Glaucoma is a progressive optic neuropathy with characteristic. In-Vivo Microstructural Anatomy of -Zone Parapapillary Atrophy in Glaucoma.
|
|
|
- Elaine Davidson
- 6 years ago
- Views:
Transcription
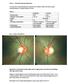
1 Glaucoma In-Vivo Microstructural Anatomy of -Zone Parapapillary Atrophy in Glaucoma Sung Chul Park, 1,2 Carlos Gustavo V. De Moraes, 1,3 Celso Tello, 1,2 Jeffrey M. Liebmann, 1,3 and Robert Ritch 1,2 PURPOSE. To assess the microstructural anatomy of clinical -zone parapapillary atrophy ( PPA) by using Fourier-domain optical coherence tomography (FD-OCT). METHODS. Color photographs and horizontal cross-sectional FD-OCT images of the optic disc and parapapillary retina were obtained in 24 eyes (24 patients with glaucoma or suspected glaucoma) with PPA. The distances between the temporal disc margin and parapapillary landmarks (clinical PPA margin and the edges of the retinal pigment epithelium [RPE], Bruch s membrane [BM], and the photoreceptor inner/outer segment [IS/OS] junction) were measured in 5 equally spaced horizontal meridians (total, 120 meridians). RESULTS. The mean age was (SD) years. In the five meridians, the mean distances from the temporal disc margin to the temporal PPA margin and the edges of RPE, BM, and the IS/OS junction were , , , and m, respectively. The RPE edge corresponded to the PPA margin in 78 (65%) of 120 meridians and ended within the PPA in 42 (35%) of 120 meridians. The BM edge corresponded to the RPE edge in 13 (11%) of 120 meridians and was closer to the disc in 107 (89%) of 120 meridians. The disc margin corresponded to the BM edge in 20 (17%) of 120 meridians and to the edge of the border tissue of Elschnig in 100 (83%) of 120 meridians. The IS/OS junction edge was farther from the disc than the temporal PPA margin was in all 24 eyes. CONCLUSIONS. The PPA was not completely denuded of RPE, and there was a crescent-shaped area of photoreceptor degeneration or atrophy peripheral to the PPA. The termination of the border tissue of Elschnig constituted the temporal disc margin in most eyes with PPA. (Invest Ophthalmol Vis Sci. 2010;51: ) DOI: /iovs Glaucoma is a progressive optic neuropathy with characteristic structural abnormalities of the optic nerve complex (optic nerve head and parapapillary retina). A variety of clinical features of the optic nerve complex, which can be evaluated by ophthalmoscope, have been attributed to glauco- From the 1 Einhorn Clinical Research Center, New York Eye and Ear Infirmary, New York, New York; the 2 Department of Ophthalmology, New York Medical College, Valhalla, New York; and the 3 New York University School of Medicine, New York, New York. Supported by The Shelley and Steven Einhorn Research Fund of the New York Glaucoma Research Institute, New York, NY. Submitted for publication December 21, 2009; revised March 29 and May 19, 2010; accepted May 25, Disclosure: S.C. Park, None; C.G.V. De Moraes, None; C. Tello, None; J.M. Liebmann, Topcon Corporation (F, C); R. Ritch, Topcon Corporation (F) Corresponding author: Jeffrey M. Liebmann, Einhorn Clinical Research Center, New York Eye and Ear Infirmary 310 East 14th Street, New York, NY 10003; jml18@earthlink.net. matous structural damage, 1 4 as well as its progression. 5 7 Systematic and careful examination of the optic nerve complex should include observation of the optic disc size, distribution of the neuroretinal rim tissue, integrity of the retinal nerve fiber layer, the presence of optic disc hemorrhage, and the presence of -zone parapapillary atrophy ( PPA). 3 PPA has received increasing attention, as several reports have demonstrated, not only its association with the presence of glaucoma, 8 11 but also its enlargement as the disease worsens 12,13 and its potential role as a predictor of future progression, although these results have been controversial PPA was initially described more than 80 years ago, 21 but its pathophysiology remains a mystery. Histologic studies have helped to correlate morphologic characteristics with the ophthalmoscopic clinical findings These studies demonstrated atrophied or degenerated outer retinal layers. However, histologic processing of enucleated or postmortem specimens may lead to the alterations of the normal architecture seen in vivo, which may affect their interpretation. Also, some subjects in these histologic studies had malignant melanoma, with or without secondary increased intraocular pressure, 22,23 and others had absolute secondary angle-closure glaucoma, 24 both of which differ substantially from open-angle glaucoma. New technologies that allow rapid, high-resolution imaging of ocular structures have become available to help evaluate glaucoma and retinal diseases. 26 It is now possible to obtain real-time, in vivo images of the optic nerve complex, with a resolution comparable to that in histologic analyses and to correlate them with clinical findings Our hypothesis was that due to the aforementioned limitations of histologic studies, in vivo morphologic characterization of PPA by highresolution imaging should allow a more accurate description of the parapapillary microstructural anatomy in glaucoma patients. To test this hypothesis, we used Fourier-domain optical coherence tomography (FD-OCT) to obtain parapapillary microstructural images in patients with glaucoma or suspected glaucoma with PPA and quantitatively analyzed them. METHODS This is a cross-sectional analysis of data obtained from an ongoing, prospective, longitudinal study approved by the New York Eye and Ear Infirmary Institutional Review Board. Written, informed consent was obtained from all subjects, and the study adhered to the tenets of the Declaration of Helsinki. We prospectively included patients with glaucoma or suspected glaucoma. All participants had open angles by gonioscopy, best corrected visual acuity of 20/40 or better, and refractive errors of 3.0 to 6.0 DS and less than 2.0 DC. Each participant had simultaneous color optic disc stereophotographs (Stereo Camera Model 3-DX; Nidek Inc., Palo Alto, CA), standard automated perimetry (Humphrey Visual Field Analyzer, 24-2 SITA-Standard strategy; Carl Zeiss Meditec, Inc., Dublin, CA), and FD-OCT (3D OCT-1000; Topcon Corporation, Tokyo, Japan) imaging of the optic nerve complex in both eyes on the same day. We Investigative Ophthalmology & Visual Science, December 2010, Vol. 51, No Copyright Association for Research in Vision and Ophthalmology
2 IOVS, December 2010, Vol. 51, No. 12 Microstructures of -Zone Parapapillary Atrophy 6409 excluded individuals with previous posterior segment intraocular surgery, secondary causes of glaucoma (uveitis, trauma, proliferative diabetic retinopathy, or retinal vascular obstruction), systemic or ocular diseases known to affect the visual field (pituitary lesions or demyelinating diseases), inability to perform visual field examinations reliably, and optic disc images of poor quality. Glaucomatous optic disc damage was defined as neuroretinal rim thinning or notching, localized or diffuse retinal nerve fiber layer defect, or a between-eye asymmetry of the vertical cup-disc ratio 0.2. Standard automated perimetry results were considered abnormal if the pattern standard deviation was triggered at the 5%, 2%, 1%, or 0.5% levels or the glaucoma hemifield test result was outside normal limits. A perimetric abnormality required confirmation with an additional visual field test. Patients with suspected glaucoma had signs of glaucomatous optic disc damage with normal visual field test results. Those with established glaucoma had optic disc damage with repeatable visual field loss. From this database (n 130), we further selected only patients with glaucoma or suspected glaucoma with clearly visible PPA on good-quality optic disc photographs and high-quality FD-OCT scans (manufacturer-provided quality factor, 60.00). Stereophotographs were reviewed by two glaucoma specialists (SCP, CGVDM). We defined PPA as an inner crescent of chorioretinal atrophy with visible sclera and choroidal vessels ( PPA) and an outer irregular area of hypoand hyperpigmentation ( -zone PPA). 8,9 The PPA had to involve at least the temporal 180 of the optic disc and have a horizontal width of 150 m in at least one meridian. FD-OCT Imaging Through integration with a nonmydriatic retinal camera, the FD-OCT unit used in the present study provides high-resolution, cross-sectional, three-dimensional volumetric images of the posterior fundus with a black-and-white en face projection image and a color photograph of the optic disc. The system utilizes a near-infrared, low-coherence superluminescent diode (840 nm) light source with a scanning speed of 25,000 A-scans/second, achieving excellent axial (6 m) and lateral (10 m) resolution. The protocol acquires a set of high-definition OCT images of the optic nerve complex in a raster pattern with a scan density of in 3.6 seconds for 65,536 A-scans. For this study, horizontal cross-sectional scans of the optic nerve complex were used, and the images with manufacturer-provided quality scores greater than 60 without motion artifacts were analyzed. Quality scores range from 0 to 100, with a higher score corresponding to better image quality. First, the en face projection image of the optic disc was aligned with the color optic disc photograph by manual overlay, in a manner described elsewhere (Fig. 1), 30 with the resultant margins of the optic disc and PPA in the en face projection image corresponding well with those in the color disc photograph in all eyes. This alignment involved zoom and/or rotation of the color disc photographs. The optic disc margin in clinical color disc photographs was delineated as has been published. 