improved the situation by addressing these issues. Specifically, her pediatric physician might have facilitated a visit where both pediatric and adult rheumatologists were present to assist with the patient s transition to adult rheumatology. In other settings, specialists are scarce, and adult rheumatologists, or even generalists, sometimes manage pediatric SLE patients. Therefore, it is important to note that the specific 3
4 doctors and specialties involved in the transition of this particular case are not the primary focus. The point is that proper transition of care between a pediatric and adult setting, and between any providers, is critical for all patient outcomes. The physicians might also have asked for the patient s permission to discuss her care with her family members, thereby engaging family members in helping the patient adhere to her treatment plan. It is important for physicians to be aware of the difficulty of the situation. Physical Exam Height: 5 8 Weight: 135 lbs Vitals: Temperature 38.3 C (100.9 F), blood pressure 125/57, pulse 112, respiratory rate 16, O2 saturation 99% on room air General: Mildly cushingoid, White female, in mild distress from pain Cardiovascular: Tachycardic, regular rhythm, no murmurs Pulmonary: Clear to auscultation bilaterally Abdomen: Gravid uterus, soft; mild epigastric tenderness, no rebound/ guarding, palpable fetal movement Musculoskeletal: Full range of motion of all joints; no evidence of synovitis or deformity Image courtesy of Dr. Wael Jarjour, Director of the Division of Rheumatology & Immunology, The Ohio State University Wexner Medical Center. The images included in this case are for example only and are not those of the individual described in the case. 4
5 Skin and mucous membranes: Oropharynx with ulcers on upper hard palate approximately 1.2 cm diameter, and multiple small ulcers on buccal mucosa Malar rash with erythematous plaques Erythematous patches over bilateral eyelids, chest, biceps (some of the rash over the biceps was ulcerated) Periungual hyperpigmentation Desquamating erythematous rash over the feet Laboratory Data Complete Blood Count (CBC): White blood cell count (WBC): 7.8 x 10 3 /µl White count differential: 2% bands, 73% neutrophils, 18% lymphocytes Hemoglobin: 10.0 g/dl* Hematocrit: 30.4%* Platelets: 179 Mean cell volume: 83 Comprehensive metabolic panel: Total protein: 6.1 g/dl* Albumin: 2.7 g/dl* All others normal Urinalysis: No proteinuria No urine sediment *Abnormal values What is your differential diagnosis for the patient s skin symptoms? What are the data for or against each item on your differential diagnosis? How would you further work this up? Revisit your original differential diagnosis, which should include infection and SLE flare. At this point, you should be able to state more specifically which infections you are concerned about. Regarding infection, consistent signs and symptoms include fever and erythematous rash. You should be concerned about herpes simplex virus (HSV), which can cause mucocutaneous ulcerations or a 5
6 bacterial infection, such as staph. However, the normal WBC is not typical of an infection, which should prompt a discussion of the WBC in SLE. One of this patient s SLE manifestations is leukopenia, so it is important to recognize that a WBC of 7.8 may be relatively elevated in this patient with SLE, which is different than in the general population. Additionally, the increased proportion of neutrophils and presence of bands might suggest infection in this patient. Keep in mind that pregnancy itself, as well as glucocorticoid use may also contribute to leukocytosis. The increased risk of infection due to immunosuppressive medications (ie, glucocorticoid use in this patient) should also be considered. Signs and symptoms suggestive of an SLE flare include the evolution of the rash, which began in a similar manner to her previous SLE skin flares, as well as oral ulcers, anemia, and hypoalbuminemia. In addition, she recently had two major changes: the advent of pregnancy and the discontinuation of her SLE medications, both of which can increase SLE activity. What specific additional labs would you send given SLE and pregnancy? For which condition are you testing? Consider the pathophysiology of this condition and its potential manifestations. SLE pregnancies are high risk for mother and baby, with increased C-sections, preterm birth, fetal loss, pre-eclampsia, gestational diabetes, and infection. An additional consideration is neonatal SLE, which is tested for by checking anti-ssa and -SSB autoantibodies, which are common in SLE as well as other conditions. Circulating anti-ssa and -SSB autoantibodies may cross the placenta into the fetal circulation, causing neonatal SLE in the fetus. This is an example of passive transfer of autoimmunity in that the autoantibodies from the mother are causing autoimmune disease in the fetus; the fetus is not producing autoantibodies on his own. The most serious manifestation of neonatal SLE is cardiac disease in which the autoantibodies deposit in developing cardiac tissue resulting in first-, second-, or third-degree heart block. Other manifestations of neonatal SLE include thrombocytopenia and/ or a transient, erythematous rash that presents in the newborn infant. Double-stranded DNA antibodies are often elevated and complement levels are often decreased during an acute flare of SLE in both pregnant and nonpregnant patients, so these should be ordered as well. What services would you consult to optimize this patient s workup and care? This patient requires coordinated care by high-risk obstetrics and rheumatology, as well as an infectious disease consult to evaluate for the possibility of infection as the cause of the rash. 6
7 Hospital Course The patient was admitted to the obstetrics (OB) service. Infectious disease, rheumatology, dermatology, and maternal-fetal medicine (high-risk OB) services were consulted to assist in her care. Infectious disease felt that HSV or varicella zoster virus (VZV) skin infections could cause this degree of skin ulceration, or a drug reaction, but that SLE was the most likely cause. They recommended withholding empiric antibiotics unless the patient worsened and sent swabs of ulcers for bacteria and viral culture. Blood cultures were also performed. Dermatology and rheumatology also felt that her clinical picture was due to a severe mucocutaneous SLE flare. Dermatology performed a skin biopsy. Anti double-stranded DNA antibodies, anti-ssa and -SSB antibodies, and complement levels were ordered. Because of the severity of her symptoms, intravenous (IV) methylprednisolone sodium succinate 30 mg every 8 hours was started, and hydroxychloroquine was restarted before these labs had returned. Topical corticosteroids were also administered. Results of Lab Testing Blood cultures and HSV, VZV cultures were negative Anti double-stranded DNA antibodies >400 U/mL*; previously was 82 U/mL 3 months ago C3 = 110 mg/dl (normal is mg/dl) C4 = 8 mg/dl* (normal is mg/dl) anti-ssa antibodies = 8 U/mL (normal <8 U/mL) anti-ssb antibodies = 11 U/mL (normal <4 U/mL) Anticardiolipin antibody, anti-β 2 -glycoprotein I antibody, and lupus anticoagulant were all negative *Abnormal values Skin Biopsy Results Degeneration of the basal layer of the epidermis. Edema at the dermo epidermal junction. Some edema and perivascular mononuclear infiltrates. Immunofluorescence microscopy shows granular deposits of immuno globulin G, C3, and immunoglobulin M, along the dermoepidermal junction. Given what you know about the pathology of SLE nephritis, how do you interpret this patient s skin biopsy? Immunoglobulin and complement deposits occur in various parts of the glomerulus, as well as around the glomerular basement 7
