The new WHO 2016 classification of brain tumors what neurosurgeons need to know
|
|
|
- Hilary Simpson
- 5 years ago
- Views:
Transcription
1 DOI /s REVIEW ARTICLE - BRAIN TUMORS The new WHO 2016 classification of brain tumors what neurosurgeons need to know Rouzbeh Banan 1 & Christian Hartmann 1 Received: 8 July 2016 /Accepted: 21 December 2016 # Springer-Verlag Wien 2017 Abstract Background The understanding of molecular alterations of tumors has severely changed the concept of classification in all fields of pathology. The availability of high-throughput technologies such as next-generation sequencing allows for a much more precise definition of tumor entities. Also in the field of brain tumors a dramatic increase of knowledge has occurred over the last years partially calling into question the purely morphologically based concepts that were used as exclusive defining criteria in the WHO 2007 classification. Methods Review of the WHO 2016 classification of brain tumors as well as a search and review of publications in the literature relevant for brain tumor classification from 2007 up to now. Results The idea of incorporating the molecular features in classifying tumors of the central nervous system led the authors of the new WHO 2016 classification to encounter inevitable conceptual problems, particularly with respect to linking morphology to molecular alterations. As a solution they introduced the concept of a layered diagnosis to the classification of brain tumors that still allows at a lower level a purely morphologically based diagnosis while partially forcing the incorporation of molecular characteristics for an integrated diagnosis at the highest diagnostic level. In this context the broad availability of molecular assays was debated. On the one hand molecular antibodies specifically targeting mutated proteins should be available in nearly all neuropathological laboratories. On the other hand, different high-throughput assays are * Christian Hartmann hartmann.christian@mh-hannover.de; pathologie-neuropat.html 1 Department of Neuropathology, Institute of Pathology, Hannover Medical School (MHH), Carl-Neuberg-Str. 1, Hannover, Germany accessible only in few first-world neuropathological institutions. As examples oligodendrogliomas are now primarily defined by molecular characteristics since the required assays are generally established, whereas molecular grouping of ependymomas, found to clearly outperform morphologically based tumor interpretation, was rejected from inclusion in the WHO 2016 classification because the required assays are currently only established in a small number of institutions. Conclusion In summary, while neuropathologists have now encountered various challenges in the transitional phase from the previous WHO 2007 version to the new WHO 2016 classification of brain tumors, clinical neurooncologists now face many new diagnoses allowing a clearly improved understanding that could offer them more effective therapeutic opportunities in neurooncological treatment. The new WHO 2016 classification presumably presents the highest number of modifications since the initial WHO classification of 1979 and thereby forces all professionals in the field of neurooncology to intensively understand the new concepts. This review article aims to present the basic concepts of the new WHO 2016 brain tumor classification for neurosurgeons with a focus on neurooncology. Keywords Brain tumors. WHO. Classification. Neuropathology. Molecular pathology Introduction The first report about brain tumor classification was published by the pathologist Rudolf Virchow in 1863 [1]. The vast majority of currently used terms for tumor entities were introduced by Harvey Cushing and Percival Bailey in 1926 [2]. Furthermore, these authors presented the first theory about the potential relationship between the developing brain and different types of brain tumors. In 1949 a complete different concept for
2 classifying brain tumors was presented by James Watson Kernohan and colleagues [3]. They dramatically reduced the number of brain tumor entities and introduced the concept of tumor grading for the first time. The WHO-based classification of brain tumors was first published by Zülch and colleagues in 1979 [4], basically using the terminology from Cushing and Bailey and combining them with Kernohan s concept of grading. In 1988 an alternative brain tumor grading system was published by Catherine Daumas-Duport and Bernd Scheithauer, known as the St Anne-Mayo grading scheme, which reached a certain popularity in the following years [5]. A second edition of the WHO classification followed in 1993 [6], a third edition in 2000 [7] and a fourth edition was released in 2007 [8]. Since then a huge number of molecular results on brain tumors have been published, calling into question some fundamentals of the current concept of understanding such lesions. In the various preliminary discussions after the recent release of the WHO 2016 classification [9], some critical questions were debated such as arguments against the current model of WHO grading: the old Zülch concept of WHO grading was based on a grade assignment due to survival time after total resection without any additional treatment [4], whereas radioand/or chemotherapy are nowadays considered the standard therapeutic procedures in most malignant brain tumors, causing a significant limitation in availability of clinical data that would allow survival analysis according to Zülch s concept. Nevertheless, this general criticism of one of the fundamentals of brain tumor grading was not further touched upon. Also debated was the question of non-tissue-based information being incorporated in the upcoming WHO 2016 classification. In this context a proposal was discussed to define pilocytic astrocytomas based only on their known morphological characteristics under the microscope along with their common radiological features including contrast enhancement on MRI. However, the most important debate was on the subject of the integration of molecular pathology in the next WHO classification. A threefold question that arose was what should be done (1) if molecular testing is not possible, (2) if histology and genetics are not congruent (e.g., diffuse astrocytoma with 1p/19q co-deletion) or (3) if specific assays have to be defined (e.g., FISH for 1p/19qanalysis). Due to a prior successful application in hematopathology [10], David Louis proposed the incorporation of a layered diagnosis concept in brain tumor classification to combine histology with molecular pathology (Fig. 1)[11]. This concept was approved by the experts of the Haarlem consensus meeting [12] and was then applied to the revised fourth edition of the WHO brain tumor classification [9]: Layer 1 Layer 2 Layer 3 Layer 4 Integrated diagnosis Histological diagnosis WHO grade Molecular information a Integrated neuropathological Diagnosis: Oligodendroglioma WHO grade II IDH-mut 1p/19q-codel b Layer 2 Layer 3 Layer 4 Layer 1 integrated diagnosis Integrated neuropathological Diagnosis: Glioblastoma WHO grade IV IDH-wt WITHOUT MGMT promoter methyla on WITH EGFR amplifica on c Layer 2 Layer 3 Layer 4 Layer 1 integrated diagnosis Addi onal molecular features Integrated neuropathological Diagnosis: Large cell/anaplas c Medulloblastoma WHO grade IV SHH-ac vated & TP53-mut WITH MYC amplifica on Addi onal molecular features Layer 2 Layer 3 Layer 4 Layer 1 integrated diagnosis Medulloblastomas, histologically defined Layer 1 integrated diagnosis Medulloblastomas, gene cally defined Fig. 1 Different diagnostic layers according to the WHO 2016 classification of brain tumors [9]. A: Syntactical structure of the diagnostic phrase of an oligodendroglioma. B: Layered phrasing of a glioblastoma; note that MGMT and EGFR status is not part of the tumor terminology but additional genetic features. C: Medulloblastomas are an exception, as they can be genetically and histologically defined; in this sense there are two different layer 1s; again, the MYC status is an additional feature but not part of the terminology of the entity The concept of a layered diagnosis basically uses a top layer, the layer 1, for the final integrated diagnosis, which is applicable only if information of all lower layers is available. Layer 2 encompasses the histological classification (e.g., astrocytoma vs. oligodendroglioma), layer 3 the grading (e.g., WHO grade II vs. III) and layer 4 molecular characteristics (e.g., IDH-mut, 1p/19q-codel). In this pure concept of a layered diagnosis the responsible neuropathologist is allowed to generate a mere layer 2 and/or 3 diagnosis in case no molecular data are available and to indicate that this is not a full, integrated layer 1 diagnosis. As a next step, some general rules were defined. First, the rule molecular beats histology was stated. For instance, a layer 2-based astrocytic tumor with layer 4-related findings of IDH-mut and 1p/19q-codel is finally a layer 1 oligodendroglioma. Second, the term NOS ( not otherwise specified ) was introduced into the WHO brain tumorclassificationtobeusedincase(1)thematerialdoesnot allow testing (e.g., the DNA is degraded), (2) the local neuropathology laboratory is not able to perform the required assay