31,32 The disc border was defined as the inner edge of the scleral ring of Elschnig. When a reflective structure was absent, the observer selected the termination of pigment as the disc margin. The FD-OCT provided simultaneous visualization of the en face projection image and the two-dimensional, horizontal, cross-sectional image of the optic nerve complex, as well as direct, real-time correlation between these two images (Figs. 2 4). The outer retinal layers, including the photoreceptor inner segment/outer segment (IS/OS) junction and the retinal pigment epithelium (RPE), Bruch s membrane (BM), and border tissue of Elschnig, were identifiable in the temporal parapapillary area. 33 The RPE could not be easily distinguished from BM outside the parapapillary area, but the edge of the RPE were identified as a steplike structure (Figs. 2C, 3C, 4C). The measurements were performed with OCT mapping software (3D OCT-1000 Truemap Software; ver. 2.1; Topcon Corporation). The distances from the temporal optic disc margin in en face projection images to the following temporal parapapillary microstructures were FIGURE 1. An en face projection image of optic disc and parapapillary retina aligned with color optic disc photograph by manual overlay. measured in the horizontal cross-sectional FD-OCT scans: (1) the temporal margin of clinical PPA, (2) the edge of the RPE, (3) the edge of BM, and (4) the edge of the photoreceptor IS/OS junction. All images were measured and analyzed in a masked fashion by two observers. To evaluate the reproducibility of measurements, we initially performed a trial using a different set of 17 FD-OCT images of the optic nerve complex, in which the two investigators independently measured the same described parameters. The interinvestigator reproducibility determined by intraclass correlation coefficients (ICCs) was excellent for all parameters (r ). After the method was validated, five horizontal, cross-sectional FD-OCT scans of the optic disc complex, which were equally spaced within the vertical diameter of the optic disc (Fig. 2A), were obtained from each eye, and the described parameters were measured from each cross-sectional scan by the two investigators together. When the two investigators disagreed on the disc margin or the parapapillary microstructures, a mutual conclusion was reached after a discussion. When the edges of the microstructures were not clearly visualized, an adjacent horizontal cross-sectional FD- OCT scan, approximately 47 m apart from the original meridian, was used for measurement. The Topcon 3D OCT-1000 provides 128 horizontal cross-sectional scans within 6 mm, with each B-scan approximately 47 m apart from the adjacent one. The level of significance was P 0.05 (two-sided) for all statistical tests (SPSS, ver. 11.0; SPSS, Chicago, IL). RESULTS A total of 24 eyes (24 subjects) with clearly visible PPA met the entry criteria. The mean ( SD) age was years (range, 27 76), and there were 7 subjects of African descent, 13 of European descent, and 4 of Asian descent. One subject had a history of uncomplicated cataract surgery, and another had undergone uncomplicated combined cataract surgery and trabeculectomy with mitomycin C. The baseline characteristics of the subjects are shown in Table 1. Among a total of 120 horizontal cross-sectional FD-OCT scans, approximately 47% (56 scans) showed an unclear edge of one or more parapapillary microstructures, so an adjacent scan was used for measurement, as described in the Methods section. The mean distances between the temporal optic disc margin and the temporal margin of clinical PPA, the edge of the RPE, the edge of BM, and the edge of the photoreceptor IS/OS junction ( PPA, RPE, BM, and IS/OS, respectively) at five equally spaced horizontal meridians crossing the optic disc are shown in Table 2. Mean horizontal and vertical optic
3 6410 Park et al. IOVS, December 2010, Vol. 51, No. 12 width of the BM segment internal (proximal) to the temporal margin of PPA toward the optic disc was m (range, m). The BM edge was closer to the optic disc than the RPE edge in 96% (23/24), 88% (21/24), 83% (20/24), 88% (21/24), and 92% (22/24) of eyes in meridians 1, 2, 3, 4, and 5, respectively (P 0.691, by Pearson s 2 test). Of the total 120 meridians, the BM edge was closer to the optic disc than the RPE edge in 107 (89%) and corresponded to the RPE edge in 13 (11%). The temporal optic disc margin corresponded to the edge of BM in all five meridians (Fig. 4) in 4 (17%) of 24 eyes. The superior edge of the border tissue of Elschnig was internal to the border tissue scleral junction (internally oblique border tissue of Elschnig) in these four eyes, as described in other reports. 31,32 In the remaining 20 eyes (100/120 meridians; 83%), the temporal optic disc margin corresponded to the edge of the border tissue of Elschnig (Figs. 2, 3), and the superior edge of the border tissue of Elschnig was external to the border tissue scleral junction (externally FIGURE 2. (A C) Direct, real-time correlation among color disc photograph, en face projection image, and horizontal, cross-sectional FD- OCT image (right eye). (D F) The same images as in (A C), without the marks. (G) Magnified FD-OCT image of the temporal disc margin and parapapillary microstructures. (A) Five meridians, along which cross-sectional FD-OCT scans were obtained, were equally spaced within the vertical diameter of the optic disc. (C) The photoreceptor IS/OS junction, RPE, Bruch s membrane, and the border tissue of Elschnig are shown in an FD-OCT image along meridian 3, in relation to the temporal margins of the optic disc and PPA. The RPE edge corresponds to the temporal PPA margin, and the termination of the externally oblique border tissue of Elschnig constitutes the temporal optic disc margin. disc diameters were m (range, ) and (range, ) m, respectively. The mean RPE was significantly smaller than the mean PPA at all five meridians (all P 0.03), which demonstrated that the clinical PPA region was not absolutely denuded of RPE. A short segment of RPE was present within the clinical PPA in 42% (10/24 eyes), 25% (6/24 eyes), 42% (10/24 eyes), 25% (6/24 eyes), and 42% (10/24 eyes) in meridians 1, 2, 3, 4, and 5, respectively (P 0.476, by Pearson s 2 test). Of the total 120 meridians, the RPE edge corresponded to the clinical temporal PPA margin in 78 (65%; Figs. 2, 4) and was within the PPA in 42 (35%; Fig. 3). The mean horizontal width of the RPE segment within the PPA was m (range, m). Mean BM was also significantly smaller than the mean PPA at all five meridians (P 0.001). The mean horizontal FIGURE 3. (A C) Direct, real-time correlation among a color disc photograph, en face projection image, and horizontal, cross-sectional FD-OCT image, which shows the presence of RPE within the PPA (right eye). (D F) The same images as in (A C), without the marks. (G) Magnified FD-OCT image of the temporal disc margin and parapapillary microstructures. The termination of the externally oblique border tissue of Elschnig constitutes the temporal optic disc margin. (A, B, horizontal line) The location of the cross-sectional FD-OCT scan.
4 IOVS, December 2010, Vol. 51, No. 12 Microstructures of -Zone Parapapillary Atrophy 6411 FIGURE 4. (A, B) Direct, real-time correlation among a color disc photograph, en face projection image, and horizontal cross-sectional FD-OCT image, which shows that the termination of Bruch s membrane constitutes the temporal optic disc margin (right eye). (D F) The same images as in (A C), without the marks. (G) Magnified FD-OCT image of the temporal disc margin and parapapillary microstructures. The border tissue of Elschnig is internally oblique in this case. (A, B, horizontal line) The location of the cross-sectional FD-OCT scan. oblique border tissue of Elschnig), as described in previous reports. 31,32 The mean IS/OS was significantly greater than the mean PPA at all five meridians (P 0.001), which demonstrated that there was photoreceptor degeneration or atrophy peripheral and adjacent to the PPA as well as inside the PPA. The photoreceptor IS/OS junction ended outside the PPA in all 24 eyes (Fig. 2, 3, 4), and the mean horizontal width of the IS/OS junction-free area outside the temporal border of PPA was m (range, m). It was difficult to demarcate the border of BM or the photoreceptor IS/OS junction ophthalmoscopically. DISCUSSION Our FD-OCT microstructural image analysis suggests that the anatomy of the parapapillary retina including PPA should probably be redefined to include more precise landmarks. The RPE border did not always correspond with the clinical PPA margin, indicating that the clinical PPA was not completely denuded of RPE. The externally oblique border tissue of Elschnig, not BM, constituted the optic disc margin in most subject eyes (83%), and the BM constituted the optic disc margin in the eyes with internally oblique border tissue of Elschnig (17%). In addition, there was an irregular, crescentshape area of photoreceptor degeneration or atrophy peripheral and adjacent to clinical PPA. The horizontal widths of the RPE segment inside the PPA, the BM segment internal (proximal) to the temporal margin of PPA toward the optic disc, and the crescent-shape area of photoreceptor degeneration or atrophy peripheral and adjacent to PPA were highly variable. A previous histologic investigation of PPA reported that the PPA represents a complete loss of RPE and an incomplete loss of adjacent photoreceptors. 23 In the present study, however, RPE was present inside the PPA in 35% of parapapillary FD-OCT images, which indicated that the PPA was not absolutely denuded of RPE but contained a small segment of RPE. This discrepancy can be attributed to the different nature of both studies. In the histologic study, eyes were used that had been enucleated for malignant uveal melanoma, and tissue processing after enucleation may have altered some of the histologic features of PPA. However, in vivo imaging of PPA using FD-OCT can provide a more accurate description of the microstructures of the parapapillary retina. Also, simultaneous visualization of the two-dimensional, horizontal, cross-sectional image of the optic nerve complex and the optic disc photographs and real-time correlation between these two images may make FD-OCT analysis more accurate than histologic study. The short segment of RPE found in the PPA in our study may not have had sufficient pigment to be visible ophthalmoscopically. Our findings regarding the temporal optic disc margin are consistent with the results of two studies performed by Strouthidis et al., 31,32 using normal monkey eyes without PPA, in that the termination of BM constituted the disc margin with internally oblique border tissue of Elschnig and the termination of border tissue of Elschnig constituted the disc margin with the externally oblique border tissue of Elschnig. Also, the BM opening was not always a clinically detectable entity, and it was especially difficult to clinically detect the BM edge in the area where the border tissue of Elschnig was externally oblique. 31,32 We additionally found that, in the human eyes with obvious PPA, the location of the edge of BM was highly variable, ranging from the peripheral border of clinical PPA to the optic disc margin, and the edge of the externally oblique border tissue of Elschnig constituted the disc margin in most eyes (20/24, 83%). In the remaining four TABLE 1. Baseline Clinical Characteristics of 24 Subjects with Clearly Visible PPA Who Had Color Photography and FD-OCT of the Optic Disc and Parapapillary Retina Characteristics Patients, n 24 (24 eyes) Age, y* (range) (27 76) Female/male 12/12 Spherical equivalent, D* (range) ( 5.75 to 3.00) Intraocular pressure, mm Hg* Visual field mean deviation, db* Diagnosis, n Suspected glaucoma 8 (8 eyes) Glaucoma 16 (16 eyes) * Data are expressed as the mean SD. Six subjects with primary open-angle glaucoma, seven with normal-tension glaucoma, two with pigmentary glaucoma, and one with exfoliative glaucoma.