8 membrane. Consider what you know about kidney biopsies and apply that to the findings of immunoglobulin and complement deposits along the dermoepidermal junction in the skin. There is some homology between the dermoepidermal junction of the skin and the glomerular basement membrane of the kidney. Understanding that SLE is a systemic disease process, you should conclude that what can occur in the kidney can also occur in the skin or other tissues affected by SLE; therefore, this biopsy might be consistent with cutaneous SLE. Certainly the findings on immunofluorescence would not be consistent with an infectious process in the skin. Given this patient s anti-ssa and -SSB antibodies, what additional testing is necessary to evaluate fetal well-being? This brings up the topic of neonatal SLE again. Positive anti-ssa and -SSB antibodies place the fetus at risk for first-, second-, or third-degree heart block that may be irreversible if not detected early. In practice, the fetus is monitored with regular ultrasound and fetal echocardiograms looking for any cardiac abnormalities that might suggest the evolution of congenital heart block. Once heart block is detected, treatment options are limited. Often the patient is treated with betamethasone, a steroid that can cross the placenta to reach the fetus. However, in the majority of cases of SLE-related neonatal heart block, this damage to the cardiac tissue is irreversible in spite of steroid treatment. Therefore, the focus is on awareness, early detection, and planning neonatal care for a baby born with a heart block. Consider what medications can be used to treat SLE during pregnancy. What medications are contraindicated? Some of the more common medications used in SLE include: hydroxychloroquine, corticosteroids, and azathioprine. These can all be used during pregnancy, if clinically warranted. Methotrexate, mycophenolate mofetil, cyclophosphamide, and warfarin must not be used during pregnancy due to known teratogenic effects. In some cases the risk of certain immunosuppressives, such as cyclophosphamide, may be justified in the third trimester. Hospital Course (cont d) The patient s skin biopsy is read as consistent with SLE. There is no viral cytopathic effect or other infiltrate to indicate concomitant infection. 8
9 By Hospital Day-4 on methylprednisolone sodium succinate, the patient s muco cutaneous lesions had improved, and she was able to tolerate some oral intake. She is started on azathioprine 50 mg daily to serve as a steroid-sparing agent, with a plan to increase this dose to 2 mg/kg over several weeks time. It is reasonable clinical practice to obtain thiopurine methyltransferase (TPMT) genetic testing to determine the safety of using high-dose azathioprine. The patient should also have regular lab follow-up. Fetal ultrasound and echocardiogram are normal. The patient continues to improve. Skin lesions show signs of healing, although there continue to be desquamating lesions on her feet. On Hospital Day-7, she feels slightly worse, with fatigue and malaise. She is noted on vitals to have a temperature of 38.4 C (101.4 F). The on-call obstetrics resident for the primary team is notified, and acetaminophen is given for fever. The next morning, the patient is afebrile on morning rounds after two doses of acetaminophen; however, she continues to feel poorly. When the rheumatologist sees her in the afternoon, she is again febrile to 39.0 C (102.2 F). Consider your differential diagnosis for the patient s fever and malaise. Why was she at risk for developing further complications? What needs to be sent for further evaluation? At this point, infection again needs to be at the top of the differential diagnosis. The patient s admission diagnosis of mucocutaneous SLE flare is being treated, and she was showing signs of improvement. With this sudden deterioration, she must be evaluated for a new problem. Given her immunosuppression with high-dose steroids and prolonged hospital stay, she is at high risk for infection. She should have immediate blood and urine cultures and a chest X-ray for further evaluation. IV sites and skin should be examined for signs of infection. Also note the delay in evaluation of her fever by the primary team. While low-grade fever in a pregnant patient without SLE is often transient, responsive to acetaminophen, and not requiring further evaluation, fever in a complicated patient with active SLE should always prompt a full exam and evaluation for underlying infection. Infection is an even more serious concern given her fever developed while on glucocorticoids, which impair the immune system s response to infection. Case Follow Up Within 8 hours, the patient s blood cultures returned positive with gram positive cocci in clusters. 9
10 Vancomycin was started for presumed Staphylococcus aureus bacteremia. Twenty-four hours later the microbiology lab confirms methicillin-resistant S. aureus in the blood. Given her staph bacteremia, she is at high risk for bacterial endocarditis. Transesophageal echocardiogram is ordered to evaluate her valves for endocarditis; however, given her oropharyngeal ulcerations, this is deferred in favor of a transthoracic echocardiogram. The patient s rash begins to worsen, with new oral ulcerations presumably precipitated by the new infection. By Hospital Day-9, the patient had responded well to antibiotics with negative follow-up blood cultures. Her rash began to heal again without any change in steroid dose, and she was slowly able to tolerate a full oral diet. By Hospital Day-14, she was stable and ready for hospital discharge. She was discharged home with close outpatient follow-up with infectious disease, rheumatology, dermatology, and high-risk obstetrics. She was continued on prednisone, hydroxychloroquine and azathioprine, and had home health nursing visits arranged to complete a 14-day course of vancomycin for staph bacteremia. In spite of a very complicated hospital course, the patient did well with her postdischarge care and at 38-weeks gestation, delivered a healthy newborn. Notes: Refer to the Lupus Initiative Lecture series for more information. The images included in this case are for example only and are not those of the individual described in the case. The production of this activity was supported by Grant Number 7 MPCMP from the U.S. Department of Health and Human Services Office of Minority Health (HHS, OMH). Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the HHS, OMH. 10
11 11
DRAFT. TW Case Discussion Guide. Key Learning Objectives
 TW Case Discussion Guide Key Learning Objectives Construct a differential diagnosis for a systemic disease presentation with primarily cutaneous manifestations Summarize barriers that impede patient follow-up
TW Case Discussion Guide Key Learning Objectives Construct a differential diagnosis for a systemic disease presentation with primarily cutaneous manifestations Summarize barriers that impede patient follow-up
AAF Case Discussion Guide Key Learning Objectives
 AAF Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation with multisystem involvement. Identify the key questions from the history to look for
AAF Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation with multisystem involvement. Identify the key questions from the history to look for
AAM Case Discussion Guide Key Learning Objectives
 AAM Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation in a young person. Discuss the key elements of diagnosing systemic lupus erythematosus
AAM Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation in a young person. Discuss the key elements of diagnosing systemic lupus erythematosus
UNDERSTANDING SYSTEMIC LUPUS ERYTHEMATOSUS
 UNDERSTANDING SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. October 20, 2012 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement Diagnosis Treatment Pregnancy
UNDERSTANDING SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. October 20, 2012 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement Diagnosis Treatment Pregnancy
Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z
 Topic Page: Systemic Lupus Erythematosus Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z What Is It? Lupus is thought to develop when the immune system
Topic Page: Systemic Lupus Erythematosus Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z What Is It? Lupus is thought to develop when the immune system
Definition Chronic autoimmune disease The body s immune system starts attacking itself Can affect most organs and tissues in the body Brain, lungs, he
 LIVING WITH SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. Rowan Diagnostic Clinic Salisbury, N.C. May 11, 2013 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement
LIVING WITH SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. Rowan Diagnostic Clinic Salisbury, N.C. May 11, 2013 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement
DRAFT. AAF Case Discussion Guide. Key Learning Objectives
 AAF Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation with multisystem involvement Identify the key questions from the history to look for
AAF Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation with multisystem involvement Identify the key questions from the history to look for
Lupus. Fast facts. What is lupus? What causes lupus? Who gets lupus?
