Status of Proton Therapy: results and future trends
|
|
|
- Jordan Cook
- 5 years ago
- Views:
Transcription
1 Status of Proton Therapy: results and future trends E. Pedroni Paul Scherrer Institute Division of Radiation Medicine CH-5232 Villigen PSI Abstract The number of centres investigating proton therapy in the hvorld is steadily increasing. This review on the present status of proton therapy is addressed to physicists not working in the field. The presentation includes a brief summary of the established medical indications and of the state of the art of the application techniques used. The future trends are seen in the new technological developments, like the use of proton gantries, beam scanning techniques, improved patient handling and in the increasing precision of treatment. The availability of modern diagnostics tools like CT and MRI, accompanied by an extremely fast growth of computer power are expected to help charged particle therapy to become more and more attractive in the future. 1, INTRODUCTION The general interest in proton therapy is slowly but steadily increasing in the world medical community. In this lecture we attempt to summtise the present situation of proton therapy and try to identify the future trends expected in this field. Section 2 is a general introduction to proton therapy with special emphasis on the medical motivation. In section 3 we describe the present status including the medical achievements and the state of the art of the techniques in use. The future trends are described in section PROTONTHERAPY 2.1 The Goal of Proton Thernp) The main purpose of proton therapy is the use of proton beams for the treatment of localised tumours and for radiosurgery with the goal to improve radiation therapy. The expected improvements are of purely technological nature and are represented by the capability of the protons to produce superior dose distributions in the patient s body compared to photons. As opposed to heavier ions, which by their enhanced high LET (linear energy transfer) produce remarkable differences in the radiation effects at the cellular level, we do not expect with protons any significant radiobiological differences compared to photon treatments. 2.2 The Need to improve Radiation Therapy Here we want to emphasise the important role which radiotherapy nowadays plays in the fight against cancer. About one person out of three is confronted in his life with cancer and one out of five dies from this disease. The overall cure rate of cancer is currently about 45% [ 11. Of these successes about half (22%) are due to surgery. The rest is more or less due to radiotherapy alone (12%) or to radiotherapy in combination with surgery (6%). All other modalities including chemotherapy (l-2%) contribute together only 5% to the cure rate. Radiation therapy is therefore the second efficient weapon available against cancer. A criticism often advanced by biologists against radiation therapy is that this method is not biologically selective at the cellular level, a hammer method. They clearly give preference to cell seeking substances like antibodies or new genetic technologies, which are perceived to fight cancer in a more intelligent way. This kind of research represents indeed the hope for a future breakthrough in the fight against cancer. The big question then is if these methods will make radiation therapy obsolete. There are justified doubts that a penicillin-like drug for cancer will appear in the foreseeable future [2]. A more realistic scenario is to assume that new cell seeking substances will be found in the near future which will be successful against the spread of single distant cancer cells (microscopic metastases). These drugs will however probably not be sufficiently effective to achieve the complete sterilisation of the primary tumour, especially in view of the difficult physiological problem of bringing the drugs to the centre of the tumour by perfusion. The task of stopping the growth of the primary tumour is likely to remain the prerogative of surgery and radiotherapy in the long term future. About 17% of patients die because of failure in controlling the primary malignancy. These patients are expected to profit from an improved radiation therapy. The general strategy in oncology today is to consider the different treatment modalities as complements to each other. In the eventuality of a breaktkrough for the treatment of distant metastases using immunologic methods, all radiation treatments, which are applied now for palliation, could become curative. Therefore radiotherapy needs to evolve in the immediate future to a higher level of precision. Technical improvements in radiation therapy are socially desirable and, due to the progress in diagnostics and computer power, are also becoming more feasible. Among the different technological possibilities for improving radiation therapy the use of protons is one of the most promising. 2.3 Why Protons? Protons have the potential to bring significant improvements to radiation therapy by virtue of their 407
2 excellent physical properties. The dose delivered by a proton beam is well localised in space, not only in the lateral direction, but also very precisely in depth, due to the presence of the characteristic Bragg peak (Figure 1). $j c MV photons Protons: Bragg curves and Bpresd-Out-Bragg-Peak Depth (cm) Figure 1. Depth dose comparison of protons and photons The presence of the Bragg peak has to be compared with the corresponding dose curve for photons, which exhibits an exponential fall-off and which is therefore not localised in depth. The advantages of protons compared to photons can be summarised in the following way: 1) The dose beyond the Bragg peak is essentially zero. This is an advantage which can be exploited for the irradiation of tumours surrounded by sensitive structures, where stopping the beam in the tumour before reaching such tissues is of crucial importance. 2) Protons can bring a significant sparing of the integral dose deposited outside the target volume, provided that multiple fields can be applied on the patient using an isocentric gantry, following the strategy used for photons in the hospital, A factor of two to five less dose can be applied outside of the target volume compared to photons [3]. 3) Protons are charged particles. As opposed to photons, they can be focused and deflected by the action of magnetic fields under computer control. The dose distribution of a proton pencil beam is well localised in all three dimensions with a dose hot spot at the Bragg peak position. This opens the perspective for a dynamic scanning of the proton pencil beam, with the goal of providing in a routine fashion a three-dimensional conformation of the therapeutic dose to the target volume. The main disadvantage of proton therapy is given by the high magnetic rigidity of the beams used for therapy. The minimal bending radius which can be applied on a 270 MeV proton beam using conventional magnets operated below saturation limits is of the order of 1.3 m. This makes the size of the accelerator and of the beam transport system correspondingly large and expensive. 2.4 Can we afford Proton Therapy? The answer is yes, provided that improved clinical results compared to photon treatments can be demonstrated in practice. Conservative estimates show that charged particles will cost about double conventional radiation therapy. This is still much cheaper than many other established modalities, for example chemotherapy. If proton therapy saves medical costs, for example from additional surgery, hospitalisation or drugs, it can be proven to be advantageous also from an economical stand point. 3. STATUS OF PROTON THERAPY 3.1 Proton Therapy world-wide. hjedica1 Indications About patients have already been treated world-wide with protons [4]. The centres which have pioneered charged particle therapy in the past are Berkeley (U.S.A *), Uppsala (Sweden 1957), Harvard (U.S.A. 1961), Dubna (Russia 1967), Moscow (Russia 1969), St. Petersburg (Russia 1975), Chiba (Japan 1979) and Tsukuba (Japan 1983) [5]. A significant part of these activities was dedicated to radiation neurosurgery. The goal here is to act with localised radiation on small targets in the brain using stereotactic techniques (sequential applications of many small beams converging on a point). The aimed end-point of the dose application is very similar as with surgery. for example the disactivation of the pituitary gland or the occlusion of arteriovenous malformations (AVM). The method is mainly indicated for inoperable lesions and has the advantage of being a non invasive technique. A large majority of the tumour treatments have been applied to solid tumours in the eye bulb (mainly melanomas) using protons of low energy (around 70 MeV). This technique was developed in Harvard and Berkeley and was then introduced in Europe at PSI (Switzerland, 1984). The success of this application is well documented by its rapid spread to other centres in Europe, in Clatterbridge (Great Britain, 1989), Louvain-la-Neuve (Belgium, 1991), Nice and Orsay (France 1991) and overseas at Indiana University (U.S.A. 1993). The success of the eye treatments has been a big help for the spreading of high energy proton therapy to other sites in the body. Recently head treatments with a high energy beam (200 MeV) have also been started at Cape Town (South Africa 1993) and at Orsay (France 1991). The most cited indications for high energy (loo-220 MeV) proton therapy are for tumours close to the base of the skull (chordomas and chondrosarcomas), tumours close the spinal chord and tumours in the abdomen (sarcomas and cervix carcinomas) surrounded by sensitive healthy structures. Also worth mentioning are the treatments of lesions in the liver pioneered by the group of Tsukuba using a respiration-gated treatment technique. * Date of the first treatment and date of the last if treatments have been ceased. 408
