Three-Dimensional Reconstruction of Normal and Early Glaucoma Monkey Optic Nerve Head Connective Tissues
|
|
|
- Chrystal Harrison
- 5 years ago
- Views:
Transcription
1 Three-Dimensional Reconstruction of Normal and Early Glaucoma Monkey Optic Nerve Head Connective Tissues Claude F. Burgoyne, 1,2 J. Crawford Downs, 1,2 Anthony J. Bellezza, 2 and Richard T. Hart 2 PURPOSE. To introduce high-resolution, digital three-dimensional (3-D) reconstruction of the connective tissues of the optic nerve head (ONH). METHODS. Trephinated ONH and peripapillary sclera from both eyes of three monkeys with early glaucoma (EG; one eye normal, one eye given laser-induced EG) were embedded in paraffin and serial sectioned at 3- m thickness from the vitreous surface through the orbital optic nerve, with the embedded tissue block face stained and imaged after each cut. Each image was aligned, and then the scleral canal wall, sclera, border tissue of Elschnig, Bruch s membrane, lamina cribrosa, optic nerve septa, pial sheath, and vasculature were delineated as unique objects. Delineated images were stacked, color mapped, and volume rendered and then serial sagittal and transverse digital sections of the resultant voxel geometries were viewed and measured. RESULTS. Substantial differences in the 3-D architecture of the peripapillary sclera, scleral canal wall, and lamina cribrosa were present among the three normal eyes. All three EG eyes displayed permanent posterior deformation of the central lamina cribrosa, as well as expansion of the anterior and posterior neural canal openings in comparison with their respective contralateral normal control eyes. Peripherally, whereas laminar deformation was greatest inferiorly or superiorly in all three EG eyes, statistically significant deformation was present in all four quadrants of all three eyes. CONCLUSIONS. High-resolution, digital 3-D reconstructions of the load-bearing connective tissues of the monkey ONH confirm that the ONH connective tissues are profoundly altered at the onset of detectable ONH surface change in experimental glaucoma. (Invest Ophthalmol Vis Sci. 2004;45: ) DOI: /iovs The connective tissues of the peripapillary sclera, scleral canal wall, and lamina cribrosa have long been thought to play a central role in the pathophysiology of glaucomatous From the 1 LSU Eye Center, Louisiana State University Health Sciences Center, New Orleans, Louisiana; and the 2 Department of Biomedical Engineering, Tulane University, New Orleans, Louisiana. Supported in part by National Eye Institute Grants R01EY (CFB) and P30EY (departmental core grant); a grant from the American Health Assistance Foundation, Rockville, Maryland (CFB); a grant from The Whitaker Foundation, Arlington, Virginia (CFB); a Career Development Award (CFB); an unrestricted departmental grant (LSU Eye Center) from Research to Prevent Blindness, Inc.; and a graduate student stipend from the Board of Regents, State of Louisiana (AJB). Submitted for publication January 9, 2004; revised July 2, 2004; accepted August 18, Disclosure: C.F. Burgoyne, None; J.C. Downs, None; A.J. Bellezza, None; R.T. Hart, None The publication costs of this article were defrayed in part by page charge payment. This article must therefore be marked advertisement in accordance with 18 U.S.C solely to indicate this fact. Corresponding author: Claude F. Burgoyne, LSU Eye Center, 2020 Gravier Street, Suite B, New Orleans, LA 70112; cburgo@lsuhsc.edu. damage to the retinal ganglion cell axons within the optic nerve head (ONH). To date, these tissues have been extensively studied using light and electron microscopy 1 42 and initial attempts have been made at three-dimensional (3-D) reconstruction. 43,44 However, until now, the high-resolution, digital, 3-D reconstructions necessary to model accurately the levels of intraocular pressure (IOP) related stress (force/crosssectional area) and strain (local deformation) to which these structures are subjected have not been attempted. Modeling IOP-related stress and strain within the ONH connective tissues is important for several reasons. First, regardless of the mechanism of insult or the level of IOP at which it occurs, we propose that IOP-related connective tissue stress and strain underlies and predicts the onset and progression of glaucomatous axonal insult. From a biomechanical standpoint, the pathophysiology of the axons in the glaucomatous optic neuropathies is likely to be multifactorial, with the principal mechanisms of axonal insult (astrocyte and glial cell activation, ischemia, and physical compression) acting alone or together according to the region of the ONH and the stage of underlying connective tissue and cellular involvement. 45,46 However, we propose that it is a defining feature of the glaucomatous optic neuropathies that, regardless of mechanism, the distribution of IOP-related stress and strain within the ONH connective tissues underlies and predicts the location of axonal insult within the ONH, whether the insult occurs at normal or elevated levels of IOP. 45,46 Second, we propose that the distribution of IOP-related stress and strain also underlies and predicts the pattern of connective tissue damage (referred to as mechanical failure) and that this pattern of connective tissue damage both explains the clinical phenomenon known as glaucomatous cupping and is a second defining feature of the neuropathy. By this, we mean that for an individual ONH to demonstrate classic glaucomatous cupping, its connective tissues must become damaged and undergo mechanical failure in a process that is again governed by the distribution of IOP-related stress and strain, regardless of the level of IOP at which it occurs. 45,46 IOP-related stress and strain within the connective tissues of the ONH can be studied using finite element modeling, which is an engineering technique for modeling the distribution of stress and strain within complicated structures. Constructing a finite element model requires a digital geometry of the structure being modeled and estimates of the structure s material properties (stiffness) and boundary and loading conditions For the past 8 years, we have worked on all three components of this process to build finite element models of the normal and EG monkey ONH We have previously demonstrated permanent deformation of the ONH connective tissues (the onset of mechanical failure) within serial histologic sections of monkey eyes with early experimental glaucoma. 41 In the present report, we introduce our method for high-resolution, digital, 3-D reconstruction of the ONH connective tissues and describe its use to compare normal and EG ONH connective tissue architecture within three new monkeys with early experimental glaucoma in one eye. Investigative Ophthalmology & Visual Science, December 2004, Vol. 45, No Copyright Association for Research in Vision and Ophthalmology
2 IOVS, December 2004, Vol. 45, No. 12 ONH Connective Tissue Damage in Glaucoma 4389 MATERIALS AND METHODS Animals All animals were treated in accordance with the ARVO Statement for the Use of Animals in Ophthalmic and Vision Research. Three male cynomolgus monkeys, approximately 8 years of age, were used (Table 1). ONH Surface Compliance Testing and EG We have described our confocal scanning laser tomography (CSLT)- based (TopSS, Laser Diagnostics Technology, San Diego, CA) ONH surface compliance testing strategy. 41,55 Briefly, compliance testing involved measurement of the parameter mean position of the disc (MPD), which describes the position of the surface of the ONH relative to the peripapillary retinal nerve fiber layer. Both eyes of each monkey were compliance tested on three separate occasions to provide the prelaser MPD Baseline 95% confidence interval (CI) for normal eyes. Then one eye of each monkey was given laser-induced experimental glaucoma (EG eye), and compliance testing of both eyes was repeated at 2-week intervals until the onset of permanent posterior deformation of the ONH surface (defined as MPD Baseline 95% CI below prelaser MPD Baseline 95% CI) in the EG eye on two successive postlaser imaging sessions, at which point the monkey was killed (Fig. 1). Monkey Euthanasia and Fixation For each monkey, deep pentobarbital anesthesia was induced, both eyes were cannulated with a 27-gauge needle, and the IOP was set to 10 mm Hg by using an adjustable saline reservoir. After a minimum of 30 minutes, the monkey was perfusion fixed via the descending aorta with1lof4%buffered hypertonic paraformaldehyde solution followed by 6Lof5% buffered hypertonic glutaraldehyde solution. Both the paraformaldehyde and glutaraldehyde were buffered in 1 M Sorenson s solution (0.15 M KH 2 PO 4 and 0.85 M Na 2 HPO 4 ). Osmolarity of each solution was approximately 0.4 osmol/l. After perfusion fixation, IOP was maintained for 1 hour, after which each eye was enucleated, all extraorbital tissues were removed, and the anterior chamber was removed 2 to 3 mm posterior to the limbus. By gross inspection, perfusion was excellent in all six eyes. The posterior scleral shells with intact ONH, choroid, and retina were placed in 5% glutaraldehyde solution for long-term storage. Generation of the Aligned Serial Section Images for Each ONH For each eye, the ONH and surrounding peripapillary sclera were trephined (6-mm diameter), pierced with four to seven 10-0 polypropylene alignment sutures (Prolene; Ethicon, Somerville, NJ), and photographed to document the position of the alignment sutures in the clinical ONH surface (Fig. 2). The tissue was dehydrated through a graded series of ethanols, cleared in chloroform, and infiltrated with paraffin (TissuePrep 2; Fisher Scientific, Pittsburgh, PA) using an automatic tissue processor (Tissue-Tek II; Ames Division, Miles Laboratories, Inc., Elkhart, IN). The specimen was oriented in the desired position, embedded in paraffin, and mounted on a microtome (RM2165; Leica, Wetzlar, Germany), so that the vitreous side of the ONH surface was visible in the block in a clinically appropriate orientation (Fig. 2). A pixel chip camera (Spot RT; Diagnostic Instruments, Sterling Heights, MI) was positioned so that an image of the centered, embedded tissue block surface could be acquired at a resolution of m per pixel (Fig. 3). The block was then sectioned without imaging until the cutting plane was just superficial to the internal limiting membrane of the retina. At that point, a 1:1 (vol/vol) mixture of Ponceau S and acid fuchsin stains, which stained only the exposed connective tissues, was manually applied to the surface of the tissue block, the excess stain was blotted away, and the stained surface of the embedded tissue block was imaged. Then another 3.0- m section was cut away, and the staining and imaging process was repeated. TABLE 1. Animal and Eye Data for Three Cynomolgus Monkeys State of Eye at Perfusion Optic Nerve Percent Neural Area Axial Length (mm) (IOP 10 mm Hg) Optic Nerve Total Area (mm 2 ) Optic Nerve Neural Area (mm 2 ) Serial Section Images (n) Duration of Measured IOP Elevation (days)* IOP (mm Hg) IOP (mm Hg) Before Death Condition Maximum (postlaser) Normal Normal (prelaser) Age (y) Eye Weight (kg) Monkey No. ID 1 AA Right Normal Left Early glaucoma AA Right Early glaucoma Left Normal AA4C Right Normal Left 9 20 NA Early glaucoma * Estimated time from detection of elevated IOP to death. Axial length at an IOP of 10 mm Hg during the final compliance testing session. Connective tissues of the pial sheath not included in the calculation. Ratio of neural area to total area (excluding the pial sheath). IOP did not exceed the normal 95% confidence intervals on two successive occasions in this eye.
