Neuroradiology/Head and Neck Imaging Original Research
|
|
|
- Delphia Sheryl Hicks
- 6 years ago
- Views:
Transcription
1 Neuroradiology/Head and Neck Imaging Original Research Lee et al. Visual Defects Noted on MRI Examination of Patients With Pituitary denomas Neuroradiology/Head and Neck Imaging Original Research In Ho Lee 1, 2 Neil R. Miller 3 Elcin Zan 1 Fabiana Tavares 1 ri M. litz 1 Heejong Sung 4 David M. Yousem 1 Michael V. oland 3 Lee IH, Miller NR, Zan E, et al. Keywords: optic chiasm, pituitary adenoma, visual deficits DOI:.2214/JR Received February 7, 215; accepted after revision pril 16, 215. The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as representing the views of the National Institutes of Health. 1 Russell H. Morgan Department of Radiology and Radiological Sciences, The Johns Hopkins Medical Institutions, 6 N Wolfe St, Phipps F, altimore, MD ddress correspondence to D. M. Yousem (dyousem1@jhu.edu). 2 Department of Radiology, Chungnam National University Hospital, Daejeon, Korea. 3 Wilmer Eye Institute, The Johns Hopkins Medical Institutions, altimore, MD. 4 Genometrics Section, Computational and Statistical Genomics ranch, National Human Genome Research Institute, National Institutes of Health, altimore, MD. WE This is a web exclusive article. JR 215; 25:W512 W X/15/255 W512 merican Roentgen Ray Society Visual Defects in Patients With Pituitary denomas: The Myth of itemporal Hemianopsia OJECTIVE. The objective of this study was to test the hypothesis that bitemporal hemianopsia (H) is the most common visual field (VF) defect in patients with pituitary macroadenoma and to assess the degree of optic pathway compression necessary to produce visual defects. MTERILS ND METHODS. We reviewed the MRI findings and medical records of 119 patients with pituitary macroadenoma who had undergone formal assessment of VFs. We then evaluated the degree of optic pathway displacement caused by the pituitary macroadenoma, as observed on MR images. The classifications of optic pathway displacement included no contact, abutment but no displacement, mild displacement (< 3 mm), and moderate displacement ( 3 mm). Qualitative analysis classified VFs as normal or as having defects that were monocular, bitemporal, mixed (bitemporal with additional defects), homonymous, or nonspecific. RESULTS. total of 89 of 115 patients had an abnormal VF. Only one patient had true H. The most common defects were bitemporal or mixed defects (in 49 of 115 patients [42.6%]), likely because more than just the chiasm is often compressed by the pituitary macroadenoma. Classification of optic pathway displacement by the pituitary macroadenoma was as follows: 23 patients had no contact, eight had abutment but no displacement, 27 had mild displacement, and 57 had moderate displacement. In 78 of the 92 patients (84.8%) with pituitary macroadenoma that had contact with the optic pathway, contact was with the optic chiasm and the prechiasmal optic nerve. Of the 49 patients with bitemporal or mixed defects, 42 had moderate displacement of the optic pathway caused by their tumors. CONCLUSION. H is exceedingly uncommon in patients with pituitary macroadenoma. However, although bitemporal and mixed defects are the most common abnormal VF findings, they were found in only 42.6% of patients. Such defects rarely occur if the tumor displaces the optic pathway less than 3 mm from baseline. W hen most neuroradiologists consider the visual field (VF) deficits associated with pituitary adenomas that compress the chiasm, they automatically think of bitemporal hemianopsia (H). This is a VF deficit in which all the vision in the temporal fields of both eyes is lost, leaving only the nasal fields to be perceived. Incomplete bitemporal VF defects are much more common than true hemianopsia and are considered by neuroophthalmologists as a sign characteristic of chiasmal syndrome, which is usually caused by lesions that affect the optic chiasm from below [1]. Pituitary adenomas are the most common of all chiasmal syndrome tumors, followed by other lesions that cause extrinsic optic chiasm compression, such as me- ningiomas, craniopharyngiomas, and aneurysms [2, 3]. The visual deficits associated with pituitary adenoma depend on the size, location, and hormonal activity of the tumor as well as the position of the chiasm as it relates to the sella turcica [4]. ccording to a recent study, the tumor volume also affects the severity of the VF defect [5, 6]. lthough a previous study of 5 patients showed a significant correlation between chiasmal compression and visual disturbances [7], to our knowledge, no MRI-based literature shows the relationship between the degree and symmetry of extrinsic anterior visual pathway compression by pituitary macroadenoma and the pattern of VF defects observed in patients. One goal of this study W512 JR:25, November 215
2 Visual Defects Noted on MRI Examination of Patients With Pituitary denomas was to test the hypothesis that bitemporal VF defects, not H, are the most common defect in patients with pituitary macroadenoma. We also wished to determine what degree of optic chiasm compression is necessary to produce such defects and how often asymmetric visual defects are associated with pituitary macroadenoma that asymmetrically affects the prechiasmal optic nerves, optic chiasm, or postchiasmal optic tracts. Materials and Methods This retrospective study was reviewed and approved by the institutional review board of The Johns Hopkins University School of Medicine. ecause of the retrospective nature of the study, informed consent was not required for review of either the medical records or the MR images. We retrospectively searched our imaging archive for patients who had pituitary macroadenoma diagnosed by MRI between November 29 and October 212. In all patients, at least one dimension of the pituitary macroadenoma measured at least mm. We then reviewed the imaging findings and medical records of the 185 patients who were identified using this strategy. Sixty-six patients were excluded either because they did not have any VF testing results available or because they had other underlying diseases, such as stroke, glaucoma, ocular or intracranial trauma, retinal artery occlusion, other retinal diseases, amblyopia, or unrelated optic neuropathy, all of which could affect the results of VF testing. Next, we reviewed the clinical findings and ophthalmologic records of the remaining 119 patients who were included in the study, including documentation of VF defects and reported visual complaints. ll VF tests were performed using a Humphrey Field nalyzer (Carl Zeiss Meditec). Test patterns were either 24 2 or 3 2, and strategies included use of the Swedish interactive threshold algorithm or full threshold. Qualitative Visual Field nalysis Qualitative analysis of the VF tests was performed by two experienced ophthalmologists (one with years of experience and one with 4 years of experience) who were blinded to the MRI findings. fter assessments were performed independently, the analyses were compared jointly, and any differences in grading were adjudicated by consensus. VF test findings were classified as normal (i.e., no defect), unreliable, or as one of the following types of defect: bitemporal (bitemporal defect only, including H), mixed (bitemporal and additional defects), monocular, homonymous, nonspecific, or other. H, which was included as one type of a bitemporal field defect, was diagnosed when the defect affected the entire outer (or lateral) half of the VF in each eye. bitemporal defect was diagnosed when the defect affected the outer (or lateral) half of the VF in each eye, whereas a mixed defect was diagnosed when the defect involved not only the outer (or lateral) half of the VF of both eyes but also other areas of the VF in one or both eyes. monocular defect was defined as the presence of any VF defect in one eye and a normal VF in the other eye. homonymous defect was defined as a defect that was present in the temporal (outer) field of one eye and the nasal (inner) field of the other eye and, for the purpose of this study, was thought to be consistent with a compressive lesion in the region of the chiasm. Nonspecific defects were defined as defects that could not clearly be attributed to a particular ocular or neurologic process. The other category identified defects that the evaluators thought were not likely caused by the tumor. Finally, unreliable test results were defined