 Lupus Systemic lupus erythematosus, referred to as SLE or lupus, is sometimes called the "great imitator." Why? Because of its wide range of symptoms, people often confuse lupus with other health problems.
Lupus Systemic lupus erythematosus, referred to as SLE or lupus, is sometimes called the "great imitator." Why? Because of its wide range of symptoms, people often confuse lupus with other health problems.
Learning about Lupus. Learning About Lupus. Lupus Society of Illinois
 Learning About Lupus Learning about Lupus Lupus Society of Illinois 525 W. Monroe Street, Suite 900 Chicago, Illinois 60661 Robert S. Katz, M.D. Professor of Medicine Rush University Medical Center Northwestern
Learning About Lupus Learning about Lupus Lupus Society of Illinois 525 W. Monroe Street, Suite 900 Chicago, Illinois 60661 Robert S. Katz, M.D. Professor of Medicine Rush University Medical Center Northwestern
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: belimumab_benlysta 6/2011 2/2018 2/2019 3/2018 Description of Procedure or Service Belimumab (Benlysta) is
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: belimumab_benlysta 6/2011 2/2018 2/2019 3/2018 Description of Procedure or Service Belimumab (Benlysta) is
YF Case Discussion Guide Key Learning Objectives
 YF Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation. Describe the key manifestations of disease on physical exam in a multisystem disease
YF Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation. Describe the key manifestations of disease on physical exam in a multisystem disease
Benlysta (belimumab) Prior Authorization Criteria Program Summary
 Benlysta (belimumab) Prior Authorization Criteria Program Summary This prior authorization applies to Commercial, NetResults A series, NetResults F series and Health Insurance Marketplace formularies.
Benlysta (belimumab) Prior Authorization Criteria Program Summary This prior authorization applies to Commercial, NetResults A series, NetResults F series and Health Insurance Marketplace formularies.
High Impact Rheumatology
 High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
Systemic examination
 PROLONGED FEVER IN AN ADOLESCENT BOY Dr.Praveena Lionel, DNB PG, Dr.Kannan (HOD) Railway Hospital, Perambur History 11 yrs old adolescent boy was admitted with c/o Fever -1 wk Myalgia -1 wk Arthralgia
PROLONGED FEVER IN AN ADOLESCENT BOY Dr.Praveena Lionel, DNB PG, Dr.Kannan (HOD) Railway Hospital, Perambur History 11 yrs old adolescent boy was admitted with c/o Fever -1 wk Myalgia -1 wk Arthralgia
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
Fever in the Newborn Period
 Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
To live with lupus, we need to know about lupus.
 To live with lupus, we need to know about lupus. Zineb Aouhab, MD Assistant Professor of Medicine Loyola University Medical Center Division of Rheumatology 1 Where did the word lupus come from? The word
To live with lupus, we need to know about lupus. Zineb Aouhab, MD Assistant Professor of Medicine Loyola University Medical Center Division of Rheumatology 1 Where did the word lupus come from? The word
DISCUSSION BY: Dr M. R. Shakeebi, MD, Rheumatologist
 Case presentations Related to some Rheumatic Diseases Lab & Clinic i Programs, Tuesday, April 24, 2012 COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD, Immunologist COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD,
Case presentations Related to some Rheumatic Diseases Lab & Clinic i Programs, Tuesday, April 24, 2012 COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD, Immunologist COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD,
Fever in neonates (age 0 to 28 days)
 Fever in neonates (age 0 to 28 days) INCLUSION CRITERIA Infant 28 days of life Temperature 38 C (100.4 F) by any route/parental report EXCLUSION CRITERIA Infants with RSV Febrile Infant 28 days old Ill
Fever in neonates (age 0 to 28 days) INCLUSION CRITERIA Infant 28 days of life Temperature 38 C (100.4 F) by any route/parental report EXCLUSION CRITERIA Infants with RSV Febrile Infant 28 days old Ill
Cases I have Learned From. Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville
 Cases I have Learned From Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville Jeffrey P. Callen, MD Disclosure (previous 12 months) Consultant/Advisory board Auxilium Consultant
Cases I have Learned From Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville Jeffrey P. Callen, MD Disclosure (previous 12 months) Consultant/Advisory board Auxilium Consultant
Good Morning! Welcome Applicants! FRIDAY, N OVEMBER, 7 TH 2014
 Good Morning! Welcome Applicants! FRIDAY, N OVEMBER, 7 TH 2014 Prep Question You are camping with a group of boys at a rural campground in the southeastern Unites States when one of the campers is bitten
Good Morning! Welcome Applicants! FRIDAY, N OVEMBER, 7 TH 2014 Prep Question You are camping with a group of boys at a rural campground in the southeastern Unites States when one of the campers is bitten
LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS LUPUS 101 SLE SUBSETS AUTOIMMUNE DISEASE 11/4/2013 HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS
 LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
DRAFT. AAM Case Discussion Guide. Key Learning Objectives
 AAM Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation in a young person Discuss the key elements of diagnosing systemic lupus erythematosus
AAM Case Discussion Guide Key Learning Objectives List the differential diagnosis for a systemic disease presentation in a young person Discuss the key elements of diagnosing systemic lupus erythematosus
9/25/2013 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE)
 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
Lupus. and the Kidneys
 Lupus and the Kidneys LupusuK 2015 This information booklet has been produced by LUPUS UK 2015 LUPUS UK LUPUS UK is the national charity caring for those with systemic lupus erythematosus (SLE) and discoid
Lupus and the Kidneys LupusuK 2015 This information booklet has been produced by LUPUS UK 2015 LUPUS UK LUPUS UK is the national charity caring for those with systemic lupus erythematosus (SLE) and discoid
Systemic Lupus Erythematosus
 A Patient s Guide to Systemic Lupus Erythematosus 2 kidneys. These changes make it impossible for the kidneys to function normally. The inflammation of SLE can be seen in the lining, covering, and muscles
