Present Status and Future Developments in Proton Therapy
|
|
|
- Toby McBride
- 6 years ago
- Views:
Transcription
1 Present Status and Future Developments in Proton Therapy Alfred R. Smith Department of Radiation Oncology, The University of Texas M. D. Anderson Cancer Center, 1515 Holcombe Blvd., Houston, TX 77030, USA Abstract. Within the past few years, interest in proton therapy has significantly increased. This interest has been generated by a number of factors including: 1) the reporting of positive clinical results using proton beams; 2) approval of reimbursement for delivery of proton therapy; 3) the success of hospital-based proton therapy centers; and 4) the availability of modern, integrated proton therapy technology for hospital-based facilities. In the United States, this increased interest has occurred particularly at the level of smaller academic hospitals, community medical centers, and large private practices; however, interest from large academic centers continues to be strong. Particular interest exists regarding smaller and less-expensive proton therapy systems, especially the so-called single-room systems. In this paper, the advantages and disadvantages of 1-room proton therapy systems will be discussed. The emphasis on smaller and cheaper proton therapy facilities has also generated interest in new proton-accelerating technologies such as superconducting cyclotrons and synchrocyclotrons, laser acceleration, and dielectric-wall accelerators. Superconducting magnets are also being developed to decrease the size and weight of isocentric gantries. Another important technical development is spot-beam scanning, which offers the ability to deliver intensity-modulated proton treatments (IMPT). IMPT has the potential to provide dose distributions that are superior to those for photon intensity modulation techniques (IMXT) and to improve clinical outcomes for patients undergoing cancer therapy. At the present time, only two facilities - one in Europe and one in the United States - have the ability to deliver IMPT treatments, however, within the next year or two several additional facilities are expected to achieve this capability. Keywords: proton therapy, cancer treatment, proton accelerators, proton therapy technology PACS: xj, Jw, bd INTRODUCTION Among major cancer sites (head and neck, gastrointestinal, gynecologic, and genitourinary tracts; lung, breast, lymphoma, skin, bone, soft tissue, and brain) treated with radiation therapy, approximately 35% of deaths from cancer are caused by the inability to locally control the tumor. The primary cause of failure of local treatment is the inability to deliver a lethal dose of radiation to the tumor cells; the reasons for this problem include: Inability to determine the exact location and extent of tumor cells and their routes of spread Failure to properly diagnose and treat the disease Presence of radio-resistant tumor cells Proximity of dose-limiting normal tissues and organs 426
2 Limitations in the dose distribution of radiation beams used for treatment The solutions to the above problems are multifaceted and complex. We will focus on the last two problems, which can be addressed to a great extent by the use of radiation beams having highly localized dose distributions that permit the delivery to the target volume of sufficiently high dose of radiation to eradicate the tumor and at the same time irradiate adjacent normal tissues at a level that does not exceed their tolerance threshold. Proton beams have the characteristic Bragg peak in their depth-dose distribution. By proper energy/dose modulation and beam-shaping, proton beams can provide a dose distribution in a patient that is highly conformal to the tumor target and thereby has the potential to deliver a high dose of radiation to the tumor, a low dose to normal tissues proximal to the tumor, and no dose distal from the tumor, as illustrated in Fig. 1. Photons 15 MV Photons vs. SOBP Protons Optimum dose distribution Protons FIGURE 1. This figure illustrates how a properly shaped proton dose distribution can be formed to deliver a high dose of radiation to the tumor volume while not exceeding the tolerable dose of nearby critical normal tissues. In contrast, the photon depth-dose distribution delivers its maximum dose of radiation at shallow tumor depths, a lower dose at the tumor, and a significant dose to normal tissues distal from the tumor. The optimum dose distribution, indicated by the box over the tumor, delivers the entire dose to the tumor and no dose to normal tissues. The proton beam more nearly approaches the optimum dose distribution than does the photon beam. One should note that in general, radiation treatments use multiple treatment beams that come from several directions and are focused on the tumor volume. In this approach the tumor dose can be increased without an equivalent increase in normal tissue dose. The advantages shown in Fig. 1 for the proton beam hold true for every beam used, and therefore, when equal numbers of beams are used in equally optimized treatment plans, protons will provide superior dose distributions. Improved dose localization is the basis for the hypothesis that proton-beam radiation therapy has the potential to improve clinical outcomes in cancer - in 427
3 particular, increased local control of tumors and decreased short- and long-term damage to normal tissues and organs. PRESENT STATUS OF PROTON THERAPY Currently, 28 facilities worldwide treat cancer patients using charged particle (proton and carbon ion) beams. The distribution of particle therapy facilities is as follows: 6 in Japan (4 hospital-based facilities): HIMAC-Chiba, NCC East-Kashiwa, HIBMC-Hyogo, PMRC-Tsukuba, WERC-Wakasa, and Shizuoka Cancer Center 6 in the United States (4 hospital-based): Loma Linda University Medical Center, California; Massachusetts General Hospital, Massachusetts; The University of Texas M. D. Anderson Cancer Center, Texas; University of Florida at Jacksonville, Florida; University of Indiana, Indiana; and University of California at Davis, California 12 in Europe/Russia 4 additional facilities (United Kingdom, China, Korea, South Africa) Worldwide, 22 institutions are developing new proton therapy facilities Approximately 55,000 cancer patients have been treated with proton beams. Three facilities treat cancer patients with carbon ion beams -1 in Germany, and 2 in Japan. A new carbon ion facility is scheduled to open in Heidelberg, Germany, in Several important changes are occurring in proton therapy that will strongly influence the future development of the field. These changes include: Research-based facilities Hospital-based facilities Large facilities Smaller facilities and, particularly in the United States, single-room installations Low-efficiency, low-patient throughput High-efficiency, high-patient throughput Minimal integration Full integration of medical services and information technology within the particle facility and within the larger medical complex Passive-scattering techniques Beam-scanning techniques Conventional accelerators - Superconducting cyclotrons and synchrocyclotrons - Laser acceleration - Dielectric wall acceleration - Fixed-Field Alternating Gradient (FFAG) accelerators Implementation of robotic technologies More carbon ion facilities 428
4 A central theme common to the above trends is the need to reduce the cost of particle therapy to make it more financially competitive with conventional radiation therapy. The most straightforward way to reduce the cost of particle therapy is to reduce the size and complexity of proton therapy technology and to greatly increase the efficiency of operations; that way, more patients can be treated and the high capital costs of proton facilities can be spread among greater numbers of patients. CURRENT PROTON THERAPY TECHNOLOGIES Accelerators that are currently used for proton therapy are synchrotrons, isochronous cyclotrons, and synchrocyclotrons that accelerate protons up to energies of MeV. Proton therapy cyclotrons and synchrocyclotrons have evolved toward smaller and less-expensive devices, as shown in Fig. 2. Commercially Available Cyclotron/Synchrocyclotron Systems IBA C230 First commercially available cyclotron for proton therapy Isochronous cyclotron; 220 tons 230 MeV protons Varian/ACCEL K250 Superconducting isochronous cyclotron 90 tons; diameter = 3.2 m 250 MeV protons, high extraction efficiency Still River Systems, Monarch 250 Superconducting synchrocyclotron 250V Protons 20 tons; diameter = 1.7 m FIGURE 2. This figure shows the recent evolution of proton therapy accelerators. The weight of the newest superconducting device is 10% of that for the first commercial proton therapy cyclotron. Implementation of super-conducting technology has resulted in accelerators that have decreased in weight - from 220 tons in 1995 to 20 tons in and in size, accordingly. Importantly, the 20-ton accelerator can be mounted on an isocentric gantry that moves the accelerator around the patient, thus eliminating the need for an accelerator vault external to the treatment room and for expensive beam-transport lines. 429