3 4390 Burgoyne et al. IOVS, December 2004, Vol. 45, No. 12 FIGURE 1. Postlaser IOP and MPD Baseline in both eyes of all three monkeys. IOP and MPD Baseline 95% CI (surface deformation) were plotted for both the normal (E) and EG eyes (Œ) of all three monkeys at each post-laser imaging session. Horizontal lines: the upper and lower boundaries of the 95% CI for the mean of the three prelaser, normal compliance testing sessions (dashed lines, normal eyes; dotted lines, EG eyes). Monkeys were to be killed at the onset of CSLT-detected ONH surface change, which was defined as the onset of permanent posterior deformation of the ONH surface (MPD Baseline 95% CI beneath the normal prelaser range) at two consecutive postlaser imaging sessions. However, the decision to kill each monkey was, by necessity, empiric, in that the systems for rapid processing, statistical analysis, and graphing the data for each monkey were not in place at the time of postlaser compliance testing. Therefore, monkeys 2 and 3 were killed 3 weeks and monkey 1 six weeks after the onset of CSLT detection of ONH surface change (permanent posterior deformation of the ONH surface). The delayed death of monkey 1 was the result of an unexpected decline in the MPD Baseline in the normal eye, which eventually returned to normal. Thus, for each ONH, imaging began at the vitreous retinal interface and continued through the lamina cribrosa, approximately 200 m into the orbital optic nerve. Depending on the degree of tilt of the embedded tissue, the number of sections obtained per eye ranged from 222 to 411. Each section image was aligned in the z-direction (anterior to posterior) by using custom software to register the cut ends of the embedded polypropylene sutures that were visible within each section (Fig. 4). Voxel Geometry Construction and Visualization The principal steps of voxel geometry construction were performed for both eyes of each monkey by a single operator. A separate operator processed the voxel geometry for visualization. The entire process is depicted in Figures 5 and 6 and outlined in the following sections. Object Segmentation within Each Section Image. Manual and semiautomated selection tools developed within custom and FIGURE 2. Generation of the aligned serial section images for each ONH. (A) CSLT image of the normal right eye of monkey 1; (B) Photograph of the 6-mm diameter trephined optic nerve head and peripapillary sclera, showing the polypropylene alignment sutures (arrows) before embedding. (C) Representative image of an individual stained section before alignment, showing the cut ends of the registration sutures (small blue dots) in the subarachnoid space and dural sheath at the 3:00, 4:30, 7:00, and 9:00 o clock positions (see also Fig. 4). Because the sutures in each section image are also present in the color photograph of the surface of the trephined ONH (B), the regional orientation of the 3-D geometry (superior, inferior, nasal, and temporal within the ONH and orbital optic nerve) can be linked to the clinical orientation of the ONH surface. (D) The same section, z-axis (anterior-to-posterior) aligned. Black borders indicate where data have been lost due to the shift within the x- and y-axes necessary to bring this image into alignment with all the images that precede it.
4 IOVS, December 2004, Vol. 45, No. 12 ONH Connective Tissue Damage in Glaucoma 4391 FIGURE 3. Imaging the stained, embedded tissue block surface. The camera (bottom left) is positioned relative to the microtome, so that the image of the stained, centered, embedded tissue block surface is acquired at a resolution of m per pixel after each 3- m section is cut away. Custom software is used for image inspection, naming, and storage; an image undergoing this process is visible on the acquisition computer monitor (top right). commercial software (Photoshop, ver 7.0; Adobe Systems, Inc., San Jose, CA) were used to isolate the connective tissues in the individual section images. First, the neural boundary, defined as the outermost extent of the neural tissues in the scleral canal, was segmented in each section image (Fig. 5). This line marked the boundary between the neural and connective tissues starting from the anteriormost sclera as it forms the anterior scleral canal wall, and continuing through the posterior pial sheath. The neural boundary thus demarcates the area in which the lamina cribrosa and retrolaminar optic nerve septa are located. Second, a mask for the nonconnective tissue areas was generated for each section image, covering the choroid, retina, nerve fiber layer, embedding medium, and subarachnoid space. The inverse of this mask covered all connective tissue objects present in each section image, including the sclera, Bruch s membrane, the border tissue of Elschnig, and the pial and dural sheaths of the optic nerve. Third, the central retinal vessels in each section image were manually segmented from the vitreous interface to the final posterior section. Finally, an automated, adaptive thresholding algorithm was applied to sequential pixel regions of the filled neural boundary to segment the lamina cribrosa and optic nerve septa from the surrounding neural tissues. The accuracy of object segmentation within each section image was then reviewed, using custom software that allowed the rapid and simultaneous viewing of each section image with its constituent segmented objects as individual and grouped overlays. Voxel Geometry Construction. For each segmented section image, the pixels for each object were assigned a standard color and saturation (Fig. 6). For each ONH, the aligned, segmented section images were compiled into a binary volume of m voxels, which ranged in size from approximately 300 to 600 megabytes. Because only the connective tissue pixels were visible in each segmented section image, only the connective tissue voxels were visualized within the volume. We thus refer to these 3-D reconstructions of the connective tissue voxels as connective tissue voxel geometries or voxel geometries. Voxel Geometry Visualization. Voxel geometries were rendered with the open-source OpenDX data visualization software ( provided in the public domain by IBM, Armonk, NY) or custom visualization software built using the Visualization Toolkit (VTK) library ( provided in the public domain by Kitware, Clifton Park, NY). Because of the size of the geometries, the ability to interact dynamically with the entire geometry was not initially possible. Therefore, four sets of standard views were generated for each ONH. First, a software-viewing camera was rotated about the vertical axis of the intact geometry (Fig. 6C), to obtain images in 2 to 5 increments (not shown). Second, standard views of serial transverse, sagittal (vertical), and coronal (horizontal) sections through each geometry were generated (Fig. 5). Custom software constructed in Visual Basic C (Microsoft, Redmond, WA) was used to visualize each standard view for both eyes of a given monkey (Fig. 7). Qualitative and Quantitative Assessment of the Digital Geometries All qualitative comparisons were performed between the two eyes of each monkey using the simultaneous bilateral viewing software, as just described (Fig. 7). Measurements of (1) anterior laminar position, (2) laminar thickness, (3) horizontal and vertical neural canal diameter, and (4) peripapillary scleral thickness were performed within the five central horizontal and vertical digital section images (each section, 1 voxel wide) for each eye by a single observer, using a modified version of software that has been described previously (Fig. 8). 41,53 Anterior laminar position and thickness data for each eye were assessed overall and by central, superior, and inferior (vertical sections) or central, nasal, and temporal (horizontal sections) regions. Neural canal diameter was measured at its internal (Bruch s membrane) and external (posterior scleral canal) openings within each section and regionalized into horizontal and vertical data for each eye. Peripapillary scleral thickness was measured at the posterior scleral canal opening within each section and pooled into superior and inferior (vertical sections) or nasal and temporal (horizontal sections) regions for each eye. FIGURE 4. The z-axis (anterior-toposterior) alignment of each stained section image. (A) Stained section image with the polypropylene suture used for orientation and alignment identified (dark blue box). (B) Crosshairs (light blue box) overlay the center of the suture. (C) Location saved along with protocol details.
5 4392 Burgoyne et al. IOVS, December 2004, Vol. 45, No. 12 FIGURE 5. Neural canal terminology and object segmentation within each section image. The neural canal consists of a prescleral and a scleral component. The prescleral neural canal extends from its internal opening (the clinically visible opening in Bruch s membrane, known as Bruch s membrane flange) along the inner surface of the border tissues of Elschnig to their insertion into the sclera. The scleral canal portion of the neural canal extends from the anterior to the posterior surface of the sclera (the external neural canal opening or posterior scleral canal opening). The principal boundaries of the neural canal are (A) magnified and (B) labeled within a representative histologic section so as to provide an orientation to the same structures within a representative section of a voxel geometry (C). Labels in (B): a, Bruch s membrane away from the neural canal opening; b, Bruch s membrane flange, the clinically visible internal neural canal opening, which is the junction of Bruch s membrane into the border tissue of Elschnig; c, the border tissue of Elschnig; d, the anterior or internal scleral canal opening, which is the start of the scleral portion of the neural canal; e, the posterior or external scleral canal opening, which marks the posterior extent of the neural canal and is the site of the posterior laminar beam and pial sheath insertions into the sclera; and f, the pial sheath. In each section image, the neural boundary (D), defined as the outermost extent of the neural tissues within the neural canal and pial sheath, is segmented. Using a combination of manual and semiautomated programs, the border and flange tissues (E), sclera (F), and pial sheath (G) pixels and the central retinal vessels not shown separately but red in (H) are segmented and colorized. Finally, an automated, adaptive thresholding algorithm is applied to sequential pixel regions of the filled neural boundary to segment the lamina cribrosa and optic nerve septa (blue in C and H) from the surrounding neural tissues. A nested ANOVA was used to assess the effects of region (central, superior, inferior, nasal, and temporal) and treatment group (normal and EG) on the parameters anterior laminar position and laminar thickness, both overall and between the eyes of each monkey. A second nested ANOVA evaluated the effects of quadrant (superior, inferior, nasal, and temporal) and treatment group on posterior scleral thickness, both overall and between the eyes of each monkey. A third nested ANOVA assessed the overall effects of treatment group on the parameters vertical and horizontal anterior neural canal diameter at Bruch s membrane and the posterior scleral canal opening, both overall and between the eyes of each monkey. Optic Nerve Neural Area Measurements For each eye, the cross-sectional areas of the neural and connective tissues of the optic nerve were measured in a single section image located 20 sections (approximately 60 m) beyond the last section image having recognizable lamina cribrosa (i.e., the last section image containing transversely oriented connective tissue fibers). The selected section image was binarized and the area within the neural boundary (excluding the pial sheath connective tissues immediately surrounding the nerve) was thresholded using image-processing software (Photoshop ver. 5.5; Adobe Systems, Inc.) so as to isolate the connective tissue septa. The areas of the neural and connective tissues within the neural boundary were then calculated with custom software. To increase our ability to compare these areas among eyes that had been cut at different angles, the ratio of neural area to total area (percent neural area relative to total ONH area) was then calculated for each eye. RESULTS Descriptive data for the three monkeys and six eyes are reported in Table 1. Experimental Glaucoma Monkeys 2 and 3 were killed three weeks and monkey 1 six weeks after the onset of CSLT detection of a change (permanent posterior deformation) in the ONH surface. The delay in killing monkey 1 was the result of an unexpected decrease in the MPD Baseline in the normal eye, which eventually returned to normal. In monkeys 1 and 2, IOP elevations were moderate, with only one measurement higher than 30 mm Hg. In monkey 3, elevated IOP was not detected (Table 1, Fig. 1). Postlaser IOP and MPD Baseline data for the study eye and the contralateral normal eye are shown for each monkey in Figure 1. In monkeys 1 and 2, the percentage of neural area of the EG eye was less than that of the normal eye (4.7% and 4.5% less, respectively), whereas in monkey 3, the percentage of neural area of the EG eye was 0.6% larger than that of the normal eye (Table 1).