5 6412 Park et al. IOVS, December 2010, Vol. 51, No. 12 TABLE 2. The Mean Distances between the Temporal Optic Disc Margin and Various Parapapillary Microstructures Meridian PPA* P RPE* P BM* P IS/OS* ( ) ( ) ( ) ( ) ( ) Mean (1 5) ( ) ( ) ( ) ( ) ( ) ( ) ( ) (0 475) (0 643) (0 750) (0 976) (0 1044) (0 1044) ( ) ( ) ( ) ( ) ( ) ( ) The following measurements were taken at five equally spaced horizontal meridians crossing the optic disc: PPA, temporal margin of clinical -zone PPA; RPE, edge of the RPE; BM, edge of Bruch s membrane; IS/OS, edge of the photoreceptor IS/OS junction. * Data are expressed in mean micrometers SD (range). PPA vs. RPE. PPA vs. BM. PPA vs. IS/OS. Wilcoxon signed rank test. Paired t-test. eyes (17%), the edge of BM constituted the disc margin with internally oblique border tissue of Elschnig. Our results are generally consistent with a recent qualitative investigation on the cross-sectional configuration of PPA in normal subjects using FD-OCT, 30 but describe the microstructural parapapillary anatomy in more detail using quantitative data. In the previous report, the authors mentioned that the photoreceptor IS/OS junction could be traced to the distal edge of the PPA in all 120 subject eyes. We could also find gradual thinning of the IS/OS junction, but the IS/OS junction eventually ended slightly outside the PPA with an intervening gap area of atrophied photoreceptor cells (mean horizontal width, m). In addition, the edge of the RPE was identified, and it was elucidated that a short segment of RPE (mean, m), the RPE-free BM of variable width (mean, m), and the externally oblique border tissue of Elschnig (mean, m) comprised the clinical PPA beneath the retinal layers. Although atrophy implies an acquired loss of tissue, the border tissue of Elschnig represents congenital collagenous tissue arising from the sclera adjacent to the optic nerve exit from the eye. Therefore, we think that PPA should be redefined to exclude the border tissue of Elschnig. Another study of PPA using microperimetry reported that the psychophysical correlate of PPA is an absolute scotoma and the correlate of the -zone PPA is a relative scotoma. 34 In our study, however, the IS/OS junction ended outside of the PPA in all 24 subject eyes, demonstrating that there is an irregular crescent-shaped zone peripheral and adjacent to the clinical PPA where the photoreceptor cells may be atrophied or degenerated. Therefore, an absolute scotoma may be slightly more extensive than clinical PPA, although the absence of visible IS/OS junction on FD-OCT does not necessarily imply loss of visual function. 35 The present study is partially limited, in that the PPA only in the temporal 180 was analyzed with horizontal scans. Therefore, our results may not be applicable to the PPA superior, nasal, or inferior to the optic disc. Also, our study investigated only the eyes with PPA with a horizontal width of 150 m in at least one meridian. Thus, the results may not apply to the eyes with smaller areas of PPA. There may be minor disagreements between the disc margins in the color disc photograph and in the en face projection image, and those disagreements, if any, may have caused errors in the measurements, especially when the measured distances were very small (e.g., the distance between the temporal margin of PPA and the edge of RPE). Careful interpretation is necessary for the distances measured in the present study (Table 2), because they are not actual distances between landmarks. In measuring the actual distance between structures, the effect of FD-OCT B-scan tilt should be corrected. We did not evaluate the -zone PPA, not only because it is difficult to clearly delineate in the optic disc photograph, but also because it has little clinical significance. Although only patients with glaucoma or suspected glaucoma were examined in the present study, we do not think that our findings are exclusive to glaucomatous optic discs, as similar findings have been reported in normal human and monkey eyes It was difficult to demarcate the border of BM or the photoreceptor IS/OS junction ophthalmoscopically in eyes with conspicuous PPA. Moreover, the RPE border was sometimes different from the ophthalmoscopically defined RPE border, which is the clinical PPA border. Since these microstructures are important landmarks that can be used for optic nerve head and retinal nerve fiber layer analyses, sophisticated machines with advanced technology that can detect those microstructures should be able to provide additional information that may be useful in the diagnosis and management of glaucoma. We hypothesize that automated detection and quantification of PPA would be helpful in glaucoma detection, risk stratification, and research. References 1. Hitchings RA, Poinoosawmy D, Poplar N, Sheth GP. Retinal nerve fibre layer photography in glaucomatous patients. Eye. 1987;1: Bowd C, Weinreb RN, Zangwill LM. Evaluating the optic disc and retinal nerve fiber layer in glaucoma, I: clinical examination and photographic methods. Semin Ophthalmol. 2000;15: Susanna R Jr, Vessani RM. New findings in the evaluation of the optic disc in glaucoma diagnosis. Curr Opin Ophthalmol. 2007; 18: Vessani RM, Moritz R, Batis L, Zagui RB, Bernardoni S, Susanna R. Comparison of quantitative imaging devices and subjective optic nerve head assessment by general ophthalmologists to differentiate normal from glaucomatous eyes. J Glaucoma. 2009;18:
6 IOVS, December 2010, Vol. 51, No. 12 Microstructures of -Zone Parapapillary Atrophy Quigley HA, Katz J, Derick RJ, Gilbert D, Sommer A. An evaluation of optic disc and nerve fiber layer examinations in monitoring progression of early glaucoma damage. Ophthalmology. 1992;99: Jampel HD, Friedman D, Quigley H, et al. Agreement among glaucoma specialists in assessing progressive disc changes from photographs in open-angle glaucoma patients. Am J Ophthalmol. 2009;147: Medeiros FA, Alencar LM, Zangwill LM, Bowd C, Sample PA, Weinreb RN. Prediction of functional loss in glaucoma from progressive optic disc damage. Arch Ophthalmol. 2009;127: Jonas JB, Nguyen XN, Gusek GC, Naumann GO. Parapapillary chorioretinal atrophy in normal and glaucoma eyes. I. Morphometric data. Invest Ophthalmol Vis Sci. 1989;30: Jonas JB, Naumann GO. Parapapillary chorioretinal atrophy in normal and glaucoma eyes, II: correlations. Invest Ophthalmol Vis Sci. 1989;30: Kono Y, Zangwill L, Sample PA, et al. Relationship between parapapillary atrophy and visual field abnormality in primary openangle glaucoma. Am J Ophthalmol. 1999;127: Park SC, Lee DH, Lee HJ, Kee C. Risk factors for normal-tension glaucoma among subgroups of patients. Arch Ophthalmol. 2009; 127: Uchida H, Ugurlu S, Caprioli J. Increasing peripapillary atrophy is associated with progressive glaucoma. Ophthalmology. 1998;105: Budde WM, Jonas JB. Enlargement of parapapillary atrophy in follow-up of chronic open-angle glaucoma. Am J Ophthalmol. 2004;137: Araie M, Sekine M, Suzuki Y, Koseki N. Factors contributing to the progression of visual field damage in eyes with normal-tension glaucoma. Ophthalmology. 1994;101: Tezel G, Kolker AE, Kass MA, Wax MB, Gordon M, Siegmund KD. Parapapillary chorioretinal atrophy in patients with ocular hypertension, I. An evaluation as a predictive factor for the development of glaucomatous damage. Arch Ophthalmol. 1997;115: Martus P, Stroux A, Budde WM, Mardin CY, Korth M, Jonas JB. Predictive factors for progressive optic nerve damage in various types of chronic open-angle glaucoma. Am J Ophthalmol. 2005; 139: Teng CC, De Moraes CG, Prata TS, Tello C, Ritch R, Liebmann JM. Beta-zone parapapillary atrophy and the velocity of glaucoma progression. Ophthalmology. 2010;117: Nevarez J, Rockwood EJ, Anderson DR. The configuration of peripapillary tissue in unilateral glaucoma. Arch Ophthalmol. 1988; 106: Rockwood EJ, Anderson DR. Acquired peripapillary changes and progression in glaucoma. Graefes Arch Clin Exp Ophthalmol. 1988;226: Derick RJ, Pasquale LR, Pease ME, Quigley HA. A clinical study of peripapillary crescents of the optic disc in chronic experimental glaucoma in monkey eyes. Arch Ophthalmol. 1994;112: Bücklers M. Anatomische Untersuchung über die Beziehung zwischen der senilen und myopischen circumpapillaren Aderhautatrophie. Unter Beifügen eines Falles von hochgradiger Anisometropie. Arch Ophthalmol. 1929;121: Fantes FE, Anderson DR. Clinical histologic correlation of human peripapillary anatomy. Ophthalmology. 1989;96: Kubota T, Jonas JB, Naumann GO. Direct clinico-histological correlation of parapapillary chorioretinal atrophy. Br J Ophthalmol. 1993;77: Dichtl A, Jonas JB, Naumann GO. Histomorphometry of the optic disc in highly myopic eyes with absolute secondary angle closure glaucoma. Br J Ophthalmol. 1998;82: Curcio CA, Saunders PL, Younger PW, Malek G. Peripapillary chorioretinal atrophy: Bruch s membrane changes and photoreceptor loss. Ophthalmology. 2000;107: Cordeiro MF, Nickells R, Drexler W, Borrás T, Ritch R. Highresolution ocular imaging: combining advanced optics and microtechnology. Ophthalmic Surg Lasers Imaging. 2009;40: Spaide RF. Age-related choroidal atrophy. Am J Ophthalmol. 2009; 147: Wang M, Hood DC, Cho JS, et al. Measurement of local retinal ganglion cell layer thickness in patients with glaucoma using frequency-domain optical coherence tomography. Arch Ophthalmol. 2009;127: Strouthidis NG, Grimm J, Williams GA, Cull GA, Wilson DJ, Burgoyne CF. A comparison of optic nerve head morphology viewed by spectral domain optical coherence tomography and by serial histology. Invest Ophthalmol Vis Sci. 2010;51: Lee KYC, Tomidokoro A, Sakata R, et al. Cross-sectional anatomic configurations of peripapillary atrophy evaluated with a spectraldomain optical coherence tomography. Invest Ophthalmol Vis Sci. 2010;51: Strouthidis NG, Yang H, Downs JC, Burgoyne CF. Comparison of clinical and three-dimensional histomorphometric optic disc margin anatomy. Invest Ophthalmol Vis Sci. 2009;50: Strouthidis NG, Yang H, Reynaud JF, et al. Comparison of clinical and spectral domain optical coherence tomography optic disc margin anatomy. Invest Ophthalmol Vis Sci. 2009;50: Srinivasan VJ, Monson BK, Wojtkowski M, et al. Characterization of outer retinal morphology with high-speed, ultrahigh-resolution optical coherence tomography. Invest Ophthalmol Vis Sci. 2008; 49: Rensch F, Jonas JB. Direct microperimetry of alpha zone and beta zone parapapillary atrophy. Br J Ophthalmol. 2008;92: Chang LK, Koizumi H, Spaide RF. Disruption of the photoreceptor inner segment-outer segment junction in eyes with macular holes. Retina. 2008;28:
Analysis of Peripapillary Atrophy Using Spectral Domain Optical Coherence Tomography
 Analysis of Peripapillary Atrophy Using Spectral Domain Optical Coherence Tomography The MIT Faculty has made this article openly available. Please share how this access benefits you. Your story matters.