as results associated with excessive false-positive responses, false-negative responses, or fixation losses still requiring interpretation. Qualitative analysis of the degree of asymmetry in VF loss between the right and left eyes was also performed for patients with bitemporal, mixed, or homonymous defects. The scale used in such analysis included the following categories of asymmetry: significantly more left, somewhat more left, symmetric, somewhat more right, and significantly more right. The four patients who were found to have unreliable results of VF testing or who received a diagnosis consistent with other ocular or neurologic diseases were excluded from further analysis. nalysis of MR Images Each patient underwent an MRI examination that consisted of a standard protocol of sagittal and coronal T1-weighted and CISS/FIEST (constructive interference in steady state fast imaging employing steady-state acquisition) sequences performed before and after gadolinium contrast agent administration. ll sections were 3 mm or thinner. We evaluated the degree of displacement of the prechiasmal optic nerve, optic chiasm, and postchiasmal optic tract by the pituitary macroadenoma. If there was symmetric displacement, we determined the degree of displacement relative to the expected normal location of the visual pathway. If there was bilateral but asymmetric displacement, we compared the displacement on each side with the expected location of the visual apparatus. Finally, if there was unilateral displacement, we determined the displacement of the affected side relative to the position of the unaffected side. In all cases, the degree of optic pathway displacement was classified as no contact, abutment but not displacement, mild displacement (< 3 mm of displacement), or moderate displacement ( 3 mm of displacement) (Fig. 1). We selected the maximum displacement when more than two parts of the optic pathway were displaced by the pituitary macroadenoma. Two neuroradiologists (one with 8 years of experience and one with 3 years of experience) independently measured displacement with the use of electronic calipers. The mean of the two recorded displacements was used, unless there was a discrepancy of more than 3 mm, in which case an adjudication was performed by a third neuroradiologist (with 25 years of experience), who was blinded to the measurements of the other two neuroradiologists. symmetry from right to left in the degree of compression of the optic pathway on MRI was evaluated subjectively (Fig. 2). djudication was performed in the same manner as it was for displacement. We also recorded changes in signal intensity on T2-weighted or FLIR sequences, contrast enhancement, and atrophy anywhere along the optic pathway and determined the presence of hemorrhage in the pituitary lesions. The imaging parameters used for the sagittal thin T1-weighted sequence were as follows: TR/TE, 45/9.5; matrix, ; FOV, mm; and section thickness, 2 mm. The coronal thin T1-weighted sequence was obtained using the following parameters: TR/TE, 45/9.5; matrix, ; FOV, mm; and section thickness, 2 mm. The parameters used to obtain the axial T2-weighted sequence were TR/TE, 45/89; matrix, ; FOV, mm; and section thickness, 4 mm. FLIR sequence parameters were as follows: TR/TE, 9/5; inversion time, 25 ms; matrix, 32 32; FOV, mm; and section thickness, 4 mm. The contrast-enhanced thin coronal T1-weighted sequence was obtained using the following parameters: TR/TE, 5/9.5; matrix, ; FOV, mm; and section thickness, 2 mm. The contrast-enhanced thin sagittal T1-weighted sequence was obtained with the use of the parameters TR/TE, 45/9.4; matrix, ; FOV, mm; and section thickness, 2 mm. The parameters used to obtain the contrast-enhanced axial T1-weighted sequence were TR/TE, 55/12; matrix, 32 32; FOV, mm; and section thickness, 4 mm. The contrast-enhanced coronal T1-weighted sequence was obtained using the following parameters: TR/TE, 65/9.1; matrix, 32 32; FOV, mm; and section thickness, 4 mm. Results Of the 115 patients (49 women and 66 men; mean [± SD] age, 54.7 ± 6.2 years; age range, JR:25, November 215 W513
3 Lee et al. C Fig. 1 MRI classification of degree of optic pathway displacement in patients with pituitary macroadenoma., MR image shows no contact between optic pathway and pituitary macroadenoma., MR image shows pituitary macroadenoma abutting but not displacing optic pathway. C, MR image shows less than 3 mm of displacement (i.e., mild displacement) of optic pathway caused by compression by pituitary macroadenoma. D, MR image shows displacement of 3 mm or more (i.e., moderate displacement) of optic pathway caused by compression by pituitary macroadenoma. Fig. 2 MRI classification of asymmetry in the degree of compression in the optic pathway in patients with pituitary macroadenoma., MR image shows asymmetric displacement of right visual field of optic pathway caused by compression by pituitary macroadenoma., MR image shows asymmetric displacement of optic pathway caused by compression by pituitary macroadenoma. D years), 7 had pathologically proven pituitary macroadenoma, whereas 45 had pituitary macroadenoma diagnosed on the basis of clinical findings, hormonal analysis, and imaging findings. The height of the 115 lesions ranged from.4 to 5 cm (mean, 2.17 ±.79 cm). Of the patients studied, 57 (49.6%) had moderate displacement (range, 3 21 mm) of the optic apparatus by the pituitary macroadenoma (Figs. 3 and 4), 27 (23.5%) had mild displacement, and eight (7%) had abutment but no displacement. In the remaining 23 patients (2%), the lesion had no contact with any optic pathway structures. Of the 92 patients with pituitary macroadenoma showing contact with parts of the optic pathway, 79 (85.9%) had contact with two or more areas. The areas of contact were the prechiasmal optic nerve and optic chiasm (58 patients); the prechiasmal optic nerve, optic chiasm, and postchiasmal optic tract (2 patients); and the optic chiasm and postchiasmal optic tract (one patient). In the remaining 13 patients, the lesion had contact with only one area: the optic chiasm (nine patients) or the prechiasmal optic nerve (four patients) (Fig. 5). Sixty-three patients had no documented visual complaints. The other 52 patients complained of visual disturbances, including blurred vision (2 patients), diplopia (four patients), or visual change (28 patients). symptomatic Subjects Sixty-three patients had no visual complaints at presentation; in 14 of these patients (22.2%), the tumors had no contact with the optic pathway. In the remainder of the patients, tumor contact with the optic pathway was as follows: four patients (6.3%) had tumor abutment but no displacement, 2 (31.7%) had mild displacement, and 25 (39.7%) had moderate displacement. The formal VF test findings for these asymptomatic patients were classified as follows: 18 patients (28.6%) had normal findings, 14 (22.2%) had bitemporal defects (without H), six (9.5%) had mixed defects, one (1.6%) had homonymous defects, eight (12.7%) had monocular defects, and 16 (25.4%) had nonspecific defects (Fig. 6). Symptomatic Subjects Fifty-two patients had visual complaints at presentation; in nine of these patients (17.3%), the tumor had no contact with the optic pathway. In the remainder of the patients, tumor contact with the optic pathway was as fol- W514 JR:25, November 215