6 IOVS, December 2004, Vol. 45, No. 12 ONH Connective Tissue Damage in Glaucoma 4393 FIGURE 6. Voxel geometry construction (A C) and visualization (D F). Within each aligned stained section image (A), the principal objects are segmented (see Fig. 5) and the pixels subserving each object are assigned a standard color and saturation (B): orange, anterior scleral canal border and flange tissue; yellow, sclera; light blue, lamina; dark blue, pial sheath; red, central retinal vasculature. (C) For each ONH, the section images are then stacked to make a voxel geometry in which the connective tissue components are isolated. The intact geometry is observed by using standard rotating views. The anterior surface is shown. Serial transverse (D), vertical (E), and horizontal (F) sagittal digital sections for each ONH are also available for simultaneous bilateral viewing (see Fig. 7). N, nasal; T, temporal; I, inferior; S, superior. Because it was not possible to control the position of the tissue tightly during embedding, each ONH was obliquely embedded (minimally to substantially) relative to the cutting plane of the microtome. This optic nerve head was embedded with the superior temporal tissue (top left portion of the image) closest to the plane and the inferior nasal tissue (bottom right portion of the image) farther back. Thus, the section plane in (A) proceeds through the dura (d), expanded arachnoid space (a), pia (p), retrolaminar optic nerve (on), lamina (l), central vascular tree (cv), prelaminar neural bundles (pla), Bruch s membrane flange, the junction with the border tissues of Elschnig (bt), and the choroid (c). The oblique embedding angle can be further appreciated within the central vertical (E) and horizontal (F) digital sagittal sections, which demonstrate the position of the connective tissues within the stacked sections (top, vitreous; bottom, orbit) relative to the orientation of the cutting plane, which is horizontal (proceeding from top to bottom) in these views. Physiologic Variation within the Three Normal Monkey Eyes Surface Views of the Intact Geometry. The clinical (CSLT) and histologic (voxel geometry) anterior scleral canal openings of each ONH are visible in Figure 9. Because the scleral voxels are partially translucent, the peripapillary sclera immediately adjacent to the canal wall is most transparent due to its relative thinness as the neural tissues become myelinated and expand to form the orbital optic nerve. Standard Serial Digital Sections. Representative horizontal and vertical sections through the midcanal are shown in Figure 10. Quantitative measurements of the central five horizontal and vertical digital sections from each eye are reported in Table 2. Note that the peripapillary sclera and lamina of the normal eye of monkey 2 are substantially thicker than they are in monkeys 1 and 3. In addition, the scleral canal is less oblique relative to the plane of the sclera in monkey 2, compared with monkeys 1 and 3. In monkey 2, the canal passes almost perpendicular to the sclera, whereas in monkeys 1 and 3 the canal shows the more common nasal-to-temporal oblique orientation. Comparison of the Normal and EG ONH of Each Monkey Standard Serial Digital Sections. The horizontal and vertical sections in Figure 10 and the quantitative measurements in Table 2 demonstrate marked posterior deformation of the central lamina in the EG eyes of all three monkeys. Central deformation was greater than peripheral deformation in all three EG eyes (greater in monkeys 1 and 3 than in monkey 2). Peripheral deformation of the lamina at its insertion into the scleral canal wall was visible in the superior, inferior, nasal, and temporal peripheral canal sections of monkey 1 (Fig. 11). Although the greatest peripheral laminar deformation was seen in the inferior (monkeys 1 and 3) and superior (monkey 2) laminar insertion zones (Table 2), statistically significant deformation of the peripheral lamina occurred in all four quadrants of all three EG eyes, relative to their respective contralateral normal control eyes (Table 2). Mild to moderate thickening of both the lamina and sclera was present at the posterior scleral canal opening in most regions of the EG eyes (Table 2). Expansion of the neural canal at both its internal (Bruch s membrane) and external (posterior scleral canal) openings was present in both the horizontal and vertical axes of two of the three EG eyes (Table 2). DISCUSSION Accurately characterizing the 3-D geometry of the lamina cribrosa within the scleral canal has been the goal of a large and important body of research In the present report, we introduce a new method for high-resolution, digital 3-D reconstruction of the ONH tissues and use it to visualize and measure differences within the connective tissue voxel geometries of both eyes of three monkeys with induced EG in one eye. Several aspects of both the method and findings are important to discuss. Our method achieves high resolution for three reasons. First, we acquired images at relatively high magnification compared with the structures being modeled ( m pixel). Second, we acquired new z-axis data every 3 m (achieving a
7 4394 Burgoyne et al. IOVS, December 2004, Vol. 45, No. 12 FIGURE 7. Custom bilateral viewing software is used to visualize digital sections of the delineated geometries of both eyes of monkey 1. The right eye (RE) is normal and the left eye (LE) has EG. To compare the geometries of the right and left eyes of an individual monkey, custom bilateral viewing software was built to allow the rotating geometries themselves (not shown) or digital sections of the geometries from both eyes of a monkey to be viewed simultaneously (central panels of A, transverse; B, horizontal; C, vertical). In the central panels for parts (B) and (C), the normal right eye is the top image and the EG left eye is the bottom image. Within the central panels, the small guide images marked with a thick green line depict the location of the viewed digital section. The CSLT image is present for reference to the ONH surface. When necessary, separate software was used to view the serial section images of each eye at the same time (the far left and right panels in A, B, and C). Viewed in this way, the serial section images (our raw data) served as an immediate reference for observations made within the digital sections of the delineated geometries m voxel) by cutting a 3- m section and obtaining a fresh, unstained block face after each cut. Third, we acquired each of the 200 to 600 section images for a given ONH with perfect 3-D registration, because we imaged the cut surface of the embedded tissue block rather than free histologic sections that shrink and become distorted relative to one another once cut from the block. The voxel geometries reported herein reconstruct the entire passageway for the ganglion cell axons through the wall of the eye. We propose that this passageway should be referred to, both clinically and histologically, as the neural canal, which extends from its internal opening at Bruch s membrane to its external opening at the posterior scleral canal and consists of prescleral and scleral components. The prescleral portion of the neural canal extends from its internal opening at the optic disc (the clinically visible opening in Bruch s membrane) along the inner surface of the border tissues of Elschnig to their insertion into the sclera. The scleral canal portion of the neural canal extends from the anterior to the posterior surface of the sclera. Our concept of the neural canal has several important implications regarding the relationship between the clinical disc (Bruch s membrane opening or the internal entrance to the neural canal) and the actual anterior and posterior openings in the sclera. First, characterizing the architecture of the entire neural canal may be more important than estimating the size and shape of the optic disc (its clinically visible internal opening). We have previously reported that differences in the architecture of the scleral portion of the neural canal (large size, elliptical shape, and thin peripapillary sclera) should markedly increase the level of IOP-related connective tissue stress for a given level of IOP. 51 The 3-D reconstructions presented herein suggest that the size and shape of the clinical disc may not adequately convey the architectural complexity of the underlying scleral canal. Second, two features of the neural canal determine the thickness of the peripapillary sclera (Fig. 5C): (1) the degree to which the nerve expands within the neural canal, which can be defined by the difference in size of the posterior relative to the anterior neural canal opening; and (2) the oblique orienta-
8 IOVS, December 2004, Vol. 45, No. 12 ONH Connective Tissue Damage in Glaucoma 4395 FIGURE 8. Screen shot from the custom histomorphometry program of a representative central horizontal digital section showing laminar, neural canal, and peripapillary scleral measurements. Using a modified version of previously described programs, 41,53 an operator placed the following landmark points within each digital section image: the termination of Bruch s membrane (light green), the anterior insertion of the lamina into the sclera (red with a green border), the anterior and posterior surfaces of the lamina cribrosa (red), the posterior scleral canal opening, defined as the posteriormost aspect of the insertion of the load-bearing sclera into the neural canal (orange), and the anterior and posterior surfaces of the peripapillary sclera (dark green). Once the section was marked, custom software divided the distance between the two Bruch s membrane termination points into nine equidistant measurement locations, dropped perpendicular lines to the anterior lamina cribrosa, and extended those lines normal to the anterior laminar surface down to the posterior laminar surface. Automatic measures of the following parameters were thus generated: nine equally spaced measurements of anterior laminar position relative to Bruch s membrane opening and laminar thickness (vertical yellow lines); one measurement each of the diameter of the neural canal opening at Bruch s membrane (horizontal yellow line) and the posterior scleral canal opening (horizontal orange line); and measurements of peripapillary scleral thickness beginning at the posterior scleral canal opening and repeated every 100 m (vertical orange lines) to the peripheral edge of the section. For this report, only scleral thickness at the posterior scleral canal opening is reported because more peripheral measurements were not available for all four quadrants of all six eyes. tion of the canal s passage through the sclera itself, which can be defined by the shift of the posterior relative to the anterior scleral canal opening. Because the flow of blood through the prelaminar, laminar, and retrolaminar posterior ciliary arteries may be influenced by the thickness of the immediate peripapillary sclera 56 and thinning of the peripapillary sclera has been reported in human 33 and experimental 52 glaucoma, clinical measures of scleral thickness immediately adjacent to the canal should be important. Although clinical, high-resolution, 3-D reconstructions of the neural canal and peripapillary sclera are not currently possible, experimental micromagnetic resonance imaging reconstructions of ex vivo human ONH tissues have achieved 30- m resolution, which may be adequate to characterize these relationships. 43 Finite element modeling of a large group of normal monkey and human ONHs will determine the magnitude and clinical relevance of these differences. The principal findings within the normal and EG connective tissue voxel geometries are as follows. First, substantial differences in the 3-D architecture of the peripapillary sclera, scleral canal wall, and lamina cribrosa architecture are apparent within the normal eyes of the three monkeys. Second, posterior deformation of the central lamina cribrosa is evident within each of the EG eyes, compared with the respective contralateral normal eye. Third, in the periphery, laminar deformation beneath Bruch s membrane is greatest inferiorly or superiorly in all three EG eyes; however, mild to moderate excavation is also present in the other three quadrants in each of these eyes. Fourth, mild thickening of the lamina and peri- FIGURE 9. Voxel geometry surface image and CSLT reflectance image for the right and left optic nerve head of each monkey. The surface of the voxel geometry and the CSLT reflectance image are shown. All structures within the voxel geometries have been made partially transparent to improve visibility of the deeper structures. The orientation of the voxel geometry relative to the CSLT image has not been aligned and is shifted somewhat clockwise in the left eye of monkey 1 and counterclockwise in the right eye of monkey 3. In the voxel geometries for monkeys 1 and 3 (right eye, normal; left eye, EG), the border and flange tissues of the anterior scleral canal opening are orange. The innermost aspect of this circle corresponds to the clinically apparent anterior scleral canal opening within the CSLT reflectance image of each eye. In monkey 2 (right eye, EG; left eye, normal), a slightly altered protocol was used, resulting in the border and flange tissues being assigned the same yellow color as the sclera. N, nasal; T, temporal.