A Patient s Guide to Systemic Lupus Erythematosus 2 kidneys. These changes make it impossible for the kidneys to function normally. The inflammation of SLE can be seen in the lining, covering, and muscles
10/25/2018. Autoimmunity and how to treat it. Disclosure. Why do we get autoimmunity? James Verbsky MD/PhD Pediatric Rheumatology/Immunology
 Autoimmunity and how to treat it James Verbsky MD/PhD Pediatric Rheumatology/Immunology Disclosure None I will mention drug names and some brand names but I have no financial interest or any other ties
Autoimmunity and how to treat it James Verbsky MD/PhD Pediatric Rheumatology/Immunology Disclosure None I will mention drug names and some brand names but I have no financial interest or any other ties
Lab 3, case 1. Is this an example of nephrotic or nephritic syndrome? Why? Which portion of the nephron would you expect to be abnormal?
 Lab 3, case 1 12-year-old Costa Rican boy is brought into clinic by his parents because of dark brownish-red urine over the last 24 hours. The family has been visiting friends in Indianapolis for two weeks.
Lab 3, case 1 12-year-old Costa Rican boy is brought into clinic by his parents because of dark brownish-red urine over the last 24 hours. The family has been visiting friends in Indianapolis for two weeks.
Fever Without a Source Age: 0-28 Day Pathway - Emergency Department Evidence Based Outcome Center
 Age: 0-28 Day Pathway - Emergency Department EXCLUSION CRITERIA Toxic appearing No fever Born < 37 weeks gestational age INCLUSION CRITERIA Non-toxic with temperature > 38 C (100.4 F) < 36 C (96.5 F) measured
Age: 0-28 Day Pathway - Emergency Department EXCLUSION CRITERIA Toxic appearing No fever Born < 37 weeks gestational age INCLUSION CRITERIA Non-toxic with temperature > 38 C (100.4 F) < 36 C (96.5 F) measured
ONE of the following:
 Medical Coverage Policy Belimumab (Benlysta) EFFECTIVE DATE: 01 01 2012 POLICY LAST UPDATED: 11 21 2017 OVERVIEW Belimumab (Benlysta ) is indicated for the treatment of adult patients with active, autoantibody-positive,
Medical Coverage Policy Belimumab (Benlysta) EFFECTIVE DATE: 01 01 2012 POLICY LAST UPDATED: 11 21 2017 OVERVIEW Belimumab (Benlysta ) is indicated for the treatment of adult patients with active, autoantibody-positive,
Learning Objectives: At the end of this exercise, the student will be able to:
 Applications in Transfusion Medicine- A CBL Exercise- Student Guide 1 Title: Applications in Transfusion Medicine A CBL Exercise Purpose: At the conclusion of this exercise, students will be able to apply
Applications in Transfusion Medicine- A CBL Exercise- Student Guide 1 Title: Applications in Transfusion Medicine A CBL Exercise Purpose: At the conclusion of this exercise, students will be able to apply
Fever in Lupus. 21 st April 2014
 Fever in Lupus 21 st April 2014 Fever in lupus Cause of fever N= 487 % SLE fever 206 42 Infection in SLE 265 54.5 Active SLE and infection 8 1.6 Tumor fever 4 0.8 Miscellaneous 4 0.8 Crucial Question Infection
Fever in Lupus 21 st April 2014 Fever in lupus Cause of fever N= 487 % SLE fever 206 42 Infection in SLE 265 54.5 Active SLE and infection 8 1.6 Tumor fever 4 0.8 Miscellaneous 4 0.8 Crucial Question Infection
CASE-BASED SMALL GROUP DISCUSSION MHD II
 MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital
 Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
MHD I SESSION X. Renal Disease
 MHD I, Session X, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION X Renal Disease Monday, November 11, 2013 MHD I, Session X, Student Copy Page 2 Case #1 Cc: I have had weeks of diarrhea
MHD I, Session X, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION X Renal Disease Monday, November 11, 2013 MHD I, Session X, Student Copy Page 2 Case #1 Cc: I have had weeks of diarrhea
OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General
![OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General OB Well Baby Nursery Admission (Term) [ ] For specialty focused order sets for your patient, refer to: General](/thumbs/85/91909911.jpg) OB Well Baby Nursery Admission (Term) [3040000234] For specialty focused order sets for your patient, refer to: 3040000424 Neonatal Circumcision Order Set 3040000522 Neonatal Herpes Viral Order Set 3040000524
OB Well Baby Nursery Admission (Term) [3040000234] For specialty focused order sets for your patient, refer to: 3040000424 Neonatal Circumcision Order Set 3040000522 Neonatal Herpes Viral Order Set 3040000524
Lupus Related Kidney Diseases. Jason Cobb MD Assistant Professor Renal Division Emory University School of Medicine October 14, 2017
 Lupus Related Kidney Diseases Jason Cobb MD Assistant Professor Renal Division Emory University School of Medicine October 14, 2017 Financial Disclosures MedImmune Lupus Nephritis Kidney Biopsy Biomarkers
Lupus Related Kidney Diseases Jason Cobb MD Assistant Professor Renal Division Emory University School of Medicine October 14, 2017 Financial Disclosures MedImmune Lupus Nephritis Kidney Biopsy Biomarkers
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS
 Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Committee Approval Date: May 9, 2014 Next Review Date: May 2015
 Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
The Diagnosis of Lupus
 The Diagnosis of Lupus LUPUSUK 2017 This information booklet has been produced by LUPUS UK 2017 LUPUS UK LUPUS UK is the registered national charity for people with systemic lupus erythematosus (SLE) and
The Diagnosis of Lupus LUPUSUK 2017 This information booklet has been produced by LUPUS UK 2017 LUPUS UK LUPUS UK is the registered national charity for people with systemic lupus erythematosus (SLE) and
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Systemic Lupus Erythematosus
 Systemic Lupus Erythematosus Marc C. Hochberg, MD, MPH Professor of Medicine and Head, Division of Rheumatology University of Maryland School of Medicine CASE: HISTORY A 26-year-old woman is seen for migratory
Systemic Lupus Erythematosus Marc C. Hochberg, MD, MPH Professor of Medicine and Head, Division of Rheumatology University of Maryland School of Medicine CASE: HISTORY A 26-year-old woman is seen for migratory
Myositis and Your Lungs
 Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
11/9/2015. Childhood Nephrotic Syndrome: The Clinical Pathway. Learning Objectives. Nephrotic Syndrome - Definition. Proteinuria.