4 Visual Defects Noted on MRI Examination of Patients With Pituitary denomas Fig. 3 Patient with pituitary macroadenoma. and, Measurement of optic pathway displacement at level of prechiasmal optic nerve. Coronal unenhanced () and contrast-enhanced () T1-weighted MR images show 6 mm of displacement of prechiasmal optic nerve. Normal position of optic pathway (bar, ) and distance from normal position (arrow, ) are shown. Fig. 4 Patient with pituitary macroadenoma. and, Measurement of optic pathway displacement at level of optic chiasm. Coronal unenhanced () and contrast-enhanced () T1-weighted MR images show 9 mm of displacement of optic chiasm. Normal position of optic pathway (bar, ) and distance from normal position (arrow, ) are shown. Pituitary Macroadenomas (no.) Prechiasmal Optic Nerve Prechiasmal Optic Nerve and Optic Chiasm Prechiasmal Optic Nerve, Optic Chiasm, and Postchiasmal Optic Tract Optic Nerve and Postchiasmal Optic Tract rea(s) of Contact With Optic Pathway Optic Chiasm Fig. 5 Graph showing relationship between optic pathway and pituitary macroadenoma in 92 patients with pituitary macroadenoma that had contact with optic pathway. lows: four patients (7.7%) had abutment but no displacement, seven patients (13.6%) had mild displacement, and 32 (61.5%) had moderate displacement. For these symptomatic patients, VF test results were graded as follows: eight patients (15.4%) had normal findings, 15 (28.8%) had bitemporal defects (with only one H noted among these 15 patients), 14 (26.9%) had mixed defects, four (7.7%) had monocular defects, and 11 (2.1%) had nonspecific defects (Fig. 7). Visual Field nalysis Overall, 89 patients (77.4%) had abnormal VFs, and 26 patients (22.6%) had normal VFs. Of the 89 patients with abnormal VFs, bitemporal or mixed defects were present in 49 patients (representing 55.1% of this group and 42.6% of all 115 subjects) and were the most common patterns, followed by nonspecific defects (27 patients), monocular defects (12 patients), and homonymous defects (one patient) (Fig. 8). Of the 49 patients with bitemporal or mixed defects, 42 (85.7%) had moderate displacement (range, 4 21 mm), five (.2%) had mild displacement, and two (4.1%) had lesions with no contact with the optic pathway. Of the 49 patients with bitemporal field deficits, only one patient had H. This patient had moderate displacement of the optic pathway. When moderate displacement (optic pathway displacement greater than 3 mm) was used as the criterion for identifying bitemporal or mixed defects, VF testing had a sensitivity of 85.7% (42/49), specificity of 75% (3/4), a positive predictive value of 8.8% (42/52), a negative predictive value of 81.1% (3/37), and accuracy of 8.9% (72/89). When the 27 patients with nonspecific VF defects were excluded, 42 of 49 patients (85.7%) with bitemporal or mixed defects had moderate optic pathway displacement resulting from masses, whereas two of 13 patients (15.4%) with atypical, homonymous, or monocular defects had moderate displacement. symmetry For 41 of 115 patients, asymmetry in the degree of compression of the optic pathway noted on MR images was from right (15 patients) to left (26 patients). symmetry in the degree of VF damage between right and left eyes was also noted in 39 of 49 patients (79.6%) with bitemporal or mixed defects, and symmetry was noted in of 49 patients (2.4%). For predicting asymmetry of the right and left VFs, MRI JR:25, November 215 W515
5 Lee et al. had a sensitivity of 43.6% (17 of 39 patients), specificity of 8% (8 of patients), a positive predictive value of 89.5% (17 of 19 patients), a negative predictive value of 26.7% (8 of 3 patients), and accuracy of 51% (25 of 49 patients) (Fig. 9). One of the 115 patients (.9%) had atrophy of the optic chiasm, and 19 (16.5%) had hemorrhage. With the exception of one patient (.9%) who had high signal intensity noted in the left postchiasmal optic tract on T2-weighted or FLIR images, we did not find any signal change on T2-weighted or FLIR images. There was no optic pathway component enhancement. The patient who had high signal intensity noted on T2-weighted or FLIR images had a mixed VF defect Moderate Mild Discussion Our study confirms that the classic finding of pure H in patients with pituitary macroadenoma is a myth; only one of the 115 patients in our cohort had this defect. In fact, the VF defects in our patients with pituitary macroadenoma were purely bitemporal (even if incomplete) in only 29 of 115 patients (25.2%); we found mixed defects with areas of VF loss outside the temporal fields in 2 of 115 patients (17.4%). These findings are comparable to those of other neuroophthalmologic studies, which found that pure Hs are rare compared with bitemporal defects, with the former occurring in only approximately 1% of patients with pituitary macroadenoma [1, 8, 9]. We also found that patients with macroadenoma may have other defects, including monocular or homonymous defects [5, 12]. Indeed, 4 of the 89 patients with VF defects (44.9%) had nontemporal defects. This may have resulted from compression of prechiasmal optic nerves or postchiasmal tracts. Involvement of prechiasmal optic nerves or postchiasmal tracts was seen in 82 and 21 patients, respectively. Of the patients with preand postchiasmal compression, 79 also had optic chiasm compression. Only nine patients had pure optic chiasm compression alone. Thus, it is more common to have extrachiasmal optic pathway involvement along with compression of the chiasm, rather than just chiasm compression alone. Previous studies did not evaluate extrachiasmal compression, evaluating only chiasmal compression instead. In general, VF defects (whether bitemporal, mixed, homonymous, or monocular) correlated with the degree of optic pathway displacement noted, with 71% of patients with VF defects having moderate optic pathway displacement that ranged from 4 to 21 mm. Eight patients in this study had abnormal VFs, a finding that was thought to be consistent with optic pathway damage resulting from their tumors, although MRI examination of these patients revealed no contact between the tumor and the optic apparatus. It is possible that in some of these patients, the VF defect was spurious or related to a process other than the tumor. lternatively, some studies have theorized that the discovery of butting Tumor Contact With Optic Pathway No Contact Normal Nonspecific defects Monocular defects Homonymous defects itemporal or misdefects Fig. 6 Graph showing relationship between displacement of optic pathway and visual fields in 63 patients without visual complaints Moderate Mild butting Tumor Contact With Optic Pathway No Contact Normal Nonspecific defects Monocular defects Homonymous defects itemporal or misdefects Fig. 7 Graph showing relationship between displacement of optic pathway and visual fields in 52 patients with visual complaints. abnormal VFs in patients who have pituitary tumors that do not appear to be in contact with the optic apparatus may be attributed to previous indentation (and subsequent tumor regression), hormonal influences, intratumor hemorrhage, autonecrosis, or vascular shunting [13]. In our study, the smallest displacement of the optic apparatus from its expected normal position in a patient with a presumed related VF defect was 4 mm on the coronal plane, compared with previous reports indicating a minimum displacement of mm [7, 9]. This discrepancy may W516 JR:25, November 215
6 Visual Defects Noted on MRI Examination of Patients With Pituitary denomas Moderate Mild be attributed to differences in the measurement methods used in our study and previous studies. The studies by Ikeda and Yoshimoto [7] and Schmalisch et al. [9] measured the degree of displacement of the optic chiasm from the upper surface of the internal carotid artery within the cavernous sinus, whereas our study measured the degree of displacement from the expected normal (presumed) location, according to the course of the optic pathway from the optic canal to the optic tract. Even if there are differences in the methods used by the three studies, the notion that optic pathway displacement by pituitary adenomas contributes to visual symptoms is supported by our study. butting Tumor Contact With Optic Pathway No Contact Normal Nonspecific defects Monocular defects Homonymous defects itemporal or misdefects Fig. 8 Graph showing relationship between displacement of optic pathway and visual fields in all 115 study patients Right symmetry Symmetry Left symmetry Results of Visual Field Testing Right asymmetry on MRI Symmetry on MRI Left asymmetry on MRI Fig. 9 Graph showing relationship of asymmetry between MRI and qualitative analysis of visual field test. In this study, a change in the signal intensity noted in the optic apparatus on T2-weighted or FLIR images was exceedingly rare, occurring in only one of 115 patients. This finding is counter to the results reported in a previous study [14]. symmetry in VF abnormalities was also noted and was confirmed by qualitative analysis of the VFs (in 39 of 49 patients [79.6%]) and by MRI (in 41 of 115 patients [35.7%]). This asymmetry has been reported to be a very common finding of VF testing of patients with pituitary adenomas [11, 15]. This asymmetry may also be attributed to a different nerve fiber strain between the nasal and temporal nerve fibers of bilateral eyes [16]. In our study, asymmetry was noted on the MR images of 41 of 115 patients (35.7%), with MRI therefore having 43.6% sensitivity and 8% specificity for predicting asymmetry on the VF test. This sensitivity