3 (for example, 1p/19q FISH analysis is not established) and (3) a specific entity is only defined by a specific molecular alteration that cannot be detected [e.g., a C19MC-negativ embryonal tumor with multilayered rosettes (ETMR), NOS]. The NOS rule, however, is now somehow diluting the pure concept of a layered diagnosis. The following years of WHO 2016 application will presumably show whether this particular exception will be frequently be used and whether the NOS diagnosis will appear more often than initially expected by the WHO authors. The main argument against the inclusion of molecular markers into a WHO tumor classification has always been the question of availability of such advanced and expensive assays in a broad sense even in underdeveloped countries. However, the WHO classification of lymphomas and leukemia has already demonstrated the possibility of applying the WHO-defined molecular markers into the definitions of tumor entities, which has widely been accepted [10]. The experts of the revised fourth edition of the WHO brain tumor classification discussed and finally approved some standards and rules for molecular testing. First, they did not define any specific assay for molecular tests. For example, it is allowed to perform 1p/19q analysis through FISH, LOH marker, arraycgh or other locally available technologies. Second, they predominantly tried to define molecular entities especially when molecular or surrogate antibodies are accessible in order to avoid DNA-based assays (e.g., antibodies detecting mutated H3.3 K27M protein as a surrogate marker for an underlying H3F3A K27M mutation). By this approach the number of molecular assays for the WHO 2016-based brain tumor classification is rather low. In the following, modifications and new entities of tumors listed in the WHO 2016 classification will be presented. At the beginning of each chapter the terms of the entities and variants are listed. New or modified entities and variants are written in italics. Diffusely infiltrating gliomas This group of brain tumors consists of diffusely infiltrating astrocytomas, oligodendrogliomas and glioblastomas. As a new entity diffuse gliomas of the midline with H3 K27M mutation were also added to this group (see below). Finding different important molecular characteristics have since the publication of the last WHO classification in 2007 strongly improved the genetically based understanding of these tumors. Especially the recognition of IDH1 and IDH2 mutation in high frequencies in diffusely infiltrating astrocytomas and oligodendrogliomas and in a small fraction of glioblastomas [13, 14] significantly influenced the concepts of such tumors and thereby led to a re-definition of these entities in the current WHO classification [9]. Over the last years and particularly with the TCGA data [15, 16], it became evident that supratentorial diffusely infiltrating gliomas can genetically and prognostically be separated into at least three basic groups: (1) gliomas with IDH mutation (IDH-mut) and 1p/ 19q co-deletion (1p/19q-codel), strongly overlapping with the histological pattern of oligodendrogliomas, (2) gliomas with IDH-mut without 1p/19q-codel, strongly overlapping with tumors of an astrocytic phenotype and (3) gliomas with an IDH wildtype (IDH-wt) status, often encompassing typical glioblastomas (GBM). Oligodendrogliomas Oligodendroglioma WHO grade II, IDH-mut and 1p/ 19q-codel Oligodendroglioma WHO grade II, NOS Anaplastic oligodendroglioma WHO grade III, IDH-mut and 1p/19q-codel Anaplastic oligodendroglioma WHO grade III, NOS Oligoastrocytoma WHO grade II, NOS Anaplastic oligoastrocytoma WHO grade III, NOS According to the new WHO 2016 classification of brain tumors, oligodendrogliomas are genetically defined as diffusely infiltrating gliomas with IDH mutation and 1p/19q co-deletion. They strongly overlap with those tumors from the WHO 2007 classification that were formally and according to histology termed oligodendrogliomas, while also now encompassing tumors with an astrocytoma-like phenotype provided that the genetic IDH-mut and 1p/19q-codel profile has been established. For oligodendrogliomas it is now required to determine the IDH status by sequencing the genes IDH1 and IDH2 in case the tumor does not express mutated IDH1 R132H protein. Oligodendroglial tumors NOS are defined by the failure or impossibility of determining the IDH and/or 1p/19q status. The WHO 2016 experts acknowledge that there are presumably pediatric diffusely infiltrating oligodendrogliomas without an IDH-mut 1p/19q-codel status. However, they were not certain enough to open up this new entity, variant or pattern and emphasized histological overlaps with other entities showing a clear cell morphology for differential diagnostic considerations. If such alternative entities are excluded no WHO-compliant assignment is offered for pediatric-type oligodendrogliomas. It might be appropriate to term such extremely rare tumors oligodendroglioma, NOS. Nevertheless, such an assignment is not in line with the concept of using the phrase NOS, which should actually be applied only in case IDH and 1p/19q analyses cannot be performed or are inconclusive. The WHO 2016 classification strongly recommends avoiding issuing the diagnosis oligoastrocytoma, since such tumors are now considered as either oligodendrogliomas IDH-mut 1p/19q-codel or
4 astrocytomas IDH-mut. In fact, tumors with microscopic evidence of both an astrocytic and an oligodendroglial component are still allowed to be diagnosed as oligoastrocytoma NOS exclusively in case of failure or impossibility to determine the IDH and/or 1p/19q status. The WHO experts acknowledged reports of single cases indicating true oligoastrocytomas with dual genotype carrying 1p/19q losses in areas with oligodendroglial morphology and such molecular alterations as loss of ATRX expression or strong p53 expression in astrocytic regions [17 20]. Commenting on potential technical drawbacks and the very low number of reported cases, the WHO experts, however, refused to define tumors with such a dual genotype as entity or variant. Genetically oligodendrogliomas carry IDH and TERT mutations in all tumor cells and show combined 1p/19q losses. TERT mutations occur in high frequencies in oligodendrogliomas and ordinary glioblastomas, but not in diffusely infiltrating astrocytomas [21]. However, the WHO experts refused to alternatively define oligodendrogliomas by the combined presence of an IDH-mut and TERT-mut status because of currently insufficient evidence for this alternative approach. However, in the meantime it was demonstrated that patients with diffuse gliomas having an IDH-mut 1p/19q-codel status have indeed a similar prognosis to those with an IDH-mut TERT-mut status [22]. Around 60% of oligodendrogliomas furthermore carry CIC and in approximately 20% FUBP1 and 20% Notch1/2 mutations [23, 24]. Presumably, even various mutations in these genes occur in different tumor locations [16]. Among these at least CIC mutations might be a progression-associated event linked to a poorer prognosis in patients with oligodendrogliomas [25]. An unsolved issue regarding oligodendrogliomas is the prognostic relevance of their grading. After IDH-mut stratification three retrospective studies failed to observe a significant difference in survival between patients with oligodendroglioma WHO grade II and those with anaplastic oligodendrogliomas WHO grade III [16, 26, 27]. Supporting this notion, the TCGA data allowed no identification of genetic signatures that only showed up in anaplastic oligodendrogliomas, thereby also calling into question the histology-driven concept of grading [15]. However, due to the lack of prospective trials this grading issue was only mentioned but not applied for fusing grade II and III oligodendrogliomas in the current WHO brain tumor classification. Diffusely infiltrating astrocytomas Diffuse astrocytoma WHO grade II, IDH-mutant Gemistocytic astrocytoma WHO grade II, IDH-mut Diffuse astrocytoma WHO grade II, IDH-wt Diffuse astrocytoma WHO grade II, NOS Anaplastic astrocytoma WHO grade III, IDH-mut Anaplastic astrocytoma WHO grade III, IDH-wt Anaplastic astrocytoma WHO grade III, NOS Also diffusely infiltrating astrocytomas are genetically defined by the presence (most cases) or absence of IDH mutations. However, compared to oligodendrogliomas, an astrocytic phenotype is still required for the diagnosis. Similar to oligodendrogliomas, IDH1 and IDH2 sequencing has to be performed if IDH1 R132H immunohistochemistry is negative, and the designation NOS is only allowed in case the determination of the IDH status is not possible. Compared to oligodendrogliomas, a significant fraction of diffusely infiltrating astrocytomas do not carry an IDH mutation. The vast majority of anaplastic astrocytomas WHO grade III IDH-wt demonstrate the genetic profile of GBM, and the patients have a poorer prognosis than those with a GBM, IDH-mut [28]. The biologic characteristics of diffuse astrocytoma WHO grade II, IDH-wt currently remain unclear. Presumably there is no prognostic difference between patients with astrocytoma WHO grade II, IDH-mut and those with astrocytoma WHO grade II, IDH-wt [29]. Furthermore, the group of astrocytoma WHO grade II, IDH-wt comprises a mixed bag of various other tumor entities [30] that may even include some kind of diffusely infiltrating pilocytic astrocytomas [31]. In the WHO 2007 classification diffuse grade II astrocytomas were classified in fibrillary, protoplasmatic and gemistocytic subtypes [8], whereas in the WHO 2016 classification the fibrillary and protoplasmatic astrocytomas are combined and termed as diffuse astrocytomas after many arguments indicated that these two subtypes are basically the same entity. Genetically, the classic diffusely infiltrating astrocytoma IDH-mut shows in addition in nearly all cases TP53 alterations (mainly mutations) as well as, in a large fraction, ATRX mutations [15, 16]. Regarding the prognostic significance of grading the astrocytomas and, similar to what was mentioned in oligodendrogliomas with IDH-mut status, a loss of this significance has also been reported in astrocytomas after IDH stratification [16, 26, 32, 33]. In addition, no specific genetic signature could predominantly be found in WHO grade II or III astrocytomas by analyzing the TCGA results either [15]. Interestingly, no difference in age was found between patients with astrocytomas WHO grade II, IDHmut and those with anaplastic astrocytomas WHO grade III, IDH-mut [33]. Owing to the fact that these studies were only based on retrospectively collected patients and due to the fact that another study was able to observe a significant effect of astrocytoma grading after IDH stratification [34], the WHO expert group felt at this time it was not safe enough to skip this traditional, histology-based grading concept [9]. Glioblastomas Glioblastoma, IDH-wt Giant cell glioblastoma Gliosarcoma