 Childhood Nephrotic Syndrome: The Clinical Pathway Cherry Mammen, MD, FRCPC, MHSc Douglas G. Matsell, MDCM, FRCPC Division of Nephrology, BC Children s Hospital Grand Rounds Nov 13th, 2015 Learning Objectives
Childhood Nephrotic Syndrome: The Clinical Pathway Cherry Mammen, MD, FRCPC, MHSc Douglas G. Matsell, MDCM, FRCPC Division of Nephrology, BC Children s Hospital Grand Rounds Nov 13th, 2015 Learning Objectives
Prof Dr Najlaa Fawzi
 1 Prof Dr Najlaa Fawzi is an acute highly infectious disease, characterized by vesicular rash, mild fever and mild constitutional symptoms. is a local manifestation of reactivation of latent varicella
1 Prof Dr Najlaa Fawzi is an acute highly infectious disease, characterized by vesicular rash, mild fever and mild constitutional symptoms. is a local manifestation of reactivation of latent varicella
.,Dr Ali Alkazzaz Babylon collage of medicine 2016
 .,Dr Ali Alkazzaz Babylon collage of medicine 2016 Lupus history Lupus is the Latin word for wolf 1 st used medically in the 10 th century Described clinically in the 19 th century Butterfly rash in 1845
.,Dr Ali Alkazzaz Babylon collage of medicine 2016 Lupus history Lupus is the Latin word for wolf 1 st used medically in the 10 th century Described clinically in the 19 th century Butterfly rash in 1845
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies
 Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
The only biologic approved to treat SLE: now with multiple delivery options
 The only biologic approved to treat SLE: now with multiple delivery options BENLYSTA (belimumab) Autoinjector SC Prefilled syringe IV Intravenous infusion Consider the options: visit Belimumab.com INDICATION
The only biologic approved to treat SLE: now with multiple delivery options BENLYSTA (belimumab) Autoinjector SC Prefilled syringe IV Intravenous infusion Consider the options: visit Belimumab.com INDICATION
Azathioprine Shared Care Guideline for GPs
 Indication: Azathioprine Shared Care Guideline for GPs Active rheumatoid arthritis and other types of inflammatory arthritis, systemic lupus erythematosus, dermatomyositis and polymyositis, vasculitis
Indication: Azathioprine Shared Care Guideline for GPs Active rheumatoid arthritis and other types of inflammatory arthritis, systemic lupus erythematosus, dermatomyositis and polymyositis, vasculitis
A summary of guidance related to viral rash in pregnancy
 A summary of guidance related to viral rash in pregnancy Wednesday 12 th July 2017 Dr Rukhsana Hussain Introduction Viral exanthema can cause rash in pregnant women and should be considered even in countries
A summary of guidance related to viral rash in pregnancy Wednesday 12 th July 2017 Dr Rukhsana Hussain Introduction Viral exanthema can cause rash in pregnant women and should be considered even in countries
Cedars Sinai Medical Center Pediatric Electives
 PE 235.03 MEDICAL GENETICS COURSE CHAIR: John M. Graham, M.D., ScD.. By arrangement - Please contact the Student Coordinator 1. Counseling techniques and the approach to the patient and family with hereditary
PE 235.03 MEDICAL GENETICS COURSE CHAIR: John M. Graham, M.D., ScD.. By arrangement - Please contact the Student Coordinator 1. Counseling techniques and the approach to the patient and family with hereditary
Red Stick ID Visual Diagnosis Questions August 22, 2014
 Red Stick ID Visual Diagnosis Questions August 22, 2014 James H. Brien, DO Case #1 The setting is a Pediatric Clinic in San Antonio, Texas on a Saturday in 1989. However, it could have been yesterday in
Red Stick ID Visual Diagnosis Questions August 22, 2014 James H. Brien, DO Case #1 The setting is a Pediatric Clinic in San Antonio, Texas on a Saturday in 1989. However, it could have been yesterday in
Beyond the Reflex Arc: An Evidence-Based Discussion of the Management of Febrile Infants
 Beyond the Reflex Arc: An Evidence-Based Discussion of the Management of Febrile Infants Cole Condra, MD MSc Division of Emergency Medical Services Children s Mercy Hospital October 1, 2011 Disclosure
Beyond the Reflex Arc: An Evidence-Based Discussion of the Management of Febrile Infants Cole Condra, MD MSc Division of Emergency Medical Services Children s Mercy Hospital October 1, 2011 Disclosure
2/23/18. Disclosures. Rheumatic Diseases of Childhood. Making Room for Rheumatology. I have nothing to disclose. James J.