and specificity may be attributed to multiple factors, including the patient s health status and hormonal status, the follow-up period, and the location and shape of tumor. However, the high positive predictive value (89.5%) of MRI in predicting asymmetry of the right and left VFs suggests that when MRI shows asymmetry to one side, there very frequently is asymmetry in VF damage. There are several limitations of this study. First, not all of the patients had pathologically proven tumors; thus, it is possible (although unlikely) that some of the lesions were not adenomas. Second, there was a wide interval (mean, 48.2 ± 42.8 days; range, 175 days) between MRI examination and VF testing, although there was no documented statistically significant change in the size of pituitary macroadenoma noted on serial MR images. Third, there were three patients without a contrast-enhanced study and two patients without T2-weighted or FLIR images. Finally, there likely is selection bias for patients with visual symptoms to be referred for VF analysis. Conclusion Complete H associated with pituitary macroadenoma is rare, occurring in only one of 115 patients in our cohort. On the other hand, bilateral temporal VF defects, either pure or associated with additional defects, are the most common defects noted in patients with pituitary macroadenoma, occurring in 42.6% of all patients. Most patients had compression of the prechiasmal optic nerves, the postchiasmal tracts, or both, in addition to compression of the chiasm, which may account for these impure VF findings that include areas outside the bitemporal zones. Such defects are typically present in patients with greater than 3 mm of displacement of the optic apparatus. In addition, patients with asymmetric compression of the optic pathway seen on MR images are likely to have asymmetric VF defects. References 1. Schiefer U, Isbert M, Mikolaschek E, et al. Distribution of scotoma pattern related to chiasmal lesions with special reference to anterior junction syndrome. Graefes rch Clin Exp Ophthalmol 24; 242: Foroozan R. Chiasmal syndromes. Curr Opin JR:25, November 215 W517
7 Lee et al. Ophthalmol 23; 14: PJ, Danesh-Meyer HV. Visual acuity and pattern manifesting as homonymous hemianopia. Jpn J 3. Jacobs D, Galetta SL. Neuro-ophthalmology for of visual field loss at presentation in pituitary ad- Ophthalmol 27; 51: neuroradiologists. JNR 27; 28:3 8 enoma. J Clin Neurosci 214; 21: Levy. Pituitary disease: presentation, diagno- 4. Kapoor S. cromegaly. N Engl J Med 27; 9. Schmalisch K, Milian M, Schimitzek T, Lagrèze sis, and management. J Neurol Neurosurg Psy- 356: [author reply, ] W, Honegger J. Predictors for visual dysfunc- chiatry 24; 75:iii47 iii52 5. Lee JP, Park IW, Chung YS. The volume of tumor tion in nonfunctioning pituitary adenomas: impli- 14. Saeki N, Uchino Y, Murai H, et al. MR imaging mass and visual field defect in patients with pituitary macroadenoma. Korean J Ophthalmol 211; 25: Kan E, Kan EK, tmaca, tmaca H, Colak R. Visual field defects in 23 acromegalic patients. Int Ophthalmol 213; 33: Ikeda H, Yoshimoto T. Visual disturbances in patients with pituitary adenoma. cta Neurol Scand 1995; 92: Ogra S, Nichols D, Stylli S, Kaye H, Savino cations for neurosurgical management. Clin Endocrinol (Oxf) 212; 77: Hershenfeld S, Sharpe J. Monocular temporal hemianopia. r J Ophthalmol 1993; 77: Rivoal O, rézin P, Feldman-illard S, Luton JP. Goldmann perimetry in acromegaly: a survey of 37 cases from 1951 through Ophthalmology 2; 7: Nishimura M, Kurimoto T, Yamagata Y, Ikemoto H, rita N, Mimura O. Giant pituitary adenoma study of edema-like change along the optic tract in patients with pituitary region tumors. JNR 23; 24: Poon, McNeill P, Harper, O Day J. Patterns of visual loss associated with pituitary macroadenomas. ust N Z J Ophthalmol 1995; 23: Wang X, Neely J, McIlwaine GG, Lueck CJ. Multi-scale analysis of optic chiasmal compression by finite element modelling. J iomech 214; 47: W518 JR:25, November 215
Criteria for early CLINICAL STUDY. N Fujimoto 1, N Saeki 2, O Miyauchi 1
 (2002) 16, 731 738 2002 Nature Publishing Group All rights reserved 0950-222X/02 $25.00 www.nature.com/eye N Fujimoto 1, N Saeki 2, O Miyauchi 1 Criteria for early and E Adachi-Usami 1 detection of temporal
(2002) 16, 731 738 2002 Nature Publishing Group All rights reserved 0950-222X/02 $25.00 www.nature.com/eye N Fujimoto 1, N Saeki 2, O Miyauchi 1 Criteria for early and E Adachi-Usami 1 detection of temporal
Factors Influencing Visual Field Recovery after Transsphenoidal Resection of a Pituitary Adenoma
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(6):488-496 https://doi.org/10.3341/kjo.2017.0094 Original Article Factors Influencing Visual Field Recovery after Transsphenoidal Resection
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(6):488-496 https://doi.org/10.3341/kjo.2017.0094 Original Article Factors Influencing Visual Field Recovery after Transsphenoidal Resection
In some patients with pituitary macroadenoma, visual acuity
 ORIGINAL RESEARCH A.M. Tokumaru I. Sakata H. Terada S. Kosuda H. Nawashiro M. Yoshii Optic Nerve Hyperintensity on T2-Weighted Images among Patients with Pituitary Macroadenoma: Correlation with Visual
ORIGINAL RESEARCH A.M. Tokumaru I. Sakata H. Terada S. Kosuda H. Nawashiro M. Yoshii Optic Nerve Hyperintensity on T2-Weighted Images among Patients with Pituitary Macroadenoma: Correlation with Visual
Visual pathways in the chiasm
 Visual pathways in the chiasm Intracranial relationships of the optic nerve Fixation of the chiasm Chiasmatic pathologies The function of the optic chiasm may be altered by the presence of : 4) Artero
Visual pathways in the chiasm Intracranial relationships of the optic nerve Fixation of the chiasm Chiasmatic pathologies The function of the optic chiasm may be altered by the presence of : 4) Artero
Visual Fields at Presentation and after Trans-sphenoidal Resection of Pituitary Adenomas
 Original Article Visual Fields at Presentation and after Trans-sphenoidal Resection of Pituitary Adenomas Renu Dhasmana, MD; Ramesh C Nagpal, MD; Rahul Sharma, MD Krishan K Bansal, MD; Harsh Bahadur, MD
Original Article Visual Fields at Presentation and after Trans-sphenoidal Resection of Pituitary Adenomas Renu Dhasmana, MD; Ramesh C Nagpal, MD; Rahul Sharma, MD Krishan K Bansal, MD; Harsh Bahadur, MD
THE OPTIC CHIASM MAY BE DAMAGED BY A VARIETY
 Clinical Features Associated With Lesions Other Than Pituitary Adenoma in Patients With an Optic Chiasmal Syndrome LUIS J. MEJICO, MD, NEIL R. MILLER, MD, AND LI MING DONG, PHD PURPOSE: Pituitary adenomas
Clinical Features Associated With Lesions Other Than Pituitary Adenoma in Patients With an Optic Chiasmal Syndrome LUIS J. MEJICO, MD, NEIL R. MILLER, MD, AND LI MING DONG, PHD PURPOSE: Pituitary adenomas
No Financial Interest
 Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
A new visual field test in empty sella syndrome: Rarebit perimetry
 European Journal of Ophthalmology / Vol. 18 no. 4, 2008 / pp. 628-632 A new visual field test in empty sella syndrome: Rarebit perimetry G.F. YAVAS 1, T. KÜSBECI 1, O. ESER 2, S.S. ERMIS 1, M. COŞAR 2,
European Journal of Ophthalmology / Vol. 18 no. 4, 2008 / pp. 628-632 A new visual field test in empty sella syndrome: Rarebit perimetry G.F. YAVAS 1, T. KÜSBECI 1, O. ESER 2, S.S. ERMIS 1, M. COŞAR 2,
Pituitary Adenomas: Patterns Of Visual Presentation And Outcome After Transsphenoidal Surgery - An Institutional Experience
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 4 Number 2 Pituitary Adenomas: Patterns Of Visual Presentation And Outcome After Transsphenoidal Surgery - An Institutional Experience
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 4 Number 2 Pituitary Adenomas: Patterns Of Visual Presentation And Outcome After Transsphenoidal Surgery - An Institutional Experience
Differences between Non-arteritic Anterior Ischemic Optic Neuropathy and Open Angle Glaucoma with Altitudinal Visual Field Defect
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
Band atrophy of the optic nerve: A report on different anatomical locations in three patients
 Saudi Journal of Ophthalmology (2013) 27, 65 69 Case Report Band atrophy of the optic nerve: A report on different anatomical locations in three patients Alberto Gálvez-Ruiz, MD a,b, ; Nawal Arishi, MD
Saudi Journal of Ophthalmology (2013) 27, 65 69 Case Report Band atrophy of the optic nerve: A report on different anatomical locations in three patients Alberto Gálvez-Ruiz, MD a,b, ; Nawal Arishi, MD