5 Epithelioid glioblastoma Glioblastoma, IDH-mut Glioblastoma, NOS In line with the other diffusely infiltrating gliomas listed above, glioblastomas (GBM) are now defined by their IDH status too (Fig. 2) [9]. Nevertheless, the IDH mutation frequency of de-novo occurring GBM is only around 5% [13]. Therefore, in case of IDH1 R132H IHC negativity further IDH1 and IDH2 sequencing is only recommended when (1) the patients are less than 55 years old and (2) there is a lowgrade lesion in the history of the patient. Other genetic and prognostically relevant features of GBM, for example, MGMT promoter methylation [35] or H3F3A G34 mutations [36], were not included in the new WHO edition. Some of the histological variants and patterns of GBM included in the WHO 2007 classification [8] have been replaced by certain other types now: The pattern glioblastoma with oligodendroglioma features is now removed from the currently released WHO classification because of a large number of different reports indicating that the definition criteria were too imprecise. For example, the reported frequency of 1p/19q codel ranged from 3% [37] to 30% [38] in glioblastoma with oligodendroglioma features showed a varying overlap with anaplastic oligodendroglioma. As a new variant, the epithelioid glioblastoma and, as new patterns, the adenoid, granular cell, metaplastic, heavily lipidized glioblastoma and glioblastoma with a primitive neuronal component have now been included (Fig. 3). The latter GBM differentiation pattern often occurs as some kind of final morphological de-differentiation of IDH-mut tumors. Epithelioid or rhabdoid glioblastomas carry BRAF V600E mutations in approximately 50% of the cases [39, 40], and no criterion was listed allowing a separation of this glioblastoma variant from anaplastic pleomorphic xanthoastrocytomas WHO grade III (see below). Therefore, it remains a subjective issue for the neuropathologists to assign either a WHO grade III or a grade IV to these rare tumors, in fact causing a new form of imprecise GBM definition, which seemed to disappear after removing the unhappy diagnosis of glioblastomas with oligodendroglioma features. Diffuse midline glioma, H3 K27M-mut Diffuse midline glioma, H3 K27M-mut As a complete new entity, the diffuse midline glioma WHO grade IV, H3 K27M-mut has been established in the new WHO 2016 classification [9]. This entity is molecularly defined through K27M mutations in the genes encoding the histones H3.3 (H3F3A), H3.1 (HIST1H3B) andh3.2 (HIST1H3C) in the context of a diffusely infiltrating glioma with a predominately astrocytic differentiation. Around 80% Juvenile GBM H3F3A G34R/V Adult GBM IDH-mut IDH1/2 ATRX TP53 Adult GBM IDH-wt EGFR & Chr.10 TERT PTEN CDKN2A Age Diffuse midline glioma WHO grade IV: H3F3A K27M TP53 ATRX DAXX Fig. 2 Location and age distribution of different GBM subgroups. Diffuse midline gliomas WHO grade IV with H3 K27M mutations only occur in midline structures ranging from the diencephalon to the spinal cord and typically involve children and young adults. All other genetic GBM subgroups are mainly found in the telencephalic hemispheres. While GBM with H3F3A G34R/V mutations are mostly observed in young adults, GBM IDH-mut lesions are commonly seen in middleaged patients. The vast majority of these tumors are GBM-wt with frequent EGFR amplification, and chromosome 10 losses have a peak incidence around 60 years of age
6 a b information is available that would allow a statement if patients with such tumors have a clinical course similar to the histological or genetic profile. It needs to be shown if all brain tumors with a H3F3A K27M mutation always demonstrate a malignant course or if this genetic alteration is not per se indicative of malignancy. In the same gene, H3F3A, however not at position K27 but at G34, mutations occur in a different variant of malignant gliomas that morphologically appear as GBM or as PNET. These gliomas with H3F3A G34R/V mutations are located in the telencephalic hemispheres (Fig. 2), and patients with such lesions seem to present a clinical course between those with glioblastoma, IDH-wt and glioblastoma, IDH-mut [36]. However, for the time being, the WHO experts did not feel secure enough to establish a new diffusely infiltrating glioma entity based on H3F3A G34R/V mutations. c d Other astrocytomas Pilocytic astrocytoma WHO grade I Pilomyxoid astrocytoma Subependymal giant cell astrocytoma WHO grade I Pleomorphic xanthoastrocytoma WHO grade II Anaplastic pleomorphic xanthoastrocytoma WHO grade III e Fig. 3 Morphological examples of newly defined groups: (a) IDH1 R132H immunhistochemistry staining of a diffuse astrocytoma grade II IDH-mut; (b) glioblastoma grade IV with an adenoid pattern; (c) the variant of epithelioid/rhabdoid glioblastoma grade IV; (d) glioblastoma grade IV with a primitive neuronal component; (e) glioblastoma grade IV with a granular cell pattern; (e) diffuse leptomeningeal glioneuronal tumor WHO grade I (DLGNT) of these tumors carry H3F3A and 20% HIST1H3B mutations. HIST1H3C mutations occur in extremely rare cases [41]. According to the rule molecular pathology beats histopathology, the detection of H3 mutations outperforms the morphological appearance of these tumors, which could even indicate a low-grade lesion [42], and enforces an assignment of WHO grade IV. Diffuse midline gliomas, H3 K27Mmut grow in all midline CNS compartments starting from the diencephalon ranging down to the spinal cord (Fig. 2). An antibody against mutated H3.3 K27M protein is available [43], so that genetic testing is only required for HIST1H3B mutations. Not discussed by the expert group of the WHO 2016 classification are a few reported cases of patients with tumors having the morphological appearance of pilocytic astrocytomas, diffuse low-grade gliomas, low-grade ganglioglioma and ependymomas WHO grade II and a H3F3A K27M mutation [44 47]. Currently, only partial f In the former classification of 2007, WHO grade II was assigned to pilomyxoid astrocytomas [8]. In the years after this classification, however, it became clear that pilomyxoid astrocytomas share the same genetic features as pilocytic astrocytomas. Furthermore, reports of multiple resections of pilocytic/pilomyxoid astrocytomas indicated that pilocytic and pilomyxoid features are not stable over the course of the disease. Instead, the morphological feature shifts from one variant to the other and back [48]. Therefore, for the new classification the WHO experts decided not to assign a particular grade to pilomyxoid astrocytomas anymore [9]. As a new entity, anaplastic pleomorphic xanthoastrocytomas WHO grade III (PXA III) have been included in the new WHO 2016 classification [9]. They are defined as pleomorphic xanthoastrocytoma WHO grade II (PXA II) but exhibit five or more mitotic figures in ten high power fields. As the biological significance of necrosis is unclear, it is not considered further. BRAF V600E mutations in PXA III occur in a lower frequency than in PXA II [49, 50]. Patients with PXA III have a poorer survival rate than patients with PXA II but a longer overall survival rate than those with ordinary GBM [49]. However, no criteria are given by the WHO 2016 classification that would allow a differentiation between PXA III and rhabdoid GBM WHO grade IV (see above). A third modification was the elimination of the gliomatosis cerebri entity. This was due to reports showing that the genetic
7 profile of gliomatosis cerebri tumors was identical to other diffusely infiltrating gliomas [51]. However, others had not been able to identify similar findings and had proposed that gliomatosis cerebri is indeed an individual entity of diffusely infiltrating brain tumors [52]. In summary, gliomatosis cerebri is currently understood as an ordinary diffusely infiltrating glioma affecting at least three lobes. Ependymomomas Subependymoma WHO grade I Myxopapillary ependymoma WHO grade I Ependymoma WHO grade II Papillary ependymoma WHO grade II Clear cell ependymoma WHO grade II Tanycytic ependymoma WHO grade II Ependymoma, RELA fusion-positive WHO grade II Anaplastic ependymoma WHO grade III Anaplastic ependymoma, RELA fusion-positive WHO grade III Only few modifications regarding ependymomas have been added to the WHO 2007 classification [8] in the new WHO 2016 blue book [9]. This is of interest, as different studies have demonstrated a limited value of the established histology-based criteria for classification and grading especially regarding pediatric ependymomas of the posterior fossa [53, 54]. Over the past years a molecular classification has been established as an alternative defining group A with a poorer and group B with a better prognosis for pediatric ependymomas of the posterior fossa [55]. Concerning the supratentorial ependymomas, the prognostically poorer RELA-fused ependymomas and prognostically better YAP1- fused ependymomas have been identified [56]. However, simple molecular markers and assays that would allow an identification of these subgroups aremissinginmostinstances. Therefore, the WHO experts nearly decided not to modify the previous classification and grading of ependymomas, acknowledging the established limitations of the current concepts. The only newly genetically defined entity is the supratentorial ependymoma with RELA fusion comprising the majority of pediatric ependymomas and, in a smaller fraction, also those tumors of adult patients at this particular location. The molecular mechanism is a fusion of the RELA gene encoding an important effector of NF-κB signaling to the C11orf95 gene, leading to activation of the NF-κB pathway [57]. RELA-fused ependymomas are graded in line with the criteria for the non-rela-fused tumors as WHO grade II and anaplastic WHO grade III tumors. The reason for defining this new entity of RELA-fused ependymomas is the availability of the molecular surrogate antibody L1CAM that shows a positive binding only in this type of ependymoma [57]. As a diagnostic alternative, a FISH break-apart probe can be applied to detect a RELA-C11orf95 fusion [57], but no commercial FISH probe is currently available. Neuronal and mixed neuronal-glial tumors Dysembryoplastic neuroepithelial tumor WHO grade I Gangliocytoma WHO grade I Ganglioglioma WHO grade I Anaplastic ganglioglioma WHO grade III Dysplastic cerebellar gangliocytoma (Lhermitte- Duclos) WHO grade I Desmoplastic Infantile astrocytoma and ganglioglioma WHO grade I Papillary glioneuronal tumor WHO grade I Rosette-forming glioneuronal tumor WHO grade I Diffuse leptomeningeal glioneuronal tumor WHO grade I Central neurocytoma WHO grade II Extraventricular neurocytoma WHO grade II Cerebellar liponeurocytoma WHO grade I Paraganglioma WHO grade I Only minor modifications were introduced in the category of neuronal and glioneuronal tumors. As the only new entity, diffuse leptomeningeal glioneuronal tumor WHO grade I (DLGNT) is now introduced. This tumor was formally termed diffuse oligodendroglial leptomeningeal tumor (DOLN) because of the fact that these lesions show oligodendroglioma-like tumor cells and grow mainly in the leptomeningeal space. However, DLGNT may also have solid areas. Due to the very frequent BRAF:KIAA1549 duplications and deletions, DLGNTs are presumably closely related to pilocytic astrocytomas. In addition, DLGNTs often carry 1p and, not that frequently, 19q deletions [58]. As a consequence, the differentiation between DLGNT and oligodendrogliomas may be challenging in case the IDH status is not determined, as DLGNTs do not exhibit such mutations. Currently, only smaller series of patients with DLGNT have been published. Since most patients showed a benign clinical course, DLGNTs have been assigned WHO grade I [9] but more malignant cases were reported as well [59]. Only minor modifications affect rosette-forming glioneuronal tumors WHO grade I (RGNT) and neurocytomas WHO II. Neurocytomas are now defined by the absence of IDH mutations. In case of RGNT, the attribute of the fourth ventricle has now been removed from the tumor name.