Analysis of Peripapillary Atrophy Using Spectral Domain Optical Coherence Tomography The MIT Faculty has made this article openly available. Please share how this access benefits you. Your story matters.
Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements
 Original article Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements Dewang Angmo, 1 Shibal Bhartiya, 1 Sanjay K Mishra,
Original article Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements Dewang Angmo, 1 Shibal Bhartiya, 1 Sanjay K Mishra,
Advances in OCT Murray Fingeret, OD
 Disclosures Advances in OCT Murray Fingeret, OD Consultant Alcon, Allergan, Bausch & Lomb, Carl Zeiss Meditec, Diopsys, Heidelberg Engineering, Reichert, Topcon Currently Approved OCT Devices OCT Devices
Disclosures Advances in OCT Murray Fingeret, OD Consultant Alcon, Allergan, Bausch & Lomb, Carl Zeiss Meditec, Diopsys, Heidelberg Engineering, Reichert, Topcon Currently Approved OCT Devices OCT Devices
Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma.
 Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma. Donald C. Hood 1,2,* and Ali S. Raza 1 1 Department of Psychology, Columbia
Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma. Donald C. Hood 1,2,* and Ali S. Raza 1 1 Department of Psychology, Columbia
The evaluation of the optic nerve and retinal nerve
 Five rules to evaluate the optic disc and retinal nerve fiber layer for glaucoma Murray Fingeret, O.D., a,b Felipe A. Medeiros, M.D., c Remo Susanna, Jr, M.D., d and Robert N. Weinreb, M.D. c a Department
Five rules to evaluate the optic disc and retinal nerve fiber layer for glaucoma Murray Fingeret, O.D., a,b Felipe A. Medeiros, M.D., c Remo Susanna, Jr, M.D., d and Robert N. Weinreb, M.D. c a Department
Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography
 Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Parapapillary Gamma Zone and Axial Elongation Associated Optic Disc Rotation: The Beijing Eye Study
 Anatomy and Pathology/Oncology Parapapillary Gamma Zone and Axial Elongation Associated Optic Disc Rotation: The Beijing Eye Study Jost B. Jonas, 1,2 Ya Xing Wang, 1 Qi Zhang, 1 Yuan Yuan Fan, 3 Liang
Anatomy and Pathology/Oncology Parapapillary Gamma Zone and Axial Elongation Associated Optic Disc Rotation: The Beijing Eye Study Jost B. Jonas, 1,2 Ya Xing Wang, 1 Qi Zhang, 1 Yuan Yuan Fan, 3 Liang
RETINAL NERVE FIBER LAYER
 CLINICAL SCIENCES The Effect of Scan Diameter on Retinal Nerve Fiber Layer Thickness Measurement Using Stratus Optic Coherence Tomography Giacomo Savini, MD; Piero Barboni, MD; Michele Carbonelli, MD;
CLINICAL SCIENCES The Effect of Scan Diameter on Retinal Nerve Fiber Layer Thickness Measurement Using Stratus Optic Coherence Tomography Giacomo Savini, MD; Piero Barboni, MD; Michele Carbonelli, MD;
Measurement of Choroidal Thickness in Normal Eyes Using 3D OCT-1000 Spectral Domain Optical Coherence Tomography
 pissn: 111-8942 eissn: 292-9382 Korean J Ophthalmol 212;26(4):255-259 http://dx.doi.org/1.3341/kjo.212.26.4.255 Original Article Measurement of Choroidal Thickness in Normal Eyes Using 3D OCT-1 Spectral
pissn: 111-8942 eissn: 292-9382 Korean J Ophthalmol 212;26(4):255-259 http://dx.doi.org/1.3341/kjo.212.26.4.255 Original Article Measurement of Choroidal Thickness in Normal Eyes Using 3D OCT-1 Spectral
Science & Technologies
 STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
Diagnostic Accuracy of OCT with a Normative Database to Detect Diffuse Retinal Nerve Fiber Layer Atrophy: Diffuse Atrophy Imaging Study METHODS
 Glaucoma Diagnostic Accuracy of OCT with a Normative Database to Detect Diffuse Retinal Nerve Fiber Layer Atrophy: Diffuse Atrophy Imaging Study Jin Wook Jeoung, 1,2 Seok Hwan Kim, 1,3 Ki Ho Park, 1,2
Glaucoma Diagnostic Accuracy of OCT with a Normative Database to Detect Diffuse Retinal Nerve Fiber Layer Atrophy: Diffuse Atrophy Imaging Study Jin Wook Jeoung, 1,2 Seok Hwan Kim, 1,3 Ki Ho Park, 1,2
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD
 New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
-Zone Parapapillary Atrophy and the Rate of Retinal Nerve Fiber Layer Thinning in Glaucoma
 Glaucoma -Zone Parapapillary Atrophy and the Rate of Retinal Nerve Fiber Layer Thinning in Glaucoma Eun Ji Lee, 1,2 Tae-Woo Kim, 1,3 Robert N. Weinreb, 4 Ki Ho Park, 1 Seok Hwan Kim, 1,5 and Dong Myung
Glaucoma -Zone Parapapillary Atrophy and the Rate of Retinal Nerve Fiber Layer Thinning in Glaucoma Eun Ji Lee, 1,2 Tae-Woo Kim, 1,3 Robert N. Weinreb, 4 Ki Ho Park, 1 Seok Hwan Kim, 1,5 and Dong Myung
Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
 Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Retinal nerve fiber layer thickness in Indian eyes with optical coherence tomography
 Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Ganglion cell complex scan in the early prediction of glaucoma
 Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
NIH Public Access Author Manuscript Arch Ophthalmol. Author manuscript; available in PMC 2010 November 18.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Ophthalmol. 2009 July ; 127(7): 875 881. doi:10.1001/archophthalmol.2009.145. Measurement of Local Retinal Ganglion Cell Layer
NIH Public Access Author Manuscript Published in final edited form as: Arch Ophthalmol. 2009 July ; 127(7): 875 881. doi:10.1001/archophthalmol.2009.145. Measurement of Local Retinal Ganglion Cell Layer
Il contributo dell'angio-oct: valutazione integrata della componente nervosa e vascolare della malattia glaucomatosa
 SIMPOSIO G.O.A.L. - LE NUOVE FRONTIERE DIAGNOSTICHE E LE LINEE DI INDIRIZZO AMBULATORIALI DEL GLAUCOMA Coordinatore e moderatore: D. Mazzacane Presidente: L. Rossetti Il contributo dell'angio-oct: valutazione
SIMPOSIO G.O.A.L. - LE NUOVE FRONTIERE DIAGNOSTICHE E LE LINEE DI INDIRIZZO AMBULATORIALI DEL GLAUCOMA Coordinatore e moderatore: D. Mazzacane Presidente: L. Rossetti Il contributo dell'angio-oct: valutazione
Characterization of Peripapillary Atrophy Using Spectral Domain Optical Coherence Tomography
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(6):353-359 DOI: 10.3341/kjo.2010.24.6.353 Characterization of Peripapillary trophy Using Spectral Domain Optical Coherence Tomography Original
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(6):353-359 DOI: 10.3341/kjo.2010.24.6.353 Characterization of Peripapillary trophy Using Spectral Domain Optical Coherence Tomography Original
Relationship Between Structure
 Original Article Relationship Between Structure and Function of the Optic Nerve Head-Glaucoma versus Normal Dr Savita Bhat, Dr Anna Elias, Dr Siddharth Pawar, Dr S.J. Saikumar, Dr Alpesh Rajput, superior,
Original Article Relationship Between Structure and Function of the Optic Nerve Head-Glaucoma versus Normal Dr Savita Bhat, Dr Anna Elias, Dr Siddharth Pawar, Dr S.J. Saikumar, Dr Alpesh Rajput, superior,
S Morishita, T Tanabe, S Yu, M Hangai, T Ojima, H Aikawa, N Yoshimura. Clinical science
 Department of Ophthalmology and Visual Sciences, Kyoto University Graduate School of Medicine, Kyoto, Japan Correspondence to: Dr T Tanabe, Department of Ophthalmology, The Tazuke Kofukai Medical Institute,
Department of Ophthalmology and Visual Sciences, Kyoto University Graduate School of Medicine, Kyoto, Japan Correspondence to: Dr T Tanabe, Department of Ophthalmology, The Tazuke Kofukai Medical Institute,
Comparison of Retinal Nerve Fiber Layer Thickness between Stratus and Spectralis OCT
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(3):166-173 DOI: 10.3341/kjo.2011.25.3.166 Original Article Comparison of Retinal Nerve Fiber Layer Thickness between Stratus and Spectralis
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(3):166-173 DOI: 10.3341/kjo.2011.25.3.166 Original Article Comparison of Retinal Nerve Fiber Layer Thickness between Stratus and Spectralis
Noel de Jesus Atienza, MD, MSc and Joseph Anthony Tumbocon, MD
 Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Parafoveal Scanning Laser Polarimetry for Early Glaucoma Detection
 Yamanashi Med. J. 18(1), 15~ 20, 2003 Original Article Parafoveal Scanning Laser Polarimetry for Early Glaucoma Detection Satoshi KOGURE, Yoshiki TODA, Hiroyuki IIJIMA and Shigeo TSUKAHARA Department of