OCT : retinal layers. Extraocular muscles. History. Central vs Peripheral vision. History: Temporal course. Optical Coherence Tomography (OCT)
 Optical Coherence Tomography (OCT) OCT : retinal layers 7 Central vs Peripheral vision Extraocular muscles RPE E Peripheral Vision: Rods (95 million) 30% Ganglion cells Central Vision: Cones (5 million)
Optical Coherence Tomography (OCT) OCT : retinal layers 7 Central vs Peripheral vision Extraocular muscles RPE E Peripheral Vision: Rods (95 million) 30% Ganglion cells Central Vision: Cones (5 million)
Topical Diagnosis of Chiasmal and Retrochiasmal Disorders
 Topical Diagnosis of Chiasmal and Retrochiasmal Disorders Leonard A. Levin CHAPTER 12 TOPICAL DIAGNOSIS OF OPTIC CHIASMAL LESIONS Visual Field Defects Etiologies of the Optic Chiasmal Syndrome Masqueraders
Topical Diagnosis of Chiasmal and Retrochiasmal Disorders Leonard A. Levin CHAPTER 12 TOPICAL DIAGNOSIS OF OPTIC CHIASMAL LESIONS Visual Field Defects Etiologies of the Optic Chiasmal Syndrome Masqueraders
3/16/2018. Perimetry
 Perimetry The normal visual field extends further away from fixation temporally and inferiorly than superiorly and nasally. From the center of the retina this sensitivity decreases towards the periphery,
Perimetry The normal visual field extends further away from fixation temporally and inferiorly than superiorly and nasally. From the center of the retina this sensitivity decreases towards the periphery,
Learn Connect Succeed. JCAHPO Regional Meetings 2015
 Learn Connect Succeed JCAHPO Regional Meetings 2015 VISUAL FIELDS No financial conflicks Florida Society of Ophthalmology 2015 Gary Schemmer, MD Definition of Visual Field The area in space perceived by
Learn Connect Succeed JCAHPO Regional Meetings 2015 VISUAL FIELDS No financial conflicks Florida Society of Ophthalmology 2015 Gary Schemmer, MD Definition of Visual Field The area in space perceived by
Disclosures. Visual Pathways. Visual Pathways. Visual Loss Understanding the Patterns. I have no financial disclosures. Tabby A.
 Visual oss Understanding the Patterns Tabby A. Kennedy, MD University of Wisconsin Department of adiology I have no financial disclosures Acknowledgements: indell Gentry Greg Avey JP Yu Judy Chen Disclosures
Visual oss Understanding the Patterns Tabby A. Kennedy, MD University of Wisconsin Department of adiology I have no financial disclosures Acknowledgements: indell Gentry Greg Avey JP Yu Judy Chen Disclosures
Imaging The Turkish Saddle. Russell Goodman, HMS III Dr. Gillian Lieberman
 Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports-
 Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
Loss and recovery of vision with suprasellar meningiomas F. KARL GREGORIUS, M.D., ROBERT S. HEPLER, M.D., AND W. EUGENE STERN, M.D.
 Loss and recovery of vision with suprasellar meningiomas F. KARL GREGORIUS, M.D., ROBERT S. HEPLER, M.D., AND W. EUGENE STERN, M.D. Department of Surgery, Division of Neurosurgery, and the Department of
Loss and recovery of vision with suprasellar meningiomas F. KARL GREGORIUS, M.D., ROBERT S. HEPLER, M.D., AND W. EUGENE STERN, M.D. Department of Surgery, Division of Neurosurgery, and the Department of
Imaging pituitary gland tumors
 November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
HOMONYMOUS VISUAL FIELD DEFECTS Perimetric findings and corresponding neuro-imaging results
 Homonymous visual field defects 511 HOMONYMOUS VISUAL FIELD DEFECTS Perimetric findings and corresponding neuro-imaging results JAN SCHILLER 1, TRAUGOTT J. DIETRICH 1, LIESE LORCH 1, MARTIN SKALEJ 2, CHRISTOPH
Homonymous visual field defects 511 HOMONYMOUS VISUAL FIELD DEFECTS Perimetric findings and corresponding neuro-imaging results JAN SCHILLER 1, TRAUGOTT J. DIETRICH 1, LIESE LORCH 1, MARTIN SKALEJ 2, CHRISTOPH
Papilledema. Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D.
 Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Neuroradiology MR Protocols
 Neuroradiology MR Protocols Brain protocols N 1: Brain MRI without contrast N 2: Pre- and post-contrast brain MRI N 3 is deleted N 4: Brain MRI without or pre-/post-contrast (seizure protocol) N 5: Pre-
Neuroradiology MR Protocols Brain protocols N 1: Brain MRI without contrast N 2: Pre- and post-contrast brain MRI N 3 is deleted N 4: Brain MRI without or pre-/post-contrast (seizure protocol) N 5: Pre-
Sensitivity and Specificity in Detection of Labral Tears with 3.0-T MRI of the Shoulder
 Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Pituitary Apoplexy. Updated: April 22, 2018 CLINICAL RECOGNITION
 Pituitary Apoplexy Zeina C Hannoush, MD. Assistant Professor of Clinical Medicine. Division of Endocrinology, Diabetes and Metabolism. University of Miami, Miller School of Medicine. Roy E Weiss, MD, PhD,
Pituitary Apoplexy Zeina C Hannoush, MD. Assistant Professor of Clinical Medicine. Division of Endocrinology, Diabetes and Metabolism. University of Miami, Miller School of Medicine. Roy E Weiss, MD, PhD,
Evaluation of ONH Pallor in Glaucoma Patients and Suspects. Leticia Rousso, O.D. Joseph Sowka, O.D
 Evaluation of ONH Pallor in Glaucoma Patients and Suspects Leticia Rousso, O.D Joseph Sowka, O.D I. Abstract This case report will evaluate a young glaucoma suspect with unilateral sectoral optic nerve
Evaluation of ONH Pallor in Glaucoma Patients and Suspects Leticia Rousso, O.D Joseph Sowka, O.D I. Abstract This case report will evaluate a young glaucoma suspect with unilateral sectoral optic nerve
IDIOPATHIC INTRACRANIAL HYPERTENSION
 IDIOPATHIC INTRACRANIAL HYPERTENSION ASSESSMENT OF VISUAL FUNCTION AND PROGNOSIS FOR VISUAL OUTCOME Doctor of Philosophy thesis Anglia Ruskin University, Cambridge Fiona J. Rowe Department of Orthoptics,
IDIOPATHIC INTRACRANIAL HYPERTENSION ASSESSMENT OF VISUAL FUNCTION AND PROGNOSIS FOR VISUAL OUTCOME Doctor of Philosophy thesis Anglia Ruskin University, Cambridge Fiona J. Rowe Department of Orthoptics,
Pituitary Tumors and Incidentalomas. Bijan Ahrari, MD, FACE, ECNU Palm Medical Group
 Pituitary Tumors and Incidentalomas Bijan Ahrari, MD, FACE, ECNU Palm Medical Group Background Pituitary incidentaloma: a previously unsuspected pituitary lesion that is discovered on an imaging study
Pituitary Tumors and Incidentalomas Bijan Ahrari, MD, FACE, ECNU Palm Medical Group Background Pituitary incidentaloma: a previously unsuspected pituitary lesion that is discovered on an imaging study
Optic Nerve Disorders: Structure and Function and Causes
 Optic Nerve Disorders: Structure and Function and Causes Using Visual Fields, OCT and B-scan Ultrasound to Diagnose and Follow Optic Nerve Visual Losses Ohio Ophthalmological Society and Ophthalmic Tech
Optic Nerve Disorders: Structure and Function and Causes Using Visual Fields, OCT and B-scan Ultrasound to Diagnose and Follow Optic Nerve Visual Losses Ohio Ophthalmological Society and Ophthalmic Tech
Pituitary Macroadenoma with Superior Orbital Fissure Syndrome
 1 CASE REPORT OPEN ACCESS Pituitary Macroadenoma with Superior Orbital Fissure Syndrome Tapan Nagpal, Ankit Singhania ABSTRACT Introduction: Pituitary adenomas are benign tumours which arise within the
1 CASE REPORT OPEN ACCESS Pituitary Macroadenoma with Superior Orbital Fissure Syndrome Tapan Nagpal, Ankit Singhania ABSTRACT Introduction: Pituitary adenomas are benign tumours which arise within the
T HE visual field changes that accompany
 J. Neurosurg. / Volume 31 / September, 1969 The Arterial Supply of the Human Optic Chiasm RICHARD BERGLAND, M.D.,* AND BRONSON S. RAY, M.D. Department of Surgery (Neurosurgery), New York Hospital-Cornell
J. Neurosurg. / Volume 31 / September, 1969 The Arterial Supply of the Human Optic Chiasm RICHARD BERGLAND, M.D.,* AND BRONSON S. RAY, M.D. Department of Surgery (Neurosurgery), New York Hospital-Cornell
CHAPTER 11 KINETIC PERIMETRY WHAT IS KINETIC PERIMETRY? LIMITATIONS OF STATIC PERIMETRY LOW SPATIAL RESOLUTION
 205 CHAPTER 11 KINETIC PERIMETRY WHAT IS KINETIC PERIMETRY? LIMITATIONS OF STATIC PERIMETRY LOW SPATIAL RESOLUTION Static perimetry is currently the most commonly used type of perimetry. With static perimetry,
205 CHAPTER 11 KINETIC PERIMETRY WHAT IS KINETIC PERIMETRY? LIMITATIONS OF STATIC PERIMETRY LOW SPATIAL RESOLUTION Static perimetry is currently the most commonly used type of perimetry. With static perimetry,
Neuro-Ocular Grand Rounds
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234)
 Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland.
Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland.
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Visual Field Testing Suzanne Hansen, M.Ed., COMT, OSC Why are these tests ordered? Visual field testing is ordered to help the physician diagnose and
Learn Connect Succeed JCAHPO Regional Meetings 2017 Visual Field Testing Suzanne Hansen, M.Ed., COMT, OSC Why are these tests ordered? Visual field testing is ordered to help the physician diagnose and
Mechanism of hyperprolactinemia
 Hyperprolactinemia Mechanism of hyperprolactinemia Causes of hyperprolactinemia Hormone-producing pituitary tumors Prolactinoma Acromegaly Hypothalamic/pituitary stalk lesion Tumors, cysts (craniopharyngeoma,
Hyperprolactinemia Mechanism of hyperprolactinemia Causes of hyperprolactinemia Hormone-producing pituitary tumors Prolactinoma Acromegaly Hypothalamic/pituitary stalk lesion Tumors, cysts (craniopharyngeoma,
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
CHAPTER 5 SELECTING A TEST PATTERN INTRODUCTION
 59 CHAPTER 5 SELECTING A TEST PATTERN INTRODUCTION Depending on the pathology or type of ability testing that is to be performed, certain test locations are far more relevant than others. As there is always
59 CHAPTER 5 SELECTING A TEST PATTERN INTRODUCTION Depending on the pathology or type of ability testing that is to be performed, certain test locations are far more relevant than others. As there is always
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings. Jonathan A. Micieli, MD Valérie Biousse, MD
 Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
Traumatic Optic Neuropathy and Monocular Blindness following Transnasal Penetrating Optic Canal Injury by a Wooden Foreign Body
 Published online: July 6, 2018 2018 The Author(s) Published by S. Karger AG, Basel This article is licensed under the Creative Commons Attribution-NonCommercial 4.0 International License (CC BY-NC) (http://www.karger.com/services/openaccesslicense).
Published online: July 6, 2018 2018 The Author(s) Published by S. Karger AG, Basel This article is licensed under the Creative Commons Attribution-NonCommercial 4.0 International License (CC BY-NC) (http://www.karger.com/services/openaccesslicense).
21st Century Visual Field Testing
 Supplement to Supported by an educational grant from Carl Zeiss Meditec, Inc. Winter 2011 21st Century Visual Field Testing the Evolution Continues 21st Century Visual Field Testing 21st Century Visual
Supplement to Supported by an educational grant from Carl Zeiss Meditec, Inc. Winter 2011 21st Century Visual Field Testing the Evolution Continues 21st Century Visual Field Testing 21st Century Visual
Science & Technologies
 STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
Large suprasellar aneurysms imitating pituitary
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 83-87 Large suprasellar aneurysms imitating pituitary tumour L. A. RAYMOND AND J. TEW From the Department of Ophthalmology and Division of Neurosurgery,
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 83-87 Large suprasellar aneurysms imitating pituitary tumour L. A. RAYMOND AND J. TEW From the Department of Ophthalmology and Division of Neurosurgery,
LISC-322 Neuroscience. Visual Field Representation. Visual Field Representation. Visual Field Representation. Visual Field Representation
 LISC-3 Neuroscience THE VISUAL SYSTEM Central Visual Pathways Each eye sees a part of the visual space that defines its visual field. The s of both eyes overlap extensively to create a binocular. eye both
LISC-3 Neuroscience THE VISUAL SYSTEM Central Visual Pathways Each eye sees a part of the visual space that defines its visual field. The s of both eyes overlap extensively to create a binocular. eye both
Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234)
 Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland. In patients
Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland. In patients
NANOS Patient Brochure
 NANOS Patient Brochure Pituitary Tumor Copyright 2015. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for informational
NANOS Patient Brochure Pituitary Tumor Copyright 2015. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for informational
Clinical Correlation of a New Practical MRI Method for Assessing Cervical Spinal Canal Compression
 Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
Suprasellar Meningioma Simulating Atypical Retrobulbar Optic Neuritis: A Diagnostic Dilemma For Neuro- Ophthalmologists
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 10 Number 1 Suprasellar Meningioma Simulating Atypical Retrobulbar Optic Neuritis: A Diagnostic Dilemma For Neuro- Ophthalmologists
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 10 Number 1 Suprasellar Meningioma Simulating Atypical Retrobulbar Optic Neuritis: A Diagnostic Dilemma For Neuro- Ophthalmologists
Saharsh Patel, 1 Kyle M Fargen, 2 Keith Peters, 3 Peter Krall, 1 Hazem Samy, 1 Brian L Hoh 2 CASE REPORT. Hemorrhagic stroke
 1 Department of Ophthalmology, 2 Department of Neurosurgery, 3 Department of Radiology, Correspondence to Dr Kyle Michael Fargen, Department of Neurosurgery, Box 100265, Gainesville, Florida 32610, USA;
1 Department of Ophthalmology, 2 Department of Neurosurgery, 3 Department of Radiology, Correspondence to Dr Kyle Michael Fargen, Department of Neurosurgery, Box 100265, Gainesville, Florida 32610, USA;
Bilateral central and centrocaecal scotomata due
 British Journal of Ophthalmology, 1984, 68, 336-342 Bilateral central and centrocaecal scotomata due to mass lesions ISAAC GUTMAN,* MYLES BEHRENS, AND JEFFREY ODEL* From the Department of Ophthalmology,
British Journal of Ophthalmology, 1984, 68, 336-342 Bilateral central and centrocaecal scotomata due to mass lesions ISAAC GUTMAN,* MYLES BEHRENS, AND JEFFREY ODEL* From the Department of Ophthalmology,
Do You See What I See!!! Shane R. Kannarr, OD
 Do You See What I See!!! Shane R. Kannarr, OD skannarr@kannarreyecare.com Define Specialty Testing Additional Test to: Prove/Disprove Diagnosis To monitor progression of a condition To document a condition
Do You See What I See!!! Shane R. Kannarr, OD skannarr@kannarreyecare.com Define Specialty Testing Additional Test to: Prove/Disprove Diagnosis To monitor progression of a condition To document a condition
The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery
 The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery The Case: Upon awakening from anesthesia, he is blind in both eyes After Non-Ocular Surgeries Nancy J. Newman,
The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery The Case: Upon awakening from anesthesia, he is blind in both eyes After Non-Ocular Surgeries Nancy J. Newman,
non-occipital lobe lesions
 Brit. 7. Ophthal. (I97I) 55, 4I6 The Riddoch phenomenon revealed in non-occipital lobe lesions R. J. ZAPPIA, J. MI. ENOCH, R. STAMPER, J. Z. WINKELMAN, AND A. J. GAY From the Departments of Ophthalmology
Brit. 7. Ophthal. (I97I) 55, 4I6 The Riddoch phenomenon revealed in non-occipital lobe lesions R. J. ZAPPIA, J. MI. ENOCH, R. STAMPER, J. Z. WINKELMAN, AND A. J. GAY From the Departments of Ophthalmology
CHAPTER 13 CLINICAL CASES INTRODUCTION
 2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
N EOPLASMS of the optic nerves occur
 Tumors of the optic nerve and optic chiasm COLLINS. MAcCARTY~ M.D., ALLEN S. BOYD, JR., M.D., AND DONALD S. CHILDS, JR,, M.D. Departments of Neurologic Surgery and Therapeutic Radiology, Mayo Clinic and
Tumors of the optic nerve and optic chiasm COLLINS. MAcCARTY~ M.D., ALLEN S. BOYD, JR., M.D., AND DONALD S. CHILDS, JR,, M.D. Departments of Neurologic Surgery and Therapeutic Radiology, Mayo Clinic and
Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic Syndrome
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
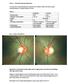 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case Report Ocular Symptomatology, Management, and Clinical Outcome of a Giant Intracranial Aneurysm
