Diffusion, Perfusion, and Histopathologic Characteristics of Desmoplastic Infantile Ganglioglioma
|
|
|
- Branden Tobias McCoy
- 6 years ago
- Views:
Transcription
1 Diffusion, Perfusion, and Histopathologic Characteristics of Desmoplastic Infantile Ganglioglioma Chang Y Ho 1*, Melissa Gener 2, Jose Bonnin 2, Stephen F Kralik 1 1. Department of Radiology, Indiana University School of Medicine, Indianapolis, USA 2. Department of Pathology, Indiana University School of Medicine, Indianapolis, USA * Correspondence: Chang Yueh Ho, 705 Riley Hospital Drive, MRI Department, Indiana University School of Medicine, Indianapolis, IN 46240, USA ( cyho@iupui.edu) :: DOI: /jrcr.v10i ABSTRACT We present a case series of a rare tumor, the desmoplastic infantile ganglioglioma (DIG) with MRI diffusion and perfusion imaging quantification as well as histopathologic characterization. Four cases with pathologically-proven DIG had diffusion weighted imaging (DWI) and two of the four had dynamic susceptibility contrast imaging. All four tumors demonstrate DWI findings compatible with low-grade pediatric tumors. For the two cases with perfusion imaging, a higher relative cerebral blood volume was associated with higher proliferation index on histopathology for one of the cases. Our results are discussed in conjunction with a literature review. CASE SERIES We report on four cases of desmoplastic infantile ganglioglioma at our institution with diffusion weighted imaging (DWI) for all four cases, dynamic susceptibility contrast (DSC) perfusion imaging for two of the cases, and described the histopathological findings in all four cases. MRI Technique: Clinical MRI imaging was performed on all patients with a 1.5T scanner (Siemens Avanto, Erlangen, Germany; and GE Signa LX, Waukesha, WI, USA). Anatomic imaging included axial T2-weighted fast spin echo, sagittal and axial T1- weighted, axial T2-weighted fluid attenuated inversion recovery (T2 FLAIR), and post contrast axial, coronal and sagittal T1-weighted sequences. Diffusion weighted images were performed with multi-slice single shot spin-echo echoplanar imaging (EPI) with 5 mm slice thickness prior to administration of contrast material with b values of 0, and 1000 s/mm2 applied in the x, y, and z directions. Processing of CASE SERIES apparent diffusion coefficient (ADC) maps was performed automatically on the MR units. DSC perfusion imaging was performed with a peripherally inserted 24 gauge angiocatheter with power injection of 4 cc/s of 0.1 mmol/kg of gadobenate dimeglumine (MultiHance, Bracco Diagnostics Inc., Princeton, NJ) diluted in normal saline for a total volume of 32 ml. DSC perfusion MR images were obtained during the first pass bolus of contrast on 1.5 MRI scanners (Siemens Avanto and Verio, Erlangen, Germany) using a gradient echo EPI sequence (TR / TE ms, flip angle 90 degrees). Diffusion Analysis: ADC maps were independently analyzed by two boardcertified neuroradiologists (C.H. and S.K.) with certificate of added qualification (CAQ) in neuroradiology. At least three regions of interest (ROI) with size ranging from 2-5 mm2 were placed in the mass at the PACS workstation using a manual/freeform ROI tool and the value was automatically calculated and expressed in 10-3 mm2/s. Sites of ROI placement were chosen by visual inspection and targeted the 1
2 darkest signal intensity regions on the ADC map. The entire brain MRI sequences were available during ADC value placement to avoid placing an ROI on an area of presumed blood products based on intrinsic T1-weighted shortening, T2- weighted shortening, or susceptibility on the b0 images. The minimum absolute ADC values of the three ROIs for each neuroradiologist were then averaged and used as the final average absolute minimum value for the tumor. This technique has been previously utilized in the literature [1]. Perfusion Analysis: Quantitative analysis of tumor relative cerebral blood volume (rcbv) was performed by two neuroradiologists (C. H. and S. K.) using a commercially available workstation (Dynasuite Neuro 3.0 workstation, InVivo Corp, Pewaukee WI). Each neuroradiologist independently obtained a rcbv maximum (rcbvmax) for each tumor by drawing at least three 2-5 mm2 ROIs within the perceived highest CBV within tumor tissue, and using the highest value divided by a similar ROI placed in normal-appearing contralateral white matter. This technique has been previously described in the perfusion evaluation of adult tumors [2]. Conventional MR images were available to assist in ROI placement within the tumor and avoid placement within vascular structures and avoid T2* artifacts. Workstation-generated corrected CBV maps were used, with CBV correction by gamma variate fitting and an algorithm developed by Boxerman et al [3]. From April 2003 to March 2012, there were four pathologically proven cases of DIG at our institution. All four cases had diffusion imaging, and two of the four cases included DSC perfusion imaging. Case 1 Clinical and Radiologic Data: A 13 month-old female infant presented with clinical history of increasing head circumference, macrocephaly, and otherwise normal development. An MRI was performed showing a large multicystic tumor within the left frontal lobe with an intensely enhancing solid nodule located in the periphery with broad dural attachment. The entire tumor measured 5.7 x 7.2 x 6.5 cm (fig. 1). The highest rcbv within the tumor coincided with the solid enhancing portion, which was qualitatively less than normal surrounding cortex. The averaged rcbvmax was 1.28 while the averaged minimum ADC measurement was 0.76 x 10-3 mm2/s (fig. 2). Gross total resection was performed shortly after the MRI scan. The craniotomy site was complicated by a pseudomeningocele that was repaired by a dural patch 2 months after tumor resection. To date, there has been no recurrence by imaging at 6 months. Pathology: The solid component of this tumor was composed of desmoplastic spindle cells within a dense eosinophilic collagenous background (fig. 3A). This tumor was tightly adherent to the dura and surrounds the penetrating vessels of the meninges (fig. 3B). Other areas of the tumor showed cells within a looser backround matrix with intervening blood vessels (fig. 4A). There was no necrosis or endothelial vascular proliferation. It had a low Ki67 proliferative index (1-2%) and mitoses were not appreciated. The neuroepithelial cells were strongly immunoreactive for glial fibrillary acidic protein (GFAP), while CD34 and smooth muscle actin (SMA) highlighted the vascular walls of the intratumoral vessels (fig. 4B). While there were no directly visible connections of the meningeal vessels to the numerous small thin-walled vessels, it was highly suggestive that the vessels of the meninges may be providing collaterals to the solid components of the tumor. Case 2 Clinical and Radiologic Data: A 6 month-old male infant presented with increasing head circumference, macrocephaly, and otherwise normal development. An MRI was performed showing a large 7.9x 8.1 x 8.7 cm multi-cystic tumor in the left frontal lobe with an intensely enhancing solid nodule located in the periphery with broad dural attachment, T2 prolongation of surrounding white matter, and midline shift (fig. 5). The highest rcbv within the tumor coincided with the solid enhancing portion, which was qualitatively less than normal surrounding cortex. The averaged rcbvmax was 3.05 while the averaged minimum ADC measurement was 0.88 x 10-3 mm2/s (fig. 6). Gross total resection was performed shortly after MRI scanning. To date, there has been no recurrence by imaging at 3 years, and the patient has no residual deficits. Pathology: Histologically this was a heterogeneous tumor with cysts and solid areas composed of desmoplastic spindle cells in a dense collagenous background, intermixed with large islands of astrocytic cells (fig. 7). The majority of this tumor had a low ki67 proliferative index (1%), but there are foci, particularly in the astrocytic regions with a proliferative index up to 7% (fig 8). Mitoses are rare, 1 per ten high power fields (400x). The tumor was highly vascular, with the vessel walls being highlighted by an SMA immunostain (fig 9). These vessels are of greater concentration in the solid components of the tumor. This may contribute to the intense contrast enhancement on MRI scans. This tumor was located very superficially in the cortex. While there was no definitive evidence of penetration of the tumor by meningeal vessels the close proximity to the meninges was suggestive that some of the meningeal vessels may be contributing collaterals to the solid tumor component. Case 3 Clinical and Radiologic Data: A seven-week old male infant presented with new onset seizures characterized by eye twitching. An MRI was performed showing a moderate 4.2 x 3.5 x 3.2 cm heterogeneous mass with a cyst in the right anterior temporal lobe with an intensely enhancing solid nodule located medially extending to the suprasellar cistern and with broad attachment to the right tentorial incisura (fig. 10). The averaged minimum ADC measurement was 0.97 x 10-3 mm2/s. Gross total resection was performed shortly after MRI imaging. At 5 years after diagnosis, the patient was hospitalized for status epilepticus; however, no tumor recurrence was seen on imaging. To date the patient has had no tumor recurrence by imaging at 6 years post resection but has had persistent developmental delay and left spastic hemiparesis. 2