Yamanashi Med. J. 18(1), 15~ 20, 2003 Original Article Parafoveal Scanning Laser Polarimetry for Early Glaucoma Detection Satoshi KOGURE, Yoshiki TODA, Hiroyuki IIJIMA and Shigeo TSUKAHARA Department of
Ultrahigh Speed Imaging of the Rat Retina Using Ultrahigh Resolution Spectral/Fourier Domain OCT
 Ultrahigh Speed Imaging of the Rat Retina Using Ultrahigh Resolution Spectral/Fourier Domain OCT The MIT Faculty has made this article openly available. Please share how this access benefits you. Your
Ultrahigh Speed Imaging of the Rat Retina Using Ultrahigh Resolution Spectral/Fourier Domain OCT The MIT Faculty has made this article openly available. Please share how this access benefits you. Your
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma
 Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
 Romanian Journal of Ophthalmology, Volume 60, Issue 3, July-September 2016. pp:158-164 GENERAL ARTICLE Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
Romanian Journal of Ophthalmology, Volume 60, Issue 3, July-September 2016. pp:158-164 GENERAL ARTICLE Translating data and measurements from stratus to cirrus OCT in glaucoma patients and healthy subjects
Seiji T. Takagi, Yoshiyuki Kita, Asuka Takeyama, and Goji Tomita. 1. Introduction. 2. Subjects and Methods
 Ophthalmology Volume 2011, Article ID 914250, 5 pages doi:10.1155/2011/914250 Clinical Study Macular Retinal Ganglion Cell Complex Thickness and Its Relationship to the Optic Nerve Head Topography in Glaucomatous
Ophthalmology Volume 2011, Article ID 914250, 5 pages doi:10.1155/2011/914250 Clinical Study Macular Retinal Ganglion Cell Complex Thickness and Its Relationship to the Optic Nerve Head Topography in Glaucomatous
Parapapillary Atrophy and Retinal Vessel Diameter in Nonglaucomatous Optic Nerve Damage
 Investigative Ophthalmology & Visual Science, Vol. 32, No. 11, October 1991 Copyright Association for Research in Vision and Ophthalmology Parapapillary Atrophy and Retinal Vessel Diameter in Nonglaucomatous
Investigative Ophthalmology & Visual Science, Vol. 32, No. 11, October 1991 Copyright Association for Research in Vision and Ophthalmology Parapapillary Atrophy and Retinal Vessel Diameter in Nonglaucomatous
Morphologic changes in the optic nerve head and functional
 Predictive Factors of the Optic Nerve Head for Development or Progression of Glaucomatous Visual Field Loss Jost B. Jonas, 1,2 Peter Martus, 3 Folkert K. Horn, 1 Anselm Jünemann, 1 Mathias Korth, 1 and
Predictive Factors of the Optic Nerve Head for Development or Progression of Glaucomatous Visual Field Loss Jost B. Jonas, 1,2 Peter Martus, 3 Folkert K. Horn, 1 Anselm Jünemann, 1 Mathias Korth, 1 and
Detection of Progressive Retinal Nerve Fiber Layer Loss in Glaucoma Using Scanning Laser Polarimetry with Variable Corneal Compensation
 Detection of Progressive Retinal Nerve Fiber Layer Loss in Glaucoma Using Scanning Laser Polarimetry with Variable Corneal Compensation Felipe A. Medeiros, Luciana M. Alencar, Linda M. Zangwill, Christopher
Detection of Progressive Retinal Nerve Fiber Layer Loss in Glaucoma Using Scanning Laser Polarimetry with Variable Corneal Compensation Felipe A. Medeiros, Luciana M. Alencar, Linda M. Zangwill, Christopher
The Optic Nerve Head In Glaucoma. Clinical Pearl #1. Characteristics of Normal Disk 9/26/2017. Initial detectable damage Structure vs function
 The Optic Nerve Head In Glaucoma Clinical Pearl #1 Eric E. Schmidt, O.D., F.A.A.O. Omni Eye Specialists Wilmington,NC schmidtyvision@msn.com Glaucoma is an optic neuropathy Initial detectable damage Structure
The Optic Nerve Head In Glaucoma Clinical Pearl #1 Eric E. Schmidt, O.D., F.A.A.O. Omni Eye Specialists Wilmington,NC schmidtyvision@msn.com Glaucoma is an optic neuropathy Initial detectable damage Structure
NIH Public Access Author Manuscript Arch Ophthalmol. Author manuscript; available in PMC 2013 October 01.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Ophthalmol. 2012 September ; 130(9): 1107 1116. doi:10.1001/archophthalmol.2012.827. A Combined Index of Structure and Function
NIH Public Access Author Manuscript Published in final edited form as: Arch Ophthalmol. 2012 September ; 130(9): 1107 1116. doi:10.1001/archophthalmol.2012.827. A Combined Index of Structure and Function
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Reproducibility of Nerve Fiber Layer Thickness Measurements by Use of Optical Coherence Tomography
 Reproducibility of Nerve Fiber Layer Thickness Measurements by Use of Optical Coherence Tomography Eytan Z. Blumenthal, MD, 1 Julia M. Williams, BS, 1 Robert N. Weinreb, MD, 1 Christopher A. Girkin, MD,
Reproducibility of Nerve Fiber Layer Thickness Measurements by Use of Optical Coherence Tomography Eytan Z. Blumenthal, MD, 1 Julia M. Williams, BS, 1 Robert N. Weinreb, MD, 1 Christopher A. Girkin, MD,
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma. Module 3a GDx
 STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
Is NTG different from POAG?
 Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
OtticaFisiopatologica
 Anno quindicesimo dicembre 2010 How to assess the retinal nerve fiber layer thickness Antonio Ferreras Miguel Servet University Hospital, Zaragoza. Aragón Health Sciences Institute University of Zaragoza
Anno quindicesimo dicembre 2010 How to assess the retinal nerve fiber layer thickness Antonio Ferreras Miguel Servet University Hospital, Zaragoza. Aragón Health Sciences Institute University of Zaragoza
Differences between Non-arteritic Anterior Ischemic Optic Neuropathy and Open Angle Glaucoma with Altitudinal Visual Field Defect
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC)
 Dada T et al Original article Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC) Dada T1, Aggarwal A1, Bali SJ2, Sharma A1, Shah
Dada T et al Original article Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC) Dada T1, Aggarwal A1, Bali SJ2, Sharma A1, Shah
CLINICAL SCIENCES. Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography
 CLINICAL SCIENCES Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography Seong Bae Park, MD; Kyung Rim Sung, MD, PhD; Sung Yong Kang, MD; Kyung Ri Kim, BS;
CLINICAL SCIENCES Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography Seong Bae Park, MD; Kyung Rim Sung, MD, PhD; Sung Yong Kang, MD; Kyung Ri Kim, BS;
Patterns of Subsequent Progression of Localized Retinal Nerve Fiber Layer Defects on Red-free Fundus Photographs in Normal-tension Glaucoma
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):330-336 http://dx.doi.org/10.3341/kjo.2014.28.4.330 Original Article Patterns of Subsequent Progression of Localized Retinal Nerve Fiber
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):330-336 http://dx.doi.org/10.3341/kjo.2014.28.4.330 Original Article Patterns of Subsequent Progression of Localized Retinal Nerve Fiber
Available online at Pelagia Research Library. Advances in Applied Science Research, 2013, 4(6):
 Available online at www.pelagiaresearchlibrary.com Advances in Applied Science Research, 2013, 4(6):201-206 ISSN: 0976-8610 CODEN (USA): AASRFC Comparison of glaucoma diagnostic ability of retinal nerve
Available online at www.pelagiaresearchlibrary.com Advances in Applied Science Research, 2013, 4(6):201-206 ISSN: 0976-8610 CODEN (USA): AASRFC Comparison of glaucoma diagnostic ability of retinal nerve
EXPERIMENTAL AND THERAPEUTIC MEDICINE 6: , 2013
 268 Comparison of optic nerve morphology in eyes with glaucoma and eyes with non-arteritic anterior ischemic optic neuropathy by Fourier domain optical coherence tomography YUXIN YANG 1, HAITAO ZHANG 1,
268 Comparison of optic nerve morphology in eyes with glaucoma and eyes with non-arteritic anterior ischemic optic neuropathy by Fourier domain optical coherence tomography YUXIN YANG 1, HAITAO ZHANG 1,
To assess the glaucoma diagnostic ability of Fourier Domain Optical Coherence Tomography
 American Journal of Engineering Research (AJER) e-issn : 2320-0847 p-issn : 2320-0936 Volume-02, Issue-11, pp-104-110 www.ajer.org Research Paper Open Access To assess the glaucoma diagnostic ability of
American Journal of Engineering Research (AJER) e-issn : 2320-0847 p-issn : 2320-0936 Volume-02, Issue-11, pp-104-110 www.ajer.org Research Paper Open Access To assess the glaucoma diagnostic ability of
Peripapillary Retinal Thickness. Maps in the Evaluation of Glaucoma Patients: A Novel Concept.