3 Common to all older facilities was the use of protons delivered by an accelerator originally built for physics experiments and put out of operation at the end of the research period. Also common to the above mentioned facilities is the use of horizontal beam lines (without gantry). Many of them suffer from practical limitations in the available energy of the beam Others had limited technical resources, like limited access to computer tomography or lack of adequate computer power for the development of modern three-dimensional treatment planning systems. It is only recently with the completion of the Loma Linda facility in 1991 [6:, that protons have become available for the first time in a hospital. Loma Linda is the first and only place in the world offering protons on an isocentric gantry. This progress has been made possible by the initiative of Fermilab in building the first proton accelerator dedicated to therapy (a small compact synchrotron of 250 MeV). Loma Linda has been operational since 1991 and more than 700 patients have been successfully treated there, demonstrating the practical feasibility of proton therapy in a hospital. Protons are also used at Lomn Linda for common diseases, like prostatic cancer. The realisation of the Loma Linda facility represents indeed the first important milestone in tht history of the promotion of proton therapy. The realisation in the U.S.A. of the second hospital-based proton therapy facility of the world has been recently approved. The new ccntre will be realised at the Massachusetts General Hospital in Boston, which has the largest experience in proton therapy. The beam will be delivered by a cyclotron. The contract for the facility in Boston, including beam delivery system and gantry has been assigned to an European company (IBA Belgium). This will certainly have major positive consequences for the future of proton therapy in Europe. While we are eagerly awaiting the decision to build the first hospital-based proton facility for Europe, which most probably will be realised in Italy using an H- synchrotron (TERA project), there is an increase in the number of physics research centres proposing proton facilities at dedicated beam lines at their laboratories. The first dedicated facility with a proton gantry in Europe is now being assembled at PSI [7]. First patient treatments are planned for beginning of For the situation of the medical facilities in Europe we refer to the presentation of Prof. F. Farley at this conference. 3.3 Dose Application Techniques The method used up to now for dose delivery is the so-called scatter foil technique. Figure 2 shows the principle at the base of this dose application method. The beam is spread about four or five meter ahead of the patient, by a system of scatterers (foils or similar devices) in such a way as to obtain a uniform illumination of the spread beam in the solid angle covering the tumour region. The shaping of the dose in the lateral direction is achieved using two-dimensionally shaped collimators in close analogy to photon treatments. The modulation of the proton range is performed using a fast spinning wheel (range shifter wheel). The beam, by traversing a variable amount of material as a function of time, deposits a layer of uniform dose distribution in depth (Spread-Out-Bragg-Peak). The distal edge of the dose is usually adjusted to coincide with the distal side of the target volume using individually shaped compensators. The dose distribution conforms in this way to the distal half of the target volume. By adding together many beam directions one can realise a reasonable conformation of the dose to the target volume. The dose distribution and the shape of collimators and compensators are calculated in the treatment planning system, using the three-dimensional information (patient body electron density) delivered by computer tomography. The advantages of this method are its safety, simplicity and reliability. The possible disadvantages are the non-complete three-dimensional conformation of the dose and the large amount of hardware needed for each beam angle on the gantry. Range Shifter Wheel Figure 2. Scatter foil tecimiqur 4. FUTURE TRENDS 4.1 New Technological Developments The major improvements to be expected in this field are characterised by the following items: 4. I. I Beam Scanning Protons are charged particles. This gives the possibility of scanning the focused proton pencil beam in the patient body by magnetic deflection of the beam. The development of the spot scanning technique is the major goal of the proton therapy facility being realised at PSI. A similar approach is under development for ion beam therapy at GSI in Darmstadt. Figure 3 shows the principle at the base of the spot scanning technique. The approach chosen for beam scanning at PSI is based on the sequential deposition of a large number of static spot applications, typically for a one litre target volume in an overall treatment time of 3-4 minutes. The dose of each spot is controlled by measuring the dose with a monitor system while the spot is being deposited and by switching the beam off with a fast kicker magnet when the required
4 dose has been delivered. The position of the dose spot in the patient is controlled by the action of a sweeper magnet (which shifts the beam in one lateral direction), a range shifter (a stack of polyethylene plates, which are moved into the beam by pneumatic valves and which change the position of the Bragg peak in depth) and by moving the patient in the other lateral direction j cm Figure 3a. Principle of the spor scanning technique: through the weighted superposition of individual spots Isocentric Gantry All new dedicated proton facilities are being proposed with an isocentric gantry. A gantry system allows one to apply the beam on the patient from many directions and to distribute the entrance dose to different regions of the body, thus increasing the local tolerance to the treatment. The beam line is moved around the patient (and not vice versa) in order to maintain the patient exactly in the same fixed supine position during all phases of the treatment, including the data taking of the CT images used for treatment planning. The major problem found in the design of a gantry for proton therapy is its size. In a gantry for the scatter foil technique the scattering of the beam is usually performed after bending the beam in the direction of the patient to avoid large aperture magnetic elements. Enough drift space between scatterer and patient has to be provided for the beam to spread out before it reaches the patient. The radius of a gantry for the scatter foil technique is expected to be of the order of 5-6 m. The gantry of Loma Linda spans for example a diameter of 12 m. I II Figure 4. Cross section of the PSI gantry. -loi..-- -J cm Figure 3b... one can obtain a complete 3D-conformal dose. The advantages expected using a beam scanning technique are the following. The deposition of the spot dose is completely under computer control without the need to adjust individual hardware in front of the patient. Dynamic treatments can routinely provide an exact 3D-conformation of the dose to the target volume and the full automation is expected to bring more precision and more flexibility. A better utilisation of the proton beam with less activation problems and less neutron background is also anticipated, and as opposed to the scatter foil technique, it is possible to implement this method on a small compact gantry. A possible disadvantage of the method is its increased sensitivity to uncontrolled organ movements during scanning. Beam scanning is still under development. It should be noted that all future facilities are proposed for the traditional scatter foil technique, but are explicitly required to be upgradable for a beam scanning method ( scanning ready facilities) at a later stage. PSI is building a compact gantry dedicated specifically to the spot scan technique. By performing the scanning of the beam ahead of the last 90 bending magnet and by mounting the patient table eccentrically on the gantry (using a rotating support which maintains the table horizontal at all times) the diameter of the rotating structure has been reduced to only 4 m. This corresponds to the minimal space needed for magnet and patient table together without any drift space in between. The cross section of the PSI gantry is shown in figure 4. The gantry will be the second proton gantry to be realised in the world and is the smallest proton gantry using conventional magnets proposed so far. It is being commissioned presently. The first beam was successfully transmitted through the beam line in April The use of superconductivity and solutions based on the use of pulsed magnets are expected to reduce further the size of future proton gantries. Another proposed idea is to rotate the accelerator around the patient. A small superconducting cyclotron which rotates around the patient has been put in operation at Detroit for neutron therapy. Although running at a lower beam energy than needed for proton therapy this installation shows the feasibility of such ideas. 410