5 The volume of shielding required for the facility, and its cost, will also decrease. Downsizing the accelerator so that it can fit inside the treatment room with the gantry also makes possible a single-room proton therapy system that can be situated more easily in a standard radiation therapy facility. It should be noted, however, that significant challenges are inherent in making such systems less expensive per treatment room than for larger facilities that have one accelerator feeding several treatment rooms. Overall costs of equipment and its maintenance for a facility having multiple treatment rooms may be reduced when one accelerator feeds several treatment rooms rather than having an accelerator for each treatment room. Superconducting technology also has been applied to the large bending magnets on isocentric gantries, dramatically reducing the weight and size of the overall gantry. For example, the carbon ion gantry at the new particle facility being built in Heidelberg, Germany, weighs 600 tons, whereas a carbon ion gantry with superconducting magnets (developed by Ion Beam Applications in Belgium) has a rotating mass of only 120 tons. Current proton gantries range in weight from about 120 to 190 tons. Superconducting technology has also enabled the design of compact cyclotrons for carbon ion acceleration. Superconducting technology may make it possible to build carbon ion facilities, which also deliver proton beams, similar in size to present-day proton facilities. To date, almost all proton treatments have used passive-scattering systems, whereby a small pencil beam entering a treatment delivery nozzle is spread out laterally by double-scattering techniques [1]. A range-modulation wheel or ridge filter modulates the energy (beam penetration) and beam weights to uniformly spread the stopping distribution of the beam in the patient. This spreading technique results in a spread-out-bragg-peak (SOBP), which has a depth dimension determined by the greatest water-equivalent thickness of the tumor target volume. Fig. 3 illustrates this concept. In the proton treatments described above, a treatment field-specific collimator is used between the nozzle exit and the patient surface to shape the field laterally to conform to the maximum beam s-eye view extent of the target volume. A range compensator also is used to correct for the patient s surface irregularities, density heterogeneities in the beam path, and changes in the shape of the distal target volume surface. The size of the SOBP is chosen to cover the greatest thickness of the target volume in the beam direction. The SOBP size is constant over the entire target volume, and therefore there is generally some pull back of the high-dose region into normal tissues proximal to the target volume (Figure 3). This dose pull back into normal tissues is a primary drawback to passive scattering techniques. The general use of several treatment fields, where the dose pull back for each field does not overlap with that of other fields, reduces the relative-dose impact to normal tissues. Another major disadvantage of this technique is its inefficiency - many protons are lost in the process of scattering and collimating the beam, and these interactions produce neutrons, which have the potential to induce unwanted biological effects in patients, such as secondary tumors, that occur many years after their initial cancer treatment. 430
6 Treatment Nozzle Beam monitors FIGURE 3. Illustration of the passive-scattering treatment technique commonly used for proton therapy. The second type of beam delivery utilizes spot scanning techniques (often called pencil beam scanning) [2]. Fig. 4 illustrates how a target can be scanned by placing Bragg peaks throughout the target volume using scanning magnets and energy changes. Energy changes in scanning techniques can be carried out with various methods including: 1) energy changes in the accelerator when a synchrotron is used; 2) energy changes made with an energy-selection system when a cyclotron is used; or 3) either of these methods plus energy absorbers in the treatment nozzle. The advantages of beam scanning are: 1) efficient use of protons - except for beam monitors, there are no scattering elements in the nozzle; 2) no neutron production in the nozzle; 3) in general, no requirement of patient-specific appliances (e.g., patientspecific collimators and range compensators); and 4) implementation of intensitymodulated proton treatments (IMPT) that provide optimized-dose distributions. The disadvantages of beam scanning include: 1) increased complexity of treatment planning and delivery; 2) requirement for additional quality assurance methods to ensure accuracy and safety of treatment delivery; and 2) potentially increased treatment errors caused by target motion during treatment. As of this writing, optimized beam scanning for proton-beam treatments is being used at only two facilities: the Paul Scherrer Institute in Switzerland and The University of Texas M. D. Anderson Cancer Center (Houston, Texas, U.S.A.). However, it is anticipated that within the next year, several more facilities will implement optimized-proton treatments utilizing beam-scanning techniques. 431
7 Treatment Nozzle Scanning Magnets Monitor High-density structure Target Volume Scanning Magnets Critical Structure Proton Pencil Beam Body Surface FIGURE 4. Illustration of the beam-scanning (or spot-scanning) treatment technique. NEW TECHNOLOGICAL DEVELOPMENTS The first hospital-based proton therapy system came on line in 1990 at Loma Linda University Medical Center in the United States [3]. Compared with their photon counterparts, proton-therapy systems are in their relative infancy and are still undergoing significant changes as they develop into mature technologies. Also, with the exception of the DICOM-RT-ION data exchange standards, no standards exist for proton therapy-specific clinical systems. Current development efforts are mainly directed toward implementation of advanced beam scanning systems, robotics (for handling patients, imaging devices, and patient appliances), imaging (cone beam computed tomography [CT], positron emission tomography [PET], and proton imaging), upgrades in control and safety systems, and new accelerator technology. The remainder of this paper will focus mainly on accelerator development. As noted above, superconducting technology has been applied to magnets in cyclotrons and synchrocyclotrons resulting in reductions in weight and size to the extent that these accelerators can now be mounted on rotating isocentric gantries. Such installations will cut costs for the accelerators, beam transport systems, and shielding. Currently, there is a great amount of interest in single-room proton therapy systems that will make it possible to implement proton therapy in small community hospitals and large private practices. The advantages of single-room systems include the following: Reduction of capital costs will make it possible to install more facilities and make proton therapy available to a greater number of cancer patients. 432
8 Single-room systems, where each room has a dedicated accelerator, do not have competition for beam time with other treatment rooms, as do larger systems where a single accelerator feeds beam to several treatment rooms. If more than one single-room system is installed, the entire proton treatment capability will not be lost when one accelerator goes down. The potential disadvantages of single-room systems include the following: Neutron shielding around the accelerator may be complex and expensive. Shielding requirements will be stringent because the accelerator and energy selection system will be in the same room as patients undergoing treatment. If the demand for proton therapy increases and additional rooms are installed, the single-room cost advantage will be lost. Single-room systems may not be cheaper, per room, than current multiple room systems. A preliminary cost analysis indicates that the equipment for a facility having 4 single-room systems will cost approximately the same as a facility having one accelerator that provides a beam for 4 treatment rooms the primary reason being that for the single-room systems, 4 accelerators would be required instead of 1. Operations and maintenance for multiple single-room systems will be more expensive because more accelerators are involved. The usability, reliability, and maintainability in clinical environments for the new single-room systems have not been determined. An alternative to having a single-room system where the accelerator is attached to the gantry is a compact accelerator installed in a separate room adjacent to the treatment room. This concept is attractive for many reasons including the ability to expand to multiple treatment rooms, reduced neutron production in the treatment room, and easier system maintenance. It should be noted that the advantages and disadvantages listed above are generally true for any single-room system, regardless of the accelerator used. A considerable amount of effort is being directed toward the development of new types of proton therapy accelerators, and these developments are discussed below. New Accelerator Development Fixed-Field Alternating Gradient Accelerators Fixed-field alternating gradient (FFAG) accelerators may be able to replace both cyclotrons and synchrotrons for hadron therapy. FFAG accelerators combine many of the positive features of cyclotrons and synchrotrons with fixed magnetic fields as in cyclotrons and pulsed acceleration as in synchrotrons. FFAG accelerators have the following potential advantages: FFAG accelerators can be cycled faster than synchrotrons and are limited only by the rate of the radiofrequency (RF) modulation. 433