3 Pathology: This tumor had both solid and cystic components. The solid components were superficial and made up of a spindle cell population interwoven with a dense collagenous stroma. Rare mitotic figures were identified (less than 1 per 10 high power fields). Many of the tumor cells were immunoreactive for GFAP. A Ki67 proliferative index was less than 1% in most of the tumor, but there were foci with a proliferative index of up to 4%. There were no other signs of anaplasia such as necrosis, apoptosis, nuclear pleomorphism or endothelial vascular proliferation. Case 4 Clinical and Radiologic Data: A 4 month-old male infant presented with new onset seizure and apneic episodes. An MRI was performed showing a large, 4.4 x 6.2 x 4.9 cm multicystic tumor centered in the right anterior temporal lobe with an intensely enhancing solid nodule extending medially to the suprasellar cistern with a broad dural attachment to the right tentorial incisura (fig. 11). The averaged minimum ADC measurement was 1.14 x 10-3 mm2/s. The patient had partial resection shortly after the MRI. At 3 months post craniotomy placement of a shunt catheter was performed within the tumor cyst due to enlargement of the cystic portion, causing greater mass effect. Finally, a near total resection of the tumor was performed at 4 months from initial craniotomy, with residual tumor adjacent and within the right cavernous sinus, encasing the right internal carotid artery. The patient was treated with two cycles of vincristine, carboplatin, and temozolomide, with shrinkage of tumor. At 6 years from diagnosis, there has been no recurrence by imaging, although the patient has behavioral issues, attention deficit hyperactivity disorder and Asperger s syndrome. Pathology: Both the initial resection and the reresection four months later had nearly identical histology. The tumor was composed of desmoplastic stroma with dense collagen and intermixed with astrocytic cells with mild to moderate nuclear pleomorphism. GFAP was strongly immunoreactive. There were no mitoses or necrosis. The Ki67 proliferative index was 1%. This tumor was highly vascular with numerous small blood vessels throughout the solid components of the tumor. A reticulin stain highlighted these vessels. There was no definitive meningeal vessel penetration into the examined tumor sections. DISCUSSION Intracranial tumors presenting in the first years of life represent a diagnostic challenge as they are commonly large and heterogeneous [1,4-9]. Despite the similar imaging appearance of these tumors, the recognition of benign versus malignant entities are crucial as complete surgical resection may be curative. Desmoplastic infantile gangliogliomas (DIG) are generally benign intra-axial tumors commonly presenting in infants. Although they can have a recognizable imaging appearance consisting of a large, cystic tumor with an intensely enhancing peripheral nodule with dural attachment, this appearance is not exclusive to a benign etiology as malignant tumors may also have enhancing solid components and cystic or necrotic changes [1,10]. Diffusion and perfusion characteristics have been used to radiologically differentiate various brain tumors, although the perfusion characteristics of DIGs have not been previously reported. Therefore we present both the diffusion and perfusion characteristics of these tumors and compare these results with other low grade tumors and demonstrate a pathologic correlate to the imaging appearance. Etiology & Demographics: DIGs are rare tumors primarily presenting in the first 18 months of life with a median age of 5-6 months at diagnosis [11]. A review by Hummel et al [12] of DIG cases within the literature show that there is a 1.7 male to female ratio. Clinical & Imaging findings: Increased head circumference is the primary presenting symptom. The second most common symptom is seizures, which were more likely to occur in patients presenting after two years of age. Only 11% of patients presented with vomiting. As previously noted, the classic appearance of a DIG is a large heterogeneous supratentorial tumor with a solid nodule that contacts the dura with a broad dural base. The solid nodule is usually hyperdense on CT with calcification and hemorrhage not typically seen. The solid component is typically T1 and T2 isointense to brain parenchyma with intense contrast enhancement. Central cysts and adjacent parenchymal vasogenic edema is typical. Treatment & Prognosis: The mainline treatment of DIGs is complete surgical resection, with adjuvant chemotherapy in case where surgical resection is not possible. Out of a total of 107 cases in the literature, only 76 had reported initial surgical outcomes. Out of these 76 cases, 47 had gross total resection, 26 had subtotal resection, and 3 had only an initial biopsy. The majority of patients (60.7%) had a clinically benign course after initial surgical resection, while the remainder required further treatment (re-resection, chemotherapy, and/ or radiotherapy). Overall, 15% of patients either developed leptomeningeal disease or died from the disease, suggesting that the remainder, 85%, had a benign clinical outcome with resection and/or adjuvant therapy. [12] (table 1). Differential Diagnosis: Other common primary infantile CNS neoplasms with similar radiologic appearance include primitive neuroectodermal tumor, atypical teratoid rhabdoid tumor, choroid plexus carcinomas, and supratentorial ependymomas [13]. Primitve neuroectodermal tumor: These are large heterogeneous lobar tumors when occurring in the supratentorial brain. Solid components may be hyperdense on CT with calcification and hemorrhage potentially present. Cystic components are common with less than expected surrounding tumoral edema for size. Diffusion weighted imaging may show decreased diffusion of the solid component. The solid component typically has heterogeneous enhancement, and may have leptomeningeal seeding. 3
4 Atypical teratoid rhabdoid tumor: When presenting in the supratentorial brain this malignant tumor presents as a large heterogeneous lobar tumor, with calcification and possible hemorrhage. The solid component may be T1 and T2 iso to hyperintense depending on hemorrhage, with areas of central cystic necrosis. Diffusion images may show decreased diffusion. There is typically heterogeneous enhancement, with possible leptomeningeal seeding. Choroid plexus carcinoma: These tumors are predominantly intraventricular, although can grow to be very large with invasion of the periventricular brain to dominate an entire hemisphere. Calcification is common and the solid components are iso to hyperdense on CT. On MRI, the solid components are T1 and T2 iso to hypointense, depending on calcification with typically intense enhancement. While not as high as the majority of low grade tumors presented in their study, our measurements differed in that we looked for the minimum ADC value within the tumor. This ensures that the area potentially representing the highest cellularity is evaluated, especially within a heterogeneous tumor [18]. In a previous paper [1], within a cohort of intracranial tumors in the first year of life, we reported a threshold for which ADC values x 10-3 mm2/s were likely to be World Health Organization grade I and II tumors for which three of these cases of DIGs were included. All minimum averaged ADC values for the DIGs in this series were above this cutoff, compatible with low grade neoplasm. Qualitatively, as the solid components of the tumors are typically peripheral and adjacent to cortex, we did not observe abnormally decreased ADC relative to the adjacent gray matter. The solid enhancing component was typically isointense or hyperintense to adjacent gray matter on ADC maps (Figs 2,6,10,11). Supratentorial ependymoma: These typically arise in a periventricular location due to ependymal rests outside the ventricle. They are typically heterogeneous and large, commonly with calcification and cystic areas. Solid components are iso to hyperdense on CT and T1 iso to hypointense and T2 iso to hyperintense on MRI. There is typically heterogeneous enhancement. There may be decreased diffusion particularly in anaplastic varieties. Many of these malignant tumors tend to have large heterogeneous appearance with cystic/ necrotic changes and enhancing solid portions (figure 1). This may represent a diagnostic challenge in differentiating a benign tumor such as DIG from these entities based on anatomic imaging alone [1,10] (table 2). To our knowledge, these are the first