9 4396 Burgoyne et al. IOVS, December 2004, Vol. 45, No. 12 FIGURE 10. Central vertical (left column of boxes) and horizontal (right column of boxes) digital section images from the normal (top, within each box) and EG (bottom, within each box) voxel geometry of each monkey. Note the substantial differences in scleral thickness, scleral canal obliqueness, and laminar tautness between the normal eyes of the three monkeys (top frames within each box). Also note the profound posterior laminar deformation in all the views of the EG versus normal monkey eyes (bottom versus top frames within each box). N, nasal; T, temporal; I, inferior; S, superior. papillary sclera (at the posterior scleral canal opening) is present in most quadrants of all three EG eyes. In a previous study, we cut 16 immersion-fixed (IOP, 0 mm Hg) and 18 perfusion-fixed (IOP, 10, 30, or 45 mm Hg) monkey ONHs from four separate groups of monkeys into serial, 4- m sagittal histologic sections and measured anterior laminar position and thickness and scleral canal diameter in digitized images of every sixth section to study the lamina cribrosa and anterior scleral canal wall in the normal and EG monkey eye at various levels of IOP. 41 That study was the first to report that the lamina cribrosa demonstrates both central and peripheral fixed posterior deformation at this early stage of the neuropathy. The implications of this early connective tissue deformation were extensively discussed in that report. The present study confirms these findings in a new group of three EG eyes. The laminar position data in the current report are similar to the values we have previously reported for histologic specimens. 41 However, laminar thickness, peripapillary thickness, and neural canal diameter at Bruch s membrane are substantially smaller in the 3-D reconstructed cynomolgus eyes of this study, compared with histologic data reported previously from nine rhesus monkey eyes perfusion fixed at an IOP of 10 mm Hg. 41,53 Overall laminar thickness in the three normal eyes in this report ranged from 87 to 115 m, compared with 182 to 215 m for two groups of eyes perfusion-fixed at an IOP of 10 mm Hg in our previous report. 41 Overall peripapillary scleral thickness at the posterior scleral canal opening ranged from 120 to 151 m in this study, compared with 200 to 250 m in another of our reports. 53 Finally, the horizontal and vertical diameters of the neural canal at Bruch s membrane in the normal cynomolgus monkey eyes of the current report (horizontal, m; vertical, m) are smaller than previously reported within histologic sections of rhesus monkey eyes (horizontal, m; vertical, m). Although this difference may be the result of tissue preparation alone (Historesin embedding for histologic measurements, paraffin embedding for 3-D reconstruction), or species differences (cynomolgus versus rhesus), we believe that these three monkeys just happen to be at the small end of the dimensions of normal cynomolgus and rhesus monkeys. To date, we have completed the initial phases of 3-D reconstruction of both eyes of 15 monkeys (six cynomolgus, nine rhesus). Of these, initial estimates of the long and short axes of an ellipse fitted to Bruch s membrane opening have been completed for five cynomolgus and five rhesus monkeys (Pottle J,
10 IOVS, December 2004, Vol. 45, No. 12 ONH Connective Tissue Damage in Glaucoma 4397 TABLE 2. Laminar, Neural Canal, and Peripapillary Scleral Thickness Measurements by Eye Monkey 1 Monkey 2 Monkey 3 Parameter Normal Eye EG Eye Normal Eye EG Eye Normal Eye EG Eye Anterior laminar position Overall * * * Central * * * Inferior * * * Nasal * * * Superior * * * Temporal * * * Laminar thickness Overall * * * Central * * * Inferior * * Nasal * * * Superior * * * Temporal * * Horizontal neural canal diameter BMO * * * PSCO * * Vertical neural canal diameter BMO * * * PSCO * * * Peripapillary scleral thickness Overall * * * Inferior * Nasal * Superior * * Temporal * * All values are in micrometers (mean 95% confidence interval). BMO, Bruch s membrane opening; PSCO, posterior scleral canal opening. * Significantly greater than the value in the contralateral eye, P 0.05, ANOVA. Posterior scleral thickness was measured at the posterior scleral canal opening only. et al. IOVS 2004;45:ARVO E-Abstract 1118). Within these data (not shown), although the cynomolgus data may cluster at the smaller end of the spectrum, both cynomolgus and rhesus data demonstrate a wide range of sizes of the opening in Bruch s membrane. For the five cynomolgus monkeys, the range for the long axis of Bruch s membrane opening was 1331 to 1535 m and the range for the short axis was 1031 to 1171 m. In the five rhesus monkeys, the range of the long axis of Bruch s membrane opening was 1233 to 1745 m and the range of the short axis was 844 to 1345 m. Although it is possible that our paraffin-embedding protocol induced greater shrinkage of the tissues, the fact that the laminar position data are not different from our previous reports argues against this. Experiments in which both eyes of rabbits are perfusion fixed, then individually embedded (one in Historesin and one in paraffin) are underway to compare shrinkage effects. To our knowledge, no data exist on speciesspecific differences in the 3-D architecture of the neural canal. Our data may therefore be the first to suggest that the neural canal of the cynomolgus monkey is smaller than that of the rhesus. A formal review of the reconstructions of both eyes of 40 monkeys will eventually be possible. These data may lead to more definitive conclusions regarding species differences in the 3-D architecture of the neural canal. Our method of 3-D reconstruction has the following limitations. First, anterior-to-posterior resolution was limited to 3 m by the fact that the current stain penetrates approximately 2.5 m into the block. Thus, cutting a 3- m section was necessary to obtain an unstained block surface after each cut. Second, because the stain is applied by hand to the block with a cotton-tipped swab and then the excess is manually removed with lens paper, staining variation between section images can be substantial for some eyes. This problem, combined with variations in illumination, has made automation of object delineation difficult. Third, the current method is laborious, requiring on average 1 month to complete the construction and visualization of the connective tissue voxel geometry for a single ONH. Two subsequent analyses are planned for each geometry. First, additional methods for quantitative connective tissue architecture characterization are under development, to enable a 3-D characterization of the location and pattern of connective tissue damage in early, and eventually in moderate and severe, experimental glaucoma. Second, continuum and micro finite element models will be built of each eye to characterize the distribution of IOPrelated stress and strain within the connective tissues of each ONH. This characterization, once completed, will allow us to establish the relationships between IOP-related stress and strain and EG connective tissue damage. These relationships, once elucidated, will direct a new generation of experiments designed to colocalize IOP-related stress and strain, early connective tissue damage, astrocyte and glial cell activation, and axonal distress within the ONHs of individual monkey eyes. The geometries presented herein reconstruct the lamina cribrosa, central retinal vessels, peripapillary sclera, and optic nerve sheath insertions. However, the internal limiting membrane of the retina, peripapillary Bruch s membrane, subarachnoid space, and principal branches of the posterior ciliary arteries within the peripapillary sclera are also present and will be included in future reconstructions. The addition of these structures will allow future models to include not only the underlying connective tissues but also the prelaminar and retrolaminar neural tissues, posterior ciliary arteries, and cerebro-
11 4398 Burgoyne et al. IOVS, December 2004, Vol. 45, No. 12 FIGURE 11. Digital section images through the peripheral anterior scleral canal opening of all four quadrants (superior, inferior, nasal, and temporal) of the normal (top image within each box) and EG (bottom image within box) voxel geometry of monkey 1. Each peripheral view (note the green line within the guide image for each section) was chosen to intersect the first point at which Bruch s membrane is intact above the lamina. Note that although deformation of the peripheral laminar beams (light blue) relative to Bruch s membrane flange (orange) is visible in all four quadrants of the EG eyes, peripheral laminar deformation is greatest within the inferior scleral canal (top right box). N, nasal; T, temporal; I, inferior; S, superior. spinal fluid pressure. Because the method ensures continuous anterior-to-posterior registration from the clinically recognizable ONH surface through the cut surface of the optic nerve, these enhanced reconstructions will offer an unprecedented opportunity to correlate the location of astrocyte activation, axonal insult, capillary collapse, and tissue oxygenation relative to the stresses and strains within the adjacent connective tissues. The reproducibility and accuracy of ONH voxel geometry and finite element model construction for individual monkey eyes will be presented in a series of future reports. Acknowledgments The authors acknowledge Anthony J. Bellezza s central role in the accomplishment of the method and J. Crawford Downs construction of the six geometries contained herein. The authors also gratefully acknowledge Stephanie Hager, Sedette Skaggs, Zenaida Peralta-Inga, PhD, Pris Zhou, Budd Hirons, and Juan Reynaud, without whom the development and implementation of this methodology would not have been possible. References 1. Kalvin NH, Hamasaki DI, Gass JD. Experimental glaucoma in monkeys. I. Relationship between intraocular pressure and cupping of the optic disc and cavernous atrophy of the optic nerve. Arch Ophthalmol. 1966;76: Hayreh SS, Vrabec F. The structure of the head of the optic nerve in rhesus monkey. Am J Ophthalmol. 1966;61: Zimmerman LE, De Venecia G, Hamasaki DI. Pathology of the optic nerve in experimental acute glaucoma. Invest Ophthalmol Vis Sci. 1967;6: Anderson DR. Ultrastructure of human and monkey lamina cribrosa and optic nerve head. Arch Ophthalmol. 1969;82: Emery JM, Landis D, Paton D, Boniuk M, Craig JM. The lamina cribrosa in normal and glaucomatous human eyes. Trans Am Acad Ophthalmol Otolaryngol. 1974;78:OP290 OP Anderson DR, Hendrickson A. Effect of intraocular pressure on rapid axoplasmic transport in monkey optic nerve. Invest Ophthalmol. 1974;13: Quigley HA, Anderson DR. The dynamics and location of axonal transport blockade by acute intraocular pressure elevation in primate optic nerve. Invest Ophthalmol. 1976;15: Minckler DS, Bunt AH, Johanson GW. Orthograde and retrograde axoplasmic transport during acute ocular hypertension in the monkey. Invest Ophthalmol Vis Sci. 1977;16: Gaasterland D, Tanishima T, Kuwabara T. Axoplasmic flow during chronic experimental glaucoma. I. Light and electron microscopic studies of the monkey optic nerve head during development of glaucomatous cupping. Invest Ophthalmol Vis Sci. 1978;17: Quigley HA, Green WR. The histology of human glaucoma cupping and optic nerve damage: clinicopathologic correlation in 21 eyes. Ophthalmology. 1979;86: Quigley HA, Addicks EM. Chronic experimental glaucoma in primates. II. Effect of extended intraocular pressure elevation on optic nerve head and axonal transport. Invest Ophthalmol Vis Sci. 1980;19: Quigley HA, Flower RW, Addicks EM, McLeod DS. The mechanism of optic nerve damage in experimental acute intraocular pressure elevation. Invest Ophthalmol Vis Sci. 1980;19: Quigley HA, Addicks EM, Green WR, Maumenee AE. Optic nerve damage in human glaucoma. II. The site of injury and susceptibility to damage. Arch Ophthalmol. 1981;99: Minckler DS, Spaeth GL. Optic nerve damage in glaucoma. Surv Ophthalmol. 1981;26: Radius RL. Regional specificity in anatomy at the lamina cribrosa. Arch Ophthalmol. 1981;99: Radius RL, Gonzales M. Anatomy of the lamina cribrosa in human eyes. Arch Ophthalmol. 1981;99: Quigley HA, Addicks EM, Green WR. Optic nerve damage in human glaucoma. III. Quantitative correlation of nerve fiber loss and visual field defect in glaucoma, ischemic neuropathy, disc edema and toxic neuropathy. Arch Ophthalmol. 1982;100:
Cupping is a clinical term that is used to describe enlargement
 3-D Histomorphometry of the Normal and Early Glaucomatous Monkey Optic Nerve Head: Prelaminar Neural Tissues and Cupping Hongli Yang, 1 J. Crawford Downs, 1,2 Anthony Bellezza, 3 Hilary Thompson, 4 and
3-D Histomorphometry of the Normal and Early Glaucomatous Monkey Optic Nerve Head: Prelaminar Neural Tissues and Cupping Hongli Yang, 1 J. Crawford Downs, 1,2 Anthony Bellezza, 3 Hilary Thompson, 4 and
The Connective Tissue Components of Optic Nerve Head Cupping in Monkey Experimental Glaucoma Part 1: Global Change
 Glaucoma The Connective Tissue Components of Optic Nerve Head Cupping in Monkey Experimental Glaucoma Part 1: Global Change Hongli Yang, 1,2 Ruojin Ren, 1,2 Howard Lockwood, 1,2 Galen Williams, 1,2 Vincent
Glaucoma The Connective Tissue Components of Optic Nerve Head Cupping in Monkey Experimental Glaucoma Part 1: Global Change Hongli Yang, 1,2 Ruojin Ren, 1,2 Howard Lockwood, 1,2 Galen Williams, 1,2 Vincent
We have proposed that intraocular pressure (IOP) related
 3-D Histomorphometry of the Normal and Early Glaucomatous Monkey Optic Nerve Head: Lamina Cribrosa and Peripapillary Scleral Position and Thickness Hongli Yang, 1,2 J. Crawford Downs, 1,2,3 Christopher
3-D Histomorphometry of the Normal and Early Glaucomatous Monkey Optic Nerve Head: Lamina Cribrosa and Peripapillary Scleral Position and Thickness Hongli Yang, 1,2 J. Crawford Downs, 1,2,3 Christopher
OCT in the Diagnosis and Follow-up of Glaucoma
 OCT in the Diagnosis and Follow-up of Glaucoma Karim A Raafat MD. Professor Of Ophthalmology Cairo University Hmmmm! Do I have Glaucoma or not?! 1 Visual Function 100% - N Gl Structure : - 5000 axon /
OCT in the Diagnosis and Follow-up of Glaucoma Karim A Raafat MD. Professor Of Ophthalmology Cairo University Hmmmm! Do I have Glaucoma or not?! 1 Visual Function 100% - N Gl Structure : - 5000 axon /
The Missing Piece in Glaucoma?
 Open Journal of Ophthalmology, 2016, 6, 56-62 Published Online February 2016 in SciRes. http://www.scirp.org/journal/ojoph http://dx.doi.org/10.4236/ojoph.2016.61008 The Missing Piece in Glaucoma? Syed
Open Journal of Ophthalmology, 2016, 6, 56-62 Published Online February 2016 in SciRes. http://www.scirp.org/journal/ojoph http://dx.doi.org/10.4236/ojoph.2016.61008 The Missing Piece in Glaucoma? Syed
Advances in OCT Murray Fingeret, OD
 Disclosures Advances in OCT Murray Fingeret, OD Consultant Alcon, Allergan, Bausch & Lomb, Carl Zeiss Meditec, Diopsys, Heidelberg Engineering, Reichert, Topcon Currently Approved OCT Devices OCT Devices
Disclosures Advances in OCT Murray Fingeret, OD Consultant Alcon, Allergan, Bausch & Lomb, Carl Zeiss Meditec, Diopsys, Heidelberg Engineering, Reichert, Topcon Currently Approved OCT Devices OCT Devices
A Comparison of Optic Nerve Head Morphology Viewed by Spectral Domain Optical Coherence Tomography and by Serial Histology METHODS.
 Glaucoma A Comparison of Optic Nerve Head Morphology Viewed by Spectral Domain Optical Coherence Tomography and by Serial Histology Nicholas G. Strouthidis, 1 Jonathan Grimm, 1 Galen A. Williams, 1 Grant
Glaucoma A Comparison of Optic Nerve Head Morphology Viewed by Spectral Domain Optical Coherence Tomography and by Serial Histology Nicholas G. Strouthidis, 1 Jonathan Grimm, 1 Galen A. Williams, 1 Grant
SOUTH-EAST EUROPEAN JOURNAL of OPHTHALMOLOGY 2015; 1 (1) 34 40
 Review article SOUTH-EAST EUROPEAN JOURNAL of OPHTHALMOLOGY 2015; 1 (1) 34 40 Retinal nerve fiber layer versus peripapillary capillary density assessment A powerful tool for detecting optic nerve head
Review article SOUTH-EAST EUROPEAN JOURNAL of OPHTHALMOLOGY 2015; 1 (1) 34 40 Retinal nerve fiber layer versus peripapillary capillary density assessment A powerful tool for detecting optic nerve head
Dr/ Marwa Abdellah EOS /16/2018. Dr/ Marwa Abdellah EOS When do you ask Fluorescein angiography for optic disc diseases???
 When do you ask Fluorescein angiography for optic disc diseases??? 1 NORMAL OPTIC DISC The normal optic disc on fluorescein angiography is fluorescent due to filling of vessels arising from the posterior
When do you ask Fluorescein angiography for optic disc diseases??? 1 NORMAL OPTIC DISC The normal optic disc on fluorescein angiography is fluorescent due to filling of vessels arising from the posterior
Il contributo dell'angio-oct: valutazione integrata della componente nervosa e vascolare della malattia glaucomatosa
 SIMPOSIO G.O.A.L. - LE NUOVE FRONTIERE DIAGNOSTICHE E LE LINEE DI INDIRIZZO AMBULATORIALI DEL GLAUCOMA Coordinatore e moderatore: D. Mazzacane Presidente: L. Rossetti Il contributo dell'angio-oct: valutazione
SIMPOSIO G.O.A.L. - LE NUOVE FRONTIERE DIAGNOSTICHE E LE LINEE DI INDIRIZZO AMBULATORIALI DEL GLAUCOMA Coordinatore e moderatore: D. Mazzacane Presidente: L. Rossetti Il contributo dell'angio-oct: valutazione
Glaucoma is recognized as a progressive optic neuropathy,
 Glaucoma Longitudinal Change Detected by Spectral Domain Optical Coherence Tomography in the Optic Nerve Head and Peripapillary Retina in Experimental Glaucoma Nicholas G. Strouthidis, 1 Brad Fortune,
Glaucoma Longitudinal Change Detected by Spectral Domain Optical Coherence Tomography in the Optic Nerve Head and Peripapillary Retina in Experimental Glaucoma Nicholas G. Strouthidis, 1 Brad Fortune,
The Optic Nerve Head In Glaucoma. Clinical Pearl #1. Characteristics of Normal Disk 9/26/2017. Initial detectable damage Structure vs function
 The Optic Nerve Head In Glaucoma Clinical Pearl #1 Eric E. Schmidt, O.D., F.A.A.O. Omni Eye Specialists Wilmington,NC schmidtyvision@msn.com Glaucoma is an optic neuropathy Initial detectable damage Structure
The Optic Nerve Head In Glaucoma Clinical Pearl #1 Eric E. Schmidt, O.D., F.A.A.O. Omni Eye Specialists Wilmington,NC schmidtyvision@msn.com Glaucoma is an optic neuropathy Initial detectable damage Structure
CLINICAL SCIENCES. Optic Nerve Hydropic Axonal Degeneration and Blocked Retrograde Axoplasmic Transport
 CLINICAL SCIENCES Optic Nerve Hydropic Axonal Degeneration and locked Retrograde Axoplasmic Transport Histopathologic Features in Human High-Pressure Secondary Glaucoma David L. Knox, MD; Ralph C. Eagle,
CLINICAL SCIENCES Optic Nerve Hydropic Axonal Degeneration and locked Retrograde Axoplasmic Transport Histopathologic Features in Human High-Pressure Secondary Glaucoma David L. Knox, MD; Ralph C. Eagle,
Peripapillary circle of Zinn Haller revealed by fundus fluorescein angiography
 British Journal of Ophthalmology 1997;81:663 667 663 Department of Ophthalmology, School of Medicine, Hanyang University, Seoul, Korea M-K Ko D-S Kim Y-K Ahn Correspondence to: Myung-Kyoo Ko, MD, Department
British Journal of Ophthalmology 1997;81:663 667 663 Department of Ophthalmology, School of Medicine, Hanyang University, Seoul, Korea M-K Ko D-S Kim Y-K Ahn Correspondence to: Myung-Kyoo Ko, MD, Department
RADIAL PERIPAPLLARY CAPILLARIES OF THE RETINA*tt
 Brit. J. Ophthal. (1968) 52, 26 RADIAL PERIPAPLLARY CAPILLARIES OF THE RETINA*tt HI. POSSIBLE ROLE IN BJERRUM SCOTOMA BY MORTON ALTERMAN AND PAUL HENKIND From the Department of Ophthalmology, New York
Brit. J. Ophthal. (1968) 52, 26 RADIAL PERIPAPLLARY CAPILLARIES OF THE RETINA*tt HI. POSSIBLE ROLE IN BJERRUM SCOTOMA BY MORTON ALTERMAN AND PAUL HENKIND From the Department of Ophthalmology, New York
Moving forward with a different perspective
 Moving forward with a different perspective The Leader In Vision Diagnostics Offers A New Perspective Marco has served the eyecare community by offering exceptional lane products and automated high tech
Moving forward with a different perspective The Leader In Vision Diagnostics Offers A New Perspective Marco has served the eyecare community by offering exceptional lane products and automated high tech
Experimental Eye Research
 Experimental Eye Research 90 (2010) 70 80 Contents lists available at ScienceDirect Experimental Eye Research journal homepage: www.elsevier.com/locate/yexer 3D morphometry of the human optic nerve head
Experimental Eye Research 90 (2010) 70 80 Contents lists available at ScienceDirect Experimental Eye Research journal homepage: www.elsevier.com/locate/yexer 3D morphometry of the human optic nerve head
THE EYE: RETINA AND GLOBE
 Neuroanatomy Suzanne Stensaas February 24, 2011, 10:00-12:00 p.m. Reading: Waxman Ch. 15. Your histology and gross anatomy books should be useful. Reading: Histology of the Eye from any histology book
Neuroanatomy Suzanne Stensaas February 24, 2011, 10:00-12:00 p.m. Reading: Waxman Ch. 15. Your histology and gross anatomy books should be useful. Reading: Histology of the Eye from any histology book
Pit-like changes of the optic nerve head
 Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Glaucoma is the second leading cause of blindness worldwide
 Glaucoma Biomechanical Changes in the Sclera of Monkey Eyes Exposed to Chronic IOP Elevations Michaël J. A. Girard, 1,2,3 J.-K. Francis Suh, 2,4 Michael Bottlang, 5 Claude F. Burgoyne, 2,6 and J. Crawford
Glaucoma Biomechanical Changes in the Sclera of Monkey Eyes Exposed to Chronic IOP Elevations Michaël J. A. Girard, 1,2,3 J.-K. Francis Suh, 2,4 Michael Bottlang, 5 Claude F. Burgoyne, 2,6 and J. Crawford
Cirrus TM HD-OCT. Details define your decisions
 Cirrus TM HD-OCT Details define your decisions 2 With high-definition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl Zeiss
Cirrus TM HD-OCT Details define your decisions 2 With high-definition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl Zeiss