 Making Room for Rheumatology James J. Nocton, MD Disclosures I have nothing to disclose Rheumatic Diseases of Childhood Juvenile Idiopathic Arthritis (JIA) Systemic Lupus Erythematosus (SLE) Juvenile Dermatomyositis
Making Room for Rheumatology James J. Nocton, MD Disclosures I have nothing to disclose Rheumatic Diseases of Childhood Juvenile Idiopathic Arthritis (JIA) Systemic Lupus Erythematosus (SLE) Juvenile Dermatomyositis
Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis
 GLOMERULONEPHRITIDES Vivette D Agati Jai Radhakrishnan Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis Heavy Proteinuria Renal failure Low serum Albumin Hypertension
GLOMERULONEPHRITIDES Vivette D Agati Jai Radhakrishnan Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis Heavy Proteinuria Renal failure Low serum Albumin Hypertension
Supplemental Figures and Legends
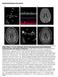 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086)
 Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity
Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity
CASE-BASED SMALL GROUP DISCUSSION
 MHD I, Session 13, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION SESSION 13 MHD I Autoimmunity November 10, 2016 STUDENT COPY MHD I, Session 13, STUDENT Copy Page 2 Case 1 CHIEF COMPLAINT: I am
MHD I, Session 13, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION SESSION 13 MHD I Autoimmunity November 10, 2016 STUDENT COPY MHD I, Session 13, STUDENT Copy Page 2 Case 1 CHIEF COMPLAINT: I am
Living with Lupus. LFA - Georgia Gary E Myerson MD Arthritis and Rheumatology of GA
 Living with Lupus LFA - Georgia Gary E Myerson MD Arthritis and Rheumatology of GA LUPUS A REALITY CHECK LUPUS A REALITY CHECK LUPUS A REALITY CHECK LUPUS A REALITY CHECK SLE 1.5 million Americans: some
Living with Lupus LFA - Georgia Gary E Myerson MD Arthritis and Rheumatology of GA LUPUS A REALITY CHECK LUPUS A REALITY CHECK LUPUS A REALITY CHECK LUPUS A REALITY CHECK SLE 1.5 million Americans: some
UNIT TWO: OBSTETRICS EDUCATIONAL TOPIC 17: MEDICAL AND SURGICAL COMPLICATIONS OF PREGNANCY
 UNIT TWO: OBSTETRICS EDUCATIONAL TOPIC 17: MEDICAL AND SURGICAL COMPLICATIONS OF PREGNANCY Rationale: Medical and surgical conditions may alter the course of pregnancy. Likewise, pregnancy may have an
UNIT TWO: OBSTETRICS EDUCATIONAL TOPIC 17: MEDICAL AND SURGICAL COMPLICATIONS OF PREGNANCY Rationale: Medical and surgical conditions may alter the course of pregnancy. Likewise, pregnancy may have an
Living with Lupus: An Insider s Perspective
 Living with Lupus: An Insider s Perspective Pamela Thorpe, MD, FACP Lupus Foundation of America, Inc. Philadelphia Tri-State Chapter Volunteer May 2014 My Own Story Is it Lupus Yet? The What What is this?
Living with Lupus: An Insider s Perspective Pamela Thorpe, MD, FACP Lupus Foundation of America, Inc. Philadelphia Tri-State Chapter Volunteer May 2014 My Own Story Is it Lupus Yet? The What What is this?
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Epatite B: fertilità, gravidanza ed allattamento, aspetti clinici e terapeutici. Ivana Maida
 Epatite B: fertilità, gravidanza ed allattamento, aspetti clinici e terapeutici Ivana Maida Positivity for HBsAg was found in 0.5% of tested women In the 70s and 80s, Italy was one of the European countries
Epatite B: fertilità, gravidanza ed allattamento, aspetti clinici e terapeutici Ivana Maida Positivity for HBsAg was found in 0.5% of tested women In the 70s and 80s, Italy was one of the European countries
Systemic Lupus Erythematosus Defining Lupus
 Autoimmune Resource and Research Centre Information Sheet Systemic Lupus Erythematosus Defining Lupus Lupus is a disorder of the immune system known as an autoimmune disease. In autoimmune diseases, the
Autoimmune Resource and Research Centre Information Sheet Systemic Lupus Erythematosus Defining Lupus Lupus is a disorder of the immune system known as an autoimmune disease. In autoimmune diseases, the
Cigna Drug and Biologic Coverage Policy
 Cigna Drug and Biologic Coverage Policy Subject Belimumab Table of Contents Coverage Policy... 1 General Background... 2 Coding/Billing Information... 4 References... 4 Effective Date... 11/15/2017 Next
Cigna Drug and Biologic Coverage Policy Subject Belimumab Table of Contents Coverage Policy... 1 General Background... 2 Coding/Billing Information... 4 References... 4 Effective Date... 11/15/2017 Next
Development of SLE among Possible SLE Patients Seen in Consultation: Long-Term Follow-Up. Disclosures. Background. Evidence-Based Medicine.
 Development of SLE among Patients Seen in Consultation: Long-Term Follow-Up Abstract # 1699 May Al Daabil, MD Bonnie L. Bermas, MD Alexander Fine Hsun Tsao Patricia Ho Joseph F. Merola, MD Peter H. Schur,
Development of SLE among Patients Seen in Consultation: Long-Term Follow-Up Abstract # 1699 May Al Daabil, MD Bonnie L. Bermas, MD Alexander Fine Hsun Tsao Patricia Ho Joseph F. Merola, MD Peter H. Schur,
Exam 1 Review. Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies
 Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
ACP Rheumatology Pearls. Adam Q Carlson MD Assistant Professor UVA Rheumatology
 ACP Rheumatology Pearls Adam Q Carlson MD Assistant Professor UVA Rheumatology Disclosures I have no personal or professional disclosures Case #1 27 yo woman with a history of systemic lupus complicated
ACP Rheumatology Pearls Adam Q Carlson MD Assistant Professor UVA Rheumatology Disclosures I have no personal or professional disclosures Case #1 27 yo woman with a history of systemic lupus complicated
Immune Thrombocytopenia (ITP)
 Immune Thrombocytopenia (ITP) ITP - What is it? ITP is a blood disorder affecting platelets in the blood. Platelets are small cells in your blood that help your blood to clot. In ITP the body s immune
Immune Thrombocytopenia (ITP) ITP - What is it? ITP is a blood disorder affecting platelets in the blood. Platelets are small cells in your blood that help your blood to clot. In ITP the body s immune
PEDIATRIC INFECTIOUS DISEASES UPDATE. Neonatal HSV. Recognition, Diagnosis, and Management Coleen Cunningham MD
 Neonatal HSV Recognition, Diagnosis, and Management Coleen Cunningham MD Important questions Who is at risk? When do you test? What tests do you perform? When do you treat? What is appropriate therapy?