5 4.1.3 Increased Flexibility Future proton treatments will be characterised by an increased flexibility in the choice of the incidence of the beam on the patient. The choice of optimal beam directions is expected to be very important, not only to avoid sensitive structures in the way of the beam but also to select those situations which minimise possible errors arising from density heterogeneities of the patient s body, such as bony structures or air inserts. In order to increase this flexibility we have decided at PSI to build our gantry to allow for an additional rotation of the patient couch in the horizontal plane. For head treatments we will be able to irradiate the patient from essentially any direction. 4. I.4 Imreased Precision Future proton treatments will be characterised by an increased precision concerning both the positioning of the patient with respect to the beam and the control of the range of the protons in the patient s body. Better positioning can be achieved using individual mould techniques. Another possible improvement is given by the direct integration of a CT unit into the therapy equipment. The same dedicated CT unit will be used for example at PSI for both acquisition of the CT slices for treatment planning and for the position control (using scout view imagesj before the delivery of each dose fraction. The patients treated at PSI will be transported from one room to another, ready for treatment, on a special carriage system (lying in their individual couch). This patient transporter has been designed to allow for reproducible mechanical coupling of the patient couch on both the tables of the CT unit and of the proton gantry. This should guarantee a more precise relation between therapy and treatment planning. In addition to the control images taken outside of the treatment room, the control of the position of the patient will also be optionally done directly on the gantry using retractable X-ray tubes and devices for proton radiography. The control of the proton range in the patient in vivo will be performed by means of in vivo dosimetry and eventually by measuring with a PET camera the beta-plus activation induced in the patient. Proton radiography as a quality assurance tool for proton therapy is presently being developed at PSI. Proton radiography images contain not only data usable for the control of the position of the patient with respect to the beam, but also information on the residual range of the protons. This information can be predicted in the treatment planning programs and can be used as a test of the range of protons in the patient in vivo Computer Power and better Diagnostics Tools Dose calculations for a conformal three-dimensional spot-scanning technique were unthinkable a decade ago. Today calculations for precise proton treatments in very complex anatomical structures are feasible. At PSI we have developed a fast Monte Carlo code capable of delivering sufficiently high statistics to resolve details of the dose at the CT pixelsize. Computers able to cope with very large data sizes describing the three-dimensional anatomy of the patient were not available until recently, Another missing prerequisite for the optimal use of proton therapy in the past was the lack of access to modern diagnostic tools like CT and MRI, which can be used to exactly define where to place the beam. Wi ith these modern instruments we now see better where we want to shoot. For this we also now need a better gun, the protons. 4.2 New Medical Oldications The availability of improved confonnal techniques on proton gantries are expected to extend the list of indications for proton therapy to include large irregular target volumes, paediatric tumours, isolated metastasis, re-treatments, tumours with partial organ infiltration, and also to increase the tolerance for the combination of radiation therapy with other new modalities. 5. CONCLUSIONS Although the use of protons for therapy was proposed for the first time about 50 years ago, their true potential is starting to be recognised only now. This is documented by the increased number of centres proposing the use of proton therapy in the world and by the practical realisation of the first hospital-based charged particles facilities in Loma Linda, Chiba and Boston. The reason for this delay comes from the dependence of proton therapy on collateral sciences, such as computer and modem diagnostic technology. The fantastic progress observed in these fields in the last years is likely to make the inherent precision of protons more readily available in clinical practice, [l] 6. REFERENCES A. Vermorken, European strategy for research on cancer therapy, EPAC90, Nice 1990, pp. S124. (21 Proceedings of the International Symposium on Hadron Therapy, held in Como (Italy) in October To be published as a special supplement to N.I.M. [3] J. 0. Archambeau et al, Proton radiation therapy, Radiology, Vol. 110, pp , [4] from Particles 13, the newsletter sponsored by the Proton Therapy Co-Operative Group (PTCOG), edited by J. Sisterson, Harvard Cyclotron Laboratory, 44 Oxford Street, Cambridge MA (U.S.A.) [S] D. E. Bonnet, Current developments in proton therapy: a review, Phys. Med. Biol. Vol. 38, pp , and references therein. [6] J. M. Slater et ai, Development of a hospital-based proton treatment center,lnt. J. Radiat. Oncol. Biol. Phys., Vol. 14, pp , E. Pedroni et al, The 200 hlev proton therapy project at PSI: conceptual design and practical realization, submitted to Medical Physics in January
Heavy Ion Tumor Therapy
 Heavy Ion Tumor Therapy Applications Bence Mitlasoczki 25.06.2018 Heidelberg 1. Source (H 2 /CO 2 ) 2. Linac 3. Synchrotron 4. Guide 5. Treatment rooms 6. X-ray system 7. Gantry 8. Treatment room with
Heavy Ion Tumor Therapy Applications Bence Mitlasoczki 25.06.2018 Heidelberg 1. Source (H 2 /CO 2 ) 2. Linac 3. Synchrotron 4. Guide 5. Treatment rooms 6. X-ray system 7. Gantry 8. Treatment room with
Introduction to Ion Beam Cancer Therapy
 Introduction to Ion Beam Cancer Therapy Andrew M. Sessler (with some slides from David Robin) Lawrence Berkeley National Laboratory Berkeley, CA 94720 Cyclotron 10, Lanzhou September 10, 2010 Contents
Introduction to Ion Beam Cancer Therapy Andrew M. Sessler (with some slides from David Robin) Lawrence Berkeley National Laboratory Berkeley, CA 94720 Cyclotron 10, Lanzhou September 10, 2010 Contents
SCIENTIFIC AND TECHNOLOGICAL DEVELOPMENT OF HADRONTHERAPY
 SCIENTIFIC AND TECHNOLOGICAL DEVELOPMENT OF HADRONTHERAPY SAVERIO BRACCINI * Albert Einstein Centre for Fundamental Physics, Laboratory for High Energy Physics (LHEP), University of Bern, Sidlerstrasse
SCIENTIFIC AND TECHNOLOGICAL DEVELOPMENT OF HADRONTHERAPY SAVERIO BRACCINI * Albert Einstein Centre for Fundamental Physics, Laboratory for High Energy Physics (LHEP), University of Bern, Sidlerstrasse
Proton Therapy Dosimetry & Clinical Implementation. Baldev Patyal, Ph.D., Chief Medical Physicist Department of Radiation Medicine
 Proton Therapy Dosimetry & Clinical Implementation Baldev Patyal, Ph.D., Chief Medical Physicist Department of Radiation Medicine Outline» Proton Therapy Basics» Why Proton Therapy? (Dosimetric Superiority)»
Proton Therapy Dosimetry & Clinical Implementation Baldev Patyal, Ph.D., Chief Medical Physicist Department of Radiation Medicine Outline» Proton Therapy Basics» Why Proton Therapy? (Dosimetric Superiority)»
State-of-the-art proton therapy: The physicist s perspective
 State-of-the-art proton therapy: Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Overview of presentation 1. State-of-the-art proton delivery 2. Current challenges 3. New
State-of-the-art proton therapy: Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Overview of presentation 1. State-of-the-art proton delivery 2. Current challenges 3. New
III. Proton-therapytherapy. Rome SB - 5/5 1
 Outline Introduction: an historical review I Applications in medical diagnostics Particle accelerators for medicine Applications in conventional radiation therapy II III IV Hadrontherapy, the frontier
Outline Introduction: an historical review I Applications in medical diagnostics Particle accelerators for medicine Applications in conventional radiation therapy II III IV Hadrontherapy, the frontier
Characterization and implementation of Pencil Beam Scanning proton therapy techniques: from spot scanning to continuous scanning
 Characterization and implementation of Pencil Beam Scanning proton therapy techniques: from spot scanning to continuous scanning Supervisors Prof. V. Patera PhD R. Van Roermund Candidate Annalisa Patriarca
Characterization and implementation of Pencil Beam Scanning proton therapy techniques: from spot scanning to continuous scanning Supervisors Prof. V. Patera PhD R. Van Roermund Candidate Annalisa Patriarca
PROGRESS IN HADRONTHERAPY
 PROGRESS IN HADRONTHERAPY Saverio Braccini TERA Foundation for Oncological Hadrontherapy IPRD06 - Siena - 01.10.06 - SB 1 Outline Introduction Radiation therapy with X rays and hadrontherapy Hadrontherapy
PROGRESS IN HADRONTHERAPY Saverio Braccini TERA Foundation for Oncological Hadrontherapy IPRD06 - Siena - 01.10.06 - SB 1 Outline Introduction Radiation therapy with X rays and hadrontherapy Hadrontherapy
The Advantages of Particle Therapy and the Status of the Heidelberg Iontherapy Center
 The Advantages of Particle Therapy and the Status of the Heidelberg Iontherapy Center Thomas Haberer, Scientific Technical Director, Heidelberg Ion Therapy Center Situation / Indications 2/3 patients suffer
The Advantages of Particle Therapy and the Status of the Heidelberg Iontherapy Center Thomas Haberer, Scientific Technical Director, Heidelberg Ion Therapy Center Situation / Indications 2/3 patients suffer
Progress of Heavy Ion Therapy
 Progress of Heavy Ion Therapy Fuminori Soga Division of Accelerator Physics and Engineering, National Institute of Radiological Sciences, 4-9-1 Anagawa. Inage-ku, Chiba 263-8555, Japan 1. Introduction
Progress of Heavy Ion Therapy Fuminori Soga Division of Accelerator Physics and Engineering, National Institute of Radiological Sciences, 4-9-1 Anagawa. Inage-ku, Chiba 263-8555, Japan 1. Introduction
Proton and heavy ion radiotherapy: Effect of LET
 Proton and heavy ion radiotherapy: Effect of LET As a low LET particle traverses a DNA molecule, ionizations are far apart and double strand breaks are rare With high LET particles, ionizations are closer
Proton and heavy ion radiotherapy: Effect of LET As a low LET particle traverses a DNA molecule, ionizations are far apart and double strand breaks are rare With high LET particles, ionizations are closer
Proton Treatment. Keith Brown, Ph.D., CHP. Associate Director, Radiation Safety University of Pennsylvania
 Proton Treatment Keith Brown, Ph.D., CHP Associate Director, Radiation Safety University of Pennsylvania Proton Dose vs. Depth Wilson,. R.R. Radiological use of fast protons. Radiology 47:487-491, 1946.