cases of DIG with the combination of perfusion and ADC analysis in the literature. In a series of 9 patients with desmoplastic infantile tumors, Jurkiewicz et al reported the minimum ADC value of solid portion of the tumor ranged from to x 10-3 mm2/s with mean ADC value of x 10-3 mm2/s [14]. Similarly, in our series of DIGs, the minimum ADC value of the solid tumor ranged from 0.76 to 1.14 x 10-3 mm2/s with mean ADC value 0.94 x 10-3 mm2/s. As demonstrated by Rumboldt et al, in a population of posterior fossa tumor in children, ADC is inversely proportional to tumor grade [15]. This is hypothetically due to increasing tumor cellularity, and thus tumor grade, leading to decrease in ADC [16]. However, Rose et al. did not find significant overlap in glioblastomas between minimum ADC and 3,4-dihydroxy-6-[18F]-fluoro-Lphenylalanine PET, which is thought to be a marker for tumor proliferation, with their conclusions suggesting that minimum ADC may represent tumor ischemia or tissue compression rather than primarily tumor cellularity [17]. Nevertheless, according to Rumboldt et al, the mean of the averaged ADC of low grade tumors, juvenile pilocytic astrocytoma and ependymoma within their study was 1.53 x 10-3 mm2/s. For high grade tumors, medulloblastomas and atypical teratoid rhabdoid tumors within their study, the mean of the averaged ADC was 0.64 x 10-3 mm2/s. Our mean of the averages of the minimum ADC values for the DIG cases is 0.94 x 10-3 mm2/s. There is a paucity of perfusion imaging of pediatric tumors within the literature. Law et al. proposed a cut off of 1.75 rcbv between low and high grade adult astrocytic glial neoplasms [19]. However, the values from previous studies cannot be used as a threshold benchmark given the differences in patient population, and tumor type. Although rcbv has been shown to positively correlate with tumor grade in astrocytic adult gliomas, there is no direct histologic correlation in the literature. Theories postulate that rcbv could be a biomarker of tumor angiogenesis, although elevated rcbv can be seen in low grade tumors due to contrast leakage [20]. Our two cases with DSC perfusion demonstrated rcbv results of 1.28 and 3.05, for cases 1 and 2 respectively. Generally, this suggests a cerebral blood volume of the tumor 1.28 and 3.05 times greater than normal white matter for these two cases. The higher rcbv value is interesting in that it does not correlate as well for the predominantly low grade nature of DIGs. However, the pathology in our patient (case 2) with the higher rcbv demonstrated a higher proliferative index (7%) compared to our other case. As previously stated, Hummel et al. suggests that a minority of patients can have leptomeningeal disease or mortality from DIG, suggesting that not all DIGs have good outcome. Analysis of a larger numbers of patients would be necessary to determine if higher rcbv correlates with a higher Ki-67 index and is associated with worse prognosis. A similar correlation has been demonstrated by Bruna et al, in atypical and anaplastic meningiomas, where Ki-67 index 9.9% was significant for increased tumor recurrence and decreased overall survival [21]. Histologically, low and high mitotic activity due to clusters of poorly differentiated cells, neuronal and glial components, and variable vascularization without endothelial proliferation are described in DIGs despite the common radiologic finding in all reported cases of intense enhancement of the solid component [10,22,23,24]. A possible explanation for the increased vascularity and resulting intense enhancement may be that the tumors receive collateral supply from the meninges as was suggested by the pathology from three of the four cases in our series. This would be analogous to a meningioma, which are highly vascular yet predominantly benign tumors, which can also demonstrate elevated rcbv [25]. 4
5 Historically, complete surgical resection of DIGs have a high likelihood of cure [26,27]. A few cases in the literature demonstrate progression to high grade tumor showing a small risk of progression in cases with subtotal resection [28, 29]. Currently, molecular and genomic features of these tumors are inconclusive [30]. As such, it is important to appropriately diagnose DIGs of infantile CNS neoplasms and attempt complete resection when feasible. Diffusion and perfusion imaging characteristics may serve as an additional useful clue to the diagnosis, especially when the anatomic images are not highly specific. Furthermore, further investigation is necessary to determine whether diffusion and perfusion data correlate with prognosis in these patients. Limitations include the small sample size and the lack of direct anatomic correlation between histologic samples and radiographic location within the tumor. However, the possibility for sampling error is low as gross total resection was achieved on three of the four cases with the fourth receiving near total resection. 4. Chung S, Wang K, Nam D, Cho B(1998) Brain tumor in the first year of life: a single institute study. J Korean Med Sci. Feb;13(1):65-70 PMID: Mehrotra N, Shamji M, Vassilyadi M, Ventureyra E (2009) Intracranial tumors in first year of life: the CHEO experience. Childs Nerv Syst Dec;25(12): PMID: Rickert C, Probst-Cousin S, Gullotta F (1997) Primary intracranial neoplasms of infancy and early childhood. Childs Nerv Syst Oct;13(10): PMID: Buetow P, Smirniotopoulos J, Done S (1990) Congenital brain tumors: a review of 45 cases. AJNR Am J Neuroradiol Jul-Aug;11(4):793-9 PMID: Dirks P, Harris L, Hoffman H, Humphreys R, Drake J, Rutka J (1996) Supratentorial primitive neuroectodermal tumors in children. J Neurooncol Jul;29(1):75-84 PMID: In summary, we present perfusion on two cases and diffusion data on four cases of DIG tumors, the combination of which to our knowledge has not been previously reported. This information may serve as an important adjunct to the diagnosis when anatomic neuroimaging are not specific. Further evaluation is necessary to determine whether these diffusion and perfusion data is related to tumor histopathology and prognosis. TEACHING POINT Desmoplastic infantile gangliogliomas are a key primary brain tumor to recognize in infants due to its commonly benign course. Although these tumors are typically large and heterogeneous with cystic components, the characteristic finding of a peripherally located enhancing nodule with a broad dural base can be helpful in differentiating this tumor from the malignant primary brain tumors which also present in the first two years of life. 9. Meyers S, Khademian Z, Biegel J, Chuang S, Korones D, Zimmerman R (2006) Primary intracranial atypical teratoid/rhabdoid tumors of infancy and childhood: MRI features and patient outcomes. AJNR Am J Neuroradiol May;27(5): PMID: Manoranjan B, Provias J (2011) Congenital brain tumors: diagnostic pitfalls and therapeutic interventions. J Child Neurol May;26(5): PMID: Trehan G, Bruge H, Vinchon M, Khalil C, Ruchoux M, Dhellemmes P, Ares G (2004) MR imaging in the diagnosis of desmoplastic infantile tumor: retrospective study of six cases. AJNR Am J Neuroradiol Jun-Jul;25(6): PMID: Hummel T, Miles L, Mangano F, Jones B, Geller J (2012) Clinical heterogeneity of desmoplastic infantile ganglioglioma: a case series and literature review. J Pediatr Hematol Oncol Aug;34(6):e PMID: REFERENCES 1. Kralik S, Taha A, Kamer A, Cardinal J, Seltman T, Ho C (2014) Diffusion imaging for tumor grading of supratentorial brain tumors in the first year of life. AJNR Am J Neuroradiol Apr;35(4): PMID: Emblem K, Nedregaard B, Nome T, et al (2008) Glioma grading by using histogram analysis of blood volume heterogeneity from MR-derived cerebral blood volume maps. Radiology Jun; 247(3): PMID: Lang S, Beslow L, Gabel B, Judkins A, Fisher M, Sutton L, Storm P, Heuer G (2012) Surgical treatment of brain tumors in infants younger than six months of age and review of the literature. World Neurosurg Jul;78(1-2): PMID: Jurkiewicz E, Grajkowska W, Nowak K et al. MR imaging, apparent diffusion coefficient and histopathological features of desmoplastic infantile tumors-own experience and review of the literature. Childs Nerv Syst, 2015 Feb; Vol. 31 (2), pp PMID: Boxerman J, Schmainda K, Weisskoff R. Relative cerebral blood volume maps corrected for contrast agent extravasation significantly correlate with glioma tumor grade, whereas uncorrected maps do not. AJNR Am J Neuroradiol 2006;27: PMID: Rumboldt Z, Camacho D, Lake D, Welsh C, Castillo M. (2006) Apparent diffusion coefficients for differentiation of cerebellar tumors in children. AJNR Am J Neuroradiol Jun- Jul;27(6): PMID:
6 16. Gupta R, Cloughesy T, Sinha U, et al (2000) Relationships between choline magnetic resonance spectroscopy, apparent diffusion coefficient and quantitative histopathology in human glioma. J Neurooncol Dec;50(3): PMID: Sugiyama K, Arita K, Shima T et al (2002) Good clinical course in infants with desmoplastic cerebral neuroepithelial tumor treated by surgery alone. J Neurooncol Aug;59(1):63-9 PMID: Rose S, Fay M, Thomas P et al (2013) Correlation of MRIderived apparent diffusion coefficients in newly diagnosed gliomas with [18F]-fluoro-L-dopa PET: what are we really measuring with minimum ADC? AJNR Am J Neuroradiol Apr;34(4): PMID: Lee E, Lee S, Agid R, Bae J, Keller A, Terbrugge K (2008) Preoperative grading of presumptive low-grade astrocytomas on MR imaging: diagnostic value of minimum apparent diffusion coefficient. AJNR Am J Neuroradiol Nov;29(10): PMID: Law M, Yang S, Wang H, Babb JS, Johnson G, Cha S, Knopp EA, Zagzag D (2003) Glioma grading: sensitivity, specificity, and predictive values of perfusion MR imaging and proton MR spectroscopic imaging compared with conventional MR imaging. AJNR Am J Neuroradiol Nov-Dec;24(10): PMID: Cha S (2006) Update on brain tumor imaging: from anatomy to physiology. AJNR Am J Neuroradiol Mar;27(3): PMID: Bruna J, Brell M, Ferrer I, Gimenez-Bonafe P, Tortosa A (2007) Ki-67 proliferative index predicts clinical outcome in patients with atypical or anaplastic meningioma. Neuropathology Apr;27(2): PMID: Alexiou G, Stefanaki K, Sfakianos G, Prodromou N (2008) Desmoplastic infantile ganglioglioma: a report of 2 cases and a review of the literature. Pediatr Neurosurg 44(5): PMID: Nikas I, Anagnostara A, Theophanopoulou M et al (2004) Desmoplastic infantile ganglioglioma: MRI and histological findings case report. Neuroradiology Dec;46(12): PMID: Al-Kharazi K, Gillis C, Steinbok P, Dunham C. (2013) Malignant desmoplastic infantile astrocytoma? a case report and review of the literature. Clin Neuropathol Mar- Apr;32(2): PMID: Prakash V, Batanian JR, Guzman MA et al (2014) Malignant transformation of a desmoplastic infantile ganglioglioma in an infant carrier of a nonsynonymous TP53 mutation. Pediatr Neurol Jul;51(1): PMID: Gessi M, Zur Mühlen A, Hammes J et al (2013) Genomewide DNA copy number analysis of desmoplastic infantile astrocytomas and desmoplastic infantile gangliogliomas. J Neuropathol Exp Neurol Sep;72(9): PMID: Uematsu H, Maeda M, Sadato N, et al (2002) Measurement of the vascularity and vascular leakage of gliomas by doubleecho dynamic magnetic resonance imaging: a preliminary study. Invest Radiol Oct;37(10):571-6 PMID: Zhang H, Rödiger LA, Shen T, Miao J, Oudkerk M (2008) Perfusion MR imaging for differentiation of benign and malignant meningiomas. Neuroradiology Jun;50(6): PMID: Gelabert-Gonzalez M, Serramito-García R, Arcos-Algaba A (2010) Desmoplastic infantile and non-infantile ganglioglioma. Review of the literature. Neurosurg Rev Apr;34(2): PMID:
7 FIGURES Figure 1: 13 month-old female infant with increasing head circumference and pathology proven DIG. A) Findings: There is a large heterogeneous mass in the left frontal lobe with multiple cysts (asterisks) deep to the periphery and an isointense to brain solid nodule (arrowhead) abutting the dural surface. There is midline shift and adjacent T2 prolongation of the white matter. Technique: Axial T2 turbo spin echo (1.5T, TR=3200, TE=91) B) Findings: There is heterogeneous enhancement of the solid nodule with a broad dural base (arrow). Technique: Axial 3D inversion recovery spoiled gradient recalled echo T1 post contrast (1.5T, TR=1900, TE=3, contrast=multihance 0.1mmol/kg, delayed phase) C) Findings: There is a heterogeneously enhancing solid component with a broad dural base (arrow) in addition to the more central cystic components (asterisks). Technique: Coronal T1 turbo spin echo fat saturated post contrast image (1.5T, TR=514, TE=10, contrast=multihance 0.1mmol/kg, delayed phase) Figure 2: 13 month-old female infant with increasing head circumference and pathology proven DIG. A) Findings: There is no no significant increased signal of the solid nodule (arrow) with respect to the normal brain parenchyma. Technique: Axial DWI b=1000 image (1.5T, TR=7199, TE=97) B) Findings: There is relative isointensity of solid tumoral ADC signal compared to adjacent brain parenchyma. Technique: Axial ADC map image (1.5T, TR=7199, TE=97) C) Findings: There is relative hypoperfusion of the solid nodule in comparison with adjacent and contralateral gray matter. Technique: Axial rcbv map from DSC (1.5T, TR=1630, TE=49, contrast=multihance 0.1mmol/kg, first pass bolus) 7
8 Figure 3: 13-month old female with increasing head circumference and pathology proven DIG. A) Hematoxylin and Eosin (H&E) 100x stains of the solid component of tumor showing a desmoplastic spindle cell tumor with densely eosinophilic collagenous background. B) H&E, 40x. Cortical surface of tumor showing the superficial location of the tumor as well as tumor growth into the leptomeninges. Leptomeningeal vessels are prominent within the superficial portions of the tumor. Figure 4: 13-month old female with increasing head circumference and pathology proven DIG. A) H&E, 100x. A small portion of the tumor shows tumor cells in a looser background matrix with many small to medium-sized blood vessels. B) CD34, 40x. A CD34 immunohistochemical stain highlights the numerous small vessels within the solid component of the tumor. 8
9 Figure 5: 6 month-old male infant with increasing head circumference and pathology proven DIG A) Findings: There is a large heterogeneous tumor with peripheral heterogeneous solid component with a broad dural base and more central multicystic components. There is midline shift and mass effect on the lateral ventricles. Note the linear areas of hypointensity within the solid component which likely represent vascular flow voids (arrow). Technique: Axial T2 turbo spin echo (1.5T, TR=3700, TE=99) B) Findings: There is an intensely enhancing solid nodule with a broad dural base (arrow). Technique: Coronal T1 turbo spin echo fat saturation post contrast image (1.5T, TR=508, TE=17, contrast=multihance 0.1mmol/kg, delayed phase) Figure 6: 6 month-old male infant with increasing head circumference and pathology proven DIG. A) Findings: ROI measurement of the lowest areas of diffusion. Technique: ADC map (1.5T, DWI b=1000, TR=7199, TE=97) B) Findings: ROI measurements to obtain an rcbv ratio. Measurement of the area with the highest signal intensity corresponds with the highest CBV values divided by the normal contralateral white matter. Technique: Grayscale rcbv map from DSC PWI (1.5T, TR=1630, TE=49, contrast=multihance 0.1mmol/kg, first pass bolus) C) Findings: Color rcbv map from DSC PWI shows areas of relative hyperperfusion (arrows) compared to the rest of the solid enhancing component within the tumor. These areas were excluded from measurement if they correspond with vessels on anatomic images. Technique: Color rcbv map from DSC PWI (1.5T, TR=1630, TE=49, contrast=multihance 0.1mmol/kg, first pass bolus) 9
10 Figure 7: 6 month-old male infant with increasing head circumference and pathology proven DIG. Variable pathology is noted in this tumor including, A) H&E 200x showing the more classically described desmoplastic cells within a densely collagenous background matrix while B) H&E 200X, shows areas of the tumor were the cells are elongated with cytoplasmic processes, reminiscent of an astrocytic neoplasm. Figure 8: 6 month-old male infant with increasing head circumference and pathology proven DIG. A) Ki67 proliferative index immunohistochemical stain, 200x, showing the low proliferation of the majority of the tumor. B) Ki67 proliferative index immunohistochemical stain, 200x, demonstrates rare areas of increased proliferation with an index rate of up to 7%. 10
11 Figure 9 (left): 6 month-old male infant with increasing head circumference and pathology proven DIG. Smooth Muscle Actin, 100x, showing the numerous intratumoral blood vessels. Figure 10: Seven-week old male infant with new onset seizures characterized by eye twitching and pathology proven DIG. A) Findings: There is a solid and cystic mass involving the right temporal lobe, expanding the middle cranial fossa. Note the solid component is medial but demonstrates a broad base of attachment with the tentorial incisura (arrow). The solid component measures 3.4 cm in the craniocaudal dimension and demonstrates T2 iso to hyperintensity with mass effect on the overlying thalamus. Technique: Coronal short TI inversion recovery (1.5T, TR=5000, TE=96) B) Findings: There is intense homogeneous enhancement of the solid component, which protrudes into the suprasellar cistern (arrow). Technique: Axial T1 turbo spin echo post contrast (1.5T, TR=450, TE=14, contrast=prohance 0.1mmol/kg, delayed phase) C) Findings: There is relative isointensity of the solid tumoral component on ADC map (arrow) compared to the adjacent brain parenchyma. Technique: Axial ADC map image (1.5T, TR=7199, TE=97) 11