 Volume 2012, Article ID 643965, 4 pages doi:10.1155/2012/643965 Case Report Ocular Symptomatology, Management, and Clinical Outcome of a Giant Intracranial Aneurysm Chryssa Terzidou, 1 Georgios Dalianis,
Volume 2012, Article ID 643965, 4 pages doi:10.1155/2012/643965 Case Report Ocular Symptomatology, Management, and Clinical Outcome of a Giant Intracranial Aneurysm Chryssa Terzidou, 1 Georgios Dalianis,
Perimetry Phobia: Don t fear the field Savory Turman, COMT, CPSS
 Perimetry Phobia: Don t fear the field Savory Turman, COMT, CPSS I have no financial interest in this presentation. Who am I? Where am I? What am I? The anatomy of the visual field Purpose of Visual Field
Perimetry Phobia: Don t fear the field Savory Turman, COMT, CPSS I have no financial interest in this presentation. Who am I? Where am I? What am I? The anatomy of the visual field Purpose of Visual Field
A neurysms arising from the cavernous portion of the
 863 PAPER Long term visual and neurological prognosis in patients with treated and untreated cavernous sinus aneurysms N Goldenberg-Cohen, C Curry, N R Miller, R J Tamargo, K P J Murphy... See end of article
863 PAPER Long term visual and neurological prognosis in patients with treated and untreated cavernous sinus aneurysms N Goldenberg-Cohen, C Curry, N R Miller, R J Tamargo, K P J Murphy... See end of article
Using CT to Localize Side and Level of Vocal Cord Paralysis
 Shy-Chyi Chin 1 Simon Edelstein 2 Cheng-Yu Chen 1 Peter M. Som 2 Received May 16, 2002; accepted after revision ugust 29, 2002. 1 Department of Radiology, Tri-Service General Hospital, National Defense
Shy-Chyi Chin 1 Simon Edelstein 2 Cheng-Yu Chen 1 Peter M. Som 2 Received May 16, 2002; accepted after revision ugust 29, 2002. 1 Department of Radiology, Tri-Service General Hospital, National Defense
Blue-domed cyst with optic nerve compression
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 987-991 Blue-domed cyst with optic nerve compression MITCHELL D. BURNBAUM, JOHN W. HARBISON, JOHN B. SELHORST, AND HAROLD F. YOUNG From the
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 987-991 Blue-domed cyst with optic nerve compression MITCHELL D. BURNBAUM, JOHN W. HARBISON, JOHN B. SELHORST, AND HAROLD F. YOUNG From the
Time-Dependent Changes in Dural Enhancement Associated With Spontaneous Intracranial Hypotension
 Neuroradiology/Head and Neck Imaging Original Research Neuroradiology/Head and Neck Imaging Original Research Peter G. Kranz 1 Timothy J. mrhein Kingshuk Roy Choudhury Teerath Peter Tanpitukpongse Linda
Neuroradiology/Head and Neck Imaging Original Research Neuroradiology/Head and Neck Imaging Original Research Peter G. Kranz 1 Timothy J. mrhein Kingshuk Roy Choudhury Teerath Peter Tanpitukpongse Linda
Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD
 Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD A 68 year old white woman had a new onset of floaters in her right eye and was found to have
Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD A 68 year old white woman had a new onset of floaters in her right eye and was found to have
Ganglion cell analysis by optical coherence tomography (OCT) Jonathan A. Micieli, MD Valérie Biousse, MD
 Ganglion cell analysis by optical coherence tomography (OCT) Jonathan A. Micieli, MD Valérie Biousse, MD Figure 1. Normal OCT of the macula (cross section through the line indicated on the fundus photo)
Ganglion cell analysis by optical coherence tomography (OCT) Jonathan A. Micieli, MD Valérie Biousse, MD Figure 1. Normal OCT of the macula (cross section through the line indicated on the fundus photo)
The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery
 The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery Edsel Kim, M.D. Otolaryngology-Head and Neck Surgery The Oregon Clinic Providence Brain and Spine Institute Pituitary, Thyroid
The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery Edsel Kim, M.D. Otolaryngology-Head and Neck Surgery The Oregon Clinic Providence Brain and Spine Institute Pituitary, Thyroid
Picture of patient with apparent lid retraction and poor elevation. Shows you Orbital CT-Scan with muscle involvement including IR and asks is this
 NEUROLOGY Q: MENINGIOMAS AND SKULL (*2) Real skull is given, and you are asked to point to tuberculum sella What kind of meningioma occurs at this location? Where is the anterior clinoid process? Where
NEUROLOGY Q: MENINGIOMAS AND SKULL (*2) Real skull is given, and you are asked to point to tuberculum sella What kind of meningioma occurs at this location? Where is the anterior clinoid process? Where
Giant aneurysms of the carotid system presenting as visual field defect
 Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 1053-1064 Giant aneurysms of the carotid system presenting as visual field defect J B PEIRIS AND R W ROSS RUSSELL From the Institute of Neurology,
Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 1053-1064 Giant aneurysms of the carotid system presenting as visual field defect J B PEIRIS AND R W ROSS RUSSELL From the Institute of Neurology,
Where Has My Vision Gone? Evaluation of Sellar Lesions. Caleb Stowell,, HMS III Gillian Lieberman, MD November 2008
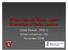 Where Has My Vision Gone? Evaluation of Sellar Lesions Caleb Stowell,, HMS III Gillian Lieberman, MD November 2008 Objectives Present a case highlighting the clinical presentation and evaluation of a sellar
Where Has My Vision Gone? Evaluation of Sellar Lesions Caleb Stowell,, HMS III Gillian Lieberman, MD November 2008 Objectives Present a case highlighting the clinical presentation and evaluation of a sellar
doi: /j.jns
 doi: 10.1016/j.jns.2014.05.055 Title: Sixth nerve palsy associated with obstruction in Dorello s canal, accompanied by nodular type muscular sarcoidosis Author: Ayako Shioya 1), Hiroshi Takuma 1), Masanari
doi: 10.1016/j.jns.2014.05.055 Title: Sixth nerve palsy associated with obstruction in Dorello s canal, accompanied by nodular type muscular sarcoidosis Author: Ayako Shioya 1), Hiroshi Takuma 1), Masanari
Neuro-imaging for the Ophthalmologist. Karl C. Golnik, MD, MEd University of Cincinnati & The Cincinnati Eye Institute
 Neuro-imaging for the Ophthalmologist Karl C. Golnik, MD, MEd University of Cincinnati & The Cincinnati Eye Institute Neuro-ophthalmology is that subspecialty where the diagnosis is made upon reinterpretation
Neuro-imaging for the Ophthalmologist Karl C. Golnik, MD, MEd University of Cincinnati & The Cincinnati Eye Institute Neuro-ophthalmology is that subspecialty where the diagnosis is made upon reinterpretation
PITUITARY AND PARAPITUITARY TUMOURS* VALUE OF PERIMETRY IN DIAGNOSIS
 Brit. J. Ophthal. (1964) 48, 590. PITUITARY AND PARAPITUITARY TUMOURS* VALUE OF PERIMETRY IN DIAGNOSIS BY J. F. CULLEN Department of Ophthalmology, University of Edinburgh THE occurrence of pallor of the
Brit. J. Ophthal. (1964) 48, 590. PITUITARY AND PARAPITUITARY TUMOURS* VALUE OF PERIMETRY IN DIAGNOSIS BY J. F. CULLEN Department of Ophthalmology, University of Edinburgh THE occurrence of pallor of the
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Clinical Characteristics of Optic Neuritis in Koreans Greater than 50 Years of Age
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(2):111-115 http://dx.doi.org/10.3341/kjo.2012.26.2.111 Original Article Clinical Characteristics of Optic Neuritis in Koreans Greater than
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(2):111-115 http://dx.doi.org/10.3341/kjo.2012.26.2.111 Original Article Clinical Characteristics of Optic Neuritis in Koreans Greater than
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Meniscal Tears: Role of Axial MRI Alone and in Combination with Other Imaging Planes
 Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
 Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD
 New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
Neuroophthalmology and otoneurology. 1. Which of the following is shown on this fundoscopy?