8 Embryonal tumors Medulloblastomas, genetically defined Medulloblastoma, WNT-activated WHO grade IV Medulloblastoma, SHH-activated and TP53-mut grade IV Medulloblastoma, SHH-activated and TP53-wt grade IV Medulloblastoma, non-wnt/non-shh grade IV Medulloblastoma, group 3 grade IV Medulloblastoma, group 4 grade IV Medulloblastomas, histologically defined Medulloblastoma, classic grade IV Medulloblastoma, desmoplastic/nodular grade IV Medulloblastoma with extensive nodularity grade IV Medulloblastoma, large cell/anaplastic grade IV Medulloblastoma, NOS grade IV Embryonal tumor with multilayered rosettes, C19MCaltered grade IV Embryonal tumor with multilayered rosettes, NOS grade IV Medulloepithelioma grade IV CNS neuroblastoma grade IV CNS ganglioneuroblastoma grade IV CNS embryonal tumor, NOS grade IV Atypical teratoid/rhabdoid tumor grade IV CNS embryonal tumor with rhabdoid features grade IV Similar to the group of diffusely infiltrating gliomas, the classification of embryonal tumors has dramatically changed between 2007 and 2016 in the WHO brain tumor classifications attempting to integrate molecular findings [8, 9]. The term CNS PNET has now been completely removed in the new classification. WHO grade IV is assigned to all embryonal tumors. Medulloblastomas (MB) are the most frequent embryonal tumor entities. Sufficient data have been published on the prognostic significance of morphological variants, showing that patients with desmoplastic or extensive nodularity MB variants have a better prognosis and those with large cell or anaplastic MB variants show a poorer clinical course [60 63]. Molecular classification using either the expression profiling or whole-genome methylation analysis has allowed classifying MB into four groups: WNT-activated, SHH-activated, group 3 and group 4 MB. These four groups have demonstrated a unique clinical course: patients with WNT-activated MB usually have low-risk tumors, patients with SHH-activated MB without TP53 mutations have standard-risk ones, and those with SHH-activated MB with TP53 mutations are classified in the high-risk group. The patients with group 3 and group 4 (with intact chromosome 11) MB are considered in the standard-risk group as well, while patients with group 4 MB with chromosome 11 losses have low-risk tumors. A certain overlap between histopathological variants and molecular groups were demonstrated: WNT-activated MBs usually have a classical phenotype, SHH-activated TP53-wt tumors often show a desmoplastic/extensive nodularity phenotype, and SHH-activated TP53-mut tumors frequently present a large cell/anaplastic appearance as well as group 3 MB [64, 65]. In this setting of two evidence-based risk stratification concepts (histopathology and molecularpathology), the WHO expert group decided to allow both strategies for classification medulloblastomas, genetically defined, and medulloblastomas, histologically defined and encourage neuropathologists to use both for each tumor. Regarding histology, four variants are now listed: classic, desmoplastic/nodular, extensive nodularity and large cell/anaplastic MB. The last variant was formerly defined as two different types, large cell MB and anaplastic MB [8]. However, in the new classification these two variants have been fused together, since both show large cell and anaplastic features in the same tumor. Regarding the genetic definition of MB three groups have now been defined by the WHO expert group: WNT-activated, SHH-activated and non-wnt/non-shh MB. The non-wnt/ non-shh group encompasses groups 3 and 4 mentioned above as variants and represents around 60% of all MBs. No diagnostic assay has been defined for the molecular classification of MB. However, the WHO expert group recommends expression profiling or methylation analysis, both of which allow identification of group 3 and 4 tumors. However, conventional assays enabling the differentiation of these two groups are not broadly available. Based on the limited availability of these high-throughput platforms in most neuropathological institutions, a set of three surrogate antibodies has been proposed for molecular classification: nuclear β-catenin+, GAB1, YAP1+ for WNT-activated MB; nuclear β-catenin, GAB1+, YAP1+ for SHH-activated MB; nuclear β- catenin, GAB1, YAP1 for non-wnt/non-shh MB (Fig.4)[66]. In case neither a histological nor a genetical classification can be established, the tumor should be assigned the diagnosis of medulloblastoma, NOS. MYC amplification is another molecular marker linked to poorer prognosis in MB [67], which is recommended to be determined despite not being included in the 2016 WHO version as a classification criterion of MB. Atypical teratoid/rhabdoid tumors (AT/RT) WHO grade IV are also now genetically defined lesions. Already in the WHO 2007 classification loss of INI1 expression due to a mutation in the corresponding SMARCB1 gene or loss of thegenelocuswasnotedtobeaspecificmarkerevenfor those tumors not presenting the typical histological features of an AT/RT [8]. In the meantime, it became clear that those cases of AT/RT without loss of INI1 expression show loss of BRG1 expression. This protein is encoded by the SMARCA4 gene [68]. In this context the WHO expert group defined AT/RT as tumors with loss of INI1 (very frequent)
9 Fig. 4 Genetic-based classification of medulloblastomas through surrogate markers according to the WHO 2016 classification of brain tumors [9]. Basically, the expression pattern of three antibodies (β-catenin, GAB1, YAP1) allows differentiating subgroups of WNT-activated, SHH-activated and non-wnt, non-shh-activated. In case of SHH-activated medulloblastomas sequencing of the TP53 gene is recommended Nuclear β-catenin GAB1 YAP1 pos neg pos Medulloblastoma, WNT-activated CTNNB1 exon 6-mut Medulloblastoma Nuclear β-catenin neg GAB1 pos YAP1 pos - TP53 + Nuclear β-catenin GAB1 YAP1 neg neg neg Medulloblastoma, Non-WNT/Non-SHH-activated Medulloblastoma, SHH-activated, TP53-wt Medulloblastoma, SHH-activated, TP53-mut or BRG1 (very rare) [9]. The typical histopathological pattern of AT/RT is no longer required for those diagnoses in case of INI1/BRG1 loss [69]. Instead, those tumors that demonstrate typical histologically features of AT/RT but express INI1 and BRG1 are now termed CNS embryonal tumorwithrhabdoidfeaturesgradeiv[9]. Very recently, a study was published indicating three sub-variants of AT/RT with differences in the demographics, tumor location and type of SMARCB1 alterations [70]. However, these results were released after the finalization of the WHO 2016 classification; therefore, they can only be considered in the next WHO classification. A new entity that is also molecularly defined is the embryonal tumor with multilayered rosettes, C19MC-altered grade IV (ETMR) in the new WHO 2016 classification [9]. These tumors have a typical amplification of the C19MC region encoding a microrna cluster on 19q13.42 and include the former entities ependymoblastoma and, partially, medulloepithelioma [71 73]. In the literature, ETMRs were also termed embryonal tumors with abundant neuropil and true rosette (ETANTR) because of the histological features of papillary-like and tubular structures that presumably resemble the primitive neuronal tube [71, 74]. ETMRs typically occur in children below the age of 4, grow in supra- as well as infratentorial locations and have a malignant clinical course. Amplification of the C19MC region can be detected by array CGH or FISH, for example. However, the diagnosis can be issued only by a limited number of specialized neuropathological departments, as no commercial FISH probe is available. Strong expression of LIN28A was suggested as a potential molecular surrogate immunohistochemistry marker for ETMR. Nevertheless, LIN28A expression was also observed in gliomas, AT/RT, germ cell tumors and non-cns tumors, leading to a limitation of the value of this marker for the diagnosis of ETMR [73, 75, 76]. In case a tumor appears morphologically like an ETANTR or ependymoblastoma and also exhibits no C19MC amplification or the test cannot be performed, they should be named embryonal tumor with multilayered rosettes NOS. The group known as CNS embryonal tumors with a WHO grade IV assignment also encompasses the remaining former CNS PNET entities: medulloepithelioma, CNS neuroblastoma, CNS ganglioneuroblastoma and, as a new entity, the CNS embryonal tumor, NOS. The last entity is basically some kind of wastebasket for those poorly differentiated embryonal neoplasms with partial expression of GFAP and neuronal markers that fit neither morphologically nor genetically in any other embryonal entity. Tumors with the histological pattern of medulloepitheliomas but without C19MC amplification should not be termed ETMR, NOS (see above) because the expert group felt that this is indeed an independent entity. In summary, these other CNS embryonal tumors are types of tumors that are currently not completely understood. In this context, it is notable that a very recent large genetic high-throughput study was published on CNS PNET after the finalization of the WHO 2016 classification. In this study the authors reported on four different groups of CNS PNETlike tumors that at least allowed the allocation of CNS neuroblastomas and CNS ganglioneuroblastomas to a genetically defined entity [77]. Tumors of the peripheral nerves Schwannoma WHO grade I Cellular schwannoma WHO grade I Plexiform schwannoma WHO grade I Melanotic schwannoma Neurofibroma WHO grade I Atypical neurofibroma WHO grade I Plexiform neurofibroma WHO grade I