T HE visual field changes that accompany
 J. Neurosurg. / Volume 31 / September, 1969 The Arterial Supply of the Human Optic Chiasm RICHARD BERGLAND, M.D.,* AND BRONSON S. RAY, M.D. Department of Surgery (Neurosurgery), New York Hospital-Cornell
J. Neurosurg. / Volume 31 / September, 1969 The Arterial Supply of the Human Optic Chiasm RICHARD BERGLAND, M.D.,* AND BRONSON S. RAY, M.D. Department of Surgery (Neurosurgery), New York Hospital-Cornell
Beyond the C/D Ratio: Evaluating a Glaucomatous Optic Nerve. Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic COPE ID#: GL
 Beyond the C/D Ratio: Evaluating a Glaucomatous Optic Nerve Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic COPE ID#: 27809-GL Points to Remember Glaucoma affects the ONH in characteristic patterns
Beyond the C/D Ratio: Evaluating a Glaucomatous Optic Nerve Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic COPE ID#: 27809-GL Points to Remember Glaucoma affects the ONH in characteristic patterns
The Pathology and Pathogenesis of Acute Glaucoma in Dogs. Richard R Dubielzig
 The Pathology and Pathogenesis of Acute Glaucoma in Dogs Richard R Dubielzig Overview of Glaucoma Intraocular Pressure too High to Support a Healthy Optic Nerve Terminology used in the classification of
The Pathology and Pathogenesis of Acute Glaucoma in Dogs Richard R Dubielzig Overview of Glaucoma Intraocular Pressure too High to Support a Healthy Optic Nerve Terminology used in the classification of
3/16/2018. Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim. Prof. of Ophthalmology Al-Azhar University
 Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim Prof. of Ophthalmology Al-Azhar University 1 Ultrasound biomicroscopy (UBM) is a recent technique to visualize anterior segment with the
Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim Prof. of Ophthalmology Al-Azhar University 1 Ultrasound biomicroscopy (UBM) is a recent technique to visualize anterior segment with the
Relevant Financial Disclosures
 DO THE EXTRAOCULAR MUSCLES CAUSE GLAUCOMA AND ANTERIOR ISCHEMIC OPTIC NEUROPATHY? Joseph L. Demer, MD, PhD Arthur L. Rosenbaum Chair of Pediatric Ophthalmology Professor of Neurology Relevant Financial
DO THE EXTRAOCULAR MUSCLES CAUSE GLAUCOMA AND ANTERIOR ISCHEMIC OPTIC NEUROPATHY? Joseph L. Demer, MD, PhD Arthur L. Rosenbaum Chair of Pediatric Ophthalmology Professor of Neurology Relevant Financial
Cirrus TM HD-OCT. Details defi ne your decisions
 Cirrus TM HD-OCT Details defi ne your decisions 2 With high-defi nition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl
Cirrus TM HD-OCT Details defi ne your decisions 2 With high-defi nition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl
C a t a r a c t G l a u c o m a R e t i n a R e f r a c t i v e. The GDxVCC Early answers and ongoing assessment for glaucoma
 C a t a r a c t G l a u c o m a R e t i n a R e f r a c t i v e The GDxVCC Early answers and ongoing assessment for glaucoma The quantifiable approach to quality care Only Humphrey GPA software Early insight
C a t a r a c t G l a u c o m a R e t i n a R e f r a c t i v e The GDxVCC Early answers and ongoing assessment for glaucoma The quantifiable approach to quality care Only Humphrey GPA software Early insight
SOCT Copernicus REVO. * - Currently import and overlay are avaibale in manual mode only
 SOCT Copernicus REVO Easy Operation (Full auto & Auto mode) Auto alignment (Z-position, C-gate, Focus, Tomogram) Voice guide (support patient through examination) Powerful analysis tools Enhanced tomograms
SOCT Copernicus REVO Easy Operation (Full auto & Auto mode) Auto alignment (Z-position, C-gate, Focus, Tomogram) Voice guide (support patient through examination) Powerful analysis tools Enhanced tomograms
Question 1: Comment on the optic nerve appearance of each eye.
 Case 2 - Right Optic Nerve Head Drusen (ONHD) A 41 year old female was referred by her optometrist for a workup for unilateral optic disc drusen, OCT, and visual field changes. The patient was otherwise
Case 2 - Right Optic Nerve Head Drusen (ONHD) A 41 year old female was referred by her optometrist for a workup for unilateral optic disc drusen, OCT, and visual field changes. The patient was otherwise
3/16/2018. Perimetry
 Perimetry The normal visual field extends further away from fixation temporally and inferiorly than superiorly and nasally. From the center of the retina this sensitivity decreases towards the periphery,
Perimetry The normal visual field extends further away from fixation temporally and inferiorly than superiorly and nasally. From the center of the retina this sensitivity decreases towards the periphery,
Optic Nerve Evaluation in Glaucoma (TPG)
 Optic Nerve Evaluation in Glaucoma (TPG) Introduction Glaucoma is a progressive optic nerve disease characterized by retinal ganglion cell death and resultant axon loss, ultimately manifesting as excavation
Optic Nerve Evaluation in Glaucoma (TPG) Introduction Glaucoma is a progressive optic nerve disease characterized by retinal ganglion cell death and resultant axon loss, ultimately manifesting as excavation
PRIMUS 200 from ZEISS The essential OCT
 PRIMUS 200 from ZEISS The essential OCT Seeing beyond the surface. ZEISS PRIMUS 200 // INNOVATION MADE BY ZEISS Clear Visualization. Advanced Technology. Reliability. Essential elements of your first OCT.
PRIMUS 200 from ZEISS The essential OCT Seeing beyond the surface. ZEISS PRIMUS 200 // INNOVATION MADE BY ZEISS Clear Visualization. Advanced Technology. Reliability. Essential elements of your first OCT.
Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed?
 Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed? Jody Piltz-Seymour, M.D. Clinical Professor Perelman School of Medicine University of Pennsylvania Wills Glaucoma Service Valley
Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed? Jody Piltz-Seymour, M.D. Clinical Professor Perelman School of Medicine University of Pennsylvania Wills Glaucoma Service Valley
The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation
 C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
Structural examina.on: Imaging
 ManaMa: Glaucoma Structural examina.on: Imaging Luís Abegão Pinto, MD, PhD Department of Ophthalmology CHLC Lisbon Faculty of Medicine, Lisbon University 1 11-10- 2013 Structural changes Qualitative changes
ManaMa: Glaucoma Structural examina.on: Imaging Luís Abegão Pinto, MD, PhD Department of Ophthalmology CHLC Lisbon Faculty of Medicine, Lisbon University 1 11-10- 2013 Structural changes Qualitative changes
Ganglion cell complex scan in the early prediction of glaucoma
 Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
T he lamina cribrosa is a sieve-like membrane in the
 1299 EXTENDED REPORT Three dimensional analysis of the lamina cribrosa in glaucoma J Morgan-Davies, N Taylor, A R Hill, P Aspinall, CJ O Brien, A Azuara-Blanco... See end of article for authors affiliations...
1299 EXTENDED REPORT Three dimensional analysis of the lamina cribrosa in glaucoma J Morgan-Davies, N Taylor, A R Hill, P Aspinall, CJ O Brien, A Azuara-Blanco... See end of article for authors affiliations...
Automated Detection of Vascular Abnormalities in Diabetic Retinopathy using Morphological Entropic Thresholding with Preprocessing Median Fitter
 IJSTE - International Journal of Science Technology & Engineering Volume 1 Issue 3 September 2014 ISSN(online) : 2349-784X Automated Detection of Vascular Abnormalities in Diabetic Retinopathy using Morphological
IJSTE - International Journal of Science Technology & Engineering Volume 1 Issue 3 September 2014 ISSN(online) : 2349-784X Automated Detection of Vascular Abnormalities in Diabetic Retinopathy using Morphological
Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
 Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Morphometric Features of Laminar Pores in Lamina Cribrosa Observed by Scanning Laser Ophthalmoscopy
 Morphometric Features of Laminar Pores in Lamina Cribrosa Observed by Scanning Laser Ophthalmoscopy Hidetaka Maeda, Makoto Nakamura and Misao Yamamoto Department of Ophthalmology, Kobe University School
Morphometric Features of Laminar Pores in Lamina Cribrosa Observed by Scanning Laser Ophthalmoscopy Hidetaka Maeda, Makoto Nakamura and Misao Yamamoto Department of Ophthalmology, Kobe University School
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma. Module 3a GDx
 STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
E, Ixperimental allergic encephalomyelitis
 Experimental allergic optic neuritis in guinea pigs: preliminary report Narsing A. Rao, Mark O. M. Tso," and Lorenz E. Zimmerman An experimental model for acute allergic optic neuritis was produced in
Experimental allergic optic neuritis in guinea pigs: preliminary report Narsing A. Rao, Mark O. M. Tso," and Lorenz E. Zimmerman An experimental model for acute allergic optic neuritis was produced in
Factors Influencing Central Lamina Cribrosa Depth: A Multicenter Study
 Glaucoma Factors Influencing Central Lamina Cribrosa Depth: A Multicenter Study Haomin Luo, 1,2 Hongli Yang, 2 Stuart K. Gardiner, 3 Christy Hardin, 2 Glen P. Sharpe, 4 Joseph Caprioli, 5 Shaban Demirel,
Glaucoma Factors Influencing Central Lamina Cribrosa Depth: A Multicenter Study Haomin Luo, 1,2 Hongli Yang, 2 Stuart K. Gardiner, 3 Christy Hardin, 2 Glen P. Sharpe, 4 Joseph Caprioli, 5 Shaban Demirel,
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD
 New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
OCT Angiography in Primary Eye Care
 OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
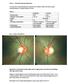 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
 Romanian Journal of Ophthalmology, Volume 60, Issue 3, July-September 2016. pp:158-164 GENERAL ARTICLE Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
Romanian Journal of Ophthalmology, Volume 60, Issue 3, July-September 2016. pp:158-164 GENERAL ARTICLE Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
Medicine. Observational Study. 1. Introduction OPEN
 Observational Study Medicine The association between prelaminar tissue thickness and peripapillary choroidal thickness in untreated normal-tension glaucoma patients Ji-Hye Park, MD, PhD a, Chungkwon Yoo,
Observational Study Medicine The association between prelaminar tissue thickness and peripapillary choroidal thickness in untreated normal-tension glaucoma patients Ji-Hye Park, MD, PhD a, Chungkwon Yoo,
Ultrasound Evaluation of the Posterior Segment of the Eye A Ready Reckoner
 180 Kerala Journal of Ophthalmology Vol. XX, No. 2 OPHTHALMIC INSTRUMENTATION Ultrasound Evaluation of the Posterior Segment of the Eye A Ready Reckoner Dr. Mahesh G. MS DO DNB FRCSEd., Dr. A. Giridhar
180 Kerala Journal of Ophthalmology Vol. XX, No. 2 OPHTHALMIC INSTRUMENTATION Ultrasound Evaluation of the Posterior Segment of the Eye A Ready Reckoner Dr. Mahesh G. MS DO DNB FRCSEd., Dr. A. Giridhar
Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma.
 Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma. Donald C. Hood 1,2,* and Ali S. Raza 1 1 Department of Psychology, Columbia
Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma. Donald C. Hood 1,2,* and Ali S. Raza 1 1 Department of Psychology, Columbia
Nature Neuroscience doi: /nn Supplementary Figure 1. Characterization of viral injections.
 Supplementary Figure 1 Characterization of viral injections. (a) Dorsal view of a mouse brain (dashed white outline) after receiving a large, unilateral thalamic injection (~100 nl); demonstrating that
Supplementary Figure 1 Characterization of viral injections. (a) Dorsal view of a mouse brain (dashed white outline) after receiving a large, unilateral thalamic injection (~100 nl); demonstrating that
Optical coherence tomography of the retinal nerve fibre layer in mild papilloedema and pseudopapilloedema
 294 SCIENTIFIC REPORT Optical coherence tomography of the retinal nerve fibre layer in mild papilloedema and pseudopapilloedema E Z Karam, T R Hedges... Aims: To determine the degree to which optical coherence
294 SCIENTIFIC REPORT Optical coherence tomography of the retinal nerve fibre layer in mild papilloedema and pseudopapilloedema E Z Karam, T R Hedges... Aims: To determine the degree to which optical coherence
Relationship between limbal incisions. angle. and the structures of the anterior chamber
 Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
RETINAL NERVE FIBER LAYER
 CLINICAL SCIENCES The Effect of Scan Diameter on Retinal Nerve Fiber Layer Thickness Measurement Using Stratus Optic Coherence Tomography Giacomo Savini, MD; Piero Barboni, MD; Michele Carbonelli, MD;
CLINICAL SCIENCES The Effect of Scan Diameter on Retinal Nerve Fiber Layer Thickness Measurement Using Stratus Optic Coherence Tomography Giacomo Savini, MD; Piero Barboni, MD; Michele Carbonelli, MD;
The Role of the RNFL in the Diagnosis of Glaucoma
 Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Lamina Cribrosa Thickness and Spatial Relationships between Intraocular Space and Cerebrospinal Fluid Space in Highly Myopic Eyes METHODS
 Lamina Cribrosa Thickness and Spatial Relationships between Intraocular Space and Cerebrospinal Fluid Space in Highly Myopic Eyes Jost B. Jonas, 1 Eduard Berenshtein, 1 and Leonard Holbach 2 PURPOSE. To
Lamina Cribrosa Thickness and Spatial Relationships between Intraocular Space and Cerebrospinal Fluid Space in Highly Myopic Eyes Jost B. Jonas, 1 Eduard Berenshtein, 1 and Leonard Holbach 2 PURPOSE. To
Science & Technologies
 STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
Visualize. Analyze. Personalize. OCT + OCTA
 Visualize. Analyze. Personalize. OCT + OCTA A New Approach to Protecting Vision AngioVue OCT Angiography brings valuable new information to clinical practice. Non-invasive visualization of retinal vasculature.
Visualize. Analyze. Personalize. OCT + OCTA A New Approach to Protecting Vision AngioVue OCT Angiography brings valuable new information to clinical practice. Non-invasive visualization of retinal vasculature.
The World s fastest OCT. As simple as pressing. the start button
 The World s fastest OCT As simple as pressing the start button lution continues Optopol engineering team, designers of the first commercially available Spectral Domain OCT in the world, are proud to present
The World s fastest OCT As simple as pressing the start button lution continues Optopol engineering team, designers of the first commercially available Spectral Domain OCT in the world, are proud to present
Biomechanical Responses of Lamina Cribrosa to Intraocular Pressure Change Assessed by Optical Coherence Tomography in Glaucoma Eyes
 Glaucoma Biomechanical Responses of Lamina Cribrosa to Intraocular Pressure Change Assessed by Optical Coherence Tomography in Glaucoma Eyes Harry Quigley, 1 Karun Arora, 1 Sana Idrees, 1 Francisco Solano,
Glaucoma Biomechanical Responses of Lamina Cribrosa to Intraocular Pressure Change Assessed by Optical Coherence Tomography in Glaucoma Eyes Harry Quigley, 1 Karun Arora, 1 Sana Idrees, 1 Francisco Solano,
Early Detection Of Glaucoma Clinical Clues. Points To Live By. Glaucoma Risk Factors 10/3/2014
 Early Detection Of Glaucoma Clinical Clues Eric E. Schmidt, O.D. Omni Eye Specialists Wilmington, NC schmidtyvision@msn.com Points To Live By 25% of G pxs NEVER have IOP >21mm 50% of G pxs have trough
Early Detection Of Glaucoma Clinical Clues Eric E. Schmidt, O.D. Omni Eye Specialists Wilmington, NC schmidtyvision@msn.com Points To Live By 25% of G pxs NEVER have IOP >21mm 50% of G pxs have trough
Cupping in the Monkey Optic Nerve Transection Model Consists of Prelaminar Tissue Thinning in the Absence of Posterior Laminar Deformation
 Glaucoma Cupping in the Monkey Optic Nerve Transection Model Consists of Prelaminar Tissue Thinning in the Absence of Posterior Laminar Deformation Eliesa Ing, 1 Kevin M. Ivers, 1,2 Hongli Yang, 1,2 Stuart
Glaucoma Cupping in the Monkey Optic Nerve Transection Model Consists of Prelaminar Tissue Thinning in the Absence of Posterior Laminar Deformation Eliesa Ing, 1 Kevin M. Ivers, 1,2 Hongli Yang, 1,2 Stuart
4/22/16. Eye. External Anatomy of Eye. Accessory Structures. Bio 40B Dr. Kandula
 Eye Bio 40B Dr. Kandula External Anatomy of Eye Accessory Structures l Eyebrows l Levator Palpebrae Superioris - opens eye l Eyelashes l Ciliary glands modified sweat glands l Small sebaceous glands l
Eye Bio 40B Dr. Kandula External Anatomy of Eye Accessory Structures l Eyebrows l Levator Palpebrae Superioris - opens eye l Eyelashes l Ciliary glands modified sweat glands l Small sebaceous glands l
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma
 Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
Ganglion cell analysis by optical coherence tomography (OCT) Jonathan A. Micieli, MD Valérie Biousse, MD
 Ganglion cell analysis by optical coherence tomography (OCT) Jonathan A. Micieli, MD Valérie Biousse, MD Figure 1. Normal OCT of the macula (cross section through the line indicated on the fundus photo)
Ganglion cell analysis by optical coherence tomography (OCT) Jonathan A. Micieli, MD Valérie Biousse, MD Figure 1. Normal OCT of the macula (cross section through the line indicated on the fundus photo)
Comparison of o Noninvasive Measurement of Optic Nervehead Mechanical Compliance With an Invasive Method
 No. 10 Reports 1735 5. National Diabetes Data Group: Classification and diagnosis of diabetes mellitus and other categories of glucose intolerance. Diabetes 28:1039, 1979. 6. Siegel S: Nonparametric Statistics.
No. 10 Reports 1735 5. National Diabetes Data Group: Classification and diagnosis of diabetes mellitus and other categories of glucose intolerance. Diabetes 28:1039, 1979. 6. Siegel S: Nonparametric Statistics.
Uveal Melanoma. Protocol applies to malignant melanoma of the uvea.
 Uveal Melanoma Protocol applies to malignant melanoma of the uvea. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Uveal Melanoma Protocol applies to malignant melanoma of the uvea. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
PRIMUS 200 from ZEISS The essential OCT
 EN 00_00I The contents of the brochure may differ from the current status of approval of the product in your country. Please contact your regional representative for more information. Subject to change
EN 00_00I The contents of the brochure may differ from the current status of approval of the product in your country. Please contact your regional representative for more information. Subject to change
ADVANCED DIAGNOSTIC TECHNIQUES
 DIVISION OF VISION SCIENCES SESSION: 2008/2009 DIET: 1ST ADVANCED DIAGNOSTIC TECHNIQUES VISP216 LEVEL:2 MODULE LEADER: DR GUNTER LOFFLER B.Sc/B.Sc. (HONS) OPTOMETRY MAY 2009 DURATION: 2 HOURS CANDIDATES
DIVISION OF VISION SCIENCES SESSION: 2008/2009 DIET: 1ST ADVANCED DIAGNOSTIC TECHNIQUES VISP216 LEVEL:2 MODULE LEADER: DR GUNTER LOFFLER B.Sc/B.Sc. (HONS) OPTOMETRY MAY 2009 DURATION: 2 HOURS CANDIDATES
CLASS-y Laser Treats Glaucoma
 Article # 404 Comments About the Author Released: Author: Category: March 12th, 2014 Issue #0314 Ehud Assia Feature S S S S S CLASS-y Laser Treats Glaucoma Transforming complex, invasive and risky glaucoma
Article # 404 Comments About the Author Released: Author: Category: March 12th, 2014 Issue #0314 Ehud Assia Feature S S S S S CLASS-y Laser Treats Glaucoma Transforming complex, invasive and risky glaucoma
Shaken Baby Syndrome (SBS) Ocular Findings with Legal Implications
 United States and Canadian Academy of Pathology 2007 Annual Meeting Shaken Baby Syndrome (SBS) Ocular Findings with Legal Implications J. Douglas Cameron, MD Professor of Ophthalmology Mayo Clinic School
United States and Canadian Academy of Pathology 2007 Annual Meeting Shaken Baby Syndrome (SBS) Ocular Findings with Legal Implications J. Douglas Cameron, MD Professor of Ophthalmology Mayo Clinic School
Histology of the Eye
 Histology of the Eye Objectives By the end of this lecture, the student should be able to describe: The general structure of the eye. The microscopic structure of:»cornea.»retina. EYE BULB Three coats
Histology of the Eye Objectives By the end of this lecture, the student should be able to describe: The general structure of the eye. The microscopic structure of:»cornea.»retina. EYE BULB Three coats
The nerve-fiber layer of the primate retina: an autoradiographic study
 The nerve-fiber layer of the primate retina: an autoradiographic study Thomas E. Ogden The intraretinal path taken by fibers of the arcuate bundle was studied in four Rhesus monkeys. The fibers incorporated
The nerve-fiber layer of the primate retina: an autoradiographic study Thomas E. Ogden The intraretinal path taken by fibers of the arcuate bundle was studied in four Rhesus monkeys. The fibers incorporated
Unit VIII Problem 8 Anatomy: Orbit and Eyeball
 Unit VIII Problem 8 Anatomy: Orbit and Eyeball - The bony orbit: it is protecting our eyeball and resembling a pyramid: With a base directed: anterolaterally. And an apex directed: posteromedially. Notes:
Unit VIII Problem 8 Anatomy: Orbit and Eyeball - The bony orbit: it is protecting our eyeball and resembling a pyramid: With a base directed: anterolaterally. And an apex directed: posteromedially. Notes:
Retinoblastoma. Protocol applies to retinoblastoma only.