 EANS/UEMS European examination in neurosurgery Part I (written) Variants of questions with answers (compilation - Vyacheslav S. Botev, Department of Neurosurgery, M.Gorky Donetsk National Medical University)
EANS/UEMS European examination in neurosurgery Part I (written) Variants of questions with answers (compilation - Vyacheslav S. Botev, Department of Neurosurgery, M.Gorky Donetsk National Medical University)
Neurology Case Presentation. Rawan Albadareen, MD 12/20/13
 Neurology Case Presentation Rawan Albadareen, MD 12/20/13 Case presentation A 49 y.o. female presented to the ED after an episode of zigzagging w a jagged bright light crossing through her Rt visual field
Neurology Case Presentation Rawan Albadareen, MD 12/20/13 Case presentation A 49 y.o. female presented to the ED after an episode of zigzagging w a jagged bright light crossing through her Rt visual field
Literature Review: Neurosurgery
 NANOS 2018 Kona, Hawaii Literature Review: Neurosurgery Neil R. Miller, MD FACS Frank B. Walsh Professor of Neuro-Ophthalmology Professor of Ophthalmology, Neurology & Neurosurgery Johns Hopkins University
NANOS 2018 Kona, Hawaii Literature Review: Neurosurgery Neil R. Miller, MD FACS Frank B. Walsh Professor of Neuro-Ophthalmology Professor of Ophthalmology, Neurology & Neurosurgery Johns Hopkins University
SWI including phase and magnitude images
 On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma. Module 3a GDx
 STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
Jacqueline Theis, O.D., F.A.A.O.
 Neuro-Ophthalmological Emergencies Presenting in Primary Care Optometry Describes the symptoms, signs, and management of neuro-ophthalmological emergencies. Signs/Symptoms to be Concerned about (especially
Neuro-Ophthalmological Emergencies Presenting in Primary Care Optometry Describes the symptoms, signs, and management of neuro-ophthalmological emergencies. Signs/Symptoms to be Concerned about (especially
Use of the Arden grating test for screening
 British Journal of Ophthalmology, 19, 64, 591-596 Use of the rden grating test for screening ROBERT G. WETHERHED From Moorfields Eye Hospital, City Road, London EC] V PD SUMMRY One hundred and forty patients
British Journal of Ophthalmology, 19, 64, 591-596 Use of the rden grating test for screening ROBERT G. WETHERHED From Moorfields Eye Hospital, City Road, London EC] V PD SUMMRY One hundred and forty patients
Changes of Visual Functions in Patients With Pituitary Adenoma
 132 :132-7 Changes of Visual Functions in Patients With Pituitary Adenoma Roberta Kasputytė 1, Girėna Slatkevičienė 2, Rasa Liutkevičienė 2, 3, Brigita Glebauskienė 2, Giedrimantas Bernotas 4, Arimantas
132 :132-7 Changes of Visual Functions in Patients With Pituitary Adenoma Roberta Kasputytė 1, Girėna Slatkevičienė 2, Rasa Liutkevičienė 2, 3, Brigita Glebauskienė 2, Giedrimantas Bernotas 4, Arimantas
3/16/2018. Optic Nerve Examination. Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital
 Optic Nerve Examination Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Examination Structure ( optic disc) Function Examination of the optic disc The only cranial nerve (brain tract) which
Optic Nerve Examination Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Examination Structure ( optic disc) Function Examination of the optic disc The only cranial nerve (brain tract) which
Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
 Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
Usefulness of Unenhanced MRI and MR Arthrography of the Shoulder in Detection of Unstable Labral Tears
 Musculoskeletal Imaging Original Research Unenhanced MRI and MR rthrography for Unstable Labral Tears Musculoskeletal Imaging Original Research Thomas 1,2 T Keywords: labral tear, MRI, shoulder DOI:10.2214/JR.14.14262
Musculoskeletal Imaging Original Research Unenhanced MRI and MR rthrography for Unstable Labral Tears Musculoskeletal Imaging Original Research Thomas 1,2 T Keywords: labral tear, MRI, shoulder DOI:10.2214/JR.14.14262
Pearls, Pitfalls and Advances in Neuro-Ophthalmology
 Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Retinal nerve fiber layer thickness in Indian eyes with optical coherence tomography
 Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Glaucoma: Diagnostic Modalities
 Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Unexplained visual loss in seven easy steps
 Unexplained visual loss in seven easy steps Andrew G. Lee, MD Chair Ophthalmology, Houston Methodist Hospital, Professor, Weill Cornell MC; Adjunct Professor, Baylor COM, U Iowa, UTMB Galveston, UT MD
Unexplained visual loss in seven easy steps Andrew G. Lee, MD Chair Ophthalmology, Houston Methodist Hospital, Professor, Weill Cornell MC; Adjunct Professor, Baylor COM, U Iowa, UTMB Galveston, UT MD
TABLES. Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging. Conclusions. Author (Year) Classification Process/Evid ence Class
 TABLES Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging Author Clark (1986) 9 Reformatted sagittal images in the differential diagnosis meningiomas and adenomas with suprasellar
TABLES Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging Author Clark (1986) 9 Reformatted sagittal images in the differential diagnosis meningiomas and adenomas with suprasellar
THE VISUAL PATHWAY FOR DENTAL STUDENTS
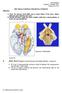 Neuroanatomy Suzanne S. Stensaas, Ph.D. February 16, 2012 Objectives: THE VISUAL PATHWAY FOR DENTAL STUDENTS A. Draw the expected visual fields seen in classic lesions of the nerve, chiasm, thalamus, optic
Neuroanatomy Suzanne S. Stensaas, Ph.D. February 16, 2012 Objectives: THE VISUAL PATHWAY FOR DENTAL STUDENTS A. Draw the expected visual fields seen in classic lesions of the nerve, chiasm, thalamus, optic