10 Perineurioma WHO grade I Hybrid nerve sheath tumor WHO grade I Malignant peripheral nerve sheath tumor Epithelioid MPNST MPNST with perineurial differentiation The former schwannoma variant melanotic schwannoma has now been assigned as an independent entity because of the results of previous studies that show that approximately 10% of patients with these lesion show a malignant clinical course [78]. In this context of potential malignancy, the melanotic schwannomas have not been assigned a WHO grade. Around 50% of patients with melanotic schwannoma and a psammomatous tumor differentiation have a Carney complex based on a mutation in the PRKAR1A gene. However, this genetic alteration has not been observed in patients with sporadic melanotic schwannomas [79]. Another new entity is hybrid nerve sheet tumors WHO grade I, which show a combined differentiation pattern of schwannomas, neurofibromas and perineuriomas. In the WHO 2007 classification, malignant peripheral nerve sheet tumors (MPNST) were listed with the WHO grades II, III and IV [8]. The former WHO grading criteria were based on the French Fédération Nationale des Centres de Lutte Contre le Cancer (FNCLCC) system [80]. However, due to the lack of available clinical studies on MPNST evaluating these grading criteria regarding the prognostication of a specific clinical course, the experts of the revised fourth edition have now removed MPSNT grading [9]. Instead, the experts have now proposed to separate these tumors in low- and highgrade MPNST [9] based on the recommendation that the first group of better differentiated MPNSTs arise in certain areas of neurofibromas [81]. This low-/high-grade strategy, however, is also not validated by clinical data, and it might be problematic to differentiate atypical neurofibromas WHO grade I from low-grade MPNST. In summary, the grading of MPNST is still an open issue with no satisfactory resolution. Meningiomas Meningothelial meningioma WHO grade I Fibrous meningioma WHO grade I Transitional meningioma WHO grade I Psammomatous meningioma WHO grade I Angiomatous meningioma WHO grade I Microcystic meningioma WHO grade I Secretory meningioma WHO grade I Lymphoplasmacyte-rich meningioma WHO grade I Metaplastic meningioma WHO grade I Chordoid meningioma WHO grade II Clear cell meningioma WHO grade II Atypical meningioma WHO grade II Papillary meningioma WHO grade III Rhabdoid meningioma WHO grade III Anaplastic (malignant) meningioma WHO grade III In the field of meningioma classification and grading, nearly nothing has changed except a now clearly given statement regarding the prognostic value of brain invasion of meningiomas. In the WHO 2007 classification brain invasion was not listed as a criterion for atypia in the corresponding grading paragraph. However, it was mentioned elsewhere in the chapter with the recommendation to shift even unsuspicious WHO grade I meningiomas to atypia in case of brain invasiveness [8]. This imprecise definition criterion for atypical meningiomas Fig. 5 The meningeal tumor cells enclosed by GFAP-stained reactive astrocytes of the surrounding CNS tissue representing brain invasion as a singular criterion of atypia in meningeal tumors
11 basically led to varying grading of these tumors depending on the local interpretation of the WHO 2007 classification. This issue has now been corrected by the WHO experts: brain invasion by meningioma cells is now clearly defined as an exclusive criterion for atypical grading (Fig. 5)[9]. Conclusion In summary, the revised fourth edition of the WHO classification of tumors of the CNS is a big step forward for pediatric and adult neurooncology. Predominately, the inclusion of molecular information now permits a more precise classification of brain tumors. This in turn allows better clinical trials as the patient cohorts are better defined; therefore, the effects of new therapeutic options can be grasped more safely. On the other hand, the molecular definition of tumors also calls into question some general and somehow traditional concepts in neurooncology. For example, the loss of prognostic significance in grading of astrocytomas and oligodendrogliomas [16, 26, 27, 32, 33] will presumably have a severe effect on the design of upcoming trials. However, the molecular definitions of diffuse gliomas and embryonal tumors will raise the question of how data from older clinical trials can be applied to the newly defined entities. However, it must be kept in mind that the modified classification itself is not responsible for such issues. Instead, the growing, especially genetic knowledge of brain tumors is the actual challenge for interpretation of such older trials. Between the WHO 2007 and the 2016 classification an extreme increase of knowledge regarding genetic features of brain tumors has become evident. However, (1) some entities still miss a better genetically driven classification concept, whereas (2) for other entities a powerful genetic classification is available but simple assays are missing, (3) important data of other entities have already been published since the finalization of the WHO 2016 classification, and (4) in many instances we now have good genetic markers for classification but still lack genetic markers that would improve grading. For example, meningiomas are still an entity lacking a more general concept for understanding: over the last years other mutated genes such as TRAF7, KLF4, SMO and ACT1 in addition to NF2 have been described and allocated to specific meningeal regions of occurrence and sometimes even to specific histological subvariants [82 85]. However, these results still do not allow a better classification of meningiomas. Ependymomas are a frustrating entity: a powerful genetic classification is available but currently requires molecular assays that are only available exclusively in some centers [55, 56]. Here we have to hope that simpler assays become available that can be utilized by standard-equipped neuropathology departments. Since the finalized WHO 2016 classification, data have been published allowing the separation of GBM with H3F3A G34 mutations as a unique entity [36], and also effective data already allow for a better classification of embryonal tumors that are currently not perfectly addressed by the WHO 2016 classification [77]. Hopefully the next edition of the WHO brain tumor classification will be able to deal with these currently unsolved issues and hopefully this edition will not first be published in the year Now we have to wait and see how the layered concept of brain tumor classification becomes adopted by all sides of the neurooncological community. Presumably each center will have certain start-up problems, and various complaints may arise because of the longer time required until an integrated, molecularly based diagnosis becomes finalized. In summary, however, the new WHO 2016 classification will be accepted as a big step forward for the treatment of brain tumor patients. Acknowledgements We would like to thank Sahar Marzieh Beheshti for editing and correcting the manuscript. References 1. Virchow R (1863) Die Krankhaften Geschwulste. Hirschwald Berlin 2. Bailey P, Cushing H (1926) A classification of tumors of the glioma group on a histogenetic basis with a correlation study of prognosis. Lippincott, Philadelphia 3. Kernohan JW, Mabon RF, Svien HJ, Adson AW (1949) A simplified classification of the gliomas. Symposium on a new simplified concept of gliomas. Mayo Clin Proc : Zülch KJ, Avtsyn AP, Barnar RO, Brucher JM, Earle KM, Fankhauser R, Ishida Y, Kunicki A, Olvera Rabiela JE, Rubinstein LJ, Sobin LH (1979) Histological typing of tumours of the central nervous system. Office of Publications, World Health Organization, Geneva Geneva 5. Daumas-Duport C, Scheithauer B, O Fallon J, Kelly P (1988) Grading of astrocytomas. A simple and reproducible method. Cancer 62: Kleihues P, Burger PC, Scheithauer BW (1993) Histological typing of tumours of the central nervous system. Springer Verlag Berlin, Heidelberg, New York 7. Kleihues P, Cavenee WK (2000) Pathology and genetics of tumours of the nervous system. IARC Press; International Agency for Research on Cancer, Lyon 8. Louis DN, International Agency for Research on Cancer (2007) WHO classification of tumours of the central nervous system. IARC Press; International Agency for Research on Cancer, Lyon 9. Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, Ellision DW, Figarella-Branger D, Reifenberger G, von Deimling A (2016) WHO classification and grading of tumours of the central nervous system. IARC Press; International Agency for Research on Cancer, Lyon 10. Swerdlow SH, Campo E, Harris NL, Jaffe ES, Pileri SA, Stein H, Thiele J, Vardiman JW (2008) WHO classification of tumours of haematopoietic and lymphoid tissues. IARC Press; International Agency for Research on Cancer, Lyon 11. Louis DN (2012) The next step in brain tumor classification: Let us now praise famous men or molecules? Acta Neuropathol 124:
WHO 2016 CNS Tumor Classification Update. DISCLOSURES (Arie Perry, MD) PATTERN RECOGNITION. Arie Perry, M.D. Director, Neuropathology
 WHO 2016 CNS Tumor Classification Update Arie Perry, M.D. Director, Neuropathology DISCLOSURES (Arie Perry, MD) I have no financial relationships to disclose. - and - I will not discuss off label use or
WHO 2016 CNS Tumor Classification Update Arie Perry, M.D. Director, Neuropathology DISCLOSURES (Arie Perry, MD) I have no financial relationships to disclose. - and - I will not discuss off label use or
Gliomas in the 2016 WHO Classification of CNS Tumors
 Gliomas in the 2016 WHO Classification of CNS Tumors Hindi N Al-Hindi, MD, FCAP Consultant Neuropathologist and Head Section of Anatomic Pathology Department of Pathology and Laboratory Medicine King Faisal
Gliomas in the 2016 WHO Classification of CNS Tumors Hindi N Al-Hindi, MD, FCAP Consultant Neuropathologist and Head Section of Anatomic Pathology Department of Pathology and Laboratory Medicine King Faisal
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
Neuropathology Evening Session: Case 3
 Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille
 Novelties in the WHO 2016 classification of brain tumours Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille The
Novelties in the WHO 2016 classification of brain tumours Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille The
WHO 2016 CNS TUMOR CLASSIFICATION UPDATE. Arie Perry, M.D. Director, Neuropathology
 WHO 2016 CNS TUMOR CLASSIFICATION UPDATE Arie Perry, M.D. Director, Neuropathology DISCLOSURES (Arie Perry, MD) I have no financial relationships to disclose. - and - I will not discuss off label use or
WHO 2016 CNS TUMOR CLASSIFICATION UPDATE Arie Perry, M.D. Director, Neuropathology DISCLOSURES (Arie Perry, MD) I have no financial relationships to disclose. - and - I will not discuss off label use or
Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls. Rob Macaulay Neuropathologist, MCC October 21, 2017
 Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls Rob Macaulay Neuropathologist, MCC October 21, 2017 Objectives Explain why the designation high grade glioma is preferable to GBM for intraoperative
Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls Rob Macaulay Neuropathologist, MCC October 21, 2017 Objectives Explain why the designation high grade glioma is preferable to GBM for intraoperative
Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS
 Multiple Primary and Histology Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways
Multiple Primary and Histology Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways
Tumours of the Central Nervous System (CNS) Molecular Information Reporting Guide
 Sponsored by Tumours of the Central Nervous System (CNS) Molecular Information Reporting Guide Family/Last name Given name(s) Date of birth DD MM YYYY Patient identifiers Date of request Accession/Laboratory
Sponsored by Tumours of the Central Nervous System (CNS) Molecular Information Reporting Guide Family/Last name Given name(s) Date of birth DD MM YYYY Patient identifiers Date of request Accession/Laboratory
Updates on the CNS classifica3on of brain tumors
 27 th Annual Mee-ng of the IAP-AD "New Horizons in Surgical Pathology Conrad Dubai, UAE Friday, 27 November 2015 Updates on the CNS classifica3on of brain tumors Eyas M Ha=ab, MD Department of Pathology
27 th Annual Mee-ng of the IAP-AD "New Horizons in Surgical Pathology Conrad Dubai, UAE Friday, 27 November 2015 Updates on the CNS classifica3on of brain tumors Eyas M Ha=ab, MD Department of Pathology