Proton Treatment Keith Brown, Ph.D., CHP Associate Director, Radiation Safety University of Pennsylvania Proton Dose vs. Depth Wilson,. R.R. Radiological use of fast protons. Radiology 47:487-491, 1946.
Status of H 1 and C 12
 Status of H 1 and C 12 Herman Suit No Conflict of Interest 1 Goal of a New Treatment Modality Tumor Control Probability or No in Complication Rate 2 Truism No Advantage to: any Patient for any Radiation
Status of H 1 and C 12 Herman Suit No Conflict of Interest 1 Goal of a New Treatment Modality Tumor Control Probability or No in Complication Rate 2 Truism No Advantage to: any Patient for any Radiation
Cancer Treatment by Charged Particles - Carbon Ion Radiotherapy -
 Cancer Treatment by Charged Particles - Carbon Ion Radiotherapy - Takeshi Murakami Research Center of Charged Particle Therapy National Institute of Radiological Sciences 2012.11.21 1. Introduction to
Cancer Treatment by Charged Particles - Carbon Ion Radiotherapy - Takeshi Murakami Research Center of Charged Particle Therapy National Institute of Radiological Sciences 2012.11.21 1. Introduction to
AMERICAN BRAIN TUMOR ASSOCIATION. Proton Therapy
 AMERICAN BRAIN TUMOR ASSOCIATION Proton Therapy ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit
AMERICAN BRAIN TUMOR ASSOCIATION Proton Therapy ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit
ABSTRACTS. of the NIRS International Seminar on the Heavy Charged Particle Therapy for Cancer and the XXVII PTCOG MEETING.
 P ROTON THERAPY C O- OPERATIVE GROUP Chair Michael Goitein Ph. D. Department of Radiation Oncology Massachusetts General Hospital Boston MA 02114 (617) 724-9529 (617) 724-9532 Fax Secret ary Janet Sisterson
P ROTON THERAPY C O- OPERATIVE GROUP Chair Michael Goitein Ph. D. Department of Radiation Oncology Massachusetts General Hospital Boston MA 02114 (617) 724-9529 (617) 724-9532 Fax Secret ary Janet Sisterson
TomoTherapy. Michelle Roach CNC Radiation Oncology Liverpool Hospital CNSA. May 2016
 TomoTherapy Michelle Roach CNC Radiation Oncology Liverpool Hospital CNSA May 2016 TomoTherapy The Facts Greek Tomo = slice Advanced form of IMRT 3D computerised tomography (CT) imaging immediately prior
TomoTherapy Michelle Roach CNC Radiation Oncology Liverpool Hospital CNSA May 2016 TomoTherapy The Facts Greek Tomo = slice Advanced form of IMRT 3D computerised tomography (CT) imaging immediately prior
Present status and future of Proton beam therapy
 Present status and future of Proton beam therapy Description At present, the types of proven treatment for cancer are surgery, radiotherapy, and chemotherapy. Depending on the characteristics of cancer
Present status and future of Proton beam therapy Description At present, the types of proven treatment for cancer are surgery, radiotherapy, and chemotherapy. Depending on the characteristics of cancer
A review of cyclotrons for Hadron Therapy. Y. Jongen Cyclotrons 2010 Lanzhou, September
 A review of cyclotrons for Hadron Therapy Y. Jongen Cyclotrons 2010 Lanzhou, September 10 2010 The early days The possible use of the Bragg peak of high energy ions in the radiotherapy of cancer was suggested
A review of cyclotrons for Hadron Therapy Y. Jongen Cyclotrons 2010 Lanzhou, September 10 2010 The early days The possible use of the Bragg peak of high energy ions in the radiotherapy of cancer was suggested
Road Map for the development of hadron therapy and associated nuclear medicine methods at JINR:
 НТС ОЭЗ, 07 октября 2011 Road Map for the development of hadron therapy and associated nuclear medicine methods at JINR: Development of 3D conformal Proton therapy Design of various devices for proton
НТС ОЭЗ, 07 октября 2011 Road Map for the development of hadron therapy and associated nuclear medicine methods at JINR: Development of 3D conformal Proton therapy Design of various devices for proton
FROM ICARO1 TO ICARO2: THE MEDICAL PHYSICS PERSPECTIVE. Geoffrey S. Ibbott, Ph.D. June 20, 2017
 FROM ICARO1 TO ICARO2: THE MEDICAL PHYSICS PERSPECTIVE Geoffrey S. Ibbott, Ph.D. June 20, 2017 1 DISCLOSURES My institution holds Strategic Partnership Research Agreements with Varian, Elekta, and Philips
FROM ICARO1 TO ICARO2: THE MEDICAL PHYSICS PERSPECTIVE Geoffrey S. Ibbott, Ph.D. June 20, 2017 1 DISCLOSURES My institution holds Strategic Partnership Research Agreements with Varian, Elekta, and Philips
A TREATMENT PLANNING STUDY COMPARING VMAT WITH 3D CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER USING PINNACLE PLANNING SYSTEM *
 Romanian Reports in Physics, Vol. 66, No. 2, P. 394 400, 2014 A TREATMENT PLANNING STUDY COMPARING VMAT WITH 3D CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER USING PINNACLE PLANNING SYSTEM * D. ADAM 1,2,
Romanian Reports in Physics, Vol. 66, No. 2, P. 394 400, 2014 A TREATMENT PLANNING STUDY COMPARING VMAT WITH 3D CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER USING PINNACLE PLANNING SYSTEM * D. ADAM 1,2,
New Treatment Research Facility Project at HIMAC
 New Treatment Research Facility Project at Koji Noda Research Center for Charged Particle Therapy National Institute of Radiological Sciences IPAC10, Kyoto, JAPAN, 25th May, 2010 Contents 1. Introduction
New Treatment Research Facility Project at Koji Noda Research Center for Charged Particle Therapy National Institute of Radiological Sciences IPAC10, Kyoto, JAPAN, 25th May, 2010 Contents 1. Introduction
ADVANCES IN RADIATION TECHNOLOGIES IN THE TREATMENT OF CANCER
 ADVANCES IN RADIATION TECHNOLOGIES IN THE TREATMENT OF CANCER Bro. Dr. Collie Miller IARC/WHO Based on trends in the incidence of cancer, the International Agency for Research on Cancer (IARC) and WHO
ADVANCES IN RADIATION TECHNOLOGIES IN THE TREATMENT OF CANCER Bro. Dr. Collie Miller IARC/WHO Based on trends in the incidence of cancer, the International Agency for Research on Cancer (IARC) and WHO
By Elizabeth Clements. Applications in cancer treatment
 Illustrations: Sandbox Studio, Chicago A new kind of detector technology that could lead to discoveries in particle physics may also lead to better 3D images of the human body and help cancer patients.
Illustrations: Sandbox Studio, Chicago A new kind of detector technology that could lead to discoveries in particle physics may also lead to better 3D images of the human body and help cancer patients.
A Patient s Guide to SRS
 A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
The Heidelberg Ion Therapy Center. Thomas Haberer Heidelberg Ion Therapy Center Hadron Therapy Workshop, Erice 2009
 The Heidelberg Ion Therapy Center Thomas Haberer Heidelberg Ion Therapy Center Hadron Therapy Workshop, Erice 2009 Goal The key element to improve the clinical outcome is local l control! entrance channel:
The Heidelberg Ion Therapy Center Thomas Haberer Heidelberg Ion Therapy Center Hadron Therapy Workshop, Erice 2009 Goal The key element to improve the clinical outcome is local l control! entrance channel:
The Heidelberg Ion Therapy Center and PARTNER. Thomas Haberer Heidelberg Ion Therapy Center
 The Heidelberg Ion Therapy Center and PARTNER Thomas Haberer Heidelberg Ion Therapy Center Goal The key element to improve the clinical outcome is local control! entrance channel: low physical dose low
The Heidelberg Ion Therapy Center and PARTNER Thomas Haberer Heidelberg Ion Therapy Center Goal The key element to improve the clinical outcome is local control! entrance channel: low physical dose low
Basic Press Information
 Basic Press Information Contact MedAustron EBG MedAustron GmbH Marie Curie-Strasse 5 A-2700 Wiener Neustadt Austria T +43 2622 26 100-0 e-mail: office@medaustron.at Internet: www.medaustron.at Press contact:
Basic Press Information Contact MedAustron EBG MedAustron GmbH Marie Curie-Strasse 5 A-2700 Wiener Neustadt Austria T +43 2622 26 100-0 e-mail: office@medaustron.at Internet: www.medaustron.at Press contact:
Present Status and Future Developments in Proton Therapy
 Present Status and Future Developments in Proton Therapy Alfred R. Smith Department of Radiation Oncology, The University of Texas M. D. Anderson Cancer Center, 1515 Holcombe Blvd., Houston, TX 77030,
Present Status and Future Developments in Proton Therapy Alfred R. Smith Department of Radiation Oncology, The University of Texas M. D. Anderson Cancer Center, 1515 Holcombe Blvd., Houston, TX 77030,
Use of radiation to kill diseased cells. Cancer is the disease that is almost always treated when using radiation.