Neonatal HSV Recognition, Diagnosis, and Management Coleen Cunningham MD Important questions Who is at risk? When do you test? What tests do you perform? When do you treat? What is appropriate therapy?
Alphaherpesvirinae. Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV)
 Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
CLINICAL GUIDELINES. Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P.
 CLINICAL GUIDELINES Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P. 11/2/15 Several practices routinely delay steroid injections
CLINICAL GUIDELINES Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P. 11/2/15 Several practices routinely delay steroid injections
Immunosuppressants. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
A RARE NEUROLOGICAL PRESENTATION OF SLE. Dr Yoganand M N Dr Prithvi P Nayak
 A RARE NEUROLOGICAL PRESENTATION OF SLE Dr Jayachandra Dr Yoganand M N Dr Prithvi P Nayak Presenter: Dr Shambhavi K R CHIEF COMPLAINTS A 30 year old lady hailing from Nepal presented to OPD with complaints
A RARE NEUROLOGICAL PRESENTATION OF SLE Dr Jayachandra Dr Yoganand M N Dr Prithvi P Nayak Presenter: Dr Shambhavi K R CHIEF COMPLAINTS A 30 year old lady hailing from Nepal presented to OPD with complaints
Patient #1. Rheumatoid Arthritis. Rheumatoid Arthritis. 45 y/o female Morning stiffness in her joints >1 hour
 Patient #1 Rheumatoid Arthritis Essentials For The Family Medicine Physician 45 y/o female Morning stiffness in her joints >1 hour Hands, Wrists, Knees, Ankles, Feet Polyarticular, symmetrical swelling
Patient #1 Rheumatoid Arthritis Essentials For The Family Medicine Physician 45 y/o female Morning stiffness in her joints >1 hour Hands, Wrists, Knees, Ankles, Feet Polyarticular, symmetrical swelling
SYSTEMIC LUPUS ERYTHEMATOSUS: CURRENT CONCEPTS AND CLINICAL PEARLS. Dr Sheila Vasoo Consultant Division of Rheumatology NUHS
 SYSTEMIC LUPUS ERYTHEMATOSUS: CURRENT CONCEPTS AND CLINICAL PEARLS Dr Sheila Vasoo Consultant Division of Rheumatology NUHS Listen to the Patient Concepts Diagnosis Immunopathogenesis Clinical Pearls Disease
SYSTEMIC LUPUS ERYTHEMATOSUS: CURRENT CONCEPTS AND CLINICAL PEARLS Dr Sheila Vasoo Consultant Division of Rheumatology NUHS Listen to the Patient Concepts Diagnosis Immunopathogenesis Clinical Pearls Disease
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
Rheumatology Primer: What Labs and When
 Rheumatology Primer: What Labs and When Irina Konon, MD Department of Internal Medicine Division of Rheumatology Medical College of Wisconsin Disclosures None 1 Objective Discuss principles of laboratory
Rheumatology Primer: What Labs and When Irina Konon, MD Department of Internal Medicine Division of Rheumatology Medical College of Wisconsin Disclosures None 1 Objective Discuss principles of laboratory
Disclosures. Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies. None
 Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies Sarah Goglin MD Assistant Professor of Medicine Division of Rheumatology Disclosures None 1 [footer
Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies Sarah Goglin MD Assistant Professor of Medicine Division of Rheumatology Disclosures None 1 [footer
Viral Infections. 1. Prophylaxis management of patient exposed to Chickenpox:
 This document covers: 1. Chickenpox post exposure prophylaxis 2. Chickenpox treatment in immunosuppressed/on treatment patients 3. Management of immunosuppressed exposed to Measles All children with suspected
This document covers: 1. Chickenpox post exposure prophylaxis 2. Chickenpox treatment in immunosuppressed/on treatment patients 3. Management of immunosuppressed exposed to Measles All children with suspected
SAUDI BOARD RESIDENCY TRAINING PROGRAM. (Physical Medicine and Rehabilitation) Part One Examination 2017
 SAUDI BOARD RESIDENCY TRAINING PROGRAM (Physical Medicine and Rehabilitation) Part One Examination 2017 Objectives: Eligibility: Part One Saudi Board Examination is designed to assess basic knowledge in
SAUDI BOARD RESIDENCY TRAINING PROGRAM (Physical Medicine and Rehabilitation) Part One Examination 2017 Objectives: Eligibility: Part One Saudi Board Examination is designed to assess basic knowledge in
CASE-BASED SMALL GROUP DISCUSSION
 MHD II, Session XII, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION Session XII MHD II April 21, 2014 STUDENT COPY Helpful Resource: ACP Medicine online available through LUHS Library Infectious
MHD II, Session XII, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION Session XII MHD II April 21, 2014 STUDENT COPY Helpful Resource: ACP Medicine online available through LUHS Library Infectious
Maternal-fetal Opiate Medical Home (MOMH) Jocelyn Davis DNP,CNM, RN, CEFMM Karen Frantz BSN, RNC
 Maternal-fetal Opiate Medical Home (MOMH) Jocelyn Davis DNP,CNM, RN, CEFMM Karen Frantz BSN, RNC Objectives 1. Discuss the effects of opiate addiction on mothers and infants. 2. Discuss a Medical Home
Maternal-fetal Opiate Medical Home (MOMH) Jocelyn Davis DNP,CNM, RN, CEFMM Karen Frantz BSN, RNC Objectives 1. Discuss the effects of opiate addiction on mothers and infants. 2. Discuss a Medical Home
Objectives. There Aren t Enough Hours in the Day
 There Aren t Enough Hours in the Day Medication monitoring and communication of results Objectives Review the types of testing being ordered on patients receiving therapies other than platforms Discuss
There Aren t Enough Hours in the Day Medication monitoring and communication of results Objectives Review the types of testing being ordered on patients receiving therapies other than platforms Discuss
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
Pediatric GU Dysfunction
 Pediatric GU Dysfunction Assessment of pediatric renal function Signs and symptoms Laboratory tests Radiological tests Nursing considerations Psychosocial and developmental considerations GU Disorders