Disclaimers. Molecular pathology of brain tumors. Some aspects only. Some details are inevitably personal opinions
 Molecular pathology of brain tumors Disclaimers Some aspects only H.K. Ng The Chinese University of Hong Kong Some details are inevitably personal opinions Free ppt : http://www.acp.cuhk.edu.hk/hkng Why
Molecular pathology of brain tumors Disclaimers Some aspects only H.K. Ng The Chinese University of Hong Kong Some details are inevitably personal opinions Free ppt : http://www.acp.cuhk.edu.hk/hkng Why
The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas
 The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas Stefan Prokop, MD Neuropathology Fellow Hospital of the University of Pennsylvania Background
The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas Stefan Prokop, MD Neuropathology Fellow Hospital of the University of Pennsylvania Background
The 2016 WHO classification of central nervous system tumors: what neurologists need to know
 REVIEW C URRENT OPINION The 2016 WHO classification of central nervous system tumors: what neurologists need to know John C. DeWitt a,, Andreas Mock a,b,c,, and David N. Louis a Purpose of review The 2016
REVIEW C URRENT OPINION The 2016 WHO classification of central nervous system tumors: what neurologists need to know John C. DeWitt a,, Andreas Mock a,b,c,, and David N. Louis a Purpose of review The 2016
Childhood Brain and Spinal Cord Tumors Treatment Overview (PDQ )
 1 di 8 04/03/2017 07.31 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 8 04/03/2017 07.31 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Protocol for the Examination of Specimens From Patients With Tumors of the Central Nervous System*
 Protocol for the Examination of Specimens From Patients With Tumors of the Central Nervous System* Version: Protocol Posting Date: December 2014 This protocol is NOT required for accreditation purposes
Protocol for the Examination of Specimens From Patients With Tumors of the Central Nervous System* Version: Protocol Posting Date: December 2014 This protocol is NOT required for accreditation purposes
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad
 Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Applications of molecular neuro-oncology - a review of diffuse glioma integrated diagnosis and emerging molecular entities
 Wood et al. Diagnostic Pathology (2019) 14:29 https://doi.org/10.1186/s13000-019-0802-8 REVIEW Applications of molecular neuro-oncology - a review of diffuse glioma integrated diagnosis and emerging molecular
Wood et al. Diagnostic Pathology (2019) 14:29 https://doi.org/10.1186/s13000-019-0802-8 REVIEW Applications of molecular neuro-oncology - a review of diffuse glioma integrated diagnosis and emerging molecular
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
Histopathological Study and Categorisation of Brain Tumors
 Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Five Most Common Problems in Surgical Neuropathology
 Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
MOLECULAR DIAGNOSTICS OF GLIOMAS
 MOLECULAR DIAGNOSTICS OF GLIOMAS Arie Perry, M.D. Director, Neuropathology Division DIFFUSE GLIOMAS Cell types Astrocytomas (A) Oligodendrogliomas (O) Mixed oligoastrocytoma (MOA) Three WHO grades: II,
MOLECULAR DIAGNOSTICS OF GLIOMAS Arie Perry, M.D. Director, Neuropathology Division DIFFUSE GLIOMAS Cell types Astrocytomas (A) Oligodendrogliomas (O) Mixed oligoastrocytoma (MOA) Three WHO grades: II,
In 1988 Dumas-Duport et al. first used
 Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Case Presentation: USCAP Jason T. Huse, MD, PhD Assistant Member Department of Pathology Memorial Sloan Kettering Cancer Center
 Case Presentation: USCAP 2016 Jason T. Huse, MD, PhD Assistant Member Department of Pathology Memorial Sloan Kettering Cancer Center Case History 53 year old female with a long standing history of migraines
Case Presentation: USCAP 2016 Jason T. Huse, MD, PhD Assistant Member Department of Pathology Memorial Sloan Kettering Cancer Center Case History 53 year old female with a long standing history of migraines
Karl Kashofer, Phd Institut für Pathologie Medizinische Universität Graz
 Expanding on WHO guideline compliant molecular testing of central nervous system tumors by low density whole genome sequencing. Karl Kashofer, Phd Institut für Pathologie Medizinische Universität Graz
Expanding on WHO guideline compliant molecular testing of central nervous system tumors by low density whole genome sequencing. Karl Kashofer, Phd Institut für Pathologie Medizinische Universität Graz
2017 Diagnostic Slide Session Case 3
 2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
Effective January 1, 2018 ICD O 3 codes, behaviors and terms are site specific
 Effective January 1, 2018 codes, behaviors and terms are site specific /N 8551/3 Acinar adenocarcinoma (C34. _) Lung primaries diagnosed prior to 1/1/2018 use code 8550/3 For prostate (all years) see 8140/3
Effective January 1, 2018 codes, behaviors and terms are site specific /N 8551/3 Acinar adenocarcinoma (C34. _) Lung primaries diagnosed prior to 1/1/2018 use code 8550/3 For prostate (all years) see 8140/3
Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord
 Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord Protocol applies to all primary neoplasms of the brain/ spinal cord/peripheral nerve and pituitary. Metastatic
Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord Protocol applies to all primary neoplasms of the brain/ spinal cord/peripheral nerve and pituitary. Metastatic
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
2018 ICD-O-3 Updates in Table Format with Annotation for Reference
 Status Histology Description (this may be preferred term or a synonym) Report Comments New term 8010 3 Urachal carcinoma (C65.9, C66.9, C67._, C68._) New term 8013 3 Combined large cell neuroendocrine
Status Histology Description (this may be preferred term or a synonym) Report Comments New term 8010 3 Urachal carcinoma (C65.9, C66.9, C67._, C68._) New term 8013 3 Combined large cell neuroendocrine
Effective January 1, 2018 ICD O 3 codes, behaviors and terms are site specific
 Effective January 1, 2018 codes, behaviors and terms are site specific Status /N 8010/3 Urachal carcinoma (C65.9, C66.9, C67. _, C68._) 8013/3 Combined large cell neuroendocrine carcinoma (C34. _, C37.9)
Effective January 1, 2018 codes, behaviors and terms are site specific Status /N 8010/3 Urachal carcinoma (C65.9, C66.9, C67. _, C68._) 8013/3 Combined large cell neuroendocrine carcinoma (C34. _, C37.9)
Tumours of the Central Nervous System (CNS) Histological Assessment Reporting Guide
 Sponsored by Tumours of the Central Nervous System (CNS) Histological Assessment Reporting Guide Family/Last name Given name(s) Date of birth DD MM YYYY Patient identifiers Date of request Accession/Laboratory
Sponsored by Tumours of the Central Nervous System (CNS) Histological Assessment Reporting Guide Family/Last name Given name(s) Date of birth DD MM YYYY Patient identifiers Date of request Accession/Laboratory
I have no conflicts of interest in relation to this presentation. Vogel FS & Burger PC 3/28/2016
 IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
Diagnostic application of SNParrays to brain cancers
 Diagnostic application of SNParrays to brain cancers Adriana Olar 4/17/2018 No disclosures 55 yo M, focal motor seizure T2 T1-post C DIAGNOSIS BRAIN, LEFT FRONTAL LOBE, BIOPSY: - DIFFUSE GLIOMA, OLIGODENDROGLIAL
Diagnostic application of SNParrays to brain cancers Adriana Olar 4/17/2018 No disclosures 55 yo M, focal motor seizure T2 T1-post C DIAGNOSIS BRAIN, LEFT FRONTAL LOBE, BIOPSY: - DIFFUSE GLIOMA, OLIGODENDROGLIAL
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Genomic analysis of childhood High grade glial (HGG) brain tumors
 Genomic analysis of childhood High grade glial (HGG) brain tumors Linda D Cooley Children s Mercy, Kansas City The Children s Mercy Hospital, 2017 Genomic analysis of childhood High grade glial (HGG) brain
Genomic analysis of childhood High grade glial (HGG) brain tumors Linda D Cooley Children s Mercy, Kansas City The Children s Mercy Hospital, 2017 Genomic analysis of childhood High grade glial (HGG) brain
Morphological features and genetic alterations
 Morphological features and genetic alterations Tutor : Audrey Rousseau Caget Lise: Université d Angers Iorio Vittoria: Seconda Università degli studi di Napoli Manaila Roxana: Iuliu Hatieganu University
Morphological features and genetic alterations Tutor : Audrey Rousseau Caget Lise: Université d Angers Iorio Vittoria: Seconda Università degli studi di Napoli Manaila Roxana: Iuliu Hatieganu University
Molecular pathology of paediatric central nervous system tumours
 Journal of Pathology J Pathol 2017; 241: 159 172 Published online 10 November 2016 in Wiley Online Library (wileyonlinelibrary.com) DOI: 10.1002/path.4813 INVITED REVIEW Molecular pathology of paediatric
Journal of Pathology J Pathol 2017; 241: 159 172 Published online 10 November 2016 in Wiley Online Library (wileyonlinelibrary.com) DOI: 10.1002/path.4813 INVITED REVIEW Molecular pathology of paediatric
SUPPLEMENTARY INFORMATION
 VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
Supplementary Information
 Rise in Glioblastoma Multiforme incidence in England 1995 2015 suggests an adverse environmental or lifestyle factor Alasdair Philips, Denis L Henshaw, Graham Lamburn, Michael J O Carroll Supplementary
Rise in Glioblastoma Multiforme incidence in England 1995 2015 suggests an adverse environmental or lifestyle factor Alasdair Philips, Denis L Henshaw, Graham Lamburn, Michael J O Carroll Supplementary
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
H3F3A K27M Mutation in Pediatric CNS Tumors. A Marker for Diffuse High-Grade Astrocytomas
 Anatomic Pathology / H3.3 Mutations in Pediatric Diffuse High-Grade Astrocytomas H3F3A K27M Mutation in Pediatric CNS Tumors A Marker for Diffuse High-Grade Astrocytomas Gerrit H. Gielen, MD, 1 Marco Gessi,
Anatomic Pathology / H3.3 Mutations in Pediatric Diffuse High-Grade Astrocytomas H3F3A K27M Mutation in Pediatric CNS Tumors A Marker for Diffuse High-Grade Astrocytomas Gerrit H. Gielen, MD, 1 Marco Gessi,
2. Subependymal giant cell astrocytoma:
 I. Astrocytomas: A. Diffusely infiltrating ( astrocytoma, anaplastic astrocytoma, GBM) B. Localised (pilocytic astrocytoma, pleomorphic xanthoastrocytoma, SGCA) *Grading: Diffuse: 1. Astrocytoma WHO grade
I. Astrocytomas: A. Diffusely infiltrating ( astrocytoma, anaplastic astrocytoma, GBM) B. Localised (pilocytic astrocytoma, pleomorphic xanthoastrocytoma, SGCA) *Grading: Diffuse: 1. Astrocytoma WHO grade
Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord
 Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord Protocol applies to all primary neoplasms of the brain/spinal cord/peripheral nerve and pituitary. Metastatic
Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord Protocol applies to all primary neoplasms of the brain/spinal cord/peripheral nerve and pituitary. Metastatic
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
Understanding general brain tumor pathology, Part I: The basics. Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky
 Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES
 MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES DISCLOSURE No conflicts of interest to disclose Patricia Bruns APRN, CNS Givens Brain Tumor Center Abbott Northwestern Hospital October 12, 2018 OBJECTIVES THEN
MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES DISCLOSURE No conflicts of interest to disclose Patricia Bruns APRN, CNS Givens Brain Tumor Center Abbott Northwestern Hospital October 12, 2018 OBJECTIVES THEN
Enterprise Interest None
 Enterprise Interest None Heterogeneous chromosomal profiles in a unique series of DIPG in children and young adults European Congress of Pathology Amsterdam, 6 th September 2017 Charlotte Dufour, Romain
Enterprise Interest None Heterogeneous chromosomal profiles in a unique series of DIPG in children and young adults European Congress of Pathology Amsterdam, 6 th September 2017 Charlotte Dufour, Romain
Childhood Brain and Spinal Cord Tumors Treatment Overview (PDQ )
 1 di 14 27/11/2016 17.42 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 14 27/11/2016 17.42 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
Supra- and infratentorial brain tumors from childhood to maternity
 Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Case #3. USCAP Neuropathology Evening Seminar/Companion Meeting
 Case #3 USCAP Neuropathology Evening Seminar/Companion Meeting Clinical History A 71-year year-old man presented with a 4-4 week history of word finding difficulty. An initial screening head CT followed
Case #3 USCAP Neuropathology Evening Seminar/Companion Meeting Clinical History A 71-year year-old man presented with a 4-4 week history of word finding difficulty. An initial screening head CT followed
Review: Diagnostic, prognostic and predictive relevance of molecular markers in gliomas
 Review: Diagnostic, prognostic and predictive relevance of molecular markers in gliomas Sebastian Brandner MD FRCPath 1 and Andreas von Deimling 2 MD 1) Division of Neuropathology, The National Hospital
Review: Diagnostic, prognostic and predictive relevance of molecular markers in gliomas Sebastian Brandner MD FRCPath 1 and Andreas von Deimling 2 MD 1) Division of Neuropathology, The National Hospital
Molecular Testing of Brain Tumor
 Journal of Pathology and Translational Medicine 2017; 51: 205-223 REVIEW Molecular Testing of Brain Tumor Sung-Hye Park 1,2 Jaekyung Won 1 Seong-Ik Kim 1 Yujin Lee 1 Chul-Kee Park 3 Seung-Ki Kim 3 Seung-Hong
Journal of Pathology and Translational Medicine 2017; 51: 205-223 REVIEW Molecular Testing of Brain Tumor Sung-Hye Park 1,2 Jaekyung Won 1 Seong-Ik Kim 1 Yujin Lee 1 Chul-Kee Park 3 Seung-Ki Kim 3 Seung-Hong
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
The 2016 WHO Classification of Tumours of the Central Nervous System: The Major Points of Revision
 REVIEW ARTICLE doi: 10.2176/nmc.ra.2017-0010 Neurol Med Chir (Tokyo) xx, xxx xxx, xxxx The 2016 WHO Classification of Tumours of the Central Nervous System: The Major Points of Revision Takashi KOMORI
REVIEW ARTICLE doi: 10.2176/nmc.ra.2017-0010 Neurol Med Chir (Tokyo) xx, xxx xxx, xxxx The 2016 WHO Classification of Tumours of the Central Nervous System: The Major Points of Revision Takashi KOMORI
SYSTEMIC MANAGEMENT OF PEDIATRIC PRIMARY BRAIN TUMORS
 SYSTEMIC MANAGEMENT OF PEDIATRIC PRIMARY BRAIN TUMORS María E. Echevarría, MD Assistant Professor University of Puerto Rico Medical Sciences Campus DISCLOSURES No disclosures INTRODUCTION Pediatric CNS
SYSTEMIC MANAGEMENT OF PEDIATRIC PRIMARY BRAIN TUMORS María E. Echevarría, MD Assistant Professor University of Puerto Rico Medical Sciences Campus DISCLOSURES No disclosures INTRODUCTION Pediatric CNS
2 Berkeley Street, Suite 403, Toronto, Ontario M5A 2W3 Visit us at: Tel: Fax:
 E-Path A.I. Engine Knowledge Base Enhancements Version 1.0.0.29 April 1, 2018 The major enhancements in the E-Path Knowledge Base from versions 1.0.0.28 through 1.0.0.29 are as follows: 1. Addition/modification
E-Path A.I. Engine Knowledge Base Enhancements Version 1.0.0.29 April 1, 2018 The major enhancements in the E-Path Knowledge Base from versions 1.0.0.28 through 1.0.0.29 are as follows: 1. Addition/modification
Clinical significance of genetic analysis in glioblastoma treatment
 Clinical significance of genetic analysis in glioblastoma treatment Department of Neurosurgery, Graduate School of Medical Sciences, Kyushu University, Fukuoka, Japan Koji Yoshimoto Can we get prognostic
Clinical significance of genetic analysis in glioblastoma treatment Department of Neurosurgery, Graduate School of Medical Sciences, Kyushu University, Fukuoka, Japan Koji Yoshimoto Can we get prognostic
INDEX. B Bailey and Cushing astrocytoma grade, 9 beta-hcg, 114 blepharoplasts, 14, brainstem glioma, 11, 33
 INDEX A abscess, 125,166-168 vs. glioblastoma multi forme, 167 acquired immunodeficiency virus (AIDS) [see also human immunodeficiency virus (HIV)], 125-127, 158, 161 acoustic neuroma (see schwanomma)
INDEX A abscess, 125,166-168 vs. glioblastoma multi forme, 167 acquired immunodeficiency virus (AIDS) [see also human immunodeficiency virus (HIV)], 125-127, 158, 161 acoustic neuroma (see schwanomma)
The WHO Classification of Tumors of the Nervous System
 Journal of Neuropathology and Experimental Neurology Vol. 61, No. 3 Copyright 2002 by the American Association of Neuropathologists March, 2002 pp. 215 225 The WHO Classification of Tumors of the Nervous
Journal of Neuropathology and Experimental Neurology Vol. 61, No. 3 Copyright 2002 by the American Association of Neuropathologists March, 2002 pp. 215 225 The WHO Classification of Tumors of the Nervous
Examining large groups of cancer patients to identify ways of predicting which therapies cancers might respond to.
 Stratified Medicine Examining large groups of cancer patients to identify ways of predicting which therapies cancers might respond to. Looking in detail at cancer cells and their genetic make up. Permit
Stratified Medicine Examining large groups of cancer patients to identify ways of predicting which therapies cancers might respond to. Looking in detail at cancer cells and their genetic make up. Permit
A clinical perspective on neuropathology and molecular genetics in brain tumors
 A clinical perspective on neuropathology and molecular genetics in brain tumors M.J. van den Bent Erasmus MC Cancer Institute Rotterdam, the Netherlands Disclosures Member speakersbureau: MSD Consultancy:
A clinical perspective on neuropathology and molecular genetics in brain tumors M.J. van den Bent Erasmus MC Cancer Institute Rotterdam, the Netherlands Disclosures Member speakersbureau: MSD Consultancy:
Supplemental Information. Molecular, Pathological, Radiological, and Immune. Profiling of Non-brainstem Pediatric High-Grade
 Cancer Cell, Volume 33 Supplemental Information Molecular, Pathological, Radiological, and Immune Profiling of Non-brainstem Pediatric High-Grade Glioma from the HERBY Phase II Randomized Trial Alan Mackay,
Cancer Cell, Volume 33 Supplemental Information Molecular, Pathological, Radiological, and Immune Profiling of Non-brainstem Pediatric High-Grade Glioma from the HERBY Phase II Randomized Trial Alan Mackay,
Pleomorphic Xanthoastrocytoma
 Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Phase II Pediatric Study With Dabrafenib in Combination With Trametinib in Patients With HGG and LGG
 Find Studies About Studies Submit Studies Resources About Site Phase II Pediatric Study With Dabrafenib in Combination With Trametinib in Patients With HGG and LGG The safety and scientific validity of
Find Studies About Studies Submit Studies Resources About Site Phase II Pediatric Study With Dabrafenib in Combination With Trametinib in Patients With HGG and LGG The safety and scientific validity of
Genomic Analysis in the Practice of Surgical Neuropathology. The Emory Experience
 Genomic Analysis in the Practice of Surgical Neuropathology The Emory Experience Stewart G. Neill, MD; Debra F. Saxe, PhD; Michael R. Rossi, PhD; Matthew J. Schniederjan, MD; Daniel J. Brat, MD, PhD The
Genomic Analysis in the Practice of Surgical Neuropathology The Emory Experience Stewart G. Neill, MD; Debra F. Saxe, PhD; Michael R. Rossi, PhD; Matthew J. Schniederjan, MD; Daniel J. Brat, MD, PhD The
Histological pattern of central nervous system neoplasms
 ecommons@aku Department of Pathology and Laboratory Medicine Medical College, Pakistan April 2001 Histological pattern of central nervous system neoplasms Z. Ahmed Aga Khan University S. Muzaffar Aga Khan
ecommons@aku Department of Pathology and Laboratory Medicine Medical College, Pakistan April 2001 Histological pattern of central nervous system neoplasms Z. Ahmed Aga Khan University S. Muzaffar Aga Khan
Neuronal and Mixed Neuronal- Glial and Embryonal Tumors
 Neuronal and Mixed Neuronal- Glial and Embryonal Tumors Alexander R. Judkins, MD, FRCP (Edin) Pathologist-in-Chief Children s Hospital Los Angeles Associate Professor (Clinical Scholar) & Vice Chair Department
Neuronal and Mixed Neuronal- Glial and Embryonal Tumors Alexander R. Judkins, MD, FRCP (Edin) Pathologist-in-Chief Children s Hospital Los Angeles Associate Professor (Clinical Scholar) & Vice Chair Department
Cynthia Hawkins. Division of Pathology, Labatt Brain Tumour Research Centre, The Hospital for Sick Children, University of Toronto, Canada
 Cynthia Hawkins Division of Pathology, Labatt Brain Tumour Research Centre, The Hospital for Sick Children, University of Toronto, Canada To apply a practical diagnostic approach to pediatric high grade
Cynthia Hawkins Division of Pathology, Labatt Brain Tumour Research Centre, The Hospital for Sick Children, University of Toronto, Canada To apply a practical diagnostic approach to pediatric high grade
monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or
 monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or vacuolated cytoplasm. The cells are surrounded by a loose fibrillary stroma that is traversed by delicate capillaries. Ill
monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or vacuolated cytoplasm. The cells are surrounded by a loose fibrillary stroma that is traversed by delicate capillaries. Ill
Collecting Cancer Data: Central Nervous System Prizes! Question of the Month! Tip of the Month! Q&A
 Collecting Cancer Data: Central Nervous NAACCR 2008 2009 Webinar Series April 2, 2009 Prizes! Question of the Month! The participant that submits the best question of the session will receive a fbl fabulous
Collecting Cancer Data: Central Nervous NAACCR 2008 2009 Webinar Series April 2, 2009 Prizes! Question of the Month! The participant that submits the best question of the session will receive a fbl fabulous
Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child
 Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