 Radiation Therapy Use of radiation to kill diseased cells. Cancer is the disease that is almost always treated when using radiation. One person in three will develop some form of cancer in their lifetime.
Radiation Therapy Use of radiation to kill diseased cells. Cancer is the disease that is almost always treated when using radiation. One person in three will develop some form of cancer in their lifetime.
I. Equipments for external beam radiotherapy
 I. Equipments for external beam radiotherapy 5 linear accelerators (LINACs): Varian TrueBeam 6, 10 & 18 MV photons, 6-18 MeV electrons, image-guided (IGRT) and intensity modulated radiotherapy (IMRT),
I. Equipments for external beam radiotherapy 5 linear accelerators (LINACs): Varian TrueBeam 6, 10 & 18 MV photons, 6-18 MeV electrons, image-guided (IGRT) and intensity modulated radiotherapy (IMRT),
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: charged_particle_radiotherapy 3/12/96 5/2017 5/2018 5/2017 Description of Procedure or Service Charged-particle
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: charged_particle_radiotherapy 3/12/96 5/2017 5/2018 5/2017 Description of Procedure or Service Charged-particle
Learning Objectives. Clinically operating proton therapy facilities. Overview of Quality Assurance in Proton Therapy. Omar Zeidan
 Overview of Quality Assurance in Proton Therapy Omar Zeidan AAPM 2012 Charlotte, NC July 30 st, 2012 Learning Objectives Understand proton beam dosimetry characteristics and compare them to photon beams
Overview of Quality Assurance in Proton Therapy Omar Zeidan AAPM 2012 Charlotte, NC July 30 st, 2012 Learning Objectives Understand proton beam dosimetry characteristics and compare them to photon beams
HEAVY PARTICLE THERAPY
 HEAVY PARTICLE THERAPY DR. G.V. GIRI KIDWAI MEMORIAL INSTITUTE OF ONCOLOGY ICRO 2012 BHATINDA HEAVY PARTICLES USED IN A EFFORT TO IMPROVE TUMOR CONTROL, THAT DO NOT RESPOND TO PHOTONS OR ELECTRONS BETTER
HEAVY PARTICLE THERAPY DR. G.V. GIRI KIDWAI MEMORIAL INSTITUTE OF ONCOLOGY ICRO 2012 BHATINDA HEAVY PARTICLES USED IN A EFFORT TO IMPROVE TUMOR CONTROL, THAT DO NOT RESPOND TO PHOTONS OR ELECTRONS BETTER
Discuss the general planning concepts used in proton planning. Review the unique handling of CTV / ITV / PTV when treating with protons
 Mark Pankuch, PhD Discuss the general planning concepts used in proton planning Review the unique handling of CTV / ITV / PTV when treating with protons Pencil Beam distributions and PBS optimization Cover
Mark Pankuch, PhD Discuss the general planning concepts used in proton planning Review the unique handling of CTV / ITV / PTV when treating with protons Pencil Beam distributions and PBS optimization Cover
An Introduction to Cancer Therapy With Hadron Radiation
 An Introduction to Cancer Therapy With Hadron Radiation Andrew M. Sessler Lawrence Berkeley National Laboratory Berkeley, CA 94720 April, 2008 Contents 1. History 2. X-Ray Machines 3. Why Hadrons? Which
An Introduction to Cancer Therapy With Hadron Radiation Andrew M. Sessler Lawrence Berkeley National Laboratory Berkeley, CA 94720 April, 2008 Contents 1. History 2. X-Ray Machines 3. Why Hadrons? Which
Radiotherapy. Marta Anguiano Millán. Departamento de Física Atómica, Molecular y Nuclear Facultad de Ciencias. Universidad de Granada
 Departamento de Física Atómica, Molecular y Nuclear Facultad de Ciencias. Universidad de Granada Overview Introduction Overview Introduction Brachytherapy Radioisotopes in contact with the tumor Overview
Departamento de Física Atómica, Molecular y Nuclear Facultad de Ciencias. Universidad de Granada Overview Introduction Overview Introduction Brachytherapy Radioisotopes in contact with the tumor Overview
Proton Beam Therapy at Mayo Clinic
 Proton Beam Therapy at Mayo Clinic Jon J. Kruse, Ph.D. Mayo Clinic Dept. of Radiation Oncology Rochester, MN History of Proton Therapy at Mayo 2002: Decided to consider particle therapy analysis and education
Proton Beam Therapy at Mayo Clinic Jon J. Kruse, Ph.D. Mayo Clinic Dept. of Radiation Oncology Rochester, MN History of Proton Therapy at Mayo 2002: Decided to consider particle therapy analysis and education
Chapter 5 Section 3.1
 Radiology Chapter 5 Section 3.1 Issue Date: March 27, 1991 Authority: 32 CFR 199.4(b)(2), (b)(2)(x), (c)(2)(viii), and (g)(15) 1.0 CPT 1 PROCEDURE CODES 37243, 61793, 61795, 77261-77421, 77427-77799, 0073T
Radiology Chapter 5 Section 3.1 Issue Date: March 27, 1991 Authority: 32 CFR 199.4(b)(2), (b)(2)(x), (c)(2)(viii), and (g)(15) 1.0 CPT 1 PROCEDURE CODES 37243, 61793, 61795, 77261-77421, 77427-77799, 0073T
Considerations when treating lung cancer with passive scatter or active scanning proton therapy
 Mini-Review Considerations when treating lung cancer with passive scatter or active scanning proton therapy Sara St. James, Clemens Grassberger, Hsiao-Ming Lu Department of Radiation Oncology, Massachusetts
Mini-Review Considerations when treating lung cancer with passive scatter or active scanning proton therapy Sara St. James, Clemens Grassberger, Hsiao-Ming Lu Department of Radiation Oncology, Massachusetts
SUMITOMO Particle Therapy Technologies
 55 th AAPM annual meeting Particle Beam Therapy Symposium SUMITOMO Particle Therapy Technologies August 3, 2013 Yukio Kumata Experience accelerators for science Current Status proton and carbon Future
55 th AAPM annual meeting Particle Beam Therapy Symposium SUMITOMO Particle Therapy Technologies August 3, 2013 Yukio Kumata Experience accelerators for science Current Status proton and carbon Future
IN VIVO IMAGING Proton Beam Range Verification With PET/CT
 IN VIVO IMAGING Proton Beam Range Verification With PET/CT Antje-Christin Knopf 1/3 K Parodi 2, H Paganetti 1, T Bortfeld 1 Siemens Medical Solutions Supports This Project 1 Department of Radiation Oncology,
IN VIVO IMAGING Proton Beam Range Verification With PET/CT Antje-Christin Knopf 1/3 K Parodi 2, H Paganetti 1, T Bortfeld 1 Siemens Medical Solutions Supports This Project 1 Department of Radiation Oncology,
COMPARISON OF RADIOBIOLOGICAL EFFECTS OF CARBON IONS TO PROTONS ON A RESISTANT HUMAN MELANOMA CELL LINE
 COMPARISON OF RADIOBIOLOGICAL EFFECTS OF CARBON IONS TO PROTONS ON A RESISTANT HUMAN MELANOMA CELL LINE I. Petrovi a, A. Risti -Fira a, L. Kori anac a, J. Požega a, F. Di Rosa b, P. Cirrone b and G. Cuttone
COMPARISON OF RADIOBIOLOGICAL EFFECTS OF CARBON IONS TO PROTONS ON A RESISTANT HUMAN MELANOMA CELL LINE I. Petrovi a, A. Risti -Fira a, L. Kori anac a, J. Požega a, F. Di Rosa b, P. Cirrone b and G. Cuttone
Proton Stereotactic Radiotherapy: Clinical Overview. Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS
 Proton Stereotactic Radiotherapy: Clinical Overview Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS Acknowledgements Radiation Oncologists and Physicists at various institutions (MGH, MDACC,
Proton Stereotactic Radiotherapy: Clinical Overview Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS Acknowledgements Radiation Oncologists and Physicists at various institutions (MGH, MDACC,
Treatment Planning (Protons vs. Photons)
 Treatment Planning Treatment Planning (Protons vs. Photons) Acquisition of imaging data Delineation of regions of interest Selection of beam directions Dose calculation Optimization of the plan Hounsfield
Treatment Planning Treatment Planning (Protons vs. Photons) Acquisition of imaging data Delineation of regions of interest Selection of beam directions Dose calculation Optimization of the plan Hounsfield
Ion Beam Therapy should we prioritise research on helium beams?