9 Higher-duty factors will permit higher average beam currents and high repetition rates for spot scanning. Fixed fields require simpler and cheaper power supplies and are more easily operated than synchrotrons. With respect to fixed-field cyclotrons, non-scaling FFAG accelerators allow strong focusing and therefore smaller aperture requirements, which lead to low beam losses and better control over the beam. FFAG accelerators (like synchrotrons) have a magnetic ring that allows beam extraction at variable energies rather than just a single energy, as in a cyclotron. Their superconducting magnets and compact size make FFAG accelerators attractive for proton therapy applications. Because of the possibility of changing energy and location with each spot and having a repetition rate of about 100 Hz, spot scanning with FFAG proton beams can be carefully controlled in three dimensions. The FFAG concept was developed in the 1950s in Japan, Russia, and the United States [4]. The first electron FFAG accelerator was developed in the late 1950s, and several others were built in the early 1960s. In the 1980s, proposals for FFAG-based neutron spallation sources were unsuccessful due to the perceived complexity of the magnets. In scaling-type FFAG accelerators, the magnetic field has to be non-linear with zero chromatic beam optics. Because the magnets are complex and expensive to manufacture, the resulting cost has limited their use in medicine. However, new magnet designs have been made possible by 3D magnetic field simulation codes and large-scale computers. In addition, for a proton FFAG, a broad-band and high-gradient RF cavity is required. A new type of RF cavity developed at the High Energy Accelerator Research Organization (KEK) in Japan [5] made it possible to overcome these problems, and in 1999, the first proton FFAG was built at KEK in Japan [6]. This machine was the proof of principle (POP) for proton FFAG accelerators and was named POP-FFAG. After the success of POP-FFAG, a 150-MeV FFAG accelerator was developed at KEK. To date, several FFAG accelerators have been built in the energy range of MeV and others have been proposed. The non-scaling FFAG accelerator was invented in 1999 [7]. This accelerator s magnet design provides a variation of orbit length with energy, which can be arranged to greatly compress the range of the orbit radii and thus the magnet aperture, while maintaining linear magnetic field dependence. In addition, the small apertures and linear fields allow for simplification and cost reduction compared with scaling FFAG accelerators. Keil et al. proposed a hadron cancer therapy system using a non-scaling FFAG accelerator and gantry composed of non-scaling FFAG cells [8]. This accelerator will accelerate carbon ions up to 400 MeV/μ and protons up to 250 MeV. Dielectric Wall Accelerators Conventional proton accelerator cavities have an accelerating field only in their gaps, which occupy only a small fraction of the cavity length and have an accelerating gradient of approximately 1 2 MeV/meter. In contrast, dielectric wall accelerators 434
10 (DWAs) have the potential of producing gradients of approximately 100 MeV/meter. In a DWA, an insulating wall replaces the beam pipe so that protons can be accelerated uniformly over the entire length of the accelerator, yielding a much higher accelerating gradient. The DWA uses fast-switched high-voltage transmission lines to generate pulsed electric fields on the inside of a high gradient insulating (HGI) acceleration tube. High electric field gradients are achieved using alternating insulators and conductors and short pulse times. An electric field propagates down the bore of the accelerator, pushing the proton packet in front of it. The system will produce individual pulses that can be varied in intensity, energy, and spot width and therefore should be suitable for IMPT applications. The enabling technologies for DWA are the HGI, fast SiC switching, and new dielectric materials. The DWA technology is being developed at the Lawrence Livermore Laboratory [9], with a full-scale prototype proton therapy system expected to be operational in approximately 4 or 5 years. The private sector partner for this development is TomoTherapy [10], and the first prototype is expected to be installed at the University of California Davis Cancer Center. Laser Accelerators Laser acceleration will be described briefly in this paper because other papers in these proceedings will address the topic in detail. Proton laser acceleration is achieved by focusing a high-power (approximately W) laser on a thin target, such as a 5 μm-thick titanium foil, or multi-layer targets, such as 100 nm-thick aluminumhydrogen. To achieve proton energies of MeV with adequate intensities focused short laser pulses to intensities of W/cm 2 or higher are required [11]. The short (~ sec) laser pulse width produces a high peak power intensity that causes massive ionization in the target, expelling a large number of relativistic electrons. The sudden loss of electrons gives the target a high-positive charge, and this transient-positive field accelerates protons to high energies. The resultant proton beams have a broad energy spectrum, and therefore a magnetic spectrometer must be used to select a narrow energy band for patient treatment. This selection process throws away about 99.5% of the beam, and thus the energy selection system must be heavily shielded against neutrons resulting from proton losses in the spectrometer. Achieving the energy and beam intensity required for proton therapy is a major challenge. Groups in several countries are working on proton laser acceleration [11-13]; however, because of the technical difficulties, the current development efforts are not expected to be able to achieve the required beams, even for treatment of ocular melanomas (~70 MeV at a dose rate of approximately Gy/min) over the next 5 7 years. Primary Requirements for Proton Therapy Accelerators Regardless of the type of accelerator, all proton therapy accelerators should meet certain basic requirements [14] that include the following: 435
11 Proton energies in the range of 70 MeV to MeV. Energy resolution should be such that changes of penetration of approximately 0.1 g/cm 2 or less are achievable. The goal for energy spread should be approximately 0.1%. Intensity of protons/sec or about 2 nanoamperes of continuous beam, which will produce a dose rate of approximately 2 Gy/min. Rapid energy changes are required. For some intensity modulation techniques (e.g., rapid volumetric repainting) energy changes must occur in time frames less than 150 ms for changes in penetration of 0.5 g/cm 2. Most single-room systems will have the energy selection system near the patient, and therefore adequate neutron shielding will be challenging. Accelerators should be capable of either being mounted on an isocentric gantry or feeding the beam directly into a gantry without long beam-transport lines. Reliability for clinical operations is very important. Clinical systems are required to have 95-98% of up time,16 hours/day, 5 days/week, for at least 50 weeks/year. All treatment parameters should have very high accuracy and precision. In radiation therapy, the goal is to have <5% error in tumor dose (considering all sources of errors), and this degree of accuracy must be reproducible over relatively long periods of time. Control and safety system requirements are very stringent, with triple redundancy required for all critical safety elements. All systems must have clearance from federal agencies, such as the U.S. Food and Drug Administration, in the United States. A pressing need exists for smaller and less-expensive proton therapy systems. Proton therapy has a significant potential to improve clinical outcomes for patients with a broad range of cancers, especially pediatric cancers. Less-expensive systems will enable more particle facilities to be built, which will make proton therapy available to greater numbers of cancer patients. Less-expensive facilities will also make it possible to reduce patient costs for proton therapy. Proton therapy is currently so expensive that most patients who do not have medical insurance, or who live in countries where federally funded health care is not available, cannot afford the cost of treatments. Advancements expected to be made within the next decade should have an appreciable impact on both the quality and cost of proton therapy. REFERENCES 1. W. T. Chu, G. A. Ludewigt, and T. R. Renner, Instrumentation for treatment of cancer using proton and light-ion beams, Rev. Sci. Instrum. 64, (1993). 2. B. Gottschalk and E. Pedroni, Treatment Delivery Systems, in Proton and Charged Particle Radiotherapy, edited by T. F. DeLaney and H. M. Kooy, Lippincott Williams & Wilkins, Philadelphia, 2008, pp J. M. Slater, J. O. Archambeau, D. W. Miller, M. I. Notarus, W. Preston and J. D. Slater, The proton treatment center at Loma Linda University Medical Center, Int. J. Radiat. Oncol. Biol. Phys. 22, (1991). 436
12 4. M. D. Craddock, New concepts in FFAG design for secondary beam facilities and other applications, Proceedings of EPAC 2005, Knoxville, Tennessee, 2005, pp Y. Mori et al., A new type of rf cavity for high intensity proton synchrotron using high permeability magnetic alloy, Proceedings of EPAC 1998, pp Y Sato et al., Development of a FFAG proton synchrotron, Proceeding of EPAC 2000, Vienna, Austria, p C. Johnstone et al., Fixed field circular accelerator designs, in Proceedings of EPAC 1999, New York, pp E. Keil, A. M. Sessler, and D. Trbojevic, Hadron cancer therapy complex using nonscaling fixed field alternating gradient accelerator and gantry design, Phys. Rev. ST Accel. Beams 10, (2007). 9. G. J Caporaso, et al., A compact linac for intensity modulated proton therapy based on a dielectric wall accelerator, Med Phys. 24, (2008). 10. T. R. Mackie et al., A proposal for a novel compact intensity modulated proton therapy system using a dielectric wall accelerator, Med. Phys. 34, 2628 (2007). 11. C.-M. Ma et al., Development of a laser-driven proton accelerator for cancer therapy, Laser Physics 16, 1-8 (2006). 12. E. Fourkal et al., Particle in cell simulation of laser-accelerated proton beams for radiation therapy, Med. Phys. 29, (2002). 13. S. S. Bulanov et al., Accelerating protons to therapeutic energies with ultraintense, ultraclean, and ultrashort laser pulses, Med. Phys. 35, (2008). 14. U. Linz and J. Alonso, What will it take for laser driven proton accelerators to be applied to tumor therapy?, Phys. Rev. ST Accel. Beams 10, (2007). 437
Proton Treatment. Keith Brown, Ph.D., CHP. Associate Director, Radiation Safety University of Pennsylvania
 Proton Treatment Keith Brown, Ph.D., CHP Associate Director, Radiation Safety University of Pennsylvania Proton Dose vs. Depth Wilson,. R.R. Radiological use of fast protons. Radiology 47:487-491, 1946.
Proton Treatment Keith Brown, Ph.D., CHP Associate Director, Radiation Safety University of Pennsylvania Proton Dose vs. Depth Wilson,. R.R. Radiological use of fast protons. Radiology 47:487-491, 1946.
PROGRESS IN HADRONTHERAPY
 PROGRESS IN HADRONTHERAPY Saverio Braccini TERA Foundation for Oncological Hadrontherapy IPRD06 - Siena - 01.10.06 - SB 1 Outline Introduction Radiation therapy with X rays and hadrontherapy Hadrontherapy