NERVOUS SYSTEM. Cambridge Illustrated Surgical Pathology
 NERVOUS SYSTEM Cambridge Illustrated Surgical Pathology Nervous System is the new atlas-oriented resource in nervous system pathology. As the fourth book in the Cambridge Illustrated Surgical Pathology
NERVOUS SYSTEM Cambridge Illustrated Surgical Pathology Nervous System is the new atlas-oriented resource in nervous system pathology. As the fourth book in the Cambridge Illustrated Surgical Pathology
Embryonal tumor with multilayered rosettes, C19MC-altered: Report of an extremely rare malignant pediatric central nervous system neoplasm
 745208SCO0010.1177/2050313X17745208SAGE Open Medical Case ReportsTariq et al. case-report2017 Case Report SAGE Open Medical Case Reports Embryonal tumor with multilayered rosettes, C19MC-altered: Report
745208SCO0010.1177/2050313X17745208SAGE Open Medical Case ReportsTariq et al. case-report2017 Case Report SAGE Open Medical Case Reports Embryonal tumor with multilayered rosettes, C19MC-altered: Report
Overview of Brain Tumors ICRO 2015 SRMS IMS, Bareilly Prof Kamal Sahni
 Overview of Brain Tumors ICRO 2015 SRMS IMS, Bareilly Prof Kamal Sahni 1 Overview of Brain Tumors Incidence, prevalence & mortality Metastatic vs. Primary CNS tumors =10:1 World wide incidence of Primary
Overview of Brain Tumors ICRO 2015 SRMS IMS, Bareilly Prof Kamal Sahni 1 Overview of Brain Tumors Incidence, prevalence & mortality Metastatic vs. Primary CNS tumors =10:1 World wide incidence of Primary
USCAP Pediatrics Evening Subspecialty Conference 2015
 USCAP Pediatrics Evening Subspecialty Conference 2015 Sunday 22 March 2015 Alexander Lazar MD/PhD Department of Pathology S Section of Bone Soft TIssue Pathology Sarcoma Research Center The Case Patient
USCAP Pediatrics Evening Subspecialty Conference 2015 Sunday 22 March 2015 Alexander Lazar MD/PhD Department of Pathology S Section of Bone Soft TIssue Pathology Sarcoma Research Center The Case Patient
TUMORS of nervous system
 TUMORS of nervous system By: Shifaa Alqa qa Done By : Ola Hijjawi CNS tumors : The annual incidence of CNS tumors ranges from 10 to 17 per 100,000 persons for intracranial tumors and 1 to 2 per 100,000
TUMORS of nervous system By: Shifaa Alqa qa Done By : Ola Hijjawi CNS tumors : The annual incidence of CNS tumors ranges from 10 to 17 per 100,000 persons for intracranial tumors and 1 to 2 per 100,000
Disclosures. An update on ancillary techniques in the diagnosis of soft tissue tumors. Ancillary techniques. Introduction
 Disclosures An update on ancillary techniques in the diagnosis of soft tissue tumors. I have nothing to disclose. Andrew Horvai, MD, PhD Clinical Professor, Pathology Introduction Ancillary techniques
Disclosures An update on ancillary techniques in the diagnosis of soft tissue tumors. I have nothing to disclose. Andrew Horvai, MD, PhD Clinical Professor, Pathology Introduction Ancillary techniques
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
2019 Neoplasms of the BRAIN/CNS. CDC & Florida DOH Attribution
 2019 Neoplasms of the BRAIN/CNS 2018-2019 FCDS Educational Webcast Series Steven Peace, BS, CTR March 21, 2019 CDC & Florida DOH Attribution Funding for this conference was made possible (in part) by the
2019 Neoplasms of the BRAIN/CNS 2018-2019 FCDS Educational Webcast Series Steven Peace, BS, CTR March 21, 2019 CDC & Florida DOH Attribution Funding for this conference was made possible (in part) by the
성균관대학교삼성창원병원신경외과학교실신경종양학 김영준. KNS-MT-03 (April 15, 2015)
 성균관대학교삼성창원병원신경외과학교실신경종양학 김영준 INTRODUCTIONS Low grade gliomas (LGG) - heterogeneous group of tumors with astrocytic, oligodendroglial, ependymal, or mixed cellular histology - In adults diffuse, infiltrating
성균관대학교삼성창원병원신경외과학교실신경종양학 김영준 INTRODUCTIONS Low grade gliomas (LGG) - heterogeneous group of tumors with astrocytic, oligodendroglial, ependymal, or mixed cellular histology - In adults diffuse, infiltrating
What yield in the last decade about Molecular Diagnostics in Neuro
 What yield in the last decade about Molecular Diagnostics in Neuro Oncology? Raphael Salles S.Medeiros Neuropathologist at HC FMUSP Clinical Research Project Manager at Oncology department at Hospital
What yield in the last decade about Molecular Diagnostics in Neuro Oncology? Raphael Salles S.Medeiros Neuropathologist at HC FMUSP Clinical Research Project Manager at Oncology department at Hospital
H Haloes cautions, 57 neurocytomas, perinuclear, 56 Headache blue cell tumors, 147 cautions, 135, 147, 152 clinical history, 132, 144, 148
 Index A ADC. See Apparent diffusion coefficient Adult. See also Supratentorial mass, adult cerebral tumor, 1 headache and ataxia cysts, mural nodules, 118 sporadic tumors, 118 headaches and visual changes,
Index A ADC. See Apparent diffusion coefficient Adult. See also Supratentorial mass, adult cerebral tumor, 1 headache and ataxia cysts, mural nodules, 118 sporadic tumors, 118 headaches and visual changes,
Whole Genome and Transcriptome Analysis of Anaplastic Meningioma. Patrick Tarpey Cancer Genome Project Wellcome Trust Sanger Institute
 Whole Genome and Transcriptome Analysis of Anaplastic Meningioma Patrick Tarpey Cancer Genome Project Wellcome Trust Sanger Institute Outline Anaplastic meningioma compared to other cancers Whole genomes
Whole Genome and Transcriptome Analysis of Anaplastic Meningioma Patrick Tarpey Cancer Genome Project Wellcome Trust Sanger Institute Outline Anaplastic meningioma compared to other cancers Whole genomes
Patients Treated with Leksell Gamma Knife
 Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
2018 Diagnostic Slide Session Case #8
 2018 Diagnostic Slide Session Case #8 Angela N. Viaene, MacLean P. Nasrallah, and Zissimos Mourelatos Hospital of the University of Pennsylvania AANP June 9, 2018 Disclosures: none Clinical History Healthy,
2018 Diagnostic Slide Session Case #8 Angela N. Viaene, MacLean P. Nasrallah, and Zissimos Mourelatos Hospital of the University of Pennsylvania AANP June 9, 2018 Disclosures: none Clinical History Healthy,
STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER
 IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Original Article STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER Grishma P. Jobanputra Tutor, Department of Pathology, B.J. Medical College,
IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Original Article STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER Grishma P. Jobanputra Tutor, Department of Pathology, B.J. Medical College,
Protocol applies to all neoplasms of the brain/spinal cord. Excludes neoplasms of the pituitary gland.
 Brain/Spinal Cord Protocol applies to all neoplasms of the brain/spinal cord. Excludes neoplasms of the pituitary gland. Protocol revision date: January 2005 No AJCC/UICC staging system Procedures Cytology
Brain/Spinal Cord Protocol applies to all neoplasms of the brain/spinal cord. Excludes neoplasms of the pituitary gland. Protocol revision date: January 2005 No AJCC/UICC staging system Procedures Cytology
Diagnostic implications of IDH1-R132H and OLIG2 expression patterns in rare and challenging glioblastoma variants
 & 2012 USCAP, Inc. All rights reserved 0893-3952/12 $32.00 1 Diagnostic implications of IDH1-R132H and OLIG2 expression patterns in rare and challenging glioblastoma variants Nancy M Joseph 1, Joanna Phillips
& 2012 USCAP, Inc. All rights reserved 0893-3952/12 $32.00 1 Diagnostic implications of IDH1-R132H and OLIG2 expression patterns in rare and challenging glioblastoma variants Nancy M Joseph 1, Joanna Phillips
Cerebral Parenchymal Lesions: I. Metastatic Neoplasms
 Chapter 4 Cerebral Parenchymal Lesions: I. Metastatic Neoplasms After one has reasonably ruled out the possibility of a nonneoplastic diagnosis (see Chap. 3), one is left with considering a diagnosis of
Chapter 4 Cerebral Parenchymal Lesions: I. Metastatic Neoplasms After one has reasonably ruled out the possibility of a nonneoplastic diagnosis (see Chap. 3), one is left with considering a diagnosis of
Brain Tumors. Medulloblastoma. Pilocytic astrocytoma: Ahmed Koriesh, MD. Pathological finding
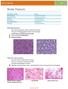 NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
Brain tumors: tumor types
 Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Case 1. Maysa Al-Hussaini MD FRCPath
 Case 1 Maysa Al-Hussaini MD FRCPath MAYSA King AL-HUSSAINI Hussein Cancer MD Center MRCPATH KING HUSSEIN Amman CANCER Jordan CENTER Clinical history 4 year old boy History of frontal headache, sleepiness.
Case 1 Maysa Al-Hussaini MD FRCPath MAYSA King AL-HUSSAINI Hussein Cancer MD Center MRCPATH KING HUSSEIN Amman CANCER Jordan CENTER Clinical history 4 year old boy History of frontal headache, sleepiness.
DNA methylation signatures for 2016 WHO classification subtypes of diffuse gliomas
 Paul et al. Clinical Epigenetics (2017) 9:32 DOI 10.1186/s13148-017-0331-9 RESEARCH Open Access DNA methylation signatures for 2016 WHO classification subtypes of diffuse gliomas Yashna Paul, Baisakhi
Paul et al. Clinical Epigenetics (2017) 9:32 DOI 10.1186/s13148-017-0331-9 RESEARCH Open Access DNA methylation signatures for 2016 WHO classification subtypes of diffuse gliomas Yashna Paul, Baisakhi
Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence
 PEDIATRIC RHABDOID MENINGIOMA Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence CLINICAL HISTORY A 3-year-old boy, with a recent history of seizures, was admitted to the Neurosurgery
PEDIATRIC RHABDOID MENINGIOMA Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence CLINICAL HISTORY A 3-year-old boy, with a recent history of seizures, was admitted to the Neurosurgery
SPECIAL SLIDE SEMINAR CASE 3
 SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
Q&A. Fabulous Prizes. Collecting Cancer Data:CNS 2/7/12. NAACCR Webinar Series Collecting Cancer Data Central Nervous System
 Collecting Cancer Data Central Nervous System NAACCR 2012 2013 Webinar Series 2/7/2013 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants
Collecting Cancer Data Central Nervous System NAACCR 2012 2013 Webinar Series 2/7/2013 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants
CODING TUMOUR MORPHOLOGY. Otto Visser
 CODING TUMOUR MORPHOLOGY Otto Visser INTRODUCTION The morphology describes the tissue of the tumour closest to normal tissue Well differentiated tumours are closest to normal Undifferentiated tumours show
CODING TUMOUR MORPHOLOGY Otto Visser INTRODUCTION The morphology describes the tissue of the tumour closest to normal tissue Well differentiated tumours are closest to normal Undifferentiated tumours show
Gamsızkan M, Kantarcıoglu CS, Yılmaz I, Yalcinkaya U, Sungur MA, Buyucek S, Onal B
 Tykhe, from Konuralp/Duzce TERT promoter mutation and HER2 gene amplification in malignant peripheral nerve sheath tumours: is there a molecular signature playing role in malignant transformation? Gamsızkan
Tykhe, from Konuralp/Duzce TERT promoter mutation and HER2 gene amplification in malignant peripheral nerve sheath tumours: is there a molecular signature playing role in malignant transformation? Gamsızkan