 Ion Beam Therapy should we prioritise research on helium beams? Stuart Green Medical Physics University Hospital Birmingham NHS Trust Follow-up from the EUCARD2 workshop, ION Beam Therapy: Clinical, Scientific
Ion Beam Therapy should we prioritise research on helium beams? Stuart Green Medical Physics University Hospital Birmingham NHS Trust Follow-up from the EUCARD2 workshop, ION Beam Therapy: Clinical, Scientific
Prof. Dr. Thomas Haberer Scientific-technical Director Heidelberg Iontherapy Center
 The Heidelberg Ion Beam Therapy Center A Hospital-based Facility Dedicated to Precision and Flexibility Prof. Dr. Thomas Haberer Scientific-technical Director Heidelberg Iontherapy Center Carbon Ion Therapy
The Heidelberg Ion Beam Therapy Center A Hospital-based Facility Dedicated to Precision and Flexibility Prof. Dr. Thomas Haberer Scientific-technical Director Heidelberg Iontherapy Center Carbon Ion Therapy
Radiotherapy in feline and canine head and neck cancer
 Bettina Kandel Like surgery radiotherapy is usually a localized type of treatment. Today it is more readily available for the treatment of cancer in companion animals and many clients are well informed
Bettina Kandel Like surgery radiotherapy is usually a localized type of treatment. Today it is more readily available for the treatment of cancer in companion animals and many clients are well informed
Applications of Particle Accelerators
 Applications of Particle Accelerators Prof. Rob Edgecock STFC Rutherford Appleton Laboratory EMMA Accelerator at Daresbury Laboratory Applications >30000 accelerators in use world-wide: 44% for radiotherapy
Applications of Particle Accelerators Prof. Rob Edgecock STFC Rutherford Appleton Laboratory EMMA Accelerator at Daresbury Laboratory Applications >30000 accelerators in use world-wide: 44% for radiotherapy
Original Date: April 2016 Page 1 of 7 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
Use of Bubble Detectors to Characterize Neutron Dose Distribution in a Radiotherapy Treatment Room used for IMRT treatments
 Use of Bubble Detectors to Characterize Neutron Dose Distribution in a Radiotherapy Treatment Room used for IMRT treatments Alana Hudson *1 1 Tom Baker Cancer Centre, Department of Medical Physics, 1331
Use of Bubble Detectors to Characterize Neutron Dose Distribution in a Radiotherapy Treatment Room used for IMRT treatments Alana Hudson *1 1 Tom Baker Cancer Centre, Department of Medical Physics, 1331
Hampton University Proton Therapy Institute
 Hampton University Proton Therapy Institute Brief introduction to proton therapy technology, its advances and Hampton University Proton Therapy Institute Vahagn Nazaryan, Ph.D. Executive Director, HUPTI
Hampton University Proton Therapy Institute Brief introduction to proton therapy technology, its advances and Hampton University Proton Therapy Institute Vahagn Nazaryan, Ph.D. Executive Director, HUPTI
H. Röcken, M. Abdel-Bary, E. Akcöltekin, P. Budz, T. Stephani, J. Wittschen
 : Medical Operation of the 2 nd Machine, Production and Commissioning Status of Machines No. 3 to 7 H. Röcken, M. Abdel-Bary, E. Akcöltekin, P. Budz, T. Stephani, J. Wittschen VARIAN Medical Systems Particle
: Medical Operation of the 2 nd Machine, Production and Commissioning Status of Machines No. 3 to 7 H. Röcken, M. Abdel-Bary, E. Akcöltekin, P. Budz, T. Stephani, J. Wittschen VARIAN Medical Systems Particle
Clinical Commissioning Policy Proposition: Proton Beam Therapy for Cancer of the Prostate
 Clinical Commissioning Policy Proposition: Proton Beam Therapy for Cancer of the Prostate Reference: NHS England B01X09 First published: March 2016 Prepared by NHS England Specialised Services Clinical
Clinical Commissioning Policy Proposition: Proton Beam Therapy for Cancer of the Prostate Reference: NHS England B01X09 First published: March 2016 Prepared by NHS England Specialised Services Clinical
PARTICLES. The deadline for the next newsletter is November , so that Particles 9 can come out in January Address all correspondence to:
 PARTICLES sponsored by P ROTON T C O G HERAPY O- PERATIVE ROUP for those interested in proton, light ion and heavy charged particle radiotherapy. A Newsletter Number 8 June 1991 Editor: Janet Sisterson
PARTICLES sponsored by P ROTON T C O G HERAPY O- PERATIVE ROUP for those interested in proton, light ion and heavy charged particle radiotherapy. A Newsletter Number 8 June 1991 Editor: Janet Sisterson
Advances in external beam radiotherapy
 International Conference on Modern Radiotherapy: Advances and Challenges in Radiation Protection of Patients Advances in external beam radiotherapy New techniques, new benefits and new risks Michael Brada
International Conference on Modern Radiotherapy: Advances and Challenges in Radiation Protection of Patients Advances in external beam radiotherapy New techniques, new benefits and new risks Michael Brada
Jefferies Healthcare Conference
 Jefferies Healthcare Conference Jean-Marc BOTHY - CSO June 8, 2017 2017 IBA SA Disclaimer This presentation may contain forward-looking statements concerning industry outlook, including growth drivers;
Jefferies Healthcare Conference Jean-Marc BOTHY - CSO June 8, 2017 2017 IBA SA Disclaimer This presentation may contain forward-looking statements concerning industry outlook, including growth drivers;
Radiation qualities in carbon-ion radiotherapy at NIRS/HIMAC
 Radiation qualities in carbon-ion radiotherapy at NIRS/ Shunsuke YONAI Radiological Protection Section Research Center for Charged Particle Therapy National Institute of Radiological Sciences (NIRS) E-mail:
Radiation qualities in carbon-ion radiotherapy at NIRS/ Shunsuke YONAI Radiological Protection Section Research Center for Charged Particle Therapy National Institute of Radiological Sciences (NIRS) E-mail:
SHIELDING TECHNIQUES FOR CURRENT RADIATION THERAPY MODALITIES
 SHIELDING TECHNIQUES FOR CURRENT RADIATION THERAPY MODALITIES MELISSA C. MARTIN, M.S., FACR, FAAPM PRESIDENT AAPM - 2017 PRESIDENT - THERAPY PHYSICS INC., GARDENA, CA MELISSA@THERAPYPHYSICS.COM AAPM Spring
SHIELDING TECHNIQUES FOR CURRENT RADIATION THERAPY MODALITIES MELISSA C. MARTIN, M.S., FACR, FAAPM PRESIDENT AAPM - 2017 PRESIDENT - THERAPY PHYSICS INC., GARDENA, CA MELISSA@THERAPYPHYSICS.COM AAPM Spring
A brief presentation of The TERA Foundation
 A brief presentation of The TERA Foundation David Watts on behalf of Prof. Ugo Amaldi and all my colleagues at TERA TERA Overview Direction: Prof. Ugo Amaldi AQUA (Advanced QUAlity Assurance) Cyclinac
A brief presentation of The TERA Foundation David Watts on behalf of Prof. Ugo Amaldi and all my colleagues at TERA TERA Overview Direction: Prof. Ugo Amaldi AQUA (Advanced QUAlity Assurance) Cyclinac
Review of Hadron machines for cancer therapy
 Review of Hadron machines for cancer therapy M. Kanazawa NIRS cancer therapy with hadron (p, C) Clinical studies at New ideas of accelerators Compact facilities (p, C) Depth dose distribution Carbon, proton
Review of Hadron machines for cancer therapy M. Kanazawa NIRS cancer therapy with hadron (p, C) Clinical studies at New ideas of accelerators Compact facilities (p, C) Depth dose distribution Carbon, proton
Status of Hadrontherapy facilities worldwide
 Status of Hadrontherapy facilities worldwide Vienna 15.03.2011 The Gantry 1 of PSI Eros Pedroni Center for Proton Radiation Therapy Paul Scherrer Institute SWITZERLAND Author s competence: Gantry with
Status of Hadrontherapy facilities worldwide Vienna 15.03.2011 The Gantry 1 of PSI Eros Pedroni Center for Proton Radiation Therapy Paul Scherrer Institute SWITZERLAND Author s competence: Gantry with
ACCELERATORS FOR HADRONTHERAPY
 ACCELERATORS FOR HADRONTHERAPY Alberto Degiovanni CERN-BE IVICFA s Fridays: Medical Physics Valencia, 31.10.2014 Introduction: the icon of hadrontherapy Position of the Bragg peak depends on beam energy
ACCELERATORS FOR HADRONTHERAPY Alberto Degiovanni CERN-BE IVICFA s Fridays: Medical Physics Valencia, 31.10.2014 Introduction: the icon of hadrontherapy Position of the Bragg peak depends on beam energy