12 Figure 11: 4 month-old male infant with new onset seizure and apneic episodes with pathology proven DIG A) Findings: There is a large heterogeneous mass in the right temporal lobe, expanding the middle cranial fossa. There is a heterogeneous solid component (arrow) which is medial to the multiple cysts and surrounding T2 white matter prolongation. Technique: Axial T2 turbo spin echo (1.5T, TR=3200, TE=91) B) Findings: The solid component has near homogeneous intense enhancement with a broad dural attachment both medial and inferior to the tumor (arrows). Technique: Coronal T1 turbo spin echo post contrast (1.5T, TR=508, TE=17, contrast=prohance 0.1mmol/kg, delayed phase) C) Findings: The solid component of the tumor (arrow) has relative iso- to hyperintensity compared to the adjacent brain parenchyma. Technique: Axial ADC map image (1.5T, TR=7199, TE=97) Etiology: Incidence: <0.1% of CNS tumors Gender Ratio: M:F = 1.7:1 Age Predilection: Risk Factors: Treatment: Prognosis: 0-2 years of age None known Gross total resection, chemotherapy if complete surgical resection not possible Good, 85% with benign clinical course Findings on Imaging: Typically large and heterogeneous lobar tumor with cystic components and a solid enhancing nodule with a broad dural base Table 1: Summary table of characteristics of. 12
13 Etiology CT MRI Pattern of enhancement Desmoplastic Infantile Ganglioglioma Primitive Neuroectodermal Tumor (Supratentorial) Atypical Teratoid Rhabdoid Tumor (supratentorial) Choroid Plexus Carcinoma Supratentorial Ependymoma Large heterogeneous lobar tumor in the supratentorial brain Hyperdense solid component. Calcification not typical. Large heterogeneous lobar tumor in the supratentorial brain. Solid components may be hyperdense. Calcification and hemorrhage may be present. Large heterogeneous lobar tumor in the supratentorial brain Calcification and possible hemorrhage Large lobular, heterogeneous tumor primarily centered in the ventricles Hydrocephalus. Calcification can be seen. The tumor is typically iso to hyperdense. Large heterogeneous lobar tumor in the supratentorial brain Commonly periventricular. Calcification and cystic areas are common. Solid components are iso to hyperdense. Table 2: Differential diagnosis table for primary CNS tumor in infants. ABBREVIATIONS ADC = apparent diffusion coefficient CAQ = certificate of additional qualification DIG = desmoplastic infantile ganglioglioma DSC = dynamic susceptibility contrast DWI = diffusion weighted imaging EPI = echo planar imaging GFAP = glial fibrillary acidic protein H&E = Hematoxylin and Eosin rcbv = relative cerebral blood volume ROI = region of interest SMA = smooth muscle actin Commonly with cysts and peritumoral edema. Solid components are T1 and T2 isointense Solid nodule has a broad dural base Cystic components are common Less than expected surrounding tumoral edema for size. Diffusion weighted imaging may show decreased diffusion. T1 and T2 iso to hyperintense depending on hemorrhage. May have areas of central necrosis. Diffusion images may show decreased diffusion. Lobular intraventricular tumor T1 and T2 iso to hypointensity depending on calcification. Periventricular invasion may be seen. Heterogeneous periventricular tumor with adjacent edema. Solid components are T1 iso to hypointense and T2 iso to hyperintense. Diffusion weighted images may be decreased in anaplastic tumors. Cysts walls may enhance. Solid components enhance intensely. A dural tail may be seen. Heterogeneous enhancement May have leptomeningeal seeding. Heterogeneous enhancement May have leptomeningeal seeding. Typically marked contrast enhancement. Heterogeneous Online access This publication is online available at: Peer discussion Discuss this manuscript in our protected discussion forum at: Interactivity This publication is available as an interactive article with scroll, window/level, magnify and more features. Available online at KEYWORDS pediatric brain tumors; desmoplastic infantile ganglioglioma; MRI; perfusion; diffusion Published by EduRad 13
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Supratentorial brain tumors in the first year of life are challenging
 ORIGINAL RESEARCH PEDIATRICS Diffusion Imaging for Tumor Grading of Supratentorial Brain Tumors in the First Year of Life S.F. Kralik, A. Taha, A.P. Kamer, J.S. Cardinal, T.A. Seltman, and C.Y. Ho ABSTRACT
ORIGINAL RESEARCH PEDIATRICS Diffusion Imaging for Tumor Grading of Supratentorial Brain Tumors in the First Year of Life S.F. Kralik, A. Taha, A.P. Kamer, J.S. Cardinal, T.A. Seltman, and C.Y. Ho ABSTRACT
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases
 Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases Ho Sung Kim, MD 1 Ho Kyu Lee, MD 1 Ae Kyung Jeong, MD 1 Ji Hoon Shin, MD 1 Choong Gon Choi, MD 1 Shin Kwang Khang, MD 2 We
Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases Ho Sung Kim, MD 1 Ho Kyu Lee, MD 1 Ae Kyung Jeong, MD 1 Ji Hoon Shin, MD 1 Choong Gon Choi, MD 1 Shin Kwang Khang, MD 2 We
Case Report. Case Report
 AJNR Am J Neuroradiol 26:274 278, February 2005 Case Report Differential Chemosensitivity of Tumor Components in a Malignant Oligodendroglioma: Assessment with Diffusion-Weighted, Perfusion- Weighted,
AJNR Am J Neuroradiol 26:274 278, February 2005 Case Report Differential Chemosensitivity of Tumor Components in a Malignant Oligodendroglioma: Assessment with Diffusion-Weighted, Perfusion- Weighted,
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
Outline. Neuroradiology. Diffusion Imaging in. Clinical Applications of. Basics of Diffusion Imaging. Basics of Diffusion Imaging
 Clinical Applications of Diffusion Imaging in Neuroradiology No disclosures Stephen F. Kralik Assistant Professor of Radiology Indiana University School of Medicine Department of Radiology and Imaging
Clinical Applications of Diffusion Imaging in Neuroradiology No disclosures Stephen F. Kralik Assistant Professor of Radiology Indiana University School of Medicine Department of Radiology and Imaging
Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors
 Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors Poster No.: C-2652 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: M. Gavrilov, T.
Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors Poster No.: C-2652 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: M. Gavrilov, T.
Case 7391 Intraventricular Lesion
 Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Structural and functional imaging for the characterization of CNS lymphomas
 Structural and functional imaging for the characterization of CNS lymphomas Cristina Besada Introduction A few decades ago, Primary Central Nervous System Lymphoma (PCNSL) was considered as an extremely
Structural and functional imaging for the characterization of CNS lymphomas Cristina Besada Introduction A few decades ago, Primary Central Nervous System Lymphoma (PCNSL) was considered as an extremely
Role of Diffusion weighted Imaging in the Evaluation of Intracranial Tumors
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 12 Ver. IX (December. 2016), PP 99-104 www.iosrjournals.org Role of Diffusion weighted Imaging
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 12 Ver. IX (December. 2016), PP 99-104 www.iosrjournals.org Role of Diffusion weighted Imaging
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
Imaging Findings of CNS Atypical Teratoid/Rhabdoid Tumors
 AJNR Am J Neuroradiol 25:476 480, March 2004 Case Report Imaging Findings of CNS Atypical Teratoid/Rhabdoid Tumors Atilla Arslanoglu, Nafi Aygun, Deapak Tekhtani, Leslie Aronson, Ken Cohen, Peter C. Burger,
AJNR Am J Neuroradiol 25:476 480, March 2004 Case Report Imaging Findings of CNS Atypical Teratoid/Rhabdoid Tumors Atilla Arslanoglu, Nafi Aygun, Deapak Tekhtani, Leslie Aronson, Ken Cohen, Peter C. Burger,
MRI Findings Of An Atypical Cystic Meningioma A Rare Case
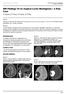 ISPUB.COM The Internet Journal of Radiology Volume 14 Number 1 MRI Findings Of An Atypical Cystic Meningioma A Rare Case D Saxena, P Rout, K Pavan, B Philip Citation D Saxena, P Rout, K Pavan, B Philip.
ISPUB.COM The Internet Journal of Radiology Volume 14 Number 1 MRI Findings Of An Atypical Cystic Meningioma A Rare Case D Saxena, P Rout, K Pavan, B Philip Citation D Saxena, P Rout, K Pavan, B Philip.
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child
 Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Posterior fossa tumors: clues to differential diagnosis with case-based review
 Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad
 Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Pleomorphic xanthoastrocytomas (PXAs) are rare neoplasms. Pleomorphic Xanthoastrocytoma of Childhood: MR Imaging and Diffusion MR Imaging Features
 Published July 3, 2014 as 10.3174/ajnr.A4011 ORIGINAL RESEARCH PEDIATRICS Pleomorphic Xanthoastrocytoma of Childhood: MR Imaging and Diffusion MR Imaging Features W. Moore, D. Mathis, L. Gargan, D.C. Bowers,
Published July 3, 2014 as 10.3174/ajnr.A4011 ORIGINAL RESEARCH PEDIATRICS Pleomorphic Xanthoastrocytoma of Childhood: MR Imaging and Diffusion MR Imaging Features W. Moore, D. Mathis, L. Gargan, D.C. Bowers,
Masses of the Corpus Callosum
 Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
Role of Diffusion Mri In Differentiation Between The Common Pediatric Posterior Fossa Brain Tumors.