PROGRESS IN HADRONTHERAPY Saverio Braccini TERA Foundation for Oncological Hadrontherapy IPRD06 - Siena - 01.10.06 - SB 1 Outline Introduction Radiation therapy with X rays and hadrontherapy Hadrontherapy
SUMITOMO Particle Therapy Technologies
 55 th AAPM annual meeting Particle Beam Therapy Symposium SUMITOMO Particle Therapy Technologies August 3, 2013 Yukio Kumata Experience accelerators for science Current Status proton and carbon Future
55 th AAPM annual meeting Particle Beam Therapy Symposium SUMITOMO Particle Therapy Technologies August 3, 2013 Yukio Kumata Experience accelerators for science Current Status proton and carbon Future
Heavy Ion Tumor Therapy
 Heavy Ion Tumor Therapy Applications Bence Mitlasoczki 25.06.2018 Heidelberg 1. Source (H 2 /CO 2 ) 2. Linac 3. Synchrotron 4. Guide 5. Treatment rooms 6. X-ray system 7. Gantry 8. Treatment room with
Heavy Ion Tumor Therapy Applications Bence Mitlasoczki 25.06.2018 Heidelberg 1. Source (H 2 /CO 2 ) 2. Linac 3. Synchrotron 4. Guide 5. Treatment rooms 6. X-ray system 7. Gantry 8. Treatment room with
Review of Hadron machines for cancer therapy
 Review of Hadron machines for cancer therapy M. Kanazawa NIRS cancer therapy with hadron (p, C) Clinical studies at New ideas of accelerators Compact facilities (p, C) Depth dose distribution Carbon, proton
Review of Hadron machines for cancer therapy M. Kanazawa NIRS cancer therapy with hadron (p, C) Clinical studies at New ideas of accelerators Compact facilities (p, C) Depth dose distribution Carbon, proton
Proton Beam Therapy at Mayo Clinic
 Proton Beam Therapy at Mayo Clinic Jon J. Kruse, Ph.D. Mayo Clinic Dept. of Radiation Oncology Rochester, MN History of Proton Therapy at Mayo 2002: Decided to consider particle therapy analysis and education
Proton Beam Therapy at Mayo Clinic Jon J. Kruse, Ph.D. Mayo Clinic Dept. of Radiation Oncology Rochester, MN History of Proton Therapy at Mayo 2002: Decided to consider particle therapy analysis and education
SCIENTIFIC AND TECHNOLOGICAL DEVELOPMENT OF HADRONTHERAPY
 SCIENTIFIC AND TECHNOLOGICAL DEVELOPMENT OF HADRONTHERAPY SAVERIO BRACCINI * Albert Einstein Centre for Fundamental Physics, Laboratory for High Energy Physics (LHEP), University of Bern, Sidlerstrasse
SCIENTIFIC AND TECHNOLOGICAL DEVELOPMENT OF HADRONTHERAPY SAVERIO BRACCINI * Albert Einstein Centre for Fundamental Physics, Laboratory for High Energy Physics (LHEP), University of Bern, Sidlerstrasse
Characterization and implementation of Pencil Beam Scanning proton therapy techniques: from spot scanning to continuous scanning
 Characterization and implementation of Pencil Beam Scanning proton therapy techniques: from spot scanning to continuous scanning Supervisors Prof. V. Patera PhD R. Van Roermund Candidate Annalisa Patriarca
Characterization and implementation of Pencil Beam Scanning proton therapy techniques: from spot scanning to continuous scanning Supervisors Prof. V. Patera PhD R. Van Roermund Candidate Annalisa Patriarca
Proton Therapy Dosimetry & Clinical Implementation. Baldev Patyal, Ph.D., Chief Medical Physicist Department of Radiation Medicine
 Proton Therapy Dosimetry & Clinical Implementation Baldev Patyal, Ph.D., Chief Medical Physicist Department of Radiation Medicine Outline» Proton Therapy Basics» Why Proton Therapy? (Dosimetric Superiority)»
Proton Therapy Dosimetry & Clinical Implementation Baldev Patyal, Ph.D., Chief Medical Physicist Department of Radiation Medicine Outline» Proton Therapy Basics» Why Proton Therapy? (Dosimetric Superiority)»
Introduction to Ion Beam Cancer Therapy
 Introduction to Ion Beam Cancer Therapy Andrew M. Sessler (with some slides from David Robin) Lawrence Berkeley National Laboratory Berkeley, CA 94720 Cyclotron 10, Lanzhou September 10, 2010 Contents
Introduction to Ion Beam Cancer Therapy Andrew M. Sessler (with some slides from David Robin) Lawrence Berkeley National Laboratory Berkeley, CA 94720 Cyclotron 10, Lanzhou September 10, 2010 Contents
Cancer Treatment by Charged Particles - Carbon Ion Radiotherapy -
 Cancer Treatment by Charged Particles - Carbon Ion Radiotherapy - Takeshi Murakami Research Center of Charged Particle Therapy National Institute of Radiological Sciences 2012.11.21 1. Introduction to
Cancer Treatment by Charged Particles - Carbon Ion Radiotherapy - Takeshi Murakami Research Center of Charged Particle Therapy National Institute of Radiological Sciences 2012.11.21 1. Introduction to
Proton and heavy ion radiotherapy: Effect of LET
 Proton and heavy ion radiotherapy: Effect of LET As a low LET particle traverses a DNA molecule, ionizations are far apart and double strand breaks are rare With high LET particles, ionizations are closer
Proton and heavy ion radiotherapy: Effect of LET As a low LET particle traverses a DNA molecule, ionizations are far apart and double strand breaks are rare With high LET particles, ionizations are closer
Learning Objectives. Clinically operating proton therapy facilities. Overview of Quality Assurance in Proton Therapy. Omar Zeidan
 Overview of Quality Assurance in Proton Therapy Omar Zeidan AAPM 2012 Charlotte, NC July 30 st, 2012 Learning Objectives Understand proton beam dosimetry characteristics and compare them to photon beams
Overview of Quality Assurance in Proton Therapy Omar Zeidan AAPM 2012 Charlotte, NC July 30 st, 2012 Learning Objectives Understand proton beam dosimetry characteristics and compare them to photon beams
Planning for the Installation of a Compact Superconducting Proton Therapy Unit in a Busy Medical Center Environment
 Planning for the Installation of a Compact Superconducting Proton Therapy Unit in a Busy Medical Center Environment Barry W. Wessels, Ph.D. Director of Medical Physics and Dosimetry Case Western Reserve
Planning for the Installation of a Compact Superconducting Proton Therapy Unit in a Busy Medical Center Environment Barry W. Wessels, Ph.D. Director of Medical Physics and Dosimetry Case Western Reserve
New Treatment Research Facility Project at HIMAC
 New Treatment Research Facility Project at Koji Noda Research Center for Charged Particle Therapy National Institute of Radiological Sciences IPAC10, Kyoto, JAPAN, 25th May, 2010 Contents 1. Introduction
New Treatment Research Facility Project at Koji Noda Research Center for Charged Particle Therapy National Institute of Radiological Sciences IPAC10, Kyoto, JAPAN, 25th May, 2010 Contents 1. Introduction
Present status and future of Proton beam therapy
 Present status and future of Proton beam therapy Description At present, the types of proven treatment for cancer are surgery, radiotherapy, and chemotherapy. Depending on the characteristics of cancer
Present status and future of Proton beam therapy Description At present, the types of proven treatment for cancer are surgery, radiotherapy, and chemotherapy. Depending on the characteristics of cancer
State-of-the-art proton therapy: The physicist s perspective
 State-of-the-art proton therapy: Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Overview of presentation 1. State-of-the-art proton delivery 2. Current challenges 3. New
State-of-the-art proton therapy: Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Overview of presentation 1. State-of-the-art proton delivery 2. Current challenges 3. New
III. Proton-therapytherapy. Rome SB - 5/5 1
 Outline Introduction: an historical review I Applications in medical diagnostics Particle accelerators for medicine Applications in conventional radiation therapy II III IV Hadrontherapy, the frontier
Outline Introduction: an historical review I Applications in medical diagnostics Particle accelerators for medicine Applications in conventional radiation therapy II III IV Hadrontherapy, the frontier
Status of Proton Therapy: results and future trends
 Status of Proton Therapy: results and future trends E. Pedroni Paul Scherrer Institute Division of Radiation Medicine CH-5232 Villigen PSI Abstract The number of centres investigating proton therapy in
Status of Proton Therapy: results and future trends E. Pedroni Paul Scherrer Institute Division of Radiation Medicine CH-5232 Villigen PSI Abstract The number of centres investigating proton therapy in
Progress of Heavy Ion Therapy
 Progress of Heavy Ion Therapy Fuminori Soga Division of Accelerator Physics and Engineering, National Institute of Radiological Sciences, 4-9-1 Anagawa. Inage-ku, Chiba 263-8555, Japan 1. Introduction
Progress of Heavy Ion Therapy Fuminori Soga Division of Accelerator Physics and Engineering, National Institute of Radiological Sciences, 4-9-1 Anagawa. Inage-ku, Chiba 263-8555, Japan 1. Introduction
H. Röcken, M. Abdel-Bary, E. Akcöltekin, P. Budz, T. Stephani, J. Wittschen
 : Medical Operation of the 2 nd Machine, Production and Commissioning Status of Machines No. 3 to 7 H. Röcken, M. Abdel-Bary, E. Akcöltekin, P. Budz, T. Stephani, J. Wittschen VARIAN Medical Systems Particle
: Medical Operation of the 2 nd Machine, Production and Commissioning Status of Machines No. 3 to 7 H. Röcken, M. Abdel-Bary, E. Akcöltekin, P. Budz, T. Stephani, J. Wittschen VARIAN Medical Systems Particle
Status of Hadrontherapy facilities worldwide
 Status of Hadrontherapy facilities worldwide Vienna 15.03.2011 The Gantry 1 of PSI Eros Pedroni Center for Proton Radiation Therapy Paul Scherrer Institute SWITZERLAND Author s competence: Gantry with
Status of Hadrontherapy facilities worldwide Vienna 15.03.2011 The Gantry 1 of PSI Eros Pedroni Center for Proton Radiation Therapy Paul Scherrer Institute SWITZERLAND Author s competence: Gantry with
Modern Hadron Therapy Gantry Developments. 16th Jan 2014
 Modern Hadron Therapy Gantry Developments 16th Jan 2014 Protect, Enhance, and Save Lives - 2 - IBA ProteusONE THE TREND: MORE COMPACT, CHEAPER Access to PT is key ProteusPLUS ProteusONE 18000 ft² / 1672
Modern Hadron Therapy Gantry Developments 16th Jan 2014 Protect, Enhance, and Save Lives - 2 - IBA ProteusONE THE TREND: MORE COMPACT, CHEAPER Access to PT is key ProteusPLUS ProteusONE 18000 ft² / 1672
ABSTRACTS. of the NIRS International Seminar on the Heavy Charged Particle Therapy for Cancer and the XXVII PTCOG MEETING.