Planning for the Installation of a Compact Superconducting Proton Therapy Unit in a Busy Medical Center Environment
 Planning for the Installation of a Compact Superconducting Proton Therapy Unit in a Busy Medical Center Environment Barry W. Wessels, Ph.D. Director of Medical Physics and Dosimetry Case Western Reserve
Planning for the Installation of a Compact Superconducting Proton Therapy Unit in a Busy Medical Center Environment Barry W. Wessels, Ph.D. Director of Medical Physics and Dosimetry Case Western Reserve
NUCLEAR PHYSICS FOR MEDICINE - HADRON THERAPY. Pawel Olko Institute of Nuclear Physics Krakow Poland
 NUCLEAR PHYSICS FOR MEDICINE - HADRON THERAPY Pawel Olko Institute of Nuclear Physics Krakow Poland The NuPECC report: Nuclear Physics in Medicine http://www.nupecc.org/pub/npmed2014.pdf Outline 1. Why
NUCLEAR PHYSICS FOR MEDICINE - HADRON THERAPY Pawel Olko Institute of Nuclear Physics Krakow Poland The NuPECC report: Nuclear Physics in Medicine http://www.nupecc.org/pub/npmed2014.pdf Outline 1. Why
Electron therapy Class 3: Clinical procedures
 Electron therapy Class 3: Clinical procedures Laurence Court lecourt@mdanderson.org Reference: Faiz M. Khan, The Physics of Radiation Therapy Slide acknowledgements: Karl Prado, Rebecca Howell, Kent Gifford,
Electron therapy Class 3: Clinical procedures Laurence Court lecourt@mdanderson.org Reference: Faiz M. Khan, The Physics of Radiation Therapy Slide acknowledgements: Karl Prado, Rebecca Howell, Kent Gifford,
Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana
 University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
Mitsubishi Heavy Industries Technical Review Vol. 51 No. 1 (March 2014)
 The Challenge of Innovative Cancer Treatments Enabled by Vero4DRT -Development of High-precision Dose Delivery Features for Reducing Radiation Exposure of Healthy Tissue- 76 YASUNOBU SUZUKI *1 KUNIO TAKAHASHI
The Challenge of Innovative Cancer Treatments Enabled by Vero4DRT -Development of High-precision Dose Delivery Features for Reducing Radiation Exposure of Healthy Tissue- 76 YASUNOBU SUZUKI *1 KUNIO TAKAHASHI
Klinikleitung: Dr. Kessler Dr. Kosfeld Dr. Tassani-Prell Dr. Bessmann. Radiotherapy in feline and canine head and neck cancer.
 Radiotherapy in feline and canine head and neck cancer Bettina Kandel Like surgery radiotherapy is usually a localized type of treatment. Today it is more readily available for the treatment of cancer
Radiotherapy in feline and canine head and neck cancer Bettina Kandel Like surgery radiotherapy is usually a localized type of treatment. Today it is more readily available for the treatment of cancer
Specifics of treatment planning for active scanning and IMPT
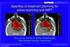 Specifics of treatment planning for active scanning and IMPT SFUD IMPT Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Treatment planning for scanning 1. Single Field,
Specifics of treatment planning for active scanning and IMPT SFUD IMPT Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Treatment planning for scanning 1. Single Field,
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Modern Hadron Therapy Gantry Developments. 16th Jan 2014
 Modern Hadron Therapy Gantry Developments 16th Jan 2014 Protect, Enhance, and Save Lives - 2 - IBA ProteusONE THE TREND: MORE COMPACT, CHEAPER Access to PT is key ProteusPLUS ProteusONE 18000 ft² / 1672
Modern Hadron Therapy Gantry Developments 16th Jan 2014 Protect, Enhance, and Save Lives - 2 - IBA ProteusONE THE TREND: MORE COMPACT, CHEAPER Access to PT is key ProteusPLUS ProteusONE 18000 ft² / 1672
First, how does radiation work?
 Hello, I am Prajnan Das, Faculty Member in the Department of Radiation Oncology at The University of Texas MD Anderson Cancer Center. We are going to talk today about some of the basic principles regarding
Hello, I am Prajnan Das, Faculty Member in the Department of Radiation Oncology at The University of Texas MD Anderson Cancer Center. We are going to talk today about some of the basic principles regarding
Colorectal Cancer Treatment
 Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Workshop on Hadron Beam Therapy of Cancer Erice, Sicily April 24-May
 IONTRIS Synchrotron based PT Solutions from Siemens AG Workshop on Hadron Beam Therapy of Cancer Erice, Sicily April 24-May 1 2009 Matthias Herforth VP Business Development and Communications Siemens AG
IONTRIS Synchrotron based PT Solutions from Siemens AG Workshop on Hadron Beam Therapy of Cancer Erice, Sicily April 24-May 1 2009 Matthias Herforth VP Business Development and Communications Siemens AG
Leksell Gamma Knife Icon. Treatment information
 Leksell Gamma Knife Icon Treatment information You may be feeling frightened or overwhelmed by your recent diagnosis. It can be confusing trying to process a diagnosis, understand a new and challenging
Leksell Gamma Knife Icon Treatment information You may be feeling frightened or overwhelmed by your recent diagnosis. It can be confusing trying to process a diagnosis, understand a new and challenging
Hong Kong Sanatorium & Hospital Introduces First-in-Asia TomoHD System
 For Immediate Release Hong Kong Sanatorium & Hospital Introduces First-in-Asia TomoHD System (8 March 2011, Hong Kong) Hong Kong Sanatorium & Hospital (HKSH) announces today the introduction of the first-in-asia
For Immediate Release Hong Kong Sanatorium & Hospital Introduces First-in-Asia TomoHD System (8 March 2011, Hong Kong) Hong Kong Sanatorium & Hospital (HKSH) announces today the introduction of the first-in-asia
REVIEW ON CYCLOTRONS FOR CANCER THERAPY
 FRM1CIO01 Proceedings of CYCLOTRONS 2010, Lanzhou, China REVIEW ON CYCLOTRONS FOR CANCER THERAPY Yves Jongen#, IBA, Louvain-la-Neuve, Belgium Abstract The science and technology of proton and carbon therapy
FRM1CIO01 Proceedings of CYCLOTRONS 2010, Lanzhou, China REVIEW ON CYCLOTRONS FOR CANCER THERAPY Yves Jongen#, IBA, Louvain-la-Neuve, Belgium Abstract The science and technology of proton and carbon therapy
Quality Assurance of TPS: comparison of dose calculation for stereotactic patients in Eclipse and iplan RT Dose
 Petrovic B Comparison of dose calculation algorithms for stereotaxy Quality Assurance of TPS: comparison of dose calculation for stereotactic patients in and RT Dose Borislava Petrovic 1, Aleksandra Grządziel
Petrovic B Comparison of dose calculation algorithms for stereotaxy Quality Assurance of TPS: comparison of dose calculation for stereotactic patients in and RT Dose Borislava Petrovic 1, Aleksandra Grządziel
MEDICAL MANAGEMENT POLICY
 PAGE: 1 of 8 This medical policy is not a guarantee of benefits or coverage, nor should it be deemed as medical advice. In the event of any conflict concerning benefit coverage, the employer/member summary
PAGE: 1 of 8 This medical policy is not a guarantee of benefits or coverage, nor should it be deemed as medical advice. In the event of any conflict concerning benefit coverage, the employer/member summary
IMPT with Carbon Ions
 IMPT with Carbon Ions PTCOG 48, Heidelberg, 28.09.-03.10.2009 Malte Ellerbrock Medical Physics Expert Heidelberg Ion-Beam Therapy Center HIT Betriebs GmbH am Universitätsklinikum Heidelberg http://www.hit-centrum.de
IMPT with Carbon Ions PTCOG 48, Heidelberg, 28.09.-03.10.2009 Malte Ellerbrock Medical Physics Expert Heidelberg Ion-Beam Therapy Center HIT Betriebs GmbH am Universitätsklinikum Heidelberg http://www.hit-centrum.de
PHYS 383: Applications of physics in medicine (offered at the University of Waterloo from Jan 2015)
 PHYS 383: Applications of physics in medicine (offered at the University of Waterloo from Jan 2015) Course Description: This course is an introduction to physics in medicine and is intended to introduce
PHYS 383: Applications of physics in medicine (offered at the University of Waterloo from Jan 2015) Course Description: This course is an introduction to physics in medicine and is intended to introduce
Today, I will present the second of the two lectures on neutron interactions.