 Peripapillary Retinal Thickness Maps in the Evaluation of Glaucoma Patients: A Novel Concept The Harvard community has made this article openly available. Please share how this access benefits you. Your
Peripapillary Retinal Thickness Maps in the Evaluation of Glaucoma Patients: A Novel Concept The Harvard community has made this article openly available. Please share how this access benefits you. Your
Structural examina.on: Imaging
 ManaMa: Glaucoma Structural examina.on: Imaging Luís Abegão Pinto, MD, PhD Department of Ophthalmology CHLC Lisbon Faculty of Medicine, Lisbon University 1 11-10- 2013 Structural changes Qualitative changes
ManaMa: Glaucoma Structural examina.on: Imaging Luís Abegão Pinto, MD, PhD Department of Ophthalmology CHLC Lisbon Faculty of Medicine, Lisbon University 1 11-10- 2013 Structural changes Qualitative changes
International Journal of Scientific & Engineering Research, Volume 4, Issue 12, December ISSN
 International Journal of Scientific & Engineering Research, Volume 4, Issue 12, December-2013 108 Name of Chief and Corresponding Author : Dr Chandrima Paul TITLE : Comparison of glaucoma diagnostic ability
International Journal of Scientific & Engineering Research, Volume 4, Issue 12, December-2013 108 Name of Chief and Corresponding Author : Dr Chandrima Paul TITLE : Comparison of glaucoma diagnostic ability
Confocal Adaptive Optics Imaging of Peripapillary Nerve Fiber Bundles: Implications for Glaucomatous Damage Seen on Circumpapillary OCT Scans
 Article DOI: 10.1167/tvst.4.2.12 Confocal Adaptive Optics Imaging of Peripapillary Nerve Fiber Bundles: Implications for Glaucomatous Damage Seen on Circumpapillary OCT Scans Donald C. Hood 1, Monica F.
Article DOI: 10.1167/tvst.4.2.12 Confocal Adaptive Optics Imaging of Peripapillary Nerve Fiber Bundles: Implications for Glaucomatous Damage Seen on Circumpapillary OCT Scans Donald C. Hood 1, Monica F.
CLINICAL SCIENCES. optic neuropathy characterized
 CLINICAL SCIENCES Spectral-Domain Optical Coherence Tomography for Detection of Localized Retinal Nerve Fiber Layer Defects in Patients With Open-Angle Glaucoma Na Rae Kim, MD; Eun Suk Lee, MD, PhD; Gong
CLINICAL SCIENCES Spectral-Domain Optical Coherence Tomography for Detection of Localized Retinal Nerve Fiber Layer Defects in Patients With Open-Angle Glaucoma Na Rae Kim, MD; Eun Suk Lee, MD, PhD; Gong
Scanning Laser Tomography to Evaluate Optic Discs of Normal Eyes
 Scanning Laser Tomography to Evaluate Optic Discs of Normal Eyes Hiroshi Nakamura,* Toshine Maeda,* Yasuyuki Suzuki and Yoichi Inoue* *Eye Division of Olympia Medical Clinic, Tokyo, Japan; Department of
Scanning Laser Tomography to Evaluate Optic Discs of Normal Eyes Hiroshi Nakamura,* Toshine Maeda,* Yasuyuki Suzuki and Yoichi Inoue* *Eye Division of Olympia Medical Clinic, Tokyo, Japan; Department of
Visual field progression outcomes in glaucoma subtypes
 Visual field progression outcomes in glaucoma subtypes Carlos Gustavo De Moraes, 1,2,3 Jeffrey M. Liebmann, 1,2 Craig A. Liebmann, 1 Remo Susanna Jr, 3 Celso Tello 1,4 and Robert Ritch 1,4 1 Einhorn Clinical
Visual field progression outcomes in glaucoma subtypes Carlos Gustavo De Moraes, 1,2,3 Jeffrey M. Liebmann, 1,2 Craig A. Liebmann, 1 Remo Susanna Jr, 3 Celso Tello 1,4 and Robert Ritch 1,4 1 Einhorn Clinical
A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT) Retinal Nerve Fiber Layer Measurements Based on Time Domain OCT Measurements
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(5):369-377 http://dx.doi.org/10.3341/kjo.2012.26.5.369 Original Article A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT)
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(5):369-377 http://dx.doi.org/10.3341/kjo.2012.26.5.369 Original Article A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT)
MATERIALS AND METHODS
 Glaucoma Analysis of Peripapillary Retinal Nerve Fiber Distribution in Normal Young Adults Seung Woo Hong, 1,2 Myung Douk Ahn, 2 Shin Hee Kang, 1,3 and Seong Kyu Im 1,4 PURPOSE. To determine the anatomic
Glaucoma Analysis of Peripapillary Retinal Nerve Fiber Distribution in Normal Young Adults Seung Woo Hong, 1,2 Myung Douk Ahn, 2 Shin Hee Kang, 1,3 and Seong Kyu Im 1,4 PURPOSE. To determine the anatomic
Change of b-zone Parapapillary Atrophy During Axial Elongation: Boramae Myopia Cohort Study Report 3 METHODS
 Glaucoma Change of b-zone Parapapillary Atrophy During Axial Elongation: Boramae Myopia Cohort Study Report 3 Kyoung Min Lee, 1,2 Ho-Kyung Choung, 1,2 Martha Kim, 3 Sohee Oh, 4 and Seok Hwan Kim 1,2 1
Glaucoma Change of b-zone Parapapillary Atrophy During Axial Elongation: Boramae Myopia Cohort Study Report 3 Kyoung Min Lee, 1,2 Ho-Kyung Choung, 1,2 Martha Kim, 3 Sohee Oh, 4 and Seok Hwan Kim 1,2 1
Case Report Peripapillary Intrachoroidal Cavitation in Myopia Evaluated with Multimodal Imaging Comprising (En-Face) Technique
 Case Reports in Ophthalmological Medicine Volume 2015, Article ID 890876, 5 pages http://dx.doi.org/10.1155/2015/890876 Case Report Peripapillary Intrachoroidal Cavitation in Myopia Evaluated with Multimodal
Case Reports in Ophthalmological Medicine Volume 2015, Article ID 890876, 5 pages http://dx.doi.org/10.1155/2015/890876 Case Report Peripapillary Intrachoroidal Cavitation in Myopia Evaluated with Multimodal
Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed?
 Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed? Jody Piltz-Seymour, M.D. Clinical Professor Perelman School of Medicine University of Pennsylvania Wills Glaucoma Service Valley
Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed? Jody Piltz-Seymour, M.D. Clinical Professor Perelman School of Medicine University of Pennsylvania Wills Glaucoma Service Valley
Relationship between the GDx VCC and Stratus OCT in Primary Open Angle Glaucoma
 Relationship between the GDx VCC and Stratus OCT in Primary Open Angle Glaucoma Reza Zarei, MD 1 Mohammad Soleimani, MD 2 Sasan Moghimi, MD 3 Mohammad Yaser Kiarudi, MD 2 Mahmoud Jabbarvand, MD 1 Yadollah
Relationship between the GDx VCC and Stratus OCT in Primary Open Angle Glaucoma Reza Zarei, MD 1 Mohammad Soleimani, MD 2 Sasan Moghimi, MD 3 Mohammad Yaser Kiarudi, MD 2 Mahmoud Jabbarvand, MD 1 Yadollah
Cirrus TM HD-OCT. Details define your decisions
 Cirrus TM HD-OCT Details define your decisions 2 With high-definition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl Zeiss
Cirrus TM HD-OCT Details define your decisions 2 With high-definition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl Zeiss
Cirrus TM HD-OCT. Details defi ne your decisions
 Cirrus TM HD-OCT Details defi ne your decisions 2 With high-defi nition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl
Cirrus TM HD-OCT Details defi ne your decisions 2 With high-defi nition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl
Preperimetric glaucoma diagnosis by confocal scanning laser tomography of the optic disc
 Br J Ophthalmol 1999;83:299 304 299 Department of Ophthalmology and Eye Hospital, Friedrich-Alexander- University Erlangen-Nürnberg, Erlangen, Germany C Y Mardin F K Horn J B Jonas W M Budde Correspondence
Br J Ophthalmol 1999;83:299 304 299 Department of Ophthalmology and Eye Hospital, Friedrich-Alexander- University Erlangen-Nürnberg, Erlangen, Germany C Y Mardin F K Horn J B Jonas W M Budde Correspondence
OPTOMETRY RESEARCH PAPER
 C L I N I C A L A N D E X P E R I M E N T A L OPTOMETRY RESEARCH PAPER Interocular symmetry of retinal nerve fibre layer thickness in healthy eyes: a spectral-domain optical coherence tomographic study
C L I N I C A L A N D E X P E R I M E N T A L OPTOMETRY RESEARCH PAPER Interocular symmetry of retinal nerve fibre layer thickness in healthy eyes: a spectral-domain optical coherence tomographic study
Posterior Displacement of the Lamina Cribrosa in Glaucoma: In Vivo Interindividual and Intereye Comparisons
 Glaucoma Posterior Displacement of the Lamina Cribrosa in Glaucoma: In Vivo Interindividual and Intereye Comparisons Rafael L. Furlanetto, 1 Sung Chul Park, 1,2 Uma J. Damle, 1 * Sandra Fernando Sieminski,
Glaucoma Posterior Displacement of the Lamina Cribrosa in Glaucoma: In Vivo Interindividual and Intereye Comparisons Rafael L. Furlanetto, 1 Sung Chul Park, 1,2 Uma J. Damle, 1 * Sandra Fernando Sieminski,
Scanning Laser Polarimetry and Optical Coherence Tomography for Detection of Retinal Nerve Fiber Layer Defects
 접수번호 : 2008-105 Korean Journal of Ophthalmology 2009;23:169-175 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.169 Scanning Laser Polarimetry and Optical Coherence Tomography for Detection of Retinal Nerve
접수번호 : 2008-105 Korean Journal of Ophthalmology 2009;23:169-175 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.169 Scanning Laser Polarimetry and Optical Coherence Tomography for Detection of Retinal Nerve
The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation
 C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
Advances in the Structural Evaluation of Glaucoma with Optical Coherence Tomography
 Curr Ophthalmol Rep (2013) 1:98 105 DOI 10.1007/s40135-013-0014-4 DIAGNOSIS AND MONITORING OF GLAUCOMA (S SMITH, SECTION EDITOR) Advances in the Structural Evaluation of Glaucoma with Optical Coherence
Curr Ophthalmol Rep (2013) 1:98 105 DOI 10.1007/s40135-013-0014-4 DIAGNOSIS AND MONITORING OF GLAUCOMA (S SMITH, SECTION EDITOR) Advances in the Structural Evaluation of Glaucoma with Optical Coherence
Reproducibility of Retinal Nerve Fiber Layer Thickness Measurements Using Spectral Domain Optical Coherence Tomography
 ORIGINAL STUDY Reproducibility of Retinal Nerve Fiber Layer Thickness Measurements Using Spectral Domain Optical Coherence Tomography Huijuan Wu, MD, PhD,*w Johannes F. de Boer, PhD,z and Teresa C. Chen,
ORIGINAL STUDY Reproducibility of Retinal Nerve Fiber Layer Thickness Measurements Using Spectral Domain Optical Coherence Tomography Huijuan Wu, MD, PhD,*w Johannes F. de Boer, PhD,z and Teresa C. Chen,
Optical coherence tomography (OCT) is a noninvasive,
 Ability of Stratus OCT to Detect Progressive Retinal Nerve Fiber Layer Atrophy in Glaucoma Eun Ji Lee, 1,2 Tae-Woo Kim, 1,2 Ki Ho Park, 2 Mincheol Seong, 3 Hyunjoong Kim, 4 and Dong Myung Kim 2 PURPOSE.
Ability of Stratus OCT to Detect Progressive Retinal Nerve Fiber Layer Atrophy in Glaucoma Eun Ji Lee, 1,2 Tae-Woo Kim, 1,2 Ki Ho Park, 2 Mincheol Seong, 3 Hyunjoong Kim, 4 and Dong Myung Kim 2 PURPOSE.
CHAPTER 13 CLINICAL CASES INTRODUCTION
 2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients
 Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients Yoshio Yamazaki, Kenji Mizuki, Fukuko Hayamizu and Chizuru Tanaka Department of Ophthalmology, Nihon
Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients Yoshio Yamazaki, Kenji Mizuki, Fukuko Hayamizu and Chizuru Tanaka Department of Ophthalmology, Nihon
Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic Syndrome
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
R&M Solutions
 Mohamed Hosny El-Bradey, MD., Assistant Professor of Ophthalmology, Tanta University. Wael El Haig, MD., Professor of Ophthalmology. Zagazeeg University. 1 Myopic CNV is considered the most common vision
Mohamed Hosny El-Bradey, MD., Assistant Professor of Ophthalmology, Tanta University. Wael El Haig, MD., Professor of Ophthalmology. Zagazeeg University. 1 Myopic CNV is considered the most common vision
Electrodiagnostics Alphabet Soup
 Nathan Lighthizer, O.D., F.A.A.O Assistant Professor, NSUOCO Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic What is electrodiagnostics testing? Visual Pathway Basic Understanding VEP
Nathan Lighthizer, O.D., F.A.A.O Assistant Professor, NSUOCO Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic What is electrodiagnostics testing? Visual Pathway Basic Understanding VEP
The optic nerve head ONH) is an important anatomic
 Glaucoma Deep Optic Nerve Head Morphology Is Associated With Pattern of Glaucomatous Visual Field Defect in Open-Angle Glaucoma Jong Chul Han, Jae Hwan Choi, Do Young Park, Eun Jung Lee, and Changwon Kee
Glaucoma Deep Optic Nerve Head Morphology Is Associated With Pattern of Glaucomatous Visual Field Defect in Open-Angle Glaucoma Jong Chul Han, Jae Hwan Choi, Do Young Park, Eun Jung Lee, and Changwon Kee
Downloaded from:
 Healey, PR; Mitchell, P; Gilbert, CE; Lee, AJ; Ge, DL; Snieder, H; Spector, TD; Hammond, CJ (2007) The inheritance of peripapillary atrophy. Investigative ophthalmology & visual science, 48 (6). pp. 2529-2534.
Healey, PR; Mitchell, P; Gilbert, CE; Lee, AJ; Ge, DL; Snieder, H; Spector, TD; Hammond, CJ (2007) The inheritance of peripapillary atrophy. Investigative ophthalmology & visual science, 48 (6). pp. 2529-2534.
Peripapillary circle of Zinn Haller revealed by fundus fluorescein angiography
 British Journal of Ophthalmology 1997;81:663 667 663 Department of Ophthalmology, School of Medicine, Hanyang University, Seoul, Korea M-K Ko D-S Kim Y-K Ahn Correspondence to: Myung-Kyoo Ko, MD, Department
British Journal of Ophthalmology 1997;81:663 667 663 Department of Ophthalmology, School of Medicine, Hanyang University, Seoul, Korea M-K Ko D-S Kim Y-K Ahn Correspondence to: Myung-Kyoo Ko, MD, Department
The Role of the RNFL in the Diagnosis of Glaucoma
 Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Reproducibility of Choroidal Thickness Measurements Across Three Spectral Domain Optical Coherence Tomography Systems
 Reproducibility of Choroidal Thickness Measurements Across Three Spectral Domain Optical Coherence Tomography Systems The MIT Faculty has made this article openly available. Please share how this access
Reproducibility of Choroidal Thickness Measurements Across Three Spectral Domain Optical Coherence Tomography Systems The MIT Faculty has made this article openly available. Please share how this access
Although measurements of the optic disc and retinal nerve
 Longitudinal Variability of Optic Disc and Retinal Nerve Fiber Layer Measurements Christopher Kai-shun Leung, 1,2 Carol Yim-lui Cheung, 1 Dusheng Lin, 1,3 Chi Pui Pang, 1 Dennis S. C. Lam, 1 and Robert
Longitudinal Variability of Optic Disc and Retinal Nerve Fiber Layer Measurements Christopher Kai-shun Leung, 1,2 Carol Yim-lui Cheung, 1 Dusheng Lin, 1,3 Chi Pui Pang, 1 Dennis S. C. Lam, 1 and Robert
Defects of the Lamina Cribrosa in Eyes with Localized Retinal Nerve Fiber Layer Loss
 Defects of the Lamina Cribrosa in Eyes with Localized Retinal Nerve Fiber Layer Loss Andrew J. Tatham, FRCOphth, Atsuya Miki, MD, PhD, Robert N. Weinreb, MD, Linda M. Zangwill, PhD, Felipe A. Medeiros,