 P ROTON THERAPY C O- OPERATIVE GROUP Chair Michael Goitein Ph. D. Department of Radiation Oncology Massachusetts General Hospital Boston MA 02114 (617) 724-9529 (617) 724-9532 Fax Secret ary Janet Sisterson
P ROTON THERAPY C O- OPERATIVE GROUP Chair Michael Goitein Ph. D. Department of Radiation Oncology Massachusetts General Hospital Boston MA 02114 (617) 724-9529 (617) 724-9532 Fax Secret ary Janet Sisterson
Plans for the Precision Cancer Medicine Institute University of Oxford
 Plans for the Precision Cancer Medicine Institute University of Oxford STFC & Particle Accelerators and Beams group workshop on particle accelerators for medicine 17 th February 2015 Claire Timlin The
Plans for the Precision Cancer Medicine Institute University of Oxford STFC & Particle Accelerators and Beams group workshop on particle accelerators for medicine 17 th February 2015 Claire Timlin The
The Heidelberg Ion Therapy Center. Thomas Haberer Heidelberg Ion Therapy Center Hadron Therapy Workshop, Erice 2009
 The Heidelberg Ion Therapy Center Thomas Haberer Heidelberg Ion Therapy Center Hadron Therapy Workshop, Erice 2009 Goal The key element to improve the clinical outcome is local l control! entrance channel:
The Heidelberg Ion Therapy Center Thomas Haberer Heidelberg Ion Therapy Center Hadron Therapy Workshop, Erice 2009 Goal The key element to improve the clinical outcome is local l control! entrance channel:
Basic Press Information
 Basic Press Information Contact MedAustron EBG MedAustron GmbH Marie Curie-Strasse 5 A-2700 Wiener Neustadt Austria T +43 2622 26 100-0 e-mail: office@medaustron.at Internet: www.medaustron.at Press contact:
Basic Press Information Contact MedAustron EBG MedAustron GmbH Marie Curie-Strasse 5 A-2700 Wiener Neustadt Austria T +43 2622 26 100-0 e-mail: office@medaustron.at Internet: www.medaustron.at Press contact:
A review of cyclotrons for Hadron Therapy. Y. Jongen Cyclotrons 2010 Lanzhou, September
 A review of cyclotrons for Hadron Therapy Y. Jongen Cyclotrons 2010 Lanzhou, September 10 2010 The early days The possible use of the Bragg peak of high energy ions in the radiotherapy of cancer was suggested
A review of cyclotrons for Hadron Therapy Y. Jongen Cyclotrons 2010 Lanzhou, September 10 2010 The early days The possible use of the Bragg peak of high energy ions in the radiotherapy of cancer was suggested
The Advantages of Particle Therapy and the Status of the Heidelberg Iontherapy Center
 The Advantages of Particle Therapy and the Status of the Heidelberg Iontherapy Center Thomas Haberer, Scientific Technical Director, Heidelberg Ion Therapy Center Situation / Indications 2/3 patients suffer
The Advantages of Particle Therapy and the Status of the Heidelberg Iontherapy Center Thomas Haberer, Scientific Technical Director, Heidelberg Ion Therapy Center Situation / Indications 2/3 patients suffer
HIMAC AND MEDICAL ACCELERATOR PROJECTS IN JAPAN
 HIMAC AND MEDICAL ACCELERATOR PROJECTS IN JAPAN S. Yamada, T. Honma, M. Kanazawa, A. Kitagawa, S. Kouda, M. Kumada, T. Murakami, M. Muramatsu, T. Nishio, K. Noda, Y. Sato, M. Suda and E. Takada, Research
HIMAC AND MEDICAL ACCELERATOR PROJECTS IN JAPAN S. Yamada, T. Honma, M. Kanazawa, A. Kitagawa, S. Kouda, M. Kumada, T. Murakami, M. Muramatsu, T. Nishio, K. Noda, Y. Sato, M. Suda and E. Takada, Research
Applications of Particle Accelerators
 Applications of Particle Accelerators Prof. Rob Edgecock STFC Rutherford Appleton Laboratory EMMA Accelerator at Daresbury Laboratory Applications >30000 accelerators in use world-wide: 44% for radiotherapy
Applications of Particle Accelerators Prof. Rob Edgecock STFC Rutherford Appleton Laboratory EMMA Accelerator at Daresbury Laboratory Applications >30000 accelerators in use world-wide: 44% for radiotherapy
Nuclear Physics in Proton Radiotherapy
 Nuclear Physics in Proton Radiotherapy Cynthia Keppel, PhD Thomas Jefferson National Accelerator Facility (Hampton University Proton Therapy institute) International Nuclear Physics Conference Adelaide,
Nuclear Physics in Proton Radiotherapy Cynthia Keppel, PhD Thomas Jefferson National Accelerator Facility (Hampton University Proton Therapy institute) International Nuclear Physics Conference Adelaide,
Practical Challenges and Opportunities for Proton Beam Therapy. M. F. Moyers Loma Linda University Medical Center
 Practical Challenges and Opportunities for Proton Beam Therapy M. F. Moyers Loma Linda University Medical Center Outline I. Introduction II. Registration and Immobilization III. Beam Shaping IV. Localization
Practical Challenges and Opportunities for Proton Beam Therapy M. F. Moyers Loma Linda University Medical Center Outline I. Introduction II. Registration and Immobilization III. Beam Shaping IV. Localization
Considerations when treating lung cancer with passive scatter or active scanning proton therapy
 Mini-Review Considerations when treating lung cancer with passive scatter or active scanning proton therapy Sara St. James, Clemens Grassberger, Hsiao-Ming Lu Department of Radiation Oncology, Massachusetts
Mini-Review Considerations when treating lung cancer with passive scatter or active scanning proton therapy Sara St. James, Clemens Grassberger, Hsiao-Ming Lu Department of Radiation Oncology, Massachusetts
HEAVY PARTICLE THERAPY
 HEAVY PARTICLE THERAPY DR. G.V. GIRI KIDWAI MEMORIAL INSTITUTE OF ONCOLOGY ICRO 2012 BHATINDA HEAVY PARTICLES USED IN A EFFORT TO IMPROVE TUMOR CONTROL, THAT DO NOT RESPOND TO PHOTONS OR ELECTRONS BETTER
HEAVY PARTICLE THERAPY DR. G.V. GIRI KIDWAI MEMORIAL INSTITUTE OF ONCOLOGY ICRO 2012 BHATINDA HEAVY PARTICLES USED IN A EFFORT TO IMPROVE TUMOR CONTROL, THAT DO NOT RESPOND TO PHOTONS OR ELECTRONS BETTER
An Introduction to Cancer Therapy With Hadron Radiation
 An Introduction to Cancer Therapy With Hadron Radiation Andrew M. Sessler Lawrence Berkeley National Laboratory Berkeley, CA 94720 April, 2008 Contents 1. History 2. X-Ray Machines 3. Why Hadrons? Which
An Introduction to Cancer Therapy With Hadron Radiation Andrew M. Sessler Lawrence Berkeley National Laboratory Berkeley, CA 94720 April, 2008 Contents 1. History 2. X-Ray Machines 3. Why Hadrons? Which
8/1/2016. Motion Management for Proton Lung SBRT. Outline. Protons and motion. Protons and Motion. Proton lung SBRT Future directions
 Motion Management for Proton Lung SBRT AAPM 2016 Outline Protons and Motion Dosimetric effects Remedies and mitigation techniques Proton lung SBRT Future directions Protons and motion Dosimetric perturbation
Motion Management for Proton Lung SBRT AAPM 2016 Outline Protons and Motion Dosimetric effects Remedies and mitigation techniques Proton lung SBRT Future directions Protons and motion Dosimetric perturbation
A TREATMENT PLANNING STUDY COMPARING VMAT WITH 3D CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER USING PINNACLE PLANNING SYSTEM *
 Romanian Reports in Physics, Vol. 66, No. 2, P. 394 400, 2014 A TREATMENT PLANNING STUDY COMPARING VMAT WITH 3D CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER USING PINNACLE PLANNING SYSTEM * D. ADAM 1,2,
Romanian Reports in Physics, Vol. 66, No. 2, P. 394 400, 2014 A TREATMENT PLANNING STUDY COMPARING VMAT WITH 3D CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER USING PINNACLE PLANNING SYSTEM * D. ADAM 1,2,
REVIEW ON CYCLOTRONS FOR CANCER THERAPY
 FRM1CIO01 Proceedings of CYCLOTRONS 2010, Lanzhou, China REVIEW ON CYCLOTRONS FOR CANCER THERAPY Yves Jongen#, IBA, Louvain-la-Neuve, Belgium Abstract The science and technology of proton and carbon therapy
FRM1CIO01 Proceedings of CYCLOTRONS 2010, Lanzhou, China REVIEW ON CYCLOTRONS FOR CANCER THERAPY Yves Jongen#, IBA, Louvain-la-Neuve, Belgium Abstract The science and technology of proton and carbon therapy
PHYS 383: Applications of physics in medicine (offered at the University of Waterloo from Jan 2015)
 PHYS 383: Applications of physics in medicine (offered at the University of Waterloo from Jan 2015) Course Description: This course is an introduction to physics in medicine and is intended to introduce
PHYS 383: Applications of physics in medicine (offered at the University of Waterloo from Jan 2015) Course Description: This course is an introduction to physics in medicine and is intended to introduce
Economic Implications of Advancements in Radiation Technology. Dramatic Growth of RT Capacity in the US
 Economic Implications of Advancements in Radiation Technology Sponsored by: OTN Anthony M. Berson, M.D. Radiation Oncology, St. Vincent s Comprehensive Cancer Center Richard Emery Vice President, Aptium
Economic Implications of Advancements in Radiation Technology Sponsored by: OTN Anthony M. Berson, M.D. Radiation Oncology, St. Vincent s Comprehensive Cancer Center Richard Emery Vice President, Aptium
A brief presentation of The TERA Foundation
 A brief presentation of The TERA Foundation David Watts on behalf of Prof. Ugo Amaldi and all my colleagues at TERA TERA Overview Direction: Prof. Ugo Amaldi AQUA (Advanced QUAlity Assurance) Cyclinac
A brief presentation of The TERA Foundation David Watts on behalf of Prof. Ugo Amaldi and all my colleagues at TERA TERA Overview Direction: Prof. Ugo Amaldi AQUA (Advanced QUAlity Assurance) Cyclinac