 Today, I will present the second of the two lectures on neutron interactions. 1 The main goal of this lecture is to tell you a little about clinical neutron therapy, first with fast neutron beams, and
Today, I will present the second of the two lectures on neutron interactions. 1 The main goal of this lecture is to tell you a little about clinical neutron therapy, first with fast neutron beams, and
HEALTH RISKS FROM EXPOSURE TO FAST NEUTRONS. Prof. Marco Durante
 HEALTH RISKS FROM EXPOSURE TO FAST NEUTRONS Prof. Marco Durante Risk from neutrons Risk from exposure to fission spectrum neutrons has been extensively studied in the 60 s at nuclear reactors using animal
HEALTH RISKS FROM EXPOSURE TO FAST NEUTRONS Prof. Marco Durante Risk from neutrons Risk from exposure to fission spectrum neutrons has been extensively studied in the 60 s at nuclear reactors using animal
Understanding Radiation Therapy. For Patients and the Public
 Understanding Radiation Therapy For Patients and the Public Introduction to Radiation Oncology Radiation has been an effective tool for treating cancer for more than 100 years. Radiation oncologists are
Understanding Radiation Therapy For Patients and the Public Introduction to Radiation Oncology Radiation has been an effective tool for treating cancer for more than 100 years. Radiation oncologists are
Clinical Results of Carbon Ion Radiotherapy: The Heidelberg Experience
 Clinical Results of Carbon Ion Radiotherapy: The Heidelberg Experience Stephanie E. Combs, MD Department of Radiation Oncology University of Heidelberg, Germany Carbon ion RT at GSI Active beam delivery
Clinical Results of Carbon Ion Radiotherapy: The Heidelberg Experience Stephanie E. Combs, MD Department of Radiation Oncology University of Heidelberg, Germany Carbon ion RT at GSI Active beam delivery
Chapters from Clinical Oncology
 Chapters from Clinical Oncology Lecture notes University of Szeged Faculty of Medicine Department of Oncotherapy 2012. 1 RADIOTHERAPY Technical aspects Dr. Elemér Szil Introduction There are three possibilities
Chapters from Clinical Oncology Lecture notes University of Szeged Faculty of Medicine Department of Oncotherapy 2012. 1 RADIOTHERAPY Technical aspects Dr. Elemér Szil Introduction There are three possibilities
Radiotherapy physics & Equipments
 Radiotherapy physics & Equipments RAD 481 Lecture s Title: An Overview of Radiation Therapy for Health Care Professionals Dr. Mohammed Emam Vision :IMC aspires to be a leader in applied medical sciences,
Radiotherapy physics & Equipments RAD 481 Lecture s Title: An Overview of Radiation Therapy for Health Care Professionals Dr. Mohammed Emam Vision :IMC aspires to be a leader in applied medical sciences,
Outline. Chapter 12 Treatment Planning Combination of Beams. Opposing pairs of beams. Combination of beams. Opposing pairs of beams
 Chapter 12 Treatment Planning Combination of Beams Radiation Dosimetry I Text: H.E Johns and J.R. Cunningham, The physics of radiology, 4 th ed. http://www.utoledo.edu/med/depts/radther Outline Combination
Chapter 12 Treatment Planning Combination of Beams Radiation Dosimetry I Text: H.E Johns and J.R. Cunningham, The physics of radiology, 4 th ed. http://www.utoledo.edu/med/depts/radther Outline Combination
Applications of Proton Therapy for Breast Cancer
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/applications-protontherapy-breast-cancer/7789/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/applications-protontherapy-breast-cancer/7789/
Radiotherapy and tumours in veterinary practice: part one
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Radiotherapy and tumours in veterinary practice: part one Author : Aleksandra Marcinowska, Jane Dobson Categories : Companion
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Radiotherapy and tumours in veterinary practice: part one Author : Aleksandra Marcinowska, Jane Dobson Categories : Companion
Radiotherapy and Radiosurgery
 RapidArc Radiotherapy and Radiosurgery RapidArc Faster. Sharper. Smarter. * It s true for the latest generation of RapidArc technology, and it can be true for your clinic. The oncology landscape has shifted
RapidArc Radiotherapy and Radiosurgery RapidArc Faster. Sharper. Smarter. * It s true for the latest generation of RapidArc technology, and it can be true for your clinic. The oncology landscape has shifted
What is head and neck cancer? How is head and neck cancer diagnosed and evaluated? How is head and neck cancer treated?
 Scan for mobile link. Head and Neck Cancer Head and neck cancer is a group of cancers that start in the oral cavity, larynx, pharynx, salivary glands, nasal cavity or paranasal sinuses. They usually begin
Scan for mobile link. Head and Neck Cancer Head and neck cancer is a group of cancers that start in the oral cavity, larynx, pharynx, salivary glands, nasal cavity or paranasal sinuses. They usually begin
High-precision Radiotherapy
 High-precision Radiotherapy a report by Professor Cai Grau and Dr Morten Hoyer Department of Oncology, Aarhus University Hospital, Denmark DOI: 10.17925/EOH.2005.0.0.40 Professor Cai Grau Dr Morten Hoyer
High-precision Radiotherapy a report by Professor Cai Grau and Dr Morten Hoyer Department of Oncology, Aarhus University Hospital, Denmark DOI: 10.17925/EOH.2005.0.0.40 Professor Cai Grau Dr Morten Hoyer
Implementing New Technologies for Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Implementing New Technologies for Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Implementation of radiosurgery and SBRT requires a fundamentally sound approach Errors don t blur out
Implementing New Technologies for Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Implementation of radiosurgery and SBRT requires a fundamentally sound approach Errors don t blur out
Clinical Quality Assurance for Particle Therapy Plus ça même Plus
 Clinical Quality Assurance for Particle Therapy Plus ça même Plus Thomas F. DeLaney, MD Medical Director Francis H. Burr Proton Center Massachusetts General Hospital Boston MA Quality Assurance Designed
Clinical Quality Assurance for Particle Therapy Plus ça même Plus Thomas F. DeLaney, MD Medical Director Francis H. Burr Proton Center Massachusetts General Hospital Boston MA Quality Assurance Designed
Stereotactic Radiosurgery. Extracranial Stereotactic Radiosurgery. Linear accelerators. Basic technique. Indications of SRS
 Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
pat hways Medtech innovation briefing Published: 24 August 2018 nice.org.uk/guidance/mib157
 pat hways AlignRT in breast cancer radiotherapy Medtech innovation briefing Published: 24 August 2018 nice.org.uk/guidance/mib157 Summary The technology described in this briefing is the AlignRT patient
pat hways AlignRT in breast cancer radiotherapy Medtech innovation briefing Published: 24 August 2018 nice.org.uk/guidance/mib157 Summary The technology described in this briefing is the AlignRT patient