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 73 (2), Page 6090-6096 Role of Diffusion Mri In Differentiation Between The Common Pediatric Posterior Fossa Brain Tumors. HanaaAbdelkader Ahmed
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 73 (2), Page 6090-6096 Role of Diffusion Mri In Differentiation Between The Common Pediatric Posterior Fossa Brain Tumors. HanaaAbdelkader Ahmed
Pleomorphic Xanthoastrocytoma
 Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
General Identification. Name: 江 X X Age: 29 y/o Gender: Male Height:172cm, Weight: 65kg Date of admission:95/09/27
 General Identification Name: 江 X X Age: 29 y/o Gender: Male Height:172cm, Weight: 65kg Date of admission:95/09/27 Chief Complaint Sudden onset of seizure for several minutes Present illness This 29-year
General Identification Name: 江 X X Age: 29 y/o Gender: Male Height:172cm, Weight: 65kg Date of admission:95/09/27 Chief Complaint Sudden onset of seizure for several minutes Present illness This 29-year
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution
 Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Joana Ramalho, MD C. Ryan Miller, MD, PhD
 Joana Ramalho, MD C. Ryan Miller, MD, PhD Case 1 3 month old baby girl Presented with new onset of seizures Newborn. Questionable blurring of the gray-white junction within the right occipital lobe. Findings
Joana Ramalho, MD C. Ryan Miller, MD, PhD Case 1 3 month old baby girl Presented with new onset of seizures Newborn. Questionable blurring of the gray-white junction within the right occipital lobe. Findings
Primary Central Nervous System Lymphoma with Lateral Ventricle Involvement
 The Open Medical Imaging Journal, 2012, 6, 103-107 103 Open Access Primary Central Nervous System Lymphoma with Lateral Ventricle Involvement Yumi Oie 1,*, Kazuhiro Murayama 1, Shinya Nagahisa 2, Masato
The Open Medical Imaging Journal, 2012, 6, 103-107 103 Open Access Primary Central Nervous System Lymphoma with Lateral Ventricle Involvement Yumi Oie 1,*, Kazuhiro Murayama 1, Shinya Nagahisa 2, Masato
MRI perfusion of brain tumors: any differences between supratentorial and infratentorial?
 MRI perfusion of brain tumors: any differences between supratentorial and infratentorial? Poster No.: C-2034 Congress: ECR 2012 Type: Scientific Paper Authors: M. Martucci, S. Gaudino, C. Schiarelli, R.
MRI perfusion of brain tumors: any differences between supratentorial and infratentorial? Poster No.: C-2034 Congress: ECR 2012 Type: Scientific Paper Authors: M. Martucci, S. Gaudino, C. Schiarelli, R.
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
New Imaging Concepts in Central Nervous System Neoplasms
 New Imaging Concepts in Central Nervous System Neoplasms Maarten Lequin Department of Pediatric Radiology Wilhelmina Children s Hospital/University Medical Center Utrecht New Imaging Concepts in Central
New Imaging Concepts in Central Nervous System Neoplasms Maarten Lequin Department of Pediatric Radiology Wilhelmina Children s Hospital/University Medical Center Utrecht New Imaging Concepts in Central
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Amide Proton Transfer Imaging: A Novel MR Method for High-grade Brain Tumors.
 Amide Proton Transfer Imaging: A Novel MR Method for High-grade Brain Tumors. Poster No.: C-1732 Congress: ECR 2013 Type: Scientific Exhibit Authors: M. Ida, M. Ishizuka, T. Suzuki, Y. Kubo, K. Hino, S.
Amide Proton Transfer Imaging: A Novel MR Method for High-grade Brain Tumors. Poster No.: C-1732 Congress: ECR 2013 Type: Scientific Exhibit Authors: M. Ida, M. Ishizuka, T. Suzuki, Y. Kubo, K. Hino, S.
Supra- and infratentorial brain tumors from childhood to maternity
 Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the
 Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the potential relation between whole-tumor apparent diffusion
Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the potential relation between whole-tumor apparent diffusion
Infratentorial and Intraparenchymal Subependymoma in the Cerebellum: Case Report
 Case Report Neuroimaging and Head and Neck http://dx.doi.org/10.3348/kjr.2014.15.1.151 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(1):151-155 Infratentorial and Intraparenchymal Subependymoma
Case Report Neuroimaging and Head and Neck http://dx.doi.org/10.3348/kjr.2014.15.1.151 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(1):151-155 Infratentorial and Intraparenchymal Subependymoma
Detection of Leptomeningeal CNS Metastases in Children
 Detection of Leptomeningeal CNS Metastases in Children Noah D. Sabin, M.D. Julie H. Harreld M.D. Kathleen J. Helton M.D. Zoltan Patay M.D., Ph.D. St. Jude Children s Research Hospital Memphis, TN Leptomeningeal
Detection of Leptomeningeal CNS Metastases in Children Noah D. Sabin, M.D. Julie H. Harreld M.D. Kathleen J. Helton M.D. Zoltan Patay M.D., Ph.D. St. Jude Children s Research Hospital Memphis, TN Leptomeningeal
Benign brain lesions
 Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Chordoid glioma: CT and MR features
 Chin J Radiol 2005; 30: 225-229 225 Chordoid glioma: CT and MR features YI-CHIH HSU HUNG-WEN KAO CHUNG-PING LO CHUN-JUNG JUAN SHY-CHYI CHIN CHENG-YU CHEN Department of Radiology, Tri-Service General Hospital
Chin J Radiol 2005; 30: 225-229 225 Chordoid glioma: CT and MR features YI-CHIH HSU HUNG-WEN KAO CHUNG-PING LO CHUN-JUNG JUAN SHY-CHYI CHIN CHENG-YU CHEN Department of Radiology, Tri-Service General Hospital
NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE
 THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
Automated Identification of Neoplasia in Diagnostic Imaging text reports
 Automated Identification of Neoplasia in Diagnostic Imaging text reports "This work has been funded in whole or in part with Federal funds from the National Cancer Institute, National Institutes of Health,
Automated Identification of Neoplasia in Diagnostic Imaging text reports "This work has been funded in whole or in part with Federal funds from the National Cancer Institute, National Institutes of Health,
Understanding general brain tumor pathology, Part I: The basics. Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky
 Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Brain Tumors. Medulloblastoma. Pilocytic astrocytoma: Ahmed Koriesh, MD. Pathological finding
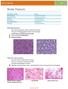 NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
Dysembryoplastic neuroepithelial tumor with atypical presentation: MRI and diffusion tensorcharacteristics
 Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons Radiology Faculty Publications Radiology 2013 Dysembryoplastic neuroepithelial tumor with atypical
Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons Radiology Faculty Publications Radiology 2013 Dysembryoplastic neuroepithelial tumor with atypical
Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results of Cerebral Perfusion MR Imaging
 pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy
 AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
Ring-shaped Lateral Ventricular Nodules Detected with Brain MR Imaging
 Magn Reson Med Sci, Vol. 12, No. 2, pp. 105 110, 2013 2013 Japanese Society for Magnetic Resonance in Medicine doi:10.2463/mrms.2012-0044 MAJOR PAPER Ring-shaped Lateral Ventricular Nodules Detected with
Magn Reson Med Sci, Vol. 12, No. 2, pp. 105 110, 2013 2013 Japanese Society for Magnetic Resonance in Medicine doi:10.2463/mrms.2012-0044 MAJOR PAPER Ring-shaped Lateral Ventricular Nodules Detected with
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Joana Ramalho, MD C. Ryan Miller, MD, PhD
 Joana Ramalho, MD C. Ryan Miller, MD, PhD Case 1 56 year old female Presented with: 3-4 weeks of visual symptoms (asymmetric vision loss, blurry & dark vision, photosensitivity & decreased peripheral vision)
Joana Ramalho, MD C. Ryan Miller, MD, PhD Case 1 56 year old female Presented with: 3-4 weeks of visual symptoms (asymmetric vision loss, blurry & dark vision, photosensitivity & decreased peripheral vision)
RINGS N THINGS: Imaging Patterns in Differential Diagnosis. Anne G. Osborn, M.D.
 RINGS N THINGS: Imaging Patterns in Differential Diagnosis Anne G. Osborn, M.D. ExpDDxs: Intra-axial (Parenchymal) Lesions Ring-enhancing lesions, solitary 1 Ring-enhancing lesion crossing corpus callosum
RINGS N THINGS: Imaging Patterns in Differential Diagnosis Anne G. Osborn, M.D. ExpDDxs: Intra-axial (Parenchymal) Lesions Ring-enhancing lesions, solitary 1 Ring-enhancing lesion crossing corpus callosum
The Radiologic Evaluation of Glioblastoma (GBM) and Differentiation from Pseudoprogression
 The Radiologic Evaluation of Glioblastoma (GBM) and Differentiation from Pseudoprogression Alexis Roy, Harvard Medical School, Year III Our Patient AB: Clinical Presentation 53 year old female with a past
The Radiologic Evaluation of Glioblastoma (GBM) and Differentiation from Pseudoprogression Alexis Roy, Harvard Medical School, Year III Our Patient AB: Clinical Presentation 53 year old female with a past
Journal of Radiology Case Reports
 Pediatric Holohemispheric Developmental Venous Anomaly: Definitive characterization by 3D Susceptibility Weighted Magnetic Resonance Angiography Michael A. Casey 1, Sourabh Lahoti 2, Ajeet Gordhan 2* 1.