A BETTER TOMORROW STARTS WITH THE BEST OF TODAY PATIENT BROCHURE
 A BETTER TOMORROW STARTS WITH THE BEST OF TODAY PATIENT BROCHURE 1 WELCOME TO THE CALIFORNIA PROTONS CANCER TREATMENT CENTER Patient Care is at the Center of Everything We Do Located in San Diego, California
A BETTER TOMORROW STARTS WITH THE BEST OF TODAY PATIENT BROCHURE 1 WELCOME TO THE CALIFORNIA PROTONS CANCER TREATMENT CENTER Patient Care is at the Center of Everything We Do Located in San Diego, California
Particle Therapy Systems by Mitsubishi Electric DG1101-KM-0034
 Particle Therapy Systems by Mitsubishi Electric DG1101-KM-0034 Saudi-Japan Business Opportunities Forum February 1 2, 2012 1 2 Types of Treatment Conventional Radiation Therapy Uses photons (energetic
Particle Therapy Systems by Mitsubishi Electric DG1101-KM-0034 Saudi-Japan Business Opportunities Forum February 1 2, 2012 1 2 Types of Treatment Conventional Radiation Therapy Uses photons (energetic
High brightness electron beam for radiation therapy A new approach
 High brightness electron beam for radiation therapy A new approach Wei Gai ( 盖炜 ) Engineering Physics Department, Tsinghua University, Beijing, China Argonne National Laboratory, Argonne, IL 60439, USA
High brightness electron beam for radiation therapy A new approach Wei Gai ( 盖炜 ) Engineering Physics Department, Tsinghua University, Beijing, China Argonne National Laboratory, Argonne, IL 60439, USA
AMERICAN BRAIN TUMOR ASSOCIATION. Proton Therapy
 AMERICAN BRAIN TUMOR ASSOCIATION Proton Therapy ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit
AMERICAN BRAIN TUMOR ASSOCIATION Proton Therapy ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit
Intensity Modulated RadioTherapy
 Intensity Modulated RadioTherapy A clinical application of a small accelerator University Medical Center Groningen A.A. van t Veld PhD I. Hoveijn PhD part 1 part2 CERN/KVI accelerator school, Zeegse, June
Intensity Modulated RadioTherapy A clinical application of a small accelerator University Medical Center Groningen A.A. van t Veld PhD I. Hoveijn PhD part 1 part2 CERN/KVI accelerator school, Zeegse, June
*Chien-Yi Yeh, Ji-Hong Hong * 葉健一洪志宏
 林口 Proton Therapy in Ti Taiwan *Chien-Yi Yeh, Ji-Hong Hong * 葉健一洪志宏 Chang Gung Memorial Hospital at Lin-Kou, Taiwan 林口長庚紀念醫院 OCPA2010 at Beijing, China Aug. 5, 2010 Outline 1. The principle of proton radiotherapy
林口 Proton Therapy in Ti Taiwan *Chien-Yi Yeh, Ji-Hong Hong * 葉健一洪志宏 Chang Gung Memorial Hospital at Lin-Kou, Taiwan 林口長庚紀念醫院 OCPA2010 at Beijing, China Aug. 5, 2010 Outline 1. The principle of proton radiotherapy
SHIELDING TECHNIQUES FOR CURRENT RADIATION THERAPY MODALITIES
 SHIELDING TECHNIQUES FOR CURRENT RADIATION THERAPY MODALITIES MELISSA C. MARTIN, M.S., FACR, FAAPM PRESIDENT AAPM - 2017 PRESIDENT - THERAPY PHYSICS INC., GARDENA, CA MELISSA@THERAPYPHYSICS.COM AAPM Spring
SHIELDING TECHNIQUES FOR CURRENT RADIATION THERAPY MODALITIES MELISSA C. MARTIN, M.S., FACR, FAAPM PRESIDENT AAPM - 2017 PRESIDENT - THERAPY PHYSICS INC., GARDENA, CA MELISSA@THERAPYPHYSICS.COM AAPM Spring
ADVANCES IN RADIATION TECHNOLOGIES IN THE TREATMENT OF CANCER
 ADVANCES IN RADIATION TECHNOLOGIES IN THE TREATMENT OF CANCER Bro. Dr. Collie Miller IARC/WHO Based on trends in the incidence of cancer, the International Agency for Research on Cancer (IARC) and WHO
ADVANCES IN RADIATION TECHNOLOGIES IN THE TREATMENT OF CANCER Bro. Dr. Collie Miller IARC/WHO Based on trends in the incidence of cancer, the International Agency for Research on Cancer (IARC) and WHO
Specifics of treatment planning for active scanning and IMPT
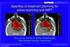 Specifics of treatment planning for active scanning and IMPT SFUD IMPT Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Treatment planning for scanning 1. Single Field,
Specifics of treatment planning for active scanning and IMPT SFUD IMPT Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Treatment planning for scanning 1. Single Field,
Use of Bubble Detectors to Characterize Neutron Dose Distribution in a Radiotherapy Treatment Room used for IMRT treatments
 Use of Bubble Detectors to Characterize Neutron Dose Distribution in a Radiotherapy Treatment Room used for IMRT treatments Alana Hudson *1 1 Tom Baker Cancer Centre, Department of Medical Physics, 1331
Use of Bubble Detectors to Characterize Neutron Dose Distribution in a Radiotherapy Treatment Room used for IMRT treatments Alana Hudson *1 1 Tom Baker Cancer Centre, Department of Medical Physics, 1331
Aspects of Industrialization of Accelerators for Particle Therapy ICABU, November 11, 2013, Daejeon
 Aspects of Industrialization of Accelerators for Particle Therapy ICABU, November 11, 2013, Daejeon Introduction Why Particle Therapy? PT Milestones What is meant by Industrialization Examples Protons-only:
Aspects of Industrialization of Accelerators for Particle Therapy ICABU, November 11, 2013, Daejeon Introduction Why Particle Therapy? PT Milestones What is meant by Industrialization Examples Protons-only:
ACCELERATORS FOR HADRONTHERAPY
 ACCELERATORS FOR HADRONTHERAPY Alberto Degiovanni CERN-BE IVICFA s Fridays: Medical Physics Valencia, 31.10.2014 Introduction: the icon of hadrontherapy Position of the Bragg peak depends on beam energy
ACCELERATORS FOR HADRONTHERAPY Alberto Degiovanni CERN-BE IVICFA s Fridays: Medical Physics Valencia, 31.10.2014 Introduction: the icon of hadrontherapy Position of the Bragg peak depends on beam energy
Medical Applications with Laser Plasma Accelerators
 Medical Applications with Laser Plasma Accelerators Victor Malka Laboratoire d Optique Appliquée ENSTA ParisTech Ecole Polytechnique ParisTech CNRS PALAISEAU, France victor.malka@ensta.fr Thanks to : J.
Medical Applications with Laser Plasma Accelerators Victor Malka Laboratoire d Optique Appliquée ENSTA ParisTech Ecole Polytechnique ParisTech CNRS PALAISEAU, France victor.malka@ensta.fr Thanks to : J.
IN VIVO IMAGING Proton Beam Range Verification With PET/CT
 IN VIVO IMAGING Proton Beam Range Verification With PET/CT Antje-Christin Knopf 1/3 K Parodi 2, H Paganetti 1, T Bortfeld 1 Siemens Medical Solutions Supports This Project 1 Department of Radiation Oncology,
IN VIVO IMAGING Proton Beam Range Verification With PET/CT Antje-Christin Knopf 1/3 K Parodi 2, H Paganetti 1, T Bortfeld 1 Siemens Medical Solutions Supports This Project 1 Department of Radiation Oncology,
Treatment Planning (Protons vs. Photons)
 Treatment Planning Treatment Planning (Protons vs. Photons) Acquisition of imaging data Delineation of regions of interest Selection of beam directions Dose calculation Optimization of the plan Hounsfield
Treatment Planning Treatment Planning (Protons vs. Photons) Acquisition of imaging data Delineation of regions of interest Selection of beam directions Dose calculation Optimization of the plan Hounsfield
Road Map for the development of hadron therapy and associated nuclear medicine methods at JINR:
 НТС ОЭЗ, 07 октября 2011 Road Map for the development of hadron therapy and associated nuclear medicine methods at JINR: Development of 3D conformal Proton therapy Design of various devices for proton
НТС ОЭЗ, 07 октября 2011 Road Map for the development of hadron therapy and associated nuclear medicine methods at JINR: Development of 3D conformal Proton therapy Design of various devices for proton
Discuss the general planning concepts used in proton planning. Review the unique handling of CTV / ITV / PTV when treating with protons
 Mark Pankuch, PhD Discuss the general planning concepts used in proton planning Review the unique handling of CTV / ITV / PTV when treating with protons Pencil Beam distributions and PBS optimization Cover
Mark Pankuch, PhD Discuss the general planning concepts used in proton planning Review the unique handling of CTV / ITV / PTV when treating with protons Pencil Beam distributions and PBS optimization Cover
PAMELA Particle Accelerator for MEdicaL Applications
 PAMELA Particle Accelerator for MEdicaL Applications Suzie Sheehy, DPhil candidate John Adams Institute for Accelerator Science Particle Physics, University of Oxford 1 Clinical Requirements Charged Particle
PAMELA Particle Accelerator for MEdicaL Applications Suzie Sheehy, DPhil candidate John Adams Institute for Accelerator Science Particle Physics, University of Oxford 1 Clinical Requirements Charged Particle
Radiotherapy. Marta Anguiano Millán. Departamento de Física Atómica, Molecular y Nuclear Facultad de Ciencias. Universidad de Granada
 Departamento de Física Atómica, Molecular y Nuclear Facultad de Ciencias. Universidad de Granada Overview Introduction Overview Introduction Brachytherapy Radioisotopes in contact with the tumor Overview
Departamento de Física Atómica, Molecular y Nuclear Facultad de Ciencias. Universidad de Granada Overview Introduction Overview Introduction Brachytherapy Radioisotopes in contact with the tumor Overview
Jefferies Healthcare Conference
 Jefferies Healthcare Conference Jean-Marc BOTHY - CSO June 8, 2017 2017 IBA SA Disclaimer This presentation may contain forward-looking statements concerning industry outlook, including growth drivers;