 Retinoblastoma Protocol applies to retinoblastoma only. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Retinoblastoma Protocol applies to retinoblastoma only. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Ultrasound B-Scan for Posterior Segment Evaluation
 Retina Ultrasound B-Scan for Posterior Segment Evaluation Shalini Singh MS Shalini Singh MS, Manisha Agarwal MS, Aditya Bansal DNB Dr. Shroff s Charity Eye Hospital, New Delhi B reproducible investigation
Retina Ultrasound B-Scan for Posterior Segment Evaluation Shalini Singh MS Shalini Singh MS, Manisha Agarwal MS, Aditya Bansal DNB Dr. Shroff s Charity Eye Hospital, New Delhi B reproducible investigation
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Retinal nerve fiber layer thickness in Indian eyes with optical coherence tomography
 Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Noel de Jesus Atienza, MD, MSc and Joseph Anthony Tumbocon, MD
 Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Glaucoma Clinical Update. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Ophthalmoscopic Evaluation of the Optic Nerve Head JOST B. JONAS, MD, WIDO M. BUDDE, MD, AND SONGHOMITRA PANDA-JONAS, MD
 SURVEY OF OPHTHALMOLOGY VOLUME 43 NUMBER 4 JANUARY FEBRUARY 1999 MAJOR REVIEW Ophthalmoscopic Evaluation of the Optic Nerve Head JOST B. JONAS, MD, WIDO M. BUDDE, MD, AND SONGHOMITRA PANDA-JONAS, MD Department
SURVEY OF OPHTHALMOLOGY VOLUME 43 NUMBER 4 JANUARY FEBRUARY 1999 MAJOR REVIEW Ophthalmoscopic Evaluation of the Optic Nerve Head JOST B. JONAS, MD, WIDO M. BUDDE, MD, AND SONGHOMITRA PANDA-JONAS, MD Department
QUANTIFICATION OF PROGRESSION OF RETINAL NERVE FIBER LAYER ATROPHY IN FUNDUS PHOTOGRAPH
 QUANTIFICATION OF PROGRESSION OF RETINAL NERVE FIBER LAYER ATROPHY IN FUNDUS PHOTOGRAPH Hyoun-Joong Kong *, Jong-Mo Seo **, Seung-Yeop Lee *, Hum Chung **, Dong Myung Kim **, Jeong Min Hwang **, Kwang
QUANTIFICATION OF PROGRESSION OF RETINAL NERVE FIBER LAYER ATROPHY IN FUNDUS PHOTOGRAPH Hyoun-Joong Kong *, Jong-Mo Seo **, Seung-Yeop Lee *, Hum Chung **, Dong Myung Kim **, Jeong Min Hwang **, Kwang
Corporate Medical Policy
 Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: Origination: Last CAP Review: Next CAP Review: Last Review: optical_coherence_tomography_(oct)_anterior_segment_of_the_eye
Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: Origination: Last CAP Review: Next CAP Review: Last Review: optical_coherence_tomography_(oct)_anterior_segment_of_the_eye
Glaucoma: Diagnostic Modalities
 Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
OtticaFisiopatologica
 Anno quindicesimo dicembre 2010 How to assess the retinal nerve fiber layer thickness Antonio Ferreras Miguel Servet University Hospital, Zaragoza. Aragón Health Sciences Institute University of Zaragoza
Anno quindicesimo dicembre 2010 How to assess the retinal nerve fiber layer thickness Antonio Ferreras Miguel Servet University Hospital, Zaragoza. Aragón Health Sciences Institute University of Zaragoza
Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature of
 1.2.4 OPHTHALMOLOGICAL ABNORMALITIES Ocular abnormalities are well documented in patients with NPS 6 62 81 95. 1.2.4.1 Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature
1.2.4 OPHTHALMOLOGICAL ABNORMALITIES Ocular abnormalities are well documented in patients with NPS 6 62 81 95. 1.2.4.1 Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature
Corporate Medical Policy
 Corporate Medical Policy Glaucoma, Evaluation by Ophthalmologic Techniques File Name: Origination: Last CAP Review: Next CAP Review: Last Review: glaucoma_evaluation_by_ophthalmologic_techniques 3/2001
Corporate Medical Policy Glaucoma, Evaluation by Ophthalmologic Techniques File Name: Origination: Last CAP Review: Next CAP Review: Last Review: glaucoma_evaluation_by_ophthalmologic_techniques 3/2001
Apoptosis in Retinal Ganglion Cell Decrease in Human Glaucomatous Eyes
 ELSEVIER Apoptosis in Retinal Ganglion Cell Decrease in Human Glaucomatous Eyes Shigekuni Okisaka, Akira Murakami, Atsushi Mizukawa and Junji Ito Department of Ophthalmology, National Defense Medical College,
ELSEVIER Apoptosis in Retinal Ganglion Cell Decrease in Human Glaucomatous Eyes Shigekuni Okisaka, Akira Murakami, Atsushi Mizukawa and Junji Ito Department of Ophthalmology, National Defense Medical College,
Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD
 Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD A 68 year old white woman had a new onset of floaters in her right eye and was found to have
Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD A 68 year old white woman had a new onset of floaters in her right eye and was found to have
A Review Of Risk Factors. Early Detection Of Glaucoma Clinical Clues. A risk factor analysis is critical. Points To Live By
 A Review Of Risk Factors Early Detection Of Glaucoma Clinical Clues Eric E. Schmidt, O.D. Omni Eye Specialists Wilmington, NC schmidtyvision@msn.com FINDACAR Family history IOP Nearsightedness Diabetes/Vascular
A Review Of Risk Factors Early Detection Of Glaucoma Clinical Clues Eric E. Schmidt, O.D. Omni Eye Specialists Wilmington, NC schmidtyvision@msn.com FINDACAR Family history IOP Nearsightedness Diabetes/Vascular
A Survey on Localizing Optic Disk
 International Journal of Information & Computation Technology. ISSN 0974-2239 Volume 4, Number 14 (2014), pp. 1355-1359 International Research Publications House http://www. irphouse.com A Survey on Localizing
International Journal of Information & Computation Technology. ISSN 0974-2239 Volume 4, Number 14 (2014), pp. 1355-1359 International Research Publications House http://www. irphouse.com A Survey on Localizing
O ptic disc cupping detected in glaucoma patients by
 251 EXTENDED REPORT Alterations in the morphology of lamina cribrosa pores in glaucomatous eyes G Tezel, K Trinkaus, M B Wax... See end of article for authors affiliations... Correspondence to: Gülgün
251 EXTENDED REPORT Alterations in the morphology of lamina cribrosa pores in glaucomatous eyes G Tezel, K Trinkaus, M B Wax... See end of article for authors affiliations... Correspondence to: Gülgün
Is NTG different from POAG?
 Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
The Orbit. The Orbit OCULAR ANATOMY AND DISSECTION 9/25/2014. The eye is a 23 mm organ...how difficult can this be? Openings in the orbit
 The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
CHAPTER 2 LITERATURE REVIEW
 CHAPTER 2 LITERATURE REVIEW 2.1 Introduction The retina is a light-sensitive tissue lining the inner surface of the eye. The optics of the eye create an image of the visual world on the retina, which serves
CHAPTER 2 LITERATURE REVIEW 2.1 Introduction The retina is a light-sensitive tissue lining the inner surface of the eye. The optics of the eye create an image of the visual world on the retina, which serves
Heterogeneous Distribution of Axonal Cytoskeleton Proteins in the Human Optic Nerve
 Heterogeneous Distribution of Axonal Cytoskeleton Proteins in the Human Optic Nerve Chandrakumar Balaratnasingam, William H. Morgan, Victoria Johnstone, Stephen J. Cringle, and Dao-Yi Yu PURPOSE. Cytoskeleton
Heterogeneous Distribution of Axonal Cytoskeleton Proteins in the Human Optic Nerve Chandrakumar Balaratnasingam, William H. Morgan, Victoria Johnstone, Stephen J. Cringle, and Dao-Yi Yu PURPOSE. Cytoskeleton
Confocal Adaptive Optics Imaging of Peripapillary Nerve Fiber Bundles: Implications for Glaucomatous Damage Seen on Circumpapillary OCT Scans
 Article DOI: 10.1167/tvst.4.2.12 Confocal Adaptive Optics Imaging of Peripapillary Nerve Fiber Bundles: Implications for Glaucomatous Damage Seen on Circumpapillary OCT Scans Donald C. Hood 1, Monica F.
Article DOI: 10.1167/tvst.4.2.12 Confocal Adaptive Optics Imaging of Peripapillary Nerve Fiber Bundles: Implications for Glaucomatous Damage Seen on Circumpapillary OCT Scans Donald C. Hood 1, Monica F.
The Number ond Diameter Distribution of Axons in the Monkey Optic Nerve
 The Number ond Diameter Distribution of Axons in the Monkey Optic Nerve Ralph M. Sanchez, Gregory R. Dunkelberger, and Harry A. Quigley Using an automated image analysis system, cross-sections from optic
The Number ond Diameter Distribution of Axons in the Monkey Optic Nerve Ralph M. Sanchez, Gregory R. Dunkelberger, and Harry A. Quigley Using an automated image analysis system, cross-sections from optic