Pediatric Holohemispheric Developmental Venous Anomaly: Definitive characterization by 3D Susceptibility Weighted Magnetic Resonance Angiography Michael A. Casey 1, Sourabh Lahoti 2, Ajeet Gordhan 2* 1.
Diffusion Restriction Precedes Contrast Enhancement in Glioblastoma Multiforme
 Diffusion Restriction Precedes Contrast Enhancement in Glioblastoma Multiforme Adil Bata 1, Jai Shankar 2 1 Faculty of Medicine, Class of 2017 2 Department of Diagnostic Radiology, Division of Neuroradiology,
Diffusion Restriction Precedes Contrast Enhancement in Glioblastoma Multiforme Adil Bata 1, Jai Shankar 2 1 Faculty of Medicine, Class of 2017 2 Department of Diagnostic Radiology, Division of Neuroradiology,
Laura Tormoehlen, M.D. Neurology and EM-Toxicology Indiana University
 Laura Tormoehlen, M.D. Neurology and EM-Toxicology Indiana University Disclosures! No conflicts of interest to disclose Neuroimaging 101! Plain films! Computed tomography " Angiography " Perfusion! Magnetic
Laura Tormoehlen, M.D. Neurology and EM-Toxicology Indiana University Disclosures! No conflicts of interest to disclose Neuroimaging 101! Plain films! Computed tomography " Angiography " Perfusion! Magnetic
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Histopathological Study and Categorisation of Brain Tumors
 Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
BRAIN TUMORS IN INFANTS
 BRAIN TUMORS IN INFANTS Dr Sergio Valenzuela M.D-( ISPN-ESPN-FLANC)&cols. Head Pediatric Neurosurgery Unit I Instituto de NeurocirugiaAsenjo Santiago CHILE RATE OF MENINGEAL,BRAIN AND OTHER CNS MALIGNANT
BRAIN TUMORS IN INFANTS Dr Sergio Valenzuela M.D-( ISPN-ESPN-FLANC)&cols. Head Pediatric Neurosurgery Unit I Instituto de NeurocirugiaAsenjo Santiago CHILE RATE OF MENINGEAL,BRAIN AND OTHER CNS MALIGNANT
Neuroradiology of AIDS
 Neuroradiology of AIDS Frank Minja,, HMS IV Gillian Lieberman MD September 2002 AIDS 90% of HIV patients have CNS involvement 1 10% of AIDS patients present first with neurological symptoms 2 73-80% of
Neuroradiology of AIDS Frank Minja,, HMS IV Gillian Lieberman MD September 2002 AIDS 90% of HIV patients have CNS involvement 1 10% of AIDS patients present first with neurological symptoms 2 73-80% of
SWI including phase and magnitude images
 On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
MRI imaging in meningeal diseases
 Original article MRI imaging in meningeal diseases 1Dr. Narendrakumar M Shah, 2 Dr Vaishali D M 1Associate professor, Department of Radiodiagnosis, SDM Medical college, Dharwad 2Consultant radiologist,
Original article MRI imaging in meningeal diseases 1Dr. Narendrakumar M Shah, 2 Dr Vaishali D M 1Associate professor, Department of Radiodiagnosis, SDM Medical college, Dharwad 2Consultant radiologist,
A Stable Secondary Gliosarcoma with Extensive Systemic Metastases: A Case Report
 CASE REPORT Brain Tumor Res Treat 2016;4(2):133-137 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2016.4.2.133 A Stable Secondary Gliosarcoma with Extensive Systemic Metastases: A
CASE REPORT Brain Tumor Res Treat 2016;4(2):133-137 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2016.4.2.133 A Stable Secondary Gliosarcoma with Extensive Systemic Metastases: A
Case 1. Maysa Al-Hussaini MD FRCPath
 Case 1 Maysa Al-Hussaini MD FRCPath MAYSA King AL-HUSSAINI Hussein Cancer MD Center MRCPATH KING HUSSEIN Amman CANCER Jordan CENTER Clinical history 4 year old boy History of frontal headache, sleepiness.
Case 1 Maysa Al-Hussaini MD FRCPath MAYSA King AL-HUSSAINI Hussein Cancer MD Center MRCPATH KING HUSSEIN Amman CANCER Jordan CENTER Clinical history 4 year old boy History of frontal headache, sleepiness.
Supratentorial multiple little meningiomas with transitory stroke symptoms like. MRI case presentation
 114 Romanian Neurosurgery (2010) XVII 1: 114-121 Supratentorial multiple little meningiomas with transitory stroke symptoms like. MRI case presentation E. Moldovanu 1,2, Adriana Moldovanu 1,2, Carmen Gherman
114 Romanian Neurosurgery (2010) XVII 1: 114-121 Supratentorial multiple little meningiomas with transitory stroke symptoms like. MRI case presentation E. Moldovanu 1,2, Adriana Moldovanu 1,2, Carmen Gherman
Sarcomatoid renal cell carcinoma: A case report and literature review
 Sarcomatoid renal cell carcinoma: A case report and literature review Michael Reiter 1*, Ryan Schwope 1, Arthur Clarkson 2 1. Department of Radiology, Brooke Army Medical Center, San Antonio USA 2. Department
Sarcomatoid renal cell carcinoma: A case report and literature review Michael Reiter 1*, Ryan Schwope 1, Arthur Clarkson 2 1. Department of Radiology, Brooke Army Medical Center, San Antonio USA 2. Department
The estimated annual incidence of central nervous system
 ORIGINAL RESEARCH Y. Hayashida T. Hirai S. Morishita M. Kitajima R. Murakami Y. Korogi K. Makino H. Nakamura I. Ikushima M. Yamura M. Kochi J.-i. Kuratsu Y. Yamashita Diffusion-weighted Imaging of Metastatic
ORIGINAL RESEARCH Y. Hayashida T. Hirai S. Morishita M. Kitajima R. Murakami Y. Korogi K. Makino H. Nakamura I. Ikushima M. Yamura M. Kochi J.-i. Kuratsu Y. Yamashita Diffusion-weighted Imaging of Metastatic
CHINESE MEDICAL ASSOCIATION
 Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Cross sectional imaging of Intracranial cystic lesions Abdel Razek A
 Cross sectional imaging of Intracranial cystic lesions Abdel Razek A Department of Radiology. Mansoura Faculty of Medicine, Mansoura. Egypt. arazek@mans.edu.eg Introduction Intracranial cystic lesions
Cross sectional imaging of Intracranial cystic lesions Abdel Razek A Department of Radiology. Mansoura Faculty of Medicine, Mansoura. Egypt. arazek@mans.edu.eg Introduction Intracranial cystic lesions
MR Tumor Staging for Treatment Decision in Case of Wilms Tumor
 MR Tumor Staging for Treatment Decision in Case of Wilms Tumor G. Schneider, M.D., Ph.D.; P. Fries, M.D. Dept. of Diagnostic and Interventional Radiology, Saarland University Hospital, Homburg/Saar, Germany
MR Tumor Staging for Treatment Decision in Case of Wilms Tumor G. Schneider, M.D., Ph.D.; P. Fries, M.D. Dept. of Diagnostic and Interventional Radiology, Saarland University Hospital, Homburg/Saar, Germany
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
NEURORADIOLOGY DIL part 5
 NEURORADIOLOGY DIL part 5 Masses and tumors K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL part
NEURORADIOLOGY DIL part 5 Masses and tumors K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL part
Radiation necrosis is a well-described toxicity that has been
 ORIGINAL RESEARCH PEDIATRICS Radiation Necrosis in Pediatric Patients with Brain Tumors Treated with Proton Radiotherapy X S.F. Kralik, C.Y. Ho, W. Finke, J.C. Buchsbaum, C.P. Haskins, and C.-S. Shih ABSTRACT
ORIGINAL RESEARCH PEDIATRICS Radiation Necrosis in Pediatric Patients with Brain Tumors Treated with Proton Radiotherapy X S.F. Kralik, C.Y. Ho, W. Finke, J.C. Buchsbaum, C.P. Haskins, and C.-S. Shih ABSTRACT
Ependymoblastoma: CT and MRI Demonstration
 Chin J Radiol 2002; 27: 21-25 21 CASE REPORT Ependymoblastoma: CT and MRI Demonstration SHU-HANG NG 1 SHEUNG-FAT KO 2 YAO-LIANG CHEN 1 HO-FAI WONG 1 YAU-YAU WAI 1 Department of Radiology 1, Chang Gung
Chin J Radiol 2002; 27: 21-25 21 CASE REPORT Ependymoblastoma: CT and MRI Demonstration SHU-HANG NG 1 SHEUNG-FAT KO 2 YAO-LIANG CHEN 1 HO-FAI WONG 1 YAU-YAU WAI 1 Department of Radiology 1, Chang Gung
MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES
 MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES DISCLOSURE No conflicts of interest to disclose Patricia Bruns APRN, CNS Givens Brain Tumor Center Abbott Northwestern Hospital October 12, 2018 OBJECTIVES THEN
MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES DISCLOSURE No conflicts of interest to disclose Patricia Bruns APRN, CNS Givens Brain Tumor Center Abbott Northwestern Hospital October 12, 2018 OBJECTIVES THEN
Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma
 From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma Marcus C de Jong, Annette C Moll, Sophia Göricke, Paul van der Valk, Wijnanda A Kors, Jonas A
From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma Marcus C de Jong, Annette C Moll, Sophia Göricke, Paul van der Valk, Wijnanda A Kors, Jonas A
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Magnetic Resonance Imaging. Basics of MRI in practice. Generation of MR signal. Generation of MR signal. Spin echo imaging. Generation of MR signal
 Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017
 AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017 SYLLABUS Papillary Tumor of the Pineal Region and the Differential
AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017 SYLLABUS Papillary Tumor of the Pineal Region and the Differential
Role of Diffusion Weighted Imaging in Intracranial Tumors with Pathological Correlation
 ORIGINAL RESEARCH www.ijcmr.com with Pathological Correlation J. S. Aswini Jyothi, P. Sree Hari 2, V. Karuna 3 ABSTRACT Introduction: Intracranial tumors can occur in all age groups and can be grossly
ORIGINAL RESEARCH www.ijcmr.com with Pathological Correlation J. S. Aswini Jyothi, P. Sree Hari 2, V. Karuna 3 ABSTRACT Introduction: Intracranial tumors can occur in all age groups and can be grossly
ADC Values and Prognosis of Malignant Astrocytomas: Does Lower ADC Predict a Worse Prognosis Independent of Grade of Tumor?