Jefferies Healthcare Conference Jean-Marc BOTHY - CSO June 8, 2017 2017 IBA SA Disclaimer This presentation may contain forward-looking statements concerning industry outlook, including growth drivers;
Radiation qualities in carbon-ion radiotherapy at NIRS/HIMAC
 Radiation qualities in carbon-ion radiotherapy at NIRS/ Shunsuke YONAI Radiological Protection Section Research Center for Charged Particle Therapy National Institute of Radiological Sciences (NIRS) E-mail:
Radiation qualities in carbon-ion radiotherapy at NIRS/ Shunsuke YONAI Radiological Protection Section Research Center for Charged Particle Therapy National Institute of Radiological Sciences (NIRS) E-mail:
Sarcoma and Radiation Therapy. Gabrielle M Kane MB BCh EdD FRCPC Muir Professorship in Radiation Oncology University of Washington
 Sarcoma and Radiation Therapy Gabrielle M Kane MB BCh EdD FRCPC Muir Professorship in Radiation Oncology University of Washington Objective: Helping you make informed decisions Introduction Process Radiation
Sarcoma and Radiation Therapy Gabrielle M Kane MB BCh EdD FRCPC Muir Professorship in Radiation Oncology University of Washington Objective: Helping you make informed decisions Introduction Process Radiation
Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy
 Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy C. Talamonti M. Bruzzi,M. Bucciolini, L. Marrazzo, D. Menichelli University of
Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy C. Talamonti M. Bruzzi,M. Bucciolini, L. Marrazzo, D. Menichelli University of
MEDICAL MANAGEMENT POLICY
 PAGE: 1 of 8 This medical policy is not a guarantee of benefits or coverage, nor should it be deemed as medical advice. In the event of any conflict concerning benefit coverage, the employer/member summary
PAGE: 1 of 8 This medical policy is not a guarantee of benefits or coverage, nor should it be deemed as medical advice. In the event of any conflict concerning benefit coverage, the employer/member summary
PRESCRIBING RECORDING AND REPORTING PROTON BEAM THERAPY ICRU 78. RAJESH THIYAGARAJAN Senior Medical Physicist & RSO Medanta The Medicity
 PRESCRIBING RECORDING AND REPORTING PROTON BEAM THERAPY ICRU 78 RAJESH THIYAGARAJAN Senior Medical Physicist & RSO Medanta The Medicity HISTORY OF PROTON THERAPY Robert Wilson proposed the use of proton
PRESCRIBING RECORDING AND REPORTING PROTON BEAM THERAPY ICRU 78 RAJESH THIYAGARAJAN Senior Medical Physicist & RSO Medanta The Medicity HISTORY OF PROTON THERAPY Robert Wilson proposed the use of proton
Advances in external beam radiotherapy
 International Conference on Modern Radiotherapy: Advances and Challenges in Radiation Protection of Patients Advances in external beam radiotherapy New techniques, new benefits and new risks Michael Brada
International Conference on Modern Radiotherapy: Advances and Challenges in Radiation Protection of Patients Advances in external beam radiotherapy New techniques, new benefits and new risks Michael Brada
Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy
 Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy C. Talamonti a*, M. Bucciolini a, L. Marrazzo a, D. Menichelli a. a) Department
Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy C. Talamonti a*, M. Bucciolini a, L. Marrazzo a, D. Menichelli a. a) Department
Feasability of protontherapy with lasers plasma accelerators : the SAPHIR project
 Palaiseau - FRANCE Feasability of protontherapy with lasers plasma accelerators : the SAPHIR project Victor Malka victor.malka@ensta.fr 1 In collaboration with : A. Flacco, F. Sylla, A. Guemnie-Tafo Laboratoire
Palaiseau - FRANCE Feasability of protontherapy with lasers plasma accelerators : the SAPHIR project Victor Malka victor.malka@ensta.fr 1 In collaboration with : A. Flacco, F. Sylla, A. Guemnie-Tafo Laboratoire
6/29/2012 WHAT IS IN THIS PRESENTATION? MANAGEMENT OF PRIMARY DEVICES INVESTIGATED MAJOR ISSUES WITH CARDIAC DEVICES AND FROM MED PHYS LISTSERVS
 6/29/2012 MANAGEMENT OF RADIOTHERAPY PATIENTS WITH IMPLANTED CARDIAC DEVICES Dimitris Mihailidis, PhD., Charleston Radiation Therapy Consultants Charleston, WV 25304 WHAT IS IN THIS PRESENTATION? Types
6/29/2012 MANAGEMENT OF RADIOTHERAPY PATIENTS WITH IMPLANTED CARDIAC DEVICES Dimitris Mihailidis, PhD., Charleston Radiation Therapy Consultants Charleston, WV 25304 WHAT IS IN THIS PRESENTATION? Types
The Heidelberg Ion Therapy Center and PARTNER. Thomas Haberer Heidelberg Ion Therapy Center
 The Heidelberg Ion Therapy Center and PARTNER Thomas Haberer Heidelberg Ion Therapy Center Goal The key element to improve the clinical outcome is local control! entrance channel: low physical dose low
The Heidelberg Ion Therapy Center and PARTNER Thomas Haberer Heidelberg Ion Therapy Center Goal The key element to improve the clinical outcome is local control! entrance channel: low physical dose low
Elekta Synergy Digital accelerator for advanced IGRT
 Elekta Synergy Digital accelerator for advanced IGRT Setting the standard for confident care The Field of Radiation Therapy is Constantly Changing Being able to take full advantage of the latest clinical
Elekta Synergy Digital accelerator for advanced IGRT Setting the standard for confident care The Field of Radiation Therapy is Constantly Changing Being able to take full advantage of the latest clinical
HEALTH RISKS FROM EXPOSURE TO FAST NEUTRONS. Prof. Marco Durante
 HEALTH RISKS FROM EXPOSURE TO FAST NEUTRONS Prof. Marco Durante Risk from neutrons Risk from exposure to fission spectrum neutrons has been extensively studied in the 60 s at nuclear reactors using animal
HEALTH RISKS FROM EXPOSURE TO FAST NEUTRONS Prof. Marco Durante Risk from neutrons Risk from exposure to fission spectrum neutrons has been extensively studied in the 60 s at nuclear reactors using animal
Nuclear Data for Radiation Therapy
 Symposium on Nuclear Data 2004 Nov. 12, 2004 @ JAERI, Tokai Nuclear Data for Radiation Therapy ~from macroscopic to microscopic~ Naruhiro Matsufuji, Yuki Kase and Tatsuaki Kanai National Institute of Radiological
Symposium on Nuclear Data 2004 Nov. 12, 2004 @ JAERI, Tokai Nuclear Data for Radiation Therapy ~from macroscopic to microscopic~ Naruhiro Matsufuji, Yuki Kase and Tatsuaki Kanai National Institute of Radiological
Workshop on Hadron Beam Therapy of Cancer Erice, Sicily April 24-May
 IONTRIS Synchrotron based PT Solutions from Siemens AG Workshop on Hadron Beam Therapy of Cancer Erice, Sicily April 24-May 1 2009 Matthias Herforth VP Business Development and Communications Siemens AG
IONTRIS Synchrotron based PT Solutions from Siemens AG Workshop on Hadron Beam Therapy of Cancer Erice, Sicily April 24-May 1 2009 Matthias Herforth VP Business Development and Communications Siemens AG
Production and dosimetry of simultaneous therapeutic photons and electrons beam by linear accelerator: a monte carlo study
 Production and dosimetry of simultaneous therapeutic photons and electrons beam by linear accelerator: a monte carlo study Navid Khledi 1, Azim Arbabi 2, Dariush Sardari 1, Mohammad Mohammadi 3, Ahmad
Production and dosimetry of simultaneous therapeutic photons and electrons beam by linear accelerator: a monte carlo study Navid Khledi 1, Azim Arbabi 2, Dariush Sardari 1, Mohammad Mohammadi 3, Ahmad
CHARACTERIZATION OF THE ELECTRON BEAM RADIATION FIELD BY CHEMICAL DOSIMETRY
 CHARACTERIZATION OF THE ELECTRON BEAM RADIATION FIELD BY CHEMICAL DOSIMETRY M. R. NEMTANU, C. OPROIU, M. BRASOVEANU, M. OANE National Institute for Laser, Plasma and Radiation Physics, Electron Accelerator
CHARACTERIZATION OF THE ELECTRON BEAM RADIATION FIELD BY CHEMICAL DOSIMETRY M. R. NEMTANU, C. OPROIU, M. BRASOVEANU, M. OANE National Institute for Laser, Plasma and Radiation Physics, Electron Accelerator
Medical Use of Radioisotopes
 Medical Use of Radioisotopes Therapy Radioisotopes prove to be useful in the application of brachytherapy, the procedure for using temporary irradiation close to the area of disease (i.e. cancer) 10% Medical
Medical Use of Radioisotopes Therapy Radioisotopes prove to be useful in the application of brachytherapy, the procedure for using temporary irradiation close to the area of disease (i.e. cancer) 10% Medical
I. Equipments for external beam radiotherapy
 I. Equipments for external beam radiotherapy 5 linear accelerators (LINACs): Varian TrueBeam 6, 10 & 18 MV photons, 6-18 MeV electrons, image-guided (IGRT) and intensity modulated radiotherapy (IMRT),
I. Equipments for external beam radiotherapy 5 linear accelerators (LINACs): Varian TrueBeam 6, 10 & 18 MV photons, 6-18 MeV electrons, image-guided (IGRT) and intensity modulated radiotherapy (IMRT),
Clinical Quality Assurance for Particle Therapy Plus ça même Plus
 Clinical Quality Assurance for Particle Therapy Plus ça même Plus Thomas F. DeLaney, MD Medical Director Francis H. Burr Proton Center Massachusetts General Hospital Boston MA Quality Assurance Designed
Clinical Quality Assurance for Particle Therapy Plus ça même Plus Thomas F. DeLaney, MD Medical Director Francis H. Burr Proton Center Massachusetts General Hospital Boston MA Quality Assurance Designed
Ion Beam Therapy should we prioritise research on helium beams?