Defects of the Lamina Cribrosa in Eyes with Localized Retinal Nerve Fiber Layer Loss Andrew J. Tatham, FRCOphth, Atsuya Miki, MD, PhD, Robert N. Weinreb, MD, Linda M. Zangwill, PhD, Felipe A. Medeiros,
Correlating Structure With Function in End-Stage Glaucoma
 C L I N I C A L S C I E N C E Correlating Structure With Function in End-Stage Glaucoma Eytan Z. Blumenthal, MD; Amjad Horani, MD; Rajesh Sasikumar, MD; Chandrasekhar Garudadri, MD; Addepalli Udaykumar,
C L I N I C A L S C I E N C E Correlating Structure With Function in End-Stage Glaucoma Eytan Z. Blumenthal, MD; Amjad Horani, MD; Rajesh Sasikumar, MD; Chandrasekhar Garudadri, MD; Addepalli Udaykumar,
A vailability of the scanning laser polarimeter now permits
 70 CLINICAL SCIENCE Specificity and sensitivity of glaucoma detection in the Japanese population using scanning laser polarimetry Shigeo Funaki, Motohiro Shirakashi, Kiyoshi Yaoeda, Haruki Abe, Shiho Kunimatsu,
70 CLINICAL SCIENCE Specificity and sensitivity of glaucoma detection in the Japanese population using scanning laser polarimetry Shigeo Funaki, Motohiro Shirakashi, Kiyoshi Yaoeda, Haruki Abe, Shiho Kunimatsu,
Detection of Glaucoma Using Scanning Laser Polarimetry with Enhanced Corneal Compensation
 Detection of Glaucoma Using Scanning Laser Polarimetry with Enhanced Corneal Compensation Felipe A. Medeiros, Christopher Bowd, Linda M. Zangwill, Chirag Patel, and Robert N. Weinreb From the Hamilton
Detection of Glaucoma Using Scanning Laser Polarimetry with Enhanced Corneal Compensation Felipe A. Medeiros, Christopher Bowd, Linda M. Zangwill, Chirag Patel, and Robert N. Weinreb From the Hamilton
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
OCT Image Analysis System for Grading and Diagnosis of Retinal Diseases and its Integration in i-hospital
 Progress Report for1 st Quarter, May-July 2017 OCT Image Analysis System for Grading and Diagnosis of Retinal Diseases and its Integration in i-hospital Milestone 1: Designing Annotation tool extraction
Progress Report for1 st Quarter, May-July 2017 OCT Image Analysis System for Grading and Diagnosis of Retinal Diseases and its Integration in i-hospital Milestone 1: Designing Annotation tool extraction
Optic Nerve: Clinical Examination
 Optic Nerve: Clinical Examination Marcelo T. Nicolela 2 Core Messages Optic disc evaluation is of fundamental importance in the management of glaucoma. Clinical examination of the optic disc is best performed
Optic Nerve: Clinical Examination Marcelo T. Nicolela 2 Core Messages Optic disc evaluation is of fundamental importance in the management of glaucoma. Clinical examination of the optic disc is best performed
Clinical decision making based on data from GDx: One year observations
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2002 Clinical decision making based on data from GDx: One year observations James C. Bobrow Washington University
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2002 Clinical decision making based on data from GDx: One year observations James C. Bobrow Washington University
OCT in the Diagnosis and Follow-up of Glaucoma
 OCT in the Diagnosis and Follow-up of Glaucoma Karim A Raafat MD. Professor Of Ophthalmology Cairo University Hmmmm! Do I have Glaucoma or not?! 1 Visual Function 100% - N Gl Structure : - 5000 axon /
OCT in the Diagnosis and Follow-up of Glaucoma Karim A Raafat MD. Professor Of Ophthalmology Cairo University Hmmmm! Do I have Glaucoma or not?! 1 Visual Function 100% - N Gl Structure : - 5000 axon /
10/27/2013. Optic Red Herrings
 Optic Red Herrings 1 Optic neuropathy Compressive Inflammatory Toxic Glaucomatous Ischemic Post traumatic GLAUCOMATOUS OPTIC NEUROPATHY Glaucoma: Traditionally defined as a progressive optic neuropathy
Optic Red Herrings 1 Optic neuropathy Compressive Inflammatory Toxic Glaucomatous Ischemic Post traumatic GLAUCOMATOUS OPTIC NEUROPATHY Glaucoma: Traditionally defined as a progressive optic neuropathy
Recent studies have suggested that the pattern of loss of
 Influence of Cilioretinal Arteries on Neuroretinal Rim and Parapapillary Atrophy in Glaucoma Wido M. Budde 1,2 and Jost B. Jonas 1,2 PURPOSE. The pattern of neuroretinal rim loss and increase in the area
Influence of Cilioretinal Arteries on Neuroretinal Rim and Parapapillary Atrophy in Glaucoma Wido M. Budde 1,2 and Jost B. Jonas 1,2 PURPOSE. The pattern of neuroretinal rim loss and increase in the area
Research Article The Pattern of Retinal Nerve Fiber Layer and Macular Ganglion Cell-Inner Plexiform Layer Thickness Changes in Glaucoma
 Hindawi Ophthalmology Volume 2017, Article ID 78365, 8 pages https://doi.org/10.1155/2017/78365 Research Article The Pattern of Retinal Nerve Fiber Layer and Macular Ganglion Cell-Inner Plexiform Layer
Hindawi Ophthalmology Volume 2017, Article ID 78365, 8 pages https://doi.org/10.1155/2017/78365 Research Article The Pattern of Retinal Nerve Fiber Layer and Macular Ganglion Cell-Inner Plexiform Layer
Early Detection Of Glaucoma Clinical Clues. Points To Live By. Glaucoma Risk Factors 10/3/2014
 Early Detection Of Glaucoma Clinical Clues Eric E. Schmidt, O.D. Omni Eye Specialists Wilmington, NC schmidtyvision@msn.com Points To Live By 25% of G pxs NEVER have IOP >21mm 50% of G pxs have trough
Early Detection Of Glaucoma Clinical Clues Eric E. Schmidt, O.D. Omni Eye Specialists Wilmington, NC schmidtyvision@msn.com Points To Live By 25% of G pxs NEVER have IOP >21mm 50% of G pxs have trough
NIH Public Access Author Manuscript Br J Ophthalmol. Author manuscript; available in PMC 2010 April 29.
 NIH Public Access Author Manuscript Published in final edited form as: Br J Ophthalmol. 2009 August ; 93(8): 1057 1063. doi:10.1136/bjo.2009.157875. Retinal nerve fibre layer thickness measurement reproducibility
NIH Public Access Author Manuscript Published in final edited form as: Br J Ophthalmol. 2009 August ; 93(8): 1057 1063. doi:10.1136/bjo.2009.157875. Retinal nerve fibre layer thickness measurement reproducibility
Optic Disk Pit with Sudden Central Visual Field Scotoma
 Optic Disk Pit with Sudden Central Visual Field Scotoma The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version
Optic Disk Pit with Sudden Central Visual Field Scotoma The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version
Unlike other cranial nerves, the optic nerve (ON) is surrounded
 Clinical and Epidemiologic Research Imaging Retrobulbar Subarachnoid Space around Optic Nerve by Swept-Source Optical Coherence Tomography in Eyes with Pathologic Myopia Kyoko Ohno-Matsui, 1 Masahiro Akiba,
Clinical and Epidemiologic Research Imaging Retrobulbar Subarachnoid Space around Optic Nerve by Swept-Source Optical Coherence Tomography in Eyes with Pathologic Myopia Kyoko Ohno-Matsui, 1 Masahiro Akiba,
Reproducibility of Bruch Membrane Opening-Minimum Rim Width Measurements With Spectral Domain Optical Coherence Tomography
 ORIGINAL STUDY Reproducibility of Bruch Membrane Opening-Minimum Rim Width Measurements With Spectral Domain Optical Coherence Tomography Keunheung Park, MD,* Jinmi Kim, PhD, and Jiwoong Lee, MD, PhD*
ORIGINAL STUDY Reproducibility of Bruch Membrane Opening-Minimum Rim Width Measurements With Spectral Domain Optical Coherence Tomography Keunheung Park, MD,* Jinmi Kim, PhD, and Jiwoong Lee, MD, PhD*
Ability of Scanning Laser Polarimetry (GDx) to Discriminate among Early Glaucomatous, Ocular Hypertensive and Normal Eyes in the Korean Population
 Korean J Ophthalmol Vol. 18:1-8, 2004 Ability of Scanning Laser Polarimetry (GDx) to Discriminate among Early Glaucomatous, Ocular Hypertensive and Normal Eyes in the Korean Population Sun Young Lee, MD,
Korean J Ophthalmol Vol. 18:1-8, 2004 Ability of Scanning Laser Polarimetry (GDx) to Discriminate among Early Glaucomatous, Ocular Hypertensive and Normal Eyes in the Korean Population Sun Young Lee, MD,
Macular Thickness Assessment in Patients with Glaucoma
 JOCGP Original Article Macular Thickness Assessment in Patients with Glaucoma 10.5005/jp-journals-10008-1207 and Its Correlation with Visual Fields Macular Thickness Assessment in Patients with Glaucoma
JOCGP Original Article Macular Thickness Assessment in Patients with Glaucoma 10.5005/jp-journals-10008-1207 and Its Correlation with Visual Fields Macular Thickness Assessment in Patients with Glaucoma
From the Massachusetts Eye and Ear Infirmary, Glaucoma Service, Harvard Medical School, Department of Ophthalmology, Boston, Massachusetts.
 SPECTRAL DOMAIN OPTICAL COHERENCE TOMOGRAPHY IN GLAUCOMA: QUALITATIVE AND QUANTITATIVE ANALYSIS OF THE OPTIC NERVE HEAD AND RETINAL NERVE FIBER LAYER (AN AOS THESIS) BY Teresa C. Chen MD ABSTRACT Purpose:
SPECTRAL DOMAIN OPTICAL COHERENCE TOMOGRAPHY IN GLAUCOMA: QUALITATIVE AND QUANTITATIVE ANALYSIS OF THE OPTIC NERVE HEAD AND RETINAL NERVE FIBER LAYER (AN AOS THESIS) BY Teresa C. Chen MD ABSTRACT Purpose:
This study was limited to those discs in which all 3 THE CRESCENT
 British Journal of Ophthalmology, 1978, 62, 16-20 The tilted disc DAVID DORRELL From the Department of Neuro-Ophthalmology, National Hospitals for Nervous Diseases, Queen Square, London SUMMARY Sixty tilted
British Journal of Ophthalmology, 1978, 62, 16-20 The tilted disc DAVID DORRELL From the Department of Neuro-Ophthalmology, National Hospitals for Nervous Diseases, Queen Square, London SUMMARY Sixty tilted