 Neuroradiology/Head and Neck Imaging Original Research Zulfiqar et al. ADC Values and Prognosis of Malignant Astrocytomas Neuroradiology/Head and Neck Imaging Original Research Maria Zulfiqar 1 David M.
Neuroradiology/Head and Neck Imaging Original Research Zulfiqar et al. ADC Values and Prognosis of Malignant Astrocytomas Neuroradiology/Head and Neck Imaging Original Research Maria Zulfiqar 1 David M.
RING ENCHANCING LESION BY M.S. HEMHNATH
 RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
Atypical ganglioneurocytoma: case report and review of literature
 CASE REPORT Atypical ganglioneurocytoma: case report and review of literature Javed Khader Eliyas 1, Peter Pytel 2, Rimas V. Lukas 3, Patrik Gabikian 4 1. Section of Neurosurgery, University of Chicago,
CASE REPORT Atypical ganglioneurocytoma: case report and review of literature Javed Khader Eliyas 1, Peter Pytel 2, Rimas V. Lukas 3, Patrik Gabikian 4 1. Section of Neurosurgery, University of Chicago,
Lara A. Brandão, MD a,b, *, Mark S. Shiroishi, MD c, Meng Law, MD c. mri.theclinics.com KEYWORDS KEY POINTS
 Brain Tumors A Multimodality Approach with Diffusion- Weighted Imaging, Diffusion Tensor Imaging, Magnetic Resonance Spectroscopy, Dynamic Susceptibility Contrast and Dynamic Contrast-Enhanced Magnetic
Brain Tumors A Multimodality Approach with Diffusion- Weighted Imaging, Diffusion Tensor Imaging, Magnetic Resonance Spectroscopy, Dynamic Susceptibility Contrast and Dynamic Contrast-Enhanced Magnetic
Case Report Cystic Meningioma Simulating Arachnoid Cyst: Report of an Unusual Case
 Case Reports in Radiology, Article ID 371969, 4 pages http://dx.doi.org/10.1155/2014/371969 Case Report Cystic Meningioma Simulating Arachnoid Cyst: Report of an Unusual Case Docampo Jorge, 1 Gonzalez
Case Reports in Radiology, Article ID 371969, 4 pages http://dx.doi.org/10.1155/2014/371969 Case Report Cystic Meningioma Simulating Arachnoid Cyst: Report of an Unusual Case Docampo Jorge, 1 Gonzalez
41 year old female with headache. Elena G. Violari MD and Leo Wolansky MD
 41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
Intracranial Lesions: MRI Signs for Localization
 Intracranial Lesions: MRI Signs for Localization Poster No.: C-1574 Congress: ECR 2017 Type: Educational Exhibit Authors: M. Cucos, A. Puiu, S. Manole ; Cluj-Napoca/RO, Cluj napoca/ RO Keywords: Cerebrospinal
Intracranial Lesions: MRI Signs for Localization Poster No.: C-1574 Congress: ECR 2017 Type: Educational Exhibit Authors: M. Cucos, A. Puiu, S. Manole ; Cluj-Napoca/RO, Cluj napoca/ RO Keywords: Cerebrospinal
Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS
 Multiple Primary and Histology Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways
Multiple Primary and Histology Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways
A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence
 A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence Poster No.: C-1347 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Hodel, A. GUILLONNET, M. Rodallec, S. GERBER, R. 1
A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence Poster No.: C-1347 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Hodel, A. GUILLONNET, M. Rodallec, S. GERBER, R. 1
Diffuse Proliferative Cerebral Angiopathy: A case report and review of the literature
 Diffuse Proliferative Cerebral Angiopathy: A case report and review of the literature Rohit 1*, Poh Sun Goh 1 1. Department of Radiology, National University hospital, Singapore * Correspondence: Dr. Rohit,
Diffuse Proliferative Cerebral Angiopathy: A case report and review of the literature Rohit 1*, Poh Sun Goh 1 1. Department of Radiology, National University hospital, Singapore * Correspondence: Dr. Rohit,
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Role of proton magnetic resonance spectroscopy in diagnosis of pilocytic astrocytoma in children
 Alexandria Journal of Medicine (2012) 48, 131 137 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Role of proton magnetic resonance spectroscopy
Alexandria Journal of Medicine (2012) 48, 131 137 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Role of proton magnetic resonance spectroscopy
Pediatric and Adolescent Oligodendrogliomas
 Pediatric and Adolescent Oligodendrogliomas Harold Tice, 1 Patrick D. Barnes, 1 Liliana Goumnerova, 2 R. Michael Scott, 2 and Nancy J. Tarbell 3 PURPOSE: To review the clinical and imaging findings in
Pediatric and Adolescent Oligodendrogliomas Harold Tice, 1 Patrick D. Barnes, 1 Liliana Goumnerova, 2 R. Michael Scott, 2 and Nancy J. Tarbell 3 PURPOSE: To review the clinical and imaging findings in
Role of functional MRI in evaluating intraaxial brain tumors Advances and pitfalls.
 Role of functional MRI in evaluating intraaxial brain tumors Advances and pitfalls. Poster No.: C-1685 Congress: ECR 2014 Type: Educational Exhibit Authors: A. R. Udare, A. Mahajan, S. Juvekar, P. Shetty,
Role of functional MRI in evaluating intraaxial brain tumors Advances and pitfalls. Poster No.: C-1685 Congress: ECR 2014 Type: Educational Exhibit Authors: A. R. Udare, A. Mahajan, S. Juvekar, P. Shetty,
Five Most Common Problems in Surgical Neuropathology
 Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Myxoma of the Vomer Bone
 Myxoma of the Vomer Bone David Besachio 1*, Edward Quigley III 1, Richard Orlandi 2, Hugh Harnsberger 1, Richard Wiggins III 1 1. Department of Radiology, University of Utah, Salt Lake City, USA 2. Department
Myxoma of the Vomer Bone David Besachio 1*, Edward Quigley III 1, Richard Orlandi 2, Hugh Harnsberger 1, Richard Wiggins III 1 1. Department of Radiology, University of Utah, Salt Lake City, USA 2. Department
Methods. Yahya Paksoy, Bülent Oğuz Genç, and Emine Genç. AJNR Am J Neuroradiol 24: , August 2003
 AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
PERFUSION MRI CONTRAST BASED TECHNIQUES
 PERFUSION MRI CONTRAST BASED TECHNIQUES by Kenny K Israni Mar 28, 2006 PERFUSION - MRI Dynamic Susceptibility contrast Dynamic Relaxivity contrast STEADY-STATE STATE TECHNIQUES Steady-state Susceptibility
PERFUSION MRI CONTRAST BASED TECHNIQUES by Kenny K Israni Mar 28, 2006 PERFUSION - MRI Dynamic Susceptibility contrast Dynamic Relaxivity contrast STEADY-STATE STATE TECHNIQUES Steady-state Susceptibility
STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER
 IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Original Article STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER Grishma P. Jobanputra Tutor, Department of Pathology, B.J. Medical College,
IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Original Article STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER Grishma P. Jobanputra Tutor, Department of Pathology, B.J. Medical College,