 Ion Beam Therapy should we prioritise research on helium beams? Stuart Green Medical Physics University Hospital Birmingham NHS Trust Follow-up from the EUCARD2 workshop, ION Beam Therapy: Clinical, Scientific
Ion Beam Therapy should we prioritise research on helium beams? Stuart Green Medical Physics University Hospital Birmingham NHS Trust Follow-up from the EUCARD2 workshop, ION Beam Therapy: Clinical, Scientific
COMPARISON OF RADIOBIOLOGICAL EFFECTS OF CARBON IONS TO PROTONS ON A RESISTANT HUMAN MELANOMA CELL LINE
 COMPARISON OF RADIOBIOLOGICAL EFFECTS OF CARBON IONS TO PROTONS ON A RESISTANT HUMAN MELANOMA CELL LINE I. Petrovi a, A. Risti -Fira a, L. Kori anac a, J. Požega a, F. Di Rosa b, P. Cirrone b and G. Cuttone
COMPARISON OF RADIOBIOLOGICAL EFFECTS OF CARBON IONS TO PROTONS ON A RESISTANT HUMAN MELANOMA CELL LINE I. Petrovi a, A. Risti -Fira a, L. Kori anac a, J. Požega a, F. Di Rosa b, P. Cirrone b and G. Cuttone
TomoTherapy. Michelle Roach CNC Radiation Oncology Liverpool Hospital CNSA. May 2016
 TomoTherapy Michelle Roach CNC Radiation Oncology Liverpool Hospital CNSA May 2016 TomoTherapy The Facts Greek Tomo = slice Advanced form of IMRT 3D computerised tomography (CT) imaging immediately prior
TomoTherapy Michelle Roach CNC Radiation Oncology Liverpool Hospital CNSA May 2016 TomoTherapy The Facts Greek Tomo = slice Advanced form of IMRT 3D computerised tomography (CT) imaging immediately prior
A Patient s Guide to SRS
 A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
Proton Therapy Market Outlook - Global Analysis
 Proton Therapy Market Outlook - Global Analysis Proton Therapy Market Outlook - Global Analysis BioPortfolio has been marketing business and market research reports from selected publishers for over fifteen
Proton Therapy Market Outlook - Global Analysis Proton Therapy Market Outlook - Global Analysis BioPortfolio has been marketing business and market research reports from selected publishers for over fifteen
Hampton University Proton Therapy Institute
 Hampton University Proton Therapy Institute Brief introduction to proton therapy technology, its advances and Hampton University Proton Therapy Institute Vahagn Nazaryan, Ph.D. Executive Director, HUPTI
Hampton University Proton Therapy Institute Brief introduction to proton therapy technology, its advances and Hampton University Proton Therapy Institute Vahagn Nazaryan, Ph.D. Executive Director, HUPTI
Spatially Fractionated Radiation Therapy: GRID Sponsored by.decimal Friday, August 22, Pamela Myers, Ph.D.
 Spatially Fractionated Radiation Therapy: GRID Sponsored by.decimal Friday, August 22, 2014 Pamela Myers, Ph.D. Introduction o o o o o Outline GRID compensator Purpose of SFRT/GRID therapy Fractionation
Spatially Fractionated Radiation Therapy: GRID Sponsored by.decimal Friday, August 22, 2014 Pamela Myers, Ph.D. Introduction o o o o o Outline GRID compensator Purpose of SFRT/GRID therapy Fractionation
Mitsubishi Heavy Industries Technical Review Vol. 51 No. 1 (March 2014)
 The Challenge of Innovative Cancer Treatments Enabled by Vero4DRT -Development of High-precision Dose Delivery Features for Reducing Radiation Exposure of Healthy Tissue- 76 YASUNOBU SUZUKI *1 KUNIO TAKAHASHI
The Challenge of Innovative Cancer Treatments Enabled by Vero4DRT -Development of High-precision Dose Delivery Features for Reducing Radiation Exposure of Healthy Tissue- 76 YASUNOBU SUZUKI *1 KUNIO TAKAHASHI
FROM ICARO1 TO ICARO2: THE MEDICAL PHYSICS PERSPECTIVE. Geoffrey S. Ibbott, Ph.D. June 20, 2017
 FROM ICARO1 TO ICARO2: THE MEDICAL PHYSICS PERSPECTIVE Geoffrey S. Ibbott, Ph.D. June 20, 2017 1 DISCLOSURES My institution holds Strategic Partnership Research Agreements with Varian, Elekta, and Philips
FROM ICARO1 TO ICARO2: THE MEDICAL PHYSICS PERSPECTIVE Geoffrey S. Ibbott, Ph.D. June 20, 2017 1 DISCLOSURES My institution holds Strategic Partnership Research Agreements with Varian, Elekta, and Philips
Efficient Dosimetry for Proton Therapy
 Efficient Dosimetry for Proton Therapy Why IBA Dosimetry? IBA Dosimetry offers the full product range tailored to fit any Proton Therapy QA needs. PT treatment safety, as well as most efficient dosimetry
Efficient Dosimetry for Proton Therapy Why IBA Dosimetry? IBA Dosimetry offers the full product range tailored to fit any Proton Therapy QA needs. PT treatment safety, as well as most efficient dosimetry
Modelling the induction of cell death and chromosome damage by therapeutic protons
 Modelling the induction of cell death and chromosome damage by therapeutic protons M.P. Carante 1,2 and F. Ballarini 1,2, * 1 University of Pavia, Physics Department, Pavia, Italy 2 INFN, Sezione di Pavia,
Modelling the induction of cell death and chromosome damage by therapeutic protons M.P. Carante 1,2 and F. Ballarini 1,2, * 1 University of Pavia, Physics Department, Pavia, Italy 2 INFN, Sezione di Pavia,
Firing Protons at Lesions
 Visionaries 2014 Firing Protons at Lesions Molecular Tracking Proton Beam Therapy System at Hokkaido University Radiotherapy is widely used as a treatment for cancer (malignant tumors) that has minimal
Visionaries 2014 Firing Protons at Lesions Molecular Tracking Proton Beam Therapy System at Hokkaido University Radiotherapy is widely used as a treatment for cancer (malignant tumors) that has minimal
Review of Heavy Ion Accelerators for Hadrontherapy
 Review of Heavy Ion Accelerators for Hadrontherapy Koji Noda Research Center for Charged Particle Therapy National Institute of Radiological Sciences 11 th Int l Conf. on Heavy Ion Accelerator Technology,
Review of Heavy Ion Accelerators for Hadrontherapy Koji Noda Research Center for Charged Particle Therapy National Institute of Radiological Sciences 11 th Int l Conf. on Heavy Ion Accelerator Technology,
Elekta - a partner and world-leading supplier
 Experience Elekta Elekta - a partner and world-leading supplier of clinical solutions for image guided radiation therapy, stereotactic radiotherapy, radiosurgery and brachytherapy, as well as advanced
Experience Elekta Elekta - a partner and world-leading supplier of clinical solutions for image guided radiation therapy, stereotactic radiotherapy, radiosurgery and brachytherapy, as well as advanced
Amendment No. 2. Item No. 2 (Rfx/ Event number )
 Amendment 2 Sub: Amendment to the Document 06.12.2018 Ref.: Notice Inviting Bid ref. HITES/PCD/NCI-AIIMS/36/18-19 dated 26.09.2018 read with its Amendment no. 1 dated 19.11.18 The following changes have
Amendment 2 Sub: Amendment to the Document 06.12.2018 Ref.: Notice Inviting Bid ref. HITES/PCD/NCI-AIIMS/36/18-19 dated 26.09.2018 read with its Amendment no. 1 dated 19.11.18 The following changes have
Protons Monte Carlo water-equivalence study of two PRESAGE formulations for proton beam dosimetry J. Phys.: Conf. Ser.
 Protons Monte Carlo water-equivalence study of two PRESAGE formulations for proton beam dosimetry T Gorjiara, Z Kuncic, J Adamovics and C Baldock 2013 J. Phys.: Conf. Ser. 444 012090 PRESAGE is a radiochromic
Protons Monte Carlo water-equivalence study of two PRESAGE formulations for proton beam dosimetry T Gorjiara, Z Kuncic, J Adamovics and C Baldock 2013 J. Phys.: Conf. Ser. 444 012090 PRESAGE is a radiochromic
Simulating Potential Layouts for a Proton Therapy Treatment Center
 Simulating Potential Layouts for a Proton Therapy Treatment Center Stuart Price-University of Maryland Bruce Golden- University of Maryland Edward Wasil- American University Howard Zhang- University of
Simulating Potential Layouts for a Proton Therapy Treatment Center Stuart Price-University of Maryland Bruce Golden- University of Maryland Edward Wasil- American University Howard Zhang- University of
The Economic Club of Florida Tallahassee August 13, 2018 Nancy P Mendenhall, MD. The Promise of Protons
 The Economic Club of Florida Tallahassee August 13, 2018 Nancy P Mendenhall, MD The Promise of Protons The Promise of Protons Cancer and radiation therapy The promise of protons UFHPTI: missions and operation
The Economic Club of Florida Tallahassee August 13, 2018 Nancy P Mendenhall, MD The Promise of Protons The Promise of Protons Cancer and radiation therapy The promise of protons UFHPTI: missions and operation
Proton Stereotactic Radiotherapy: Clinical Overview. Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS
 Proton Stereotactic Radiotherapy: Clinical Overview Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS Acknowledgements Radiation Oncologists and Physicists at various institutions (MGH, MDACC,
Proton Stereotactic Radiotherapy: Clinical Overview Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS Acknowledgements Radiation Oncologists and Physicists at various institutions (MGH, MDACC,