Pediatric GU Dysfunction Assessment of pediatric renal function Signs and symptoms Laboratory tests Radiological tests Nursing considerations Psychosocial and developmental considerations GU Disorders
The chemical name of acyclovir, USP is 2-amino-1,9-dihydro-9-[(2-hydroxyethoxy)methyl]-6Hpurin-6-one; it has the following structural formula:
![The chemical name of acyclovir, USP is 2-amino-1,9-dihydro-9-[(2-hydroxyethoxy)methyl]-6Hpurin-6-one; it has the following structural formula: The chemical name of acyclovir, USP is 2-amino-1,9-dihydro-9-[(2-hydroxyethoxy)methyl]-6Hpurin-6-one; it has the following structural formula:](/thumbs/74/71271167.jpg) Acyclovir Ointment, USP 5% DESCRIPTION Acyclovir, USP, is a synthetic nucleoside analogue active against herpes viruses. Acyclovir ointment, USP 5% is a formulation for topical administration. Each gram
Acyclovir Ointment, USP 5% DESCRIPTION Acyclovir, USP, is a synthetic nucleoside analogue active against herpes viruses. Acyclovir ointment, USP 5% is a formulation for topical administration. Each gram
Sample Selection- Vignettes
 Sample Selection- Vignettes Rangaraj Selvarangan, BVSc, PhD, D(ABMM) Professor, UMKC School of Medicine Director, Microbiology, Virology and Molecular Infectious Diseases Laboratory Director, Laboratory
Sample Selection- Vignettes Rangaraj Selvarangan, BVSc, PhD, D(ABMM) Professor, UMKC School of Medicine Director, Microbiology, Virology and Molecular Infectious Diseases Laboratory Director, Laboratory
LUPUS. and Medication LUPUSUK 2015
 9 LUPUS and Medication LUPUSUK 2015 LUPUS and Medication The types of drugs used in lupus can be broadly divided into those that treat the disease itself (e.g. hydroxychloroquine and prednisolone) and
9 LUPUS and Medication LUPUSUK 2015 LUPUS and Medication The types of drugs used in lupus can be broadly divided into those that treat the disease itself (e.g. hydroxychloroquine and prednisolone) and
Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study
 Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study BMJ 2017; 356 doi: https://doi.org/10.1136/bmj.j895 (Published
Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study BMJ 2017; 356 doi: https://doi.org/10.1136/bmj.j895 (Published
Burrowing Bugs in a 5 week-old that Mite be Difficult to Diagnosis
 Burrowing Bugs in a 5 week-old that Mite be Difficult to Diagnosis Farbod Bahadori-Esfahani,MD Pediatrics LSU Health Shreveport Louisiana Chapter AAP Red Stick Potpourri Disclosure I have nothing to disclose
Burrowing Bugs in a 5 week-old that Mite be Difficult to Diagnosis Farbod Bahadori-Esfahani,MD Pediatrics LSU Health Shreveport Louisiana Chapter AAP Red Stick Potpourri Disclosure I have nothing to disclose
History Data Panel. Case 030 Preg Trauma. Presenting Complaint Altered mental status s/p MVC. Person Giving Information EMS
 History Data Panel Presenting Complaint Altered mental status s/p MVC Person Giving Information EMS History of Present Illness 28 year old woman, 35 weeks pregnant per report of her husband the passenger.
History Data Panel Presenting Complaint Altered mental status s/p MVC Person Giving Information EMS History of Present Illness 28 year old woman, 35 weeks pregnant per report of her husband the passenger.
Patient Encounters in the Primary Care Setting
 Patient Encounters in the Primary Care Setting Carmine D Amico, D.O. Clinical Cases Overview Learning objectives Clinical case presentations Questions for audience participation 1 Clinical Cases Learning
Patient Encounters in the Primary Care Setting Carmine D Amico, D.O. Clinical Cases Overview Learning objectives Clinical case presentations Questions for audience participation 1 Clinical Cases Learning
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
Chapter 06 Lecture Outline. See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes.
 Chapter 06 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. 2012 Pearson Permission Education,
Chapter 06 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. 2012 Pearson Permission Education,
SLE-key Case Studies
 SLE-key Case Studies Ellen M. Field, M.D. Lehigh Valley Health Network, Bethlehem, PA Donald E. Thomas, Jr., M.D., FACP, FACR, RhMSUS, CCD Arthritis and Pain Assoc. of PG County, Greenbelt, MD Case Study
SLE-key Case Studies Ellen M. Field, M.D. Lehigh Valley Health Network, Bethlehem, PA Donald E. Thomas, Jr., M.D., FACP, FACR, RhMSUS, CCD Arthritis and Pain Assoc. of PG County, Greenbelt, MD Case Study
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin
 Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Document Information Version: 2 Date: 28 th December 2013 Authors (incl. job title): Professor David Rees (Consultant
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Document Information Version: 2 Date: 28 th December 2013 Authors (incl. job title): Professor David Rees (Consultant
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
A Challenging Case: Von Willebrand Disease and Pulmonary Hypertension in Pregnancy
 A Challenging Case: Von Willebrand Disease and Pulmonary Hypertension in Pregnancy Diana S. Wolfe, MD, MPH Assistant Professor Department of Obstetrics & Gynecology and Women s Health Associate Fellowship
A Challenging Case: Von Willebrand Disease and Pulmonary Hypertension in Pregnancy Diana S. Wolfe, MD, MPH Assistant Professor Department of Obstetrics & Gynecology and Women s Health Associate Fellowship
NORTH AND EAST DEVON HEALTHCARE COMMUNITY SHARED CARE PRESCRIBING GUIDELINE
 NORTH AND EAST DEVON HEALTHCARE COMMUNITY SHARED CARE PRESCRIBING GUIDELINE http://www.devonpct.nhs.uk/treatments/ne_devon_shared_care_guidelines.aspx#a Azathioprine Treatment of rheumatological conditions
NORTH AND EAST DEVON HEALTHCARE COMMUNITY SHARED CARE PRESCRIBING GUIDELINE http://www.devonpct.nhs.uk/treatments/ne_devon_shared_care_guidelines.aspx#a Azathioprine Treatment of rheumatological conditions
